Bilateral Pulmonary Embolism in a 12-Year-Old Girl with Steroid-Resistant Nephrotic Syndrome
Abstract
1. Introduction
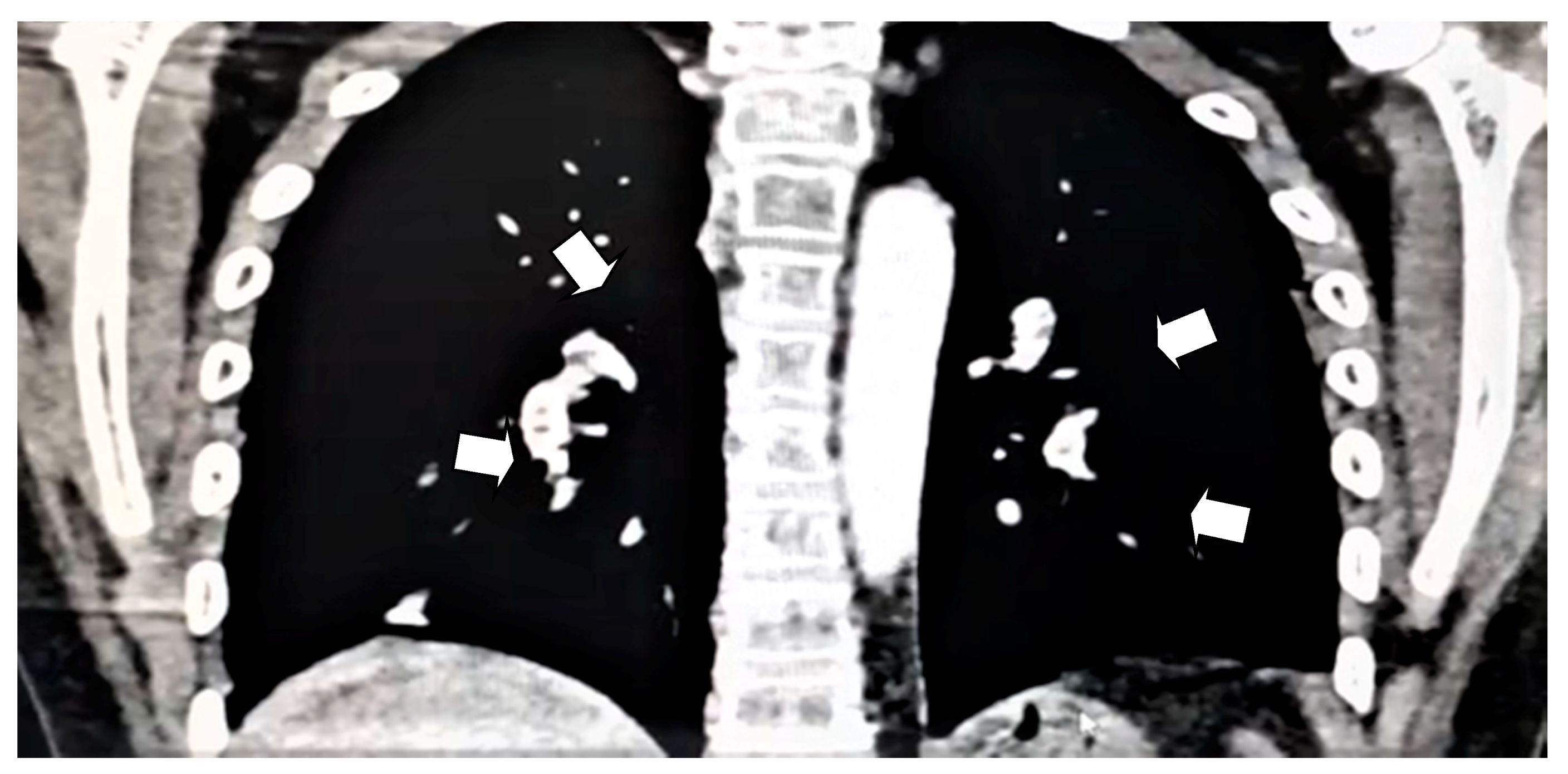
2. Case Presentation
3. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Mirrakhimov, A.E.; Ali, A.M.; Barbaryan, A.; Prueksaritanond, S.; Hussain, N. Primary nephrotic syndrome in adults as a risk factor for pulmonary embolism: An up-to-date review of the literature. Int. J. Nephrol. 2014, 2014, 916760. [Google Scholar] [CrossRef] [PubMed]
- Gigante, A.; Barbano, B.; Sardo, L.; Martina, P.; Gasperini, M.L.; Labbadia, R.; Liberatori, M.; Amoroso, A.; Cianci, R. Hypercoagulability and nephrotic syndrome. Curr. Vasc. Pharmacol. 2014, 12, 512–517. [Google Scholar] [CrossRef] [PubMed]
- Fahal, I.H.; McClelland, P.; Hay, C.R.; Bell, G.M. Arterial thrombosis in the nephrotic syndrome. Postgrad. Med. J. 1994, 70, 905–909. [Google Scholar] [CrossRef] [PubMed]
- Kerlin, B.A.; Ayoob, R.; Smoyer, W.E. Epidemiology and pathophysiology of nephrotic syndrome—Associated thromboembolic disease. Clin. J. Am. Soc. Nephrol. 2012, 7, 513–520. [Google Scholar] [CrossRef]
- Song, Z.; Wu, H.; Cao, H.; Tang, M.; Yang, S.; Qin, L. Nephrotic syndrome with acute pulmonary embolism in young adults: Two case reports. Medicine 2018, 97, 29. [Google Scholar] [CrossRef]
- Zhang, L.J.; Zhang, Z.; Li, S.J.; Meinel, F.G.; Nance, J.W., Jr.; Zhou, C.S. Pulmonary embolism and renal vein thrombosis in patients with nephrotic syndrome: Prospective evaluation of prevalence and risk factors with CT. Radiology 2014, 273, 897–906. [Google Scholar] [CrossRef]
- Mahmoodi, B.K.; ten Kate, M.K.; Waanders, F.; Veeger, N.J.; Brouwer, J.L.; Vogt, L.; Navis, G.; van der Meer, J. High absolute riskand predictors of venous and arterial thromboembolic events in patients with nephrotic syndrome: Results from a large retrospective cohort study. J. Vasc. Surg. 2008, 48, 1633. [Google Scholar] [CrossRef]
- Lilova, M.I.; Velkovski, I.G.; Topalov, I.B. Thromboembolic complications in children with nephrotic syndrome in Bulgaria (1974–1996). Pediatr. Nephrol. 2000, 15, 74–718. [Google Scholar] [CrossRef]
- Skrzypczyk, P.; Mizerska-Wasiak, M.; Ofiara, A.; Szyszka, M.; Kułagowska, J.; Biejat, A. Pulmonary embolism in a girl with nephrotic syndrome and factor V Leiden-case report. Pol. Merkur. Lek. Organ Pol. Tow. Lek. 2018, 45, 114–118. [Google Scholar]
- Guenther, R.A.; Kemp, W.L. Delayed death due to saddle pulmonary thromboembolus in child with nephrotic syndrome induced by focal segmental glomerulosclerosis. Am. J. Forensic Med. Pathol. 2018, 39, 370–374. [Google Scholar] [CrossRef]
- McPheeters, R.A.; Purcell, T.B.; Snyder, D.L.; Peterson, R.T. Fatal pulmonary embolism in a 10-year old with nephrotic syndrome. Calif. J. Emerg. Med. 2003, 4, 36. [Google Scholar]
- Reid, C.J.D.; Segal, T. Pulmonary thrombo-embolism in nephrotic syndrome treated with tissue plasminogen activator. Eur. J. Pediatr 1997, 156, 647–649. [Google Scholar] [PubMed]
- Deshpande, P.V.; Griffiths, M. Pulmonary thrombosis in steroid-sensitive nephrotic syndrome. Pediatr. Nephrol. 2005, 20, 665–669. [Google Scholar] [CrossRef]
- Tetsuhara, K.; Tsuji, S.; Uematsu, S.; Kamei, K. Pulmonary embolism mimicking infectious pleuritis. Pediatr. Emerg. Care 2018, 34, e201–e203. [Google Scholar] [CrossRef]
- Apostol, E.L.; Kher, K.K. Cavitating pulmonary infarction in nephrotic syndrome. Pediatr. Nephrol. 1994, 8, 347–348. [Google Scholar] [PubMed]
- Kumar, M.; Malhotra, A.; Gupta, S.; Singh, R. Thromboembolic complications at the onset of nephrotic syndrome. Sudan. J. Paediatr. 2017, 17, 60. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Zimmerman, R.L.; Novek, S.; Chen, J.T.T.; Roggli, V. Pulmonary thrombosis in a 10-year-old child with minimal change disease and nephrotic syndrome: A clinical, radiologic, and pathologic correlation with literature review. Am. J. Clin. Pathol. 1994, 101, 230–236. [Google Scholar] [CrossRef] [PubMed]
- Janda, J.; Zábrodský, V.; Spatenka, J.; Tuma, S. Thrombosis of the inferior vena cava with successive lung embolization in a 15-year-old boy with nephrotic syndrome. Padiatr. Padol. 1986, 21, 69–74. [Google Scholar]
- Van Ommen, C.H.; Heyboer, H.; Groothoff, J.W.; Teeuw, R.; Aronson, D.C.; Peters, M. Persistent tachypnea in children: Keep pulmonary embolism in mind. J. Pediatr. Hematol. Oncol. 1998, 20, 570–573. [Google Scholar] [CrossRef]
- Mittal, B.R.; Singh, S.; Bhattacharya, A.; Prasad, V.; Singh, B. Lung scintigraphy in the diagnosis and follow-up of pulmonary thromboembolism in children with nephrotic syndrome. Clin. Imaging 2005, 29, 313–316. [Google Scholar] [CrossRef]
- Dabbous, M.K.; Sakr, F.R.; Malaeb, D.N. Anticoagulant therapy in pediatrics. J. Basic Clin. Pharm. 2014, 5, 27. [Google Scholar] [CrossRef] [PubMed]
- Jones, C.L.; Hébert, D. Pulmonary thrombo-embolism in the nephrotic syndrome. Pediatr. Nephrol. 1991, 5, 56–58. [Google Scholar] [CrossRef] [PubMed]
- Share, A.; Uzun, O.; Gibbs, J.L.; Blackburn, M.E.C. Prolonged local infusion of streptokinase in pulmonary artery thrombosis with nephrotic syndrome. Pediatr. Nephrol. 1996, 10, 734–736. [Google Scholar] [CrossRef] [PubMed]
- Ma, F.; Zhou, K.; Hua, Y.; Liu, X.; Duan, H.; Li, Y.; Wang, C. Chronic thromboembolic pulmonary hypertension as the first manifestation of nephrotic syndrome in a 12-year-old child. Medicine 2018, 97, e12349. [Google Scholar] [CrossRef] [PubMed]
- Sinha, I.; Klafkowski, G.; Harrington, B.; Minchom, P.; Judd, B. Pulmonary embolism in a 3-year-old boy with nephrotic syndrome. J. Radiol. Case Rep. 2007, 2, 87. [Google Scholar] [CrossRef]
- Costa, R.; Gomes, S.; Stone, R.; Ferreira, R. Pediatric pulmonary embolism and nephrotic syndrome. Port. J. Nephrol. Hypert. 2018, 32, 99–102. [Google Scholar]
- Madken, M.; Nagaraju, S.P.; Attur, R.P.; Vanalakunti, M. Pulmonary thromboembolism as first presentation of childhood membranous nephropathy. Saudi J. Kidney Dis Transpl. 2017, 28, 1192–1195. [Google Scholar] [CrossRef]
- Connor-Schuler, R.; Hrabec, D.; Corrales, J.P. Cardiac arrest from massive PE in nephrotic syndrome successfully treated with embolectomy and ECMO. Respir. Med. Case Rep. 2018, 24, 163–164. [Google Scholar] [CrossRef]
- Fung, L.S.; Klockau, C. Effects of age and weight-based dosing of enoxaparin on anti-factor xa levels in pediatric patients. J. Pediatr. Pharmacol. Ther. 2010, 15, 119–11925. [Google Scholar]
| Test Name | Result | Unit | Reference Range |
|---|---|---|---|
| White blood cell count | 13.86 | K/UL | 4.5–13.5 |
| Red blood cell count | 4.50 | M/UL | 4–5.40 |
| Hemoglobin | 12.6 | g/dL | 12–15 |
| Hematocrit | 37 | % | 35–49 |
| Mean cell volume | 84.0 | FL | 80–96 |
| Mean cell hemoglobin | 28.0 | Pg | 32–36 |
| Platelet count | 328 | K/UL | 150–450 |
| C-reactive protein | 3.13 | mg/L | 0–3 |
| Prothrombin time | 10.8 | s | 10–13 |
| Activated partial thrombin time | 45.4 | s | 25.1–36.5 |
| D-Dimer | 43.783 | mg/L | 0–0.5 |
| International Normalized Ratio | 0.96 | Ratio | 0.85–1.3 |
| Sodium | 137 | mmol/L | 136–145 |
| Potassium | 3.9 | mmol/L | 3.5–5.1 |
| Chloride | 106 | mmol/L | 98–107 |
| Urea | 4.7 | mmol/L | 2.5–6.4 |
| Creatinine | 22 | µmol/L | 53–115 |
| Total protein | 46 | g/L | 64–82 |
| Albumin | 5 | g/L | 40.2–47.6 |
| Alkaline phosphatase | 146 | U/L | 141–460 |
| Aspartate amino transferase | 16 | U/L | 15–37 |
| Alanine amino transferase | 18 | U/L | 12–78 |
| Gamma glutamyl transferase | 155 | U/L | 5–85 |
| Total bilirubin | 2 | U/L | 0–17 |
| Antinuclear antibody titer | 1:640 | Negative |
| Age (Years) | Underlining Disease | Presented Symptoms | Prompt Diagnosis of PE | Method of Diagnosis | Prompt Treatment of PE | Outcome | Reference |
|---|---|---|---|---|---|---|---|
| 17 | Factor V Leiden nephrotic syndrome | Respiratory tract infection with cough and back pain | Presumptive | Echocardiography | Yes | Improvement and disappearance of pain and cough (lived) | [9] |
| 10 | Focal segmental glomerulosclerosis nephrotic syndrome | Autopsy | Delayed death due to saddle pulmonary thromboembolism | [10] | |||
| 10 | Nephrotic syndrome | Shortness of breath | NO | Autopsy | NO | Died | [11] |
| 2.6 | Nephrotic syndrome | Pyrexia, vomiting, poor fluid intake, and poorly localized chest/abdominal pain | YES | Pulmonary angiography | YES | Resolved and lived | [12] |
| 12 | Nephrotic syndrome | Increasing weight, abdominal pain, and reduced urine output | YES | CTPA with contrast | YES | Resolved and lived | [13] |
| 12 | Nephrotic syndrome | Abdominal pain, edema, and diarrhea | YES | CTPA | YES | Resolved and lived | [13] |
| 14 | Nephrotic syndrome | Vomiting, watery diarrhea, abdominal pain, and chest pain. | YES | Contrast enhanced CT | YES | Resolved and lived | [14] |
| 6 | Nephrotic syndrome | Non-productive cough and dyspnea on exertion | NO | Autopsy | NO | Died | [15] |
| 5 | Nephrotic syndrome | Difficulty in breathing and decreased urine output | YES | CTPA | YES | Resolved and lived | [16] |
| 10 | Nephrotic syndrome | Sharp chest pain, dyspnea, and perioral cyanosis | NO | Autopsy | NO | Died | [17] |
| 15 | Nephrotic syndrome | Signs of complications | NO | Autopsy | NO | Died | [18] |
| 2 | Asthmatic bronchitis and nephrotic syndrome | Tachypnea Edema of eyelids and legs Ascites Hypertension | YES | Ventilation–perfusion lung scanning | YES | Resolved and lived | [19] |
| 2 | Nephrotic syndrome | Relapse and spontaneous bacterial peritonitis features | YES | Lung perfusion scan | YES | Resolution and lived | [20] |
| 4.5 | Nephrotic syndrome | Submandibular swelling, cough, abdominal distention | YES | Lung perfusion scan | YES | PE resolved but she died | [21] |
| 10.5 | Nephrotic syndrome | Mild right-sided pleuritic pain | YES | Radionuclide ventilation and perfusion scans | YES | Resolved and lived | [22] |
| 3 | Nephrotic Syndrome | Malaise, breathlessness, and tachycardia | YES | Pulmonary angiography | YES | Resolved and lived | [23] |
| 12 | Nephrotic Syndrome | Hemoptysis, cough, and shortness of breath | YES | Contrast enhanced CT | YES | Resolved and lived | [24] |
| 3 | Nephrotic syndrome | Mild respiratory distress | YES | Ventilation–perfusion lung scanning | YES | Resolved and lived | [25] |
| 10 | Nephrotic syndrome | Chest pain and shortness of breath | YES | CTPA | YES | Resolved and lived | [26] |
| 16 | Nephrotic syndrome | Severe left-sided chest pain and hemoptysis | YES | CTPA | YES | Resolved and lived | [27] |
| 20 | Nephrotic syndrome | Abdominal discomfort and fatigue | YES | CTPA | YES | Resolved and lived | [28] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Safdar, O.Y.; Rajab, R.H.; Alghanemi, R.G.; Tantawi, G.A.; Alsulami, N.A.; Alsayed, A.A.; Habiballah, A.K. Bilateral Pulmonary Embolism in a 12-Year-Old Girl with Steroid-Resistant Nephrotic Syndrome. Children 2020, 7, 62. https://doi.org/10.3390/children7060062
Safdar OY, Rajab RH, Alghanemi RG, Tantawi GA, Alsulami NA, Alsayed AA, Habiballah AK. Bilateral Pulmonary Embolism in a 12-Year-Old Girl with Steroid-Resistant Nephrotic Syndrome. Children. 2020; 7(6):62. https://doi.org/10.3390/children7060062
Chicago/Turabian StyleSafdar, Osama Y., Rahaf H. Rajab, Rand G. Alghanemi, Gazal A. Tantawi, Noora A. Alsulami, Aeshah A. Alsayed, and Abdullah K. Habiballah. 2020. "Bilateral Pulmonary Embolism in a 12-Year-Old Girl with Steroid-Resistant Nephrotic Syndrome" Children 7, no. 6: 62. https://doi.org/10.3390/children7060062
APA StyleSafdar, O. Y., Rajab, R. H., Alghanemi, R. G., Tantawi, G. A., Alsulami, N. A., Alsayed, A. A., & Habiballah, A. K. (2020). Bilateral Pulmonary Embolism in a 12-Year-Old Girl with Steroid-Resistant Nephrotic Syndrome. Children, 7(6), 62. https://doi.org/10.3390/children7060062




