Clinical and Molecular Characteristics of Rare Malignant Tumors of Colon and Rectum
Abstract
Simple Summary
Abstract
1. Introduction
2. Methods
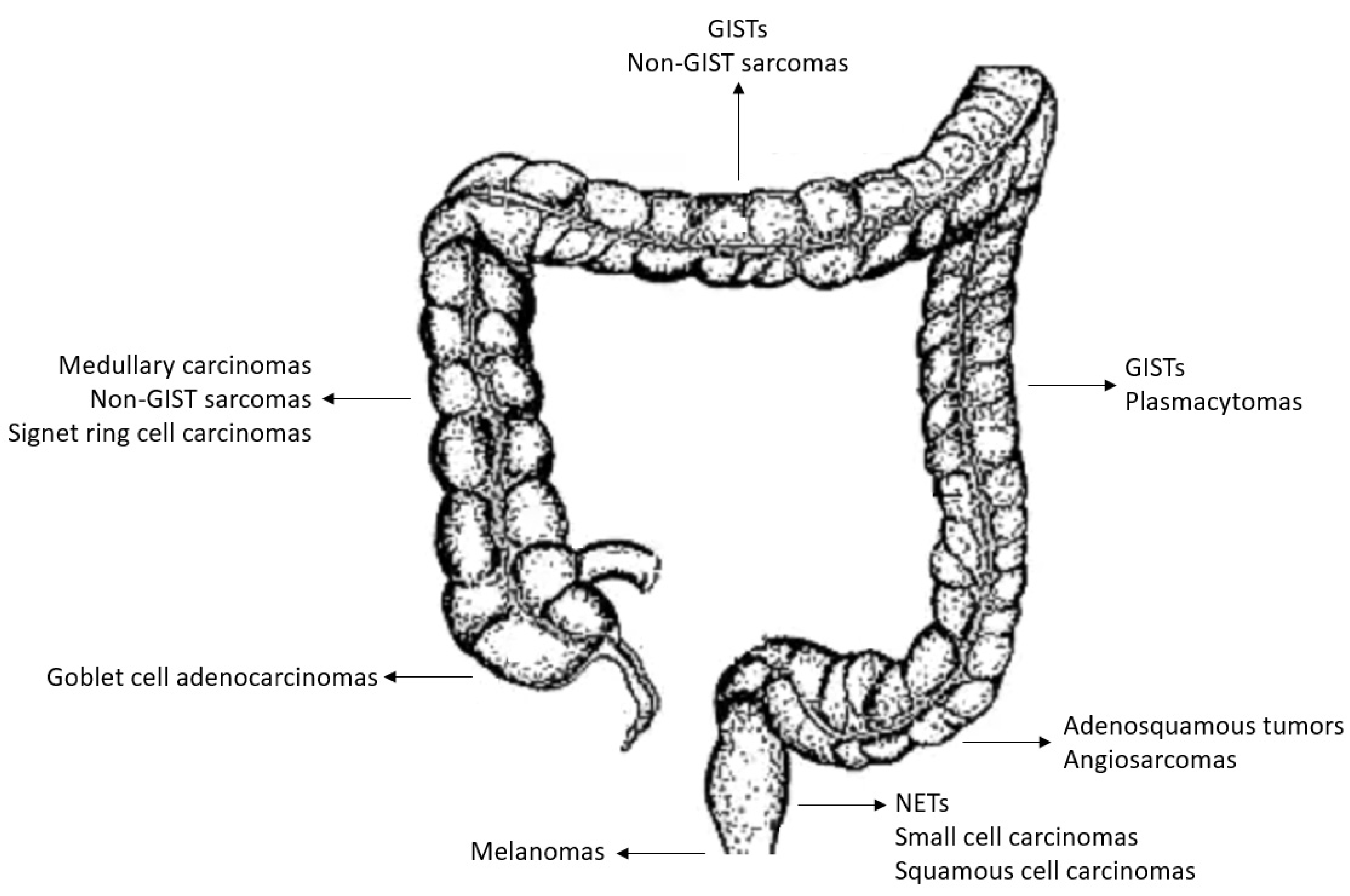
3. Rare Tumors of Colon and Rectum
3.1. Lymphomas
3.2. Mesenchymal Tumors
3.2.1. GISTs
3.2.2. Non-GIST Sarcomas
3.3. Neuroendocrine Tumors
4. Exceptional Tumors of Colon and Rectum
4.1. Adenosquamous
4.2. Angiosarcoma
4.3. Goblet Cell Adenocarcinomas
4.4. Medullary Carcinoma
4.5. Melanomas
4.6. Plasmacytoma
4.7. Signet Ring Cell Carcinoma
4.8. Small Cell Carcinomas
4.9. Squamous Cell Carcinoma
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Siegel, R.L.; Miller, K.D.; Goding Sauer, A.; Fedewa, S.A.; Butterly, L.F.; Anderson, J.C.; Cercek, A.; Smith, R.A.; Jemal, A. Colorectal cancer statistics, 2020. CA Cancer J. Clin. 2020, 70, 145–164. [Google Scholar] [CrossRef] [PubMed]
- Gustafsson, B.I.; Siddique, L.; Chan, A.; Dong, M.; Drozdov, I.; Kidd, M.; Modlin, I.M. Uncommon cancers of the small intestine, appendix and colon: An analysis of SEER 1973-2004, and current diagnosis and therapy. Int. J. Oncol. 2008, 33, 1121–1131. [Google Scholar] [PubMed]
- Small, S.; Barnea Slonim, L.; Williams, C.; Karmali, R. B Cell Lymphomas of the GI Tract. Curr. Gastroenterol. Rep. 2021, 23, 9. [Google Scholar] [CrossRef] [PubMed]
- Wong, M.T.; Eu, K.W. Primary colorectal lymphomas. Colorectal Dis. 2006, 8, 586–591. [Google Scholar] [CrossRef]
- Erginoz, E.; Askar, A.; Cavus, G.H.; Velidedeoglu, M. Primary diffuse large B-cell lymphoma of the sigmoid colon. Int. J. Surg. Case Rep. 2021, 87, 106454. [Google Scholar] [CrossRef] [PubMed]
- Xia, B.; Zhang, L.; Guo, S.Q.; Li, X.W.; Qu, F.L.; Zhao, H.F.; Zhang, L.Y.; Sun, B.C.; You, J.; Zhang, Y.Z. Coexpression of MYC and BCL-2 predicts prognosis in primary gastrointestinal diffuse large B-cell lymphoma. World J. Gastroenterol. 2015, 21, 2433–2442. [Google Scholar] [CrossRef] [PubMed]
- Hori, Y.; Yamamoto, H.; Nozaki, Y.; Torisu, T.; Fujiwara, M.; Taguchi, K.; Nishiyama, K.; Nakamura, S.; Kitazono, T.; Oda, Y. Colorectal diffuse large B-cell lymphoma: Molecular subclassification and prognostic significance of immunoglobulin gene translocation. Hum. Pathol. 2020, 96, 67–78. [Google Scholar] [CrossRef] [PubMed]
- Li, P.; Chai, J.; Chen, Z.; Liu, Y.; Wei, J.; Liu, Y.; Zhao, D.; Ma, J.; Wang, K.; Li, X.; et al. Genomic Mutation Profile of Primary Gastrointestinal Diffuse Large B-Cell Lymphoma. Front. Oncol. 2021, 11, 622–648. [Google Scholar] [CrossRef] [PubMed]
- Greenson, J.K. Gastrointestinal stromal tumors and other mesenchymal lesions of the gut. Mod. Pathol. 2003, 16, 366–375. [Google Scholar] [CrossRef] [PubMed]
- Spałek, M.J.; Kozak, K.; Czarnecka, A.M.; Bartnik, E.; Borkowska, A.; Rutkowski, P. Neoadjuvant Treatment Options in Soft Tissue Sarcomas. Cancers 2020, 12, 2061. [Google Scholar] [CrossRef]
- Blay, J.Y.; Kang, Y.K.; Nishida, T.; von Mehren, M. Gastrointestinal stromal tumours. Nat. Rev. Dis. Primers 2021, 7, 22. [Google Scholar] [CrossRef] [PubMed]
- Kelley, K.A.; Byrne, R.; Lu, K.C. Gastrointestinal Stromal Tumors of the Distal Gastrointestinal Tract. Clin. Colon Rectal Surg. 2018, 31, 295–300. [Google Scholar] [CrossRef]
- Mei, L.; Du, W.; Idowu, M.; von Mehren, M.; Boikos, S.A. Advances and Challenges on Management of Gastrointestinal Stromal Tumors. Front. Oncol. 2018, 8, 135. [Google Scholar] [CrossRef] [PubMed]
- Braconi, C.; Bracci, R.; Cellerino, R. Molecular targets in Gastrointestinal Stromal Tumors (GIST) therapy. Curr. Cancer Drug Targets 2008, 8, 359–366. [Google Scholar] [CrossRef] [PubMed]
- Astolfi, A.; Pantaleo, M.A.; Indio, V.; Urbini, M.; Nannini, M. The Emerging Role of the FGF/FGFR Pathway in Gastrointestinal Stromal Tumor. Int. J. Mol. Sci. 2020, 21, 3313. [Google Scholar] [CrossRef]
- Niinuma, T.; Suzuki, H.; Sugai, T. Molecular characterization and pathogenesis of gastrointestinal stromal tumor. Transl. Gastroenterol. Hepatol. 2018, 3, 2. [Google Scholar] [CrossRef] [PubMed]
- Dermawan, J.K.; Rubin, B.P. Molecular Pathogenesis of Gastrointestinal Stromal Tumor: A Paradigm for Personalized Medicine. Annu. Rev. Pathol. 2021, 17, 323–344. [Google Scholar] [CrossRef] [PubMed]
- Nannini, M.; Rizzo, A.; Indio, V.; Schipani, A.; Astolfi, A.; Pantaleo, M.A. Targeted therapy in SDH-deficient GIST. Ther. Adv. Med. Oncol. 2021, 13. [Google Scholar] [CrossRef] [PubMed]
- Guo, J.U.; Su, Y.; Zhong, C.; Ming, G.L.; Song, H. Hydroxylation of 5-methylcytosine by TET1 promotes active DNA demethylation in the adult brain. Cell 2011, 145, 423–434. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, G.; Sharma, S.; Zheng, M.; Reid, M.D.; Crosby, J.H.; Chamberlain, S.M.; Nayak-Kapoor, A.; Lee, J.R. Primary leiomyosarcomas of the gastrointestinal tract in the post-gastrointestinal stromal tumor era. Ann. Diagn. Pathol. 2012, 16, 532–540. [Google Scholar] [CrossRef] [PubMed]
- Kallen, M.E.; Hornick, J.L. The 2020 WHO Classification: What’s New in Soft Tissue Tumor Pathology? Am. J. Surg. Pathol. 2021, 45, e1–e23. [Google Scholar] [CrossRef]
- Yamamoto, H.; Handa, M.; Tobo, T.; Setsu, N.; Fujita, K.; Oshiro, Y.; Mihara, Y.; Yoshikawa, Y.; Oda, Y. Clinicopathological features of primary leiomyosarcoma of the gastrointestinal tract following recognition of gastrointestinal stromal tumours. Histopathology 2013, 63, 194–207. [Google Scholar] [CrossRef]
- Ikoma, N.; Roland, C.L.; Cormier, J.N.; Chiang, Y.J.; Torres, K.E.; Hunt, K.K.; You, Y.N.; Feig, B.W. Nongastrointestinal Stromal Tumor Spindle Cell Sarcomas of the Colon or Rectum. Am. Surg. 2018, 84, 570–575. [Google Scholar] [CrossRef] [PubMed]
- McGovern, Y.; Zhou, C.D.; Jones, R.L. Systemic Therapy in Metastatic or Unresectable Well-Differentiated/Dedifferentiated Liposarcoma. Front. Oncol. 2017, 7, 292. [Google Scholar] [CrossRef] [PubMed]
- Blay, J.Y. Treatment of advanced soft tissue sarcoma by histological subtype: Wish, prediction or reality? Future Oncol. 2019, 15, 5–10. [Google Scholar] [CrossRef] [PubMed]
- Hollowoa, B.; Lamps, L.W.; Mizell, J.S.; English GW 3rd Bridge, J.A.; Ram, R.; Gardner, J.M. Dedifferentiated Liposarcoma Mimicking a Primary Colon Mass. Int. J. Surg. Pathol. 2018, 26, 174–179. [Google Scholar] [CrossRef]
- Guadagno, E.; Peltrini, R.; Stasio, L.; Fiorentino, F.; Bucci, L.; Terracciano, L.; Insabato, L. A challenging diagnosis of mesenchymal neoplasm of the colon: Colonic dedifferentiated liposarcoma with lymph node metastases–A case report and review of the literature. Int. J. Colorectal Dis. 2019, 34, 1809–1814. [Google Scholar] [CrossRef] [PubMed]
- Abeshouse, A.; Adebamowo, C.; Adebamowo, S.N.; Akbani, R.; Akeredolu, T.; Ally, A.; Anderson, M.L.; Anur, P.; Appelbaum, E.L.; Armenia, J.; et al. Comprehensive and Integrated Genomic Characterization of Adult Soft Tissue Sarcomas. Cell 2017, 171, 950–965.e28. [Google Scholar] [CrossRef] [PubMed]
- Bohlok, A.; El Khoury, M.; Bormans, A.; Galdon, M.G.; Vouche, M.; El Nakadi, I.; Donckier, V.; Liberale, G. Schwannoma of the colon and rectum: A systematic literature review. World J. Surg. Oncol. 2018, 16, 125. [Google Scholar] [CrossRef] [PubMed]
- Mekras, A.; Krenn, V.; Perrakis, A.; Croner, R.S.; Kalles, V.; Atamer, C.; Grützmann, R.; Vassos, N. Gastrointestinal schwannomas: A rare but important differential diagnosis of mesenchymal tumors of gastrointestinal tract. BMC Surg. 2018, 18, 47. [Google Scholar] [CrossRef]
- Wang, W.B.; Chen, W.B.; Lin, J.J.; Xu, J.H.; Wang, J.H.; Sheng, Q.S. Schwannoma of the colon: A case report and review of the literature. Oncol. Lett. 2016, 11, 2580–2582. [Google Scholar] [CrossRef] [PubMed]
- Kim, G.; Kim, S.I.; Lee, K.Y. Case Report: Schwannoma of the sigmoid colon: A case report of a rare colonic neoplasm and review of literature. F1000Research 2019, 8, 652. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Li, B.; Zheng, C.; He, X. Clinical Characteristics and Surgical Management of Gastrointestinal Schwannomas. Biomed. Res. Int. 2020, 2020, 9606807. [Google Scholar] [CrossRef] [PubMed]
- Lasota, J.; Wasag, B.; Dansonka-Mieszkowska, A.; Karcz, D.; Millward, C.L.; Ryś, J.; Stachura, J.; Sobin, L.H.; Miettinen, M. Evaluation of NF2 and NF1 tumor suppressor genes in distinctive gastrointestinal nerve sheath tumors traditionally diagnosed as benign schwannomas: S study of 20 cases. Lab. Investig. 2003, 83, 1361–1371. [Google Scholar] [CrossRef] [PubMed]
- Twist, E.C.; Ruttledge, M.H.; Rousseau, M.; Sanson, M.; Papi, L.; Merel, P.; Delattre, O.; Thomas, G.; Rouleau, G.A. The neurofibromatosis type 2 gene is inactivated in schwannomas. Hum. Mol. Genet. 1994, 3, 147–151. [Google Scholar] [CrossRef]
- Ahmed, M. Gastrointestinal neuroendocrine tumors in 2020. World J. Gastrointest. Oncol. 2020, 12, 791–807. [Google Scholar] [CrossRef]
- Bräutigam, K.; Rodriguez-Calero, A.; Kim-Fuchs, C.; Kollár, A.; Trepp, R.; Marinoni, I.; Perren, A. Update on Histological Reporting Changes in Neuroendocrine Neoplasms. Curr. Oncol. Rep. 2021, 23, 65. [Google Scholar] [CrossRef]
- Feola, T.; Centello, R.; Sesti, F.; Puliani, G.; Verrico, M.; Di Vito, V.; Di Gioia, C.; Bagni, O.; Lenzi, A.; Isidori, A.M.; et al. Neuroendocrine Carcinomas with Atypical Proliferation Index and Clinical Behavior: A Systematic Review. Cancers 2021, 13, 1247. [Google Scholar] [CrossRef]
- Hrabe, J. Neuroendocrine Tumors of the Appendix, Colon, and Rectum. Surg. Oncol. Clin. N. Am. 2020, 29, 267–279. [Google Scholar] [CrossRef]
- Gong, P.; Chen, C.; Wang, Z.; Zhang, X.; Hu, W.; Hu, Z.; Li, X. Prognostic significance for colorectal well-differentiated neuroendocrine tumor tumors based on the 8th edition TNM staging system. Cancer Med. 2020, 9, 7979–7987. [Google Scholar] [CrossRef]
- McDermott, F.D.; Heeney, A.; Courtney, D.; Mohan, H.; Winter, D. Rectal well-differentiated neuroendocrine tumors: A systematic review. Surg. Endosc. 2014, 28, 2020–2026. [Google Scholar] [CrossRef] [PubMed]
- Janson, E.T.; Knigge, U.; Dam, G.; Federspiel, B.; Grønbaek, H.; Stålberg, P.; Langer, S.W.; Kjaer, A.; Arola, J.; Schalin-Jäntti, C.; et al. Nordic guidelines 2021 for diagnosis and treatment of gastroenteropancreatic neuroendocrine neoplasms. Acta Oncol. 2021, 60, 931–941. [Google Scholar] [CrossRef] [PubMed]
- Kwekkeboom, D.J.; Kam, B.L.; van Essen, M.; Teunissen, J.J.; van Eijck, C.H.; Valkema, R.; de Jong, M.; de Herder, W.W.; Krenning, E.P. Somatostatin-receptor-based imaging and therapy of gastroenteropancreatic neuroendocrine tumors. Endocr. Relat. Cancer 2010, 17, R53–R73. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Law, C. Chromogranin A: A sensitive biomarker for the detection and post-treatment monitoring of gastroenteropancreatic neuroendocrine tumors. Expert. Rev. Gastroenterol. Hepatol. 2012, 6, 313–334. [Google Scholar] [CrossRef]
- Yong, J.N.; Lim, X.C.; Nistala, K.R.Y.; Lim, L.K.E.; Lim, G.E.H.; Quek, J.; Tham, H.Y.; Wong, N.W.; Tan, K.K.; Chong, C.S. Endoscopic submucosal dissection versus endoscopic mucosal resection for rectal well-differentiated neuroendocrine tumor tumor. A meta-analysis and meta-regression with single-arm analysis. J. Dig. Dis. 2021, 22, 562–571. [Google Scholar] [CrossRef]
- Clift, A.K.; Frilling, A. Neuroendocrine, goblet cell and mixed adeno-neuroendocrine tumours of the appendix: Updates, clinical applications and the future. Expert. Rev. Gastroenterol. Hepatol. 2017, 11, 237–247. [Google Scholar] [CrossRef] [PubMed]
- Mohamed, A.; Strosberg, J.R. Medical Management of Gastroenteropancreatic Neuroendocrine Tumors: Current Strategies and Future Advances. J. Nucl. Med. 2019, 60, 721–727. [Google Scholar] [CrossRef]
- Mitsuhashi, K.; Yamamoto, I.; Kurihara, H.; Kanno, S.; Ito, M.; Igarashi, H.; Ishigami, K.; Sukawa, Y.; Tachibana, M.; Takahashi, H.; et al. Analysis of the molecular features of rectal well-differentiated neuroendocrine tumor tumors to identify new biomarkers that predict biological malignancy. Oncotarget 2015, 6, 22114–22125. [Google Scholar] [CrossRef]
- Park, H.Y.; Kwon, M.J.; Kang, H.S.; Kim, Y.J.; Kim, N.Y.; Kim, M.J.; Min, K.W.; Choi, K.C.; Nam, E.S.; Cho, S.J.; et al. Targeted next-generation sequencing of well-differentiated rectal, gastric, and appendiceal neuroendocrine tumors to identify potential targets. Hum. Pathol. 2019, 87, 83–94. [Google Scholar] [CrossRef]
- Nasseri, Y.; Cox, B.; Shen, W.; Zhu, R.; Stettler, I.; Cohen, J.; Artinyan, A.; Gangi, A. Adenosquamous carcinoma: An aggressive histologic sub-type of colon cancer with poor prognosis. Am. J. Surg. 2021, 221, 649–653. [Google Scholar] [CrossRef]
- Shafaghi, A.; Askari, K.; Ashoobi, M.T.; Mansour-Ghanaei, F. Adenosquamous carcinoma of the sigmoid colon: A case report and review of literature. Int. J. Clin. Exp. Med. 2013, 6, 390–392. [Google Scholar] [PubMed]
- Sunkara, T.; Caughey, M.E.; Makkar, P.; John, F.; Gaduputi, V. Adenosquamous Carcinoma of the Colon. Case Rep. Gastroenterol. 2018, 11, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Thompson, J.T.; Paschold, E.H.; Levine, E.A. Paraneoplastic hypercalcemia in a patient with adenosquamous cancer of the colon. Am. Surg. 2001, 67, 585–588. [Google Scholar] [PubMed]
- Wang, Q.; Zhao, T.; Mi, B.T.; Zhang, Y.L.; Wei, R.; Tong, H.L.; Wu, M. Primary Colonic Angiosarcoma Seen in a Patient on Calcium Channel Blocker: A Case Report with Summary Analysis of 32 Other Cases from the Literature. Am. J. Case Rep. 2018, 19, 254–261. [Google Scholar] [CrossRef]
- Sherid, M.; Sifuentes, H.; Brasky, J.; Shah, D.A.; Ehrenpreis, E.D. Clinical and endoscopic features of angiosarcoma of the colon: Two case reports and a review of the literature. J. Gastrointest. Cancer 2013, 44, 12–21. [Google Scholar] [CrossRef]
- Brown, C.J.; Falck, V.G.; MacLean, A. Angiosarcoma of the colon and rectum: Report of a case and review of the literature. Dis. Colon Rectum. 2004, 47, 2202–2207. [Google Scholar] [CrossRef]
- Holt, N.; Grønbæk, H. Goblet cell adenocarcinomas of the appendix. Sci. World J. 2013, 2013, 543696. [Google Scholar] [CrossRef] [PubMed]
- Pahlavan, P.S.; Kanthan, R. Goblet cell adenocarcinoma of the appendix. World J. Surg. Oncol. 2005, 3, 36. [Google Scholar] [CrossRef]
- Sluiter, N.R.; van der Bilt, J.D.; Croll, D.M.R.; Vriens, M.R.; de Hingh, I.H.J.T.; Hemmer, P.; Aalbers, A.G.J.; Bremers, A.J.A.; Ceelen, W.; D’Hoore, A.; et al. Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) Versus Surgery Without HIPEC for Goblet-Cell Well-differentiated neuroendocrine tumors and Mixed Adenoneuroendocrine Carcinomas: Propensity Score-Matched Analysis of Centers in the Netherlands and Belgium. Clin. Colorectal Cancer 2020, 19, e87–e99. [Google Scholar] [CrossRef]
- Jesinghaus, M.; Konukiewitz, B.; Foersch, S.; Stenzinger, A.; Steiger, K.; Muckenhuber, A.; Groß, C.; Mollenhauer, M.; Roth, W.; Detlefsen, S.; et al. Appendiceal goblet cell adenocarcinomas and adenocarcinomas ex-goblet cell adenocarcinoma are genetically distinct from primary colorectal-type adenocarcinoma of the appendix. Mod. Pathol. 2018, 31, 829–839. [Google Scholar] [CrossRef]
- Scott, N.; West, N.P.; Cairns, A.; Rotimi, O. Is medullary carcinoma of the colon underdiagnosed? An audit of poorly differentiated colorectal carcinomas in a large national health service teaching hospital. Histopathology 2021, 78, 963–969. [Google Scholar] [CrossRef] [PubMed]
- Fatima, Z.; Sharma, P.; Youssef, B.; Krishnan, K. Medullary Carcinoma of the Colon: A Histopathologic Challenge. Cureus 2021, 13, e15831. [Google Scholar] [CrossRef] [PubMed]
- Pyo, J.S.; Sohn, J.H.; Kang, G. Medullary carcinoma in the colorectum: A systematic review and meta-analysis. Hum. Pathol. 2016, 53, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Winn, B.; Tavares, R.; Fanion, J.; Noble, L.; Gao, J.; Sabo, E.; Resnick, M.B. Differentiating the undifferentiated: Immunohistochemical profile of medullary carcinoma of the colon with an emphasis on intestinal differentiation. Hum. Pathol. 2009, 40, 398–404. [Google Scholar] [CrossRef] [PubMed]
- Colarossi, C.; Mare, M.; La Greca, G.; De Zuanni, M.; Colarossi, L.; Aiello, E.; Piombino, E.; Memeo, L. Medullary Carcinoma of the Gastrointestinal Tract: Report on Two Cases with Immunohistochemical and Molecular Features. Diagnostics 2021, 11, 1775. [Google Scholar] [CrossRef] [PubMed]
- D’Orazio, B.; Bonventre, S.; Cudia, B.; Di Vita, G.; Geraci, G. Early diagnosis of primary melanoma of caecum. Case report and review of the literature. Acta Biomed. 2021, 92, e2021112. [Google Scholar] [CrossRef] [PubMed]
- Khalid, U.; Saleem, T.; Imam, A.M.; Khan, M.R. Pathogenesis, diagnosis and management of primary melanoma of the colon. World J. Surg. Oncol. 2011, 9, 14. [Google Scholar] [CrossRef] [PubMed]
- Miliaras, S.; Ziogas, I.A.; Mylonas, K.S.; Papadopoulos, V.N. Primary malignant melanoma of the ascending colon. BMJ Case Rep. 2018, 2018, bcr-2017. [Google Scholar] [CrossRef] [PubMed]
- Mirea, M.A.; Eckensperger, S.; Hengstschläger, M.; Mikula, M. Insights into Differentiation of Melanocytes from Human Stem Cells and Their Relevance for Melanoma Treatment. Cancers 2020, 12, 2508. [Google Scholar] [CrossRef] [PubMed]
- Chang, A.E.; Karnell, L.H.; Menck, H.R. The National Cancer Data Base report on cutaneous and noncutaneous melanoma: A summary of 84,836 cases from the past decade. The American College of Surgeons Commission on Cancer and the American Cancer Society. Cancer 1998, 83, 1664–1678. [Google Scholar] [CrossRef]
- Guo, J.; Si, L.; Kong, Y.; Flaherty, K.T.; Xu, X.; Zhu, Y.; Corless, C.L.; Li, L.; Li, H.; Sheng, X.; et al. Phase II, open-label, single-arm trial of imatinib mesylate in patients with metastatic melanoma harboring c-Kit mutation or amplification. J. Clin. Oncol. 2011, 29, 2904–2909. [Google Scholar] [CrossRef] [PubMed]
- Moreira, A.; Heinzerling, L.; Bhardwaj, N.; Friedlander, P. Current Melanoma Treatments: Where Do We Stand? Cancers 2021, 13, 221. [Google Scholar] [CrossRef]
- Yang, H.M.; Hsiao, S.J.; Schaeffer, D.F.; Lai, C.; Remotti, H.E.; Horst, D.; Mansukhani, M.M.; Horst, B.A. Identification of recurrent mutational events in anorectal melanoma. Mod. Pathol. 2017, 30, 286–296. [Google Scholar] [CrossRef] [PubMed]
- Parnell, K.; Ahmed, M.; Smalligan, R.D.; Nadesan, S. Extramedullary plasmacytoma mimicking colon carcinoma: An unusual presentation and review of the literature. BMJ Case Rep. 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Han, Y.J.; Park, S.J.; Park, M.I.; Moon, W.; Kim, S.E.; Ku, K.H.; Ock, S.Y. Solitary extramedullary plasmacytoma in the gastrointestinal tract: Report of two cases and review of literature. Korean J. Gastroenterol. 2014, 63, 316–320. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ligato, S.; El-Naggar, A.; Cleary, K.R.; Manning, J. Extramedullary plasmacytoma mimicking primary colonic carcinoma in a patient with Crohn’s disease. Case report and literature review. Arch. Pathol. Lab. Med. 1996, 120, 279–282. [Google Scholar] [PubMed]
- Talamo, G.; Cavallo, F.; Zangari, M.; Barlogie, B.; Lee, C.K.; Pineda-Roman, M.; Kiwan, E.; Krishna, S.; Tricot, G. Clinical and biological features of multiple myeloma involving the gastrointestinal system. Haematologica 2006, 91, 964–967. [Google Scholar]
- Gupta, V.; Nahak, B.; Sakhuja, P.; Agarwal, A.K.; Kumar, N.; Mishra, P.K. Primary isolated extramedullary plasmacytoma of colon. World J. Surg. Oncol. 2007, 5, 47. [Google Scholar] [CrossRef] [PubMed]
- Farraj, F.A.; Sabbagh, H.; Aridi, T.; Fakhruddin, N.; Farhat, F. Signet Ring Cell Carcinoma of the Colon in Young Adults: A Case Report and Literature Review. Case Rep. Oncol. Med. 2019, 2019, 3092674. [Google Scholar] [CrossRef]
- Sugimoto, S.; Shimoda, M.; Iwao, Y.; Mutaguchi, M.; Nanki, K.; Mizuno, S.; Kameyama, K.; Ogata, H.; Naganuma, M.; Kanai, T. Intramucosal poorly differentiated and signet-ring cell components in patients with ulcerative colitis-associated high-grade dysplasia. Dig. Endosc. 2019, 31, 706–711. [Google Scholar] [CrossRef]
- Pozos-Ochoa, L.I.; Lino-Silva, L.S.; León-Takahashi, A.M.; Salcedo-Hernández, R.A. Prognosis of Signet Ring Cell Carcinoma of the Colon and Rectum and their Distinction of Mucinous Adenocarcinoma with Signet Ring Cells. A Comparative Study. Pathol. Oncol. Res. 2018, 24, 609–616. [Google Scholar] [CrossRef]
- Wei, Q.; Wang, X.; Gao, J.; Li, J.; Li, J.; Qi, C.; Li, Y.; Li, Z.; Shen, L. Clinicopathologic and Molecular Features of Colorectal Adenocarcinoma with Signet-Ring Cell Component. PLoS ONE 2016, 11, e0156659. [Google Scholar] [CrossRef] [PubMed]
- Marchioni Beery, R.M.; Devers, T.J.; Clement, J.M. A case of primary colonic small-cell carcinoma arising in a patient with long-standing ulcerative colitis. Gastrointest. Cancer Res. 2014, 7, 119–122. [Google Scholar]
- Fields, A.C.; Lu, P.; Vierra, B.M.; Hu, F.; Irani, J.; Bleday, R.; Goldberg, J.E.; Nash, G.M.; Melnitchouk, N. Survival in Patients with High-Grade Colorectal Neuroendocrine Carcinomas: The Role of Surgery and Chemotherapy. Ann. Surg. Oncol. 2019, 26, 1127–1133. [Google Scholar] [CrossRef]
- Li, A.F.; Li, A.C.; Hsu, C.Y.; Li, W.Y.; Hsu, H.S.; Chen, J.Y. Small cell carcinomas in gastrointestinal tract: Immunohistochemical and clinicopathological features. J. Clin. Pathol. 2010, 63, 620–625. [Google Scholar] [CrossRef] [PubMed]
- Balasubramanyam, S.; O’Donnell, B.P.; Musher, B.L.; Jhaveri, P.M.; Ludwig, M.S. Evaluating Treatment Patterns for Small Cell Carcinoma of the Colon Using the National Cancer Database (NCDB). J. Gastrointest. Cancer 2019, 50, 244–253. [Google Scholar] [CrossRef] [PubMed]
- Hayashi, H.; Miyagi, Y.; Sekiyama, A.; Yoshida, S.; Nakao, S.; Okamoto, N.; Koganei, K.; Sugita, A. Colorectal small cell carcinoma in ulcerative colitis with identical rare p53 gene mutation to associated adenocarcinoma and dysplasia. J. Crohns Colitis 2012, 6, 112–115. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dikshit, V.; Ali, I.; Patil, C.; Manerikar, K.; Mody, P. Squamous Cell Carcinoma of Colon-an Etiopathological Surprise. J. Gastrointest. Cancer 2019, 50, 604–608. [Google Scholar] [CrossRef] [PubMed]
- Ambrosio, M.R.; Vernillo, R.; De Carolis, S.; Carducci, A.; Mundo, L.; Ginori, A.; Rocca, B.J.; Nardone, V.; Lucenti Fei, A.; Carfagno, T.; et al. Putative Role of Circulating Human Papillomavirus DNA in the Development of Primary Squamous Cell Carcinoma of the Middle Rectum: A Case Report. Front Oncol. 2019, 21, 93. [Google Scholar] [CrossRef] [PubMed]
- Lu, D.W.; El-Mofty, S.K.; Wang, H.L. Expression of p16, Rb, and p53 proteins in squamous cell carcinomas of the anorectal region harboring human papillomavirus DNA. Mod. Pathol. 2003, 16, 692–699. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Gardner, I.H.; Watson, K.M. Diagnosis and Treatment of Anal Squamous Cell Carcinoma. Dis. Colon Rectum. 2020, 63, 1358–1361. [Google Scholar] [CrossRef] [PubMed]
- Ozuner, G.; Aytac, E.; Gorgun, E.; Bennett, A. Colorectal squamous cell carcinoma: A rare tumor with poor prognosis. Int. J. Colorectal Dis. 2015, 30, 127–130. [Google Scholar] [CrossRef] [PubMed]
- O’Grady, T.J.; Gates, M.A.; Boscoe, F.P. Thyroid cancer incidence attributable to overdiagnosis in the United States 1981-2011. Int. J. Cancer 2015, 137, 2664–2673. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; Wang, L.; Dai, S.; Chen, M.; Li, F.; Sun, J.; Luo, F. Epidemiologic Trends of and Factors Associated with Overall Survival for Patients With Gastroenteropancreatic Neuroendocrine Tumors in the United States. JAMA Netw. Open 2021, 4, e2124750. [Google Scholar] [CrossRef] [PubMed]

| Histotype | Incidence * | Main Negative Pathologic Prognostic Factors | Overall 5-Year Survival in Advanced Disease | Described Association with Inflammatory Bowel Diseases? | Putative Altered Genes |
|---|---|---|---|---|---|
| Lymphoma | 1/50,000 | Involvement of loco-regional lymph-nodes co-mutations of MYC and BCL2 | 40% | Yes | MYC, BCL2, translocations: API2 (11q21), BCL2 (18q21), BCL6 (3q27), IGH (14q32), IGK (2p12), IGL (22q11), MYC (8q24), and MALT1 (18q21) |
| GIST (Gastro-Intestinal Stromal Tumor) | 1/100,000 | Size > 2 cm high mitotic index | 50% | No | BRAF, KIT, PDGFRA, K- N-RAS, SDH |
| Well-differentiated neuroendocrine tumor | 1/100,000 | Size > 2 cm high mitotic index | 15% | No | ATM, CDKN2A, EGFR, ERBB4, FBXW7, KIT, MET, PTEN, K- N-RAS, RB-1, SMAD4, TP53 (commonly mutated genes). Others: AKT1, ALK, BRAF, CTNNB1, ERBB2, EZH2, FLT3, HNF1A, IDH1, RET, SMARCB1, SMO, STK11, VHL |
| Signet ring cell | 1/125,000 | Involvement of loco-regional lymph-nodes | <5% | Yes | APC, PIK3CA, K- N- RAS, TP53 (lower compared to adenocarcinoma) |
| Small cell carcinoma | 1/250,000 | Involvement of loco-regional lymph-nodes | 5% | Yes | TP53 |
| Adenosquamous carcinoma | 1/375,000 | Involvement of loco-regional lymph-nodes High percent of squamous cell component | 10% | Yes | Unknown |
| Non-GIST mesenchymal tumor | 1/500,000 | High mitotic index | 5% | No | Amplifications of CDK4, HMGA2, MDM2, SAS, of 1q21–24, 6q22–24, 20q13, 12q24 regions, deletions of 13q14–21 or 11q22–23. TP53 |
| Medullary carcinoma | 1/3,000,000 | Involvement of loco-regional lymph-nodes | Not definable *** | Yes | ARID1A, BRAF, CDX2, GBP1, GBP4, GBP5, IDO1, MLH1, PD-1, PD-L1, WARS |
| Goblet cell adenocarcinoma | 1/10,000,000 | High mitotic index | 18% | No | BRAF, CTNNA1, ERBB2, NOTCH1, NUMA1, TGFBR2, TP53, USP9X |
| Angiosarcoma | Unknown ** | Involvement of loco-regional lymph-nodes | 10% | No | Unknown |
| Melanoma | Unknown ** | Involvement of loco-regional lymph-nodes | 5% | No | BRAF, NRAS (mutations are less frequent compared to cutaneous melanomas). BRCA1, HRAS, KIT, MLH1, NF1, PDGFRA, SF3B1 |
| Plasmacytoma | Unknown ** | Involvement of loco-regional lymph-nodes High mitotic index | 70% | No | Unknown |
| Squamous cell carcinoma | Unknown ** | Involvement of loco-regional lymph-nodes | 30% | Yes | Unknown |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ottaiano, A.; Santorsola, M.; Perri, F.; Pace, U.; Marra, B.; Correra, M.; Sabbatino, F.; Cascella, M.; Petrillo, N.; Ianniello, M.; et al. Clinical and Molecular Characteristics of Rare Malignant Tumors of Colon and Rectum. Biology 2022, 11, 267. https://doi.org/10.3390/biology11020267
Ottaiano A, Santorsola M, Perri F, Pace U, Marra B, Correra M, Sabbatino F, Cascella M, Petrillo N, Ianniello M, et al. Clinical and Molecular Characteristics of Rare Malignant Tumors of Colon and Rectum. Biology. 2022; 11(2):267. https://doi.org/10.3390/biology11020267
Chicago/Turabian StyleOttaiano, Alessandro, Mariachiara Santorsola, Francesco Perri, Ugo Pace, Bruno Marra, Marco Correra, Francesco Sabbatino, Marco Cascella, Nadia Petrillo, Monica Ianniello, and et al. 2022. "Clinical and Molecular Characteristics of Rare Malignant Tumors of Colon and Rectum" Biology 11, no. 2: 267. https://doi.org/10.3390/biology11020267
APA StyleOttaiano, A., Santorsola, M., Perri, F., Pace, U., Marra, B., Correra, M., Sabbatino, F., Cascella, M., Petrillo, N., Ianniello, M., Casillo, M., Misso, G., Delrio, P., Caraglia, M., & Nasti, G. (2022). Clinical and Molecular Characteristics of Rare Malignant Tumors of Colon and Rectum. Biology, 11(2), 267. https://doi.org/10.3390/biology11020267









