Development of the Mental Synthesis Evaluation Checklist (MSEC): A Parent-Report Tool for Mental Synthesis Ability Assessment in Children with Language Delay
Abstract
:1. Introduction
2. Phase I Instrument Development
2.1. Methods
2.1.1. Literature Review
2.1.2. Interviews with Key Opinion Leaders
2.1.3. Concept Elicitation
2.1.4. Cognitive Debriefing
2.2. Results
2.2.1. Literature Review and Interviews with Key Opinion Leaders
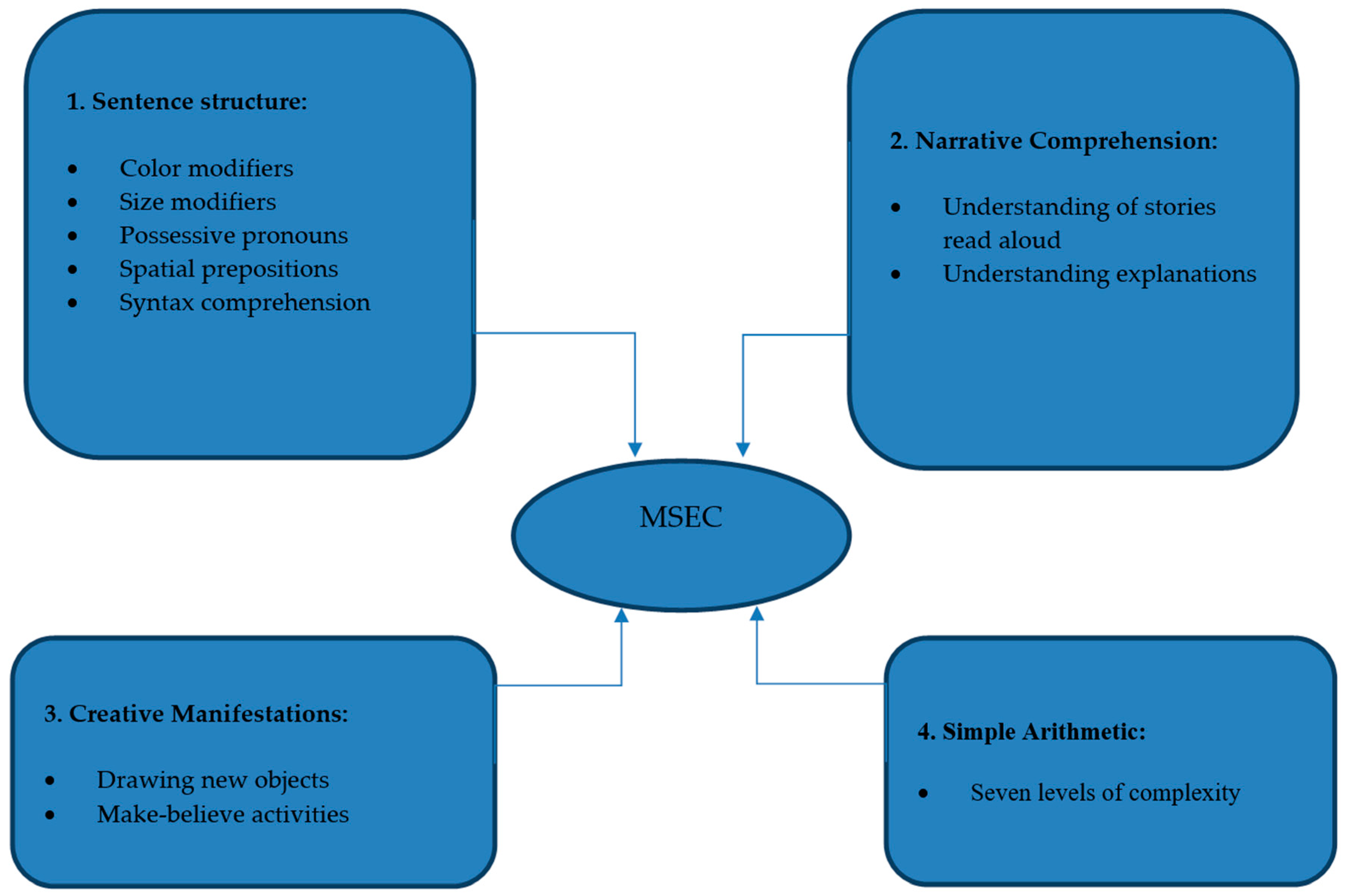
Sentence Structure: Understanding of Noun-Adjective Combinations, Spatial Prepositions, and Flexible Syntax
Narrative Comprehension: Understanding of Stories and Explanations
Creative Manifestations: Drawing and Make-Believe Activities
Simple Arithmetic: Number Manipulations with Increasing Complexity
2.2.2. Existing Assessment Instruments
2.2.3. Conceptual Framing
2.2.4. Concept Elicitation
2.2.5. Item Generation
2.2.6. Cognitive Debriefing
3. Phase II. Psychometric Validation
3.1. Methods
3.1.1. Data Collection
3.1.2. Participants
3.1.3. Measurements
3.2. Results
3.2.1. Reliability
3.2.2. Validity
4. Discussion
5. Compliance with Ethical Standards
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Vyshedskiy, A. Linguistically deprived children: Meta-analysis of published research underlines the importance of early syntactic language use for normal brain development. Res. Ideas Outcomes 2017, 3, e20696. [Google Scholar] [CrossRef]
- Vyshedskiy, A.; Dunn, R.; Piryatinsky, I. Neurobiological mechanisms for nonverbal IQ tests: Implications for instruction of nonverbal children with autism. Res. Ideas Outcomes 2017, 3, e13239. [Google Scholar] [CrossRef]
- Vyshedskiy, A.; Dunn, R. Mental synthesis involves the synchronization of independent neuronal ensembles. Res. Ideas Outcomes 2015, 1, e7642. [Google Scholar] [CrossRef]
- Braun, A.R.; Balkin, T.J.; Wesenten, N.J.; Carson, R.E.; Varga, M.; Baldwin, P.; Selbie, S.; Belenky, G.; Herscovitch, P. Regional cerebral blood flow throughout the sleep-wake cycle. Brain 1997, 20, 1173–1197. [Google Scholar] [CrossRef]
- Solms, M. The Neuropsychology of Dreams: A Clinico-Anatomical Study; L. Erlbaum: Mahwah, NJ, USA, 1997. [Google Scholar]
- Christoff, K.; Gabrieli, J.D. The frontopolar cortex and human cognition: Evidence for a rostrocaudal hierarchical organization within the human prefrontal cortex. Psychobiology 2000, 28, 168–186. [Google Scholar]
- Waltz, J.A.; Knowlton, B.J.; Holyoak, K.J.; Boone, K.B.; Mishkin, F.S.; de Menezes Santos, M.; Thomas, C.R.; Miller, B.L. A system for relational reasoning in human prefrontal cortex. Psychol. Sci. 1999, 10, 119–125. [Google Scholar] [CrossRef]
- Duncan, J.; Burgess, P.; Emslie, H. Fluid intelligence after frontal lobe lesions. Neuropsychologia 1995, 33, 261–268. [Google Scholar] [CrossRef]
- Luria, A.R. Higher Cortical Functions in Man; Springer Science & Business Media: Berlin, Germany, 2012. [Google Scholar]
- Fuster, J. The Prefrontal Cortex, 4th ed.; Academic Press: Cambridge, MA, USA, 2008. [Google Scholar]
- Baker, S.C.; Rogers, R.D.; Owen, A.M.; Frith, C.D.; Dolan, R.J.; Frackowiak, R.S.J.; Robbins, T.W. Neural systems engaged by planning: A PET study of the Tower of London task. Neuropsychologia 1996, 34, 515–526. [Google Scholar] [CrossRef]
- Gerbino, W.; Salmaso, D. The effect of amodal completion on visual matching. Acta Psychol. (Amst.) 1987, 65, 25–46. [Google Scholar] [CrossRef]
- Weigelt, S.; Singer, W.; Muckli, L. Separate cortical stages in amodal completion revealed by functional magnetic resonance adaptation. BMC Neurosci. 2007, 8, 70. [Google Scholar] [CrossRef] [PubMed]
- Salvi, C.; Bricolo, E.; Kounios, J.; Bowden, E.; Beeman, M. Insight solutions are correct more often than analytic solutions. Think. Reason 2016, 22, 443–460. [Google Scholar] [CrossRef] [PubMed]
- Halford, G.S. Can young children integrate premises in transitivity and serial order tasks? Cognit. Psychol. 1984, 16, 65–93. [Google Scholar] [CrossRef]
- Schreibman, L. Diagnostic features of autism. J. Child Neurol. 1988, 3, S57–S64. [Google Scholar] [CrossRef] [PubMed]
- Lovaas, O.I.; Koegel, R.L.; Schreibman, L. Stimulus overselectivity in autism: A review of research. Psychol. Bull. 1979, 86, 1236–1254. [Google Scholar] [CrossRef] [PubMed]
- Ploog, B.O. Stimulus overselectivity four decades later: A review of the literature and its implications for current research in autism spectrum disorder. J. Autism Dev. Disord. 2010, 40, 1332–1349. [Google Scholar] [CrossRef] [PubMed]
- Lovaas, O.I.; Schreibman, L.; Koegel, R.; Rehm, R. Selective responding by autistic children to multiple sensory input. J. Abnorm. Psychol. 1971, 77, 211. [Google Scholar] [CrossRef] [PubMed]
- Fombonne, E. Epidemiological surveys of autism and other pervasive developmental disorders: An update. J. Autism Dev. Disord. 2003, 33, 365–382. [Google Scholar] [CrossRef] [PubMed]
- Beglinger, L.J.; Smith, T.H. A review of subtyping in autism and proposed dimensional classification model. J. Autism Dev. Disord. 2001, 31, 411–422. [Google Scholar] [CrossRef] [PubMed]
- Boucher, J.; Mayes, A.; Bigham, S. Memory, Language and Intellectual Ability in Low-Functioning Autism; Memory in Autism; Boucher, J., Bowler, D.M., Eds.; Cambridge University Press: Cambridge, UK, 2008. [Google Scholar]
- Dawson, G.; Rogers, S.; Munson, J.; Smith, M.; Winter, J.; Greenson, J.; Donaldson, A.; Varley, J. Randomized, controlled trial of an intervention for toddlers with autism: The Early Start Denver Model. Pediatrics 2010, 125, e17–e23. [Google Scholar] [CrossRef] [PubMed]
- American Speech-Language-Hearing Association. Scope of Practice in Speech-Language Pathology; American Speech Language Hearing Association: Rockville, MD, USA, 2016. [Google Scholar]
- Axe, J.B. Conditional discrimination in the intraverbal relation: A review and recommendations for future research. Anal. Verbal Behav. 2008, 24, 159–174. [Google Scholar] [CrossRef] [PubMed]
- Michael, J.; Palmer, D.C.; Sundberg, M.L. The multiple control of verbal behavior. Anal. Verbal Behav. 2011, 27, 3–22. [Google Scholar] [CrossRef] [PubMed]
- Eikeseth, S.; Smith, D.P. An analysis of verbal stimulus control in intraverbal behavior: Implications for practice and applied research. Anal. Verbal Behav. 2013, 29, 125–135. [Google Scholar] [CrossRef] [PubMed]
- Lowenkron, B. Joint control and the selection of stimuli from their description. Anal. Verbal Behav. 2006, 22, 129–151. [Google Scholar] [CrossRef] [PubMed]
- Rimland, B.; Edelson, S.M. Autism Treatment Evaluation Checklist (ATEC); Autism Research Institute: San Diego, CA, USA, 1999. [Google Scholar]
- Dunn, R.; Elgart, J.; Lokshina, L.; Faisman, A.; Waslick, M.; Gankin, Y.; Vyshedskiy, A. Tablet-Based Cognitive Exercises as an Early Parent-Administered Intervention Tool for Toddlers with Autism—Evidence from a Field Study. Clin. Psychiatry 2017, 3. [Google Scholar] [CrossRef]
- Dunn, R.; Elgart, J.; Lokshina, L.; Faisman, A.; Khokhlovich, E.; Gankin, Y.; Vyshedskiy, A. Children with Autism Appear to Benefit from Parent-Administered Computerized Cognitive and Language Exercises Independent of the Child’s Age or Autism Severity. Autism Open Access 2017, 7. [Google Scholar] [CrossRef]
- Dunn, R.; Lokshina, L.; Faisman, A.; Elgart, J.; Khokhlovich, E.; Gankin, Y.; Vyshedskiy, A. Comparison of performance on verbal and nonverbal multiple-cue responding tasks in children with ASD. Autism Open Access 2017, 7, 218. [Google Scholar]
- Curtiss, S. Genie: A Psycholinguistic Study of a Modern-Day “Wild Child”; Academic Press: New York, NY, USA, 1977. [Google Scholar]
- Curtiss, S. The case of Chelsea: The effects of late age at exposure to language on language performance and evidence for the modularity of language and mind. UCLA Work. Pap. Linguist. 2014, 18, 115–146. [Google Scholar]
- Gabay, S.; Kalanthroff, E.; Henik, A.; Gronau, N. Conceptual size representation in ventral visual cortex. Neuropsychologia 2016, 81, 198–206. [Google Scholar] [CrossRef] [PubMed]
- Hauser, M.D.; Chomsky, N.; Fitch, W.T. The faculty of language: What is it, who has it, and how did it evolve? Science 2002, 298, 1569–1579. [Google Scholar] [CrossRef] [PubMed]
- Bickerton, D. Language and Species; University of Chicago Press: Chicago, IL, USA, 1992. [Google Scholar]
- Fortunato-Tavares, T.; Andrade, C.R.; Befi-Lopes, D.; Limongi, S.O.; Fernandes, F.D.; Schwartz, R.G. Syntactic comprehension and working memory in children with specific language impairment, autism or Down syndrome. Clin. Linguist. Phon. 2015, 29, 499–522. [Google Scholar] [CrossRef] [PubMed]
- Vyshedskiy, A. On the Origin of the Human Mind; MobileReference: Boston, MA, USA, 2014. [Google Scholar]
- Vygotsky, L.S. Play and its role in the mental development of the child. Translated by Catherine Mulholland from Voprosy psikhologii 1933. Sov. Psychol. 1967, 5, 6–18. [Google Scholar]
- Goldman, L.R. Child’s Play: Myth, Mimesis and Make-Believe; ERIC: Washington, DC, USA, 1998. [Google Scholar]
- Hauser, M.D.; Carey, S.; Hauser, L.B. Spontaneous number representation in semi–free–ranging rhesus monkeys. Proc. R. Soc. Lond. B Biol. Sci. 2000, 267, 829–833. [Google Scholar] [CrossRef] [PubMed]
- Dehaene, S. The Number Sense: How the Mind Creates Mathematics; OUP: Oxford, UK, 2011. [Google Scholar]
- Brown, L.; Sherbenou, R.J.; Johnsen, S.K. Test of Nonverbal Intelligence: TONI; Pro-Ed: Austin, TX, USA, 1982. [Google Scholar]
- Brown, L.; Sherbenou, R.J.; Johnsen, S.K. TONI-3, Test of Nonverbal Intelligence: A Language-Free Measure of Cognitive Ability; Pro-Ed: Austin, TX, USA, 1997. [Google Scholar]
- Raven, J.C. Mental Tests Used in Genetic Studies: The Performance of Related Individuals on Tests Mainly Educative and Mainly Reproductive. Master’s Thesis, University of London, London, UK, 1936. [Google Scholar]
- Raven, J. Manual for Raven’s Progressive Matrices and Vocabulary Scales Section 3: Standard Progressive Matrices: Introducing the Parallel and Plus Versions of the Tests; OPP: Oxford, UK, 2000. [Google Scholar]
- Wechsler, D. Wechsler Intelligence Scale for Children; Psychological Corporation: San Antonio, TX, USA, 1949. [Google Scholar]
- Klingberg, T.; O’Sullivan, B.T.; Roland, P.E. Bilateral activation of fronto-parietal networks by incrementing demand in a working memory task. Cereb. Cortex 1997, 7, 465–471. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.H.; Choi, Y.Y.; Gray, J.R.; Cho, S.H.; Chae, J.H.; Lee, S.; Kim, K. Neural correlates of superior intelligence: Stronger recruitment of posterior parietal cortex. Neuroimage 2006, 29, 578–586. [Google Scholar] [CrossRef] [PubMed]
- Braver, T.S.; Cohen, J.D.; Nystrom, L.E.; Jonides, J.; Smith, E.E.; Noll, D.C. A parametric study of prefrontal cortex involvement in human working memory. Neuroimage 1997, 5, 49–62. [Google Scholar] [CrossRef] [PubMed]
- Vyshedskiy, A.; Dunn, R. Mental Imagery Therapy for Autism (MITA)-An Early Intervention Computerized Brain Training Program for Children with ASD. Autism Open Access 2015, 5, 2. [Google Scholar]
- Al Backer, N.B. Correlation between Autism Treatment Evaluation Checklist (ATEC) and Childhood Autism Rating Scale (CARS) in the evaluation of autism spectrum disorder. Sudan. J. Paediatr. 2016, 16, 17. [Google Scholar] [PubMed]
- Geier, D.A.; Kern, J.K.; Geier, M.R. A comparison of the Autism Treatment Evaluation Checklist (ATEC) and the Childhood Autism Rating Scale (CARS) for the quantitative evaluation of autism. J. Ment. Health Res. Intellect. Disabil. 2013, 6, 255–267. [Google Scholar] [CrossRef] [PubMed]
- Jarusiewicz, B. Efficacy of Neurofeedback for Children in the Autistic Spectrum: A Pilot Study. J. Neurother. 2002, 6, 39–49. [Google Scholar] [CrossRef]
- Mahapatra, S.; Vyshedsky, D.; Martinez, S.; Kannel, B.; Braverman, J.; Edelson, S.M.; Vyshedskiy, A. Autism Treatment Evaluation Checklist (ATEC) norms: A “growth chart” for ATEC score changes as a function of age. Children 2018, 5, 25, accepted. [Google Scholar] [CrossRef] [PubMed]
- Mahapatra, S.; Khokhlovich, E.; Martinez, S.; Kannel, B.; Edelson, S.M.; Vyshedskiy, A. Epidemiological Study of Autism Subgroups Using Autism Treatment Evaluation Checklist (ATEC) Score. bioRxiv 2018. [Google Scholar] [CrossRef]
- Venkatesh, S.; Phung, D.; Duong, T.; Greenhill, S.; Adams, B. TOBY: Early intervention in autism through technology. In Proceedings of the SIGCHI Conference on Human Factors in Computing Systems, Paris, France, 27 April–2 May 2013; ACM: New York, NY, USA, 2013; pp. 3187–3196. [Google Scholar]
- Maljaars, J.; Noens, I.; Scholte, E.; van Berckelaer-Onnes, I. Language in low-functioning children with autistic disorder: Differences between receptive and expressive skills and concurrent predictors of language. J. Autism Dev. Disord. 2012, 42, 2181–2191. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hudry, K.; Leadbitter, K.; Temple, K.; Slonims, V.; McConachie, H.; Aldred, C.; Howlin, P.; Charman, T.; PACT Consortium. Preschoolers with autism show greater impairment in receptive compared with expressive language abilities. Int. J. Lang. Commun. Disord. 2010, 45, 681–690. [Google Scholar] [CrossRef] [PubMed]
- US Food and Drug Administration (FDA). Guidance for Industry: Patient-Reported Outcome Measures: Use in Medical Product Development to Support Labeling Claims; Department of Health and Human Services: Rockville, MD, USA, 2009.
| My Child | Domain of Mental Synthesis | |
|---|---|---|
| 1 | Understands some simple modifiers (i.e., green apple vs. red apple or big apple vs. small apple) | Sentence structure: understanding of noun-adjective combinations, spatial prepositions, and flexible syntax |
| 2 | Understands several modifiers in a sentence (i.e., small green apple) | |
| 3 | Understands size (can select the largest/smallest object out of a collection of objects) | |
| 4 | Understands possessive pronouns (i.e., your apple vs. her apple) | |
| 5 | Understands spatial prepositions (i.e., put the apple ON TOP of the box vs. INSIDE the box vs. BEHIND the box) | |
| 6 | Understands verb tenses (i.e., I will eat an apple vs. I ate an apple) | |
| 7 | Understands the change in meaning when the order of words is changed (i.e., understands the difference between “a cat ate a mouse" vs. “a mouse ate a cat”) | |
| 8 | Understands simple stories that are read aloud | Narrative comprehension: understanding of stories and explanations |
| 9 | Understands elaborate fairy tales that are read aloud (i.e., stories describing FANTASY creatures) | |
| 10 | Understands explanations about people, objects, or situations beyond the immediate surroundings (e.g., “Mom is walking the dog,” “The snow has turned to water”) | |
| 11 | Draws a VARIETY of RECOGNIZABLE images (objects, people, animals, etc.) | Creative manifestations: drawing and make-believe activities |
| 12 | Can draw a NOVEL image following YOUR description (e.g., a three-headed animal) | |
| 13 | Engages in a VARIETY of make-believe activities (such as: playing house, playing with toy soldiers, building forts, and castles, etc.) | |
| 14 | Understands NUMBERS (i.e., two apples vs. three apples) | Simple arithmetic: number manipulations with increasing complexity |
| 15 | Can perform simple arithmetic: 2 + 3 = ? | |
| 16 | Can add larger numbers: 7 + 6 = ? | |
| 17 | Can perform simple subtraction: 3 − 2 = ? | |
| 18 | Can subtract larger numbers: 15 − 7 = ? | |
| 19 | Can perform simple multiplication: 2 × 2 = ? | |
| 20 | Can multiply larger numbers: 6 × 7 = ? |
| ASD Severity | n (%) | MSEC | |
|---|---|---|---|
| Mean (SD) | Contrast F for Adjacent Groups | ||
| Mild | 636 (17%) | 24.89 (7.96) | 194.53 (Mild vs. Moderate; p < 0.001) |
| Moderate | 1586 (43%) | 30.23 (7.23) | 13.00 (Moderate vs. Severe; p < 0.001) |
| Severe | 1493 (40%) | 31.29 (9.10) | |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Braverman, J.; Dunn, R.; Vyshedskiy, A. Development of the Mental Synthesis Evaluation Checklist (MSEC): A Parent-Report Tool for Mental Synthesis Ability Assessment in Children with Language Delay. Children 2018, 5, 62. https://doi.org/10.3390/children5050062
Braverman J, Dunn R, Vyshedskiy A. Development of the Mental Synthesis Evaluation Checklist (MSEC): A Parent-Report Tool for Mental Synthesis Ability Assessment in Children with Language Delay. Children. 2018; 5(5):62. https://doi.org/10.3390/children5050062
Chicago/Turabian StyleBraverman, Julia, Rita Dunn, and Andrey Vyshedskiy. 2018. "Development of the Mental Synthesis Evaluation Checklist (MSEC): A Parent-Report Tool for Mental Synthesis Ability Assessment in Children with Language Delay" Children 5, no. 5: 62. https://doi.org/10.3390/children5050062
APA StyleBraverman, J., Dunn, R., & Vyshedskiy, A. (2018). Development of the Mental Synthesis Evaluation Checklist (MSEC): A Parent-Report Tool for Mental Synthesis Ability Assessment in Children with Language Delay. Children, 5(5), 62. https://doi.org/10.3390/children5050062






