The Relationship between Subjective Cognitive Decline and Health Literacy in Healthy Community-Dwelling Older Adults
Abstract
1. Introduction
2. Materials and Methods
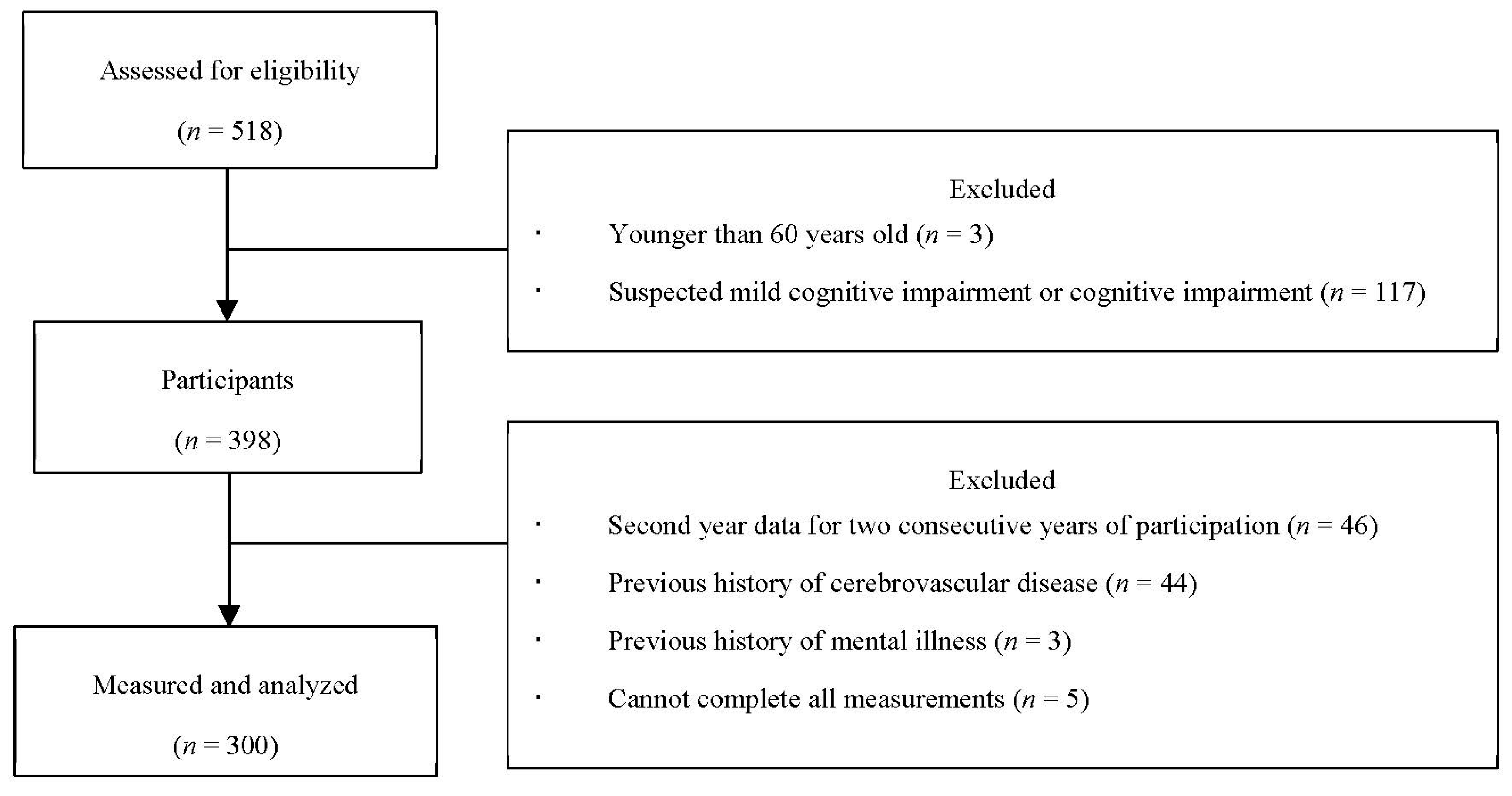
- Older adults aged ≥ 60 years;
- Not suspected to have MCI or cognitive decline, measured via a Mini-Mental State Examination (MMSE) score ≥ 27 [23].
- Participation in this study for two consecutive years;
- History of cerebrovascular disease;
- Past medical history of mental illness;
- Inability to complete all the questionnaires.
3. Results
4. Discussion
- Due to this study’s cross-sectional design, we cannot ascertain the causal direction of the relationships discovered. It is also possible that other factors not examined in this study (e.g., low intelligence, low literacy, lack of sophistication, low cognitive reserve, early brain disease) may mediate these relationships. Future longitudinal research with the addition of other relevant factors is thus needed to clarify the relationship between the changes in each of these included measures and SCD onset.
- Functional aspects were not considered in the health literacy assessment tool used in this study. This topic should be examined using a more multifaceted approach, for example, using instruments that incorporate the functional aspects of health literacy, such as the European Health Literacy Survey Questionnaire [63] or the 14-item Health Literacy Scale for Japanese adults [64].
- We did not explore any associations with lifestyle habits, lifestyle disease morbidity, or genetic factors. Inactive lifestyle and the prevalence of lifestyle diseases may mediate the association between low HL and the development of SCD. Meanwhile, the presence of genetic factors [65] associated with the development of dementia may influence the development of SCD without being associated with low HL. These topics should be explored in future research.
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Prince, M.J.; Wu, F.; Guo, Y.; Gutierrez Robledo, L.M.; O’Donnell, M.; Sullivan, R.; Yusuf, S. The burden of disease in older people and implications for health policy and practice. Lancet 2015, 385, 549–562. [Google Scholar] [CrossRef]
- Dodge, H.H.; Du, Y.; Saxton, J.A.; Ganguli, M. Cognitive domains and trajectories of functional independence in nondemented elderly persons. J. Gerontol. A Biol. Sci. Med. Sci. 2006, 61, 1330–1337. [Google Scholar] [CrossRef] [PubMed]
- Deuschl, G.; Beghi, E.; Fazekas, F.; Varga, T.; Christoforidi, K.A.; Sipido, E.; Bassetti, C.L.; Vos, T.; Feigin, V.L. The burden of neurological diseases in Europe: An analysis for the Global Burden of Disease Study 2017. Lancet Public Health 2020, 5, e551–e567. [Google Scholar] [CrossRef]
- Crous-Bou, M.; Minguillón, C.; Gramunt, N.; Molinuevo, J.L. Alzheimer’s disease prevention: From risk factors to early intervention. Alzheimers Res. Ther. 2017, 9, 71. [Google Scholar] [CrossRef]
- Frankish, H.; Horton, R. Prevention and management of dementia: A priority for public health. Lancet 2017, 390, 2614–2615. [Google Scholar] [CrossRef]
- Petersen, R.C. Clinical practice. Mild cognitive impairment. N. Engl. J. Med. 2011, 364, 2227–2234. [Google Scholar] [CrossRef]
- Jessen, F.; Amariglio, R.E.; van Boxtel, M.; Breteler, M.; Ceccaldi, M.; Chételat, G.; Dubois, B.; Dufouil, C.; Ellis, K.A.; van der Flier, W.M.; et al. A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease. Alzheimers Dement. 2014, 10, 844–852. [Google Scholar] [CrossRef]
- Jessen, F.; Amariglio, R.E.; Buckley, R.F.; van der Flier, W.M.; Han, Y.; Molinuevo, J.L.; Rabin, L.; Rentz, D.M.; Rodriguez-Gomez, O.; Saykin, A.J.; et al. Characterisation of subjective cognitive decline. Lancet Neurol. 2020, 19, 271–278. [Google Scholar] [CrossRef]
- Mitchell, A.J.; Beaumont, H.; Ferguson, D.; Yadegarfar, M.; Stubbs, B. Risk of dementia and mild cognitive impairment in older people with subjective memory complaints: Meta-analysis. Acta Psychiatr. Scand. 2014, 130, 439–451. [Google Scholar] [CrossRef]
- Reisberg, B.; Shulman, M.B.; Torossian, C.; Leng, L.; Zhu, W. Outcome over seven years of healthy adults with and without subjective cognitive impairment. Alzheimers Dement. 2010, 6, 11–24. [Google Scholar] [CrossRef]
- Smart, C.M.; Segalowitz, S.J.; Mulligan, B.P.; Koudys, J.; Gawryluk, J.R. Mindfulness training for older adults with subjective cognitive decline: Results from a pilot randomized controlled trial. J. Alzheimers Dis. 2016, 52, 757–774. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.B.; Chen, Y.L.; Xue, H.P.; Hou, P. Health literacy risk in older adults with and without mild cognitive impairment. Nurs. Res. 2019, 68, 433–438. [Google Scholar] [CrossRef] [PubMed]
- Rostamzadeh, A.; Stapels, J.; Genske, A.; Haidl, T.; Jünger, S.; Seves, M.; Woopen, C.; Jessen, F. Health literacy in individuals at risk for Alzheimer’s dementia: A systematic review. J. Prev. Alzheimers Dis. 2020, 7, 47–55. [Google Scholar] [PubMed]
- Nutbeam, D. Health Promotion Glossary. Health Promot. Int. 1998, 13, 349–364. [Google Scholar] [CrossRef]
- Lee, Y.; Chi, I. Do cognitive leisure activities really matter in the relationship between education and cognition? Evidence from the aging, demographics, and memory study (ADAMS). Aging Ment. Health 2016, 20, 252–261. [Google Scholar] [CrossRef] [PubMed]
- Rovner, B.W.; Casten, R.J.; Leiby, B.E. Determinants of activity levels in African Americans with mild cognitive impairment. Alzheimer Dis. Assoc. Disord. 2016, 30, 41–46. [Google Scholar] [CrossRef]
- Then, F.S.; Luck, T.; Luppa, M.; König, H.H.; Angermeyer, M.C.; Riedel-Heller, S.G. Differential effects of enriched environment at work on cognitive decline in old age. Neurology 2015, 84, 2169–2176. [Google Scholar] [CrossRef]
- Oliveira, D.; Bosco, A.; di Lorito, C. Poor health literacy a risk factor for dementia in older adults? Syst. Lit. Rev. Prospect. Cohort Stud. Matur. 2019, 124, 8–14. [Google Scholar]
- Lovett, R.M.; Curtis, L.M.; Persell, S.D.; Griffith, J.W.; Cobia, D.; Federman, A.; Wolf, M.S. Cognitive impairment without dementia and associations with health literacy, self-management skills, and functional health status. Patient Educ. Couns. 2020, 103, 1805–1811. [Google Scholar] [CrossRef]
- Wilson, R.S.; Yu, L.; James, B.D.; Bennett, D.A.; Boyle, P.A. Association of financial and health literacy with cognitive health in old age. Neuropsychol. Dev. Cogn. B Aging Neuropsychol. Cogn. 2017, 24, 186–197. [Google Scholar] [CrossRef]
- Yu, L.; Wilson, R.S.; Han, S.D.; Leurgans, S.; Bennett, D.A.; Boyle, P.A. Decline in Literacy and Incident AD Dementia Among Community-Dwelling Older Persons. J. Aging Health 2018, 30, 1389–1405. [Google Scholar] [CrossRef] [PubMed]
- Yu, L.; Wilson, R.S.; Schneider, J.A.; Bennett, D.A.; Boyle, P.A. Financial and Health Literacy Predict Incident Alzheimer’s Disease Dementia and Pathology. J. Alzheimers Dis. 2017, 56, 1485–1493. [Google Scholar] [CrossRef] [PubMed]
- Miyata, K.; Yoshikawa, T.; Morikawa, M.; Mine, M.; Okamoto, N.; Kurumatani, N.; Ogata, N. Effect of cataract surgery on cognitive function in elderly: Results of Fujiwara-kyo Eye Study. PLoS ONE 2018, 13, e0192677. [Google Scholar] [CrossRef] [PubMed]
- Hirose, J.; Takehiro, N.; Miki, O.; Nobukazu, O.; Takuya, T.; Kiyoshi, O.; Wakana, T.T.; Hiroaki, K.; Kunio, H.; Koichiro, U.; et al. Validation of each category of the Kihon Checklist for Assessing Physical Functioning, Nutrition and Cognitive Status in a Community-Dwelling Older Japanese Cohort. Epidemiol. Open Access 2017, 7, 326. [Google Scholar]
- Satake, S.; Senda, K.; Hong, Y.J.; Miura, H.; Endo, H.; Sakurai, T.; Kondo, I.; Toba, K. Validity of the Kihon Checklist for assessing frailty status. Geriatr. Gerontol. Int. 2016, 16, 709–715. [Google Scholar] [CrossRef]
- Sampaio, P.; Sampaio, R.A.C.; Yamada, M.; Arai, H. Systematic review of the Kihon Checklist: Is it a reliable assessment of frailty? Kihon Checklist: Systematic review. Geriatr. Gerontol. Int. 2016, 16, 893–902. [Google Scholar] [CrossRef]
- Tomata, Y.; Sugiyama, K.; Kaiho, Y.; Sugawara, Y.; Hozawa, A.; Tsuji, I. Predictive ability of a simple subjective memory complaints scale for incident dementia: Evaluation of Japan’s national checklist, the “Kihon Checklist”. Geriatr. Gerontol. Int. 2017, 17, 1300–1305. [Google Scholar] [CrossRef]
- Nemoto, Y.; Sato, S.; Takahashi, M.; Takeda, N.; Matsushita, M.; Kitabatake, Y.; Maruo, K.; Arao, T. The association of single and combined factors of sedentary behavior and physical activity with subjective cognitive complaints among community-dwelling older adults: A cross-sectional study. PLoS ONE 2018, 13, e0195384. [Google Scholar] [CrossRef]
- Okura, M.; Ogita, M.; Arai, H. Self-Reported Cognitive Frailty Predicts Adverse Health Outcomes for Community-Dwelling Older Adults based on an analysis of sex and age. J. Nutr. Health Aging 2019, 23, 654–664. [Google Scholar] [CrossRef]
- Ishikawa, H.; Nomura, K.; Sato, M.; Yano, E. Developing a measure of communicative and critical health literacy: A pilot study of Japanese office workers. Health Promot. Int. 2008, 23, 269–274. [Google Scholar] [CrossRef]
- Folstein, M.F.; Folstein, S.E.; McHugh, P.R. “Mini-mental state” A practical method for grading the cognitive state of patients for clinicians. J. Psychiatr. Res. 1975, 12, 189–198. [Google Scholar] [CrossRef]
- Ideno, Y.; Takayama, M.; Hayashi, K.; Takagi, H.; Sugai, Y. Evaluation of a Japanese version of the Mini-Mental State Examination in elderly persons. Geriatr. Gerontol. Int. 2012, 12, 310–316. [Google Scholar] [CrossRef] [PubMed]
- Sugishita, M.; Hemmi, I.; Takeuchi, T. Reexamination of the validity and reliability of the Japanese version of the Mini-Mental State Examination (MMSE-J). Jpn. J. Cogn. Neurosci. 2016, 18, 168–183. [Google Scholar]
- Hoyl, M.T.; Alessi, C.A.; Harker, J.O.; Josephson, K.R.; Pietruszka, F.M.; Koelfgen, M.; Mervis, J.R.; Fitten, L.J.; Rubenstein, L.Z. Development and testing of a five-item version of the Geriatric Depression Scale. J. Am. Geriatr. Soc. 1999, 47, 873–878. [Google Scholar] [CrossRef] [PubMed]
- Wada, Y.; Murata, C.; Hirai, H.; Kondo, N.; Kondo, K.; Ueda, K.; Ichida, N. Predictive validity of GDS5 using AGES project data. Kousei no Shihyou 2014, 61, 7–12. (In Japanese) [Google Scholar]
- Okura, M.; Ogita, M.; Yamamoto, M.; Nakai, T.; Numata, T.; Arai, H. The relationship of community activities with cognitive impairment and depressive mood is independent of mobility disorder in Japanese older adults. Arch. Gerontol. Geriatr. 2017, 70, 54–61. [Google Scholar] [CrossRef]
- Goda, A.; Murata, S.; Nakano, H.; Shiraiwa, K.; Abiko, T.; Nonaka, K.; Iwase, H.; Anami, K.; Horie, J. Subjective and Objective Mental and Physical Functions Affect Subjective Cognitive Decline in Community-Dwelling Elderly Japanese People. Healthcare (Basel) 2020, 8, 347. [Google Scholar] [CrossRef]
- Tomata, Y.; Sugiyama, K.; Kaiho, Y.; Honkura, K.; Watanabe, T.; Zhang, S.; Sugawara, Y.; Tsuji, I. Green tea consumption and the risk of incident dementia in elderly Japanese: The Ohsaki Cohort 2006 Study. Am. J. Geriatr. Psychiatry 2016, 24, 881–889. [Google Scholar] [CrossRef]
- Fukutomi, E.; Okumiya, K.; Wada, T.; Sakamoto, R.; Ishimoto, Y.; Kimura, Y.; Chen, W.L.; Imai, H.; Kasahara, Y.; Fujisawa, M.; et al. Relationships between each category of 25-item frailty risk assessment (Kihon Checklist) and newly certified older adults under long-term care insurance: A 24-month follow-up study in a rural community in Japan. Geriatr. Gerontol. Int. 2015, 15, 864–871. [Google Scholar] [CrossRef]
- Clarnette, R.M.; Almeida, O.P.; Forstl, H.; Paton, A.; Martins, R.N. Clinical characteristics of individuals with subjective memory loss in Western Australia: Results from a cross-sectional survey. Int. J. Geriatr. Psychiatry 2001, 16, 168–174. [Google Scholar] [CrossRef]
- Montejo, P.; Montenegro, M.; Fernandez, M.A.; Maestu, F. Subjective memory complaints in the elderly: Prevalence and influence of temporal orientation, depression, and quality of life in a population-based study in the city of Madrid. Aging Ment. Health 2011, 15, 85–96. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Benavides, G.; Grau-Rivera, O.; Cacciaglia, R.; Suárez-Calvet, M.; Falcon, C.; Minguillon, C.; Gramunt, N.; Sala-Vila, A.; Gispert, J.D.; Molinuevo, J.L. Distinct Cognitive and Brain Morphological Features in Healthy Subjects Unaware of Informant-Reported Cognitive Decline. J. Alzheimers Dis. 2018, 65, 181–191. [Google Scholar] [CrossRef] [PubMed]
- Wei, Y.C.; Huang, L.Y.; Chen, C.K.; Lin, C.; Shyu, Y.C.; Chen, Y.L.; Huang, W.Y.; Lin, C.P. Subjective Cognitive Decline in the Community Is Affected at Multiple Aspects of Mental Health and Life Quality: A Cross-Sectional Study of the Community Medicine of Keelung Chang Gung Memorial Hospital. Dement. Geriatr. Cogn. Dis. Extra 2019, 9, 152–162. [Google Scholar] [CrossRef] [PubMed]
- Aaby, A.; Friis, K.; Christensen, B.; Rowlands, G.; Maindal, H.T. Health literacy is associated with health behavior and self-reported health: A large population-based study in individuals with cardiovascular disease. Eur. J. Prev. Cardiol. 2017, 24, 1880–1888. [Google Scholar] [CrossRef] [PubMed]
- Svendsen, M.T.; Bak, C.K.; Sørensen, K.; Pelikan, J.; Riddersholm, S.J.; Skals, R.K.; Mortensen, R.N.; Maindal, H.T.; Bøggild, H.; Nielsen, G.; et al. Associations of health literacy with socioeconomic position, health risk behavior, and health status: A large national population-based survey among Danish adults. BMC Public Health 2020, 20, 565. [Google Scholar] [CrossRef]
- Shi, D.; Li, J.; Wang, Y.; Wang, S.; Liu, K.; Shi, R.; Zhang, Q.; Chen, X. Association between health literacy and hypertension management in a Chinese community: A retrospective cohort study. Intern. Emerg. Med. 2017, 12, 765–776. [Google Scholar] [CrossRef]
- Ishikawa, H.; Takeuchi, T.; Yano, E. Measuring Functional, Communicative, and Critical Health Literacy among Diabetic Patients. Diabetes Care 2008, 31, 874. [Google Scholar] [CrossRef]
- Luo, H.; Chen, Z.; Bell, R.; Rafferty, A.P.; Gaskins, N.R.; Winterbauer, N. Health Literacy and Health Behaviors Among Adults with Prediabetes, 2016 Behavioral Risk Factor Surveillance System. Public Health Rep. 2020, 135, 492–500. [Google Scholar] [CrossRef]
- Fabbri, M.; Yost, K.; Finney Rutten, L.J.; Manemann, S.M.; Boyd, C.M.; Jensen, D.; Weston, S.A.; Jiang, R.; Roger, V.L. Health literacy and outcomes in patients with heart failure: A prospective community study. Mayo Clin. Proc. 2018, 93, 9–15. [Google Scholar] [CrossRef]
- Hawkins, M.A.W.; Dolansky, M.A.; Levin, J.B.; Schaefer, J.T.; Gunstad, J.; Redle, J.D.; Josephson, R.; Hughes, J.W. Cognitive function and health literacy are independently associated with HF knowledge. Heart Lung J. Crit. Care 2016, 45, 386–391. [Google Scholar] [CrossRef]
- Yokokawa, H.; Fukuda, H.; Yuasa, M.; Sanada, H.; Hisaoka, T.; Naito, T. Association between health literacy and metabolic syndrome or healthy lifestyle characteristics among community-dwelling Japanese people. Diabetol. Metab. Syndr. 2016, 8, 30. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Wu, Y.; Zhang, D.; Nie, J. Associations between heart failure and risk of dementia: A PRISMA-compliant meta-analysis. Medicine (Baltimore) 2020, 99, e18492. [Google Scholar] [CrossRef] [PubMed]
- Livingston, G.; Sommerlad, A.; Orgeta, V.; Costafreda, S.G.; Huntley, J.; Ames, D.; Ballard, C.; Banerjee, S.; Burns, A.; Cohen-Mansfield, J.; et al. Dementia Prevention, Intervention, and Care. Lancet 2017, 390, 2673–2734. [Google Scholar] [CrossRef]
- Taylor, C.; Bouldin, E.; McGuire, L. Subjective Cognitive Decline among Adults Aged ≥45 Years—United States, 2015–2016. MMWR 2018, 67, 753–757. [Google Scholar] [CrossRef] [PubMed]
- Villemagne, V.L.; Rowe, C.C. Amyloid imaging. Int. Psychogeriatr. 2011, 23 (Suppl. 2), S41–S49. [Google Scholar] [CrossRef] [PubMed]
- Crary, J.F.; Trojanowski, J.Q.; Schneider, J.A.; Abisambra, J.F.; Abner, E.L.; Alafuzoff, I.; Arnold, S.E.; Attems, J.; Beach, T.G.; Bigio, E.H.; et al. Primary age-related tauopathy (PART): A common pathology associated with human aging. Acta Neuropathol. 2014, 128, 755–766. [Google Scholar] [CrossRef]
- López-Sanz, D.; Bruña, R.; Garcés, P.; Martín-Buro, M.C.; Walter, S.; Delgado, M.L.; Montenegro, M.; López Higes, R.; Marcos, A.; Maestú, F. Functional connectivity disruption in subjective cognitive decline and mild cognitive impairment: A common pattern of alterations. Front Aging Neurosci. 2017, 9, 109. [Google Scholar] [CrossRef]
- Comijs, H.C.; Deeg, D.J.; Dik, M.G.; Twisk, J.W.; Jonker, C. Memory complaints; the association with psycho-affective and health problems and the role of personality characteristics. A 6-year follow-up study. J. Affect Disord. 2002, 72, 157–165. [Google Scholar] [CrossRef]
- Montejo Carrasco, P.; Montenegro-Peña, M.; López-Higes, R.; Estrada, E.; Prada Crespo, D.; Montejo Rubio, C.; García Azorín, D. Subjective memory complaints in healthy older adults: Fewer complaints associated with depression and perceived health, more complaints are associated with lower memory performance. Arch. Gerontol. Geriatr. 2017, 70, 28–37. [Google Scholar] [CrossRef]
- Turvey, C.L.; Schultz, S.; Arndt, S.; Wallace, R.B.; Herzog, R. Memory complaint in a community sample aged 70 and older. J. Am. Geriatr. Soc. 2000, 48, 1435–1441. [Google Scholar] [CrossRef]
- Watson, D. Intraindividual and interindividual analyses of positive and negative affect: Their relation to health complaints, perceived stress, and daily activities. J. Pers. Soc. Psychol. 1988, 54, 1020–1030. [Google Scholar] [CrossRef] [PubMed]
- Dux, M.C.; Woodard, J.L.; Calamari, J.E.; Messina, M.; Arora, S.; Chik, H.; Pontarelli, N. The moderating role of negative affect on objective verbal memory performance and subjective memory complaints in healthy older adults. J. Int. Neuropsychol. Soc. 2008, 14, 327–336. [Google Scholar] [CrossRef] [PubMed]
- Sørensen, K.; Van den Broucke, S.; Pelikan, J.M.; Fullam, J.; Doyle, G.; Slonska, Z.; Kondilis, B.; Stoffels, V.; Osborne, R.H.; Brand, H. Measuring health literacy in populations: Illuminating the design and development process of the European Health Literacy Survey Questionnaire (HLS-EU-Q). BMC Public Health 2013, 13, 948. [Google Scholar] [CrossRef] [PubMed]
- Suka, M.; Odajima, T.; Kasai, M.; Igarashi, A.; Ishikawa, H.; Kusama, M.; Nakayama, T.; Sumitani, M.; Sugimori, H. The 14-item Health Literacy Scale for Japanese adults (HLS-14) Environ. Health Prev. Med. 2013, 18, 407–415. [Google Scholar] [CrossRef] [PubMed]
- Loy, C.T.; Schofield, P.R.; Turner, A.M.; Kwok, J.B. Genetics of dementia. Lancet 2014, 383, 828–840. [Google Scholar] [CrossRef]
| Variable | Number of Participants/Frequencies |
|---|---|
| KCL-CF score (0/1/2/3; n) | 194/82/24/0 |
| Frequency of subjective memory item endorsement | |
| Do your family or your friends point out your memory loss? | 17.7% |
| Do you make a call by looking up phone numbers? | 0.0% |
| Do you find yourself not knowing today’s date? | 25.7% |
| Variable | Total (n = 300) | SCD (n = 106) | Non-SCD (n = 194) | Effect Size (r, V) | p | |
|---|---|---|---|---|---|---|
| Sex: Male/Female (n) | 48/252 | 15/91 | 33/161 | 0.04 | 0.52 | a |
| Age (yr) | 73.3 ± 5.8 | 75.0 ± 5.8 | 72.4 ± 5.5 | 0.22 | <0.01 | |
| BMI (kg/m2) | 22.5 ± 3.0 | 22.6 ± 3.1 | 22.4 ± 2.9 | 0.03 | 0.57 | |
| Educational history (yr) | 12.0 ± 2.3 | 11.7 ± 2.2 | 12.2 ± 2.4 | 0.10 | 0.08 | |
| CCHL (score) | 4.0 ± 0.5 | 3.8 ± 0.4 | 4.0 ± 0.5 | 0.19 | <0.01 | b |
| MMSE (score) | 28.9 ± 1.1 | 28.7 ± 1.1 | 29.0 ± 1.1 | 0.17 | <0.01 | b |
| GDS-5 (score) | 0.9 ± 1.0 | 1.2 ± 1.1 | 0.7 ± 0.8 | 0.21 | <0.01 | b |
| Variable | B | S.E. | Wald | p | Exp (B) | 95% CI for Exp (B) | |
|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||
| Sex: Female | 1.00 | ||||||
| Sex: Male | −0.32 | 0.38 | 0.71 | 0.40 | 0.72 | 0.34 | 1.54 |
| Age (yr) | 0.08 | 0.02 | 9.96 | <0.01 | 1.08 | 1.03 | 1.14 |
| BMI (kg/m2) | 0.02 | 0.04 | 0.26 | 0.61 | 1.02 | 0.94 | 1.11 |
| Educational history (yr) | 0.00 | 0.06 | 0.00 | 0.98 | 1.00 | 0.89 | 1.13 |
| CCHL (score) | −0.65 | 0.31 | 4.42 | 0.04 | 0.52 | 0.28 | 0.96 |
| MMSE (score) | −0.18 | 0.12 | 2.29 | 0.13 | 0.84 | 0.67 | 1.05 |
| GDS-5 (score) | 0.40 | 0.14 | 8.16 | <0.01 | 1.49 | 1.13 | 1.96 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Goda, A.; Murata, S.; Nakano, H.; Nonaka, K.; Iwase, H.; Shiraiwa, K.; Abiko, T.; Anami, K.; Horie, J. The Relationship between Subjective Cognitive Decline and Health Literacy in Healthy Community-Dwelling Older Adults. Healthcare 2020, 8, 567. https://doi.org/10.3390/healthcare8040567
Goda A, Murata S, Nakano H, Nonaka K, Iwase H, Shiraiwa K, Abiko T, Anami K, Horie J. The Relationship between Subjective Cognitive Decline and Health Literacy in Healthy Community-Dwelling Older Adults. Healthcare. 2020; 8(4):567. https://doi.org/10.3390/healthcare8040567
Chicago/Turabian StyleGoda, Akio, Shin Murata, Hideki Nakano, Koji Nonaka, Hiroaki Iwase, Kayoko Shiraiwa, Teppei Abiko, Kunihiko Anami, and Jun Horie. 2020. "The Relationship between Subjective Cognitive Decline and Health Literacy in Healthy Community-Dwelling Older Adults" Healthcare 8, no. 4: 567. https://doi.org/10.3390/healthcare8040567
APA StyleGoda, A., Murata, S., Nakano, H., Nonaka, K., Iwase, H., Shiraiwa, K., Abiko, T., Anami, K., & Horie, J. (2020). The Relationship between Subjective Cognitive Decline and Health Literacy in Healthy Community-Dwelling Older Adults. Healthcare, 8(4), 567. https://doi.org/10.3390/healthcare8040567





