Human Milk Fatty Acid Composition and Its Effect on Preterm Infants’ Growth Velocity
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Sample Collection
2.3. Lipid Extraction and Methylation
2.4. Gas Chromatography
2.5. Statistical Analysis
3. Results
3.1. Descriptive Data
3.2. Classes of Fatty Acids in Human Milk
3.3. Fatty Acid Profile of Human Milk Samples
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- American Academy of Pediatrics. Policy statement: Breastfeeding and the use of human milk. Pediatrics 2012, 129, e827–e841. [Google Scholar] [CrossRef] [PubMed]
- Koletzko, B.; Rodriguez-Palmero, M.; Demmelmair, H.; Fidler, N.; Jensen, R.; Sauerwald, T. Physiological aspects of human milk lipids. Early Hum. Dev. 2001, 65, S3–S18. [Google Scholar] [CrossRef] [PubMed]
- Mazzocchi, A.; D’Oria, V.; Cosmi, V.D.; Bettocchi, S.; Milani, G.P.; Silano, M.; Agostoni, C. The role of lipids in human milk and infant formulae. Nutrients 2018, 10, 567. [Google Scholar] [CrossRef] [PubMed]
- Innis, S.M. Human milk: Maternal dietary lipids and infant development. Proc. Nutr. Soc. 2007, 66, 397–404. [Google Scholar] [CrossRef] [PubMed]
- Kilari, A.S.; Mehendale, S.S.; Dangat, K.D.; Yadav, H.R.; Gupta, A.; Taralekar, V.S.; Joshi, S.R. Long chain polyunsaturated fatty acids in mothers of preterm babies. J. Perinat. Med. 2010, 38, 659–664. [Google Scholar] [CrossRef]
- Duttaroy, A.K.; Basak, S. Maternal dietary fatty acids and their roles in human placental development. Prostaglandins Leukot. Essent. Fatty Acids 2020, 155, 102080. [Google Scholar] [CrossRef]
- Van Elten, T.M.; van Rossem, L.; Wijga, A.H.; Brunekreef, B.; De Jongste, J.C.; Koppelman, G.H.; Smit, H.A. Breast milk fatty acid composition has a long-term effect on the risk of asthma, eczema, and sensitization. Allergy 2015, 70, 1468–1476. [Google Scholar] [CrossRef]
- Hurtado, J.A.; Iznaola, C.; Peña, M.; Ruíz, J.; Peña-Quintana, L.; Kajarabille, N.; Rodriguez-Santana, Y.; Sanjurjo, P.; Aldámiz-Echevarría, L.; Ochoa, J.; et al. Effects of maternal Ω-3 supplementation on fatty acids and on visual and cognitive development. J. Pediatr. Gastroenterol. Nutr. 2015, 61, 472–480. [Google Scholar] [CrossRef]
- Schanler, R.J.; Hurst, N.M.; Lau, C. The use of human milk and breastfeeding in premature infants. Clin. Perinatol. 1999, 26, 379–398. [Google Scholar] [CrossRef]
- Callen, J.; Pinelli, J. A review of the literature examining the benefits and challenges, incidence and duration, and barriers to breastfeeding in preterm infants. Adv. Neonatal. Care 2005, 5, 72–88. [Google Scholar] [CrossRef]
- Ziegler, E.E. Human milk and human milk fortifiers. Nutr. Care Preterm Infants 2014, 110, 215–227. [Google Scholar] [CrossRef]
- Ehrenkranz, R.A.; Dusick, A.M.; Vohr, B.R.; Wright, L.L.; Wrage, L.A.; Poole, W.K.; National Institutes of Child Health and Human Development Neonatal Research Network. Growth in the neonatal intensive care unit influences neurodevelopmental and growth outcomes of extremely low birth weight infants. Pediatrics 2006, 117, 1253–1261. [Google Scholar] [CrossRef] [PubMed]
- Quigley, M.; Embleton, N.D.; McGuire, W. Formula versus donor breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst. Rev. 2018, 6, CD002971. [Google Scholar] [CrossRef]
- Moltó-Puigmartí, C.; Castellote, A.I.; Carbonell-Estrany, X.; López-Sabater, M.C. Differences in fat content and fatty acid proportions among colostrum, transitional, and mature milk from women delivering very preterm, preterm, and term infants. Clin. Nutr. 2011, 30, 116–123. [Google Scholar] [CrossRef] [PubMed]
- Dror, D.K.; Allen, L.H. Overview of nutrients in human milk. Adv. Nutr. 2018, 9 (Suppl. S1), 278S–294S. [Google Scholar] [CrossRef] [PubMed]
- Innis, S.M. Polyunsaturated fatty acids in human milk: An essential role in infant development. Adv. Exp. Med. Biol. 2004, 554, 27–43. [Google Scholar] [PubMed]
- Ahmed, B.; Freije, A.; Alhakim, F.; Alhaddad, F.; Elbehery, A.; Perna, S. The Effects of Energy and Macronutrient Content of Human Milk on the Growth of Preterm Infants: A Prospective Cohort Pilot Study. Bahrain Med. Bull. 2021, 43, 560–566. [Google Scholar]
- Patel, A.L.; Engstrom, J.L.; Meier, P.P.; Jegier, B.J.; Kimura, R.E. Calculating postnatal growth velocity in very low birth weight (VLBW) premature infants. J. Perinatol. 2009, 29, 618–622. [Google Scholar] [CrossRef]
- Ballard, O.; Morrow, A.L. Human milk composition: Nutrients and bioactive factors. Pediatr. Clin. N. Am. 2013, 60, 49–74. [Google Scholar] [CrossRef]
- Folch, J.; Lees, M.; Stanley, G.S. A simple method for the isolation and purification of total lipides from animal tissues. J. Biol. Chem. 1957, 226, 497–509. [Google Scholar] [CrossRef]
- Ozogul, Y.; Şimşek, A.; BalIkçI, E.; Kenar, M. The effects of extraction methods on the contents of fatty acids, especially EPA and DHA in marine lipids. Int. J. Food Sci. Nutr. 2012, 63, 326–331. [Google Scholar] [CrossRef] [PubMed]
- Association of Official Analytical Chemists. Official Methods of Analysis: Changes in Official Methods of Analysis Made at the Annual Meeting; Association of Official Analytical Chemists: Rockville, ML, USA, 1990. [Google Scholar]
- Thakkar, S.K.; De Castro, C.A.; Beauport, L.; Tolsa, J.F.; Fischer Fumeaux, C.J.; Affolter, M.; Giuffrida, F. Temporal progression of fatty acids in preterm and term human milk of mothers from Switzerland. Nutrients 2019, 11, 112. [Google Scholar] [CrossRef] [PubMed]
- Wan, Z.X.; Wang, X.L.; Xu, L.; Geng, Q.; Zhang, Y. Lipid content and fatty acids composition of mature human milk in rural North China. Br. J. Nutr. 2010, 103, 913–916. [Google Scholar] [CrossRef]
- Miliku, K.; Duan, Q.L.; Moraes, T.J.; Becker, A.B.; Mandhane, P.J.; Turvey, S.E.; Lefebvre, D.L.; Sears, M.R.; Subbarao, P.; Field, C.J.; et al. Human milk fatty acid composition is associated with dietary, genetic, sociodemographic, and environmental factors in the CHILD Cohort Study. Am. J. Clin. Nutr. 2019, 110, 1370–1383. [Google Scholar] [CrossRef] [PubMed]
- Donnelly, K.L.; Smith, C.I.; Schwarzenberg, S.J.; Jessurun, J.; Boldt, M.D.; Parks, E.J. Sources of fatty acids stored in liver and secreted via lipoproteins in patients with nonalcoholic fatty liver disease. J. Clin. Investig. 2005, 115, 1343–1351. [Google Scholar] [CrossRef]
- Innis, S.M. Dietary triacylglycerol structure and its role in infant nutrition. Adv. Nutr. 2011, 2, 275–283. [Google Scholar] [CrossRef]
- Kashyap, S.; Towers, H.M.; Sahni, R.; Ohira-Kist, K.; Abildskov, K.; Schulze, K.F. Effects of quality of energy on substrate oxidation in enterally fed, low-birth-weight infants. Am. J. Clin. Nutr. 2001, 74, 374–380. [Google Scholar] [CrossRef]
- Koletzko, B. Human milk lipids. Ann. Nutr. Metab. 2016, 69 (Suppl. S2), 27–40. [Google Scholar] [CrossRef]
- Bzikowska-Jura, A.; Czerwonogrodzka-Senczyna, A.; Jasińska-Melon, E.; Mojska, H.; Olędzka, G.; Wesołowska, A.; Szostak-Węgierek, D. The concentration of omega-3 fatty acids in human milk is related to their habitual but not current intake. Nutrients 2019, 11, 1585. [Google Scholar] [CrossRef]
- Freitas, R.F.; Macedo, M.D.; Lessa, A.D.; Ferraz, V.P.; Soares, N.O.; Martins, B.E.; Pinto, N.A.; Teixeira, R.A. Composition in fatty acids of mature milk of nursing mothers. Rev. Bras. Saúde Matern. Infant. 2020, 19, 817–825. [Google Scholar] [CrossRef]
- Gobbetti, T.; Ducheix, S.; Le Faouder, P.; Perez, T.; Riols, F.; Boué, J.; Bertrand-Michel, J.; Dubourdeau, M.; Guillou, H.; Perretti, M.; et al. Protective effects of n-6 fatty acids-enriched diet on intestinal ischaemia/reperfusion injury involve lipoxin A 4 and its receptor. Br. J. Pharmacol. 2015, 172, 910–923. [Google Scholar] [CrossRef] [PubMed]
- Freije, A. Fatty acid profile of the erythrocyte membranes of healthy Bahraini citizens in comparison with coronary heart disease patients. J. Oleo Sci. 2009, 58, 379–388. [Google Scholar] [CrossRef] [PubMed]
- Ehrenkranz, R.A.; Younes, N.; Lemons, J.A.; Fanaroff, A.A.; Donovan, E.F.; Wright, L.L.; Katsikiotis, V.; Tyson, J.E.; Oh, W.; Shankaran, S.; et al. Longitudinal growth of hospitalized very low birth weight infants. Pediatrics 1999, 104, 280–289. [Google Scholar] [CrossRef] [PubMed]
- Much, D.; Brunner, S.; Vollhardt, C.; Schmid, D.; Sedlmeier, E.-M.; Brüderl, M.; Heimberg, E.; Bartke, N.; Boehm, G.; Bader, B.L.; et al. Breast milk fatty acid profile in relation to infant growth and body composition: Results from the INFAT study. Pediatr. Res. 2013, 74, 230–237. [Google Scholar] [CrossRef] [PubMed]
- Simopoulos, A.P. Importance of the omega-6/omega-3 balance in health and disease: Evolutionary aspects of diet. In Healthy Agriculture, Healthy Nutrition, Healthy People; Karger Publishers: Basel, Switzerland, 2011; Volume 102, pp. 10–21. [Google Scholar]
- Simopoulos, A.P. An increase in the omega-6/omega-3 fatty acid ratio increases the risk for obesity. Nutrients 2016, 8, 128. [Google Scholar] [CrossRef]
- Chaves, H.; Singh, R.B.; Khan, S.; Wilczynska, A.; Takahashi, T. High omega-6/omega-3 fatty acid ratio diets and risk of noncommunicable diseases: Is the tissue, the main issue? In The Role of Functional Food Security in Global Health; Academic Press: Cambridge, MA, USA, 2019; pp. 217–259. [Google Scholar] [CrossRef]
- Saini, R.K.; Keum, Y.S. Omega-3 and omega-6 polyunsaturated fatty acids: Dietary sources, metabolism, and significance—A review. Life Sci. 2018, 203, 255–267. [Google Scholar] [CrossRef]
- Bhardwaj, K.; Verma, N.; Trivedi, R.K.; Bhardwaj, S.; Shukla, N. Significance of ratio of omega-3 and omega-6 in human health with special reference to flaxseed oil. Int. J. Biol. Chem. 2016, 10, 1–6. [Google Scholar] [CrossRef]
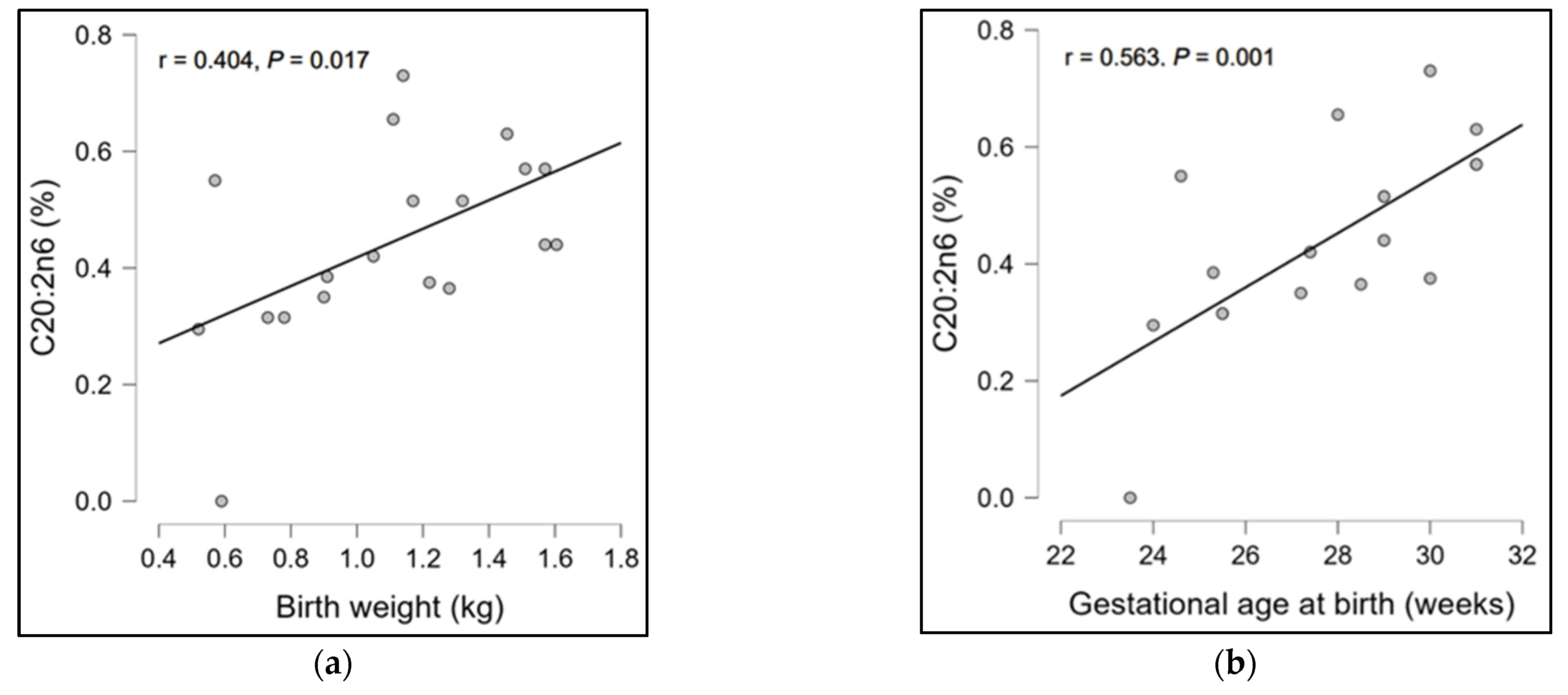
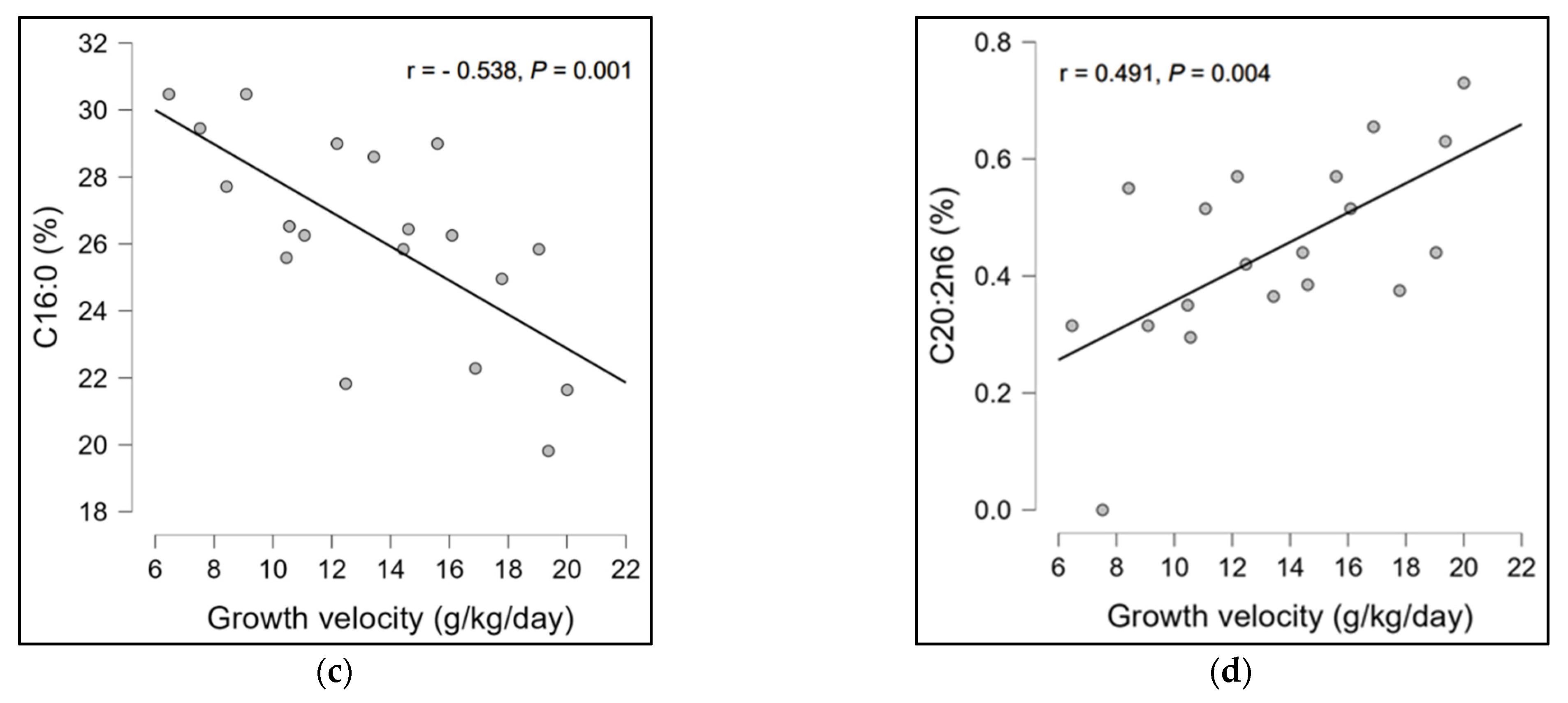
| Characteristic | Mean ± SD |
|---|---|
| Gestational age at birth (weeks) | 28.09 ± 2.33 |
| Birth weight (kg) | 1.14 ± 0.353 |
| Growth velocity (GV) (g/kg/day) | 13.85 ± 4.10 |
| Head circumference growth rate (HC) (cm/week) | 0.63 ± 0.18 |
| Total lipids (g/100 mL) | 3.61 ± 1.57 |
| Fatty Acids Classes | Mean ± SD mg/100 mL | Mean ± SD % |
|---|---|---|
| Σ SFAs | 852.10 ± 234.80 | 43.54 ± 11.16 |
| Σ UFAs | 1079.02 ± 227.05 | 52.22 ±10.89 |
| Σ MUFAs | 761.02 ± 291.28 | 36.52 ± 13.90 |
| Σ PUFAs | 318.00 ± 142.92 | 15.70 ± 7.10 |
| Σ n-6 | 307.98 ± 165.59 | 15.23 ±8.23 |
| Σ n-3 | 10.02 ± 6.84 | 0.46 ± 0.18 |
| n-6/n-3 ratio | 30.73:1 | 32.83:1 |
| Fatty Acids | mg/100 mL of Human Milk | % of Fatty Acids | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Mean | Var | SD | Min | Max | Mean | Var | SD | Min | Max | |
| 14:0 | 211.60 | 6848.97 | 82.76 | 61.96 | 335.51 | 11.67 | 17.70 | 4.21 | 6.03 | 19.01 |
| 16:0 | 526.41 | 54,281.49 | 232.98 | 114.12 | 955.30 | 26.12 | 11.37 | 3.37 | 19.82 | 31.47 |
| 16:1n9 | 50.83 | 769.71 | 27.74 | 10.31 | 103.08 | 2.51 | 0.55 | 0.74 | 0.57 | 3.41 |
| 16:1n7 | 6.04 | 111.35 | 10.55 | 0.78 | 44.97 | 0.27 | 0.18 | 0.42 | 0.09 | 1.85 |
| 18:0 | 107.91 | 2380.59 | 48.79 | 27.36 | 179.40 | 5.43 | 0.79 | 0.89 | 3.93 | 7.06 |
| 18:1n9 | 672.33 | 113,088.66 | 336.29 | 103.54 | 1301.31 | 32.12 | 16.62 | 4.08 | 26.04 | 41.30 |
| 18:1n7 | 21.45 | 221.37 | 14.88 | 6.43 | 66.54 | 1.13 | 0.24 | 0.49 | 0.38 | 1.93 |
| 18:2n6 | 293.85 | 20,688.57 | 143.84 | 42.66 | 550.22 | 14.58 | 10.38 | 3.22 | 11.01 | 21.42 |
| 18:3n6 | 5.17 | 22.55 | 4.75 | 0.00 | 20.35 | 0.22 | 0.03 | 0.18 | 0.00 | 0.84 |
| 18:3n3 | 10.02 | 46.82 | 6.84 | 1.32 | 28.36 | 0.46 | 0.03 | 0.18 | 0.27 | 0.90 |
| 20:0 | 6.18 | 10.68 | 3.27 | 1.63 | 13.45 | 0.33 | 0.01 | 0.11 | 0.18 | 0.61 |
| 20:1n9 | 10.37 | 29.50 | 5.43 | 0.00 | 22.36 | 0.50 | 0.04 | 0.20 | 0.00 | 0.82 |
| 20:2n6 | 8.96 | 22.40 | 4.73 | 0.00 | 18.96 | 0.43 | 0.03 | 0.18 | 0.00 | 0.73 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ahmed, B.; Freije, A.; Omran, A.; Rondanelli, M.; Marino, M.; Perna, S. Human Milk Fatty Acid Composition and Its Effect on Preterm Infants’ Growth Velocity. Children 2023, 10, 939. https://doi.org/10.3390/children10060939
Ahmed B, Freije A, Omran A, Rondanelli M, Marino M, Perna S. Human Milk Fatty Acid Composition and Its Effect on Preterm Infants’ Growth Velocity. Children. 2023; 10(6):939. https://doi.org/10.3390/children10060939
Chicago/Turabian StyleAhmed, Batool, Afnan Freije, Amina Omran, Mariangela Rondanelli, Mirko Marino, and Simone Perna. 2023. "Human Milk Fatty Acid Composition and Its Effect on Preterm Infants’ Growth Velocity" Children 10, no. 6: 939. https://doi.org/10.3390/children10060939
APA StyleAhmed, B., Freije, A., Omran, A., Rondanelli, M., Marino, M., & Perna, S. (2023). Human Milk Fatty Acid Composition and Its Effect on Preterm Infants’ Growth Velocity. Children, 10(6), 939. https://doi.org/10.3390/children10060939






