Metabolic Characteristics of Frail Older People with Diabetes Mellitus—A Systematic Search for Phenotypes
Abstract
1. Introduction
2. Aims
3. Materials and Methods
3.1. Data Source
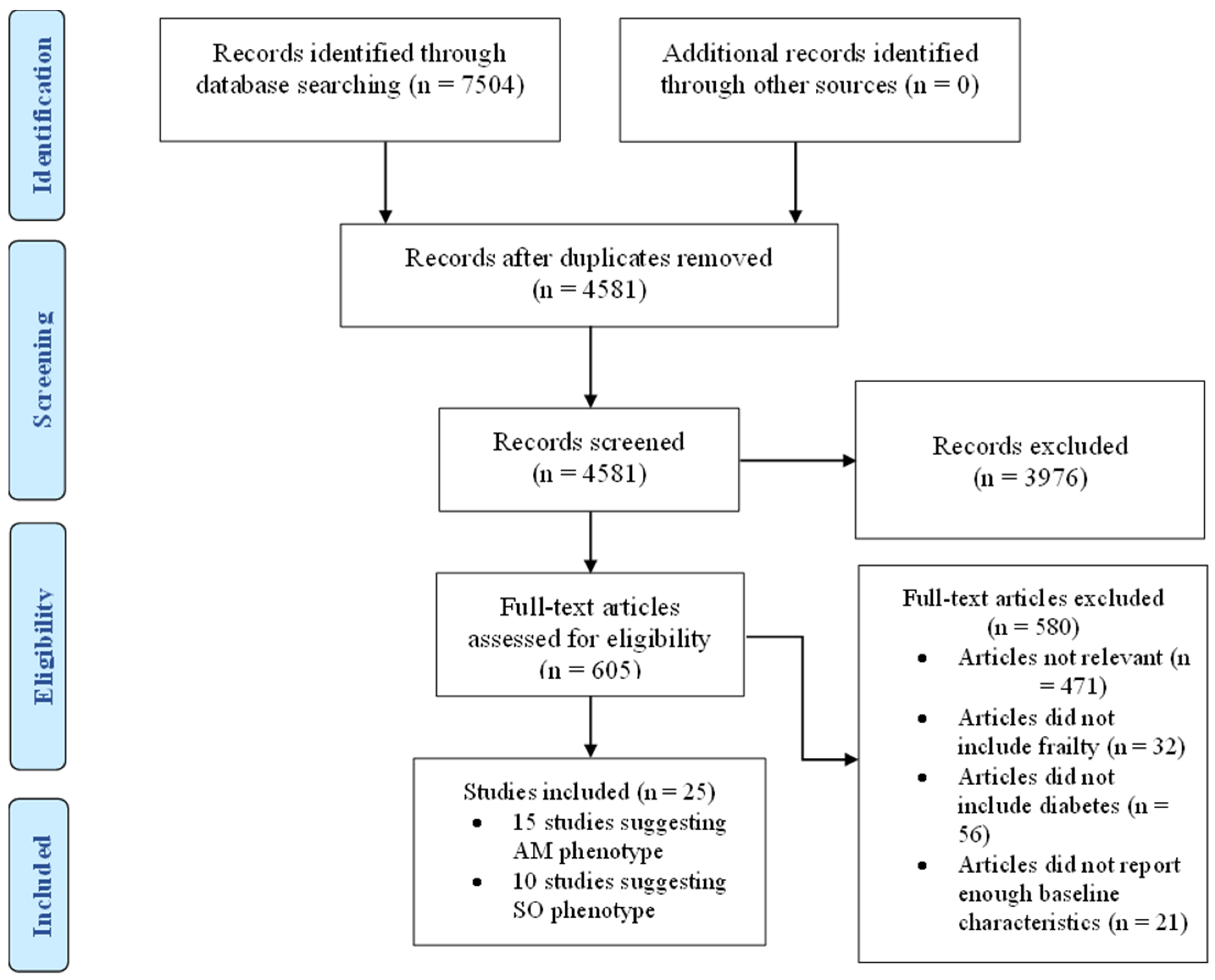
3.2. Study Selection
3.3. Data Extraction
4. Results
4.1. Studies Suggesting AM Phenotype
4.2. Studies Suggesting SO Phenotype
5. Discussion
6. Conclusions
7. Future Perspectives
8. Key Points
- In older people, frailty is an important diabetes-related complication;
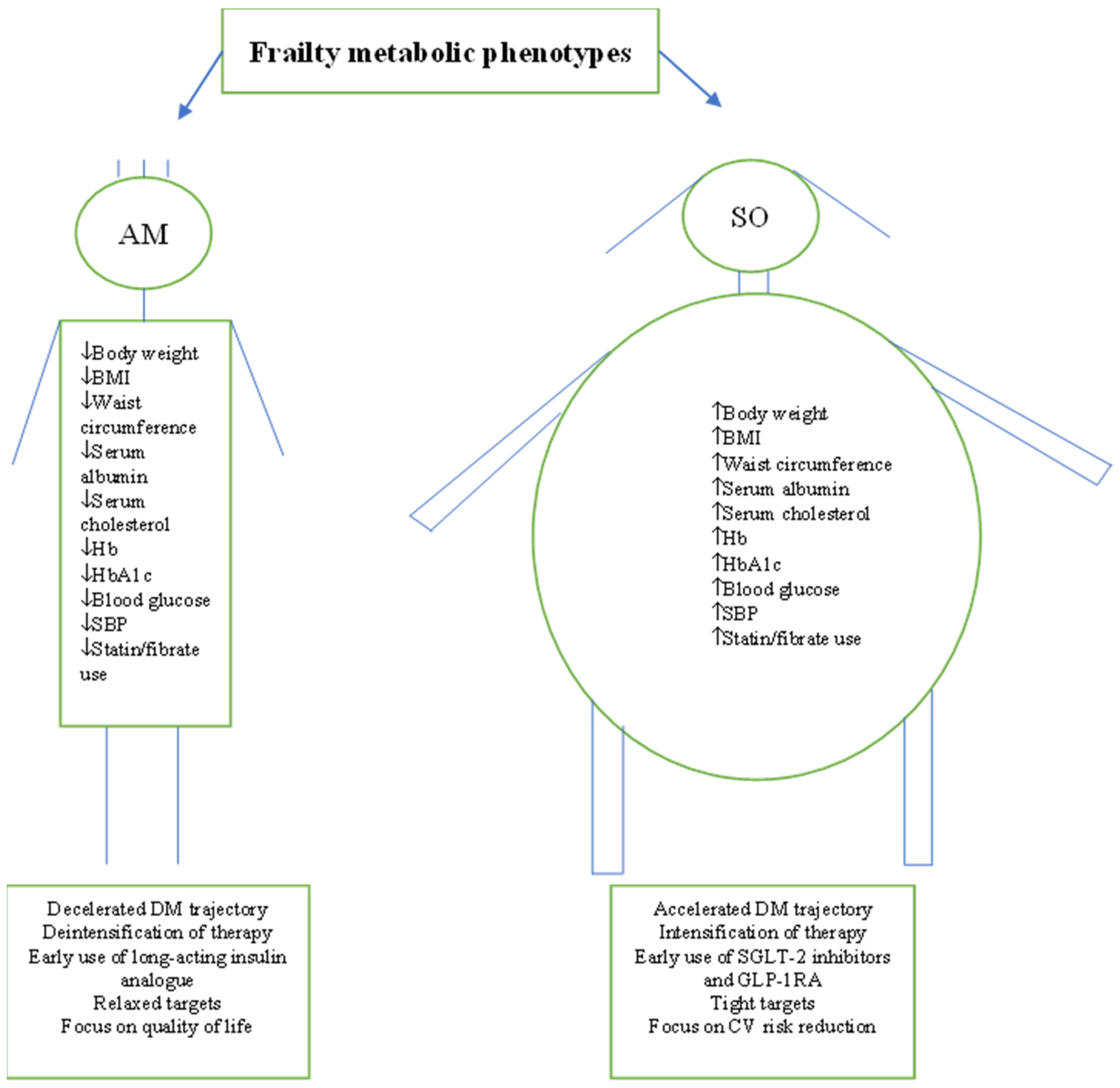
- Frailty is not a metabolically homogeneous condition;
- Current literature suggests that frailty is a spectrum that spans from an anorexic malnourished to sarcopenic obese phenotypes;
- The anorexic malnourished phenotype is associated with less insulin resistance and a high risk of hypoglycaemia while the sarcopenic obese phenotype is characterised by high insulin resistance and less risk of hypoglycaemia;
- Future studies are still required to further characterise the metabolic spectrum of frailty.
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Sun, H.; Saeedi, P.; Karuranga, S.; Pinkepank, M.; Ogurtsova, K.; Duncan, B.B.; Stein, C.; Basit, A.; Chan, J.C.; Mbanya, J.C.; et al. IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res. Clin. Pract. 2022, 183, 109119. [Google Scholar] [CrossRef]
- Sinclair, A.J.; Abdelhafiz, A.H.; Rodríguez-Mañas, L. Frailty and sarcopenia—Newly emerging and high impact complications of diabetes. J. Diabetes Complicat. 2017, 31, 1465–1473. [Google Scholar] [CrossRef]
- Assar, M.E.; Laosa, O.; Rodríguez Mañas, L. Diabetes and frailty. Curr. Opin. Clin. Nutr. Metab. Care. 2019, 22, 52–57. [Google Scholar] [CrossRef]
- Collard, R.M.; Boter, H.; Schoevers, R.A.; Voshaar, R.C.O. Prevalence of Frailty in Community-Dwelling Older Persons: A Systematic Review. J. Am. Geriatr. Soc. 2012, 60, 1487–1492. [Google Scholar] [CrossRef]
- Sinclair, A.J.; Rodriguez-Mañas, L. Diabetes and Frailty: Two Converging Conditions? Can. J. Diabetes 2016, 40, 77–83. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association Professional Practice Committee. Older Adults: Standards of Medical Care in Diabetes-2022. Diabetes Care. 2022, 45 (Suppl. 1), S195–S207. [Google Scholar] [CrossRef]
- Sinclair, A.J.; Abdelhafiz, A.; Dunning, T.; Izquierdo, M.; Manas, L.R.; Bourdel-Marchasson, I.; Morley, J.E.; Munshi, M.; Woo, J.; Vellas, B. An International Position Statement on the Management of Frailty in Diabetes Mellitus: Summary of Recommendations 2017. J. Frailty Aging 2018, 7, 10–20. [Google Scholar] [CrossRef]
- Abdelhafiz, A.H.; Emmerton, D.; Sinclair, A.J. Impact of frailty metabolic phenotypes on the management of older people with type 2 diabetes mellitus. Geriatr. Gerontol. Int. 2021, 21, 614–622. [Google Scholar] [CrossRef]
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in Older adults: Evidence for a phenotype. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2001, 56, M146–M156. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, D.; Yoshida, T.; Watanabe, Y.; Yamada, Y.; Kimura, M.; Kyoto-Kameoka Study Group. A U-Shaped Relationship between the Prevalence of Frailty and Body Mass Index in Community-Dwelling Japanese Older Adults: The Kyoto–Kameoka Study. J. Clin. Med. 2020, 9, 1367. [Google Scholar] [CrossRef] [PubMed]
- Rockwood, K.; Mitnitski, A. Frailty in Relation to the Accumulation of Deficits. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2007, 62, 722–727. [Google Scholar] [CrossRef] [PubMed]
- Sonjak, V.; Jacob, K.; Morais, J.A.; Rivera-Zengotita, M.; Spendiff, S.; Spake, C.; Taivassalo, T.; Chevalier, S.; Hepple, R.T. Fidelity of muscle fibre reinnervation modulates ageing muscle impact in elderly women. J. Physiol. 2019, 597, 5009–5023. [Google Scholar] [CrossRef] [PubMed]
- St-Jean-Pelletier, F.; Pion, C.H.; Leduc-Gaudet, J.-P.; Sgarioto, N.; Zovilé, I.; Barbat-Artigas, S.; Reynaud, O.; Alkaterji, F.; Lemieux, F.C.; Grenon, A.; et al. The impact of ageing, physical activity, and pre-frailty on skeletal muscle phenotype, mitochondrial content, and intramyocellular lipids in men. J. Cachexia Sarcopenia Muscle 2017, 8, 213–228. [Google Scholar] [CrossRef] [PubMed]
- Chao, C.-T.; Wang, J.; Huang, J.-W.; Chan, D.-C.; Chien, K.-L.; COhort of GEriatric Nephrology in NTUH (COGENT) Study Group. Hypoglycemic episodes are associated with an increased risk of incident frailty among new onset diabetic patients. J. Diabetes Its Complicat. 2020, 34, 107492. [Google Scholar] [CrossRef]
- Chao, C.-T.; Wang, J.; Chien, K.-L.; COhort of GEriatric Nephrology in NTUH (COGENT) Study Group. Both pre-frailty and frailty increase healthcare utilization and adverse health outcomes in patients with type 2 diabetes mellitus. Cardiovasc. Diabetol. 2018, 17, 130. [Google Scholar] [CrossRef]
- Nguyen, T.T.H.; Vu, H.T.T.; Nguyen, T.N.; Dao, H.T.; Nguyen, T.X.; Nguyen, H.T.T.; Dang, A.K.; Nguyen, A.T.; Pham, T.; Vu, G.T.; et al. Assessment of nutritional status in older diabetic outpatients and related factors in Hanoi, Vietnam. J. Multidiscip. Health 2019, 12, 601–606. [Google Scholar] [CrossRef]
- Yanagita, I.; Fujihara, Y.; Eda, T.; Tajima, M.; Yonemura, K.; Kawajiri, T.; Yamaguchi, N.; Asakawa, H.; Nei, Y.; Kayashima, Y.; et al. Low glycated hemoglobin level is associated with severity of frailty in Japanese elderly diabetes patients. J. Diabetes Investig. 2018, 9, 419–425. [Google Scholar] [CrossRef]
- McAlister, F.A.; Lethebe, B.C.; Lambe, C.; Williamson, T.; Lowerison, M. Control of glycemia and blood pressure in British adults with diabetes mellitus and subsequent therapy choices: A comparison across health states. Cardiovasc. Diabetol. 2018, 17, 27. [Google Scholar] [CrossRef]
- de Decker, L.; Hanon, O.; Boureau, A.-S.; Chapelet, G.; Dibon, C.; Pichelin, M.; Berrut, G.; Cariou, B. Association Between Hypoglycemia and the Burden of Comorbidities in Hospitalized Vulnerable Older Diabetic Patients: A Cross-Sectional, Population-Based Study. Diabetes Ther. 2017, 8, 1405–1413. [Google Scholar] [CrossRef]
- Cacciatore, F.; Testa, G.; Galizia, G.; Della-Morte, D.; Mazzella, F.; Langellotto, A.; Pirozzi, G.; Ferro, G.; Gargiulo, G.; Ferrara, N.; et al. Clinical frailty and long-term mortality in elderly subjects with diabetes. Acta Diabetol. 2013, 50, 251–260. [Google Scholar] [CrossRef]
- Abdelhafiz, A.H.; Chakravorty, P.; Gupta, S.; Haque, A.; Sinclair, A.J. Can hypoglycaemic medications be withdrawn in older people with type 2 diabetes? Int. J. Clin. Pract. 2014, 68, 790–792. [Google Scholar] [CrossRef]
- Sjöblom, P.; AndersTengblad Löfgren, U.B.; Lannering, C.; Anderberg, N.; Rosenqvist, U.; Mölstad, S.; Ostgren, C.J. Can diabetes medication be reduced in elderly patients? An observational study of diabetes drug withdrawal in nursing home patients with tight glycaemic control. Dib. Res. Clin. Pract. 2008, 82, 197–202. [Google Scholar] [CrossRef]
- Morita, T.; Okuno, T.; Himeno, T.; Watanabe, K.; Nakajima, K.; Koizumi, Y.; Yano, H.; Iritani, O.; Okuro, M.; Morimoto, S. Glycemic control and disability-free survival in hypoglycemic agent-treated community-dwelling older patients with type 2 diabetes mellitus. Geriatr. Gerontol. Int. 2017, 17, 1858–1865. [Google Scholar] [CrossRef]
- Perez, S.I.A.; Senior, P.A.; Field, C.J.; Jindal, K.; Mager, D.R. Frailty, Health-Related Quality of Life, Cognition, Depression, Vitamin D and Health-Care Utilization in an Ambulatory Adult Population with Type 1 or Type 2 Diabetes Mellitus and Chronic Kidney Disease: A Cross-Sectional Analysis. Can. J. Diabetes 2019, 43, 90–97. [Google Scholar] [CrossRef]
- Kitamura, A.; Taniguchi, Y.; Seino, S.; Yokoyama, Y.; Amano, H.; Fujiwara, Y.; Shinkai, S. Combined effect of diabetes and frailty on mortality and incident disability in older Japanese adults. Geriatr. Gerontol. Int. 2019, 19, 423–428. [Google Scholar] [CrossRef]
- Thorpe, C.T.; Gellad, W.F.; Good, C.B.; Zhang, S.; Zhao, X.; Mor, M.; Fine, M.J. Tight Glycemic Control and Use of Hypoglycemic Medications in Older Veterans With Type 2 Diabetes and Comorbid Dementia. Diabetes Care 2015, 38, 588–595. [Google Scholar] [CrossRef]
- Sussman, J.B.; Kerr, E.A.; Saini, S.D.; Holleman, R.G.; Klamerus, M.L.; Min, L.C.; Vijan, S.; Hofer, T.P. Rates of Deintensification of Blood Pressure and Glycemic Medication Treatment Based on Levels of Control and Life Expectancy in Older Patients with Diabetes Mellitus. JAMA Intern. Med. 2015, 175, 1942–1949. [Google Scholar] [CrossRef]
- Yotsapon, T.; Sirinate, K.; Ekgaluck, W.; Somboon, V.; Tawee, A.; Worawit, K.; Soontaree, N.; Thep, H. Clinical characteristics and outcomes of the oldest old people with type 2 diabetes—Perspective from a tertiary diabetes center in Thailand. BMC Endocr. Disord. 2016, 16, 30. [Google Scholar] [CrossRef] [PubMed]
- Kong, L.; Zhao, H.; Fan, J.; Wang, Q.; Li, J.; Bai, J.; Mao, J. Predictors of frailty among Chinese community-dwelling older adults with type 2 diabetes: A cross-sectional survey. BMJ Open 2021, 11, e041578. [Google Scholar] [CrossRef] [PubMed]
- Ferri-Guerra, J.; Aparicio-Ugarriza, R.; Salguero, D.; Baskaran, D.; Mohammed, Y.N.; Florez, H.; Ruiz, J.G. The Association of Frailty with Hospitalizations and Mortality among Community Dwelling Older Adults with Diabetes. J. Frailty Aging 2020, 9, 94–100. [Google Scholar] [CrossRef] [PubMed]
- Hyde, Z.; Smith, K.; Flicker, L.; Atkinson, D.; Fenner, S.; Skeaf, L.; Malay, R.; Giudice, D.L. HbA1c Is Associated with Frailty in a Group of Aboriginal Australians. J. Frailty Aging 2019, 8, 17–20. [Google Scholar] [CrossRef] [PubMed]
- Aguayo, G.A.; Hulman, A.; Vaillant, M.T.; Donneau, A.-F.; Schritz, A.; Stranges, S.; Malisoux, L.; Huiart, L.; Guillaume, M.; Sabia, S.; et al. Prospective Association Among Diabetes Diagnosis, HbA1c, Glycemia, and Frailty Trajectories in an Elderly Population. Diabetes Care 2019, 42, 1903–1911. [Google Scholar] [CrossRef]
- García-Esquinas, E.; Graciani, A.; Guallar-Castillón, P.; López-García, E.; Rodríguez-Mañas, L.; Rodríguez-Artalejo, F. Diabetes and Risk of Frailty and Its Potential Mechanisms: A Prospective Cohort Study of Older Adults. J. Am. Med. Dir. Assoc. 2015, 16, 748–754. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, T.N.; Harris, K.; Woodward, M.; Chalmers, J.; Cooper, M.; Hamet, P.; Harrap, S.; Heller, S.; MacMahon, S.; Mancia, G.; et al. The Impact of Frailty on the Effectiveness and Safety of Intensive Glucose Control and Blood Pressure–Lowering Therapy for People with Type 2 Diabetes: Results From the ADVANCE Trial. Diabetes Care 2021, 44, 1622–1629. [Google Scholar] [CrossRef]
- Bilgin, S.; Aktas, G.; Kurtkulagi, O.; Atak, B.M.; Duman, T.T. Edmonton frail score is associated with diabetic control in elderly type 2 diabetic subjects. J. Diabetes Metab. Disord. 2020, 19, 511–514. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.; Yu, N.; Wu, H.; Liu, Y. Risk factors associated with frailty in older adults with type 2 diabetes: A cross-sectional study. J. Clin. Nurs. 2022, 31, 967–974. [Google Scholar] [CrossRef]
- Lipska, K.J.; Ross, J.S.; Miao, Y.; Shah, N.D.; Lee, S.J.; Steinman, M.A. Potential Overtreatment of Diabetes Mellitus in Older Adults With Tight Glycemic Control. JAMA Intern. Med. 2015, 175, 356–362. [Google Scholar] [CrossRef]
- Thein, F.S.; Li, Y.; Nyunt, M.S.Z.; Gao, Q.; Wee, S.L.; Ng, T.P. Physical frailty and cognitive impairment is associated with diabetes and adversely impact functional status and mortality. Postgrad. Med. 2018, 130, 561–567. [Google Scholar] [CrossRef]
- DeFronzo, R.A.; Jacot, E.; Jequier, E.; Maeder, E.; Wahren, J.; Felber, J.P. The Effect of Insulin on the Disposal of Intravenous Glucose: Results from Indirect Calorimetry and Hepatic and Femoral Venous Catheterization. Diabetes 1981, 30, 1000–1007. [Google Scholar] [CrossRef] [PubMed]
- Pette Peuker, D.H.; Staron, R.S. The impact of biochemical methods for single fiber analysis. Acta Physiol. Scand. 1999, 166, 261–277. [Google Scholar] [CrossRef]
- Henriksen, E.J.; Bourey, R.E.; Rodnick, K.J.; Koranyi, L.; Permutt, M.A.; Holloszy, J.O. Glucose transporter protein content and glucose transport capacity in rat skeletal muscles. Am. J. Physiol. Endocrinol. Metab. 1990, 259, E593–E598. [Google Scholar] [CrossRef]
- Nilwik, R.; Snijders, T.; Leenders, M.; Groen, B.B.; van Kranenburg, J.; Verdijk, L.B.; van Loon, L.J. The decline in skeletal muscle mass with aging is mainly attributed to a reduction in type II muscle fiber size. Exp. Gerontol. 2013, 48, 492–498. [Google Scholar] [CrossRef]
- Miljkovic, N.; Lim, J.Y.; Miljkovic, I.; Frontera, W.R. Aging of skeletal muscle fibers. Ann. Rehabil. Med. 2015, 39, 155–162. [Google Scholar] [CrossRef]
- Kramer, I.F.; Snijders, T.; Smeets, J.S.J.; Leenders, M.; van Kranenburg, J.; Hoed, M.D.; Verdijk, L.B.; Poeze, M.; van Loon, L.J.C. Extensive Type II Muscle Fiber Atrophy in Elderly Female Hip Fracture Patients. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2017, 72, 1369–1375. [Google Scholar] [CrossRef]
- Abdelhafiz, A.H.; Sinclair, A.J. Low HbA1c and Increased Mortality Risk-is Frailty a Confounding Factor? Aging Dis. 2015, 6, 262–270. [Google Scholar] [CrossRef] [PubMed]
- Daradkeh, G.; Essa, M.M. Nutritional status and cognitive impairment in elderly. Pak. J. Biol. Sci. 2014, 17, 1098–1105. [Google Scholar] [CrossRef][Green Version]
- Vellas, B.; Lauque, S.; Gillette-Guyonnet, S.; Andrieu, S.; Cortes, F.; Nourhashémi, F.; Cantet, C.; Ousset, P.J.; Grandjean, H.; REAL.FR Group. Impact of nutritional status on the evolution of Alzheimer’s disease and on response to acetylcholinesterase inhibitor treatment. J. Nutr. Health Aging 2005, 9, 75–80. [Google Scholar]
- Abdelhafiz, A.H.; Loo, B.E.; Hensey, N.; Bailey, C.; Sinclair, A. The U-shaped Relationship of Traditional Cardiovascular Risk Factors and Adverse Outcomes in Later Life. Aging Dis. 2012, 3, 454–464. [Google Scholar] [PubMed]
- Abdelhafiz, A.H.; Koay, L.; Sinclair, A.J. The Emergence of Frailty May Lead to a State of Burnt Out Type 2 Diabetes. J. Frailty Aging 2016, 5, 162–167. [Google Scholar] [CrossRef]
- McClinchy, J. Dietary management of older people with diabetes. Br. J. Community Nurs. 2018, 23, 248–251. [Google Scholar] [CrossRef] [PubMed][Green Version]
- González-Castro, T.B.; Escobar-Chan, Y.M.; Fresan, A.; López-Narváez, M.L.; Tovilla-Zárate, C.A.; Juárez-Rojop, I.E.; Ble-Castillo, J.L.; Genis-Mendoza, A.D.; Arias-Vázquez, P.I. Higher risk of depression in individuals with type 2 diabetes and obesity: Results of a meta-analysis. J. Health Psychol. 2021, 26, 1404–1419. [Google Scholar] [CrossRef]
- Soysal, P.; Veronese, N.; Thompson, T.; Kahl, K.G.; Fernandes, B.S.; Prina, A.M.; Solmi, M.; Schofield, P.; Koyanagi, A.; Tseng, P.-T.; et al. Relationship between depression and frailty in older adults: A systematic review and meta-analysis. Ageing Res. Rev. 2017, 36, 78–87. [Google Scholar] [CrossRef]
- Ting, M.J.M.; Hyde, Z.; Flicker, L.; Almeida, O.P.; Golledge, J.; Hankey, G.J.; Yeap, B.B. Associations between diabetes, body mass index and frailty: The Western Australian Health In Men Study. Maturitas 2022, 161, 58–64. [Google Scholar] [CrossRef]
- Sinclair, A.J.; Abdelhafiz, A.H. Metabolic Impact of Frailty Changes Diabetes Trajectory. Metabolites 2023, 13, 295. [Google Scholar] [CrossRef]
- Sinclair, A.J.; Pennells, D.; Abdelhafiz, A.H. Hypoglycaemic therapy in frail older people with type 2 diabetes mellitus—A choice determined by metabolic phenotype. Aging Clin. Exp. Res. 2022, 34, 1949–1967. [Google Scholar] [CrossRef] [PubMed]
- Yang, B.-Y.; Zhai, G.; Gong, Y.-L.; Su, J.-Z.; Peng, X.-Y.; Shang, G.-H.; Han, D.; Jin, J.-Y.; Liu, H.-K.; Du, Z.-Y.; et al. Different physiological roles of insulin receptors in mediating nutrient metabolism in zebrafish. Am. J. Physiol. Metab. 2018, 315, E38–E51. [Google Scholar] [CrossRef]
- Hatting, M.; Tavares, C.D.; Sharabi, K.; Rines, A.K.; Puigserver, P. Insulin regulation of gluconeogenesis. Ann. N. Y. Acad. Sci. 2018, 1411, 21–35. [Google Scholar] [CrossRef] [PubMed]
- Bouchi, R.; Fukuda, T.; Takeuchi, T.; Nakano, Y.; Murakami, M.; Minami, I.; Izumiyama, H.; Hashimoto, K.; Yoshimoto, T.; Ogawa, Y. Insulin Treatment Attenuates Decline of Muscle Mass in Japanese Patients with Type 2 Diabetes. Calcif. Tissue Int. 2017, 101, 1–8. [Google Scholar] [CrossRef]
- Ferrari, U.; Then, C.; Rottenkolber, M.; Selte, C.; Seissler, J.; Conzade, R.; Linkohr, B.; Peters, A.; Drey, M.; Thorand, B. Longitudinal association of type 2 diabetes and insulin therapy with muscle parameters in the KORA-Age study. Acta Diabetol. 2020, 57, 1057–1063. [Google Scholar] [CrossRef]
- Sugimoto, K.; Ikegami, H.; Takata, Y.; Katsuya, T.; Fukuda, M.; Akasaka, H.; Tabara, Y.; Osawa, H.; Hiromine, Y.; Rakugi, H. Glycemic Control and Insulin Improve Muscle Mass and Gait Speed in Type 2 Diabetes: The MUSCLES-DM Study. J. Am. Med. Dir. Assoc. 2021, 22, 834–838.e1. [Google Scholar] [CrossRef] [PubMed]
- Fujimoto, K.; Iwakura, T.; Aburaya, M.; Matsuoka, N. Twice-daily insulin degludec/insulin aspart effectively improved morning and evening glucose levels and quality of life in patients previously treated with premixed insulin: An observational study. Diabetol. Metab. Syndr. 2018, 10, 64. [Google Scholar] [CrossRef] [PubMed]
- Bradley, M.C.; Chillarige, Y.; Lee, H.; Wu, X.; Parulekar, S.; Muthuri, S.; Wernecke, M.; MaCurdy, T.E.; Kelman, J.A.; Graham, D.J. Severe Hypoglycemia Risk With Long-Acting Insulin Analogs vs Neutral Protamine Hagedorn Insulin. JAMA Intern. Med. 2021, 181, 598. [Google Scholar] [CrossRef] [PubMed]
- Betônico, C.C.; Titan, S.M.O.; Lira, A.; Pelaes, T.S.; Correa-Giannella, M.L.C.; Nery, M.; Queiroz, M. Insulin Glargine U100 Improved Glycemic Control and Reduced Nocturnal Hypoglycemia in Patients with Type 2 Diabetes Mellitus and Chronic Kidney Disease Stages 3 and 4. Clin. Ther. 2019, 41, 2008–2020.e3. [Google Scholar] [CrossRef] [PubMed]
- Özçelik, S.; Çelik, M.; Vural, A.; Aydın, B.; Özçelik, M.; Gozu, H. Outcomes of transition from premixed and intensive insulin therapies to insulin aspart/degludec co-formulation in type 2 diabetes mellitus: A real-world experience. Arch. Med. Sci. 2021, 17, 1–8. [Google Scholar] [CrossRef]
- Bollig, C.; Torbahn, G.; Bauer, J.; Brefka, S.; Dallmeier, D.; Denkinger, M.; Eidam, A.; Klöppel, S.; Zeyfang, A.; MedQoL-Group (Medication and Quality of Life in Frail Older Persons); et al. Evidence gap on antihyperglycemic pharmacotherapy in frail older adults. Z. Gerontol. Geriat. 2020, 54, 278–284. [Google Scholar] [CrossRef]
- Huang, E.S.; Zhang, Q.; Gandra, N.; Chin, M.H.; Meltzer, D.O. The Effect of Comorbid Illness and Functional Status on the Expected Benefits of Intensive Glucose Control in Older Patients with Type 2 Diabetes: A Decision Analysis. Ann. Intern. Med. 2008, 149, 11–19. [Google Scholar] [CrossRef]
- Rodriguez-Mañas, L.; Laosa, O.; Vellas, B.; Paolisso, G.; Topinkova, E.; Oliva-Moreno, J.; Bourdel-Marchasson, I.; Izquierdo, M.; Hood, K.; Zeyfang, A.; et al. Effectiveness of a multimodal intervention in functionally impaired older people with type 2 diabetes mellitus. J. Cachex—Sarcopenia Muscle 2019, 10, 721–733. [Google Scholar] [CrossRef]
- Xia, M.-F.; Chen, L.-Y.; Wu, L.; Ma, H.; Li, X.-M.; Li, Q.; Aleteng, Q.; Hu, Y.; He, W.-Y.; Gao, J.; et al. Sarcopenia, sarcopenic overweight/obesity and risk of cardiovascular disease and cardiac arrhythmia: A cross-sectional study. Clin. Nutr. 2020, 40, 571–580. [Google Scholar] [CrossRef]
- Cho, H.-W.; Chung, W.; Moon, S.; Ryu, O.-H.; Kim, M.K.; Kang, J.G. Effect of Sarcopenia and Body Shape on Cardiovascular Disease According to Obesity Phenotypes. Diabetes Metab. J. 2021, 45, 209–218. [Google Scholar] [CrossRef]
- Uchida, S.; Kamiya, K.; Hamazaki, N.; Matsuzawa, R.; Nozaki, K.; Ichikawa, T.; Suzuki, Y.; Nakamura, T.; Yamashita, M.; Kariya, H.; et al. Association between sarcopenia and atherosclerosis in elderly patients with ischemic heart disease. Heart Vessel. 2020, 35, 769–775. [Google Scholar] [CrossRef]
- Yoo, J.H.; Park, S.W.; Jun, J.E.; Jin, S.; Hur, K.Y.; Lee, M.; Kang, M.; Kim, G.; Kim, J.H. Relationship between low skeletal muscle mass, sarcopenic obesity and left ventricular diastolic dysfunction in Korean adults. Diabetes/Metab. Res. Rev. 2020, 37, e3363. [Google Scholar] [CrossRef]
- Marsico, F.; Paolillo, S.; Gargiulo, P.; Bruzzese, D.; Dell’aversana, S.; Esposito, I.; Renga, F.; Esposito, L.; Marciano, C.; Dellegrottaglie, S.; et al. Effects of glucagon-like peptide-1 receptor agonists on major cardiovascular events in patients with Type 2 diabetes mellitus with or without established cardiovascular disease: A meta-analysis of randomized controlled trials. Eur. Heart J. 2020, 41, 3346–3358. [Google Scholar] [CrossRef] [PubMed]
- Zinman, B.; Wanner, C.; Lachin, J.M.; Fitchett, D.; Bluhmki, E.; Hantel, S.; Mattheus, M.; Devins, T.; Johansen, O.E.; Woerle, H.J.; et al. Empagliflozin, cardiovascular outcomes, and mortality in Type 2 diabetes. N. Engl. J. Med. 2015, 373, 2117–2128. [Google Scholar] [CrossRef] [PubMed]
- Wiviott, S.D.; Raz, I.; Bonaca, M.P.; Mosenzon, O.; Kato, E.T.; Cahn, A.; Silverman, M.G.; Zelniker, T.A.; Kuder, J.F.; Murphy, S.A.; et al. Dapagliflozin and Cardiovascular Outcomes in Type 2 Diabetes. N. Engl. J. Med. 2019, 380, 347–357. [Google Scholar] [CrossRef] [PubMed]
- McMurray, J.J.V.; Solomon, S.D.; Inzucchi, S.E.; Køber, L.; Kosiborod, M.N.; Martinez, F.A.; Ponikowski, P.; Sabatine, M.S.; Anand, I.S.; Bělohlávek, J.; et al. Dapagliflozin in patients with heart failure and reduced ejection fraction. N. Engl. J. Med. 2019, 381, 1995–2008. [Google Scholar] [CrossRef]
- Bae, J.H.; Park, E.-G.; Kim, S.; Kim, S.G.; Hahn, S.; Kim, N.H. Effects of Sodium-Glucose Cotransporter 2 Inhibitors on Renal Outcomes in Patients with Type 2 Diabetes: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Sci. Rep. 2019, 9, 13009. [Google Scholar] [CrossRef]
- Wanner, C.; Inzucchi, S.E.; Lachin, J.M.; Fitchett, D.; Von Eynatten, M.; Mattheus, M.; Johansen, O.E.; Woerle, H.J.; Broedl, U.C.; Zinman, B.; et al. Empagliflozin and Progression of Kidney Disease in Type 2 Diabetes. N. Engl. J. Med. 2016, 375, 323–334. [Google Scholar] [CrossRef]
- Vasilakou, D.; Karagiannis, T.; Athanasiadou, E.; Mainou, M.; Liakos, A.; Bekiari, E.; Sarigianni, M.; Matthews, D.R.; Tsapas, A. Sodium–glucose cotransporter 2 inhibitors for Type 2 diabetes: A systematic review and meta-analysis. Ann. Intern. Med. 2013, 159, 262–274. [Google Scholar] [CrossRef]
- Karagiannis, T.; Tsapas, A.; Athanasiadou, E.; Avgerinos, I.; Liakos, A.; Matthews, D.R.; Bekiari, E. GLP-1 receptor agonists and SGLT2 inhibitors for older people with type 2 diabetes: A systematic review and meta-analysis. Diabetes Res. Clin. Pract. 2021, 174, 108737. [Google Scholar] [CrossRef]
- Lv, X.; Dong, Y.; Hu, L.; Lu, F.; Zhou, C.; Qin, S. Glucagon-like peptide-1 receptor agonists (GLP-1 RAs) for the management of nonalcoholic fatty liver disease (NAFLD): A systematic review. Endocrinol. Diabetes Metab. 2020, 3, e00163. [Google Scholar] [CrossRef]
- Zhang, X.; Bai, R.; Jia YZong, J.; Wang, Y.; Dong, Y. The effect of liraglutide on nonalcoholic fatty liver disease in type 2 diabetes mellitus. Int. J. Diabetes Dev. Ctries. 2020, 40, 491–499. [Google Scholar] [CrossRef]
- Liu, H.-M.; Zhang, Q.; Shen, W.-D.; Li, B.-Y.; Lv, W.-Q.; Xiao, H.-M.; Deng, H.-W. Sarcopenia-related traits and coronary artery disease: A bi-directional Mendelian randomization study. Aging 2020, 12, 3340–3353. [Google Scholar] [CrossRef] [PubMed]
- Villareal, D.T.; Aguirre, L.; Gurney, A.B.; Waters, D.L.; Sinacore, D.R.; Colombo, E.; Armamento-Villareal, R.; Qualls, C. Aerobic or Resistance Exercise, or Both, in Dieting Obese Older Adults. N. Engl. J. Med. 2017, 376, 1943–1955. [Google Scholar] [CrossRef]
- Don, B.R.; Kaysen, G. Serum Albumin: Relationship to Inflammation and Nutrition. Semin. Dial. 2004, 17, 432–437. [Google Scholar] [CrossRef] [PubMed]
- Malafarina, V.; Uriz-Otano, F.; Iniesta, R.; Gil-Guerrero, L. Effectiveness of Nutritional Supplementation on Muscle Mass in Treatment of Sarcopenia in Old Age: A Systematic Review. J. Am. Med. Dir. Assoc. 2013, 14, 10–17. [Google Scholar] [CrossRef]
- Abdelhafiz, A.; Sinclair, A. Metabolic phenotypes explain the relationship between dysglycaemia and frailty in older people with type 2 diabetes. J. Diabetes Its Complicat. 2022, 36, 108144. [Google Scholar] [CrossRef] [PubMed]
- Ahlqvist, E.; Storm, P.; Käräjämäki, A.; Martinell, M.; Dorkhan, M.; Carlsson, A.; Vikman, P.; Prasad, R.B.; Aly, D.M.; Almgren, P.; et al. Novel subgroups of adult- onset diabetes and their association with outcomes: A data-driven cluster analysis of six variables. Lancet Diabetes Endocrinol. 2018, 6, 361–369. [Google Scholar] [CrossRef] [PubMed]
- Abdelhafiz, A.H.; McNicholas, E.; Sinclair, A.J. Hypoglycemia, frailty and dementia in older people with diabetes: Reciprocal relations and clinical implications. J. Diabetes Its Complicat. 2016, 30, 1548–1554. [Google Scholar] [CrossRef]
| Study | Patients | Aim to | Main Findings |
|---|---|---|---|
| Chao CT, et al., prospective, Taiwan, 2020 [14] | 2119 patients with and 8432 without hypoglycaemia (control), mean (SD) age 65.9 (14) Y. | Examine whether hypoglycaemia increases the risk of frailty. | Patients with compared to those without hypoglycaemia had: A. Less obesity (1.4% vs. 2.4%, p = 0.006). B. Less hyperlipidaemia (55.5% vs. 63.0%, p < 0.001). C. Higher mean (SD) CCIS, 4.2 (2.4) vs. 3.4 (2.2), p < 0.001. D. Higher mean (SD) aDCSI, 1.3 (1.5) vs. 0.8 (1.2), p < 0.001. D. Less patients using statin (36.4% vs. 44.8%, p < 0.001) or fibrate (12.4% vs. 16.1%, p < 0.001). E. No difference in hypoglycaemic therapy use. |
| Chao CT, et al., prospective, Taiwan, 2018 [15] | 560,795 patients with DM, mean (SD) age 56.4 (13.8) Y. | Examine the association of pre-frailty and frailty with mortality. | Frail (≥3 components in FRAIL scale) compared to non-frail patients had: A. Higher mean (SD) age, 75.1 (11.2) vs. 54.8 (13.2), p < 0.01. B. Higher mean (SD) aDCSI, 1.4 (1.5) vs. 0.2 (0.6), p < 0.01. C. Higher mean (SD) CCIS, 5.4 (2.4) vs. 1.7 (1.4), p < 0.01. D. More prevalence of hypertension, CKD, CLD, COPD, AF, CAD, PVD, gout, OA, malignancy, osteoporosis, mental illness, and CVD, all p < 0.01. E. Less hyperlipidaemia, 31.9% vs. 41.2%, p < 0.01. F. Less obesity, 0.9% vs. 1.6%, p < 0.01. G. More hypoglycaemia, 1.2% vs. 0.1%, p < 0.01. H. Less statin and fibrate use, p < 0.01. I. More insulin users, 7.7% vs. 4.8%, p < 0.01. J. Less oral hypoglycaemic use, p < 0.01. |
| Nguyen TTH, et al., cross-sectional, Vietnam, 2019 [16] | 158 subjects with DM, mean (SD) age 69.52 (6.76) Y. | Assess nutritional status using the Mini-Nutrition Assessment Short Form tool, and describe the relationship among related factors. | Malnourished compared to well-nourished had: A. Older (≥80 Y) subjects, 11.5% vs. 6.6%, p = 0.27. B. More underweight (10.2% vs. 0.0%) and less overweight subjects (30.6 vs. 71.6), p < 0.001. C. More exhausted subjects, 30.8% vs. 11.0%, p < 0.01. D. More cognitive impairment, 53.1% vs. 27.5%, p = 0.002. E. More frail subjects, 20.4% vs. 2.8%, p < 0.001. F. Malnutrition risk increased by frailty (OR 9.06, 95% CI 2.37 to 34.65, p = 0.001) and cognitive impairment, 2.98, 1.48 to 6.0, p = 0.002. |
| Yanagita I, et al., cross-sectional, prospective, Japan, 2018 [17] | 132 hospitalised patients with DM, mean (SD) age 78.3 (8.0) Y. | Evaluate frailty risk factors including HbA1c using CFS. | Frail compared to non-frail had: A. Higher mean (SD) age, 82.78 (8.16) vs. 75.17 (6.20) Y, p < 0.001. B. Lower mean (SD) HbA1c, 6.6 (0.93) vs. 7.27 (1.04)%, p < 0.001). B. Lower mean (SD) albumin, 35.62 (4.82) vs. 41.73 g/L, p < 0.001). C. Lower mean (SD) HDL-cholesterol, 1.23 (0.39) vs. 1.46 9 (0.43) mmol/L, p < 0.01). D. Lower mean (SD) Hb, 117.89 (17.28) vs. 132.38 (17.02) g/L, p < 0.001. E. Lower mean (SD) SBP (KPa) 16.81 (2.12) vs. 17.60 (1.92), p < 0.05). F. Lower mean (SD) body weight, 51.64 (12.72) vs. 59.17 (10.94) Kg, p < 0.001). G. Fewer patients using statin or fibrate (%) 34.54 vs. 54.54, p < 0.05. H. No difference in hypoglycaemic therapy use. |
| McAlister FA, et al., retrospective, UK, 2018 [18] | 292,170 subjects with DM, mean (SD) age 61.7 (15.6) Y. | Examine glycaemic control across health states. | Frail compared to non-frail subjects had: A. Higher mean (SD) age, 72.2 (11.2) vs. 60.8 (15.5), p < 0.0001. B. Higher mean (SD) CCIS, 2.73 (1.6) vs. 1.04 (0.86), p < 0.0001. C. Lower mean (SD) BMI, 26.0 (6.8) vs. 30.17 (6.9), p < 0.0001. D. Lower mean (SD) HbA1c, 7.1 (1.46) vs. 7.38 (1.64)%, p < 0.0001. E. Lower total cholesterol (p = 0.007), triglycerides (p = 0.05) and LDL-cholesterol (0.001). F. More comorbidities and diabetes complications, p < 0.0001. |
| De Decker L, et al., cross-sectional, France, 2017 [19] | 1552 patients with DM, mean (SD) age 86.4 (4.4) Y. | Determine the association between hypoglycaemia and a high burden of comorbidities. | Patients with compared to those without hypoglycaemia had the mean (SD): A. Lower body weight (Kg) 65.80 (14.7) vs. 69.5 (24.5), p = 0.004). B. Lower eGFR (ml/min) 46.1 (20.8) vs. 51.9 (26.1), p < 0.001. C. Higher CCIS 4.7 (2.3) vs. 3.8 (2.1), p < 0.001. C. Greater level of dependency (p < 0.001). D. Higher prevalence of CV disease (%) 68.6% vs. 54.3%, p < 0.001. E. Higher prevalence of dementia (%) 67% vs. 59.3%, p < 0.006. F. More use of insulin, p < 0.001 G. More SMBG (%) 84.6% vs. 67.8, p < 0.001. H. Lower use of SU, metformin, p < 0.001 and glinides, p = 0.002. |
| Cacciatore F, et al., prospective, Italy, 2013 [20] | 1288 subjects, mean (SD) 72.4 (6.3) Y, F/U 12 Y. | Examine the predictive role of frailty on long-term mortality. | Severely frail compared to non-frail patients had: A. Higher mean (SD) age, 78.9 (6.0) vs. 72.1 (4.7), p < 0.001. B. Lower mean (SD) BMI, 26.4 (5.1) vs. 27.0 (3.6), p = 0.087. C. Lower mean (SD) waist circumference, 94.8 (19.2) vs. 98.8 (14.9), p = 0.672. D. Higher mean (SD) CCIS, 4.8 (2.2) vs. 2.2 (1.6), p < 0.001. E. More insulin users, 26.0% vs. 13.4%, p = 0.004. F. More hypoglycaemic drug users 87.2% vs. 73.1, p = 0.008. G. More comorbidities of CHF, CKD, low MMSE, high GDS, disability, and mortality, all p < 0.001. |
| Abdelhafiz AH, case series, UK, 2014 [21] | 8.0 patients with type 2 DM, mean (SD) age 86.5 (3.2) Y and tight glycaemic control. | Describe whether hypoglycaemic therapy can be withdrawn in patients with HbA1c ≤6.0% or having recurrent hypoglycaemia. | Mean (SD) HbA1c was: A. 6.2% (0.8) at the point of medication withdrawal. B. 6.5% (0.7) after one year of follow-up, p = 0.4. At the point of medication withdrawal compared to the initial point of starting medication: A. Increased mean number of comorbidities 6.8 vs. 4.1, p = 0.002. B. Decreased mean weight 75.4 vs. 88.0 Kg, p = 0.003. C. Increased mean number of medications 10.1 vs. 6.4, p = 0.01. D. 50.0% of patients had a new diagnosis of dementia. |
| Sjoblom P, et al., observational, Sweden, 2008 [22] | 32.0 nursing home patients with DM, mean (SD) age 84.4 (6.8) Y. | Explore the feasibility of hypoglycaemic medication withdrawal in patients with HbA1c ≤6.0%. | Intervention compared to the non-intervention group had: A. Lower mean (SD) BMI, 25.6 (4.5) vs. 26.5 (5.1). B. Lower eGFR 50 vs. 55 mL/min/1.73 m2. C. Longer mean (SD) duration of DM, 10.6 (8.9) vs. 9.0 (7.4) Y. D. Lower mean (SD) HbA1c 5.2 (0.4) vs. 7.1 (1.6). |
| Morita T, et al., prospective, Japan, 2017 [23] | 184 patients with diabetes aged 65–94 Y, F/U 5 Y. | Investigate if low HbA1c is associated with risk of support/care need certification. | 42 (22.8%) patients developed disability defined as a requirement of first support/care-need certification. Compared to patients with HbA1c ≥ 7.0%, patients with HbA1c < 0.6% were: A. Older, mean (SD) age 77.5 (6.5) vs. 75.1 (6.3) Y, and had more people aged >75 Y, 68.5% vs. 54.5%, Kruskal–Wallis p < 0.05/3 and 0.20/3 respectively. B. Had less insulin use 37.8% vs. 63.6%, p < 0.20/3. C. Had less dyslipidaemia 37.0% vs. 59.1%, p < 0.05/3. D. Had more hypoalbuminaemia 14.8% vs. 6.8%, p < 0.20/3. |
| Adame Perez SI, et al., cross-sectional, Canada, 2019 [24] | 41 subjects with DM, median (IQR) age 70.0 (65.0–74.0) Y. | Compare differences in body composition by frailty status. | Frail compared to non-frail patients had: A. Lower mean (SD) ASMI (kg/m2), 6.8 (1.0) vs. 7.7 (0.9), p = 0.02. B. More patients with low lean body mass, 57.1% vs. 14.7%, p = 0.01. C. Higher mean (SD) comorbidities, 6.0 (2.0) vs. 4.0 (2.0), p = 0.03. C. No difference in body weight, BMI, HbA1c, hypoglycaemic therapies, or hypoglycaemic episodes. |
| Kitamura A, et al., prospective, Japan, 2019 [25] | 1271 subjects, mean (SD) age 71.0 (5.6) Y, 176 had DM. | Clarify risks of death and disability. | A. Frail compared to non-frail were older 72.5 vs. 69.6 Y, p = 0.05, more patients had hypoalbuminaemia, 20.7 vs. 5.9%, p = 0.02 and lower BMI 20.8 vs. 2.0%, p = 0.06. B. There was no difference in HbA1c, lipid profile, average BMI, hypoglycaemic medications, and comorbidities. |
| Thorpe CT, retrospective, US, 2015 [26] | 15,880 patients ≥ 65.0 years old with DM and dementia. | Examine: A. Risk factors for tight glycaemic control B. Medications associated with the risk of hypoglycaemia. | A. 52.0% of patients had tight glycaemic control (HbA1c < 7.0%). B. Factors associated with tight control were: 1. Older age (75.0–84.0 years, OR 1.16, 95.0% CI 1.07 to 1.126, p = 0.001, ≥75.0 years, (1.13, 1.02 to 1.125, p = 0.021. 2. Heart valve disease (OR 1.16, 95.0% CI 1.01 to 1.32, p = 0.033), chronic lung disease OR 1.10, 95.0% CI 1.01 to 1.21, p = 0.038), and deficiency anaemia (OR 1.12, 95.0% CI 1.02 to 1.22, p = 0.016). 3. Weight loss (OR 1.36, 95.0% CI 1.09 to 1.69, p = 0.006). C. Among tightly controlled patients, 75.0% used SU and/or insulin. |
| Sussman JB, et al., retrospective, US, 2015 [27] | 179,991 patients > 70.0 years old on active treatment for DM. | Examine the rate of medications deintensification. | Patients with very low HbA1c (<6.0%) compared to those with higher HbA1c (≥6.5%) were: A. Older (mean age 78.6 vs. 77.8 years). B. More comorbidities (mean CCIS 1.44 vs. 1.27). C. More low life expectancy <5.0 years (19.9% vs. 15.7%). D. More dementia (2.3 vs. 1.6%). E. More palliation in prior year (0.5 vs. 0.3%). F. More metastatic cancer (0.7 vs. 0.4%). |
| Yotsapont, et al., retrospective, Thailand, 2015 [28] | 143.0 patients > 85.0 years old with DM. | Describe clinical characteristics and outcomes of “oldest old” patients with DM. | Patients had: 1. Long duration of diabetes, mean (SD) 22.1 (11.1) Y. 2. Severe comorbidities, CCIS ≥ 5.0 in 35.3%. 3. Tight glycaemic control, HbA1c < 7.0% in 66.9%. 4. Frequent hypoglycaemia in 10.5%. 5. Multiple comorbidities: 23.4% diabetic retinopathy, 54.9% CKD, 15.8% CV disease, 18.0% stroke, 22.6% dementia. 6. Only 20.0% of those with HbA1c <6.0% received medication deintensification. |
| Study | Patients | Aim to | Main Findings |
|---|---|---|---|
| Kong L, et al., cross-sectional, China, 2021 [29] | 291 community-dwelling older people, median (IQR) age 69 Y (IQR 67–72) with DM. | Identify predictors of frailty. | Frail compared with non-frail patients were: A. Older (% ≥ 75 Y) 19.6% vs. 9.4%. B. Significantly higher HbA1c, median (IQR) 6.97% (5.95, 8.42) vs. 6.74% (5.96, 7.20), p = 0.055. C. Significant comorbidities, median (IQR) 5.0 (4,7) vs. 4.0 (3,6), p = 0.030. D. Higher BMI (% ≥ 28) 17.9% vs. 11.8%. |
| Ferri-Guerra J, et al., retrospective, US, 2020 [30] | 763 patients with DM, mean (SD) age 72.9 (6.8) Y. | Determine the association of frailty with all-cause hospitalisations and mortality. | Frail compared to non-frail patients had: A. Higher mean (SD) age, 73.33 (7.26) vs. 72.4 (6.23), p = 0.19. B. Higher mean (SD) BMI, 30.07 (6.0) vs. 29.82(5.15), p = 0.54. C. More end-organ damage, 36.4% vs. 28.3%, p = 0.02 D. Higher mean (SD) DM duration, 9.48 (5.21) vs. 8.46 (5.36), p < 0.009. E. Less patients with HbA1c ≤ 7 and more patients with HbA1c > 7%, p = 0.15. F. Higher mean (SD) CCIS, 6.91 (2.0) vs. 5.75 (1.65), p < 0.0001. F. More hypoglycaemic drug users 87.2% vs. 73.1, p = 0.008. G. More polypharmacy, hospitalisation and mortality, all p < 0.0001. |
| Hyde Z, et al., cross-sectional, Australia, 2019 [31] | 141 Aboriginal Australian, mean (SD) age 62.2 (11.1) Y. | Explore whether HbA1c is associated with frailty. | A. Mean (SD) BMI of participants 28.5 (7.1) kg/m2 (range 13.9–52.1). B. 31.2% obese (BMI ≥ 30.0), 29.1% overweight (25.0–29.9), 19.2 normal (20.0–24.9), and 8.5 underweight (≤19.9). C. Association between HbA1c ≥ 6.5% and frailty was attenuated after adjustment for BMI (OR 2.10, 95% CI 0.92 to 4.80). D. Frailty is more common in obese subjects (70.5%) but similar in other groups, 50.0% in underweight, 59.3% in normal weight, and 53.7% in overweight. E. BMI was a possible confounder in the association between HbA1c and frailty. |
| Aguayo GA, et al., prospective, UK, 2019 [32] | 5377 participants, median (IQR) 70 (65, 77 Y, F/U 10 Y. | Examine whether individuals with DM or high HbA1c experience different frailty trajectories with ageing. | Patients with compared to those without DM had, mean (SD): A. HbA1c 7.0% (0.4) vs. 5.5% (0.5). B. BMI 30.1 (4.8) vs. 27.4 (4.8). C. More obesity 45% vs. 26%. D. Lower income 27% vs. 35%. E. Less high social class 29% vs. 34%. F. Less high physical activity 51% vs. 67%. G. Frailty index (%frailty) 53% vs. 32%. H. EFS (%frail) 19% vs. 10%. I. Phenotype of frailty (%frail) 23% vs. 13% |
| García-Esquinas E, et al., prospective, Spain, 2015 [33] | 1750 subjects aged ≥60 Y, 346 with DM, F/U 3.5 Y. | Assess the risk of incident frailty. | 115 Cases of incident frailty were ascertained, baseline variables and risk of frailty were: age (OR 1.13, 95% CI 1.10 to 1.16), abdominal obesity (2.64, 1.61 to 4.33), triglycerides (1.04, 1.02 to 1.05) and HbA1c 1.48, 1.20 to 1.81). |
| Nguyen TN et al., retrospective, multicentre, 2021 [34] | Total 11,140 subjects with DM, mean (SD) age 65.78 (6.39) Y. | Develop a FI and explore the relationship of frailty to subsequent adverse outcomes. | Frail compared with non-frail patients had: A. Higher mean (SD) age 66.27 (6.79) vs. 65.60 (6.24). B. Higher mean (SD) SBP 153.47 (23.72) vs. 142.09 (19.91). C. More overweight, 86.1% vs. 68.0%. D. Higher mean (SD) waist circumference, 104.40 (13.05) vs. 96.49 (12.51). E. Higher mean (SD) HbA1c, 7.85 (1.70) vs. 7.40 (1.48). F. More comorbidities, DM-related complications, and polypharmacy. |
| Bilgin S, et al., cross-sectional, Turkey, 2020 [35] | 101 patients with DM (41 frail, 60 not frail). Mean (SD) age 64.2 (8.0) Y frail, 62.2 (7.0) Y non-frail. | Observe clinical and laboratory indices of frail and non-frail patients with DM using Edmonton frail score. | Frail compared with non-frail patients: A. Median (IQR) Edmonton frail score 9.0 (7, 13) frail and 4.0 (1, 6) non-frail, p < 0.001. B. 71% frail and 48% non-frail had poorly controlled DM, p = 0.03. C. Fasting blood glucose (p = 0.02), HDL cholesterol (p = 0.005), and HbA1c (p = 0.04) were significantly higher in frail compared to non-frail. D. Serum triglyceride (p = 0.04), serum albumin (p = 0.006), Hb (p = 0.04), and eGFR (p = 0.01) were significantly lower in frail compared to non-frail. E. BMI, body weight, waist circumference, LDL-cholesterol, and total cholesterol were not significantly different between both groups. |
| Lin CL, et al., cross-sectional, Taiwan, 2022 [36] | 248 subjects with DM, mean (SD) age 73.9 (5.9) Y. | Estimate prevalence and investigate risk factors of frailty. | Frail compared to non-frail had: A. Higher mean (SD) age 75.9 (5.7) vs. 73.1 (5.8), p = 0.001. B. More patients with HbA1c >8.0%, 22.7%vs 12.1%, p = 0.04. C. Similar BMI and lipid profile. D. Higher frequency of hyperglycaemic episodes, p = 0.001. E. More ADL disability, cognitive impairment, and depression, p < 0.001. |
| Lipska KJ, et al., cross-sectional, US, 2015 [37] | 1288 non-institutionalised older people ≥ 65.0 years with DM. | Explore the prevalence of overtreatment of DM by health status. | Poor health status compared to healthy patients had: A. Higher mean (SD) age, 74.9 (6.0) vs. 72.0 (5.2) Y. B. Higher mean (SD) BMI, 32.6 (8.4) vs. 30.0 (5.6). C. More mean (SD) comorbidities, 2.9 (1.4) vs. 1.2 (0.7). D. More impairment in ≥1 ADL, 98.5% vs. 13.1%. E. More impairment in ≥1 IADL, 81.7% vs. 17.1%. F. No differences in HbA1c levels. |
| Thein FS, et al., prospective, Singapore, 2018 [38] | 486 subjects with DM, mean (SD) age 67.3 (7.5) Y. | Investigate the prevalence of cognitive impairment and/or physical frailty. | Frail compared to non-frail subjects had: A. Higher mean (SD) age 76.9 (8.0) vs. 66.0 (6.7), p < 0.0001. B. Longer mean (SD) duration of DM, 13.7 (8.8) vs. 8.6 (7.5), p = 0.04. C. More mean (SD) number of morbidities, 1.9 (1.5) vs. 1.4 (1.1), p = 0.01. D. More patients with polypharmacy, 47.8% vs. 28.6%, p = 0.04. E. Less physical exercise per week, p = 0.014. F. Similar mean (SD) BMI, 25.1 (8.7) vs. 24.9 (3.7), p = 0.9. G. Similar mean (SD) waist circumference, 86.9 (14.0) vs. 86.5 (9.4), p = 0.84. H. Similar mean (SD) total cholesterol, 5.1 (1.02) vs. 5.0 (0.97), p = 0.13. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Abdelhafiz, A.H.; Keegan, G.L.; Sinclair, A.J. Metabolic Characteristics of Frail Older People with Diabetes Mellitus—A Systematic Search for Phenotypes. Metabolites 2023, 13, 705. https://doi.org/10.3390/metabo13060705
Abdelhafiz AH, Keegan GL, Sinclair AJ. Metabolic Characteristics of Frail Older People with Diabetes Mellitus—A Systematic Search for Phenotypes. Metabolites. 2023; 13(6):705. https://doi.org/10.3390/metabo13060705
Chicago/Turabian StyleAbdelhafiz, Ahmed H., Grace L. Keegan, and Alan J. Sinclair. 2023. "Metabolic Characteristics of Frail Older People with Diabetes Mellitus—A Systematic Search for Phenotypes" Metabolites 13, no. 6: 705. https://doi.org/10.3390/metabo13060705
APA StyleAbdelhafiz, A. H., Keegan, G. L., & Sinclair, A. J. (2023). Metabolic Characteristics of Frail Older People with Diabetes Mellitus—A Systematic Search for Phenotypes. Metabolites, 13(6), 705. https://doi.org/10.3390/metabo13060705





