Participation in an Online Course about Death and Dying: Exploring Enrolment Motivations and Learning Goals of Health Care Workers
Abstract
1. Introduction
- To provide a vehicle for the Australian public to openly discuss and learn about issues around living, death, and dying in a supportive environment.
- To explore the opinions and views of Australians around death and dying.
2. Materials and Methods
3. Results
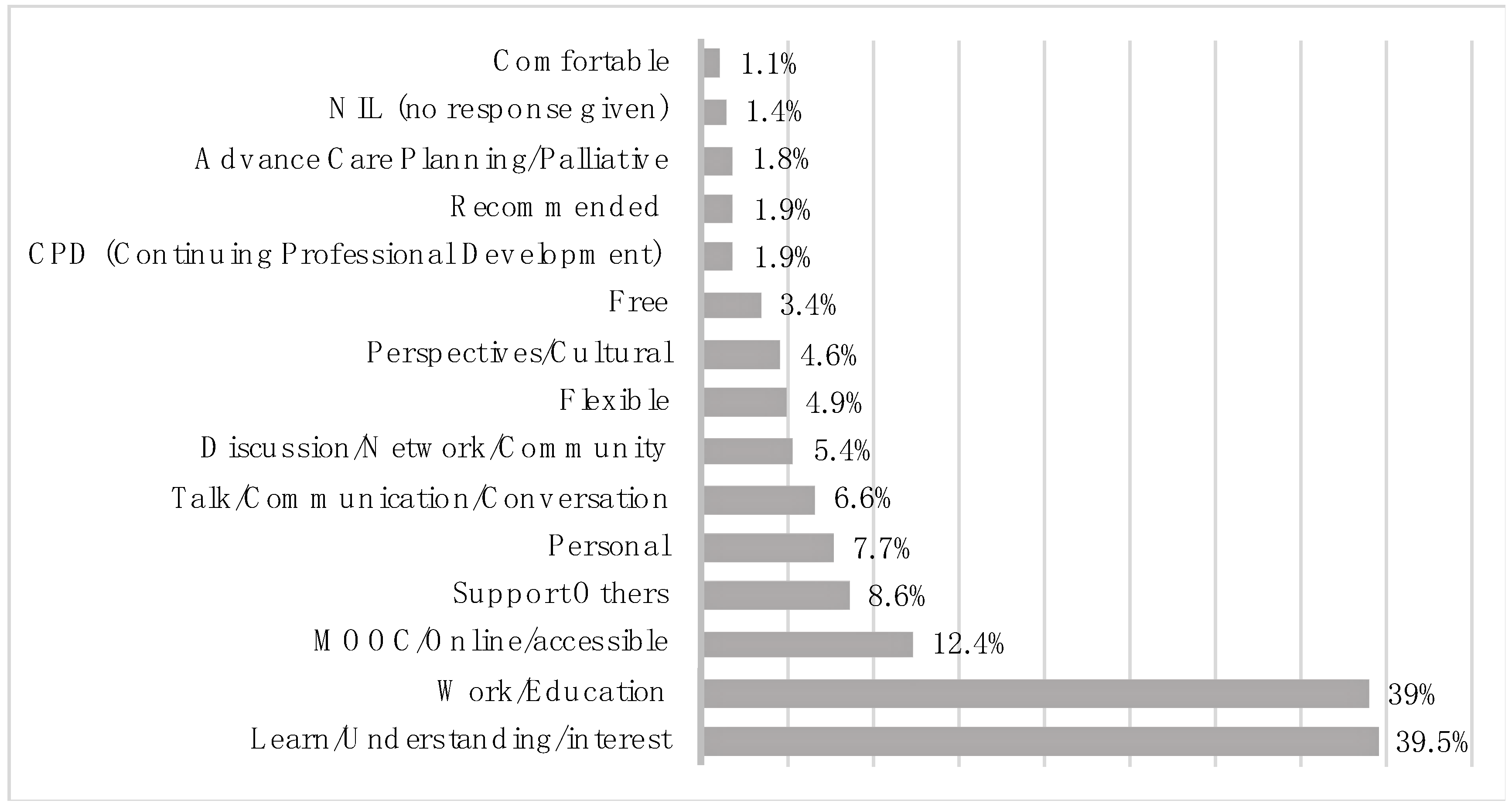
3.1. Responses Relating to Why Participants Enrolled in the MOOC
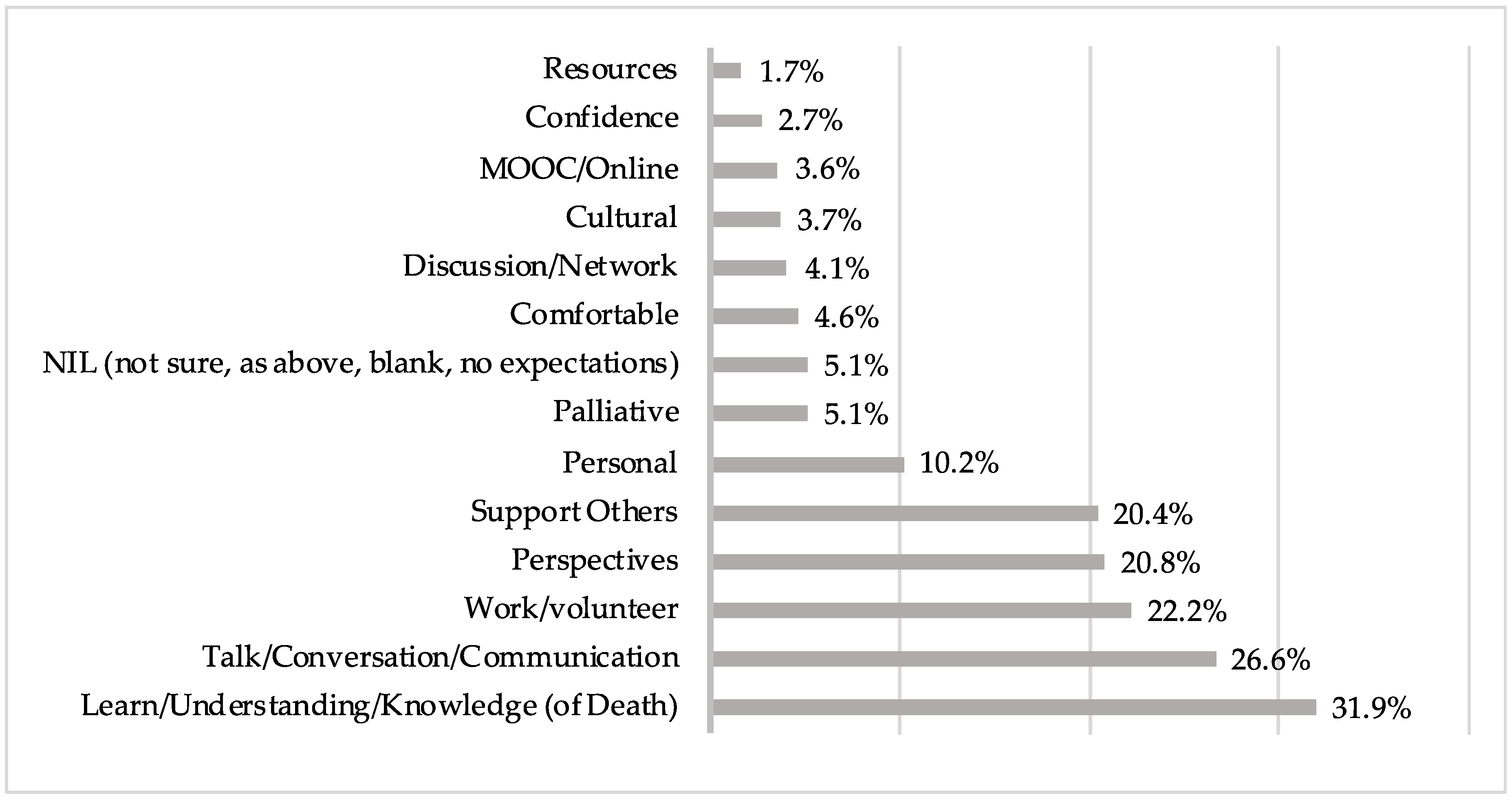
3.2. Responses Relating to Learning Goals
4. Discussion
4.1. Differences between Demographic Groups
4.2. HCW Responses
4.3. Doctors’ Responses in the MOOC
4.4. MOOCs as a Potential Learning Vehicle for Death Education
4.5. Limitations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
| Theme | Definition | Examples | Number of Participants with This Theme Present in Their Response | Percentage of Participants with This Theme Present in Their Response (%) |
|---|---|---|---|---|
| Learn/Understanding/Interest | Motivated by an interest on the topic, the course content, to learn more about the process of death and dying and gaining a better understanding | “Would like to learn more about death and dealing with persons dealing with death” “Death and dying interests me and I want to learn more.” “I am fascinated by death. Been reading “Staring at the sun” by Irvin Yalom and it has re-ignited my interest” | 309 | 39.5 |
| Work/Education | Motivated by desire to perform better in their roles at the workplace—Includes wanting to improve on clinical practice, communication skills, supporting patients better, or seeking a career associated with death and dying | “Death and dying are of particular interest to me because I work in aged care.” “I wanted to up skill and also be better prepared in my job and have a better way to help our clients and their carers prepare for the final stage” “I’m considering a career in Palliative Care and want to gain a better understanding of how death affects other people and hopefully what I can do to better support those facing it.” “I am currently establishing a new career as an End of Life Doula, having recently become a Funeral Celebrant. I saw the Dying2Learn course available through a Facebook page I follow.” | 305 | 39 |
| MOOC/Online/accessible | Interest in participating and completing an educational course online, including the ability to participate in the course wherever they are located. Also includes responses with previous experience in online learning leading to further interest in participating in more of such courses | “It is convenient to do from home, I have never experienced this type of online or interactive learning, I usually avoid this! Feel I will benefit from learning in this way a new experience. Always keen to add to my knowledge of death and dying.” “I did the University of Tasmania’s MOOC on Dementia three years ago and found it a wonderful way to learn about a field both of personal and professional interest.” “This course has come recommended to me by my facilities educator. I like that it is online and can be completed in my own time at my own pace. I also love that the group has many people with different jobs from nurses to carers giving various aspects on death and dying.” | 97 | 12.4 |
| Support Others | Seeking to pick up skills to support others who are going through or experiencing death, helping them to cope with death | “Have wanted to become more comfortable with the subject so I can be more supportive when friends and family are going through the end of life process themselves or with a loved one.” “I’m interested as to why people are so frightened of the topic of death, what happens when we die, why people react differently to death, how can I best comfort someone during a palliative stage and the different outlooks on death.” | 67 | 8.6 |
| Personal | Seeking an opportunity to reflect on their personal views on death and dying | “I want to participate to learn all I can about death and dying. I need to accept that death is going to happen and I want to conquer my fear of death and hopefully I can help others accept and not be afraid.” “I have end stage lymphoma, and am now in palliative care. I am not afraid of death, and my excellent Pall Care team gives me a great deal of reassurance that I need not fear the dying process. However, I have difficulty discussing this with family and friends who say ‘Oh, you’ll live to be 100’ Or ‘Stay positive, don’t talk about dying’ and other such unhelpful things. I’d like to have some tips on how to better navigate these discussions.” | 60 | 7.7 |
| Talk/Communication/Conversation | To learn how to talk about death and dying with others, to be better at conducting these “difficult” conversations, to know what to say in these situations, and make better responses when confronted with death and dying | “To help to become more confident with open discussions about death and dying” “I want to be able to respond appropriately to everyone I ever converse with, about whatever we wish to discuss.” “Since I work as a Palliative Care Psychologist for advanced cancer patients I come across deaths of our patients. Sometimes I feel some blocks on me while talking about death to few patients and caregivers. I am looking forward to this program to develop my skills in dealing with my problems with talking about death and help patients and caregivers.” | 52 | 6.6 |
| Discussion/Network/Community | Motivated by the desire to talk about death and dying, and discuss the topic with like-minded people on the internet–hearing others’ views on the matter as well as sharing their opinions | “I am interested in discussing death and dying and discovering and exploring different persons views on this topic. I am anticipating that this course will attract a diverse group of individuals that are willing to share their views, experiences and ideas on death and dying. I am sure this will assist in improving my knowledge and expertise in this area and support not only my personal development but also my professional.” “After being retrenched from my job of 12 years my path has taken an unexpected way into which is death and the dying. I want to know as much as I can about dying and every aspect and the only way to learn is to study and ask people. The MOOC has given me the opportunity to do both at the same time and to chat to like-minded people.” | 42 | 5.4 |
| Flexible | Motivated by the ability to complete the course at their own pace, without needing to adhere to a fixed class schedule. | “It’s an interesting topic where there is not much information about yet. Studying online on my own pace works for me, with my busy schedule and daily life.” “I felt that it might be beneficial in my practice as an Aged Care RN. The idea of being able to participate in an online format appealed because I thought it might be easier to fit into my schedule than other formats.” | 38 | 4.9 |
| Perspectives/Cultural | Seeking to learn more about how people from different cultures view and deal with death and dying. To be able to expand their view on the topic, to see new perspectives as they hear from other participants in the MOOC | “Always interested to learn from others experiences and reflect on practice.” “I am interested in open discussion around dying and death as well as to learn as much as I can about this subject. When I saw this course through a Facebook link, I decided it was a great opportunity to engage with my own thoughts and feelings around dying and death as well as to hear the views of others. It is also a great opportunity to connect with a diverse community.” | 36 | 4.6 |
| Theme | Definition | Examples | Number of Participants with This Theme Present in Their Response | Percentage of Participants with This Theme Present in Their Response (%) |
|---|---|---|---|---|
| Learn/Understanding/Knowledge (of Death) | To learn more about the topic of death, understanding what death and dying means and the process of dying, to improve on their knowledge on the topic | “Having a better understanding of death and dying and seeing how other people react and feel.” “Explore and clarify thoughts and expectations around death and dying for the person and their loved ones, before and after death.” | 250 | 31.9 |
| Talk/Conversation/Communication | To improve on communicating with others about death and dying, to make better conversations with others about death and dying | “Being more open to the discussions with families about the journey their loved one is on. Improve concepts of death and dying and improve my communication skills in these discussions.” “I am hoping for more understanding of peoples’ ideas about death and dying and to learn how to better communicate when needed with others.” “I want to be able to talk openly about death and dying and not feel that I am talking about a taboo subject.” | 208 | 26.6 |
| Work/volunteer | To gain skills to perform well or better in their roles at work, or volunteering activities | “How best to serve and support my Palliative Care clients.” “I’m not entirely sure. I am hoping to have some really interesting conversations and hopefully come away with more knowledge about an industry that I would really like to work in.” “Other strategies to speak with residents and families about end of life” | 174 | 22.2 |
| Perspectives | To be able to expand their view on the topic, to see new perspectives as they hear from other participants in the MOOC | “A better understanding of how different people feel about death. Maybe learn how best to approach the subject personally and at work. Broaden my understanding and appreciation of other perspectives.” “I am inspired to be surrounded (even virtually!) by like-minded people. I am passionate about Palliative care and I aim to continue broadening my understanding and perspectives to better hold space and provide care to my clients and their families.” | 163 | 20.8 |
| Support Others | To be able to apply what they have learnt in the course to support people who are going through or experiencing death, helping them to cope with death | “I hope that, with a better understanding of death and dying, I would be better able to journey with these people-to ally their fears, help them to accept their situations, bring some positives to their final days.” “To improve my knowledge and understanding and to be able to support people at this time in life, to be able to initiate open discussion around death and dying and to reduce any fear, stress or anxiety.” | 160 | 20.4 |
| Personal | To have an opportunity to reflect on the topic in a personal capacity, and explore what their own views on death and dying | “What I hope to learn is how to become more accepting of the process as a person and to be more comfortable talking about death and dying when dealing with those on Palliative and their families.” “How to approach death in conversations and in reflection” “I don’t know. I am open to being challenged in the way I work but also for myself personally in how I approach it for myself.” | 80 | 10.2 |
| Palliative | To learn more about palliative care specifically | “I hope to understand the palliative care aspect of EOL in more depth, & to have a greater understanding of the palliative care lexicon.” “I had done a Palliative Care course four years ago, I have since looked after a friend who had terminal cancer. It’s always good to know new information in Palliative Care” | 40 | 5.1 |
| Comfortable | To feel comfortable with talking about dying, being around the idea of death and to engage people who are at the end of their lives-The main aim is to eliminate feelings of anxiety when conducting such conversations and thus be better conversationalists at a personal level. | “Death and discussing it makes people uncomfortable. I want to learn how to make these conversations easier for people.” “Wanting to feel more comfortable having conversations with dying patients and their family and loved ones.” | 36 | 4.6 |
| Discussion/Network | To have an opportunity to discuss death and dying in a safe environment with like-minded people | “I’d like to know some of the ways death and dying are looked at in today’s world. The only conversations I have had so far have been with my partner (who died some years ago) and with a friend (whose mother died a few years ago). I would like to be part of a space and discourse where there is no fear attached and where there is only respect, learning and acceptance.” “I hope to gain new perspective and ways of thinking about death and dying. Being an online course, (there) will be so many different cultures and global views of death that I may not had the opportunity to connect with otherwise.” | 32 | 4.1 |
| Cultural | To learn more about how people from different cultures view death and dying, and the different ways of dealing with death | “I hope to discuss more about death and dying and maybe see how other cultures deal with these issues. I hope to understand more the process of grief and mourning- and for that I need to discuss more about death and dying.” “How others feel and handle death, how he communities we live in handle death. How best we can help each other handle death better. As a multi-cultural country if we can also learn about other cultures death rituals and their understandings about death and how we can fuse all this together and cater for our aged in our work places be it aged care, hospice or hospital.” | 29 | 3.7 |
| MOOC/Online | To experience online learning or to participate in a MOOC specifically | “Know what a MOOC is! Get ideas and inspiration for my work and my life.” “More confidence in undertaking online learning and more knowledge about death and dying” “Ways people approach death and dying in a dignified and graceful way. Tips to help me prepare for aging and death. Appreciate the linking of education, technology, staff and students in the MOOC way.” | 28 | 3.6 |
| Confidence | To feel confident with talking about dying and to engage people who are at the end of their lives. The main aim of the participant is to eliminate feelings of anxiety when conducting such conversations and thus be better conversationalists, with the end goal of being more competent at it from a work perspective. | “Increased confidence when discussing death and palliative care options with patients and colleagues in the workplace and potentially family members as well.” “I hope to come away with more confidence discussing dying with residents and their loved ones.” “I hope to be become competent and confident enough to talk about death and the dying process” | 21 | 2.7 |
| Resources | To gain access to sources of information or tools associated with dealing with death | “Learn of new resources, meet and connect with others (hopefully some local people to), to have my thinking challenged.” “Tools to improve the death experience for families and their loved ones.” “More resources, networking with like-minded and the opportunity to learn from the wisdom being shared.” | 13 | 1.7 |
| NIL | (not sure, as above, blank, no expectations) | N/A | 40 | 5.1 |
| Free | The course is free of charge for participants | “Because I am interested and because this is a free course, my training budget for 2017 is completely accounted for. This is also a format that is manageable in my busy life.” “I have been looking for further education in this area and I thought this sounded interesting and like something I would enjoy, it was right up my ally, It will help get my education points up, and it was FREE” | 27 | 3.4 |
| CPD (Continuing Professional Development) | Motivation was specific to gaining CPD points from participating in the course | “I was looking for something that would add to my CPD points that was relevant to my work but more importantly enhance my insight and performance into the what I feel is the most important part of my work, supporting individuals and families through the end of life process.” “Looked interesting, well set up, interactive and adds to my learning and CPD points” | 15 | 1.9 |
| Recommended | Participation in the MOOC was due to a recommendation from a contact | “It was recommended by a colleague who I respect and she sent link-interested in the subject matter feel passionate about I’m proving communication and people and families and dying especially in public hospital setting. Also interested as an educator and how online learning and this subject can work effectively together. Ready to learn new ideas, and new ways of teaching” “This course has come recommended to me by my facilities educator. I like that it is online and can be completed in my own time at my own pace. I also love that the group has many people with different jobs from nurses to carers giving various aspects on death and dying.” | 15 | 1.9 |
| Advance Care Planning/Palliative | Motivated by an interest in learning more about ACP/Palliative Care specifically | “I like to keep informed on any new information in Palliative Care to help me support my patients, family or friends more affectively” “I am interested in learning more about ACP (Advanced Care Planning) and how to go about discussing end of life with patients. To give me more ways to discuss and learn about dying.” | 14 | 1.8 |
| Comfortable | Seeking to feel more comfortable in conducting conversations related to death and dying | “To help to become more confident with open discussions about death and dying” “I want to feel more comfortable when talking to others about death and dying. I work in residential care and people often say they have moved here to die or living in ‘God’s waiting room” | 9 | 1.1 |
| NIL | (no response given) | N/A | 11 | 1.4 |
References
- Corr, C.A. Teaching about Life and Living in Courses on Death and Dying. Omega-J. Death Dying 2016, 73, 174–187. [Google Scholar] [CrossRef]
- Gellie, A.; Mills, A.; Levinson, M.; Stephenson, G.; Flynn, E. Death: A foe to be conquered? Questioning the paradigm. Age Ageing 2015, 44, 7–10. [Google Scholar] [CrossRef] [PubMed]
- Zhao, S.X.; Qiang, W.M.; Zheng, X.N.; Luo, Z.Q. Development of death education training content for adult cancer patients: A mixed methods study. J. Clin. Nurs. 2018, 27, 4400–4410. [Google Scholar] [CrossRef] [PubMed]
- Corr, C.A.; Nabe, C.M. Death and Dying, Life and Living; Cengage Learning: Belmont, CA, USA, 1997. [Google Scholar]
- Affifi, R.; Christie, B. Facing loss: Pedagogy of death. Environ. Educ. Res. 2019, 25, 1143–1157. [Google Scholar] [CrossRef]
- Rieber, L.P. Participation patterns in a massive open online course (MOOC) about statistics. Br. J. Educ. Technol. 2017, 48, 1295–1304. [Google Scholar] [CrossRef]
- Margaryan, A.; Bianco, M.; Littlejohn, A. Instructional quality of Massive Open Online Courses (MOOCs). Comput. Educ. 2015, 80, 77–83. [Google Scholar] [CrossRef]
- Miller-Lewis, L.; Tieman, J.; Rawlings, D.; Parker, D.; Sanderson, C. Can Exposure to Online Conversations about Death and Dying Influence Death Competence? An Exploratory Study within an Australian Massive Open Online Course. Omega 2018. [Google Scholar] [CrossRef]
- Tieman, J.; Miller-Lewis, L.; Rawlings, D.; Parker, D.; Sanderson, C. The contribution of a MOOC to community discussions around death and dying. BMC Palliat. Care 2018, 17, 31. [Google Scholar] [CrossRef]
- World Health Organization. Strengthening of Palliative Care as a Component of Integrated Treatment throughout the Life Course. J. Pain Palliat. Care Pharmacother. 2014, 28, 130–134. [Google Scholar] [CrossRef]
- Gibbins, J.; McCoubrie, R.; Forbes, K. Why are newly qualified doctors unprepared to care for patients at the end of life? Med. Educ. 2011, 45, 389–399. [Google Scholar] [CrossRef]
- Carey, E.C.; Paniagua, M.; Morrison, L.; Levine, S.K.; Klick, J.C.; Buckholz, G.T.; Rotella, J.; Bruno, J.; Liao, S.; Arnold, R.M. Palliative Care Competencies and Readiness for Independent Practice: A Report on the American Academy of Hospice and Palliative Medicine Review of the U.S. Medical Licensing Step Examinations. J. Pain Symptom Manag. 2018, 56, 371–378. [Google Scholar] [CrossRef] [PubMed]
- Whitaker, K.; Kross, E.K.; Hough, C.L.; Hurd, C.; Back, A.L.; Curtis, J.R. A Procedural Approach to Teaching Residents to Conduct Intensive Care Unit Family Conferences. J. Palliat. Med. 2016, 19, 1106–1109. [Google Scholar] [CrossRef] [PubMed]
- Morgan, D.D.; Rawlings, D.; Moores, C.J.; Button, L.; Tieman, J.J. The Changing Nature of Palliative Care: Implications for Allied Health Professionals‘ Educational and Training Needs. Healthcare 2019, 7, 112. [Google Scholar] [CrossRef] [PubMed]
- White, N.; Oostendorp, L.J.; Minton, O.; Yardley, S.; Stone, P. Palliative care training in undergraduate medical, nursing and allied health: A survey. BMJ Support. Palliat. Care 2019. [Google Scholar] [CrossRef] [PubMed]
- Saldaña, J. The Coding Manual for Qualitative Researchers, 3rd ed.; SAGE: Los Angeles, CA, USA, 2016. [Google Scholar]
- Ahpra. Continuing Professional Development. Available online: https://www.ahpra.gov.au/Registration/Registration-Standards/CPD.aspx (accessed on 10 February 2020).
- Maurer, T.J.; Weiss, E.M.; Barbeite, F.G. A Model of Involvement in Work-Related Learning and Development Activity: The Effects of Individual, Situational, Motivational, and Age Variables. J. Appl. Psychol. 2003, 88, 707–724. [Google Scholar] [CrossRef] [PubMed]
- Clanton, J.; Gardner, A.; Cheung, M.; Mellert, L.; Evancho-Chapman, M.; George, R.L. The Relationship between Confidence and Competence in the Development of Surgical Skills. J. Surg. Educ. 2014, 71, 405–412. [Google Scholar] [CrossRef]
- Sarabia-Cobo, C.M.; Torres-Manrique, B.; Ortego-Mate, M.C.; Salvadores-Fuentes, P.; Saenz-Jalon, M. CNE Quiz Continuing Education in Patient Safety: Massive Open Online Courses as a New Training Tool. J. Contin. Educ. Nurs. 2015, 46, 446–447. [Google Scholar] [CrossRef]
- Rawlings, D.; Miller-Lewis, L.; Collien, D.; Tieman, J.; Parker, D.; Sanderson, C. Lessons Learned from the Dying2Learn MOOC: Pedagogy, Platforms and Partnerships. Educ. Sci. 2017, 7, 67. [Google Scholar] [CrossRef]
- Betcher, D.K. Elephant in the room project: Improving caring efficacy through effective and compassionate communication with palliative care patients. Med.-Surg. Nurs. 2010, 19, 101–105. [Google Scholar]
- Reader, T.W.; Gillespie, A.; Roberts, J. Patient complaints in healthcare systems: A systematic review and coding taxonomy. BMJ Qual. Saf. 2014, 23, 678. [Google Scholar] [CrossRef]
- Bernacki, R.; Block, S.D. Communication About Serious Illness Care Goals A Review and Synthesis of Best Practices. JAMA Intern. Med. 2014, 174, 1994–2003. [Google Scholar] [CrossRef] [PubMed]
- Fraser, H.C.; Kutner, J.S.; Pfeifer, M.P. Senior Medical Students’ Perceptions of the Adequacy of Education on End-of-Life Issues. J. Palliat. Med. 2001, 4, 337–343. [Google Scholar] [CrossRef] [PubMed]
- Weber, M.; Schmiedel, S.; Nauck, F.; Alt-Epping, B. Knowledge and attitude of final-year medical students in Germany towards palliative care—An interinstitutional questionnaire-based study. BMC Palliat. Care 2011, 10, 19. [Google Scholar] [CrossRef] [PubMed]
- Gillett, K.; O’Neill, B.; Bloomfield, J.G. Factors influencing the development of End-of-life communication skills: A focus group study of nursing and medical students. Nurse Educ. Today 2016, 36, 395–400. [Google Scholar] [CrossRef]
- Gardner, D.B. Quality in life and death: Can we have the conversations? Nurs. Econ. 2012, 30, 224. [Google Scholar]
- Wass, H. A perspective on the current state of death education. Death Stud. 2004, 28, 289–308. [Google Scholar] [CrossRef]
- Goodhead, A.; Hartley, N. PA6 Death chat: Engaging with dying and death. BMJ Support. Palliat. Care 2015, 5 (Suppl. 1), A21. [Google Scholar] [CrossRef]
- Henoch, I.; Melin-Johansson, C.; Bergh, I.; Strang, S.; Ek, K.; Hammarlund, K.; Hagelin, C.L.; Westin, L.; Österlind, J.; Brovall, M. Undergraduate nursing students’ attitudes and preparedness toward caring for dying persons—A longitudinal study. Nurse Educ. Pract. 2017, 26, 12–20. [Google Scholar] [CrossRef]
- Rodenbach, R.A.; Rodenbach, K.E.; Tejani, M.A.; Epstein, R.M. Relationships between personal attitudes about death and communication with terminally ill patients: How oncology clinicians grapple with mortality. Patient Educ. Couns. 2016, 99, 356–363. [Google Scholar] [CrossRef]
- Nedjat-Haiem, F.R.; Carrion, I.V.; Gonzalez, K.; Ell, K.; Thompson, B.; Mishra, S.I. Exploring Health Care Providers’ Views about Initiating End-of-Life Care Communication. Am. J. Hosp. Palliat. Care 2017, 34, 308–317. [Google Scholar] [CrossRef]
- Ravenscroft, A. Dialogue and connectivism: A new approach to understanding and promoting dialogue-rich networked learning. Int. Rev. Res. Open Distance Learn. 2011, 12, 139. [Google Scholar] [CrossRef]
- Allchin, L. Caring for the Dying: Nursing Student Perspectives. J. Hosp. Palliat. Nurs. 2006, 8, 118–119. [Google Scholar] [CrossRef]
- Pardo, A.; Feifei, H.; Ellis, R.A. Combining University Student Self-Regulated Learning Indicators and Engagement with Online Learning Events to Predict Academic Performance. IEEE Trans. Learn. Technol. 2017, 10, 82–92. [Google Scholar] [CrossRef]
- Rienties, B.; Toetenel, L. The impact of learning design on student behaviour, satisfaction and performance: A cross-institutional comparison across 151 modules. Comput. Hum. Behav. 2016, 60, 333–341. [Google Scholar] [CrossRef]
| Frequency | Percent | |
|---|---|---|
| Not a health professional | 183 | 23.4 |
| Aged care worker | 122 | 15.6 |
| Allied health | 112 | 14.3 |
| Doctor | 5 | 0.6 |
| Nurse | 282 | 36.0 |
| Other | 79 | 10.1 |
| Total | 783 | 100.0 |
| No. of Judgements Made | Total Disagreement | Agreement Rate | Cohen’s Kappa |
|---|---|---|---|
| C1 1 vs. C2 | |||
| Learning goals (n = 490) | 35 | 92.86% | 0.675, p < 0.0005 |
| Why (n = 490) | 39 | 92.04% | 0.652, p < 0.0005 |
| C1 vs. C3 | |||
| Learning goals (n = 588) | 47 | 92.01% | 0.644, p < 0.0005 |
| Why (n = 637) | 49 | 92.31% | 0.657, p < 0.0005 |
| Themes | Not a Health Worker % | Aged Care Worker % | Allied Health Worker % | Nurse % | Total HCW Overall % |
|---|---|---|---|---|---|
| Learn/Understanding/Interest | 43.2 | 37.7 | 34.8 | 40.1 | 38.4 |
| Work/Education | 29.5 | 47.5 | 46.4 | 36.5 | 41.3 * |
| MOOC/Online/Accessible | 10.9 | 10.7 | 13.4 | 13.1 | 12.6 |
| Support Others | 8.2 | 13.1 | 4.5 | 7.4 | 8.1 * |
| Personal | 7.1 | 5.7 | 15.2 | 6.4 | 8.1 * |
| Talk/Communication/Conversation | 8.7 | 5.7 | 7.1 | 5.3 | 5.8 |
| Discussion/Network/Community | 11.5 | 2.5 | 2.7 | 4.3 | 3.5 |
| Flexible | 3.3 | 3.3 | 6.3 | 6.4 | 5.6 |
| Perspectives/Cultural | 6.0 | 0 | 1.8 | 6.0 | 3.7 * |
| Free | 3.8 | 1.6 | 4.5 | 3.5 | 3.3 |
| CPD (Continuing Professional Development) | 0 | 0.8 | 2.7 | 3.5 | 2.7 |
| Recommended | 1.6 | 0.8 | 2.7 | 2.8 | 2.3 |
| Advance Care Planning/Palliative | 1.1 | 2.5 | 0.9 | 2.5 | 2.1 |
| NIL (no response given) | 1.6 | 1.6 | 2.7 | 1.1 | 1.6 |
| Comfortable | 0 | 2.5 | 1.8 | 1.1 | 1.6 |
| Theme | Not a Health Worker % | Aged Care Worker % | Allied Health Worker % | Nurse % | Total HCW Overall % |
|---|---|---|---|---|---|
| Learn/Understanding/Knowledge (of Death) | 34.6 | 34.4 | 30.4 | 29.8 | 31.0 |
| Talk/Conversation/Communication | 20.5 | 27.0 | 27.7 | 29.1 | 28.3 |
| Work/volunteer | 13.5 | 23.0 | 21.4 | 27.0 | 24.8 |
| Perspectives | 23.8 | 12.3 | 24.1 | 21.3 | 19.8 * |
| Support Others | 18.4 | 22.1 | 18.8 | 21.6 | 21.1 |
| Personal | 14.6 | 10.7 | 12.5 | 7.1 | 9.1 |
| Palliative | 1.1 | 9.8 | 6.3 | 4.3 | 6.0 |
| Comfortable | 5.4 | 4.9 | 8.0 | 3.9 | 5.0 |
| Discussion/Network | 5.4 | 0 | 2.7 | 3.9 | 2.7 |
| Cultural | 2.2 | 2.5 | 5.4 | 4.6 | 4.3 |
| MOOC/Online | 5.4 | 1.6 | 6.3 | 2.5 | 3.1 |
| Confidence | 2.2 | 1.6 | 6.3 | 2.1 | 2.9 |
| Resources | 2.2 | 2.5 | 2.7 | 1.1 | 1.7 |
| NIL (not sure, as above, blank, no expectations) | 4.3 | 4.1 | 4.5 | 5.7 | 5.0 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oh, C.; Miller-Lewis, L.; Tieman, J. Participation in an Online Course about Death and Dying: Exploring Enrolment Motivations and Learning Goals of Health Care Workers. Educ. Sci. 2020, 10, 112. https://doi.org/10.3390/educsci10040112
Oh C, Miller-Lewis L, Tieman J. Participation in an Online Course about Death and Dying: Exploring Enrolment Motivations and Learning Goals of Health Care Workers. Education Sciences. 2020; 10(4):112. https://doi.org/10.3390/educsci10040112
Chicago/Turabian StyleOh, Claris, Lauren Miller-Lewis, and Jennifer Tieman. 2020. "Participation in an Online Course about Death and Dying: Exploring Enrolment Motivations and Learning Goals of Health Care Workers" Education Sciences 10, no. 4: 112. https://doi.org/10.3390/educsci10040112
APA StyleOh, C., Miller-Lewis, L., & Tieman, J. (2020). Participation in an Online Course about Death and Dying: Exploring Enrolment Motivations and Learning Goals of Health Care Workers. Education Sciences, 10(4), 112. https://doi.org/10.3390/educsci10040112





