Abstract
(1) Background: Cardiorespiratory fitness (CRF) is known to be a prognostic factor regarding long-term morbidity and mortality. This study aimed to develop a standardized Stair Climbing Test (SCT) with a reliable correlation to spiroergometry and the 6MWT which can be used in healthy children as well as patients with congenital heart disease (CHD) and a restricted exercise capacity. (2) Methods: A total of 28 healthy participants aged 10–18 years were included. We tested the individuals’ CRF by cardiopulmonary exercise testing (CPET) on a treadmill, the 6MWT, and a newly developed Stair Climbing Test (SCT). For the SCT, we defined a standardized SCT protocol with a total height of 13.14 m to achieve maximal exercise effects while recording time and vital parameters. To compare the SCT, the 6 Min Walking Test, and CPET, we introduced an SCT-Index that included patient data (weight, height) and time. To assess the SCT’s feasibility for clinical practice, we also tested our protocol with five adolescents with complex congenital heart disease (i.e., Fontan circulation). (3) Results: A strong correlation was observed between SCT-Index and O2 pulse (r = 0.921; p < 0.001). In addition, when comparing the time achieved during SCT (tSCT) with VO2max (mL/min/kg) and VO2max (mL/min), strong correlations were found (r = −0.672; p < 0.001 and r = −0.764; p < 0.001). Finally, we determined a very strong correlation between SCT-Index and VO2max (mL/min) (r = 0.927; p = <0.001). When comparing the 6MWD to tSCT, there was a moderate correlation (r = −0.544; p = 0.003). It appears to be feasible in patients with Fontan circulation. (4) Conclusions: We were able to demonstrate that there is a significant correlation between our standardized SCT and treadmill CPET. Therefore, we can say that the SCT can be used as an easy supplement to CPET and in certain contexts, it can also be used as a screening tool when CPET is not available. The advantages would be that the SCT is a simple, quick, cost-effective, and reliable standardized (sub)maximal exercise test to evaluate CRF in healthy children on a routine basis. We can even assume that it can be used in patients with congenital heart disease.
1. Introduction
Physical activity offers fundamental health benefits for children and adolescents. Research has consistently shown that individuals with high cardiorespiratory fitness (CRF) present with obesity significantly less often [1,2,3], suggesting a link between fitness and body composition. Furthermore, generally elevated CRF levels are inversely related to a more favorable cardiovascular profile, indicating a protective role for cardiovascular health [1]. These effects extend even further, showing an association between increased CRF levels and a lower risk of all-cause mortality and reduced susceptibility to coronary heart disease and cardiovascular events [4,5]. These results underscore the overall benefits of physical fitness and highlight its potential to reduce risks across multiple health domains, including cardiovascular, metabolic, and psychiatric outcomes [2,6]. This is one of the reasons why the World Health Organization (WHO) recommends that children and young people aged 5–17 years should do at least 60 min of moderate to vigorous aerobic activity per day throughout the week, along with three days a week of intense aerobic activities and movements that strengthen the muscles and bones [7].
With this knowledge in mind, it is even more important for children and young adults with congenital heart disease to assess cardiorespiratory fitness on a routine basis and to maintain and/or increase the fitness level in these individuals.
To measure cardiorespiratory fitness, there are basically two types of exercise tests: maximal exercise tests and submaximal exercise tests. Maximal exercise tests require maximal effort, whereas submaximal exercise tests, on the other hand, do not require maximal effort. Cardiorespiratory fitness is therefore often estimated using equations or nomograms, leading to possible inaccuracies. Nevertheless, submaximal testing is used when maximal testing is not practical for safety, physiological, logistical, or cost reasons, and it is useful for identifying individuals with low cardiorespiratory fitness [8]. An example of a maximal exercise test is CPET on a bicycle or treadmill; the 6 Min Walking Test (6MWT) is an example of a submaximal test [8,9,10].
In Europe, bicycle ergometry is the preferred choice over treadmill ergometry due to its ability to minimize artifacts in stress ECG and alleviate the potential insecurity or anxiety caused by the moving surface of a treadmill. However, this preference comes with a trade-off, as bicycle ergometry activates less muscle mass, leading to a maximal performance level approximately 10% lower than that achievable on a treadmill. The treadmill also offers the advantage of achieving a higher heart rate compared to the bicycle [6,11].
The 6MWT is a standardized, simple, cheap, submaximal exercise test that can be carried out almost anywhere without great effort. It measures the maximum distance a subject can walk within 6 min [8,12].
In the literature, Stair Climbing Tests (SCTs) are described in many ways, with the majority of studies assessing functional mobility in patients after orthopedic surgery or with neuromuscular diseases, rather than those with congenital heart disease. However, there is currently no standardized and thereby comparable protocol for SCTs. Therefore, our working group developed a standardized SCT protocol. Our goal was to develop a simple, standardized test which is applicable in patients with congenital heart disease. Therefore, we studied the approaches described in the literature and aimed for a protocol that would induce maximal exertion in order for it to be comparable to CPET results. We had already tested it in healthy normal-weight and obese 18–30-year-old adult subjects. The results showed a significant correlation to the 6MWT and spiroergometry [13].
The aim of this study was to evaluate CRF in healthy children and adolescents aged 10–18 years using the SCT and comparing the results with spiroergometry (maximal oxygen uptake, oxygen pulse) and the 6MWT. Further, our aim was to assess CRF in children and adolescents with complex congenital heart disease, i.e., Fontan patients.
2. Materials and Methods
2.1. Ethical Statement
The “Step by Step” study was considered ethically and legally innocuous by the ethics committee at LMU Munich, No.: 22-0029, on 22 September 2022 and was conducted in accordance with the ethical standards of the Declaration of Helsinki. Informed consent was given by all subjects.
2.2. Study Design and Study Population
This study was a pilot study. A total number of 28 healthy participants, aged 10–18 years, were included. To be eligible for this study, subjects had to have a BMI <25 kg/m2. Only children and adolescents with no known pre-existing diseases and no regular medication were included. Those with an abnormal physical examination, echocardiography, or pathological finding in the 12-lead electrocardiogram (ECG) were excluded. In addition, individuals with a respiratory exchange ratio (RER) of >1.0 [14,15,16] at maximal exercise in spiroergometry were defined as eligible. Participants who terminated the exercise before a RER >1.0 were excluded. Additional five Fontan patients were comparable regarding age and had a functioning Fontan circulation with normal saturation and a normal ventricular function without significant valvular regurgitation. For the Stair Climbing Test, the test subjects only needed to be physically capable of performing the test. There were no further exclusion criteria. The examinations were performed on one or two days in the pediatric cardiology outpatient unit of LMU Munich.
2.3. Assessment of Cardiorespiratory Fitness
In order to measure cardiorespiratory fitness, the study participants initially had to perform a 6MWT. Following adequate rest, the SCT was conducted according to our standardized protocol. Before CPET on the treadmill, a resting period of at least 30 min was employed to ensure sufficient recovery time. This allowed the individuals to feel subjectively recovered and attain their resting heart rate.
The 6MWT was performed according to the guidelines of the German Society for Pediatric Cardiology (DGPK), which translated the instructions from the American Thorax Society and European Respiratory Society into German [9,17]. Heart rate (HR, bpm), oxygen saturation (%), and blood pressure (mmHg) were measured immediately before and after the test. Furthermore, the 6 min walking distance (6MWD) achieved was recorded.
The Stair Climbing Test required, according to our protocol and to achieve maximal exercise levels, 4 floors and/or a staircase with a total of at least 12 m height [18,19] and a chest strap to measure the subject’s heart rate during the test. Oxygen saturation, heart rate, and blood pressure were monitored before and after the test. In our study, a height of 13.14 m was used, which is the equivalent of 4 floors. The subjects had to run up and down these 4 floors as fast as possible, without gripping the handrail or skipping any steps. During the SCT, the children and adolescents were encouraged and motivated by the person conducting the test so they would achieve maximum performance. There was no upper time limit. In addition, an SCT index was calculated, which was defined as SCT-Index = ().
The cardiopulmonary exercise test (CPET) was performed on a treadmill according to the recommendations of the DGPK using a step-protocol [10]. The speed and incline of the treadmill were increased every 90 s until the subjects were exhausted. The speed started at 2.5 km/h and was increased by 0.5 km/h every 90 s; the incline started at 0% and was increased by 3% every 90 s up to a maximum incline of 21%. After that, only the speed was increased [10]. Different CPET parameters (VO2max (mL/min; mL/min/kg); oxygen pulse (mL), RER) were measured and the subjective feeling of exertion was recorded using the Borg scale [6].
To practically assess the feasibility of our SCT in clinical routines, we additionally enrolled five patients with Fontan circulation.
2.4. Statistical Analysis
The IBM SPSS (version 29.0.1 Statistics for Windows, IBM Corp., Armonk, NY, USA) program was utilized for statistical analysis. A descriptive analysis was conducted and reported as means ± standard deviations. Simple correlations were performed using the Spearman rho and Pearson correlation coefficients, depending on whether the correlated variables were normally distributed or not. The significance level was set at p < 0.05.
3. Results
In our study, we included 28 healthy children and young adults (12 male and 16 female) aged 13.89 years (±2.63 years) with a BMI of 18.9 kg/m2 (±2.34 kg/m2), as detailed in Table 1. These participants achieved a mean 6MWD of 753.0 m (±74.1 m) in the 6MWT, with a mean tSCT of 50.2s (±5.57 s) and a mean SCT-Index of 14.1 (±4.88). Additionally, the subjects attained a mean VO2max of 2573.9 mL/min (±983.61 mL/min) and a mean VO2max/kg of 48.3 mL/min/kg (±8.2 mL/min/kg). Maximal O2 pulse was measured at 13.1 mL (±5.83 mL). (Table 2).

Table 1.
Descriptive statistics of the cohort (showing means and standard deviations). N = number.

Table 2.
Descriptive statistics of the exercise test (showing means and standard deviations).
A very strong correlation was observed between SCT-Index and O2 pulse (r = 0.921; p < 0.001). In addition, when comparing the time achieved during SCT (tSCT) with VO2max/kg (mL/min/kg) and VO2max (mL/min), strong correlations were found (r = −0.672; p < 0.001 and r = −0.764; p < 0.001) (see Figure 1). Finally, we determined a very strong correlation between SCT-Index and VO2max (mL/min) (r = 0.927; p < 0.001) and a moderate correlation between SCT-Index and VO2max/kg (mL/min/kg) (r = 0.407; p = 0.054). There was a moderate correlation between the distance walked during the 6MWT and VO2max/kg (mL/min/kg) (r = 0.569; p = 0.002) and only a moderate correlation with VO2max (mL/min) (r = 0.473; p = 0.011). When comparing the SCT-Index with the 6MWD, there was a weak correlation (r = 0.351; p = 0.067).
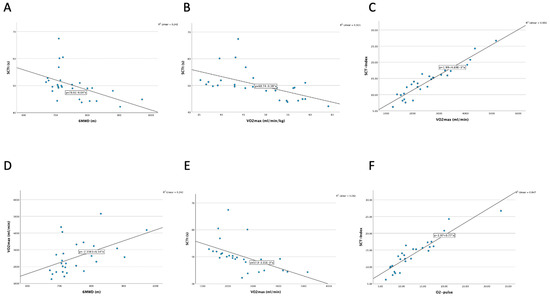
Figure 1.
(A) Moderate correlation of 6MWD to tSCT (r = −0.544; p = 0.003). (B) Strong correlation of tSCT to VO2max (mL/min/kg) (r = −0.672, p < 0.001. (C) Very strong correlation of SCT-Index to VO2max (mL/min) (r = 0.927; p ≤ 0.001). (D) Moderate correlation of 6MWD to VO2max (mL/min) (r = 0.473, p = 0.011). (E) Strong correlation of tSCT to VO2max (mL/min) (r = −0.764; p ≤ 0.001). (F) Very strong correlation of oxygen pulse to SCT-Index (r = 0.921, p ≤ 0.001).
For the Fontan patients, we found a very strong correlation between the SCT-Index and VO2max (mL/min) (r = 0.929; p = 0.022) and between the SCT-Index and maximum O2 pulse (r = 0.928; p = 0.023).
4. Discussion
CPET has various indications and it is still not universally accessible as it is an expensive examination requiring a lot of equipment and time.
Our study was a pilot study with the aim to define a simple Stair Climbing Test (SCT) for the assessment of the fitness of healthy children and adolescents comparable to CPET and the 6MWT. A previous study by our working group had already shown a significant correlation between the SCT using our standardized protocol and the parameters measured in spiroergometry in healthy and obese adults [20]. In this study, we also tested this assumption for healthy 10–18-year-old children and adolescents. We also performed the SCT in five patients with complex congenital heart disease and a priori reduced exercise performance to evaluate whether it can also be used in individuals with CHD.
The gold standard for assessing aerobic fitness is VO2max and VO2peak, measured by CPET [2,21]. It can be challenging to reach a plateau in VO2 during exercise tests, especially for untrained subjects unfamiliar with the discomfort of strenuous activities. Therefore, in many cases, only VO2peak is attained, serving as a substitute for VO2max [11], while other criteria such as RER, heart rate, and the Borg scale are used to determine VO2max [16]. The VO2max reported in our results corresponds to the maximum amount of oxygen absorbed by the test subjects at the maximum load attained. As previously mentioned, the subjects had to achieve an RER of >1.0. RER objectively describes an individual’s level of exertion.
O2 pulse is the amount of oxygen absorbed per heartbeat and is calculated as follows: oxygen pulse = VO2 (mL/min)/heart rate [22,23]. Since O2 pulse is dependent on VO2, it is understandable that both VO2max and O2 pulse correlate very well with the SCT-Index, with only a minimal difference in the correlation.
In adults, other variations of the Stair Climbing Test have primarily been utilized in patients with lung diseases [18,24], orthopedic conditions, or neuromuscular impairment, each using different protocols and SCT procedures. These tests may serve as a predictive tool for postoperative complications and aid in identifying patients who could potentially benefit from an extra CPET [25]. In the orthopedic setting, the SCT offers valuable information to assess mobility in general and an individual’s capability to ascend and descend stairs, as well as evaluate lower limb strength [26]. Zaino et al. used an SCT including 14 steps to examine functional mobility in 47 children, 20 of them with cerebral palsy [27]. Regarding the level of exertion, which is needed to aim for a maximal exercise test, the needed vertical height seems to be 12meters or more. Therefore, our protocol includes four flights of stairs with a total vertical height over 12 m. Devendra et. al. also used a protocol including four flights of stairs to assess desaturation during exercise in patients with patent foramen ovale [28]. In contrast, in pediatrics, the 4 Stairs Climb Test (4SC) is used for the assessment of motion capability. This pediatric test is primarily intended for sick children and involves ascending and descending only over a height of 4 steps; therefore, it is hardly comparable to our study. It has demonstrated particular success in children and is widely employed for evaluating the motor function of patients with neuromuscular diseases [20,29]. It is essential to note that the 4SC test, although also assessing stair climbing, differs from the adult-focused SCT.
To the best of our knowledge, there are no comparable data for an SCT or SCT-Index in the literature for healthy 10–18-year-old children and adolescents that would be comparable to the test we present here. Nevertheless, there is a relevant approach for adults that aligns with our methodology and lends support to the results we presented. Cataneo et al. [30] conducted a study wherein they reported a moderate correlation (r = 0.515; p < 0.005) in their variation of the SCT-Index (called ) and a strong correlation (r = −0.707; p < 0.005) in tSCT with VO2max/KG. These results strengthen our general assumption and findings.
Our test protocol and measurements also revealed a strong correlation between the SCT-Index and VO2max. However, when considering VO2max/kg, the correlation was moderate. This could be due to the fact that physical performance, especially in children and adolescents, is complex and cannot simply be related to weight [21]. Blais et al. [21] therefore even suggest abandoning the indexing of VO2max based on weight. Instead, they advocate for more precise adjustments based on body size, emphasizing the importance of such adjustments to attain more accurate and meaningful results. However, for the sake of simplicity, we included only body weight as a factor in our SCT-Index as the body weight had to be lifted across the four floors. Since the subjects we included neither had a pre-existing disease nor were obese, the results should not be over- or underestimated.
The 6MWT is a submaximal test and is primarily used to evaluate functional status and monitor the response to medical interventions in individuals struggling with impaired exercise capacity and moderate to severe heart and lung diseases [17,31]. Additional unique challenges when using it with children include a potential lack of motivation and understanding regarding the necessity of the 6MWT [32]. This highlights the importance of considering age-specific factors in the interpretation of results.
In our study, we identified a moderate correlation between 6MWD and VO2max. These findings are in line with the results of two other studies. Specifically, Jalil et al. observed a strong correlation between the 6MWT and VO2max (p < 0.01, r = 0.723) in their research involving 8–17-year-old boys. Additionally, they reported similar outcomes from other studies encompassing sick children and adolescents, with correlations ranging from r = 0.34 to r = 0.76 [33]. Furthermore, Li et al. conducted a study focusing on 12–16 year old children and adolescents, and their results also indicated a moderate correlation between 6MWD and VO2max (r = 0.44, p ≤ 0.0001) [34]. The consistency across these studies reinforces the association between the distance covered in the 6 Min Walking Test and maximal oxygen uptake, mainly in healthy children.
Furthermore, we observed a weak correlation between the SCT Index and the 6MWD in our results. This may be explained by the fact that the SCT is a maximal exercise test and should be considered either complementary to or as a potential replacement for a maximal exercise test, e.g., spiroergometry, in some fields, or as a screening tool in institutions or countries without access to spiroergometry.
The excellent clinical correlation of the SCT in healthy children and adolescents was replicable in patients with univentricular hearts and Fontan physiology. We therefore aim to use this test in a larger population with congenital heart disease.
Limitations
As our study is a pilot study, the data naturally only relate to a small cohort and may need confirmation on a larger scale and in different patient groups, for instance, subjects with congenital heart disease—in moderate cases maybe even before and after surgery—and children of a younger age. As all tests were performed on the same day, subjects potentially experienced exhaustion toward the end of the test period. However, we ensured that the subjects had adequate rest periods between tests and could recover effectively. We waited until the heart rate had returned to the baseline value, and the subjects subjectively reported feeling recovered before proceeding with each test. Treadmill spiroergometry was intentionally scheduled as the final test, as subjects were expected to put maximal effort into it.
It is important to note that the performance of children and adolescents may be highly dependent on their motivation. To attenuate this, we ensured consistent motivation and encouragement for all test subjects, employing identical sentences and wording for both the stair climbing test and spiroergometry. Furthermore, it is worth mentioning that the expressions to be used with the 6MWT are fixed anyways. Additionally, a specific minimum load was attained during spiroergometry by reaching the prescribed minimum RER.
5. Conclusions
Physical activity, especially high cardiorespiratory fitness (CRF), offers essential health benefits for children and adolescents. We were able to show that there is a significant correlation between our newly developed and standardized SCT and a standardized treadmill CPET in healthy children as well as in patients with Fontan circulation. Consequently, the SCT can serve as a valuable supplement to CPET and, in specific contexts, even as a substitution for treadmill CPET, especially when the primary goal is assessing fitness or exercise capacity rather than detecting cardiorespiratory diseases. This underscores the SCT’s advantages as a simple, quick, affordable, and reliable standardized exercise test for routine CRF assessment in healthy children, with potential applications in patients with congenital heart disease.
Author Contributions
Conceptualization, S.K.D. and N.A.H.; methodology, S.K.D., M.P.M., J.W. and A.L.; software, M.P.M., J.W. and A.L.; validation, S.K.D., F.S.O. and N.A.H.; formal analysis, S.K.D., F.S.O. and N.A.H.; investigation, M.P.M. and S.K.D.; resources, M.P.M.; data curation, M.P.M.; writing—original draft preparation, M.P.M.; writing—review and editing, S.K.D., F.S.O., G.M., A.J. and N.A.H.; visualization, M.P.M. and S.K.D.; supervision, N.A.H.; project administration, S.K.D.; funding acquisition, S.K.D. All authors have read and agreed to the published version of the manuscript.
Funding
This research was funded by “kinderherzen Fördergemeinschaft Deutsche Kinderherzzentren e.V” (www.kinderherzen.de, URL accessed on 20 January 2024), grant number W-M-011/2022.
Institutional Review Board Statement
This study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of the Medical Faculty of Ludwig Maximilians University Munich (Ethikkommission der Medizinischen Fakultät der Ludwig-Maximilians-Universität München, Pettenkoferstraße 8a, 80336 Munich, Germany; approval number: No.: 22-0029 on the 22 September 2022).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available in article.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Ortega, F.B.; Ruiz, J.R.; Castillo, M.J.; Sjostrom, M. Physical fitness in childhood and adolescence: A powerful marker of health. Int. J. Obes. 2008, 32, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Takken, T.; Bongers, B.C.; van Brussel, M.; Haapala, E.A.; Hulzebos, E.H.J. Cardiopulmonary Exercise Testing in Pediatrics. Ann. Am. Thorac. Soc. 2017, 14 (Suppl. 1), S123–S128. [Google Scholar] [CrossRef]
- Meng, C.; Yucheng, T.; Shu, L.; Yu, Z. Effects of school-based high-intensity interval training on body composition, cardiorespiratory fitness and cardiometabolic markers in adolescent boys with obesity: A randomized controlled trial. BMC Pediatr. 2022, 22, 112. [Google Scholar] [CrossRef]
- Kodama, S.; Saito, K.; Tanaka, S.; Maki, M.; Yachi, Y.; Asumi, M.; Sugawara, A.; Totsuka, K.; Shimano, H.; Ohashi, Y.; et al. Cardiorespiratory fitness as a quantitative predictor of all-cause mortality and cardiovascular events in healthy men and women: A meta-analysis. JAMA 2009, 301, 2024–2035. [Google Scholar] [CrossRef] [PubMed]
- Lollgen, H.; Bachl, N. Cardiovascular prevention and regular physical exercise: Activity and training as the true “polypill”. Herz 2016, 41, 664–670. [Google Scholar] [CrossRef]
- Lollgen, H.; Leyk, D. Exercise Testing in Sports Medicine. Dtsch. Ärzteblatt Int. 2018, 115, 409–416. [Google Scholar] [CrossRef]
- World Health Organization. WHO Guidelines on Physical Activity and Sedentary Behaviour; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Raghuveer, G.; Hartz, J.; Lubans, D.R.; Takken, T.; Wiltz, J.L.; Mietus-Snyder, M.; Perak, A.M.; Baker-Smith, C.; Pietris, N.; Edwards, N.M.; et al. Cardiorespiratory Fitness in Youth: An Important Marker of Health: A Scientific Statement from the American Heart Association. Circulation 2020, 142, e101–e118. [Google Scholar] [CrossRef] [PubMed]
- Baden, W.; Hager, A.; Lammers, A. Positionspapier zum 6-Minuten Gehtest der Arbeitsgruppe Belastungsuntersuchungen der DGPK. 2018. Available online: https://www.yumpu.com/de/document/view/23833715/positionspapier-zum-6-minuten-gehtest-der-arbeitsgruppe- (accessed on 20 January 2024).
- Lawrenz, W.; Dubowy, K.-O.; Baden, W.; Hager, A. Ergometrie und Spiroergometrie bei Kindern und Jugendlichen; Positionspapier; Deutsche Gesellschaft für Pädiatrische Kardiologie: Düsseldorf, Germany, 2019. [Google Scholar]
- Breuer, H.W. Spiroergometry. Indications, methods, relevance. Dtsch. Med. Wochenschr. 1997, 122, 447–449. [Google Scholar] [CrossRef]
- Bartels, B.; de Groot, J.F.; Terwee, C.B. The six-minute walk test in chronic pediatric conditions: A systematic review of measurement properties. Phys. Ther. 2013, 93, 529–541. [Google Scholar] [CrossRef]
- Uhl, M.; Huber, K.V.; Haas, N.A.; Dold, S.K. Stairway to Heaven: Evaluation of Cardiorespiratory Fitness with a Simple Standardized Stair Climbing Test in Comparison to Standard Treadmill Cardiopulmonary Exercise Testing and 6-Minute Walking Test. Thorac. Cardiovasc. Surg. 2023, 71, S73–S106. [Google Scholar] [CrossRef]
- Davis, J.A.; Storer, T.W.; Caiozzo, V.J.; Pham, P.H. Lower reference limit for maximal oxygen uptake in men and women. Clin. Physiol. Funct. Imaging 2002, 22, 332–338. [Google Scholar] [CrossRef]
- Jackson, A.S.; Blair, S.N.; Mahar, M.T.; Wier, L.T.; Ross, R.M.; Stuteville, J.E. Prediction of functional aerobic capacity without exercise testing. Med. Sci. Sports Exerc. 1990, 22, 863–870. [Google Scholar] [CrossRef]
- Edvardsen, E.; Hem, E.; Anderssen, S.A. End criteria for reaching maximal oxygen uptake must be strict and adjusted to sex and age: A cross-sectional study. PLoS ONE 2014, 9, e85276. [Google Scholar] [CrossRef]
- ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: Guidelines for the six-minute walk test. Am. J. Respir. Crit. Care Med. 2002, 166, 111–117. [Google Scholar] [CrossRef]
- Novoa, N.M.; Rodriguez, M.; Gomez, M.T.; Jimenez, M.F.; Varela, G. Fixed-altitude stair-climbing test replacing the conventional symptom-limited test. A pilot study. Arch. Bronconeumol. 2015, 51, 268–272. [Google Scholar] [CrossRef]
- Garcia-Rio, F. The Stair-climbing Test. The Quest for Much-needed Simplicity. Arch. Bronconeumol. 2015, 51, 259–260. [Google Scholar] [CrossRef] [PubMed]
- Schorling, D.C.; Rawer, R.; Kuhlmann, I.; Muller, C.; Pechmann, A.; Kirschner, J. Mechanographic analysis of the timed 4 stair climb test—Methodology and reference data of healthy children and adolescents. J. Musculoskelet. Neuronal Interact. 2023, 23, 4–25. [Google Scholar] [PubMed]
- Blais, S.; Berbari, J.; Counil, F.P.; Dallaire, F. A Systematic Review of Reference Values in Pediatric Cardiopulmonary Exercise Testing. Pediatr. Cardiol. 2015, 36, 1553–1564. [Google Scholar] [CrossRef] [PubMed]
- Mezzani, A. Cardiopulmonary Exercise Testing: Basics of Methodology and Measurements. Ann. Am. Thorac. Soc. 2017, 14 (Suppl. 1), S3–S11. [Google Scholar] [CrossRef] [PubMed]
- Oliveira, R.B.; Myers, J.; Araujo, C.G. Long-term stability of the oxygen pulse curve during maximal exercise. Clinics 2011, 66, 203–209. [Google Scholar] [CrossRef] [PubMed]
- Brunelli, A. Risk assessment for pulmonary resection. Semin. Thorac. Cardiovasc. Surg. 2010, 22, 2–13. [Google Scholar] [CrossRef]
- Rodriguez, M. Stair-climbing test: Beyond the height. Thorax 2020, 75, 716. [Google Scholar] [CrossRef]
- Bennell, K.; Dobson, F.; Hinman, R. Measures of physical performance assessments: Self-Paced Walk Test (SPWT), Stair Climb Test (SCT), Six-Minute Walk Test (6MWT), Chair Stand Test (CST), Timed Up & Go (TUG), Sock Test, Lift and Carry Test (LCT), and Car Task. Arthritis Care Res. 2011, 63 (Suppl. 11), S350–S370. [Google Scholar] [CrossRef]
- Zaino, C.A.; Marchese, V.G.; Westcott, S.L. Timed up and down stairs test: Preliminary reliability and validity of a new measure of functional mobility. Pediatr. Phys. Ther. 2004, 16, 90–98. [Google Scholar] [CrossRef] [PubMed]
- Devendra, G.P.; Rane, A.A.; Krasuski, R.A. Provoked exercise desaturation in patent foramen ovale and impact of percutaneous closure. JACC Cardiovasc. Interv. 2012, 5, 416–419. [Google Scholar] [CrossRef] [PubMed]
- Bora, M.; Yalcin, A.; Bulut, N.; Yilmaz, O.; Karaduman, A.; Topuz, S.; Alemdaroglu-Gurbuz, I. Investigation of surface electromyography amplitude values during stair climbing task in children with Duchenne muscular dystrophy. Neurol. Sci. 2022, 43, 2791–2801. [Google Scholar] [CrossRef] [PubMed]
- Cataneo, D.C.; Kobayasi, S.; Carvalho, L.R.; Paccanaro, R.C.; Cataneo, A.J. Accuracy of six minute walk test, stair test and spirometry using maximal oxygen uptake as gold standard. Acta Cir. Bras. 2010, 25, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Enright, P.L. The six-minute walk test. Respir. Care 2003, 48, 783–785. [Google Scholar] [PubMed]
- Geiger, R.; Strasak, A.; Treml, B.; Gasser, K.; Kleinsasser, A.; Fischer, V.; Geiger, H.; Loeckinger, A.; Stein, J.I. Six-minute walk test in children and adolescents. J. Pediatr. 2007, 150, 395–399.e2. [Google Scholar] [CrossRef] [PubMed]
- Jalili, M.; Nazem, F.; Sazvar, A.; Ranjbar, K. Prediction of Maximal Oxygen Uptake by Six-Minute Walk Test and Body Mass Index in Healthy Boys. J. Pediatr. 2018, 200, 155–159. [Google Scholar] [CrossRef] [PubMed]
- Li, A.M.; Yin, J.; Yu, C.C.; Tsang, T.; So, H.K.; Wong, E.; Chan, D.; Hon, E.K.; Sung, R. The six-minute walk test in healthy children: Reliability and validity. Eur. Respir. J. 2005, 25, 1057–1060. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).

