Readiness to Change among Adolescents with Chronic Pain and Their Parents: Is the German Version of the Pain Stages of Change Questionnaire a Useful Tool?
Abstract
1. Introduction
2. Materials and Methods
2.1. Study 1
2.1.1. Participants, Setting and Procedure
2.1.2. Measures
2.1.3. Ethics
2.1.4. Statistical Analyses
2.2. Study 2
2.2.1. Participants and Procedure
2.2.2. Measures
2.2.3. Ethics
2.2.4. Statistical Analyses
3. Results
3.1. Study 1
3.1.1. Factor Structure Prior to Intake (Sample A)
3.1.2. Factor Structure at Admission to IIPT (Sample B)
3.2. Study 2
3.2.1. Factor Structure and Internal Consistency
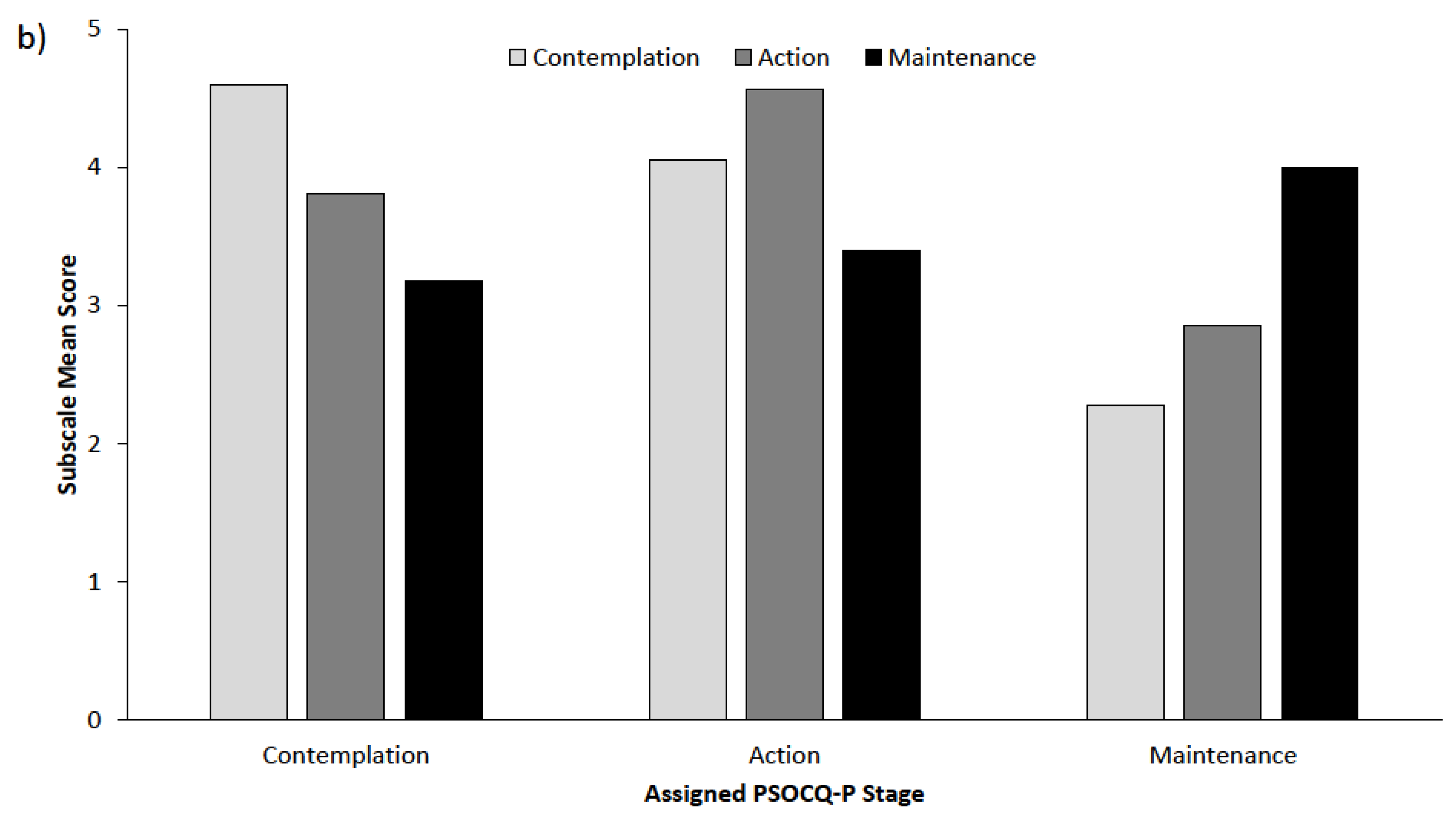
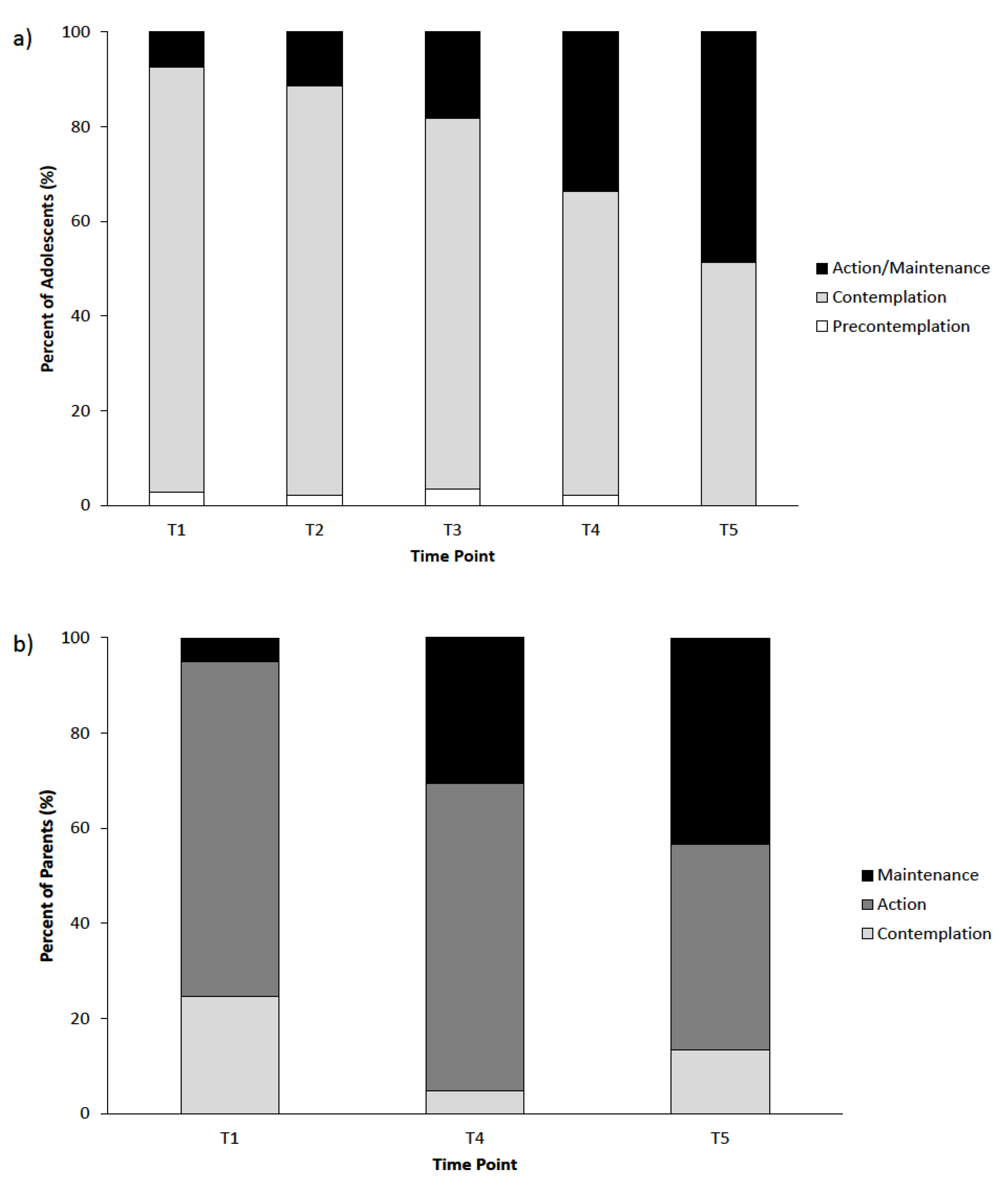
3.2.2. Stage Assignment and Sensitivity to Change
3.2.3. Concurrent Criterion Validity: Association of Stage of Change with Pain Characteristics
3.2.4. Predictive Criterion Validity: Association of Stage of Change with Non-Response to Treatment
4. Discussion
4.1. Clinical Implications
4.2. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Original Item Number | Item Description | Subscale |
|---|---|---|
| PSOCQ-A | ||
| 1 | Ich denke schon länger darüber nach, dass mein Umgang mit Schmerzen besser werden könnte. (I have been thinking that the way I cope with my pain could get better.) | Contemplation |
| 3 | Ich habe einige gute Strategien gelernt, damit mein Schmerzproblem nicht mein Leben beeinträchtigt. (I have learned some good ways to keep my pain problem from getting in the way of my life.) | Action/ Maintenance |
| 5 | Ich wende einige Strategien an, die mir helfen, im Alltag besser mit meinen Schmerzen umzugehen. (I am using some strategies that help me better deal with my pain on a day-to-day basis.) | Action/ Maintenance |
| 6 | Ich habe begonnen, Strategien zu entwickeln, um meine Schmerzen zu kontrollieren. (I have started to come up with strategies to help myself control my pain.) | Action/ Maintenance |
| 8 | Selbst wenn meine Schmerzen nicht vollständig weggehen, bin ich bereit, meinen Umgang mit den Schmerzen zu verändern. (Even if my pain doesn’t go away, I am ready to start changing how I deal with it.) | Contemplation |
| 9 | Ich weiß jetzt, dass es an der Zeit ist, einen besseren Umgang mit meinen Schmerzen zu entwickeln. (I realize now that it’s time for me to come up with a better plan to cope with my pain problem.) | Contemplation |
| 12 | Ich glaube, meine Schmerzen sind ein medizinisches Problem und ich sollte mich deshalb ausschließlich von Ärzten behandeln lassen. (My pain is a medical problem and I should be dealing with medical doctors about it.) | Precontemplation |
| 15 | Ich habe kürzlich erkannt, dass vor allem ich selber etwas für einen besseren Umgang mit meinen Schmerzen tun kann. (I have recently figured out that it’s up to me to deal better with my pain.) | Contemplation |
| 17 | Ich habe Schmerzbewältigungsstrategien entwickelt, die ich in meinem Alltag nutze. (I have built strategies for dealing with my pain into my everyday life.) | Action/ Maintenance |
| 18 | Ich habe große Fortschritte im Umgang mit meinen Schmerzen gemacht. (I have made a lot of progress in coping with my pain.) | Action/ Maintenance |
| 22 | Obwohl Ärzte mir etwas anderes sagen, denke ich noch immer, dass meine Schmerzen mit Hilfe einer Operation oder durch Medikamente verschwinden können. (I still think despite what doctors tell me, there must be some surgery or medicine that would get rid of my pain.) | Precontemplation |
| 27 | Ich probiere einige Bewältigungsstrategien aus, um meine Schmerzen besser in den Griff zu bekommen. (I am testing out some coping skills to manage my pain better.) | Action/ Maintenance |
| 29 | All das Gerede, wie man besser mit Schmerzen umgehen kann, ist für mich Zeitverschwendung. (All of this talk about how to cope better is a waste of my time.) | Precontemplation |
| PSOCQ-P | ||
| 2 | Ich ermutige mein Kind, neue Strategien im Umgang mit seinen/ihren Schmerzen zu entwickeln. (I am encouraging my child to develop new ways to cope with his/her pain.) | Action |
| 3 | Mein Kind hat einige gute Strategien gelernt, damit das Schmerzproblem nicht sein/ihr Leben beeinträchtigt. (My child has learned some good ways to keep his/her pain problem from interfering with life.) | Maintenance |
| 4 | Wenn Schmerzen auftreten, wendet mein Kind sofort Bewältigungsstrategien an, die ihm/ihr in der Vergangenheit geholfen haben, z.B. Entspannungsübungen oder Ablenkung. (When my child’s pain flares up, s/he is automatically using coping strategies that have worked in the past, such as a relaxation exercise or a mental distraction technique.) | Maintenance |
| 5 | Mein Kind wendet einige Strategien an, die ihm/ihr helfen, im Alltag besser mit den Schmerzen umzugehen. (My child is using some strategies that help him/her better deal with his/her pain problem on a day-to-day basis.) | Maintenance |
| 6 | Ich ermutige mein Kind, Strategien zu entwickeln, um seine/ihre Schmerzen zu kontrollieren. (I am encouraging my child to come up with strategies to help him/her control pain.) | Action |
| 9 | Ich weiß jetzt, dass es an der Zeit ist, einen besseren Umgang mit den Schmerzen meines Kindes zu entwickeln. (I realize now that it’s time to come up with a better plan to cope with my child’s pain problem.) | Contemplation |
| 10 | Mein Kind wendet das an, was er/sie gelernt hat, um die Schmerzen in den Griff zu bekommen. (My child uses what s/he has learned to help keep his/her pain under control.) | Maintenance |
| 13 | Mein Kind setzt aktuell einige Empfehlungen um, damit er/sie mit den Schmerzen leben kann. (My child is currently using some suggestions people have made about how to live with his/her pain problem.) | Maintenance |
| 14 | Seit Kurzem frage ich mich, ob mein Kind Hilfe benötigt, Strategien zu entwickeln, die ihm/ihr im Umgang mit den Schmerzen helfen. (I am beginning to wonder if my child needs to get some help to develop skills for dealing with his/her pain.) | Contemplation |
| 15 | Ich habe kürzlich erkannt, dass vor allem mein Kind selber etwas für einen besseren Umgang mit den Schmerzen tun kann. (I have recently figured out that it’s up to my child to deal better with his/her pain.) | Contemplation |
| 17 | Mein Kind hat Schmerzbewältigungsstrategien entwickelt, die er/sie im Alltag nutzen kann. (My child has incorporated strategies for dealing with pain into his/her everyday life.) | Maintenance |
| 18 | Mein Kind hat große Fortschritte im Umgang mit den Schmerzen gemacht. (My child has made a lot of progress in coping with his/her pain.) | Maintenance |
| 19 | Ich habe kürzlich erkannt, dass mein Kind den Umgang mit den Schmerzen verändern muss. (I have recently come to the conclusion that it’s time for my child to change how s/he copes with his/her pain.) | Contemplation |
| 20 | Ich ermutige mein Kind Unterstützung in Anspruch zu nehmen, um Strategien für einen besseren Umgang mit den Schmerzen zu erlernen. (I am encouraging my child to get help with learning some strategies for coping better with his/her pain.) | Action |
| 27 | Ich ermutige mein Kind, einige Bewältigungsstrategien auszuprobieren, um die Schmerzen besser in den Griff zu bekommen. (I am encouraging my child to test out some coping skills to manage his/her pain better.) | Action |
| 30 | Ich ermutige mein Kind andere Möglichkeiten als Medikamente und Operationen kennenzulernen, um die Schmerzen in den Griff zu bekommen. (I am encouraging my child to learn ways to control his/her pain other than with medications or surgery.) | Action |
References
- Stahlschmidt, L.; Zernikow, B.; Wager, J. Specialized Rehabilitation Programs for Children and Adolescents with Severe Disabling Chronic Pain: Indications, Treatment and Outcomes. Children 2016, 3, 33. [Google Scholar] [CrossRef] [PubMed]
- Guite, J.W.; Logan, D.E.; Simons, L.E.; Blood, E.A.; Kerns, R.D. Readiness to change in pediatric chronic pain: Initial validation of adolescent and parent versions of the Pain Stages of Change Questionnaire. Pain 2011, 152, 2301–2311. [Google Scholar] [CrossRef] [PubMed]
- Logan, D.E.; Conroy, C.; Sieberg, C.B.; Simons, L.E. Changes in willingness to self-manage pain among children and adolescents and their parents enrolled in an intensive interdisciplinary pediatric pain treatment program. Pain 2012, 153, 1863–1870. [Google Scholar] [CrossRef]
- Simons, L.E.; Sieberg, C.B.; Conroy, C.; Randall, E.T.; Shulman, J.; Borsook, D.; Berde, C.; Sethna, N.F.; Logan, D.E. Children With Chronic Pain: Response Trajectories After Intensive Pain Rehabilitation Treatment. J. Pain 2018, 19, 207–218. [Google Scholar] [CrossRef] [PubMed]
- Kerns, R.D.; Rosenberg, R. Predicting responses to self-management treatments for chronic pain: Application of the pain stages of change model. Pain 2000, 84, 49–55. [Google Scholar] [CrossRef]
- Jensen, M.P.; Nielson, W.R.; Turner, J.A.; Romano, J.M.; Hill, M.L. Changes in readiness to self-manage pain are associated with improvement in multidisciplinary pain treatment and pain coping. Pain 2004, 111, 84–95. [Google Scholar] [CrossRef]
- Kerns, R.D.; Rosenberg, R.; Jamison, R.N.; Caudill, M.A.; Haythornthwaite, J. Readiness to adopt a self-management approach to chronic pain: The Pain Stages of Change Questionnaire (PSOCQ). Pain 1997, 72, 227–234. [Google Scholar] [CrossRef]
- Prochaska, J.O.; Wright, J.A.; Velicer, W.F. Evaluating theories of health behavior change: A hierarchy of criteria applied to the transtheoretical model. Appl. Psychol. 2008, 57, 561–588. [Google Scholar] [CrossRef]
- Maurischat, C.; Härter, M.; Auclair, P.; Kerns, R.D.; Bengel, J. Preliminary validation of a German version of pain stages of change questionnaire. Eur. J. Pain 2002, 6, 43–48. [Google Scholar] [CrossRef]
- Maaßen, K.; Wager, J.; Hirschfeld, G.; Zernikow, B. Development and preliminary validation of the German Pain Stages of Change Questionnaire for adolescents. Schmerz (Berl. Ger.) 2015, 29, S75. [Google Scholar]
- Beaton, D.E.; Bombardier, C.; Guillemin, F.; Ferraz, M.B. Guidelines for the process of cross-cultural adaptation of self-report measures. Spine (Phila Pa 1976) 2000, 24, 3186–3191. [Google Scholar] [CrossRef] [PubMed]
- von Baeyer, C.L.; Spagrud, L.J.; McCormick, J.C.; Choo, E.; Neville, K.; Connelly, M.A. Three new datasets supporting use of the numerical rating scale (NRS-11) for children’s self-reports of pain intensity. Pain 2009, 143, 223–227. [Google Scholar] [CrossRef] [PubMed]
- Castarlenas, E.; Jensen, M.P.; von Baeyer, C.L.; Miró, J. Psychometric Properties of the Numerical Rating Scale to Assess Self-Reported Pain Intensity in Children and Adolescents: A Systematic Review. Clin. J. Pain 2017, 33, 376–383. [Google Scholar] [CrossRef]
- Tsze, D.S.; von Baeyer, C.L.; Pahalyants, V.; Dayan, P.S. Validity and reliability of the verbal numerical rating scale for children aged 4 to 17 years with acute pain. Ann. Emerg. Med. 2018, 71, 691–702. [Google Scholar] [CrossRef] [PubMed]
- Hübner, B.; Hechler, T.; Dobe, M.; Damschen, U.; Kosfelder, J.; Denecke, H.; Schroeder, S.; Zernikow, B. Pain-related disability in adolescents suffering from chronic pain: Preliminary examination of the Pediatric Pain Disability Index (P-PDI). Schmerz 2009, 23, 20–32. [Google Scholar] [CrossRef] [PubMed]
- Stahlschmidt, L.; Friedrich, Y.; Zernikow, B.; Wager, J. Assessment of pain-related disability in pediatric chronic pain: A comparison of the Functional Disability Inventory and the Paediatric Pain Disability Index. Clin. J. Pain 2018, 34, 1173–1179. [Google Scholar] [CrossRef] [PubMed]
- Schermelleh-Engel, K.; Moosbrugger, H.; Müller, H. Evaluating the fit of structural equation models: Tests of significance and descriptive goodness-of-fit measures. Methods Psychol. Res. Online 2003, 8, 23–74. [Google Scholar]
- Evans, J.R.; Mano, K.J.; Guite, J.W.; Weisman, S.J.; Hainsworth, K.R. Psychometric Properties of the Pain Stages of Change Questionnaire: New Insights on the Measurement of Readiness to Change in Adolescents, Mothers, and Fathers. J. Pain 2015, 16, 645–656. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Kosfelder, J.; Denecke, H.; Dobe, M.; Hübner, B.; Martin, A.; Menke, A.; Schroeder, S.; Marbach, S.; Zernikow, B. Pain-related coping strategies in children and adolescents with chronic pain. Validation of a German version of the Paediatric Pain Coping Inventory (PPCI revised). Schmerz 2008, 22, 442–457. [Google Scholar] [CrossRef]
- Wager, J.; Hechler, T.; Darlington, A.S.; Hirschfeld, G.; Vocks, S.; Zernikow, B. Classifying the severity of paediatric chronic pain - an application of the chronic pain grading. Eur. J. Pain 2013, 17, 1393–1402. [Google Scholar] [CrossRef]
- Stahlschmidt, L.; Barth, F.; Zernikow, B.; Wager, J. Therapy outcome one year after pediatric outpatient chronic pain evaluation: Chronic Pain Grading (CPG) for adolescent pain patients. Schmerz 2017, 31, 601–609. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Ruhe, A.; Schmidt, P.; Hirsch, J.; Wager, J.; Dobe, M.; Krummenauer, F.; Zernikow, B. Inpatient-based intensive interdisciplinary pain treatment for highly impaired children with severe chronic pain: Randomized controlled trial of efficacy and economic effects. Pain 2014, 155, 118–128. [Google Scholar] [CrossRef] [PubMed]
- Guite, J.W.; Kim, S.; Chen, C.-P.; Sherker, J.L.; Sherry, D.D.; Rose, J.B.; Hwang, W.-T. Pain beliefs and readiness to change among adolescents with chronic musculoskeletal pain and their parents before an initial pain clinic evaluation. Clin. J. Pain 2014, 30, 27–35. [Google Scholar] [CrossRef] [PubMed]
- Jensen, M.P.; Nielson, W.R.; Romano, J.M.; Hill, M.L.; Turner, J.A. Further evaluation of the pain stages of change questionnaire: Is the transtheoretical model of change useful for patients with chronic pain? Pain 2000, 86, 255–264. [Google Scholar] [CrossRef]
- Strong, J.; Westbury, K.; Smith, G.; McKenzie, I.; Ryan, W. Treatment outcome in individuals with chronic pain: Is the Pain Stages of Change Questionnaire (PSOCQ) a useful tool? Pain 2002, 97, 65–73. [Google Scholar] [CrossRef]
- Sherry, D.D.; Brake, L.; Tress, J.L.; Sherker, J.; Fash, K.; Ferry, K.; Weiss, P.F. The treatment of juvenile fibromyalgia with an intensive physical and psychosocial program. J. Pediatr. 2015, 167, 731–737. [Google Scholar] [CrossRef]

| Study 1 | Study 2 | ||
|---|---|---|---|
| Sample A (N = 501) a | Sample B (N = 240) a | (N = 150) a | |
| Demographics | |||
| Sex (female), N (%) | 353 (70.5) | 164 (68.3) | 105 (70.0) |
| Age (years), Mean (SD) | 14.4 (1.8) | 14.5 (1.8) | 14.4 (1.9) |
| Pain characteristics | |||
| Maximum pain intensity b, Mean (SD) | 8.2 (1.5) | 7.5 (1.9) | 8.3 (1.4) |
| Average pain intensity b, Mean (SD) | 6.5 (1.8) | 5.9 (2.1) | 6.0 (2.0) |
| Pain duration (months), Mean (SD) | 34.5 (37.9) | 40.6 (39.5) | 28.6 (28.2) |
| Pain-related school absence c, Mean (SD) | 2.9 (3.9) | 4.5 (6.7) | 3.9 (5.7) |
| Pain-related disability d, Mean (SD) | 36.1 (9.5) | 32.3 (9.3) | 34.8 (8.6) |
| Primary pain location | |||
| Head, N (%) | 254 (51.2) | 110 (47.0) | 64 (43.0) |
| Abdomen, N (%) | 74 (14.9) | 30 (12.8) | 22 (14.8) |
| Musculoskeletal system, N (%) | 107 (21.6) | 58 (24.8) | 38 (25.5) |
| Other, N (%) | 12 (2.4) | 7 (3.0) | 2 (1.3) |
| >1 primary pain location, N (%) | 49 (9.9) | 29 (12.4) | 23 (15.4) |
| χ2 | df | χ2/df a | CFI b | RMSEA c | SRMR d | |
|---|---|---|---|---|---|---|
| PSOCQ-A | ||||||
| Sample A | ||||||
| 4-factor model (P, C, A, M) | 1349.9 | 399 | 3.4 | 0.79 | 0.07 | 0.08 |
| 3-factor model (P, C, A/M) | 1394.4 | 402 | 3.5 | 0.79 | 0.07 | 0.08 |
| Sample B | ||||||
| 4-factor model (P, C, A, M) | 759.0 | 399 | 1.9 | 0.83 | 0.06 | 0.08 |
| 3-factor model (P, C, A/M) | 797.7 | 402 | 2.0 | 0.82 | 0.06 | 0.08 |
| 3-factor model short version (P, C, A/M) | 121.1 | 62 | 2.0 | 0.94 | 0.06 | 0.06 |
| PSOCQ-P | ||||||
| Sample A | ||||||
| 4-factor model (P, C, A, M) | 1232.8 | 399 | 3.1 | 0.76 | 0.07 | 0.08 |
| 3-factor model (P, C, A/M) | 1775.9 | 402 | 4.4 | 0.61 | 0.09 | 0.12 |
| Sample B | ||||||
| 4-factor model (P, C, A, M) | 790.1 | 399 | 2.0 | 0.80 | 0.07 | 0.08 |
| 3-factor model (P, C, A/M) | 1117.2 | 402 | 2.8 | 0.64 | 0.09 | 0.12 |
| 3-factor model short version (C, A, M) | 181.1 | 101 | 1.8 | 0.95 | 0.06 | 0.07 |
| Predictor | Odds Ratio | 95% CI | p |
|---|---|---|---|
| Adolescents (n = 108) | |||
| PSOCQ-A stage improved during treatment (T1–T4) | 0.70 | 0.25–1.98 | 0.501 |
| Per increase in stage of PSOCQ-A at T4 a | 0.66 | 0.26–1.66 | 0.379 |
| Parents (n = 103) | |||
| PSOCQ-P stage improved during treatment (T1–T4) | 0.62 | 0.23–1.65 | 0.336 |
| Per increase in stage of PSOCQ-P at T4 a | 1.10 | 0.47–2.60 | 0.828 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stahlschmidt, L.; Grothus, S.; Brown, D.; Zernikow, B.; Wager, J. Readiness to Change among Adolescents with Chronic Pain and Their Parents: Is the German Version of the Pain Stages of Change Questionnaire a Useful Tool? Children 2020, 7, 42. https://doi.org/10.3390/children7050042
Stahlschmidt L, Grothus S, Brown D, Zernikow B, Wager J. Readiness to Change among Adolescents with Chronic Pain and Their Parents: Is the German Version of the Pain Stages of Change Questionnaire a Useful Tool? Children. 2020; 7(5):42. https://doi.org/10.3390/children7050042
Chicago/Turabian StyleStahlschmidt, Lorin, Susanne Grothus, Donnamay Brown, Boris Zernikow, and Julia Wager. 2020. "Readiness to Change among Adolescents with Chronic Pain and Their Parents: Is the German Version of the Pain Stages of Change Questionnaire a Useful Tool?" Children 7, no. 5: 42. https://doi.org/10.3390/children7050042
APA StyleStahlschmidt, L., Grothus, S., Brown, D., Zernikow, B., & Wager, J. (2020). Readiness to Change among Adolescents with Chronic Pain and Their Parents: Is the German Version of the Pain Stages of Change Questionnaire a Useful Tool? Children, 7(5), 42. https://doi.org/10.3390/children7050042







