Infected with Scabies Again? Focus in Management in Long-Term Care Facilities
Abstract
1. Introduction
1.1. Epidemiology
1.2. Transmission
1.3. Parasite Lifecycle and Incubation Period
2. Clinical Presentation
2.1. Distribution of Rash
2.2. Host Immune Response
2.3. Complications
3. Diagnosis
Differential Diagnoses
4. Management
4.1. Principles of Treatment
4.2. Topical and Oral Agents
4.3. Drug Resistance and Other Treatments
4.4. Environmental Disinfestation
4.5. Management of Complications or Treatment Failure
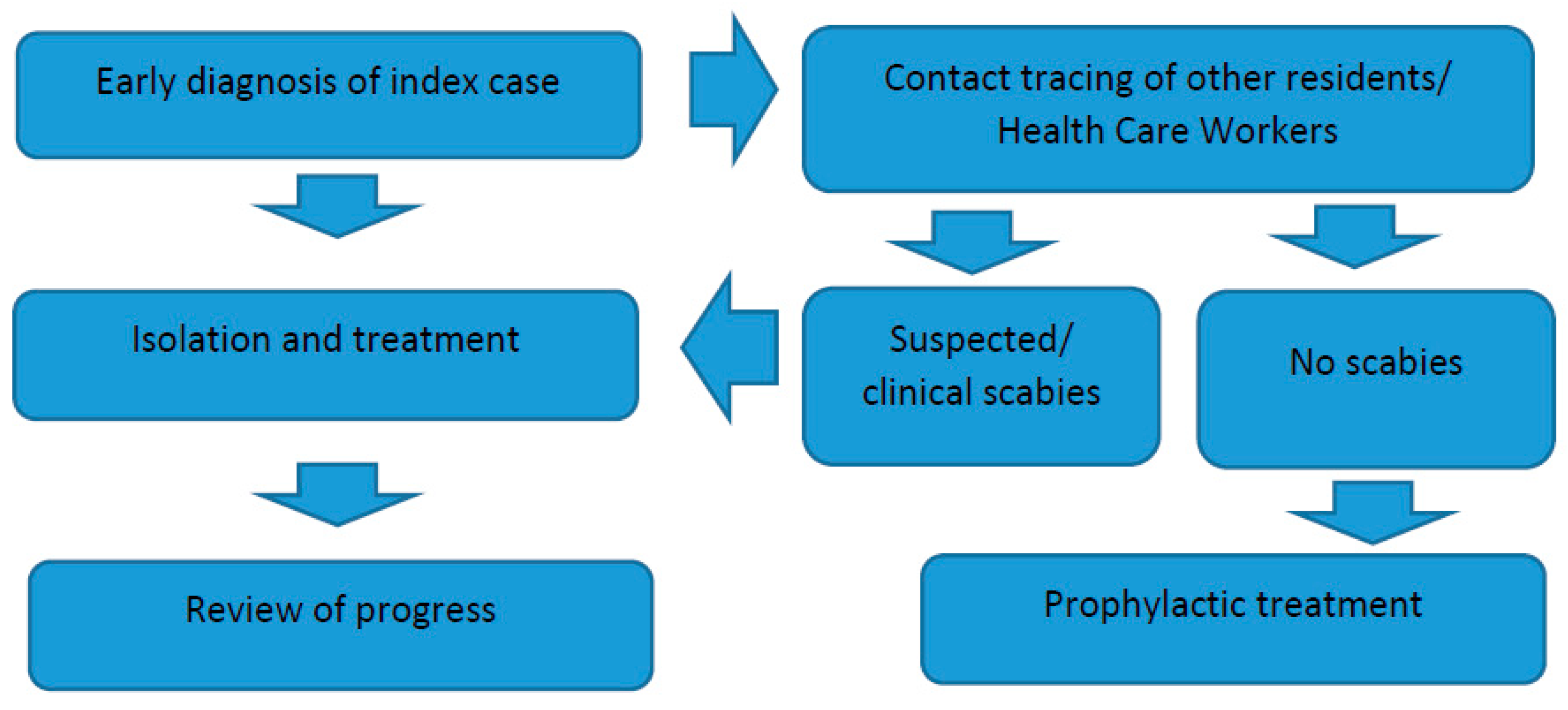
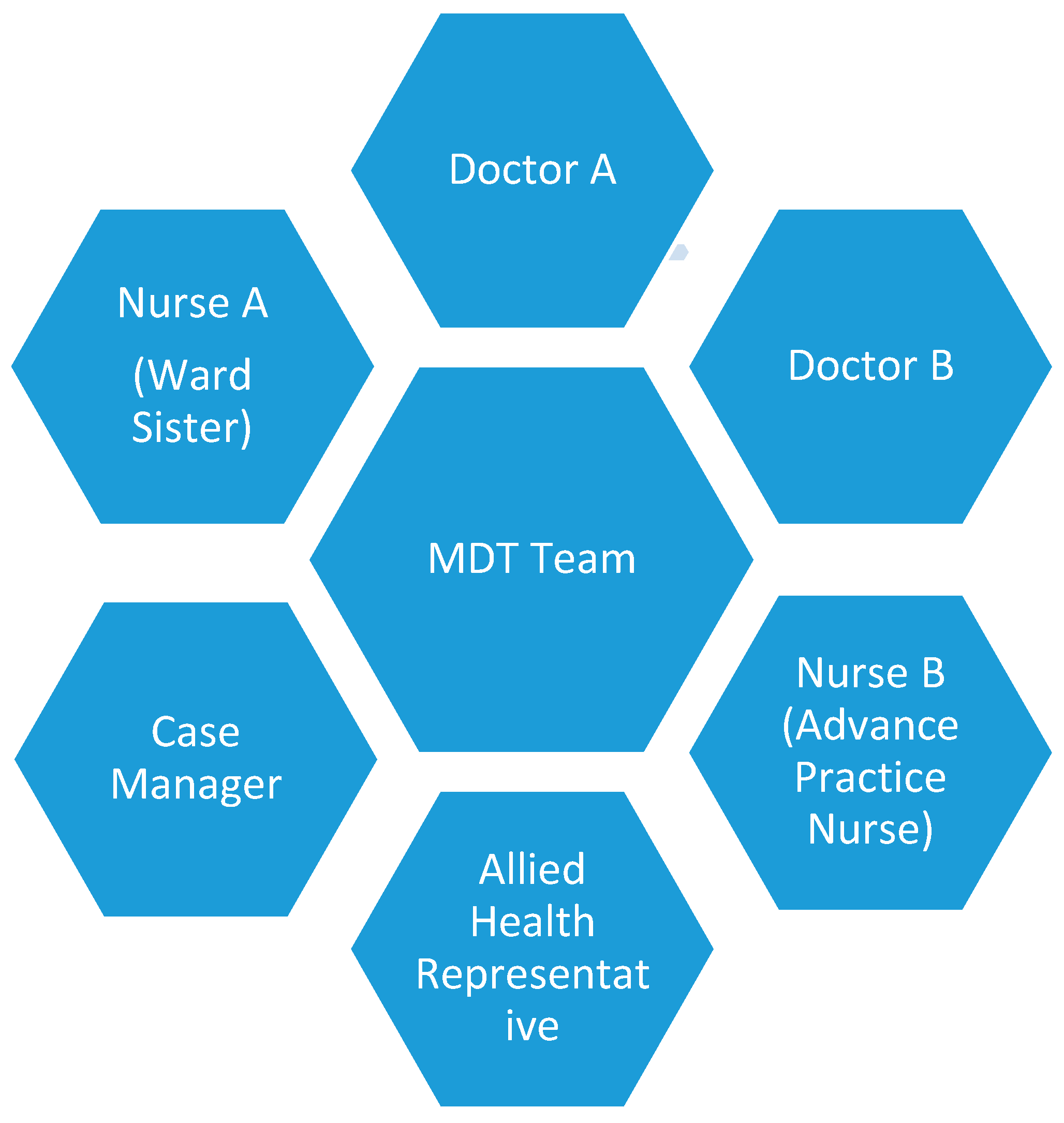
4.6. Management of Outbreak and Prevention Program
4.7. Contact Tracing
5. Recommendations
Author Contributions
Funding
Conflicts of Interest
References
- Ramos-e-Silva, M. Giovan Cosimo Bonomo (1663–1696): Discoverer of the etiology of scabies. Int. J. Derm. 1998, 37, 625–630. [Google Scholar] [CrossRef] [PubMed]
- Hengge, U.R.; Currie, B.J.; Jäger, G.; Lupi, O.; Schwartz, R.A. Scabies: A ubiquitous neglected skin disease. Lancet Infect. Dis. 2006, 6, 769–779. [Google Scholar] [CrossRef]
- Walton, S.F.; Currie, B.J. Problems in diagnosing scabies, a global disease in human and animal Populations. Clin. Microbiol. Rev. 2007, 20, 268–279. [Google Scholar] [CrossRef]
- Heukelbach, J.; Feldmeier, H. Scabies. Lancet 2006, 367, 1767–1774. [Google Scholar] [CrossRef]
- Currie, B.J.; Connors, C.M.; Krause, V.L. Scabies programs in aboriginal communities. Med. J. Aust. 1994, 161, 636. [Google Scholar]
- Heukelbach, J.; Wilcke, T.; Winter, B.; Feldmeier, H. Epidemiology and morbidity of scabies and pediculosis capitis in resource-poor communities in Brazil. Br. J. Derm. 2005, 153, 150–156. [Google Scholar] [CrossRef] [PubMed]
- Holness, D.L.; DeKoven, J.G.; Nethercott, J.R. Scabies in chronic health care institutions. Arch. Dermatol. 1992, 128, 1257–1260. [Google Scholar] [CrossRef]
- Parish, L.C.; Witkowski, J.A.; Mililikan, L.E. Scabies in extended care facility. Int. J. Dermatol. 1991, 30, 703–706. [Google Scholar] [CrossRef]
- Cassell, J.A.; Middleton, J.; Nalabanda, A.; Lanza, S.; Head, M.G.; Bostock, J. Scabies outbreaks in ten care homes for elderly people: A prospective study of clinical features, epidemiology, and treatment outcomes. Lancet Infect. Dis. 2018, 18, 894–902. [Google Scholar] [CrossRef]
- Romani, L.; Whitefield, M.J.; Koroivueta, J.; Kama, M.; Wand, H.; Tikoduadua, L. Mass Drug Administration for Scabies Control in a Population with Endemic Disease. N. Engl. J. Med. 2015, 37, 2305–2313. [Google Scholar] [CrossRef]
- Karimkhani, C.; Colombara, D.V.; Drucker, A.M.; Norton, S.A.; Hay, R.; Engelman, D. Article The global burden of scabies: A cross-sectional analysis from the Global Burden of Disease Study 2015. Lancet Infect. 2015, 17, 1247–1254. [Google Scholar] [CrossRef]
- Mounsey, K.E.; Murray, H.C.; King, M.; Oprescu, F. Retrospective analysis of institutional scabies outbreak from 1984 to 2013: Lessons learned and moving forward. Epidemiol. Infect. 2016, 144, 2462–2471. [Google Scholar] [CrossRef]
- White, L.C.J.; Lanza, S.; Middleton, J.; Hewitt, K. The management of scabies outbreaks in residential care facilities for the elderly in England: A review of current health protection guidelines. Epidemiol. Infect. 2016, 144, 3121–3130. [Google Scholar] [CrossRef] [PubMed]
- Bouvresse, S.; Chosidow, O. Scabies in healthcare settings. Curr. Opin. Infect. Dis. 2010, 23, 111–118. [Google Scholar] [CrossRef] [PubMed]
- Utsumi, M.; Makimoto, K.; Quroshi, N.; Ashida, N. Types of infectious outbreaks and their impact in elderly care facilities: A review of the literature. Age Ageing 2010, 3, 299–305. [Google Scholar] [CrossRef] [PubMed]
- Currie, B.J.; McCarthy, J.S. Permethrin and Ivermectin for Scabies. N. Engl. J. Med. 2010, 362, 717–725. [Google Scholar] [CrossRef]
- Mellanby, K. Transmission of scabies. Br. Med. J. 1941, 2, 405–406. [Google Scholar] [CrossRef]
- Mellanby, K. The development of symptoms, parasitic infection and immunity in human scabies. Parasitology 1944, 35, 197–206. [Google Scholar] [CrossRef]
- Health Protection Programs and the Communicable Disease Control Branch; Department of Health and Ageing SA. Scabies Management in Care Facilities, 2012: Management Guidelines for the Control of Scabies in Health and Residential Care Facilities; Department for Health and Ageing, Government of South Australia: Adelaide, Australia, 2012.
- Green, M. Epidemiology of scabies. Epidemiol. Rev. 1989, 11, 126–150. [Google Scholar] [CrossRef]
- Arlian, L.G.; Morgan, M.S. A review of Sarcoptes scabiei: Past, present and future. Parasit. Vectors 2017, 10, 297. [Google Scholar] [CrossRef]
- Haag, M.; Brozena, S.; Fenske, N.A. Attack of the scabies: What to do when an outbreak occurs. Geriatrics 1993, 48, 45–46. [Google Scholar] [PubMed]
- Sterling, G.; Jamiger, C.; Kihiczak, G.; Schwartz, R.; Fox, M. Scabies. Am. Fam. Physician 1992, 46, 1237–1241. [Google Scholar]
- Chosidow, O. Scabies. N. Engl. J. Med. 2006, 354, 1718–1727. [Google Scholar] [CrossRef] [PubMed]
- Hewitt, K.; England, P.H.; Nalabanda, A.; Cassell, J. Scabies outbreaks in residential care homes: Factors associated with late recognition, burden and impact. A mixed methods study in England Scabies outbreaks in residential care homes: Factors associated with late recognition, burden and impact. A mixed methods study in England. Epidemiol. Infect. 2015, 143, 1542–1551. [Google Scholar] [CrossRef] [PubMed]
- Tsutsumi, M.; Nishiura, H.; Kobayashi, T. Dementia-specific risks of scabies: Retrospective epidemiologic analysis of an unveiled nosocomial outbreak in Japan from 1989–90. BMC Infect. 2005, 5, 85. [Google Scholar] [CrossRef] [PubMed]
- Currie, B.J.; Huffam, S.; O’Brien, D.; Walton, S. Ivermectin for scabies. Lancet 1997, 350, 1551. [Google Scholar] [CrossRef]
- Cestari, T.F.; Martignago, B.F. Scabies, pediculosis, bedbugs, and stinkbugs: Uncommon presentations. Clin. Derm. 2005, 23, 545–554. [Google Scholar] [CrossRef]
- Chosidow, O. Scabies and pediculosis. Lancet 2000, 355, 819–826. [Google Scholar] [CrossRef]
- Elosua-González, M.; García-Zamora, E. Crusted scabies. N. Eng. J. Med. 2017, 377, 476. [Google Scholar] [CrossRef]
- Lanza, S.; Middleton, J.; Head, M.G.; Bostock, J.; Nalabanda, A.; Walker, S.L. Can outbreak research be achieved in a population with impaired capacity? Findings from a study of a scabies outbreak in residential care. Lancet 2015, 386, S48. [Google Scholar] [CrossRef]
- Sirera, G.; Romeu, J.; Ribera, M.; Tor, J.; Rius, F.; Llibre, J.M.; Soriano, V.; Ferrandiz, C.; Clotet, B. Hospital outbreak of scabies stemming from two AIDS patients with Norwegian scabies. Lancet 1990, 335, 1227. [Google Scholar] [CrossRef]
- Estes, S.A.; Estes, J. Scabies research: Another dimension. Semin. Dermatol. 1993, 12, 34–38. [Google Scholar] [PubMed]
- Esposito, L.; Veraldi, S. Skin bactrerial colonizations and superinfections in immunocompetent patients with scabies. Int. J. Dermatol. 2018, 57, 1218–1220. [Google Scholar] [CrossRef] [PubMed]
- Hersch, C. Acute glomerulonephritis due to skin disease, with special reference to scabies. S. Afr. Med. J. 1967, 41, 29–34. [Google Scholar] [PubMed]
- Woodley, D.; Saurat, J.H. The burrow ink test and the scabies mite. J. Am. Acad. Dermatol. 1981, 4, 715–722. [Google Scholar] [CrossRef]
- Micali, G.; Lacarrubba, F.L.G.G. Scraping versus videodermatoscopy for the diagnosis of scabies: A comparative study. Acta Dermatol. Venereol. 1999, 79, 396. [Google Scholar]
- Leung, V.; Miller, M. Detection of scbies: A systematic review of diagnostic methods. Can. J. Infect. Dis. Med. Microbiol. 2011, 22, 143–146. [Google Scholar] [CrossRef] [PubMed]
- Dupuy, A.; Dehen, L.; Bourrat, E.; Lacroix, C.; Benderdouche, M.; Dubertret, L. Accuracy of standard dermoscopy for diagnosing scabies. J. Am. Acad. Dermatol. 2007, 56, 53–62. [Google Scholar] [CrossRef] [PubMed]
- Argenziano, G.; Fabbrocini, G.; Delfino, M. Epiluminescence microscopy. A new approach to in vivo detection of Sarcoptes scabies. Arch. Dermatol. 1997, 133, 751–753. [Google Scholar] [CrossRef]
- Brunetti, B.; Vitiello, A.; Delfino, S.; Sammarcco, E. Findings of in vivo of Sarcoptes scabiei with inident light microscopy. Eur. J. Dermatol. 1998, 8, 266–267. [Google Scholar]
- Bauer, J.; Blum, A.; Sonnichsen, K.; Metzler, G.; Rassner, G.; Garbe, C. Nodular scabies detected by computed dermatoscopy. Dermatology 2001, 203, 190–191. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, C.; Lucius, R.; Matthes, H.F.; Meuseul, G.; Reich, B.; Kalinna, B.H. Characterisation of recombinant immunreactive antigens of the scab mite Sarcoptes scabiei. Vet. Parasitol. 2008, 153, 329–337. [Google Scholar] [CrossRef] [PubMed]
- Casais, R.; Prieto, M.; Balseiro, A.; Solano, P.; Parra, F.; Martin Alonso, J.M. Identification and heterologous expression of a Sarcoptes scabiei cDNA encoding a structural antigen with immunodiagnostic potential. Vet. Res. 2007, 38, 435–450. [Google Scholar] [CrossRef] [PubMed]
- Alasaaad, S.; Rossi, L.; Soriguer, R.C.; Rambozzi, L.; Soglia, D.; Perez, J.M. Sarcoptes mite from collection to DNA extraction: The lost realm of the neglected parasite. Parasitol. Res. 2009, 104, 723–732. [Google Scholar] [CrossRef] [PubMed]
- Engelman, D.; Fuller, L.C.; Steer, A.C. Consensus criteria for the diagnosis of scabies: A Delphi study of international experts. PLoS Negl. Trop. Dis. 2018, 12, e0006549. [Google Scholar] [CrossRef] [PubMed]
- Andersen, B.M.; Haugen, H.; Rasch, M.; Haugen, A.H.; Tageson, A. Outbreak of scabies in Norwegian nursing homes and home care patients: Control and prevention. J. Hosp. Infect. 2000, 160–164. [Google Scholar] [CrossRef] [PubMed]
- Fitzgerald, D.; Grainger, R.J.; Reid, A. Interventions for preventing the spread of infestation in close contacts of people with scabies (Review). Cochrane Database Syst. Rev. 2014. [Google Scholar] [CrossRef] [PubMed]
- Chouela, E.; Abeldano, A.; Pellerano, G.; Hernandez, M.I. Diagnosis and treatment of scabies. Am. J. Clin. Dermatol. 2002, 3, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Schienfield, N. Controlling scabies in institutional settings: A review of medication, treatment models, and implementation. Am. J. Clin. Dermatol. 2004, 5, 31–37. [Google Scholar] [CrossRef] [PubMed]
- Strong, M.; Johnstone, P. Interventions for treating scabies (Review). Cochrane Database Syst. Rev. 2010, 3, CD000320. [Google Scholar]
- Paasch, U.; Haustein, U.F. Management of endemic outbreaks of scabies with allethrin, permethrin, and ivermectin. Int. J. Dermatol. 2000, 39, 463–470. [Google Scholar] [CrossRef] [PubMed]
- Ladbury, G.; Morroy, G.; van Hoeven-Dekkers, S.; Bottermans, C.; Veelenturf, C.; Bastiaens, M. An outbreak of scabies in multiple limked healthcare settings in the Netherlands. Infect. Control. Hosp. Epidemiol. 2012, 33, 1047–1050. [Google Scholar] [CrossRef] [PubMed]
- Strong, M.; Johnstone, P. Cochrane review: Interventions for treating scabies. Evid.-Based Child. Health A Cochrane Rev. J. 2011, 6, 1790–1862. [Google Scholar] [CrossRef]
- Mounsey, K.E.; Holt, D.C.; McCarthy, J.S.; Currie, B.J.; Walton, S.F. Longitudinal evidence of increasing in vitro tolerance of scabies mites to ivermectin in scabies-endemic communities. Arch. Dermatol. 2009, 145, 840–841. [Google Scholar] [CrossRef] [PubMed]
- Currie, B.J.; Harumal, P.; McKinnon, M.; Walton, S.F. First documentation of in vivo and in vitro ivermectin resistance in Sarcoptes scabiei. Clin. Infect. Dis. 2004, 39, e8–e12. [Google Scholar] [CrossRef] [PubMed]
- Khalil, S.; Abbas, O.; Kibbi, A.G.; Kurban, M. Scabies in the age of increasing drug resistance. PLoS Negl. Trop. Dis. 2017, 11, e0005920. [Google Scholar] [CrossRef] [PubMed]
- Thomas, J.; Peterson, G.M.; Walton, S.F.; Carson, C.F.; Naunton, M.; Baby, K.E. Scabies: An ancient global disease with a need for new therapies. BMC Infect Dis. 2015, 15, 250. [Google Scholar] [CrossRef]
- Roth, W. Scabies resistant to lindane 1% lotion and crotamiton 10% cream. J. Am. Acad. Dermatol. 1991, 24, 502–503. [Google Scholar] [CrossRef]
- Mounsey, K.E.; Walton, S.F.; Innes, A.; Cash-deans SMcCarthy, J.S. In Vitro Efficacy of Moxidectin versus Ivermectin against Sarcoptes scabiei. Antimicrob. Agents Chemother. 2017, 61, 1–5. [Google Scholar] [CrossRef]
- Mounsey, K.E.; Bernigaud, C.; Chosidow, O.; Mccarthy, J.S. Prospects for Moxidectin as a New Oral Treatment for Human Scabies. PLoS Negl. Trop. Dis. 2016, e0004389. [Google Scholar] [CrossRef]
- Bernigaud, C.; Fang, F.; Fischer, K.; Lespine, A.; Aho, S.; Dreau, D. Preclinical Study of Single-Dose Moxidectin, a New Oral Treatment for Scabies: Efficacy, Safety, and Pharmacokinetics Compared to Two-Dose Ivermectin in a Porcine Model. PLoS Negl. Trop. Dis. 2016, 10, e0005030. [Google Scholar] [CrossRef] [PubMed]
- Bhunu, C.P.; Mushayabasa, S.; Monera, T.G. Assessing the Impact of Vaccination on Controlling the Spread of Human Scabies. ISRN Comput. Bio. 2013, 2013, 362973. [Google Scholar] [CrossRef]
- Liu, X.; Walton, S.; Mounsey, K. Vaccine against scabies: Necessity and possibility. Parasitology 2014, 141, 725–732. [Google Scholar] [CrossRef] [PubMed]
- Karthikeyan, K. Treatment of scabies: Newer perspectives. Postgrad. Med. J. 2005, 81, 7–11. [Google Scholar] [CrossRef] [PubMed]
- Wilson, M.G.; Philpott, C.D.; Breer, W.A. Atypical Presentation of Scabies Among Nursing Home Residents. J. Gerentol. Ser. A Biol. Sci. Med. Sci. 2001, 56, 424–427. [Google Scholar] [CrossRef]
- Stoevesandt, J.; Carle, L.; Leverkus, M.; Hamm, H. Control of large istitutional settings: A review of medication, treatment models, and implementation. J. Dtsch. Dermatol. Ges. 2012, 10, 637–647. [Google Scholar] [CrossRef]
- Sunderkötter, C.; Feldmeier, H.; Fölster-Holst, R.; Geisel, B.; Klinke-Rehbein, S.; Nast, A. S1 guidelines on the diagnosis and treatment of scabies–short version. JDDG 2016, 14, 1155–1167. [Google Scholar] [CrossRef]
- Buehlmann, M.; Beltraminelli, H.; Strub, C.; Bircher, A.; Jordan, X.; Battegay, M. Scabies outbreak in an intensive care unit with 1,659 exposed individuals- key factors for controlling the outbreak. Infect. Control. Hosp. Epidemiol. 2009, 30, 354–360. [Google Scholar] [CrossRef]
- Ejidokun, O.O.; Aruna, O.S.; O’Neill, B. A scabies outbreak in a further education college in Glouchestershire. Epidemiol. Infect. 2007, 135, 455–457. [Google Scholar] [CrossRef]
- Vorou, R.; Remoudaki, H.D.; Maltezou, H.C. Nosocomial scabies. J. Hosp. Infect. 2007, 65, 9–14. [Google Scholar] [CrossRef]
- California Department of Public Health. Prevention and Control Long-Term Care Facilities; California Department of Public Health: Sacramento, CA, USA, 2008.
- Jimenez-Lucho, V.E.; Fallon, F.; Caputo, C.; Ramsey, K. Role of prolonged surveillance in the eradication of nosocomial scabies in an extended care Veterans Affairs medical center. Am. J. Infect. Control. 1995, 23, 44–49. [Google Scholar] [CrossRef]
- Yonkosky, D.; Ladia, L.; Gackenheimer, L.; Schultz, M.W.; Marlborough, M.P.H. Scabies in nursing homes: An eradication program with permethrin 5 % cream. J. Am. Acad. Dermatol. 1990, 23, 1133–1136. [Google Scholar] [CrossRef]
- Khan, A.; O’ Grady, S.; Muller, M.P. Rapid control of a scabies outbreak at a tertiary care hospital without ward closure. Am. J. Infect. Control. 2012, 40, 451–455. [Google Scholar] [CrossRef] [PubMed]
| A: Confirmed scabies At least one of: A1: Mites, eggs, or feces on light microscopy of skin samples A2: Mites, eggs, or feces visualized on individual using high-powered imaging device A3: Mite visualized on individual using dermoscopy B: Clinical scabies At least one of: B1: Scabies burrows B2: Typical lesions affecting male genitalia B3: Typical lesions in a typical distribution and two history features C: Suspected scabies One of: C1: Typical lesions in a typical distribution and one history feature C2: Atypical lesions or atypical distribution and two history features History features H1: Itch H2: Close contact with an individual who has itch or typical lesions in a typical distribution Notes: 1. These criteria should be used in conjunction with the full explanatory notes and definitions (in preparation). 2. Diagnosis can be made at one of the three levels (A, B, or C). 3. A diagnosis of clinical and suspected scabies should only be made if other differential diagnoses are considered less likely than scabies. |
| Drug Name and Preparation | Dosage and Instruction | Major Side Effects | Notes or Contraindications |
|---|---|---|---|
| Topical | |||
| Permethrin | 5% cream. Rinse off after 8–14 h. Second application one week after the first. Crusted scabies: Apply daily for 7 days, then 2x/week until cured. Combination therapy with oral ivermectin. | Itch and sting on application. | Not to be used in infants under age two months. Can be used in infants and breastfeeding mothers. |
| Benzyl benzoate | 10–25% lotion. Rinse off after 24 h. Alternatively, apply overnight for 2 consecutive days. Second application 1 week after the first. Crusted scabies: Apply daily for 7 days, then 2x/week until cured. Combination therapy with oral ivermectin. | Burning and sting on application. | Not recommended in infants below 6 months (dilutional doses) required. Disulfiram-like effects if alcohol is consumed less than 48 h prior to application. |
| Crotamiton | 10% cream. Apply to nodules for 24 h, rinse off, and reapply for another 24 h. | None | Safety in children has not been established. |
| Precipitated sulfur | 3–6% lotion, 5–40% petrolatum. Apply for 24 h and then reapply every 24 h for the next 2 days. Alternatively, apply overnight for 3 consecutive days. | None | Inexpensive. Used in neonates, pregnant women, and breastfeeding mothers. |
| Malathion | 0.5% lotion. Rinse off after 24 h. Repeat application after one week. | Burning and sting on application. | |
| Oral | |||
| Ivermectin | 3 mg tablets. Single dose of 200 mcg/kg body weight. Second dose 2 weeks later. Crusted scabies: 200 mcg/kg/dose on days 1, 2, 8, 9, and 15. Combination use with permethrin/or benzyl benzoate. Apply for 7 days, then 2x/week until cure. | Contraindicated in children less than 15 kg or pregnant and breastfeeding mothers. Absorption can be improved with fatty meals. Care must be taken when administered with drugs that can augment GABA activity (valproate, barbiturates, and benzodiazepines). | |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ong, C.Y.; Vasanwala, F.F. Infected with Scabies Again? Focus in Management in Long-Term Care Facilities. Diseases 2019, 7, 3. https://doi.org/10.3390/diseases7010003
Ong CY, Vasanwala FF. Infected with Scabies Again? Focus in Management in Long-Term Care Facilities. Diseases. 2019; 7(1):3. https://doi.org/10.3390/diseases7010003
Chicago/Turabian StyleOng, Chong Yau, and Farhad Fakhrudin Vasanwala. 2019. "Infected with Scabies Again? Focus in Management in Long-Term Care Facilities" Diseases 7, no. 1: 3. https://doi.org/10.3390/diseases7010003
APA StyleOng, C. Y., & Vasanwala, F. F. (2019). Infected with Scabies Again? Focus in Management in Long-Term Care Facilities. Diseases, 7(1), 3. https://doi.org/10.3390/diseases7010003





