PTSD in U.S. Veterans: The Role of Social Connectedness, Combat Experience and Discharge
Abstract
:1. Introduction
2. Materials and Methods
2.1. Measures
2.2. Analyses
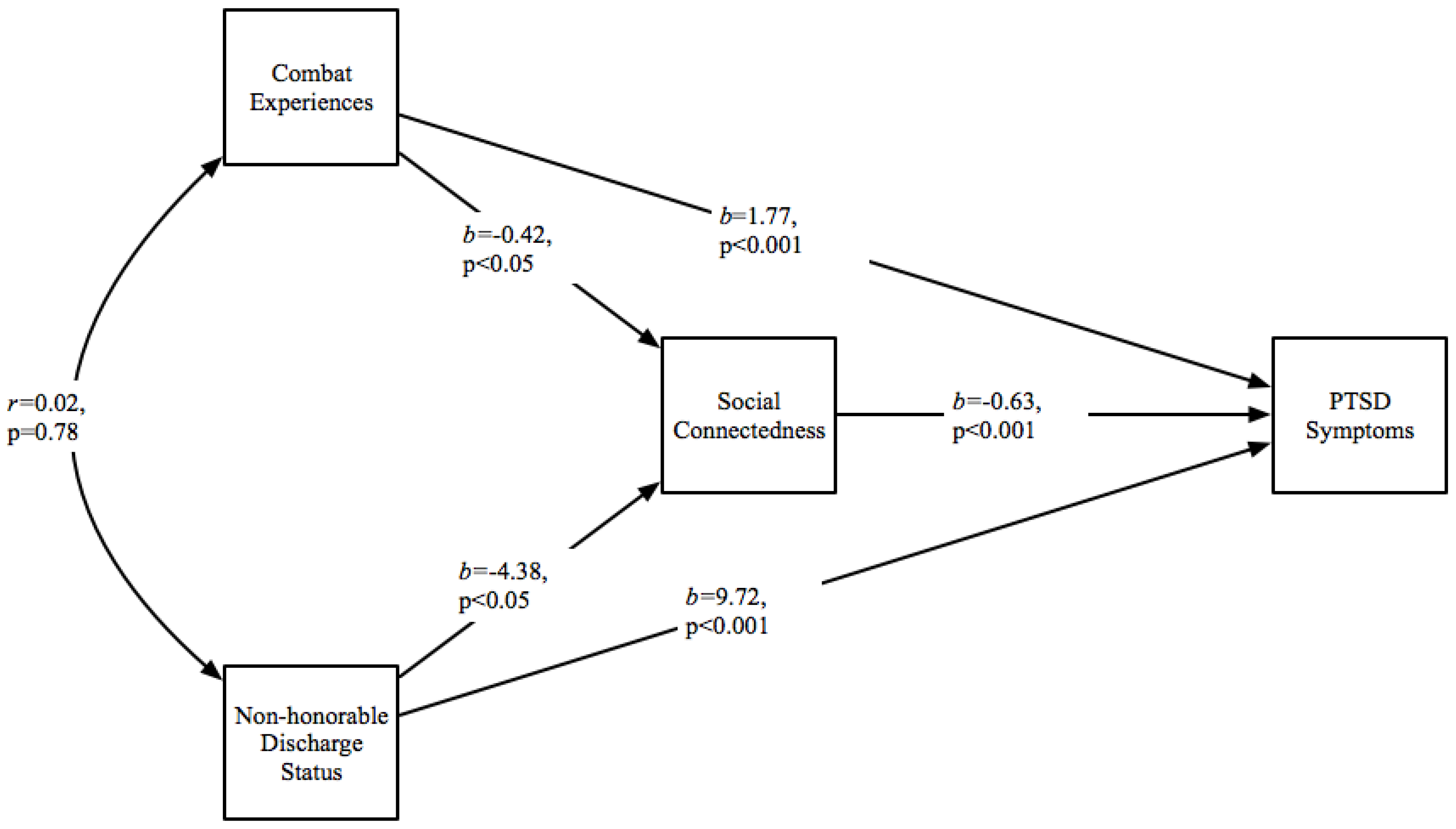
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Muller, J.; Ganeshamoorthy, S.; Myers, J. Risk factors associated with posttraumatic stress disorder in US veterans: A cohort study. PLoS ONE 2017, 12, e0181647. [Google Scholar]
- Richardson, L.K.; Frueh, B.C.; Acierno, R. Prevalence estimates of combat—Related post-traumatic stress disorder: Critical review. Aust. N. Z. J. Psychiatry 2010, 44, 4–19. [Google Scholar]
- Knowles, K.A.; Sripada, R.K.; Defever, M.; Rauch, S.A.M. Comorbid mood and anxiety disorder and severity of posttraumatic stress symptoms in treatment seeking veterans. Psychol. Trauma 2018, 1–8. [Google Scholar] [CrossRef]
- Sippel, L.M.; Watkins, L.E.; Pietrzak, R.H.; Hoff, R.; Harpaz-Rtem, I. The unique roles of emotional numbing and arousal symptoms in relation to social connectedness among military veterans in residential treatment for PTSD. Psychiatry 2018. [Google Scholar] [CrossRef]
- Xue, C.; Ge, Y.; Tang, B.; Liu, Y.; Kang, P.; Wang, M.; Zhang, L. A meta-analysis of risk factors for combat related PTSD among military personnel and veterans. PLoS ONE 2015, 10, e0120270. [Google Scholar]
- Amdur, D.; Batres, A.; Beslisle, J.; Brown, J.H.; Cornis-Pop, M.; Matthewson-Chapman, M.; Harms, G.; Hunt, S.C.; Kennedy, P.; Mahoney-Gleason, H.; et al. VA Integrated post-combat care: A systemic approach to caring for returning combat veterans. Sci. Work Healthc. 2011, 50, 564–575. [Google Scholar] [CrossRef] [PubMed]
- Buttner, M.M.; Godfrey, K.M.; Floto, E.; Pittman, J.; Lindamer, L.; Afari, N. Combat exposure and pain in male and female afghanistan and iraq veterans: The role of mediators and moderators. Psychiatr. Res. 2017, 257, 7–13. [Google Scholar]
- Holliday, S.B.; Pedersen, E.R. The association between discharge status, mental health, and substance misuse among young adult veterans. Psychiatr. Res. 2017, 256, 428–434. [Google Scholar] [CrossRef] [PubMed]
- Veterans Legal Clinic. Underserved: How the VA Wrongfully Excludes Veterans with Bad Paper. Available online: https://www.swords-to-plowshares.org/wp-content/uploads/Underserved.pdf (accessed on 6 August 2018).
- Barr, N.; Kintzle, S.; Alday, E.; Castro, C.A. How does discharge status impact suicide risk in military veterans? Health Soc. Work 2018, 1–11. [Google Scholar] [CrossRef]
- Lee, R.M.; Draper, M.; Lee, S. Social connectedness, dysfunctional interpersonal behaviors, and psychological distress: Testing a mediator model. J. Couns. Psychol. 2001, 48, 310–318. [Google Scholar]
- Williams, K.L.; Galliher, R.V. Predicting depression and self-esteem from social connectedness, support and competence. J. Soc. Clin. Psychol. 2006, 25, 855–874. [Google Scholar]
- Satici, S.A.; Uysal, R.; Deniz, M.E. Linking Social connectedness to loneliness: The mediating role of subjective happiness. Pers. Indiv. Differ. 2016, 97, 306–310. [Google Scholar]
- Fanning, J.F.; Peirrzak, R.H. Suicidality among older male veterans in the United States: Results from the national health and resilience in veterans study. J. Psychiatr. Res. 2013, 47, 1766–1775. [Google Scholar] [CrossRef] [PubMed]
- Mauss, I.B.; Shallcross, A.J.; Troy, A.S.; John, O.P.; Ferrer, E.; Wilhelm, F.H.; Gross, J.J. Don’t hide your happiness! Positive emotion dissociation, social connectedness, and psychological functioning. J. Pers. Soc. Psychol. 2011, 100, 738–748. [Google Scholar]
- Castro, C.A.; Kintzle, S. The State of the American Veteran: The San Francisco Veterans Study; USC CIR: San Francisco, CA, USA, 2017; Available online: http://cir.usc.edu/wp-content/uploads/2017/05/USC-CIR-SF-VET-2017_FINAL-Pgs.pdf (accessed on 6 August 2018).
- PTSD Checklist for DSM-5 (PCL-5)—PTSD: National Center for PTSD. Available online: https://www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-checklist.asp (accessed on 6 August 2018).
- PTSD: National Center for PTSD. Treatment of PTSD: Recommended Treatments. Available online: https://www.ptsd.va.gov/public/treatment/therapy-med/treatment-ptsd.asp (accessed on 8 June 2018).
- Hoge, C.W.; Castro, C.A.; Messer, S.C.; McGurk, D.; Cotting, D.I.; Koffman, R.L. Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. N. Engl. J. Med. 2004, 351, 13–22. [Google Scholar] [CrossRef] [PubMed]
- Lee, R.M.; Robbins, S.B. Measuring belongingness: The social connectedness and the social assurance scales. J. Couns. Psychol. 1995, 42, 232–241. [Google Scholar] [CrossRef]
- StataCorp LLC. Stata Data Analysis and Statistical Software; Special Edition Release; StataCorp LLC: College Station, TX, USA, 2007; Volume 10, p. 733. Available online: https://www.stata.com/order/GS35F0108W-Rel12.pdf (accessed on 6 August 2018).
- Lo, S.K.; Li, I.T.; Tsou, T.S.; See, L. Non-significant in univariate but significant in multivariate analysis: A discussion with examples. Changgeng Yi Xue Za Zhi 1995, 18, 95–101. [Google Scholar] [PubMed]
- Ashida, S.; Heaney, C.A. Differential associations of social support and social connectedness with structural features of social networks and the health status of older adults. J. Aging Health 2008, 20, 872–893. [Google Scholar] [CrossRef] [PubMed]
- Cornwell, E.Y.; Waite, L.J. Social disconnectedness, perceived isolation, and health among older adults. J. Health Soc. Behav. 2009, 50, 31–48. [Google Scholar] [CrossRef] [PubMed]
- Bond, L.; Butler, H.; Thomas, L.; Carlin, J.; Glover, S.; Bowes, G.; Patton, G. Social and school connectedness in early secondary school as predictors of late teenage substance use, mental health, and academic outcomes. J. Adolesc. Health 2007, 40, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Pflum, S.R.; Testa, R.J.; Balsam, K.F.; Goldblum, P.B.; Bongar, B. Social support, trans community connectedness, and mental health symptoms among transgender and gender nonconforming adults. Psychol. Sex. Orientat. Gend. Divers. 2015, 2, 281–286. [Google Scholar] [CrossRef]
- Armstrong, S.; Oomen-Early, J. Social connectedness, self-esteem, and depression symptomatology among collegiate athletes versus nonathletes. J. Am. Coll. Health 2009, 57, 521–526. [Google Scholar] [CrossRef] [PubMed]
| Variable | Combat Experiences | Non-Honorable Discharge Status | Social Connectedness | PTSD Symptoms |
|---|---|---|---|---|
| Combat experiences | 1 | |||
| Non-honorable discharge status | 0.01 | 1 | ||
| Social connectedness | −0.14 * | −0.09 | 1 | |
| PTSD symptoms | 0.40 *** | 0.26 *** | −0.40 *** | 1 |
| Variable | Variable Descriptors | % | N = 722 | M | SD |
|---|---|---|---|---|---|
| Age | 18–29 | 8.61% | 62 | ||
| 30–39 | 37.36% | 269 | |||
| 40–49 | 16.25% | 117 | |||
| 50–59 | 12.91% | 93 | |||
| 60 and older | 15.69% | 179 | |||
| 70 and older | 9.17% | 66 | |||
| Gender | Male | 80.56% | 580 | ||
| Female | 19.03% | 137 | |||
| Transgender | 0.40% | 3 | |||
| Marital Status | Single | 28.02% | 202 | ||
| Married/Domestic Partnership | 51.04% | 368 | |||
| Divorced/separated | 17.89% | 129 | |||
| Widowed | 3.05% | 22 | |||
| Race/Ethnicity | American Indian/Alaska Native | 2.78% | 20 | ||
| Asian | 6.40% | 46 | |||
| Black | 17.25% | 124 | |||
| Hawaiian/Pacific Islander | 2.50% | 18 | |||
| White | 54.38% | 391 | |||
| Hispanic/Latino | 11.82% | 85 | |||
| Other | 4.87% | 35 | |||
| Education | Some High School | 2.22% | 16 | ||
| GED | 3.47% | 25 | |||
| High school diploma | 9.29% | 67 | |||
| Some college | 26.49% | 191 | |||
| Associate degree | 12.48% | 90 | |||
| Bachelor’s | 23.30% | 168 | |||
| Master’s | 18.45% | 133 | |||
| Doctorate | 2.50% | 18 | |||
| Other | 1.80% | 13 | |||
| Non-Honorable Discharge Status | 29.64% | 214 | |||
| Combat Experiences | 6.64 | 4.38 | |||
| Social Connectedness | 32.15 | 13.27 | |||
| PTSD Symptoms | 36.07 | 21.6 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kintzle, S.; Barr, N.; Corletto, G.; Castro, C.A. PTSD in U.S. Veterans: The Role of Social Connectedness, Combat Experience and Discharge. Healthcare 2018, 6, 102. https://doi.org/10.3390/healthcare6030102
Kintzle S, Barr N, Corletto G, Castro CA. PTSD in U.S. Veterans: The Role of Social Connectedness, Combat Experience and Discharge. Healthcare. 2018; 6(3):102. https://doi.org/10.3390/healthcare6030102
Chicago/Turabian StyleKintzle, Sara, Nicholas Barr, Gisele Corletto, and Carl A. Castro. 2018. "PTSD in U.S. Veterans: The Role of Social Connectedness, Combat Experience and Discharge" Healthcare 6, no. 3: 102. https://doi.org/10.3390/healthcare6030102
APA StyleKintzle, S., Barr, N., Corletto, G., & Castro, C. A. (2018). PTSD in U.S. Veterans: The Role of Social Connectedness, Combat Experience and Discharge. Healthcare, 6(3), 102. https://doi.org/10.3390/healthcare6030102





