Modern Paediatric Emergency Department: Potential Improvements in Light of New Evidence
Abstract
1. Introduction
2. How to Optimise Workflow in Paediatric Emergency Departments?
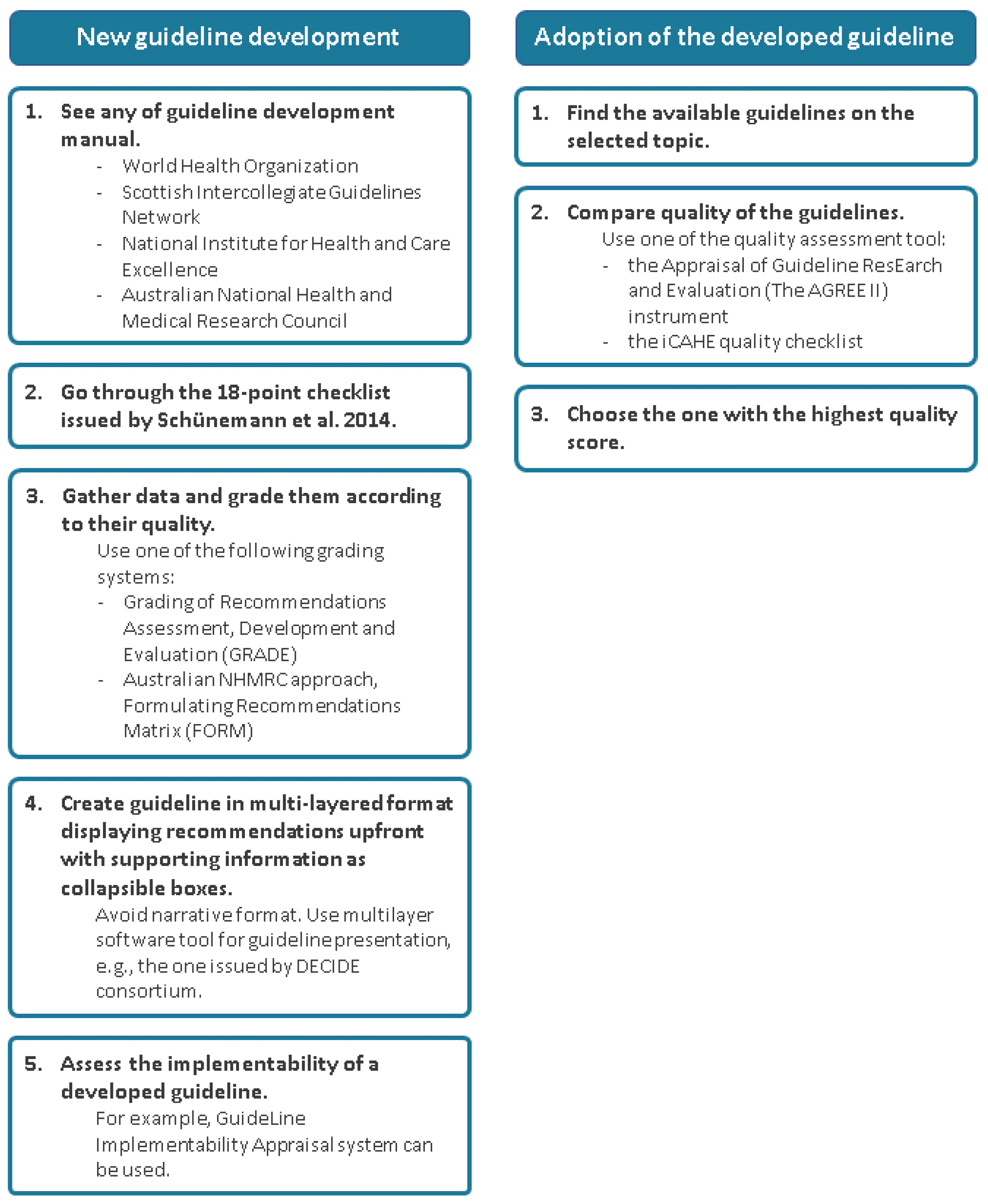
3. How to Optimise the Use of Structural Approach?
4. How to Rationalise the Use of Imaging Methods?
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lindner, G.; Woitok, B.K. Emergency Department Overcrowding. Wien. Klin. Wochenschr. 2021, 133, 229–233. [Google Scholar] [CrossRef] [PubMed]
- Moylan, A.; Maconochie, I. Demand, Overcrowding and the Pediatric Emergency Department. CMAJ 2019, 191, E625–E626. [Google Scholar] [CrossRef] [PubMed]
- Westbrook, J.I.; Raban, M.Z.; Walter, S.R.; Douglas, H. Task Errors by Emergency Physicians Are Associated with Interruptions, Multitasking, Fatigue and Working Memory Capacity: A Prospective, Direct Observation Study. BMJ Qual. Saf. 2018, 27, 655–663. [Google Scholar] [CrossRef] [PubMed]
- Doan, Q.; Wong, H.; Meckler, G.; Johnson, D.; Stang, A.; Dixon, A.; Sawyer, S.; Principi, T.; Kam, A.J.; Joubert, G.; et al. The Impact of Pediatric Emergency Department Crowding on Patient and Health Care System Outcomes: A Multicentre Cohort Study. CMAJ 2019, 191, E627–E635. [Google Scholar] [CrossRef]
- Kennebeck, S.S.; Timm, N.L.; Kurowski, E.M.; Byczkowski, T.L.; Reeves, S.D. The Association of Emergency Department Crowding and Time to Antibiotics in Febrile Neonates. Acad. Emerg. Med. 2011, 18, 1380–1385. [Google Scholar] [CrossRef]
- Shenoi, R.; Ma, L.; Syblik, D.; Yusuf, S. Emergency Department Crowding and Analgesic Delay in Pediatric Sickle Cell Pain Crises. Pediatr. Emerg. Care 2011, 27, 911–917. [Google Scholar] [CrossRef]
- Sills, M.R.; Fairclough, D.; Ranade, D.; Kahn, M.G. Emergency Department Crowding Is Associated with Decreased Quality of Care for Children with Acute Asthma. Ann. Emerg. Med. 2011, 57, e1–e7. [Google Scholar] [CrossRef]
- Jung, H.M.; Kim, M.J.; Kim, J.H.; Park, Y.S.; Chung, H.S.; Chung, S.P.; Lee, J.H. The Effect of Overcrowding in Emergency Departments on the Admission Rate According to the Emergency Triage Level. PLoS ONE 2021, 16, e0247042. [Google Scholar] [CrossRef]
- Weiss, S.J.; Ernst, A.A.; Sills, M.R.; Quinn, B.J.; Johnson, A.; Nick, T.G. Development of a Novel Measure of Overcrowding in a Pediatric Emergency Department. Pediatr. Emerg. Care 2007, 23, 641–645. [Google Scholar] [CrossRef]
- Noel, G.; Jouve, E.; Fruscione, S.; Minodier, P.; Boiron, L.; Viudes, G.; Gentile, S. Real-Time Measurement of Crowding in Pediatric Emergency Department: Derivation and Validation Using Consensual Perception of Crowding (SOTU-PED). Pediatr. Emerg. Care 2021, 37, e1244–e1250. [Google Scholar] [CrossRef]
- Abudan, A.; Merchant, R.C. Multi-Dimensional Measurements of Crowding for Pediatric Emergency Departments: A Systematic Review. Glob. Pediatr. Health 2021, 8, 2333794X21999153. [Google Scholar] [CrossRef]
- Oredsson, S.; Jonsson, H.; Rognes, J.; Lind, L.; Göransson, K.E.; Ehrenberg, A.; Asplund, K.; Castrén, M.; Farrohknia, N. A Systematic Review of Triage-Related Interventions to Improve Patient Flow in Emergency Departments. Scand. J. Trauma Resusc. Emerg. Med. 2011, 19, 43. [Google Scholar] [CrossRef]
- Weinick, R.M.; Burns, R.M.; Mehrotra, A. Many Emergency Department Visits Could Be Managed at Urgent Care Centers and Retail Clinics. Health Aff. 2010, 29, 1630–1636. [Google Scholar] [CrossRef]
- Hampers, L.C.; Cha, S.; Gutglass, D.J.; Binns, H.J.; Krug, S.E. Fast Track and the Pediatric Emergency Department: Resource Utilization and Patient Outcomes. Acad. Emerg. Med. 1999, 6, 1153–1159. [Google Scholar] [CrossRef]
- Hinson, J.S.; Martinez, D.A.; Cabral, S.; George, K.; Whalen, M.; Hansoti, B.; Levin, S. Triage Performance in Emergency Medicine: A Systematic Review. Ann. Emerg. Med. 2019, 74, 140–152. [Google Scholar] [CrossRef]
- Ebrahimi, M.; Mirhaghi, A.; Najafi, Z.; Shafaee, H.; Hamechizfahm Roudi, M. Are Pediatric Triage Systems Reliable in the Emergency Department? Emerg. Med. Int. 2020, 2020, 9825730. [Google Scholar] [CrossRef]
- FitzGerald, G.; Jelinek, G.A.; Scott, D.; Gerdtz, M.F. Emergency Department Triage Revisited. Emerg. Med. J. 2010, 27, 86–92. [Google Scholar] [CrossRef]
- Jeyaraman, M.M.; Alder, R.N.; Copstein, L.; Al-Yousif, N.; Suss, R.; Zarychanski, R.; Doupe, M.B.; Berthelot, S.; Mireault, J.; Tardif, P.; et al. Impact of Employing Primary Healthcare Professionals in Emergency Department Triage on Patient Flow Outcomes: A Systematic Review and Meta-Analysis. BMJ Open 2022, 12, e052850. [Google Scholar] [CrossRef]
- Abdulwahid, M.A.; Booth, A.; Kuczawski, M.; Mason, S.M. The Impact of Senior Doctor Assessment at Triage on Emergency Department Performance Measures: Systematic Review and Meta-Analysis of Comparative Studies. Emerg. Med. J. 2016, 33, 504–513. [Google Scholar] [CrossRef]
- Kuo, Y.-H.; Chan, N.B.; Leung, J.M.Y.; Meng, H.; So, A.M.-C.; Tsoi, K.K.F.; Graham, C.A. An Integrated Approach of Machine Learning and Systems Thinking for Waiting Time Prediction in an Emergency Department. Int. J. Med. Inform. 2020, 139, 104143. [Google Scholar] [CrossRef]
- Levin, S.; Toerper, M.; Hamrock, E.; Hinson, J.S.; Barnes, S.; Gardner, H.; Dugas, A.; Linton, B.; Kirsch, T.; Kelen, G. Machine-Learning-Based Electronic Triage More Accurately Differentiates Patients With Respect to Clinical Outcomes Compared With the Emergency Severity Index. Ann. Emerg. Med. 2018, 71, 565–574.e2. [Google Scholar] [CrossRef] [PubMed]
- Boonstra, A.; Laven, M. Influence of Artificial Intelligence on the Work Design of Emergency Department Clinicians a Systematic Literature Review. BMC Health Serv. Res. 2022, 22, 669. [Google Scholar] [CrossRef] [PubMed]
- Worster, A.; Gilboy, N.; Fernandes, C.M.; Eitel, D.; Eva, K.; Geisler, R.; Tanabe, P. Assessment of Inter-Observer Reliability of Two Five-Level Triage and Acuity Scales: A Randomized Controlled Trial. CJEM 2004, 6, 240–245. [Google Scholar] [CrossRef] [PubMed]
- Recznik, C.T.; Simko, L.M. Pediatric Triage Education: An Integrative Literature Review. J. Emerg. Nurs. 2018, 44, 605–613.e9. [Google Scholar] [CrossRef]
- Cicero, M.X.; Auerbach, M.A.; Zigmont, J.; Riera, A.; Ching, K.; Baum, C.R. Simulation Training with Structured Debriefing Improves Residents’ Pediatric Disaster Triage Performance. Prehospital Disaster Med. 2012, 27, 239–244. [Google Scholar] [CrossRef]
- Cicero, M.X.; Whitfill, T.; Overly, F.; Baird, J.; Walsh, B.; Yarzebski, J.; Riera, A.; Adelgais, K.; Meckler, G.D.; Baum, C.; et al. Pediatric Disaster Triage: Multiple Simulation Curriculum Improves Prehospital Care Providers’ Assessment Skills. Prehospital Emerg. Care 2017, 21, 201–208. [Google Scholar] [CrossRef]
- Sanddal, T.L.; Loyacono, T.; Sanddal, N.D. Effect of JumpSTART Training on Immediate and Short-Term Pediatric Triage Performance. Pediatr. Emerg. Care 2004, 20, 749–753. [Google Scholar] [CrossRef]
- Tuyisenge, L.; Kyamanya, P.; Van Steirteghem, S.; Becker, M.; English, M.; Lissauer, T. Knowledge and Skills Retention Following Emergency Triage, Assessment and Treatment plus Admission Course for Final Year Medical Students in Rwanda: A Longitudinal Cohort Study. Arch. Dis. Child. 2014, 99, 993–997. [Google Scholar] [CrossRef]
- Alberti, S.G. Transforming Emergency Care in England 2004. Available online: http://aace.org.uk/wp-content/uploads/2011/11/Transforming-Emergency-Care-in-England.pdf (accessed on 20 March 2023).
- Lamont, S.S. “See and Treat”: Spreading like Wildfire? A Qualitative Study into Factors Affecting Its Introduction and Spread. Emerg. Med. J. 2005, 22, 548–552. [Google Scholar] [CrossRef]
- Sakr, M.; Angus, J.; Perrin, J.; Nixon, C.; Nicholl, J.; Wardrope, J. Care of Minor Injuries by Emergency Nurse Practitioners or Junior Doctors: A Randomised Controlled Trial. Lancet 1999, 354, 1321–1326. [Google Scholar] [CrossRef]
- Blick, C.; Vinograd, A.; Chung, J.; Nguyen, E.; Abbadessa, M.K.F.; Gaines, S.; Chen, A. Procedural Competency for Ultrasound-Guided Peripheral Intravenous Catheter Insertion for Nurses in a Pediatric Emergency Department. J. Vasc. Access 2021, 22, 232–237. [Google Scholar] [CrossRef]
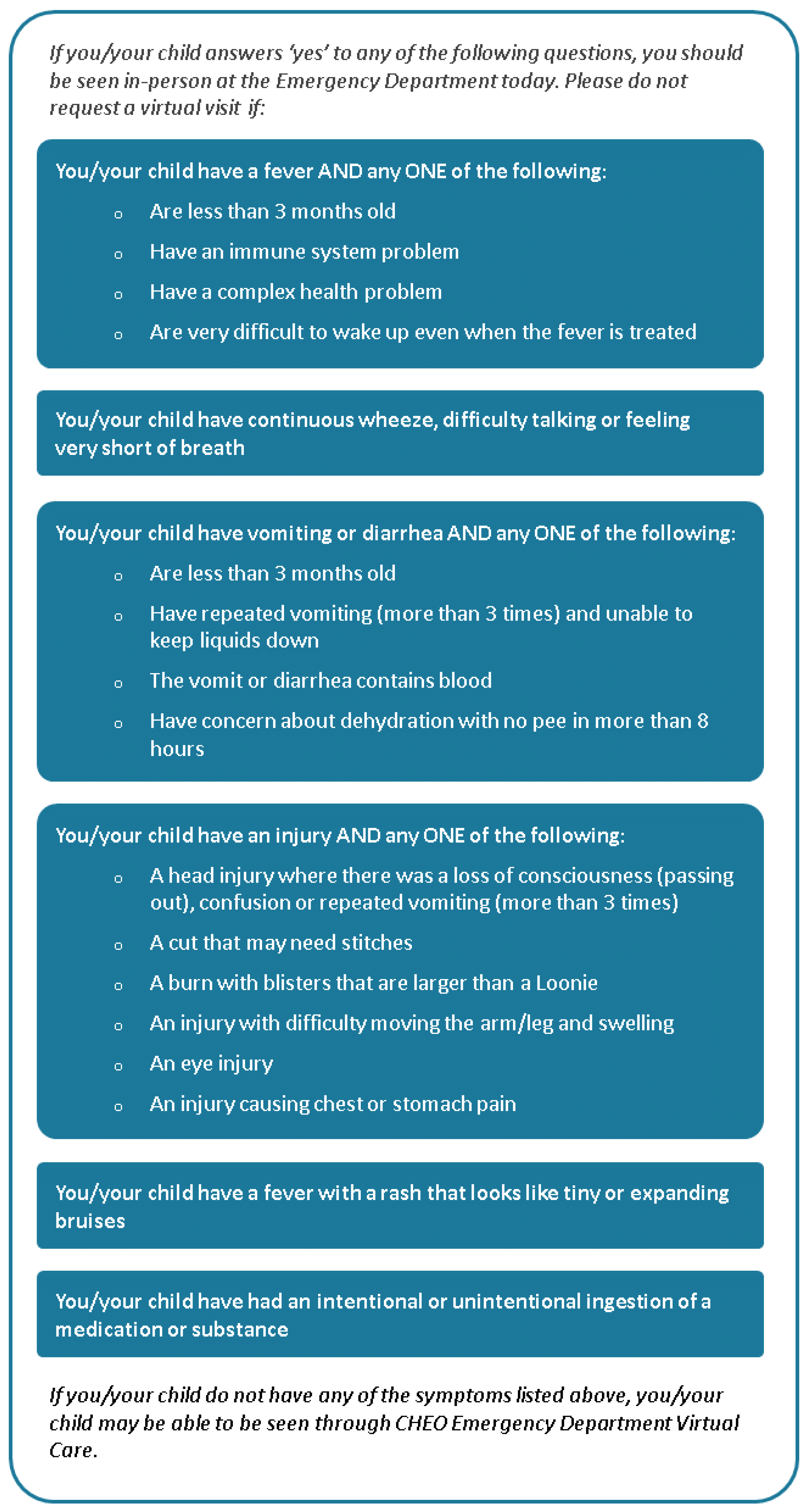
- Reid, S.; Bhatt, M.; Zemek, R.; Tse, S. Virtual Care in the Pediatric Emergency Department: A New Way of Doing Business? Can. J. Emerg. Med. 2021, 23, 80–84. [Google Scholar] [CrossRef]
- Brova, M.; Boggs, K.M.; Zachrison, K.S.; Freid, R.D.; Sullivan, A.F.; Espinola, J.A.; Boyle, T.P.; Camargo, C.A. Pediatric Telemedicine Use in United States Emergency Departments. Acad. Emerg. Med. 2018, 25, 1427–1432. [Google Scholar] [CrossRef]
- Cotton, J.; Bullard-Berent, J.; Sapien, R. Virtual Pediatric Emergency Department Telehealth Network Program: A Case Series. Pediatr. Emerg. Care 2020, 36, 217–221. [Google Scholar] [CrossRef]
- Stang, A.S.; McGillivray, D.; Bhatt, M.; Colacone, A.; Soucy, N.; Léger, R.; Afilalo, M. Markers of Overcrowding in a Pediatric Emergency Department. Acad. Emerg. Med. 2010, 17, 151–156. [Google Scholar] [CrossRef]
- Doan, Q.; Genuis, E.D.; Yu, A. Trends in Use in a Canadian Pediatric Emergency Department. CJEM 2014, 16, 405–410. [Google Scholar] [CrossRef]
- Ajmi, I.; Zgaya, H.; Gammoudi, L.; Hammadi, S.; Martinot, A.; Beuscart, R.; Renard, J.-M. Mapping Patient Path in the Pediatric Emergency Department: A Workflow Model Driven Approach. J. Biomed. Inform. 2015, 54, 315–328. [Google Scholar] [CrossRef]
- Aronsky, D.; Jones, I.; Lanaghan, K.; Slovis, C.M. Supporting Patient Care in the Emergency Department with a Computerized Whiteboard System. J. Am. Med. Inform. Assoc. 2008, 15, 184–194. [Google Scholar] [CrossRef]
- Hong, W.S.; Haimovich, A.D.; Taylor, R.A. Predicting Hospital Admission at Emergency Department Triage Using Machine Learning. PLoS ONE 2018, 13, e0201016. [Google Scholar] [CrossRef]
- Parker, C.A.; Liu, N.; Wu, S.X.; Shen, Y.; Lam, S.S.W.; Ong, M.E.H. Predicting Hospital Admission at the Emergency Department Triage: A Novel Prediction Model. Am. J. Emerg. Med. 2019, 37, 1498–1504. [Google Scholar] [CrossRef]
- Roquette, B.P.; Nagano, H.; Marujo, E.C.; Maiorano, A.C. Prediction of Admission in Pediatric Emergency Department with Deep Neural Networks and Triage Textual Data. Neural Netw. 2020, 126, 170–177. [Google Scholar] [CrossRef] [PubMed]
- Kadri, F.; Chaabane, S.; Tahon, C. A Simulation-Based Decision Support System to Prevent and Predict Strain Situations in Emergency Department Systems. Simul. Model. Pract. Theory 2014, 42, 32–52. [Google Scholar] [CrossRef]
- Mazzocato, P.; Holden, R.J.; Brommels, M.; Aronsson, H.; Bäckman, U.; Elg, M.; Thor, J. How Does Lean Work in Emergency Care? A Case Study of a Lean-Inspired Intervention at the Astrid Lindgren Children’s Hospital, Stockholm, Sweden. BMC Health Serv. Res. 2012, 12, 28. [Google Scholar] [CrossRef] [PubMed]
- Murrell, K.L.; Offerman, S.R.; Kauffman, M.B. Applying Lean: Implementation of a Rapid Triage and Treatment System. West J. Emerg. Med. 2011, 12, 184–191. [Google Scholar]
- Kuhlmann, S.; Piel, M.; Wolf, O.T. Impaired Memory Retrieval after Psychosocial Stress in Healthy Young Men. J. Neurosci. 2005, 25, 2977–2982. [Google Scholar] [CrossRef]
- Xiao, Y.; Mackenzie, C.F.; Group, L. Decision Making in Dynamic Environments: Fixation Errors and Their Causes. Proc. Hum. Factors Ergon. Soc. Annu. Meet. 1995, 39, 469–473. [Google Scholar] [CrossRef]
- Lingard, L.; Espin, S.; Whyte, S.; Regehr, G.; Baker, G.R.; Reznick, R.; Bohnen, J.; Orser, B.; Doran, D.; Grober, E. Communication Failures in the Operating Room: An Observational Classification of Recurrent Types and Effects. Qual. Saf. Health Care 2004, 13, 330–334. [Google Scholar] [CrossRef]
- Marshall, S.D.; Sanderson, P.; McIntosh, C.A.; Kolawole, H. The Effect of Two Cognitive Aid Designs on Team Functioning during Intra-Operative Anaphylaxis Emergencies: A Multi-Centre Simulation Study. Anaesthesia 2016, 71, 389–404. [Google Scholar] [CrossRef]
- Marshall, S.D.; Mehra, R. The Effects of a Displayed Cognitive Aid on Non-Technical Skills in a Simulated “can’t Intubate, Can’t Oxygenate” Crisis. Anaesthesia 2014, 69, 669–677. [Google Scholar] [CrossRef]
- Hepner, D.L.; Arriaga, A.F.; Cooper, J.B.; Goldhaber-Fiebert, S.N.; Gaba, D.M.; Berry, W.R.; Boorman, D.J.; Bader, A.M. Operating Room Crisis Checklists and Emergency Manuals. Anesthesiology 2017, 127, 384–392. [Google Scholar] [CrossRef]
- Weller, J.; Boyd, M. Making a Difference Through Improving Teamwork in the Operating Room: A Systematic Review of the Evidence on What Works. Curr. Anesthesiol. Rep. 2014, 4, 77–83. [Google Scholar] [CrossRef]
- Sacks, G.D.; Shannon, E.M.; Dawes, A.J.; Rollo, J.C.; Nguyen, D.K.; Russell, M.M.; Ko, C.Y.; Maggard-Gibbons, M.A. Teamwork, Communication and Safety Climate: A Systematic Review of Interventions to Improve Surgical Culture. BMJ Qual. Saf. 2015, 24, 458–467. [Google Scholar] [CrossRef]
- Hall, C.; Robertson, D.; Rolfe, M.; Pascoe, S.; Passey, M.E.; Pit, S.W. Do Cognitive Aids Reduce Error Rates in Resuscitation Team Performance? Trial of Emergency Medicine Protocols in Simulation Training (TEMPIST) in Australia. Hum. Resour. Health 2020, 18, 1. [Google Scholar] [CrossRef]
- McGlynn, E.A.; Asch, S.M.; Adams, J.; Keesey, J.; Hicks, J.; DeCristofaro, A.; Kerr, E.A. The Quality of Health Care Delivered to Adults in the United States. N. Engl. J. Med. 2003, 348, 2635–2645. [Google Scholar] [CrossRef]
- Sheldon, T.A.; Cullum, N.; Dawson, D.; Lankshear, A.; Lowson, K.; Watt, I.; West, P.; Wright, D.; Wright, J. What’s the Evidence That NICE Guidance Has Been Implemented? Results from a National Evaluation Using Time Series Analysis, Audit of Patients’ Notes, and Interviews. BMJ 2004, 329, 999. [Google Scholar] [CrossRef]
- Runciman, W.B.; Hunt, T.D.; Hannaford, N.A.; Hibbert, P.D.; Westbrook, J.I.; Coiera, E.W.; Day, R.O.; Hindmarsh, D.M.; McGlynn, E.A.; Braithwaite, J. CareTrack: Assessing the Appropriateness of Health Care Delivery in Australia. Med. J. Aust. 2012, 197, 100–105. [Google Scholar] [CrossRef]
- Sabharwal, S.; Patel, N.K.; Gauher, S.; Holloway, I.; Athanasiou, T.; Athansiou, T. High Methodologic Quality but Poor Applicability: Assessment of the AAOS Guidelines Using the AGREE II Instrument. Clin. Orthop. Relat. Res. 2014, 472, 1982–1988. [Google Scholar] [CrossRef]
- Hogeveen, S.E.; Han, D.; Trudeau–Tavara, S.; Buck, J.; Brezden–Masley, C.B.; Quan, M.L.; Simmons, C.E. Comparison of International Breast Cancer Guidelines: Are We Globally Consistent? Cancer Guideline AGREEment. Curr. Oncol. 2012, 19, e184–e190. [Google Scholar] [CrossRef]
- Sabharwal, S.; Patel, V.; Nijjer, S.S.; Kirresh, A.; Darzi, A.; Chambers, J.C.; Malik, I.; Kooner, J.S.; Athanasiou, T. Guidelines in Cardiac Clinical Practice: Evaluation of Their Methodological Quality Using the AGREE II Instrument. J. R. Soc. Med. 2013, 106, 315–322. [Google Scholar] [CrossRef]
- Knai, C.; Brusamento, S.; Legido-Quigley, H.; Saliba, V.; Panteli, D.; Turk, E.; Car, J.; McKee, M.; Busse, R. Systematic Review of the Methodological Quality of Clinical Guideline Development for the Management of Chronic Disease in Europe. Health Policy 2012, 107, 157–167. [Google Scholar] [CrossRef]
- Brosseau, L.; Rahman, P.; Toupin-April, K.; Poitras, S.; King, J.; De Angelis, G.; Loew, L.; Casimiro, L.; Paterson, G.; McEwan, J. A Systematic Critical Appraisal for Non-Pharmacological Management of Osteoarthritis Using the Appraisal of Guidelines Research and Evaluation II Instrument. PLoS ONE 2014, 9, e82986. [Google Scholar] [CrossRef] [PubMed]
- Jin, Y.; Tan, L.-M.; Khan, K.S.; Deng, T.; Huang, C.; Han, F.; Zhang, J.; Huang, Q.; Huang, D.; Wang, D.; et al. Determinants of Successful Guideline Implementation: A National Cross-Sectional Survey. BMC Med. Inform. Decis. Mak. 2021, 21, 19. [Google Scholar] [CrossRef] [PubMed]
- Kredo, T.; Bernhardsson, S.; Machingaidze, S.; Young, T.; Louw, Q.; Ochodo, E.; Grimmer, K. Guide to Clinical Practice Guidelines: The Current State of Play. Int. J. Qual. Health Care 2016, 28, 122–128. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Handbook for Guideline Development; World Health Organization: Geneva, Switzerland, 2014; ISBN 978-92-4-154896-0. [Google Scholar]
- Scottish Intercollegiate Guidelines Network. Sign 50: A Guideline Developer’s Handbook; Healthcare Improvement Scotland: Edinburgh, UK, 2014; ISBN 978-1-909103-30-6. [Google Scholar]
- National Institute for Health and Care Excellence. The Guidelines Manual; NICE Process and Methods Guides; National Institute for Health and Care Excellence (NICE): London, UK, 2012; ISBN 978-1-4731-1906-2. [Google Scholar]
- National Health & Medical Research Council (Australia), H.A.C. A Guide to the Development, Implementation and Evaluation of Clinical Practice Guidelines; AGPS: Canberra, Australia, 1999; ISBN 978-1-86496-048-8. [Google Scholar]
- Schünemann, H.J.; Wiercioch, W.; Etxeandia, I.; Falavigna, M.; Santesso, N.; Mustafa, R.; Ventresca, M.; Brignardello-Petersen, R.; Laisaar, K.-T.; Kowalski, S.; et al. Guidelines 2.0: Systematic Development of a Comprehensive Checklist for a Successful Guideline Enterprise. CMAJ 2014, 186, E123–E142. [Google Scholar] [CrossRef]
- Guyatt, G.H.; Oxman, A.D.; Vist, G.E.; Kunz, R.; Falck-Ytter, Y.; Alonso-Coello, P.; Schünemann, H.J.; GRADE Working Group. GRADE: An Emerging Consensus on Rating Quality of Evidence and Strength of Recommendations. BMJ 2008, 336, 924–926. [Google Scholar] [CrossRef]
- Hillier, S.; Grimmer-Somers, K.; Merlin, T.; Middleton, P.; Salisbury, J.; Tooher, R.; Weston, A. FORM: An Australian Method for Formulating and Grading Recommendations in Evidence-Based Clinical Guidelines. BMC Med. Res. Methodol. 2011, 11, 23. [Google Scholar] [CrossRef]
- Shiffman, R.N.; Dixon, J.; Brandt, C.; Essaihi, A.; Hsiao, A.; Michel, G.; O’Connell, R. The GuideLine Implementability Appraisal (GLIA): Development of an Instrument to Identify Obstacles to Guideline Implementation. BMC Med. Inform. Decis. Mak. 2005, 5, 23. [Google Scholar] [CrossRef]
- Brandt, L.; Vandvik, P.O.; Alonso-Coello, P.; Akl, E.A.; Thornton, J.; Rigau, D.; Adams, K.; O’Connor, P.; Guyatt, G.; Kristiansen, A. Multilayered and Digitally Structured Presentation Formats of Trustworthy Recommendations: A Combined Survey and Randomised Trial. BMJ Open 2017, 7, e011569. [Google Scholar] [CrossRef]
- Treweek, S.; Oxman, A.D.; Alderson, P.; Bossuyt, P.M.; Brandt, L.; Brożek, J.; Davoli, M.; Flottorp, S.; Harbour, R.; Hill, S.; et al. Developing and Evaluating Communication Strategies to Support Informed Decisions and Practice Based on Evidence (DECIDE): Protocol and Preliminary Results. Implement Sci. 2013, 8, 6. [Google Scholar] [CrossRef]
- Brouwers, M.C.; Kho, M.E.; Browman, G.P.; Burgers, J.S.; Cluzeau, F.; Feder, G.; Fervers, B.; Graham, I.D.; Hanna, S.E.; Makarski, J.; et al. Development of the AGREE II, Part 1: Performance, Usefulness and Areas for Improvement. CMAJ 2010, 182, 1045–1052. [Google Scholar] [CrossRef]
- Brouwers, M.C.; Kho, M.E.; Browman, G.P.; Burgers, J.S.; Cluzeau, F.; Feder, G.; Fervers, B.; Graham, I.D.; Hanna, S.E.; Makarski, J.; et al. Development of the AGREE II, Part 2: Assessment of Validity of Items and Tools to Support Application. CMAJ 2010, 182, E472–E478. [Google Scholar] [CrossRef]
- Chiappini, E.; Bortone, B.; Galli, L.; de Martino, M. Guidelines for the Symptomatic Management of Fever in Children: Systematic Review of the Literature and Quality Appraisal with AGREE II. BMJ Open 2017, 7, e015404. [Google Scholar] [CrossRef]
- Grimmer, K.; Dizon, J.M.; Milanese, S.; King, E.; Beaton, K.; Thorpe, O.; Lizarondo, L.; Luker, J.; Machotka, Z.; Kumar, S. Efficient Clinical Evaluation of Guideline Quality: Development and Testing of a New Tool. BMC Med. Res. Methodol. 2014, 14, 63. [Google Scholar] [CrossRef]
- Ben-Haddour, M.; Colas, M.; Lefevre-Scelles, A.; Durand, Z.; Gillibert, A.; Roussel, M.; Joly, L.-M. A Cognitive Aid Improves Adherence to Guidelines for Critical Endotracheal Intubation in the Resuscitation Room: A Randomized Controlled Trial With Manikin-Based In Situ Simulation. Simul. Healthc. 2021, 17, 156–162. [Google Scholar] [CrossRef]
- Koers, L.; van Haperen, M.; Meijer, C.G.F.; van Wandelen, S.B.E.; Waller, E.; Dongelmans, D.; Boermeester, M.A.; Hermanides, J.; Preckel, B. Effect of Cognitive Aids on Adherence to Best Practice in the Treatment of Deteriorating Surgical Patients: A Randomized Clinical Trial in a Simulation Setting. JAMA Surg. 2020, 155, e194704. [Google Scholar] [CrossRef]
- Haynes, A.B.; Weiser, T.G.; Berry, W.R.; Lipsitz, S.R.; Breizat, A.-H.S.; Dellinger, E.P.; Herbosa, T.; Joseph, S.; Kibatala, P.L.; Lapitan, M.C.M.; et al. A Surgical Safety Checklist to Reduce Morbidity and Mortality in a Global Population. N. Engl. J. Med. 2009, 360, 491–499. [Google Scholar] [CrossRef]
- Bergs, J.; Lambrechts, F.; Simons, P.; Vlayen, A.; Marneffe, W.; Hellings, J.; Cleemput, I.; Vandijck, D. Barriers and Facilitators Related to the Implementation of Surgical Safety Checklists: A Systematic Review of the Qualitative Evidence. BMJ Qual. Saf. 2015, 24, 776–786. [Google Scholar] [CrossRef]
- Burian, B.K.; Clebone, A.; Dismukes, K.; Ruskin, K.J. More Than a Tick Box: Medical Checklist Development, Design, and Use. Anesth. Analg. 2018, 126, 223–232. [Google Scholar] [CrossRef]
- Goldhaber-Fiebert, S.N.; Pollock, J.; Howard, S.K.; Bereknyei Merrell, S. Emergency Manual Uses During Actual Critical Events and Changes in Safety Culture From the Perspective of Anesthesia Residents: A Pilot Study. Anesth. Analg. 2016, 123, 641–649. [Google Scholar] [CrossRef]
- Watkins, S.C.; Anders, S.; Clebone, A.; Hughes, E.; Patel, V.; Zeigler, L.; Shi, Y.; Shotwell, M.S.; McEvoy, M.D.; Weinger, M.B. Mode of Information Delivery Does Not Effect Anesthesia Trainee Performance During Simulated Perioperative Pediatric Critical Events: A Trial of Paper Versus Electronic Cognitive Aids. Simul. Healthc. 2016, 11, 385–393. [Google Scholar] [CrossRef]
- Clebone, A.; Burian, B.K.; Watkins, S.C.; Gálvez, J.A.; Lockman, J.L.; Heitmiller, E.S.; Members of the Society for Pediatric Anesthesia Quality and Safety Committee (see Acknowledgments). The Development and Implementation of Cognitive Aids for Critical Events in Pediatric Anesthesia: The Society for Pediatric Anesthesia Critical Events Checklists. Anesth. Analg. 2017, 124, 900–907. [Google Scholar] [CrossRef] [PubMed]
- Marshall, S.D. Lost in Translation? Comparing the Effectiveness of Electronic-Based and Paper-Based Cognitive Aids. Br. J. Anaesth. 2017, 119, 869–871. [Google Scholar] [CrossRef] [PubMed]
- Grundgeiger, T.; Hahn, F.; Wurmb, T.; Meybohm, P.; Happel, O. The Use of a Cognitive Aid App Supports Guideline-Conforming Cardiopulmonary Resuscitations: A Randomized Study in a High-Fidelity Simulation. Resusc. Plus 2021, 7, 100152. [Google Scholar] [CrossRef] [PubMed]
- Lelaidier, R.; Balança, B.; Boet, S.; Faure, A.; Lilot, M.; Lecomte, F.; Lehot, J.-J.; Rimmelé, T.; Cejka, J.-C. Use of a Hand-Held Digital Cognitive Aid in Simulated Crises: The MAX Randomized Controlled Trial. BJA Br. J. Anaesth. 2017, 119, 1015–1021. [Google Scholar] [CrossRef]
- McEvoy, M.D.; Hand, W.R.; Stoll, W.D.; Furse, C.M.; Nietert, P.J. Adherence to Guidelines for the Management of Local Anesthetic Systemic Toxicity Is Improved by an Electronic Decision Support Tool and Designated ‘Reader’. Reg. Anesth. Pain Med. 2014, 39, 299–305. [Google Scholar] [CrossRef]
- Burden, A.R.; Carr, Z.J.; Staman, G.W.; Littman, J.J.; Torjman, M.C. Does Every Code Need a “Reader?” Improvement of Rare Event Management with a Cognitive Aid “Reader” during a Simulated Emergency: A Pilot Study. Simul. Healthc. 2012, 7, 1–9. [Google Scholar] [CrossRef]
- Reed, S.; Ganyani, R.; King, R.; Pandit, M. Does a Novel Method of Delivering the Safe Surgical Checklist Improve Compliance? A Closed Loop Audit. Int. J. Surg. 2016, 32, 99–108. [Google Scholar] [CrossRef]
- Safar, P.; Brown, T.C.; Holtey, W.J.; Wilder, R.J. Ventilation and Circulation with Closed-Chest Cardiac Massage in Man. JAMA 1961, 176, 574–576. [Google Scholar] [CrossRef]
- Moretti, M.A.; Cesar, L.A.M.; Nusbacher, A.; Kern, K.B.; Timerman, S.; Ramires, J.A.F. Advanced Cardiac Life Support Training Improves Long-Term Survival from in-Hospital Cardiac Arrest. Resuscitation 2007, 72, 458–465. [Google Scholar] [CrossRef]
- Peran, D.; Kodet, J.; Pekara, J.; Mala, L.; Truhlar, A.; Cmorej, P.C.; Lauridsen, K.G.; Sari, F.; Sykora, R. ABCDE Cognitive Aid Tool in Patient Assessment—Development and Validation in a Multicenter Pilot Simulation Study. BMC Emerg. Med. 2020, 20, 95. [Google Scholar] [CrossRef]
- Olgers, T.J.; Dijkstra, R.S.; Drost-de Klerck, A.M.; Ter Maaten, J.C. The ABCDE Primary Assessment in the Emergency Department in Medically Ill Patients: An Observational Pilot Study. Neth. J. Med. 2017, 75, 106–111. [Google Scholar]
- Weng, T.-I.; Huang, C.-H.; Ma, M.H.-M.; Chang, W.-T.; Liu, S.-C.; Wang, T.-D.; Chen, W.-J. Improving the Rate of Return of Spontaneous Circulation for Out-of-Hospital Cardiac Arrests with a Formal, Structured Emergency Resuscitation Team. Resuscitation 2004, 60, 137–142. [Google Scholar] [CrossRef]
- Ornato, J.P.; Peberdy, M.A.; Reid, R.D.; Feeser, V.R.; Dhindsa, H.S. Impact of Resuscitation System Errors on Survival from In-Hospital Cardiac Arrest. Resuscitation 2012, 83, 63–69. [Google Scholar] [CrossRef]
- Soar, J.; Böttiger, B.W.; Carli, P.; Couper, K.; Deakin, C.D.; Djärv, T.; Lott, C.; Olasveengen, T.; Paal, P.; Pellis, T.; et al. European Resuscitation Council Guidelines 2021: Adult Advanced Life Support. Resuscitation 2021, 161, 115–151. [Google Scholar] [CrossRef]
- Abdolrazaghnejad, A.; Banaie, M.; Safdari, M. Ultrasonography in Emergency Department; a Diagnostic Tool for Better Examination and Decision-Making. Adv. J. Emerg. Med. 2017, 2, e7. [Google Scholar] [CrossRef]
- Valle Alonso, J.; Turpie, J.; Farhad, I.; Ruffino, G. Protocols for Point-of-Care-Ultrasound (POCUS) in a Patient with Sepsis; An Algorithmic Approach. BEAT 2019, 7, 67–71. [Google Scholar] [CrossRef]
- Atkinson, P.R.; Milne, J.; Diegelmann, L.; Lamprecht, H.; Stander, M.; Lussier, D.; Pham, C.; Henneberry, R.; Fraser, J.M.; Howlett, M.K.; et al. Does Point-of-Care Ultrasonography Improve Clinical Outcomes in Emergency Department Patients With Undifferentiated Hypotension? An International Randomized Controlled Trial From the SHoC-ED Investigators. Ann. Emerg. Med. 2018, 72, 478–489. [Google Scholar] [CrossRef]
- Mosier, J.M.; Stolz, U.; Milligan, R.; Roy-Chaudhury, A.; Lutrick, K.; Hypes, C.D.; Billheimer, D.; Cairns, C.B. Impact of Point-of-Care Ultrasound in the Emergency Department on Care Processes and Outcomes in Critically Ill Nontraumatic Patients. Crit. Care Explor. 2019, 1, e0019. [Google Scholar] [CrossRef]
- Goldsmith, A.J.; Shokoohi, H.; Loesche, M.; Patel, R.C.; Kimberly, H.; Liteplo, A. Point-of-Care Ultrasound in Morbidity and Mortality Cases in Emergency Medicine: Who Benefits the Most? West J. Emerg. Med. 2020, 21, 172–178. [Google Scholar] [CrossRef]
- Ultrasound Guidelines: Emergency, Point-of-Care and Clinical Ultrasound Guidelines in Medicine. Ann. Emerg. Med. 2017, 69, e27–e54. [CrossRef]
- Vieira, R.L.; Hsu, D.; Nagler, J.; Chen, L.; Gallagher, R.; Levy, J.A. Pediatric Emergency Medicine Fellow Training in Ultrasound: Consensus Educational Guidelines. Acad. Emerg. Med. 2013, 20, 300–306. [Google Scholar] [CrossRef] [PubMed]
- Blehar, D.J.; Barton, B.; Gaspari, R.J. Learning Curves in Emergency Ultrasound Education. Acad. Emerg. Med. 2015, 22, 574–582. [Google Scholar] [CrossRef] [PubMed]
- Lewiss, R.E.; Hoffmann, B.; Beaulieu, Y.; Phelan, M.B. Point-of-Care Ultrasound Education. J. Ultrasound Med. 2014, 33, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Rao, S.; van Holsbeeck, L.; Musial, J.L.; Parker, A.; Bouffard, J.A.; Bridge, P.; Jackson, M.; Dulchavsky, S.A. A Pilot Study of Comprehensive Ultrasound Education at the Wayne State University School of Medicine. J. Ultrasound Med. 2008, 27, 745–749. [Google Scholar] [CrossRef]
- Bahner, D.P.; Royall, N.A. Advanced Ultrasound Training for Fourth-Year Medical Students: A Novel Training Program at The Ohio State University College of Medicine. Acad. Med. 2013, 88, 206–213. [Google Scholar] [CrossRef]
- Boccatonda, A. Emergency Ultrasound: Is It Time for Artificial Intelligence? JCM 2022, 11, 3823. [Google Scholar] [CrossRef]
- Nti, B.; Lehmann, A.S.; Haddad, A.; Kennedy, S.K.; Russell, F.M. Artificial Intelligence-Augmented Pediatric Lung POCUS: A Pilot Study of Novice Learners. J. Ultrasound Med. 2022, 41, 2965–2972. [Google Scholar] [CrossRef]
- Zhang, J.; Gajjala, S.; Agrawal, P.; Tison, G.H.; Hallock, L.A.; Beussink-Nelson, L.; Lassen, M.H.; Fan, E.; Aras, M.A.; Jordan, C.; et al. Fully Automated Echocardiogram Interpretation in Clinical Practice. Circulation 2018, 138, 1623–1635. [Google Scholar] [CrossRef]
- Zheng, X.; Yao, Z.; Huang, Y.; Yu, Y.; Wang, Y.; Liu, Y.; Mao, R.; Li, F.; Xiao, Y.; Wang, Y.; et al. Deep Learning Radiomics Can Predict Axillary Lymph Node Status in Early-Stage Breast Cancer. Nat. Commun. 2020, 11, 1236. [Google Scholar] [CrossRef]
- Chartier, L.B.; Bosco, L.; Lapointe-Shaw, L.; Chenkin, J. Use of Point-of-Care Ultrasound in Long Bone Fractures: A Systematic Review and Meta-Analysis. CJEM 2017, 19, 131–142. [Google Scholar] [CrossRef]
- Ozkaya, E.; Topal, F.E.; Bulut, T.; Gursoy, M.; Ozuysal, M.; Karakaya, Z. Evaluation of an Artificial Intelligence System for Diagnosing Scaphoid Fracture on Direct Radiography. Eur. J. Trauma Emerg. Surg. 2022, 48, 585–592. [Google Scholar] [CrossRef]
- Harjai, M.M.; Sharma, A.K. Head Injuries in Children: Role of X-ray Skull, CT Scan Brain and in-Hospital Observation. Med. J. Armed Forces India 1998, 54, 322–324. [Google Scholar] [CrossRef]
- Chawla, H.; Malhotra, R.; Yadav, R.K.; Griwan, M.S.; Paliwal, P.K.; Aggarwal, A.D. Diagnostic Utility of Conventional Radiography in Head Injury. J. Clin. Diagn. Res. 2015, 9, TC13–TC15. [Google Scholar] [CrossRef]
- Radiation Risks and Pediatric Computed Tomography—NCI. Available online: https://www.cancer.gov/about-cancer/causes-prevention/risk/radiation/pediatric-ct-scans (accessed on 18 July 2022).
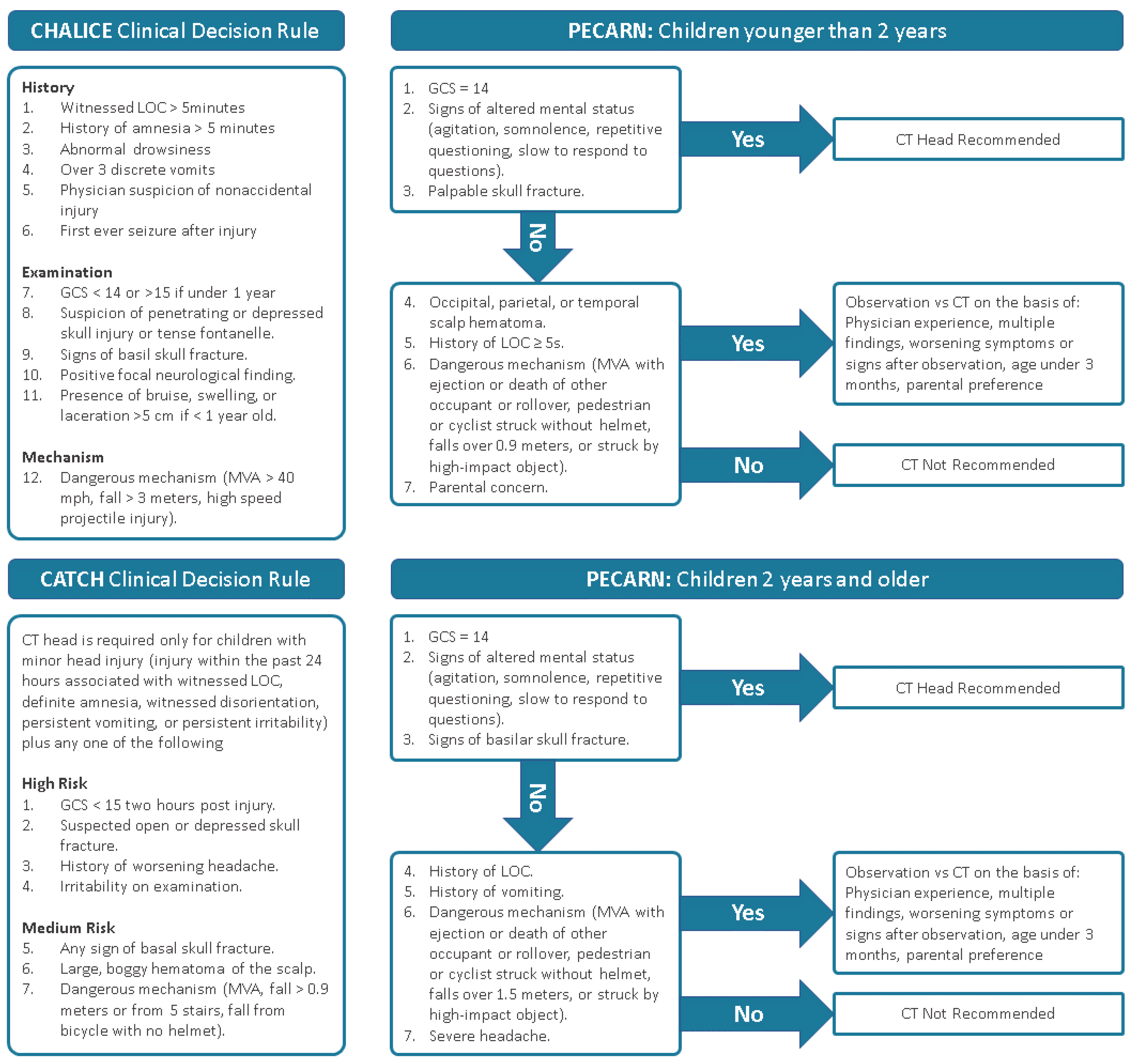
- McGraw, M.; Way, T. Comparison of PECARN, CATCH, and CHALICE Clinical Decision Rules for Pediatric Head Injury in the Emergency Department. CJEM 2019, 21, 120–124. [Google Scholar] [CrossRef]
- Easter, J.S.; Bakes, K.; Dhaliwal, J.; Miller, M.; Caruso, E.; Haukoos, J.S. Comparison of PECARN, CATCH, and CHALICE Rules for Children with Minor Head Injury: A Prospective Cohort Study. Ann. Emerg. Med. 2014, 64, 145–152.e1–e5. [Google Scholar] [CrossRef]
- Babl, F.E.; Borland, M.L.; Phillips, N.; Kochar, A.; Dalton, S.; McCaskill, M.; Cheek, J.A.; Gilhotra, Y.; Furyk, J.; Neutze, J.; et al. Accuracy of PECARN, CATCH, and CHALICE Head Injury Decision Rules in Children: A Prospective Cohort Study. Lancet 2017, 389, 2393–2402. [Google Scholar] [CrossRef]
- Schonfeld, D.; Bressan, S.; Da Dalt, L.; Henien, M.N.; Winnett, J.A.; Nigrovic, L.E. Pediatric Emergency Care Applied Research Network Head Injury Clinical Prediction Rules Are Reliable in Practice. Arch. Dis. Child. 2014, 99, 427–431. [Google Scholar] [CrossRef]
- Parri, N.; Crosby, B.J.; Glass, C.; Mannelli, F.; Sforzi, I.; Schiavone, R.; Ban, K.M. Ability of Emergency Ultrasonography to Detect Pediatric Skull Fractures: A Prospective, Observational Study. J. Emerg. Med. 2013, 44, 135–141. [Google Scholar] [CrossRef]

| Triage System | CTAS | ESI | MTS | ATS | SATS |
|---|---|---|---|---|---|
| Stated objective | Provide patients with timely care | Prioritise patients by immediacy of care needs and resource | Rapidly assess a patient and assign a priority based on clinical need | Ensure patients are treated in order of clinical urgency and allocate patients to the most appropriate treatment area | Prioritise patients based on medical urgency in contexts where there is a mismatch between demand and capacity |
| Recommended time to physician contact, min | 1: immediate | 1: immediate | Red: immediate | 1: immediate | Red: immediate |
| 2: ≤15 | 2: ≤15 | Orange: ≤10 | 2: ≤15 | Orange: ≤10 | |
| 3: ≤30 | 3: none | Yellow: ≤60 | 3: ≤30 | Yellow: ≤60 | |
| 4: ≤60 | 4: none | Green: ≤120 | 4: ≤60 | Green: ≤120 | |
| 5: ≤120 | 5: none | >Blue: ≤240 | 5: ≤120 | Blue: ≤240 | |
| Discriminators | |||||
| Clinical | Yes | No | Yes | Yes | Yes |
| Vital signs | Yes | Yes | Yes | Yes | Yes |
| Pain score | Yes (10-point) | Yes (visual scale) | Yes (3-point) | No | Yes (4-point) |
| Resource use | No | Yes | No | No | No |
| Paediatrics | Separate version | Separate vital sign differentiators | Considered within algorithm | Considered within algorithm | Separate flowchart |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kula, R.; Popela, S.; Klučka, J.; Charwátová, D.; Djakow, J.; Štourač, P. Modern Paediatric Emergency Department: Potential Improvements in Light of New Evidence. Children 2023, 10, 741. https://doi.org/10.3390/children10040741
Kula R, Popela S, Klučka J, Charwátová D, Djakow J, Štourač P. Modern Paediatric Emergency Department: Potential Improvements in Light of New Evidence. Children. 2023; 10(4):741. https://doi.org/10.3390/children10040741
Chicago/Turabian StyleKula, Roman, Stanislav Popela, Jozef Klučka, Daniela Charwátová, Jana Djakow, and Petr Štourač. 2023. "Modern Paediatric Emergency Department: Potential Improvements in Light of New Evidence" Children 10, no. 4: 741. https://doi.org/10.3390/children10040741
APA StyleKula, R., Popela, S., Klučka, J., Charwátová, D., Djakow, J., & Štourač, P. (2023). Modern Paediatric Emergency Department: Potential Improvements in Light of New Evidence. Children, 10(4), 741. https://doi.org/10.3390/children10040741






