Quercetin as a Natural Therapeutic Candidate for the Treatment of Influenza Virus
Abstract
1. Introduction
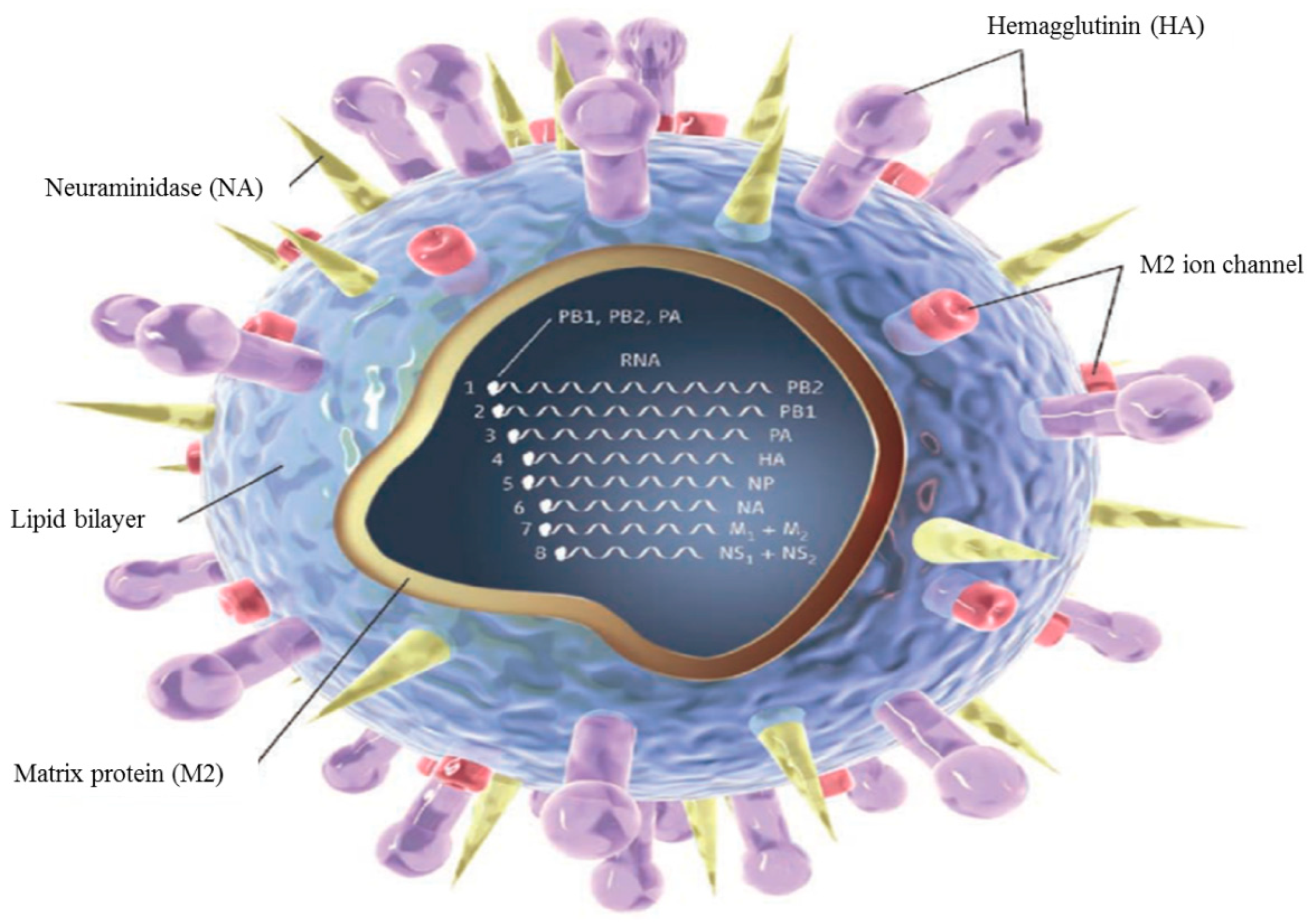
1.1. Influenza Virus
1.2. Viral Pathogenesis
1.3. Medicinal Plants
1.4. Quercetin and Its Derivatives
2. Materials and Methods
2.1. In Vitro and In Silico Studies against Influenza Virus
2.1.1. General Overview
2.1.2. No Activity against Influenza Virus
2.1.3. Anti-Inflammatory and Immunomodulatory Effects
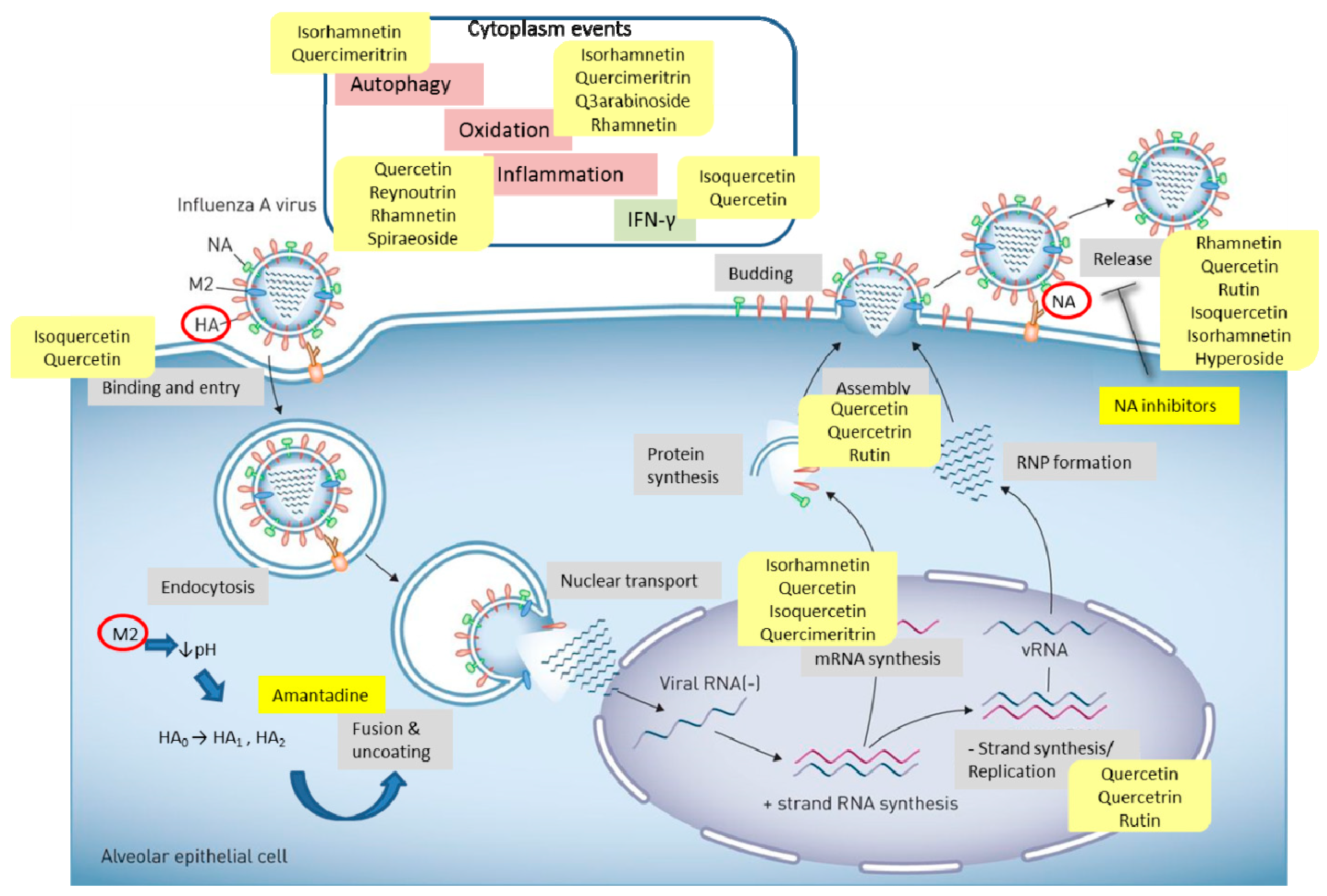
2.1.4. Influence on Molecular Pathways
2.1.5. Neuraminidase Inhibitory Activity
2.1.6. In Silico and Docking Studies
2.1.7. Hemagglutinin Inhibitory Activity
2.2. In Vivo and Human Studies against Influenza Virus
3. Conclusions
4. Future Perspective
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| AP-1 | activator protein-1 |
| APND | amidopyrine-N-demethylase |
| ANND | analgin-N-demethylase |
| CDK4 | cyclin-dependent kinase 4 |
| CPE | cytopathic effect |
| dpi | days postinfection |
| DAD | diode array detector |
| EC50 | effective concentration 50% |
| EGC | epigallocatechin |
| EGCG | epigallocatechin gallate |
| GFP | green fluorescent protein |
| HPLC | high-performance liquid chromatography |
| HNE | 4-hydroxynonenal |
| hpi | hour postinfection |
| 16HBE | human bronchial epithelial cells |
| HSF | human skin fibroblasts |
| iNOS | inducible nitric oxide synthase |
| IV | influenza virus |
| IAV | influenza A virus |
| IC50 | inhibitory concentration 50% |
| IFN | interferon |
| IL | interleukin |
| LPO | lipid peroxidation |
| MIP | macrophage inflammatory protein |
| MHC | major histocompatibility complex |
| MDA | malondialdehyde |
| MST | microscale thermophoresis |
| MCP-1 | monocyte chemoattractant protein-1 |
| Nox2 | NADPH oxidase 2 |
| NBT | nitro blue tetrazolium |
| NMR | nuclear magnetic resonance |
| 2-5 OAS | 20:50-oligoadenylate synthetase |
| PBMC | peripheral blood mononuclear cell |
| Q3R | quercetin 3-rhamnoside |
| RNS | reactive nitrogen species |
| ROS | reactive oxygen species |
| Ra | receptor antagonist |
| rhGM-CSF | recombinant human granulocyte-macrophage colony-stimulating factor |
| RANTES | regulated on activation: normal T lymphocytes expressed |
| SI | selectivity index |
| S | spike protein |
| SAR | structure–activity relationship |
| SOD | superoxide dismutase |
| SPR | surface plasmon resonance |
| Th | T helper |
| TBARS | thiobarbituric acid reactive substances |
| TLR7 | toll-like receptor 7 |
| TRAIL | TNF-related apoptosis-inducing ligand |
| TNF | tumor necrosis factor |
| UPLC | ultrahigh performance liquid chromatography |
| VSMC | vascular smooth muscle cell |
| XO | xanthine oxidase |
| WBC | white blood cells |
References
- Rajasekaran, D.; Palombo, E.A.; Yeo, T.C.; Ley, D.L.S.; Tu, C.L.; Malherbe, F.; Grollo, L. Identification of Traditional Medicinal Plant Extracts with Novel Anti-Influenza Activity. PLoS ONE 2013, 8, e79293. [Google Scholar] [CrossRef]
- Bouvier, N.M.; Palese, P. The biology of influenza viruses. Vaccine 2008, 26, D49–D53. [Google Scholar] [CrossRef]
- Palese, P.; Shaw, M. Orthomyxoviridae: The Viruses and their Replication. Fields Virol. 2007, 26, 1647–1689. [Google Scholar]
- WHO. Vaccines against Influenza. In The Weekly Epidemiological Record; WHO Position Paper—November 2012; WHO: Geneva, Switzerland, 2012; pp. 461–476. [Google Scholar]
- Iuliano, A.D.; Roguski, K.M.; Chang, H.H.; Muscatello, D.J.; Palekar, R.; Tempia, S.; Cohen, C.; Gran, J.M.; Schanzer, D.; Cowling, B.J.; et al. Estimates of global seasonal influenza-associated respiratory mortality: A modelling study. Lancet 2018, 391, 1285–1300. [Google Scholar] [CrossRef]
- Macias, A.E.; McElhaney, J.; Chaves, S.S.; Nealon, J.; Nunes, M.C.; Samson, S.I.; Seet, B.T.; Weinke, T.; Yu, H. The disease burden of influenza beyond respiratory illness. Vaccine 2020, 264. [Google Scholar] [CrossRef]
- Mehrbod, P.; Ande, S.R.; Alizadeh, J.; Rahimizadeh, S.; Shariati, A.; Malek, H.; Hashemi, M.; Glover, K.K.M.; Sher, A.A.; Coombs, K.M.; et al. The roles of apoptosis, autophagy and unfolded protein response in arbovirus, influenza virus, and HIV infections. Virulence 2019, 10, 376–413. [Google Scholar] [CrossRef] [PubMed]
- Putri, W.C.; Muscatello, D.J.; Stockwell, M.S.; Newall, A. Economic burden of seasonal influenza in the United States. Vaccine 2018, 36, 3960–3966. [Google Scholar] [CrossRef] [PubMed]
- Khorramdelazad, H.; Kazemi, M.H.; Najafi, A.; Keykhaee, M.; Emameh, R.Z.; Falak, R. Immunopathological similarities between COVID-19 and influenza: Investigating the consequences of Co-infection. Microb. Pathog. 2020, 104554. [Google Scholar] [CrossRef] [PubMed]
- Ding, Q.; Lu, P.; Fan, Y.; Xia, Y.; Liu, M. The clinical characteristics of pneumonia patients coinfected with 2019 novel coronavirus and influenza virus in Wuhan, China. J. Med. Virol. 2020, 92, 1549–1555. [Google Scholar] [CrossRef]
- Ge, W.; Jingdong, M.; Jialun, G.; Yang, S.; Yue, W.; Dan, F.; Muru, W.; De-an, T.; Peiyuan, L. Is Co-Infection with Influenza Virus a Protective Factor of COVID-19? Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Zhang, A.J.; Chan, J.F.; Liu, F.; Li, C.; Chen, Y.; Chu, H.; Lau, S.Y.; Wang, P.; Chan, C.C.; Poon, V.K.; et al. Co-infection by severe acute respiratory syndrome coronavirus 2 and influenza A(H1N1)pdm09 virus enhances the severity of pneumonia in golden Syrian hamsters. Clin. Infect. Dis. 2020, ciaa1747. [Google Scholar] [CrossRef]
- Drake, T.; Ho, A.; Turtle, L.; Russell, C.; Harrison, E.; Semple, C. Influenza Infection in Patients Hospitalized with COVID-19: Rapid Report from CO-CIN Data. In Proceedings of the 59 SAGE Meeting, London, UK, 24 September 2020. [Google Scholar]
- Hayden, F.G. Respiratory viral threats. Curr. Opin. Infect. Dis. 2006, 19, 169–178. [Google Scholar] [CrossRef] [PubMed]
- Soema, P.C.; Kompier, R.; Amorij, J.-P.; Kersten, G.F. Current and next generation influenza vaccines: Formulation and production strategies. Eur. J. Pharm. Biopharm. 2015, 94, 251–263. [Google Scholar] [CrossRef] [PubMed]
- Barik, S. New treatments for influenza. BMC Med. 2012, 10, 104. [Google Scholar] [CrossRef] [PubMed]
- Meijer, A.; Rebelo-De-Andrade, H.; Correia, V.; Besselaar, T.; Drager-Dayal, R.; Fry, A.; Gregory, V.; Gubareva, L.V.; Kageyama, T.; Lackenby, A.; et al. Global update on the susceptibility of human influenza viruses to neuraminidase inhibitors, 2012–2013. Antivir. Res. 2014, 110, 31–41. [Google Scholar] [CrossRef] [PubMed]
- WHO. Global Influenza Strategy 2019–2030; Weekly Prevention, Control and Preparation 2019; WHO: Geneva, Switzerland, 2019; Available online: https://apps.who.int/iris/handle/10665/311184 (accessed on 20 June 2020).
- Fedson, D.S. Confronting an influenza pandemic with inexpensive generic agents: Can it be done? Lancet Infect. Dis. 2008, 8, 571–576. [Google Scholar] [CrossRef]
- Rodriguez, W.J.; Hall, C.B.; Welliver, R.; Simoes, E.A.F.; Ryan, M.E.; Stutman, H.; Johnson, G.; Van Dyke, R.; Groothuis, J.R.; Arrobio, J.; et al. Efficacy and safety of aerosolized ribavirin in young children hospitalized with influenza: A double-blind, multicenter, placebo-controlled trial. J. Pediatr. 1994, 125, 129–135. [Google Scholar] [CrossRef]
- Gubareva, L.V.; Webster, R.G.; Hayden, F.G. Comparison of the Activities of Zanamivir, Oseltamivir, and RWJ-270201 against Clinical Isolates of Influenza Virus and Neuraminidase Inhibitor-Resistant Variants. Antimicrob. Agents Chemother. 2001, 45, 3403–3408. [Google Scholar] [CrossRef]
- Treanor, J.J.; Hayden, F.G.; Vrooman, P.S.; Barbarash, R.; Bettis, R.; Riff, D.; Singh, S.; Kinnersley, N.; Ward, P.; Mills, R.G. Efficacy and safety of the oral neuraminidase inhibitor oseltamivir in treating acute influenza—A randomized controlled trial. J. Am. Med. Assoc. 2000, 283, 1016–1024. [Google Scholar] [CrossRef]
- Intharathep, P.; Laohpongspaisan, C.; Rungrotmongkol, T.; Loisruangsin, A.; Malaisree, M.; Decha, P.; Aruksakunwong, O.; Chuenpennit, K.; Kaiyawet, N.; Sompornpisut, P.; et al. How amantadine and rimantadine inhibit proton transport in the M2 protein channel. J. Mol. Graph. Model. 2008, 27, 342–348. [Google Scholar] [CrossRef]
- Bouvier, N.M.; Lowen, A.C.; Palese, P. Oseltamivir-Resistant Influenza A Viruses Are Transmitted Efficiently among Guinea Pigs by Direct Contact but Not by Aerosol. J. Virol. 2008, 82, 10052–10058. [Google Scholar] [CrossRef] [PubMed]
- Bouvier, N.M.; Rahmat, S.; Pica, N. Enhanced Mammalian Transmissibility of Seasonal Influenza A/H1N1 Viruses Encoding an Oseltamivir-Resistant Neuraminidase. J. Virol. 2012, 86, 7268–7279. [Google Scholar] [CrossRef] [PubMed]
- Ginting, T.E.; Shinya, K.; Kyan, Y.; Makino, A.; Matsumoto, N.; Kaneda, S.; Kawaoka, Y. Amino acid changes in hemagglutinin contribute to the replication of Ooeltamivir-resistant H1N1 influenza viruses. J. Virol. 2012, 86, 121–127. [Google Scholar] [CrossRef] [PubMed]
- Hussain, M.; Galvin, H.D.; Haw, T.Y.; Nutsford, A.N.; Husain, M. Drug resistance in influenza A virus: The epidemiology and management. Infect. Drug Resist. 2017, 10, 121–134. [Google Scholar] [CrossRef] [PubMed]
- Lampejo, T. Influenza and antiviral resistance: An overview. Eur. J. Clin. Microbiol. Infect. Dis. 2020, 39, 1201–1208. [Google Scholar] [CrossRef]
- Yeganeh, B.; Ghavami, S.; Kroeker, A.L.; Mahood, T.H.; Stelmack, G.L.; Klonisch, T.; Coombs, K.M.; Halayko, A.J. Suppression of influenza A virus replication in human lung epithelial cells by noncytotoxic concentrations bafilomycin A1. Am. J. Physiol. Cell. Mol. Physiol. 2015, 308, L270–L286. [Google Scholar] [CrossRef]
- Yeganeh, B.; Moghadam, A.R.; Tran, A.T.; Rahim, M.N.; Ande, S.R.; Hashemi, M.; Coombs, K.M.; Ghavami, S. Asthma and influenza virus infection:focusing on cell death and stress pathways in influenza virus replication. Iran. J. Allergy Asthma Immunol. 2013, 12, 1–17. [Google Scholar]
- Wang, J. Pathogenesis of Influenza. In Radiology of Influenza: A Practical Approach; Springer: Dordrecht, The Netherlands, 2016; p. 9. [Google Scholar]
- Fukuyama, S.; Kawaoka, Y. The pathogenesis of influenza virus infections: The contributions of virus and host factors. Curr. Opin. Immunol. 2011, 23, 481–486. [Google Scholar] [CrossRef]
- Oda, T.; Akaike, T.; Hamamoto, T.; Suzuki, F.; Hirano, T.; Maeda, H. Oxygen radicals in influenza-induced pathogenesis and treatment with pyran polymer-conjugated SOD. Science 1989, 244, 974–976. [Google Scholar] [CrossRef]
- Buffinton, G.D.; Christen, S.; Peterhans, E.; Stocker, R. Oxidative Stress in Lungs of Mice Infected with Influenza a Virus. Free Radic. Res. Commun. 1992, 16, 99–110. [Google Scholar] [CrossRef]
- Schwarz, K.B. Oxidative stress during viral infection: A review. Free. Radic. Biol. Med. 1996, 21, 641–649. [Google Scholar] [CrossRef]
- Akaike, T.; Noguchi, Y.; Ijiri, S.; Setoguchi, K.; Suga, M.; Zheng, Y.M.; Dietzschold, B.; Maeda, H. Pathogenesis of influenza virus-induced pneumonia: Involvement of both nitric oxide and oxygen radicals. Proc. Natl. Acad. Sci. USA 1996, 93, 2448–2453. [Google Scholar] [CrossRef] [PubMed]
- Peterhans, E. Oxidants and Antioxidants in Viral Diseases: Disease Mechanisms and Metabolic Regulation. J. Nutr. 1997, 127, 962S–965S. [Google Scholar] [CrossRef] [PubMed]
- Murphy, A.W.; Platts-Mills, T.A.; Lobo, M.; Hayden, F. Respiratory nitric oxide levels in experimental human influenza. Chest 1998, 114, 452–456. [Google Scholar] [CrossRef] [PubMed]
- Cox, N.J.; Hughes, J.M. New Options for the Prevention of Influenza. N. Engl. J. Med. 1999, 341, 1387–1388. [Google Scholar] [CrossRef] [PubMed]
- Han, S.N.; Meydani, S.N. Antioxidants, Cytokines, and Influenza Infection in Aged Mice and Elderly Humans. J. Infect. Dis. 2000, 182, S74–S80. [Google Scholar] [CrossRef]
- De Maeyer, E.; De Maeyer-Guignard, J. Interferons. In The Cytokine Handbook; Academic Press: London, UK, 1994; pp. 265–288. [Google Scholar]
- Samuel, C.E. Antiviral actions of interferon interferon-regulated cellular proteins and their surprisingly selective antiviral activities. Virology 1991, 183, 1–11. [Google Scholar] [CrossRef]
- Pavlovic, J.; Haller, O.; Staeheli, P. Human and mouse Mx proteins inhibit different steps of the influenza virus multiplication cycle. J. Virol. 1992, 66, 2564–2569. [Google Scholar] [CrossRef]
- Tough, D.F.; Borrow, P.; Sprent, J. Induction of Bystander T Cell Proliferation by Viruses and Type I Interferon in Vivo. Science 1996, 272, 1947–1950. [Google Scholar] [CrossRef]
- Boehm, U.; Klamp, T.; Groot, M.; Howard, J.C. Cellular responses to interferon-γ. Annu. Rev. Immunol. 1997, 15, 749–795. [Google Scholar] [CrossRef]
- Marrack, P.; Kappler, J. Subversion of the immune system by pathogens. Cell 1994, 76, 323–332. [Google Scholar] [CrossRef]
- Epstein, F.H.; Dinarello, C.A.; Wolff, S.M. The Role of Interleukin-1 in Disease. N. Engl. J. Med. 1993, 328, 106–113. [Google Scholar] [CrossRef] [PubMed]
- Zhang, M.; Tracey, K. Cytokine Handbook. In Tumor Necrosis Factor; Academic Press: San Diego, CA, USA, 1998; pp. 517–548. [Google Scholar]
- Van Campen, H. Influenza A virus replication is inhibited by tumor necrosis factor-α in vitro. Arch. Virol. 1994, 136, 439–446. [Google Scholar] [CrossRef] [PubMed]
- Snapper, C.M. The cytokine handbook. Immunol. Today 1992, 13, 466–467. [Google Scholar] [CrossRef]
- Jacoby, D.B. Virus-Induced Asthma Attacks. JAMA 2002, 287, 755. [Google Scholar] [CrossRef]
- Ji, C.; Rouzer, C.A.; Marnett, L.J.; Pietenpol, J.A. Induction of cell cycle arrest by the endogenous product of lipid peroxidation, malondialdehyde. Carcinogenesis 1998, 19, 1275–1283. [Google Scholar] [CrossRef]
- Kakishita, H.; Hattori, Y. Vascular smooth muscle cell activation and growth by 4-hydroxynonenal. Life Sci. 2001, 69, 689–697. [Google Scholar] [CrossRef]
- Palamara, A.T.; Nencioni, L.; Aquilano, K.; De Chiara, G.; Hernandez, L.; Cozzolino, F.; Ciriolo, M.R.; Garaci, E. Inhibition of Influenza A Virus Replication by Resveratrol. J. Infect. Dis. 2005, 191, 1719–1729. [Google Scholar] [CrossRef]
- Fraternale, A.; Paoletti, M.F.; Casabianca, A.; Oiry, J.; Clayette, P.; Vogel, J.-U.; Cinatl, J.J.; Palamara, A.T.; Sgarbanti, R.; Garaci, E.; et al. Antiviral and Immunomodulatory Properties of New Pro-Glutathione (GSH) Molecules. Curr. Med. Chem. 2006, 13, 1749–1755. [Google Scholar] [CrossRef] [PubMed]
- Akhand, A.A.; Du, J.; Liu, W.; Hossain, K.; Miyata, T.; Nagase, F.; Kato, M.; Suzuki, H.; Nakashima, I. Redox-Linked Cell Surface-Oriented Signaling for T-Cell Death. Antioxid. Redox Signal. 2002, 4, 445–454. [Google Scholar] [CrossRef]
- Nakamura, H.; Nakamura, K.; Yodoi, J. Redox regulation of cellular activation. Annu. Rev. Immunol. 1997, 15, 351–369. [Google Scholar] [CrossRef] [PubMed]
- Saladino, R.; Barontini, M.; Crucianelli, M.; Nencioni, L.; Sgarbanti, R.; Palamara, A.T. Current advances in anti-influenza therapy. Curr. Med. Chem. 2010, 17, 2101–2140. [Google Scholar] [CrossRef] [PubMed]
- Liu, B.; Mori, I.; Hossain, J.; Dong, L.; Chen, Z.; Kimura, Y. Local immune responses to influenza virus infection in mice with a targeted disruption of perforin gene. Microb. Pathog. 2003, 34, 161–167. [Google Scholar] [CrossRef]
- Mileva, M.; Bakalova, R.; Tancheva, L.; Galabov, S. Effect of immobilization, cold and cold-restraint stress on liver monooxygenase activity and lipid peroxidation of influenza virus-infected mice. Arch. Toxicol. 2002, 76, 96–103. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mileva, M.; Bakalova, R.; Tancheva, L.; Galabov, A.; Ribarov, S. Effect of vitamin E supplementation on lipid peroxidation in blood and lung of influenza virus infected mice. Comp. Immunol. Microbiol. Infect. Dis. 2002, 25, 1–11. [Google Scholar] [CrossRef]
- Valyi-Nagy, T.; Dermody, T.S. Role of oxidative damage in the pathogenesis of viral infections of the nervous system. Histol. Histopathol. 2005, 20, 957–967. [Google Scholar] [PubMed]
- Vlahos, R.; Stambas, J.; Selemidis, S. Suppressing production of reactive oxygen species (ROS) for influenza A virus therapy. Trends Pharmacol. Sci. 2012, 33, 3–8. [Google Scholar] [CrossRef]
- Mileva, M. Oxidative stress as a target for medication of influenza virus infection. Acta Microbiol. Bulg. 2016, 32, 3–9. [Google Scholar]
- Khalafalla, M.M. Active principle from moringa oleifera Lam leaves effective against two leukemias and a hepatocarcinoma. Afr. J. Biotechnol. 2010, 9, 8467–8471. [Google Scholar]
- Gurib-Fakim, A.; Brendler, T.; Philips, L.D.; Eloff, J.N. Green Gold: Success Stories Using Southern African Medicinal Plant Species; AAMPS Publishing: Totnes, UK, 2010. [Google Scholar]
- Lin, L.-T.; Hsu, W.-C.; Lin, C.-C. Antiviral Natural Products and Herbal Medicines. J. Tradit. Complement. Med. 2014, 4, 24–35. [Google Scholar] [CrossRef]
- Aqil, F.; Ahmad, I.; Mehmood, Z. Antioxidant and free radical scavenging properties of twelve traditionally used Indian medicinal plants. Turk. J. Biol. 2006, 30, 177–183. [Google Scholar]
- Karimi, A.; Majlesi, M.; Rafieian-Kopaei, M. Herbal versus synthetic drugs; beliefs and facts. J. Nephropharmacol. 2015, 4, 27–30. [Google Scholar]
- Zink, T.; Chaffin, J. Herbal ’health’ products: What family physicians need to know. Am. Fam. Physician 1998, 58, 1133–1140. [Google Scholar] [PubMed]
- Milugo, T.K.; Omosa, L.K.; Ochanda, J.; Owuor, B.; Wamunyokoli, F.; Oyugi, J.; Ochieng, J.W. Antagonistic effect of alkaloids and saponins on bioactivity in the quinine tree (Rauvolfia caffra sond.): Further evidence to support biotechnology in traditional medicinal plants. BMC Complement. Altern. Med. 2013, 13, 285. [Google Scholar] [CrossRef] [PubMed]
- Palhares, R.M.; Drummond, M.G.; Brasil, B.D.S.A.F.; Cosenza, G.P.; Brandão, M.D.G.L.; Oliveira, G. Medicinal Plants Recommended by the World Health Organization: DNA Barcode Identification Associated with Chemical Analyses Guarantees Their Quality. PLoS ONE 2015, 10, e0127866. [Google Scholar] [CrossRef] [PubMed]
- Geldenhuys, C.; Mitchell, D. Sustainable Harvesting Technologies in Commercialising Medicinal Plants—A Southern African Guide; Sun Press: Stellenbosch, South Africa, 2006. [Google Scholar]
- Street, R.A.; Prinsloo, G. Commercially Important Medicinal Plants of South Africa: A Review. J. Chem. 2013, 2013, 1–16. [Google Scholar] [CrossRef]
- Gansukh, E.; Muthu, M.; Paul, D.; Ethiraj, G.; Chun, S.; Gopal, J. Nature nominee quercetin’s anti-influenza combat strategy-Demonstrations and remonstrations. Rev. Med. Virol. 2017, 27, e1930. [Google Scholar] [CrossRef]
- Parasuraman, S.; David, A.V.A.; Arulmoli, R. Overviews of biological importance of quercetin: A bioactive flavonoid. Pharmacogn. Rev. 2016, 10, 84–89. [Google Scholar] [CrossRef]
- Chun, O.K.; Chung, S.-J.; Claycombe, K.J.; Song, W.O. Serum C-Reactive Protein Concentrations Are Inversely Associated with Dietary Flavonoid Intake in U.S. Adults. J. Nutr. 2008, 138, 753–760. [Google Scholar] [CrossRef]
- Mehrbod, P.; Abdalla, M.A.; Fotouhi, F.; Heidarzadeh, M.; Aro, A.O.; Eloff, J.N.; McGaw, L.J.; Fasina, F.O. Immunomodulatory properties of quercetin-3-O-α-L-rhamnopyranoside from Rapanea melanophloeos against influenza a virus. BMC Complement. Altern. Med. 2018, 18, 184. [Google Scholar] [CrossRef]
- Lin, C.-F.; Leu, Y.-L.; Al-Suwayeh, S.A.; Ku, M.-C.; Hwang, T.-L.; Fang, J.-Y. Anti-inflammatory activity and percutaneous absorption of quercetin and its polymethoxylated compound and glycosides: The relationships to chemical structures. Eur. J. Pharm. Sci. 2012, 47, 857–864. [Google Scholar] [CrossRef] [PubMed]
- Delgado, L.; Fernandes, I.; González-Manzano, S.; De Freitas, V.; Mateus, N.; Santos-Buelga, C. Anti-proliferative effects of quercetin and catechin metabolites. Food Funct. 2014, 5, 797. [Google Scholar] [CrossRef] [PubMed]
- Gansukh, E.; Kazibwe, Z.; Pandurangan, M.; Judy, G.; Kim, D.H. Probing the impact of quercetin-7-O-glucoside on influenza virus replication influence. Phytomedicine 2016, 23, 958–967. [Google Scholar] [CrossRef] [PubMed]
- Li, M.Y.; Xu, Z. Quercetin in a lotus leaves extract may be responsible for antibacterial activity. Arch. Pharmacal Res. 2008, 31, 640–644. [Google Scholar] [CrossRef]
- Atashpour, S.; Fouladdel, S.; Movahhed, T.K.; Barzegar, E.; Ghahremani, M.H.; Ostad, S.N.; Azizi, E. Quercetin induces cell cycle arrest and apoptosis in CD133+ cancer stem cells of human colorectal HT29 cancer cell line and enhances anticancer effects of doxorubicin. Iran J. Basic Med. Sci 2015, 18, 635–643. [Google Scholar]
- Dajas, F. Life or death: Neuroprotective and anticancer effects of quercetin. J. Ethnopharmacol. 2012, 143, 383–396. [Google Scholar] [CrossRef]
- Yu, B.; Liu, Y.-H.; Yu, B.; Wang, Z.-Y.; Zang, J.-N.; Yu, C. Dietary quercetin ameliorates nonalcoholic steatohepatitis induced by a high-fat diet in gerbils. Food Chem. Toxicol. 2013, 52, 53–60. [Google Scholar] [CrossRef]
- Choi, H.J.; Song, J.H.; Park, K.S.; Kwon, D.-H. Inhibitory effects of quercetin 3-rhamnoside on influenza A virus replication. Eur. J. Pharm. Sci. 2009, 37, 329–333. [Google Scholar] [CrossRef]
- Mehrbod, P.; Ebrahimi, S.N.; Fotouhi, F.; Eskandari, F.; Eloff, J.N.; McGaw, L.; Fasina, F.O. Experimental validation and computational modeling of anti-influenza effects of quercetin-3-O-α-L-rhamnopyranoside from indigenous south African medicinal plant Rapanea melanophloeos. BMC Complement. Altern. Med. 2019, 19, 1–11. [Google Scholar] [CrossRef]
- Murota, K.; Terao, J. Antioxidative flavonoid quercetin: Implications of its intenstinal absorption and metabolism. Arch. Biochem. Biophys. 2003, 417, 12–17. [Google Scholar] [CrossRef]
- Dayem, A.A.; Choi, H.Y.; Kim, Y.B.; Cho, S.-G. Antiviral Effect of Methylated Flavonol Isorhamnetin against Influenza. PLoS ONE 2015, 10, e0121610. [Google Scholar] [CrossRef] [PubMed]
- Pawlikowska-Pawlęga, B.; Gruszecki, W.I.; Misiak, L.; Paduch, R.; Piersiak, T.; Zarzyka, B.; Pawelec, J.; Gawron, A. Modification of membranes by quercetin, a naturally occurring flavonoid, via its incorporation in the polar head group. Biochim. Biophys. Acta Biomembr. 2007, 1768, 2195–2204. [Google Scholar] [CrossRef] [PubMed]
- Albuquerque, U.P.; De Medeiros, P.M.; De Almeida, A.L.S.; Monteiro, J.M.; Neto, E.M.D.F.L.; De Melo, J.G.; Dos Santos, J.P. Medicinal plants of the caatinga (semi-arid) vegetation of NE Brazil: A quantitative approach. J. Ethnopharmacol. 2007, 114, 325–354. [Google Scholar] [CrossRef] [PubMed]
- De Almeida, C.; Silva, T.D.L.E.; De Amorim, E.; Maia, M.D.S.; De Albuquerque, U.P. Life strategy and chemical composition as predictors of the selection of medicinal plants from the caatinga (Northeast Brazil). J. Arid. Environ. 2005, 62, 127–142. [Google Scholar] [CrossRef]
- Luz, L.D.R.; Porto, D.D.; Castro, C.B.; Silva, M.F.S.; Filho, E.D.G.A.; Canuto, K.M.; De Brito, E.S.; Becker, H.; Pessoa, C.D.Ó.; Zocolo, G.J. Metabolomic profile of Schinopsis brasiliensis via UPLC-QTOF-MS for identification of biomarkers and evaluation of its cytotoxic potential. J. Chromatogr. B 2018, 1099, 97–109. [Google Scholar] [CrossRef]
- Ding, F.; Liu, J.; Du, R.; Yu, Q.; Gong, L.; Jiang, H.; Rong, R. Qualitative and Quantitative Analysis for the Chemical Constituents of Tetrastigma hemsleyanum Diels et Gilg Using Ultra-High Performance Liquid Chromatography/Hybrid Quadrupole-Orbitrap Mass Spectrometry and Preliminary Screening for Anti-Influenza Virus Components. Evid. Based Complement. Altern. Med. 2019, 2019, 9414926. [Google Scholar] [CrossRef]
- Kim, Y.; Narayanan, S.; Chang, K.-O. Inhibition of influenza virus replication by plant-derived isoquercetin. Antivir. Res. 2010, 88, 227–235. [Google Scholar] [CrossRef]
- Ibrahim, A.K.; Youssef, A.I.; Arafa, A.S.; Ahmed, S. Anti-H5N1 virus flavonoids fromCapparis sinaicaVeill. Nat. Prod. Res. 2013, 27, 2149–2153. [Google Scholar] [CrossRef]
- Yang, Z.; Bai, L.; Huang, W.-B.; Li, X.-Z.; Zhao, S.-S.; Zhong, N.; Jiang, Z. Comparison of in vitro antiviral activity of tea polyphenols against influenza A and B viruses and structure–activity relationship analysis. Fitoterapia 2014, 93, 47–53. [Google Scholar] [CrossRef]
- Sekizawa, H.; Ikuta, K.; Ohnishi-Kameyama, M.; Nishiyama, K.; Suzutani, T. Identification of the Components in a Vaccinium oldhamii Extract Showing Inhibitory Activity against Influenza Virus Adsorption. Foods 2019, 8, 172. [Google Scholar] [CrossRef]
- Thapa, M.; Kim, Y.; Desper, J.; Chang, K.-O.; Hua, D.H. Synthesis and antiviral activity of substituted quercetins. Bioorg. Med. Chem. Lett. 2012, 22, 353–356. [Google Scholar] [CrossRef] [PubMed]
- Liu, A.; Wang, H.-D.; Lee, S.M.-Y.; Wang, Y.-T.; Du, G. Structure–activity relationship of flavonoids as influenza virus neuraminidase inhibitors and their in vitro anti-viral activities. Bioorg. Med. Chem. 2008, 16, 7141–7147. [Google Scholar] [CrossRef] [PubMed]
- Karimova, E.; Baltina, L.; Spirikhin, L.; Gabbasov, T.; Orshanskaya, Y.; Zarubaev, V. Synthesis and Antiviral Activity of Quercetin Brominated Derivatives. Nat. Prod. Commun. 2015, 10, 1565–1568. [Google Scholar] [CrossRef] [PubMed]
- Lall, N.; Hussein, A.; Meyer, J. Antiviral and antituberculous activity of Helichrysum melanacme constituents. Fitoterapia 2006, 77, 230–232. [Google Scholar] [CrossRef] [PubMed]
- Vasas, A.; Orbán-Gyapai, O.; Hohmann, J. The Genus Rumex: Review of traditional uses, phytochemistry and pharmacology. J. Ethnopharmacol. 2015, 175, 198–228. [Google Scholar] [CrossRef] [PubMed]
- El-Kashak, W.A.; ElShamy, A.I.; Mohamed, T.A.; Farag, M.A.; Saleh, I.A.; Umeyama, A. Rumpictuside A: Unusual 9,10-anthraquinone glucoside from Rumex pictus Forssk. Carbohydr. Res. 2017, 448, 74–78. [Google Scholar] [CrossRef]
- Eropkin, M.I.; Gudkova, T.M.; Konovalova, N.; Shchekanova, S.M.; Iaglovskaia, I.B.; Eropkina, E.M.; Kiselev, O. Antiviral action of some antioxidants/antihypoxants and their combinations with remantadine against human influenza A(H3N2) virus studied in in vitro models. Exp. Clin. Farmacol. 2007, 70, 33–37. [Google Scholar]
- Bertelli, A.; Mannari, C.; Santi, S.; Filippi, C.; Migliori, M.; Giovannini, L. Immunomodulatory activity of shikimic acid and quercitin in comparison with oseltamivir (Tamiflu) in an “in vitro” model. J. Med. Virol. 2008, 80, 741–745. [Google Scholar] [CrossRef]
- Xu, L.; Kelvin, D.J.; Ye, G.Q.; Taub, D.D.; Ben-Baruch, A.; Oppenheim, J.J.; Wang, J.M. Modulation of IL-8 receptor expression on purified human T lymphocytes is associated with changed chemotactic responses to IL-8. J. Leukoc. Biol. 1995, 57, 335–342. [Google Scholar] [CrossRef]
- Huber, A.; Kunkel, S.; Todd, R.; Weiss, S. Regulation of transendothelial neutrophil migration by endogenous interleukin-8. Science 1991, 254, 99–102. [Google Scholar] [CrossRef]
- Tsan, M.F.; White, J.; Del Vecchio, P.J.; Shaffer, J.B. IL-6 enhances TNF-alpha- and IL-1-induced increase of Mn superoxide dismutase mRNA and O2 tolerance. Am. J. Physiol. Content 1992, 263, 22. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Cheng, Y.-X.; Liu, A.-L.; Wang, H.-D.; Wang, Y.-L.; Du, G.-H. Antioxidant, Anti-Inflammatory and Anti-Influenza Properties of Components from Chaenomeles speciosa. Molecules 2010, 15, 8507–8517. [Google Scholar] [CrossRef] [PubMed]
- Cho, W.-K.; Weeratunga, P.; Lee, B.-H.; Park, J.-S.; Kim, C.-J.; Ma, J.Y.; Lee, J.-S. Epimedium koreanum Nakai Displays Broad Spectrum of Antiviral Activity in Vitro and in Vivo by Inducing Cellular Antiviral State. Viruses 2015, 7, 352–377. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.-G.; Lee, H.; Hwang, Y.-H.; Lee, J.-S.; Cho, W.-K.; Ma, J.Y. Eupatorium fortunei and Its Components Increase Antiviral Immune Responses against RNA Viruses. Front. Pharmacol. 2017, 8, 511. [Google Scholar] [CrossRef]
- Mehrbod, P.; Abdalla, M.A.; Njoya, E.M.; Ahmed, A.S.; Fotouhi, F.; Farahmand, B.; Gado, D.A.; Tabatabaian, M.; Fasanmi, O.G.; Eloff, J.N.; et al. South African medicinal plant extracts active against influenza A virus. BMC Complement. Altern. Med. 2018, 18, 112. [Google Scholar] [CrossRef]
- Donelan, N.R.; Basler, C.F.; Garcia-Sarstre, A. A Recombinant Influenza A Virus Expressing anRNA-Binding-Defective NS1 Protein Induces High Levels of BetaInterferon and Is Attenuated inMice. J. Virol. 2003, 77, 13257–13266. [Google Scholar] [CrossRef]
- Yeganeh, B.; Ghavami, S.; Rahim, N.; Klonisch, T.; Halayko, A.; Coombs, K.M. Autophagy activation is required for influenza A virus-induced apoptosis and replication. Biochim. Biophys. Acta Mol. Cell Res. 2018, 1865, 364–378. [Google Scholar] [CrossRef]
- Chen, C.; Jiang, Z.-Y.; Yu, B.; Wu, X.-L.; Dai, C.-Q.; Zhao, C.; Ju, D.-H.; Chen, X. Study on the anti-H1N1 virus effects of quercetin and oseltamivir and their mechanism related to TLR7 pathway. J. Asian Nat. Prod. Res. 2012, 14, 877–885. [Google Scholar] [CrossRef]
- Wan, Q.; Wang, H.; Lin, Y.; Gu, L.; Han, M.; Yang, Z.; Zhang, Y.; Ma, R.; Wang, L.; Wang, Z. Effects of quercetin on CDK4 mRNA and protein expression in A549 cells infected by H1N1. Biomed. Rep. 2013, 1, 766–770. [Google Scholar] [CrossRef][Green Version]
- Cheng, J.; Ohsaki, Y.; Tauchi-Sato, K.; Fujita, A.; Fujimoto, T. Cholesterol depletion induces autophagy. Biochem. Biophys. Res. Commun. 2006, 351, 246–252. [Google Scholar] [CrossRef]
- Gannagé, M.; Dormann, D.; Albrecht, R.; Dengjel, J.; Torossi, T.; Rämer, P.C.; Lee, M.; Strowig, T.; Arrey, F.; Conenello, G.; et al. Matrix Protein 2 of Influenza A Virus Blocks Autophagosome Fusion with Lysosomes. Cell Host Microbe 2009, 6, 367–380. [Google Scholar] [CrossRef] [PubMed]
- Rossman, J.S.; Lamb, R.A. Autophagy, Apoptosis, and the Influenza Virus M2 Protein. Cell Host Microbe 2009, 6, 299–300. [Google Scholar] [CrossRef] [PubMed]
- Das, K.; Aramini, J.M.; Ma, L.-C.; Krug, R.M.; Arnold, E. Structures of influenza A proteins and insights into antiviral drug targets. Nat. Struct. Mol. Biol. 2010, 17, 530–538. [Google Scholar] [CrossRef]
- Byrn, R.A.; Jones, S.M.; Bennett, H.B.; Bral, C.; Clark, M.P.; Jacobs, M.D.; Kwong, A.D.; Ledeboer, M.W.; Leeman, J.R.; McNeil, C.F.; et al. Preclinical Activity of VX-787, a First-in-Class, Orally Bioavailable Inhibitor of the Influenza Virus Polymerase PB2 Subunit. Antimicrob. Agents Chemother. 2015, 59, 1569–1582. [Google Scholar] [CrossRef] [PubMed]
- Jang, K.S. Effects of various sub-ingredients on sensory quality of Korean cabbage kimchi. Korean J. Food Nutr. 1991, 20, 233–240. [Google Scholar]
- Vaidya, B.; Cho, S.-Y.; Oh, K.-S.; Kim, S.H.; Kim, Y.; Jeong, E.-H.; Nguyen, T.T.; Kim, S.H.; Kim, I.S.; Kwon, J.; et al. Effectiveness of Periodic Treatment of Quercetin against Influenza A Virus H1N1 through Modulation of Protein Expression. J. Agric. Food Chem. 2016, 64, 4416–4425. [Google Scholar] [CrossRef]
- Choi, J.-G.; Lee, H.; Kim, Y.S.; Hwang, Y.-H.; Oh, Y.-C.; Lee, B.; Moon, K.M.; Cho, W.-K.; Ma, J.Y. Aloe vera and its Components Inhibit Influenza A Virus-Induced Autophagy and Replication. Am. J. Chin. Med. 2019, 47, 1307–1324. [Google Scholar] [CrossRef]
- Nejatzadeh-Barandozi, F. Antibacterial activities and antioxidant capacity of Aloe vera. Org. Med. Chem. Lett. 2013, 3, 5. [Google Scholar] [CrossRef]
- Glatthaar-Saalmüller, B.; Fal, A.M.; Schönknecht, K.; Conrad, F.; Sievers, H.; Saalmuller, A. Antiviral activity of an aqueous extract derived from Aloe arborescens Mill. against a broad panel of viruses causing infections of the upper respiratory tract. Phytomedicine 2015, 22, 911–920. [Google Scholar] [CrossRef]
- Li, S.-W.; Yang, T.-C.; Lai, C.-C.; Huang, S.-H.; Liao, J.-M.; Wan, L.; Lin, Y.-J.; Lin, C.-W. Antiviral activity of aloe-emodin against influenza A virus via galectin-3 up-regulation. Eur. J. Pharmacol. 2014, 738, 125–132. [Google Scholar] [CrossRef]
- López-Expósito, I.; Castillo, A.; Yang, N.; Liang, B.; Li, X.-M. Chinese herbal extracts of Rubia cordifolia and Dianthus superbus suppress IgE production and prevent peanut-induced anaphylaxis. Chin. Med. 2011, 6, 35. [Google Scholar] [CrossRef] [PubMed]
- Nile, S.H.; Kim, D.H.; Nile, A.; Park, G.S.; Gansukh, E.; Kai, G. Probing the effect of quercetin 3-glucoside from Dianthus superbus L against influenza virus infection- in vitro and in silico biochemical and toxicological screening. Food Chem. Toxicol. 2020, 135, 110985. [Google Scholar] [CrossRef] [PubMed]
- Rakers, C.; Schwerdtfeger, S.-M.; Mortier, J.; Duwe, S.; Wolff, T.; Wolber, G.; Melzig, M.F. Inhibitory potency of flavonoid derivatives on influenza virus neuraminidase. Bioorg. Med. Chem. Lett. 2014, 24, 4312–4317. [Google Scholar] [CrossRef] [PubMed]
- Duan, J.; Lou, J.; Zhang, Q.; Ke, J.; Qi, Y.; Shen, N.; Zhu, B.; Zhong, R.; Wang, Z.; Liu, L.; et al. A Genetic Variant rs1801274 in FCGR2A as a Potential Risk Marker for Kawasaki Disease: A Case-Control Study and Meta-Analysis. PLoS ONE 2014, 9, e103329. [Google Scholar] [CrossRef]
- Lee, I.-K.; Hwang, B.S.; Kim, D.-W.; Kim, J.-Y.; Woo, E.-E.; Lee, Y.-J.; Choi, H.J.; Yun, B.-S. Characterization of Neuraminidase Inhibitors in Korean Papaver rhoeas Bee Pollen Contributing to Anti-Influenza Activities In Vitro. Planta Med. 2016, 82, 524–529. [Google Scholar] [CrossRef]
- Graikou, K.; Kapeta, S.; Aligiannis, N.; Sotiroudis, G.; Chondrogianni, N.; Gonos, E.S.; Chinou, I. Chemical analysis of Greek pollen—Antioxidant, antimicrobial and proteasome activation properties. Chem. Cent. J. 2011, 5, 33. [Google Scholar] [CrossRef]
- Kim, D.H.; Park, G.S.; Nile, A.S.; Kwon, Y.D.; Gansukh, E.; Nile, S.H. Utilization of Dianthus superbus L and its bioactive compounds for antioxidant, anti-influenza and toxicological effects. Food Chem. Toxicol. 2019, 125, 313–321. [Google Scholar] [CrossRef]
- Liu, Z.; Zhao, J.; Li, W.; Wang, X.; Xu, J.; Xie, J.; Tao, K.; Shen, L.; Zhang, R. Molecular Docking of Potential Inhibitors for Influenza H7N9. Comput. Math. Methods Med. 2015, 2015, 480764. [Google Scholar] [CrossRef]
- Liu, Z.; Zhao, J.; Li, W.; Shen, L.; Huang, S.; Tang, J.; Duan, J.; Fang, F.; Huang, Y.; Chang, H.; et al. Computational screen and experimental validation of anti-influenza effects of quercetin and chlorogenic acid from traditional Chinese medicine. Sci. Rep. 2016, 6, 19095. [Google Scholar] [CrossRef]
- Yin, J.; Ma, L.; Wang, H.; Yan, H.; Huiqiang, W.; Jiang, W.; Li, Y. Chinese herbal medicine compound Yi-Zhi-Hao pellet inhibits replication of influenza virus infection through activation of heme oxygenase-1. Acta Pharm. Sin. B 2017, 7, 630–637. [Google Scholar] [CrossRef]
- Sadati, S.M.; Gheibi, N.; Ranjbar, S.; Hashemzadeh, M.S. Docking study of flavonoid derivatives as potent inhibitors of influenza H1N1 virus neuraminidase. Biomed. Rep. 2018, 10, 33–38. [Google Scholar] [CrossRef] [PubMed]
- Xu, L.; Jiang, W.; Jia, H.; Zheng, L.; Xing, J.; Liu, A.; Du, G. Discovery of Multitarget-Directed Ligands Against Influenza A Virus From Compound Yizhihao Through a Predictive System for Compound-Protein Interactions. Front. Cell. Infect. Microbiol. 2020, 10, 16. [Google Scholar] [CrossRef] [PubMed]
- Wu, W.; Li, R.; Li, X.; He, J.; Jiang, S.; Liu, S.; Yang, J. Quercetin as an Antiviral Agent Inhibits Influenza A Virus (IAV) Entry. Viruses 2015, 8, 6. [Google Scholar] [CrossRef] [PubMed]
- Eşanu, V.; Prahoveanu, E.; Crişan, I.; Cioca, A. The effect of an aqueous propolis extract, of rutin and of a rutin-quercetin mixture on experimental influenza virus infection in mice. Virology 1981, 32, 213–215. [Google Scholar]
- Msc, T.A.N.R.; Lakshmi, A.N.V.; Anand, T.; Rao, L.V.; Sharma, G. Protective effects of quercetin during influenza virus-induced oxidative stress. Asia Pac. J. Clin. Nutr. 2000, 9, 314–317. [Google Scholar] [CrossRef]
- Kumar, P.; Sharma, S.; Khanna, M.; Raj, H.G. Effect of Quercetin on lipid peroxidation and changes in lung morphology in experimental influenza virus infection. Int. J. Exp. Pathol. 2003, 84, 127–134. [Google Scholar] [CrossRef]
- Kumar, P.; Khanna, M.; Srivastava, V.; Tyagi, Y.K.; Raj, H.G.; Ravi, K. Effect of quercetin supplementation on lung antioxidants after experimental influenza virus infection. Exp. Lung Res. 2005, 31, 449–459. [Google Scholar] [CrossRef]
- Savov, V.M.; Galabov, A.S.; Tantcheva, L.P.; Mileva, M.M.; Pavlova, E.; Stoeva, E.S.; Braykova, A.A. Effects of rutin and quercetin on monooxygenase activities in experimental influenza virus infection. Exp. Toxicol. Pathol. 2006, 58, 59–64. [Google Scholar] [CrossRef]
- Chan, M.C.W.; Cheung, C.Y.; Chui, W.H.; Tsao, G.S.-W.; Nicholls, J.M.; Chan, Y.; Chan, R.W.Y.; Long, H.T.; Poon, L.L.M.; Guan, Y.; et al. Proinflammatory cytokine responses induced by influenza A (H5N1) viruses in primary human alveolar and bronchial epithelial cells. Respir. Res. 2005, 6, 135. [Google Scholar] [CrossRef]
- Lee, D.C.W.; Cheung, C.-Y.; Law, A.H.Y.; Mok, C.K.P.; Peiris, M.; Lau, A.S.Y. p38 Mitogen-Activated Protein Kinase-Dependent Hyperinduction of Tumor Necrosis Factor Alpha Expression in Response to Avian Influenza Virus H5N1. J. Virol. 2005, 79, 10147–10154. [Google Scholar] [CrossRef]
- Friel, H.; Lederman, H. A nutritional supplement formula for influenza A (H5N1) infection in humans. Med. Hypotheses 2006, 67, 578–587. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.S.; Davis, J.M.; Murphy, E.A.; Carmichael, M.D.; Ghaffar, A.; Mayer, E.P. Gender Differences in Viral Infection after Repeated Exercise Stress. Med. Sci. Sports Exerc. 2004, 36, 1290–1295. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.S.; Davis, J.M.; Murphy, E.A.; Carmichael, M.D.; Carson, J.; Ghaffar, A.; Mayer, E.P. Susceptibility to HSV-1 infection and exercise stress in female mice: Role of estrogen. J. Appl. Physiol. 2007, 103, 1592–1597. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Davis, J.M.; Kohut, M.L.; Colbert, L.H.; Jackson, D.A.; Ghaffar, A.; Mayer, E.P. Exercise, alveolar macrophage function, and susceptibility to respiratory infection. J. Appl. Physiol. 1997, 83, 1461–1466. [Google Scholar] [CrossRef] [PubMed]
- Davis, J.M.; Murphy, E.A.; McClellan, J.L.; Carmichael, M.D.; Gangemi, J.D. Quercetin reduces susceptibility to influenza infection following stressful exercise. Am. J. Physiol. Integr. Comp. Physiol. 2008, 295, R505–R509. [Google Scholar] [CrossRef]
- Fan, D.; Zhou, X.; Zhao, C.; Chen, H.; Zhao, Y.; Gong, X. Anti-inflammatory, antiviral and quantitative study of quercetin-3-O-β-D-glucuronide in Polygonum perfoliatum L. Fitoterapia 2011, 82, 805–810. [Google Scholar] [CrossRef]
- Choi, H.-J.; Song, J.H.; Kwon, D.-H. Quercetin 3-rhamnoside Exerts Antiinfluenza A Virus Activity in Mice. Phytother. Res. 2011, 26, 462–464. [Google Scholar] [CrossRef]
- Smith, M.; Smith, J.C. Repurposing therapeutics for COVID-19: Supercomputer-based docking to the SARS-CoV-2 viral spike protein and viral spike protein-human ACE2 interface. ChemRxiv 2020. [Google Scholar] [CrossRef]
- Omar, S. In-silico identification of potent inhibitors of COVID-19 main protease (Mpro) and angiotensin converting enzyme 2 (ACE2) from natural products: Quercetin, hispidulin, and cirsimaritin exhibited better potential inhibition than hydroxy-chloroquine against COVID-19 main protease active site and ACE2. ChemRxiv 2020. [Google Scholar] [CrossRef]
- Adem, S.; Eyupoglu, V.; Sarfraz, I.; Rasul, A.; Ali, M. Identification of potent COVID-19 main protease (Mpro) inhibitors from natural polyphenols: An in silico strategy unveils a hope against Corona. Preprints 2020. [Google Scholar] [CrossRef]
- Das, S.; Sarmah, S.; Lyndem, S.; Roy, A.S. An investigation into the identification of potential inhibitors of SARS-CoV-2 main protease using molecular docking study. J. Biomol. Struct. Dyn. 2020. [Google Scholar] [CrossRef] [PubMed]
- Mullen, W.; Boitier, A.; Stewart, A.J.; Crozier, A. Flavonoid metabolites in human plasma and urine after the consumption of red onions: Analysis by liquid chromatography with photodiode array and full scan tandem mass spectrometric detection. J. Chromatogr. A 2004, 1058, 163–168. [Google Scholar] [CrossRef]
- Zhao, J.; Yang, J.; Xie, Y. Improvement strategies for the oral bioavailability of poorly water-soluble flavonoids: An overview. Int. J. Pharm. 2019, 570, 118642. [Google Scholar] [CrossRef] [PubMed]
- Williamson, G.; Kerimi, A. Testing of natural products in clinical trials targeting the SARS-CoV-2 (Covid-19) viral spike protein-angiotensin converting enzyme-2 (ACE2) interaction. Biochem. Pharmacol. 2020, 178, 114123. [Google Scholar] [CrossRef]
| Common Name (Systematic Name) | Molecular Formula (MW) | Structure |
|---|---|---|
| Quercetin (3,5,7,3′,4′- pentahydroxyflavon) | C15H10O7 (302.2) | 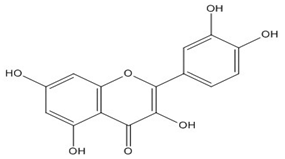 |
| Hyperoside (quercetin- 3-O-galactoside) | C21H20O12 (464.3) | 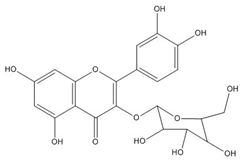 |
| Isoquercetin (quercetin- 3-O-glucoside) | C21H20O12 (464.3) | 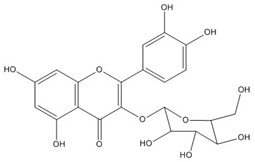 |
| Reynoutrin (quercetin- 3-O-xyloside) | C20H18O11 (434.3) | 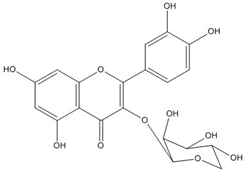 |
| Miquelianin (quercetin- 3-O-glucuronide) | C21H18O13 (478.3) | 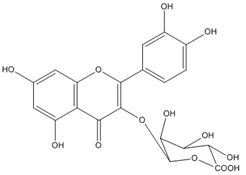 |
| Quercimeritrin (quercetin- 7-O-glucoside) | C21H20O12 (464.3) | 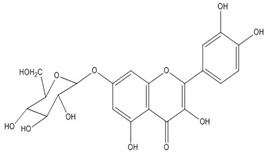 |
| Quercetin 3,4′- diglucoside | C27H30O17 (626.4) | 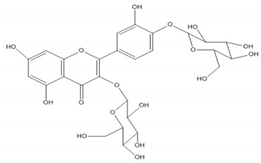 |
| Quercetin-3-glucoside- 7-rhamnoside | C27H30O16 (610.5) | 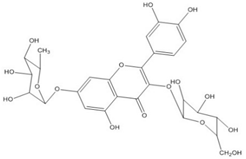 |
| Quercetin 3,7- diglucoside | C27H30O17 (626.5) | 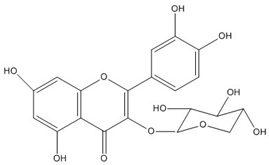 |
| Rutin (quercetin- 3-rutinoside) | C27H30O16 (610.5) |  |
| Quercetrin (quercetin 3-O-rhamnoside) | C21H20O11 (448.4) | 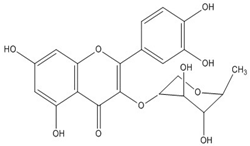 |
| Spiraeoside (quercetin 4-O-glucoside) | C21H20O12 (464.3) | 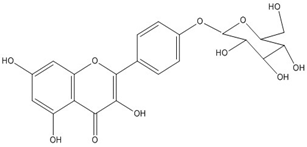 |
| Quercetin 4,7- O-diglucoside | C27H30O17 (626.5) | 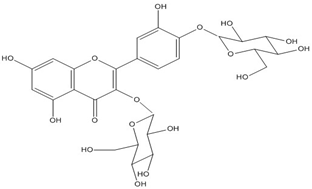 |
| Quercetin 3- O-arabinoside | C20H18O11 (434.3) | 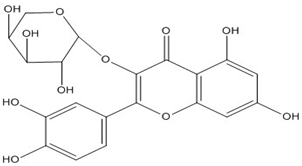 |
| Rhamnetin (quercetin 7-O-methyl) | C16H12O7 (316.2) |  |
| Quercetin 3′- methyl ether | C16H12O7 (316.3) | 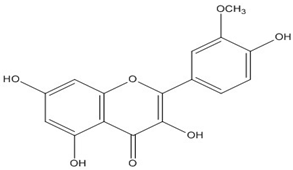 |
| Quercetin-3-O-α-L-rhamnopyranoside | C21H20O11 (228.4) | 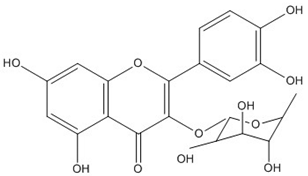 |
| Compound Studied | Human/Animal Study | Study | Reference |
|---|---|---|---|
| Aqueous extract of propolis containing rutin and quercetin | In mice infected with A/PR8/34 (H1N1) | Experimental postinfection of the extract, decrease HA titer in the lung suspensions, slight decrease in mortality and increase in survival length | [142] |
| Quercetin | 1 mg/mL administered orally. In adult male Swiss albino mice infected with influenza virus (A/Hong Kong/8/68) | Decreased oxidative stress by decreasing lipid peroxidation, and antioxidant enzymes; superoxide dismutase and catalase | [143] |
| Quercetin | In mice infected with A/Udorn/317/72 (H3N2) influenza virus | Decreased lipid peroxidation, protected lungs by maintaining the levels of endogenous antioxidant enzymes | [145] |
| Rutin and quercetin | In mice infected with A/Aichi/2/68 (H3N2) | Quercetin showed stronger activity and caused oxidative damage in healthy mice but antioxidant activity in infected animals | [146] |
| Combination of selenium, vitamin E, N-acetyl-cysteine/glutathione, resveratrol and quercetin | Against H5N1 influenza in humans | Antagonized the pathogenic processes of H5N1 influenza in humans | [149] |
| Short-term quercetin feeding before viral challenge | In 4-week-old male ICR mice forced to run on a treadmill for 3 consecutive days to fatigue, inoculated with A/PR8/34 (H1N1) | Reduced the susceptibility to infection | [153] |
| Isoquercetin | In 4-week-old female BALB/c mice infected with human influenza A virus | Decreased IFN-γ, RANTES, and iNOS as indicators of lung inflammation and virus titers | [95] |
| Quercetin-3-O-β-D-glucuronide isolated form Polygonum perfoliatum L. | In 3 and 6 mg/kg concentrations. In mice infected with influenza virus | It could suppress lung edema caused by virus at 28% and 20%, respectively | [154] |
| quercetin 3-rhamnoside (Q3R) | In mice infected with A/WS/33 influenza virus | Decreased weight loss, necrosis, inflammation, mortality, and lung virus titer | [155] |
| Epimedium koreanum Nakai aqueous extract containing quercetin | In BALB/c mice infected with 5MLD50 of H1N1, H5N2, H7N3, and H9N2 influenza viruses | Reduced viral titers and body weight loss. Inhibited viral replication and promoted the survival | [111] |
| Quercetin and chlorogenic acid | In BALB/c female mice infected with A/PR8/34 (H1N1) | Improved lung index and survival rate | [137] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mehrbod, P.; Hudy, D.; Shyntum, D.; Markowski, J.; Łos, M.J.; Ghavami, S. Quercetin as a Natural Therapeutic Candidate for the Treatment of Influenza Virus. Biomolecules 2021, 11, 10. https://doi.org/10.3390/biom11010010
Mehrbod P, Hudy D, Shyntum D, Markowski J, Łos MJ, Ghavami S. Quercetin as a Natural Therapeutic Candidate for the Treatment of Influenza Virus. Biomolecules. 2021; 11(1):10. https://doi.org/10.3390/biom11010010
Chicago/Turabian StyleMehrbod, Parvaneh, Dorota Hudy, Divine Shyntum, Jarosław Markowski, Marek J. Łos, and Saeid Ghavami. 2021. "Quercetin as a Natural Therapeutic Candidate for the Treatment of Influenza Virus" Biomolecules 11, no. 1: 10. https://doi.org/10.3390/biom11010010
APA StyleMehrbod, P., Hudy, D., Shyntum, D., Markowski, J., Łos, M. J., & Ghavami, S. (2021). Quercetin as a Natural Therapeutic Candidate for the Treatment of Influenza Virus. Biomolecules, 11(1), 10. https://doi.org/10.3390/biom11010010








