The Clinical Researcher Journey in the Artificial Intelligence Era: The PAC-MAN’s Challenge
Abstract
1. Introduction
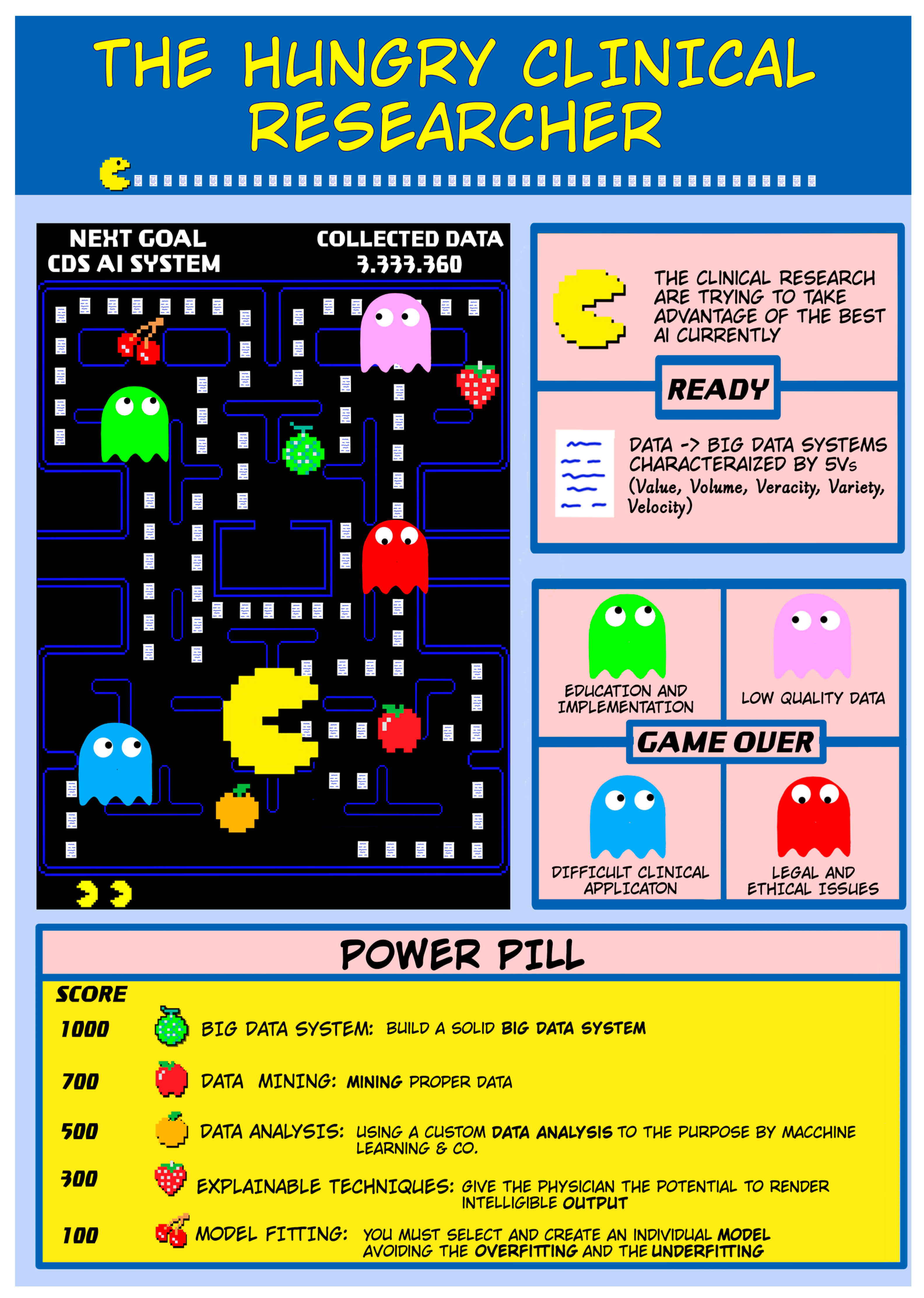
2. The PAC-MAN Metaphor
3. Game Rules for a Clinical Researcher
4. AI in Anesthesia
5. Clinical Practice and Research Perspectives
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Harnett, J.D. Research Ethics for Clinical Researchers. Methods Mol. Biol. 2021, 2249, 53–64. [Google Scholar] [CrossRef]
- Cobianchi, L.; Piccolo, D.; Dal Mas, F.; Agnoletti, V.; Ansaloni, L.; Balch, J.; Biffl, W.; Butturini, G.; Catena, F.; Coccolini, F.; et al. Surgeons’ Perspectives on Artificial Intelligence to Support Clinical Decision-Making in Trauma and Emergency Contexts: Results from an International Survey. World J. Emerg. Surg. 2023, 18, 1. [Google Scholar] [CrossRef]
- Weissler, E.H.; Naumann, T.; Andersson, T.; Ranganath, R.; Elemento, O.; Luo, Y.; Freitag, D.F.; Benoit, J.; Hughes, M.C.; Khan, F.; et al. The Role of Machine Learning in Clinical Research: Transforming the Future of Evidence Generation. Trials 2021, 22, 537. [Google Scholar] [CrossRef] [PubMed]
- Klumpp, M.; Hintze, M.; Immonen, M.; Ródenas-Rigla, F.; Pilati, F.; Aparicio-Martínez, F.; Çelebi, D.; Liebig, T.; Jirstrand, M.; Urbann, O.; et al. Artificial Intelligence for Hospital Health Care: Application Cases and Answers to Challenges in European Hospitals. Healthcare 2021, 9, 961. [Google Scholar] [CrossRef]
- Dolezel, D.; McLeod, A. Big Data Analytics in Healthcare: Investigating the Diffusion of Innovation. Perspect. Health Inf. Manag. 2019, 16, 1a. [Google Scholar] [PubMed]
- Garcia-Vidal, C.; Sanjuan, G.; Puerta-Alcalde, P.; Moreno-García, E.; Soriano, A. Artificial Intelligence to Support Clinical Decision-Making Processes. EBioMedicine 2019, 46, 27–29. [Google Scholar] [CrossRef]
- Yu, K.-H.; Beam, A.L.; Kohane, I.S. Artificial Intelligence in Healthcare. Nat. Biomed. Eng. 2018, 2, 719–731. [Google Scholar] [CrossRef]
- Hogg, H.D.J.; Al-Zubaidy, M.; Technology Enhanced Macular Services Study Reference Group; Talks, J.; Denniston, A.K.; Kelly, C.J.; Malawana, J.; Papoutsi, C.; Teare, M.D.; Keane, P.A.; et al. Stakeholder Perspectives of Clinical Artificial Intelligence Implementation: Systematic Review of Qualitative Evidence. J. Med. Internet Res. 2023, 25, e39742. [Google Scholar] [CrossRef] [PubMed]
- Gallagher, M.; Ryan, A. Learning to Play Pac-Man: An Evolutionary, Rule-Based Approach. In Proceedings of the IEEE Conference Publication The 2003 Congress on Evolutionary Computation, Canberra, ACT, Australia, 8–12 December 2003; Available online: https://ieeexplore.ieee.org/document/1299397 (accessed on 10 January 2023).
- “DeNero, J.; Klein, D. Teaching Introductory Artificial Intelligence with Pac-Man. In Proceedings of the AAAI Conference on Artificial Intelligence, Atlanta, GA, USA, 11–15 July 2010; Available online: https://ojs.aaai.org/index.php/AAAI/article/view/18829 (accessed on 10 January 2023).
- Ahn, E. Introducing Big Data Analysis Using Data from National Health Insurance Service. Korean J. Anesthesiol. 2020, 73, 205–211. [Google Scholar] [CrossRef]
- Bellini, V.; Cascella, M.; Cutugno, F.; Russo, M.; Lanza, R.; Compagnone, C.; Bignami, E.G. Understanding Basic Principles of Artificial Intelligence: A Practical Guide for Intensivists. Acta Biomed. 2022, 93, e2022297. [Google Scholar] [CrossRef]
- Algoretica-Parole Nuove-Accademia Della Crusca. Available online: https://accademiadellacrusca.it/it/parole-nuove/algoretica/18479 (accessed on 11 February 2023).
- Mantini, A. Technological Sustainability and Artificial Intelligence Algor-Ethics. Sustainability 2022, 14, 3215. [Google Scholar] [CrossRef]
- Recommendation on the Ethics of Artificial Intelligence-UNESCO Digital Library. Available online: https://unesdoc.unesco.org/ark:/48223/pf0000381137 (accessed on 11 February 2023).
- Laptev, V.A.; Ershova, I.V.; Feyzrakhmanova, D.R. Medical Applications of Artificial Intelligence (Legal Aspects and Future Prospects). Laws 2022, 11, 3. [Google Scholar] [CrossRef]
- Zhang, J.; Zhang, Z. Ethics and Governance of Trustworthy Medical Artificial Intelligence. BMC Med. Inform. Decis. Mak. 2023, 23, 7. [Google Scholar] [CrossRef] [PubMed]
- Petrucci, E.; Vittori, A.; Cascella, M.; Vergallo, A.; Fiore, G.; Luciani, A.; Pizzi, B.; Degan, G.; Fineschi, V.; Marinangeli, F. Litigation in Anesthesia and Intensive Care Units: An Italian Retrospective Study. Healthcare 2021, 9, 1012. [Google Scholar] [CrossRef] [PubMed]
- Bellini, V.; Valente, M.; Pelosi, P.; Del Rio, P.; Bignami, E. Big Data and Artificial Intelligence in Intensive Care Unit: From “Bla, Bla, Bla” to the Incredible Five V’s. Neurocrit. Care 2022, 37, 170–172. [Google Scholar] [CrossRef] [PubMed]
- Hatherley, J.; Sparrow, R.; Howard, M. The Virtues of Interpretable Medical Artificial Intelligence. Camb. Q. Healthc. Ethics 2022, 1–10. [Google Scholar] [CrossRef]
- Bellini, V.; Montomoli, J.; Bignami, E. Poor Quality Data, Privacy, Lack of Certifications: The Lethal Triad of New Technologies in Intensive Care. Intensive Care Med. 2021, 47, 1052–1053. [Google Scholar] [CrossRef]
- Luo, W.; Phung, D.; Tran, T.; Gupta, S.; Rana, S.; Karmakar, C.; Shilton, A.; Yearwood, J.; Dimitrova, N.; Ho, T.B.; et al. Guidelines for Developing and Reporting Machine Learning Predictive Models in Biomedical Research: A Multidisciplinary View. J. Med. Internet Res. 2016, 18, e323. [Google Scholar] [CrossRef]
- Cruz Rivera, S.; Liu, X.; Chan, A.-W.; Denniston, A.K.; Calvert, M.J.; SPIRIT-AI and CONSORT-AI Working Group; SPIRIT-AI and CONSORT-AI Steering Group. SPIRIT-AI and CONSORT-AI Consensus Group Guidelines for Clinical Trial Protocols for Interventions Involving Artificial Intelligence: The SPIRIT-AI Extension. Nat. Med. 2020, 26, 1351–1363. [Google Scholar] [CrossRef]
- Crossnohere, N.L.; Elsaid, M.; Paskett, J.; Bose-Brill, S.; Bridges, J.F.P. Guidelines for Artificial Intelligence in Medicine: Literature Review and Content Analysis of Frameworks. J. Med. Internet Res. 2022, 24, e36823. [Google Scholar] [CrossRef]
- Liu, X.; Cruz Rivera, S.; Moher, D.; Calvert, M.J.; Denniston, A.K. SPIRIT-AI and CONSORT-AI Working Group Reporting Guidelines for Clinical Trial Reports for Interventions Involving Artificial Intelligence: The CONSORT-AI Extension. Lancet Digit. Health 2020, 2, e537–e548. [Google Scholar] [CrossRef] [PubMed]
- Sounderajah, V.; Ashrafian, H.; Aggarwal, R.; De Fauw, J.; Denniston, A.K.; Greaves, F.; Karthikesalingam, A.; King, D.; Liu, X.; Markar, S.R.; et al. Developing Specific Reporting Guidelines for Diagnostic Accuracy Studies Assessing AI Interventions: The STARD-AI Steering Group. Nat. Med. 2020, 26, 807–808. [Google Scholar] [CrossRef] [PubMed]
- Collins, G.S.; Dhiman, P.; Andaur Navarro, C.L.; Ma, J.; Hooft, L.; Reitsma, J.B.; Logullo, P.; Beam, A.L.; Peng, L.; Van Calster, B.; et al. Protocol for Development of a Reporting Guideline (TRIPOD-AI) and Risk of Bias Tool (PROBAST-AI) for Diagnostic and Prognostic Prediction Model Studies Based on Artificial Intelligence. BMJ Open 2021, 11, e048008. [Google Scholar] [CrossRef] [PubMed]
- Norgeot, B.; Quer, G.; Beaulieu-Jones, B.K.; Torkamani, A.; Dias, R.; Gianfrancesco, M.; Arnaout, R.; Kohane, I.S.; Saria, S.; Topol, E.; et al. Minimum Information about Clinical Artificial Intelligence Modeling: The MI-CLAIM Checklist. Nat. Med. 2020, 26, 1320–1324. [Google Scholar] [CrossRef]
- Hernandez-Boussard, T.; Bozkurt, S.; Ioannidis, J.P.A.; Shah, N.H. MINIMAR (MINimum Information for Medical AI Reporting): Developing Reporting Standards for Artificial Intelligence in Health Care. J. Am. Med. Inform Assoc. 2020, 27, 2011–2015. [Google Scholar] [CrossRef]
- Vasey, B.; Nagendran, M.; Campbell, B.; Clifton, D.A.; Collins, G.S.; Denaxas, S.; Denniston, A.K.; Faes, L.; Geerts, B.; Ibrahim, M.; et al. Reporting Guideline for the Early-Stage Clinical Evaluation of Decision Support Systems Driven by Artificial Intelligence: DECIDE-AI. Nat. Med. 2022, 28, 924–933. [Google Scholar] [CrossRef]
- Rogers, W.A.; Draper, H.; Carter, S.M. Evaluation of Artificial Intelligence Clinical Applications: Detailed Case Analyses Show Value of Healthcare Ethics Approach in Identifying Patient Care Issues. Bioethics 2021, 35, 623–633. [Google Scholar] [CrossRef]
- Reddy, S.; Rogers, W.; Makinen, V.-P.; Coiera, E.; Brown, P.; Wenzel, M.; Weicken, E.; Ansari, S.; Mathur, P.; Casey, A.; et al. Evaluation Framework to Guide Implementation of AI Systems into Healthcare Settings. BMJ Health Care Inform. 2021, 28, e100444. [Google Scholar] [CrossRef]
- Szajewska, H. Evidence-Based Medicine and Clinical Research: Both Are Needed, Neither Is Perfect. Ann. Nutr. Metab. 2018, 72 (Suppl. 3), 13–23. [Google Scholar] [CrossRef]
- Garg, R.; Patel, A.; Hoda, W. Emerging Role of Artificial Intelligence in Medical Sciences-Are We Ready! J. Anaesthesiol. Clin. Pharmacol. 2021, 37, 35–36. [Google Scholar] [CrossRef]
- Finlayson, S.G.; Subbaswamy, A.; Singh, K.; Bowers, J.; Kupke, A.; Zittrain, J.; Kohane, I.S.; Saria, S. The Clinician and Dataset Shift in Artificial Intelligence. N. Engl. J. Med. 2021, 385, 283–286. [Google Scholar] [CrossRef]
- Esteva, A.; Kuprel, B.; Novoa, R.A.; Ko, J.; Swetter, S.M.; Blau, H.M.; Thrun, S. Dermatologist-Level Classification of Skin Cancer with Deep Neural Networks. Nature 2017, 542, 115–118. [Google Scholar] [CrossRef]
- Lee, S.; Summers, R.M. Clinical Artificial Intelligence Applications in Radiology: Chest and Abdomen. Radiol. Clin. N. Am. 2021, 59, 987–1002. [Google Scholar] [CrossRef]
- Groot Lipman, K.B.W.; de Gooijer, C.J.; Boellaard, T.N.; van der Heijden, F.; Beets-Tan, R.G.H.; Bodalal, Z.; Trebeschi, S.; Burgers, J.A. Artificial Intelligence-Based Diagnosis of Asbestosis: Analysis of a Database with Applicants for Asbestosis State Aid. Eur. Radiol. 2022. [Google Scholar] [CrossRef]
- Cascella, M.; Montomoli, J.; Bellini, V.; Bignami, E. Evaluating the Feasibility of ChatGPT in Healthcare: An Analysis of Multiple Clinical and Research Scenarios. J. Med. Syst. 2023, 47, 33. [Google Scholar] [CrossRef] [PubMed]
- Cascella, M.; Monaco, F.; Nocerino, D.; Chinè, E.; Carpenedo, R.; Picerno, P.; Migliaccio, L.; Armignacco, A.; Franceschini, G.; Coluccia, S.; et al. Bibliometric Network Analysis on Rapid-Onset Opioids for Breakthrough Cancer Pain Treatment. J. Pain Symptom Manag. 2022, 63, 1041–1050. [Google Scholar] [CrossRef] [PubMed]
- Saputra, D.C.E.; Sunat, K.; Ratnaningsih, T. A New Artificial Intelligence Approach Using Extreme Learning Machine as the Potentially Effective Model to Predict and Analyze the Diagnosis of Anemia. Healthcare 2023, 11, 697. [Google Scholar] [CrossRef] [PubMed]
- Cascella, M.; Coluccia, S.; Monaco, F.; Schiavo, D.; Nocerino, D.; Grizzuti, M.; Romano, M.C.; Cuomo, A. Different Machine Learning Approaches for Implementing Telehealth-Based Cancer Pain Management Strategies. J. Clin. Med. 2022, 11, 5484. [Google Scholar] [CrossRef]
- Lee, T.-S.; Lu, C.-J. Health Informatics: The Foundations of Public Health. Healthcare 2023, 11, 798. [Google Scholar] [CrossRef]
- Cascella, M.; Racca, E.; Nappi, A.; Coluccia, S.; Maione, S.; Luongo, L.; Guida, F.; Avallone, A.; Cuomo, A. Bayesian Network Analysis for Prediction of Unplanned Hospital Readmissions of Cancer Patients with Breakthrough Cancer Pain and Complex Care Needs. Healthcare 2022, 10, 1853. [Google Scholar] [CrossRef]
- Moussaid, A.; Zrira, N.; Benmiloud, I.; Farahat, Z.; Karmoun, Y.; Benzidia, Y.; Mouline, S.; El Abdi, B.; Bourkadi, J.E.; Ngote, N. On the Implementation of a Post-Pandemic Deep Learning Algorithm Based on a Hybrid CT-Scan/X-Ray Images Classification Applied to Pneumonia Categories. Healthcare 2023, 11, 662. [Google Scholar] [CrossRef] [PubMed]
- Linardatos, P.; Papastefanopoulos, V.; Kotsiantis, S. Explainable AI: A Review of Machine Learning Interpretability Methods. Entropy 2020, 23, 18. [Google Scholar] [CrossRef] [PubMed]
- Sghir, N.; Adadi, A.; Lahmer, M. Recent Advances in Predictive Learning Analytics: A Decade Systematic Review (2012–2022). Educ. Inf. Technol. 2022, 1–35. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.; Roberts, K.; Datta, S.; Du, J.; Ji, Z.; Si, Y.; Soni, S.; Wang, Q.; Wei, Q.; Xiang, Y.; et al. Deep Learning in Clinical Natural Language Processing: A Methodical Review. J. Am. Med. Inform. Assoc. 2020, 27, 457–470. [Google Scholar] [CrossRef]
- Fu, J.; Wang, H.; Na, R.; Jisaihan, A.; Wang, Z.; Ohno, Y. Recent Advancements in Digital Health Management Using Multi-Modal Signal Monitoring. Math. Biosci. Eng. 2023, 20, 5194–5222. [Google Scholar] [CrossRef]

| RELEVANT ISSUES | MAIN SPECIFIC ITEMS |
|---|---|
| ETHICAL ISSUES |
|
| LEGAL ISSUES |
|
| EDUCATION AND IMPLEMENTATION |
|
| QUALITY OF DATA |
|
| CLINICAL APPLICATION |
|
| Guideline | Description | Setting |
|---|---|---|
| SPIRIT-AI [23] | Standard Protocol Items: Recommendations for Interventional Trials—Artificial Intelligence | This promotes transparency and completeness for clinical trial protocols for AI interventions. |
| CONSORT-AI [25] | Consolidated Standards of Reporting Trials—Artificial Intelligence | This was developed to supplement SPIRIT-AI in order to improve the quality of trials for AI interventions. |
| STARD-AI [26] | Standards For Reporting Diagnostic Accuracy Studies—Artificial Intelligence | These guidelines help to improve transparency and completeness of reporting of diagnostic accuracy studies. |
| TRIPOD-AI [27] | Development of a reporting guideline for diagnostic and prognostic prediction studies based on artificial intelligence. Transparent Reporting of a multivariable prediction model for Individual Prognosis Or Diagnosis–Aritificial Intelligence | They will both be published to improve the reporting and critical appraisal of prediction model studies that applied ML techniques for diagnosis and prognosis. |
| PROBAST-AI [27] | Statement and the Prediction model Risk Of Bias ASsessment Tool–Artificial Intelligence | |
| MI-CLAIM [28] | Minimum Information about CLinical Artificial Intelligence Modeling | This improves the reporting of information regarding clinical AI algorithms. |
| MINIMAR [29] | MINimum Information for Medical AI Reporting | This establishes the minimum information necessary to understand intended predictions, target populations, hidden biases, and the ability to generalize these emerging technologies. |
| DECIDE-AI [30] | Developmental and Exploratory Clinical Investigation of DEcision-support systems driven by Artificial Intelligence | This improves the evaluation and reporting of human factors in clinical AI studies. This guideline will address the essential role that human factors will have in how a clinical AI algorithm performs. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bignami, E.G.; Vittori, A.; Lanza, R.; Compagnone, C.; Cascella, M.; Bellini, V. The Clinical Researcher Journey in the Artificial Intelligence Era: The PAC-MAN’s Challenge. Healthcare 2023, 11, 975. https://doi.org/10.3390/healthcare11070975
Bignami EG, Vittori A, Lanza R, Compagnone C, Cascella M, Bellini V. The Clinical Researcher Journey in the Artificial Intelligence Era: The PAC-MAN’s Challenge. Healthcare. 2023; 11(7):975. https://doi.org/10.3390/healthcare11070975
Chicago/Turabian StyleBignami, Elena Giovanna, Alessandro Vittori, Roberto Lanza, Christian Compagnone, Marco Cascella, and Valentina Bellini. 2023. "The Clinical Researcher Journey in the Artificial Intelligence Era: The PAC-MAN’s Challenge" Healthcare 11, no. 7: 975. https://doi.org/10.3390/healthcare11070975
APA StyleBignami, E. G., Vittori, A., Lanza, R., Compagnone, C., Cascella, M., & Bellini, V. (2023). The Clinical Researcher Journey in the Artificial Intelligence Era: The PAC-MAN’s Challenge. Healthcare, 11(7), 975. https://doi.org/10.3390/healthcare11070975







