Escherichia coli of Ready-to-Eat (RTE) Meats Origin Showed Resistance to Antibiotics Used by Farmers
Abstract
1. Introduction
2. Results
2.1. Demographic Characteristics and Livestock Species Reared by Farmers
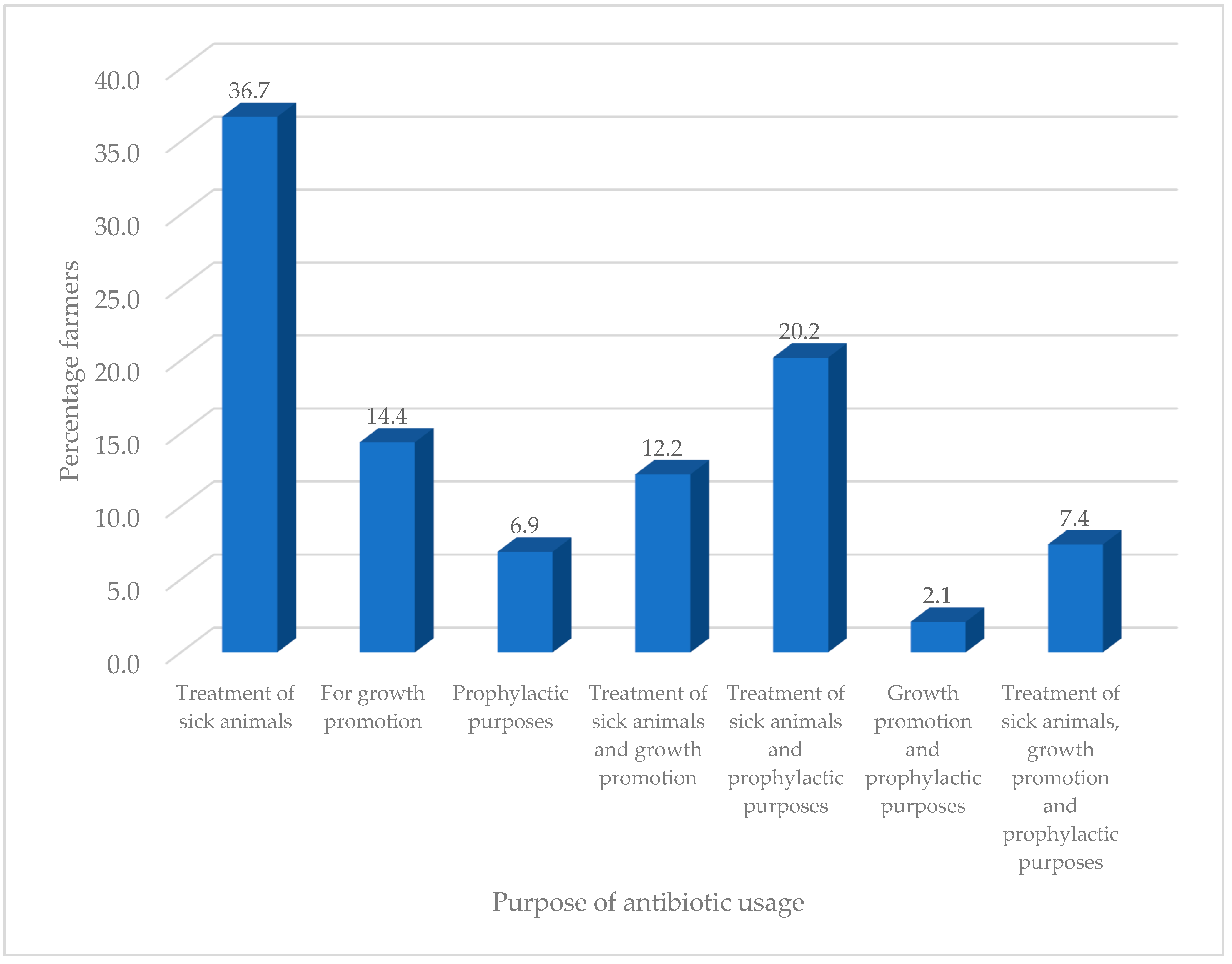
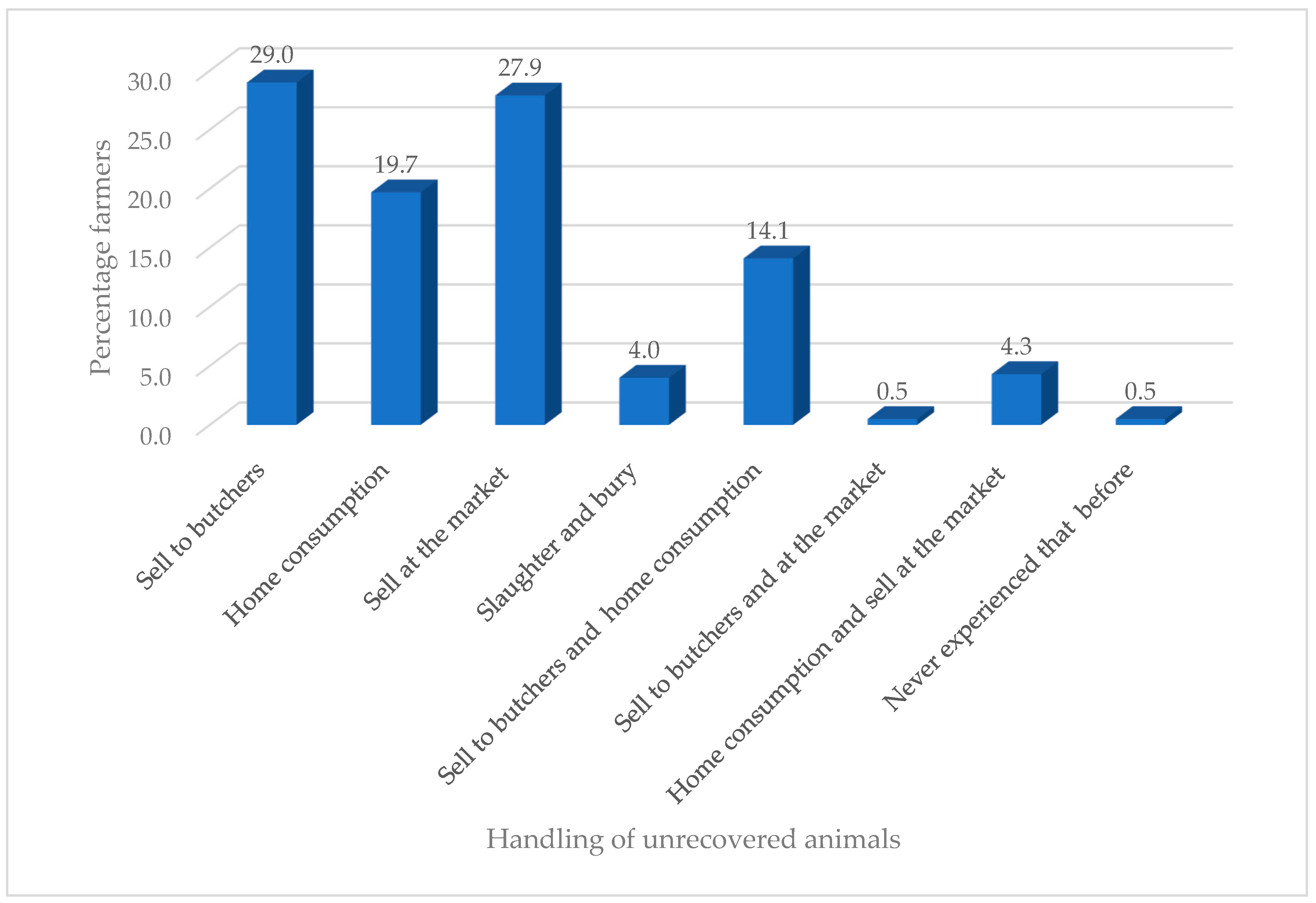
2.2. Usage of Antibiotics by Livestock Farmers
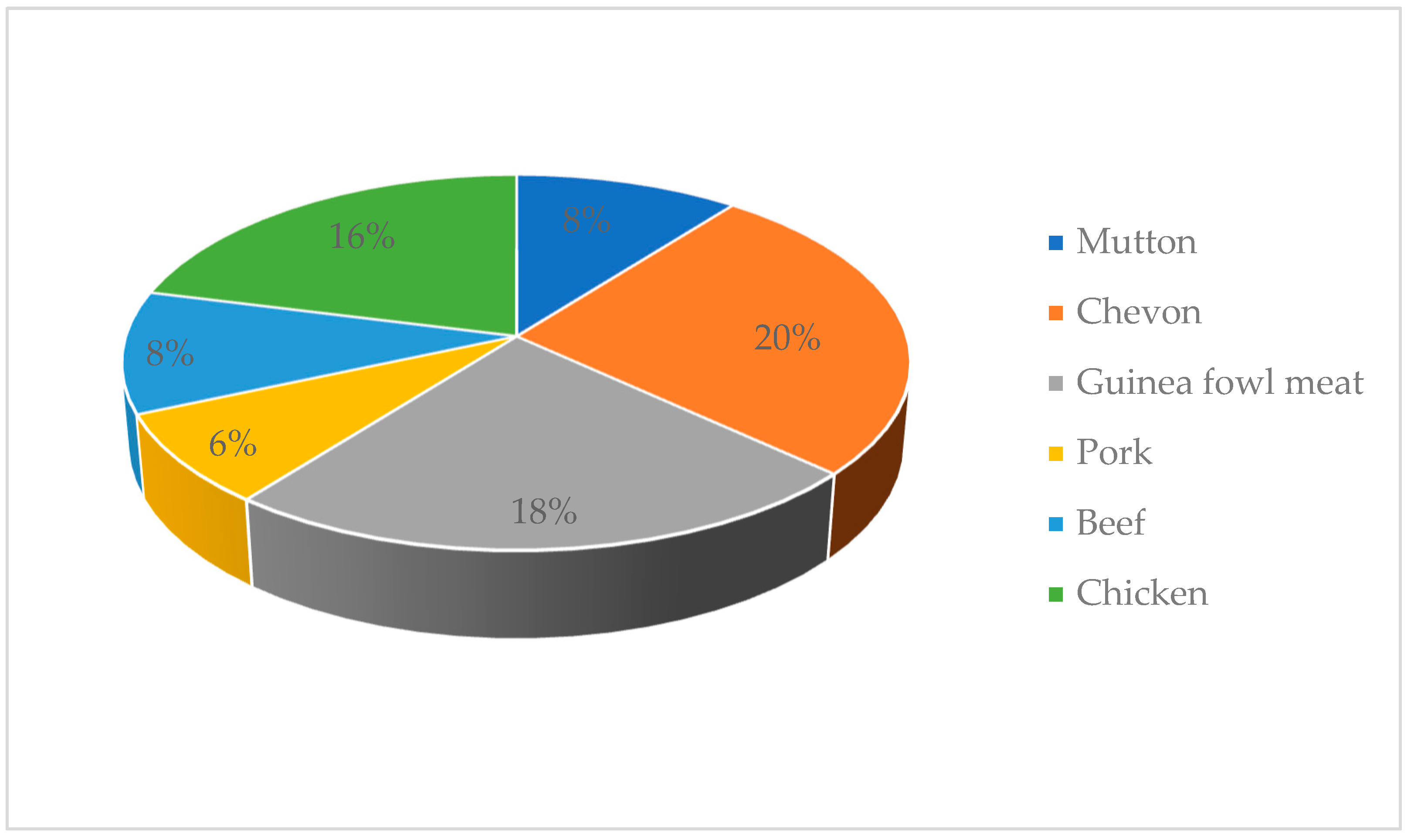
2.3. Prevalence of E. coli in Ready-to-Eat Meats
2.4. Antibiotic Resistance of E. coli from RTE Meats
2.5. Multidrug Resistance of Individual E. coli Isolates
3. Discussions
4. Materials and Methods
4.1. Study Area
4.2. Study Population, Sample Size and Sampling Method
4.3. Structure of Questionnaire
4.4. Sampling of Ready-to-Eat Meats
4.5. Isolation and Confirmation of E. coli
4.6. Antimicrobial Susceptibility Test
4.7. Analysis of Data
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- McAfee, A.J.; McSorley, E.M.; Cuskelly, G.J.; Moss, B.W.; Wallace, J.M.; Bonham, M.P.; Fearon, A.M. Red meat consumption: An overview of the risks and benefits. Meat Sci. 2010, 84, 1–13. [Google Scholar] [CrossRef]
- Rao, V.A.; Thulasi, G.; Ruban, S.W. Meat quality characteristics of non-descript buffalo as affected by age and sex. World Appl. Sci. J. 2009, 6, 1058–1065. [Google Scholar]
- Akbar, A.; Anal, A.K. Food safety concerns and food-borne pathogens, Salmonella, Escherichia coli and Campylobacter. FUUAST J. Biol. 2011, 1, 5–17. [Google Scholar]
- Hughes, C.; Gillespie, I.A.; O‘Brien, S.J. The breakdowns in food safety group. foodborne transmission of infectious intestinal disease in England and Wales, 1992–2003. Food Control 2007, 18, 766–772. [Google Scholar] [CrossRef]
- Akanele, A.E.; Chukwu, U.S.M.O.; Ahudie, B.C.M. Microbiological contamination of food: the mechanisms, impacts and prevention. Int. J. Sci. Tech. Res. 2016, 5, 65–79. [Google Scholar]
- Adzitey, F. Incidence and antimicrobial susceptibility of Escherichia coli isolated from beef (meat muscle, liver and kidney) samples in Wa Abattoir, Ghana. Cogent Food Agric. 2020, 6, 2–10. [Google Scholar] [CrossRef]
- Yousef, A.E.; Balasubramaniam, V.M. Physical methods of food preservation. In Food Microbiology: Fundamentals and Frontiers, 4th ed.; Doyle, M.P., Buchanan, R.L., Eds.; ASM Press: Washington, DC, USA, 2012. [Google Scholar]
- Henriques, A.R.; Fraqueza, M.J. Listeria monocytogenes and ready-to-eat meat-based food products: Incidence and control. In Listeria Monocytogenes: Incidence, Growth Behavior and Control, 1st ed.; Nova Science Publishers: New York, NY, USA, 2015; pp. 71–103. [Google Scholar]
- Mor-Mur, M.; Yuste, J. Emerging bacterial pathogens in meat and poultry: An overview. Food Biop. Tech. 2010, 3, 24. [Google Scholar] [CrossRef]
- Syne, S.-M.; Ramsubhag, A.; Adesiyun, A.A. Microbiological hazard analysis of ready-to-eat meats processed at a food plant in Trinidad, West Indies. Infect. Ecol. Epid. 2013, 3, 1. [Google Scholar] [CrossRef]
- Adzitey, F.; Ekli, R.; Abu, A. Prevalence and antibiotic susceptibility of Staphylococcus aureus isolated from raw and grilled beef in Nyankpala community in the Northern Region of Ghana. Cogent Food Agric. 2019, 5, 1671115. [Google Scholar] [CrossRef]
- Adzitey, F.; Ekli, R.; Aduah, M. Incidence and antibiotic susceptibility of Staphylococcus aureus isolated from ready-to-eat meats in the environs of Bolgatanga Municipality of Ghana. Cogent Environ. Sci. 2020, 6, 1791463. [Google Scholar] [CrossRef]
- Pitout, J. Extraintestinal pathogenic Escherichia coli: A combination of virulence with antibiotic resistance. Front. Microbial. 2012, 3, 9. [Google Scholar] [CrossRef] [PubMed]
- Painter, J.A.; Hoekstra, R.M.; Ayers, T.; Tauxe, R.V.; Braden, C.R.; Angulo, F.J.; Griffin, P.M. Attribution of foodborne illnesses, hospitalizations, and deaths to food commodities by using outbreak data, United States, 1998–2008. Emerg. Infect. Dis. 2013, 19, 407. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. E. coli. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/e-coli (accessed on 9 September 2020).
- Rane, S. Street vended food in developing world: Hazard analyses. Indian J. Microbiol. 2011, 51, 100–106. [Google Scholar] [CrossRef] [PubMed]
- Agbodaze, D.; Nmai, P.N.; Robertson, F.; Yeboah-Manu, D.; Owusu-Darko, K.; Addo, K. Microbiological quality of khebab consumed in the Accra metropolis. Ghana Med. J. 2015, 39, 46–49. [Google Scholar] [CrossRef] [PubMed]
- Abakari, G.; Cobbina, S.J.; Yeleliere, E. Microbial quality of ready-to-eat vegetable salads vended in the central business district of Tamale, Ghana. Int. J. Food Cont. 2018, 5, 3. [Google Scholar] [CrossRef]
- Ofosu, A.H.; Dzigbede, B.A.; Agidi, J.E.L.; Adjei, J.; Koranteng, A. A study into microbial quality of ready to eat foods sold in the Sunyani Municipality of Ghana. Glob. J. Biol. Agric. Health Sci. 2014, 3, 84–91. [Google Scholar]
- Adzitey, F.; Teye, G.A.; Anachinaba, I.A. Microbial quality of fresh and smoked guinea fowl meat sold in the Bolgatanga Municipality, Ghana. Asian J. Poult. Sci. 2015, 9, 165–171. [Google Scholar] [CrossRef][Green Version]
- Pelaez, F. The historical delivery of antibiotics from microbial natural products—Can history repeat? Biochem. Pharm. 2006, 71, 981–990. [Google Scholar] [CrossRef]
- Ventola, C.L. The antibiotic resistance crisis: Part 1: Causes and threats. Pharm. Therap. 2015, 40, 277. [Google Scholar]
- Smith, D.L.; Harris, A.D.; Johnson, J.A.; Silbergeld, E.K.; Morris, J.G. Animal antibiotic use has an early but important impact on the emergence of antibiotic resistance in human commensal bacteria. Proc. Nat. Acad. Sci. USA 2002, 99, 6434–6439. [Google Scholar] [CrossRef]
- Huijbers, P.M.C. Transmission of Antibiotic Resistance from Animals to Humans: Broilers as a Reservoir of ESBL-Producing Bacteria. Ph.D. Thesis, Wageningen University, Wageningen, The Netherlands, 2016. Available online: https://research.wur.nl/en/publications/transmission-of-antibiotic-resistance-from-animals-to-humans-broi (accessed on 5 November 2020).
- Muloi, D.; Ward, M.J.; Pedersen, A.B.; Fèvre, E.M.; Woolhouse, M.E.J.; van Bunnik, B.A.D. Are food animals responsible for transfer of antimicrobial-resistant Escherichia coli or their resistance determinants to human populations? A systematic review. Foodborne Path. Dis. 2018, 15, 467–474. [Google Scholar] [CrossRef] [PubMed]
- Adesokan, H.K.; Akanbi, I.O.; Akanbi, I.M.; Obaweda, R.A. Pattern of antimicrobial usage in livestock animals in south-western Nigeria: The need for alternative plans. Onderstepoort J. Vet. Res. 2015, 82, 1–6. [Google Scholar] [CrossRef]
- Katakweba, A.A.S.; Mtambo, M.M.A.; Olsen, J.E.; Muhairwa, A.P. Awareness of human health risks associated with the use of antibiotics among livestock keepers and factors that contribute to selection of antibiotic resistance bacteria within livestock in Tanzania. Livest. Res. Rur. Dev. 2012, 24, 170. [Google Scholar]
- Akansale, R.; Adzitey, F.; Teye, G. Knowledge of farmers in antibiotic usage and investigation of antibiotic residues in meats in the Sunyani Municipality of Ghana. J. Food Safe. Hyg. 2019, 5, 155–164. [Google Scholar]
- Ozturk, Y.; Celik, S.; Sahin, E.; Acik, M.N.; Cetinkaya, B. Assessment of farmers’ knowledge, attitudes and practices on antibiotics and antimicrobial resistance. Animals 2019, 9, 653. [Google Scholar] [CrossRef] [PubMed]
- Ferdous, J.; Sachi, S.; Noman, Z.A.; Hussani, S.M.A.K.; Sarker, Y.A.; Sikder, M.H. Assessing farmers’ perspective on antibiotic usage and management practices in small-scale layer farms of Mymensingh district, Bangladesh. Vet. World. 2019, 2, 1441. [Google Scholar] [CrossRef]
- Oluwasile, B.B.; Agbaje, M.; Ojo, O.E.; Dipeolu, M.A. Antibiotic usage pattern in selected poultry farms in Ogun state. Sokoto J. Vet. Sci. 2014, 12, 45–50. [Google Scholar] [CrossRef]
- World Health Organization and WHO Advisory Group on Integrated Surveillance of Antimicrobial Resistance. Critically Important Antimicrobials for human Medicine: Ranking of Antimicrobial Agents for Risk Management of Antimicrobial Resistance Due to non-Human Use, 5th rev. World Health Organization. 2017. Available online: https://apps.who.int/iris/handle/10665/255027 (accessed on 9 September 2020).
- Nobili, G.; Franconieri, I.; La Bella, G.; Basanisi, M.G.; La Salandra, G. Prevalence of verocytotoxigenic Escherichia coli strains isolated from raw beef in southern Italy. Int. J. Food Microbiol. 2017, 257, 201–205. [Google Scholar] [CrossRef]
- Rajpura, A.; Lamden, K.; Forster, S.; Clarke, S.; Cheesbrough, J.; Gornall, S.; Waterworth, S. Large outbreak of infection with Escherichia coli O157 PT21/28 in Eccleston, Lancashire, due to cross contamination at a butcher’s counter. Com. Dis. Pub. Health 2003, 6, 279–284. [Google Scholar]
- CDC (2015) Foodborne outbreak online database (FOOD). Centers for Disease Control and Prevention, Atlanta. Available online: http://wwwn.cdc.gov/foodborneoutbreaks/ (accessed on 3 February 2016).
- Hassanin, F.S.; Reham, A.A.; Shawky, N.A.; Gomaa, W.M. Incidence of Escherichia coli and Salmonella in ready to eat foods. Benha Vet. Med. J. 2014, 27, 84–91. [Google Scholar]
- Ahmadi, S.A.; Panda, A.K.; Kumar, Y.; Brahmne, H.G. Prevalence of Escherichia coli and Salmonella spp. in ready-to-eat meat and meat products in Himachal Pradesh. J. Com. Dis. 2012, 44, 71–77. [Google Scholar]
- Rahman, M.A.; Rahman, A.K.; Islam, M.A.; Alam, M.M. Antimicrobial resistance of Escherichia coli isolated from milk, beef and chicken meat in Bangladesh Bangl. J. Vet. Med. 2017, 2. [Google Scholar]
- Ciekure, E.; Siksna, I.; Valcina, O.; Viksna, L.; Krumina, A. Microbiological quality of ready-to-eat products and potential risks for consumers in Latvia. Nat. Exact Appl. Sci. 2016, 70, 245–251. [Google Scholar]
- EFSA and ECDC (European Food Safety Authority and European Centre for Disease Prevention and Control). The European Union summary report on trends and sources of zoonoses, zoonotic agents and food-borne outbreaks in 2017. EFSA J. 2018, 16, 262. [Google Scholar]
- Chopra, I.; Roberts, M. Tetracycline antibiotics: Mode of action, applications, molecular biology, and epidemiology of bacterial resistance. Microbiol. Mol. Bio. Rev. 2001, 65, 232–260. [Google Scholar] [CrossRef]
- Hannoodee, E.J.; Wittler, M.M. Amoxicillin Clavulanate. 2020. Available online: https://www.ncbi.nlm.nih.gov/books/NBK538164/ (accessed on 9 September 2020).
- Weinstein, R.A.; Fridkin, S.K. Vancomycin-intermediate and-resistant Staphylococcus aureus: What the infectious disease specialist needs to know. Clin. Infect. Dis. 2001, 32, 108–115. [Google Scholar] [CrossRef]
- Adzitey, F.; Rusul, G.; Huda, N.; Cogan, T.; Corry, J. Prevalence, antibiotic resistance and RAPD typing of Campylobacter species isolated from ducks, duck rearing and processing environments in Penang, Malaysia. Int. J. Food Microbiol. 2012, 154, 197–205. [Google Scholar] [CrossRef]
- Fair, R.J.; Tor, Y. Antibiotics and bacterial resistance in the 21st century. Perspect. Med. Chem. 2014, 6, 25–64. [Google Scholar] [CrossRef]
- Harakeh, S.; Yassine, H.; Gharios, M.; Barbour, E.; Hajjar, S.; El-Fadel, M.; Toufeili, I.; Tannous, R. Isolation, molecular characterization and antibiotic resistance patterns of Salmonella and Escherichia coli isolates from meat-based fast food in Lebanon. Sci. Total Environ. 2005, 341, 33–44. [Google Scholar] [CrossRef]
- Heredia, N.; García, S. Animals as sources of food-borne pathogens: A review. Anim. Nutr. 2018, 4, 250–255. [Google Scholar] [CrossRef]
- Ghana Statistical Service. Population and Housing Census. 2012. Available online: https://www.statsghana.gov.gh/gssmain/storage/img/marqueeupdater/Census2010_Summary_report_of_final_results.pdf (accessed on 9 September 2020).
- Anonymous. Sample Size Calculator. 2020. Available online: https://www.calculator.net/sample-size-calculator.html?type=1&cl=95&ci=5&pp=50&ps=66685&x=39&y=22 (accessed on 23 August 2019).
- Feng, P.; Weagant, S.D.; Jinneman, K. Bacteriological Analytical Manuel Chapter 4A: Diarrheagenic Escherichia coli. Available online: https://www.fda.gov/food/laboratory-methods-food/bam-chapter-4a-diarrheagenic-escherichia-coli (accessed on 23 April 2019).
- Bauer, A.W.; Kirby, W.M.M.; Sherris, J.C.; Turk, M. Antibiotic susceptibility testing by a standardized single disc method. American J. Clin. Pathol. 1966, 45, 493–496. [Google Scholar] [CrossRef]
- Clinical and Laboratory Standard Institute. Document M31-A3. In Performance Standards for Antimicrobial Disk and Dilution Susceptibility Tests for Bacteria Isolated from Animals, Approved Standard, 3rd ed.; Wayne: Pennsylvania, PA, USA, 2017. [Google Scholar]
| Variable | Frequency | Percentage |
|---|---|---|
| Gender | ||
| Male | 280 | 74.5 |
| Female | 96 | 25.5 |
| Age | ||
| 20–29 | 48 | 12.8 |
| 30–39 | 107 | 28.5 |
| 40–49 | 103 | 27.4 |
| 50–60 | 84 | 22.3 |
| 61 and above | 34 | 9.0 |
| Educational status | ||
| Nonformal | 89 | 23.7 |
| Primary | 60 | 16.0 |
| Junior high | 54 | 14.4 |
| Senior high | 50 | 13.3 |
| Tertiary | 114 | 30.3 |
| Others | 9 | 2.4 |
| Years in livestock business | ||
| 0–11 months | 24 | 6.4 |
| 1–2 years | 61 | 16.2 |
| 3–5 years | 101 | 26.9 |
| 6–10 years | 119 | 31.6 |
| More than 10 years | 71 | 18.9 |
| Species of animals reared | ||
| Sheep | 247 | 65.7 |
| Chicken | 246 | 65.4 |
| Goats | 243 | 64.6 |
| Cattle | 177 | 47.1 |
| Guinea fowls | 175 | 46.5 |
| Pigs | 93 | 24.7 |
| Variable | Frequency | Percentage |
|---|---|---|
| Have you ever encountered infections on your farm? | ||
| Yes | 349 | 92.8 |
| No | 27 | 7.2 |
| Did you consult a veterinarian? | ||
| Yes | 292 | 77.7 |
| No | 84 | 22.3 |
| Which antibiotics did you use? | ||
| Gentamicin | 27 | 7.2 |
| Tetracycline | 104 | 27.7 |
| Amoxicillin/clavulanic acid | 70 | 18.6 |
| Trimethoprim/sulfamethoxazole | 44 | 11.7 |
| Ciprofloxacin | 29 | 7.7 |
| Erythromycin | 16 | 4.3 |
| Chloramphenicol | 37 | 9.8 |
| Penicillin | 16 | 4.3 |
| Herbal drug | 33 | 8.8 |
| Who recommended the antibiotics? | ||
| Colleague farmers | 132 | 35.1 |
| Veterinarians | 119 | 31.6 |
| Drug sellers | 68 | 18.1 |
| Colleague farmers and veterinarians | 14 | 3.7 |
| Colleague farmers and drug sellers | 26 | 6.9 |
| Drug sellers and veterinarians | 8 | 2.1 |
| Colleague farmers, drug sellers and veterinarians | 9 | 2.4 |
| Would you say you have knowledge of antibiotics usage? | ||
| Yes | 211 | 56.1 |
| No | 165 | 43.9 |
| Where did you get the information from? | ||
| Extension officers | 56 | 14.9 |
| Nongovernmental organization (NGO) | 45 | 12.0 |
| Colleague farmers | 123 | 32.7 |
| Veterinary staff | 82 | 21.8 |
| Extension officers and NGO | 10 | 2.7 |
| Extension officers and colleague farmers | 27 | 7.2 |
| Extension and veterinary staff | 8 | 2.1 |
| NGO and colleague farmers | 15 | 4.0 |
| NGO and veterinary staff | 3 | 0.8 |
| Extension officers, NGO, colleague farmers and veterinary staff | 7 | 1.9 |
| Have you ever treated your animals yourself? | ||
| Yes | 254 | 67.6 |
| No | 122 | 32.4 |
| Did you observe safety and dosage instructions? | ||
| Yes | 271 | 72.1 |
| No | 105 | 27.9 |
| Do you follow antibiotic withdrawal period instructions? | ||
| Yes | 247 | 65.7 |
| No | 129 | 34.3 |
| Antimicrobial | %R | %I | %S |
|---|---|---|---|
| Amoxicillin/clavulanic acid 30 µg (Amc) | 70.97 | 0.00 | 29.03 |
| Azithromycin 15 µg (Azm) | 70.97 | 16.13 | 12.90 |
| Ceftriaxone 30 µg (Cro) | 19.35 | 22.58 | 58.06 |
| Chloramphenicol 30 µg (C) | 6.45 | 0.00 | 93.55 |
| Ciprofloxacin 5 µg (Cip) | 22.58 | 16.13 | 61.29 |
| Gentamicin 10 µg (CN) | 22.58 | 38.71 | 38.71 |
| Teicoplanin 30 µg (Tec) | 96.77 | 0.00 | 3.23 |
| Tetracycline 30 µg (Te) | 93.55 | 6.45 | 0.00 |
| Sulfamethoxazole/trimethoprim (Sxt) | 58.06 | 25.81 | 16.13 |
| Code | Sources | Number of Antibiotics | Antibiotic Resistance Profile | MAR Index |
|---|---|---|---|---|
| GO18 | Goat | 7 | CipAmcAzmTecTeCSxt | 0.78 |
| P12 | Pig | 7 | AzmTecCnTeCCroSxt | 0.78 |
| C17 | Chicken meat | 7 | AmcAzmTecCnTeCroSxt | 0.78 |
| GO4 | Goat | 6 | AmcAzmTecTeCroSxt | 0.67 |
| P5 | Pig | 6 | CipAmcTecCnTeSxt | 0.67 |
| B7 | Beef | 6 | CipAmcAzmTecTeSxt | 0.67 |
| C19 | Chicken meat | 6 | AmcAzmTecCnTeSxt | 0.67 |
| GO1 | Goat | 5 | CipAmcTecTeCro | 0.56 |
| GO16 | Goat | 5 | AmcAzmTecCnTe | 0.56 |
| S26 | Sheep | 5 | AzmTecTeCroSxt | 0.56 |
| G33 | Guinea fowl | 5 | AmcTecTeCroSxt | 0.56 |
| B37 | Beef | 5 | AmcAzmTecTeSxt | 0.56 |
| C7 | Beef | 5 | AmcTecCnTeSxt | 0.56 |
| C13 | Chicken meat | 5 | AmcAzmTecTeSxt | 0.56 |
| C18 | Chicken meat | 5 | AmcAzmTecTeSxt | 0.56 |
| C20 | Chicken meat | 5 | AmcAzmTecTeSxt | 0.56 |
| C23 | Chicken meat | 5 | CipAmcAzmTecTe | 0.56 |
| GO30 | Goat | 4 | AzmTecTeSxt | 0.44 |
| GO40 | Goat | 4 | AmcAzmTecTe | 0.44 |
| S11 | Goat | 4 | AzmTecTeSxt | 0.44 |
| G11 | Pig | 4 | CipAmcAzmTec | 0.44 |
| B4 | Guinea fowl | 4 | AmcAzmTecSxt | 0.44 |
| B49 | Beef | 4 | CipAmcAzmTe | 0.44 |
| C15 | Chicken meat | 4 | AmcAzmTecTe | 0.44 |
| G046 | Goat | 3 | AmcAzmSxt | 0.33 |
| GO49 | Goat | 3 | AzmTecTe | 0.33 |
| P3 | Sheep | 3 | TecTeSxt | 0.33 |
| G14 | Guinea fowl | 3 | AzmTecTe | 0.33 |
| G30 | Guinea fowl | 3 | TecCnTe | 0.33 |
| GO6 | Goat | 2 | TecTe | 0.22 |
| S3 | Sheep | 2 | TecTe | 0.22 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Abass, A.; Adzitey, F.; Huda, N. Escherichia coli of Ready-to-Eat (RTE) Meats Origin Showed Resistance to Antibiotics Used by Farmers. Antibiotics 2020, 9, 869. https://doi.org/10.3390/antibiotics9120869
Abass A, Adzitey F, Huda N. Escherichia coli of Ready-to-Eat (RTE) Meats Origin Showed Resistance to Antibiotics Used by Farmers. Antibiotics. 2020; 9(12):869. https://doi.org/10.3390/antibiotics9120869
Chicago/Turabian StyleAbass, Abdulai, Frederick Adzitey, and Nurul Huda. 2020. "Escherichia coli of Ready-to-Eat (RTE) Meats Origin Showed Resistance to Antibiotics Used by Farmers" Antibiotics 9, no. 12: 869. https://doi.org/10.3390/antibiotics9120869
APA StyleAbass, A., Adzitey, F., & Huda, N. (2020). Escherichia coli of Ready-to-Eat (RTE) Meats Origin Showed Resistance to Antibiotics Used by Farmers. Antibiotics, 9(12), 869. https://doi.org/10.3390/antibiotics9120869






