Body Mass Index Changes from Before to 3 Years After the COVID-19 Lockdown: A Retrospective Longitudinal Study in a Single Elementary School
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Methods
2.3. Statistical Analyses
2.4. Ethical Statement
3. Results
3.1. Clinical Characteristics of the Study Population
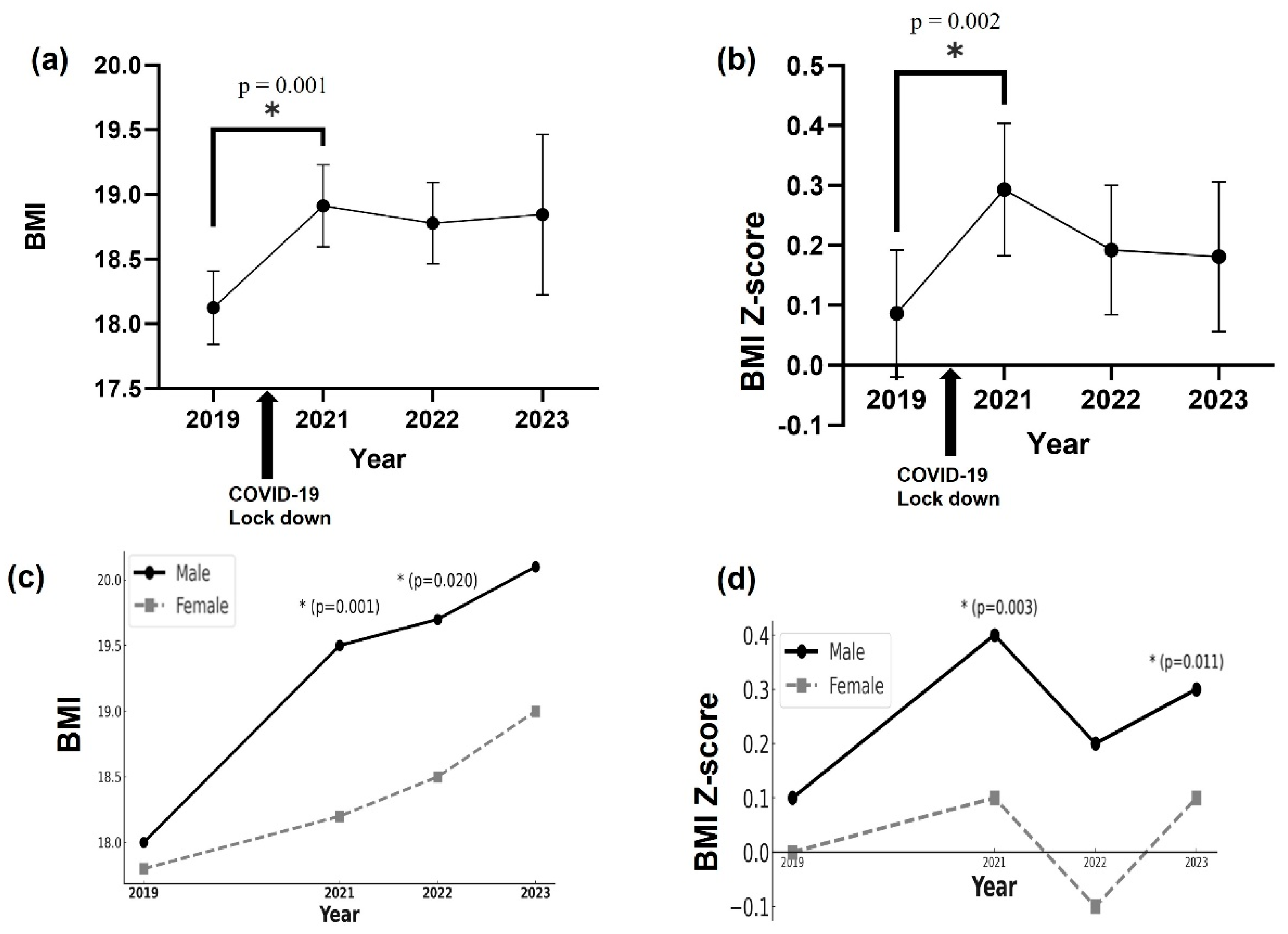
3.2. Changes in BMI and BMI Z-Scores Among All Students from 2019 to 2023 During the COVID-19 Lockdown: Cross-Sectional Study
3.3. Changes in BMI and BMI Z-Scores of Students in Each Grade During the COVID-19 Lockdown: Longitudinal Study
3.3.1. 2019 First-Grade Students: Longitudinal Analysis
3.3.2. 2019 Second Grade Students: Longitudinal Analysis
3.3.3. 2019 Third-Grade Students: Longitudinal Analysis
3.3.4. 2019 Fourth-Grade Students: Longitudinal Analysis
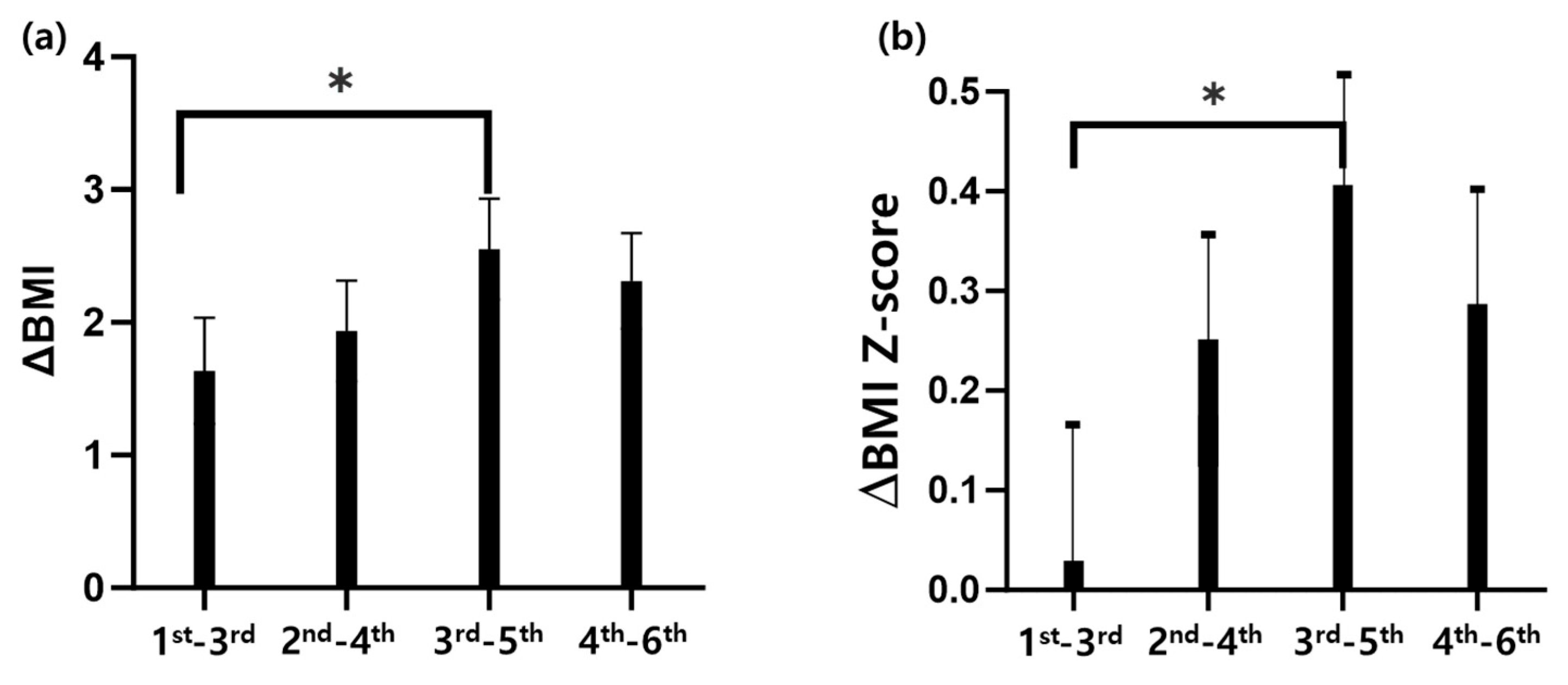
3.4. Difference in BMI and BMI Z-Score of Students Between 2019 and 2021: Longitudinal Study
3.5. Changes in BMI and BMI Z-Score of First and Second Graders According to Pre-COVID-19 Lockdown Obesity Status: Longitudinal Study
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| BMI | Body mass index |
| COVID-19 | Coronavirus disease 2019 |
| IRB | Institutional review board |
References
- Goel, A.; Reddy, S.; Goel, P. Causes, consequences, and preventive strategies for childhood obesity: A narrative review. Cureus 2024, 16, e64985. [Google Scholar] [CrossRef]
- Anderson, L.N.; Yoshida-Montezuma, Y.; Dewart, N.; Jalil, E.; Khattar, J.; De Rubeis, V.; Carsley, S.; Griffith, L.E.; Mbuagbaw, L. Obesity and weight change during the COVID-19 pandemic in children and adults: A systematic review and meta-analysis. Obes. Rev. 2023, 24, e13550. [Google Scholar] [CrossRef]
- Viner, R.; Russell, S.; Saulle, R.; Croker, H.; Stansfield, C.; Packer, J.; Nicholls, D.; Goddings, A.L.; Bonell, C.; Hudson, L.; et al. School closures during social lockdown and mental health, health behaviors, and well-being among children and adolescents during the first COVID-19 wave: A systematic review. JAMA Pediatr. 2022, 176, 400–409. [Google Scholar] [CrossRef]
- Kharel, M.; Sakamoto, J.L.; Carandang, R.R.; Ulambayar, S.; Shibanuma, A.; Yarotskaya, E.; Basargina, M.; Jimba, M. Impact of COVID-19 pandemic lockdown on movement behaviours of children and adolescents: A systematic review. BMJ Glob. Health 2022, 7, e007190. [Google Scholar] [CrossRef]
- Wilke, J.; Rahlf, A.L.; Füzéki, E.; Groneberg, D.A.; Hespanhol, L.; Mai, P.; de Oliveira, G.M.; Robbin, J.; Tan, B.; Willwacher, S.; et al. Physical activity during lockdowns associated with the COVID-19 pandemic: A systematic review and multilevel meta-analysis of 173 studies with 320,636 participants. Sports Med. Open 2022, 8, 125. [Google Scholar] [CrossRef]
- Ludwig-Walz, H.; Siemens, W.; Heinisch, S.; Dannheim, I.; Loss, J.; Bujard, M. How the COVID-19 pandemic and related school closures reduce physical activity among children and adolescents in the WHO European region: A systematic review and meta-analysis. Int. J. Behav. Nutr. Phys. Act. 2023, 20, 149. [Google Scholar] [CrossRef]
- Madigan, S.; Eirich, R.; Pador, P.; McArthur, B.A.; Neville, R.D. Assessment of changes in child and adolescent screen time during the COVID-19 pandemic: A systematic review and meta-analysis. JAMA Pediatr. 2022, 176, 1188–1198. [Google Scholar] [CrossRef]
- Whelan, J.; Hayward, J.; Nichols, M.; Brown, A.D.; Orellana, L.; Brown, V.; Becker, D.; Bell, C.; Swinburn, B.; Peeters, A.; et al. Reflexive Evidence and Systems interventions to Prevention Obesity and Non-communicable Disease (RESPOND): Protocol and baseline outcomes for a stepped-wedge cluster-randomised prevention trial. BMJ Open 2022, 12, e057187. [Google Scholar] [CrossRef]
- Storz, M.A. The COVID-19 pandemic: An unprecedented tragedy in the battle against childhood obesity. Clin. Exp. Pediatr. 2020, 63, 477–482. [Google Scholar] [CrossRef]
- Maggio, A.B.R.; Gal-Dudding, C.; Martin, X.; Chamay-Weber, C. Evaluation of the impact of the COVID-19 lockdown on BMI in children and adolescents with or without obesity. BMC Pediatr. 2022, 22, 509. [Google Scholar] [CrossRef]
- Ban, C.Y.; Shin, H.; Eum, S.; Yon, H.; Lee, S.W.; Choi, Y.S.; Shin, Y.H.; Shin, J.U.; Koyanagi, A.; Jacob, L.; et al. 17-year trends of body mass index, overweight, and obesity among adolescents from 2005 to 2021, including the COVID-19 pandemic: A Korean national representative study. Eur. Rev. Med. Pharmacol. Sci. 2023, 27, 1565–1575. [Google Scholar] [CrossRef]
- Yang, Y.; Zhang, M.; Yu, J.; Pei, Z.; Sun, C.; He, J.; Qian, T.; Luo, F.; Zhang, S.; Xu, Z. Nationwide trends of pediatric obesity and BMI Z-score from 2017–2021 in China: Comparable findings from real-world mobile- and hospital-based data. Front. Endocrinol. 2022, 13, 859245. [Google Scholar] [CrossRef]
- Adams, E.L.; Caccavale, L.J.; Smith, D.; Bean, M.K. Food insecurity, the home food environment, and parent feeding practices in the era of COVID-19. Obesity 2020, 28, 2056–2063. [Google Scholar] [CrossRef]
- Baskind, M.J.; Taveras, E.M.; Gerber, M.W.; Fiechtner, L.; Horan, C.; Sharifi, M. Parent-perceived stress and its association with children’s weight and obesity-related behaviors. Prev. Chronic Dis. 2019, 16, E39. [Google Scholar] [CrossRef]
- Natilli, M.; Rossi, A.; Trecroci, A.; Cavaggioni, L.; Merati, G.; Formenti, D. The long-tail effect of the COVID-19 lockdown on Italians’ quality of life, sleep and physical activity. Sci. Data 2022, 9, 250. [Google Scholar] [CrossRef]
- Kim, J.H.; Yun, S.; Hwang, S.S.; Shim, J.O.; Chae, H.W.; Lee, Y.J.; Lee, J.H.; Kim, S.C.; Lim, D.; Yang, S.W.; et al. The 2017 Korean National Growth Charts for children and adolescents: Development, improvement, and prospects. Korean J. Pediatr. 2018, 61, 135–149. [Google Scholar] [CrossRef]
- Baron, E.J.; Goldstein, E.G.; Wallace, C.T. Suffering in silence: How COVID-19 school closures inhibit the reporting of child maltreatment. J. Public Econ. 2020, 190, 104258. [Google Scholar] [CrossRef]
- Pereda, N.; Díaz-Faes, D.A. Family violence against children in the wake of COVID-19 pandemic: A review of current perspectives and risk factors. Child Adolesc. Psychiatry Ment. Health 2020, 14, 40. [Google Scholar] [CrossRef]
- Hammons, A.J.; Fiese, B.H. Is frequency of shared family meals related to the nutritional health of children and adolescents? Pediatrics 2011, 127, e1565–e1574. [Google Scholar] [CrossRef]
- Mazzolani, B.C.; Smaira, F.I.; Astley, C.; Iraha, A.Y.; Pinto, A.J.; Marques, I.G.; Cordeiro Amarante, M.; Rezende, N.S.; Sieczkowska, S.M.; Franco, T.C.; et al. Changes in eating habits and sedentary behavior during the COVID-19 pandemic in adolescents with chronic conditions. Front. Pediatr. 2021, 9, 714120. [Google Scholar] [CrossRef]
- Brazendale, K.; Beets, M.W.; Weaver, R.G.; Pate, R.R.; Turner-McGrievy, G.M.; Kaczynski, A.T.; Chandler, J.L.; Bohnert, A.; von Hippel, P.T. Understanding differences between summer vs. school obesogenic behaviors of children: The structured days hypothesis. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 100. [Google Scholar] [CrossRef]
- Wang, G.; Zhang, Y.; Zhao, J.; Zhang, J.; Jiang, F. Mitigate the effects of home confinement on children during the COVID-19 outbreak. Lancet 2020, 395, 945–947. [Google Scholar] [CrossRef]
- Díaz-Rodríguez, M.; Carretero-Bravo, J.; Pérez-Muñoz, C.; Deudero-Sánchez, M. Lockdown due to COVID-19 in Spanish children up to 6 years: Consequences on diet, lifestyle, screen viewing, and sleep. Int. J. Public Health 2022, 67, 1604088. [Google Scholar] [CrossRef]
- Pourghazi, F.; Eslami, M.; Ehsani, A.; Ejtahed, H.-S.; Qorbani, M. Eating habits of children and adolescents during the COVID-19 era: A systematic review. Front. Nutr. 2022, 9, 1004953. [Google Scholar] [CrossRef]
- Da Silva, F.R.; Junior, A.H.L.; Brant, V.M.; Lôbo, I.L.B.; Lancha, L.O.P.; Silva, A.; de Mello, M.T. The effects of COVID-19 quarantine on eating and sleeping behaviors. Nutrire 2020, 45, 25. [Google Scholar] [CrossRef]
- Ferentinou, E.; Koutelekos, I.; Pappa, D.; Manthou, P.; Dafogianni, C. The impact of the COVID-19 pandemic on childhood obesity: A review. Cureus 2023, 15, e45470. [Google Scholar] [CrossRef]
- Khan, M.A.; Menon, P.; Govender, R.; Abu Samra, A.M.; Allaham, K.K.; Nauman, J.; Östlundh, L.; Mustafa, H.; Smith, J.E.M.; AlKaabi, J.M. Systematic review of the effects of pandemic confinements on body weight and their determinants. Br. J. Nutr. 2022, 127, 298–317. [Google Scholar] [CrossRef]
- Nour, T.Y.; Altintaş, K.H. Obesity after natural disasters and associated risk factors: A systematic review. Disaster Med. Public Health Prep. 2025, 19, e8. [Google Scholar] [CrossRef]
- Yokomichi, H.; Matsubara, H.; Ishikuro, M.; Kikuya, M.; Isojima, T.; Yokoya, S.; Kato, N.; Tanaka, T.; Chida, S.; Ono, A.; et al. Impact of the great East Japan earthquake on body mass index, weight, and height of infants and toddlers: An infant survey. J. Epidemiol. 2018, 28, 237–244. [Google Scholar] [CrossRef]
- Liu, G.T.; Dancause, K.N.; Elgbeili, G.; Laplante, D.P.; King, S. Disaster-related prenatal maternal stress explains increasing amounts of variance in body composition through childhood and adolescence: Project ice storm. Environ. Res. 2016, 150, 1–7. [Google Scholar] [CrossRef]
- McCurry, J. Fukushima residents still struggling 2 years after disaster. Lancet 2013, 381, 791–792. [Google Scholar] [CrossRef]
- Tremblay, M.S.; LeBlanc, A.G.; Carson, V.; Choquette, L.; Connor Gorber, S.; Dillman, C.; Duggan, M.; Gordon, M.J.; Hicks, A.; Janssen, I.; et al. Canadian physical activity guidelines for the early years (aged 0–4 years). Appl. Physiol. Nutr. Metab. 2012, 37, 345–369. [Google Scholar] [CrossRef]
- O’Brien, M.; Nader, P.R.; Houts, R.M.; Bradley, R.; Friedman, S.L.; Belsky, J.; Susman, E. The ecology of childhood overweight: A 12-year longitudinal analysis. Int. J. Obes. 2007, 31, 1469–1478. [Google Scholar] [CrossRef]
- Glinianowicz, M.; Ciura, D.; Burnatowska, E.; Olszanecka-Glinianowicz, M. Psychological effects of the COVID-19 pandemic—What do we know about them? Eur. Rev. Med. Pharmacol. Sci. 2023, 27, 6445–6458. [Google Scholar] [CrossRef]
- Kroska, E.B.; O’Hara, M.W.; Elgbeili, G.; Hart, K.J.; Laplante, D.P.; Dancause, K.N.; King, S. The impact of maternal flood-related stress and social support on offspring weight in early childhood. Arch. Womens Ment. Health 2018, 21, 225–233. [Google Scholar] [CrossRef]
- Dancause, K.N.; Laplante, D.P.; Fraser, S.; Brunet, A.; Ciampi, A.; Schmitz, N.; King, S. Prenatal exposure to a natural disaster increases risk for obesity in 5½-year-old children. Pediatr. Res. 2012, 71, 126–131. [Google Scholar] [CrossRef]
- Harbec, M.J.; Pagani, L.S. Associations between early family meal environment quality and later well-being in school-age children. J. Dev. Behav. Pediatr. 2018, 39, 136–143. [Google Scholar] [CrossRef]
- Oliver, G.; Wardle, J.; Gibson, E.L. Stress and food choice: A laboratory study. Psychosom. Med. 2000, 62, 853–865. [Google Scholar] [CrossRef]
- Peng, L.; Hu, R.; Feng, Y.; Shi, W.; Zhao, L.; Jiang, L. The relationship between family diet consumption, family environment, parent anxiety and nutrition status children during the COVID-19 pandemic: A longitudinal study. Front. Public Health 2023, 11, 1228626. [Google Scholar] [CrossRef]
- Rawal, T.; Muris, J.W.M.; Mishra, V.K.; Arora, M.; Tandon, N.; van Schayck, O.C.P. Effect of an educational intervention on diet and physical activity among school-aged adolescents in Delhi -The i-PROMISe (PROMoting health literacy in Schools) Plus Study. Dialogues Health 2023, 2, 100123. [Google Scholar] [CrossRef]



| Year | Grade | Number | Ht | Ht-Zscore | Wt | Wt-Zscore | BMI | BMI-Zscore |
|---|---|---|---|---|---|---|---|---|
| 2019 | 1 | 91 | 120.5 ± 5.4 | 0.1 ± 1.0 | 25.2 ± 5.4 | 0.3 ± 1.0 | 17.2 ± 2.5 | 0.4 ± 1.1 |
| 2 | 102 | 127.0 ± 5.3 | 0.1 ± 0.9 | 27.4 ± 5.3 | 0.0 ± 1.0 | 16.8 ± 2.5 | 0.0 ± 1.1 | |
| 3 | 105 | 133.4 ± 5.6 | 0.1 ± 1.0 | 31.4 ± 6.9 | 0.0 ± 1.1 | 17.5 ± 3.0 | 0.0 ± 1.2 | |
| 4 | 76 | 139.3 ± 5.7 | 0.2 ± 0.9 | 37.1 ± 9.4 | 0.2 ± 1.4 | 18.9 ± 3.6 | 0.2 ± 1.6 | |
| 5 | 96 | 145.8 ± 6.8 | 0.1 ± 1.0 | 40.3 ± 10.6 | 0.0 ± 1.2 | 18.7 ± 3.6 | −0.1 ± 1.2 | |
| 6 | 71 | 153.1 ± 7.8 | 0.3 ± 1.1 | 47.5 ± 10.7 | 0.2 ± 1.1 | 20.1 ± 3.8 | 0.1 ± 1.3 | |
| 2021 | 1 | 75 | 122.2 ± 4.9 | 0.1 ± 1.0 | 25.5 ± 5.4 | 0.1 ± 1.2 | 16.8 ± 2.8 | 0.1 ± 1.4 |
| 2 | 91 | 128.7 ± 5.3 | 0.2 ± 0.9 | 28.8 ± 6.0 | 0.2 ± 1.0 | 17.2 ± 2.7 | 0.0 ± 1.1 | |
| 3 | 90 | 134.4 ± 6.3 | 0.3 ± 1.0 | 34.6 ± 9.2 | 0.5 ± 1.2 | 18.9 ± 3.6 | 0.5 ± 1.3 | |
| 4 | 106 | 139.7 ± 6.0 | 0.2 ± 0.9 | 37.4 ± 8.5 | 0.2 ± 1.1 | 19.0 ± 3.5 | 0.2 ± 1.2 | |
| 5 | 105 | 146.7 ± 6.8 | 0.2 ± 1.0 | 43.4 ± 10.3 | 0.3 ± 1.2 | 20.0 ± 3.7 | 0.3 ± 1.2 | |
| 6 | 74 | 154.0 ± 6.5 | 0.4 ± 0.9 | 50.6 ± 12.3 | 0.5 ± 1.2 | 21.1 ± 4.1 | 0.4 ± 1.3 | |
| 2022 | 1 | 78 | 122.5 ± 4.2 | 0.1 ± 0.8 | 24.3 ± 3.8 | −0.0 ± 0.9 | 16.1 ± 2.1 | −0.1 ± 1.1 |
| 2 | 73 | 127.9 ± 5.2 | 0.2 ± 1.0 | 28.5 ± 6.4 | 0.1 ± 1.1 | 17.3 ± 3.0 | 0.1 ± 1.3 | |
| 3 | 91 | 134.9 ± 5.7 | 0.3 ± 0.9 | 33.5 ± 7.7 | 0.3 ± 1.1 | 18.2 ± 3.2 | 0.2 ± 1.2 | |
| 4 | 90 | 140.8 ± 6.9 | 0.2 ± 1.0 | 39.4 ± 11.0 | 0.4 ± 1.2 | 19.6 ± 3.9 | 0.4 ± 1.3 | |
| 5 | 106 | 146.6 ± 6.8 | 0.3 ± 1.0 | 42.8 ± 10.1 | 0.3 ± 1.1 | 19.7 ± 3.7 | 0.2 ± 1.3 | |
| 6 | 106 | 154.3 ± 6.7 | 0.5 ± 1.0 | 48.9 ± 11.2 | 0.4 ± 1.1 | 20.4 ± 3.8 | 0.2 ± 1.2 | |
| 2023 | 1 | 82 | 122.5 ± 5.4 | 0.4 ± 0.9 | 25.2 ± 5.2 | 0.3 ± 1.1 | 16.6 ± 2.4 | 0.1 ± 1.2 |
| 2 | 75 | 128.3 ± 4.6 | 0.3 ± 0.8 | 27.5 ± 4.8 | 0.0 ± 0.9 | 16.6 ± 2.3 | −0.1 ± 1.1 | |
| 3 | 73 | 134.0 ± 5.4 | 0.2 ± 1.0 | 32.5 ± 7.8 | 0.1 ± 1.1 | 17.9 ± 3.4 | 0.0 ± 1.3 | |
| 4 | 91 | 139.8 ± 6.0 | 0.2 ± 0.9 | 37.5 ± 8.7 | 0.3 ± 1.1 | 19.0 ± 3.5 | 0.2 ± 1.2 | |
| 5 | 85 | 146.8 ± 7.0 | 0.4 ± 1.0 | 43.8 ± 12.2 | 0.4 ± 1.2 | 20.0 ± 4.0 | 0.3 ± 1.3 | |
| 6 | 107 | 152.9 ± 6.9 | 0.3 ± 1.0 | 50.2 ± 29.0 | 0.4 ± 1.5 | 21.4 ± 13.7 | 0.3 ± 1.9 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choi, I.H.; Park, E.; Lee, E.-J.; Kim, S.-Y.; Kim, M.; Chung, S. Body Mass Index Changes from Before to 3 Years After the COVID-19 Lockdown: A Retrospective Longitudinal Study in a Single Elementary School. Children 2025, 12, 1157. https://doi.org/10.3390/children12091157
Choi IH, Park E, Lee E-J, Kim S-Y, Kim M, Chung S. Body Mass Index Changes from Before to 3 Years After the COVID-19 Lockdown: A Retrospective Longitudinal Study in a Single Elementary School. Children. 2025; 12(9):1157. https://doi.org/10.3390/children12091157
Chicago/Turabian StyleChoi, Iee Ho, Esther Park, Eun-Jee Lee, Sun-Young Kim, Minsun Kim, and Sochung Chung. 2025. "Body Mass Index Changes from Before to 3 Years After the COVID-19 Lockdown: A Retrospective Longitudinal Study in a Single Elementary School" Children 12, no. 9: 1157. https://doi.org/10.3390/children12091157
APA StyleChoi, I. H., Park, E., Lee, E.-J., Kim, S.-Y., Kim, M., & Chung, S. (2025). Body Mass Index Changes from Before to 3 Years After the COVID-19 Lockdown: A Retrospective Longitudinal Study in a Single Elementary School. Children, 12(9), 1157. https://doi.org/10.3390/children12091157






