1. Introduction
Urban areas, broadly understood as cities and towns, occupy less than 5% of the Earth’s land area and are estimated to produce as much as 80% of the CO
2 pollution [
1]. The ever-increasing size of the population in urban centers, and associated anthropogenic activities with changing land use patterns, have resulted in changes of cities’ local environmental conditions which further aggravate the exiting micro-climate and, thus, create great complexities for the city dwellers [
2,
3]. These complexities that have emerged have been exhibited in the form of housing and infrastructure shortages, traffic and transportation problems, proliferation of slums and squatter settlements, paucity of water supply, inadequate latrines and drainage facilities, poor sewage and the absence of cleanliness, lack of open spaces, carbon emission, and the accumulation of waste and air pollution [
3,
4,
5,
6,
7,
8].
Air pollution is a major threat to human health. The United Nations Environment Programme has estimated that, globally, 1.1 billion people breathe in unhealthy air [
9]. Epidemiological studies have shown that concentrations of ambient air particles are associated with a wide range of effects on human health, especially on the cardio-respiratory system [
10,
11]. The World Health Organization (WHO) has estimated that urban air pollution is responsible for approximately 800,000 deaths and 4.6 million people lose their lives every year around the globe [
12]. Air pollution is associated with increased risk of acute respiratory infections (ARI), the principal cause of infant and child mortality in developing countries [
13].
Changes in the air quality are predicted to be leading to increasing rates of respiratory and allergenic diseases in many regions. Ground-level ozone and particulate matters are of particular concern [
14]. Studies demonstrate that the presence of ultrafine particles due to automobile traffic and exposure to it in the urban atmosphere can have negative health implications which can further be taken as the basis for epidemiologic study [
15]. Gurjar et al. have pointed out that urban air pollution poses a significant threat to human health in both developed and developing parts of the world [
16]. Epidemiological studies have shown that air pollution in developing countries annually accounts for tens of thousands of excess deaths and billions of dollars in medical costs and lost productivity [
17]. Brashier et al., has hypothesised that non-communicable respiratory morbidities such as asthma and chronic obstructive pulmonary diseases (COPD) are rapidly rising and can emerge as leading causes of mortality worldwide [
18]. It is also being predicted that the four leading causes of death in the world in 2030 will be ischaemic heart disease, cerebrovascular disease (stroke), COPD, and lower respiratory infections (mainly pneumonia) [
19].
Epidemiological research on air pollution over the past 20 years has demonstrated cardio-respiratory health effects ranging from minor respiratory symptoms to increased hospital admission and mortality [
20]. Amongst the air pollutants, nitrogen dioxide (NO
2) is highly reactive and has been responsible for bronchitis and pneumonia, and also increasing susceptibility to respiratory infections. A review of epidemiological studies suggests that children exposed to NO
2 are at increased risk of respiratory illness [
21]. NO
2 has also been associated with daily mortality in children less than five years old [
22]. Chronic bronchitis and individuals with emphysema (respiratory disorder) or other chronic respiratory diseases may also be sensitive to NO
2 exposure [
23]. Smith demonstrates that around 40–60% of ARI are due to environmental causes [
24]. There is growing evidence that the poor are affected relatively more by ambient air pollution due to greater exposure, weaker biological defence mechanisms against air pollution, inadequate nutrition, and limited access to medical care [
25,
26,
27].
Looking at the growing urban spaces associated with increasing number of city inhabitants, demand for higher consumption and the plan to build 100 new smart cities in India; it is needed to take initiative with a vision and commitment to the
Sustainable Cities and Human Settlements goal (SHS) with targets that cover urban planning, resilience preparedness, urban sustainability, health and wellbeing, and the integration of housing, transportation, and open spaces [
28,
29,
30]. Future development of low-carbon cities based on alternative non-polluting energy resources should be a priority concern [
31]. With this little background, the subject matter of the current paper has been framed under three broader headings; namely, status of the urban environment in terms of air quality, health outcomes of air pollution, and addressing some suitable measures with a view to mitigate the menace of air pollution to pave the way for bringing sustainable urban development to Kolkata.
2. Study Area
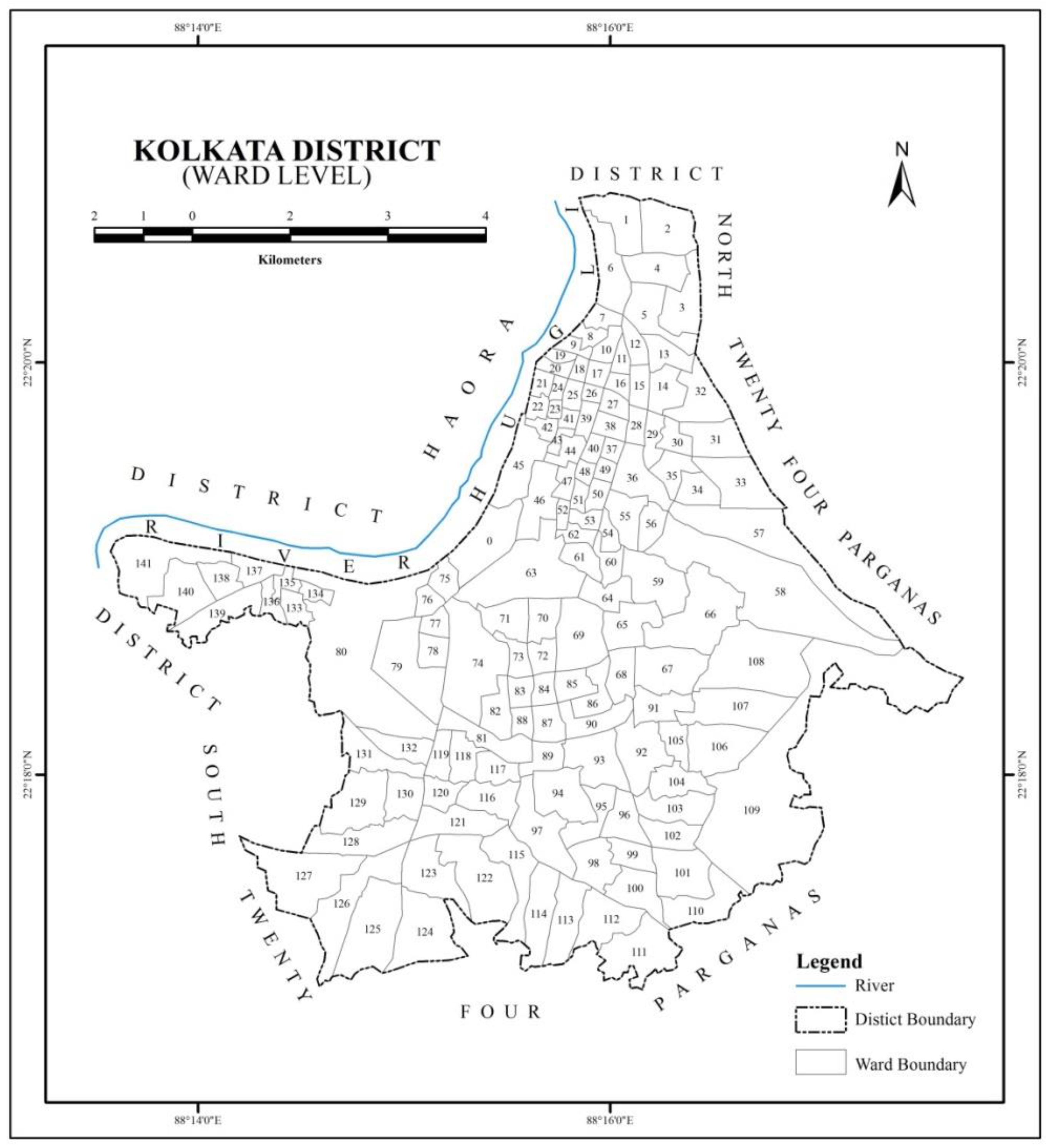
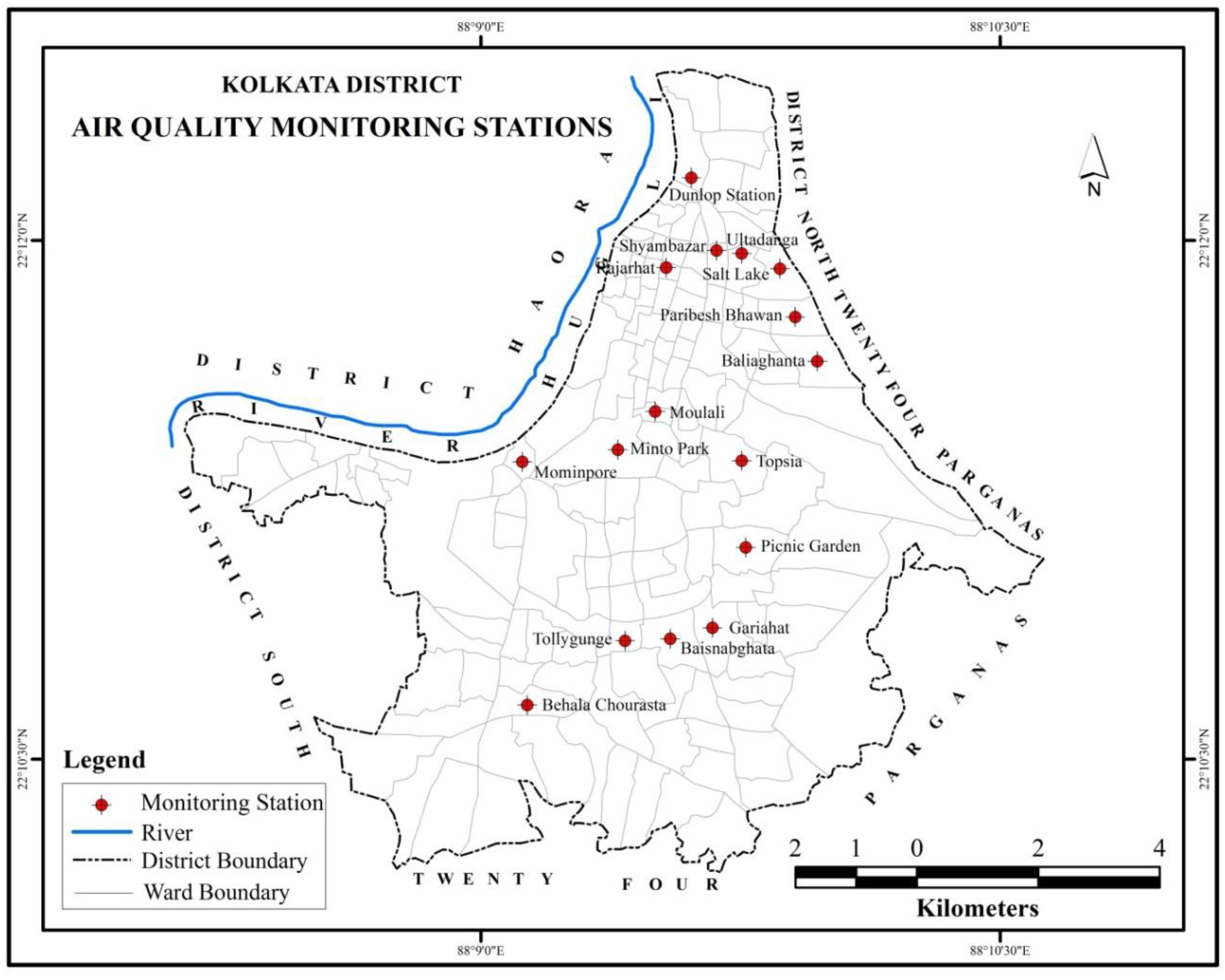
The study has been conducted in Kolkata, the capital city of West Bengal state in India (
Figure 1). According to the Census of India (2011), Kolkata had 4.5 million population, with the urban agglomeration, which comprises the city and its suburbs, home to approximately 14.1 million people, which makes it the third most densely populated metropolitan area in the country [
32]. The first count is for Kolkata City (4.5 million), which is under the Kolkata Municipal Corporation (KMC), while the second count (14.1 million) is for the Kolkata Metropolitan Authority (KMA), which comprises the city (KMC) and its suburbs. The city of Kolkata has been dubbed as one of the most unplanned and polluted cities in the world [
33]. A study in comparison of air quality data among four metropolitan areas in India indicates a higher pollution level in Kolkata in comparison to Mumbai and Chennai, and is close to Delhi [
34]. It has also been termed as the dusty city [
2]. Air pollution in Kolkata becomes acute during winter, when pollution ranges higher than at other times [
35]. On the other hand, the worst-polluted traffic intersections double the city's average pollutants during busy hours [
36].
A joint study by Chittaranjan National Cancer Institute (CNCI), West Bengal Department of Environment and the Central Pollution Control Board (CPCB) has found that around 70% of people in the city of Kolkata suffer from respiratory disorders caused by air pollution [
37]. In 1995, an estimated 10,647 premature deaths were attributed to air pollution in Kolkata [
38,
39]. Studies have demonstrated that children inhaling polluted air in Kolkata suffer from adverse lung reactions and genetic abnormalities in exposed lung tissues [
40]. Approximately 47% of Kolkata’s population suffers from lower respiratory tract symptoms with the lungs of city residents being approximately seven times more burdened compared to their rural counterparts due to air pollution [
39,
41,
42]. Other air pollution-related health problems, including haematological abnormalities, impaired liver function, genetic changes, and neurobehavioral problems, are found to be more prevalent amongst those categories of workers exposed to high levels of vehicular emission. They include roadside hawkers, traffic policemen, and taxi and auto drivers [
37].
2.1 Sources of Air Pollution in Kolkata
Several factors cause air pollution in Kolkata and among them the main factor is transportation [
43,
44], where the abundance of poorly-maintained vehicles, use of petrol fuel, and poor controlling are making transportation the major air polluting sector [
45,
46]. Additionally, there are three thermal power plants operating in and around Kolkata, and some small-scale industries which also affects the air quality [
47]. An analysis of different sources of air pollution in Kolkata has revealed that motor vehicles are the leading contributor to air pollution (51.4%) which is followed by industry (24.5%) and dust particles (21.1%), respectively (
Table 1) [
48].
The vehicular pollution in Kolkata is attributed to a large number of automobiles plying daily over only 6% available road space, causing congestion which reduces the average vehicular speed and also results in heavy vehicular emission [
49]. The number of vehicles has a growth of about 2.00 times, numbering to 1.20 million in 2011 from 0.73 million in 1996 [
50]. The vehicular population in Kolkata has increased at an annual growth rate of 4%. Private cars have increased from 0.26 million in 2000 to 0.65 million in 2011, which indicates a 2.5 times increase [
51]. The heavy concentration of private motor vehicles has been one of the key reasons for congestion, increased travel times, pollution, and accidents. In terms of available surface road length, Kolkata has the least coverage, with about 1416 km, whereas the vehicular density is one of the highest, nearing 823/km [
52].
5. Conclusions
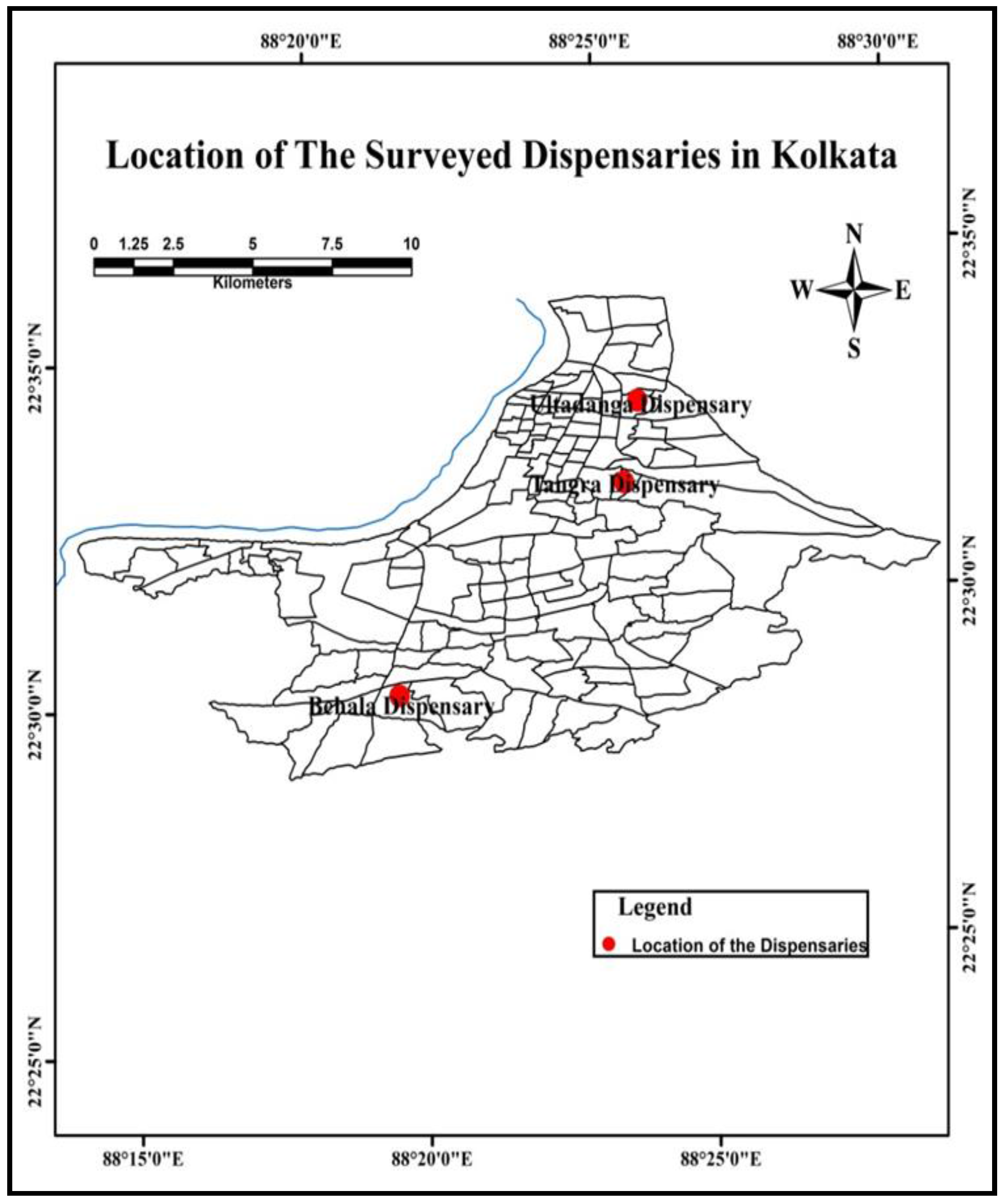
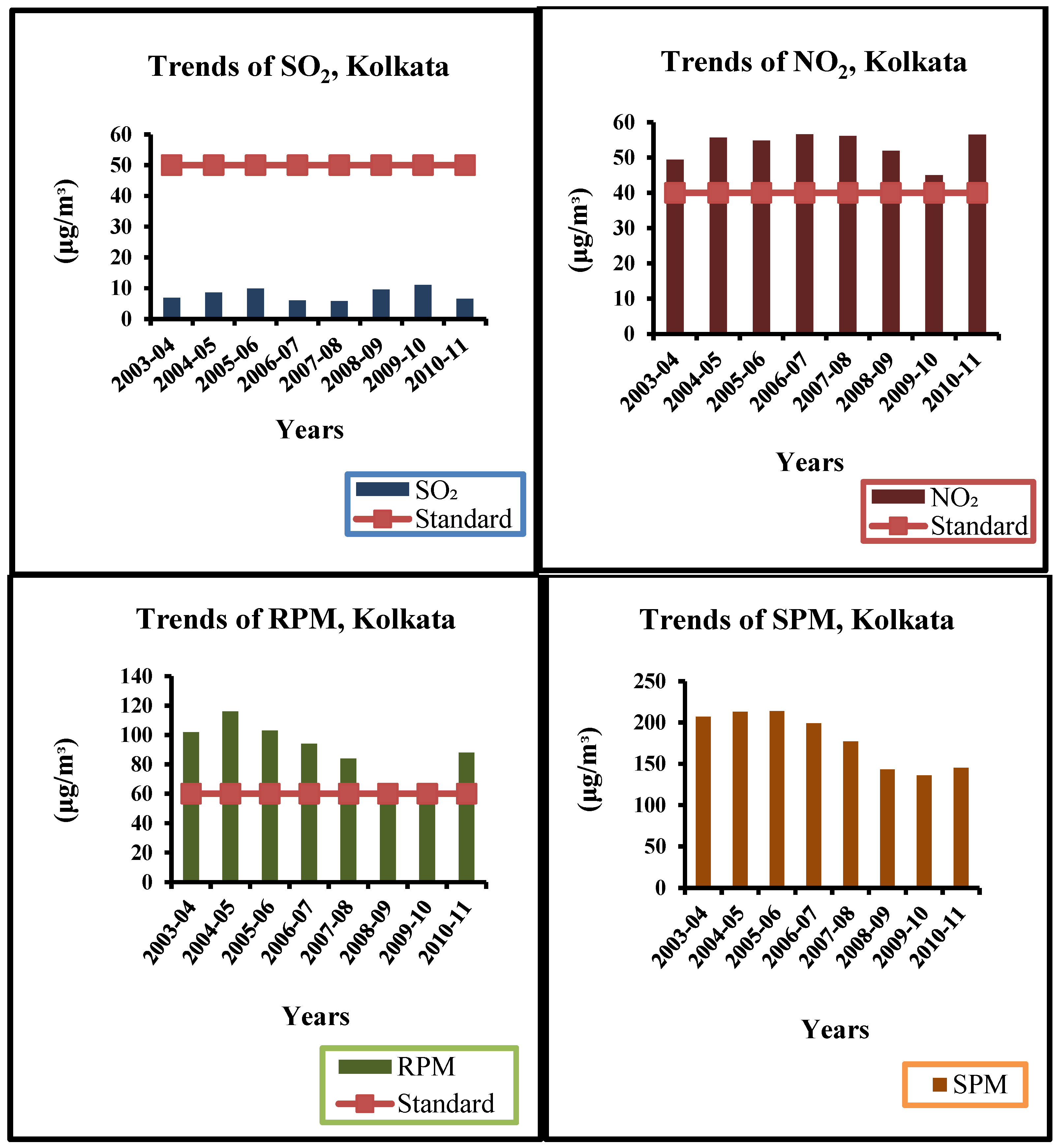
The concentration of RPM and NO2 in the ambient air has been found to have violated the national standards and exceeded the NAAQS. While interpreting the pollution concentration, most of the monitoring stations have been found to fall under the critical and high pollution categories. The pollution categories, thus, emerged have been used for the selection of dispensaries to conduct the health survey. While evaluating the responses (mainly patients with respiratory diseases which share 85%) from the three surveyed dispensaries, it emerges that people who reside in slums are found to be have a significant share among the total participants. It may not be a sound interpretation to say that those who are residing in slums are exposed more to the pollution, which is why they experience a greater number of diseases of respiratory origin. There may be some other causes towards their susceptibility to the kind of diseases the study is evaluating, and for that further exploration could be required. Along with exposure; poor living conditions, less awareness towards avoiding pollution sources, lack of knowledge about pollution, indoor cooking, and poor resistance to air pollution could be some of the reasons that make slum-dwellers susceptible to the pollution-induced diseases. Cooking inside the living room has emerged as the major issue practiced by those living in the slums of Kolkata as expressed in this study. Although the study has not been framed to assess the susceptibility of people to the indoor pollution, it could infer the level of vulnerability the slum-dwellers are having while being exposed to the indoor gases released due to domestic fuel exhaust. As the study was made to assess the disease frequencies of respiratory origin at dispensaries, it resulted in the following disease types, i.e., ARI, COPD, Influenza, UTRI, bronchitis, asthma, AFB, etc. The cases with ARI infection have emerged as the leading disease type. The study thus carried out has talked about the cases and not included the control group, which may be taken as a drawback. In the end, it would be worthwhile to suggest introducing a comprehensive framework for slum development with focusses on their health and habitation so that they could be brought under mainstream city living, which may further help in bringing sustainable urban development in Kolkata.