Signs in People with Intellectual Disabilities: Interviews with Managers and Staff on the Identification Process of Dementia
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Setting
2.2. Sampling and Participants
2.2.1. The Selection of Managers
2.2.2. The Selection of Staff
2.3. Data Collection
2.4. Analysis
2.5. Ethics Approval and Consent to Participate
3. Results
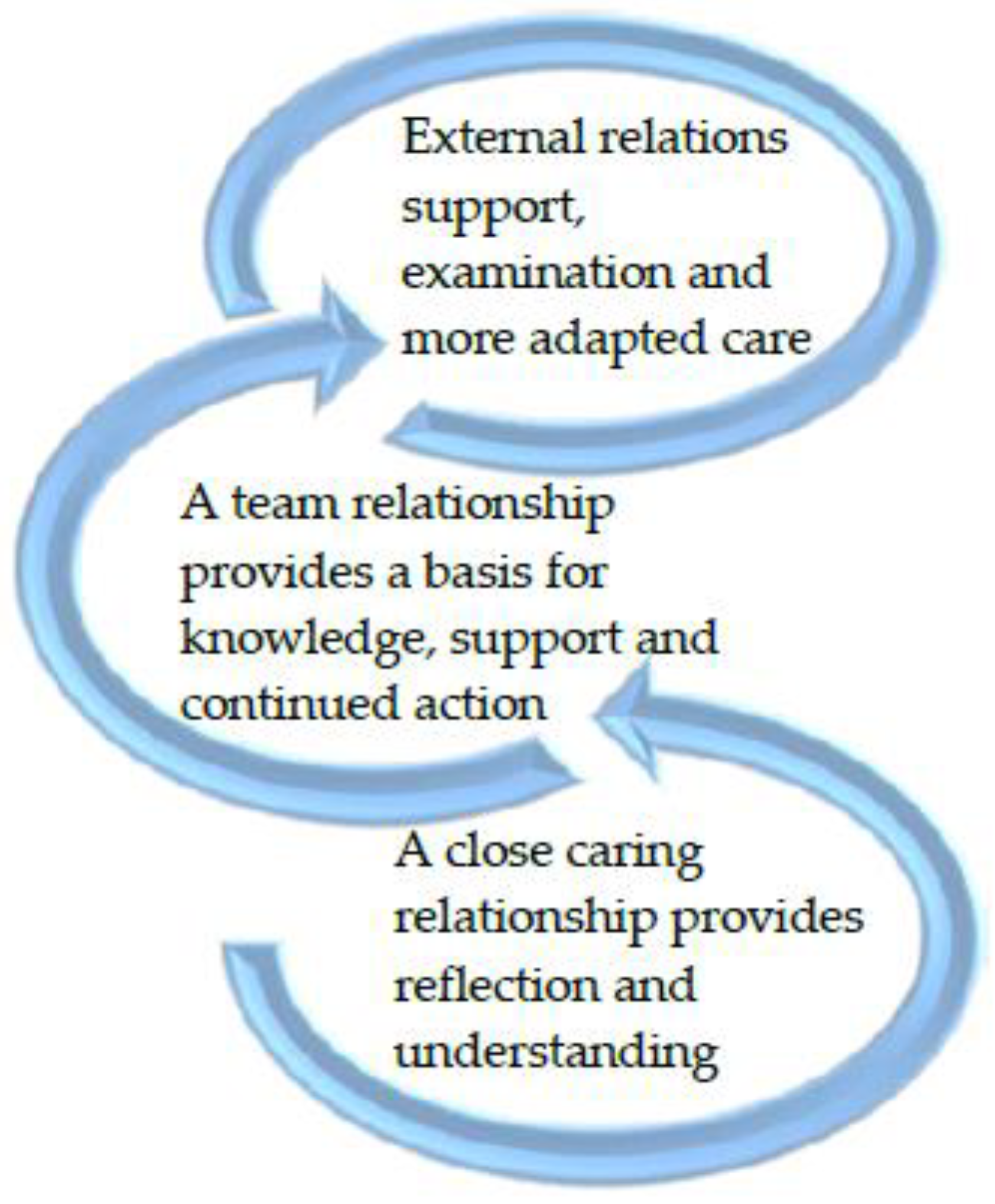
3.1. A Close Caring Relationship Provides Reflection and Understanding
“I can’t say how many years ago it was. His behavior just changed completely and we didn’t understand a thing. He’d been the nicest man in the world and then he just changed completely.”(Member of staff, group home, female)
“A person’s memory gets worse. But if you know what it’s been like over time, you can see that there’s a new situation.”(Member of staff, daily activity center, female)
“There are two whose behavior indicates dementia, though not quite in the same way. The fact that they don’t talk makes things a bit more difficult, of course. But you do notice changes in behavior especially in the case of one of them. For instance, you’ll suddenly find him standing in the shower at four in the afternoon, which hasn’t happened before. He has a shower in the morning and he’s always been careful to keep to that routine.”(Member of staff, group home, female)
“But you have the same problem with people with dementia who don’t talk. A person can hit themselves and it can be a sign that they’re in pain. And I think, I really do think, that we all need to know what happens when we get older.”(Member of staff, group home, female)
3.2. A Team Relationship Provides a Basis for Knowledge, Support, and Continued Action
“You’ve got to take the situation as it comes, so to speak. And then, of course, we talk a lot about it in the staff group, so that everybody’s alert to the fact that something’s happened with regard to the person. As when one person went around picking up this, that and the other—collecting little things. She hadn’t done that before.”(Member of staff, daily activity centre, female)
“Well, what made the staff start to suspect dementia was that the person became confused and couldn’t find the way home and …”(Manager, group home, male)
“I mean, it’s where they live, and if they feel a sense of security there, you mustn’t make them move just because they’re older and you can’t make somebody move because they suffer from dementia.”(Member of staff, daily activity center, female)
“Is it dementia that should determine where he’s going to live or is it quality of life? It’s maybe more important that he’s here where he knows the staff and his neighbors and the environment and the area. Yes, that’s maybe more important.”(Member of staff, group home, female)
“I don’t think the person would have been better off in an ordinary home for people with dementia. On the other hand, the staff at the group home do need greater competence concerning dementia.”(Manager, group home, female)
3.3. External Relations Support Examination and More Adapted Care
“In connection with a person being diagnosed as having Alzheimer’s, this wonderful nurse came here one morning and talked to us all. Very committed. She’s attached to the primary healthcare center where the person with Alzheimer’s is registered. She’s fantastic and so is the doctor.”(Member of staff, daily activity center, female)
“It felt as if nothing we did was right, but then the dementia nurse was an enormous help, simply by being able to put it into words and showing it was normal. She said there was nothing more we could do.”(Manager, daily activity center, male)
“Our nurses from this part of town were brought in and her own general practitioner made regular calls towards the end. We worked together in the palliative care when the person was dying. This gave me a firm sense of security.”(Member of staff, group home, male)
“When we furnish a flat in co-operation with the person, what do we have to think about? No dark mats on a light-coloured floor, for instance… You don’t want to feel as if you’re falling into a hole! And the curtains mustn’t be made of a material that reflects the light … You don’t want a situation where the person can’t really see whether there’s someone standing outside the window or not, or where, when it’s dark, the artificial light is reflected. These are things you don’t think about until they’re pointed out to you.”(Member of staff, group home, female)
“What can you ask of them and how important is it? It differs from one person to another. The staff must always adjust to the person’s individual needs; find what aid or appliance the person requires at the particular time.”(Manager, group home, female)
“Of course, the person needs to be accompanied by a member of staff that works closely with them. If the person goes unaccompanied to a healthcare center, the examination can be just who knows what because the dementia isn’t visible. All you see is the intellectual impairment. It needs to be made clear how the person functioned until a year ago before we started thinking that something was not as it should be.”(Manager, daily activity center, female)
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Towards a Dementia Plan: A Who Guide; World Health Organization: Geneva, Switzerland, 2018; pp. 6–8. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- Schalock, R.L.; Borthwick-Duffy, S.A.; Bradley, V.J.; Buntinx, W.H.E.; Coulter, D.L.; Craig, E.M.; Gomez, S.C.; Lachapelle, Y.; Luckasson, R.; Reeve, A.; et al. Intellectual Disability: Definition, Classification, and Systems of Supports, 11th ed.; American Association on Intellectual and Developmental Disabilities: Washington, DC, USA, 2010. [Google Scholar]
- McCarron, M.; McCallion, P.; Reilly, E.; Dunne, P.; Carroll, R.; Mulryan, N. A prospective 20-year longitudinal follow-up of dementia in persons with down syndrome. J. Intellect. Disabil. Res. 2017, 61, 843–852. [Google Scholar] [CrossRef] [PubMed]
- Strydom, A.; Chan, T.; King, M.; Hassiotis, A.; Livingston, G. Incidence of dementia in older adults with intellectual disabilities. Res. Dev. Disabil. 2013, 34, 1881–1885. [Google Scholar] [CrossRef] [PubMed]
- Kelly, C.; O’Donohoe, A. Hrb Statistics Series 24 Annual Report of the National Intellectual Disability Database Committee 2013; Health Research Board: Dublin, Ireland, 2014. [Google Scholar]
- Nagdee, M. Dementia in intellectual disability: A review of diagnostic challenges. Afr. J. Psychiatry 2011, 14, 194–199. [Google Scholar] [CrossRef]
- Strydom, A.; Al-Janabi, T.; Houston, M.; Ridley, J. Best practice in caring for adults with dementia and learning disabilities. Nurs. Stand. 2016, 31, 42–51. [Google Scholar] [CrossRef] [PubMed]
- Sheehan, R.; Ali, A.; Hassiotis, A. Dementia in intellectual disability. Curr. Opin. Psychiatry 2014, 27, 143–148. [Google Scholar] [CrossRef] [PubMed]
- McCarron, M.; McCallion, P.; Coppus, A.; Fortea, J.; Stemp, S.; Janicki, M.; Wtachman, K. Supporting advanced dementia in people with down syndrome and other intellectual disability: Consensus statement of the international summit on intellectual disability and dementia. J. Intellect. Disabil. Res. 2018, 62, 617–624. [Google Scholar] [CrossRef] [PubMed]
- McKenzie, K.; Metcalfe, D.; Murray, G. A review of measures used in the screening, assessment and diagnosis of dementia in people with an intellectual disability. J. Appl. Res. Intellect. Disabil. 2018, 31, 725–742. [Google Scholar] [CrossRef] [PubMed]
- Elliott-King, J.; Shaw, S.; Bandelow, S.; Devshi, R.; Kassam, S.; Hogervorst, E. A critical literature review of the effectiveness of various instruments in the diagnosis of dementia in adults with intellectual disabilities. Alzheimer’s Dement Diagn. Assess. Dis. Monit. 2016, 4, 126–148. [Google Scholar] [CrossRef] [PubMed]
- Froggatt, K.; Payne, S.; Morbey, H.; Edwards, M.; Finne-Soveri, H.; Gambassi, G.; Pasman, H.R.; Szczerbinska, K.; Van den Block, L. Palliative care development in european care homes and nursing homes: Application of a typology of implementation. J. Am. Med. Dir. Assoc. 2017, 18, 550.e7–550.e14. [Google Scholar] [CrossRef] [PubMed]
- Zeilinger, E.L.; Stiehl, K.A.; Weber, G. A systematic review on assessment instruments for dementia in persons with intellectual disabilities. Res. Dev. Disabil. 2013, 34, 3962–3977. [Google Scholar] [CrossRef] [PubMed]
- The National Board of Health and Welfare. Swedish Disability Policy—Service and Care for People with Functional Impairments; Measures under the Act Concerning Support and Service for Persons with Certain Functional Impairments; The National Board of Health and Welfare: Stockholm, Sweden, 2009; pp. 126–188.
- The British Psychological Society; Royal College of Psychiatrists; Division of Clinical Psychology. Dementia and People with Intellectual Disabilities: Guidance on the Assessment, Diagnosis, Interventions and Support of People with Intellectual Disabilities Who Develop Dementia; The British Psychological Society: Leicester, UK, 2015. [Google Scholar]
- Moran, J.A.; Rafii, M.S.; Keller, S.M.; Singh, B.K.; Janicki, M.P. The national task group on intellectual disabilities and dementia practices consensus recommendations for the evaluation and management of dementia in adults with intellectual disabilities. Mayo Clin. Proc. 2013, 88, 831–840. [Google Scholar] [CrossRef] [PubMed]
- Cleary, J.; Doody, O. Nurses’ experience of caring for people with intellectual disability and dementia. J. Clin. Nurs. 2017, 26, 620–631. [Google Scholar] [CrossRef] [PubMed]
- Cleary, J.; Doody, O. Professional carers’ experiences of caring for individuals with intellectual disability and dementia. J. Intellect. Disabil. 2017, 21, 68–86. [Google Scholar] [CrossRef] [PubMed]
- Clement, T.; Bigby, C. Competencies of front-line managers in supported accommodation: Issues for practice and future research. J. Intellect. Dev. Disabil. 2012, 37, 131–140. [Google Scholar] [CrossRef] [PubMed]
- Beadle-Brown, J.; Mansell, J.; Ashman, B.; Ockenden, J.; Iles, R.; Whelton, B. Practice leadership and active support in residential services for people with intellectual disabilities: An exploratory study. J. Intellect. Disabil. Res. 2014, 58, 838–850. [Google Scholar] [CrossRef] [PubMed]
- Swedish Parliament. Act Concerning Support and Service for Persons with Certain Functional Impairments; Independent Living Institute: Stockholm, Sweden, 1993. [Google Scholar]
- The United Nations. Convention on the Rights of Persons with Disabilities (CRPD). 2006. Available online: http://www.un.org/disabilities/documents/convention/convoptprot-e.pdf (accessed on 4 August 2018).
- Wiles, J.L.; Leibing, A.; Guberman, N.; Reeve, J.; Allen, R.E.S. The meaning of “aging in place” to older people. Gerontologist 2012, 52, 357–366. [Google Scholar] [CrossRef] [PubMed]
- Elo, S.; Kyngas, H. The qualitative content analysis process. J. Adv. Nurs. 2008, 62, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Vaismoradi, M.; Turunen, H.; Bondas, T. Content analysis and thematic analysis: Implications for conducting a qualitative descriptive study. Nurs. Health Sci. 2013, 15, 398–405. [Google Scholar] [CrossRef] [PubMed]
- Northway, R.; Holland-Hart, D.; Jenkins, R. Meeting the health needs of older people with intellectual disabilities: Exploring the experiences of residential social care staff. Health Soc. Care Community 2017, 25, 923–931. [Google Scholar] [CrossRef] [PubMed]
- Llewellyn, P. The needs of people with learning disabilities who develop dementia: A literature review. Dementia 2011, 10, 235–247. [Google Scholar] [CrossRef]
- Robinson, L.; Dickinson, C.; Magklara, E.; Newton, L.; Prato, L.; Bamford, C. Proactive approaches to identifying dementia and dementia risk: A qualitative study of public attitudes and preferences. BMJ Open 2018, 8, e018677. [Google Scholar] [CrossRef] [PubMed]
- Janicki, M.P. Quality outcomes in group home dementia care for adults with intellectual disabilities. J. Intellect. Disabil. Res. 2011, 55, 763–776. [Google Scholar] [CrossRef] [PubMed]
- McCarron, M.; Reilly, E. Supporting Persons with Intellectual Disability and Dementia: Quality Dementia Care Standards. A Guide to Practice; Daughters of Charity Service: San Antonio, TX, USA, 2010. [Google Scholar]
- Costello, H.; Bouras, N.; Davis, H. The role of training in improving community care staff awareness of mental health problems in people with intellectual disabilities. J. Appl. Res. Intellect. Disabil. 2007, 20, 228–235. [Google Scholar] [CrossRef]
- Tsiantis, J.; Diareme, S.; Dimitrakaki, C.; Kolaitis, G.; Flios, A.; Christogiorgos, S.; Weber, G.; Salvador-Carulla, L.; Hillery, J.; Costello, H. Care staff awareness training on mental health needs of adults with learning disabilities: Results from a greek sample. J. Learn. Disabili. 2004, 8, 221–234. [Google Scholar] [CrossRef]
- Van Knippenberg, R.J.M.; De Vugt, M.E.; Ponds, R.W.; Myin-Germeys, I.; Van Twillert, B.; Verhey, F.R.J. Dealing with daily challenges in dementia (deal-id study): An experience sampling study to assess caregiver functioning in the flow of daily life. Int. J. Geriatr. Psychiatry 2017, 32, 949–958. [Google Scholar] [CrossRef] [PubMed]
- Barbosa, A.; Lord, K.; Blighe, A.; Mountain, G. Dementia care mapping in long-term care settings: A systematic review of the evidence. Int. Psychogeriatr. 2017, 29, 1609–1618. [Google Scholar] [CrossRef] [PubMed]
- Kitwood, T.; Bredin, K. Towards a theory of dementia care: Personhood and well-being. Ageing Soc. 1992, 12, 269–287. [Google Scholar] [CrossRef] [PubMed]
- Schaap, F.D.; Dijkstra, G.J.; Finnema, E.J.; Reijneveld, S.A. The first use of dementia care mapping in the care for older people with intellectual disability: A process analysis according to the re-aim framework. Aging Ment. Health 2017. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, H.; Kerr, D.; Cunningham, C. Equipping staff to support people with an intellectual disability and dementia in care home settings. Dementia 2005, 4, 387–400. [Google Scholar] [CrossRef]
- Sandberg, M.; Ahlstrom, G.; Kristensson, J. Patterns of somatic diagnoses in older people with intellectual disability: A swedish eleven year case-control study of inpatient data. J. Appl. Res. Intellect. Disabil. 2017, 30, 157–171. [Google Scholar] [CrossRef] [PubMed]
- Axmon, A.; Bjorne, P.; Nylander, L.; Ahlstrom, G. Psychiatric diagnoses in older people with intellectual disability in comparison with the general population: A register study. Epidemiol. Psychiatr. Sci. 2017. [Google Scholar] [CrossRef] [PubMed]
- McCarron, M.; McCallion, P.; Reilly, E.; Mulryan, N. A prospective 14-year longitudinal follow-up of dementia in persons with down syndrome. J. Intellect. Disabil. Res. 2014, 58, 61–70. [Google Scholar] [CrossRef] [PubMed]
- Axmon, A.; Kristensson, J.; Ahlstrom, G.; Midlov, P. Use of antipsychotics, benzodiazepine derivatives, and dementia medication among older people with intellectual disability and/or autism spectrum disorder and dementia. Res. Dev. Disabil. 2017, 62, 50–57. [Google Scholar] [CrossRef] [PubMed]
- Axmon, A.; Sandberg, M.; Ahlstrom, G.; Midlov, P. Prescription of potentially inappropriate medications among older people with intellectual disability: A register study. BMC Pharmacol. Toxicol. 2017, 18, 68. [Google Scholar] [CrossRef] [PubMed]
- WHO. Global Health Ethics; Key Issues; Global Network of Who Collaborating Centres for Bioethics. Available online: http://apps.who.int/iris/bitstream/handle/10665/164576/9789240694033_eng.pdf;jsessionid=4835FE3B07E6988565CE7C3FAE67E83C?sequence=1 (accessed on 14 July 2018).
| Level: Themes | Actors and Patterns of Core Content |
|---|---|
| First level: A close caring relationship provides reflection and understanding | Actors in this part of the caring process consist of the person with an ID and staff. |
| |
| |
| |
| Second level: A team relationship provides a basis for knowledge, support and continued action | Actors in this second part of the caring process consist of staff and managers in their own workplace. |
| |
| |
| |
| Third level: External relations support examination and more adapted care | Actors on this third level consist of, beside the staff and managers in the ID-service, external staff from other municipal units, primary health care, and specialist care. |
| |
| |
|
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Holst, G.; Johansson, M.; Ahlström, G. Signs in People with Intellectual Disabilities: Interviews with Managers and Staff on the Identification Process of Dementia. Healthcare 2018, 6, 103. https://doi.org/10.3390/healthcare6030103
Holst G, Johansson M, Ahlström G. Signs in People with Intellectual Disabilities: Interviews with Managers and Staff on the Identification Process of Dementia. Healthcare. 2018; 6(3):103. https://doi.org/10.3390/healthcare6030103
Chicago/Turabian StyleHolst, Göran, Maria Johansson, and Gerd Ahlström. 2018. "Signs in People with Intellectual Disabilities: Interviews with Managers and Staff on the Identification Process of Dementia" Healthcare 6, no. 3: 103. https://doi.org/10.3390/healthcare6030103
APA StyleHolst, G., Johansson, M., & Ahlström, G. (2018). Signs in People with Intellectual Disabilities: Interviews with Managers and Staff on the Identification Process of Dementia. Healthcare, 6(3), 103. https://doi.org/10.3390/healthcare6030103






