Medicinal Plants for Treating Musculoskeletal Disorders among Karen in Thailand
Abstract
1. Introduction
2. Results
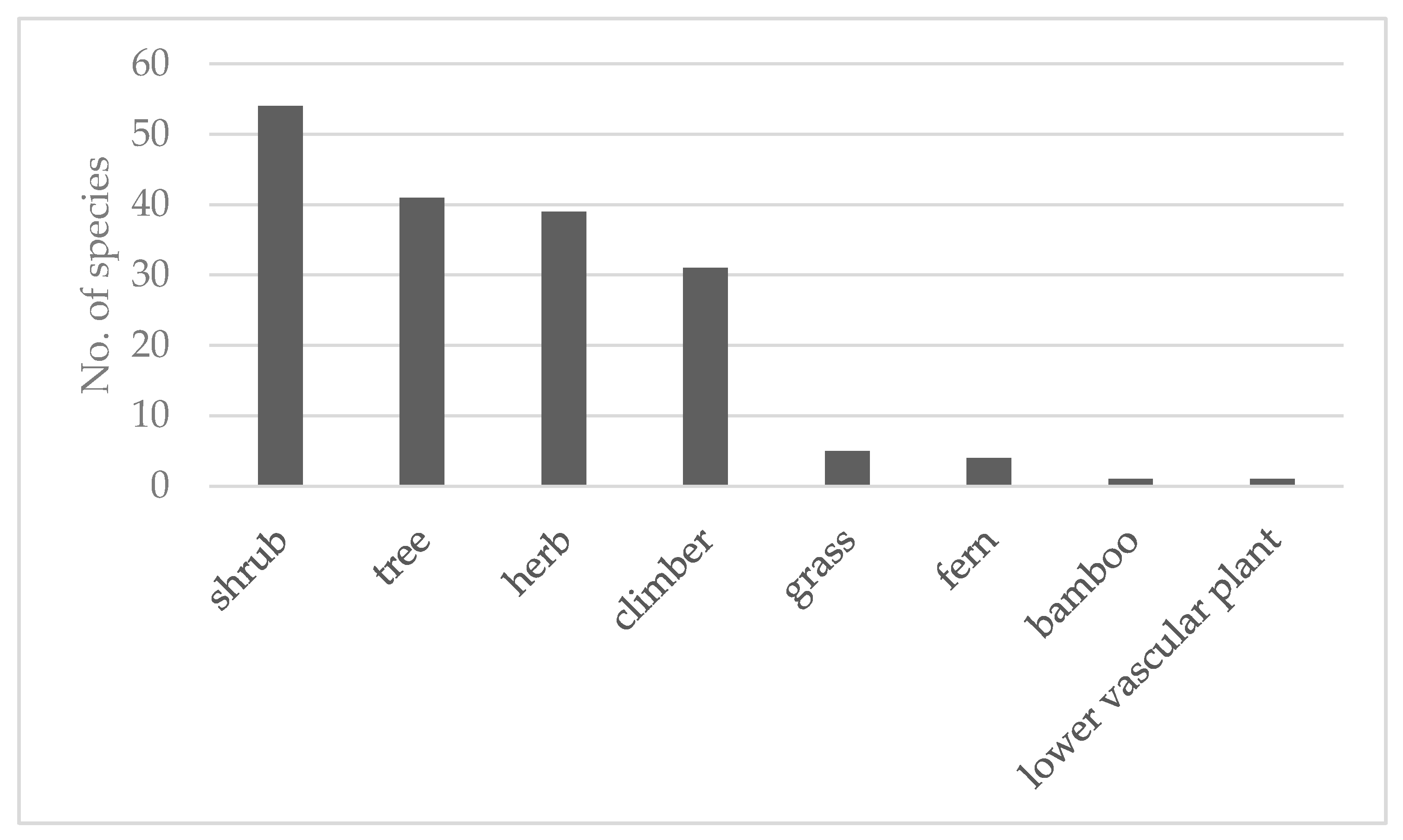
2.1. Medicinal Plant Diversity
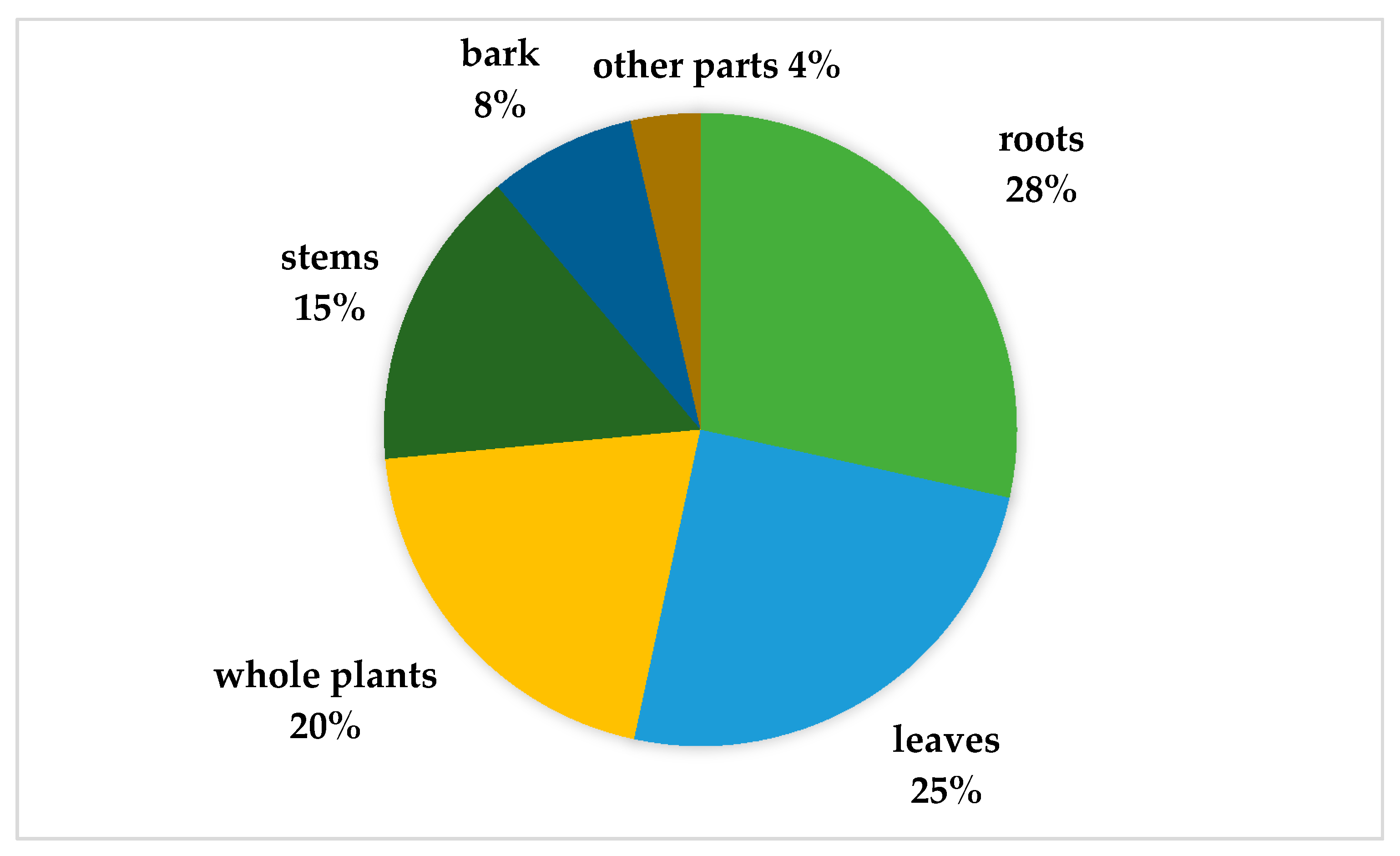
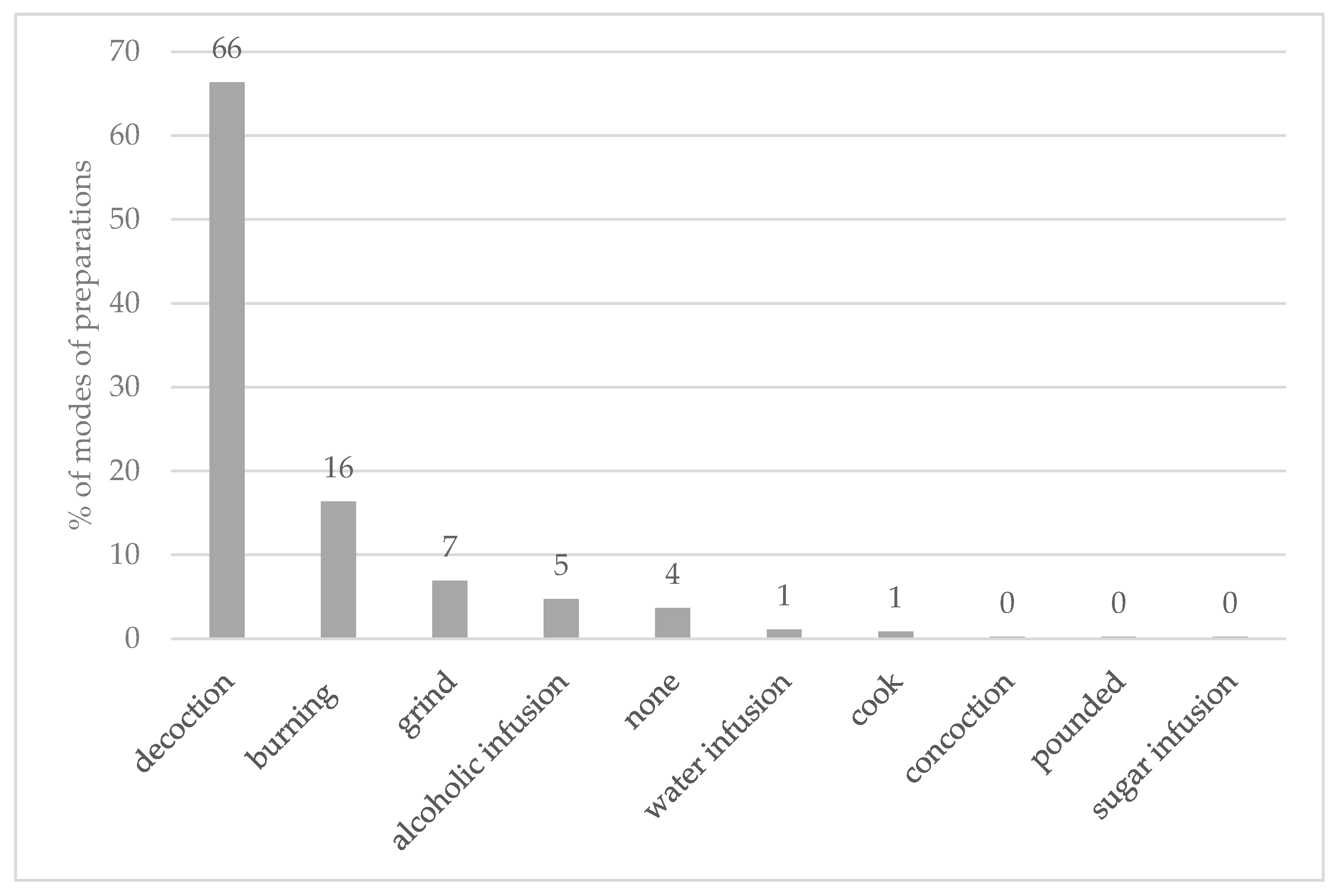
2.2. Plant Part Used, Preparation and Routes of Administration
2.3. Ethnobotanical Indices: UV, RFC, and ICF
2.3.1. Use Values (UV) of the Ethnomedicinal Plants for Treating MSDs
2.3.2. The Relative Frequency of Citations (RFC) of the Ethnomedicinal Plants
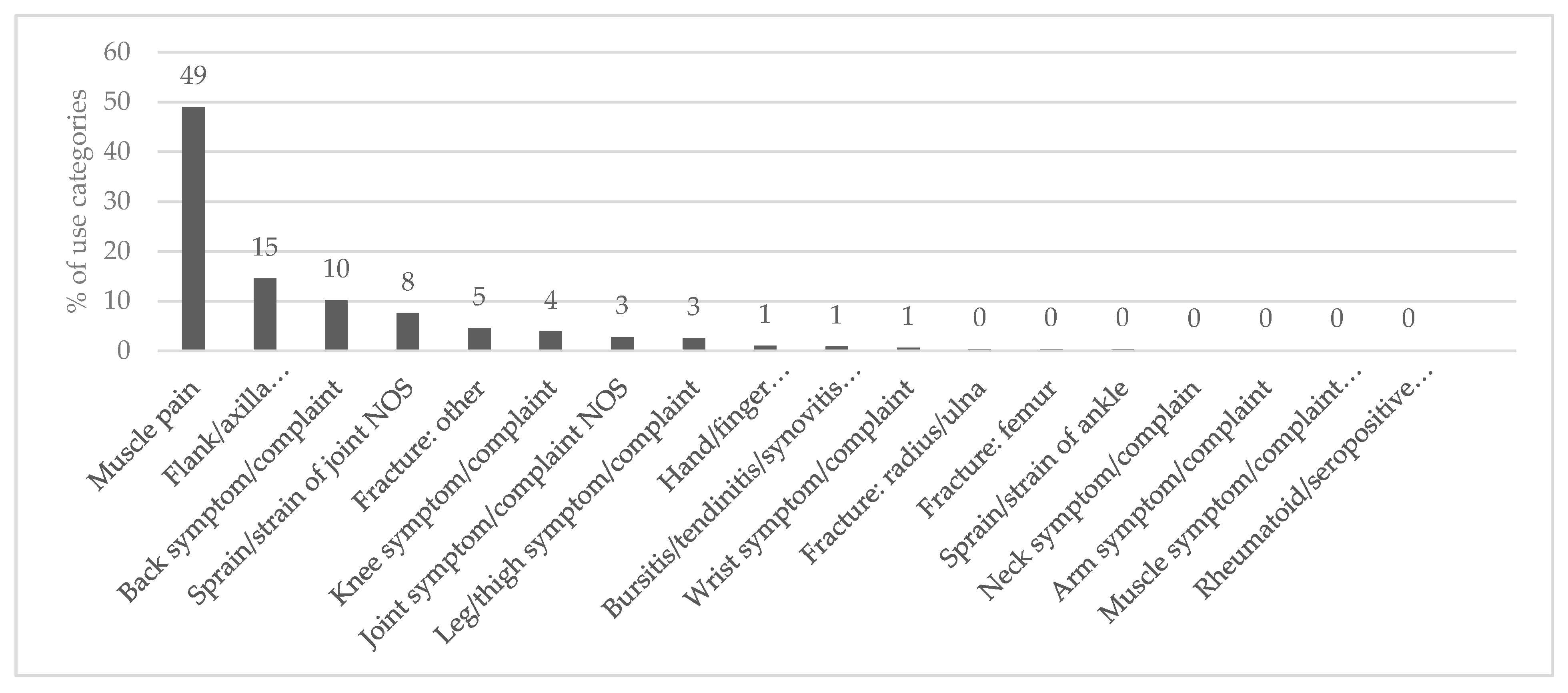
2.3.3. The Information Consensus Factors (ICF) of MSD Categories
3. Discussion
3.1. Diversity of Medicinal Plant Used to Treat MSD
3.2. Plant Utilization: Parts, Preparation, and Routes of Administration
3.3. Important Disorder Categories
3.4. Important Plants for Treating MSD
3.4.1. Most Preferred Species for Treating MSD
3.4.2. Important Species in Important Disorders
4. Materials and Methods
4.1. Data Source
4.2. Data Organization
4.3. Data Analysis
4.3.1. Use Value (UV) Modified from:
4.3.2. Relative Frequency of Citation (RFC)
4.3.3. Informant Consensus Factor (ICF)
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pieroni, A.; Quave, C.L. Traditional pharmacopoeias and medicines among Albanians and Italians in southern Italy: A comparison. J. Ethnopharmacol. 2005, 101, 258–270. [Google Scholar] [CrossRef]
- Lamxay, V.; de Boer, H.J.; Björk, L. Traditions and plant use during pregnancy, childbirth and postpartum recovery by the Kry ethnic group in Lao PDR. J. Ethnobiol. Ethnomed. 2011, 7, 14. [Google Scholar] [CrossRef]
- WHO. WHO Traditional Medicine Strategy 2002–2005; World Health Organization: Geneva, Switzerland, 2002; p. 74. [Google Scholar]
- Lu, Y.; Hernandez, P.; Abegunde, D.; Edejer, T. The World Medicines Situation 2011. Medicine Expenditures; World Health Organization: Geneva, Switzerland, 2011. [Google Scholar]
- Bussmann, R.W. The globalization of traditional medicine in Northern Perú: From shamanism to molecules. Evid. Based Complement. Altern. Med. 2013, 2013. [Google Scholar] [CrossRef]
- Asase, A.; Kadera, M.L. Herbal medicines for child healthcare from Ghana. J. Herb. Med. 2014, 4, 24–36. [Google Scholar] [CrossRef]
- Giday, K.; Lenaerts, L.; Gebrehiwot, K.; Yirga, G.; Verbist, B.; Muys, B. Ethnobotanical study of medicinal plants from degraded dry afromontane forest in northern Ethiopia: Species, uses and conservation challenges. J. Herb. Med. 2016, 6, 96–104. [Google Scholar] [CrossRef]
- Kpodar, M.S.; Lawson-Evi, P.; Bakoma, B.; Eklu-Gadegbeku, K.; Agbonon, A.; Aklikokou, K.; Gbeassor, M. Ethnopharmacological survey of plants used in the treatment of diabetes mellitus in south of Togo (Maritime Region). J. Herb. Med. 2015, 5, 147–152. [Google Scholar] [CrossRef]
- Fisher, P.; Ward, A. Complementary medicine in Europe. Br. Med. J. 1994, 309, 107–111. [Google Scholar] [CrossRef] [PubMed]
- Malik, K.; Ahmad, M.; Zhang, G.; Rashid, N.; Zafar, M.; Sultana, S.; Shah, S.N. Traditional plant based medicines used to treat musculoskeletal disorders in Northern Pakistan. Eur. J. Integr. Med. 2018, 19, 17–64. [Google Scholar] [CrossRef]
- Payyappallimana, U. Role of traditional medicine in primary health care: An overview of perspectives and challenging. Yokohama J. Soc. Sci. 2010, 14, 723–743. [Google Scholar]
- Puntumetakul, R.; Siritaratiwat, W.; Boonprakob, Y.; Eungpinichpong, W.; Puntumetakul, M. Prevalence of musculoskeletal disorders in farmers: Case study in Sila, Muang Khon Kaen, Khon Kaen province. J. Med. Tech. Phys. Ther. 2011, 23, 297–303. [Google Scholar]
- Hignett, S.; Fray, M. Manual handling in healthcare. In Proceedings of the 1st Conference of the Federation of the European Ergonomics Societies (FEES), Bruges, Belgium, 10–12 October 2010; pp. 10–12. [Google Scholar]
- Musculoskeletal Conditions. 2019. Available online: https://www.who.int/news-room/fact-sheets/detail/musculoskeletal-conditions (accessed on 5 February 2019).
- Musculoskeletal Health in Europe, Report v5.0 (internet). 2012. Musculoskeletal Health in Europe, Report v5.0. eumusc.net. Available online: http://www.eumusc.net/myuploaddata/files/musculoskeletal health in Europe report v5.pdf (accessed on 5 February 2019).
- Brennan-Olsen, S.L.; Cook, S.; Leech, M.; Bowe, S.J.; Kowal, P.; Naidoo, N.; Ackerman, I.; Page, R.; Hosking, S.; Pasco, J. Prevalence of arthritis according to age, sex and socioeconomic status in six low and middle income countries: Analysis of data from the World Health Organization study on global AGEing and adult health (SAGE) Wave 1. BMC Musculoskelet. Disord. 2017, 18, 271. [Google Scholar] [CrossRef] [PubMed]
- Tümen, İ.; Akkol, E.K.; Taştan, H.; Süntar, I.; Kurtca, M. Research on the antioxidant, wound healing, and anti-inflammatory activities and the phytochemical composition of maritime pine (Pinus pinaster Ait). J. Ethnopharmacol. 2018, 211, 235–246. [Google Scholar] [CrossRef] [PubMed]
- Rosecrance, J.; Rodgers, G.; Merlino, L. Low back pain and musculoskeletal symptoms among Kansas farmers. Am. J. Ind. Med. 2006, 49, 547–556. [Google Scholar] [CrossRef] [PubMed]
- Hartman, E.; Oude Vrielink, H.H.; Huirne, R.B.; Metz, J.H. Risk factors for sick leave due to musculoskeletal disorders among self-employed Dutch farmers: A case-control study. Am. J. Ind. Med. 2006, 49, 204–214. [Google Scholar] [CrossRef] [PubMed]
- Whelan, S.; Ruane, D.J.; McNamara, J.; Kinsella, A.; McNamara, A. Disability on Irish farms—A real concern. J. Agromed. 2009, 14, 157–163. [Google Scholar] [CrossRef] [PubMed]
- Collins, J.; O’Sullivan, L. Psychosocial risk exposures and musculoskeletal disorders across working-age males and females. Hum. Factors Ergon. Man. Serv. Ind. 2010, 20, 272–286. [Google Scholar] [CrossRef]
- Area of Holding by Land Use. 2013. Available online: http://web.nso.go.th/en/census/agricult/cen_agri03.htm (accessed on 20 February 2019).
- Holmberg, S.; Stiernström, E.-L.; Thelin, A.; Svärdsudd, K. Musculoskeletal symptoms among farmers and non-farmers: A population-based study. Int. J. Occup. Environ. Health 2002, 8, 339–345. [Google Scholar] [CrossRef]
- Walker-Bone, K.; Palmer, K. Musculoskeletal disorders in farmers and farm workers. Occup. Med. 2002, 52, 441–450. [Google Scholar] [CrossRef]
- Luangwilai, T.; Norkaew, S.; Siriwong, W. Factors associated with musculoskeletal disorders among rice farmers: Cross sectional study in Tarnlalord sub-district, Phimai district, Nakhonratchasima province, Thailand. J. Health Res. 2014, 28, S85–S91. [Google Scholar]
- Gomez, M.; Hwang, S.; Stark, A.; May, J.; Hallman, E.; Pantea, C. An analysis of self-reported joint pain among New York farmers. J. Agric. Saf. Health 2003, 9, 143. [Google Scholar] [CrossRef]
- Douphrate, D.I.; Nonnenmann, M.W.; Rosecrance, J.C. Ergonomics in industrialized dairy operations. J. Agromed. 2009, 14, 406–412. [Google Scholar] [CrossRef] [PubMed]
- Kantasrila, R. Ehtnobotany of Karen at Ban Wa Do Kro, Mae Song Sub-District, Tha Song Yang District, Tak Province. Master’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 2016. [Google Scholar]
- Kaewsangsai, S. Ethnobotany of Karen in the Royal Project Extended Area Khun Tuen Noi Village, Omkoi District, Chiang Mai Province. Master’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 2017. [Google Scholar]
- Sinphiphat, S. Hill Tribe People in Thailand; Hill Tribe Research Institute Department of Public Welfare, Ministry of Interior: Bangkok, Thailand, 1983. [Google Scholar]
- Junsongduang, A.; Balslev, H.; Inta, A.; Jampeetong, A.; Wangpakapattanawong, P. Medicinal plants from swidden fallows and sacred forest of the Karen and the Lawa in Thailand. J. Ethnobiol. Ethnomed. 2013, 9, 44. [Google Scholar] [CrossRef] [PubMed]
- Wonca International Classification Committee (WICC). International Classification of Primary Care, 2nd ed.; Oxford University Press: Oxford, UK, 1998. [Google Scholar]
- Phumthum, M.; Srithi, K.; Inta, A.; Junsongduang, A.; Tangjitman, K.; Pongamornkul, W.; Trisonthi, C.; Balslev, H. Ethnomedicinal plant diversity in Thailand. J. Ethnopharmacol. 2018, 214, 90–98. [Google Scholar] [CrossRef] [PubMed]
- Prabhu, S.; Vijayakumar, S.; Yabesh, J.M.; Ravichandran, K.; Sakthivel, B. Documentation and quantitative analysis of the local knowledge on medicinal plants in Kalrayan hills of Villupuram district, Tamil Nadu, India. J. Ethnopharmacol. 2014, 157, 7–20. [Google Scholar] [CrossRef] [PubMed]
- Ong, H.G.; Kim, Y.-D. Quantitative ethnobotanical study of the medicinal plants used by the Ati Negrito indigenous group in Guimaras island, Philippines. J. Ethnopharmacol. 2014, 157, 228–242. [Google Scholar] [CrossRef]
- Verma, R.K. An ethnobotanical study of plants used for the treatment of livestock diseases in Tikamgarh District of Bundelkhand, Central India. Asian Pac. J. Trop. Biomed. 2014, 4, S460–S467. [Google Scholar] [CrossRef]
- Parthiban, R.; Vijayakumar, S.; Prabhu, S.; Yabesh, J.G.E.M. Quantitative traditional knowledge of medicinal plants used to treat livestock diseases from Kudavasal taluk of Thiruvarur district, Tamil Nadu, India. Rev. Bras. Farmacogn. 2016, 26, 109–121. [Google Scholar] [CrossRef]
- Sreekeesoon, D.P.; Mahomoodally, M.F. Ethnopharmacological analysis of medicinal plants and animals used in the treatment and management of pain in Mauritius. J. Ethnopharmacol. 2014, 157, 181–200. [Google Scholar] [CrossRef]
- Sutjaritjai, N.; Wangpakapattanawong, P.; Balslev, H.; Inta, A. Traditional uses of Leguminosae among the Karen in Thailand. Plant J. 2019, 8, 600. [Google Scholar] [CrossRef]
- Marles, R.J.; Farnsworth, N.R. Antidiabetic plants and their active constituents. Phytomedicine 1995, 2, 137–189. [Google Scholar] [CrossRef]
- Ong, H.G.; Kim, Y.D. Medicinal plants for gastrointestinal diseases among the Kuki-Chin ethnolinguistic groups across Bangladesh, India, and Myanmar: A comparative and network analysis study. J. Ethnopharmacol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Pooma, R.; Suddee, S. Tem Smitinand’s Thai Plant Names, Revised; The Office of the Forest Herbarium, Department of National Parks, Wildlife and Plant Conservation: Bangkok, Thailand, 2014.
- Stevens, P.F. Angiosperm Phylogeny Website. Version 14. 2001. Available online: http://www.mobot.org/MOBOT/research/APweb/ (accessed on 18 November 2019).
- Addo-Fordjour, P.; Kofi Anning, A.; Durosimi Belford, E.J.; Akonnor, D. Diversity and conservation of medicinal plants in the Bomaa community of the Brong Ahafo region, Ghana. Med. Plant Res. 2008, 2, 226–233. [Google Scholar]
- Sanz-Biset, J.; Campos-de-la-Cruz, J.; Epiquién-Rivera, M.A.; Canigueral, S. A first survey on the medicinal plants of the Chazuta valley (Peruvian Amazon). J. Ethnopharmacol. 2009, 122, 333–362. [Google Scholar] [CrossRef] [PubMed]
- Srithi, K.; Balslev, H.; Wangpakapattanawong, P.; Srisanga, P.; Trisonthi, C. Medicinal plant knowledge and its erosion among the Mien (Yao) in northern Thailand. J. Ethnopharmacol. 2009, 123, 335–342. [Google Scholar] [CrossRef] [PubMed]
- Panyaphu, K.; Van On, T.; Sirisa-Ard, P.; Srisa-Nga, P.; ChansaKaow, S.; Nathakarnkitkul, S. Medicinal plants of the Mien (Yao) in Northern Thailand and their potential value in the primary healthcare of postpartum women. J. Ethnopharmacol. 2011, 135, 226–237. [Google Scholar] [CrossRef] [PubMed]
- Ouelbani, R.; Bensari, S.; Mouas, T.N.; Khelifi, D. Ethnobotanical investigations on plants used in folk medicine in the regions of Constantine and Mila (North-East of Algeria). J. Ethnopharmacol. 2016, 194, 196–218. [Google Scholar] [CrossRef] [PubMed]
- Yemele, M.; Telefo, P.; Lienou, L.; Tagne, S.; Fodouop, C.; Goka, C.; Lemfack, M.; Moundipa, F. Ethnobotanical survey of medicinal plants used for pregnant women’ s health conditions in Menoua division-West Cameroon. J. Ethnopharmacol. 2015, 160, 14–31. [Google Scholar] [CrossRef]
- Pompermaier, L.; Marzocco, S.; Adesso, S.; Monizi, M.; Schwaiger, S.; Neinhuis, C.; Stuppner, H.; Lautenschläger, T. Medicinal plants of northern Angola and their anti-inflammatory properties. J. Ethnopharmacol. 2018, 216, 26–36. [Google Scholar] [CrossRef]
- Fortini, P.; Di Marzio, P.; Guarrera, P.; Iorizzi, M. Ethnobotanical study on the medicinal plants in the Mainarde Mountains (central-southern Apennine, Italy). J. Ethnopharmacol. 2016, 184, 208–218. [Google Scholar] [CrossRef]
- Mukungu, N.; Abuga, K.; Okalebo, F.; Ingwela, R.; Mwangi, J. Medicinal plants used for management of malaria among the Luhya community of Kakamega East sub-County, Kenya. J. Ethnopharmacol. 2016, 194, 98–107. [Google Scholar] [CrossRef]
- Koch, M.; Kehop, D.A.; Kinminja, B.; Sabak, M.; Wavimbukie, G.; Barrows, K.M.; Matainaho, T.K.; Barrows, L.R.; Rai, P.P. An ethnobotanical survey of medicinal plants used in the East Sepik province of Papua New Guinea. J. Ethnobiol. Ethnomed. 2015, 11, 79. [Google Scholar] [CrossRef] [PubMed]
- Asowata-Ayodele, A.M.; Afolayan, A.J.; Otunola, G.A. Ethnobotanical survey of culinary herbs and spices used in the traditional medicinal system of Nkonkobe Municipality, Eastern Cape, South Africa. S. Afr. J. Bot. 2016, 104, 69–75. [Google Scholar] [CrossRef]
- Giday, M.; Asfaw, Z.; Woldu, Z. Medicinal plants of the Meinit ethnic group of Ethiopia: An ethnobotanical study. J. Ethnopharmacol. 2009, 124, 513–521. [Google Scholar] [CrossRef] [PubMed]
- Bhattarai, S.; Chaudhary, R.P.; Taylor, R.S. Ethnomedicinal plants used by the people of Manang district, central Nepal. J. Ethnobiol. Ethnomed. 2006, 2, 41. [Google Scholar] [CrossRef]
- Ashraf, M.U.; Muhammad, G.; Hussain, M.A.; Bukhari, S.N. Cydonia oblonga M.—A medicinal plant rich in phytonutrients for pharmaceuticals. Front. Pharmacol. 2016, 7, 163. [Google Scholar] [CrossRef]
- Anderson, E.F. Plant and People of the Golden Triangle: Ethnobotany of the Hill Tribe of the Northern Thailand; Whitman College and Desert Botanical Garden: Portland, OR, USA, 1993. [Google Scholar]
- Simbo, D.J. An ethnobotanical survey of medicinal plants in Babungo, Northwest Region, Cameroon. J. Ethnobiol. Ethnomed. 2010, 6, 8. [Google Scholar] [CrossRef]
- Liu, Y.; Dao, Z.; Yang, C.; Liu, Y.; Long, C. Medicinal plants used by Tibetans in Shangri-la, Yunnan, China. J. Ethnobiol. Ethnomed. 2009, 5, 15. [Google Scholar] [CrossRef]
- Coe, F.G.; Anderson, G.J. Ethnobotany of the Garifuna of eastern Nicaragua. Econ. Bot. 1996, 50, 71–107. [Google Scholar] [CrossRef]
- Ayyanar, M.; Ignacimuthu, S. Ethnobotanical survey of medicinal plants commonly used by Kani tribals in Tirunelveli hills of Western Ghats, India. J. Ethnopharmacol. 2011, 134, 851–864. [Google Scholar] [CrossRef]
- Balangcod, T.D.; Balangcod, A.K.D. Ethnomedical knowledge of plants and healthcare practices among the Kalanguya tribe in Tinoc, Ifugao, Luzon, Philippines. Indian J. Tradit. Knowl. 2011, 10, 227–238. [Google Scholar]
- Panyadee, P.; Balslev, H.; Wangpakapattanawong, P.; Inta, A. Medicinal plants in homegardens of four ethnic groups in Thailand. J. Ethnopharmacol. 2019, 239, 111927. [Google Scholar] [CrossRef] [PubMed]
- Waruruai, J.; Sipana, B.; Koch, M.; Barrows, L.R.; Matainaho, T.K.; Rai, P.P. An ethnobotanical survey of medicinal plants used in the Siwai and Buin districts of the Autonomous Region of Bougainville. J. Ethnopharmacol. 2011, 138, 564–577. [Google Scholar] [CrossRef] [PubMed]
- Jorim, R.Y.; Korape, S.; Legu, W.; Koch, M.; Barrows, L.R.; Matainaho, T.K.; Rai, P.P. An ethnobotanical survey of medicinal plants used in the eastern highlands of Papua New Guinea. J. Ethnobiol. Ethnomed. 2012, 8, 47. [Google Scholar] [CrossRef] [PubMed]
- Baruah, A.; Bordoloi, M.; Baruah, H.P.D. Aloe vera: A multipurpose industrial crop. Ind. Crops Prod. 2016, 94, 951–963. [Google Scholar] [CrossRef]
- Jahandideh, M.; Hajimehdipoor, H.; Mortazavi, S.A.; Dehpour, A.; Hassanzadeh, G. A wound healing formulation based on Iranian traditional medicine and its HPTLC fingerprint. Iran. J. Pharm. Res. 2016, 15, 149. [Google Scholar]
- Cavero, R.Y.; Calvo, M.I. Medicinal plants used for musculoskeletal disorders in Navarra and their pharmacological validation. J. Ethnopharmacol. 2015, 168, 255–259. [Google Scholar] [CrossRef]
- Moskowitz, R.W. Role of collagen hydrolysate in bone and joint disease. Semin. Arthritis Rheu. 2000, 30, 87–99. [Google Scholar] [CrossRef]
- Inta, A.; Trisonthi, P.; Trisonthi, C. Analysis of traditional knowledge in medicinal plants used by Yuan in Thailand. J. Ethnopharmacol. 2013, 149, 344–351. [Google Scholar] [CrossRef]
- Bennett, B.C.; Husby, C.E. Patterns of medicinal plant use: An examination of the Ecuadorian Shuar medicinal flora using contingency table and binomial analyses. J. Ethnopharmacol. 2008, 116, 422–430. [Google Scholar] [CrossRef]
- Inta, A. Ethnobotany and Crop Diversity of Tai Lue and Akha Communities in the Upper Northern Thailand and the Xishuangbanna Dai Autonomous Prefecture, China. Ph.D. Thesis, Chiang Mai Graduate School, Chiang Mai University, Chiang Mai, Thailand, 2008. [Google Scholar]
- Srithi, K. Comparative Ethnobotany in Nan Province, Thailand. Ph.D. Thesis, Chiang Mai University, Chiang Mai, Thailand, 2012. [Google Scholar]
- Xiao, H.H.; Zhang, Y.; Cooper, R.; Yao, X.S.; Wong, M.S. Phytochemicals and potential health effects of Sambucus williamsii Hance (Jiegumu). Chin. Med. 2016, 11, 36. [Google Scholar] [CrossRef]
- Lemmens, R.H.M.J.; Bunyapraphatsara, N. Plant Resources of South-East Asia No. 12: Medicinal and poisonous plants 3; Prosea Foundation: Bogor, Indonesia, 2003; p. 664. [Google Scholar]
- Barros, L.; Cabrita, L.; Boas, M.V.; Carvalho, A.M.; Ferreira, I.C. Chemical, biochemical and electrochemical assays to evaluate phytochemicals and antioxidant activity of wild plants. Food Chem. 2011, 127, 1600–1608. [Google Scholar] [CrossRef]
- De Padua, L.S.; Bubypraphatsara, N.; Lemmens, R.H.M.J. Plant Resources of South-East Asia No. 12: Medicinal and Poisonous Plants I.; Backhuys Publishers: Leiden, The Netherlands, 1999; p. 711. [Google Scholar]
- Areekun, S.; Onlamun, A. Food Plants and Medicinal Plants of Ethnic Groups in Doi Ang Khang, Chiangmai. Agricultural Development Projects; Kasetsart University: Bankok, Thailand, 1978. (In Thai) [Google Scholar]
- Pang, Y.; Wang, D.; Fan, Z.; Chen, X.; Yu, F.; Hu, X.; Wang, K.; Yuan, L. Blumea balsamifera—A phytochemical and pharmacological review. Molecules 2014, 19, 9453–9477. [Google Scholar] [CrossRef] [PubMed]
- Pang, Y.; Wang, D.; Hu, X.; Wang, H.; Fu, W.; Fan, Z.; Chen, X.; Yu, F. Effect of volatile oil from Blumea balsamifera (L.) DC. leaves on wound healing in mice. J. Tradit. Chin. Med. 2014, 34, 716–724. [Google Scholar] [CrossRef]
- Nessa, F.; Ismail, Z.; Mohamed, N.; Haris, M.R.H.M. Free radical-scavenging activity of organic extracts and of pure flavonoids of Blumea balsamifera DC leaves. Food Chem. 2004, 88, 243–252. [Google Scholar] [CrossRef]
- Kaswala, R.; Patel, V.; Chakraborty, M.; Kamath, J. Phytochemical and pharmacological profile of Gmelina arborea: An overview. Int. Res. J. Pharm. 2012, 3, 61–64. [Google Scholar]
- Gandigawad, P.; Poojar, B.; Hodlur, N.; Sori, R.K. Evaluation of anti-inflammatory activity of ethanolic extract of Gmelina arborea in experimental acute and sub-acute inflammatory models in wistar rats. Int. J. Basic Clin. Pharmacol. 2019, 8, 128. [Google Scholar] [CrossRef][Green Version]
- Kabeer, F.A.; Prathapan, R. Phytopharmacological profile of Elephantopus scaber. Pharmacologia 2014, 2, 272–285. [Google Scholar] [CrossRef]
- Nurtamin, T.; Sudayasa, I.P.; Tien, T. In vitro anti-inflammatory activities of ethanolic extract Elephantopus scaber leaves. Indones. J. Med. Health. 2018, 9, 46–52. [Google Scholar] [CrossRef]
- Kalola, J.; Shah, R.; Patel, A.; Lahiri, S.K.; Shah, M.B. Anti-inflammatory and immunomodulatory activities of Inula cappa roots (Compositae). J. Complement. Integr. Med. 2017. [Google Scholar] [CrossRef]
- Tangjitman, K.; Wongsawad, C.; Kamwong, K.; Sukkho, T.; Trisonthi, C. Ethnomedicinal plants used for digestive system disorders by the Karen of northern Thailand. J. Ethnobiol. Ethnomed. 2015, 11, 27. [Google Scholar] [CrossRef]
- Gazzaneo, L.R.S.; De Lucena, R.F.P.; de Albuquerque, U.P. Knowledge and use of medicinal plants by local specialists in an region of Atlantic Forest in the state of Pernambuco (Northeastern Brazil). J. Ethnobiol. Ethnomed. 2005, 1, 9. [Google Scholar] [CrossRef] [PubMed]
- Junsongduang, A. Roles and Importance of Sacred Forest in Biodiversity Conservation in Mae Chaem District, Chiang Mai Province. Ph.D. Thesis, Chiang Mai University, Chiang Mai, Thailand, 2013. [Google Scholar]
- Kamwong, K. Ethnobotany of Karens at Ban Mai Sawan and Ban Huay Pu Ling, Ban Luang Sub-District, Chom Thong District, Chiang Mai Province. Master’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 2009. [Google Scholar]
- Mahawongsanan, A. Change of Herbal Plants Utilization of the Pga K’nyau: A Case study of Ban Huay Som Poy, Mae Tia Watershed, Chom Thong District. Master’s Thesis, Chiang Mai Province. Chiang Mai University, Chiang Mai, Thailand, 2008. [Google Scholar]
- Pongamornkul, W. An Ethnobotanical Study of the Karen at Ban Yang Pu Toh and Ban Yang Thung Pong, Chiang Dao District, Chiang Mai Province. Master’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 2003. [Google Scholar]
- Puling, W. Ethnobotany of Karen for Studying Medicinal Plants at Angka Noi and Mae Klangluang Villages, Chomthong District, Chiang Mai. Bachelor’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 2001. [Google Scholar]
- Sukkho, T. A Survey of Medicinal Plants Used by Karen People at Ban Chan and Chaem Luang Subdistricts, Mae Chaem District. Master’s Thesis, Chiang Mai Province. Chiang Mai University, Chiang Mai, Thailand, 2008. [Google Scholar]
- Tangjitman, K. Vulnerability Prediction of Medicinal Plants Used by Karen People in Chiang Mai Province to Climatic Change Using Species Distribution Model (SDM). Ph.D. Thesis, Chiang Mai University, Chiang Mai, Thailand, 2014. [Google Scholar]
- Winjchiyanan, P. Ethnobotany of Karen in Chiang Mai. Master’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 1995. [Google Scholar]
- Sonsupub, B. Ethnobotany of Karen Community in Raipa Village, Huaykhayeng Subdistrict, Thongphaphume District, Kanchanaburi Province. Master’s Thesis, Kasetsart University, Bankok, Thailand, 2010. [Google Scholar]
- Moonjai, J. Ethnobotany of Ethnic Group in Mae La Noi District, Mae Hong Son Province. Master’s Thesis, Chiang Mai University, Chiang Mai, Thailand, 2017. [Google Scholar]
- Trisonthi, C.; Trisonthi, P. Ethnobotanical study in Thailand, a case study in Khun Yuam district Maehongson province. Thai J. Bot. 2009, 1, 1–23. [Google Scholar]
- Junkhonkaen, J. Ethnobotany of Ban Bowee, Amphoe Suan Phueng, Changwat Ratchaburi. Master’s Thesis, Kasetsart University, Bankok, Thailand, 2012. [Google Scholar]
- Tangjitman, K. Ethnobotany of the Karen at Huay Nam Nak village, Tanaosri subdistrict, Suanphueng district, Ratchaburi province. Thai J. Bot. 2017, 9, 253–272. [Google Scholar]
- Kantasrila, P.; Pongamornkul, W.; Panyadee, P.; Inta, A. Ethnobotany of medicinal plants used by Karen, Tak province in Thailand. Thai J. Bot. 2017, 9, 193–216. [Google Scholar]
- Phillips, O.; Gentry, A.H. The useful plants of Tambopata, Peru: I. Statistical hypotheses tests with a new quantitative technique. Econ. Bot. 1993, 47, 15–32. [Google Scholar] [CrossRef]
- Reyes-García, V.; Huanca, T.; Vadez, V.; Leonard, W.; Wilkie, D. Cultural, practical, and economic value of wild plants: A quantitative study in the Bolivian Amazon. Econ. Bot. 2006, 60, 62–74. [Google Scholar] [CrossRef]
- Mosaddegh, M.; Naghibi, F.; Moazzeni, H.; Pirani, A.; Esmaeili, S. Ethnobotanical survey of herbal remedies traditionally used in Kohghiluyeh va Boyer Ahmad province of Iran. J. Ethnopharmacol. 2012, 141, 80–95. [Google Scholar] [CrossRef]
- Trotter, R.; Logan, M. Informant Consensus: A New Approach for Identifying Potentially Effective Medicinal Plants, Plants in Indigenous Medicine and Diet, Behavioural Approaches; Redgrave Publishing Company: Bredfort Hill, NY, USA, 1986. [Google Scholar]
- Heinrich, M.; Ankli, A.; Frei, B.; Weimann, C.; Sticher, O. Medicinal plants in Mexico: Healers’ consensus and cultural importance. Soc. Sci. Med. 1998, 47, 1859–1871. [Google Scholar] [CrossRef]
| Scientific Name | Family | Habit | UV | RFC | Part Used | Preparation | Administration | MSD Categories |
|---|---|---|---|---|---|---|---|---|
| Acanthus montanus (Nees) T. Anderson | ACANTHACEAE | Tree | 0.037 | 0.037 | Leaves | Decoction | Oral ingestion | Muscle pain |
| Acmella oleracea (L.) R.K. Jansen | ASTERACEAE | Herb | 0.037 | 0.037 | Roots | Alcoholic infusion | Oral ingestion | Muscle pain |
| Ageratina adenophora (Spreng.) R.M. King and H. Rob. | ASTERACEAE | Herb | 0.037 | 0.037 | Leaves | Burning | Poultices | Muscle pain |
| Ageratum conyzoides L. | ASTERACEAE | Herb | 0.074 | 0.037 | Whole plants | Decoction | Oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint |
| Aglaia lawii (Wight) C.J. Saldanha | MELIACEAE | Tree | 0.037 | 0.037 | Leaves | Decoction | Bath, oral ingestion | Muscle pain |
| Alpinia galanga (L.) Willd. | ZINGIBERACEAE | Herb | 0.074 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint |
| Alpinia roxburghii Sweet | ZINGIBERACEAE | Herb | 0.074 | 0.037 | Roots | Decoction | Bath, oral ingestion | Muscle pain |
| Alstonia macrophylla Wall. ex G. Don | APOCYNACEAE | Tree | 0.037 | 0.037 | Bark | Water infusion | Oral ingestion | Muscle pain |
| Alstonia rostrata C.E.C. Fisch. | APOCYNACEAE | Tree | 0.074 | 0.037 | Bark | Decoction, water infusion | Oral ingestion | Muscle pain |
| Anredera cordifolia (Ten.) Steenis | BASELLACEAE | Herb | 0.074 | 0.037 | Bulbil | Cook | Eaten as food | Back symptom/complaint, Flank/axilla symptom/complaint |
| Antidesma bunius (L.) Spreng. | EUPHORBIACEAE | Tree | 0.074 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint |
| Asparagus filicinus Buch.-Ham. ex D. Don | ASPARAGACEAE | Climber | 0.074 | 0.074 | Roots, whole plants | Decoction | Bath, oral ingestion | Muscle pain |
| Baccaurea ramiflora Lour. | EUPHORBIACEAE | Tree | 0.074 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint |
| Betula alnoides Buch.-Ham. ex D. Don | BETULACEAE | Tree | 0.185 | 0.148 | Bark, leaves | Alcoholic infusion, decoction, none | Eaten as food, oral ingestion | Flank/axilla symptom/complaint, muscle pain |
| Biancaea sappan (L.) Tod. | LEGUMINOSAE | Tree | 0.370 | 0.148 | Stems | Decoction | Oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint |
| Bistorta paleacea (Wall. ex Hook.f.) Yonek. and H. Ohashi | POLYGONACEAE | Herb | 0.111 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, Bursitis/tendinitis/synovitis NOS, Flank/axilla symptom/complaint |
| Blumea balsamifera (L.) DC. | ASTERACEAE | Shrub | 0.407 | 0.074 | Leaves, roots, whole plants | Burning, decoction, grind | Oral ingestion, poultices, steaming | Back symptom/complaint, Flank/axilla symptom/complaint, muscle pain, Sprain/strain of joint NOS |
| Boehmeria glomerulifera Miq. | URTICACEAE | Herb | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Brachypterum scandens (Roxb.) Miq. | LEGUMINOSAE | Climber | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Buddleja asiatica Lour. | SCROPHULARIACEAE | Shrub | 0.074 | 0.037 | Leaves | Decoction | Oral ingestion | Flank/axilla symptom/complaint, Leg/thigh symptom/complaint |
| Canscora andrographioides Griff. ex C.B. Clarke | GENTIANACEAE | Herb | 0.037 | 0.037 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Cassytha filiformis L. | LAURACEAE | Herb | 0.111 | 0.074 | Stems, whole plants | Alcoholic infusion, decoction | Oral ingestion | Muscle pain |
| Celastrus paniculatus Willd. | CELASTRACEAE | Climber | 0.037 | 0.037 | Aerial parts | Decoction | Oral ingestion | Muscle pain |
| Centella asiatica (L.) Urb. | APIACEAE | Herb | 0.185 | 0.074 | Leaves, whole plants | Decoction, none | Eaten as food, oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint, muscle pain |
| Chloranthus erectus (Buch.-Ham.) Verdc. | CHLORANTHACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Flank/axilla symptom/complaint |
| Chromolaena odorata (L.) R.M. King and H. Rob. | ASTERACEAE | Herb | 0.074 | 0.074 | Roots, stems | Decoction | Oral ingestion | Muscle pain |
| Cissus discolor Blume | VITACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Citrus medica L. | RUTACEAE | Tree | 0.037 | 0.037 | Leaves | Decoction | Oral ingestion | Muscle pain |
| Clausena excavata Burm.f. | RUTACEAE | Shrub | 0.222 | 0.037 | Inflorescences, leaves, whole plants | Burning, cook, none | Eaten as food, poultices, steaming | Back symptom/complaint, Flank/axilla symptom/complaint, muscle pain |
| Clematis smilacifolia Wall. | RANUNCULACEAE | Climber | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Clerodendrum disparifolium Blume | LAMIACEAE | Shrub | 0.037 | 0.037 | Leaves | Grind | Poultices | Muscle symptom/complaint NOS |
| Clerodendrum indicum (L.) Kuntze | LAMIACEAE | Shrub | 0.037 | 0.037 | Inflorescences, leaves | Decoction | Oral ingestion | Muscle pain |
| Cnestis palala (Lour.) Merr. | CONNARACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Codariocalyx motorius (Houtt.) H. Ohashi | LEGUMINOSAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Coix lacryma-jobi L. var. monilifer Watt | POACEAE | Grass | 0.148 | 0.074 | Whole plants, roots | Decoction | Oral ingestion | Back symptom/complaint, Flank/axilla symptom/complaint, muscle pain |
| Crateva religiosa G. Forst. | CAPPARACEAE | Tree | 0.037 | 0.037 | Leaves | Grind | Poultices | Sprain/strain of ankle |
| Cratoxylum formosum (Jacq.) Benth. and Hook.f. ex Dyer subsp. pruniflorum (Kurz) Gogelein | HYPERICACEAE | Tree | 0.037 | 0.037 | Roots, stems | Decoction | Oral ingestion | Muscle pain |
| Crinum asiaticum L. | AMARYLLIDACEAE | Herb | 0.111 | 0.111 | Leaves | Burning | Oral ingestion, poultices | Muscle pain, sprain/strain of joint NOS |
| Croton kongensis Gagnep. | EUPHORBIACEAE | Shrub | 0.037 | 0.037 | Leaves, roots | Decoction | Oral ingestion | Muscle pain |
| Croton mangelong Y.T. Chang | EUPHORBIACEAE | Shrub | 0.074 | 0.074 | Leaves | Decoction | Oral ingestion | Muscle pain |
| Curcuma elata Roxb. | ZINGIBERACEAE | Herb | 0.074 | 0.037 | Roots | Grind | Poultices | Hand/finger symptom/complaint, knee symptom/complaint |
| Curcuma longa L. | ZINGIBERACEAE | Herb | 0.111 | 0.111 | Roots | Burning, grind | Poultices | Fracture: other, leg/thigh symptom/complaint |
| Curcuma zedoaria (Christm.) Roscoe | ZINGIBERACEAE | Herb | 0.074 | 0.037 | Roots | None | Chewing | Back symptom/complaint, flank/axilla symptom/complaint |
| Cuscuta chinensis Lam. | CONVOLVULACEAE | Herb | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Cyclocodon celebicus (Blume) D.Y. Hong | CAMPANULACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Cymbopogon citratus (DC.) Stapf | POACEAE | Grass | 0.074 | 0.074 | Stems, whole plants | Burning, grind | Poultices | Fracture: other, muscle pain |
| Dendrocalamus brandisii (Munro) Kurz | POACEAE | Bamboo | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Dendrophthoe pentandra (L.) Miq. | LORANTHACEAE | Shrub | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Knee symptom/complaint |
| Desmos macrocarpus Bân | ANNONACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Dimetia ampliflora (Hance) Neupane and N. Wikstr. | RUBIACEAE | Herb | 0.074 | 0.037 | Roots, whole plants | Decoction | Oral ingestion, steaming | Muscle pain |
| Diplazium esculentum (Retz.) Sw. | ATHYRIACEAE | Fern | 0.037 | 0.037 | Roots | Decoction | Poultices | Sprain/strain of joint NOS |
| Dischidia nummularia R. Br. | APOCYNACEAE | Herb | 0.074 | 0.074 | Leaves | Decoction, grind, none | Eaten as food, oral ingestion, poultices | Knee symptom/complaint, muscle pain |
| Dracaena fragrans (L.) Ker Gawl. | ASPARAGACEAE | Shrub | 0.037 | 0.037 | Leaves | Burning | Poultices | Sprain/strain of joint NOS |
| Dracaena terniflora Roxb. | ASPARAGACEAE | Shrub | 0.037 | 0.037 | Leaves, stems | Decoction | Oral ingestion | Muscle pain |
| Duabanga grandiflora (DC.) Walp. | LYTHRACEAE | Tree | 0.074 | 0.074 | Bark | Decoction | Oral ingestion | Muscle pain |
| Dufrenoya collettii (Gamble) Stauffer | SANTALACEAE | Herb | 0.148 | 0.037 | Roots, whole plants | Decoction | Liniment, oral ingestion, poultices | Flank/axilla symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Dufrenoya sessilis (Craib) Stauffer | SANTALACEAE | Shrub | 0.111 | 0.037 | Leaves, stems | Burning, decoction | Oral ingestion, poultices | Leg/thigh symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Duhaldea cappa (Buch.-Ham. ex D. Don) Pruski and Anderb. | ASTERACEAE | Shrub | 0.407 | 0.259 | Inflorescences, leaves, roots | Burning, decoction, grind | Oral ingestion, poultices | Joint symptom/complaint NOS, knee symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Elephantopus scaber L. | ASTERACEAE | Herb | 0.222 | 0.222 | Roots, whole plants | Decoction | Oral ingestion | Flank/axilla symptom/complaint, muscle pain |
| Eleutherine bulbosa (Mill.) Urb. | IRIDACEAE | Herb | 0.037 | 0.037 | Roots | Grind | Liniment | Muscle pain |
| Embelia ribes Burm.f. | PRIMULACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Engelhardia spicata Lesch. ex Blume | JUGLANDACEAE | Tree | 0.074 | 0.074 | Bark, stems | Decoction | Oral ingestion | Muscle pain |
| Ensete glaucum (Roxb.) Cheesman | MUSACEAE | Herb | 0.037 | 0.037 | Seeds | Decoction | Compress | Muscle pain |
| Equisetum ramosissimum Desf. subsp. debile (Roxb. ex Vaucher) Hauke | EQUISETACEAE | Low vascular plant | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Erythrina subumbrans (Hassk.) Merr. | LEGUMINOSAE | Tree | 0.074 | 0.074 | Bark, leaves | Burning, decoction | Oral ingestion, poultices | Fracture: radius/ulna, leg/thigh symptom/complaint |
| Eurycoma longifolia Jack | SIMAROUBACEAE | Shrub | 0.074 | 0.074 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Ficus semicordata Buch.-Ham. ex Sm. | MORACEAE | Tree | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Flacourtia jangomas (Lour.) Raeusch. | SALICACEAE | Tree | 0.037 | 0.037 | Bark | Decoction | Oral ingestion | Muscle pain |
| Flacourtia rukam Zoll. and Moritzi | SALICACEAE | Tree | 0.148 | 0.074 | Roots | Decoction | Oral ingestion | Bursitis/tendinitis/synovitis NOS, muscle pain |
| Flemingia strobilifera (L.) W.T. Aiton | LEGUMINOSAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Flueggea leucopyrus Willd. | PHYLLANTHACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Gmelina arborea Roxb. | LAMIACEAE | Tree | 0.333 | 0.296 | Bark, inflorescences | Burning, decoction | Oral ingestion, poultices, soak | Fracture: other, knee symptom/complaint, Muscle pain |
| Gynostemma pentaphyllum (Thunb.) Makino | CUCURBITACEAE | Climber | 0.037 | 0.037 | Whole plants | Decoction | Poultices | Muscle pain |
| Heliciopsis terminalis (Kurz) Sleumer | PROTEACEAE | Tree | 0.037 | 0.037 | Bark | Decoction | Oral ingestion | Muscle pain |
| Hellenia speciosa (J. Koenig) S.R. Dutta | COSTACEAE | Herb | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Flank/axilla symptom/complaint |
| Hiptage benghalensis (L.) Kurz | MALPIGHIACEAE | Climber | 0.111 | 0.074 | Bark, roots, stems | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Hiptage benghalensis (L.) Kurz subsp. candicans (Hook.f.) Sirirugsa | MALPIGHIACEAE | Shrub | 0.037 | 0.037 | Bark | Decoction | Oral ingestion | Flank/axilla symptom/complaint |
| Huangtcia renifolia (L.) H. Ohashi and K. Ohashi | LEGUMINOSAE | Shrub | 0.037 | 0.037 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Hydrocotyle javanica Thunb. | ARALIACEAE | Herb | 0.111 | 0.074 | Leaves, whole plants | Decoction, none | Eaten as food, oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Hymenasplenium apogamum (N. Murak. and Hatan.) Nakaike | ASPLENIACEAE | Fern | 0.037 | 0.037 | Leaves | Burning | Poultices | Sprain/strain of ankle |
| Illigera trifoliata (Griff.) Dunn | HERNANDIACEAE | Climber | 0.074 | 0.037 | Leaves, whole plants | Decoction | Oral ingestion, steaming | Muscle pain |
| Imperata cylindrica (L.) Raeusch. | POACEAE | Grass | 0.074 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Indigofera caloneura Kurz | LEGUMINOSAE | Shrub | 0.037 | 0.037 | Whole plants | Decoction | Oral ingestion | Knee symptom/complaint |
| Ixora henryi H. Lév. | RUBIACEAE | Tree | 0.037 | 0.037 | Leaves | Decoction | Oral ingestion | Muscle pain |
| Kaempferia rotunda L. | ZINGIBERACEAE | Herb | 0.037 | 0.037 | Roots | Grind | Compress | Muscle pain, knee symptom/complaint |
| Leea indica (Burm.f.) Merr. | VITACEAE | Shrub | 0.074 | 0.074 | Leaves, roots | Decoction | Oral ingestion | Knee symptom/complaint |
| Lilium primulinum Baker var. burmanicum (W.W. Sm.) Stearn | LILIACEAE | Herb | 0.074 | 0.037 | Roots | Decoction | Bath | Back symptom/complaint, flank/axilla symptom/complaint |
| Litsea martabanica (Kurz) Hook.f. | LAURACEAE | Tree | 0.037 | 0.037 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Lycopodiella cernua cernua (L.) Pic. Serm. | LYCOPODIACEAE | Fern | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Lygodium flexuosum (L.) Sw. | LYGODIACEAE | Fern | 0.259 | 0.148 | Aerial parts, roots, whole plants | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, leg/thigh symptom/complaint |
| Macaranga denticulata (Blume) Müll. Arg. | EUPHORBIACEAE | Tree | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Fracture: femur |
| Maesa glomerata K. Larsen and C.M. Hu | PRIMULACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Mangifera indica L. | ANACARDIACEAE | Tree | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Mansoa alliacea (Lam.) A. Gentry | BIGNONIACEAE | Climber | 0.037 | 0.037 | Leaves | Decoction | Oral ingestion | Joint symptom/complaint NOS |
| Melicope lunu-ankenda (Gaertn.) T.G. Hartley | RUTACEAE | Shrub | 0.111 | 0.037 | Leaves, whole plants | Decoction, none | Bath, poultices | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Melicope pteleifolia (Champ. ex Benth.) T.G. Hartley | RUTACEAE | Tree | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Memecylon pauciflorum Blume | MELASTOMATACEAE | Shrub | 0.037 | 0.037 | Leaves | Decoction | Oral ingestion | Muscle pain |
| Microcos paniculata L. | MALVACEAE | Tree | 0.037 | 0.037 | Leaves, roots | Decoction | Oral ingestion | Muscle pain |
| Miliusa thorelii Finet and Gagnep. | ANNONACEAE | Shrub | 0.704 | 0.259 | Bark, leaves, roots, stems | Alcoholic infusion, decoction | Oral ingestion | Fracture: other, Joint symptom/complaint NOS, Knee symptom/complaint, Muscle pain |
| Miliusa velutina (Dunal) Hook.f. and Thomson | ANNONACEAE | Tree | 0.074 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Mimosa pudica L. | LEGUMINOSAE | Herb | 0.111 | 0.111 | Roots, whole plants | Decoction | Oral ingestion, soak | Muscle pain |
| Mitragyna rotundifolia (Roxb.) Kuntze | RUBIACEAE | Tree | 0.037 | 0.037 | Roots, stems | Decoction | Oral ingestion | Rheumatoid/seropositive arthritis |
| Momordica charantia L. | CUCURBITACEAE | Climber | 0.037 | 0.037 | Whole plants | Cook | Eaten as food | Muscle pain |
| Monosis volkameriifolia (DC.) H. Rob. and Skvarla | ASTERACEAE | Shrub | 0.074 | 0.037 | Roots, stems | Decoction | Oral ingestion | Leg/thigh symptom/complaint, muscle pain |
| Mussaenda sanderiana Ridl. | RUBIACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Poultices | Muscle pain |
| Nyctocalos brunfelsiiflora Teijsm. and Binn. | BIGNONIACEAE | Climber | 0.074 | 0.037 | Roots, stems, whole plants | Decoction | Oral ingestion | Flank/axilla symptom/complaint, muscle pain |
| Oenanthe javanica (Blume) DC. | APIACEAE | Herb | 0.037 | 0.037 | Leaves | None | Eaten as food | Muscle pain |
| Oroxylum indicum (L.) Benth. ex Kurz | BIGNONIACEAE | Tree | 0.074 | 0.074 | Bark, stems | Decoction, none | Chewing, oral ingestion | Muscle pain |
| Orthosiphon aristatus (Blume) Miq. | LAMIACEAE | Herb | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Osbeckia chinensis L. | MELASTOMATACEAE | Shrub | 0.037 | 0.037 | Roots, whole plants | Decoction | Oral ingestion | Muscle pain |
| Oxyceros bispinosus (Griff.) Tirveng. | RUBIACEAE | Shrub | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Paris polyphylla Sm. | MELANTHIACEAE | Herb | 0.111 | 0.074 | Roots | Alcoholic infusion, decoction | Oral ingestion | Flank/axilla symptom/complaint, muscle pain |
| Peliosanthes caesia J.M.H. Shaw | ASPARAGACEAE | Herb | 0.037 | 0.037 | Leaves, whole plants | Decoction | Oral ingestion | Neck symptom/complain |
| Phlogacanthus curviflorus Nees | ACANTHACEAE | Shrub | 0.148 | 0.074 | Inflorescences, leaves, whole plants | Burning, none | Eaten as food, poultices | Muscle pain |
| Phyllanthus amarus Schumach. and Thonn. | PHYLLANTHACEAE | Herb | 0.111 | 0.111 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Phyllanthus emblica L. | PHYLLANTHACEAE | Tree | 0.037 | 0.037 | Bark | Decoction | Oral ingestion | Muscle pain |
| Phyllodium pulchellum (L.) Desv. | LEGUMINOSAE | Shrub | 0.074 | 0.074 | Roots, whole plants | Decoction | Oral ingestion | Muscle pain |
| Picrasma javanica Blume | SIMAROUBACEAE | Tree | 0.037 | 0.037 | Bark | Water infusion | Oral ingestion | Muscle pain |
| Piper boehmeriifolium (Miq.) C. DC. | PIPERACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Piper interruptum Opiz | PIPERACEAE | Climber | 0.074 | 0.074 | Stems | Decoction | Oral ingestion | Muscle pain |
| Piper nigrum L. | PIPERACEAE | Climber | 0.074 | 0.037 | Infructescences | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Piper retrofractum Vahl | PIPERACEAE | Climber | 0.074 | 0.037 | Infructescences | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Piper ribesioides (Wall.) C. DC | PIPERACEAE | Climber | 0.037 | 0.037 | Stems | Grind | Oral ingestion | Muscle pain |
| Plantago major L. | PLANTAGINACEAE | Herb | 0.852 | 0.370 | Leaves, roots, whole plants | Burning, grind, decoction, none, pounded | Compress, eaten as food, oral ingestion, poultices | Back symptom/complaint, flank/axilla symptom/complaint, hand/finger symptom/complaint, joint symptom/complaint NOS, knee symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Plumbago indica L. | PLUMBAGINACEAE | Herb | 0.148 | 0.074 | Roots | Alcoholic infusion, decoction | Oral ingestion | Flank/axilla symptom/complaint, knee symptom/complaint, muscle pain |
| Plumbago zeylanica L. | PLUMBAGINACEAE | Shrub | 0.074 | 0.037 | Roots | Alcoholic infusion | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Plumeria obtusa L. | APOCYNACEAE | Tree | 0.037 | 0.037 | Leaves | Decoction | Oral ingestion | Muscle pain |
| Plumeria rubra L. | APOCYNACEAE | Tree | 0.074 | 0.037 | Bark | Decoction, water infusion | Oral ingestion | Muscle pain |
| Polygala arillata Buch.-Ham. ex D. Don | POLYGALACEAE | Shrub | 0.037 | 0.037 | Inflorescences, roots | Decoction | Oral ingestion | Muscle pain |
| Polygala chinensis L. | POLYGALACEAE | Herb | 0.074 | 0.074 | Whole plants | Burning, decoction | Oral ingestion | Muscle pain |
| Pothos chinensis (Raf.) Merr. | ARACEAE | Climber | 0.111 | 0.074 | Leaves, stems, whole plants | Decoction | Oral ingestion | Leg/thigh symptom/complaint, muscle pain |
| Pothos scandens L. | ARACEAE | Climber | 0.630 | 0.259 | Whole plants | Alcoholic infusion, decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Psychotria yunnanensis Hutch. | RUBIACEAE | Shrub | 0.037 | 0.037 | Stems | Decoction | Oral ingestion | Muscle pain |
| Putranjiva roxburghii Wall. | PUTRANJIVACEAE | Tree | 0.037 | 0.037 | Leaves | Burning | Poultices | Muscle pain |
| Rhinacanthus nasutus (L.) Kurz | ACANTHACEAE | Shrub | 0.037 | 0.037 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Rotheca serrata Steane and Mabb. | LAMIACEAE | Shrub | 0.111 | 0.111 | Barks, leaves | Decoction, grind | Oral ingestion, poultices | Muscle pain |
| Rubia cordifolia L. | RUBIACEAE | Herb | 0.037 | 0.037 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Saccharum officinarum L. | POACEAE | Grass | 0.074 | 0.037 | Leaves, stems | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Salacia chinensis L. | CELASTRACEAE | Shrub | 0.037 | 0.037 | Stems | Alcoholic infusion | Oral ingestion | Muscle pain |
| Salacia verrucosa Wight | CELASTRACEAE | Climber | 0.111 | 0.074 | Roots | Decoction | Oral ingestion | Leg/thigh symptom/complaint, muscle pain |
| Sambucus javanica Reinw. ex Blume | ADOXACEAE | Shrub | 1.148 | 0.593 | Leaves, roots, whole plants | Burning, grind, decoction | Compress, oral ingestion, poultices | Flank/axilla symptom/complaint, fracture: other, fracture: radius/ulna, joint symptom/complaint NOS, leg/thigh symptom/complaint, muscle pain, sprain/strain of joint NOS, wrist symptom/complaint |
| Sambucus simpsonii Rehder | ADOXACEAE | Shrub | 0.481 | 0.259 | Leaves, roots | Burning, decoction | Compress, oral ingestion, poultices | Fracture: other, muscle pain, sprain/strain of joint NOS |
| Sarcandra glabra (Thunb.) Nakai var. brachystachys (Blume) Verdc. | CHLORANTHACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Saurauia roxburghii Wall. | ACTINIDIACEAE | Tree | 0.037 | 0.037 | Roots | Decoction | Decoction | Muscle pain |
| Schefflera leucantha R. Vig. | ARALIACEAE | Shrub | 0.259 | 0.148 | Stems, whole plants | Burning and decoction | Bath, oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, joint symptom/complaint NOS, muscle pain |
| Schima wallichii (DC.) Korth. | THEACEAE | Tree | 0.037 | 0.037 | Leaves | Water infusion | Oral ingestion | Muscle pain |
| Scleropyrum maingayi Hook.f. | SANTALACEAE | Tree | 0.148 | 0.037 | Whole plants | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, joint symptom/complaint NOS, muscle pain |
| Scleropyrum pentandrum (Dennst.) Mabb. | SANTALACEAE | Tree | 0.111 | 0.074 | Roots | Decoction | Oral ingestion | Back symptom/complaint, muscle pain |
| Scoparia dulcis L. | PLANTAGINACEAE | Herb | 0.111 | 0.111 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Senna occidentalis (L.) Link | LEGUMINOSAE | Shrub | 0.037 | 0.037 | Seeds | Burning and decoction | Oral ingestion | Muscle pain |
| Sida acuta Burm.f. | MALVACEAE | Shrub | 0.148 | 0.074 | Roots, whole plants | Decoction | Oral ingestion | Flank/axilla symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Sida cordifolia L. | MALVACEAE | Shrub | 0.111 | 0.037 | Roots | Decoction | Oral ingestion | Flank/axilla symptom/complaint, muscle pain, sprain/strain of joint NOS |
| Sida rhombifolia L. | MALVACEAE | Shrub | 0.037 | 0.037 | Leaves, roots, whole plants | Decoction | Oral ingestion | Flank/axilla symptom/complaint |
| Smilax corbularia Kunth | SMILACACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Smilax glabra Roxb. | SMILACACEAE | Climber | 0.148 | 0.074 | Roots | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Smilax griffithii A. DC. | SMILACACEAE | Climber | 0.074 | 0.074 | Whole plants | Decoction | Oral ingestion | Muscle pain |
| Smilax luzonensis C. Presl | SMILACACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Sohmaea teres (Wall. ex Benth.) H. Ohashi and K. Ohashi | LEGUMINOSAE | Shrub | 0.074 | 0.037 | Roots | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Solanum erianthum D. Don | SOLANACEAE | Shrub | 0.074 | 0.037 | Stems | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint |
| Styrax benzoides Craib | STYRACACEAE | Tree | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Tadehagi triquetrum (L.) H. Ohashi | LEGUMINOSAE | Shrub | 0.222 | 0.111 | Roots, whole plants | Alcoholic infusion, decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Tetrastigma cruciatum Craib and Gagnep. | VITACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Thunbergia coccinea Wall. ex D. Don | ACANTHACEAE | Climber | 0.148 | 0.074 | Stems, whole plants | Decoction | Oral ingestion | Arm symptom/complaint, knee symptom/complaint, muscle pain |
| Thunbergia laurifolia Lindl. | ACANTHACEAE | Climber | 0.111 | 0.111 | Leaves, roots, stems, whole plants | Decoction | Oral ingestion | Muscle pain |
| Thysanolaena latifolia (Roxb. ex Hornem.) Honda | POACEAE | Grass | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Tinospora crispa (L.) Hook.f. and Thomson | MENISPERMACEAE | Climber | 0.185 | 0.148 | Aerial parts, stems | Alcoholic infusion, sugar infusion, decoction | Oral ingestion, poultices | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Tupistra muricata (Gagnep.) N. Tanaka | ASPARAGACEAE | Herb | 0.222 | 0.074 | Leaves, roots | Burning, decoction | Poultices | Fracture: femur, leg/thigh symptom/complaint, sprain/strain of joint NOS, wrist symptom/complaint |
| Turpinia pomifera (Roxb.) DC. | STAPHYLEACEAE | Tree | 0.074 | 0.037 | Roots | Alcoholic infusion, decoction | Oral ingestion | Muscle pain |
| Uncaria laevigata Wall. ex G. Don | RUBIACEAE | Climber | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Muscle pain |
| Xantolis burmanica (Collett and Hemsl.) P. Royen | SAPOTACEAE | Tree | 0.037 | 0.037 | Bark | Decoction | Oral ingestion | Muscle pain |
| Zingiber latifolium Theilade and Mood | ZINGIBERACEAE | Shrub | 0.037 | 0.037 | Roots | Decoction | Oral ingestion | Fracture: other |
| Zingiber officinale Roscoe | ZINGIBERACEAE | Shrub | 0.037 | 0.037 | Roots | Grind | Oral ingestion | Muscle pain |
| Zingiber ottensii Valeton | ZINGIBERACEAE | Shrub | 0.111 | 0.074 | Roots | Decoction | Oral ingestion | Back symptom/complaint, flank/axilla symptom/complaint, muscle pain |
| Zingiber purpureum Roscoe | ZINGIBERACEAE | Shrub | 0.074 | 0.074 | Roots | Concoction, grind | Poultices | Muscle pain, sprain/strain of joint NOS |
| Ziziphus cambodianus Pierre | RHAMNACEAE | Tree | 0.074 | 0.074 | Barks | Decoction | Oral ingestion | Muscle pain |
| Code | Category | Number of Use Reports (Nur) | Number of Species (Nt) | ICF |
|---|---|---|---|---|
| L12 | Hand/finger symptom/complaint | 5 | 2 | 0.75 |
| L76 | Fracture: other | 19 | 7 | 0.67 |
| L79 | Sprain/strain of joint | 32 | 14 | 0.58 |
| L20 | Joint symptom/complaint | 10 | 5 | 0.56 |
| L87 | Bursitis/tendinitis/synovitis | 3 | 2 | 0.50 |
| L11 | Wrist symptom/complaint | 3 | 2 | 0.50 |
| L15 | Knee symptom/complaint | 18 | 11 | 0.41 |
| L18 | Muscle pain | 187 | 117 | 0.38 |
| L05 | Flank/axilla symptom/complaint | 65 | 47 | 0.28 |
| L02 | Back symptom/complaint | 44 | 32 | 0.28 |
| L14 | Leg/thigh symptom/complaint | 11 | 10 | 0.10 |
| L09 | Arm symptom/complaint | 1 | 1 | 0.00 |
| L75 | Fracture: femur | 2 | 2 | 0.00 |
| L72 | Fracture: radius/ulna | 2 | 2 | 0.00 |
| L19 | Muscle symptom/complaint | 1 | 1 | 0.00 |
| L01 | Neck symptom/complain | 1 | 1 | 0.00 |
| L88 | Rheumatoid/seropositive arthritis | 1 | 1 | 0.00 |
| L77 | Sprain/strain of ankle | 2 | 2 | 0.00 |
| Source | Village | Subdistrict | District | Province | #Species |
|---|---|---|---|---|---|
| Junsongduang et al. [90] | Mae Hae Tai | Pang Hin Fon | Mae Chaem | Chiang Mai | 8 |
| Kaewsangsai [29] | Khun Khun Noi | Mae Tuen | Omkoi | Chiang Mai | 52 |
| Kamwong [91] | Mai Sa Wan | Ban Luang | Chom Thong | Chiang Mai | 8 |
| Huay Poo Ling | Ban Luang | Chom Thong | Chiang Mai | 15 | |
| Mahawongsanan [92] | Huai Sompoi | Doi Kaew | Chom Thong | Chiang Mai | 3 |
| Pongamornkul [93] | Yang Tung Pong | Mae Na | Chiang Dao | Chiang Mai | 5 |
| Yang Poo To | Chiang Dao | Chiang Dao | Chiang Mai | 6 | |
| Puling [94] | Mae Klang Luang | Ban Luang | Chom Thong | Chiang Mai | 3 |
| Ang Ka Noi | Ban Luang | Chom Thong | Chiang Mai | 3 | |
| Sukkho [95] | Kio Pong | Chaem Luang | Mae Chaem | Chiang Mai | 13 |
| Chaem Noi | Ban Chan | Mae Chaem | Chiang Mai | 10 | |
| San Muang | Ban Chan | Mae Chaem | Chiang Mai | 10 | |
| Huay Bong | Ban Chan | Mae Chaem | Chiang Mai | 11 | |
| Huay Hom | Ban Chan | Mae Chaem | Chiang Mai | 9 | |
| Tangjitman [96] | Huay Hea | Samoeng Tai | Samoeng District | Chiang Mai | 12 |
| Mai Lan Kam | Samoeng Tai | Samoeng District | Chiang Mai | 17 | |
| Winjchiyanan [97] | Thung Luang | Mae Wang | Mae Wang | Chiang Mai | 13 |
| Pa Tak | Sop Poeng | Mae Tang | Chiang Mai | 2 | |
| Mae Lod Tai | Sop Poeng | Mae Tang | Chiang Mai | 11 | |
| Mae Hae Nuea | Na Chor | Mae Chaem | Chiang Mai | 4 | |
| Huay Tong | Mae Wang | Mae Wang | Chiang Mai | 3 | |
| Sonsupub [98] | Rai Pa | Huay Khayen | Thongphaphume | Kanchanaburi | 3 |
| Moonjai [99] | Huay Hom | Huay Hom | Mae La Noi | Mae Hong Son | 1 |
| Trisonthi and Trisonthi [100] | Six small sub-villages (Hua Mae Surin, Hua Hua, Mae Surin Noi, Payoi, Kano, and Mae U Kor Noi) | Mae Ukho | Khun Yuam | Mae Hong Son | 5 |
| Junkhonkaen [101] | Bo Wee | Tanao Si | Suan Phueng | Ratchaburi | 10 |
| Tangjitman [102] | Huay Nam Nak | Tanao Si | Suan Phueng | Ratchaburi | 3 |
| Kantasrila [103] | Wa Do Kro | Mae Song | Tha Song Yang District | Tak | 61 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kantasrila, R.; Pandith, H.; Balslev, H.; Wangpakapattanawong, P.; Panyadee, P.; Inta, A. Medicinal Plants for Treating Musculoskeletal Disorders among Karen in Thailand. Plants 2020, 9, 811. https://doi.org/10.3390/plants9070811
Kantasrila R, Pandith H, Balslev H, Wangpakapattanawong P, Panyadee P, Inta A. Medicinal Plants for Treating Musculoskeletal Disorders among Karen in Thailand. Plants. 2020; 9(7):811. https://doi.org/10.3390/plants9070811
Chicago/Turabian StyleKantasrila, Rapeeporn, Hataichanok Pandith, Henrik Balslev, Prasit Wangpakapattanawong, Prateep Panyadee, and Angkhana Inta. 2020. "Medicinal Plants for Treating Musculoskeletal Disorders among Karen in Thailand" Plants 9, no. 7: 811. https://doi.org/10.3390/plants9070811
APA StyleKantasrila, R., Pandith, H., Balslev, H., Wangpakapattanawong, P., Panyadee, P., & Inta, A. (2020). Medicinal Plants for Treating Musculoskeletal Disorders among Karen in Thailand. Plants, 9(7), 811. https://doi.org/10.3390/plants9070811







