Abstract
Vitiligo is a complex disorder with an important effect on the self-esteem and social life of patients. It is the commonest acquired depigmentation disorder characterized by the development of white macules resulting from the selective loss of epidermal melanocytes. The pathophysiology is complex and involves genetic predisposition, environmental factors, oxidative stress, intrinsic metabolic dysfunctions, and abnormal inflammatory/immune responses. Although several therapeutic options have been proposed to stabilize the disease by stopping the depigmentation process and inducing durable repigmentation, no specific cure has yet been defined, and the long-term persistence of repigmentation is unpredictable. Recently, due to the progressive loss of functional melanocytes associated with failure to spontaneously recover pigmentation, several different cell-based and cell-free regenerative approaches have been suggested to treat vitiligo. This review gives an overview of clinical and preclinical evidence for innovative regenerative approaches for vitiligo patients.
1. Introduction
Vitiligo is the commonest acquired pigmentary disorder, affecting 0.1–2% of the population worldwide [1,2], with no incidence difference between male and female [3]. While it can affect people of all ages, vitiligo appears more frequently before 20 years of age [4]. It is characterized by the progressive disappearance of skin melanocytes resulting in cosmetically white patches of skin depigmentation, occasionally associated with premature whiting, or graying of the hairs, eyelashes, eyebrows, beard, or mucous membranes, usually without clinical symptoms [1]. However, vitiligo has devastating impacts on the quality of life in affected individuals. Patients with vitiligo present lowered self-esteem, which, in turn, affects social life, frequently culminating in the development of depression [5]. Clinically, vitiligo is broadly categorized into segmental vitiligo (characterized by the unilateral distribution of lesions matching a dermatome) and nonsegmental vitiligo (generalized, including acrofacial) [6,7,8], mixed, and unclassified vitiligo (focal/mucosal) [9]. Rare subtypes comprise vitiligo punctata, follicular vitiligo, and hypochromic vitiligo [7]. The distinction between different subtypes of vitiligo is important for the prognosis and for treatment choice [10]. However, the choice of therapy considers several different parameters including the distribution and extension of the diseases, the patient’s age, the eventual presence of comorbidities, and patient preference. In vitiligo, treatment is challenging because of a complex multifactorial disease whose precise etiology is still unclear. The intricate disease puzzling combines multiple interconnected elements including genetic predisposition, environmental triggers, oxidative stress, intrinsic metabolic dysfunctions, and abnormal inflammatory/immune responses [6,11,12] (Figure 1). Several studies reported that over-activation of intracellular stress-related pathways in vitiligo melanocytes leads to the paracrine release of damage-associated molecular patterns (DAMPs) that locally stimulate the skin innate immune system that precedes adaptative immune response against melanocytes [13,14,15]. Moreover, melanocytes act as a sensor of specific pathogenic molecules produced by surrounding stressed cells via pattern recognition receptors (PRR) and then alert macrophages, neutrophils, fibroblasts, and keratinocytes through the release of interferon (IFN) type I and a wide range of cytokines and chemokines [16]. Melanocytes carry TLR 2, TLR4, TLR6, TLR7, TLR9, and TLR10, providing the potential to respond to pathogen infections and alarmins [17,18]. However, the intrinsic capacity to enhance inflammation makes melanocytes exposed to immune-based destruction [17]. The involvement of natural immunity in vitiligo is also supported by the more frequent presence of genetic DNA sequence variants in a critical innate immunity regulator gene, the NOD-like receptor 1 (NALP1), which has been also confirmed by immunohistochemical analysis [19]. Further, NLRP3 inflammasomes are activated in response to ROS [20] and mitochondrial stress [21], leading to subsequent processing of proinflammatory cytokine precursors (particularly IL1β and IL18) into mature forms that are subsequently secreted [22]. Expressions of NLRP3 and downstream cytokine IL1β are significantly increased in perilesional keratinocytes of patients with vitiligo. Correspondingly, the amount of circulating IL-1β correlates with disease activity and severity [23]. Macrophages, natural killer (NK) cells, and dendritic cells (DCs) all infiltrate active vitiligo lesional and to a lesser extent nonlesional skin [24]. In addition, the presence of high levels of the serine protease, granzyme B in the cytoplasmic granules of NK cells in vitiligo skin, is evidence of the remarkable cytotoxic capacity of these cells [24]. DCs present melanocyte-derived peptides to T cells, leading to their differentiation and production of interferon-γ (IFNγ) [25]. IFNγ is the key mediator that leads to the activation of the immune effector STAT1 by Janus kinases (JAK) 1 and 2. IFNγ-dependent genes, such as (C-X-C chemokine ligands) CXCL9 and CXCL10, are responsible for the recruitment of autoreactive CD8+ T cells, expressing the C-X-C chemokine receptor 3A (CXCR3A) [26]. In vivo studies using vitiligo mouse models also support the critical role of the IFNγ/CXCR3/CXCL10 signaling [27,28,29]. Analysis of the transcriptional profile of lesional vitiligo skin demonstrated an IFNγ-specific signature [28]. Independently of their roles in regulating the immune system, IFNγ and TNFα induce melanocyte detachment through the increase in keratinocyte-derived MMP9, the activation of JAK/STAT in melanocytes, E-cadherin cleavage, and consequent melanocytes detachment from the epidermal basal layer [30]. The process of melanocyte detachment unaccompanied to active inflammation has been also related to anomalous expression of the melanoma inhibitory activity (MIA) protein in achromic vitiligo patches since MIA perturbs the normal attachment of melanocytes to the basal membrane mediated by integrin α5β1 [31]. In vitro, persistent exposure to IFNγ stimulation reduces pigment production and induces viability loss and senescence in healthy melanocytes [32,33,34,35,36,37]. Conspicuous CD8+ and CD4+ T cells infiltrate, and their related cytokines have been found at the margins of active lesions [38]. However, a major role of CD8+ T cells in melanocyte loss has been demonstrated since CD8+ T cells were found more abundant in patients with active disease compared to patients with stable disease or healthy controls [39,40]. Further, the frequent melanogenic antigen-positive CD8+ T cells in the blood of vitiligo patients correlate with disease severity [41,42]. In addition, suppression of immune tolerance in vitiligo likely implies an altered proportion and/or function of effector and regulatory T cells (Tregs) [43]. In the skin of healthy subjects, Tregs represent about half of the CD4+ T cell population [44]. In vitiligo, a significantly lower percentage of Tregs is repeatedly measured in perilesional skin [45], which has been connected to reduced levels of Treg growth and differentiation factors TGFβ and IL10 [46]. The leading hypothesis is that in vitiligo, the organ-specific autoimmunity, anticipated by innate immunity activation, is caused by persistent endogenous cellular stress. Oxidative stress is retained one of the most crucial initiators of vitiligo [12,47]. Augmented reactive oxygen species (ROS) could be due to an abnormal intrinsic ROS generation or impairment of detoxifying apparatus, as well as extrinsic factors, such as sunburns, trauma, environmental pollutants, and phenolic compounds [47]. Additionally, the activity of the melanogenic biosynthetic pathways augments the risk of oxidative stress since melanin synthesis (particularly pheomelanin) involves oxidation reactions and superoxide anion (O2−) and hydrogen peroxide (H2O2) generation [48,49]. In vitiligo, oxidative stress is associated with the accumulation of immature/misfolded proteins in the endoplasmic reticulum, which lowers the rate of protein synthesis, strengths the autophagic recycling and other degradative pathways, and activates the unfolded protein response (UPR) [50,51,52]. As a consequence of increased intracellular oxidative stress and metabolic alterations, vitiligo melanocytes from apparently healthy skin display modification of intracellular signal transduction pathways referable to stress-induced premature senescence [52,53]. The acquisition of the senescent phenotype is characterized by the production of many proteins among the senescence-associated secretory phenotypes (IL6, matrix metalloproteinase 3 (MMP3), cyclooxygenase-2, insulin-like growth factor-binding protein 3 (IGFPB3 and 7) suggesting a possible premature degenerative process that culminates in melanocytes disappearance [53,54]. Melanocytes in patients with vitiligo have an overall greater vulnerability to oxidative damage and UV radiation compared to the normal controls [53,55,56]. Several studies documented high concentrations of H2O2 and peroxynitrite and reduced levels of the antioxidant enzymes catalase, glutathione reductase, thioredoxin/thioredoxin reductase, and methionine sulfoxide reductases in vitiligo skin [57,58,59]. Correspondingly, melanocytes isolated from nonlesional skin and cultured in vitro have lower levels of catalase, heme-oxygenase (HO-1), superoxide dismutase 2 (SOD2), and ubiquinone expression [53,60]. Further evidence for the primary role of oxidative stress in vitiligo arises from genetic studies [61]. Particularly, since in vitiligo there are abnormalities in the location and function of Nrf2 as well as polymorphisms of the corresponding gene that increase the risk of this disease, molecules targeting Nrf2 are currently under investigation [62,63]. The absence of melanocytes in depigmented areas impacts skin homeostasis, skin architecture, dermal neural responses, and photoadaptation [64,65,66,67]. Keratinocyte cell cultures from involved vitiligo skin have a lower proliferative potential than uninvolved skin [68] and increased apoptosis propensity [69]. However, the demonstration that most of the vitiligo-specific features are already present in normal-appearing skin [70] suggests that cells other than melanocytes, particularly for keratinocytes and fibroblasts [71,72,73,74,75], are involved in vitiligo pathogenesis. Nonlesional vitiligo keratinocytes demonstrated altered differentiation capacity that correlated to deregulated biosynthesis and metabolism of skin barrier lipids in normal-appearing skin [76]. Moreover, vitiligo keratinocytes share with vitiligo melanocytes impaired energy metabolism, culminating in lower production of ATP and compensatory overactivation of glycolysis-related enzymes [75,76]. Once stimulated by stressful events or inflammatory mediators, keratinocytes release CXCL9, CXCL10, and CXCL16, attracting cytotoxic CD8+ T cells [29,77,78]. Melanocyte function is also deeply influenced by the crosstalk with dermal cells [74,79,80]. A marked decline in fibroblast-derived growth factors sustaining melanocytes’ physiological activities may contribute to the occurrence of vitiligo disorder. In vitiligo lesions, the levels of bFGF, SCF, ET-1, GM-CSF, and α-melanocyte-stimulating hormone (α-MSH), released by keratinocytes and fibroblasts, are lower compared to healthy controls. At the same time, increased MC1R expression on melanocytes membrane in the nonlesional skin of vitiligo patients matching to controls may represent an attempt to restore normal pigmentation [81,82]. Furthermore, plasma levels of α-melanotropin are lower in vitiligo patients [83], confirming a functional impairment of the main promelanogenic pathways. Of interest, besides the function of regulating pigmentation, additional functions for α-MSH have been documented in the skin, including antagonist actions on inflammatory and fibrotic responses [84,85,86]. Thus, exogenous supplementation of MC1R agonist is a possible therapeutic strategy for vitiligo. Like vitiligo melanocytes, related nonlesional fibroblasts showed some senescent-associated features, including enlarged shape, higher expression of α-smooth muscle actin (α-SMA) and extracellular matrix proteins such as fibronectin and vimentin [74]. Dermal cells also contribute to immune system stimulation. IFNγ-responsive fibroblasts alone are sufficient for local recruitment of CD8+ T cells that target epidermal melanocytes. According to these data, this study proposed that the regional distribution of highly IFNγ-responsible fibroblasts may explain the pattern distribution of vitiligo disease [87]. Despite the numerous medical and UV-based therapies available for vitiligo, no treatment effectively promotes complete and durable repigmentation in all patients. Thus, recently, cellular, and acellular strategies in the field of regenerative medicine have received major attention. This review gives an overview of clinical and preclinical evidence for innovative regenerative interventions for vitiligo patients.
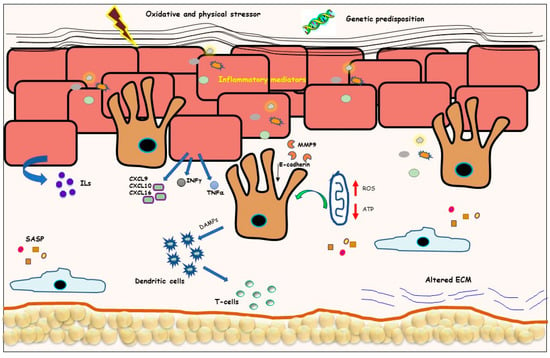
Figure 1.
Combined factors concurred with vitiligo pathogenesis. Graphic representation of the different alterations of vitiligo skin. Normal-appearing vitiligo skin is characterized by a thicker epidermis and a progressive loss of functional melanocyte rate. Oxidative stress in keratinocytes leads to the production of several inflammatory mediators. Intrinsic metabolic defects increase reactive oxygen species (ROS) production and decrease ATP content involving dermal and epidermal cells. In addition, vitiligo cells present reduced antioxidant ability and release senescence-associated proteins.
2. Therapeutic Approaches for Vitiligo Patients
Vitiligo treatments aim to provide good cosmetic outcomes, extend remission periods, prevent recurrences, and ensure patient satisfaction. Based on the described scenario, current medical strategies basically aim to offer antioxidant supplementation, immune system modulation, and melanocyte precursor mobilization. Recently, due to the progressive loss of functional melanocytes associated with failure to spontaneously recover pigmentation, it has been proposed to treat vitiligo as a degenerative disease [53,88]. Accordingly, along with pharmacological treatment, several cell-based and cell-free regenerative approaches have been proposed.
2.1. Medical Therapies
Commonly used repigmentation therapies for vitiligo include topical immunosuppressor agents (corticosteroids, calcineurin inhibitors, calcipotriol) and UV light (whole-body irradiation or UV targeted to lesions). Corticosteroids repress the cellular immune response and melanocyte destruction while stimulating melanocyte regeneration and melanogenesis [89]. Topical corticosteroids are the foremost treatment for localized vitiligo, while low-dose systemic corticosteroids are used for the stabilization of the rapidly progressive disease. Topical calcineurin inhibitors (tacrolimus and pimecrolimus) are preferred to corticosteroids for patients with involvement of the face or areas at high risk for skin atrophy [90]. Oral cyclosporine is employed as it can contract T cell activation due to inhibition of IL-2 production [91]. Targeting oxidative stress aims to modulate the integrated network inside the cells deputed to the ROS scavenger. Topical application of Pseudocatalase, a complex able to produce O2 and H2O from H2O2 at a rate higher than catalase, aims to recover the deficiency of catalase activity in vitiligo skin [57]. The efficacy of this treatment consists mostly in stopping disease progression. Regarding the possibility of inducing pigmentation recovery, however, no large clinical trials have been published. Systemic vitamin E was demonstrated to improve the NBUVB-induced pigmentation rate, reducing the UV dosage [92]. Vitiligo can be treated by different modalities of phototherapy. Phototherapy is used for treatment of extensive vitiligo involving more 20% of the skin surface for patients with refractory disease. UV acts both as an immunomodulator and as a stimulator of resident melanocytes precursors. Among noninvasive treatments used for vitiligo are phototherapy psoralen plus ultraviolet A (PUVA) and narrowband ultraviolet B (NBUVB). Multiple studies have proven the efficacy and safety of light therapy, such as 308 nm excimer laser and 308 nm excimer lamp, in localized, nonsegmental vitiligo [93]. Excimer therapy offers the advantage of focusing the irradiation on the affected lesions, thus reducing the total cumulative UV dose, and providing a higher penetration depth without the requirement of pharmaceutical photosensitization, as in the case of PUVA. However, the procedure is laborious and expensive. Phototherapy is frequently associated with medical and surgical treatments for enhanced and accelerated repigmentation. The synthetic analogue of α-MSH, Afamelanotide (also called Melanotan I), in association with phototherapy, demonstrated some positive effects due to its capacity to promote melanocyte proliferation and pigment production [94]. Enhancing the therapeutic effect of NBUVB, Afamelanotide reduces the cumulative UV dose required [95]. IFNγ-chemokine axis has been identified as a potential pathway in the initiation and progression of vitiligo [96]. IFNγ activates the JAKs/STAT pathway, increasing the expression of CXCR3 and its ligands CXCL9, CXCL10, and CXCL11, responsible for CD8+ T cell recruitment and apoptosis in melanocytes. Thus, the use of topical and systemic JAK inhibitors (tofacitinib, ruxolitinib, and baricitinib) is currently under intense clinical investigation (phase 2 and phase 3 trials) [97]. JAK/STAT inhibitors stimulate Hedgehog and Wnt signaling in epidermal pigmentation, both involved in the migration, proliferation, and differentiation of melanocytes [98]. Topical tofacitinib prevents the increase in the size of the patch and induces repigmentation when applied as a 2% topical solution twice daily, whereas approximately 50% repigmentation was seen in 45–50% of the subjects in a study investigating 1.5% topical ruxolitinib solution applied once and twice daily [99,100]. Even if both tofacitinib and ruxolitinib have shown better results in photo-exposed sites or associated with low-level NBUVB therapy [101,102], the impact of phototherapy associated with JAK inhibitors is still controversial.
2.2. Introduction to Interventional Therapies
From a general point of view in humans, the term “regeneration” is used to describe the replacement of specialized tissue by proliferation and differentiation of undamaged cells. However, in the skin and mucosa, normal replacement of individual cells is a continuous process, even in absence of specific stimuli. In the case of vitiligo, lack of repigmentation suggests that persistent stress-induced melanocyte damage may demand a permanent regenerative request leading to an abnormal turnover of melanocyte stem cells, resulting in the loss of regeneration ability. On the other hand, the lack of spontaneous skin color recovery may reflect the persistent loss of physiological skin homeostasis, suggesting that in white areas the entire microenvironment needs to be treated or reprogrammed to achieve normal pigmentation [103]. Repair is an adaptation to loss of tissue integrity and leads to production of scar tissue, sometimes without complete recovery of the normal structure and function. Thus, considering the endpoint, white skin, vitiligo lesions may be considered as a “scar following injury”, where injury is the autoimmune attack. Hence, for patients with stable disease pigmentation, recovery may take advantage of regenerative medicine tools. Further, the demonstration that vitiligo is a disease not restricted to melanocytes motivates the development of therapies that can regenerate the whole organ (including dermis, hypodermis, and annexes) and decrease reliance on transplantations. One of the challenges is to establish how to target the disease-specific microenvironment and how to improve cell graft persistence since a hostile microenvironment could also be improper for cell engraftment. The biological bases for regenerative therapeutic approaches are mostly two: enhancement of the tissue-intrinsic regenerative capacity of the receiving tissue and cell replacement by grafting. Correspondingly, repigmentation of vitiligo requires an increase in the number and migration of melanocytes to the depigmented epidermis. This could be realized by stimulating resident melanocyte precursors or by autologous melanocyte transplantation. However, the intrinsic defect may limit the use of autologous melanocytes and precursor cells in vitiligo due to the high vulnerability to stressful conditions and consequent reduced ability of regeneration [104].
3. Grafting Procedures (Skin-to-Skin Graft)
Surgical therapeutic modalities are effective interventions for patients with stable vitiligo who have experienced failure of medical treatment. Surgical procedures aim to replace the melanocytes with ones from a normally pigmented autologous donor skin. The first graft technique used was the transplantation of an epidermal sheet into the vitiliginous patch [105,106]. Then, grafting for vitiligo evolved in more sophisticated techniques, sometimes supported by laboratory-assisted in vitro culture. However, culturing epidermal cells is a delicate process due to the delicacy of keratinocytes and melanocytes. Surgical modalities are weakly recommended interventions due to their invasiveness and the high requirements in terms of laboratory equipment and professional expertise. A prerequisite for successful repigmentation is the accurate selection of patients. In principle, however, it is indicated for all stable forms (disease inactivity ranging from 6 months to 4 years is recommended) of segmental and focal vitiligo [107] in absence of Koebner phenomenon history and keloidal tendency if conventional therapies demonstrated unsuccessful [108]. Grafting techniques are usually combined with other medical treatment modalities, including phototherapy (PUVA or PUVAsol therapy) [109,110], narrowband UVB (NBUVB) [111], topical immunosuppressors [112], and even excimer laser treatment [113] to enhance repigmentation. Surgical transplantation modalities for vitiligo patients are classified according to the nature of the grafted material (punch graft, split-thickness skin grafts, smashed skin grafting, blister graft) and cellular grafts (cultured and noncultured cells) (Figure 2).
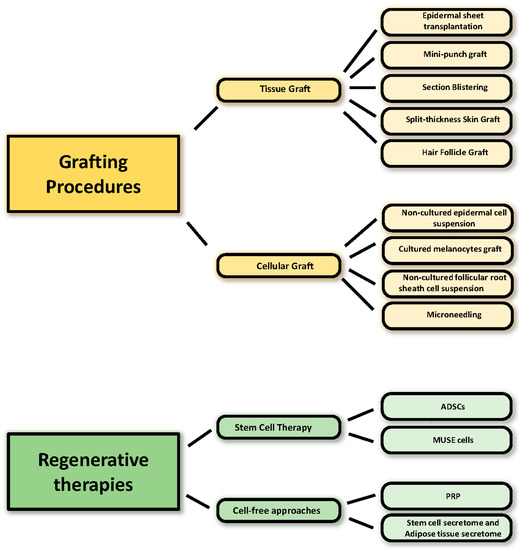
Figure 2.
Schematic summary of current procedures in vitiligo treatment.
3.1. Tissue Graft
3.1.1. Epidermal Sheet Transplantation
Intraoperative epidermal sheet transplantation represents the first surgical method to treat vitiliginous patches [105,106]. Based on the clinical experience of epidermal cell cultures for burns and chronic nonhealing wound purposes, layered sheets have been also used for vitiligo patients obtaining good repigmentation and satisfying color matching with the surrounding skin [114,115]. The disadvantage of this method resides in the cost and the requirement of highly qualified labor that limit layered sheet usage.
3.1.2. Minipunch Graft
A punch graft is one of the most used techniques since it is economical and easy to perform even with minimal equipment. Epidermal–dermal punches of 1–2 mm sizes are collected from a donor uninvolved skin to be immediately transplanted into the depigmented area. The efficacy of repigmentation is assessed at 90% [116]. The anatomic site selected for harvesting the punch deeply influences the clinical results [117,118]. Adverse effects include hypertrophic scarring, halo or complete depigmentation of the graft, and poor cosmetic outcome due to color mismatch between donor and recipient skin. To test the individual treatment outcome and the effective disease stability, the transplantation of a few minigrafts onto the recipient area before the main surgical procedure has been proposed [115]. The last stage of treatment includes phototherapy, which promotes repigmentation [119]. Kato and co-authors reported a significantly greater area of repigmentation in patients with segmental vitiligo compared to the generalized form [117]. Abdallah et al. reported the number of cytotoxic T lymphocytes and lymphocyte function-associated antigen-1 (LFA-1)-positive cells as a marker of poor outcome, indicating the autoimmune reaction against grafted melanocytes as major problem impacting procedure outcome [120]. Immunohistochemical analysis of biopsies collected in repigmented skin of vitiligo patients at different time points after punch graft showed that melanocytes move easily from the edges of the grafted skin toward the depigmented areas in the case of smaller punches [121]. Thus, the use of large punches is not recommended.
3.1.3. Suction Blistering
Suction blister epidermal grafting is used to obtain very thin skin grafts by causing a split at the dermo–epidermal junction. This technique creates a subepidermal bulla at the donor site from which the roof is surgically removed and transplanted onto the recipient site. Generally, inducing the bulla is usually obtained by applying a cup or syringe under constant pressure. The blistering process persists from 30 min to 3 h, and it is followed by the surgical removal of the subepidermal bulla, which is grafted in the recipient area. One or two days before the transplantation, the recipient area is prepared using liquid nitrogen freezing, ablative lasers dermabrasion, or suction blisters [122]. This method is simple and safe and can be successfully used around the sensitive area of the mouth and eyelids [123]. The typical complications are temporary hyperpigmentation or color mismatching. To accelerate repigmentation, complementary postoperative NBUVB or PUVA phototherapy can be applied [109].
3.1.4. Split-Thickness Skin Graft
Similarly to other surgical techniques, in split-thickness skin grafts, the site of the graft collection is most often the area of the thighs, buttocks, back, arms, or forearms [124]. Basing on the thickness of the tissue collected for transplantation, we can distinguish thin (0.15–0.3 mm), intermediate (0.3–0.45 mm), and thick (0.45–0.75 mm) grafts. Ultrathin grafts (0.08–0.15 mm) are also used with satisfying results since less hypopigmentation of the donor site has been observed after healing is complete [124]. Ultrathin skin grafting is not definitively retained by the recipient site, probably due to the complete absence of dermal tissue [125], and usually falls off after 2 weeks, leaving uniform repigmentation. It was reported that the use of thinner skin flaps, compared to thicker grafts, was associated with fewer side effects [126]. Also in this case, the recipient site is prepared by using a dermabrader, ablation laser, or cryotherapy, separating the epidermis from the dermis [127]. Despite the fact that the technique concurs to the treatment of a relatively extended region of hypopigmentation rapidly, a split-thickness skin graft has some disadvantages, as well as an insufficient color and texture correspondence between the treated and donor area: disturbance of sensation within the recipient area could develop displacement of the grafts, milia formation, perigraft depigmentation, and imperfect scarring at recipient or donor areas [128,129].
3.1.5. Hair Follicle Graft
Skin precursor of the melanocyte lineage are localized in the hair bulge as well as in the epidermis to pigment the hair and skin, respectively [130,131,132]. However, since clinical observation and experimental data concluded that repigmentation of vitiligo skin occurs primarily from hair follicle melanocytes, either spontaneously or after UV therapy and punch grafting [133,134,135], hair follicle grafting has received greater attention. Moreover, in vitiligo patients, repigmentation develops best in the areas with a higher density of hair follicles (face, arms, forearms, legs, back, and abdomen) compared to depigmented areas where hair follicles are absent or in low density (palms, soles, genital sites, and mucosal) [136,137]. Follicular melanocyte stem cells are maintained in an immune-privileged location far from the skin surface [130], suggesting that are naturally less prone to premature exhaustion. To obtain hair follicles for transplantation, small rectangular or punch fragments of skin should be collected, usually from the scalp. Then the follicles are separated and finally transplanted into previously formed wells, located at regular intervals of 3–5 mm in the affected area [138]. Adjuvant treatment with calcineurin inhibitors, corticosteroids, or photochemotherapy with psoralen and natural sun exposure are frequently employed as adjuvant treatments.
3.2. Cellular Graft
Unlike tissue grafting, cellular grafting permits treatment of a depigmented skin area significantly larger than the harvesting area. Particularly, in the case of in vitro expansion, the material can be expanded and long-term cryopreserved to facilitate future grafts.
3.2.1. Noncultured Epidermal Cells Suspension
This technique was firstly proposed by Gauthier and Surleve-Bazeille in 1992 [139]. While several different modifications of the original method have been proposed, the procedure consists of taking a small fragment of normally pigmented skin, usually from the occipital area. Then the harvested skin obtained from the donor site is enzymatically digested to separate the epidermis from the dermis, obtaining a melanocytes and keratinocytes mixed-cell suspension ready to be inoculated into the recipient area [140]. Since growth factors released by keratinocytes deeply influence melanocyte growth, it is preferred not to separate the two cell lines. At the same time, the advantage is to limit graft material manipulation. In noncultured cellular transplantation protocols, melanocytes and keratinocytes are transplanted on the same day (hot trypsinization) or the next day (cold trypsinization). A study published by Li and collaborators evidenced the beneficial effect of repeated long-term trypsinization on the proliferation, differentiation capacity, and purity of melanocyte colonies that could be used for clinical application in patients with vitiligo [141]. Recently, the use of a single-enzyme solution (trypsin, collagenase, or dispase) has been replaced by an increased number of commercially available kits that offer more standardized reagents and protocols requiring less operative expertise [142]. The main advantage of a noncultured epidermal cell suspension graft consists of the possibility to treat a large area using a small sized portion of donor skin (1:10 donor–recipient size ratio) [143]. In fact, the repigmentation outcome is like that of tissue grafts, even if starting with a smaller donor area [144]. Long-term studies on patients with vitiligo receiving grafts of noncultivated epidermal cells showed stable repigmentation in 93% of cases after an average of four years [145]. Similarly, another study demonstrated stable repigmentation five years after autologous noncultivated cells grafting in all patients (12/12) with segmental vitiligo, although in some cases, retransplantation was performed [143]. However, the process itself is more forceful among younger patients [146]. Among the complications occurring with this method were reported incomplete color matching as well as scarring and a modification in the skin texture. Some authors also observed undesired hypopigmentation on the donor site [142,145].
3.2.2. Cultured Melanocytes Graft
The improvement of the epidermal cells graft has made it possible to culture melanocytes in a melanocyte-specific defined medium enriched with various factors. After extracting single cells from skin fragments, melanocytes cultured for 3–4 weeks are transplanted into the recipient’s skin. The procedure requires the support of specialized laboratory equipment and staff with a consequent increase in the overall cost of the treatments. The culture medium contains chemical mitogen and growth factors [147,148]. However, some components contained in the culture medium may exert a promutagenic effect [149]. To avoid excessive use of chemicals, the use of keratinocytes and of a mesenchymal stem cells feeder layer has been proposed [149]. Even if both cell types increase melanocytes proliferation and migration, mesenchymal stem is preferred due to a lesser differentiation propensity of melanocytes before grafting [150]. Studies comparing cultured and noncultured melanocyte graft techniques are not conclusive since using different temporal end points, inferior cosmetic results [151], and better [152] repigmentation have been reported.
3.2.3. Noncultured Follicular Root Sheath Cells Suspension
Another technique that allows us to obtain melanocytes, melanocytes, and keratinocytes precursors and hair follicle stem cells is based on the enzymatic extraction from skin follicle units [153]. The preparation of material for grafting single-cell suspension in the follicular cell suspension method involves repeated cycles of trypsinization–neutralization [154]. Excellent repigmentation with noncultured follicular root sheath suspension has been documented by several studies [154,155,156]. Comparative trials did not evidence differences in terms of cosmetic results between noncultured follicular root sheath and epidermal noncultured cell suspension techniques [157,158]. In particular, the suspension includes not only pigment cells but also melanocyte stem cells, keratinocyte stem cells, and hair follicle stem cells [159]. For better results, is indicated to collect hair in the anagen phase from the occipital area of the scalp, preserving the hair follicles’ integrity. The site to be treated is usually prepared using a dermabrader and, as a final step, is covered with collagen [154]. Given the possibility of achieving very good clinical results, including color match and the absence of scarring, this treatment’s results are attractive [154], although it requires both high laboratory and high manual skills [156]. The amount of 15–25 follicular units (about 300,000 to two million cells) in the form of a suspension is considered adequate to treat about 20 cm2 of achromic skin [155].
3.2.4. Microneedling
The microneedling technique uses very thin needles to create microinjuries on the skin, inducing reparative/regenerative processes similar to a wound healing response with concomitant production of cytokines and mitogenic factor, including propigmentary factors [160]. It is mostly used for skin rejuvenation [160]. Further, microneedling procedures facilitate drug penetration through the stratum corneum [161]. Two different studies reported effective repigmentation using microneedling in combination with 5-fluorouracil [162,163]. However, in another study microneedling in combination with NBUVB phototherapy, tacrolimus, and topical latanoprost failed to confirm therapeutical advantage [164]. Microchannels created by microneedling are for delivering cells in the grafting procedure, enhancing their survival and persistence [165,166].
4. Regenerative Therapies Based on Nonmelanocytic Cells
The field of regenerative medicine encompasses numerous strategies to overcome physiological as well as pathological limited regenerative capacity in adult humans. The biological basis for regenerative therapeutic approaches is to enhance the intrinsic regenerative capacity of pathologic tissue or to replace damaged/missing cells by immature committed cells or a pluripotent stem precursor cells graft.
4.1. Mesenchymal Stem Cell-Based Therapy
4.1.1. ADSCs
Adult mesenchymal stem cell-based therapy demonstrated effectiveness in some clinical indications for both autologous and allogeneic purposes, thus becoming one of the most promising therapies in the regenerative medicine field, including the dermatologic one [167,168,169,170]. Blood, bone marrow, and adipose tissue represent important stem cell resources for cell-based therapies [171]. Because of their accessibility, high cell number availability, and noninvasive collection, adipose-derived stem cells (ADSCs) recently received major attention from researchers and clinicians. In addition, ADSCs are more resistant to stress-induced senescence than bone marrow-derived stem cells [172]. Their multipotent differentiation potential toward various cell lineages [173,174,175,176] makes these cells very useful in treating different pathological conditions. In vitro, in the presence of trophic factors promoting melanocytic differentiation, ADSCs progressively acquire a bipolar shape or a more dendritic morphology, like fully differentiated skin melanocytes, and express major proteins involved in pigmentation (Microftalmia transcription factor, Mitf, Tyrosinase, tyrosinase-related protein 1, Trp1 and tyrosinase-related protein 2, Trp2) [176,177]. Nevertheless, it is well documented that the therapeutic potential of the adipose tissue (and associated mesenchymal stem cells) is largely ascribable to a multitude of bioactive factors released by adipocytes and associated stromal cells that combines mitogenic and antiapoptotic factors, cytokines, chemokines, and extracellular matrix components [178,179]. Hence, the secretome’s ability to modulate multiple targets simultaneously demonstrated preclinical and clinical competence in reversing pathological mechanisms of complex diseases such as vitiligo [88,180]. Thus, the management of vitiligo might benefit from several properties of ADSC including immune system modulation and antioxidant capacity. Mesenchymal stem cells suppress T cell proliferation mediated by IFNγ/STAT1 signaling [181]. Grafting procedures for vitiligo might benefit from the modulation of the immune response exerted by ADSCs since the persistence of cytotoxic T cells is retained as the prime cause of disease maintenance [6,182]. ADSC-based immunomodulation also includes the production of anti-inflammatory IL10 and the induction of regulatory T cells (Tregs) [183,184]. Furthermore, since the reduced release and function of growth factors/receptor signaling contributes to melanocyte loss in vitiligo skin, the ADSC-derived growth factors could compensate for the well-described impaired dermal-epidermal paracrine activity [180]. Kim et al. demonstrated that in vitro cocultures with ADSCs increase melanocyte proliferation and migration due to the secretion of bFGF and melanocyte growth factor (MGF) [150]. In addition to the possibility to use ADSCs as a feeder layer to prepare cultured melanocytes for autologous grafting, in an animal model, the use of a mix of ADSC–melanocyte prepared immediately before its clinical usage improved pigmentation efficiency compared to the grafting of melanocytes alone [185]. ADSCs possess ROS-scavenging properties due to the capacity to increase the expression and activity of SODs, GPx, catalase, and HO-1 in target cells [88,174,186]. Considering chronic oxidative stress as a key player involved in vitiligo pathogenesis, this ADSC peculiarity could represent a strategy to overcome the detrimental effect of ROS. Thus, targeting a locally compromised microenvironment with adipose tissue secretome might be used as a complementary agent to enhance transplantation efficacy in patients undergoing an autologous melanocyte graft.
4.1.2. MUSE Cells
Alternative stem cells that may be suitable for treating vitiligo are multilineage-differentiating stress-enduring (MUSE) cells [187]. They can be isolated from human dermis and adipose tissue using the embryonic antigen-3 marker selectively expressed by undifferentiated human embryonic stem cells [188]. MUSE cells are normally preserved in a quiescent state but can be specifically activated by stressful inputs both in vivo and in vitro [187]. MUSE cells can self-renew and regenerate cells from all three germ layers while being nontumorigenic. Thus, MUSE cells appear to be a strategic tool for skin regenerative purpose due to their successful differentiation into keratinocytes, fibroblasts, and melanocytes in vitro [189]. Ex vivo studies have identified factors that induce MUSE cells to differentiate into fully differentiated melanin-producing melanocytes [190] that, when incorporated into three-dimensional skin culture models, correctly localize at the basal layers of the epidermis [187,188]. Of interest, a recent study demonstrated the existence of melanocyte precursor cells residing in human subcutaneous adipose tissue and the possibility to differentiate these cells into mature, fully differentiated melanocytes [191].
4.2. Cell-Free Approaches
4.2.1. PRP
Platelet-rich plasma (PRP) is a biological product, a portion of a plasma with a platelet concentration above the baseline containing a great source of cytokines, growth factors, and other biologically active substances with a regenerative potential [192]. Autologous PRP, originally designed for wound healing and dermatological cosmetic problems, has recently received considerable attention for application for several other diseases, especially in the dermatological field [167,168,193,194]. Side effects of PRP therapy are few, consisting of irritation, pain at the recipient site, infections, and blood clots [192]. Once activated platelets release from their α granules, growth factors with a capital role in tissue hemostasis and repair such as CTGF (conjunctive tissue growing factor), EGF (epidermal growing factor), FGF2 (fibroblast growing factor), FGF9, IGF-1 (insulin growing factor), PDGF-αα (platelet-derived growing factor), PDGF αβ, PDGF ββ, TGFα (transforming growing factor), TGFβ1, TGFβ2, and VEGF (vascular endothelial growing factor). However, PRP preparation may as well include undesired factors. For example, contamination with erythrocytes when collecting PRP produces unwanted inflammatory reactions at the recipient site since they contain a high amount of ROS [195]. The usage of PRP treatment in vitiligo is motivated by the concentration of growth factors considered key players in melanocyte biology such as bFGF, SCF, and TGFβ (Parambath); by the broad immune system modulatory effect; and by the peculiar presence of extracellular matrix component fibrin, fibronectin, and vitronectin that serve to achieve cell adhesion between epidermal and dermal cells [196]. Notably, PRP could stimulate stem cells reservoir [197]. A report by Mahajan and colleagues presented that treatment with intralesional PRP injections, consisting of six injections at two-week intervals, is effective for chronic localized vitiligo patients who did not respond to traditional therapies. Kadry et al., collecting clinical and histopathological data, demonstrated that PRP and PRP combined with combined fractional CO2 laser induced significant repigmentation of vitiliginous lesions except for some resistant lesions on the hands and feet [198]. The efficacy of PRP-based combination therapies has been further confirmed using PRP plus NBUVB [199]. The combined therapies achieved the best results [200]. Similarly, PRP ameliorated the outcome of autologous graft of noncultured epidermal cell suspension [201]. However, no standard protocols regarding PRP preparation exist, making it difficult to compare results from different clinical studies. Recently, a meta-analysis considered six similar studies comparing PRP plus 308 nm excimer laser therapy to 308 nm excimer l therapy alone. Authors concluded that combination therapy offers a significant benefit in terms of repigmentation and recurrence rates compared to monotherapy [202].
4.2.2. Stem Cell Secretome and Extracellular Portion of Lipoaspirate
Acellular therapeutics in regenerative medicine are becoming more attractive, especially for nonvolumizing purposes, such as most dermatological conditions. Stem cell secretomes containing a multitude of bioactive peptides possess similar protective and reparative properties as their cellular counterparts [203]. Because of the high concentration of growth factors, the extracellular components of whole adipose tissue (lipoaspirate) could be used as an innovative cell-free therapy [88]. The usage of extracellular elements of adipose tissue aims to stimulate a self-autonomous, regenerative microenvironment in the treated area. However, omitting stem cell counterparts for regenerative purposes implies that dermal and epidermal cells might be locally present, and this is not the case with missing melanocytes in vitiligo-involved skin. In in vitro vitiligo melanocytes extracted from normal-appearing, skin is fully competent for mitogenic stimulation by growth factors contained in adipose tissue secretome [180]. Further investigations are necessary to verify the efficacy of the melanocyte stem cell reservoir. High levels of Wnt agonist in acellular fraction of fat tissue are also promising for vitiligo management since a pivotal role of Wnt/β-catenin signaling has been attributed to NBUVB-induced repigmentation of vitiligo skin [135]. Moreover, Ragazzetti et al., obtained repigmentation of vitiligo skin in an ex vivo model by treating with WNT agonists or GSK3β inhibitors that activate resident melanocyte stem cells [204]. An alternative possibility for vitiligo patients is to employ stem cell secretome as adjuvant therapy in transplantation treatments and pre- and postoperative care of the recipient site. The role of tissue microenvironment in graft retention is particularly important for a multifactorial complex disease such as vitiligo. Several beneficial features of stem cell secretome might be desirable for vitiligo patients, including mitogenic and prosurvival molecules [88]. Moreover, the extracellular liquid extracted by lipoaspirate has a moderate direct scavenger capacity, whereas activates intrinsic cell defense mechanisms up-modulating antioxidant genes. Additionally, under continuous exposure of dermal and epidermal cells to adipose tissue secretome, intracellular ROS decreases, and mitochondria appear more energized [88], suggesting the possible restoration of normal metabolic functions in vitiligo skin. This suggests a feasible strategy to exceed the detrimental effect of ROS released during surgical treatments, which may cause death and dysfunction in melanocytes, once again leading to depigmentation. In line of principle, adipose tissue secretome represents the autologous correspondent to the melagenine (concentrated extract of human placenta) previously studied in proof-of-concept studies on vitiligo patients [205,206]. In addition to melanocytes, several studies proved significant biochemical alterations and increased production of ROS in other skin cell types, particularly keratinocytes and fibroblasts [74,180]. This suggests that cell defects common to different elements of the epidermal and dermal compartments are involved in loss of melanocytes and chronic depigmentation. Consequently, the association of cell grafts to treatments capable of counteracting dysfunctions of the whole skin may be promising to treat vitiligo.
5. Conclusions
The treatment of vitiligo is one of the most difficult dermatological challenges. Ideally, vitiligo treatments aim to stop the immune destruction of melanocytes, to stimulate repigmentation, and prevent recurrences, providing good cosmetic outcomes. Regenerative medicine offers new therapeutic opportunity intrinsically related to its reparative character. However, we cannot exclude that in vitiligo, like in other degenerative and metabolic diseases, a therapeutic success limitation could reside in the use of autologous cells presenting crucial pathogenic features and consequent minor regenerative capacity compared to healthy cells. Successful repigmentation of vitiligo skin may be achieved by three different routes: First, melanocytes, melanocyte precursors, or pluripotent stem cells graft; second, melanocyte precursor mobilization; thirdly, creating a pro-regeneration environment. For all these mechanisms, targeting the entire microenvironment seems to be a requisite. Particularly, the association of surgical techniques with protective biological factors such as those contained in PRP or adipose tissue secretome may overcome oxidative disequilibrium and immunological rejection of grafted material.
Author Contributions
B.B. and F.P. performed the literature research and wrote the manuscript. M.P. supervised the work and revised the paper. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Picardo, M.; Dell’Anna, M.L.; Ezzedine, K.; Hamzavi, I.; Harris, J.E.; Parsad, D.; Taieb, A. Vitiligo. Nat. Rev. Dis. Primers 2015, 1, 15011. [Google Scholar] [CrossRef] [PubMed]
- Bergqvist, C.; Ezzedine, K. Vitiligo: A Review. Dermatology 2020, 236, 571–592. [Google Scholar] [PubMed]
- Krüger, C.; Schallreuter, K.U. A review of the worldwide prevalence of vitiligo in children/adolescents and adults. Int. J. Dermatol. 2012, 51, 1206–1212. [Google Scholar] [CrossRef] [PubMed]
- Matin, R. Vitiligo in adults and children. BMJ Clin. Evid. 2011, 2011, 1717. [Google Scholar] [PubMed]
- Wang, G.; Qiu, D.; Yang, H.; Liu, W. The prevalence and odds of depression in patients with vitiligo: A meta-analysis. J. Eur. Acad. Dermatol. Venereol. 2018, 32, 1343–1351. [Google Scholar] [CrossRef]
- Boniface, K.; Seneschal, J.; Picardo, M.; Taïeb, A. Vitiligo: Focus on Clinical Aspects, Immunopathogenesis, and Therapy. Clin. Rev. Allergy Immunol. 2018, 54, 52–67. [Google Scholar]
- Ezzedine, K.; Lim, H.W.; Suzuki, T.; Katayama, I.; Hamzavi, I.; Lan, C.C.; Goh, B.K.; Anbar, T.; Silva de Castro, C.; Lee, A.Y.; et al. Vitiligo Global Issue Consensus Conference Panelists Revised classification/nomenclature of vitiligo and related issues: The Vitiligo Global Issues Consensus Conference. Pigment Cell Melanoma Res. 2012, 25, E1–E13. [Google Scholar] [CrossRef]
- Speeckaert, R.; van Geel, N. Vitiligo: An Update on Pathophysiology and Treatment Options. Am. J. Clin. Dermatol. 2017, 18, 733–744. [Google Scholar] [CrossRef]
- Prignano, F.; D’Erme, A.M.; Bonciolini, V.; Lotti, T. Mucosal psoriasis: A new insight toward a systemic inflammatory disease. Int. J. Dermatol. 2011, 50, 1579–1581. [Google Scholar] [CrossRef]
- Anbar, T.S.; Hegazy, R.A.; Picardo, M.; Taieb, A. Beyond vitiligo guidelines: Combined stratified/personalized approaches for the vitiligo patient. Exp. Dermatol. 2014, 23, 219–223. [Google Scholar] [CrossRef]
- Seneschal, J.; Boniface, K.; D’Arino, A.; Picardo, M. An update on Vitiligo pathogenesis. Pigment Cell Melanoma Res. 2021, 34, 236–243. [Google Scholar] [CrossRef] [PubMed]
- Abdel-Malek, Z.A.; Jordan, C.; Ho, T.; Upadhyay, P.R.; Fleischer, A.; Hamzavi, I. The enigma and challenges of vitiligo pathophysiology and treatment. Pigment Cell Melanoma Res. 2020, 33, 778–787. [Google Scholar] [CrossRef] [PubMed]
- van den Boorn, J.G.; Picavet, D.I.; van Swieten, P.F.; van Veen, H.A.; Konijnenberg, D.; van Veelen, P.A.; van Capel, T.; Jong, E.C.; Reits, E.A.; Drijfhout, J.W.; et al. Skin-depigmenting agent monobenzone induces potent T-cell autoimmunity toward pigmented cells by tyrosinase haptenation and melanosome autophagy. J. Investig. Dermatol. 2011, 131, 1240–1251. [Google Scholar] [CrossRef]
- Kroll, T.M.; Bommiasamy, H.; Boissy, R.E.; Hernandez, C.; Nickoloff, B.J.; Mestril, R.; Caroline Le Poole, I. 4-Tertiary butyl phenol exposure sensitizes human melanocytes to dendritic cell-mediated killing: Relevance to vitiligo. J. Investig. Dermatol. 2005, 124, 798–806. [Google Scholar] [CrossRef]
- Wang, J.; Pan, Y.; Wei, G.; Mao, H.; Liu, R.; He, Y. Damage-associated molecular patterns in vitiligo: Igniter fuse from oxidative stress to melanocyte loss. Redox Rep. 2022, 27, 193–199. [Google Scholar] [CrossRef] [PubMed]
- Gasque, P.; Jaffar-Bandjee, M.C. The immunology and inflammatory responses of human melanocytes in infectious diseases. J. Infect. 2015, 71, 413–421. [Google Scholar]
- Yu, N.; Zhang, S.; Zuo, F.; Kang, K.; Guan, M.; Xiang, L. Cultured human melanocytes express functional toll-like receptors 2–4, 7 and 9. J. Dermatol. Sci. 2009, 56, 113–120. [Google Scholar] [CrossRef]
- Jin, S.H.; Kang, H.Y. Activation of Toll-like Receptors 1, 2, 4, 5, and 7 on Human Melanocytes Modulate Pigmentation. Ann. Dermatol. 2010, 22, 486–489. [Google Scholar] [CrossRef]
- Faraj, S.; Kemp, E.H.; Gawkrodger, D.J. Patho-immunological mechanisms of vitiligo: The role of the innate and adaptive immunities and environmental stress factors. Clin. Exp. Immunol. 2022, 207, 27–43. [Google Scholar]
- Zhou, R.; Tardivel, A.; Thorens, B.; Choi, I.; Tschopp, J. Thioredoxin-interacting protein links oxidative stress to inflammasome activation. Nat. Immunol. 2010, 11, 136–140. [Google Scholar] [CrossRef]
- Zhou, R.; Yazdi, A.S.; Menu, P.; Tschopp, J. A role for mitochondria in NLRP3 inflammasome activation. Nature 2011, 469, 221–225. [Google Scholar] [CrossRef]
- Rathinam, V.A.; Vanaja, S.K.; Fitzgerald, K.A. Regulation of inflammasome signaling. Nat. Immunol. 2012, 13, 333–342. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Kang, P.; Zhang, W.; Jian, Z.; Zhang, Q.; Yi, X.; Guo, S.; Guo, W.; Shi, Q.; Li, B.; et al. Activated NLR family pyrin domain containing 3 (NLRP3) inflammasome in keratinocytes promotes cutaneous T-cell response in patients with vitiligo. J. Allergy Clin. Immunol. 2020, 145, 632–645. [Google Scholar] [CrossRef] [PubMed]
- Yu, R.; Broady, R.; Huang, Y.; Wang, Y.; Yu, J.; Gao, M.; Levings, M.; Wei, S.; Zhang, S.; Xu, A.; et al. Transcriptome analysis reveals markers of aberrantly activated innate immunity in vitiligo lesional and non-lesional skin. PLoS ONE 2012, 7, e51040. [Google Scholar] [CrossRef] [PubMed]
- Hlača, N.; Žagar, T.; Kaštelan, M.; Brajac, I.; Prpić-Massari, L. Current Concepts of Vitiligo Immunopathogenesis. Biomedicines 2022, 10, 1639. [Google Scholar] [CrossRef]
- Howell, M.D.; Kuo, F.I.; Smith, P.A. Targeting the Janus Kinase Family in Autoimmune Skin Diseases. Front. Immunol. 2019, 10, 2342. [Google Scholar] [CrossRef]
- Harris, J.E.; Harris, T.H.; Weninger, W.; Wherry, E.J.; Hunter, C.A.; Turka, L.A. A mouse model of vitiligo with focused epidermal depigmentation requires IFN-γ for autoreactive CD8+ T-cell accumulation in the skin. J. Investig. Dermatol. 2012, 132, 1869–1876. [Google Scholar] [CrossRef]
- Rashighi, M.; Agarwal, P.; Richmond, J.M.; Harris, T.H.; Dresser, K.; Su, M.W.; Zhou, Y.; Deng, A.; Hunter, C.A.; Luster, A.D.; et al. CXCL10 is critical for the progression and maintenance of depigmentation in a mouse model of vitiligo. Sci. Transl. Med. 2014, 6, 223ra23. [Google Scholar] [CrossRef]
- Richmond, J.M.; Masterjohn, E.; Chu, R.; Tedstone, J.; Youd, M.E.; Harris, J.E. CXCR3 Depleting Antibodies Prevent and Reverse Vitiligo in Mice. J. Investig. Dermatol. 2017, 137, 982–985. [Google Scholar] [CrossRef]
- Boukhedouni, N.; Martins, C.; Darrigade, A.S.; Drullion, C.; Rambert, J.; Barrault, C.; Garnier, J.; Jacquemin, C.; Thiolat, D.; Lucchese, F.; et al. Type-1 cytokines regulate MMP-9 production and E-cadherin disruption to promote melanocyte loss in vitiligo. JCI Insight 2020, 5, e133772. [Google Scholar] [CrossRef]
- Bordignon, M.; Castellani, C.; Fedrigo, M.; Thiene, G.; Peserico, A.; Alaibac, M.; Angelini, A. Role of alpha5beta1 integrin and MIA (melanoma inhibitory activity) in the pathogenesis of vitiligo. J. Dermatol. Sci. 2013, 71, 142–145. [Google Scholar] [CrossRef]
- Wang, S.; Zhou, M.; Lin, F.; Liu, D.; Hong, W.; Lu, L.; Zhu, Y.; Xu, A. Interferon-γ induces senescence in normal human melanocytes. PLoS ONE 2014, 9, e93232. [Google Scholar] [CrossRef] [PubMed]
- Krasagakis, K.; Garbe, C.; Krüger, S.; Orfanos, C.E. Effects of interferons on cultured human melanocytes in vitro: Interferon-beta but not-alpha or -gamma inhibit proliferation and all interferons significantly modulate the cell phenotype. J. Investig. Dermatol. 1991, 97, 364–372. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Richmond, J.M.; Frisoli, M.L.; Harris, J.E. Innate immune mechanisms in vitiligo: Danger from within. Curr. Opin. Immunol. 2013, 25, 676–682. [Google Scholar] [CrossRef] [PubMed]
- Singh, M.; Mansuri, M.S.; Kadam, A.; Palit, S.P.; Dwivedi, M.; Laddha, N.C.; Begum, R. Tumor Necrosis Factor-alpha affects melanocyte survival and melanin synthesis via multiple pathways in vitiligo. Cytokine 2021, 140, 155432. [Google Scholar] [CrossRef]
- Englaro, W.; Bahadoran, P.; Bertolotto, C.; Buscà, R.; Dérijard, B.; Livolsi, A.; Peyron, J.F.; Ortonne, J.P.; Ballotti, R. Tumor necrosis factor alpha-mediated inhibition of melanogenesis is dependent on nuclear factor kappa B activation. Oncogene 1999, 18, 1553–1559. [Google Scholar] [CrossRef]
- Natarajan, V.T.; Ganju, P.; Singh, A.; Vijayan, V.; Kirty, K.; Yadav, S.; Puntambekar, S.; Bajaj, S.; Dani, P.P.; Kar, H.K.; et al. IFN-γ signaling maintains skin pigmentation homeostasis through regulation of melanosome maturation. Proc. Natl. Acad. Sci. USA 2014, 111, 2301–2306. [Google Scholar] [CrossRef]
- Badri, A.M.; Todd, P.M.; Garioch, J.J.; Gudgeon, J.E.; Stewart, D.G.; Goudie, R.B. An immunohistological study of cutaneous lymphocytes in vitiligo. J. Pathol. 1993, 170, 149–155. [Google Scholar] [CrossRef]
- Sandoval-Cruz, M.; García-Carrasco, M.; Sánchez-Porras, R.; Mendoza-Pinto, C.; Jiménez-Hernández, M.; Munguía-Realpozo, P.; Ruiz-Argüelles, A. Immunopathogenesis of vitiligo. Autoimmun. Rev. 2011, 10, 762–765. [Google Scholar] [CrossRef]
- Le Poole, I.C.; Wañkowicz-Kaliñska, A.; van den Wijngaard, R.M.; Nickoloff, B.J.; Das, P.K. Autoimmune aspects of depigmentation in vitiligo. J. Investig. Dermatol. Symp. Proc. 2004, 9, 68–72. [Google Scholar] [CrossRef]
- Ogg, G.S.; Rod Dunbar, P.; Romero, P.; Chen, J.L.; Cerundolo, V. High frequency of skin-homing melanocyte-specific cytotoxic T lymphocytes in autoimmune vitiligo. J. Exp. Med. 1998, 188, 1203–1208. [Google Scholar] [CrossRef] [PubMed]
- Wańkowicz-Kalińska, A.; van den Wijngaard, R.M.; Tigges, B.J.; Westerhof, W.; Ogg, G.S.; Cerundolo, V.; Storkus, W.J.; Das, P.K. Immunopolarization of CD4+ and CD8+ T cells to Type-1-like is associated with melanocyte loss in human vitiligo. Lab. Investig. 2003, 83, 683–695. [Google Scholar] [CrossRef] [PubMed]
- Dwivedi, M.; Kemp, E.H.; Laddha, N.C.; Mansuri, M.S.; Weetman, A.P.; Begum, R. Regulatory T cells in vitiligo: Implications for pathogenesis and therapeutics. Autoimmun. Rev. 2015, 14, 49–56. [Google Scholar] [CrossRef] [PubMed]
- Sanchez Rodriguez, R.; Pauli, M.L.; Neuhaus, I.M.; Yu, S.S.; Arron, S.T.; Harris, H.W.; Yang, S.H.; Anthony, B.A.; Sverdrup, F.M.; Krow-Lucal, E.; et al. Memory regulatory T cells reside in human skin. J. Clin. Investig. 2014, 124, 1027–1036. [Google Scholar] [CrossRef] [PubMed]
- Klarquist, J.; Denman, C.J.; Hernandez, C.; Wainwright, D.A.; Strickland, F.M.; Overbeck, A.; Mehrotra, S.; Nishimura, M.I.; Le Poole, I.C. Reduced skin homing by functional Treg in vitiligo. Pigment. Cell Melanoma Res. 2010, 23, 276–286. [Google Scholar] [CrossRef]
- Plaza-Rojas, L.; Guevara-Patiño, J.A. The Role of the NKG2D in Vitiligo. Front. Immunol. 2021, 12, 624131. [Google Scholar] [CrossRef] [PubMed]
- Xuan, Y.; Yang, Y.; Xiang, L.; Zhang, C. The Role of Oxidative Stress in the Pathogenesis of Vitiligo: A Culprit for Melanocyte Death. Oxid. Med. Cell Longev. 2022, 2022, 8498472. [Google Scholar] [CrossRef]
- Koga, S.; Nakano, M.; Tero-Kubota, S. Generation of superoxide during the enzymatic action of tyrosinase. Arch. Biochem. Biophys. 1992, 292, 570–575. [Google Scholar] [CrossRef]
- Simon, J.D.; Peles, D.; Wakamatsu, K.; Ito, S. Current challenges in understanding melanogenesis: Bridging chemistry, biological control, morphology, and function. Pigment Cell Melanoma Res. 2009, 22, 563–579. [Google Scholar] [CrossRef]
- Cao, S.S.; Kaufman, R.J. Endoplasmic reticulum stress and oxidative stress in cell fate decision and human disease. Antioxid. Redox. Signal. 2014, 21, 396–413. [Google Scholar] [CrossRef]
- Toosi, S.; Orlow, S.J.; Manga, P. Vitiligo-inducing phenols activate the unfolded protein response in melanocytes resulting in upregulation of IL6 and IL8. J. Investig. Dermatol. 2012, 132, 2601–2609. [Google Scholar] [CrossRef] [PubMed]
- Qiao, Z.; Wang, X.; Xiang, L.; Zhang, C. Dysfunction of Autophagy: A Possible Mechanism Involved in the Pathogenesis of Vitiligo by Breaking the Redox Balance of Melanocytes. Oxid. Med. Cell. Longev. 2016, 2016, 3401570. [Google Scholar] [CrossRef] [PubMed]
- Bellei, B.; Pitisci, A.; Ottaviani, M.; Ludovici, M.; Cota, C.; Luzi, F.; Dell’Anna, M.L.; Picardo, M. Vitiligo: A possible model of degenerative diseases. PLoS ONE 2013, 8, e59782. [Google Scholar] [CrossRef]
- Bellei, B.; Picardo, M. Premature cell senescence in human skin: Dual face in chronic acquired pigmentary disorders. Ageing Res. Rev. 2020, 57, 100981. [Google Scholar] [CrossRef] [PubMed]
- Jimbow, K.; Chen, H.; Park, J.S.; Thomas, P.D. Increased sensitivity of melanocytes to oxidative stress and abnormal expression of tyrosinase-related protein in vitiligo. Br. J. Dermatol. 2001, 144, 55–65. [Google Scholar] [CrossRef] [PubMed]
- Dell’Anna, M.L.; Ottaviani, M.; Bellei, B.; Albanesi, V.; Cossarizza, A.; Rossi, L.; Picardo, M. Membrane lipid defects are responsible for the generation of reactive oxygen species in peripheral blood mononuclear cells from vitiligo patients. J. Cell Physiol. 2010, 223, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Schallreuter, K.U.; Wood, J.M.; Berger, J. Low catalase levels in the epidermis of patients with vitiligo. J. Investig. Dermatol. 1991, 97, 1081–1085. [Google Scholar] [CrossRef]
- Schallreuter, K.U.; Moore, J.; Wood, J.M.; Beazley, W.D.; Gaze, D.C.; Tobin, D.J.; Marshall, H.S.; Panske, A.; Panzig, E.; Hibberts, N.A. In vivo and in vitro evidence for hydrogen peroxide (H2O2) accumulation in the epidermis of patients with vitiligo and its successful removal by a UVB-activated pseudocatalase. J. Investig. Dermatol. Symp. Proc. 1999, 4, 91–96. [Google Scholar] [CrossRef]
- Schallreuter, K.U.; Salem, M.A.; Holtz, S.; Panske, A. Basic evidence for epidermal H2O2/ONOO(-)-mediated oxidation/nitration in segmental vitiligo is supported by repigmentation of skin and eyelashes after reduction of epidermal H2O2 with topical NB-UVB-activated pseudocatalase PC-KUS. FASEB J. 2013, 27, 3113–3122. [Google Scholar] [CrossRef]
- Maresca, V.; Roccella, M.; Roccella, F.; Camera, E.; Del Porto, G.; Passi, S.; Grammatico, P.; Picardo, M. Increased sensitivity to peroxidative agents as a possible pathogenic factor of melanocyte damage in vitiligo. J. Investig. Dermatol. 1997, 109, 310–313. [Google Scholar] [CrossRef]
- Jain, A.; Mal, J.; Mehndiratta, V.; Chander, R.; Patra, S.K. Study of oxidative stress in vitiligo. Indian J. Clin. Biochem. 2011, 26, 78–81. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Romano-Lozano, V.; Cruz-Avelar, A.; Peralta Pedrero, M.L. Nuclear Factor Erythroid 2-Related Factor 2 in Vitiligo. Actas Dermosifiliogr. 2022, 113, 705–711. [Google Scholar] [CrossRef] [PubMed]
- Lin, X.; Meng, X.; Song, Z.; Lin, J. Nuclear factor erythroid 2-related factor 2 (Nrf2) as a potential therapeutic target for vitiligo. Arch. Biochem. Biophys. 2020, 696, 108670. [Google Scholar] [CrossRef] [PubMed]
- Taïeb, A.; Picardo, M. Clinical practice. Vitiligo. N. Engl. J. Med. 2009, 360, 160–169. [Google Scholar] [CrossRef] [PubMed]
- Jung, S.E.; Kang, H.Y.; Lee, E.S.; Kim, Y.C. Changes of epidermal thickness in vitiligo. Am. J. Dermatopathol. 2015, 37, 289–292. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Man, W.Y.; Lv, C.Z.; Song, S.P.; Shi, Y.J.; Elias, P.M.; Man, M.Q. Epidermal permeability barrier recovery is delayed in vitiligo-involved sites. Skin. Pharmacol. Physiol. 2010, 23, 193–200. [Google Scholar] [CrossRef]
- Al’Abadie, M.S.; Warren, M.A.; Bleehen, S.S.; Gawkrodger, D.J. Morphologic observations on the dermal nerves in vitiligo: An ultrastructural study. Int. J. Dermatol. 1995, 34, 837–840. [Google Scholar] [CrossRef]
- Bondanza, S.; Maurelli, R.; Paterna, P.; Migliore, E.; Giacomo, F.D.; Primavera, G.; Paionni, E.; Dellambra, E.; Guerra, L. Keratinocyte cultures from involved skin in vitiligo patients show an impaired in vitro behaviour. Pigment. Cell Res. 2007, 20, 288–300. [Google Scholar] [CrossRef]
- Lee, A.Y.; Kim, N.H.; Choi, W.I.; Youm, Y.H. Less keratinocyte-derived factors related to more keratinocyte apoptosis in depigmented than normally pigmented suction-blistered epidermis may cause passive melanocyte death in vitiligo. J. Investig. Dermatol. 2005, 124, 976–983. [Google Scholar] [CrossRef]
- Wagner, R.Y.; Luciani, F.; Cario-André, M.; Rubod, A.; Petit, V.; Benzekri, L.; Ezzedine, K.; Lepreux, S.; Steingrimsson, E.; Taieb, A.; et al. Altered E-Cadherin Levels and Distribution in Melanocytes Precede Clinical Manifestations of Vitiligo. J. Investig. Dermatol. 2015, 135, 1810–1819. [Google Scholar] [CrossRef]
- Elsherif, R.; Mahmoud, W.A.; Mohamed, R.R. Melanocytes and keratinocytes morphological changes in vitiligo patients. A histological, immunohistochemical and ultrastructural analysis. Ultrastruct. Pathol. 2022, 46, 217–235. [Google Scholar] [CrossRef] [PubMed]
- Becatti, M.; Prignano, F.; Fiorillo, C.; Pescitelli, L.; Nassi, P.; Lotti, T.; Taddei, N. The involvement of Smac/DIABLO, p53, NF-kB, and MAPK pathways in apoptosis of keratinocytes from perilesional vitiligo skin: Protective effects of curcumin and capsaicin. Antioxid. Redox. Signal. 2010, 13, 1309–1321. [Google Scholar] [CrossRef] [PubMed]
- Bastonini, E.; Bellei, B.; Filoni, A.; Kovacs, D.; Iacovelli, P.; Picardo, M. Involvement of non-melanocytic skin cells in vitiligo. Exp. Dermatol. 2019, 28, 667–673. [Google Scholar] [CrossRef] [PubMed]
- Kovacs, D.; Bastonini, E.; Ottaviani, M.; Cota, C.; Migliano, E.; Dell’Anna, M.L.; Picardo, M. Vitiligo Skin: Exploring the Dermal Compartment. J. Investig. Dermatol. 2018, 138, 394–404. [Google Scholar] [CrossRef] [PubMed]
- Kovacs, D.; Bastonini, E.; Briganti, S.; Ottaviani, M.; D’Arino, A.; Truglio, M.; Sciuto, L.; Zaccarini, M.; Pacifico, A.; Cota, C.; et al. Altered epidermal proliferation, differentiation, and lipid composition: Novel key elements in the vitiligo puzzle. Sci. Adv. 2022, 8, eabn9299. [Google Scholar] [CrossRef]
- Dell’Anna, M.L.; Ottaviani, M.; Kovacs, D.; Mirabilii, S.; Brown, D.A.; Cota, C.; Migliano, E.; Bastonini, E.; Bellei, B.; Cardinali, G.; et al. Energetic mitochondrial failing in vitiligo and possible rescue by cardiolipin. Sci. Rep. 2017, 7, 13663. [Google Scholar] [CrossRef]
- Tulic, M.K.; Cavazza, E.; Cheli, Y.; Jacquel, A.; Luci, C.; Cardot-Leccia, N.; Hadhiri-Bzioueche, H.; Abbe, P.; Gesson, M.; Sormani, L.; et al. Innate lymphocyte-induced CXCR3B-mediated melanocyte apoptosis is a potential initiator of T-cell autoreactivity in vitiligo. Nat. Commun. 2019, 10, 2178. [Google Scholar] [CrossRef]
- Li, S.; Zhu, G.; Yang, Y.; Jian, Z.; Guo, S.; Dai, W.; Shi, Q.; Ge, R.; Ma, J.; Liu, L.; et al. Oxidative stress drives CD8(+) T-cell skin trafficking in patients with vitiligo through CXCL16 upregulation by activating the unfolded protein response in keratinocytes. J. Allergy Clin. Immunol. 2017, 140, 177–189.e9. [Google Scholar] [CrossRef]
- Yamaguchi, Y.; Itami, S.; Watabe, H.; Yasumoto, K.; Abdel-Malek, Z.A.; Kubo, T.; Rouzaud, F.; Tanemura, A.; Yoshikawa, K.; Hearing, V.J. Mesenchymal-epithelial interactions in the skin: Increased expression of dickkopf1 by palmoplantar fibroblasts inhibits melanocyte growth and differentiation. J. Cell Biol. 2004, 165, 275–285. [Google Scholar] [CrossRef]
- Choi, W.; Wolber, R.; Gerwat, W.; Mann, T.; Batzer, J.; Smuda, C.; Liu, H.; Kolbe, L.; Hearing, V.J. The fibroblast-derived paracrine factor neuregulin-1 has a novel role in regulating the constitutive color and melanocyte function in human skin. J. Cell Sci. 2010, 123, 3102–3111. [Google Scholar]
- Yuan, X.; Meng, D.; Cao, P.; Sun, L.; Pang, Y.; Li, Y.; Wang, X.; Luo, Z.; Zhang, L.; Liu, G. Identification of pathogenic genes and transcription factors in vitiligo. Dermatol. Ther. 2019, 32, e13025. [Google Scholar] [CrossRef] [PubMed]
- Kingo, K.; Aunin, E.; Karelson, M.; Philips, M.A.; Rätsep, R.; Silm, H.; Vasar, E.; Soomets, U.; Kõks, S. Gene expression analysis of melanocortin system in vitiligo. J. Dermatol. Sci. 2007, 48, 113–122. [Google Scholar] [PubMed]
- Pichler, R.; Sfetsos, K.; Badics, B.; Gutenbrunner, S.; Auböck, J. Vitiligo patients present lower plasma levels of alpha-melanotropin immunoreactivities. Neuropeptides 2006, 40, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Böhm, M.; Schiller, M.; Luger, T.A. Non-pigmentary actions of alpha-melanocyte-stimulating hormone—Lessons from the cutaneous melanocortin system. Cell Mol. Biol. 2006, 52, 61–68. [Google Scholar]
- Haycock, J.W.; Rowe, S.J.; Cartledge, S.; Wyatt, A.; Ghanem, G.; Morandini, R.; Rennie, I.G.; MacNeil, S. Alpha-melanocyte-stimulating hormone reduces impact of proinflammatory cytokine and peroxide-generated oxidative stress on keratinocyte and melanoma cell lines. J. Biol. Chem. 2000, 275, 15629–15636. [Google Scholar]
- Moustafa, M.; Szabo, M.; Ghanem, G.E.; Morandini, R.; Kemp, E.H.; MacNeil, S.; Haycock, J.W. Inhibition of tumor necrosis factor-alpha stimulated NFkappaB/p65 in human keratinocytes by alpha-melanocyte stimulating hormone and adrenocorticotropic hormone peptides. J. Investig. Dermatol. 2002, 119, 1244–1253. [Google Scholar]
- Xu, Z.; Chen, D.; Hu, Y.; Jiang, K.; Huang, H.; Du, Y.; Wu, W.; Wang, J.; Sui, J.; Wang, W.; et al. Anatomically distinct fibroblast subsets determine skin autoimmune patterns. Nature 2022, 601, 118–124. [Google Scholar]
- Bellei, B.; Migliano, E.; Tedesco, M.; Caputo, S.; Papaccio, F.; Lopez, G.; Picardo, M. Adipose tissue-derived extracellular fraction characterization: Biological and clinical considerations in regenerative medicine. Stem. Cell Res. Ther. 2018, 9, 207. [Google Scholar] [CrossRef]
- Daniel, B.S.; Wittal, R. Vitiligo treatment update. Australas J. Dermatol. 2015, 56, 85–92. [Google Scholar]
- Luger, T.; Paul, C. Potential new indications of topical calcineurin inhibitors. Dermatology 2007, 215 (Suppl. 1), 45–54. [Google Scholar]
- Kuga, K.; Nishifuji, K.; Iwasaki, T. Cyclosporine A inhibits transcription of cytokine genes and decreases the frequencies of IL-2 producing cells in feline mononuclear cells. J. Vet. Med. Sci. 2008, 70, 1011–1016. [Google Scholar] [CrossRef] [PubMed]
- Colucci, R.; Dragoni, F.; Conti, R.; Pisaneschi, L.; Lazzeri, L.; Moretti, S. Evaluation of an oral supplement containing Phyllanthus emblica fruit extracts, vitamin E, and carotenoids in vitiligo treatment. Dermatol. Ther. 2015, 28, 17–21. [Google Scholar] [CrossRef]
- Le Duff, F.; Fontas, E.; Giacchero, D.; Sillard, L.; Lacour, J.P.; Ortonne, J.P.; Passeron, T. 308-Nm Excimer Lamp Vs. 308-Nm Excimer Laser for Treating Vitiligo: A Randomized Study. Br. J. Dermatol. 2010, 163, 188–192. [Google Scholar] [CrossRef] [PubMed]
- Parsad, D. A new era of vitiligo research and treatment. J. Cutan. Aesthet. Surg. 2013, 6, 63–64. [Google Scholar] [CrossRef]
- Lim, H.W.; Grimes, P.E.; Agbai, O.; Hamzavi, I.; Henderson, M.; Haddican, M.; Linkner, R.V.; Lebwohl, M. Afamelanotide and narrowband UV-B phototherapy for the treatment of vitiligo: A randomized multicenter trial. JAMA Dermatol. 2015, 151, 42–50. [Google Scholar] [CrossRef] [PubMed]
- He, S.; Xu, J.; Wu, J. The Promising Role of Chemokines in Vitiligo: From Oxidative Stress to the Autoimmune Response. Oxid. Med. Cell Longev. 2022, 2022, 8796735. [Google Scholar] [CrossRef]
- Qi, F.; Liu, F.; Gao, L. Janus Kinase Inhibitors in the Treatment of Vitiligo: A Review. Front. Immunol. 2021, 12, 790125. [Google Scholar] [CrossRef]
- Birlea, S.A.; Costin, G.E.; Roop, D.R.; Norris, D.A. Trends in Regenerative Medicine: Repigmentation in Vitiligo Through Melanocyte Stem Cell Mobilization. Med. Res. Rev. 2017, 37, 907–935. [Google Scholar] [CrossRef]
- Mobasher, P.; Guerra, R.; Li, S.J.; Frangos, J.; Ganesan, A.K.; Huang, V. Open-label pilot study of tofacitinib 2% for the treatment of refractory vitiligo. Br. J. Dermatol. 2020, 182, 1047–1049. [Google Scholar] [CrossRef]
- Kubelis-López, D.E.; Zapata-Salazar, N.A.; Said-Fernández, S.L.; Sánchez-Domínguez, C.N.; Salinas-Santander, M.A.; Martínez-Rodríguez, H.G.; Vázquez-Martínez, O.T.; Wollina, U.; Lotti, T.; Ocampo-Candiani, J. Updates and new medical treatments for vitiligo (Review). Exp. Ther. Med. 2021, 22, 797. [Google Scholar] [CrossRef]
- Joshipura, D.; Plotnikova, N.; Goldminz, A.; Deverapalli, S.; Turkowski, Y.; Gottlieb, A.; Rosmarin, D. Importance of light in the treatment of vitiligo with JAK-inhibitors. J. Dermatolog. Treat. 2018, 29, 98–99. [Google Scholar] [CrossRef] [PubMed]
- Gianfaldoni, S.; Wollina, U.; Tirant, M.; Tchernev, G.; Lotti, J.; Satolli, F.; Rovesti, M.; França, K.; Lotti, T. Herbal Compounds for the Treatment of Vitiligo: A Review. Open Access Maced. J. Med. Sci. 2018, 6, 203–207. [Google Scholar] [CrossRef] [PubMed]
- Yannas, I.V. Similarities and differences between induced organ regeneration in adults and early foetal regeneration. J. R. Soc. Interface 2005, 2, 403–417. [Google Scholar] [CrossRef] [PubMed]
- Ramos, M.G.; Ramos, D.G.; Ramos, C.G. Evaluation of treatment response to autologous transplantation of noncultured melanocyte/keratinocyte cell suspension in patients with stable vitiligo. An. Bras. Dermatol. 2017, 92, 312–318. [Google Scholar] [CrossRef] [PubMed]
- Olsson, M.J.; Juhlin, L. Epidermal sheet grafts for repigmentation of vitiligo and piebaldism, with a review of surgical techniques. Acta Derm. Venereol. 1997, 77, 463–466. [Google Scholar]
- Lu, N.; Xu, A.; Wu, X. Follow-up study of vitiligo patients treated with autologous epidermal sheet transplants. J. Dermatolog. Treat. 2014, 25, 200–204. [Google Scholar] [CrossRef]
- Juhlin, L. How unstable is the concept of stability in surgical repigmentation of vitiligo. Dermatology 2000, 201, 183. [Google Scholar]
- Mulekar, S.V.; Isedeh, P. Surgical interventions for vitiligo: An evidence-based review. Br. J. Dermatol. 2013, 169 (Suppl. S3), 57–66. [Google Scholar] [CrossRef]
- Hann, S.K.; Im, S.; Bong, H.W.; Park, Y.K. Treatment of stable vitiligo with autologous epidermal grafting and PUVA. J. Am. Acad. Dermatol. 1995, 32, 943–948. [Google Scholar] [CrossRef]
- Awad, S.S.; Abdel-Raof, H.; Hosam El-Din, W.; El-Domyati, M. Epithelial grafting for vitiligo requires ultraviolet A phototherapy to increase success rate. J. Cosmet. Dermatol. 2007, 6, 119–124. [Google Scholar] [CrossRef]
- Pianigiani, E.; Risulo, M.; Andreassi, A.; Taddeucci, P.; Ierardi, F.; Andreassi, L. Autologous epidermal cultures and narrow-band ultraviolet B in the surgical treatment of vitiligo. Dermatol. Surg. 2005, 31, 155–159. [Google Scholar] [CrossRef] [PubMed]
- Barman, K.D.; Khaitan, B.K.; Verma, K.K. A comparative study of punch grafting followed by topical corticosteroid versus punch grafting followed by PUVA therapy in stable vitiligo. Dermatol. Surg. 2004, 30, 49–53. [Google Scholar] [PubMed]
- Al-Mutairi, N.; Manchanda, Y.; Al-Doukhi, A.; Al-Haddad, A. Long-term results of split-skin grafting in combination with excimer laser for stable vitiligo. Dermatol. Surg. 2010, 36, 499–505. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, N.E.; Mulliken, J.B.; Banks-Schlegel, S.; Kehinde, O.; Green, H. Grafting of burns with cultured epithelium prepared from autologous epidermal cells. Lancet 1981, 1, 75–78. [Google Scholar] [CrossRef]
- Falabella, R.; Arrunategui, A.; Barona, M.I.; Alzate, A. The minigrafting test for vitiligo: Detection of stable lesions for melanocyte transplantation. J. Am. Acad. Dermatol. 1995, 32, 228–232. [Google Scholar] [CrossRef]
- Khalili, M.; Amiri, R.; Mohammadi, S.; Iranmanesh, B.; Aflatoonian, M. Efficacy and safety of traditional and surgical treatment modalities in segmental vitiligo: A review article. J. Cosmet. Dermatol. 2022, 21, 2360–2373. [Google Scholar] [CrossRef]
- Kato, A.; Okamoto, O.; Ishikawa, K.; Sumiyoshi, H.; Matsuo, N.; Yoshioka, H.; Nomizu, M.; Shimada, T.; Fujiwara, S. Dermatopontin interacts with fibronectin, promotes fibronectin fibril formation, and enhances cell adhesion. J. Biol. Chem. 2011, 286, 14861–14869. [Google Scholar] [CrossRef]
- Feetham, H.J.; Chan, J.L.; Pandya, A.G. Characterization of clinical response in patients with vitiligo undergoing autologous epidermal punch grafting. Dermatol. Surg. 2012, 38, 14–19. [Google Scholar] [CrossRef]
- Lei, T.C.; Hearing, V.J. Deciphering skin re-pigmentation patterns in vitiligo: An update on the cellular and molecular events involved. Chin. Med. J. 2020, 133, 1231–1238. [Google Scholar] [CrossRef]
- Abdallah, M.; Abdel-Naser, M.B.; Moussa, M.H.; Assaf, C.; Orfanos, C.E. Sequential immunohistochemical study of depigmenting and repigmenting minigrafts in vitiligo. Eur. J. Dermatol. 2003, 13, 548–552. [Google Scholar]
- Kovacs, D.; Abdel-Raouf, H.; Al-Khayyat, M.; Abdel-Azeem, E.; Hanna, M.R.; Cota, C.; Picardo, M.; Anbar, T.S. Vitiligo: Characterization of melanocytes in repigmented skin after punch grafting. J. Eur. Acad. Dermatol. Venereol. 2015, 29, 581–590. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.Y.; Park, J.H.; Choi, S.C.; Lee, J.H. Comparison of recipient site preparations in epidermal grafting for vitiligo: Suction blister and CO2 laser. J. Eur. Acad. Dermatol. Venereol. 2009, 23, 1448–1449. [Google Scholar] [CrossRef] [PubMed]
- Kar, B.R.; Raj, C. Suction Blister Epidermal Grafting for Vitiligo Involving Angles of Lip: Experience of 112 Patients. J. Cutan. Aesthet. Surg. 2018, 11, 13–19. [Google Scholar] [CrossRef]
- Frączek, A.; Kasprowicz-Furmańczyk, M.; Placek, W.; Owczarczyk-Saczonek, A. Surgical Treatment of Vitiligo. Int. J. Environ. Res. Public. Health. 2022, 19, 4812. [Google Scholar] [CrossRef]
- Kahn, A.M.; Cohen, M.J. Repigmentation in vitiligo patients. Melanocyte transfer via ultra-thin grafts. Dermatol. Surg. 1998, 24, 365–367. [Google Scholar] [CrossRef] [PubMed]
- Sameem, F.; Sultan, S.J.; Ahmad, Q.M. Split thickness skin grafting in patients with stable vitiligo. J. Cutan. Aesthet. Surg. 2011, 4, 38–40. [Google Scholar] [PubMed]
- Al-Hadidi, N.; Griffith, J.L.; Al-Jamal, M.S.; Hamzavi, I. Role of Recipient-site Preparation Techniques and Post-operative Wound Dressing in the Surgical Management of Vitiligo. J. Cutan. Aesthet. Surg. 2015, 8, 79–87. [Google Scholar] [PubMed]
- Braza, M.E.; Fahrenkopf, M.P. Split-Thickness Skin Grafts. In StatPearls; StatPearls Publishing LLC: Treasure Island, FL, USA, 2022. [Google Scholar]
- Chopra, A.; Lekshmipriya, K. A comparative study of efficacy of split-thickness skin grafting versus autologous melanocyte transfer in the management of stable vitiligo. Med. J. Armed. Forces India 2022, 78, S42–S48. [Google Scholar] [CrossRef]
- Mayer, T.C. The migratory pathway of neural crest cells into the skin of mouse embryos. Dev. Biol. 1973, 34, 39–46. [Google Scholar] [CrossRef]
- Nishimura, E.K.; Yoshida, H.; Kunisada, T.; Nishikawa, S.I. Regulation of E- and P-cadherin expression correlated with melanocyte migration and diversification. Dev. Biol. 1999, 215, 155–166. [Google Scholar] [CrossRef]
- Silver, A.F.; Chase, H.B.; Potten, C.S. Melanocyte precursor cells in the hair follicle germ during the dormat stage (telogen). Experientia 1969, 25, 299–301. [Google Scholar] [CrossRef]
- Ortonne, J.P. Pigmentary changes of the ageing skin. Br. J. Dermatol. 1990, 122 (Suppl. 35), 21–28. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, N.B.; Koster, M.I.; Hoaglin, L.G.; Spoelstra, N.S.; Kechris, K.J.; Robinson, S.E.; Robinson, W.A.; Roop, D.R.; Norris, D.A.; Birlea, S.A. Narrow Band Ultraviolet B Treatment for Human Vitiligo Is Associated with Proliferation, Migration, and Differentiation of Melanocyte Precursors. J. Investig. Dermatol. 2015, 135, 2068–2076. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, N.B.; Koster, M.I.; Jones, K.L.; Gao, B.; Hoaglin, L.G.; Robinson, S.E.; Wright, M.J.; Birlea, S.I.; Luman, A.; Lambert, K.A.; et al. Repigmentation of Human Vitiligo Skin by NBUVB Is Controlled by Transcription of GLI1 and Activation of the β-Catenin Pathway in the Hair Follicle Bulge Stem Cells. J. Investig. Dermatol. 2018, 138, 657–668. [Google Scholar] [CrossRef] [PubMed]
- Parsad, D.; Pandhi, R.; Dogra, S.; Kumar, B. Clinical study of repigmentation patterns with different treatment modalities and their correlation with speed and stability of repigmentation in 352 vitiliginous patches. J. Am. Acad. Dermatol. 2004, 50, 63–67. [Google Scholar] [PubMed]
- Cui, J.; Shen, L.Y.; Wang, G.C. Role of hair follicles in the repigmentation of vitiligo. J. Investig. Dermatol. 1991, 97, 410–416. [Google Scholar] [CrossRef] [PubMed]
- Thakur, P.; Sacchidanand, S.; Nataraj, H.V.; Savitha, A.S. A Study of Hair Follicular Transplantation as a Treatment Option for Vitiligo. J. Cutan. Aesthet. Surg. 2015, 8, 211–217. [Google Scholar] [CrossRef]
- Gauthier, Y.; Surleve-Bazeille, J.E. Autologous grafting with noncultured melanocytes: A simplified method for treatment of depigmented lesions. J. Am. Acad. Dermatol. 1992, 26, 191–194. [Google Scholar] [CrossRef]
- van Geel, N.; Ongenae, K.; De Mil, M.; Haeghen, Y.V.; Vervaet, C.; Naeyaert, J.M. Double-blind placebo-controlled study of autologous transplanted epidermal cell suspensions for repigmenting vitiligo. Arch. Dermatol. 2004, 140, 1203–1208. [Google Scholar] [CrossRef][Green Version]
- Li, D.; Zhang, R.Z.; Shi, H.X.; Yang, Y.H.; Tian, T.; Wang, L. Melanocyte spheroids are formed by repetitive long-term trypsinization. Indian. J. Dermatol. Venereol. Leprol. 2019, 85, 258–265. [Google Scholar]
- El-Zawahry, B.M.; Esmat, S.; Bassiouny, D.; Zaki, N.S.; Sobhi, R.; Saleh, M.A.; Abdel-Halim, D.; Hegazy, R.; Gawdat, H.; Samir, N.; et al. Effect of Procedural-Related Variables on Melanocyte-Keratinocyte Suspension Transplantation in Nonsegmental Stable Vitiligo: A Clinical and Immunocytochemical Study. Dermatol. Surg. 2017, 43, 226–235. [Google Scholar] [CrossRef] [PubMed]
- Mulekar, S.V. Long-term follow-up study of segmental and focal vitiligo treated by autologous, noncultured melanocyte-keratinocyte cell transplantation. Arch. Dermatol. 2004, 140, 1211–1215. [Google Scholar] [CrossRef] [PubMed]
- Lahiri, K. Evolution and evaluation of autologous mini punch grafting in vitiligo. Indian, J. Dermatol. 2009, 54, 159–167. [Google Scholar] [CrossRef] [PubMed]
- Silpa-Archa, N.; Griffith, J.L.; Huggins, R.H.; Henderson, M.D.; Kerr, H.A.; Jacobsen, G.; Mulekar, S.V.; Lim, H.W.; Hamzavi, I.H. Long-term follow-up of patients undergoing autologous noncultured melanocyte-keratinocyte transplantation for vitiligo and other leukodermas. J. Am. Acad. Dermatol. 2017, 77, 318–327. [Google Scholar] [CrossRef]
- Thakur, V.; Kumar, S.; Kumaran, M.S.; Kaushik, H.; Srivastava, N.; Parsad, D. Efficacy of Transplantation of Combination of Noncultured Dermal and Epidermal Cell Suspension vs Epidermal Cell Suspension Alone in Vitiligo: A Randomized Clinical Trial. JAMA Dermatol. 2019, 155, 204–210. [Google Scholar] [CrossRef]
- Swope, V.B.; Medrano, E.E.; Smalara, D.; Abdel-Malek, Z.A. Long-term proliferation of human melanocytes is supported by the physiologic mitogens alpha-melanotropin, endothelin-1, and basic fibroblast growth factor. Exp. Cell Res. 1995, 217, 453–459. [Google Scholar]
- Szabad, G.; Kormos, B.; Pivarcsi, A.; Széll, M.; Kis, K.; Kenderessy Szabó, A.; Dobozy, A.; Kemény, L.; Bata-Csörgo, Z. Human adult epidermal melanocytes cultured without chemical mitogens express the EGF receptor and respond to EGF. Arch. Dermatol. Res. 2007, 299, 191–200. [Google Scholar] [CrossRef]
- Ghosh, D.; Shenoy, S.; Kuchroo, P. Cultured melanocytes: From skin biopsy to transplantation. Cell Transplant. 2008, 17, 351–360. [Google Scholar]
- Kim, J.Y.; Park, C.D.; Lee, J.H.; Lee, C.H.; Do, B.R.; Lee, A.Y. Co-culture of melanocytes with adipose-derived stem cells as a potential substitute for co-culture with keratinocytes. Acta Derm. Venereol. 2012, 92, 16–23. [Google Scholar]
- Pathak, S.M.; Jindal, A.K.; Verma, A.K.; Mahen, A. An epidemiological study of road traffic accident cases admitted in a tertiary care hospital. Med. J. Armed. Forces India 2014, 70, 32–35. [Google Scholar] [CrossRef][Green Version]
- Verma, G.; Varkhande, S.R.; Kar, H.K.; Rani, R. Evaluation of Repigmentation with Cultured Melanocyte Transplantation (CMT) Compared with Non-Cultured Epidermal Cell Transplantation in Vitiligo at 12th Week Reveals Better Repigmentation with CMT. J. Investig. Dermatol. 2015, 135, 2533–2535. [Google Scholar] [CrossRef] [PubMed]
- Jiang, S.; Liao, Z.K.; Jia, H.Y.; Liu, X.M.; Wan, J.; Lei, T.C. The regional distribution of melanosomes in the epidermis affords a localized intensive photoprotection for basal keratinocyte stem cells. J. Dermatol. Sci. 2021, 103, 130–134. [Google Scholar] [CrossRef] [PubMed]
- Shah, A.N.; Marfatia, R.K.; Saikia, S.S. A Study of Noncultured Extracted Hair Follicle Outer Root Sheath Cell Suspension for Transplantation in Vitiligo. Int. J. Trichology 2016, 8, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A.; Mohanty, S.; Sahni, K.; Kumar, R.; Gupta, S. Extracted hair follicle outer root sheath cell suspension for pigment cell restoration in vitiligo. J. Cutan. Aesthet. Surg. 2013, 6, 121–125. [Google Scholar]
- Mohanty, S.; Kumar, A.; Dhawan, J.; Sreenivas, V.; Gupta, S. Noncultured extracted hair follicle outer root sheath cell suspension for transplantation in vitiligo. Br. J. Dermatol. 2011, 164, 1241–1246. [Google Scholar] [CrossRef]
- Singh, C.; Parsad, D.; Kanwar, A.J.; Dogra, S.; Kumar, R. Comparison between autologous noncultured extracted hair follicle outer root sheath cell suspension and autologous noncultured epidermal cell suspension in the treatment of stable vitiligo: A randomized study. Br. J. Dermatol. 2013, 169, 287–293. [Google Scholar]
- Hamza, A.M.; Hussein, T.M.; Shakshouk, H.A.R. Noncultured Extracted Hair Follicle Outer Root Sheath Cell Suspension versus Noncultured Epidermal Cell Suspension in the Treatment of Stable Vitiligo. J. Cutan. Aesthet. Surg. 2019, 12, 105–111. [Google Scholar]
- Kumaresan, M. Single-hair follicular unit transplant for stable vitiligo. J. Cutan. Aesthet. Surg. 2011, 4, 41–43. [Google Scholar] [CrossRef]
- Liebl, H.; Kloth, L.C. Skin cell proliferation stimulated by microneedles. J. Am. Coll. Clin. Wound Spec. 2012, 4, 2–6. [Google Scholar] [CrossRef]
- Donnelly, R.F.; Raj Singh, T.R.; Woolfson, A.D. Microneedle-based drug delivery systems: Microfabrication, drug delivery, and safety. Drug. Deliv. 2010, 17, 187–207. [Google Scholar] [CrossRef]
- Mina, M.; Elgarhy, L.; Al-Saeid, H.; Ibrahim, Z. Comparison between the efficacy of microneedling combined with 5-fluorouracil vs microneedling with tacrolimus in the treatment of vitiligo. J. Cosmet. Dermatol. 2018, 17, 744–751. [Google Scholar] [CrossRef] [PubMed]
- Chhabra, S.; Chahar, Y.S.; Singh, A. A Comparative Study of Microneedling Combined with Topical 5-Fluorouracil versus Microneedling Alone in Treatment of Localized Stable Vitiligo. Indian J. Dermatol. 2021, 66, 574. [Google Scholar] [PubMed]
- Korobko, I.V.; Lomonosov, K.M. A pilot comparative study of topical latanoprost and tacrolimus in combination with narrow-band ultraviolet B phototherapy and microneedling for the treatment of nonsegmental vitiligo. Dermatol. Ther. 2016, 29, 437–441. [Google Scholar] [PubMed]
- Feily, A.; Firoozifard, A.; Sokhandani, T.; Elosegui-Rodriguez, P.; Perez-Rivera, E.; Lange, C.S.; Hosseinpoor, M.; Ramirez-Fort, M.K. Follicular Transplantation, Microneedling, and Adjuvant Narrow-band Ultraviolet-B Irradiation as Cost-Effective Regimens for Palmar-Plantar Vitiligo: A Pilot Study. Cureus 2020, 12, e7878. [Google Scholar] [CrossRef]
- Regazzetti, C.; Alcor, D.; Chignon-Sicard, B.; Passeron, T. Micro holes for delivering melanocytes into the skin: An ex vivo approach. Pigment. Cell Melanoma Res. 2016, 29, 481–483. [Google Scholar] [CrossRef]
- Bellei, B.; Migliano, E.; Picardo, M. Research update of adipose tissue-based therapies in regenerative dermatology. Stem Cell Rev. Rep. 2022, 18, 1956–1973. [Google Scholar]
- Bellei, B.; Migliano, E.; Picardo, M. Therapeutic potential of adipose tissue-derivatives in modern dermatology. Exp. Dermatol. 2022. [Google Scholar] [CrossRef]
- Gentile, P.; Scioli, M.G.; Bielli, A.; De Angelis, B.; De Sio, C.; De Fazio, D.; Ceccarelli, G.; Trivisonno, A.; Orlandi, A.; Cervelli, V.; et al. Platelet-Rich Plasma and Micrografts Enriched with Autologous Human Follicle Mesenchymal Stem Cells Improve Hair Re-Growth in Androgenetic Alopecia. Biomolecular Pathway Analysis and Clinical Evaluation. Biomedicines 2019, 7, 27. [Google Scholar] [CrossRef]
- Sierra-Sánchez, Á.; Montero-Vilchez, T.; Quiñones-Vico, M.I.; Sanchez-Diaz, M.; Arias-Santiago, S. Current Advanced Therapies Based on Human Mesenchymal Stem Cells for Skin Diseases. Front. Cell Dev. Biol. 2021, 9, 643125. [Google Scholar]
- Pittenger, M.F.; Discher, D.E.; Péault, B.M.; Phinney, D.G.; Hare, J.M.; Caplan, A.I. Mesenchymal stem cell perspective: Cell biology to clinical progress. NPJ Regen. Med. 2019, 4, 22. [Google Scholar]
- El-Badawy, A.; Amer, M.; Abdelbaset, R.; Sherif, S.N.; Abo-Elela, M.; Ghallab, Y.H.; Abdelhamid, H.; Ismail, Y.; El-Badri, N. Adipose Stem Cells Display Higher Regenerative Capacities and More Adaptable Electro-Kinetic Properties Compared to Bone Marrow-Derived Mesenchymal Stromal Cells. Sci. Rep. 2016, 6, 37801. [Google Scholar] [CrossRef]
- Ferrero, R.; Rainer, P.; Deplancke, B. Toward a Consensus View of Mammalian Adipocyte Stem and Progenitor Cell Heterogeneity. Trends Cell Biol. 2020, 30, 937–950. [Google Scholar] [CrossRef]
- Gentile, P.; Garcovich, S. Concise Review: Adipose-Derived Stem Cells (ASCs) and Adipocyte-Secreted Exosomal microRNA (A-SE-miR) Modulate Cancer Growth and proMote Wound Repair. J. Clin. Med. 2019, 8, 855. [Google Scholar] [CrossRef] [PubMed]
- Ong, W.K.; Chakraborty, S.; Sugii, S. Adipose Tissue: Understanding the Heterogeneity of Stem Cells for Regenerative Medicine. Biomolecules 2021, 11, 918. [Google Scholar] [CrossRef] [PubMed]
- Bellei, B.; Migliano, E.; Tedesco, M.; Caputo, S.; Picardo, M. Maximizing non-enzymatic methods for harvesting adipose-derived stem from lipoaspirate: Technical considerations and clinical implications for regenerative surgery. Sci. Rep. 2017, 7, 10015. [Google Scholar] [CrossRef] [PubMed]
- Zavala, G.; Sandoval, C.; Meza, D.; Contreras, R.; Gubelin, W.; Khoury, M. Differentiation of adipose-derived stem cells to functional CD105(neg) CD73(low) melanocyte precursors guided by defined culture condition. Stem Cell Res. Ther. 2019, 10, 249. [Google Scholar] [CrossRef]
- Dubey, N.K.; Mishra, V.K.; Dubey, R.; Deng, Y.H.; Tsai, F.C.; Deng, W.P. Revisiting the Advances in Isolation, Characterization and Secretome of Adipose-Derived Stromal/Stem Cells. Int. J. Mol. Sci. 2018, 19, 2200. [Google Scholar] [CrossRef]
- Markov, A.; Thangavelu, L.; Aravindhan, S.; Zekiy, A.O.; Jarahian, M.; Chartrand, M.S.; Pathak, Y.; Marofi, F.; Shamlou, S.; Hassanzadeh, A. Mesenchymal stem/stromal cells as a valuable source for the treatment of immune-mediated disorders. Stem Cell Res. Ther. 2021, 12, 192. [Google Scholar] [CrossRef]
- Bellei, B.; Papaccio, F.; Filoni, A.; Caputo, S.; Lopez, G.; Migliano, E.; Picardo, M. Extracellular fraction of adipose tissue as an innovative regenerative approach for vitiligo treatment. Exp. Dermatol. 2019, 28, 695–703. [Google Scholar] [CrossRef]
- Esquivel, D.; Mishra, R.; Srivastava, A. Stem Cell Therapy Offers a Possible Safe and Promising Alternative Approach for Treating Vitiligo: A Review. Curr. Pharm. Des. 2020, 26, 4815–4821. [Google Scholar] [CrossRef]
- Riding, R.L.; Harris, J.E. The Role of Memory CD8(+) T Cells in Vitiligo. J. Immunol. 2019, 203, 11–19. [Google Scholar] [CrossRef] [PubMed]
- Spallanzani, R.G. Visceral adipose tissue mesenchymal stromal cells in the intersection of immunology and metabolism. Am. J. Physiol. Endocrinol. Metab. 2021, 320, E512–E519. [Google Scholar] [CrossRef] [PubMed]
- Pfisterer, K.; Lipnik, K.M.; Hofer, E.; Elbe-Bürger, A. CD90(+) human dermal stromal cells are potent inducers of FoxP3(+) regulatory T cells. J. Investig. Dermatol. 2015, 135, 130–141. [Google Scholar] [CrossRef] [PubMed]
- Lim, W.S.; Kim, C.H.; Kim, J.Y.; Do, B.R.; Kim, E.J.; Lee, A.Y. Adipose-derived stem cells improve efficacy of melanocyte transplantation in animal skin. Biomol. Ther. 2014, 22, 328–333. [Google Scholar]
- Li, L.; Ngo, H.T.T.; Hwang, E.; Wei, X.; Liu, Y.; Liu, J.; Yi, T.H. Conditioned Medium from Human Adipose-Derived Mesenchymal Stem Cell Culture Prevents UVB-Induced Skin Aging in Human Keratinocytes and Dermal Fibroblasts. Int. J. Mol. Sci. 2019, 21, 49. [Google Scholar] [CrossRef]
- Fisch, S.C.; Gimeno, M.L.; Phan, J.D.; Simerman, A.A.; Dumesic, D.A.; Perone, M.J.; Chazenbalk, G.D. Pluripotent nontumorigenic multilineage differentiating stress enduring cells (Muse cells): A seven-year retrospective. Stem. Cell Res. Ther. 2017, 8, 227. [Google Scholar]
- Tsuchiyama, K.; Wakao, S.; Kuroda, Y.; Ogura, F.; Nojima, M.; Sawaya, N.; Yamasaki, K.; Aiba, S.; Dezawa, M. Functional melanocytes are readily reprogrammable from multilineage-differentiating stress-enduring (muse) cells, distinct stem cells in human fibroblasts. J. Investig. Dermatol. 2013, 133, 2425–2435. [Google Scholar]
- Yamauchi, T.; Yamasaki, K.; Tsuchiyama, K.; Koike, S.; Aiba, S. The Potential of Muse Cells for Regenerative Medicine of Skin: Procedures to Reconstitute Skin with Muse Cell-Derived Keratinocytes, Fibroblasts, and Melanocytes. J. Investig. Dermatol. 2017, 137, 2639–2642. [Google Scholar] [CrossRef]
- Tian, T.; Zhang, R.Z.; Yang, Y.H.; Liu, Q.; Li, D.; Pan, X.R. Muse Cells Derived from Dermal Tissues Can Differentiate into Melanocytes. Cell Reprogram 2017, 19, 116–122. [Google Scholar]
- Ikeda, Y.; Wada, A.; Hasegawa, T.; Yokota, M.; Koike, M.; Ikeda, S. Melanocyte progenitor cells reside in human subcutaneous adipose tissue. PLoS ONE 2021, 16, e0256622. [Google Scholar]
- Cengiz, I.F.; Oliveira, J.M.; Reis, R.L. PRP Therapy. Adv. Exp. Med. Biol. 2018, 1059, 241–253. [Google Scholar] [PubMed]
- Lin, M.Y.; Lin, C.S.; Hu, S.; Chung, W.H. Progress in the Use of Platelet-rich Plasma in Aesthetic and Medical Dermatology. J. Clin. Aesthet. Dermatol. 2020, 13, 28–35. [Google Scholar] [PubMed]
- Tedesco, M.; Garelli, V.; Bellei, B.; Sperduti, I.; Chichierchia, G.; Latini, A.; Foddai, M.L.; Bertozzi, E.; Bonadies, A.; Pallara, T.; et al. Platelet-rich plasma for genital lichen sclerosus: Analysis and results of 94 patients. Are there gender-related differences in symptoms and therapeutic response to PRP? J. Dermatolog. Treat. 2022, 33, 1558–1562. [Google Scholar] [CrossRef] [PubMed]
- Magalon, J.; Bausset, O.; Serratrice, N.; Giraudo, L.; Aboudou, H.; Veran, J.; Magalon, G.; Dignat-Georges, F.; Sabatier, F. Characterization and comparison of 5 platelet-rich plasma preparations in a single-donor model. Arthroscopy 2014, 30, 629–638. [Google Scholar] [CrossRef] [PubMed]
- Cho, J.W.; Kim, S.A.; Lee, K.S. Platelet-rich plasma induces increased expression of G1 cell cycle regulators, type I collagen, and matrix metalloproteinase-1 in human skin fibroblasts. Int. J. Mol. Med. 2012, 29, 32–36. [Google Scholar]
- Modarressi, A. Platlet Rich Plasma (PRP) Improves Fat Grafting Outcomes. World J. Plast. Surg. 2013, 2, 6–13. [Google Scholar] [PubMed]
- Kadry, M.; Tawfik, A.; Abdallah, N.; Badawi, A.; Shokeir, H. Platelet-rich plasma versus combined fractional carbon dioxide laser with platelet-rich plasma in the treatment of vitiligo: A comparative study. Clin. Cosmet. Investig. Dermatol. 2018, 11, 551–559. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, Z.A.; El-Ashmawy, A.A.; El-Tatawy, R.A.; Sallam, F.A. The effect of platelet-rich plasma on the outcome of short-term narrowband-ultraviolet B phototherapy in the treatment of vitiligo: A pilot study. J. Cosmet. Dermatol. 2016, 15, 108–116. [Google Scholar] [CrossRef]
- Abdelghani, R.; Ahmed, N.A.; Darwish, H.M. Combined treatment with fractional carbon dioxide laser, autologous platelet-rich plasma, and narrow band ultraviolet B for vitiligo in different body sites: A prospective, randomized comparative trial. J. Cosmet. Dermatol. 2018, 17, 365–372. [Google Scholar] [CrossRef]
- Parambath, N.; Sharma, V.K.; Parihar, A.S.; Sahni, K.; Gupta, S. Use of platelet-rich plasma to suspend noncultured epidermal cell suspension improves repigmentation after autologous transplantation in stable vitiligo: A double-blind randomized controlled trial. Int. J. Dermatol. 2019, 58, 472–476. [Google Scholar] [CrossRef]
- Chen, J.; Yu, N.; Li, H.; Tang, Y.; Zhu, H. Meta-analysis of the efficacy of adding platelet-rich plasma to 308-nm excimer laser for patients with vitiligo. J. Int. Med. Res. 2022, 50, 3000605221119646. [Google Scholar] [CrossRef] [PubMed]
- Vizoso, F.J.; Eiro, N.; Cid, S.; Schneider, J.; Perez-Fernandez, R. Mesenchymal Stem Cell Secretome: Toward Cell-Free Therapeutic Strategies in Regenerative Medicine. Int. J. Mol. Sci. 2017, 18, 1852. [Google Scholar] [CrossRef] [PubMed]
- Regazzetti, C.; Joly, F.; Marty, C.; Rivier, M.; Mehul, B.; Reiniche, P.; Mounier, C.; Rival, Y.; Piwnica, D.; Cavalié, M.; et al. Transcriptional Analysis of Vitiligo Skin Reveals the Alteration of WNT Pathway: A Promising Target for Repigmenting Vitiligo Patients. J. Investig. Dermatol. 2015, 135, 3105–3114. [Google Scholar] [CrossRef] [PubMed]
- Xu, A.E.; Wei, X.D. Topical melagenine for repigmentation in twenty-two child patients with vitiligo on the scalp. Chin. Med. J. 2004, 117, 199–201. [Google Scholar] [PubMed]
- Mal’tsev, V.I.; Kaliuzhnaia, L.D.; Gubko, L.M. Experience in introducing the method of placental therapy in vitiligo in Ukraine. Lik Sprava 1995, 7–8, 123–125. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).