Bioengineered Skin Intended as In Vitro Model for Pharmacosmetics, Skin Disease Study and Environmental Skin Impact Analysis
Abstract
1. Advances in Tissue Engineering
2. Human Artificial Skin
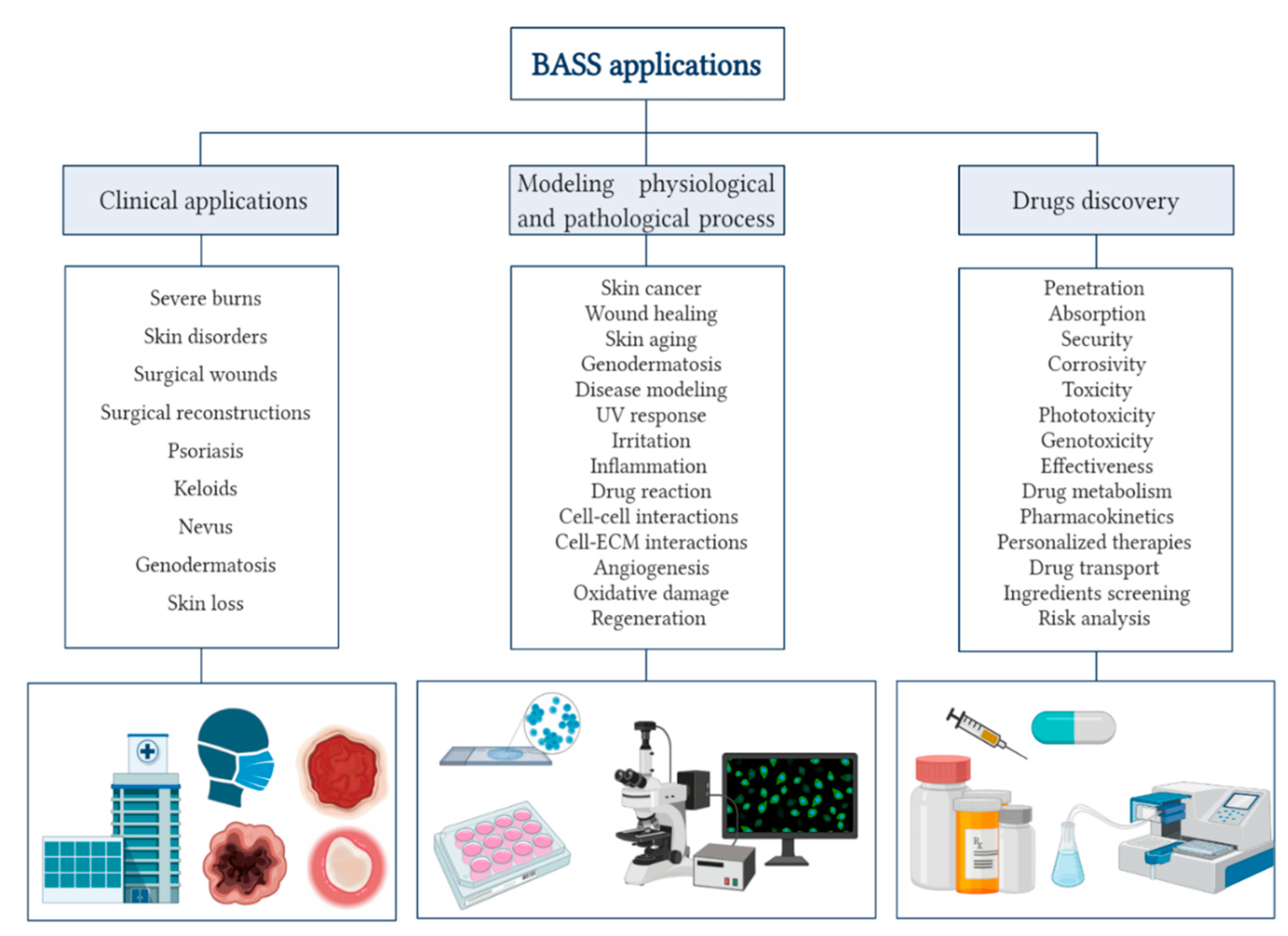
3. Applications
3.1. Uses on Cosmetic and Pharmaceutic Research
3.2. Alternative Method to Animal Experimentation
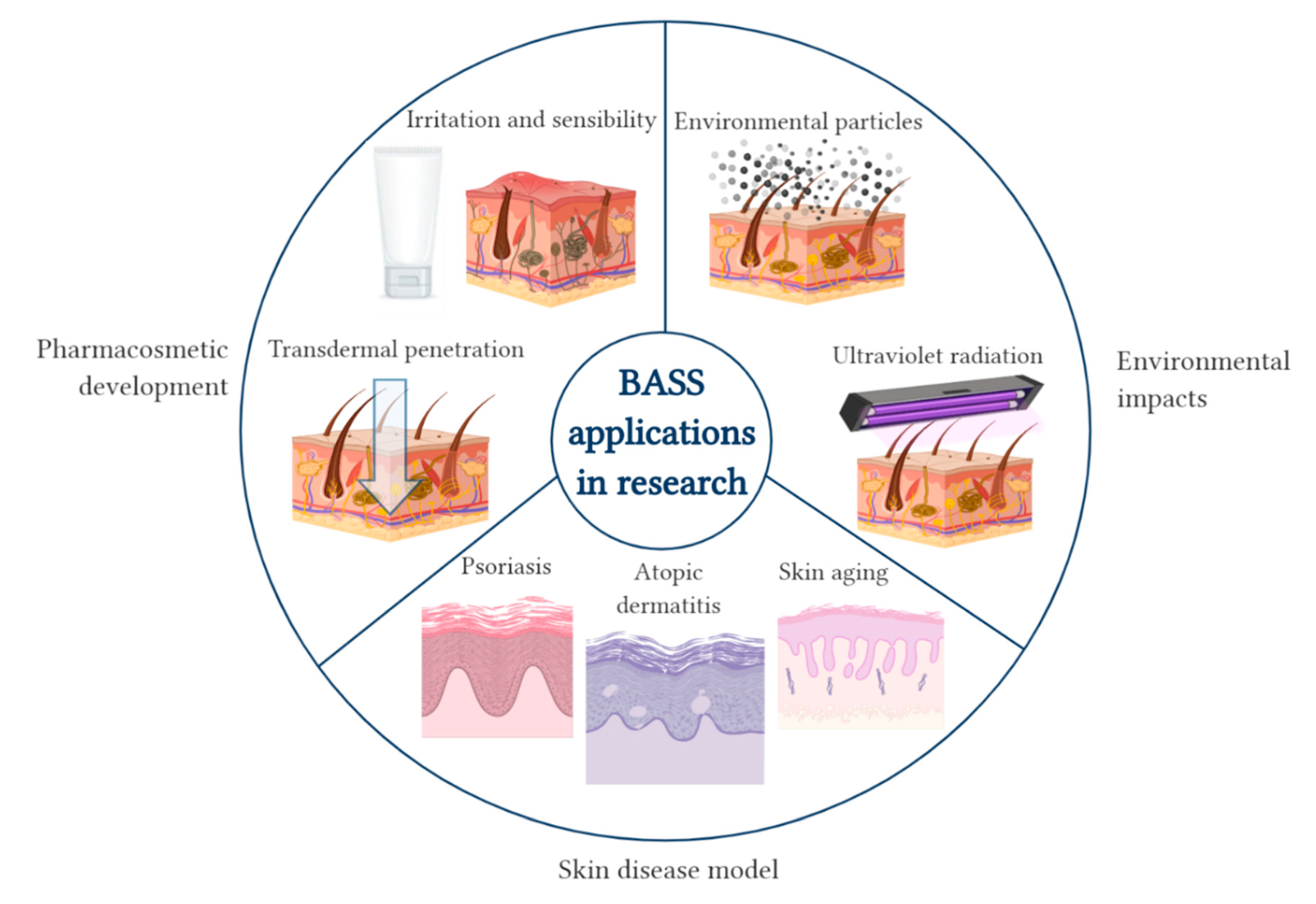
4. Human Artificial Skin: In Vitro Model to Research
4.1. Pharmacosmetic Development
4.1.1. Irritation and Sensibility Test
Cellular Model
Reconstructed Human Epithelium
Limitations and Perspectives
4.1.2. Transdermal Penetration Studies
Penetration Studies through a Damaged Epithelium
Limitations
4.2. Skin Characterization
4.2.1. Tritiated Water Flux (TWF)
4.2.2. Electrical Resistance (ER)
4.2.3. TransEpidermal Water Loss (TEWL)
4.3. Skin Disease Models
4.3.1. Skin Substitute with Atopic Dermatitis (AD)
4.3.2. Human Psoriatic Skin Substitute
4.3.3. Skin Aging Model
4.4. Assessment of Environmental Impacts on the Skin
4.4.1. Impact of Fine Environmental Particles
4.4.2. Impact of Ultraviolet Radiation
5. Perspectives
Funding
Conflicts of Interest
Abbreviations
| AD | Atopic Dermatitis |
| AhR | Aryl Hydrocarbon Receptor |
| BASS | Bioengineered Artificial Skin Substitutes |
| ECM | Extracellular Matrix |
| ER | Electrical Resistance |
| FBS | Fetal Bovine Serum |
| FDA | Food and Drug Administration |
| FLG | Filaggrin |
| GMP | Good Manufacturing Practices |
| GTP | Good Tissue Practices |
| HF | Human Fibroblasts |
| IL | Interleukins |
| IMT | Intima-Media Thickness |
| iPSC | Induced Pluripotent Stem Cells |
| ITG | Integrin |
| IVL | Involucrin |
| KG | Dipotassium Glycyrrhizinate |
| KRT | Keratin |
| MF | Murine Fibroblasts |
| MMP | Matrix Metalloproteinase |
| NK | Natural Killer Cell Conditioned Medium (NK-CdM) |
| NLC | Nanostructured Lipid Carrier |
| NR | Neutral Color |
| LDH | Lactate Dehydrogenase |
| LN | Laminin |
| LOR | Loricrin |
| NLC | Nanostructured Lipid Carrier |
| OECD | Organisation for Economic Co-operation and Development |
| OECD TG | Organisation for Economic Co-operation and Development Test Guideliness |
| PAMPA | Parallel Artificial Membrane Permeability Assay |
| ROS | Reactive Oxygen Species |
| SC | Stratum Corneum |
| TE | Tissue Engineering |
| TEWL | Transepidermal Water Loss |
| TIMP | Tissue Inhibitor Metallopeptidase |
| TSLP | Thymic Stromal Lymphopoeitin |
| TWF | Tritiated Water Flux |
| UV | Ultraviolet Radiation |
| VEGF | Vascular Endothelial Growth Factor |
References
- Chandra, P.K.; Soker, S.; Atala, A. Tissue engineering: Current status and future perspectives. In Principles of Tissue Engineering; Lanza, R., Langer, R., Vacanti, J., Atala, A., Eds.; Academic Press: Winston-Salem, NC, USA, 2020; Volume 7, p. 1800457. ISBN 9780128184226. [Google Scholar]
- Lee, K.H. Tissue-engineered Human Living Skin Substitutes: Development and Clinical Application. Yonsei Med. J. 2000, 41, 774–779. [Google Scholar] [CrossRef] [PubMed]
- Burger, S.R. Current regulatory issues in cell and tissue therapy. Cytotherapy 2003, 5, 289–298. [Google Scholar] [CrossRef] [PubMed]
- Fernández-González, A.; Lizana-Moreno, A.; Ruiz-Garcia, A.; Guerrero-Calvo, J.; Espinosa, O.; Fernández, N.; Ordonez-Luque, A.; Sierra-Sanchez, A.; Arias-Santiago, S. Optimization of an autologous human skin model under GMP guidelines. Cytotherapy 2017, 19, S232–S233. [Google Scholar] [CrossRef]
- Carriel, V.; Garzón, I.; Jiménez, J.M.; Oliveira, A.C.X.; Arias-Santiago, S.; Campos, A.; Sánchez-Quevedo, M.C.; Alaminos, M. Epithelial and stromal developmental patterns in a novel substitute of the human skin generated with fibrin-agarose biomaterials. Cells Tissues Organs 2012, 196, 1–12. [Google Scholar] [CrossRef]
- Egea-Guerrero, J.J.; Carmona, G.; Correa, E.; Mata, R.; Arias-Santiago, S.; Alaminos, M.; Gacto, P.; Cuende, N. Transplant of Tissue-Engineered Artificial Autologous Human Skin in Andalusia: An Example of Coordination and Institutional Collaboration. Transplant. Proc. 2019, 51, 3047–3050. [Google Scholar] [CrossRef] [PubMed]
- Fernández-González, A.; Lizana-Moreno, A.; Fernández, N.; Guerrero-Calvo, J.; Ruiz-Garcia, A.; Espinosa, O.; Ordonez-Luque, A.; Sierra-Sanchez, A.; Arias-Santiago, S. Clinical, histological and homeostasis evaluation of an autologous tissue bio-engineered skin substitute in a patient with 70% of total body surface area (TBSA) burn. Cytotherapy 2017, 19, S233. [Google Scholar] [CrossRef]
- Sierra-Sánchez, A.; Fernández-González, A.; Lizana-Moreno, A.; Espinosa-Ibáñez, O.; Martinez-Lopez, A.; Guerrero-Calvo, J.; Fernández-Porcel, N.; Ruiz-García, A.; Ordóñez-Luque, A.; Carriel, V.; et al. Hyaluronic acid biomaterial for human tissue-engineered skin substitutes: Preclinical comparative in vivo study of wound healing. J. Eur. Acad. Dermatol. Venereol. 2020, 34, 2414–2427. [Google Scholar] [CrossRef]
- Ścieżyńska, A.; Nogowska, A.; Sikorska, M.; Konys, J.; Karpińska, A.; Komorowski, M.; Ołdak, M.; Malejczyk, J. Isolation and culture of human primary keratinocytes—A methods review. Exp. Dermatol. 2019, 28, 107–112. [Google Scholar] [CrossRef]
- Dragúňová, J.; Kabát, P.; Koller, J. Skin explant cultures as a source of keratinocytes for cultivation. Cell Tissue Bank. 2013, 14, 317–324. [Google Scholar] [CrossRef]
- Park, H.S.; Kang, H.J.; Kim, C.H.; Kim, C.H.; Han, E.S.; Han, K.; Kim, T.H.; Gin, Y.J.; Son, Y.S. Application of Physical Force Is Essential to Enrich for Epidermal Stem Cells in Primary Human Keratinocyte Isolation. Tissue Eng. 2004, 10, 343–351. [Google Scholar] [CrossRef]
- Daniels, J.T.; Kearney, J.N.; Ingham, E. Human keratinocyte isolation and cell culture: A survey of current practices in the UK. Burns 1996, 22, 35–39. [Google Scholar] [CrossRef]
- Orazizadeh, M.; Hashemitabar, M.; Bahramzadeh, S.; Dehbashi, F.N.; Saremy, S. Comparison of the enzymatic and explant methods for the culture of keratinocytes isolated from human foreskin. Biomed. Rep. 2015, 3, 304–308. [Google Scholar] [CrossRef]
- Rheinwald, J.G.; Green, H. Formation of a keratinizing epithelium in culture by a cloned cell line derived from a teratoma. Cell 1975, 6, 317–330. [Google Scholar] [CrossRef]
- Tenchini, M.L.; Ranzati, C.; Malcovati, M. Culture techniques for human keratinocytes. Burns 1992, 18, S11–S16. [Google Scholar] [CrossRef]
- Limat, A.; Hunziker, T.; Boillat, C.; Bayreuther, K.; Noser, F. Post-mitotic human dermal fibroblasts efficiently support the growth of human follicular keratinocytes. J. Investig. Dermatol. 1989, 92, 758–762. [Google Scholar] [CrossRef]
- ter Horst, B.; Chouhan, G.; Moiemen, N.S.; Grover, L.M. Advances in keratinocyte delivery in burn wound care. Adv. Drug Deliv. Rev. 2018, 123, 18–32. [Google Scholar] [CrossRef] [PubMed]
- Boyce, S.T.; Ham, R.G. Calcium-regulated differentiation of normal human epidermal keratinocytes in chemically defined clonal culture and serum-free serial culture. J. Investig. Dermatol. 1983, 81, 33–40. [Google Scholar] [CrossRef] [PubMed]
- Tjin, M.S.; Chua, A.W.C.; Tryggvason, K. Chemically defined and xenogeneic-free culture method for human epidermal keratinocytes on laminin-based matrices. Nat. Protoc. 2020, 15, 694–711. [Google Scholar] [CrossRef]
- Lamb, R.; Ambler, C.A. Keratinocytes Propagated in Serum-Free, Feeder-Free Culture Conditions Fail to Form Stratified Epidermis in a Reconstituted Skin Model. PLoS ONE 2013, 8, e52494. [Google Scholar] [CrossRef] [PubMed]
- Coolen, N.A.; Verkerk, M.; Reijnen, L.; Vlig, M.; Van Den Bogaerdt, A.J.; Breetveld, M.; Gibbs, S.; Middelkoop, E.; Ulrich, M.M.W. Culture of keratinocytes for transplantation without the need of feeder layer cells. Cell Transplant. 2007, 16, 649–661. [Google Scholar] [CrossRef]
- Guerrero-Calvo, J.; Fernández-González, A.; Lizana-Moreno, A.; Montes-Ramos, P.; Fernández, N.; Ruiz-Garcia, A.; Espinosa, O.; Ordonez-Luque, A.; Sierra-Sanchez, A.; Arias-Santiago, S. Optimization of human keratinocyte culture to develop a tissue bio-engineered human skin model. Cytotherapy 2017, 19, S233–S234. [Google Scholar] [CrossRef]
- Ng, W.L.; Wang, S.; Yeong, W.Y.; Naing, M.W. Skin Bioprinting: Impending Reality or Fantasy? Trends Biotechnol. 2016, 34, 689–699. [Google Scholar] [CrossRef] [PubMed]
- Admane, P.; Gupta, A.C.; Jois, P.; Roy, S.; Chandrasekharan Lakshmanan, C.; Kalsi, G.; Bandyopadhyay, B.; Ghosh, S. Direct 3D bioprinted full-thickness skin constructs recapitulate regulatory signaling pathways and physiology of human skin. Bioprinting 2019, 15, e00051. [Google Scholar] [CrossRef]
- Dolbashid, A.S.; Mokhtar, M.S.; Muhamad, F.; Ibrahim, F. Potential applications of human artificial skin and electronic skin (e-skin): A review. Bioinspired Biomim. Nanobiomater. 2018, 7, 53–64. [Google Scholar] [CrossRef]
- Levin, J.; Maibach, H. The correlation between transepidermal water loss and percutaneous absorption: An overview. J. Control. Release 2005, 103, 291–299. [Google Scholar] [CrossRef]
- Walker, M.; Dugard, P.H.; Scott, R.C. Invitro percutaneous-absorption studies-A comparison of human and laboratory species. Hum. Toxicol. 1983, 2, 561–562. [Google Scholar]
- Bronaugh, R.L.; Stewart, R.F. Methods for in vitro percutaneous absorption studies V: Permeation through damaged skin. J. Pharm. Sci. 1985, 75, 487–491. [Google Scholar] [CrossRef]
- Sun, T.; Jackson, S.; Haycock, J.W.; MacNeil, S. Culture of skin cells in 3D rather than 2D improves their ability to survive exposure to cytotoxic agents. J. Biotechnol. 2006, 112, 372–381. [Google Scholar] [CrossRef]
- Robinson, M.K.; Osborne, R.; Perkins, M.A. Strategies for the assessment of acute skin irritation potential. J. Pharmacol. Toxicol. Methods 1999, 42, 1–9. [Google Scholar] [CrossRef]
- Tulloch, G. Animal ethics: The capabilities approach. Anim. Welf. 2011, 20, 3–10. [Google Scholar]
- Pervin, S.; Ranchhod, A.; Wilman, M. Trends in cosmetics purchase: Ethical perceptions of consumers in different cultures. A cross country comparative study between South Asian and Western consumers. J. Cust. Behav. 2014, 13, 57–72. [Google Scholar] [CrossRef]
- Broom, D.M. A History of Animal Welfare Science. Acta Biotheor. 2011, 59, 121–137. [Google Scholar] [CrossRef] [PubMed]
- Pfuhler, S.; Kirst, A.; Aardema, M.; Banduhn, N.; Goebel, C.; Araki, D.; Costabel-Farkas, M.; Dufour, E.; Fautz, R.; Harvey, J.; et al. A tiered approach to the use of alternatives to animal testing for the safety assessment of cosmetics: Genotoxicity. A COLIPA analysis. Regul. Toxicol. Pharmacol. 2010, 57, 315–324. [Google Scholar] [CrossRef]
- Weltzien, H.U.; Corsini, E.; Gibbs, S.; Lindstedt, M.; Borrebaeck, C.; Budde, P.; Schulz-Knappe, P.; Thierse, H.J.; Martin, S.F.; Roggen, E.L. Safe cosmetics without animal testing? Contributions of the EU Project Sens-it-iv. J. Verbrauch. Leb. 2009, 4, 41–48. [Google Scholar] [CrossRef][Green Version]
- Becker, R.A.; Borgert, C.J.; Webb, S.; Ansell, J.; Amundson, S.; Portier, C.J.; Goldberg, A.; Bruner, L.H.; Rowan, A.; Curren, R.D.; et al. Report of an ISRTP Workshop: Progress and barriers to incorporating alternative toxicological methods in the U.S. Regul. Toxicol. Pharmacol. 2006, 46, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Bottini, A.A.; Hartung, T. Food for thought... on the economics of animal testing. ALTEX 2009, 26, 3–16. [Google Scholar] [CrossRef]
- Adler, S.; Basketter, D.; Creton, S.; Pelkonen, O.; Van Benthem, J.; Zuang, V.; Andersen, K.E.; Angers-Loustau, A.; Aptula, A.; Bal-Price, A.; et al. Alternative (non-animal) methods for cosmetics testing: Current status and future prospects-2010. Arch. Toxicol. 2011, 85, 367–485. [Google Scholar] [CrossRef]
- Bertolini, M.; Ramot, Y.; Gherardini, J.; Heinen, G.; Chéret, J.; Welss, T.; Giesen, M.; Funk, W.; Paus, R. Theophylline exerts complex anti-ageing and anti-cytotoxicity effects in human skin ex vivo. Int. J. Cosmet. Sci. 2020, 42, 79–88. [Google Scholar] [CrossRef]
- Gherardini, J.; Wegner, J.; Chéret, J.; Ghatak, S.; Lehmann, J.; Alam, M.; Jimenez, F.; Funk, W.; Böhm, M.; Botchkareva, N.V.; et al. Transepidermal UV radiation of scalp skin ex vivo induces hair follicle damage that is alleviated by the topical treatment with caffeine. Int. J. Cosmet. Sci. 2019, 41, 164–182. [Google Scholar] [CrossRef]
- Fischer, T.W.; Bergmann, A.; Kruse, N.; Kleszczynski, K.; Skobowiat, C.; Slominski, A.T.; Paus, R. New effects of caffeine on corticotropin-releasing hormone (CRH)-induced stress along the intrafollicular classical hypothalamic–pituitary–adrenal (HPA) axis (CRH-R1/2, IP3-R, ACTH, MC-R2) and the neurogenic non-HPA axis (substance P, p75NTR and TrkA) in ex vivo human male androgenetic scalp hair follicles. Br. J. Dermatol. 2020. [Google Scholar] [CrossRef]
- Jimenez, F.; López, E.; Bertolini, M.; Alam, M.; Chéret, J.; Westgate, G.; Rinaldi, F.; Marzani, B.; Paus, R. Topical odorant application of the specific olfactory receptor OR2AT4 agonist, Sandalore®, improves telogen effluvium-associated parameters. J. Cosmet. Dermatol. 2020, 1–8, Online ahead of print. [Google Scholar] [CrossRef] [PubMed]
- Schuppli, C.A. Decisions about the use of animals in research: Ethical reflection by animal ethics committee members. Anthrozoos 2011, 24, 409–425. [Google Scholar] [CrossRef]
- Danilenko, D.M.; Phillips, G.D.L.; Diaz, D. In Vitro Skin Models and Their Predictability in Defining Normal and Disease Biology, Pharmacology, and Toxicity. Toxicol. Pathol. 2016, 44, 555–563. [Google Scholar] [CrossRef] [PubMed]
- Johnson, E.W.; Meunier, S.F.; Roy, C.J.; Parenteau, N.L. Serial cultivation of normal human keratinocytes: A defined system for studying the regulation of growth and differentiation. Vitr. Cell. Dev. Biol. Anim. 1992, 28, 429–435. [Google Scholar] [CrossRef]
- Boehnke, K.; Mirancea, N.; Pavesio, A.; Fusenig, N.E.; Boukamp, P.; Stark, H.J. Effects of fibroblasts and microenvironment on epidermal regeneration and tissue function in long-term skin equivalents. Eur. J. Cell Biol. 2007, 86, 731–746. [Google Scholar] [CrossRef] [PubMed]
- Welss, T.; Basketter, D.A.; Schröder, K.R. In vitro skin irritation: Facts and future. State of the art review of mechanisms and models. Toxicol. Vitr. 2004, 18, 231–243. [Google Scholar] [CrossRef] [PubMed]
- Groeber, F.; Holeiter, M.; Hampel, M.; Hinderer, S.; Schenke-Layland, K. Skin tissue engineering—In vivo and in vitro applications. Adv. Drug Deliv. Rev. 2011, 63, 352–366. [Google Scholar] [CrossRef]
- Lee, M.; Hwang, J.H.; Lim, K.M. Alternatives to in vivo Draize rabbit eye and skin irritation tests with a focus on 3D reconstructed human cornea-like epithelium and epidermis models. Toxicol. Res. 2017, 33, 191–203. [Google Scholar] [CrossRef]
- Wilhelmus, K.R. The Draize eye test. Surv. Ophthalmol. 2001, 45, 493–515. [Google Scholar] [CrossRef]
- Sanchez, L.; Mitjans, M.; Infante, M.R.; Vinardell, M.P. Potential irritation of lysine derivative surfactants by hemolysis and HaCaT cell viability. Toxicol. Lett. 2006, 161, 53–60. [Google Scholar] [CrossRef]
- Roguet, R. Use of skin cell cultures for in vitro assessment of corrosion and cutaneous irritancy. Cell Biol. Toxicol. 1999, 15, 63–75. [Google Scholar] [CrossRef]
- OECD. In Vitro Skin Irritation—Reconstructed Human Epidermis Test Method. In OECD Guidelines for the Testing of Chemicals; No. 439; Section 4; OECD: Paris, France, 2015. [Google Scholar]
- Zungu, I.L.; Hawkins Evans, D.; Abrahamse, H. Mitochondrial responses of normal and injured human skin fibroblasts following low level laser irradiation—An in vitro study. Photochem. Photobiol. 2009, 85, 987–996. [Google Scholar] [CrossRef] [PubMed]
- Bauhammer, I.; Sacha, M.; Haltner, E. Validation and stability analysis of a modified lactate dehydrogenase (LDH)test method to be employed for an in vitro viable skin model. Heliyon 2019, 5, e01618. [Google Scholar] [CrossRef] [PubMed]
- Eun, H.C.; Suh, D.H. Comprehensive outlook of in vitro tests for assessing skin irritancy as alternatives to Draize tests. J. Dermatol. Sci. 2000, 24, 77–91. [Google Scholar] [CrossRef]
- Schmidt, F.F.; Nowakowski, S.; Kluger, P.J. Improvement of a Three-Layered in vitro Skin Model for Topical Application of Irritating Substances. Front. Bioeng. Biotechnol. 2020, 8. [Google Scholar] [CrossRef]
- Jusoh, N.; Ko, J.; Jeon, N.L. Microfluidics-based skin irritation test using in vitro 3D angiogenesis platform. APL Bioeng. 2019, 3, 036101. [Google Scholar] [CrossRef]
- Coquette, A.; Berna, N.; Poumay, Y.; Pittelkow, M. The keratinocyte in cutaneous irritation and sensitization: Chapter 9. In Biochemical Modulation of Skin Reactions. Transdermals, Topicals, Cosmetics; Agis, F., John, K., Wille, J., Eds.; CRC Press: Boca Raton, FL, USA, 2000; pp. 125–143. [Google Scholar]
- Zsikó, S.; Csányi, E.; Kovács, A.; Budai-Szűcs, M.; Gácsi, A.; Berkó, S. Methods to evaluate skin penetration in vitro. Sci. Pharm. 2019, 87, 19. [Google Scholar] [CrossRef]
- Traynor, M.J.; Wilkinson, S.C.; Williams, F.M. The influence of water mixtures on the dermal absorption of glycol ethers. Toxicol. Appl. Pharmacol. 2007, 218, 128–134. [Google Scholar] [CrossRef]
- Williams, A.C.; Barry, B.W. Penetration enhancers. Adv. Drug Deliv. Rev. 2012, 64, 128–137. [Google Scholar] [CrossRef]
- Zsikó, S.; Cutcher, K.; Kovács, A.; Budai-Szűcs, M.; Gácsi, A.; Baki, G.; Csányi, E.; Berkó, S. Nanostructured lipid carrier gel for the dermal application of lidocaine: Comparison of skin penetration testing methods. Pharmaceutics 2019, 11, 310. [Google Scholar] [CrossRef]
- Davies, D.J.; Heylings, J.R.; Gayes, H.; McCarthy, T.J.; Mack, M.C. Further development of an in vitro model for studying the penetration of chemicals through compromised skin. Toxicol. Vitr. 2017, 38, 101–107. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Davies, D.J.; Heylings, J.R.; McCarthy, T.J.; Correa, C.M. Development of an in vitro model for studying the penetration of chemicals through compromised skin. Toxicol. Vitr. 2015, 29, 176–181. [Google Scholar] [CrossRef]
- Trebilcock, K.L.; Heylings, J.R.; Wilks, M.F. In vitro tape stripping as a model for in vivo skin stripping. Toxicol. Vitr. 1994, 8, 665–667. [Google Scholar] [CrossRef]
- Dong, P.; Nikolaev, V.; Kröger, M.; Zoschke, C.; Darvin, M.E.; Witzel, C.; Lademann, J.; Patzelt, A.; Schäfer-Korting, M.; Meinke, M.C. Barrier-disrupted skin: Quantitative analysis of tape and cyanoacrylate stripping efficiency by multiphoton tomography. Int. J. Pharm. 2020, 574, 118843. [Google Scholar] [CrossRef]
- Fasano, W.J.; Manning, L.A.; Green, J.W. Rapid integrity assessment of rat and human epidermal membranes for in vitro dermal regulatory testing: Correlation of electrical resistance with tritiated water permeability. Toxicol. Vitr. 2002, 16, 731–740. [Google Scholar] [CrossRef]
- Nangia, A.; Patil, S.; Berner, B.; Boman, A.; Maibach, H. In vitro measurement of transepidermal water loss: A rapid alternative to tritiated water permeation for assessing skin barrier functions. Int. J. Pharm. 1998, 170, 33–40. [Google Scholar] [CrossRef]
- Zhang, Q.; Murawsky, M.; LaCount, T.; Kasting, G.B.; Li, S.K. Transepidermal water loss and skin conductance as barrier integrity tests. Toxicol. Vitr. 2018, 51, 129–135. [Google Scholar] [CrossRef]
- Elmahjoubi, E.; Frum, Y.; Eccleston, G.M.; Wilkinson, S.C.; Meidan, V.M. Transepidermal water loss for probing full-thickness skin barrier function: Correlation with tritiated water flux, sensitivity to punctures and diverse surfactant exposures. Toxicol. Vitr. 2009, 23, 1429–1435. [Google Scholar] [CrossRef]
- Davies, D.J.; Ward, R.J.; Heylings, J.R. Multi-species assessment of electrical resistance as a skin integrity marker for in vitro percutaneous absorption studies. Toxicol. Vitr. 2004, 18, 351–358. [Google Scholar] [CrossRef]
- Alexander, H.; Brown, S.; Danby, S.; Flohr, C. Research Techniques Made Simple: Transepidermal Water Loss Measurement as a Research Tool. J. Investig. Dermatol. 2018, 138, 2295–2300. [Google Scholar] [CrossRef] [PubMed]
- Farahmand, S.; Tien, L.; Hui, X.; Maibach, H.I. Measuring transepidermal water loss: A comparative in vivo study of condenser-chamber, unventilated-chamber and open-chamber systems. Ski. Res. Technol. 2009, 15, 392–398. [Google Scholar] [CrossRef] [PubMed]
- Fluhr, J.W.; Feingold, K.R.; Elias, P.M. Transepidermal water loss reflects permeability barrier status: Validation in human and rodent in vivo and ex vivo models. Exp. Dermatol. 2006, 15, 483–492. [Google Scholar] [CrossRef]
- Brancaleon, L.; Bamberg, M.P.; Sakamaki, T.; Kollias, N. Attenuated total reflection-fourier transfrom infrared spectroscopy as a possible method to investigate biophysical parameters of stratum corneum in vivo. J. Investig. Dermatol. 2001, 116, 380–386. [Google Scholar] [CrossRef] [PubMed]
- Kelleher, M.; Dunn-Galvin, A.; Hourihane, J.O.B.; Murray, D.; Campbell, L.E.; McLean, W.H.I.; Irvine, A.D. Skin barrier dysfunction measured by transepidermal water loss at 2 days and 2 months predates and predicts atopic dermatitis at 1 year. J. Allergy Clin. Immunol. 2015, 135, 930–935. [Google Scholar] [CrossRef]
- Kuntsche, J.; Bunjes, H.; Fahr, A.; Pappinen, S.; Rönkkö, S.; Suhonen, M.; Urtti, A. Interaction of lipid nanoparticles with human epidermis and an organotypic cell culture model. Int. J. Pharm. 2008, 354, 180–195. [Google Scholar] [CrossRef]
- Chilcott, R.P.; Dalton, C.H.; Emmanuel, A.J.; Allen, C.E.; Bradley, S.T. Transepidermal water loss does not correlate with skin barrier function in vitro. J. Investig. Dermatol. 2002, 118, 871–875. [Google Scholar] [CrossRef]
- Cristiano, M.C.; Froiio, F.; Mancuso, A.; Iannone, M.; Fresta, M.; Fiorito, S.; Celia, C.; Paolino, D. In vitro and in vivo trans-epidermal water loss evaluation following topical drug delivery systems application for pharmaceutical analysis. J. Pharm. Biomed. Anal. 2020, 186. [Google Scholar] [CrossRef]
- Feingold, K.R. The outer frontier: The importance of lipid metabolism in the skin. J. Lipid Res. 2009, 50, S417–S422. [Google Scholar] [CrossRef]
- Drucker, A.M.; Wang, A.R.; Li, W.Q.; Sevetson, E.; Block, J.K.; Qureshi, A.A. The Burden of Atopic Dermatitis: Summary of a Report for the National Eczema Association. J. Investig. Dermatol. 2017, 137, 26–30. [Google Scholar] [CrossRef]
- Huet, F.; Severino-Freire, M.; Chéret, J.; Gouin, O.; Praneuf, J.; Pierre, O.; Misery, L.; Le Gall-Ianotto, C. Reconstructed human epidermis for in vitro studies on atopic dermatitis: A review. J. Dermatol. Sci. 2018, 89, 213–218. [Google Scholar] [CrossRef]
- Searing, D.A.; Leung, D.Y.M. Vitamin D in atopic dermatitis, asthma and allergic diseases. Immunol. Allergy Clin. North Am. 2010, 30, 397–409. [Google Scholar] [CrossRef]
- Bieber, T. Atopic dermatitis. Ann. Dermatol. 2010, 358, 1483–1494. [Google Scholar] [CrossRef] [PubMed]
- Viada Peláez, M.C.; Leschinsky, V.; Gomila, A. Atopic dermatitis in children and vitamin D. A retrospective analytical study. Rev. Methodo 2019, 4. [Google Scholar]
- Frankart, A.; Malaisse, J.; De Vuyst, E.; Minner, F.; de Rouvroit, C.L.; Poumay, Y. Epidermal morphogenesis during progressive in vitro 3D reconstruction at the air-liquid interface. Exp. Dermatol. 2012, 21, 871–875. [Google Scholar] [CrossRef] [PubMed]
- Le Lamer, M.; Pellerin, L.; Reynier, M.; Cau, L.; Pendaries, V.; Leprince, C.; Méchin, M.C.; Serre, G.; Paul, C.; Simon, M. Defects of corneocyte structural proteins and epidermal barrier in atopic dermatitis. Biol. Chem. 2015, 396, 1163–1179. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.E.; Leung, D.Y.M.; Boguniewicz, M.; Howell, M.D. Loricrin and involucrin expression is down-regulated by Th2 cytokines through STAT-6. Clin. Immunol. 2008, 126, 332–337. [Google Scholar] [CrossRef]
- Weidinger, S.; Rodríguez, E.; Stahl, C.; Wagenpfeil, S.; Klopp, N.; Illig, T.; Novak, N. Filaggrin mutations strongly predispose to early-onset and extrinsic atopic dermatitis. Investig. Dermatol. 2007, 127, 0022-202X. [Google Scholar] [CrossRef]
- Janssens, M.; Van Smeden, J.; Gooris, G.S.; Bras, W.; Portale, G.; Caspers, P.J.; Vreeken, R.J.; Hankemeier, T.; Kezic, S.; Wolterbeek, R.; et al. Increase in short-chain ceramides correlates with an altered lipid organization and decreased barrier function in atopic eczema patients. J. Lipid Res. 2012, 53, 2755–2766. [Google Scholar] [CrossRef]
- Heratizadeh, A.; Werfel, T. Anti-inflammatory therapies in atopic dermatitis. Allergy Eur. J. Allergy Clin. Immunol. 2016, 71, 1666–1675. [Google Scholar] [CrossRef]
- Lebonvallet, N.; Jeanmaire, C.; Danoux, L.; Sibille, P.; Pauly, G.; Misery, L. The evolution and use of skin explants: Potential and limitations for dermatological research. Eur. J. Dermatol. 2010, 20, 671–684. [Google Scholar]
- Lee, S.H.; Bae, I.H.; Choi, H.; Choi, H.W.; Oh, S.; Marinho, P.A.; Min, D.J.; Kim, D.Y.; Lee, T.R.; Lee, C.S.; et al. Ameliorating effect of dipotassium glycyrrhizinate on an IL-4- and IL-13-induced atopic dermatitis-like skin-equivalent model. Arch. Dermatol. Res. 2019, 311, 131–140. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Michael, S.; Bharti, K.; Ferrer, M.; Song, M.J. A biofabricated vascularized skin model of atopic dermatitis for preclinical studies. Biofabrication 2020, 12, 035002. [Google Scholar] [CrossRef] [PubMed]
- Lowes, M.A.; Bowcock, A.M.; Krueger, J.G. Pathogenesis and therapy of psoriasis. Nature 2007, 445, 866–873. [Google Scholar] [CrossRef]
- Grozdev, I.; Korman, N.; Tsankov, N. Psoriasis as a systemic disease. Clin. Dermatol. 2014, 32, 343–350. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Lopez, A.; Blasco-Morente, G.; Perez-Lopez, I.; Tercedor-Sanchez, J.; Arias-Santiago, S. Studying the effect of systemic and biological drugs on intima-media thickness in patients suffering from moderate and severe psoriasis. J. Eur. Acad. Dermatol. Venereol. 2018, 32, 1492–1498. [Google Scholar] [CrossRef]
- Rachakonda, T.D.; Schupp, C.W.; Armstrong, A.W. Psoriasis prevalence among adults in the United States. J. Am. Acad. Dermatol. 2014, 70, 512–516. [Google Scholar] [CrossRef]
- Zollner, T.M.; Renz, H.; Igney, F.H.; Asadullah, K. Animal models of T-cell-mediated skin diseases. BioEssays 2004, 255. [Google Scholar] [CrossRef]
- Benam, K.H.; Dauth, S.; Hassell, B.; Herland, A.; Jain, A.; Jang, K.J.; Karalis, K.; Kim, H.J.; MacQueen, L.; Mahmoodian, R.; et al. Engineered in vitro disease models. Annu. Rev. Pathol. Mech. Dis. 2015, 10, 195–262. [Google Scholar] [CrossRef]
- Rioux, G.; Pouliot-Bérubé, C.; Simard, M.; Benhassine, M.; Soucy, J.; Guérin, S.L.; Pouliot, R. The tissue-engineered human psoriatic skin substitute: A valuable in vitro model to identify genes with altered expression in lesional psoriasis. Int. J. Mol. Sci. 2018, 19, 2923. [Google Scholar] [CrossRef]
- Niehues, H.; van den Bogaard, E.H. Past, present and future of in vitro 3D reconstructed inflammatory skin models to study psoriasis. Exp. Dermatol. 2018, 27, 512–519. [Google Scholar] [CrossRef]
- Oestreicher, J.L.; Walters, I.B.; Kikuchi, T.; Gilleaudeau, P.; Surette, J.; Schwertschlag, U.; Dorner, A.J.; Krueger, J.G.; Trepicchio, W.L. Molecular classification of psoriasis diseaseassociated genes through pharmacogenomic expression profiling. Pharmacogenom. J. 2001, 1, 272–287. [Google Scholar] [CrossRef]
- Martin, G.; Guérard, S.; Fortin, M.M.R.; Rusu, D.; Soucy, J.; Poubelle, P.E.; Pouliot, R. Pathological crosstalk in vitro between T lymphocytes and lesional keratinocytes in psoriasis: Necessity of direct cell-to-cell contact. Lab. Investig. 2012, 92, 1058–1070. [Google Scholar] [CrossRef] [PubMed]
- Hohl, D. Expression patterns of loricrin in dermatological disorders. Am. J. Dermatopathol. 1993, 15, 20–27. [Google Scholar] [CrossRef]
- Rashmi, R.; Rao, K.S.J.; Basavaraj, K.H. A comprehensive review of biomarkers in psoriasis. Clin. Exp. Dermatol. 2009, 34, 658–663. [Google Scholar] [CrossRef] [PubMed]
- Slominski, A.; Zbytek, B.; Szczesniewski, A.; Wortsman, J. Cultured human dermal fibroblasts do produce cortisol. J. Investig. Dermatol. 2006, 126, 1177. [Google Scholar] [CrossRef]
- Hannen, R.F.; Michael, A.E.; Jaulim, A.; Bhogal, R.; Burrin, J.M.; Philpott, M.P. Steroid synthesis by primary human keratinocytes; implications for skin disease. Biochem. Biophys. Res. Commun. 2011, 404, 62–67. [Google Scholar] [CrossRef] [PubMed]
- Simard, M.; Morin, S.; Rioux, G.; Séguin, R.; Loing, E.; Pouliot, R. A tissue-engineered human psoriatic skin model to investigate the implication of camp in psoriasis: Differential impacts of cholera toxin and isoproterenol on camp levels of the epidermis. Int. J. Mol. Sci. 2020, 21, 5215. [Google Scholar] [CrossRef]
- Popa, R.S. Psoriasis. Lancet 1997, 350, 349–353. [Google Scholar]
- Choi, D.H.; Hwang, H.S. Anti-inflammation activity of brazilin in TNF-α induced human psoriasis dermatitis skin model. Appl. Biol. Chem. 2019, 62, 46. [Google Scholar] [CrossRef]
- Uitto, J. Understanding Premature Skin Aging. N. Engl. J. Med. 1997, 337, 1463–1465. [Google Scholar] [CrossRef]
- Ganceviciene, R.; Liakou, A.I.; Theodoridis, A.; Makrantonaki, E.; Zouboulis, C.C. Skin anti-aging strategies. Dermatoendocrinology 2012, 4, 308–319. [Google Scholar] [CrossRef] [PubMed]
- Asselineau, D.; Ricois, S.; Pageon, H.; Zucchi, H.; Girardeau-Hubert, S.; Deneuville, C.; Haydont, V.; Neiveyans, V.; Lorthois, I. Reconstructed Skin to Create In Vitro Flexible Models of Skin Aging: New Results and Prospects. In Textbook of Aging Skin; Farage, M., Miller, K., Maibach, H., Eds.; Springer: Berlin/Heidelberg, Germany, 2017; pp. 1203–1228. ISBN 978-3-662-47398-6. [Google Scholar]
- Mine, S.; Fortunel, N.O.; Pageon, H.; Asselineau, D. Aging alters functionally human dermal papillary fibroblasts but not reticular fibroblasts: A new view of skin morphogenesis and aging. PLoS ONE 2008, 3, e4066. [Google Scholar] [CrossRef] [PubMed]
- Pageon, H.; Zucchi, H.; Asselineau, D. Distinct and complementary roles of papillary and reticular fibroblasts in skin morphogenesis and homeostasis. Eur. J. Dermatol. 2012, 22, 324–332. [Google Scholar] [CrossRef]
- Pageon, H.; Poumès-Ballihaut, C.; Zucchi, H.; Bastien, P.; Tancrede, E.; Asselineau, D. Aged Human Skin is More Susceptible than Young Skin to Accumulate Advanced Glycoxidation Products Induced by Sun Exposure. J. Aging Sci. 2013, 1, 112. [Google Scholar]
- Bernerd, F.; Asselineau, D.; Vioux, C.; Chevallier-Lagente, O.; Bouadjar, B.; Sarasin, A.; Magnaldo, T. Clues to epidermal cancer proneness revealed by reconstruction of DNA repair-deficient xeroderma pigmentosum skin in vitro. Proc. Natl. Acad. Sci. USA 2001, 98, 7817–7822. [Google Scholar] [CrossRef] [PubMed]
- Pageon, H.; Técher, M.P.; Asselineau, D. Reconstructed skin modified by glycation of the dermal equivalent as a model for skin aging and its potential use to evaluate anti-glycation molecules. Exp. Gerontol. 2008, 43, 584–588. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.J.; Chang, S.S.; Lee, J. Anti-aging potential of substance P-based hydrogel for human skin longevity. Int. J. Mol. Sci. 2019, 20, 4453. [Google Scholar] [CrossRef]
- Bataillon, M.; Lelièvre, D.; Chapuis, A.; Thillou, F.; Autourde, J.B.; Durand, S.; Boyera, N.; Rigaudeau, A.S.; Besné, I.; Pellevoisin, C. Characterization of a new reconstructed full thickness skin model, t-skinTM, and its application for investigations of anti-aging compounds. Int. J. Mol. Sci. 2019, 20, 2240. [Google Scholar] [CrossRef]
- Tran, C.; Michelet, J.F.; Simonetti, L.; Fiat, F.; Garrigues, A.; Potter, A.; Segot, E.; Watson, R.E.B.; Griffiths, C.E.M.; De Lacharrière, O. In vitro and in vivo studies with tetra-hydro-jasmonic acid (LR2412) reveal its potential to correct signs of skin ageing. J. Eur. Acad. Dermatol. Venereol. 2014, 28, 415–423. [Google Scholar] [CrossRef]
- Kim, K.E.; Cho, D.; Park, H.J. Air pollution and skin diseases: Adverse effects of airborne particulate matter on various skin diseases. Life Sci. 2016, 152, 126–134. [Google Scholar] [CrossRef]
- Dréno, B.; Bettoli, V.; Araviiskaia, E.; Sanchez Viera, M.; Bouloc, A. The influence of exposome on acne. J. Eur. Acad. Dermatol. Venereol. 2018, 32, 812–819. [Google Scholar] [CrossRef] [PubMed]
- Krutmann, J.; Bouloc, A.; Sore, G.; Bernard, B.A.; Passeron, T. The skin aging exposome. J. Dermatol. Sci. 2017, 85, 152–161. [Google Scholar] [CrossRef]
- Buendía-Eisman, A.; Prieto, L.; Abarquero, M.; Arias-Santiago, S. Study of the Exposome Ageing-related Factors in the Spanish Population. Acta Derm Venereol. 2020, 100. [Google Scholar] [CrossRef] [PubMed]
- Stefanovic, N.; Flohr, C.; Irvine, A.D. The exposome in atopic dermatitis. Allergy Eur. J. Allergy Clin. Immunol. 2020, 75, 63–74. [Google Scholar] [CrossRef] [PubMed]
- Hüls, A.; Vierkötter, A.; Gao, W.; Krämer, U.; Yang, Y.; Ding, A.; Stolz, S.; Matsui, M.; Kan, H.; Wang, S.; et al. Traffic-Related Air Pollution Contributes to Development of Facial Lentigines: Further Epidemiological Evidence from Caucasians and Asians. J. Investig. Dermatol. 2016, 136, 1053. [Google Scholar] [CrossRef]
- Puizina-Ivić, N. Skin aging. Acta Dermatovenerol. Alpina Pannonica Adriat. 2008, 17, 47. [Google Scholar]
- Krutmann, J.; Liu, W.; Li, L.; Pan, X.; Crawford, M.; Sore, G.; Seite, S. Pollution and skin: From epidemiological and mechanistic studies to clinical implications. J. Dermatol. Sci. 2014, 76, 163–168. [Google Scholar] [CrossRef]
- Bae, O.N.; Noh, M.; Chun, Y.J.; Jeong, T.C. Keratinocytic vascular endothelial growth factor as a novel biomarker for pathological skin condition. Biomol. Ther. 2015, 23, 12. [Google Scholar] [CrossRef]
- Pan, T.L.; Wang, P.W.; Aljuffali, I.A.; Huang, C.T.; Lee, C.W.; Fang, J.Y. The impact of urban particulate pollution on skin barrier function and the subsequent drug absorption. J. Dermatol. Sci. 2015, 78, 51–60. [Google Scholar] [CrossRef]
- Kandárová, H.; Liebsch, M.; Spielmann, H.; Genschow, E.; Schmidt, E.; Traue, D.; Guest, R.; Whittingham, A.; Warren, N.; Gamer, A.O.; et al. Assessment of the human epidermis model SkinEthic RHE for in vitro skin corrosion testing of chemicals according to new OECD TG 431. Toxicol. Vitr. 2006, 20, 547–559. [Google Scholar] [CrossRef]
- Verdin, A.; Cazier, F.; Fitoussi, R.; Blanchet, N.; Vié, K.; Courcot, D.; Momas, I.; Seta, N.; Achard, S. An in vitro model to evaluate the impact of environmental fine particles (PM 0.3-2.) on skin damage. Toxicol. Lett. 2019, 305, 94–102. [Google Scholar] [CrossRef] [PubMed]
- Boo, Y.C. Can plant phenolic compounds protect the skin from airborne particulate matter? Antioxidants 2019, 8, 379. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, B.K.; Kricker, A. The epidemiology of UV induced skin cancer. J. Photochem. Photobiol. B Biol. 2001, 63, 8–18. [Google Scholar] [CrossRef]
- Ramasamy, K.; Shanmugam, M.; Balupillai, A.; Govindhasamy, K.; Gunaseelan, S.; Muthusamy, G.; Robert, B.; Nagarajan, R. Ultraviolet radiation-induced carcinogenesis: Mechanisms and experimental models. J. Radiat. Cancer Res. 2017, 8, 4. [Google Scholar]
- Knak, A.; Regensburger, J.; Maisch, T.; Bäumler, W. Exposure of vitamins to UVB and UVA radiation generates singlet oxygen. Photochem. Photobiol. Sci. 2014, 13, 820–829. [Google Scholar] [CrossRef]
- Archambault, M.; Yaar, M.; Gilchrest, B.A. Keratinocytes and fibroblasts in a human skin equivalent model enhance melanocyte survival and melanin synthesis after ultraviolet irradiation. J. Investig. Dermatol. 1995, 104, 859–867. [Google Scholar] [CrossRef]
- Robinson, E.S.; Werth, V.P. The role of cytokines in the pathogenesis of cutaneous lupus erythematosus. Cytokine 2015, 73, 326–334. [Google Scholar] [CrossRef]
- Zhao, B.; Shah, P.; Qiang, L.; He, T.C.; Budanov, A.; He, Y.Y. Distinct Role of Sesn2 in Response to UVB-Induced DNA Damage and UVA-Induced Oxidative Stress in Melanocytes. Photochem. Photobiol. 2017, 93, 375–381. [Google Scholar] [CrossRef]
- Begović, L.; Antunovic, M.; Matic, I.; Furcic, I.; Baricevic, A.; Vojvoda Parcina, V.; Peharec Štefanić, P.; Nagy, B.; Marijanovic, I. Effect of UVC radiation on mouse fibroblasts deficient for FAS-associated protein with death domain. Int. J. Radiat. Biol. 2016, 92, 475–482. [Google Scholar] [CrossRef]
- Wang, Y.; Lauer, M.E.; An, S.; Mack, J.A.; Maytin, E.V. Hyaluronan synthase 2 protects skin fibroblasts against apoptosis induced by environmental stress. J. Biol. Chem. 2014, 289, 32253–32265. [Google Scholar] [CrossRef]
- Niu, T.; Tian, Y.; Ren, Q.; Wei, L.; Li, X.; Cai, Q. Red light interferes in UVA-induced photoaging of human skin fibroblast cells. Photochem. Photobiol. 2014, 90, 1349–1358. [Google Scholar] [CrossRef]
- Schreiber, S.; Mahmoud, A.; Vuia, A.; Rübbelke, M.K.; Schmidt, E.; Schaller, M.; Kandárová, H.; Haberland, A.; Schäfer, U.F.; Bock, U.; et al. Reconstructed epidermis versus human and animal skin in skin absorption studies. Toxicol. Vitr. 2005, 19, 813–822. [Google Scholar] [CrossRef]
- Park, G.; Baek, S.; Kim, J.E.; Lim, T.G.; Lee, C.C.; Yang, H.; Kang, Y.G.; Park, J.S.; Augustin, M.; Mrosek, M.; et al. Flt3 is a target of coumestrol in protecting against UVB-induced skin photoaging. Biochem. Pharmacol. 2015, 98, 473–483. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Liu, J.; Pang, D.; Li, T.; Liu, R.H. Mechanisms underlying the protective effects of blueberry extract against ultraviolet radiation in a skin cell co-culture system. J. Funct. Foods 2019, 52, 603–610. [Google Scholar] [CrossRef]
- Lee, S.E.; Kwon, T.R.; Kim, J.H.; Lee, B.C.; Oh, C.T.; Im, M.; Hwang, Y.K.; Paik, S.H.; Han, S.; Kim, J.Y.; et al. Anti-photoaging and anti-oxidative activities of natural killer cell conditioned medium following UV-B irradiation of human dermal fibroblasts and a reconstructed skin model. Int. J. Mol. Med. 2019, 44, 1641–1652. [Google Scholar] [CrossRef] [PubMed]
- Goyer, B.; Pereira, U.; Magne, B.; Larouche, D.; Kearns-Turcotte, S.; Rochette, P.J.; Martin, L.; Germain, L. Impact of ultraviolet radiation on dermal and epidermal DNA damage in a human pigmented bilayered skin substitute. J. Tissue Eng. Regen. Med. 2019, 13, 2300–2311. [Google Scholar] [CrossRef]
- Hill, D.S.; Robinson, N.D.P.; Caley, M.P.; Chen, M.; O’Toole, E.A.; Armstrong, J.L.; Przyborski, S.; Lovat, P.E. A novel fully humanized 3D skin equivalent to model early melanoma invasion. Mol. Cancer Ther. 2015, 14, 2665–2673. [Google Scholar] [CrossRef]
- Khademhosseini, A.; Langer, R. A decade of progress in tissue engineering. Nat. Protoc. 2016, 11, 1775–1781. [Google Scholar] [CrossRef]
- Schaller, M.; Schäfer, W.; Korting, H.C.; Hube, B. Differential expression of secreted aspartyl proteinases in a model of human oral candidosis and in patient samples from the oral cavity. Mol. Microbiol. 1998, 29, 605–615. [Google Scholar] [CrossRef]
- Graf, R.; Kock, M.; Bock, A.; Schubert-zsilavecz, M.; Steinhilber, D.; Kaufmann, R.; Gassenmeier, T.; Beschmann, H.; Bernd, A.; Kippenberger, S. Lipophilic prodrugs of amino acids and vitamin E as osmolytes for the compensation of hyperosmotic stress in human keratinocytes. Exp. Dermatol. 2009, 18, 370–377. [Google Scholar] [CrossRef]
- Wolff, E.F.; Altun, T.; Madankumar, R.; Pal, L.; Santoro, N.; Taylor, H.S. Skin wrinkles and rigidity in early postmenopausal women vary by race/ethnicity: Baseline characteristics of participants enrolled in the skin ancillary study of the keeps trial. Fertil. Steril. 2008, 90, S252. [Google Scholar] [CrossRef]
- McColl, M.; Boozalis, E.; Aguh, C.; Eseonu, A.C.; Okoye, G.A.; Kwatra, S.G. Pruritus in Black Skin: Unique Molecular Characteristics and Clinical Features. J. Natl. Med. Assoc. 2020. [Google Scholar] [CrossRef] [PubMed]
- Girardeau-Hubert, S.; Deneuville, C.; Pageon, H.; Abed, K.; Tacheau, C.; Cavusoglu, N.; Donovan, M.; Bernard, D.; Asselineau, D. Reconstructed Skin Models Revealed Unexpected Differences in Epidermal African and Caucasian Skin. Sci. Rep. 2019, 9, 1–12. [Google Scholar] [CrossRef]
- Muller, Q.; Beaudet, M.J.; De Serres-Bérard, T.; Bellenfant, S.; Flacher, V.; Berthod, F. Development of an innervated tissue-engineered skin with human sensory neurons and Schwann cells differentiated from iPS cells. Acta Biomater. 2018, 82, 93–101. [Google Scholar] [CrossRef]
| Toxicity Test | Genotoxicity Test | Efficacy Trials | Other Tests |
|---|---|---|---|
| Eye irritation (Invittox hemolysis test n 37, Model test of reconstituted human skin, Fluorescein leakage test method) Dermal irritation OECD 439 Dermal corrosion OECD 431; OECD 435 Nasal irritation Oral irritation Phototoxicity OECD 432 Cytotoxicity (MTT, XTT, Neutral red, Alamar Blue, LDH, MTS, Wst-8) | Ames test OECD 471 Mouse lymphoma assay OECD 476 Micronucleus test OECD 487 Comet assay | Cleaning efficacy Anti-angiogenic efficacy Anti-inflammatory efficacy Antioxidant efficacy Cell proliferation assay Cell cohesion test Anti-itch efficacy Lipolytic efficacy Collagen synthesis enhancement test Elastin synthesis test β-defensin synthesis increase assay Epidermal protease release assay Metalloprotease decrease assay Anti-growth factor action test Test of decrease in levels of human cathelicidin Healing efficacy Thermo-protective efficacy Reparative and regenerative efficacy Efficacy of anti-protective against dryness Moisturizing efficacy Antimicrobial efficacy | Percutaneous absorption and penetration OECD 428 Challenge test Microbiological controls Determination of active ingredients by chromatography Development and validation of analytical methods Nanotoxicology |
| Country | Average Expense |
|---|---|
| China | 32.14 |
| Saudi Arabia | 109.37 |
| Spain | 151.93 |
| Italy | 160.84 |
| Germany | 182.19 |
| United Kingdom | 206.06 |
| United States | 223.05 |
| Switzerland | 246.52 |
| Japan | 260.62 |
| OECD n | Trial Name and Description | Cell or Tissue |
|---|---|---|
| 428 | Skin absorption | Human or rodent skin |
| 430 | Dermal corrosion | Rat skin discs |
| 431 | Skin corrosion | Untransformed human keratinocytes |
| 432 | Phototoxicity | 3T3 cells |
| 435 | Dermal corrosion | Aqueous protein gel membrane |
| 439 | Skin irritation | Epidermal keratinocytes |
| 442D | Dermal sensitization | Immortalized transfected stable human keratinocytes |
| 442E | Dermal sensitization in vitro | THP-1 monocytic leukemia cells |
| 455 | Estrogen receptor agonists and antagonists | ERα-HeLa-9903 |
| 456 | Steroidogenesis | NCI-H295R cells |
| 458 | Transcriptional activation of stable receptor transfection human androgen | AR-EcoScreen cell line |
| 460 | Corrosion and severe eye irritation | MDCK CB997 cells |
| 471 | Bacterial reverse mutation | Salmonella typhimurium bacteria |
| 473 | Chromosomal aberrations in mammals | CHO, V79, CHL /IU, TK6 cells, primary lymphocytes |
| 476 | Cytotoxicity, genetic stability and gene mutations inmammals, like p53 | CHO, CHL, V79, L5178Y and TK6 cells |
| 487 | Mammalian micro-nuclei | CHO, CHL, V79, L5178Y and TK6 cells |
| 490 | Cytotoxicity, mutations in mammalian genes such as that of timidin-kinase | L5178Y and TK6 cells |
| 491 | Assessment of severe eye damage | SIRC monolayer cells |
| 492 | Serious eye damage or irritation | Human keratinocytes or human cornea cells |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sanabria-de la Torre, R.; Fernández-González, A.; Quiñones-Vico, M.I.; Montero-Vilchez, T.; Arias-Santiago, S. Bioengineered Skin Intended as In Vitro Model for Pharmacosmetics, Skin Disease Study and Environmental Skin Impact Analysis. Biomedicines 2020, 8, 464. https://doi.org/10.3390/biomedicines8110464
Sanabria-de la Torre R, Fernández-González A, Quiñones-Vico MI, Montero-Vilchez T, Arias-Santiago S. Bioengineered Skin Intended as In Vitro Model for Pharmacosmetics, Skin Disease Study and Environmental Skin Impact Analysis. Biomedicines. 2020; 8(11):464. https://doi.org/10.3390/biomedicines8110464
Chicago/Turabian StyleSanabria-de la Torre, Raquel, Ana Fernández-González, María I. Quiñones-Vico, Trinidad Montero-Vilchez, and Salvador Arias-Santiago. 2020. "Bioengineered Skin Intended as In Vitro Model for Pharmacosmetics, Skin Disease Study and Environmental Skin Impact Analysis" Biomedicines 8, no. 11: 464. https://doi.org/10.3390/biomedicines8110464
APA StyleSanabria-de la Torre, R., Fernández-González, A., Quiñones-Vico, M. I., Montero-Vilchez, T., & Arias-Santiago, S. (2020). Bioengineered Skin Intended as In Vitro Model for Pharmacosmetics, Skin Disease Study and Environmental Skin Impact Analysis. Biomedicines, 8(11), 464. https://doi.org/10.3390/biomedicines8110464









