Abstract
Colistin is a last resort antibiotic medication for the treatment of infections caused by carbapenem-resistant Klebsiella pneumoniae. In recent years, various mechanisms have been reported to mediate colistin resistance in K. pneumoniae. This study reports a bibliometric analysis of published articles retrieved from the Scopus database relating to colistin resistance in K. pneumoniae. The research trends in colistin resistance and mechanisms of resistance were considered. A total of 1819 research articles published between 1995 and 2019 were retrieved, and the results indicated that 50.19% of the documents were published within 2017–2019. The USA had the highest participation with 340 (14.31%) articles and 14087 (17.61%) citations. Classification based on the WHO global epidemiological regions showed that the European Region contributed 42% of the articles while the American Region contributed 21%. The result further indicated that 45 countries had published at least 10 documents with strong international collaborations amounting to 272 links and a total linkage strength of 735. A total of 2282 keywords were retrieved; however, 57 keywords had ≥15 occurrences with 764 links and a total linkage strength of 2388. Furthermore, mcr-1, colistin resistance, NDM, mgrB, ceftazidime-avibactam, MDR, combination therapy, and carbapenem-resistant Enterobacteriaceae were the trending keywords. Concerning funders, the USA National Institute of Health funded 9.1% of the total research articles, topping the list. The analysis indicated poor research output, collaboration, and funding from Africa and South-East Asia and demands for improvement in international research collaboration.
1. Introduction
Bacterial resistance to chemotherapeutic antibiotics has become a global public health threat. The current annual death rate associated with infections caused by drug-resistant microorganisms is estimated at 700,000 and might increase to 10 million by 2050 if urgent action is not taken [1]. In 2017, the WHO global priority list classified drug-resistant pathogens into three tiers, with carbapenem-resistant Enterobacteriaceae as critical and requiring immediate attention [2]. The increased prevalence of resistance to carbapenems associated with the expression of specific virulence factors and the spread of new clones, limits treatment options for infections caused by multidrug-resistant Enterobacteriaceae such as Klebsiella pneumoniae [3,4]. This has led to the reintroduction of polymyxins which were previously discontinued for use in humans [5]. Colistin, also known as polymyxin E, is an antibacterial cationic polypeptide that binds to the negatively charged lipid A of Gram-negative outer membrane lipopolysaccharide. The antibacterial agent competitively displaces membrane-stabilizing divalent cations (Ca2+ and Mg2+) from the lipopolysaccharide, resulting in cell membrane disruption and cell death [6]. Gram-negative bacteria are known to be intrinsically susceptible to colistin except for bacteria of the genera Proteus, Providencia, Morganella, Serratia, Edwardsiella, and Burkholderia [6]. Colistin is a last-resort antibiotic therapy against multidrug-resistant infections caused by Gram-negative carbapenem-resistant bacteria; however, the overuse of colistin has resulted in the acquisition of resistance by several bacterial genera.
The emergence of colistin-resistant Enterobacteriaceae poses a severe challenge to the continued reliance on antibiotics chemotherapy. The spread of carbapenemase-producing colistin-resistant K. pneumoniae has been reported by researchers from different regions of the world, including Africa [7,8,9], Asia [10,11,12], Australia [13], Europe [14,15], North America [16], and South America [17]. Recently, a 71.3% prevalence was reported for colistin resistance among Escherichia coli, and K. pneumoniae isolates from Thailand [18]. Up to 2015, colistin resistance was related to chromosomal mutations resulting in the alteration of Gram-negative outer membrane lipopolysaccharide, which reduces the negative charge of the lipid A component and affinity for colistin. However, in 2016 the emergence of a plasmid-borne mcr-1 gene, a gene of the phosphoethanolamine transferase enzyme family was first reported [19,20,21,22]. This has raised concerns due to the potential rapid dissemination of resistant mediating plasmid between strains and subsequent selection pressure.
Colistin resistance in K. pneumoniae is mediated by several factors, including alterations of capsular polysaccharide and capsular type, efflux pumps, outer-membrane alterations, and alterations in lipid A and lipopolysaccharides. The inactivation of the mgrB gene, by products of the pmr operon encoding a negative feedback regulator of PhoQ-PhoP signaling system, is majorly responsible for acquired chromosomal related colistin resistance. Upregulation of PhoQ-PhoP activates the Pmr system responsible for lipopolysaccharide modification [23,24]. Alterations in the mgrB gene coupled with the disruption of pmrH operon, mutation in phoQ, elevated expression of phoPQ, and mutations of the crrAB two-component regulatory system with elevated expression of pmrCAB were reported in colistin-resistant K. pneumoniae. In addition, genes involved in cation transport and maintenance of membrane integrity were upregulated [25]. Studies have shown that the interruption of transcripts and amino acid mutation in mgrB are major mechanisms contributing to colistin resistance [26]. Amino acid substitutions in K. pneumoniae CrrB protein were associated with resistance to colistin [27]. A hospital outbreak of colistin-resistant carbapenemase-producing K. pneumoniae was traceable to the clonal expansion of an mgrB deletion mutant of a ST512 strain [28]. Furthermore, the presence of insertion sequences and nonsense/missense mutations on the cell chromosomal components were responsible for the inactivation of the mgrB gene [29]. Insertion sequences in the mgrB gene or surrounding region of crrCAB disrupted the regulatory function of the gene [30]. An IS-like element at the nucleotide position 75 of the mgrB and substitutions in PhoQ were identified as mechanisms of resistance [31]. In addition, an epidemiological investigation of colistin-resistant K. pneumoniae strains revealed that capsular type K64 and ST11 are the prevalent capsular and sequence types amongst colistin-resistant strains [26]. Atomic force microscopy revealed an altered capsule in a susceptible strain and intact capsules in a resistant strain suggesting that capsular polysaccharides influenced the response of K. pneumoniae to colistin [32]. Similarly, the presence of an efflux pump attributed to mutations in the two-component systems induced a high resistance to colistin in sequence type ST147 K. pneumoniae [33].
The spread of plasmid-mediated colistin resistance presents a critical threat. The carriage of resistant mediating genes on self-transmissible broad-host-range plasmid accentuates the potential to spread to a wider range of pathogens. Although the mcr plasmid that mediates colistin resistance was first reported between 2015–2016, recent research findings suggest a wide range of spread amongst Enterobacteriaceae, including K. pneumoniae and E. coli with the emergence of several variants. The mcr-2 to mcr-9, share 81%, 32.5%, 34%, 36%, 83%, 35%, 31% and 36% identical amino acid sequences with mcr-1, respectively [34,35,36]. In addition, minor variants have been reported for mcr-2, -4, -5, -6, -7, -8 and -9; however, a greater number of minor variants were identified for mcr-1 and mcr-3 with 18 and 28 variants, respectively [37].
A study aimed at investigating the prevalence of the mcr-1 in clinical E. coli and K. pneumoniae isolates in Thailand reported that 1.4% of K. pneumoniae isolates harboured the mcr-1 gene. The minimum inhibitory concentrations of colistin for the resistant isolates ranged between 4 and 64 mg/L [18]. Also, among 64 isolates of colistin-resistant E. coli and K. pneumoniae obtained in Iran, 1.7% harboured the mcr-1 gene [38]. Recently, a novel variant of the mcr-1 named mcr-1.2 associated with the pIncX4 plasmid was detected [39]. Also, an mcr-1.2 gene encoding a Gln3–Leu functional variant of mcr-1 was detected in ST512 K. pneumoniae isolates obtained from a rectal swab of a leukemic child. The variant mcr-1.2 gene was carried on a transferable IncX4 plasmid [40]. The mcr-gene has been reported in environmental and food samples, which calls for prompt surveillance and intervention to limit its spread. The mcr-1 gene was reported in bacterial isolates from meat samples collected from European countries, including Poland, Germany, and Czech Republic. Isolation of microorganisms from the meat samples yielded forty-two isolates carrying the mcr-1 gene with E. coli (n = 39) and K. pneumoniae (n = 3) [41]. Screening of retail fruits in China revealed the presence of mcr-1 carrying E. coli and K. pneumoniae on fruits surfaces [42], whereas in India K. pneumoniae isolated from raw food samples showed the presence of the mcr-1 gene [43]. The presence of resistant genes along the food chain presents a substantial risk for the dissemination of plasmid-mediated colistin resistance in meat and fresh-cut products. Furthermore, the colistin resistance gene mcr-1 was found in a K. pneumoniae strain of sequence type 313 recovered from hospital sewage [44]. Norman and co-workers reported the presence of clinically relevant antibiotic-resistant genes, including the plasmid-mediated mcr-1 gene in wastewater treatment plants in Germany [45]. Metagenomic analysis of wastewater sampled from 9 locations in Germany revealed the presence of the mcr-1 gene. The authors further reported a high prevalence of other gene variants with a relative abundance of mcr-1, mcr-3, mcr-4, mcr-5, and mcr-7 [46]. In addition, K. pneumoniae isolated from a stool sample from healthy volunteer in Northern Thailand harboured both mcr-1 and mcr-3 with a MIC of 16 mg/L [47]. Novel variants of mcr-3 named mcr-3.21, mcr-3.26, and mcr-3.28, located on plasmids IncP1, IncFII, and IncI1 type have been identified in K. pneumoniae strains from Laos and Thailand. The genetic environment of the mcr-3.21 and mcr-3.26 genes was composed of a composite transposon [37]. Whole Genome Sequencing of three K. pneumoniae isolates from chickens in China identified a novel variant of colistin resistance gene mcr-7.1 that shared a 70% amino acid identity with the mcr-3 gene. The mcr-7.1 gene was found in an IncI2-type plasmid (pSC20141012) that co-harboured the blaCTX-M-55 gene in one isolate [48]. The emergence of various variants of the mcr-gene is suggested to be driven by unknown selective pressure within the environment, animals, and humans [49]. In China, mcr-8, was found located on a transferrable 95,983-bp IncFII-type plasmid in K. pneumoniae. The mcr-8 showed 31.08%, 30.26%, 39.96%, 37.85%, 33.51%, 30.43%, and 37.46% identity to mcr-1, mcr-2, mcr-3, mcr-4, mcr-5, mcr-6, and mcr-7, respectively [50]. An mcr-8.1 variant discovered from a whole genome sequencing in Lebanon, was carried in a conjugative ~300 kb multi-replicon plasmid having IncFIA, IncR and IncHI1B [51]. K. pneumoniae isolates harbouring the mcr-8 gene and other resistant genes, including blaOXA-48, blaCTX-M-15 β-lactamases was reported by a whole-genome sequence study in Algeria [52]. Similarly, plasmid-mediated gene mcr-8.1 variant was recovered from infected patients in Bangladesh. The transferable mcr-8.1 was harboured in an identical highly stable multidrug-resistant IncFIB(pQil) plasmid of ~113 kb, which belonged to an epidemiologically successful K. pneumoniae clone, ST15 [53]. In addition, whole-genome sequencing of K. pneumoniae strains revealed 4 colistin-resistant strains that harboured the mcr-8.2 variant that differed from mcr-8.1 by four amino acid substitutions. The mcr-8.2 was located on a nonself-transmissible plasmid containing IncQ, IncR, and IncFII replicon [54]. Likewise, a plasmids co-harbouring both tmexCD1-toprJ1 pump responsible for tigecycline resistance and mcr-8 plasmid and blaNDM-harbouring IncX3 plasmid was isolated from humans in a nationwide surveillance [55]. Novel colistin-resistant gene mcr-9 has been reported from Klebsiella oxytoca, an opportunistic human pathogen that causes nosocomial infection and Klebsiella quasipneumoniae subsp. Quasipneumoniae from Qatar and Latin America, respectively [56,57]. The co-occurrence of multiple transferable plasmids within an isolate is a threat to public health and might further stretch the burden of antimicrobial resistance by developing pandrug-resistant isolates. The novel variant mcr-10 was found in Enterobacter roggenkampii with a 79.69% nucleotide identified with mcr-9. The mcr-10 gene encodes a protein with 82.93% identical amino acids with mcr-9 and conferred 4-fold increase in colistin MIC. The authors reported that the mcr-10 gene was located adjacent to a site-specific recombinase-encoding gene and was bracketed by IS903, and thus may be mobilized by site-specific recombination or composite transposon [58].
As antimicrobial resistance spreads, it has become essential to monitor the trends, patterns, and prevalence of resistance emergence and spread across the globe. This will provide reliable information and will enable proper surveillance. Thus, the present study summarizes the current scientific research literatures. It collates data on the reported mechanisms and prevalence of colistin resistance in K. pneumoniae. The study aims to provide quantitative analysis and statistics on the trends of publications on the subject matter over time and explore the structure of networking amongst researchers and countries in the field. This will help to identify areas of weakness such as countries and regions with research gaps and deficiencies, and thus inform researchers and public health policy makers of the realities as reflected in research outputs. Using bibliometric analysis, research gaps, risk areas, and key players (authors, institutions, funding agencies, and countries) in the field can be identified.
2. Results
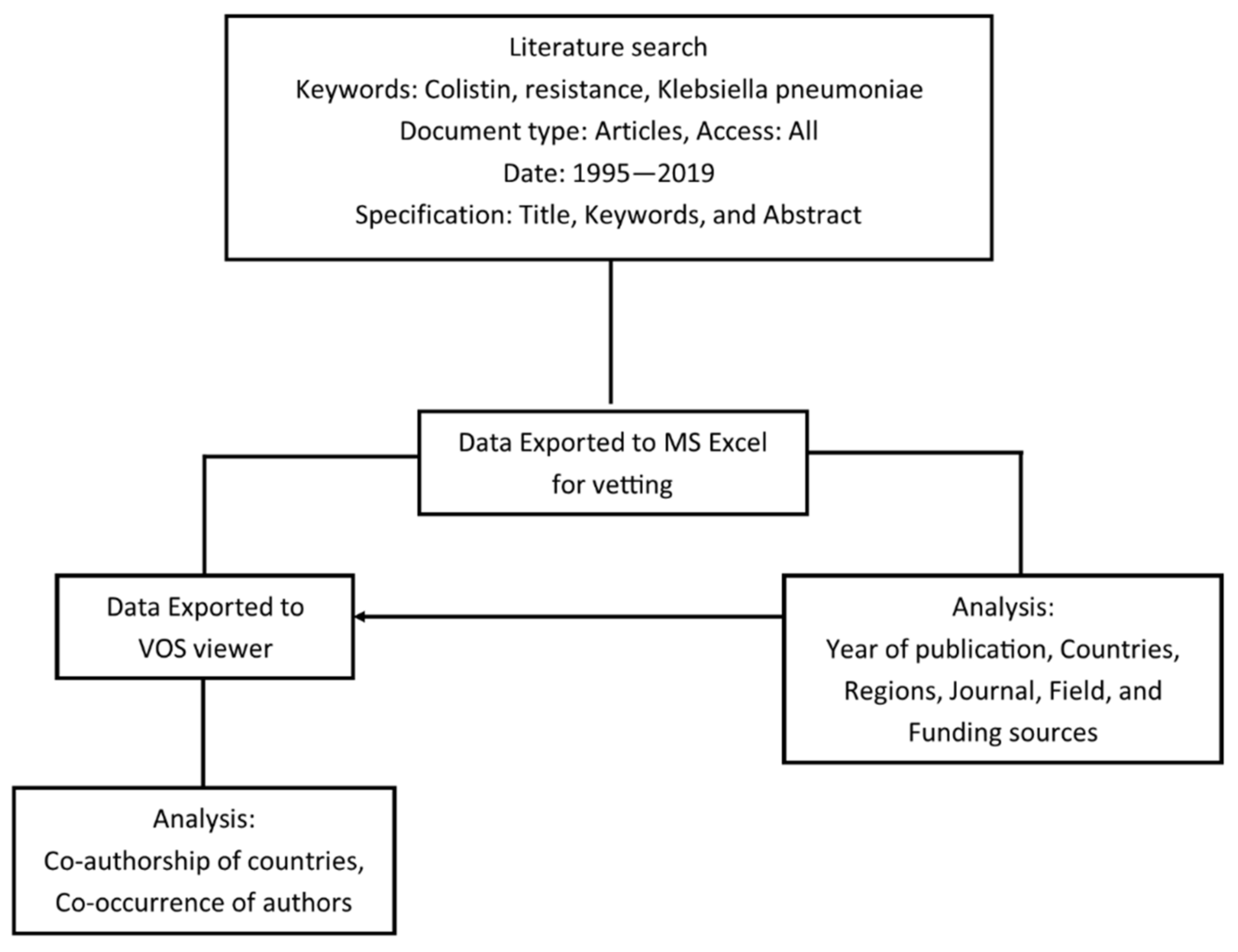
A meta-analysis of the data obtained from 1995–2019 on the Scopus database was performed by bibliometrics. The retrieved data was analyzed based on the year of publication, countries and regions, co-authorship of countries, co-occurrence of authors keywords, and funding sources. Analysis parameters were chosen to highlight the key drivers of research relating to colistin resistance in K. pneumoniae. Figure 1 presents the process flowchart employed in the study. Table 1 presents a collection of colistin-resistant mechanisms published in the literature from 1995 to June 2020, and Table 2 presents the reported prevalence of colistin resistance in K. pneumoniae from different countries.
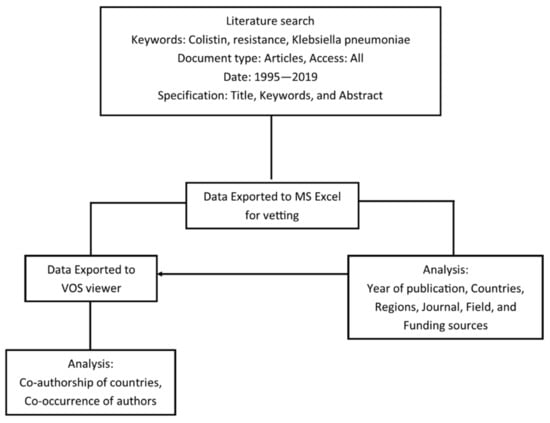
Figure 1.
Process flowchart for meta-analysis of data retrieved from the Scopus database.

Table 1.
Reported mechanisms of colistin resistance in Klebsiella pneumoniae.

Table 2.
Reported prevalence of colistin resistance in Klebsiella pneumoniae isolates.
2.1. Trend of Publication by Year
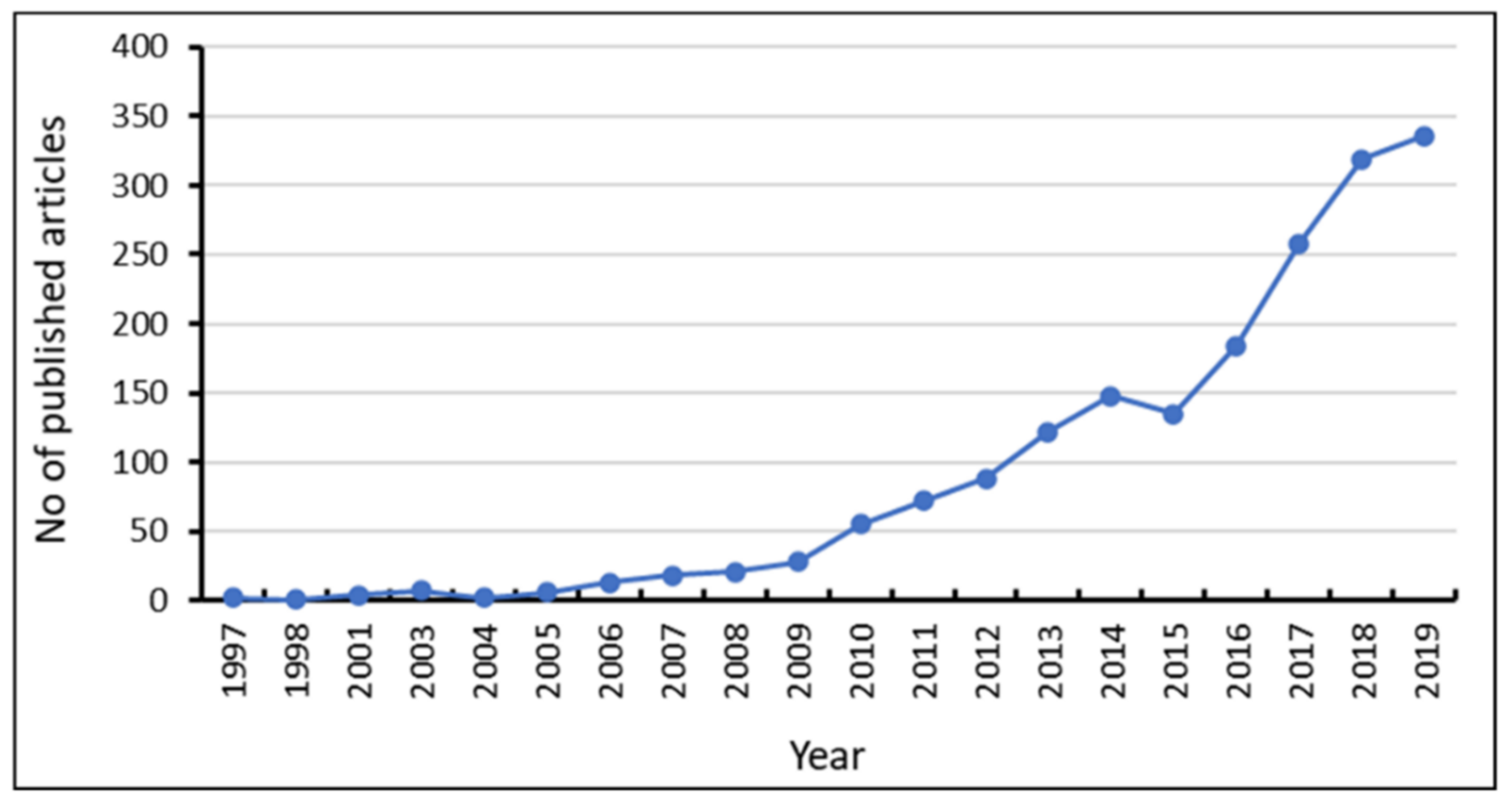
A total of 1819 research articles relating to colistin resistance in K. pneumoniae were exported from the Scopus database into VOS viewer software. The results indicated that early articles relating to the topic were published from 1997, as no preceding document was found (Figure 2). The results suggested a progressive increase in literatures pertaining to colistin resistance, with a steep increase from 2016 to 2019.
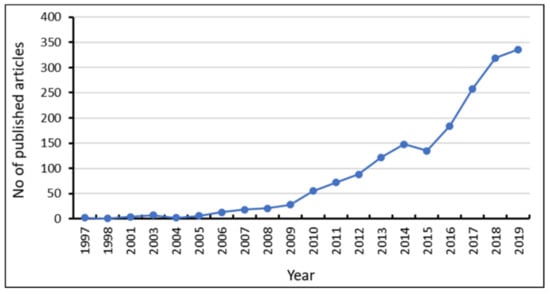
Figure 2.
Yearly research trends on colistin-resistant Klebsiella pneumoniae.
2.2. Distribution of Publications Based on Region and Country
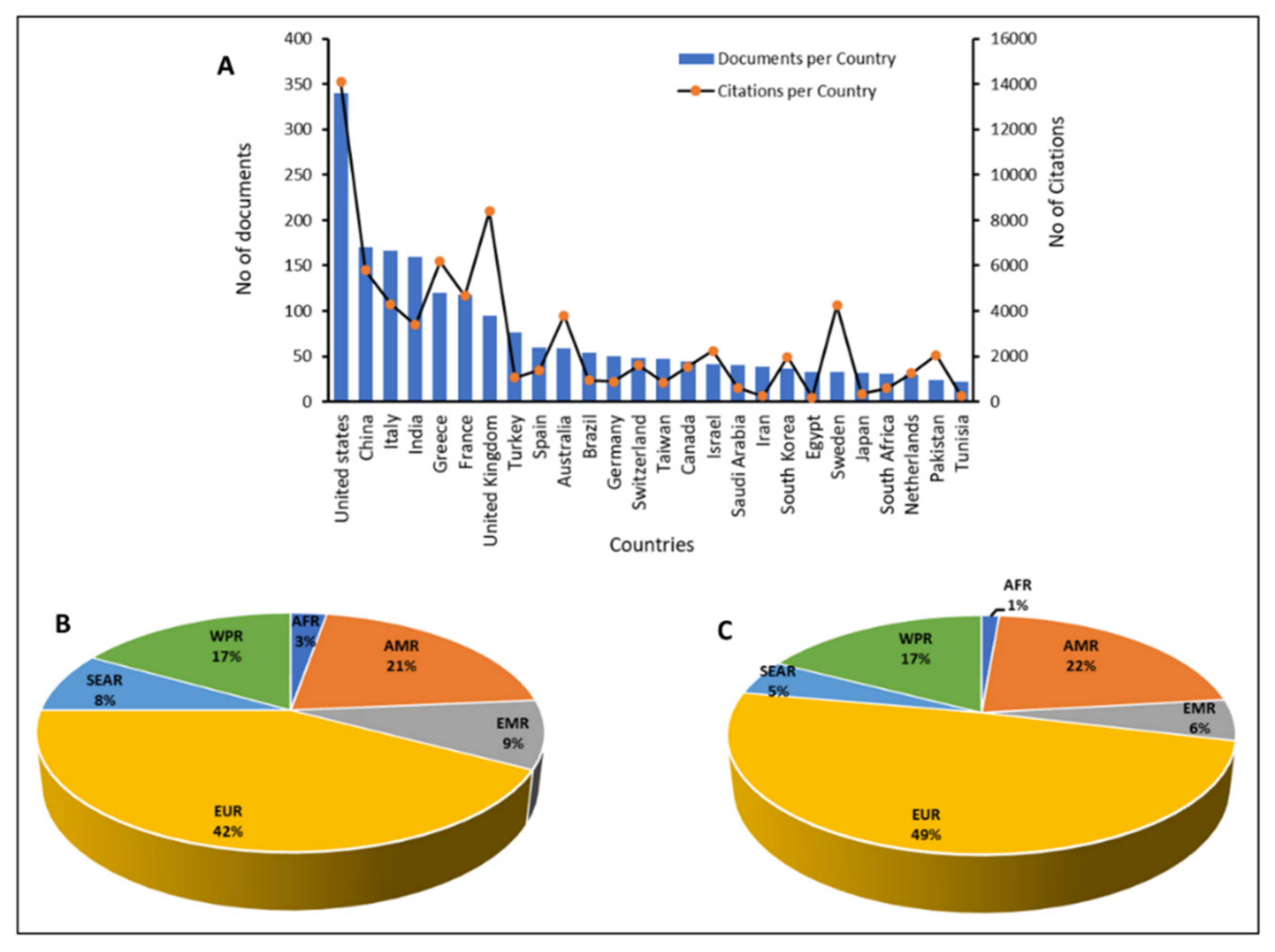
Research outputs on colistin resistance in K. pneumoniae were analyzed based on the number of publications and citations per country. It was observed that 99 countries had published contributions on colistin resistance in K. pneumoniae. Figure 3A shows the publication and citation stratification for countries with at least 20 publications relating to the topic. The results revealed that the 26 countries with a minimum of 20 publications accounted for 82.83% of all the published documents and 91.22% of citations. The United States of America had the highest contribution with 340 published research articles and 14,087 citations, amounting to 14.31 and 17.61%, respectively. China contributed 170 published articles with 5790 citations, equal to 7.15 and 7.24%, respectively. The top European countries included Italy, Greece, France, and the United Kingdom, while Egypt, South Africa, and Tunisia represented the Africa continent. Based on citations, the United Kingdom contributed 10.5%, second to the United States of America. Stratification of documents based on WHO global epidemiological regions indicated the following: that the European Region contributed (1002; 42%); American Region (496; 21%),; West Pacific Region (397; 17%); Eastern Mediterranean Region (219; 9%); Southeast Asia Region (197; 8%); and the African Region (65; 3%) (Figure 3B). Based on citations, the European Region contributed (39,264; 49%); America Region (17,465; 22%); West Pacific Region (13,848; 17%); Eastern Mediterranean Region (4466; 6%); Southeast Asia Region (3881; 5%); and the African Region (1076; 1%) (Figure 3C). The results supported the conclusions of the world health organization that “information on the true extent of antimicrobial resistance in the African region is limited due to poor surveillance and scarcity of accurate and reliable data on antimicrobial resistance in general, and on antibacterial resistance in particular” [107]. Similarly, a recent study aimed at characterizing the global distribution and diversity of mcr-9 plasmid reservoirs noted that the plasmid was distributed in 21 countries across six continents. Stratification based on the continent revealed a larger number of mcr-9 positive isolates in Europe (n = 72; 52.2%), and lower numbers in South America (n = 1; 0.7%) and Africa (n = 1; 0.7%). The authors noted that the global prevalence of mcr-9 might be underestimated due to lack of epidemiological investigations [108].
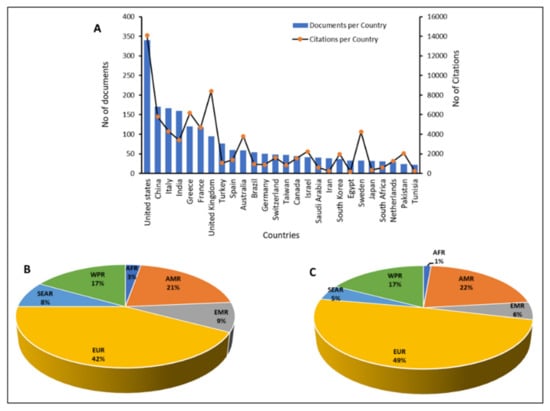
Figure 3.
Country and regional participation in research related to colistin resistance in K. pneumoniae. AFR: African Region; AMR: American Region; EUR: European Region; WPR: West Pacific Region; EMR: Eastern Mediterranean Region; SEAR: Southeast Asia Region. (A): shows publications and citation based on countries; (B): shows publications based on WHO global epidemiological regions; (C): shows citations based on WHO global epidemiological regions.
2.3. Co-Authorship of Countries
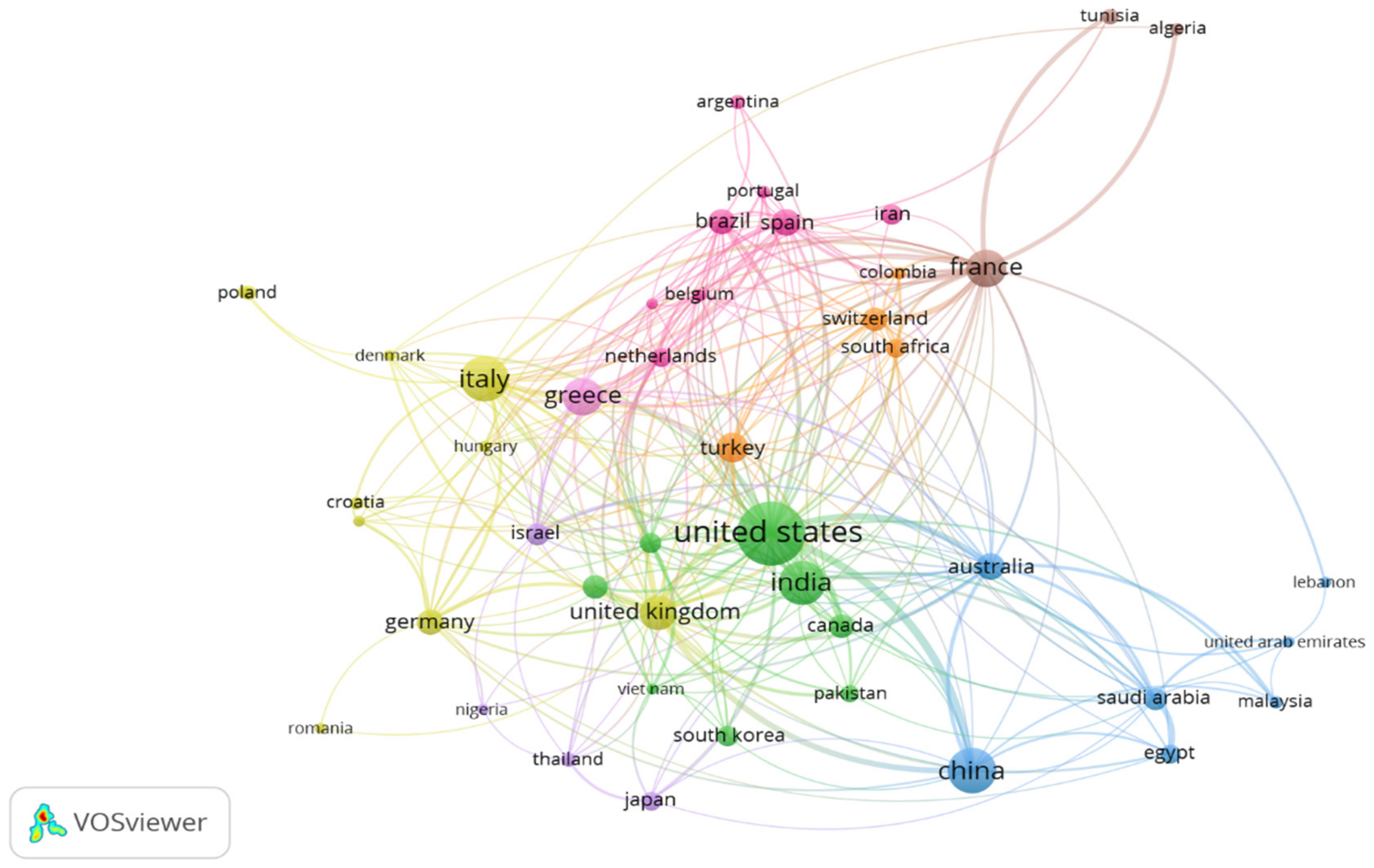
Co-authorship of countries analysis helps to understand the international research collaborations in the field of colistin resistance in K. pneumoniae. Data retrieved from the Scopus tdatabase was exported to VOS viewer software and analyzed at ≤10 countries per document for countries with at least ten published articles. The result indicated that 45 countries fitted the parameter settings distributed into 9 clusters, 272 links, and a total linkage strength of 735. The network visualization (Figure 4) showed that the United States of America had the largest collaboration network distributed into 2 clusters, 33 links, and a total linkage strength of 194 with 343 documents. The relative strength of the collaboration, measured by the thickness of the connecting lines between countries, [109] revealed that the USA had the highest collaboration with China and Australia. Research collaborations within Europe were high, with France in the lead, involved in 8 clusters, 31 links, total linkage strength of 114, and a total document of 121. Switzerland, Germany, the UK, Spain, Italy, Greece, and the Netherlands were the top European countries with elaborate research collaboration. From the Asian continent, China showed elaborate international collaborations, and was involved in 3 clusters, with 15 links, total linkage strength of 70, and 171 documents. India was involved in 2 clusters, 16 links, and atotal linkage strength of 42, and 161 documents. The African continent was led by South Africa with 7 clusters, ten links, total linkage strength of 19, and 31 documents. The results suggested poor international collaboration between Africa and Southeast Asia and the international community. The overlay visualization (Figure S1) presented the countries with the most currently published articles relating to colistin resistance in K. pneumoniae. The result indicates that Japan, Turkey, Switzerland, Vietnam, Portugal, Thailand, and Egypt are currently involved in research relating to the topic.
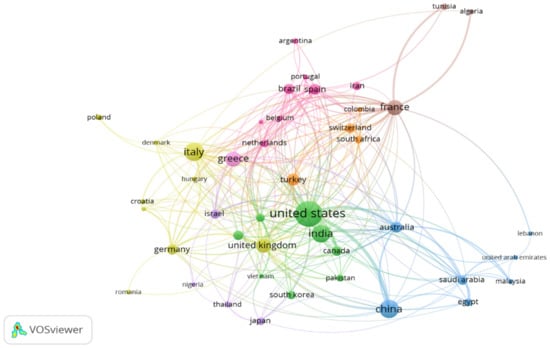
Figure 4.
Co-authorship network of countries with at least 10 publications on colistin resistance in K. pneumoniae-related research within 1995 and 2019.
2.4. Co-Occurrence of Authors Keywords
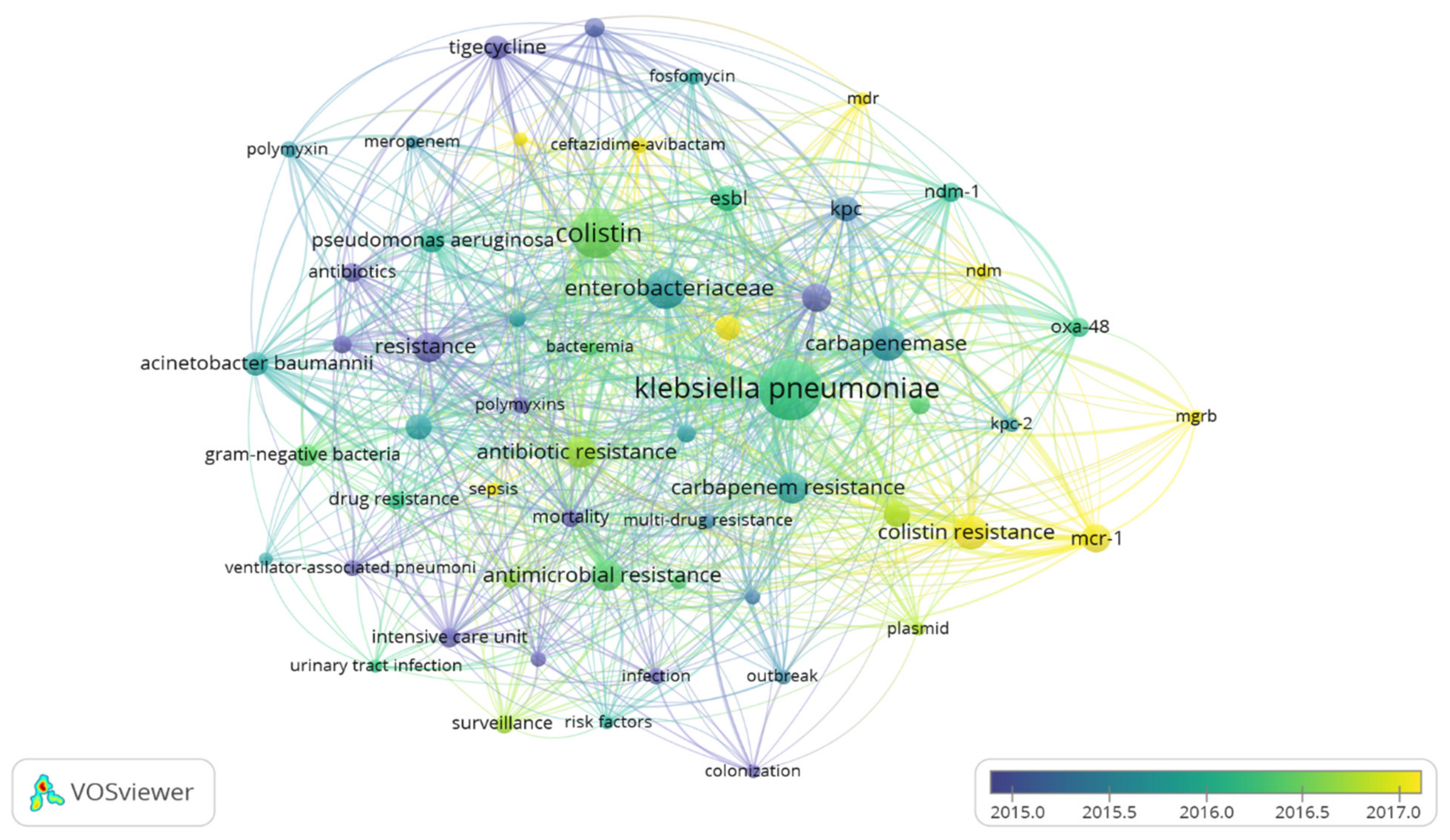
Keywords used by the authors were retrieved and analysed based on occurrence and co-occurrence. A total of 2282 keywords were retrieved; however, to ensure that only the most frequently occurring keywords were used, the analysis was restricted to keywords with at least 15 occurrences. Analysis based on the specified parameters highlighted 57 keywords classified into 6 clusters based on relatedness, 764 links, and a total linkage strength of 2388. The most occurring keywords were, K. pneumoniae, colistin, Enterobacteriaceae, colistin-resistance, mcr-1, carbapenemase, carbapenem resistance, resistance, and antimicrobial resistance. K. pneumoniae had a total occurrence of 302, with 52 links and a total linkage strength of 555 whereas colistin and colistin resistance had an occurrence of 205 and 95, respectively. Colistin resistance was associated with 5 clusters, 34 links, and a total linkage strength of 148, whereas colistin showed involvement with 3 clusters 52 links and a total linkage strength of 397. mcr-1 and mgrB were both associated with all 5 clusters, mcr-1 had 27 links, a total linkage strength of 133 and 69 occurrences, while mgrB had 13 links, and a total linkage strength of 38 with 15 occurrences. Other keywords included “carbapenem-resistant Enterobacteriaceae”, plasmid, multidrug resistance, NDM, combination therapy, and antibiotic resistance. The co-occurrence of keywords showed the relatedness of individual keywords and frequency of co-usage. The overlay visualization of co-occurrence of keywords shows the trend and evolution of keywords to reflect the dynamism of keywords with respect to shifts in research interest andthe emergence of new issues such as mechanisms and antibiotics approval. The analysis indicated that keywords such as carbapenems, carbapenemase, carbapenemases, mortality, tigecycline, polymyxin, and antibiotics were popularly used between 2015 and 2016, and the years preceding. However, keywords including mcr-1, colistin resistance, NDM, mgrB, ceftazidime-avibactam, MDR, combination therapy, and carbapenem-resistant Enterobacteriaceae are currently trending as indicated (Figure 5). This signifies the current progress in antimicrobial resistance and recent emerging resistant mechanisms.
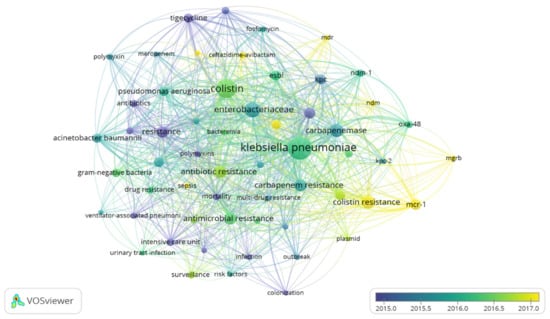
Figure 5.
Network of authors keywords with at least 15 co-occurrences on colistin-resistance in K. pneumoniae-related research within 1995 and 2019.
2.5. Funding Agencies
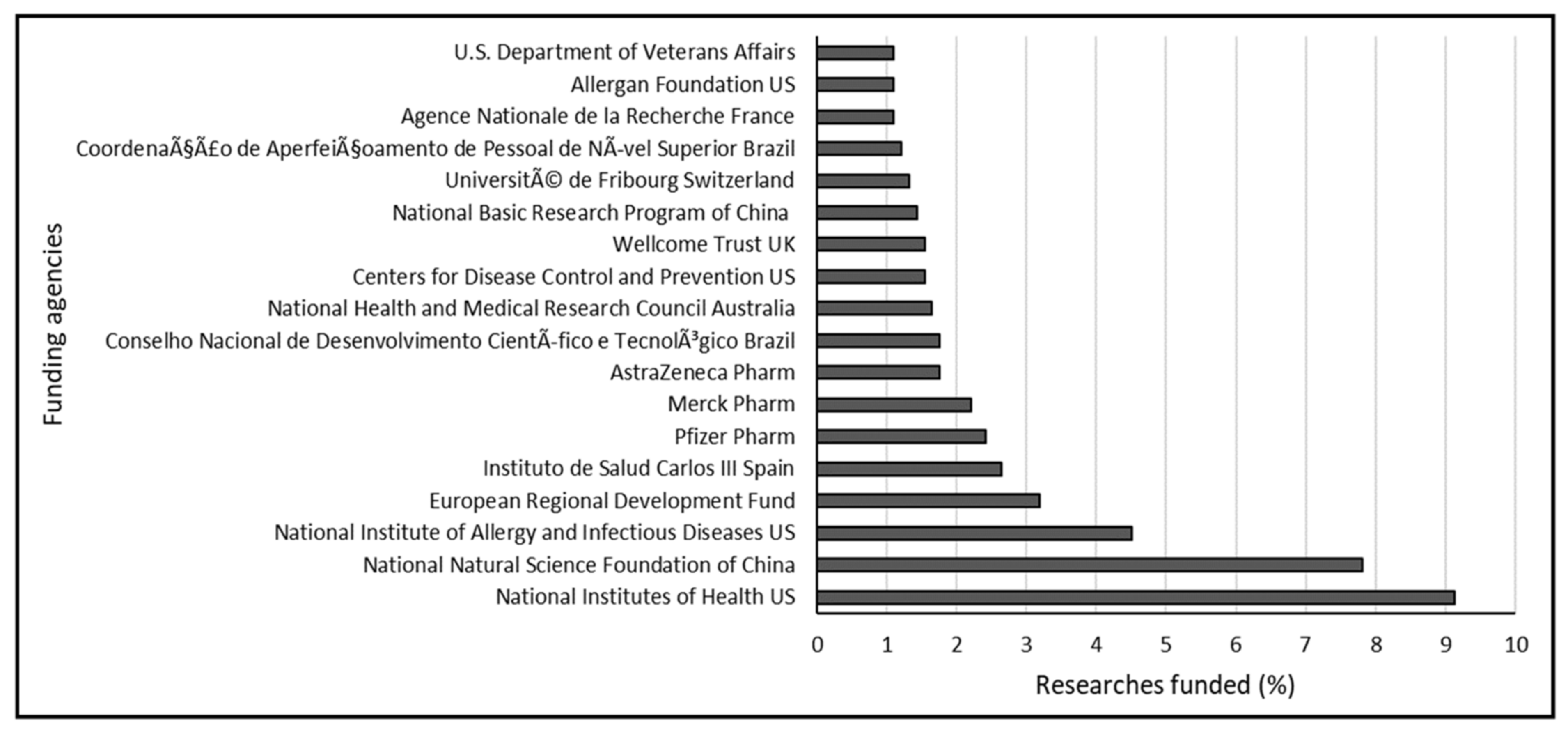
To understand the research trend, the data obtained from the Scopus database was analyzed based on funders. This helps picture the involvement of government institutions, agencies, and companies such as the pharmaceutical industries in driving the antimicrobial search and research. The results revealed the involvement of 159 funders with 909 funded research outputs. Analysis of the top funding agencies with a minimum of 10 funded documents indicated that 18 agencies funded 47.41 % of the research with 431 documents (Figure 6). The top 5 leading funders werethe National Institutes of Health US, National Natural Science Foundation of China, National Institute of Allergy and Infectious Diseases US, European Regional Development Fund, and Instituto de Salud Carlos III Spain with 9.1% (83 documents), 7.8% (71 documents), 4.5% (41 documents), 3.2% (29 documents), and 2.6% (24 documents), respectively. Some of the companies involved in research funding included Pfizer, Merck, AstraZeneca Pharma, Basilea Pharma, Meso Scale Diagnostics, Gilead Science, Allergan, Astellas Pharma, and Novartis. However, Pfizer, Merck, and AstraZeneca Pharma topped the list with contributions of 2.42% (22 documents), 2.20% (20 documents), and 1.76% (16 documents), respectively. Independent non-governmental charitable organizations involved in research funding included Wellcome Trust UK with a contribution of 1.54% (14 documents) and Allergan Foundation USA with a contribution of 1.10% (10 documents). It is also worth pointing out that the United States topped the list of funders with 3 national representatives amongst the top 18 funders including, National Institutes of Health, the National Institutes of Allergy and Infectious Diseases, and the Center for Disease Control and Prevention.
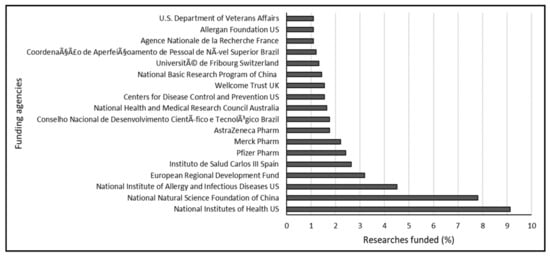
Figure 6.
Research funders with at least 10 funded documents on colistin resistance in K. pneumoniae-related research between 1995 and 2019.
3. Discussion
The revitalization of colistin as the re-emerging choice drug for the management of infections caused by carbapenem-resistant Gram-negative bacteria faced a sudden setback following the emergence of resistance in Enterobacteriaceae. This has left the health sector vulnerable to assault from carbapenem-resistant bacterial isolates, leading to increased morbidity and mortality. K. pneumoniae, an opportunistic bacterial species associated with mild to severe infections is a potential threat due to the recent emergence and spread of hypervirulent strains that havebroadened the number of people susceptible to infections, including both healthy and immunosufficient individuals [110]. Currently, researchers are overwhelmed in the search for alternative effective options, with synergistic combination therapies serving as an interim option [111]. This bibliometric analysis of research publications relating to colistin resistance in K. pneumoniae presents an overview of the research trends. The date obtained indicated the availability of articles relating to colistin and K. pneumoniae between 1997 and 2006. However, the first published multiclonal cluster of colistin resistance in K. pneumoniae on the Scopus database was reported by a retrospective observational study conducted in a Greek hospital intensive care unit which reported minimum inhibitory concentrations >4 mg/L for K. pneumoniae isolates [112]. Preceding articles published between 2005 and 2006 presented colistin as the re-emerging antibiotic of choice for the management of drug-resistant Gram-negatives including K. pneumoniae. Although colistin is effective against Gram-negative carbapenemase-producing Enterobacteriaceae, the re-emergence and revitalization of colistin were met with the sudden development of resistance following the first detection of carbapenem-resistant Enterobacteriaceae. Analysis of research output relating to colistin-resistant K. pneumoniae indicates a progressive increase beginning in 2009. However, 50.19% of all the retrieved documents were published within the last three years (2017–2019). This is due to the surge in cases of colistin resistance resulting from the extensive use and misuse of colistin in chemotherapy, and veterinaries, leading to an increased severity of colistin resistance as well as the heightened interest prompted by the categorization of antimicrobial resistance and prioritization of carbapenem-resistant Enterobacteriaceae in the critical class of the WHO global priority pathogens list [2]. In addition, the steep rise over the last three years stems from the elevated interest due to the emergence and rapid spread of colistin resistance arising from the emergence of the transferrable plasmid-mediated mcr-genes first reported in 2016, and its variants. Moreover, the acquisition of resistance in environmental isolates and reports of resistant mediating genes in both food and water might have widened the horizon of researchers interested in the topic, thus contributing to the rapid growth of research output. In addition, our results further suggested poor research outputs from the Eastern Mediterranean, Southeast Asia, and Africa, which calls for improved investment and surveillance on antimicrobial resistance. The available data on the prevalence of antimicrobial resistance across the globe indicated high levels in Africa and Asia. The yearly death attributable to AMR by 2050 according to the review on antimicrobial resistance estimates 4,150,000 and 4,730,000 annual deaths for Africa and Asia respectively [113]. The low research output on antimicrobial resistance suggests that irrespective of the World Health Assembly global and national action plan on AMR, there might be a lack of awareness and intervention policies within countries in the regions. Global AMR maps viewed at resistancebank.org indicated a high rate of resistance in Asia and Africa, with colistin resistance hotspots in Asia, and Latin America. Furthermore, resistance maps reveal the absence of major colistin resistance hotspots in Africa, and this probably suggests low surveillance and research activities regarding resistance. A recent work on the global trends in antimicrobial resistance in animals in low- and middle-income countries identified Asia as possessing the largest hotspot of AMR [114]. Similar to the findings of Sweileh and Moh’d Mansour [115], the results of the present study indicated that the United States and China dominated the research on colistin resistance in K. pneumoniae. In this study, China and India which are hotspots of AMR ranked 2nd and 4th in research output. The high rate of AMR in China has been linked to the unregulated usage of antimicrobial drugs in food-producing animals [116]. This might likewise be applicable in neighbouring countries such as India and other Asian countries. In addition, the dissemination of resistant genes through the trade route in food products, especially imported animal products are possible factors which could promote the spread of resistance. Our results further showed that the United States and China besides producing the highest number of publications also led in funding research on the topic.
To the best of our knowledge, this work presents initial data on bibliometric analysis of colistin resistance in K. pneumoniae. However, although the authors tried to ensure that the information presented represents the true trend as obtained from the Scopus database and vetted documents to avoid duplications, it is necessary to point out that the study is not without limitations. A previous bibliometric study [117], reported some challenges encountered while carrying out bibliometric studies. In the present study, the search was based on article title, abstract, and keyword. This was done to minimize loss of vital documents and to ensure the maximum retrieval of documents associated with the research topic. However, this might introduce false-positive results by delivering closely related topics which are not specific to the research title [115]. Furthermore, given the specificity of the search keywords, articles relevant to the study which were not constructed based on the keywords might be lost. Secondly, the total number of documents used may not reflect 100% accurate information on colistin-resistant K. pneumoniae since some articles relating to the field might not all be available on the Scopus database [118]. In addition, to ensure the logical presentation of the retrieved information, authors employed certain benchmarks such as a minimum number of documents, the maximum number of authors per document, and the minimum number of occurrences. Although this was done to identify front liners in every aspect of the study, previous studies have recognized it as a drawback [119]. It is also important to note that the information presented in this study might not necessarily represent the current state of AMR in the various countries and regions of the world, given that the study was not a surveillance of AMR across the regions but was based on published articles from different countries and regions. Hence, it is possible that those countries which failed to publish or whose publications are not indexed in Scopus might be underestimated.
4. Materials and Methods
4.1. Protocol for Systematic Review
The systematic review and bibliometric analysis were carried out following the PRISMA guidelines [120].
4.2. Inclusion Criteria
Data on K. pneumoniae resistance to colistin in published scientific papers were accessed from the Scopus Database on 19 July 2020. Initially, the data were obtained from the Web of Science core and Scopus.com to compare the volume and similarity of the documents available on each database. The Scopus database had 1821 published scientific papers relating to the topic, while the Web of Science core yielded 1303 published papers. An outline of the data retrieval process and analysis is presented in Figure 1. Search keywords were colistin-resistant K. pneumoniae. The year of publication was set as 1995–2019, and the search was restricted to original research articles with experimental findings relating to colistin resistance in K. pneumoniae, excluding reviews, proceedings, communications, abstracts, opinions, and letters. To ensure the retrieval of all articles relating to the subject, the search was broadened and extended to titles, abstracts, and keywords.
4.3. Study Selection
The documents were reviewed for duplication, and the abstract of selected papers were evaluated. The studies were independently screened by OZN, and TP based on titles, abstracts, and relevance. Discrepancies were resolved through consultation with the supervisors SPV and CS.
4.4. Data Analyses
The 1819 data obtained from the Scopus database were imported into the VOS viewer software and MS Excel for analysis. Data exported to MS Excel were edited, sorted, and categorized based on year of publications, countries, region, and fields, whereas data imported to the VOS viewer were used to create network maps of co-authorships of countries, journal participation, and co-occurrence of authors keywords.
5. Conclusions
The present study conducted a bibliometric analysis of published articles relating to colistin-resistant K. pneumoniae for a period of 24 years (1995–2019), to help understand the research status and trends relating to the topic. Major findings of the work include:
- A total of 1819 published articles excluding reviews, communications, proceedings, and editorials were retrieved from the Scopus database for the period from 1995 to 2019.
- There is a steep increase in the number of published articles over the last three years (2017–2019), amounting to 50.19% of all the retrieved documents.
- 99 countries had published contributions on colistin resistance in K. pneumoniae; however, 26 countries had a minimum of 20 publications and accounted for 82.83% of all the published documents and 91.22% of citations.
- Europe had the highest contribution, followed by America and the West Pacific. Research contributions from the Eastern Mediterranean, Southeast Asia, and Africa were relatively low.
- A total of 455 journals participated in the publications; however, the top 31 active journals accounted for 56.5% of publications and 64.7% of citations.
- International collaborations were highest between America and China and America and Australia. There were also high collaborations between the European nations. International collaborations were low for Africa and Asia.
- Research funders included government agencies, institutions, pharmaceutical industries, and charitable organizations. The United States of America, however, topped the list of funders, whereas no funding agencies were from Africa.
Supplementary Materials
The following are available online at https://www.mdpi.com/article/10.3390/diseases9020044/s1, Figure S1: Overlay of countries, showing countries with the most currently published articles relating to colistin resistance in K. pneumoniae.
Author Contributions
O.F.N. collated, analyzed, and interpreted the study data and wrote the manuscript. P.T. formatted the manuscript and prepared at for submission. S.P.V., and S.C., supervised the writing, corrected the draft, and provided advice where needed. All authors have read and approved the manuscript. All authors have read and agreed to the published version of the manuscript.
Funding
Postdoctoral Fellowship, Prince of Songkla University.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Acknowledgments
The authors wish to acknowledge the Postdoctoral Fellowship, Prince of Songkla University, National Research Council of Thailand.
Conflicts of Interest
The authors declare that they have no competing interest.
Abbreviations
MCR: Mobilized colistin resistance; NDM: New Delhi metallo-beta-lactamase; MDR: Multi-drug Resistance; IS: Insertion sequence; ST: Sequence type; MIC: Minimum inhibitory concentration; CTX: cefotaxime-beta lactamases; OXA: Oxacillinase, RND: Resistance-nodulation-division; CRKP: Carbapenem-resistant K. pneumoniae; KP: K. pneumoniae; Col-R: Colistin-resistant; EUR: European Region; AMR: America Region; WPR: West Pacific Region; EMR: Eastern Mediterranean Region; SEAR: South East Asia Region; AFR: Africa Region.
References
- WHO. No Time to Wait: Securing the Future from Drug-Resistant Infections; World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- WHO. Global Priority List of Antibiotic-Resistant Bacteria to Guide Research, Discovery, and Development of New Antibiotics; WHO: Geneva, Switzerland, 2017. [Google Scholar]
- Fasciana, T.; Gentile, B.; Aquilina, M.; Ciammaruconi, A.; Mascarella, C.; Anselmo, A.; Fortunato, A.; Fillo, S.; Petralito, G.; Lista, F. Co-existence of virulence factors and antibiotic resistance in new Klebsiella pneumoniae clones emerging in south of Italy. BMC Infect. Dis. 2019, 19, 1–10. [Google Scholar] [CrossRef]
- Geraci, D.; Bonura, C.; Giuffrè, M.; Saporito, L.; Graziano, G.; Aleo, A.; Fasciana, T.; Di Bernardo, F.; Stampone, T.; Palma, D. Is the monoclonal spread of the ST258, KPC-3-producing clone being replaced in southern Italy by the dissemination of multiple clones of carbapenem-nonsusceptible, KPC-3-producing Klebsiella pneumoniae? Clin. Microbiol. Infect. 2015, 21, e15–e17. [Google Scholar] [CrossRef]
- Berglund, B. Acquired resistance to colistin via chromosomal and plasmid-mediated mechanisms in Klebsiella pneumoniae. Infect. Microbes Dis. 2019, 1, 10–19. [Google Scholar] [CrossRef]
- Biswas, S.; Brunel, J.-M.; Dubus, J.-C.; Reynaud-Gaubert, M.; Rolain, J.-M. Colistin: An update on the antibiotic of the 21st century. Expert Rev. Anti Infect. Ther. 2012, 10, 917–934. [Google Scholar] [CrossRef]
- Newton-Foot, M.; Snyman, Y.; Maloba, M.R.B.; Whitelaw, A.C. Plasmid-mediated mcr-1 colistin resistance in Escherichia coli and Klebsiella spp. clinical isolates from the Western Cape region of South Africa. Antimicrob. Resist. Infect. Control 2017, 6, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kumwenda, G.P.; Sugawara, Y.; Abe, R.; Akeda, Y.; Kasambara, W.; Chizani, K.; Takeuchi, D.; Sakamoto, N.; Tomono, K.; Hamada, S. First Identification and genomic characterization of multidrug-resistant carbapenemase-producing Enterobacteriaceae clinical isolates in Malawi, Africa. J. Med. Microbiol. 2019, 68, 1707–1715. [Google Scholar] [CrossRef]
- Coetzee, J.; Corcoran, C.; Prentice, E.; Moodley, M.; Mendelson, M.; Poirel, L.; Nordmann, P.; Brink, A.J. Emergence of plasmid-mediated colistin resistance (MCR-1) among Escherichia coli isolated from South African patients. S. Afr. Med. J. 2016, 106, 449–450. [Google Scholar] [CrossRef]
- Tada, T.; Tsuchiya, M.; Shimada, K.; Nga, T.T.T.; Phu, T.T.; Ohmagari, N.; Kirikae, T. Dissemination of carbapenem-resistant Klebsiella pneumoniae clinical isolates with various combinations of Carbapenemases (KPC-2, NDM-1, NDM-4, and OXA-48) and 16S rRNA Methylases (RmtB and RmtC) in Vietnam. BMC Infect. Dis. 2017, 17, 467. [Google Scholar] [CrossRef] [PubMed]
- Mobasseri, G.; Teh, C.S.J.; Ooi, P.T.; Thong, K.L. The emergence of colistin-resistant Klebsiella pneumoniae strains from swine in Malaysia. J. Glob. Antimicrob. Resist. 2019, 17, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Jubair, H.H.; Hadi, Z.J.; Almohana, A.M. First Report of Colistin Resistance Gene mcr-1 in Carbapenem-Resistant Clinical Isolates of Klebsiella pneumoniae in Iraq. Med. Leg. Update 2020, 20, 461–466. [Google Scholar]
- Sherry, N.L.; Lane, C.R.; Kwong, J.C.; Schultz, M.; Sait, M.; Stevens, K.; Ballard, S.; da Silva, A.G.; Seemann, T.; Gorrie, C.L. Genomics for molecular epidemiology and detecting transmission of carbapenemase-producing Enterobacterales in Victoria, Australia, 2012 to 2016. J. Clin. Microbiol. 2019, 57, e00573-19. [Google Scholar] [CrossRef] [PubMed]
- Zafer, M.M.; El-Mahallawy, H.A.; Abdulhak, A.; Amin, M.A.; Al-Agamy, M.H.; Radwan, H.H. Emergence of colistin resistance in multidrug-resistant Klebsiella pneumoniae and Escherichia coli strains isolated from cancer patients. Ann. Clin. Microbiol. Antimicrob. 2019, 18, 40. [Google Scholar] [CrossRef]
- Novović, K.; Trudić, A.; Brkić, S.; Vasiljević, Z.; Kojić, M.; Medić, D.; Ćirković, I.; Jovčić, B. Molecular epidemiology of colistin-resistant, carbapenemase-producing Klebsiella pneumoniae in Serbia from 2013 to 2016. Antimicrob. Agents Chemother. 2017, 61, e02550-16. [Google Scholar] [CrossRef]
- Macesic, N.; Nelson, B.; Mcconville, T.H.; Giddins, M.J.; Green, D.A.; Stump, S.; Gomez-Simmonds, A.; Annavajhala, M.K.; Uhlemann, A.-C. Emergence of polymyxin resistance in clinical Klebsiella pneumoniae through diverse genetic adaptations: A genomic, retrospective cohort study. Clin. Infect. Dis. 2020, 70, 2084–2091. [Google Scholar] [CrossRef]
- Rapoport, M.; Faccone, D.; Pasteran, F.; Ceriana, P.; Albornoz, E.; Petroni, A.; Corso, A.; Group, M. First description of mcr-1-mediated colistin resistance in human infections caused by Escherichia coli in Latin America. Antimicrob. Agents Chemother. 2016, 60, 4412–4413. [Google Scholar] [CrossRef]
- Eiamphungporn, W.; Yainoy, S.; Jumderm, C.; Tan-Arsuwongkul, R.; Tiengrim, S.; Thamlikitkul, V. Prevalence of the colistin resistance gene mcr-1 in colistin-resistant Escherichia coli and Klebsiella pneumoniae isolated from humans in Thailand. J. Glob. Antimicrob. Resist. 2018, 15, 32–35. [Google Scholar] [CrossRef]
- Yao, X.; Doi, Y.; Zeng, L.; Lv, L.; Liu, J.-H. Carbapenem-resistant and colistin-resistant Escherichia coli co-producing NDM-9 and MCR-1. Lancet Infect. Dis. 2016, 16, 288–289. [Google Scholar] [CrossRef]
- Skov, R.L.; Monnet, D.L. Plasmid-mediated colistin resistance (mcr-1 gene): Three months later, the story unfolds. Eurosurveillance 2016, 21, 30155. [Google Scholar] [CrossRef]
- Liu, Y.-Y.; Wang, Y.; Walsh, T.R.; Yi, L.-X.; Zhang, R.; Spencer, J.; Doi, Y.; Tian, G.; Dong, B.; Huang, X. Emergence of plasmid-mediated colistin resistance mechanism MCR-1 in animals and human beings in China: A microbiological and molecular biological study. Lancet Infect. Dis. 2016, 16, 161–168. [Google Scholar] [CrossRef]
- Arcilla, M.S.; van Hattem, J.M.; Matamoros, S.; Melles, D.C.; Penders, J.; de Jong, M.D.; Schultsz, C. Dissemination of the mcr-1 colistin resistance gene. Lancet Infect. Dis. 2016, 16, 147–149. [Google Scholar] [CrossRef]
- Cannatelli, A.; Giani, T.; D’Andrea, M.M.; Di Pilato, V.; Arena, F.; Conte, V.; Tryfinopoulou, K.; Vatopoulos, A.; Rossolini, G.M. MgrB inactivation is a common mechanism of colistin resistance in KPC-producing Klebsiella pneumoniae of clinical origin. Antimicrob. Agents Chemother. 2014, 58, 5696–5703. [Google Scholar] [CrossRef]
- Cannatelli, A.; D’Andrea, M.M.; Giani, T.; Di Pilato, V.; Arena, F.; Ambretti, S.; Gaibani, P.; Rossolini, G.M. In vivo emergence of colistin resistance in Klebsiella pneumoniae producing KPC-type carbapenemases mediated by insertional inactivation of the PhoQ/PhoP mgrB regulator. Antimicrob. Agents Chemother. 2013, 57, 5521–5526. [Google Scholar] [CrossRef] [PubMed]
- Wright, M.S.; Suzuki, Y.; Jones, M.B.; Marshall, S.H.; Rudin, S.D.; van Duin, D.; Kaye, K.; Jacobs, M.R.; Bonomo, R.A.; Adams, M.D. Genomic and transcriptomic analyses of colistin-resistant clinical isolates of Klebsiella pneumoniae reveal multiple pathways of resistance. Antimicrob. Agents Chemother. 2015, 59, 536–543. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.-H.; Lin, T.-L.; Pan, Y.-J.; Wang, Y.-P.; Lin, Y.-T.; Wang, J.-T. Colistin resistance mechanisms in Klebsiella pneumoniae strains from Taiwan. Antimicrob. Agents Chemother. 2015, 59, 2909–2913. [Google Scholar] [CrossRef]
- Cheng, Y.-H.; Lin, T.-L.; Lin, Y.-T.; Wang, J.-T. Amino acid substitutions of CrrB responsible for resistance to colistin through CrrC in Klebsiella pneumoniae. Antimicrob. Agents Chemother. 2016, 60, 3709–3716. [Google Scholar] [CrossRef] [PubMed]
- Giani, T.; Arena, F.; Vaggelli, G.; Conte, V.; Chiarelli, A.; De Angelis, L.H.; Fornaini, R.; Grazzini, M.; Niccolini, F.; Pecile, P. Large nosocomial outbreak of colistin-resistant, carbapenemase-producing Klebsiella pneumoniae traced to clonal expansion of an mgrB deletion mutant. J. Clin. Microbiol. 2015, 53, 3341–3344. [Google Scholar] [CrossRef] [PubMed]
- Mouna, H.; Stylianos, C.; Linda, H.; Efthimia, P.; Sophia, P.; Nikoletta, C.; Sophia, T.; Vassiliki, P.; Nikoletta, S.; Iris, S. Inactivation of mgrB gene regulator and resistance to colistin is becoming endemic in carbapenem-resistant Klebsiella pneumoniae in Greece: A nationwide study from 2014 to 2017: Carbapenem and colistin-resistant Klebsiella pneumoniae. Int. J. Antimicrob. Agents 2020, 55, 105930. [Google Scholar]
- Yang, T.-Y.; Wang, S.-F.; Lin, J.-E.; Griffith, B.T.S.; Lian, S.-H.; Hong, Z.-D.; Lin, L.; Lu, P.-L.; Tseng, S.-P. Contributions of insertion sequences conferring colistin resistance in Klebsiella pneumoniae. Int. J. Antimicrob. Agents 2020, 55, 105894. [Google Scholar] [CrossRef]
- Zhu, Y.; Galani, I.; Karaiskos, I.; Lu, J.; Aye, S.M.; Huang, J.; Heidi, H.Y.; Velkov, T.; Giamarellou, H.; Li, J. Multifaceted mechanisms of colistin resistance revealed by genomic analysis of multidrug-resistant Klebsiella pneumoniae isolates from individual patients before and after colistin treatment. J. Infect. 2019, 79, 312–321. [Google Scholar] [CrossRef]
- Formosa, C.; Herold, M.; Vidaillac, C.; Duval, R.E.; Dague, E. Unravelling of a mechanism of resistance to colistin in Klebsiella pneumoniae using atomic force microscopy. J. Antimicrob. Chemother. 2015, 70, 2261–2270. [Google Scholar] [CrossRef]
- Dey, S.; Gaur, M.; Sahoo, R.K.; Das, A.; Jain, B.; Pati, S.; Subudhi, E. Genomic characterization of XDR Klebsiella pneumoniae ST147 co-resistant to carbapenem and colistin-The first report in India. J. Glob. Antimicrob. Resist. 2020, 22, 54–56. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Wang, Y.; Zhou, Y.; Wang, Z.; Wang, Y.; Zhang, S.; Shen, Z. Emergence of colistin resistance gene mcr-8 and its variant in Raoultella ornithinolytica. Front. Microbiol. 2019, 10, 228. [Google Scholar] [CrossRef] [PubMed]
- Carroll, L.M.; Gaballa, A.; Guldimann, C.; Sullivan, G.; Henderson, L.O.; Wiedmann, M. Identification of novel mobilized colistin resistance gene mcr-9 in a multidrug-resistant, colistin-susceptible Salmonella enterica serotype Typhimurium isolate. mBio 2019, 10, e00853-19. [Google Scholar] [CrossRef] [PubMed]
- Nang, S.C.; Li, J.; Velkov, T. The rise and spread of mcr plasmid-mediated polymyxin resistance. Crit. Rev. Microbiol. 2019, 45, 131–161. [Google Scholar] [CrossRef]
- Hadjadj, L.; Baron, S.A.; Olaitan, A.O.; Morand, S.; Rolain, J.-M. Co-occurrence of Variants of mcr-3 and mcr-8 Genes in a Klebsiella pneumoniae Isolate From Laos. Front. Microbiol. 2019, 10, 2720. [Google Scholar] [CrossRef]
- Moosavian, M.; Emam, N. The first report of emerging mobilized colistin-resistance (Mcr) genes and ERIC-PCR typing in Escherichia coli and Klebsiella pneumoniae clinical isolates in southwest Iran. Infect. Drug Resist. 2019, 12, 1001–1010. [Google Scholar] [CrossRef]
- Giordano, C.; Klak, A.; Barnini, S.; Chlebowicz, M.A.; Menconi, M.; Rossen, J.W.; Friedrich, A.W.; Bathoorn, E. Reduced fitness costs of mcr-1.2 compared to mutated pmrB in isogenic colistin-resistant KPC-3-producing Klebsiella pneumoniae. mSphere 2019, 4. [Google Scholar] [CrossRef]
- Di Pilato, V.; Arena, F.; Tascini, C.; Cannatelli, A.; Henrici De Angelis, L.; Fortunato, S.; Giani, T.; Menichetti, F.; Rossolini, G.M. mcr-1.2, a new mcr variant carried on a transferable plasmid from a colistin-resistant KPC carbapenemase-producing Klebsiella pneumoniae strain of sequence type 512. Antimicrob. Agents Chemother. 2016, 60, 5612–5615. [Google Scholar] [CrossRef] [PubMed]
- Gelbicova, T.; Kolackova, I.; Krutova, M.; Karpiskova, R. The emergence of mcr-1-mediated colistin-resistant Escherichia coli and Klebsiella pneumoniae in domestic and imported turkey meat in the Czech Republic 2017–2018. Folia Microbiol. 2020, 65, 211–216. [Google Scholar] [CrossRef] [PubMed]
- Yang, F.; Shen, C.; Zheng, X.; Liu, Y.; Ahmed, M.A.E.G.E.S.; Zhao, Z.; Liao, K.; Shi, Y.; Guo, X.; Zhong, R.; et al. Plasmid-mediated colistin resistance gene mcr-1 in Escherichia coli and Klebsiella pneumoniae isolated from market retail fruits in Guangzhou, China. Infect. Drug Resist. 2019, 12, 385–389. [Google Scholar] [CrossRef]
- Ghafur, A.; Shankar, C.; GnanaSoundari, P.; Venkatesan, M.; Mani, D.; Thirunarayanan, M.; Veeraraghavan, B. Detection of chromosomal and plasmid-mediated mechanisms of colistin resistance in Escherichia coli and Klebsiella pneumoniae from Indian food samples. J. Glob. Antimicrob. Resist. 2019, 16, 48–52. [Google Scholar] [CrossRef] [PubMed]
- Zhao, F.; Feng, Y.; Lü, X.; McNally, A.; Zong, Z. IncP plasmid carrying colistin resistance gene mcr-1 in Klebsiella pneumoniae from hospital sewage. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef] [PubMed]
- Hembach, N.; Schmid, F.; Alexander, J.; Hiller, C.; Rogall, E.T.; Schwartz, T. Occurrence of the mcr-1 colistin resistance gene and other clinically relevant antibiotic resistance genes in microbial populations at different municipal wastewater treatment plants in Germany. Front. Microbiol. 2017, 8, 1282. [Google Scholar] [CrossRef] [PubMed]
- Kneis, D.; Berendonk, T.U.; Heß, S. High prevalence of colistin resistance genes in German municipal wastewater. Sci. Total Environ. 2019, 694, 133454. [Google Scholar] [CrossRef]
- Yu, Y.; Andrey, D.O.; Yang, R.S.; Sands, K.; Tansawai, U.; Li, M.; Portal, E.; Gales, A.C.; Niumsup, P.R.; Sun, J.; et al. A Klebsiella pneumoniae strain co-harbouring mcr-1 and mcr-3 from a human in Thailand. J. Antimicrob. Chemother. 2020, 75, 2372–2374. [Google Scholar] [CrossRef]
- Yang, Y.Q.; Li, Y.X.; Lei, C.W.; Zhang, A.Y.; Wang, H.N. Novel plasmid-mediated colistin resistance gene mcr-7.1 in Klebsiella pneumoniae. J. Antimicrob. Chemother. 2018, 73, 1791–1795. [Google Scholar] [CrossRef]
- Sun, J.; Zhang, H.; Liu, Y.-H.; Feng, Y. Towards understanding MCR-like colistin resistance. Trends Microbiol. 2018, 26, 794–808. [Google Scholar] [CrossRef]
- Wang, X.; Wang, Y.; Zhou, Y.; Li, J.; Yin, W.; Wang, S.; Zhang, S.; Shen, J.; Shen, Z.; Wang, Y. Emergence of a novel mobile colistin resistance gene, mcr-8, in NDM-producing Klebsiella pneumoniae article. Emerg. Microbes Infect. 2018, 7. [Google Scholar] [CrossRef] [PubMed]
- Salloum, T.; Panossian, B.; Bitar, I.; Bitar, I.; Hrabak, J.; Hrabak, J.; Araj, G.F.; Tokajian, S. First report of plasmid-mediated colistin resistance mcr-8.1 gene from a clinical Klebsiella pneumoniae isolate from Lebanon. Antimicrob. Resist. Infect. Control 2020, 9. [Google Scholar] [CrossRef]
- Nabti, L.Z.; Sahli, F.; Ngaiganam, E.P.; Radji, N.; Mezaghcha, W.; Lupande-Mwenebitu, D.; Baron, S.A.; Rolain, J.M.; Diene, S.M. Development of real-time PCR assay allowed describing the first clinical Klebsiella pneumoniae isolate harboring plasmid-mediated colistin resistance mcr-8 gene in Algeria. J. Glob. Antimicrob. Resist. 2020, 20, 266–271. [Google Scholar] [CrossRef]
- Farzana, R.; Jones, L.S.; Barratt, A.; Rahman, M.A.; Sands, K.; Portal, E.; Boostrom, I.; Espina, L.; Pervin, M.; Nasir Uddin, A.K.M.; et al. Emergence of mobile colistin resistance (mcr-8) in a highly successful Klebsiella pneumoniae sequence type 15 clone from clinical infections in Bangladesh. mSphere 2020, 5. [Google Scholar] [CrossRef]
- Ma, K.; Feng, Y.; Liu, L.; Yao, Z.; Zong, Z. A Cluster of Colistin- and Carbapenem-Resistant Klebsiella pneumoniae Carrying blaNDM-1 and mcr-8.2. J. Infect. Dis. 2020, 221, S237–S242. [Google Scholar] [CrossRef]
- Sun, S.; Gao, H.; Liu, Y.; Jin, L.; Wang, R.; Wang, X.; Wang, Q.; Yin, Y.; Zhang, Y.; Wang, H. Co-existence of a novel plasmid-mediated efflux pump with colistin resistance gene mcr in one plasmid confers transferable multidrug resistance in Klebsiella pneumoniae. Emerg. Microbes Infect. 2020, 9, 1102–1113. [Google Scholar] [CrossRef] [PubMed]
- Faccone, D.; Martino, F.; Albornoz, E.; Gomez, S.; Corso, A.; Petroni, A. Plasmid carrying mcr-9 from an extensively drug-resistant NDM-1-producing Klebsiella quasipneumoniae subsp. quasipneumoniae clinical isolate. Infec. Genet. Evol. 2020, 81. [Google Scholar] [CrossRef]
- Tsui, C.K.M.; Tsui, C.K.M.; Tsui, C.K.M.; Sundararaju, S.; Al Mana, H.; Al Mana, H.; Hasan, M.R.; Hasan, M.R.; Tang, P.; Tang, P.; et al. Draft genome sequence of an extended-spectrum β-lactamase-producing Klebsiella oxytoca strain bearing mcr-9 from Qatar. Micro. Res. Ann. 2020, 9. [Google Scholar] [CrossRef]
- Wang, C.; Feng, Y.; Liu, L.; Wei, L.; Kang, M.; Zong, Z. Identification of novel mobile colistin resistance gene mcr-10. Emerg. Microbes Infect. 2020, 9, 508–516. [Google Scholar] [CrossRef]
- Olaitan, A.O.; Diene, S.M.; Kempf, M.; Berrazeg, M.; Bakour, S.; Gupta, S.K.; Thongmalayvong, B.; Akkhavong, K.; Somphavong, S.; Paboriboune, P.; et al. Worldwide emergence of colistin resistance in Klebsiella pneumoniae from healthy humans and patients in Lao PDR, Thailand, Israel, Nigeria and France owing to inactivation of the PhoP/PhoQ regulator mgrB: An epidemiological and molecular study. Int. J. Antimicrob. Agents 2014, 44, 500–507. [Google Scholar] [CrossRef] [PubMed]
- Sassera, D.; Comandatore, F.; Gaibani, P.; D’Auria, G.; Mariconti, M.; Landini, M.P.; Sambri, V.; Marone, P. Comparative genomics of closely related strains of Klebsiella pneumoniae reveals genes possibly involved in colistin resistance. Ann. Microbiol. 2014, 64, 887–890. [Google Scholar] [CrossRef]
- Jayol, A.; Nordmann, P.; Brink, A.; Villegas, M.V.; Dubois, V.; Poirela, L. High-level resistance to colistin mediated by various mutations in the crrB gene among carbapenemase-producing Klebsiella pneumoniae. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef] [PubMed]
- Esposito, E.P.; Cervoni, M.; Bernardo, M.; Crivaro, V.; Cuccurullo, S.; Imperi, F.; Zarrilli, R. Molecular epidemiology and virulence profiles of colistin-resistant Klebsiella pneumoniae blood isolates from the hospital agency “Ospedale dei Colli”, Naples, Italy. Front. Microbiol. 2018, 9. [Google Scholar] [CrossRef]
- Jaidane, N.; Bonnin, R.A.; Mansour, W.; Girlich, D.; Creton, E.; Cotellon, G.; Chaouch, C.; Boujaafar, N.; Bouallegue, O.; Naas, T. Genomic insights into colistin-resistant Klebsiella pneumoniae from a Tunisian teaching hospital. Antimicrob. Agents Chemother. 2018, 62. [Google Scholar] [CrossRef]
- Malli, E.; Florou, Z.; Tsilipounidaki, K.; Voulgaridi, I.; Stefos, A.; Xitsas, S.; Papagiannitsis, C.C.; Petinaki, E. Evaluation of rapid polymyxin NP test to detect colistin-resistant Klebsiella pneumoniae isolated in a tertiary Greek hospital. J. Microbiol. Methods 2018, 153, 35–39. [Google Scholar] [CrossRef] [PubMed]
- Mathur, P.; Veeraraghavan, B.; Devanga Ragupathi, N.K.; Inbanathan, F.Y.; Khurana, S.; Bhardwaj, N.; Kumar, S.; Sagar, S.; Gupta, A. Multiple mutations in lipid-A modification pathway & novel fosA variants in colistin-resistant Klebsiella pneumoniae. Future Sci. OA 2018, 4. [Google Scholar] [CrossRef]
- Zaman, T.U.; Albladi, M.; Siddique, M.I.; Aljohani, S.M.; Balkhy, H.H. Insertion element mediated mgrB disruption and presence of ISKpn28 in colistin-resistant Klebsiella pneumoniae isolates from Saudi Arabia. Infect. Drug Resist. 2018, 11, 1183–1187. [Google Scholar] [CrossRef] [PubMed]
- Al-Farsi, H.M.; Al-Adwani, S.; Ahmed, S.; Vogt, C.; Ambikan, A.T.; Leber, A.; Al-Jardani, A.; Al-Azri, S.; Al-Muharmi, Z.; Toprak, M.S.; et al. Effects of the Antimicrobial Peptide LL-37 and Innate Effector Mechanisms in Colistin-Resistant Klebsiella pneumoniae With mgrB Insertions. Front. Microbiol. 2019, 10. [Google Scholar] [CrossRef] [PubMed]
- Lalaoui, R.; Bakour, S.; Livnat, K.; Assous, M.V.; Diene, S.M.; Rolain, J.M. Spread of Carbapenem and Colistin-Resistant Klebsiella pneumoniae ST512 Clinical Isolates in Israel: A Cause for Vigilance. Microb. Drug Resist. 2019, 25, 63–71. [Google Scholar] [CrossRef]
- Nawfal Dagher, T.; Azar, E.; Al-Bayssari, C.; Chamieh, A.S.; Rolain, J.M. First Detection of Colistin-Resistant Klebsiella pneumoniae in Association with NDM-5 Carbapenemase Isolated from Clinical Lebanese Patients. Microb. Drug Resist. 2019, 25, 925–930. [Google Scholar] [CrossRef]
- Shankar, C.; Venkatesan, M.; Rajan, R.; Mani, D.; Lal, B.; Prakash, J.A.J.; Anandan, S.; Pragasam, A.K.; Walia, K.; Ohri, V.C.; et al. Molecular characterization of colistin-resistant Klebsiella pneumoniae & its clonal relationship among Indian isolates. Indian J. Med. Res. 2019, 149, 199–207. [Google Scholar] [CrossRef]
- Palmieri, M.; D’Andrea, M.M.; Pelegrin, A.C.; Mirande, C.; Brkic, S.; Cirkovic, I.; Goossens, H.; Rossolini, G.M.; van Belkum, A. Genomic Epidemiology of Carbapenem- and Colistin-Resistant Klebsiella pneumoniae Isolates From Serbia: Predominance of ST101 Strains Carrying a Novel OXA-48 Plasmid. Front. Microbiol. 2020, 11. [Google Scholar] [CrossRef]
- Yang, X.; Peng, K.; Zhang, Y.; Liu, L.; Li, R. Characterization of a novel mcr-8.2-bearing plasmid in ST395 Klebsiella pneumoniae of chicken origin. Infect. Drug Resist. 2020, 13, 1781–1784. [Google Scholar] [CrossRef]
- Yap, P.S.X.; Ahmad Kamar, A.; Chong, C.W.; Ngoi, S.T.; Teh, C.S.J. Genomic Insights into Two Colistin-Resistant Klebsiella pneumoniae Strains Isolated from the Stool of Preterm Neonate during the First Week of Life. Microb. Drug Resist. 2020, 26, 190–203. [Google Scholar] [CrossRef]
- Xu, J.; Zhao, Z.; Ge, Y.; He, F. Rapid emergence of a pandrug-resistant Klebsiella pneumoniae ST11 isolate in an inpatient in a teaching hospital in China after treatment with multiple broad-spectrum antibiotics. Infect. Drug Resist. 2020, 13, 799–804. [Google Scholar] [CrossRef]
- Shamina, O.V.; Kryzhanovskaya, O.A.; Lazareva, A.V.; Alyabieva, N.M.; Polikarpova, S.V.; Karaseva, O.V.; Mayanskiy, N.A. Emergence of a ST307 clone carrying a novel insertion element MITEKpn1 in the mgrB gene among carbapenem-resistant Klebsiella pneumoniae from Moscow, Russia. Int. J. Antimicrob. Agents 2020, 55. [Google Scholar] [CrossRef]
- Sękowska, A.; Chudy, M.; Gospodarek-Komkowska, E. Emergence of colistin-resistant Klebsiella pneumoniae in Poland. Acta Microbiol. Immunol. Hung. 2020, 67, 18–22. [Google Scholar] [CrossRef]
- Naha, S.; Sands, K.; Mukherjee, S.; Roy, C.; Rameez, M.J.; Saha, B.; Dutta, S.; Walsh, T.R.; Basu, S. KPC-2-producing Klebsiella pneumoniae ST147 in a neonatal unit: Clonal isolates with differences in colistin susceptibility attributed to AcrAB-TolC pump. Int. J. Antimicrob. Agents 2020, 55. [Google Scholar] [CrossRef] [PubMed]
- Gentile, B.; Grottola, A.; Orlando, G.; Serpini, G.F.; Venturelli, C.; Meschiari, M.; Anselmo, A.; Fillo, S.; Fortunato, A.; Lista, F.; et al. A retrospective whole-genome sequencing analysis of carbapenem and colistin-resistant Klebsiella pneumoniae nosocomial strains isolated during an MDR surveillance program. Antibiotics 2020, 9, 246. [Google Scholar] [CrossRef] [PubMed]
- Fournier, C.; Aires-de-Sousa, M.; Nordmann, P.; Poirel, L. Occurrence of CTX-M-15- and MCR-1-producing Enterobacterales in pigs in Portugal: Evidence of direct links with antibiotic selective pressure. Int. J. Antimicrob. Agents 2020, 55. [Google Scholar] [CrossRef] [PubMed]
- D’Onofrio, V.; Conzemius, R.; Varda-Brkić, D.; Bogdan, M.; Grisold, A.; Gyssens, I.C.; Bedenić, B.; Barišić, I. Epidemiology of colistin-resistant, carbapenemase-producing Enterobacteriaceae and Acinetobacter baumannii in Croatia. Infect. Genet. Evol. 2020, 81. [Google Scholar] [CrossRef]
- Shen, Y.; Lv, Z.; Yang, L.; Liu, D.; Ou, Y.; Xu, C.; Liu, W.; Yuan, D.; Hao, Y.; He, J.; et al. Integrated aquaculture contributes to the transfer of mcr-1 between animals and humans via the aquaculture supply chain. Environ. Int. 2019, 130. [Google Scholar] [CrossRef]
- Rodrigues, A.C.S.; Santos, I.C.D.O.; Campos, C.C.; Rezende, I.N.; Ferreira, Y.M.; Chaves, C.E.V.; Rocha-De-Souza, C.M.; Carvalho-Assef, A.P.D.; Chang, M.R. Non-clonal occurrence of pmrb mutations associated with polymyxin resistance in carbapenem-resistant Klebsiella pneumoniae in Brazil. Mem. Inst. Oswaldo Cruz 2019, 114. [Google Scholar] [CrossRef]
- Perdigão Neto, L.V.; Corscadden, L.; Martins, R.C.R.; Nagano, D.S.; Cunha, M.P.V.; Neves, P.R.; Franco, L.A.M.; Moura, M.L.N.; Rizek, C.F.; Guimarães, T.; et al. Simultaneous colonization by Escherichia coli and Klebsiella pneumoniae harboring mcr-1 in Brazil. Infection 2019, 47, 661–664. [Google Scholar] [CrossRef]
- Le, L.; Tran, L.K.; Le-Ha, T.D.; Tran, B.P.; Le-Vo, H.N.; Nguyen, Y.N.; Nguyen, H.L.; Hoang-Ngoc, K.Q.; Matsumoto, Y.; Motooka, D.; et al. Coexistence Of plasmid-mediated mcr-1 And blaNDM-4 genes in a Klebsiella pneumoniae clinical strain in Vietnam. Infect. Drug Resist. 2019, 12, 3703–3707. [Google Scholar] [CrossRef] [PubMed]
- Gelbíčová, T.; Baráková, A.; Florianová, M.; Jamborová, I.; Zelendová, M.; Pospíšilová, L.; Koláčková, I.; Karpíšková, R. Dissemination and Comparison of Genetic Determinants of mcr-Mediated Colistin Resistance in Enterobacteriaceae via Retailed Raw Meat Products. Front. Microbiol. 2019, 10. [Google Scholar] [CrossRef]
- Di Tella, D.; Tamburro, M.; Guerrizio, G.; Fanelli, I.; Sammarco, M.L.; Ripabelli, G. Molecular epidemiological insights into colistin-resistant and carbapenemases-producing clinical Klebsiella pneumoniae isolates. Infect. Drug Resist. 2019, 12, 3783–3795. [Google Scholar] [CrossRef] [PubMed]
- Borsa, B.A.; Demirci, M.; Gungordu-Dalar, Z.; Karabiyik, G.; Aygun, G.; Kucukbasmaci, O. Molecular mechanisms of colistin resistance among Klebsiella pneumoniae strains. Clin. Lab. 2019, 65, 1125–1130. [Google Scholar] [CrossRef]
- Poirel, L.; Aires-de-Sousa, M.; Kudyba, P.; Kieffer, N.; Nordmann, P. Screening and characterization of multidrug-resistant gram-negative bacteria from a remote African Area, São Tomé and Príncipe. Antimicrob. Agents Chemother. 2018, 62. [Google Scholar] [CrossRef]
- Lin, J.; Hou, Y.; Lu, H.; Cao, J.; Chen, L.; Sun, Y.; Zhou, T. Molecular mechanism of colistin resistance in Klebsiella pneumoniae. Chin. J. Microbiol. Immunol. 2018, 38, 605–610. [Google Scholar] [CrossRef]
- Ruan, Z.; Wu, J.; Chen, H.; Draz, M.S.; Xu, J.; He, F. Hybrid genome assembly and annotation of a pandrug-resistant Klebsiella pneumoniae strain using nanopore and illumina sequencing. Infect. Drug Resist. 2020, 13, 199–206. [Google Scholar] [CrossRef]
- Nishida, S.; Ono, Y. Genomic analysis of a pan-resistant Klebsiella pneumoniae sequence type 11 identified in Japan in 2016. Int. J. Antimicrob. Agents 2020, 55. [Google Scholar] [CrossRef] [PubMed]
- Nawfal Dagher, T.; Al-Bayssari, C.; Chabou, S.; Baron, S.; Hadjadj, L.; Diene, S.M.; Azar, E.; Rolain, J.M. Intestinal carriage of colistin-resistant Enterobacteriaceae at Saint Georges Hospital in Lebanon. J. Glob. Antimicrob. Resist. 2020, 21, 386–390. [Google Scholar] [CrossRef] [PubMed]
- Cheong, H.S.; Kim, S.Y.; Seo, J.; Wi, Y.M.; Peck, K.R.; Ko, K.S. Colistin resistance and extensive genetic variations in pmrab and phopq in Klebsiella pneumoniae isolates from south korea. Curr. Microbiol. 2020, 77, 2307–2311. [Google Scholar] [CrossRef]
- Yousfi, H.; Hadjadj, L.; Dandachi, I.; Lalaoui, R.; Merah, A.; Amoura, K.; Dahi, A.; Dekhil, M.; Messalhi, N.; Diene, S.M.; et al. Colistin- and carbapenem-resistant Klebsiella pneumoniae clinical_isolates: Algeria. Microb. Drug Resist. 2019, 25, 258–263. [Google Scholar] [CrossRef] [PubMed]
- Sun, Q.; Wang, Y.; Dong, N.; Shen, L.; Zhou, H.; Hu, Y.; Gu, D.; Chen, S.; Zhang, R.; Ji, Q. Application of CRISPR/Cas9-based genome editing in studying the mechanism of pandrug resistance in Klebsiella pneumoniae. Antimicrob. Agents Chemother. 2019, 63. [Google Scholar] [CrossRef]
- Sun, L.; Rasmussen, P.K.; Bai, Y.; Chen, X.; Cai, T.; Wang, J.; Guo, X.; Xie, Z.; Ding, X.; Niu, L.; et al. Proteomic Changes of Klebsiella pneumoniae in Response to Colistin Treatment and crrB Mutation-Mediated Colistin Resistance. Antimicrob. Agents Chemother. 2020, 64. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.H.; Lin, T.L.; Lin, Y.T.; Wang, J.T. A putative RND-type efflux pump, H239_3064, contributes to colistin resistance through CrrB in Klebsiella pneumoniae. J. Antimicrob. Chemother. 2018, 73, 1509–1516. [Google Scholar] [CrossRef] [PubMed]
- Castanheira, M.; Deshpande, L.M.; Mills, J.C.; Jones, R.N.; Soave, R.; Jenkins, S.G.; Schuetz, A.N. Klebsiella pneumoniae isolate from a New York city hospital belonging to sequence type 258 and carrying blaKPC-2 and blaVIM-4. Antimicrob. Agents Chemother. 2016, 60, 1924–1927. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Srinivasan, V.B.; Rajamohan, G. KpnEF, a new member of the Klebsiella pneumoniae cell envelope stress response regulon, is an SMR-type efflux pump involved in broad-spectrum antimicrobial resistance. Antimicrob. Agents Chemother. 2013, 57, 4449–4462. [Google Scholar] [CrossRef]
- Parisi, S.G.; Bartolini, A.; Santacatterina, E.; Castellani, E.; Ghirardo, R.; Berto, A.; Franchin, E.; Menegotto, N.; De Canale, E.; Tommasini, T.; et al. Prevalence of Klebsiella pneumoniae strains producing carbapenemases and increase of resistance to colistin in an Italian teaching hospital from January 2012 To December 2014. BMC Infect. Dis. 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Prim, N.; Turbau, M.; Rivera, A.; Rodríguez-Navarro, J.; Coll, P.; Mirelis, B. Prevalence of colistin resistance in clinical isolates of Enterobacteriaceae: A four-year cross-sectional study. J. Infect. 2017, 75, 493–498. [Google Scholar] [CrossRef]
- Gales, A.C.; Jones, R.N.; Sader, H.S. Contemporary activity of colistin and polymyxin B against a worldwide collection of Gram-negative pathogens: Results from the SENTRY Antimicrobial Surveillance Program (2006–09). J. Antimicrob. Chemother. 2011, 66, 2070–2074. [Google Scholar] [CrossRef]
- Wang, X.; Liu, Y.; Qi, X.; Wang, R.; Jin, L.; Zhao, M.; Zhang, Y.; Wang, Q.; Chen, H.; Wang, H. Molecular epidemiology of colistin-resistant Enterobacteriaceae in inpatient and avian isolates from China: High prevalence of mcr-negative Klebsiella pneumoniae. Int. J. Antimicrob. Agents 2017, 50, 536–541. [Google Scholar] [CrossRef]
- Wang, R.; Liu, Y.; Zhang, Q.; Jin, L.; Wang, Q.; Zhang, Y.; Wang, X.; Hu, M.; Li, L.; Qi, J. The prevalence of colistin resistance in Escherichia coli and Klebsiella pneumoniae isolated from food animals in China: Coexistence of mcr-1 and blaNDM with low fitness cost. Int. J. Antimicrob. Agents 2018, 51, 739–744. [Google Scholar] [CrossRef]
- Pishnian, Z.; Haeili, M.; Feizi, A. Prevalence and molecular determinants of colistin resistance among commensal Enterobacteriaceae isolated from poultry in northwest of Iran. Gut Pathog. 2019, 11. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.; Feng, Y.; McNally, A.; Zong, Z. The occurence of colistin-resistant hypervirulent klebsiellapneumoniae in china. Front. Microbiol. 2018, 9, 2568. [Google Scholar] [CrossRef] [PubMed]
- WHO. Antimicrobial Resistance: Global Surveillance Report, 2014; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- Li, Y.; Dai, X.; Zeng, J.; Gao, Y.; Zhang, Z.; Zhang, L. characterization of the global distribution and diversified plasmid reservoirs of the colistin resistance gene mcr-9. Sci. Rep. 2020, 10, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Sweileh, W.M. Global research output on HIV/AIDS–related medication adherence from 1980 to 2017. BMC Health Serv. Res. 2018, 18, 765. [Google Scholar] [CrossRef]
- Paczosa, M.K.; Mecsas, J. Klebsiella pneumoniae: Going on the offense with a strong defense. Microbiol. Mol. Biol. Rev. 2016, 80, 629–661. [Google Scholar] [CrossRef] [PubMed]
- Ontong, J.C.; Ozioma, N.F.; Voravuthikunchai, S.P.; Chusri, S. Synergistic antibacterial effects of colistin in combination with aminoglycoside, carbapenems, cephalosporins, fluoroquinolones, tetracyclines, fosfomycin, and piperacillin on multidrug resistant Klebsiella pneumoniae isolates. PLoS ONE 2021, 16, e0244673. [Google Scholar] [CrossRef]
- Antoniadou, A.; Kontopidou, F.; Poulakou, G.; Koratzanis, E.; Galani, I.; Papadomichelakis, E.; Kopterides, P.; Souli, M.; Armaganidis, A.; Giamarellou, H. Colistin-resistant isolates of Klebsiella pneumoniae emerging in intensive care unit patients: First report of a multiclonal cluster. J. Antimicrob. Chemother. 2007, 59, 786–790. [Google Scholar] [CrossRef]
- The Review on Antimicrobial Resistance. Final Report. Chaired by Jim O’Neill, December 2014. Available online: http://amr-review.org/Publicatio (accessed on 16 June 2021).
- Van Boeckel, T.P.; Pires, J.; Silvester, R.; Zhao, C.; Song, J.; Criscuolo, N.G.; Gilbert, M.; Bonhoeffer, S.; Laxminarayan, R. Global trends in antimicrobial resistance in animals in low-and middle-income countries. Science 2019, 365. [Google Scholar] [CrossRef]
- Sweileh, W.M. A bibliometric analysis of global research output on health and human rights (1900–2017). Glob. Health Res. Policy 2018, 3, 30. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.; Zhu, D.; Wang, F.; Wang, M. Current status and trends of antibacterial resistance in China. Clin. Infect. Dis. 2018, 67, S128–S134. [Google Scholar] [CrossRef]
- Yataganbaba, A.; Ozkahraman, B.; Kurtbas, I. Worldwide trends on encapsulation of phase change materials: A bibliometric analysis (1990–2015). Appl. Energy 2017, 185, 720–731. [Google Scholar] [CrossRef]
- Sa’ed, H.Z.; Waring, W.S.; Al-Jabi, S.W.; Sweileh, W.M. Global cocaine intoxication research trends during 1975–2015: A bibliometric analysis of Web of Science publications. Subst. Abus. Treat. Prev. Policy 2017, 12, 1–15. [Google Scholar]
- Omoregbe, O.; Mustapha, A.N.; Steinberger-Wilckens, R.; El-Kharouf, A.; Onyeaka, H. Carbon capture technologies for climate change mitigation: A bibliometric analysis of the scientific discourse during 1998–2018. Energy Rep. 2020, 6, 1200–1212. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Group, P. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e100009. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).