Medicinal Plants and Their Traditional Uses in Local Communities around Cherangani Hills, Western Kenya
Abstract
1. Introduction
2. Material and Methods
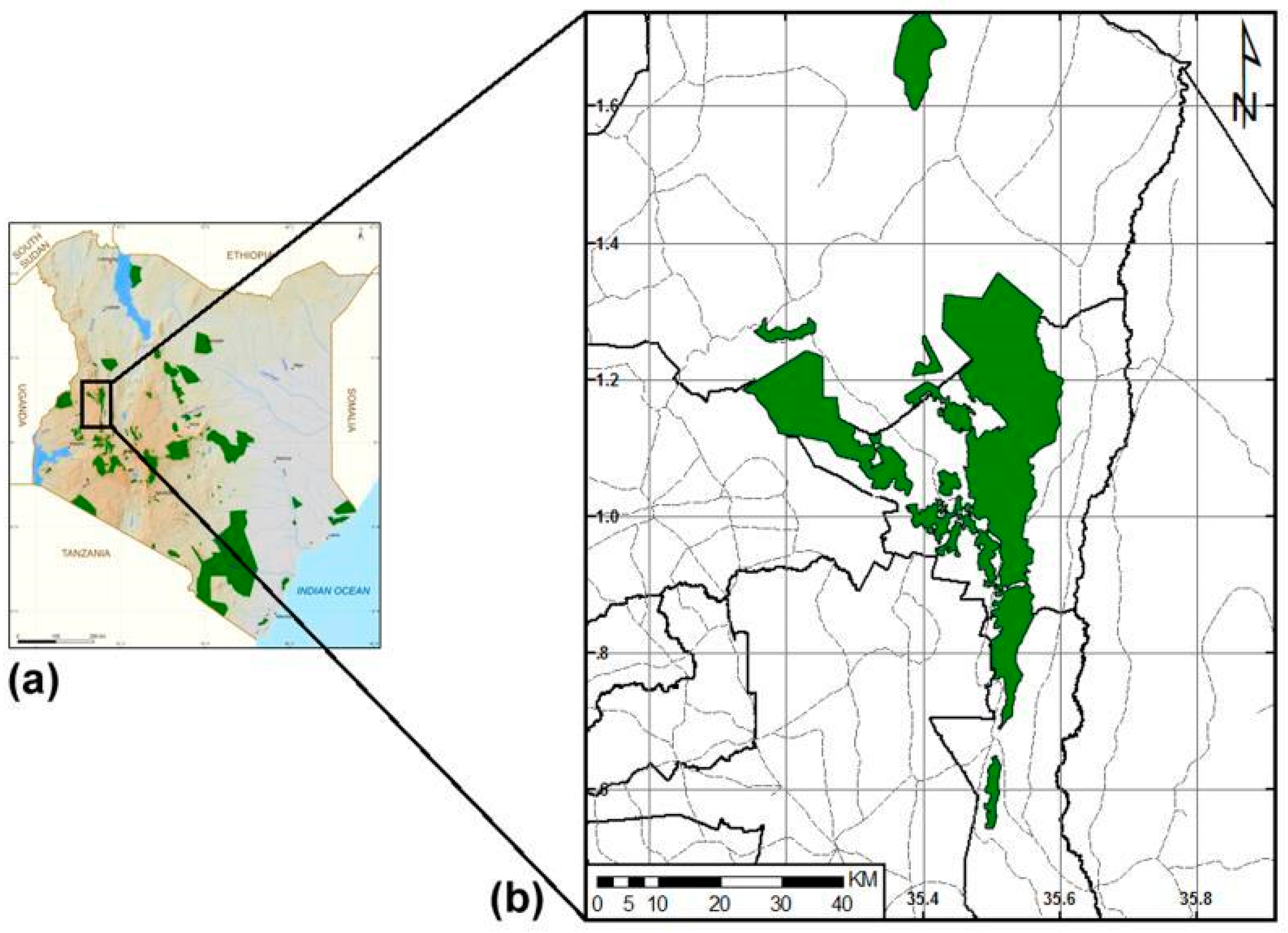
2.1. Study Area
2.2. Selection of Respondents
2.3. Ethnobotanical Data Collection and Plant Identification
2.4. Data Analysis
2.4.1. Informant Consensus Factor
2.4.2. Fidelity Level (FL)
2.4.3. Jaccard’s Coefficient of Similarity (JCS)
3. Results
3.1. Demographic Profile of Respondents
3.2. Diversity of Medicinal Plant Use
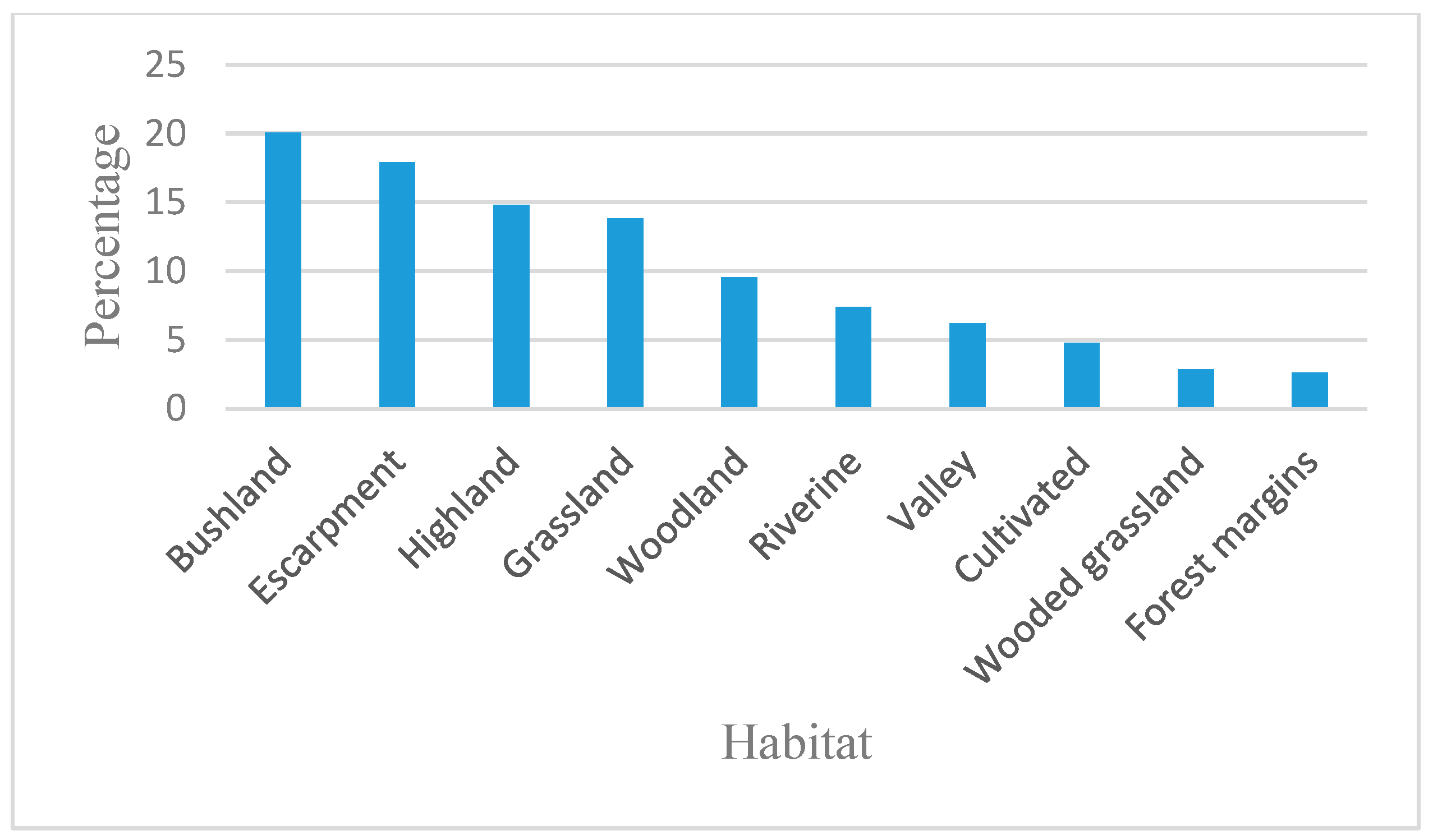
3.3. The Habitat for Medicinal Plants
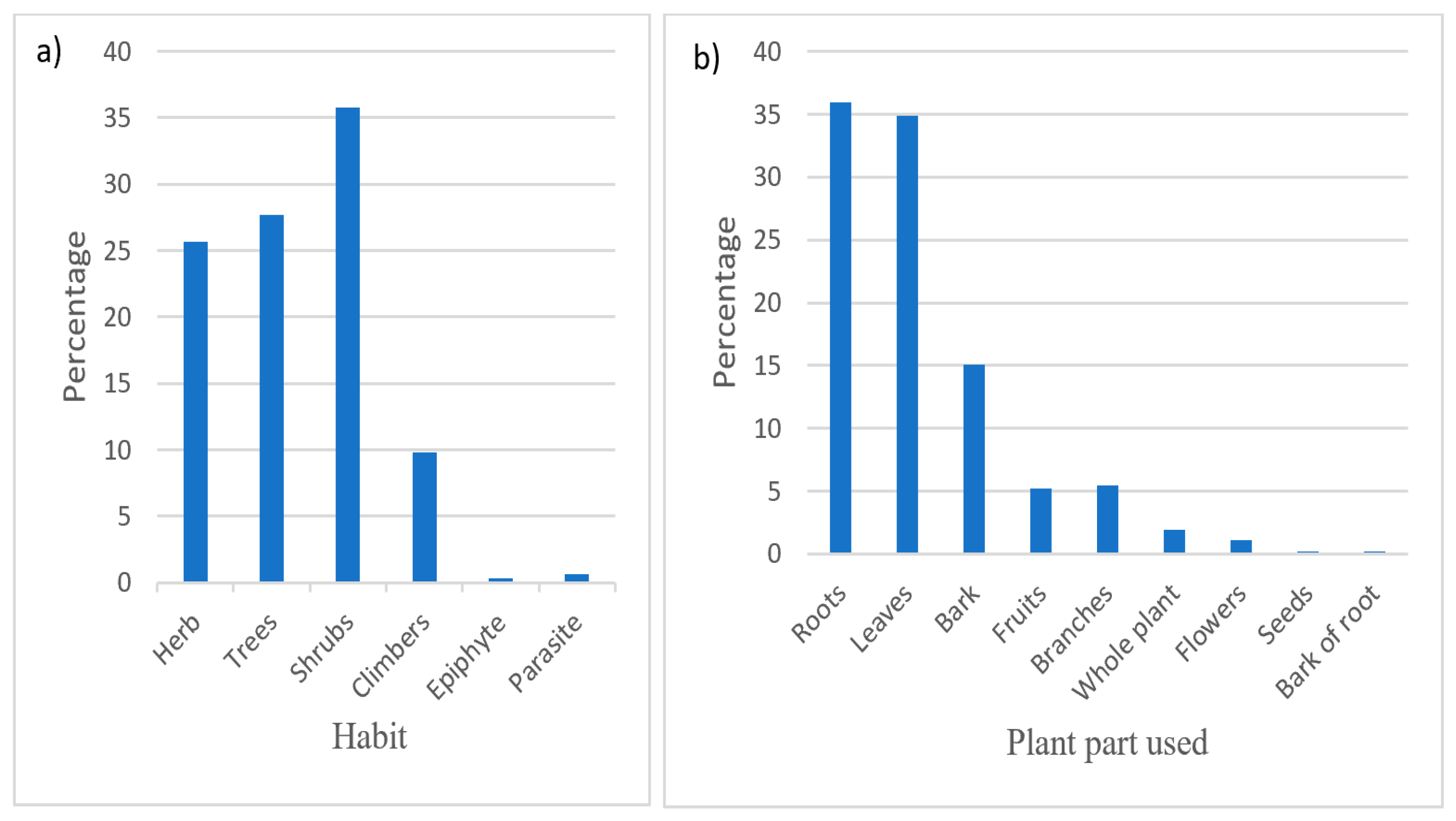
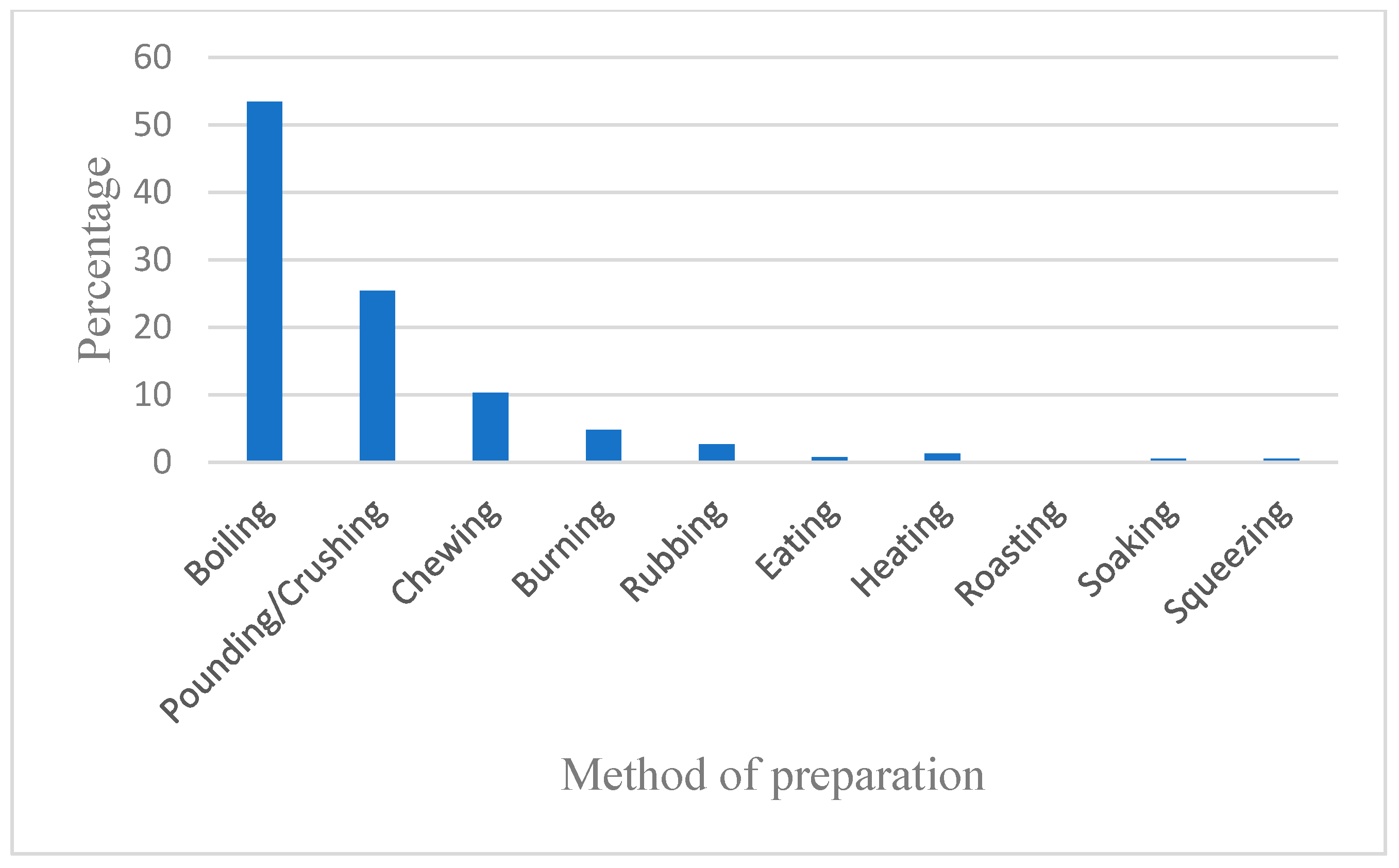
3.4. Habit, Parts Used for Medicine and Methods of Preparation
3.5. Informant Consensus Factor (ICF)
3.6. Fidelity Level (FL)
3.7. Jaccard’s Coefficient of Similarity
3.8. Threats to Medicinal Plants
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lambert, J.; Srivastava, J.; Vietmeyer, N. Medicinal Plants. Rescuing a Global Heritage; World Bank: Washington, DC, USA, 1997. [Google Scholar]
- Thirumalai, T.; Kelumalai, E.; Senthilkumar, B.; David, E. Ethnobotanical study of medicinal plants used by the local people in Vellore District, Tamilnadu. Indian Ethnobot. Leafl. 2009, 13, 1302–1311. [Google Scholar]
- Rasool, H.B. Medicinal Plants. Importance and Uses. Pharmaceut. Anal. Acta 2012, 3, e139. [Google Scholar] [CrossRef]
- Musila, W.; Kisangau, D.; Muema, J. Conservation Status and Use of Medicinal Plants by Traditional Medical Practitioners in Machakos District; Kenya National Museums of Kenya: Nairobi, Kenya, 2000. [Google Scholar]
- Mahwasane, S.T.; Middelton, L.; Boaduo, N. An ethnobotanical survey of indigenous knowledge on medicinal plants used by the traditional healers of the Lwamondo area, Limpopo province. S. Afr. J. Bot. 2013, 88, 69–75. [Google Scholar] [CrossRef]
- Kinyanjui, M.J.; Latva-Käyrä, P.; Bhuwneshwar, P.S.; Kariuki, P.; Gichu, A.; Wamichwe, K. An Inventory of the above ground biomass in the Mau forest ecosystem, Kenya. Open J. Ecol. 2014, 4, 619–627. [Google Scholar] [CrossRef]
- Popovic, Z.; Matic, R.; Bojovic, S.; Stefanovic, M.; Vidakovic, V. Ethnobotany and herbal medicine in modern complementary and alternative medicine: An overview of publications in the field of I&C medicine 2001–2013. J. Ethnopharmacol. 2016, 181, 182–192. [Google Scholar] [CrossRef] [PubMed]
- Maroyi, A.; Cheikhyoussef, A. A comprehensive study of medicinal plants used in rural areas of Namibia and Zimbabwe. Indian J. Tradit. Knowl. 2015, 14, 401–406. [Google Scholar]
- Petrovska, B.B. Historical review of medicinal plants’ usage. Pharmacogn. Rev. 2012, 6, 1–5. [Google Scholar] [CrossRef]
- MEWNR. RDA; Kenya Biodiversity Atlas, Ministry of Environment, Natural Resources and Regional Development Authorities: Nairobi, Kenya, 2015. [Google Scholar]
- Kipkore, W.; Wanjohi, B.; Rono, H.; Kigen, G. A study of the medicinal plants used by the Marakwet Community in Kenya. J. Ethnobiol. Ethnomed. 2014, 10, 24. [Google Scholar] [CrossRef]
- Leaman, D.; Walter, S.; Laird, S.; Alan, R.P.; Dagmar, L.; Sonia, L.; Kumba, F.F.; Katjivena, H.; Natalie, H.; Nirmal, B.; et al. Medicinal Plant Conservation; Newsletter of the Medicinal Plant Specialist Group of the IUCN Survival Commission: Russel Avenue, Ottawa, ON, Canada, 2002; Volume 8, p. 40. [Google Scholar]
- Olembo, N.K.; Fedha, S.S.; Ngaira, S.E. Medicinal and Agricultural Plants of Ikolomani Division Kakamega District; Signal Press Ltd.: Kenya, Nairobi, 1995. [Google Scholar]
- Maundu, P.; Tengnas, B. Useful Trees and Shrubs for Kenya Technical Handbook No.35; World Agroforestry Centre, Eastern and Central Africa Regional Programme, World Agroforestry Centre-Eastern and Central Africa Regional Programme (ICRAF -ECA): Nairobi, Kenya, 2005. [Google Scholar]
- Kokwaro, J.O. Medicinal Plants of East Africa, 3rd ed.; University of Nairobi Press: Nairobi, Kenya, 2009. [Google Scholar]
- Dharani, N.; Yenesew, A. Medicinal Plants of East Africa: An Illustrated Guide; Najma Dharani in Association with Drongo Editing and Publishing, Sterling Publishers Pvt. Ltd.: New Delhi, India, 2010. [Google Scholar]
- Koné, M.W.; Atindehou, K.K. Ethnobotanical inventory of medicinal plants used in traditional veterinary medicine in Northern Côte d’Ivoire (West Africa). S. Afr. J. Bot. 2008, 74, 76–84. [Google Scholar] [CrossRef]
- Lindsay, R.S.; Hepper, F.N. Medicinal Plants of Marakwet, Kenya; Royal Botanic Gardens, Kew: Richmond, UK, 1978; p. 49. [Google Scholar]
- Ichikawa, M. A preliminary report on the ethnobotany of the Suiei Dorobi in Northern Kenya. Afr. Study Monogr. 1987, 7, 1–52. [Google Scholar]
- Johns, T.; Kokwaro, J.O.; Kimanani, E.K. Herbal Remedies of the Luo of Siaya District Kenya. Establishing Quantitative Criteria for Consensus. Econ. Bot. 1990, 44, 369–381. [Google Scholar] [CrossRef]
- Githinji, C.W.; Kokwaro, J.O. Ethnobotanical study of some major species in the family Labiatae from Kenya. J. Ethnopharmacol. 1993, 39, 197–203. [Google Scholar] [CrossRef]
- Munguti, K. Indigenous Knowledge in the Management of Malaria and Visceral Leishmaniasis among the Tugen of Kenya. Indig. Knowl. Dev. Monit. 1997, 5, 10–12. [Google Scholar]
- Keter, K.L.; Mutiso, C.P. Ethnobotanical studies of medicinal plants used by traditional health practitioners in the management of diabetes in Lower Eastern Province, Kenya. J. Ethnopharmacol. 2012, 139, 74–80. [Google Scholar] [CrossRef]
- Kaingu, K.J.; Oduma, A.J.; Kanui, I.T. Practices of traditional birth attendants in Machakos District, Kenya. J. Ethnopharmacol. 2011, 137, 495–502. [Google Scholar] [CrossRef]
- Bussmann, R.W. Ethnobotany of the Samburu of Mt. Nyiru, South Turkana, Kenya. J. Ethnobiol. Ethnomed. 2006, 2, 35. [Google Scholar] [CrossRef]
- Nanyigi, M.O.; Mbaria, J.M.; Lanyasunya, A.L.; Wagate, C.G.; Koros, K.B.; Kaburia, H.F.; Munenge, R.W.; Ogara, W.O. Ethno pharmacological survey of Samburu district, Kenya. J. Ethnobiol. Ethnomed. 2008, 4, 14. [Google Scholar] [CrossRef]
- Omwenga, E.; Okemo, P.; Mbugua, P.; Ogol, C.K. Ethnobotanical survey and antimicrobial evaluation of medicinal plants used by the Samburu Community (Kenya) for treatment of Diarrhea. Pharm. Mag. 2009, 5, 165–172. [Google Scholar] [CrossRef]
- Bussmann, R.W.; Paniagua-Zambrana, N.Y.; Wood, N.; Njapit, S.O.; Njapit, J.N.O.; Osoi, G.S.E.; Kasoe, S.P. Knowledge loss and change between 2002 and 2017. A revisit of plant use of the Maasai of Sekenani Valley, Maasai Mara, Kenya. Econ. Bot. 2018, 72, 207–216. [Google Scholar] [CrossRef]
- Kiringe, J.W. Ecological and anthropological threats to ethno-medicinal plant resources and their utilization in Maasai communal ranches in the Amboseli region of Kenya. Ethnobot. Res. Appl. 2005, 3, 231–242. [Google Scholar] [CrossRef]
- Kiringe, J.W. A survey on the use of Ethnomedicinal health remedies among the Maasai of Southern Kajiado District, Kenya. Ethnobot. Res. Appl. 2006, 73, 61–73. [Google Scholar] [CrossRef]
- Muthee, J.K.; Gakuya, D.W.; Mbaria, J.M.; Kareru, P.G.; Mulei, C.M.; Njonge, F.K. Ethnobotanical study of anthelmintic and other medicinal plants traditionally used in Loitoktok district of Kenya. J. Ethnopharmacol. 2011, 135, 15–21. [Google Scholar] [CrossRef]
- Kimondo, J.; Miaron, J.; Mutai, P.; Njogu, P. Ethnobotanical survey of food and medicinal plants of the Ilkisonko Maasai community in Kenya. J. Ethnopharmacol. 2015, 175, 463–469. [Google Scholar] [CrossRef] [PubMed]
- Nankaya, J.; Nampushi, J.; Petenya, S.; Balslev, H. Ethnomedicinal plants of the Loita Maasai of Kenya. J. Environ. Dev. Sustain. 2019. [Google Scholar] [CrossRef]
- Kareru, P.G.; Kenji, G.M.; Gachanja, A.N.; Keriko, J.M.; Mungai, G. Traditional medicines among the Embu and Mbeere Peoples of Kenya. Afr. J. Tradit. Complement. Altern. Med. 2007, 4, 75–86. [Google Scholar] [CrossRef] [PubMed]
- Kisangau, D.P.; Herrmann, T.M. Utilization and conservation of medicinal plants used for primary health care in Makueni district, Kenya. Int. J. Biodivers. Sci. Manag. 2010, 3, 184–192. [Google Scholar] [CrossRef]
- Okello, S.V.; Nyunja, R.O.; Netondo, G.W.; Onyango, J.C. Ethnobotanical study of medicinal plants used by Sabaots of Mt. Elgon Kenya. Afr. J. Tradit. Complement. Altern. Med. 2010, 7, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Ngari, E.W.; Chiuri, L.W.; Kariuki, S.T.; Huckett, S. Ethnomedicine of Ogiek of River Njoro watershed. Ethnobot. Res. Appl. 2010, 8, 135–8152. [Google Scholar] [CrossRef]
- Jeruto, P.; Lukhoba, C.; Ouma, G.; Otieno, D.; Mutai, C. An ethnobotanical study of medicinal plants used by the Nandi people in Kenya. J. Ethnopharmacol. 2008, 116, 370–376. [Google Scholar] [CrossRef]
- Pascaline, J.; Charles, M.; Lukhoba, C.; George, O. Phytochemical constituents of some medicinal plants used by the Nandis of South Nandi district, Kenya. J. Anim. Plant Sci. 2011, 9, 1201–1210. [Google Scholar]
- Jeruto, P.; Too, E.; Mwamburia, L.A.; Amukab, O. An Inventory of Medicinal Plants used to Treat Gynaecological-Obstetric-Urino-Genital disorders in South Nandi Sub County in Kenya. J. Nat. Sci. Res. 2015, 5, 18. [Google Scholar]
- Kigen, G.; Maritim, A.; Some, F.; Kibosia, J.; Rono, H.; Chepkwony, S.; Kipkore, W.; Wanjoh, B. Ethnopharmacological survey of the medicinal plants used in Tindiret, Nandi County, Kenya. Afr. J. Tradit. Complement. Altern. Med. 2016, 13, 156–168. [Google Scholar] [CrossRef]
- Kaigongi, M.; Musila, F. Ethnobotanical study of medicinal plants used by Tharaka people of Kenya. Int. J. Ethnobiol. Ethnomed. 2015, 1, 1–8. [Google Scholar]
- Otieno, N.E.; Analo, C. Local indigenous knowledge about some medicinal plants in and around Kakamega forest in western Kenya. F1000Research 2012, 2, 1–40. [Google Scholar] [CrossRef]
- Ochwang’i, D.O.; Kimwele, C.N.; Oduma, J.A.; Gathumbi, P.K.; Mbaria, J.M.; Kiama, S.G. Medicinal plants used in treatment and management of cancer in Kakamega County, Kenya. J. Ethnopharmacol. 2014, 151, 1040–1055. [Google Scholar] [CrossRef]
- Mukungu, N.; Abuga, K.; Okalebo, F.; Ingwela, R.; Mwangi, J. Medicinal plants used for management of malaria among the Luhya community of Kakamega East sub-County, Kenya. J. Ethnopharmacol. 2016, 98–107. [Google Scholar] [CrossRef]
- Sikolia, S.F. Medicinal plants of Kakamega forests and their consistency applications: Opportunities and Challenges to-date. J. Pharm. Biol. Sci. 2018, 13, 48–54. [Google Scholar]
- Odongo, E.; Mungai, N.; Mutai, P.; Karumi, E.; Mwangi, J.; Omale, J. Ethnobotanical survey of the medicinal plants used in Kakamega County, western Kenya. Appl. Med. Res. 2018, 4, 22–40. [Google Scholar] [CrossRef]
- Kisangau, D.P.; Kauti, M.; Mwobobia, R.; Kanui, T.; Musimba, N. Traditional knowledge on medicinal plants in Kitui County, Kenya. Int. J. Biodivers. Sci. Manag. 2017, 4, 1–10. [Google Scholar]
- Kigen, G.; Some, F.; Kibosia, J.; Rono, H.; Kiprop, E.; Wanjohi, B.; Kigen, P.; Kipkore, W. Ethnomedicinal Plants Traditionally Used by the Keiyo Community in Elgeyo Marakwet County, Kenya. J. Biodivers. Bioprospect. Dev. 2014, 1, 3. [Google Scholar] [CrossRef]
- Chepchumba, P.B.; Nyanchongi, B.; Masai, R. Ethnobotanical survey of medicinal plants used for treatment of malaria by Kipsigis people in Kericho County, Kenya. J. Pharm. Biol. Sci. 2018, 13, 24–30. [Google Scholar] [CrossRef]
- Mutwiwa, C.; Rotich, B.; Kauti, M.; Rithaa, J. Ethnobotanical Survey of Medicinal Plants in Mwala Sub-County, Machakos County, Kenya. J. Dis. Med. Plants 2018, 4, 110–119. [Google Scholar] [CrossRef]
- Kigondu, E.V.M.; Rukunga, G.M.; Gathirwa, J.W.; Irungu, B.N.; Mwikwabe, N.M.; Amalemba, G.M.; Omar, S.A.; Kirira, P.G. Antiplasmodial and cytotoxicity activities of some selected plants used by the Maasai community, Kenya. S. Afr. J. Bot. 2011, 77, 725–729. [Google Scholar] [CrossRef][Green Version]
- Nyang’au, H.O.; Maingi, J.; Kebira, A. The efficacy of some medicinal plants used locally within Transmara west, Narok County, Kenya against selected Enterobacteria and Candida. J. Pharm. Biol. Sci. 2017, 12, 1. [Google Scholar] [CrossRef]
- Kigen, G.; Kamuren, Z.; Njiru, E.; Wanjohi, B.; Kipkore, W. Ethnomedical Survey of the Plants Used by Traditional Healers in Narok County, Kenya. Complement. Altern. Med. 2019, 2019, 8976937. [Google Scholar] [CrossRef]
- Nyambati, G.K.; Maranga, R.O.; Ozwara, H.; Mbugua, P.K. Use of putative antimalarial herbal medicines among communities in Trans-Mara, Kuria and Suba Districts of Kenya. SEJ Pharmacogn. 2018, 1, 1–14. [Google Scholar]
- Gathirwa, J.W.; Rukunga, G.M.; Mwitari, P.G.; Mwikwabe, N.M.; Kimani, C.W.; Muthaura, C.N.; Kiboi, D.M.; Nyangacha, R.M.; Omara, S.A. Traditional herbal antimalarial therapy in Kilifi district, Kenya. J. Ethnopharmacol. 2011, 134, 434–442. [Google Scholar] [CrossRef]
- Mbuni, Y.M.; Zhou, Y.; Wang, S.; Ngumbau, V.M.; Musili, P.M.; Mutie, F.M.; Njoroge, B.; Kirika, P.M.; Mwachala, G.; Vivian, K.; et al. An annotated checklist of vascular plants of Cherangani hills, Western Kenya. PhytoKeys 2019, 120, 1–90. [Google Scholar] [CrossRef]
- Gakuubi, M.M.; Wanzala, W. A survey of plants and plant products traditionally used in livestock health management in Buuri district, Meru County, Kenya. J. Ethnobiol. Ethnomed. 2012, 8, 39. [Google Scholar] [CrossRef]
- Davis, A.; Wagner, J.R. Who knows? On the importance of identifying, Experts, when researching local ecological knowledge. Hum. Ecol. 2003, 31, 463–489. [Google Scholar] [CrossRef]
- Shiracko, N.; Owuor, B.O.; Gakuubi, M.M.; Wanzala, W. A survey of ethnobotany of the AbaWanga people in Kakamega County, western province of Kenya. Indian J. Tradit. Knowl. 2016, 15, 93–102. [Google Scholar]
- Tugume, P.; Kakudidi, E.K.; Buyinza, M.; Namaalwa, J.; Kamatenesi, M.; Mucunguzi, P.; Kalema, J. Ethnobotanical survey of medicinal plant species used by communities around Mabira Central Forest Reserve, Uganda. J. Ethnobiol. Ethnomed. 2016, 12, 5. [Google Scholar] [CrossRef] [PubMed]
- Trotter, R.T.; Logan, M.H. Informant consensus: A new approach for identifying potentially effective medicinal plants. In Plants in Indigenous Medicine and Diet: Bio-behavioral Approaches; Etkin, N.L., Ed.; Redgrave Publishing Company: New York, NY, USA, 1986; pp. 91–112. [Google Scholar]
- Canales, M.; Hernandez, T.; Caballero, J.; Romo de Vivar, A.; Avila, G.; Duran, A.; Lira, R. Informant consensus factor and antibacterial activity of the medicinal plants used by the people of San Rafael Coxcatlan, Puebla, Mexico. J. Ethnopharmacol. 2005, 97, 429–439. [Google Scholar] [CrossRef] [PubMed]
- Friedman, J.; Zohara, Y.; Amotz, D.; Palewitch, D. A preliminary classification of the healing potential of medicinal plants, based on a rational analysis of an ethnopharmacological field survey among Bedouins in the Negev Desert, Israel. J. Ethnopharmacol. 1986, 16, 275–278. [Google Scholar] [CrossRef]
- Ouelbani, R.; Bensari, S.; Mouas, T.N.; Kheli, D. Ethnobotanical investigations on plants used in folk medicine in the regions of Constantine and Mila (North-East of Algeria). J. Ethnopharmacol. 2016, 194, 196–218. [Google Scholar] [CrossRef]
- Tefera, B.N.; Kim, Y. Ethnobotanical study of medicinal plants in the Hawassa Zuria District, Sidama zone, Southern Ethiopia. J. Ethnobiol. Ethnomed. 2019, 7, 1–21. [Google Scholar] [CrossRef]
- Asowata-Ayodele, A.M.; Afolayan, A.J.; Otunola, G.A. Ethnobotanical survey of culinary herbs and spices used in the traditional medicine system of Nkonkobe Municipality, Eastern Cape, South Africa. S. Afr. J. Bot. 2016, 104, 69–75. [Google Scholar] [CrossRef]
- Pakia, M.; Cooke, J.A. The ethnobotany of the Midzichenda tribes of the coastal forest areas in Kenya: Medicinal plant uses. S. Afr. J. Bot. 2003, 69, 382–395. [Google Scholar] [CrossRef]
- Chauke, M.A.; Shai, L.J.; Mogale, M.A.; Tshisikhawe, M.P.; Mokgotho, M.P. Medicinal plant use of villagers in the Mopani district, Limpopo province, South Africa. Afr. J. Tradit. Complement. Altern. Med. 2015, 12, 9–26. [Google Scholar] [CrossRef]
- Kigen, G.; Kipkore, W.; Wanjohi, B.; Haruki, B.; Kemboi, J. Medicinal plants used by traditional healers in Sangurur, Elgeyo Marakwet County, Kenya. Phcog. Res. 2017, 9, 333–347. [Google Scholar] [CrossRef]
- Njoroge, G.; Rainer, W.; Eric, L.; Ngumi, W.V. Utilization of weed species as sources of traditional medicines in Central Kenya. Lyonia 2004, 7, 71–87. [Google Scholar]
- Joshi, R.A.; Joshi, K. Indigenous knowledge and uses of medicinal plants by local communities of the Kali Gandaki Watershed Area, Nepal. J. Ethnopharmacol. 2000, 73, 175–183. [Google Scholar] [CrossRef]
- Timberlake, J. Vernacular names and uses of plants in northern Kenya. J. East Afr. Nat. Hist. 1994, 83, 31–69. [Google Scholar] [CrossRef][Green Version]
- Tsigemelak, D.; Dharani, J.; Kinyamario, J.I.; Kiboi, S. The utilization of medicinal plants by the Masaai community in arid lands of Kajiado county, Kenya. Int. J. Plant. Anim. Environ. Sci. 2016, 6, 3. [Google Scholar]
- Katema, T.; Etana, D.; Spiridoula, A.; Adugna, T.; Gebeyehu, G.; Jos, G.M.H. Ethnomedical study of plants used for treatment of human and livestock ailments by traditional healers in South Omo, Southern Ethiopia. J. Ethnobiol. Ethnomed. 2013, 9, 32. [Google Scholar] [CrossRef]
- Srithi, K.; Balslev, H.; Wangpakapattanawong, P.; Srisanga, P.; Trisonthi, C. Medicinal plant knowledge and its erosion among the Mien (Yao) in northern Thailand. J. Ethnopharmacol. 2009, 123, 335–342. [Google Scholar] [CrossRef]
- Aziz, M.A.; Khan, A.H.; Adnan, M.; Izatullah, I. Traditional uses of medicinal plants reported by the indigenous communities and local herbal practitioners of Bajaur agency, federally administrated tribal areas, Pakistan. J. Ethnopharmacol. 2017, 198, 268–281. [Google Scholar] [CrossRef]
- Phumthum, M.; Srithi, K.; Inta, A.; Junsongduang, A.; Tangjitman, K.; Pongamornkul, W.; Trisonthi, C.; Balslev, H. Ethnomedicinal plant diversity in Thailand. J. Ethnopharmacol. 2018, 214, 90–98. [Google Scholar] [CrossRef]
- Passulacqua, N.G.; Guariera, P.M.; De Fine, G. Contribution to the knowledge of folk plant medicine in Calabria region. Southern Italy. Filoterapia 2007, 78, 52–68. [Google Scholar] [CrossRef]
- Fortini, P.; Di Marzio, P.; Guarrera, P.; Iorizzi, P.M. Ethnobotanical study on the medicinal plants in the Mainarde Mountains (central-southern Apennine, Italy). J. Ethnopharmacol. 2016, 184, 208–218. [Google Scholar] [CrossRef]
- Salinitro, M.; Vicentini, R.; Bonomi, C.; Tasson, A. Traditional knowledge on wildand cultivated plants in the Kilombero Valley Morogoro Region, Tanzania. J. Ethnobiol. Ethnomed. 2017, 13, 17. [Google Scholar] [CrossRef] [PubMed]
- Sargin, S.A.; Selvi, S.; Büyükcengiz, M. Ethnomedicinal plants of Aydincik District of Mersin, Turkey. J. Ethnopharmacol. 2015, 174, 200–216. [Google Scholar] [CrossRef] [PubMed]
- Gruca, M.; Blach-Overgaard, A.; Balslev, H. African palm ethno-medicine. J. Ethnopharmacol. 2015, 165, 227–237. [Google Scholar] [CrossRef] [PubMed]
- Ansari, I.; Patil, D.T. A brief review on phytochemical and pharmacological profile of Carissa spinarum. Asian J. Pharm. Clin. Res. 2018, 11, 12–18. [Google Scholar] [CrossRef]
- Duncan, C.M.; Buchanan, C.; Chalo, P.M. An ethnobotanical study of medicinal plants used by the Masaai People of Losho, Kenya. Int. J. Pharm. Res. 2016, 6, 2. [Google Scholar]
- Asiimwe, S.; Namutebi, A.; Borg-Karlsson, A.; Kamatenesi-Mugisha, M.; Oryem-Origa, H. Documentation and consensus of indigenous knowledge on medicinal plants used by the local communities in Western Uganda. J. Nat. Prod. Plant Res. 2014, 4, 34–42. [Google Scholar]
- Amri, E.; Kisangau, D.P. Ethnomedicinal study of plants used in villages around Kimboza forest reserve in Morogoro, Tanzania. J. Ethnobiol. Ethnomed. 2012, 8, 1. [Google Scholar] [CrossRef]
- Bouasla, A.; Bouasla, I. Ethnobotanical survey of medicinal plants in northeastern of Algeria. Phytomedicine 2017, 36, 68–81. [Google Scholar] [CrossRef]
- Ndob, B.I.; Mengome, E.L.; Bourobou, H.H.; Banfora, L.Y.; Bivigou, F. Ethnobotanical survey of medicinal plants used as anthelmintic remedies in Gabon. J. Ethnopharmacol. 2016, 191, 360–371. [Google Scholar] [CrossRef]
- Magwede, K.; Wyk, B.E.V.; Wyk, A.E.V. An inventory of Vhavenḓa useful plants. S. Afr. J. Bot. 2018, 122, 57–89. [Google Scholar] [CrossRef]
- Cheikhyoussef, A.; Shapi, M.; Matengu, K.; Ashekele, H.M.U. Ethnobotanical study of indigenous knowledge on medicinal plant use by traditional healers in Oshikoto region, Namibia. J. Ethnobiol. Ethnomed. 2011, 7, 10. [Google Scholar] [CrossRef] [PubMed]
- Umair, M.; Altaf, M.; Abbasi, A.M. An ethnobotanical survey of indigenous medicinal plants in Hafizabad district, Punjab-Pakistan. PLoS ONE 2017, 12, e0177912. [Google Scholar] [CrossRef] [PubMed]
- De Wet, H.; Ngubane, S.C. Traditional herbal remedies used by women in a rural community in northern Maputaland, South Africa, for the treatment of gynaecology and obstetric complaints. S. Afr. J. Bot. 2014, 94, 129–139. [Google Scholar] [CrossRef]
| Count | % | Expected Mean Observation | Statistics | |
|---|---|---|---|---|
| Gender | p value 0.820847 | |||
| Male | 40 | 51.28 | 39 | |
| Female | 38 | 48.72 | 39 | |
| Age * | % | p value < 0.001 | ||
| 15–25 | 1 | 1.28 | 13 | |
| 26–30 | 3 | 3.85 | 13 | |
| 36–45 | 5 | 6.41 | 13 | |
| 46–55 | 10 | 12.82 | 13 | |
| 56–65 | 15 | 19.23 | 13 | |
| 66–75 | 24 | 30.77 | 13 | |
| 76–85 | 20 | 25.64 | 13 | |
| Educational status * | % | p value < 0.001 | ||
| illiterate | 33 | 42.31 | 19.5 | |
| primary | 26 | 33.33 | 19.5 | |
| secondary | 17 | 21.79 | 19.5 | |
| tertiary | 2 | 2.7 | 19.5 |
| Family | Species | Genera | Genera | Family | Species |
|---|---|---|---|---|---|
| Asteraceae | 32 | 21 | Acacia | Leguminosae | 7 |
| Leguminosae | 28 | 15 | Vernonia | Vernonia | 6 |
| Lamiaceae | 18 | 11 | Crotalaria | Leguminosae | 5 |
| Rubiaceae | 14 | 9 | Rhus | Anacardiaceae | 5 |
| Euphorbiaceae | 12 | 8 | Maytenus | Celastraceae | 5 |
| Apocynaceae | 10 | 8 | Solanum | Solanaceae | 5 |
| Malvaceae | 10 | 6 | Helichrysum | Asteraceae | 4 |
| Anacardiaceae | 8 | 4 | Dombeya | Malvaceae | 4 |
| Amaranthaceae | 6 | 4 | Ficus | Moraceae | 4 |
| Celastraceae | 6 | 2 | Polygonum | Polygonaceae | 4 |
| Solanaceae | 6 | 2 |
| Ailment Categories | Specific Conditions | Number of Used Reports | % of Total Species | No. of Taxa | ICF |
|---|---|---|---|---|---|
| Digestive system disorders | Ulcers, diarrhea, stomachache, dysentery, constipation, low appetite, nausea, purgative, intestinal worms, gastrointestinal disorders, amoeba. | 139 | 25.18 | 108 | 0.22 |
| Respiratory tract infections | Cold, cough, respiratory infections, asthma, bronchitis, flue, sore throat, tuberculosis | 101 | 18.30 | 74 | 0.27 |
| Parasitic diseases and other infections | Malaria, fever, measles, headache, yellow fever, ear, conjunctivitis, toothache, mouth blisters eye infections | 99 | 17.93 | 61 | 0.62 |
| Erectile dysfunctions and importance | Male sexual vitality, aphrodisiac | 12 | 7.07 | 10 | 0.18 |
| Gynecological issues | Fertility enhancer, heavy menstrual flows, uterine cleansing, weakness during pregnancy, induction of labor, sterility in women, induce pregnancy, removing placenta, regulation of monthly periods, abortion, after birth pains, menstrual pains | 31 | 5.98 | 8 | 0.76 |
| Skin infections | Wounds, burns, smallpox, ringworms, warts, skin rashes, leprosy, astringent, boils | 33 | 5.62 | 9 | 0.75 |
| Circulatory system diseases | Hypertension, anemia, cuts, hemorrhoids, blood cleanser, hemorrhage, heart attack reduce bleeding, edema. | 22 | 3.99 | 8 | 0.67 |
| Blood and Urinary system disorders | Urinary infections, kidney inflammations. | 11 | 3.8 | 4 | 0.70 |
| Poisonous and animal bites | Snake, centipede and insect bites | 16 | 2.89 | 8 | 0.53 |
| Muscular-skeletal problems inflammation | Backache, joint pains, rheumatism, fractures, joints inflammation, swollen body parts. | 21 | 2.72 | 10 | 0.50 |
| Neurological and nervous System disorders | Convulsions, epilepsy, memory and neurological disorders, madness reduction. | 5 | 2.17 | 4 | 0.50 |
| Genital apparatus diseases | Genital organs infection, sterility, infertility, prostate infections, syphilis, and gonorrhea | 39 | 1.99 | 12 | 0.71 |
| Metabolic disorders | Liver diseases, hepatic. | 15 | 1.45 | 6 | 0.79 |
| Cancers | Breast cancer, prostate cancer, skin cancer | 8 | 0.91 | 4 | 0.57 |
| Frequently Used Species | Local Name | Part Used | Popular Use | NP | N | FL% | References |
|---|---|---|---|---|---|---|---|
| Sclerocarya birrea (A.Rich.) Hochst. | Arolwa (M), Roluwo (P) | R, B | Enlarged spleen and liver | 32 | 59 | 54.3 | [15] |
| Carissa spinarum L. | Loketetwo (P) Eshikata (L) | R, L | Malaria | 38 | 42 | 90.5 | [15,50,54,67] |
| Clerodendrum myricoides (Hochst.) R.Br. ex Vatke | Chebobet (M), Shikuma (L) | R | Chest pains | 16 | 25 | 64.0 | [34,36,39,40,42,47,61] |
| Aloe volkensii Engl. | Cherotwo (M), Tolkos (P), Linakha (L) | L | Pneumonia | 24 | 27 | 88.9 | [11,15,30,44,47,68,69] |
| Mondia whitei (Hook.f.) Skeels | Mukombelo (L) | R | Aphrodisiac | 24 | 36 | 66.7 | [15,22,61] |
| Toddalia asiatica (L.) Lam. | Kipkeres (M), Katamwa (P) | R, Fr, B | Coughs, Colds | 35 | 47 | 74.5 | [15,18,36,38,40,43,46,70,71,72] |
| Syzygium guineense (Willd.) DC. | Lamaiwo (M), Cheptimanwa (P) | B, Fr | Abdominal pains | 13 | 17 | 76.5 | [40,44,47,70,72] |
| Ricinus communis L. | Kimonwo (M), Pondon (P) Libono (L) | R, L | Diarrhea | 20 | 28 | 71.4 | [11,15,36,40,46,47,51,61,71] |
| Erythrina abyssinica DC. | Gorgorwa (P), Korkorwo (M) Omurembe (L) | B, L | Indigestion | 23 | 34 | 67.6 | [11,15,18,34,36,40,42,46,47,61,73] |
| Prunus africana (Hook.f.) Kalkman | Tendwo (M) | B, L | Prostate cancer | 9 | 14 | 64.3 | [11,15,34,36,40,43,44,61,70,72] |
| Asparagus racemosus Willd. | Kabungai (M) | R | Kidney diseases | 17 | 47 | 36.2 | [18,36,39,40,68] |
| Warburgia ugandensis Sprague | Sokwo (M) | B, L | Respiratory disorders | 20 | 22 | 90.9 | [15,32] |
| Withania somnifera (L.) Dunal | Tarkukai (M), Akakagh (P) | R, L | Relives labor pains | 21 | 29 | 72.4 | [15,18,34,36,42,67,71,72] |
| Basella alba L. | Inderema (L), | L | Regulates monthly periods | 24 | 28 | 85.7 | [15,34,36,39,40,61,71,73] |
| Clausena anisata (Willd.) Hook.f. ex Benth. | Cheboinoiywa (M), Kisimbari (L) | R, B, Br | Heart diseases | 6 | 10 | 60.0 | [15,18,36,46,67,68] |
| Periploca linearifolia Quart.-Dill. and A.Rich. | Sinindet (M), Sinendet (P) | Br, L | Syphilis and Gonorrhea | 32 | 43 | 74.4 | [11,15,18,36,38,40] |
| Urtica massaica Mildbr. | Kimelei (M) | R, L | Ulcers | 27 | 31 | 87.0 | [15,40,44,71] |
| Tragia brevipes Pax | Kimelei (M), Chemelei (P) | Br, L, R | Rheumatism | 5 | 13 | 38.5 | [15,18,34,40,42,44,67,71] |
| Study Area (County) | Year of Study | Species No. (x and y) | Common Species (z) | Jaccard’s Coefficient | % Similarity | References |
|---|---|---|---|---|---|---|
| Cherangani | 2019 | 286 | This review | |||
| Machakos | 2018 | 51 | 23 | 0.06 | 6 | [51] |
| Kakamega | 2018 | 250 | 66 | 0.13 | 13 | [46] |
| Kakamega | 2018 | 94 | 54 | 0.12 | 12 | [47] |
| Sungurur | 2017 | 99 | 72 | 0.16 | 16 | [70] |
| Makueni | 2017 | 42 | 21 | 0.06 | 6 | [35] |
| Nandi | 2015 | 56 | 34 | 0.09 | 9 | [40] |
| Tharaka Nithi | 2015 | 72 | 21 | 0.06 | 6 | [42] |
| Marakwet | 1978 | 111 | 86 | 0.18 | 18 | [18] |
| Kakamega | 2014 | 65 | 25 | 0.07 | 7 | [44] |
| Keiyo | 2014 | 73 | 59 | 0.14 | 14 | [49] |
| Mt. Elgon | 2010 | 107 | 52 | 0.12 | 12 | [36] |
| Nandi | 2008 | 40 | 19 | 0.05 | 5 | [38] |
| Embu and Mbeere | 2007 | 86 | 45 | 0.11 | 11 | [34] |
| Threats | Frequency (N = 78) | Percentage (%) |
|---|---|---|
| Agricultural expansion | 30 | 38.5 |
| Overgrazing | 16 | 20.5 |
| Overharvesting | 14 | 17.9 |
| Firewood and Charcoal production | 8 | 10.3 |
| Environmental degradation | 6 | 7.7 |
| Others | 4 | 5.1 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mbuni, Y.M.; Wang, S.; Mwangi, B.N.; Mbari, N.J.; Musili, P.M.; Walter, N.O.; Hu, G.; Zhou, Y.; Wang, Q. Medicinal Plants and Their Traditional Uses in Local Communities around Cherangani Hills, Western Kenya. Plants 2020, 9, 331. https://doi.org/10.3390/plants9030331
Mbuni YM, Wang S, Mwangi BN, Mbari NJ, Musili PM, Walter NO, Hu G, Zhou Y, Wang Q. Medicinal Plants and Their Traditional Uses in Local Communities around Cherangani Hills, Western Kenya. Plants. 2020; 9(3):331. https://doi.org/10.3390/plants9030331
Chicago/Turabian StyleMbuni, Yuvenalis M., Shengwei Wang, Brian N. Mwangi, Ndungu J. Mbari, Paul M. Musili, Nyamolo O. Walter, Guangwan Hu, Yadong Zhou, and Qingfeng Wang. 2020. "Medicinal Plants and Their Traditional Uses in Local Communities around Cherangani Hills, Western Kenya" Plants 9, no. 3: 331. https://doi.org/10.3390/plants9030331
APA StyleMbuni, Y. M., Wang, S., Mwangi, B. N., Mbari, N. J., Musili, P. M., Walter, N. O., Hu, G., Zhou, Y., & Wang, Q. (2020). Medicinal Plants and Their Traditional Uses in Local Communities around Cherangani Hills, Western Kenya. Plants, 9(3), 331. https://doi.org/10.3390/plants9030331








