Addition of Care for Transgender-Related Patient Care into Doctorate of Pharmacy Curriculum: Implementation and Preliminary Evaluation
Abstract
:1. Introduction
2. Materials and Methods
|
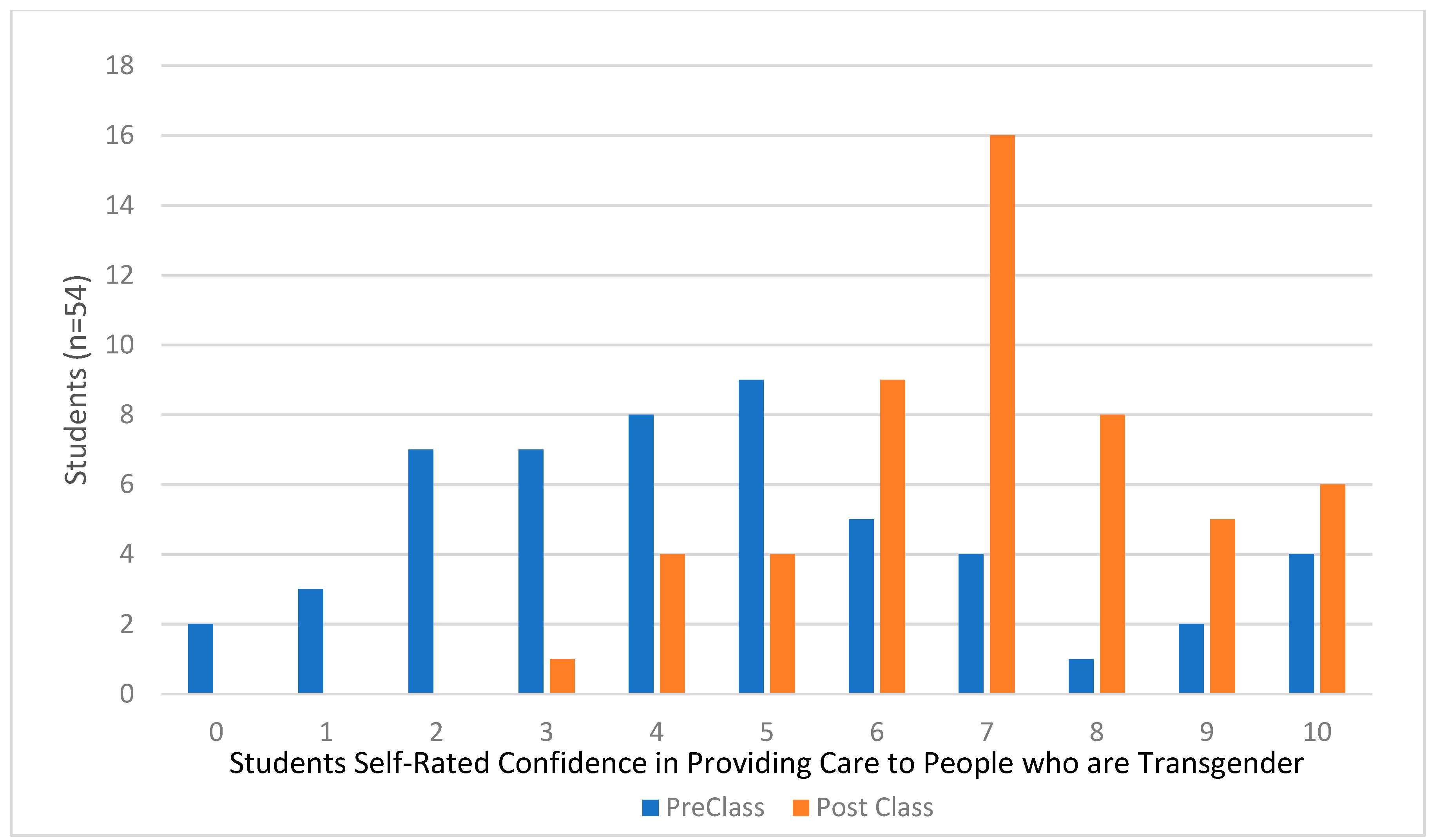
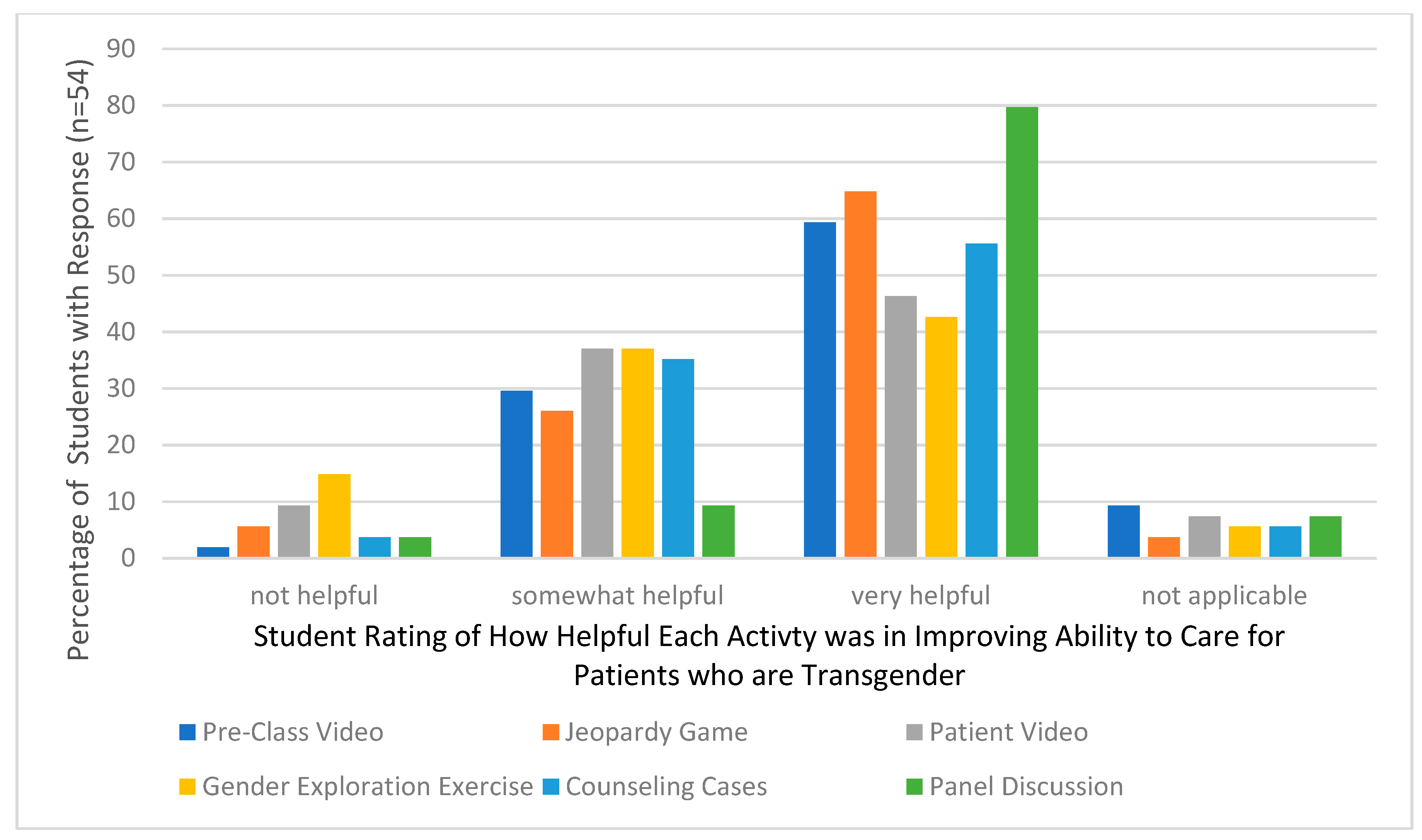
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Meerwijk, E.L.; Sevelius, J.M. Transgender Population Size in the United States: Meta-Regression of Population-Based Probability Samples. Am. J. Public Health 2017, 107, e1–e8. [Google Scholar] [CrossRef] [PubMed]
- Clements-Nolle, K.; Marx, R.; Guzman, R.; Katz, M. HIV Prevalence, Risk Behaviors, Health Care Use, and Mental Health Status of Transgender Persons: Implications for Public Health Intervention. Am. J. Public Health 2001, 91, 915–921. [Google Scholar] [PubMed]
- James, S.E.; Herman, J.L.; Rankin, S.; Keisling, M.; Mottet, L.; Anafi, M. The Report of the 2015 U.S. Transgender Survey; National Center for Transgender Equality: Washington, DC, USA, 2015. [Google Scholar]
- Kelly, L.; Chou, C.L.; Dibble, S.L.; Robertson, P.A. A Critical Intervention in Lesbian, Gay, Bisexual, and Transgender Health: Knowledge and Attitude Outcomes Among Second-Year Medical Students. Teach. Learn. Med. Int. J. 2008, 20, 248–253. [Google Scholar] [CrossRef] [PubMed]
- Garofalo, R.; Deleon, J.; Osmer, E.; Doll, M.; Harper, G.W. Overlooked, misunderstood and at-risk: Exploring the lives and HIV risk of ethnic minority male-to-female transgender youth. J. Adolescent Health 2006, 38, 230–236. [Google Scholar] [CrossRef] [PubMed]
- Sanchez, N.F.; Sanchez, J.P.; Danoff, A. Health Care Utilization, Barrier to Care, and Hormone Usage Among Male-to-Female Transgender Persons in New York City. Am. J. Public Health 2009, 99, 713–719. [Google Scholar] [CrossRef] [PubMed]
- Rotondi, N.K.; Bauer, G.R.; Scanlon, K.; Kaay, M.; Travers, R.; Travers, A. Nonprescribed Hormone Use and Self-Performed Surgeries: “Do-It-Yourself” Transitions in Trangender Communities in Ontario, Canada. Am. J. Public Health 2013, 103, 1830–1836. [Google Scholar] [CrossRef] [PubMed]
- Friedman, O.; Arad, E.; Ben Amotz, O. Body Builder’s Nightmare: Black Market Steroid Injection Gone Wrong: A Case Report. Plast. Reconstr. Surg. Glob. Open 2016, 4, e1040. [Google Scholar] [CrossRef] [PubMed]
- Mackey, T.K.; Liang, B.A. The global counterfeit drug trade: Patient safety and public health risks. J. Pharm. Sci. 2011, 100, 4571–4579. [Google Scholar] [CrossRef] [PubMed]
- Leach, C.; Layson-Wolf, C. Survey of community pharmacy residents’ perceptions of transgender health management. J. Am. Pharm. Assoc. 2016, 56, 441–445. [Google Scholar] [CrossRef] [PubMed]
- Parkhill, A.L.; Gainsburg, J.; Fearing, S.; Mathews, J.L. The need for Transgender Health Content in the Pharmacy Curriculum. Innov. Pharm. 2011, 2, 58. [Google Scholar] [CrossRef]
- Sawning, S.; Steinbock, S.; Croley, R.; Combs, R.; Shaw, A.; Ganzel, T. A First Step in Addressing Medical Education Curriculum Gaps in Lesbian-, Gay-, Bisexual-, and Transgender-Related Content: The University of Louisville Lesbian, Gay, Bisexual, and Transgender Health Certificate Program. Educ. Health 2017, 30, 108–115. [Google Scholar] [CrossRef] [PubMed]
- Yingling, C.; Cotler, K.; Hughes, T.L. Building nurse’ capacity to address health inequities: Incorporating lesbian, gay, bisexual and transgender health content in a family nurse practitioner programme. J. Clin. Nurs. 2016, 26, 2807–2817. [Google Scholar] [CrossRef] [PubMed]
- Copti, N.; Shahriari, R.; Wanek, L.; Fitzsimmons, A. Lesbian, Gay, Bisexual, and Transgender Inclusion in Physical Therapy: Advocating for Cultural Competency in Physical Therapist Education Across the United States. J. Phys. Ther. Educ. 2016, 30, 11–16. [Google Scholar] [CrossRef]
- Maxwell, E.; Salch, S.; Boliko, M.; Anakwe-Charles, G. Discrepancies in Lesbian, Gay, Bisexual and Transgender Patient Care and How Pharmacists Can Support an Evolved Practice. Am. J. Pharm. Educ. 2017, 81, 6181. [Google Scholar] [PubMed]
- Newsome, C.; Collip, L.; Sharon, N.; Conklin, J. Incorporating a Pharmacist in a Transgender Medical Home: An Innovative Practice Description. AJHP 2017, 74, 135–139. [Google Scholar] [PubMed]
- Cocohoba, J. Pharmacists caring for transgender persons. Am. J. Health-Syst. Pharm. 2017, 74, 170–174. [Google Scholar] [CrossRef] [PubMed]
- HealthyPeople.gov. 2020 Topics and Objectives: Lesbian, Gay, Bisexual, and Transgender Health. 2013. Available online: https://www.healthypeople.gov/2020/topics-objectives/topic/lesbian-gay-bisexual-and-transgender-health (accessed on 3 April 2018).
- Accreditation Council for Pharmacy Education. Accreditation Standards and Key Elements for the Professional Program in Pharmacy Leading to the Doctor of Pharmacy Degree. 2015. Available online: https://www.acpe-accredit.org/pdf/Standards2016FINAL.pdf (accessed on 20 July 2018).
- Association of American Medical Colleges. Integrating LGBT and DSD Content into Medical School Curricula; AAMC Videos and Resources; Association of American Medical Colleges: Washington, DC, USA, 2015; Available online: https://www.aamc.org/initiatives/diversity/449506/integratingcontent.html (accessed on 30 November 2016).
- Ostroff, J.L.; Ostroff, M.L.; Billings, S.; Nemec, E.C. Integration of transgender care into a pharmacy therapeutics curriculum. Curr. Pharm. Teach. Learn. 2018, 10, 463–468. [Google Scholar] [CrossRef] [PubMed]
- Bergmann, J.; Sams, A. Flip Your Classroom: Reach Every Student in Every Class Every Day; International Society for Technology in Education: Washington, DC, USA, 2012. [Google Scholar]
- Hamdan, N.; McKnight, P.; McKnight, K.; Arfstrom, K.M. The Flipped Learning Model: A White Paper Based on the Literature Review Titled A Review of Flipped Learning; Flipped Learning Network/Pearson/George Mason University: Fairfax, VA, USA, 2013. [Google Scholar]
- Lage, M.J.; Platt, G.J.; Treglia, M. Inverting the classroom: A gateway to creating an inclusive learning environment. J. Econ. Educ. 2000, 31, 30–43. [Google Scholar] [CrossRef]
- Reisner, S.L.; Bradford, J.; Hopwood, R.; Gonzalez, A.; Makadon, H.; Todisco, D.; Cavanaugh, T.; VanDerwarker, R.; Grasso, C.; Zaslow, S.; et al. Comprehensive transgender healthcare: The gender affirming clinical and public health model of Fenway Health. J. Urban Health 2015, 92, 584–592. [Google Scholar] [CrossRef] [PubMed]
- Flores, A.R.; Herman, J.L.; Gates, G.J.; Brown, T.N.T. How Many Adults Identify as Transgender in the United States? The Williams Institute: Los Angeles, CA, USA, 2016. [Google Scholar]
- Guidelines for the Primary and Gender-Affirming Care of Transgender and Gender Nonbinary People, 2nd ed.; Deutsch, M.B. (Ed.) University of California: San Francisco, CA, USA, 2016. [Google Scholar]
- WPATH12: World Professional Association for Transgender Health (WPATH). Standards of Care for the Health of Transsexual, Transgender, and Gender-Nonconforming People; Version 7; WPATH: Minneapolis, MN, USA, 2012.
- Frequently Asked Questions about Transgender People. National Center for Transgender Equality. 2016. Available online: transequality.org/sites/default/files/docs/resources/Understanding-Trans-Full-July-2016_0.pdf (accessed on 12 August 2017).
- LGBTQ Health Resource Center. Lavender Health. Available online: https://lavenderhealth.files.wordpress.com/2014/01/b15-gender-role-socialization.pdf (accessed on 12 August 2017).
- Nelson, E.S.; Krieger, S.L. Changes in attitudes toward homosexuality in college students: Implementation of a gay men and lesbian peer panel. J. Homosex. 1997, 33, 63–81. [Google Scholar] [CrossRef] [PubMed]
- Broockman, D.; Kalla, J. Durably reducing transphobia: A field experiment on door-to-door canvassing. Science 2016, 352, 220–224. [Google Scholar] [CrossRef] [PubMed]
- University of Waterloo, McMaster University, Trans. Ed. Educating Health-Care Students about Transgender Patients. Available online: https://uwaterloo.ca/stories/educating-health-care-students-about-transgender-patients (accessed on 30 November 2016).
- Wilkening, G.L. The current status of transgender health education in doctor of pharmacy curricula in North America. Ment. Health Clin. 2018, 7, 168–171. [Google Scholar] [CrossRef] [PubMed]
| Pre-Class Learning Objectives |
|
| In-Class Learning Objectives |
|
| I didn’t learn anything medically related to their therapies; I feel that a lot of people were afraid to ask questions since the panelists focused on how people offend them |
| I wish the transgender panel was longer |
| n/a—I wish the panel was longer though. It was very interesting. |
| I think the patient panel was pretty useful. I would suggest the patients talk about their medications and specific side effects more though rather than almost completely about their life story. That was pretty interesting tho’ and I will be able to apply it to practice. |
| I would prefer the jeopardy game be more of a team activity than individual. Also during the panel, I felt one panelist made it not fine to “mess up” and I appreciated how the other two were more open to saying as long as you try or apologize then it will be fine. |
| The panel discussion was a really helpful tool to further understand the material. It was helpful to have real patients give their experiences and helpful advice on how to appropriately and effectively approach and discuss the topic without offending them. |
| The least effective activity this week was the Small Group Discussion on Gender because no one really knew what to say. We all just kind of sat there like, “I don’t know when I knew what I was I just was.” |
| the patient panel was extremely helpful and enlightening and gave me tips for how to make things less awkward |
| The panel was great. I appreciated the counselling case because some people felt a little awkward but it was an open environment to work out any issues. |
| I wish we had used the longer class period for the panel discussion and the shorter class period for small group discussion and counseling cases |
| I understand the panel discussion and the opinions they provided, but it was a very biased liberal based panel. It’s not your fault, but this topic is very opinion oriented and hard to capture. |
| Though the panel was very insightful, it would’ve been great to hear about the panel members’ experience with medications. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Newsome, C.; Chen, L.-W.; Conklin, J. Addition of Care for Transgender-Related Patient Care into Doctorate of Pharmacy Curriculum: Implementation and Preliminary Evaluation. Pharmacy 2018, 6, 107. https://doi.org/10.3390/pharmacy6040107
Newsome C, Chen L-W, Conklin J. Addition of Care for Transgender-Related Patient Care into Doctorate of Pharmacy Curriculum: Implementation and Preliminary Evaluation. Pharmacy. 2018; 6(4):107. https://doi.org/10.3390/pharmacy6040107
Chicago/Turabian StyleNewsome, Cheyenne, Li-Wei Chen, and Jessica Conklin. 2018. "Addition of Care for Transgender-Related Patient Care into Doctorate of Pharmacy Curriculum: Implementation and Preliminary Evaluation" Pharmacy 6, no. 4: 107. https://doi.org/10.3390/pharmacy6040107
APA StyleNewsome, C., Chen, L.-W., & Conklin, J. (2018). Addition of Care for Transgender-Related Patient Care into Doctorate of Pharmacy Curriculum: Implementation and Preliminary Evaluation. Pharmacy, 6(4), 107. https://doi.org/10.3390/pharmacy6040107




