Non-Alcoholic Fatty Liver Disease (NAFLD) and Potential Links to Depression, Anxiety, and Chronic Stress
Abstract
:1. Introduction
2. Methods
3. Depression
3.1. Depression/Anxiety and Metabolic Syndrome
3.2. Depression/Anxiety and NAFLD
4. Chronic Psychosocial Stress
4.1. Chronic Psychosocial Stress and Metabolic Syndrome
4.2. Chronic Psychosocial Stress and NAFLD
5. Health Related Quality of Life (HRQoL)
5.1. HRQoL and Metabolic Syndrome
5.2. HRQoL and NAFLD
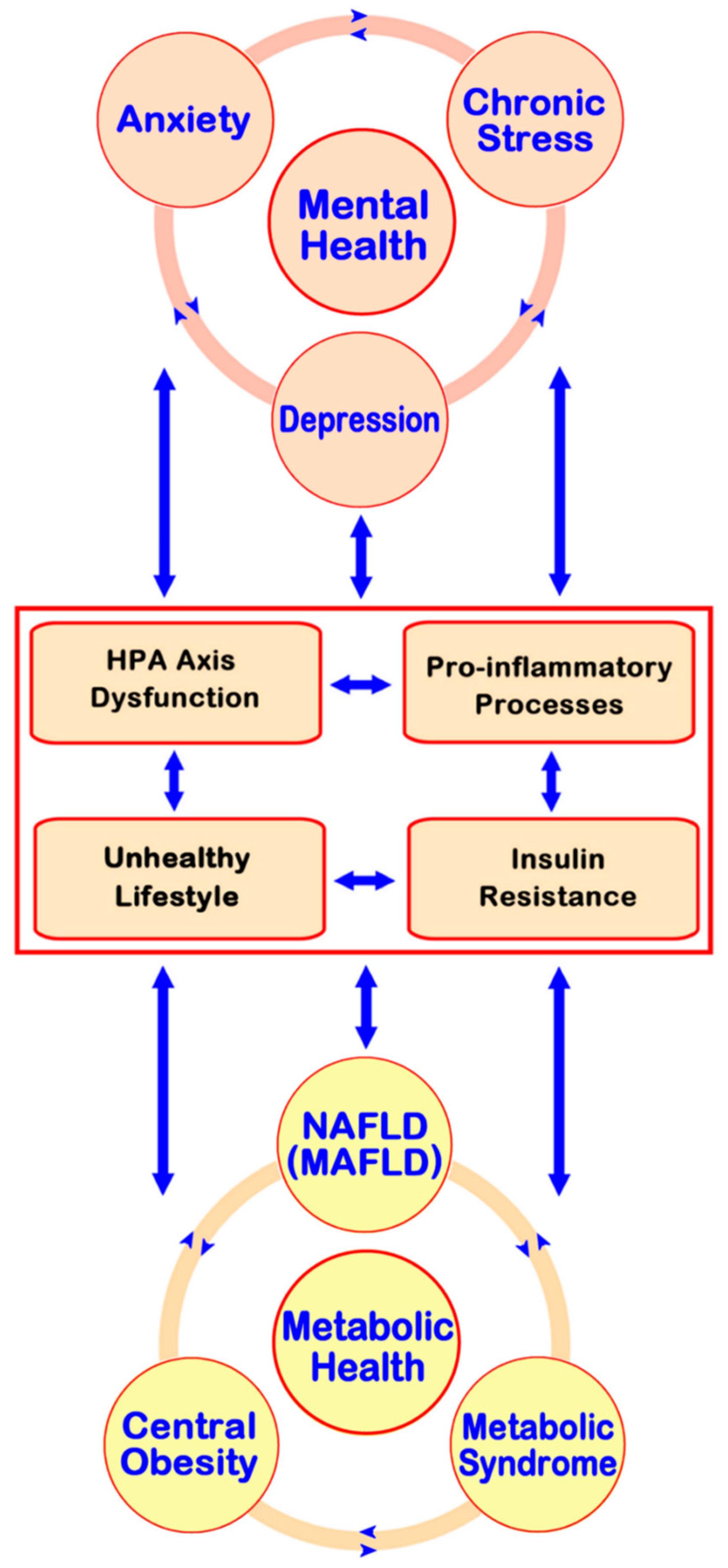
6. Potential Underlying Mechanisms Linking NAFLD with Depression, Anxiety, and Stress
6.1. Chronic Stress and HPA Axis Dysregulation
6.2. Obesity-Related Inflammation and Insulin Resistance
6.3. Gut Microbiome Dysbiosis in Metabolic Diseases and Its Association with Psychological Disorders
7. Future Research Directions and Concluding Remarks
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lazarus, J.V.; Colombo, M.; Cortez-Pinto, H.; Huang, T.T.; Miller, V.; Ninburg, M.; Schattenberg, J.M.; Seim, L.; Wong, V.W.S.; Zelber-Sagi, S. NAFLD—sounding the alarm on a silent epidemic. Nat. Rev. Gastroenterol. Hepatol. 2020, 17, 377–379. [Google Scholar] [CrossRef]
- Murag, S.; Ahmed, A.; Kim, D. Recent Epidemiology of Nonalcoholic Fatty Liver Disease. Gut Liver 2021, 15, 206–216. [Google Scholar] [CrossRef]
- Asrih, M.; Jornayvaz, F.R. Metabolic syndrome and nonalcoholic fatty liver disease: Is insulin resistance the link? Mol. Cell Endocrinol. 2015, 418 Pt 1, 55–65. [Google Scholar] [CrossRef] [Green Version]
- Estes, C.; Anstee, Q.M.; Arias-Loste, M.T.; Bantel, H.; Bellentani, S.; Caballeria, J.; Colombo, M.; Craxi, A.; Crespo, J.; Day, C.P.; et al. Modeling NAFLD disease burden in China, France, Germany, Italy, Japan, Spain, United Kingdom, and United States for the period 2016–2030. J. Hepatol. 2018, 69, 896–904. [Google Scholar] [CrossRef]
- Rinaldi, L.; Pafundi, P.C.; Galiero, R.; Caturano, A.; Morone, M.V.; Silvestri, C.; Giordano, M.; Salvatore, T.; Sasso, F.C. Mechanisms of Non-Alcoholic Fatty Liver Disease in the Metabolic Syndrome. A Narrative Review. Antioxidants 2021, 10, 270. [Google Scholar] [CrossRef]
- Godoy-Matos, A.F.; Silva Junior, W.S.; Valerio, C.M. NAFLD as a continuum: From obesity to metabolic syndrome and diabetes. Diabetol. Metab. Syndr. 2020, 12, 60. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.; Liu, X.; Yu, Y. Depression and Chronic Liver Diseases: Are There Shared Underlying Mechanisms? Front. Mol. Neurosci. 2017, 10, 134. [Google Scholar] [CrossRef] [Green Version]
- Katsiki, N.; Perez-Martinez, P.; Anagnostis, P.; Mikhailidis, D.P.; Karagiannis, A. Is Nonalcoholic Fatty Liver Disease Indeed the Hepatic Manifestation of Metabolic Syndrome? Curr. Vasc. Pharmacol. 2018, 16, 219–227. [Google Scholar] [CrossRef]
- Russ, T.C.; Kivimaki, M.; Morling, J.R.; Starr, J.M.; Stamatakis, E.; Batty, G.D. Association Between Psychological Distress and Liver Disease Mortality: A Meta-analysis of Individual Study Participants. Gastroenterology 2015, 148, 958–966.e4. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kyrou, I.; Randeva, H.S.; Tsigos, C.; Kaltsas, G.; Weickert, M.O. Clinical Problems Caused by Obesity. In Endotext; Feingold, K.R., Anawalt, B., Boyce, A., Chrousos, G., de Herder, W.W., Dhatariya, K., Dungan, K., Grossman, A., Hershman, J.M., Hofland, J., et al., Eds.; MDText.com, Inc.: South Dartmouth, MA, USA, 2018. [Google Scholar]
- Lim, S.; Kim, J.W.; Targher, G. Links between metabolic syndrome and metabolic dysfunction-associated fatty liver disease. Trends Endocrinol. Metab. 2021, 32, 500–514. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.H.; Lee, D.K.; Liu, M.; Portincasa, P.; Wang, D.Q. Novel Insights into the Pathogenesis and Management of the Metabolic Syndrome. Pediatric Gastroenterol. Hepatol. Nutr. 2020, 23, 189–230. [Google Scholar] [CrossRef] [PubMed]
- Chan, K.L.; Cathomas, F.; Russo, S.J. Central and Peripheral Inflammation Link Metabolic Syndrome and Major Depressive Disorder. Physiology 2019, 34, 123–133. [Google Scholar] [CrossRef]
- Gheshlagh, R.; Parizad, N.; Sayehmiri, K. The relationship between depression and metabolic syndrome: Systematic review and meta-analysis study. Iran. Red. Crescent Med. J. 2016, 18, e26523. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Huang, P.L. A comprehensive definition for metabolic syndrome. Dis. Model. Mech. 2009, 2, 231–237. [Google Scholar] [CrossRef] [Green Version]
- Kahn, C.R.; Wang, G.; Lee, K.Y. Altered adipose tissue and adipocyte function in the pathogenesis of metabolic syndrome. J. Clin. Investig. 2019, 129, 3990–4000. [Google Scholar] [CrossRef] [PubMed]
- Zafar, U.; Khaliq, S.; Ahmad, H.U.; Manzoor, S.; Lone, K.P. Metabolic syndrome: An update on diagnostic criteria, pathogenesis, and genetic links. Hormones 2018, 17, 299–313. [Google Scholar] [CrossRef]
- Banerjee, A.; Jana, A.; Praharaj, S.; Mukherjee, D.; Chakraborty, S. Depression and anxiety in patients with chronic liver disease and their relationship with quality of life. Ann. Indian Psychiatry 2020, 4, 28–32. [Google Scholar] [CrossRef]
- Kucerova, J.; Babinska, Z.; Horska, K.; Kotolova, H. The common pathophysiology underlying the metabolic syndrome, schizophrenia and depression. A review. Biomed. Pap. Med. Fac. Univ. Palacky Olomouc Czech. Repub. 2015, 159, 208–214. [Google Scholar] [CrossRef] [Green Version]
- Liang, Y.; Zou, L.; Tian, Y.; Zhou, S.; Chen, X.; Lin, C. Dietary and metabolic risk of neuropsychiatric disorders: Insights from animal models. Br. J. Nutr. 2021, 1–17. [Google Scholar] [CrossRef]
- Kyrou, I.; Randeva, H.S.; Tsigos, C. Stress, Insulin Resistance and Type II Diabetes; Academic Press: San Diego, CA, USA, 2017. [Google Scholar]
- Kyrou, I.; Tsigos, C. Stress mechanisms and metabolic complications. Horm. Metab. Res. 2007, 39, 430–438. [Google Scholar] [CrossRef]
- Tsigos, C.; Kyrou, I.; Kassi, E.; Chrousos, G.P. Stress: Endocrine Physiology and Pathophysiology. In Endotext; Feingold, K.R., Anawalt, B., Boyce, A., Chrousos, G., de Herder, W.W., Dhatariya, K., Dungan, K., Grossman, A., Hershman, J.M., Hofland, J., et al., Eds.; MDText.com, Inc.: South Dartmouth, MA, USA, 2020. [Google Scholar]
- Colognesi, M.; Gabbia, D.; De Martin, S. Depression and Cognitive Impairment-Extrahepatic Manifestations of NAFLD and NASH. Biomedicines 2020, 8, 229. [Google Scholar] [CrossRef]
- Tomeno, W.; Kawashima, K.; Yoneda, M.; Saito, S.; Ogawa, Y.; Honda, Y.; Kessoku, T.; Imajo, K.; Mawatari, H.; Fujita, K.; et al. Non-alcoholic fatty liver disease comorbid with major depressive disorder: The pathological features and poor therapeutic efficacy. J. Gastroenterol. Hepatol. 2015, 30, 1009–1014. [Google Scholar] [CrossRef]
- Valderas, J.M.; Starfield, B.; Sibbald, B.; Salisbury, C.; Roland, M. Defining comorbidity: Implications for understanding health and health services. Ann. Fam. Med. 2009, 7, 357–363. [Google Scholar] [CrossRef]
- Baumann, N. How to use the medical subject headings (MeSH). Int. J. Clin. Pract. 2016, 70, 171–174. [Google Scholar] [CrossRef] [Green Version]
- GBD 2017 Disease and Injury Incidence and Prevalence Collaborators (2018). Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1789–1858. [Google Scholar] [CrossRef] [Green Version]
- Liu, Y.Z.; Wang, Y.X.; Jiang, C.L. Inflammation: The Common Pathway of Stress-Related Diseases. Front. Hum. Neurosci. 2017, 11, 316. [Google Scholar] [CrossRef] [PubMed]
- Elwing, J.E.; Lustman, P.J.; Wang, H.L.; Clouse, R.E. Depression, anxiety, and nonalcoholic steatohepatitis. Psychosom. Med. 2006, 68, 563–569. [Google Scholar] [CrossRef] [PubMed]
- Kyrou, I.; Kollia, N.; Panagiotakos, D.; Georgousopoulou, E.; Chrysohoou, C.; Tsigos, C.; Randeva, H.S.; Yannakoulia, M.; Stefanadis, C.; Papageorgiou, C.; et al. Association of depression and anxiety status with 10-year cardiovascular disease incidence among apparently healthy Greek adults: The ATTICA Study. Eur. J. Prev. Cardiol. 2017, 24, 145–152. [Google Scholar] [CrossRef] [PubMed]
- Bica, T.; Castello, R.; Toussaint, L.L.; Monteso-Curto, P. Depression as a Risk Factor of Organic Diseases:An International Integrative Review. J. Nurs. Scholarsh. 2017, 49, 389–399. [Google Scholar] [CrossRef]
- Butnoriene, J.; Steibliene, V.; Saudargiene, A.; Bunevicius, A. Does presence of metabolic syndrome impact anxiety and depressive disorder screening results in middle aged and elderly individuals? A population based study. BMC Psychiatry 2018, 18, 5. [Google Scholar] [CrossRef] [Green Version]
- Shinkov, A.; Borissova, A.M.; Kovatcheva, R.; Vlahov, J.; Dakovska, L.; Atanassova, I.; Petkova, P. Increased prevalence of depression and anxiety among subjects with metabolic syndrome and known type 2 diabetes mellitus—a population-based study. Postgrad. Med. 2018, 130, 251–257. [Google Scholar] [CrossRef] [PubMed]
- Tang, F.; Wang, G.; Lian, Y. Association between anxiety and metabolic syndrome: A systematic review and meta-analysis of epidemiological studies. Psychoneuroendocrinology 2017, 77, 112–121. [Google Scholar] [CrossRef] [PubMed]
- Dunbar, J.A.; Reddy, P.; Davis-Lameloise, N.; Philpot, B.; Laatikainen, T.; Kilkkinen, A.; Bunker, S.J.; Best, J.D.; Vartiainen, E.; Kai Lo, S.; et al. Depression: An important comorbidity with metabolic syndrome in a general population. Diabetes Care 2008, 31, 2368–2373. [Google Scholar] [CrossRef] [Green Version]
- Skilton, M.R.; Moulin, P.; Terra, J.L.; Bonnet, F. Associations between anxiety, depression, and the metabolic syndrome. Biol. Psychiatry 2007, 62, 1251–1257. [Google Scholar] [CrossRef] [PubMed]
- Raikkonen, K.; Matthews, K.A.; Kuller, L.H. Depressive symptoms and stressful life events predict metabolic syndrome among middle-aged women: A comparison of World Health Organization, Adult Treatment Panel III, and International Diabetes Foundation definitions. Diabetes Care 2007, 30, 872–877. [Google Scholar] [CrossRef] [Green Version]
- Takeuchi, T.; Nakao, M.; Nomura, K.; Yano, E. Association of metabolic syndrome with depression and anxiety in Japanese men. Diabetes Metab. 2009, 35, 32–36. [Google Scholar] [CrossRef]
- Akbari, H.; Sarrafzadegan, N.; Aria, H.; Garaei, A.G.; Zakeri, H. Anxiety but not depression is associated with metabolic syndrome: The Isfahan Healthy Heart Program. J. Res. Med. Sci. 2017, 22, 90. [Google Scholar] [CrossRef]
- Weinstein, A.A.; Kallman Price, J.; Stepanova, M.; Poms, L.W.; Fang, Y.; Moon, J.; Nader, F.; Younossi, Z.M. Depression in patients with nonalcoholic fatty liver disease and chronic viral hepatitis B and C. Psychosomatics 2011, 52, 127–132. [Google Scholar] [CrossRef]
- Youssef, N.A.; Abdelmalek, M.F.; Binks, M.; Guy, C.D.; Omenetti, A.; Smith, A.D.; Diehl, A.M.; Suzuki, A. Associations of depression, anxiety and antidepressants with histological severity of nonalcoholic fatty liver disease. Liver Int. 2013, 33, 1062–1070. [Google Scholar] [CrossRef]
- Jung, J.Y.; Park, S.K.; Oh, C.M.; Chung, P.W.; Ryoo, J.H. Non-Alcoholic Fatty Liver Disease and Its Association with Depression in Korean General Population. J. Korean Med. Sci. 2019, 34, e199. [Google Scholar] [CrossRef]
- Choi, J.M.; Chung, G.E.; Kang, S.J.; Kwak, M.S.; Yang, J.I.; Park, B.; Yim, J.Y. Association Between Anxiety and Depression and Nonalcoholic Fatty Liver Disease. Front. Med. 2020, 7, 585618. [Google Scholar] [CrossRef]
- Bashir, T.; Shafi, A.; Khalil, F. Frequency of depression in patients with non-alcoholic fatty liver disease. J. FatimaJinnah Med. Univ. 2020, 12, 25–27. [Google Scholar]
- Kim, D.; Yoo, E.R.; Li, A.A.; Tighe, S.P.; Cholankeril, G.; Harrison, S.A.; Ahmed, A. Depression is associated with non-alcoholic fatty liver disease among adults in the United States. Aliment. Pharmacol. Ther. 2019, 50, 590–598. [Google Scholar] [CrossRef] [PubMed]
- Cho, I.Y.; Chang, Y.; Sung, E.; Kang, J.H.; Wild, S.H.; Byrne, C.D.; Shin, H.; Ryu, S. Depression and increased risk of non-alcoholic fatty liver disease in individuals with obesity. Epidemiol. Psychiatr. Sci. 2021, 30, e23. [Google Scholar] [CrossRef] [PubMed]
- Labenz, C.; Huber, Y.; Michel, M.; Nagel, M.; Galle, P.R.; Kostev, K.; Schattenberg, J.M. Nonalcoholic Fatty Liver Disease Increases the Risk of Anxiety and Depression. Hepatol. Commun. 2020, 4, 1293–1301. [Google Scholar] [CrossRef]
- Sayiner, M.; Arshad, T.; Golabi, P.; Paik, J.; Farhat, F.; Younossi, Z.M. Extrahepatic manifestations and healthcare expenditures of non-alcoholic fatty liver disease in the Medicare population. Hepatol. Int. 2020, 14, 556–566. [Google Scholar] [CrossRef]
- Xiao, J.; Lim, L.K.E.; Ng, C.H.; Tan, D.J.H.; Lim, W.H.; Ho, C.S.H.; Tan, E.X.X.; Sanyal, A.J.; Muthiah, M.D. Is Fatty Liver Associated With Depression? A Meta-Analysis and Systematic Review on the Prevalence, Risk Factors, and Outcomes of Depression and Non-alcoholic Fatty Liver Disease. Front. Med. 2021, 8, 691696. [Google Scholar] [CrossRef] [PubMed]
- Selye, H. Stress and disease. Science 1955, 122, 625–631. [Google Scholar] [CrossRef]
- Osborne, M.T.; Shin, L.M.; Mehta, N.N.; Pitman, R.K.; Fayad, Z.A.; Tawakol, A. Disentangling the Links Between Psychosocial Stress and Cardiovascular Disease. Circ. Cardiovasc. Imaging 2020, 13, e010931. [Google Scholar] [CrossRef]
- Cuevas, A.G.; Chen, R.; Thurber, K.A.; Slopen, N.; Williams, D.R. Psychosocial Stress and Overweight and Obesity: Findings From the Chicago Community Adult Health Study. Ann. Behav. Med. 2019, 53. [Google Scholar] [CrossRef]
- Aschbacher, K.; Kornfeld, S.; Picard, M.; Puterman, E.; Havel, P.J.; Stanhope, K.; Lustig, R.H.; Epel, E. Chronic stress increases vulnerability to diet-related abdominal fat, oxidative stress, and metabolic risk. Psychoneuroendocrinology 2014, 46, 14–22. [Google Scholar] [CrossRef] [Green Version]
- Bergmann, N.; Gyntelberg, F.; Faber, J. The appraisal of chronic stress and the development of the metabolic syndrome: A systematic review of prospective cohort studies. Endocr. Connect. 2014, 3, R55–R80. [Google Scholar] [CrossRef] [PubMed]
- Kang, D.; Zhao, D.; Ryu, S.; Guallar, E.; Cho, J.; Lazo, M.; Shin, H.; Chang, Y.; Sung, E. Perceived stress and non-alcoholic fatty liver disease in apparently healthy men and women. Sci. Rep. 2020, 10, 38. [Google Scholar] [CrossRef]
- Kuo, W.C.; Bratzke, L.C.; Oakley, L.D.; Kuo, F.; Wang, H.; Brown, R.L. The association between psychological stress and metabolic syndrome: A systematic review and meta-analysis. Obes. Rev. 2019, 20, 1651–1664. [Google Scholar] [CrossRef] [PubMed]
- Han, A.L. Association between Non-Alcoholic Fatty Liver Disease and Dietary Habits, Stress, and Health-Related Quality of Life in Korean Adults. Nutrients 2020, 12, 1555. [Google Scholar] [CrossRef] [PubMed]
- Cohen, B.E.; Edmondson, D.; Kronish, I.M. State of the Art Review: Depression, Stress, Anxiety, and Cardiovascular Disease. Am. J. Hypertens. 2015, 28, 1295–1302. [Google Scholar] [CrossRef] [Green Version]
- Satyjeet, F.; Naz, S.; Kumar, V.; Aung, N.H.; Bansar, K.; Irfan, S.; Rizwan, A. Psychological stress as a risk factor for cardiovascular disease: A case-control study. Cureus 2020, 12, e10757. [Google Scholar] [CrossRef]
- Li, C.; Xing, J.J.; Shan, A.Q.; Leng, L.; Liu, J.C.; Yue, S.; Yu, H.; Chen, X.; Tian, F.S.; Tang, N.J. Increased risk of nonalcoholic fatty liver disease with occupational stress in Chinese policemen: A 4-year cohort study. Medicine 2016, 95, e5359. [Google Scholar] [CrossRef]
- Zhang, S.; Ma, C.; Wang, X.; Wang, Q.; Song, W.; Li, C.; Zhai, C.; Qi, Y.; Fan, S.; Cheng, F. Impact of chronic psychological stress on nonalcoholic fatty liver disease. Int. J. Clin. Exp. Med. 2019, 12, 7991–7998. [Google Scholar]
- Assimakopoulos, K.; Karaivazoglou, K.; Tsermpini, E.E.; Diamantopoulou, G.; Triantos, C. Quality of life in patients with nonalcoholic fatty liver disease: A systematic review. J. Psychosom. Res. 2018, 112, 73–80. [Google Scholar] [CrossRef]
- Ford, E.S.; Li, C. Metabolic syndrome and health-related quality of life among U.S. adults. Ann. Epidemiol. 2008, 18, 165–171. [Google Scholar] [CrossRef]
- Saboya, P.P.; Bodanese, L.C.; Zimmermann, P.R.; Gustavo, A.D.; Assumpcao, C.M.; Londero, F. Metabolic syndrome and quality of life: A systematic review. Rev. Lat. Am. Enferm. 2016, 24, e2848. [Google Scholar] [CrossRef] [Green Version]
- Tziallas, D.; Kastanioti, C.; Savvas, K.; Kostapanos, M.; Tziallas, V.; Skapinakis, P.; Elisaf, M.; Mavreas, V. Evaluation of health related quality of life in patients with metabolic syndrome. Health Sci. J. 2012, 6, 116–128. [Google Scholar]
- Lee, Y.J.; Woo, S.Y.; Ahn, J.H.; Cho, S.; Kim, S.R. Health-related quality of life in adults with metabolic syndrome: The Korea national health and nutrition examination survey, 2007–2008. Ann. Nutr. Metab. 2012, 61, 275–280. [Google Scholar] [CrossRef]
- Younossi, Z.M.; Guyatt, G.; Kiwi, M.; Boparai, N.; King, D. Development of a disease specific questionnaire to measure health related quality of life in patients with chronic liver disease. Gut 1999, 45, 295–300. [Google Scholar] [CrossRef]
- Younossi, Z.M.; Stepanova, M.; Henry, L.; Racila, A.; Lam, B.; Pham, H.T.; Hunt, S. A disease-specific quality of life instrument for non-alcoholic fatty liver disease and non-alcoholic steatohepatitis: CLDQ-NAFLD. Liver Int. 2017, 37, 1209–1218. [Google Scholar] [CrossRef] [PubMed]
- Dan, A.A.; Kallman, J.B.; Wheeler, A.; Younoszai, Z.; Collantes, R.; Bondini, S.; Gerber, L.; Younossi, Z.M. Health-related quality of life in patients with non-alcoholic fatty liver disease. Aliment. Pharmacol. Ther. 2007, 26, 815–820. [Google Scholar] [CrossRef] [PubMed]
- Tapper, E.B.; Lai, M. Weight loss results in significant improvements in quality of life for patients with nonalcoholic fatty liver disease: A prospective cohort study. Hepatology 2016, 63, 1184–1189. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Castellanos-Fernandez, M.I.; Borges-Gonzalez, S.A.; Stepanova, M.; Infante-Velazquez, M.E.; Ruenes-Domech, C.; Gonzalez-Suero, S.M.; Dorta-Guridi, Z.; Arus-Soler, E.R.; Racila, A.; Younossi, Z.M. Health-related quality of life in Cuban patients with chronic liver disease: A real-world experience. Ann. Hepatol. 2021, 22, 100277. [Google Scholar] [CrossRef]
- Golabi, P.; Otgonsuren, M.; Cable, R.; Felix, S.; Koenig, A.; Sayiner, M.; Younossi, Z.M. Non-alcoholic Fatty Liver Disease (NAFLD) is associated with impairment of Health Related Quality of Life (HRQOL). Health Qual. Life Outcomes 2016, 14, 18. [Google Scholar] [CrossRef] [Green Version]
- Bonavita, V.; De Simone, R. Towards a definition of comorbidity in the light of clinical complexity. Neurol. Sci. 2008, 29 (Suppl. S1), S99–S102. [Google Scholar] [CrossRef]
- Van der Feltz-Cornelis, C.M.; van Os, J.; Knappe, S.; Schumann, G.; Vieta, E.; Wittchen, H.U.; Lewis, S.W.; Elfeddali, I.; Wahlbeck, K.; Linszen, D.; et al. Towards Horizon 2020: Challenges and advances for clinical mental health research—Outcome of an expert survey. Neuropsychiatr. Dis. Treat. 2014, 10, 1057–1068. [Google Scholar] [CrossRef] [Green Version]
- Marrie, R.A.; Bernstein, C.N. Psychiatric comorbidity in immune-mediated inflammatory diseases. World Psychiatry 2021, 20, 298–299. [Google Scholar] [CrossRef]
- Murphy, M.O.; Loria, A.S. Sex-specific effects of stress on metabolic and cardiovascular disease: Are women at higher risk? Am. J. Physiol. Regul. Integr. Comp. Physiol. 2017, 313, R1–R9. [Google Scholar] [CrossRef]
- Goldfarb, E.V.; Seo, D.; Sinha, R. Sex differences in neural stress responses and correlation with subjective stress and stress regulation. Neurobiol. Stress 2019, 11, 100177. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Ko, Y.; Kwak, C.; Yim, E.S. Gender differences in metabolic syndrome components among the Korean 66-year-old population with metabolic syndrome. BMC Geriatr. 2016, 16, 27. [Google Scholar] [CrossRef] [Green Version]
- Tramunt, B.; Smati, S.; Grandgeorge, N.; Lenfant, F.; Arnal, J.F.; Montagner, A.; Gourdy, P. Sex differences in metabolic regulation and diabetes susceptibility. Diabetologia 2020, 63, 453–461. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Daly, M. The relationship of C-reactive protein to obesity-related depressive symptoms: A longitudinal study. Obesity 2013, 21, 248–250. [Google Scholar] [CrossRef]
- Delgado, I.; Huet, L.; Dexpert, S.; Beau, C.; Forestier, D.; Ledaguenel, P.; Aubert, A.; Sauvant, J.; Aouizerate, B.; Magne, E.; et al. Depressive symptoms in obesity: Relative contribution of low-grade inflammation and metabolic health. Psychoneuroendocrinology 2018, 91, 55–61. [Google Scholar] [CrossRef]
- Webb, M.; Davies, M.; Ashra, N.; Bodicoat, D.; Brady, E.; Webb, D.; Moulton, C.; Ismail, K.; Khunti, K. The association between depressive symptoms and insulin resistance, inflammation and adiposity in men and women. PLoS ONE 2017, 12, e0187448. [Google Scholar] [CrossRef] [Green Version]
- Lee, J.W.; Park, S.H. Association between depression and nonalcoholic fatty liver disease: Contributions of insulin resistance and inflammation. J. Affect. Disord. 2021, 278, 259–263. [Google Scholar] [CrossRef] [PubMed]
- Barber, T.M.; Valsamakis, G.; Mastorakos, G.; Hanson, P.; Kyrou, I.; Randeva, H.S.; Weickert, M.O. Dietary Influences on the Microbiota-Gut-Brain Axis. Int. J. Mol. Sci. 2021, 22, 3502. [Google Scholar] [CrossRef] [PubMed]
- Butler, M.I.; Morkl, S.; Sandhu, K.V.; Cryan, J.F.; Dinan, T.G. The Gut Microbiome and Mental Health: What Should We Tell Our Patients?: Le microbiote Intestinal et la Sante Mentale: Que Devrions-Nous dire a nos Patients? Can. J. Psychiatry 2019, 64, 747–760. [Google Scholar] [CrossRef] [PubMed]
- Barber, T.M.; Kyrou, I.; Randeva, H.S.; Weickert, M.O. Mechanisms of Insulin Resistance at the Crossroad of Obesity with Associated Metabolic Abnormalities and Cognitive Dysfunction. Int. J. Mol. Sci. 2021, 22, 546. [Google Scholar] [CrossRef]
- Agusti, A.; Garcia-Pardo, M.P.; Lopez-Almela, I.; Campillo, I.; Maes, M.; Romani-Perez, M.; Sanz, Y. Interplay Between the Gut-Brain Axis, Obesity and Cognitive Function. Front. Neurosci. 2018, 12, 155. [Google Scholar] [CrossRef] [PubMed]
- Caturano, A.; Acierno, C.; Nevola, R.; Parfundi, P.C.; Galiero, R.; Rinaldi, L.; Salvatore, T.; Adinolfi, L.E.; Sasso, F.C. Non-Alcoholic Fatty Liver Disease: From Pathogenesis to Clinical Impact. Processes 2021, 9, 135. [Google Scholar] [CrossRef]
- American Psychiatric Association. DSM-5 Task Force. In Diagnostic and Statistical Manual of Mental Disorders: DSM-5, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013; 947 p. [Google Scholar]
- Koukopoulos, A.; Sani, G. DSM-5 criteria for depression with mixed features: A farewell to mixed depression. Acta Psychiatr. Scand. 2014, 129, 4–16. [Google Scholar] [CrossRef]
- Park, S.C.; Kim, Y.K. Anxiety Disorders in the DSM-5: Changes, Controversies, and Future Directions. Adv. Exp. Med. Biol. 2020, 1191, 187–196. [Google Scholar] [CrossRef]
- World Health Organization. The ICD-10 Classification of Mental and Behavioural Disorders: Clinical Descriptions and Diagnostic Guidelines; World Health Organization: Geneva, Switzerland, 1992; 362 p. [Google Scholar]
- Kroenke, K. Depression screening and management in primary care. Fam. Pract. 2018, 35, 1–3. [Google Scholar] [CrossRef]
- Kroenke, K. PHQ-9: Global uptake of a depression scale. World Psychiatry 2021, 20, 135–136. [Google Scholar] [CrossRef]
- Sapra, A.; Bhandari, P.; Sharma, S.; Chanpura, T.; Lopp, L. Using Generalized Anxiety Disorder-2 (GAD-2) and GAD-7 in a Primary Care Setting. Cureus 2020, 12, e8224. [Google Scholar] [CrossRef]
- Pai, A.; Suris, A.M.; North, C.S. Posttraumatic Stress Disorder in the DSM-5: Controversy, Change, and Conceptual Considerations. Behav. Sci. 2017, 7, 7. [Google Scholar] [CrossRef]
- Du Preez, A.; Eum, J.; Eiben, I.; Eiben, P.; Zunszain, P.A.; Pariante, C.M.; Thuret, S.; Fernandes, C. Do different types of stress differentially alter behavioural and neurobiological outcomes associated with depression in rodent models? A systematic review. Front. Neuroendocrinol. 2021, 61, 100896. [Google Scholar] [CrossRef]
- Vallejo, M.A.; Vallejo-Slocker, L.; Fernandez-Abascal, E.G.; Mananes, G. Determining Factors for Stress Perception Assessed with the Perceived Stress Scale (PSS-4) in Spanish and Other European Samples. Front. Psychol. 2018, 9, 37. [Google Scholar] [CrossRef] [PubMed]
- Hasnain, M.; Vieweg, W.V. Weight considerations in psychotropic drug prescribing and switching. Postgrad. Med. 2013, 125, 117–129. [Google Scholar] [CrossRef]
- Alonso-Pedrero, L.; Bes-Rastrollo, M.; Marti, A. Effects of antidepressant and antipsychotic use on weight gain: A systematic review. Obes. Rev. 2019, 20, 1680–1690. [Google Scholar] [CrossRef] [PubMed]
- Gill, H.; Gill, B.; El-Halabi, S.; Chen-Li, D.; Lipsitz, O.; Rosenblat, J.D.; Van Rheenen, T.E.; Rodrigues, N.B.; Mansur, R.B.; Majeed, A.; et al. Antidepressant Medications and Weight Change: A Narrative Review. Obesity 2020, 28, 2064–2072. [Google Scholar] [CrossRef] [PubMed]
- Wharton, S.; Raiber, L.; Serodio, K.J.; Lee, J.; Christensen, R.A. Medications that cause weight gain and alternatives in Canada: A narrative review. Diabetes Metab. Syndr. Obes. 2018, 11, 427–438. [Google Scholar] [CrossRef] [Green Version]
- Kalinichenko, L.S.; Kornhuber, J.; Muller, C.P. Individual differences in inflammatory and oxidative mechanisms of stress-related mood disorders. Front. Neuroendocrinol. 2019, 55, 100783. [Google Scholar] [CrossRef]
- Spinosa, J.; Christiansen, P.; Dickson, J.M.; Lorenzetti, V.; Hardman, C.A. From Socioeconomic Disadvantage to Obesity: The Mediating Role of Psychological Distress and Emotional Eating. Obesity 2019, 27, 559–564. [Google Scholar] [CrossRef] [Green Version]
- Funuyet-Salas, J.; Perez-San-Gregorio, M.A.; Martin-Rodriguez, A.; Romero-Gomez, M. Psychological Biomarkers and Fibrosis: An Innovative Approach to Non-alcoholic Fatty Liver Disease. Front. Med. 2020, 7, 585425. [Google Scholar] [CrossRef] [PubMed]
- Eslam, M.; Sanyal, A.J.; George, J.; International Consensus, P. MAFLD: A Consensus-Driven Proposed Nomenclature for Metabolic Associated Fatty Liver Disease. Gastroenterology 2020, 158, 1999–2014.e1. [Google Scholar] [CrossRef]
- Fouad, Y.; Waked, I.; Bollipo, S.; Gomaa, A.; Ajlouni, Y.; Attia, D. What’s in a name? Renaming ‘NAFLD’ to ‘MAFLD’. Liver Int. 2020, 40, 1254–1261. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Prince, M.; Patel, V.; Saxena, S.; Maj, M.; Maselko, J.; Phillips, M.R.; Rahman, A. No health without mental health. Lancet 2007, 370, 859–877. [Google Scholar] [CrossRef]
| Study [Reference] | Country | Study Design/Cohort | Mental Health Related Outcome Assessed and Method | Outcome/Main Findings |
|---|---|---|---|---|
| Tang, Wang, & Lian (2016) [34] | China | Systematic review and meta-analysis 18 cross-sectional studies N = 41,168 2 cohort studies N = 1388 | Anxiety Various | Supports a significant relationship between anxiety and metabolic syndrome. |
| Akbari et al. (2017) [39] | Iran | Cross-Sectional Community-based cohort N = 470 (male: 50.2%) Mean Age: 55.7 ys | Depression/Anxiety HADS | No significant association between depression, concurrent depression, and anxiety with metabolic syndrome. Patients with anxiety had lower prevalence of metabolic syndrome than healthy subjects. |
| Butnoriene et al. (2018) [32] | Lithuania | Cross-Sectional Metabolic syndrome: N = 384 (female: 53.6%) Mean Age: 63.7 ys Without Metabolic Syndrome: N = 731 (male: 52.5%) Mean Age: 61.1 ys | Depression/Anxiety HADS MINI | Depression and anxiety was identified as being more common in individuals with metabolic syndrome in comparison with those without. |
| Dunbar et al. (2008) [35] | Australia | Cross-Sectional N = 409 (male: 50.9%) Mean Age: 60.5 ys | Depression/Anxiety HADS Kessler 10 | Results show an association between metabolic syndrome and depression, but not with psychological distress and anxiety. |
| Shinkov et al. (2018) [33] | Bulgaria | Cross-sectional N = 2111 (female: 54.7%) Mean Age: 46.4 ys | Depression/Anxiety Zung Self-Rating Depression and Anxiety Scales | Depression and anxiety scores were higher for those with metabolic syndrome. |
| Skilton Moulin et al. (2007) [36] | France | Observational N = 1598 (male: 62.9%) Mean Age: 51.8 ys | Depression/Anxiety HADS | Metabolic syndrome was associated with depressive symptoms, but not with anxiety in men and women, irrespective of body weight. |
| Kuo et al. (2019) [56] | USA | Systematic review and meta-analysis 30 studies N = 67,037 | Stress Various | Different sources of frequently occurring stress should be investigated. Usual methods (e.g., lifestyle change) for preventing metabolic syndrome, may be less effective if psychosocial stress is overlooked. |
| Ford et al. (2008) [63] | USA | Cross-Sectional Metabolic syndrome: N = 737 (female: 50.4%) Mean Age: 52.2 ys Without metabolic syndrome: N = 1122 (female: 50.5%) Mean Age: 41.8 ys | HRQoL Centers for Disease Control and Prevention HRQOL-4 tool | HRQoL was worse in people with metabolic syndrome compared with those without. |
| Lee et al. (2012) [66] | Korea | Cross-sectional Metabolic Syndrome: N = 2635 (male: 56%) Mean Age: 52.8 ys Without Metabolic Syndrome: N = 6306 (male: 52.3%) Mean Age: 40.8 ys | HRQoL EQ-5D EQ VAS | Unable to identify and independent association in relation to impaired HRQoL in people with metabolic syndrome after adjusting for confounding variables. |
| Saboya et al. (2016) [64] | Brazil | Systematic review 30 studies N = 62,063 | HRQoL SF-36 was the most frequently utilized | Evidence suggests association between metabolic syndrome and poorer HRQoL. |
| Tziallas et al. (2012) [65] | Greece | Cross-Sectional Metabolic Syndrome: N = 206 (female: 54.8%) Mean Age: 58.4 ys Controls: N = 153 (male: 53%) Mean Age: 50.1 ys | HRQoL SF-36 | Study identified impaired HRQoL on almost all subscales of the SF-36 for patients with metabolic syndrome compared to controls. |
| Study [Reference] | Country | Study Design/Cohort | Mental Health Related Outcome Assessed & Method | Outcome/Main Findings |
|---|---|---|---|---|
| Bashir, Shafi, & Khalil (2020) [44] | Pakistan | Observational Newly US-diagnosed NAFLD N = 170 (male: 64.1%) Mean Age: 39.8 ys | Depression PHQ-9 | 24.1% of NAFLD patients suffered from clinical depression, implying frequency of depression in people with NAFLD. |
| Cho et al. (2021) [46] | Korea | Longitudinal N = 142,005 (female: 64.6%) Mean Age: 35.6 ys | Depression CES-D | Depression was associated with increased risk of incident hepatic steatosis and higher probability of advanced liver fibrosis, particularly among individuals with obesity. |
| Jung et al. (2019) [42] | Korea | Observational N = 112,797 (female: 51.5%) Mean Age: 40 ys Degree of NAFLD assessed by US, FLI, and FIB-4 | Depression CES-D | Evidence of an association between the severity of NAFLD and depression. |
| Kim et al. (2019) [45] | USA | Cross-sectional N = 10,484 (female: 51.2%) Mean Age: 47 ys NAFLD defined by USFLI, HSI, and FLI | Depression PHQ-9 | Study identified a higher prevalence of depression among individuals with NAFLD compared to those without. |
| Sayiner et al. (2020) [48] | USA | N = 30,908,679 (random 5% sample of Medicare data from 2005–2016; female: 54.59%) Mean Age: 70.11 | Depression Based on ICD-9 and ICD-10 codes | Depression identified as one of the most common extrahepatic diseases associated with NAFLD. |
| Tomeno et al. (2015) [24] | Intervention study N = 258 NAFLD comorbid with MDD: N = 32 (male: 56.2%) Mean Age: 46.5 ys NAFLD without MDD: N = 226 (male: 52.6%) Mean Age: 50.7 ys NAFLD diagnosis based on liver biopsy | Depression MDD diagnosed according to the DSM-IV criteria. | Following a 48-week lifestyle intervention, patients with NAFLD demonstrated a poor response with less effective treatment outcomes. | |
| Weinstein et al. (2011) [40] | USA | Retrospective NAFLD: N = 184 (female: 69.4%) Mean Age: 46.7 ys Hepatitis B: N = 190 (male: 61.9%) Mean Age: 43.6 ys Hepatitis C: N = 504 (male: 59.7%) Mean Age: 48.6 ys | Depression Self-reported Diagnosis confirmed by history of prescription medication. | Study identified a higher prevalence of depression in patients with NAFLD and HCV, compared with patients with HBV and members of the general population. |
| Xiao et al. (2021) [49] | Singapore | Systematic review and meta-analysis including 10 studies N = 2,041,752 | Depression Various | High prevalence of depression in NAFLD patients was identified. Risk factors include BMI, diabetes, and being female. |
| Choi et al. (2021) [43] | South Korea | Retrospective Cross-Sectional N = 25,333 (male: 56.2%) Mean Age: 47 ys US-diagnosed NAFLD prevalence: 30.9% | Depression/Anxiety BDI State-Trait Anxiety Inventory | Severe steatosis is significantly related to both state and trait anxiety in patients with NAFLD. When gender was taken into consideration, a 44% increase in the risk of depression among women with NAFLD was demonstrated. |
| Labenz et al. (2020) [47] | Germany | Retrospective cohort study Patients with NAFLD: N = 19,871 (male: 57.5%) Mean Age: 58.5 ys Patients without NAFLD: N = 19,871 (male: 57.5%) Mean Age: 58.5 | Depression/Anxiety ICD-10 Codes | Study highlighted a significant association between NAFLD and development of depression/anxiety was noted, independent of comorbidities. |
| Youssef et al. (2013) [41] | USA | Cross-sectional N = 567 (female: 67%) Mean Age: 48 ys NAFLD diagnosis based on liver biopsy | Depression/Anxiety HADS | Symptoms of depression and anxiety common in patients with NAFLD. Study identified a positive association between greater hepatocyte ballooning and depression in patients with NAFLD. |
| Han (2020) [57] | Korea | Cross-Sectional Total: N = 17,726 (male: 50.6%) Mean Age: 43.9 ys HSI ≥ 36: N = 3764 (male: 61.3%) Mean Age: 45.1 ys HSI < 36: N = 13,962 (female: 52.5%) Mean Age: 43.5 ys NAFLD definition based on an HSI value ≥ 36 | Stress EQ-5D Stress perception rate | Decrease in the EQ-5D score by one unit increased the risk of NAFLD by more than threefold. Indication of an increased risk of NAFLD (by 1.3 times) in individuals with increased perceived stress. |
| Kang et al. (2020) [55] | Korea | Cross-sectional Total: N = 171,321 (male: 50.1%) Mean Age: 39.8 ys With NAFLD: N = 47,538 (male: 76.6%) Mean Age: 42 ys Without NAFLD: N = 123,783 (female: 60.1%) Mean Age: 38.9 ys NAFLD diagnosed by ultrasonography | Stress PSI | An independent association between higher levels of perceived stress and a greater prevalence of NAFLD was identified. |
| Li et al. (2016) [60] | China | Cross-sectional Total: N = 2367 (male: 100%) Mean Age: 36.65 ys NAFLD new onset: N = 739 (male: 100%) Mean Age: 36.9 ys NAFLD non-onset: N = 1628 (male: 100%) Mean Age: 36.54 ys | Stress OSI-R | High occupational stress and high personal strain identified as independent risk factors for NAFLD. Presence of NAFLD was significantly higher in traffic police officers. |
| Russ et al. (2015) [8] | UK | Meta-analysis of Individual Study Participants N = 166,631 (female: 55%) Mean Age: 46.6 ys | Stress GHQ | Psychological distress associated with liver disease mortality. |
| Assimakopoulos et al. (2018) [62] | Greece | Systematic review 14 studies N = 5000 | HRQoL Various | NAFLD patients have poorer HRQoL compared with healthy controls. |
| Castellanos-Fernández et al. (2020) [71] | Cuba | Cross-sectional NAFLD: N = 221 (female: 67.9%) Mean Age: 54 ys Hepatitis B: N = 91 (male: 56%) Mean Age: 45.9 ys AILD: N = 43 (female: 90.7%) Mean Age: 49.3 ys | HRQoL CLDQ | CLDQ and HRQoL scores were significantly lower for patients with NAFLD and AILD compared with HBV. |
| Dan et al. (2007) [69] | USA | Observational NAFLD: N = 106 (female: 69.8%) Mean Age: 46.4 ys Hepatitis B: N = 56 (male: 73,2%) Mean Age: 45.4 ys Hepatitis C: N = 75 (male: 57.3%) Mean Age: 47.0 ys | HRQoL CLDQ | Patients were identified from the Liver Disease Quality of Life Database. HRQoL scores were significantly lower for NAFLD patients compared with patients with hepatitis B or hepatitis C on multiple CLDQ domains. |
| Golabi et al. (2016) [72] | USA | Cross-sectional NAFLD: N = 3333 (male: 54.5%) Mean Age: 51.31 ys Controls: N = 5982 (male: 51.8%) Mean Age: 47.5 ys NAFLD was determined by the FLI | HRQoL HRQOL-4 | NAFLD is associated with impaired HRQoL. |
| Tapper & Lai (2016) [70] | USA | Prospective longitudinal study N = 151 (male: 60%) Mean Age: 51.5 ys NAFLD diagnosis: histologic | HRQoL CLDQ | At the 6-month follow-up of a weight loss intervention programme, this study revealed that patients achieving a 5% weight reduction showed significantly improved HRQoL. |
| Funuyet-Salas et al. (2020) [92] | Spain | Cross-sectional N = 492 (male: 58.9%) Mean Age: 54.9 ys Biopsy-proven NAFLD | Multiple SF-12 CLDQ-NAFLD HADS BD-II COPE-28 MSPSS | Low perceived social support, significant fibrosis, and female sex were independently associated with a higher-risk psychosocial profile in NAFLD. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shea, S.; Lionis, C.; Kite, C.; Atkinson, L.; Chaggar, S.S.; Randeva, H.S.; Kyrou, I. Non-Alcoholic Fatty Liver Disease (NAFLD) and Potential Links to Depression, Anxiety, and Chronic Stress. Biomedicines 2021, 9, 1697. https://doi.org/10.3390/biomedicines9111697
Shea S, Lionis C, Kite C, Atkinson L, Chaggar SS, Randeva HS, Kyrou I. Non-Alcoholic Fatty Liver Disease (NAFLD) and Potential Links to Depression, Anxiety, and Chronic Stress. Biomedicines. 2021; 9(11):1697. https://doi.org/10.3390/biomedicines9111697
Chicago/Turabian StyleShea, Sue, Christos Lionis, Chris Kite, Lou Atkinson, Surinderjeet S. Chaggar, Harpal S. Randeva, and Ioannis Kyrou. 2021. "Non-Alcoholic Fatty Liver Disease (NAFLD) and Potential Links to Depression, Anxiety, and Chronic Stress" Biomedicines 9, no. 11: 1697. https://doi.org/10.3390/biomedicines9111697
APA StyleShea, S., Lionis, C., Kite, C., Atkinson, L., Chaggar, S. S., Randeva, H. S., & Kyrou, I. (2021). Non-Alcoholic Fatty Liver Disease (NAFLD) and Potential Links to Depression, Anxiety, and Chronic Stress. Biomedicines, 9(11), 1697. https://doi.org/10.3390/biomedicines9111697








