Abstract
Rutin is a well-known antioxidant from the group of flavonoids. Its use in cosmetic dermal products is, however, limited due to its poor water solubility. In order to increase rutin saturation solubility and improve the diffusion to the skin, rutin nanocrystals were produced by the smartCrystal process, e.g., bead milling followed by high pressure homogenization. Rutin nanocrystals were further incorporated into hydroxypropyl cellulose (HPC) gel and its long-term stability was assessed. Determination of the antioxidant activity was made by the DPPH (2,2-diphenyl-1-picrylhydrazyl) assay for these formulations: rutin nanocrystals (mean size 300 nm), rutin raw drug powder (mean size 33 μm) and commercial product. Furthermore, the skin penetration profile of rutin was investigated by the tape-stripping method on porcine skin. This study demonstrated that rutin nanocrystal gel had the highest neutralizing activity (90%), followed by a commercial product and rutin raw drug powder. According to the skin study, rutin nanocrystals penetrated to the deeper layers of the stratum corneum, the horny layer of the skin.
1. Introduction
The human skin is constantly and directly exposed to stressful environmental factors such as solar radiation or pollution, both of which induce the generation of aggressive free radicals as well as reactive oxygen species (ROS). Free radicals are characterized by one or more unpaired electrons and are able to enter into destructive chemical bonds with proteins of the skin, causing chemical and functional changes of the skin matrix [1]. ROS also attack and react with the skin cell molecules in the dermis, causing wrinkles due to the cross-linking of collagen and elastin [2]. In addition, it lessens the self-repair ability of the skin [3]. To a certain degree, endogenous melanin and enzymatic antioxidants are able to neutralize ROS. For prevention of oxidative stress, a term referring to the imbalance between the generation of ROS and the antioxidant defense activity [4], and to enhance the reparation of the DNA, exogenous antioxidants should be applied topically.
Flavonoids, in particular rutin, proved its pronounced antioxidant property on molecular level in several studies [5]. The exceptional antioxidant activity of rutin can be ascribed to its phenolic compound characterized by an aromatic ring linked to a hydroxyl group, which has an ability to donate electron and hydrogen [6]. Nevertheless, rutin cannot be used efficiently in dermal products because of its insufficient penetration rate into the skin. However, a pronounced penetration of the antioxidant is required, since the antioxidant has to neutralize the reaction of ROS within cell molecules located in the dermis [2]. The poor penetration of rutin into the skin is a result of its low solubility in both aqueous and organic solvents. Generally, skin penetration can by described by a passive diffusion process, which is more pronounced, the higher is the concentration gradient to the skin. Since only dissolved rutin is able to create such a concentration gradient, insufficient penetration occurs. Thus, the solubility of rutin has to be increased significantly for its efficient use as dermal antioxidant.
Nanocrystals were originally developed for oral and intravenous administration of poorly soluble drugs. Several years later, the dermal application of nanocrystals was described in a patent [7,8]. In comparison to other drug formulations (such as polymeric nanoparticles), nanocrystals are made from pure cosmetic active and do not require the use of organic solvents. Nanocrystals dermal penetration enhancement might be explained by three various effects:
- The increased saturation solubility of nanosized rutin and subsequently increased concentration gradient between dermal formulation and skin, leading to increased diffusion into the skin.
- The increased dissolution velocity caused by the large surface area of the nanocrystals.
- High adhesion to skin, as all nanosized materials are adhesive.
Due to their size in the nano-dimension, nanocrystals possess higher kinetic saturation solubility, and, in combination with the large surface, it leads to fast dissolution. These effects have already been described for rutin nanocrystals developed for oral administration [9,10]. Thus, rutin nanocrystals were produced for dermal application in this study.
The production technology employed is the smartCrystal process, a combination technology. The raw drug powder is dispersed in a surfactant solution (= macro-suspension), and then passed several times through a bead mill containing milling beads. The obtained nano-suspension is subsequently passed through a high pressure homogenizer at low pressure [9,11]. This yields a more uniform product in size with increased physical stability compared to applying a mono process, e.g., bead milling or high pressure homogenization only [7]. This is of special interest for dermal formulations, because they often contain suspension-destabilizing agents such as electrolytes or preservatives.
An increased in vivo bioactivity in the skin for rutin nanocrystals has already been observed in a human study. The subjects were irradiated after application of the two test formulations, and the increase in the sun protection factor (SPF) was determined (= measure for antioxidant activity in the skin). A formulation with water-soluble rutin derivative (glucoside) in a concentration of 5.0% versus a formulation with only 0.01% dissolved rutin from rutin nanocrystals was applied. Despite the 500 times lower dissolved concentration, the rutin nanocrystal formulation had a two-fold increased SPF [7], which in simpler terms means a 1000-fold higher bioactivity in skin.
2. Experimental Section
2.1. Materials
2,2-Diphenyl-1-picrylhydrazyl, polysorbate 80 and hydroxypropyl cellulose (HPC) were purchased from Sigma-Aldrich (St. Louis, MO, USA), Glycerol 85% was purchased from LS Labor-Service GmbH (Gründau, Germany) and euxyl® PE 9010 was purchased from Schülke & Mayr GmbH (Norderstedt, Germany). Methanol, dimethyl sulfoxide and acetonitrile were obtained from VWR International (Radnor, PA, USA) in High-Performance Liquid Chromatography (HPLC) quality. Purified water was from a Milli-Q system of Merck KGaA (Darmstadt, Germany). Rutin raw drug powder was kindly provided from PharmaSol GmbH (Berlin, Germany).
2.2. Production of Rutin Nanocrystal (smartCrystal) Suspension
The rutin nano-suspension was produced by combining wet bead milling with high pressure homogenization (HPH), the so-called smartCrystal process [7]. First, a rutin nano-suspension concentrate consisting of 18.0% rutin, 2.0% polysorbate 80, 1.0% euxyl® PE 9010 and water for injection up to 100% was prepared by wet bead milling using a PML-2 (Bühler AG, Uzwil, Switzerland) at 2000 rpm and pump capacity of 10% with 0.4–0.6 mm yttria oxide stabilized zirconium oxide beads (Hosokawa Alpine, Augsburg, Germany). This concentrate was further diluted to the final concentration of 5.0% rutin, 2.0% polysorbate 80, 5.0% glycerol 85.0%, and 1.0% euxyl® PE 9010 and processed for two cycles of HPH at 300 bar using an EmulsiFlex-C50 (Avestin Europe GmbH, Mannheim, Germany).
2.3. Production of Rutin Containing Gel Formulation
The hydrophilic gel base for rutin incorporation was prepared by dispersing 5.0% hydroxypropyl cellulose (HPC) in 85 °C hot purified water at 87.5%. Mortar and pestle were used to stir the dispersion until room temperature was reached and a homogenous gel was formed. A deficiency in weight occurs due to evaporated water. Thus, it was complemented. For the improvement of spreading properties, glycerol 85% at 2.5% was added dropwise as well as the preserving agent euxyl® PE 9010 at 1.0%. Finally, 4.0% rutin nanocrystal suspension was incorporated into the prepared gel base, corresponding to 0.2% pure rutin nanocrystals in the whole formulation (= 100%). For the production of a reference gel, identical gel base as that mentioned above was used. Instead of incorporating the rutin nano-suspension (Section 2.2), 4.0% of a rutin bulk powder suspension with identical composition as the nano-suspension (5.0% rutin, 2.0% polysorbate 80, 5.0% glycerol 85%, 1.0% euxyl® PE 9010, up to 100.0% water) was incorporated.
2.4. Characterization of Nanocrystals
2.4.1. Photon Correlation Spectroscopy (PCS)
z-averages (intensity weighted mean diameter of the bulk population) and polydispersity indices (representing the width of the size distribution) of produced nanocrystal suspensions were analyzed by PCS using a Zetasizer Nano ZS (Malvern Instruments, Worcestershire, UK). The samples were diluted (10 μL nanocrystal suspension in 5.0 mL purified water) and the mean values were calculated from 10 single measurements. To analyze the particle size of rutin incorporated into gel, 50.0 mg of the prepared rutin gel was suspended in 100 mL purified water and 1.0 mL of it was diluted with purified water up to 100 mL.
2.4.2. Laser Diffractometry (LD)
For the detection of larger particles or agglomerations outside of the PCS measurement range, LD measurements were performed using a Mastersizer 2000 (Malvern Instruments, Worcestershire, UK). As dispersion medium purified water was used. The real refractive index of rutin particles was set to 1.456 with an imaginary refractive index of 0.01. The obscuration range was set between 4% and 6% and the stirring speed to 750 rpm with no sonication. As characteristic parameters, LD volume weighted diameters LD 50%, 90% and 99% were used.
2.4.3. Light Microscopy (LM)
For fast detection of large particles and aggregates within the formulation and for the confirmation of LD data, LM was performed with an Orthoplan Leitz (Wetzlar, Germany) at magnifications of 100, 400 and 1000. For visual documentation, the microscope was connected to a digital camera CMEX 3200 (Arnhem, The Netherlands). Samples were analyzed undiluted to increase the probability of finding even a few large particles or aggregates.
2.4.4. Zeta Potential (ZP)
For the prediction of the suspension’s long-term stability, the electrophoretic mobilities of the particles were determined using a Zetasizer Nano ZS (Malvern Instruments, Worcestershire, UK). The measurement was performed in both conductivity-adjusted water (50 μS/cm with NaCl solution and pH of 5.5) and original dispersion medium. To convert the electrophoretic mobility into the zeta potential, the Helmholtz–Smoluchowski equation was applied. Measurement in conductivity-adjusted water yields the Stern potential, which is proportional to the surface charge (Nernst potential) measurement in the original dispersion medium the ZP value suitable for predicting long-term stability.
2.5. In-Vitro Antioxidant Activity
For the comparison of the antioxidant activity of the prepared rutin nanocrystal gel with rutin bulk powder gel (both described in Section 2.3), a DPPH (2,2-diphenyl-1-picrylhydrazyl) assay was performed using a methanolic DPPH solution having its absorbance adjusted at 1 by a wavelength of 517 nm (UV maximum of methanolic DPPH solution). The UV absorbance was controlled with an UV-1700 PharmaSpec (Shimadzu Deutschland GmbH, Duisburg, Germany) using optically clear cuvettes with a total volume of 4.5 mL (VWR International GmbH, Darmstadt, Germany). Samples were prepared by suspending 0.5 g of gel in 2.5 g methanol using an Edmund BühlerSwip KS-10 (Hechingen, Germany) for one hour at 20 °C and 150 rpm. With an Eppendorf Centrifuge 5451 C (Hamburg, Germany), undissolved particles were separated from supernatant, since particles can scatter UV light and thus take influence on UV measurement. Seventy-five microliters of the clear supernatant was added into a cuvette with 1.5 mL methanolic DPPH solution and the UV absorbance was measured over a time period of 60 min again at 517 nm with the PharmaSpec UV-1700. For zero adjustment, 1.5 mL methanolic DPPH solution was diluted with 75 μL Miglyol 812. The rutin nanocrystal gel was also compared with already marketed dermal products, having rutin or its water-soluble derivatives, i.e., disodium rutinyl disulfate and troxerutin, as active compound. The price of the products varied strongly from €8.00 to €220.00 (retail shop price). All samples were measured six-fold.
2.6. Ex-Vivo Penetration Study on Porcine Ear Skin
To determine the penetration profiles of the rutin nanocrystal gel and raw drug powder gel (Section 2.3), an ex vivo penetration study was performed using the tape stripping method on porcine ears directly on the day of slaughter. The fresh ears were prepared by removing the hair neatly with a scissor and cleaning the surface with purified water at 20 °C. The ears were then patted dry with a soft paper tissue. As investigation area of 2 cm × 4 cm was defined and only intact skin was used showing no injuries or other visible skin changes.
Thus, on one porcine ear, only two to maximum three investigation areas can fit, but for a sufficient explanatory power a three-fold determination and thus at least six areas were necessary. Since the porcine ears are strongly varying among each other from biological side, it was pointless to pool together penetration profiles of one formulation observed on different porcine ears. Therefore the idea was not to compare the penetration profiles directly with each other from different ears but the relation between the penetration profiles of the rutin nanocrystal and raw drug powder gel (Section 2.3) investigated on one and the same ear with the relation investigated on another ear. Thus, in this study, two investigation areas were set on one porcine ear investigating the penetration of the rutin nanocrystal gel and raw drug powder gel.
Onto one investigation area, 20 mg of gel was applied homogenously. After a penetration time of 40 min, 30 adhesive tapes (tesa Film No. 5529, Beiersdorf, Germany) were used to remove the stratum corneum layer by layer. The amount of adhering corneocytes represents the thickness of removed horny layer with the tape and was determined for a 1 cm × 1 cm area by UV analysis using a Lambda 20 (PerkinElmer, Waltham, MA, USA) at a wavelength of 800 nm. Afterwards, removed rutin was quantitatively extracted from the tapes having a size of 1.9 cm × 3.5 cm in 2.0 mL of acetonitrile and dimethyl sulfoxide (ration of 1:1) by shaking with an Edmund BühlerSwip KS-10 (Hechingen, Germany) for 1 h at 150 rpm. The concentration of rutin was analyzed using high-performance liquid chromatography (Section 2.7). The relative amount of rutin in each tape was calculated by following equation:
2.7. High-Performance Liquid Chromatography (HPLC)
Rutin concentrations were determined using a Kroma System 2000 version 1.7 (Kontron Instruments GmbH, Augsburg, Germany) combined with a solvent delivery pump equipped (Kontron Instruments SpA, Milano, Italy) consisted of a 20 μL loop, an auto sampler model 560 and an UV detector model 430 measuring at a wavelength of 255 nm. A Eurospere® C18 RS (250 mm × 4.6 mm) was used as analytical column and acetic buffer (pH 4.8) with acetonitrile in a ratio of 8:2 (v/v) were used as solvent system. Each sample was measured in duplicate.
3. Results and Discussion
3.1. Characterization of Rutin Nanocrystal Suspension and the Nanocrystal Gel
Directly after production, the rutin nanocrystal suspension showed a mean PCS particle size of 240 nm with a polydispersity index of 0.215, consistent with the LD diameter 50% of 285 nm. A slight increase in particle size was observed after six months of storage at 25 °C ± 2 °C, where the mean particle size was 318 nm with unchanged polydispersity index and the LD diameter 50% of 311 nm. For comparison, rutin raw drug powder suspension had a LD diameter 50% of 32.2 μm, which was unchanged after six months of storage at 25 °C ± 2 °C. The PCS z-average and polydispersity index of the suspension could not been determined, since the size exceeded the measurement range of PCS. Based on these data, both suspensions on their own possessed a good physical stability, fulfilling the precondition for incorporating into a gel base.
Particle growth can be induced when incorporating the suspension into the gel base. Thus, the particle size of rutin was also investigated in the gel using PCS, LD and LM. A negligible growth of particle size from 240 nm to 282 nm was observed for rutin nanocrystals, directly after incorporating it into the gel base. The storage of this gel for three months at 25 °C ± 2 °C did not lead to further growth; thus, the nanocrystals were physically stable. Results obtained for the rutin raw drug powder also proved physical stability. After incorporation, the LD diameter 50% showed no significant change (32.2 μm before and 33.0 μm after incorporation), and remained unchanged during storage. Thus, there was no destabilizing influence of the gel base onto the particles.
3.2. Safety of Rutin and Rutin Nanocrystals in Dermal Formulations
From the Material Safety Data Sheets (MSDS), rutin as a molecule itself is declared as a save compound. Admix it into dermal formulations does not affect its safety, proven by the high number of consumer care and cosmetic products on the market (e.g., Yves Rocher–Sensitive Vegetal, La mer–MED Couperose Konzentrat Feuchtigkeitspflege, Bio Specific Active–Sensitive Augenpflege, aMENity–After Shave & Face Moisturizer). Commonly, in the marketed dermal formulations, the active rutin is either dissolved in very low concentrations or dispersed as raw drug powder. In contrast, the present formulation (Section 2.3) has rutin incorporated as nanocrystals with particle sizes still being outside the nanoparticle definition of the legal regulations of the European Cosmetic Decree. In addition to the particle size above 100 nm, the rutin nanocrystals are biodegradable and thus belong to the green class (class I) of the nanotoxicological classification system (NCS) [12] underlining the safety of rutin nanocrystal in the present formulation.
3.3. In-Vitro Antioxidant Activity
To prove that a particle size reduction of rutin into the nanometer range will increase its antioxidant activity, a DPPH assay was performed with both rutin nanocrystal gel and raw drug powder gel (Section 2.3). In addition, the results were compared with the antioxidant activities of facial cosmetic products available on the market containing rutin, one of its water-soluble derivatives or a combination of both as active ingredient.
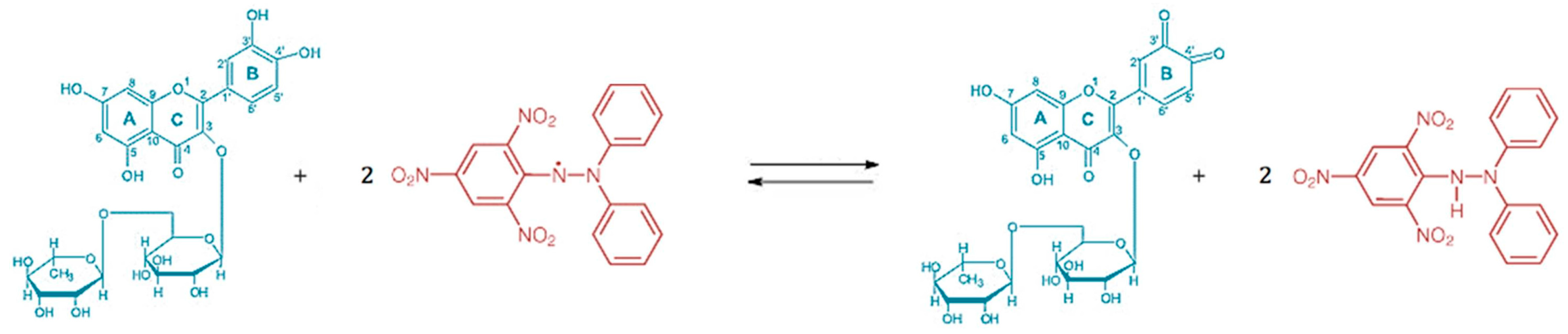
The DPPH is an exceptionally stable free radical since the spare electron is strongly delocalized over the whole molecule. Thus, the dimerization potential is significantly reduced and this property enables the DPPH radical to be used for antioxidant activity studies. Two DPPH radicals were neutralized by one molecule of rutin, which get itself oxidized at the catechol 3′,4′-dihydroxyl group (Figure 1).
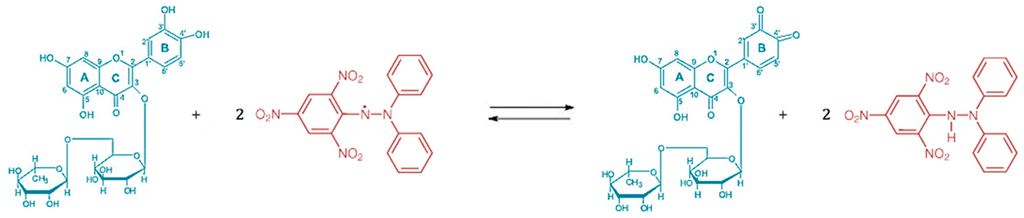
Figure 1.
Reaction equation of rutin (blue) and DPPH (red) [13].
Even if the DPPH radical shows artificially high chemical stability, reduction to DPPH-H molecules can occur during the long measurement period of 60 min by the contact with ambient air. To avoid incorrect determinations of the antioxidant activity, the reduction of the methanolic DPPH solution on ambient air was also measured and considered in the equation as A(control). The A(control) sample was prepared and treated in the same manner as the other samples. Only instead of adding 75 μL extract of product, neutral oil Miglyol 812 was used. For the conversion of investigated reduction of absorption to the inhibition of DPPH activity in %, the following equation was used:
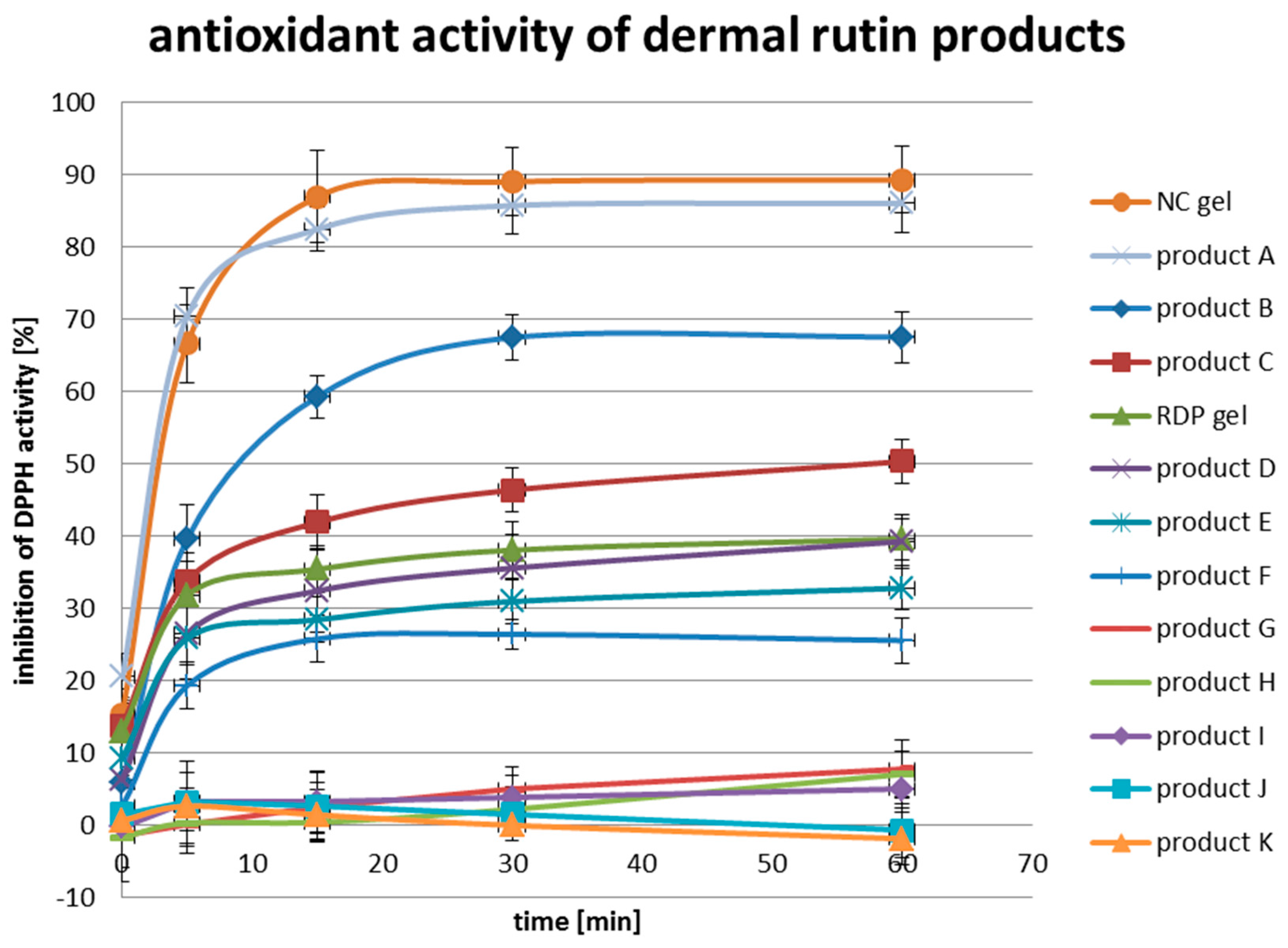
Comparing the antioxidant activity of rutin nanocrystal gel (NC gel) with raw drug powder gel (RDP gel), the superiority in neutralize radicals can be clearly identified for the nanocrystal gel (Figure 2). Already after a reaction time of 5 min, more than 60% of the free radicals were neutralized to innocuous molecules by the nanocrystal gel. Within the same reaction time, only half (30%) of the DPPH was reduced to DPPH-H by the raw drug powder gel. The maximum inhibition of DPPH activity for the nanocrystal gel was reached after 30 min and amounted 90%. For the raw drug powder gel, the maximum was reached after 60 min and amounted to only 40%. Thus, the nanocrystal gel showed more than twice as strong antioxidant activity as the raw drug powder gel. This result can be explained by the significantly increased saturation solubility (Cs) of rutin as nanocrystal during, and also for a long time after the dissolution compared to the μm-sized raw drug powder.
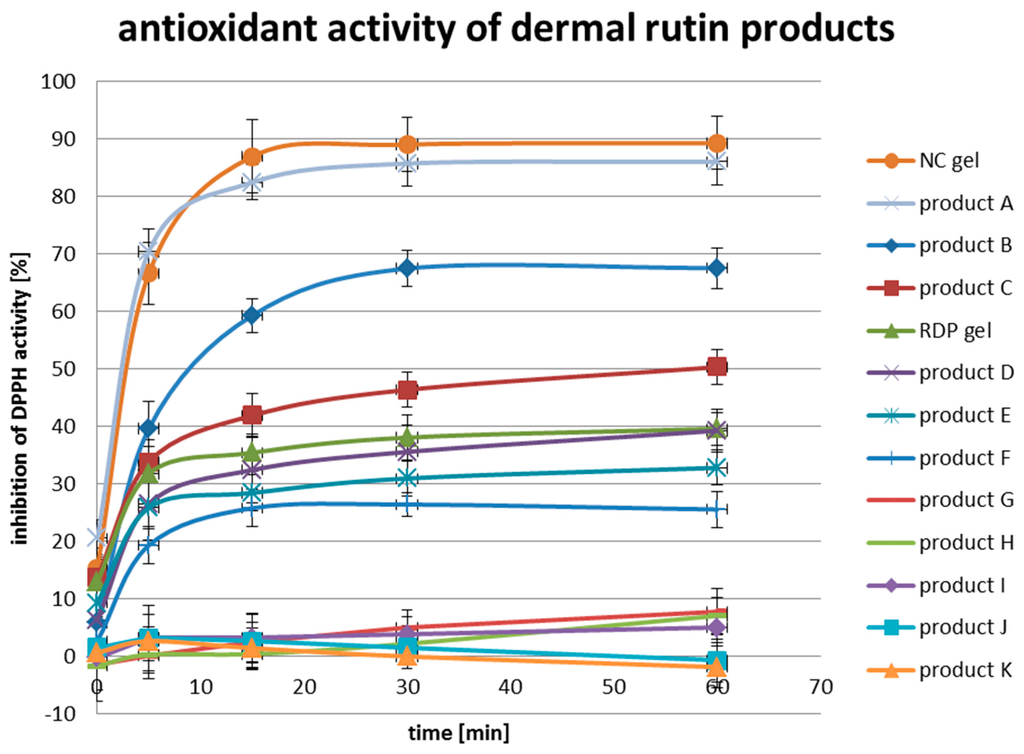
Figure 2.
Comparison of the antioxidant activities with DPPH assay of rutin nanocrystal gel, raw drug powder gel and facial cosmetic products, having rutin, its water-soluble derivative or a combination of both as active ingredient.
In addition, both gels were compared with marketed facial cosmetic products, having rutin, one of its water-soluble derivative or a combination of both as active ingredient. Although the investigated products cannot be named directly, their official retail prices and active compounds can be mentioned, categorized and published. Low price products with an official selling price lower than €20.00 were the products B, C, F and H. Middle price products were D, E, G and I, having an official selling price between €20.00 and €100.00. The products more expensive than €100.00 included A and K. Four different types of rutin were found in the products: rutin nanocrystals (A), rutin raw drug powder (E and G), disodium rutinyl disulfate (C, D, H, I and K) and troxerutin (J). Combined products were also on the marked: B with troxerutin and rutin raw drug powder, E with disodium rutinyl disulfate and rutin raw drug powder and F with troxerutin and disodium rutinyl disulfate.
Since the antioxidant activity depends on structural features, such as hydroxyl bound dissociation energy, resonance delocalization of phenol radicals and steric hindrance derived from groups substituting the hydrogen in the aromatic ring [14], it is to be expected that the change of the chemical structure to obtain increased water solubility will reduce the antioxidant activity. This assumption was confirmed by the results of the DPPH assay (Figure 2). While the rutin nanocrystal gel was able to inhibit 90% of the DPPH activity, the maximum DPPH inhibition among all tested products with water-soluble derivatives of rutin (C, D, F, H, I, J and K) was less than 50%.
Generally, the antioxidant activities of the tested products can be categorized into three classes: I, II and III, where class I products were able to neutralize more than 80% of the DPPH radicals to DPPH-H molecules (A), class II products less than 80% but more than 20% (B, C, D, E and F) and class III, showing almost no reduction in DPPH activity and thus had no antioxidant properties (G, H, I, J and K).
No relationship between the price of a product and its antioxidant activity can be drawn. For example, the product B with the second highest DPPH inhibition of just below 70% can be purchased for €10.99 and has the same price as product H with a DPPH inhibition below 10% (Figure 2). Both A and K are also in the same price category with official selling prices above €100.00. While product A exhibits the highest DPPH inhibition of 85% among the tested marketed products, K shows no antioxidant activity reflected by the DPPH inhibition of 0% (Figure 2).
Even more interesting was the finding that there are also no clear relationships between the type of incorporated rutin and the antioxidant activity of the product exhibited. For example, rutin raw drug powder was the active agent in both product E and G. Product E was able to neutralize more than 30% of the DPPH radicals, while G could not even inhibit 10% of the DPPH radical activity. The same pattern was observed for the products C and D and H, I, and K. All five products have disodium rutinyl disulfate incorporated, but only product C and D showed inhibition effects on DPPH of 50% and 40%, respectively. In contrast, the products H, I and K had nearly no neutralizing effect on the free radical DPPH. The highest antioxidant activity among the products was obtained for product A. It showed almost the same curve progression as the nanocrystal gel. By reading through the advertisement of the company, it was found that this product has rutin incorporated as nanocrystal as well.
To summarize, this in vitro antioxidant activity study revealed the superiority of rutin nanocrystal gel compared to rutin raw drug powder and its water-soluble derivatives with respect to the antioxidant activity.
3.4. Ex-Vivo Penetration Study on Porcine Ears
One of the well-known advantages of nanocrystals is the increased saturation solubility and increased dissolution velocity of actives. The solubility reported for rutin nanocrystals is 133 μg/mL [15]. Since the penetration into the skin takes place by passive diffusion, the increased saturation solubility will automatically lead to a higher concentration gradient between gel and skin and thus to an improved skin penetration. To assess this theory, an ex vivo penetration study on porcine ear skin was performed and the penetration depth and relative amount of penetrated rutin within the stratum corneum was investigated for rutin nanocrystal gel (LD diameter 50% of 353 nm) and rutin raw drug powder gel (LD diameter 50% of 33.0 μm).
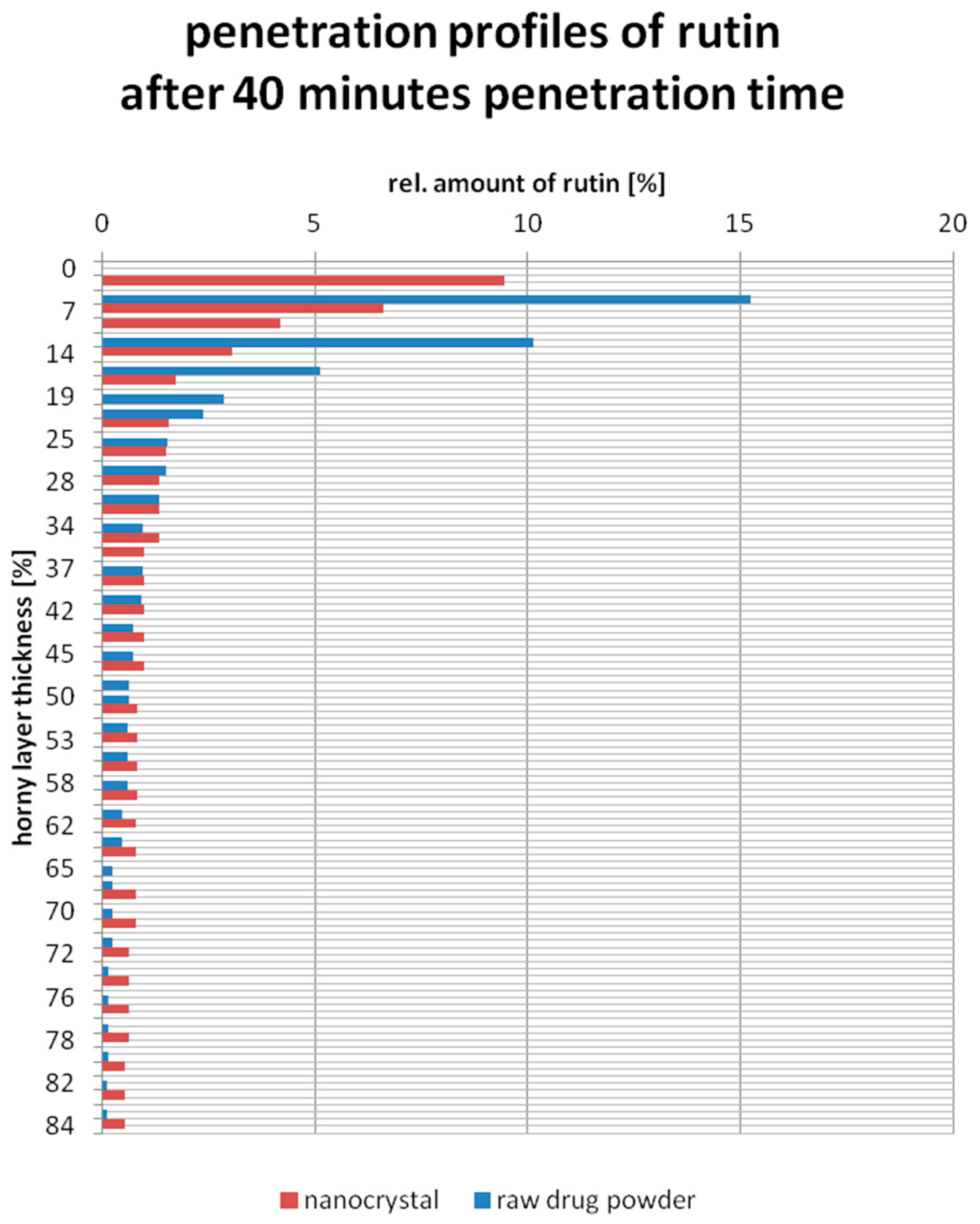
An improved penetration of rutin into the porcine ear skin is given when rutin with lower concentrations remains in the upper part of the stratum corneum (first 20%) and in contrast penetrates in the deeper layers (70% to 100%) of the stratum corneum with higher concentrations. Comparing the penetration profile of both gels determined on one and the same porcine ear (Figure 3), this applies to the rutin nanocrystal gel. In the upper part of the stratum corneum, represented by the depths of 10% and 17%, 2.5- and 2.0-fold less relative amount of rutin could be found, respectively. The middle part of the stratum corneum reveals no major differences according to the rutin concentration. In the deeper part of the stratum corneum, represented by the depths of 70% and 80%, 3.0- and 5.0-fold increased concentration was obtained for the rutin nanocrystal gel.
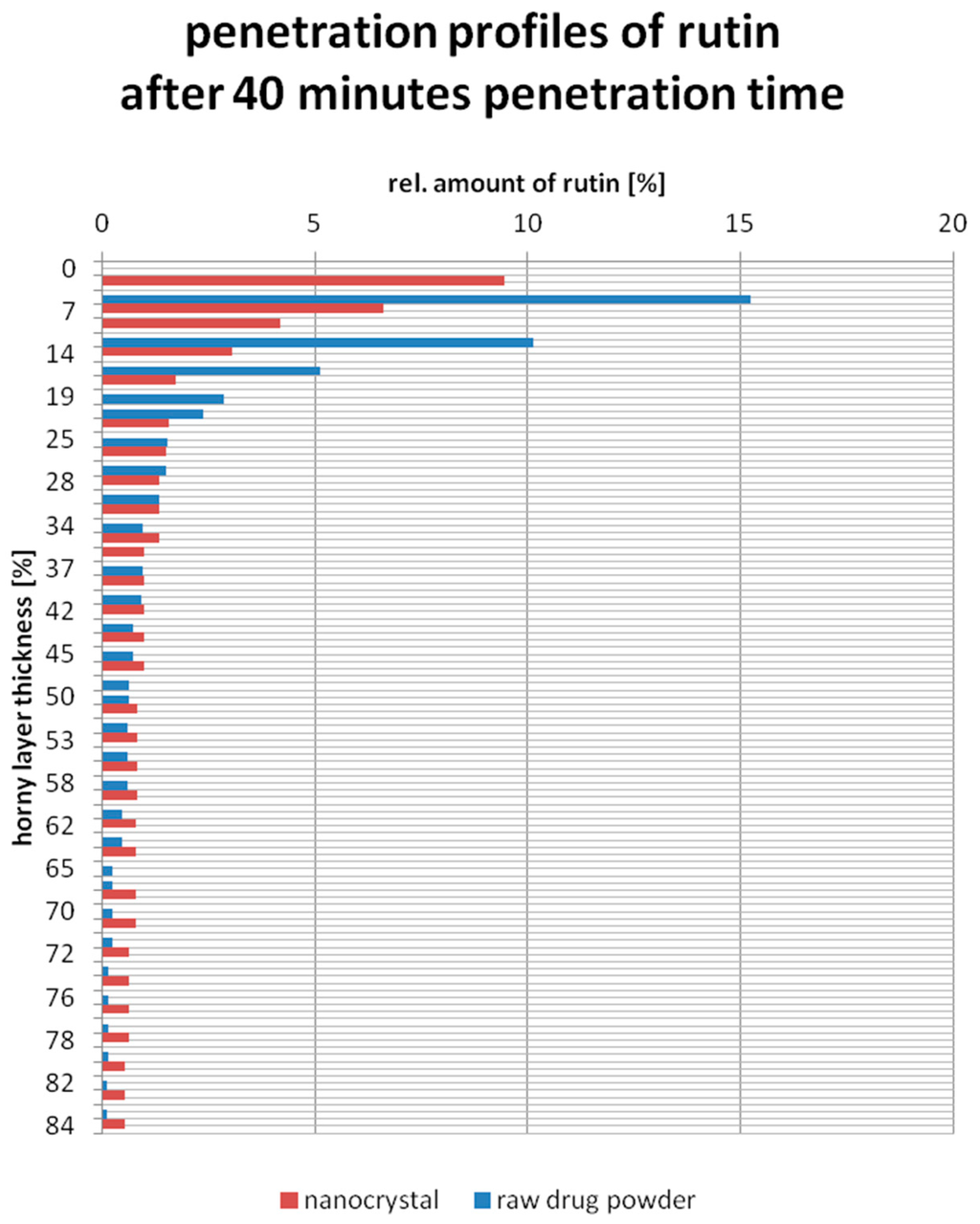
Figure 3.
Penetration profiles of rutin nanocrystal gel (red) and rutin raw drug powder gel (blue) on porcine ear skin after 40 min application time.
Similar observations were made for the other two investigated porcine ears. In the upper part of the stratum corneum, represented by the depths of 15%, 1.8- and 2.4-fold less relative amount of rutin could be found, where in the deeper part of the stratum corneum, represented by the depths of 80%, 4.7- and 5.4-fold increased concentrations were obtained for the rutin nanocrystal gel.
No difference in penetration depth was investigated between both formulations since the used 30 tapes only removed approximately 84% [16] of the whole stratum corneum. However, the course of the penetration curve suggests that the penetration depth would have been deeper for the rutin nanocrystal gel.
In summary, the results of the ex vivo penetration study reveal clearly the improved penetration profile of rutin applied as nanocrystal gel. The increase in skin penetration pared with the superior antioxidant activity suggests a promising dermal bioactivity.
4. Conclusions
The transfer of the μm-sized rutin raw drug powder into nanocrystals could distinctly increase the in vitro antioxidant activity of rutin. In addition, rutin nanocrystals showed increased skin penetration. Both effects are attributed to the increase in the saturation solubility by nanocrystal formation (e.g., increased concentration gradient between dermal formulation and skin, thus increased passive flux into the skin). Both the developed rutin nanocrystal gel and the commercial nanocrystal based product A showed the highest antioxidant activity compared to products with rutin raw drug powder and/or water-soluble rutin derivatives.
The enhanced radical scavenging properties in combination with higher penetration increase the bioactivity in the skin. Thus, nanocrystal technology is promising for increasing the bioactivity of the poorly soluble rutin, as the technology proved to increase the bioavailability of various poorly soluble drugs before. Therefore, the mechanistic principle should be transferable to other poorly soluble antioxidants.
Author Contributions
All authors conceived and designed the experiments; Sung Min Pyo performed the experiments and analyzed the data; after result discussion with all co-authors, Sung Min Pyo wrote the paper, which was finally reviewed by all co-authors.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Imber, G.M.D. Antioxidants, free radicals and skin care. In The Youth Corridor: Your Guide to Timeless Beauty; KCM Publishing: Carol Stream, IL, USA, 2013. [Google Scholar]
- Howard, D. Structural Changes Associated with Aging Skin; The International Dermal Institute: Burlington, MA, USA, 2012. [Google Scholar]
- Del Rosso, J.Q.; Levin, J. The clinical relevance of maintaining the functional integrity of the stratum corneum in both healthy and disease-affected skin. J. Clin. Aesthet. Dermatol. 2011, 4, 22–42. [Google Scholar] [PubMed]
- Halliwell, B.; Gutteridge, J.M. Free Radicals in Biology and Medicine; Oxford University Press: New York, NY, USA, 1999; Volume 3, pp. 1–543. [Google Scholar]
- Yuting, C.; Rongliang, Z.; Zhongjian, J.; Yong, J. Flavonoids as superoxide scavengers and antioxidants. Free Radic. Biol. Med. 1990, 9, 19–21. [Google Scholar] [CrossRef]
- Silva, A.R.; Menezes, P.F.C.; Martinello, T.; Novakovich, G.F.L.; Praes, C.E.O.; Feferman, I.H.S. Antioxidant kinetics of plant-derived substances and extracts. Int. J. Cosmet. Sci. 2010, 32, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R. Nanocrystals for Use in Topical Cosmetic Formulations and Method of Production Thereof. U.S. Patent 12/514,621, 25 February 2010. [Google Scholar]
- Lai, F.; Schlich, M.; Pireddu, R.; Corrias, F.; Maria Fadda, A.; Sinico, C. Production of nanosuspensions as a tool to improve drug bioavailability: Focus on topical delivery. Curr. Pharm. Des. 2015, 21, 6089–6103. [Google Scholar] [CrossRef] [PubMed]
- Al Shaal, L.; Müller, R.H.; Shegokar, R. smartCrystal combination technology—Scale up from lab to pilot scale and long term stability. Die Pharm. Int. J. Pharm. Sci. 2010, 65, 877–884. [Google Scholar]
- Mauludin, R.; Müller, R.H.; Keck, C.M. Kinetic solubility and dissolution velocity of rutin nanocrystals. Eur. J. Pharm. Sci. 2009, 36, 502–510. [Google Scholar] [CrossRef] [PubMed]
- Keck, C.M.; Kobierski, S.; Mauludin, R.; Müller, R.H. Second generation of drug nanocrystals for delivery of poorly soluble drugs: smartCrystals technology. Dosis 2008, 24, 124–128. [Google Scholar]
- Keck, C.M.; Müller, R.H. Nanotoxicological classification system (NCS)—A guide for the risk-benefit assessment of nanoparticulate drug delivery systems. Eur. J. Pharm. Biopharm. 2013, 84, 445–448. [Google Scholar] [CrossRef] [PubMed]
- Santos, S.X.D.; Mazo, L.H.; Cavalheiro, É.T. The use of a graphite-silicone rubber composite electrode in the determination of rutin in pharmaceutical formulation. J. Braz. Chem. Soc. 2008, 19, 1600–1606. [Google Scholar] [CrossRef]
- Craft, B.D.; Kerrihard, A.L.; Amarowicz, R.; Pegg, R.B. Phenol-based antioxidants and the in vitro methods used for their assessment. Compr. Rev. Food Sci. Food Saf. 2012, 11, 148–173. [Google Scholar] [CrossRef]
- Mauludin, R.; Müller, R.H. Preparation and storage stability of rutin nanosuspensions. J. Pharm. Investig. 2013, 43, 395–404. [Google Scholar] [CrossRef]
- Lindemann, U.; Wilken, K.; Schaefer, H.; Sterry, W. Quantification of the horny layer using tape stripping and microscopic techniques. J. Biomed. Opt. 2003, 8, 601–607. [Google Scholar] [CrossRef] [PubMed]
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).