Abnormal Characterization and Distribution of Circulating Regulatory T Cells in Patients with Chronic Spinal Cord Injury According to the Period of Evolution
Abstract
Simple Summary
Abstract
1. Introduction
2. Patients and Methods
2.1. Study Design
2.2. Sample Collection and Inclusion/Exclusion Criteria
2.3. Isolation of Peripheral Blood Mononuclear Cells and Immunophenotype Studies
2.4. Statistical Analysis
3. Results
3.1. Patients Demographics
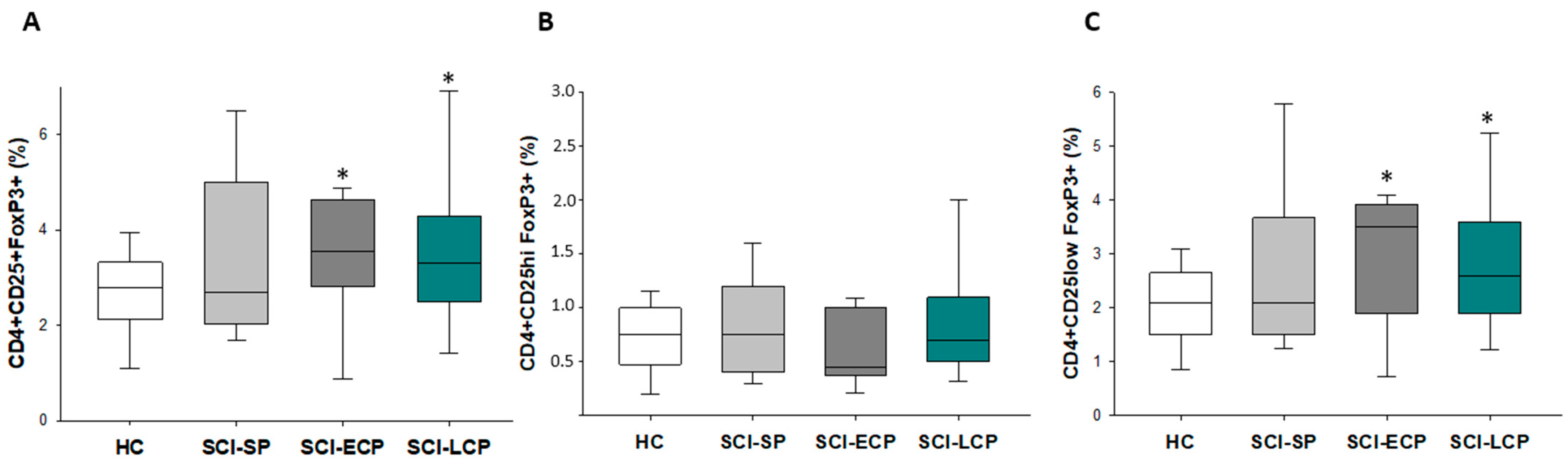
3.2. Patients with a Long Period of Chronic Spinal Cord Injury Present Significant Differences in Circulating CD4+ Foxp3+ CD25+/CD25low Regulatory T Cells Populations
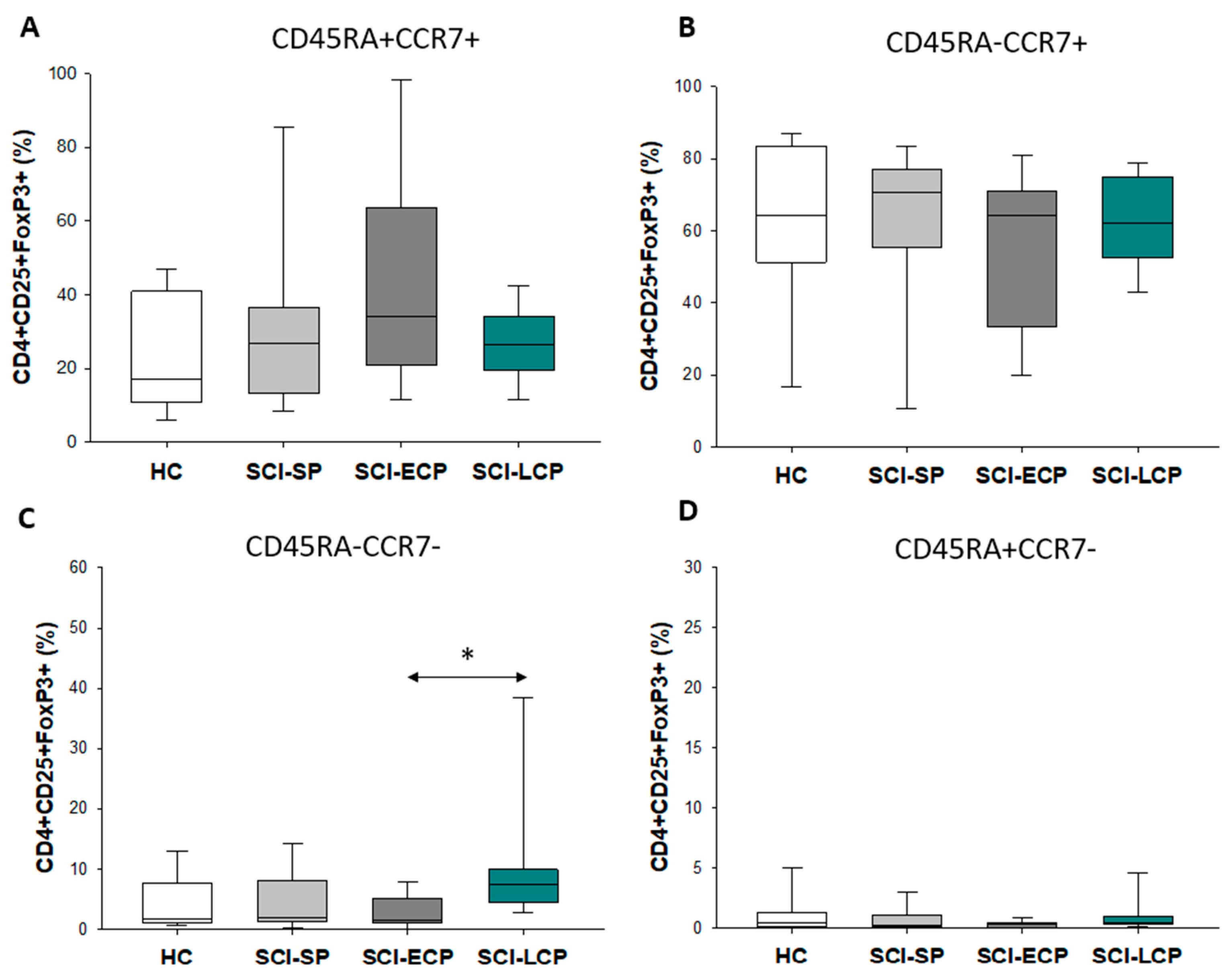
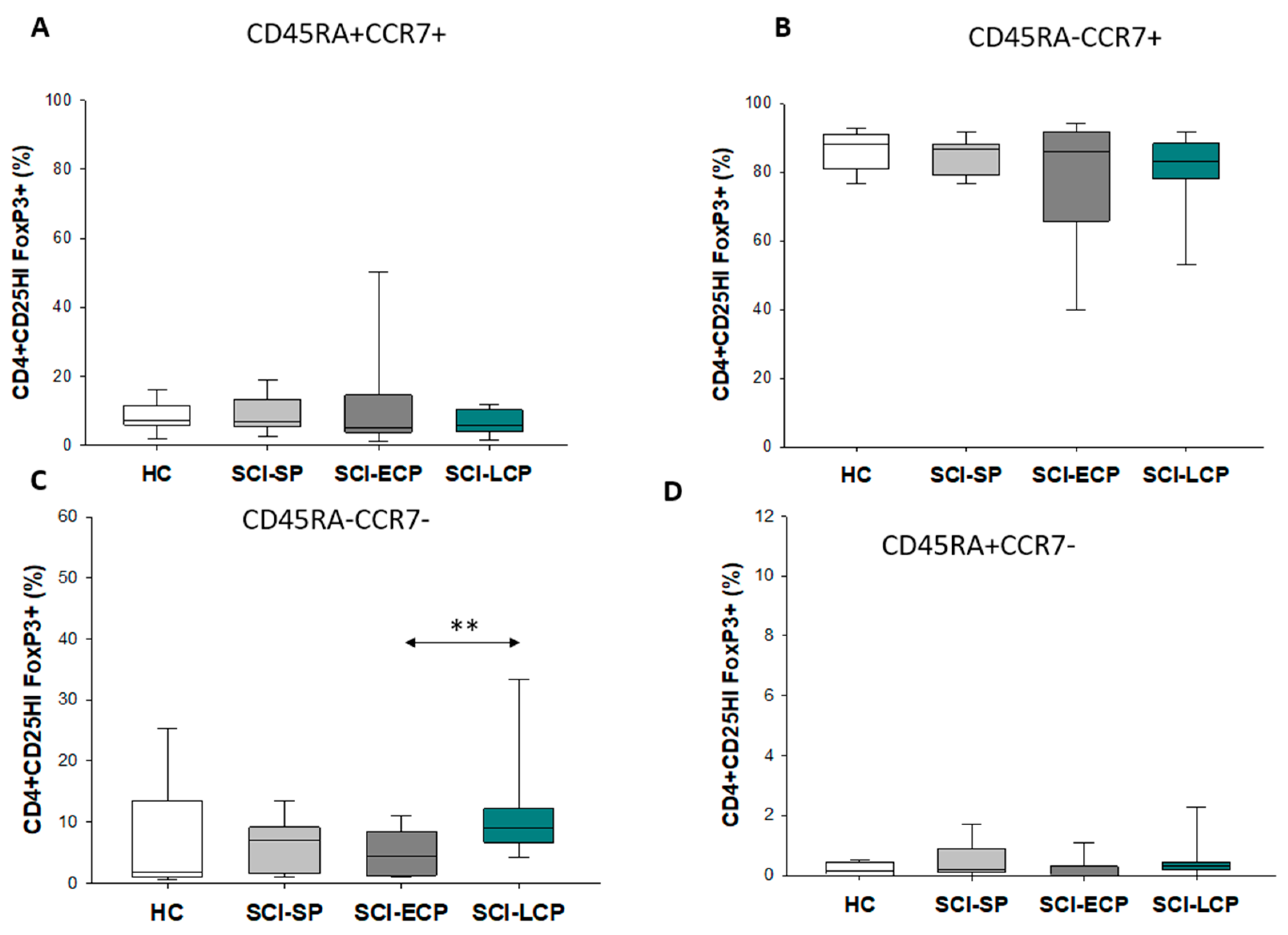
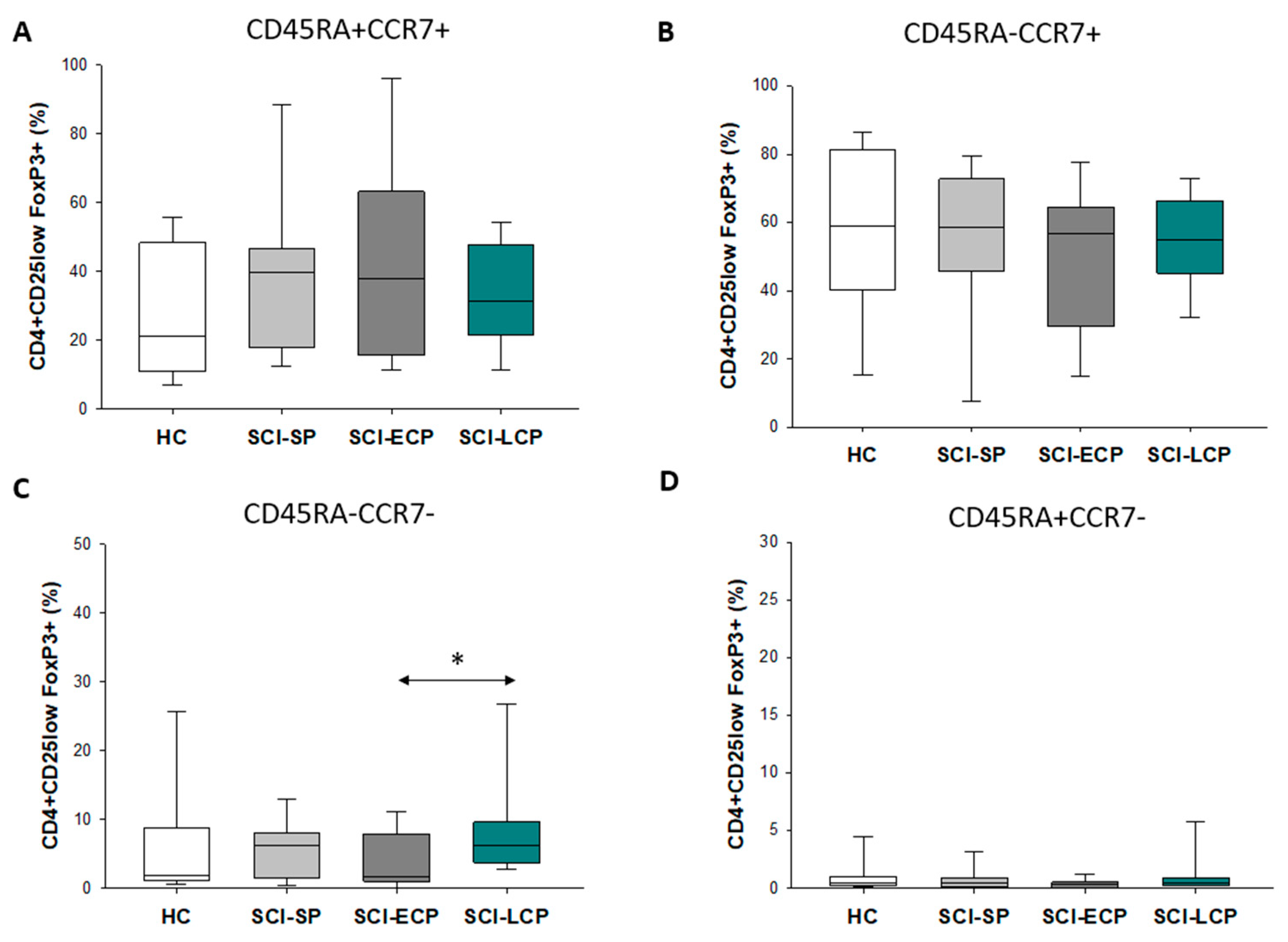
3.3. Patients with a Long Duration of Chronic Spinal Cord Injury Present a Significant Increase in Circulating CD4+ CD25+ Foxp3+ Regulatory T Cell Populations Negative for CD45RA and CCR7 Expression
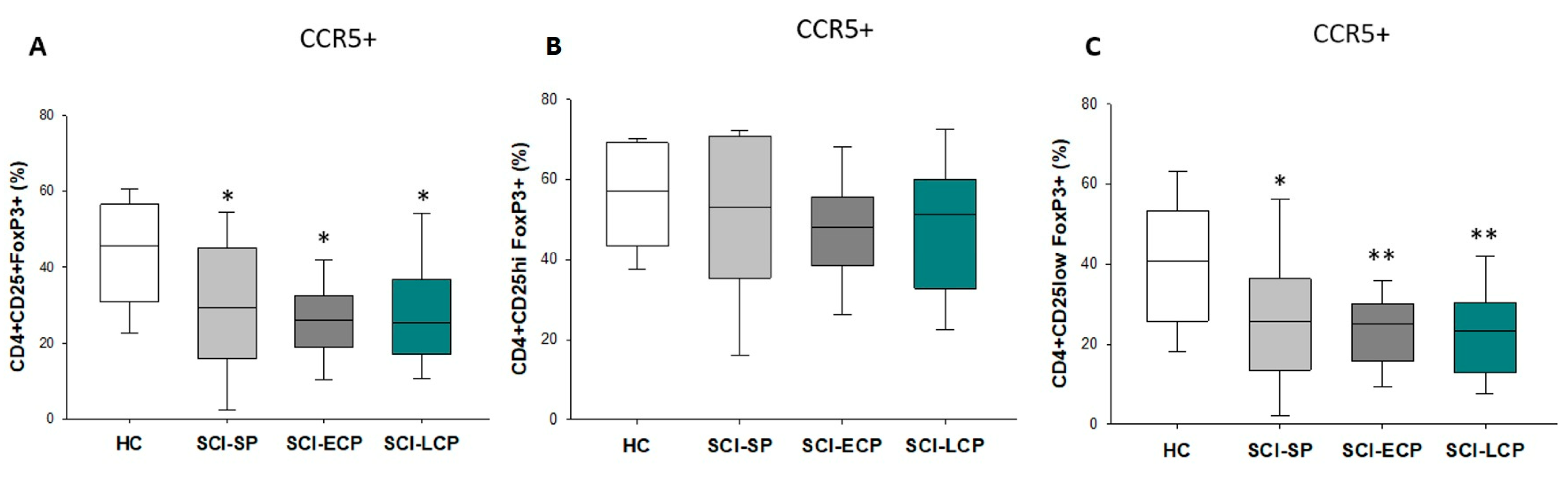
3.4. Patients with a Long Period of Chronic Spinal Cord Injury Present Statistically Significant Differences in Circulating CD4+ CD25+ Foxp3+ Regulatory T Cells Populations Positive for CCR5 Expression
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ali, Z.S.; Whitmore, R.G. Spinal Cord Injuries. In Surgical Intensive Care Medicine, 3rd ed.; Springer: Berlin/Heidelberg, Germany, 2021; pp. 181–193. [Google Scholar] [CrossRef]
- Silva, N.A.; Sousa, N.; Reis, R.L.; Salgado, A.J. From Basics to Clinical: A Comprehensive Review on Spinal Cord Injury. Prog. Neurobiol. 2014, 114, 25–57. [Google Scholar] [CrossRef] [PubMed]
- Varma, A.K.; Das, A.; Wallace, G.; Barry, J.; Vertegel, A.A.; Ray, S.K.; Banik, N.L. Spinal Cord Injury: A Review of Current Therapy, Future Treatments, and Basic Science Frontiers. Neurochem. Res. 2013, 38, 895–905. [Google Scholar] [CrossRef] [PubMed]
- Jazayeri, S.B.; Beygi, S.; Shokraneh, F.; Hagen, E.M.; Rahimi-Movaghar, V. Incidence of Traumatic Spinal Cord Injury Worldwide: A Systematic Review. Eur. Spine J. 2015, 24, 905–918. [Google Scholar] [CrossRef] [PubMed]
- Oyinbo, C.A. Secondary Injury Mechanisms in Traumatic Spinal Cord Injury: A Nugget of This Multiply Cascade. Acta Neurobiol. Exp. 2011, 71, 281–299. [Google Scholar]
- Sun, X.; Jones, Z.B.; Chen, X.-M.; Zhou, L.; So, K.-F.; Ren, Y. Multiple Organ Dysfunction and Systemic Inflammation after Spinal Cord Injury: A Complex Relationship. J. Neuroinflamm. 2016, 13, 1–11. [Google Scholar] [CrossRef]
- Jeffries, M.A.; Tom, V.J. Peripheral Immune Dysfunction: A Problem of Central Importance after Spinal Cord Injury. Biology 2021, 10, 928. [Google Scholar] [CrossRef]
- Kasinathan, N.; Vanathi, M.; Subrahmanyam, V.; Rao, J. A Review on Response of Immune System in Spinal Cord Injury and Therapeutic Agents Useful in Treatment. Curr. Pharm. Biotechnol. 2015, 16, 26–34. [Google Scholar] [CrossRef]
- Schwab, J.M.; Zhang, Y.; Kopp, M.A.; Brommer, B.; Popovich, P.G. The Paradox of Chronic Neuroinflammation, Systemic Immune Suppression and Autoimmunity after Traumatic Chronic Spinal Cord Injury. Exp. Neurol. 2014, 258, 121–129. [Google Scholar] [CrossRef]
- Carpenter, R.S.; Marbourg, J.M.; Brennan, F.H.; Mifflin, K.A.; Hall, J.C.E.; Jiang, R.R.; Mo, X.M.; Karunasiri, M.; Burke, M.H.; Dorrance, A.M.; et al. Spinal Cord Injury Causes Chronic Bone Marrow Failure. Nat. Commun. 2020, 11, 3702. [Google Scholar] [CrossRef]
- Brommer, B.; Engel, O.; Kopp, M.A.; Watzlawick, R.; Müller, S.; Prüss, H.; Chen, Y.; DeVivo, M.J.; Finkenstaedt, F.W.; Dirnagl, U.; et al. Spinal Cord Injury-Induced Immune Deficiency Syndrome Enhances Infection Susceptibility Dependent on Lesion Level. Brain 2016, 139, 692–707. [Google Scholar] [CrossRef]
- Bigford, G.E.; Garshick, E. Systemic Inflammation after Spinal Cord Injury: A Review of Biological Evidence, Related Health Risks, and Potential Therapies. Curr. Opin. Pharmacol. 2022, 67, 102303. [Google Scholar] [CrossRef] [PubMed]
- Pavlicek, D.; Krebs, J.; Capossela, S.; Bertolo, A.; Engelhardt, B.; Pannek, J.; Stoyanov, J. Immunosenescence in Persons with Spinal Cord Injury in Relation to Urinary Tract Infections—A Cross-Sectional Study. Immun. Ageing 2017, 14, 22. [Google Scholar] [CrossRef] [PubMed]
- Ahuja, C.S.; Wilson, J.R.; Nori, S.; Kotter, M.R.N.; Druschel, C.; Curt, A.; Fehlings, M.G. Traumatic Spinal Cord Injury. Nat. Rev. Dis. Prim. 2017, 3, 17018. [Google Scholar] [CrossRef] [PubMed]
- Cardenas, D.D.; Hoffman, J.M.; Kirshblum, S.; McKinley, W. Etiology and Incidence of Rehospitalization after Traumatic Spinal Cord Injury: A Multicenter Analysis. Arch. Phys. Med. Rehabil. 2004, 85, 1757–1763. [Google Scholar] [CrossRef]
- Huang, W.; Vodovotz, Y.; Kusturiss, M.B.; Barclay, D.; Greenwald, K.; Boninger, M.L.; Coen, P.M.; Brienza, D.; Sowa, G. Identification of Distinct Monocyte Phenotypes and Correlation with Circulating Cytokine Profiles in Acute Response to Spinal Cord Injury: A Pilot Study. PM R 2014, 6, 332. [Google Scholar] [CrossRef]
- Gao, T.Y.; Huang, F.F.; Xie, Y.Y.; Wang, W.Q.; Wang, L.D.; Mu, D.; Cui, Y.; Wang, B. Dynamic Changes in the Systemic Immune Responses of Spinal Cord Injury Model Mice. Neural Regen. Res. 2021, 16, 382–387. [Google Scholar] [CrossRef]
- Diaz, D.; Lopez-Dolado, E.; Haro, S.; Monserrat, J.; Martinez-Alonso, C.; Balomeros, D.; Albillos, A.; Alvarez-Mon, M. Systemic Inflammation and the Breakdown of Intestinal Homeostasis Are Key Events in Chronic Spinal Cord Injury Patients. Int. J. Mol. Sci. 2021, 22, 744. [Google Scholar] [CrossRef]
- Sauls, R.S.; McCausland, C.; Taylor, B.N. Histology, T-Cell Lymphocyte. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2022. [Google Scholar]
- Carpenter, R.S.; Jiang, R.R.; Brennan, F.H.; Hall, J.C.E.; Gottipati, M.K.; Niewiesk, S.; Popovich, P.G. Human Immune Cells Infiltrate the Spinal Cord and Impair Recovery after Spinal Cord Injury in Humanized Mice. Sci. Rep. 2019, 9, 1910. [Google Scholar] [CrossRef]
- Vignali, D.A.A.; Collison, L.W.; Workman, C.J. How Regulatory T Cells Work. Nat. Rev. Immunol. 2008, 8, 523–532. [Google Scholar] [CrossRef]
- Staats, J. Immunophenotyping of Human Regulatory T Cells. Methods Mol. Biol. 2019, 2032, 141–177. [Google Scholar] [CrossRef]
- Hornero, R.A.; Betts, G.J.; Sawitzki, B.; Vogt, K.; Harden, P.N.; Wood, K.J. CD45RA Distinguishes CD4+ CD25+ CD127−/Low TSDR Demethylated Regulatory T Cell Subpopulations With Differential Stability and Susceptibility to Tacrolimus-Mediated Inhibition of Suppression. Transplantation 2017, 101, 302. [Google Scholar] [CrossRef] [PubMed]
- Schneider, M.A.; Meingassner, J.G.; Lipp, M.; Moore, H.D.; Rot, A. CCR7 Is Required for the in Vivo Function of CD4+ CD25+ Regulatory T Cells. J. Exp. Med. 2007, 204, 735–745. [Google Scholar] [CrossRef] [PubMed]
- De Oliveira, C.E.; Gasparoto, T.H.; Pinheiro, C.R.; Amôr, N.G.; Nogueira, M.R.S.; Kaneno, R.; Garlet, G.P.; Lara, V.S.; Silva, J.S.; Cavassani, K.A.; et al. CCR5-Dependent Homing of T Regulatory Cells to the Tumor Microenvironment Contributes to Skin Squamous Cell Carcinoma Development. Mol. Cancer Ther. 2017, 16, 2871–2880. [Google Scholar] [CrossRef] [PubMed]
- Zhan, Y.; Wang, N.; Vasanthakumar, A.; Zhang, Y.; Chopin, M.; Nutt, S.L.; Kallies, A.; Lew, A.M. CCR2 Enhances CD25 Expression by FoxP3+ Regulatory T Cells and Regulates Their Abundance Independently of Chemotaxis and CCR2+ Myeloid Cells. Cell. Mol. Immunol. 2020, 17, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, H.X.; Beck, K.D.; Anderson, A.J. Quantitative Assessment of Immune Cells in the Injured Spinal Cord Tissue by Flow Cytometry: A Novel Use for a Cell Purification Method. J. Vis. Exp. 2011, 50, e2698. [Google Scholar] [CrossRef]
- Raposo, C.; Graubardt, N.; Cohen, M.; Eitan, C.; London, A.; Berkutzki, T.; Schwartz, M. CNS Repair Requires Both Effector and Regulatory T Cells with Distinct Temporal and Spatial Profiles. J. Neurosci. 2014, 34, 10141–10155. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Xiong, W.; Wan, B.; Kong, G.; Wang, S.; Wang, Y.; Fan, J. Role of Peripheral Immune Cells in Spinal Cord Injury. Cell Mol. Life Sci. 2023, 80, 2. [Google Scholar] [CrossRef]
- Walsh, J.T.; Zheng, J.; Smirnov, I.; Lorenz, U.; Tung, K.; Kipnis, J. Regulatory T Cells in Central Nervous System Injury: A Double-Edged Sword. J. Immunol. 2014, 193, 5013. [Google Scholar] [CrossRef]
- Monahan, R.; Stein, A.; Gibbs, K.; Bank, M.; Bloom, O. Circulating T Cell Subsets Are Altered in Individuals with Chronic Spinal Cord Injury. Immunol. Res. 2015, 63, 3–10. [Google Scholar] [CrossRef]
- Fraussen, J.; Beckers, L.; van Laake-Geelen, C.C.M.; Depreitere, B.; Deckers, J.; Cornips, E.M.J.; Peuskens, D.; Somers, V. Altered Circulating Immune Cell Distribution in Traumatic Spinal Cord Injury Patients in Relation to Clinical Parameters. Front. Immunol. 2022, 13, 3296. [Google Scholar] [CrossRef]
- Roberts, T.T.; Leonard, G.R.; Cepela, D.J. Classifications In Brief: American Spinal Injury Association (ASIA) Impairment Scale. Clin. Orthop. Relat. Res. 2017, 475, 1499. [Google Scholar] [CrossRef] [PubMed]
- Bauman, W.A.; Wecht, J.M.; Biering-Sorensen, F. International Spinal Cord Injury Endocrine and Metabolic Extended Data Set. Spinal Cord 2017, 55, 466–477. [Google Scholar] [CrossRef]
- Biering-Sørensen, F.; Charlifue, S.; DeVivo, M.; Noonan, V.; Post, M.; Stripling, T.; Wing, P. International Spinal Cord Injury Data Sets. Spinal Cord 2006, 44, 530–534. [Google Scholar] [CrossRef] [PubMed]
- Alvarez-Mon, M.A.; Gomez-Lahoz, A.M.; Orozco, A.; Lahera, G.; Sosa-Reina, M.D.; Diaz, D.; Albillos, A.; Quintero, J.; Molero, P.; Monserrat, J.; et al. Blunted Expansion of Regulatory T Lymphocytes Is Associated With Increased Bacterial Translocation in Patients With Major Depressive Disorder. Front. Psychiatry 2021, 11, 1530. [Google Scholar] [CrossRef]
- Tang, X.; Li, Q.; Huang, T.; Zhang, H.; Chen, X.; Ling, J.; Yang, Y. Regenerative Role of T Cells in Nerve Repair and Functional Recovery. Front. Immunol. 2022, 13, 3389. [Google Scholar] [CrossRef]
- Xu, L.; Ye, X.; Wang, Q.; Xu, B.; Zhong, J.; Chen, Y.; Wang, L. T-cell Infiltration, Contribution and Regulation in the Central Nervous System Post-traumatic Injury. Cell Prolif. 2021, 54, e13092. [Google Scholar] [CrossRef]
- Walsh, J.T.; Kipnis, J. Regulatory T Cells in CNS Injury: The Simple, the Complex, and the Confused. Trends Mol. Med. 2011, 17, 541. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, P.; Eder, R.; Boeld, T.J.; Doser, K.; Piseshka, B.; Andreesen, R.; Edinger, M. Only the CD45RA+ Subpopulation of CD4+CD25high T Cells Gives Rise to Homogeneous Regulatory T-Cell Lines upon in Vitro Expansion. Blood 2006, 108, 4260–4267. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Wu, C.; Xu, G.; Liu, Y.; Chen, J.; Zhang, J.; Hong, H.; Ji, C.; Cui, Z. CCR7-Mediated T Follicular Helper Cell Differentiation Is Associated with the Pathogenesis and Immune Microenvironment of Spinal Cord Injury-Induced Immune Deficiency Syndrome. Front. Neurosci. 2022, 16, 1019406. [Google Scholar] [CrossRef]
- Li, F.; Cheng, B.; Cheng, J.; Wang, D.; Li, H.; He, X. CCR5 Blockade Promotes M2 Macrophage Activation and Improves Locomotor Recovery after Spinal Cord Injury in Mice. Inflammation 2015, 38, 126–133. [Google Scholar] [CrossRef] [PubMed]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gómez-Lahoz, A.M.; Girón, S.H.; Sanz, J.M.; Fraile-Martínez, O.; Garcia-Montero, C.; Jiménez, D.J.; de Leon-Oliva, D.; Ortega, M.A.; Atienza-Perez, M.; Diaz, D.; et al. Abnormal Characterization and Distribution of Circulating Regulatory T Cells in Patients with Chronic Spinal Cord Injury According to the Period of Evolution. Biology 2023, 12, 617. https://doi.org/10.3390/biology12040617
Gómez-Lahoz AM, Girón SH, Sanz JM, Fraile-Martínez O, Garcia-Montero C, Jiménez DJ, de Leon-Oliva D, Ortega MA, Atienza-Perez M, Diaz D, et al. Abnormal Characterization and Distribution of Circulating Regulatory T Cells in Patients with Chronic Spinal Cord Injury According to the Period of Evolution. Biology. 2023; 12(4):617. https://doi.org/10.3390/biology12040617
Chicago/Turabian StyleGómez-Lahoz, Ana M., Sergio Haro Girón, Jorge Monserrat Sanz, Oscar Fraile-Martínez, Cielo Garcia-Montero, Diego J. Jiménez, Diego de Leon-Oliva, Miguel A. Ortega, Mar Atienza-Perez, David Diaz, and et al. 2023. "Abnormal Characterization and Distribution of Circulating Regulatory T Cells in Patients with Chronic Spinal Cord Injury According to the Period of Evolution" Biology 12, no. 4: 617. https://doi.org/10.3390/biology12040617
APA StyleGómez-Lahoz, A. M., Girón, S. H., Sanz, J. M., Fraile-Martínez, O., Garcia-Montero, C., Jiménez, D. J., de Leon-Oliva, D., Ortega, M. A., Atienza-Perez, M., Diaz, D., Lopez-Dolado, E., & Álvarez-Mon, M. (2023). Abnormal Characterization and Distribution of Circulating Regulatory T Cells in Patients with Chronic Spinal Cord Injury According to the Period of Evolution. Biology, 12(4), 617. https://doi.org/10.3390/biology12040617







