Meropenem/Vaborbactam—A Mechanistic Review for Insight into Future Development of Combinational Therapies
Abstract
1. Introduction
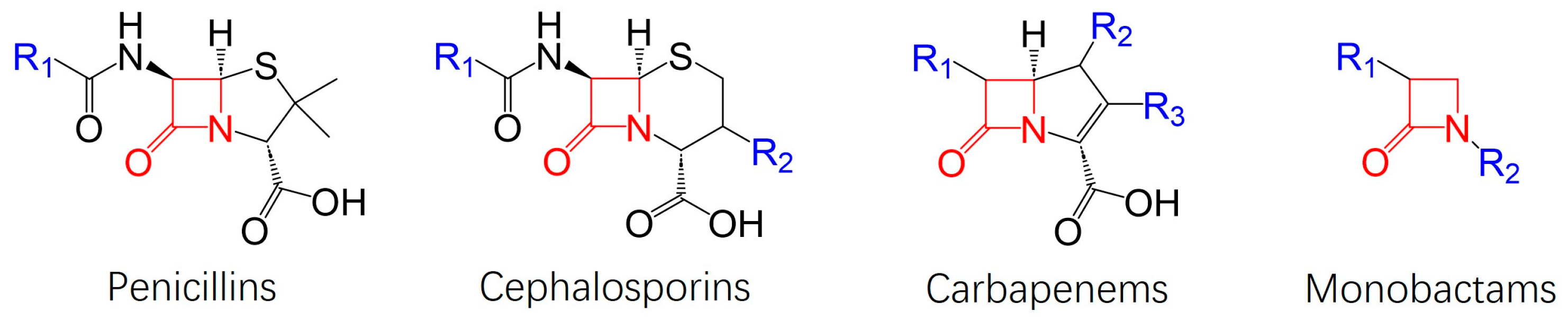
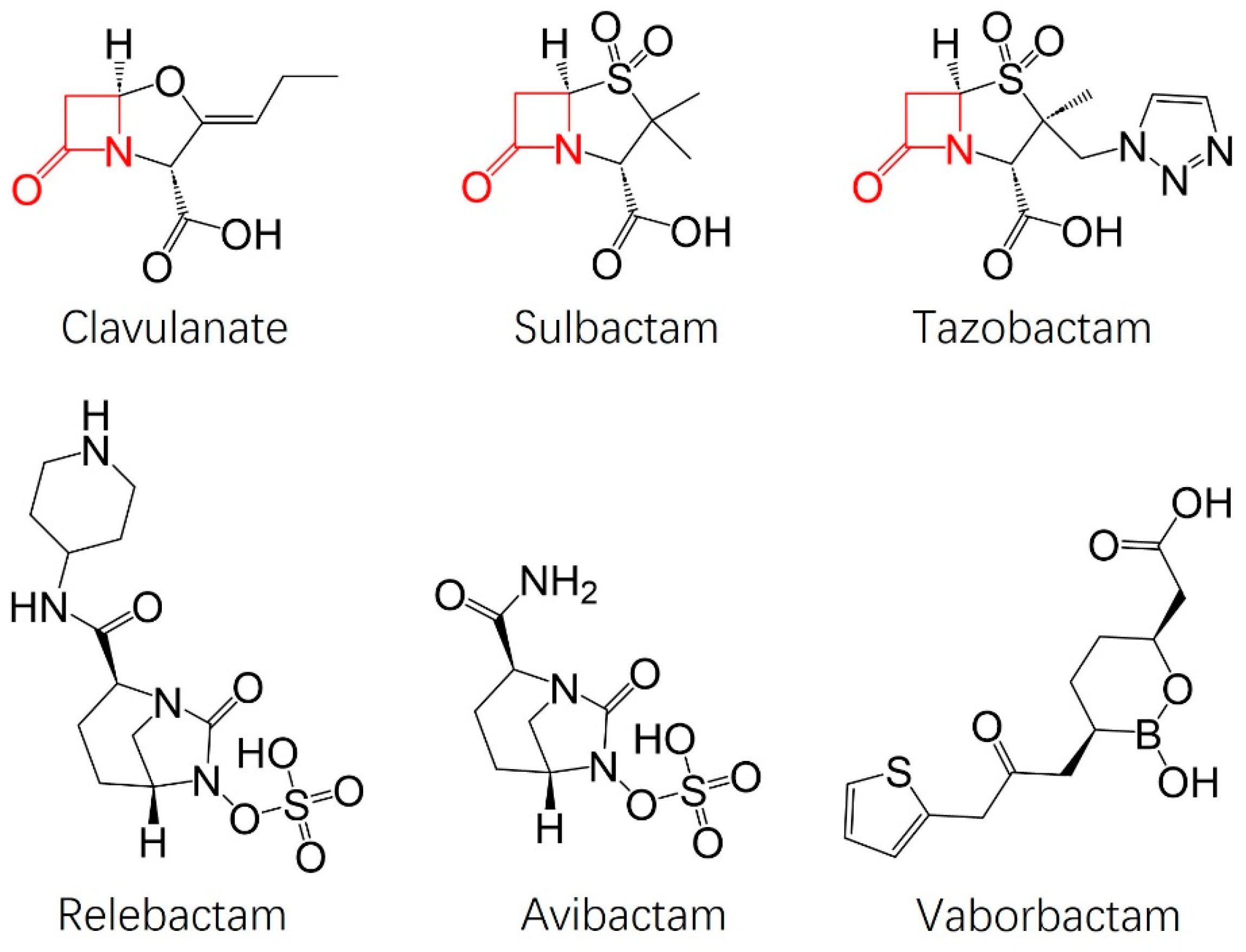
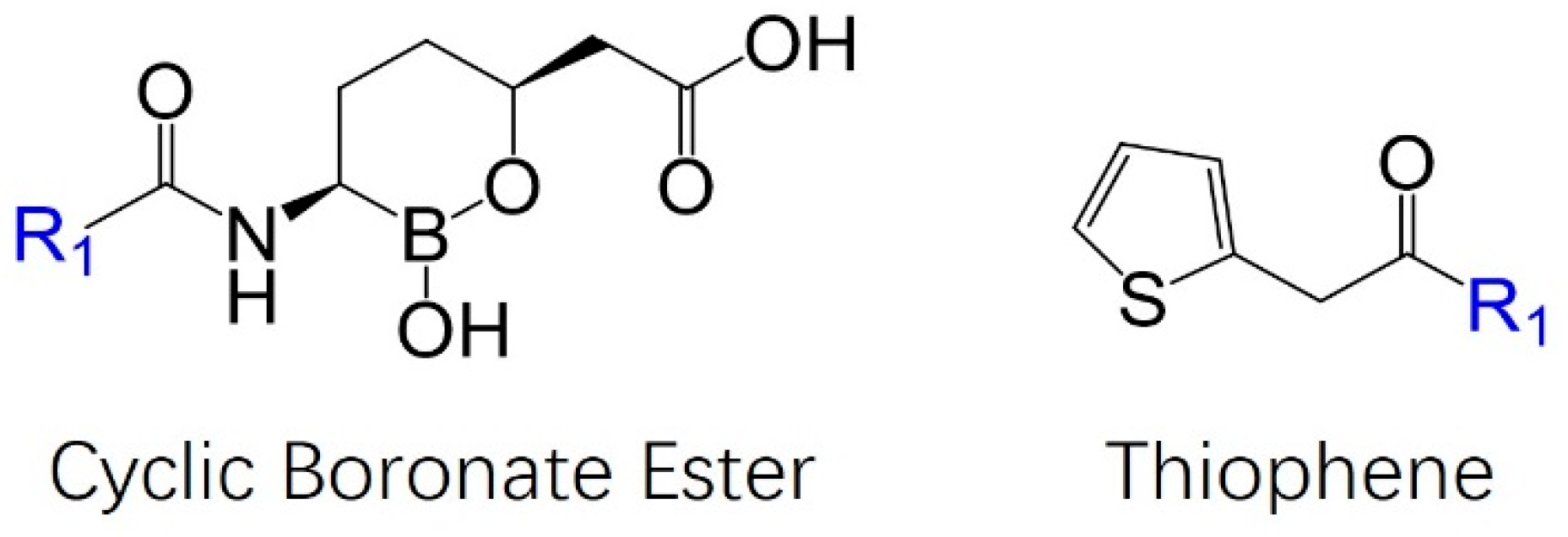
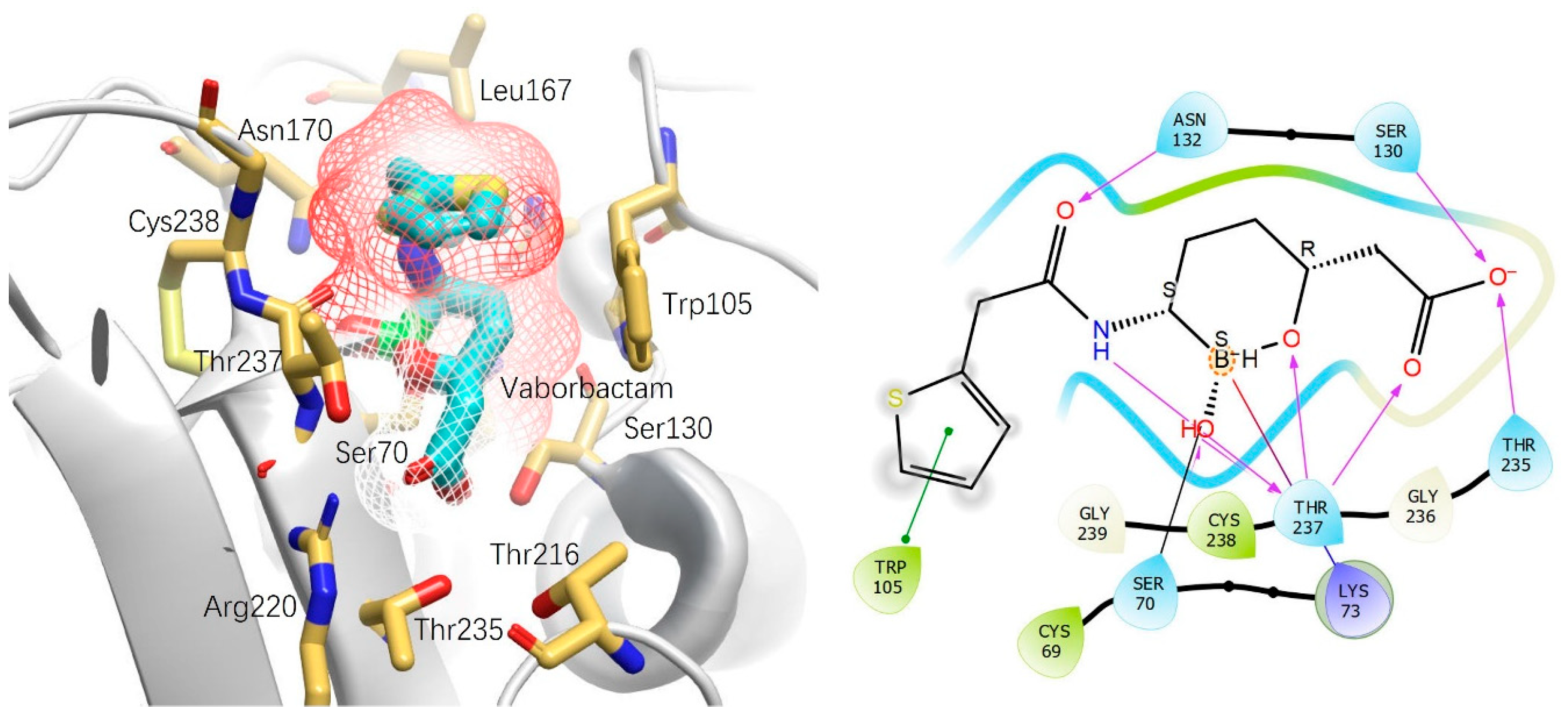
2. Structural Development of Vaborbactam
Clinical Use and PD/PK Data
3. Discussion and Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pandey, N.; Cascella, M. Beta Lactam Antibiotics. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2021. [Google Scholar]
- Gaynes, R. The Discovery of Penicillin—New Insights after More Than 75 Years of Clinical Use. Emerg. Infect. Dis. 2017, 23, 849–853. [Google Scholar] [CrossRef]
- Thakuria, B.; Lahon, K. The Beta Lactam Antibiotics as an Empirical Therapy in a Developing Country: An Update on Their Current Status and Recommendations to Counter the Resistance against Them. J. Clin. Diagn. Res. JCDR 2013, 7, 1207–1214. [Google Scholar] [CrossRef] [PubMed]
- Lupoli, T.J.; Tsukamoto, H.; Doud, E.H.; Wang, T.-S.A.; Walker, S.; Kahne, D. Transpeptidase-Mediated Incorporation of D-Amino Acids into Bacterial Peptidoglycan. J. Am. Chem. Soc. 2011, 133, 10748–10751. [Google Scholar] [CrossRef]
- Bush, K.; Bradford, P.A. β-Lactams and β-Lactamase Inhibitors: An Overview. Cold Spring Harb. Perspect. Med. 2016, 6, a025247. [Google Scholar] [CrossRef] [PubMed]
- Popham, D.L.; Young, K.D. Role of Penicillin-Binding Proteins in Bacterial Cell Morphogenesis. Curr. Opin. Microbiol. 2003, 6, 594–599. [Google Scholar] [CrossRef] [PubMed]
- Auer, G.K.; Weibel, D.B. Bacterial Cell Mechanics. Biochemistry 2017, 56, 3710–3724. [Google Scholar] [CrossRef] [PubMed]
- Zeng, X.; Lin, J. Beta-Lactamase Induction and Cell Wall Metabolism in Gram-Negative Bacteria. Front. Microbiol. 2013, 4, 128. [Google Scholar] [CrossRef] [PubMed]
- Lobanovska, M.; Pilla, G. Penicillin’s Discovery and Antibiotic Resistance: Lessons for the Future? Yale J. Biol. Med. 2017, 90, 135–145. [Google Scholar] [PubMed]
- Rosenblatt-Farrell, N. The Landscape of Antibiotic Resistance. Environ. Health Perspect. 2009, 117, A244–A250. [Google Scholar] [CrossRef]
- Dever, L.A.; Dermody, T.S. Mechanisms of Bacterial Resistance to Antibiotics. Arch. Intern. Med. 1991, 151, 886–895. [Google Scholar] [CrossRef]
- Benin, B.M.; Hillyer, T.; Shin, W.S. Quercetin, A Potential Metallo-β-Lactamase Inhibitor for Use in Combination Therapy Against β-Lactam Antibiotic-Resistant Bacteria. Open J. Pathol. Toxicol. Res. 2021, 1, 1–5. [Google Scholar]
- Tooke, C.L.; Hinchliffe, P.; Bragginton, E.C.; Colenso, C.K.; Hirvonen, V.H.A.; Takebayashi, Y.; Spencer, J. β-Lactamases and β-Lactamase Inhibitors in the 21st Century. J. Mol. Biol. 2019, 431, 3472–3500. [Google Scholar] [CrossRef] [PubMed]
- Ball, P. The Clinical Development and Launch of Amoxicillin/Clavulanate for the Treatment of a Range of Community-Acquired Infections. Int. J. Antimicrob. Agents 2007, 30, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Khanna, N.R.; Gerriets, V. Beta Lactamase Inhibitors. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2021. [Google Scholar]
- Tsivkovski, R.; Lomovskaya, O. Biochemical Activity of Vaborbactam. Antimicrob. Agents Chemother. 2020, 64, e01935-19. [Google Scholar] [CrossRef] [PubMed]
- Lomovskaya, O.; Sun, D.; Rubio-Aparicio, D.; Nelson, K.; Tsivkovski, R.; Griffith, D.C.; Dudley, M.N. Vaborbactam: Spectrum of Beta-Lactamase Inhibition and Impact of Resistance Mechanisms on Activity in Enterobacteriaceae. Antimicrob. Agents Chemother. 2017, 61, e01443-17. [Google Scholar] [CrossRef] [PubMed]
- Tooke, C.L.; Hinchliffe, P.; Lang, P.A.; Mulholland, A.J.; Brem, J.; Schofield, C.J.; Spencer, J. Molecular Basis of Class A β-Lactamase Inhibition by Relebactam. Antimicrob. Agents Chemother. 2019, 63, e00564-19. [Google Scholar] [CrossRef] [PubMed]
- Swarén, P.; Golemi, D.; Cabantous, S.; Bulychev, A.; Maveyraud, L.; Mobashery, S.; Samama, J.-P. X-ray Structure of the Asn276Asp Variant of the Escherichia coli TEM-1 β-Lactamase: Direct Observation of Electrostatic Modulation in Resistance to Inactivation by Clavulanic Acid. Biochemistry 1999, 38, 9570–9576. [Google Scholar] [CrossRef]
- Cheng, Q.; Xu, C.; Chai, J.; Zhang, R.; Wai chi Chan, E.; Chen, S. Structural Insight into the Mechanism of Inhibitor Resistance in CTX-M-199, a CTX-M-64 Variant Carrying the S130T Substitution. ACS Infect. Dis. 2020, 6, 577–587. [Google Scholar] [CrossRef]
- Shields, R.K.; Potoski, B.A.; Haidar, G.; Hao, B.; Doi, Y.; Chen, L.; Press, E.G.; Kreiswirth, B.N.; Clancy, C.J.; Nguyen, M.H. Clinical Outcomes, Drug Toxicity, and Emergence of Ceftazidime-Avibactam Resistance among Patients Treated for Carbapenem-Resistant Enterobacteriaceae Infections. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2016, 63, 1615–1618. [Google Scholar] [CrossRef]
- Patel, T.S.; Pogue, J.M.; Mills, J.P.; Kaye, K.S. Meropenem–Vaborbactam: A New Weapon in the War against Infections due to Resistant Gram-Negative Bacteria. Future Microbiol. 2018, 13, 971–983. [Google Scholar] [CrossRef]
- Bhowmick, T.; Weinstein, M.P. Microbiology of Meropenem-Vaborbactam: A Novel Carbapenem Beta-Lactamase Inhibitor Combination for Carbapenem-Resistant Enterobacterales Infections. Infect. Dis. Ther. 2020, 9, 757–767. [Google Scholar] [CrossRef] [PubMed]
- Kiener, P.A.; Waley, S.G. Reversible Inhibitors of Penicillinases. Biochem. J. 1978, 169, 197–204. [Google Scholar] [CrossRef] [PubMed]
- Smoum, R.; Rubinstein, A.; Dembitsky, V.M.; Srebnik, M. Boron Containing Compounds as Protease Inhibitors. Chem. Rev. 2012, 112, 4156–4220. [Google Scholar] [CrossRef] [PubMed]
- Hecker, S.J.; Reddy, K.R.; Totrov, M.; Hirst, G.C.; Lomovskaya, O.; Griffith, D.C.; King, P.; Tsivkovski, R.; Sun, D.; Sabet, M.; et al. Discovery of a Cyclic Boronic Acid β-Lactamase Inhibitor (RPX7009) with Utility vs Class A Serine Carbapenemases. J. Med. Chem. 2015, 58, 3682–3692. [Google Scholar] [CrossRef] [PubMed]
- Ness, S.; Martin, R.; Kindler, A.M.; Paetzel, M.; Gold, M.; Jensen, S.E.; Jones, J.B.; Strynadka, N.C.J. Structure-Based Design Guides the Improved Efficacy of Deacylation Transition State Analogue Inhibitors of TEM-1 β-Lactamase. Biochemistry 2000, 39, 5312–5321. [Google Scholar] [CrossRef] [PubMed]
- Structural Basis and Binding Kinetics of Vaborbactam in Class A β-Lactamase Inhibition|Antimicrobial Agents and Chemotherapy. Available online: https://journals.asm.org/doi/10.1128/AAC.00398-20?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed (accessed on 24 November 2021).
- Delmas, J.; Leyssene, D.; Dubois, D.; Birck, C.; Vazeille, E.; Robin, F.; Bonnet, R. Structural Insights into Substrate Recognition and Product Expulsion in CTX-M Enzymes. J. Mol. Biol. 2010, 400, 108–120. [Google Scholar] [CrossRef] [PubMed]
- Beadle, B.M.; Trehan, I.; Focia, P.J.; Shoichet, B.K. Structural Milestones in the Reaction Pathway of an Amide Hydrolase: Substrate, Acyl, and Product Complexes of Cephalothin with AmpC β-Lactamase. Structure 2002, 10, 413–424. [Google Scholar] [CrossRef]
- PubChem. Meropenem. Available online: https://pubchem.ncbi.nlm.nih.gov/compound/441130 (accessed on 24 November 2021).
- Meropenem. Available online: https://go.drugbank.com/drugs/DB00760 (accessed on 24 November 2021).
- PubChem. Vaborbactam. Available online: https://pubchem.ncbi.nlm.nih.gov/compound/56649692 (accessed on 24 November 2021).
- Vaborbactam. Available online: https://go.drugbank.com/drugs/DB12107 (accessed on 24 November 2021).
- Drusano, G. Meropenem: Laboratory and Clinical Data. Clin. Microbiol. Infect. 1997, 3, 4S51–4S59. [Google Scholar] [CrossRef]
- McCarthy, M.W. Clinical Pharmacokinetics and Pharmacodynamics of Imipenem–Cilastatin/Relebactam Combination Therapy. Clin. Pharmacokinet. 2020, 59, 567–573. [Google Scholar] [CrossRef]
- Fukasawa, M.; Sumita, Y.; Harabe, E.T.; Tanio, T.; Nouda, H.; Kohzuki, T.; Okuda, T.; Matsumura, H.; Sunagawa, M. Stability of Meropenem and Effect of 1 Beta-Methyl Substitution on Its Stability in the Presence of Renal Dehydropeptidase I. Antimicrob. Agents Chemother. 1992, 36, 1577–1579. [Google Scholar] [CrossRef]
- Tomasello, C.; Leggieri, A.; Cavalli, R.; Di Perri, G.; D’Avolio, A. In Vitro Stability Evaluation of Different Pharmaceutical Products Containing Meropenem. Hosp. Pharm. 2015, 50, 296–303. [Google Scholar] [CrossRef]
- Singlas, E. Clinical pharmacokinetics of an imipenem-cilastatin combination. Presse Medicale Paris Fr. 1983 1990, 19, 598–605. [Google Scholar]
- VABOMERE (Meropenem and Vaborbactam) for Injection. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/label/2017/209776lbl.pdf (accessed on 1 May 2024).
- New FDA Approval: Vabomere. Available online: https://www.tldrpharmacy.com/content/new-fda-approval-vabomere (accessed on 26 November 2021).
- Griffith, D.C.; Sabet, M.; Tarazi, Z.; Lomovskaya, O.; Dudley, M.N. Pharmacokinetics/Pharmacodynamics of Vaborbactam, a Novel Beta-Lactamase Inhibitor, in Combination with Meropenem. Antimicrob. Agents Chemother. 2018, 63, e01659-18. [Google Scholar] [CrossRef]
- Trang, M.; Griffith, D.C.; Bhavnani, S.M.; Loutit, J.S.; Dudley, M.N.; Ambrose, P.G.; Rubino, C.M. Population Pharmacokinetics of Meropenem and Vaborbactam Based on Data from Noninfected Subjects and Infected Patients. Antimicrob. Agents Chemother. 2021, 65, e02606-20. [Google Scholar] [CrossRef]
- Rubino, C.M.; Bhavnani, S.M.; Loutit, J.S.; Morgan, E.E.; White, D.; Dudley, M.N.; Griffith, D.C. Phase 1 Study of the Safety, Tolerability, and Pharmacokinetics of Vaborbactam and Meropenem Alone and in Combination Following Single and Multiple Doses in Healthy Adult Subjects. Antimicrob. Agents Chemother. 2018, 62, e02228-17. [Google Scholar] [CrossRef]
- Kaye, K.S.; Bhowmick, T.; Metallidis, S.; Bleasdale, S.C.; Sagan, O.S.; Stus, V.; Vazquez, J.; Zaitsev, V.; Bidair, M.; Chorvat, E.; et al. Effect of Meropenem-Vaborbactam vs Piperacillin-Tazobactam on Clinical Cure or Improvement and Microbial Eradication in Complicated Urinary Tract Infection: The TANGO I Randomized Clinical Trial. JAMA 2018, 319, 788–799. [Google Scholar] [CrossRef]
- Mohr, J.F., III. Update on the Efficacy and Tolerability of Meropenem in the Treatment of Serious Bacterial Infections. Clin. Infect. Dis. 2008, 47 (Suppl. 1), S41–S51. [Google Scholar] [CrossRef]
- Linden, P. Safety Profile of Meropenem. Drug Saf. 2007, 30, 657–668. [Google Scholar] [CrossRef]
- Meropenem. LiverTox: Clinical and Research Information on Drug-Induced Liver Injury; National Institute of Diabetes and Digestive and Kidney Diseases: Bethesda, MD, USA, 2012. [Google Scholar]
- Schumaker, A.L.; Okulicz, J.F. Meropenem-Induced Vanishing Bile Duct Syndrome. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2010, 30, 953. [Google Scholar] [CrossRef]
- Khalel, M.H.; Fattah Saleh, S.A.; F El-Gamal, A.-H.; Najem, N. Acute Generalized Exanthematous Pustulosis: An Unusual Side Effect of Meropenem. Indian J. Dermatol. 2010, 55, 176–177. [Google Scholar] [CrossRef]
- Yahav, D.; Giske, C.G.; Grāmatniece, A.; Abodakpi, H.; Tam, V.H.; Leibovici, L. New β-Lactam–β-Lactamase Inhibitor Combinations. Clin. Microbiol. Rev. 2020, 34, e00115-20. [Google Scholar] [CrossRef]
- Biedenbach, D.J.; Kazmierczak, K.; Bouchillon, S.K.; Sahm, D.F.; Bradford, P.A. In Vitro Activity of Aztreonam-Avibactam against a Global Collection of Gram-Negative Pathogens from 2012 and 2013. Antimicrob. Agents Chemother. 2015, 59, 4239–4248. [Google Scholar] [CrossRef]
- Dimude, J.U.; Amyes, S.G.B. Molecular Characterisation and Diversity in Enterobacter Cloacae from Edinburgh and Egypt Carrying BlaCTX-M-14 and BlaVIM-4 β-Lactamase Genes. Int. J. Antimicrob. Agents 2013, 41, 574–577. [Google Scholar] [CrossRef]
- Galani, I.; Souli, M.; Chryssouli, Z.; Katsala, D.; Giamarellou, H. First Identification of an Escherichia coli Clinical Isolate Producing Both Metalloβ-Lactamase VIM-2 and Extended-Spectrum β-Lactamase IBC-1. Clin. Microbiol. Infect. 2004, 10, 757–760. [Google Scholar] [CrossRef][Green Version]
- Assawatheptawee, K.; Kiddee, A.; Na-udom, A.; Wangteeraprasert, A.; Treebupachatsakul, P.; Niumsup, P.R. Acquisition of Extended-Spectrum β-Lactamase-Producing Escherichia Coli and Klebsiella pneumoniae in Intensive Care Units in Thailand. J. Infect. Chemother. 2021, 27, 401–405. [Google Scholar] [CrossRef]
- Tiseo, G.; Galfo, V.; Riccardi, N.; Suardi, L.R.; Pogliaghi, M.; Giordano, C.; Leonildi, A.; Barnini, S.; Falcone, M. Real-world experience with meropenem/vaborbactam for the treatment of infections caused by ESBL-producing Enterobacterales and carbapenem-resistant Klebsiella pneumoniae. Eur. J. Clin. Microbiol. Infect. Dis. 2024. [Google Scholar] [CrossRef]
- Tiseo, G.; Suardi, L.R.; Leonildi, A.; Giordano, C.; Barnini, S.; Falcone, M. Meropenem/vaborbactam plus aztreonam for the treatment of New Delhi metallo-β-lactamase-producing Klebsiella pneumoniae infections. J. Antimicrob. Chemother. 2023, 78, 2377–2379. [Google Scholar] [CrossRef]
- Cienfuegos-Gallet, A.V.; Shashkina, E.; Chu, T.; Zhu, Z.; Wang, B.; Kreiswirth, B.N.; Chen, L. In vitro activity of meropenem-vaborbactam plus aztreonam against metallo-β-lactamase-producing Klebsiella pneumoniae. Antimicrob. Agents Chemother. 2024, 68, e01346-23. [Google Scholar] [CrossRef]

| Enzyme | Class | Ki (µM) |
|---|---|---|
| KPC-2 | A | 0.069 |
| KPC-3 | A | 0.050 |
| CTX-M-14 | A | 0.033 |
| CTX-M-15 | A | 0.030 |
| SHV-12 | A | 0.029 |
| TEM-10 | A | 0.110 |
| TEM-43 | A | 1.04 |
| AmpC | C | 0.035 |
| P99 | C | 0.053 |
| CMY-2 | C | 0.099 |
| OXA-48 | D | 14 |
| OXA-23 | D | 66 |
| NDM-1 | B | >160 |
| VIM-1 | B | >160 |
| References [16,26] | ||
| Property | Meropenem | Vaborbactam |
|---|---|---|
| LogP | −0.6 | 1.86 |
| pKa | 3.47/9.39 | 3.75/−2.6 |
| Molecular Weight | 383.5 g/mol | 297.14 g/mol |
| Formal Charge | 0 | 0 |
| Solubility in Water | 5.63 mg/mL | 0.155 mg/mL |
| H-Bond Donors | 3 | 3 |
| H-Bond Acceptors | 7 | 6 |
| Rotatable Bonds | 5 | 5 |
| References [31,32,33,34] | ||
| Parameter | Meropenem | Vaborbactam |
|---|---|---|
| CLR,max (L/h) | 6.58 | 8.86 |
| CLNR (L/h) | 3.85 | 0.157 |
| CLd (L/h) | 1.36 | 2.75 |
| Vc (L) | 17.0 | 17.1 |
| Vp (L) | 2.32 | 1.77 |
| eGFR50 (mL/min/1.73 m2) | 40.0 | 49.7 |
| Reference [43] | ||
| Parameter | Meropenem | Vaborbactam |
|---|---|---|
| Cmax (µg/mL) | 55.4 | 68.7 |
| Day 1 AUC0–24 (µg h/mL) | 593 | 776 |
| Steady-state AUC0–24 (µg h/mL) | 586 | 766 |
| CL (L/h) | 8.68 | 6.22 |
| t1/2,alpha | 0.771 | 0.379 |
| t1/2,beta | 1.89 | 2.04 |
| Reference [43] | ||
| Adverse Event | Meropenem | Vaborbactam | Meropenem + Vaborbactam |
|---|---|---|---|
| Headache | 0.4 | 29.2 | 8.8 |
| Diarrhea | 2.5 | ND | 3.3 |
| Nausea/Lathargy | 1.2 | 20.8 | 1.8 |
| Rash | 1.4 | 12.5 | ND |
| Injection site reaction | 0.9 | 41.7 | 2.2 |
| Sepsis | 0.1 | ND | ND |
| Reference | [46] | [44] | [45] |
| Enzyme | IC50 (µM) |
|---|---|
| Trypsin | >1000 |
| Chymotrypsin | >1000 |
| Plasmin | >1000 |
| Thrombin | >1000 |
| Elastase | >1000 |
| Urokinase | >1000 |
| Tissue plasminogen activator (TPA) | >1000 |
| Chymase | >1000 |
| D-dipeptidyl peptidase 7 (DPP7) | >1000 |
| Neutrophil elastase | >1000 |
| Cathepsin A | 1000 |
| Reference [26] | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hillyer, T.; Shin, W.S. Meropenem/Vaborbactam—A Mechanistic Review for Insight into Future Development of Combinational Therapies. Antibiotics 2024, 13, 472. https://doi.org/10.3390/antibiotics13060472
Hillyer T, Shin WS. Meropenem/Vaborbactam—A Mechanistic Review for Insight into Future Development of Combinational Therapies. Antibiotics. 2024; 13(6):472. https://doi.org/10.3390/antibiotics13060472
Chicago/Turabian StyleHillyer, Trae, and Woo Shik Shin. 2024. "Meropenem/Vaborbactam—A Mechanistic Review for Insight into Future Development of Combinational Therapies" Antibiotics 13, no. 6: 472. https://doi.org/10.3390/antibiotics13060472
APA StyleHillyer, T., & Shin, W. S. (2024). Meropenem/Vaborbactam—A Mechanistic Review for Insight into Future Development of Combinational Therapies. Antibiotics, 13(6), 472. https://doi.org/10.3390/antibiotics13060472






