Affinity Assays for Cannabinoids Detection: Are They Amenable to On-Site Screening?
Abstract
:1. Introduction
- -
- -
- Phytocannabinoids (cannabinoids that occur naturally in the cannabis plant) such as THC and CBD [5];
- -
2. Main Matrices for Cannabinoids Screening
2.1. Oral Fluid
2.2. Exhaled Breath
2.3. Sweat
2.4. Plasma
2.5. Urine
3. Trending Methods for Rapid Detection
3.1. Electrochemical Detection
3.1.1. SWV- and DPV-Based Biosensors
3.1.2. EIS-Based Biosensors
3.1.3. Chronoamperometric Biosensors
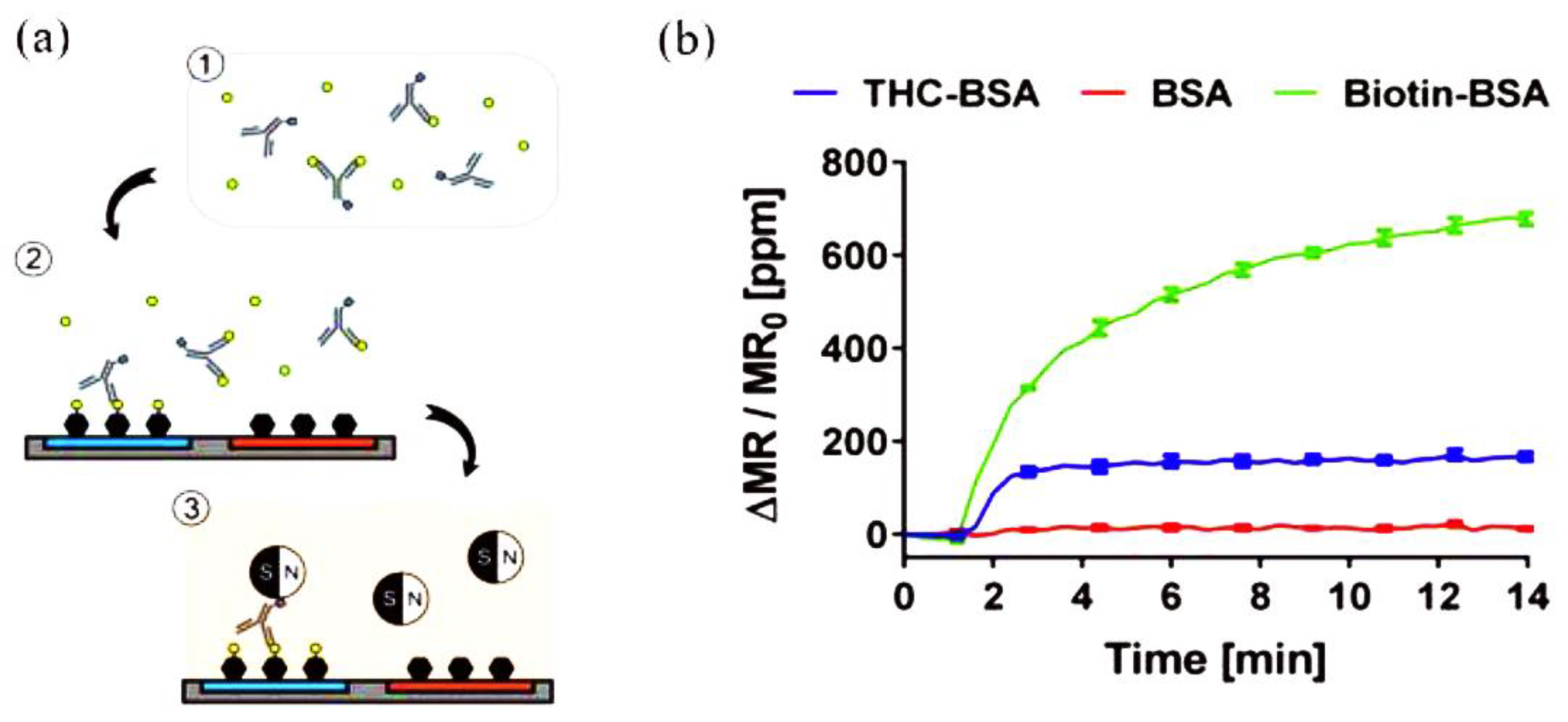
3.2. Magnetoresistive Biosensors
3.3. Optical Detection
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kumar, A.; Premoli, M.; Aria, F.; Bonini, S.A.; Maccarinelli, G.; Gianoncelli, A.; Memo, M.; Mastinu, A. Cannabimimetic plants: Are they new cannabinoidergic modulators? Planta 2019, 249, 1681–1694. [Google Scholar] [CrossRef] [PubMed]
- Hall, W.; Weier, M. Assessing the public health impacts of legalizing recreational cannabis use in the USA. Clin. Pharmacol. Ther. 2015, 97, 607–615. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ahmed, S.A.; Ross, S.A.; Slade, D.; Radwan, M.M.; Khan, I.A.; ElSohly, M.A. Minor oxygenated cannabinoids from high potency Cannabis sativa L. Phytochemistry 2015, 117, 194–199. [Google Scholar] [CrossRef] [Green Version]
- Cooray, R.; Gupta, V.; Suphioglu, C. Current Aspects of the Endocannabinoid System and Targeted THC and CBD phytocannabinoids as potential therapeutics for parkinson’s and alzheimer’s diseases: A review. Mol. Neurobiol. 2020, 57, 4878–4890. [Google Scholar] [CrossRef] [PubMed]
- Di Marzo, V. The endocannabinoidome as a substrate for noneuphoric phytocannabinoid action and gut microbiome dysfunction in neuropsychiatric disorders. Dialogues Clin. Neurosci. 2020, 22, 259–269. [Google Scholar] [CrossRef] [PubMed]
- Fattore, L.; Fratta, W. Beyond THC: The new generation of cannabinoid designer drugs. Front. Behav. Neurosci. 2011, 5, 60. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Broers, B.; Patà, Z.; Mina, A.; Wampfler, J.; de Saussure, C.; Pautex, S. Prescription of a THC/CBD-Based medication to patients with dementia: A pilot study in Geneva. Med. Cannabis Cannabinoids 2019, 2, 56–59. [Google Scholar] [CrossRef]
- Withey, S.L.; Bergman, J.; Huestis, M.A.; George, S.R.; Madras, B.K. THC and CBD blood and brain concentrations following daily administration to adolescent primates. Drug Alcohol Depend. 2020, 213, 108129. [Google Scholar] [CrossRef]
- Pertwee, R.G. Pharmacological and therapeutic targets for Δ9 tetrahydrocannabinol and cannabidiol. Euphytica 2004, 140, 73–82. [Google Scholar] [CrossRef]
- Elkashef, A.; Vocci, F.; Huestis, M.; Haney, M.; Budney, A.; Gruber, A.; el-Guebaly, N. Marijuana neurobiology and treatment. Subst. Abus. 2008, 29, 17–29. [Google Scholar] [CrossRef] [Green Version]
- Alsherbiny, M.A.; Li, C.G. Medicinal Cannabis—Potential drug interactions. Medicines 2019, 6, 3. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- De Petrocellis, L.; Di Marzo, V. Non-CB1, Non-CB2 receptors for endocannabinoids, plant cannabinoids, and synthetic cannabimimetics: Focus on G-protein-coupled receptors and transient receptor potential channels. J. Neuroimmune Pharmacol. 2010, 5, 103–121. [Google Scholar] [CrossRef] [PubMed]
- Sartore, D.M.; Vargas Medina, D.A.; Costa, J.L.; Lanças, F.M.; Santos-Neto, Á.J. Automated microextraction by packed sorbent of cannabinoids from human urine using a lab-made device packed with molecularly imprinted polymer. Talanta 2020, 219, 121185. [Google Scholar] [CrossRef] [PubMed]
- Pandopulos, A.J.; Bade, R.; O’Brien, J.W.; Tscharke, B.J.; Mueller, J.F.; Thomas, K.; White, J.M.; Gerber, C. Towards an efficient method for the extraction and analysis of cannabinoids in wastewater. Talanta 2020, 217, 121034. [Google Scholar] [CrossRef] [PubMed]
- Renaud-Young, M.; Mayall, R.M.; Salehi, V.; Goledzinowski, M.; Comeau, F.J.E.; MacCallum, J.L.; Birss, V.I. Development of an ultra-sensitive electrochemical sensor for Δ9-tetrahydrocannabinol (THC) and its metabolites using carbon paper electrodes. Electrochim. Acta 2019, 307, 351–359. [Google Scholar] [CrossRef]
- Comeau, Z.J.; Boileau, N.T.; Lee, T.; Melville, O.A.; Rice, N.A.; Troung, Y.; Harris, C.S.; Lessard, B.H.; Shuhendler, A.J. On-the-spot detection and speciation of cannabinoids using organic thin-film transistors. ACS Sens. 2019, 4, 2706–2715. [Google Scholar] [CrossRef]
- Ujváry, I.; Hanuš, L. Human metabolites of cannabidiol: A review on their formation, biological activity, and relevance in therapy. Cannabis Cannabinoid Res. 2016, 1, 90–101. [Google Scholar] [CrossRef] [Green Version]
- Niedbala, R.S.; Kardos, K.W.; Fritch, D.F.; Kardos, S.; Fries, T.; Waga, J.; Robb, J.; Cone, E.J. Detection of marijuana use by oral fluid and urine analysis following single-dose administration of smoked and oral marijuana. J. Anal. Toxicol. 2001, 25, 289–303. [Google Scholar] [CrossRef] [Green Version]
- Stevenson, H.; Bacon, A.; Joseph, K.M.; Gwandaru, W.R.W.; Bhide, A.; Sankhala, D.; Dhamu, V.N.; Prasad, S. A rapid response electrochemical biosensor for detecting Thc In Saliva. Sci. Rep. 2019, 9, 12701. [Google Scholar] [CrossRef] [Green Version]
- Sanli, S.; Ghorbani-Zamani, F.; Moulahoum, H.; Gumus, Z.P.; Coskunol, H.; Odaci Demirkol, D.; Timur, S. Application of biofunctionalized magnetic nanoparticles based-sensing in abused drugs diagnostics. Anal. Chem. 2020, 92, 1033–1040. [Google Scholar] [CrossRef]
- Marusich, J.A.; Wiley, J.L.; Lefever, T.W.; Patel, P.R.; Thomas, B.F. Finding order in chemical chaos—Continuing characterization of synthetic cannabinoid receptor agonists. Neuropharmacology 2018, 134, 73–81. [Google Scholar] [CrossRef] [PubMed]
- Castaneto, M.S.; Wohlfarth, A.; Desrosiers, N.A.; Hartman, R.L.; Gorelick, D.A.; Huestis, M.A. Synthetic cannabinoids pharmacokinetics and detection methods in biological matrices. Drug Metab. Rev. 2015, 47, 124–174. [Google Scholar] [CrossRef] [PubMed]
- Piggee, C. Investigating a not-so-natural high. Anal. Chem. 2009, 81, 3205–3207. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cannaert, A.; Storme, J.; Franz, F.; Auwärter, V.; Stove, C.P. Detection and activity profiling of synthetic cannabinoids and their metabolites with a newly developed bioassay. Anal. Chem. 2016, 88, 11476–11485. [Google Scholar] [CrossRef] [Green Version]
- Hilderbrand, R.L. High-performance sport, marijuana, and cannabimimetics. J. Anal. Toxicol. 2011, 35, 624–637. [Google Scholar] [CrossRef] [Green Version]
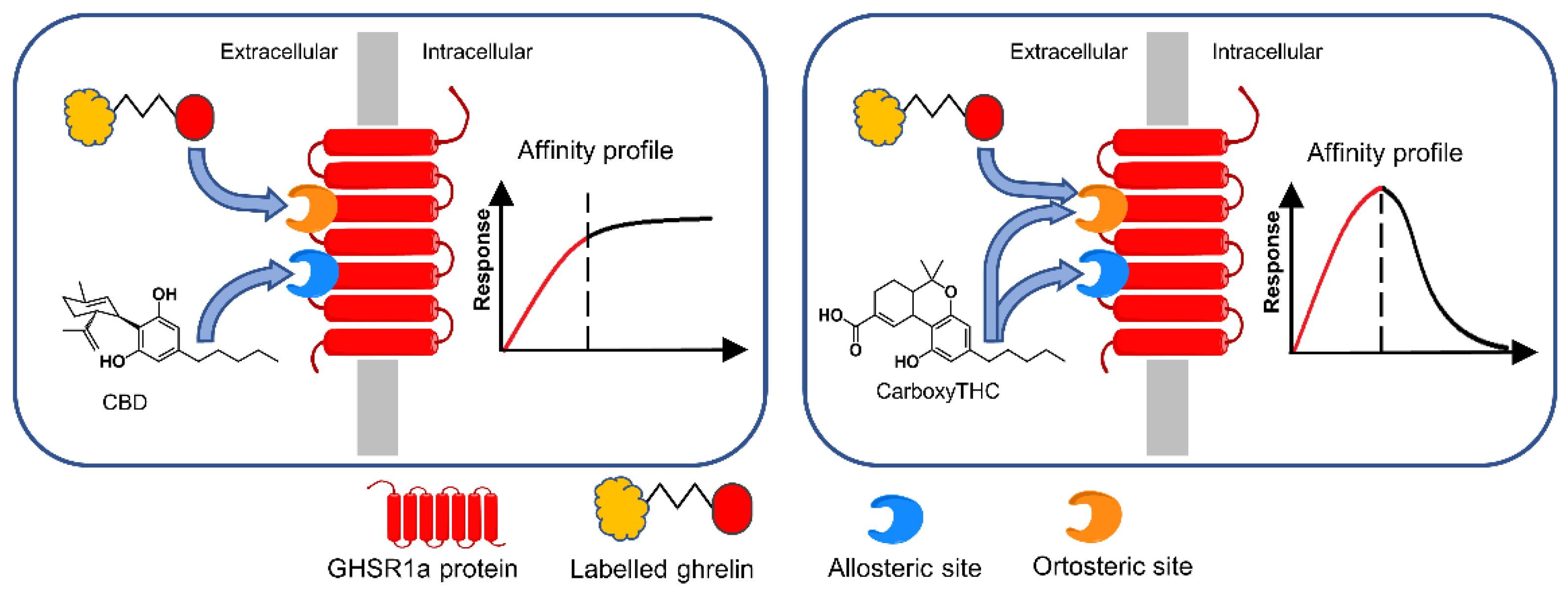
- Danila, G.M.; Puiu, M.; Zamfir, L.-G.; Bala, C. Early detection of cannabinoids in biological samples based on their affinity interaction with the growth hormone secretagogue receptor. Talanta 2022, 237, 122905. [Google Scholar] [CrossRef]
- Sharma, P.; Murthy, P.; Bharath, M.M.S. Chemistry, metabolism, and toxicology of cannabis: Clinical implications. Iran J. Psychiatry 2012, 7, 149–156. [Google Scholar]
- Fraser, A.D.; Worth, D. Monitoring urinary excretion of cannabinoids by fluorescence-polarization immunoassay: A cannabinoid-to-creatinine ratio study. Ther. Drug Monit. 2002, 24, 746–750. [Google Scholar] [CrossRef]
- Abd-Elsalam, W.H.; Alsherbiny, M.A.; Kung, J.Y.; Pate, D.W.; Löbenberg, R. LC–MS/MS quantitation of phytocannabinoids and their metabolites in biological matrices. Talanta 2019, 204, 846–867. [Google Scholar] [CrossRef]
- Bindesri, S.D.; Jebailey, R.; Albarghouthi, N.; Pye, C.C.; Brosseau, C.L. Spectroelectrochemical and computational studies of tetrahydrocannabinol (THC) and carboxy-tetrahydrocannabinol (THC-COOH). Analyst 2020, 145, 1849–1857. [Google Scholar] [CrossRef]
- Brunelle, E.; Thibodeau, B.; Shoemaker, A.; Halámek, J. Step toward roadside sensing: Noninvasive detection of a THC metabolite from the sweat content of fingerprints. ACS Sens. 2019, 4, 3318–3324. [Google Scholar] [CrossRef] [PubMed]
- Klimuntowski, M.; Alam, M.M.; Singh, G.; Howlader, M.M.R. Electrochemical sensing of cannabinoids in biofluids: A noninvasive tool for drug detection. ACS Sens. 2020, 5, 620–636. [Google Scholar] [CrossRef] [PubMed]
- Zanfrognini, B.; Pigani, L.; Zanardi, C. Recent advances in the direct electrochemical detection of drugs of abuse. J. Solid State Electrochem. 2020, 24, 2603–2616. [Google Scholar] [CrossRef]
- Backofen, U.; Matysik, F.-M.; Lunte, C.E. Determination of cannabinoids in hair using high-pH∗ non-aqueous electrolytes and electrochemical detection: Some aspects of sensitivity and selectivity. J. Chromatogr. A 2002, 942, 259–269. [Google Scholar] [CrossRef]
- Ramzy, V.; Priefer, R. THC detection in the breath. Talanta 2021, 222, 121528. [Google Scholar] [CrossRef] [PubMed]
- Huestis, M.A. Human cannabinoid pharmacokinetics. Chem. Biodivers. 2007, 4, 1770–1804. [Google Scholar] [CrossRef] [Green Version]
- Lee, D.; Milman, G.; Barnes, A.J.; Goodwin, R.S.; Hirvonen, J.; Huestis, M.A. Oral Fluid cannabinoids in chronic, daily cannabis smokers during sustained, monitored abstinence. Clin. Chem. 2011, 57, 1127–1136. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pedersen, A.M.; Bardow, A.; Jensen, S.B.; Nauntofte, B. Saliva and gastrointestinal functions of taste, mastication, swallowing and digestion. Oral Dis. 2002, 8, 117–129. [Google Scholar] [CrossRef]
- Huestis, M.A.; Cone, E.J. Relationship of Δ9-tetrahydrocannabinol concentrations in oral fluid and plasma after controlled administration of smoked cannabis. J. Anal. Toxicol. 2004, 28, 394–399. [Google Scholar] [CrossRef] [Green Version]
- Anizan, S.; Milman, G.; Desrosiers, N.; Barnes, A.J.; Gorelick, D.A.; Huestis, M.A. Oral fluid cannabinoid concentrations following controlled smoked cannabis in chronic frequent and occasional smokers. Anal. Bioanal. Chem. 2013, 405, 8451–8461. [Google Scholar] [CrossRef] [Green Version]
- Desrosiers, N.A.; Scheidweiler, K.B.; Huestis, M.A. Quantification of six cannabinoids and metabolites in oral fluid by liquid chromatography-tandem mass spectrometry. Drug Test. Anal. 2015, 7, 684–694. [Google Scholar] [CrossRef] [PubMed]
- Kintz, P.; Mura, P.; Jamey, C.; Raul, J.-S. Detection of ∆9-tetrahydrocannabinol in exhaled breath after cannabis smoking and comparison with oral fluid. Forensic Toxicol. 2017, 35, 173–178. [Google Scholar] [CrossRef]
- Coucke, L.; Massarini, E.; Ostijn, Z.; Beck, O.; Verstraete, A.G. Δ9-Tetrahydrocannabinol concentrations in exhaled breath and physiological effects following cannabis intake—A pilot study using illicit cannabis. Clin. Biochem. 2016, 49, 1072–1077. [Google Scholar] [CrossRef] [PubMed]
- Castillo-Peinado, L.S.; Luque de Castro, M.D. An overview on forensic analysis devoted to analytical chemists. Talanta 2017, 167, 181–192. [Google Scholar] [CrossRef] [PubMed]
- Namera, A.; Kawamura, M.; Nakamoto, A.; Saito, T.; Nagao, M. Comprehensive review of the detection methods for synthetic cannabinoids and cathinones. Forensic Toxicol. 2015, 33, 175–194. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jadon, N.; Jain, R.; Sharma, S.; Singh, K. Recent trends in electrochemical sensors for multianalyte detection—A review. Talanta 2016, 161, 894–916. [Google Scholar] [CrossRef]
- Grotenhermen, F. Pharmacokinetics and pharmacodynamics of cannabinoids. Clin. Pharmacokinet. 2003, 42, 327–360. [Google Scholar] [CrossRef]
- Huestis, M.A.; Henningfield, J.E.; Cone, E.J. Blood Cannabinoids. I. Absorption of THC and formation of 11-OH-THC and THCCOOH during and after smoking Marijuana*. J. Anal. Toxicol. 1992, 16, 276–282. [Google Scholar] [CrossRef]
- Li, J.; Zhang, Y.; Zhou, Y.; Feng, X.-S. Cannabinoids: Recent updates on public perception, adverse reactions, pharmacokinetics, pretreatment methods and their analysis methods. Crit. Rev. Anal. Chem. 2021, 1–26. [Google Scholar] [CrossRef]
- Musshoff, F.; Madea, B. Review of biologic matrices (Urine, Blood, Hair) as indicators of recent or ongoing cannabis use. Ther. Drug Monit. 2006, 28, 155–163. [Google Scholar] [CrossRef] [Green Version]
- Dinis-Oliveira, R.J. Metabolomics of Δ9-tetrahydrocannabinol: Implications in toxicity. Drug Metab. Rev. 2016, 48, 80–87. [Google Scholar] [CrossRef] [PubMed]
- Jogschies, L.; Klaas, D.; Kruppe, R.; Rittinger, J.; Taptimthong, P.; Wienecke, A.; Rissing, L.; Wurz, M.C. Recent developments of magnetoresistive sensors for industrial applications. Sensors 2015, 15, 28665–28689. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Santillo, M.F. Trends using biological target-based assays for drug detection in complex sample matrices. Anal. Bioanal. Chem. 2020, 412, 3975–3982. [Google Scholar] [CrossRef] [PubMed]
- Hulme, E.C.; Trevethick, M.A. Ligand binding assays at equilibrium: Validation and interpretation. Br. J. Pharmacol. 2010, 161, 1219–1237. [Google Scholar] [CrossRef] [Green Version]
- Anzar, N.; Suleman, S.; Parvez, S.; Narang, J. A review on Illicit drugs and biosensing advances for its rapid detection. Process Biochem. 2022, 113, 113–124. [Google Scholar] [CrossRef]
- Nissim, R.; Compton, R.G. Absorptive stripping voltammetry for cannabis detection. Chem. Cent. J. 2015, 9, 41. [Google Scholar] [CrossRef] [Green Version]
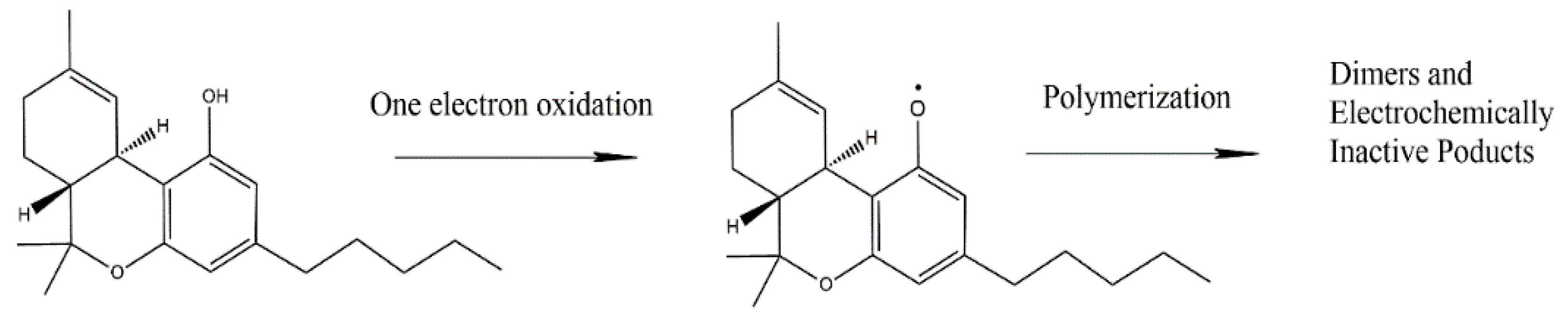
- Balbino, M.A.; de Menezes, M.M.T.; Eleotério, I.C.; Saczk, A.A.; Okumura, L.L.; Tristão, H.M.; de Oliveira, M.F. Voltammetric determination of Δ9-THC in glassy carbon electrode: An important contribution to forensic electroanalysis. Forensic Sci. Int. 2012, 221, 29–32. [Google Scholar] [CrossRef]
- Gattrell, M.; Kirk, D.W. The electrochemical oxidation of aqueous phenol at a glassy carbon electrode. Can. J. Chem. Eng. 1990, 68, 997–1003. [Google Scholar] [CrossRef]
- Balbino, M.A.; Oiye, É.N.; Ribeiro, M.F.M.; Júnior, J.W.C.; Eleotério, I.C.; Ipólito, A.J.; de Oliveira, M.F. Use of screen-printed electrodes for quantification of cocaine and Δ 9-THC: Adaptions to portable systems for forensic purposes. J. Solid State Electrochem. 2016, 20, 2435–2443. [Google Scholar] [CrossRef]
- Mirceski, V.; Gulaboski, R.; Lovric, M.; Bogeski, I.; Kappl, R.; Hoth, M. Square-wave voltammetry: A review on the recent progress. Electroanalysis 2013, 25, 2411–2422. [Google Scholar] [CrossRef] [Green Version]
- Mirceski, V.; Stojanov, L.; Gulaboski, R. Double-sampled differential square-wave voltammetry. J. Electroanal. Chem. 2020, 872, 114384. [Google Scholar] [CrossRef]
- Uslu, B.; Ozkan, S.A. Electroanalytical methods for the determination of pharmaceuticals: A review of recent trends and developments. Anal. Lett. 2011, 44, 2644–2702. [Google Scholar] [CrossRef]
- Özkan, S.A.; Uslu, B.; Aboul-Enein, H.Y. Analysis of pharmaceuticals and biological fluids using modern electroanalytical techniques. Crit. Rev. Anal. Chem. 2003, 33, 155–181. [Google Scholar] [CrossRef]
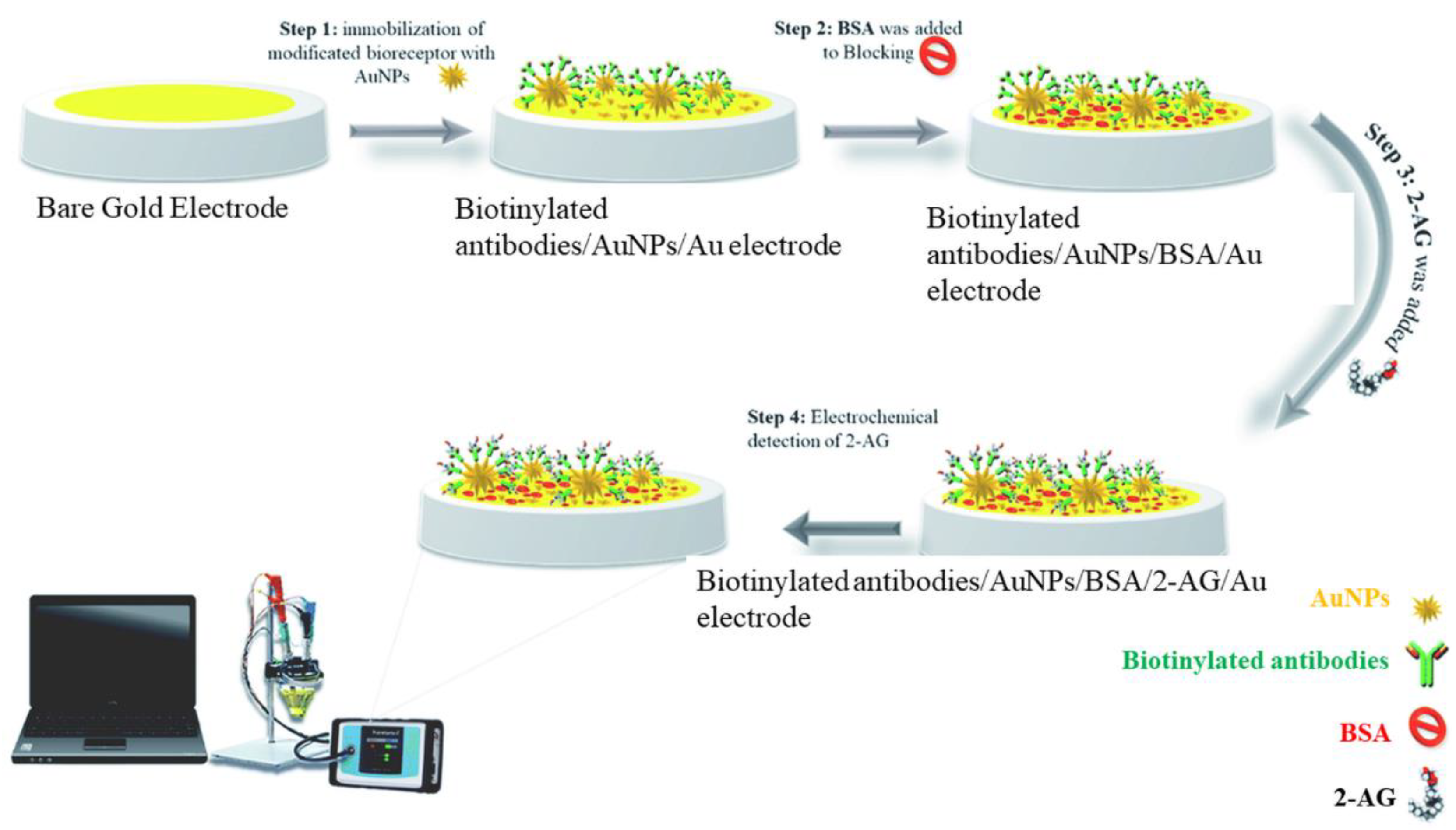
- Kohansal, F.; Mobed, A.; Ansari, R.; Hasanzadeh, M.; Ahmadalipour, A.; Shadjou, N. An innovative electrochemical immuno-platform towards ultra-sensitive monitoring of 2-arachidonoyl glycerol in samples from rats with sleep deprivation: Bioanalysis of endogenous cannabinoids using biosensor technology. RSC Adv. 2022, 12, 14154–14166. [Google Scholar] [CrossRef] [PubMed]
- Bahadır, E.B.; Sezgintürk, M.K. A review on impedimetric biosensors. Artif. Cells Nanomed. Biotechnol. 2016, 44, 248–262. [Google Scholar] [CrossRef]
- Schrattenecker, J.D.; Heer, R.; Melnik, E.; Maier, T.; Fafilek, G.; Hainberger, R. Hexaammineruthenium (II)/(III) as alternative redox-probe to Hexacyanoferrat (II)/(III) for stable impedimetric biosensing with gold electrodes. Biosens. Bioelectron. 2019, 127, 25–30. [Google Scholar] [CrossRef]
- Ertürk, G.; Mattiasson, B. Capacitive biosensors and molecularly imprinted electrodes. Sensors 2017, 17, 390. [Google Scholar] [CrossRef] [Green Version]
- Zamfir, L.-G.; Puiu, M.; Bala, C. Advances in Electrochemical Impedance Spectroscopy Detection of Endocrine Disruptors. Sensors 2020, 20, 6443. [Google Scholar] [CrossRef]
- Majak, D.; Fan, J.; Kang, S.; Gupta, M. Delta-9-tetrahydrocannabinol (Δ9-THC) sensing using an aerosol jet printed organic electrochemical transistor (OECT). J. Mater. Chem. B 2021, 9, 2107–2117. [Google Scholar] [CrossRef]
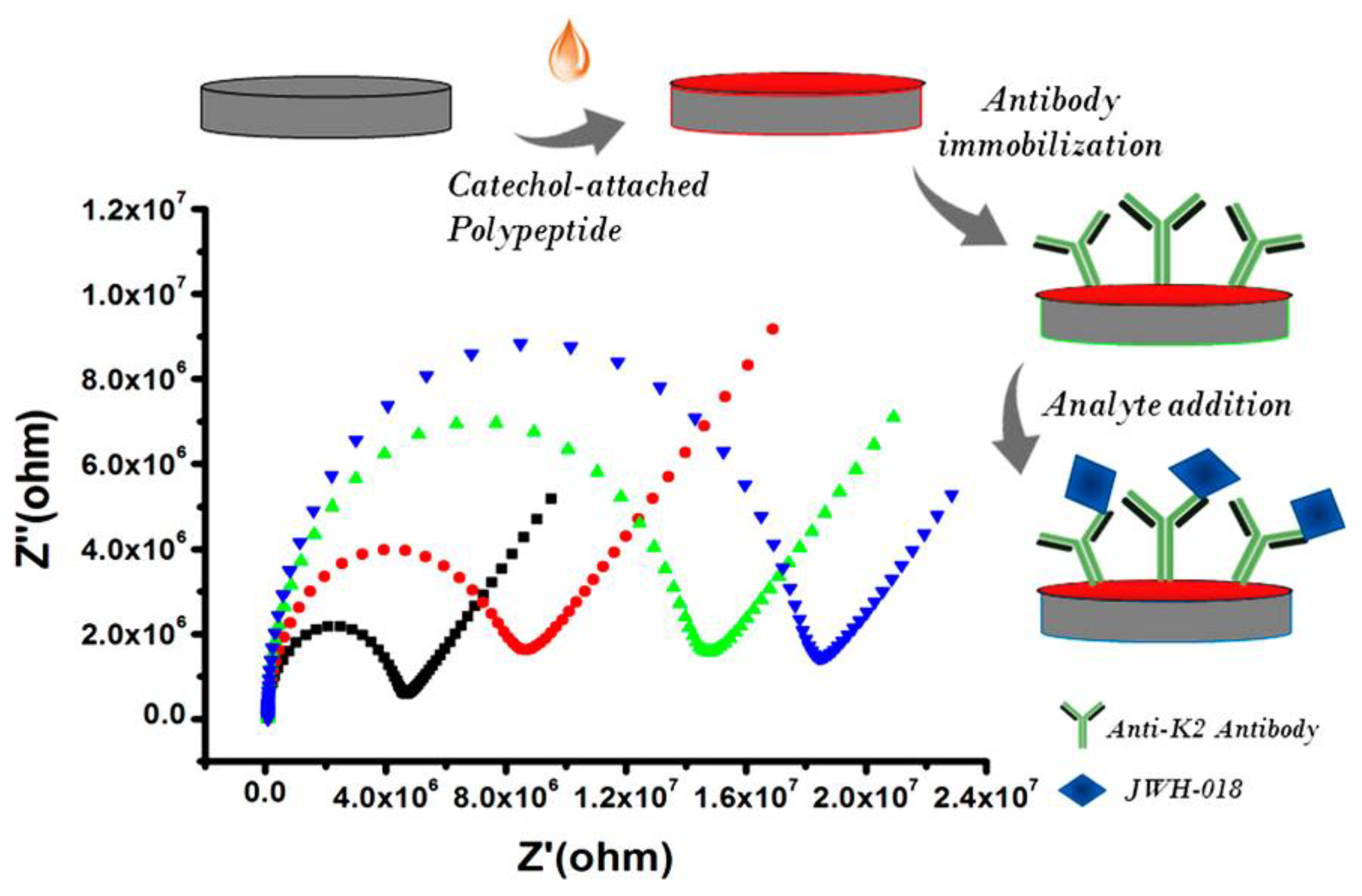
- Durmus, C.; Aydindogan, E.; Gumus, Z.P.; Endo, T.; Yamada, S.; Coskunol, H.; Timur, S.; Yagci, Y. Catechol-attached polypeptide with functional groups as electrochemical sensing platform for synthetic cannabinoids. ACS Appl. Polym. Mater. 2020, 2, 172–177. [Google Scholar] [CrossRef]
- Rojas, J.; Fontana Tachon, A.; Chevalier, D.; Noguer, T.; Marty, J.L.; Ghommidh, C. Chemometric analysis of screen-printed biosensor chronoamperometric responses. Sens. Actuators B Chem. 2004, 102, 284–290. [Google Scholar] [CrossRef]
- Lu, D.; Lu, F.; Pang, G. A novel tetrahydrocannabinol electrochemical nano immunosensor based on horseradish peroxidase and double-layer gold nanoparticles. Molecules 2016, 21, 1377. [Google Scholar] [CrossRef] [PubMed] [Green Version]
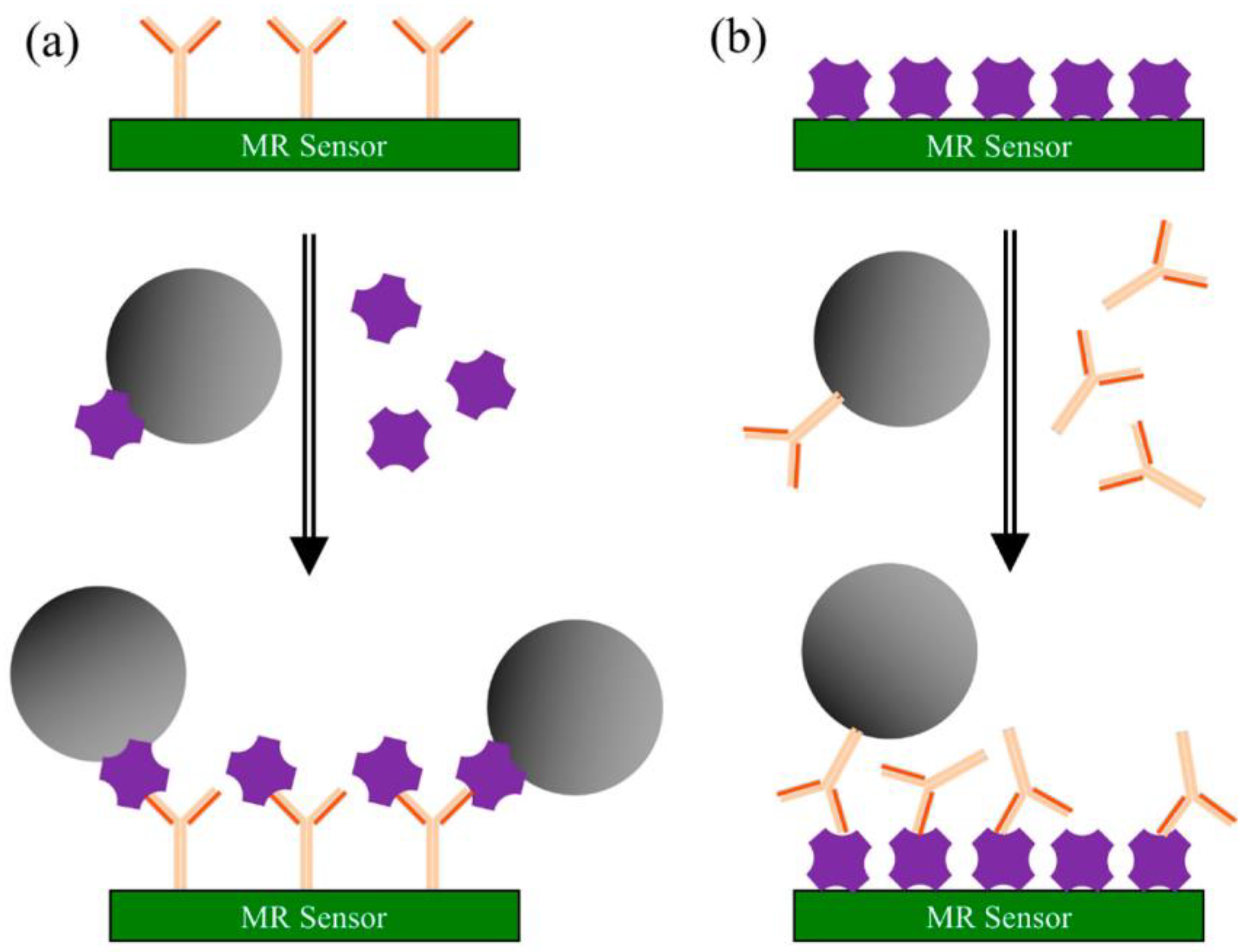
- Su, D.; Wu, K.; Saha, R.; Peng, C.; Wang, J.-P. Advances in magnetoresistive biosensors. Micromachines 2020, 11, 34. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, Y.; Wang, W.; Yu, L.; Tu, L.; Feng, Y.; Klein, T.; Wang, J.-P. Giant magnetoresistive-based biosensing probe station system for multiplex protein assays. Biosens. Bioelectron. 2015, 70, 61–68. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.-R.; Choi, J.; Shultz, T.O.; Wang, S.X. Small molecule detection in saliva facilitates portable tests of marijuana abuse. Anal. Chem. 2016, 88, 7457–7461. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Puiu, M.; Bala, C. Microfluidics-integrated biosensing platforms as emergency tools for on-site field detection of foodborne pathogens. TrAC Trends Anal. Chem. 2020, 125, 115831. [Google Scholar] [CrossRef]
- Xu, Y.; Wang, X.; Zhang, W.L.; Lv, F.; Guo, S. Recent progress in two-dimensional inorganic quantum dots. Chem. Soc. Rev. 2018, 47, 586–625. [Google Scholar] [CrossRef]
- Plouffe, B.D.; Murthy, S.K. Fluorescence-based lateral flow assays for rapid oral fluid roadside detection of cannabis use. Electrophoresis 2017, 38, 501–506. [Google Scholar] [CrossRef]
- Calabria, D.; Calabretta, M.M.; Zangheri, M.; Marchegiani, E.; Trozzi, I.; Guardigli, M.; Michelini, E.; Di Nardo, F.; Anfossi, L.; Baggiani, C.; et al. Recent advancements in Enzyme-Based lateral flow immunoassays. Sensors 2021, 21, 3358. [Google Scholar] [CrossRef]
- Namera, A.; Nakamoto, A.; Saito, T.; Nagao, M. Colorimetric detection and chromatographic analyses of designer drugs in biological materials: A comprehensive review. Forensic Toxicol. 2011, 29, 1–24. [Google Scholar] [CrossRef]
- Huang, L.; Tian, S.; Zhao, W.; Liu, K.; Ma, X.; Guo, J. Multiplexed detection of biomarkers in lateral-flow immunoassays. Analyst 2020, 145, 2828–2840. [Google Scholar] [CrossRef] [PubMed]
- Ragavan, K.V.; Ahmed, S.R.; Weng, X.; Neethirajan, S. Chitosan as a peroxidase mimic: Paper based sensor for the detection of hydrogen peroxide. Sens. Actuators B Chem. 2018, 272, 8–13. [Google Scholar] [CrossRef]
- Cannaert, A.; Storme, J.; Hess, C.; Auwärter, V.; Wille, S.M.R.; Stove, C.P. Activity-based detection of cannabinoids in serum and plasma samples. Clin. Chem. 2018, 64, 918–926. [Google Scholar] [CrossRef] [PubMed] [Green Version]
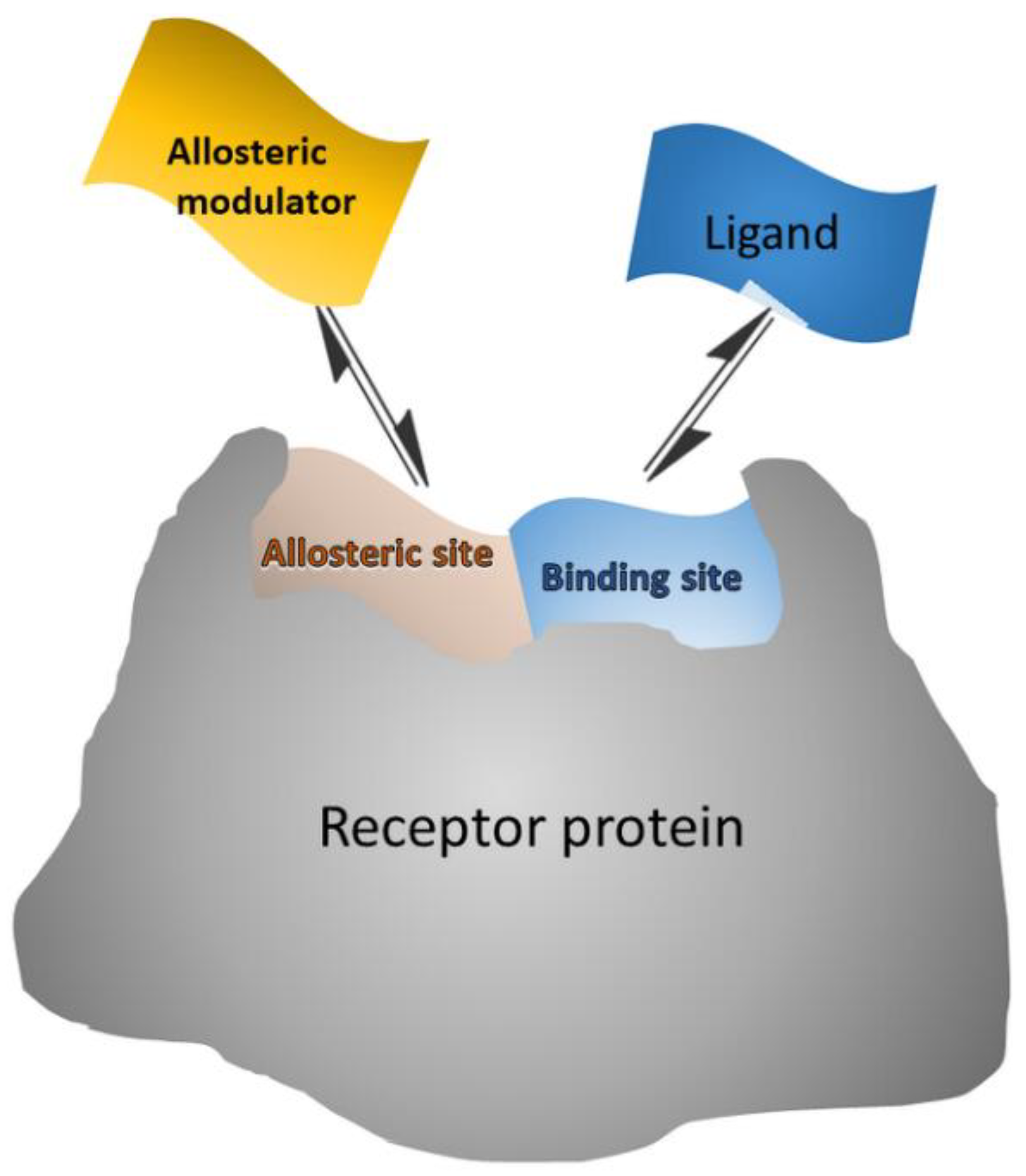
- Chatzigoulas, A.; Cournia, Z. Rational design of allosteric modulators: Challenges and successes. WIREs Comput. Mol. Sci. 2021, 11, e1529. [Google Scholar] [CrossRef]
- May, L.T.; Leach, K.; Sexton, P.M.; Christopoulos, A. Allosteric modulation of G protein–Coupled receptors. Annu. Rev. Pharmacol. Toxicol. 2007, 47, 1–51. [Google Scholar] [CrossRef]
- Moulahoum, H.; Ghorbanizamani, F.; Timur, S. Paper-based lateral flow assay using rhodamine B–loaded polymersomes for the colorimetric determination of synthetic cannabinoids in saliva. Microchim. Acta 2021, 188, 402. [Google Scholar] [CrossRef]
- Sengel, T.Y.; Celik, E.G.; Aydogan, C.; Gumus, Z.P.; Ilktac, R.; Aydindogan, E.; Ciftci, M.; Aldemir, E.; Coskunol, H.; Timur, S.; et al. A functional platform for the detection of JWH-073 as a model for synthetic cannabinoids. ChemElectroChem 2018, 5, 1253–1258. [Google Scholar] [CrossRef]
- Canfarotta, F.; Czulak, J.; Guerreiro, A.; Cruz, A.G.; Piletsky, S.; Bergdahl, G.E.; Hedström, M.; Mattiasson, B. A novel capacitive sensor based on molecularly imprinted nanoparticles as recognition elements. Biosens. Bioelectron. 2018, 120, 108–114. [Google Scholar] [CrossRef]
- Eissa, S.; Almthen, R.A.; Zourob, M. Disposable electrochemical immunosensor array for the multiplexed detection of the drug metabolites morphine, tetrahydrocannabinol and benzoylecgonine. Microchim. Acta 2019, 186, 523. [Google Scholar] [CrossRef]
- Boonyayothin, W.; Kobtrakul, K.; Khositanon, P.; Vimolmangkang, S.; Phoolcharoen, W. Development of a plant-produced recombinant monoclonal antibody against Δ-9-tetrahydrocannabinol (Δ9-THC) for immunoassay application. Biotechnol. Rep. 2022, 34, e00725. [Google Scholar] [CrossRef]
| Cannabinoid | Structure | Function |
|---|---|---|
| Δ9-tetrahydrocannabinol (THC) | 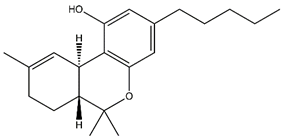 | Primary psychoactive component |
| 11-OH-Δ9-tetrahydrocannabinol (11-OH-THC) | 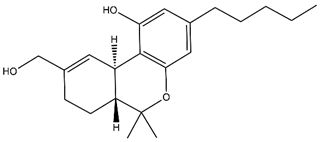 | Primary metabolite of THC, psychoactive |
| 11-nor-9-carboxy-Δ9-tetrahydrocannabinol (carboxy-THC) | 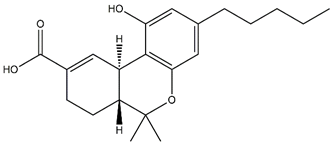 | Primary metabolite of 11-OH-THC, non-psychoactive |
| Cannabidiol (CBD) | 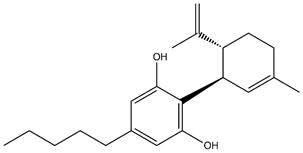 | Major component, non-psychoactive, has medicinal use |
| Cannabinol (CBN) | 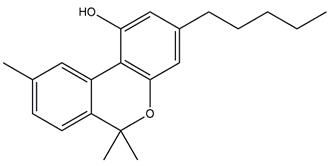 | Common product of THC degradation |
| JWH-073 | 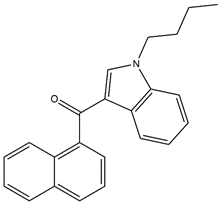 | Synthetic psychoactive cannabinoid Mimics the body’s naturally produced endocannabinoid hormones |
| Platform | Target | Capturing Element/Assay Format | Detection Technique | Matrix | LOD/Linear Range | Benefits | Drawbacks | Ref. |
|---|---|---|---|---|---|---|---|---|
| Paper substrate Whatman grade 1 chromatography | THC | Anti-THC antibodies conjugated to phycoerythrin-fluorescent particles/sandwich | Fluorescence/LFIA | Oral fluid | 0.1 ng/mL/Not reported | Rapid detection nonradioactive, high-throughput, low sample volume | Poor stability of the florescent probe, low reproducibility | [78] |
| Nitrocellulose membrane | JWH-073 | Anti-K2 antibodies conjugated to Rhodamine B–loaded polymersome/ sandwich | Colorimetric/LFIA | Saliva | 0.53 ng/mL 5.0–1000 ng/mL | High-throughput, low sample volume | Smaller molecules cannot be detected by two antibodies (sandwich assays) | [86] |
| HBC-2-dimethylamino ethyl methacrylate DMAEMA-modified glassy carbon electrode (GCE) | JWH-073 | Anti-K2 antibodies /direct binding | Electrochemical/DPV | Synthetic urine | 31.87 ng/mL 25–500 ng/mL | Rapid detection, high specificity | LOD above the cutoff limit for cannabinoids levels | [87] |
| Chit/AuNP-modified (GCE) | THC | Anti-THC antibodies conjugated to AuNPs/direct binding | Electrochemical/ chronoamperometry | Buffer | 3 pg/mL/ 0.01–0.01 × 103 ng/mL | Rapid detection, enhanced sensitivity | Use of labeled reagents, additional signal amplification steps, low stability of nanomaterials | [72] |
| Au deposited onto polyethylene terephthalate (PET) substrate | THC | Anti-THC antibodies immobilized onto dithiobis(succinimidyl propionate) (DSP) SAM/direct competitive | Electrochemical/ EIS | Human saliva | 100 pg/mL/ 100 pg/mL–100 ng/mL | High selectivity, suitable for on-site detection | Extended time range for sensor equilibration, multiple washing steps | [19] |
| Au electrode | THC | NanoMIP for THC | Electrochemical/ capacitive | Buffer | 1.0 × 10–14 M 1.0 × 10−12–1.0 × 10−5 M | High sensitivity suitable for on-site detection | Extended time range for sensor equilibration, multiple washing steps | [88] |
| AuNP-modified screen-printed carbon array electrodes | THC | Anti-THC antibodies immobilized onto AuNP-modified electrode/direct competitive | Electrochemical/SWV | Spiked urine sample | 7 pg/mL/ 10 pg/mL–10 μg/mL | Multiplexing capability, enhanced sensitivity | Risk of cross-reactivity | [89] |
| ELISA microplates | THC | Plant-produced monoclonal anti-THC antibody/indirect competitive | Colorimetric | Buffer | 0.625 μg/mL 0.625–10 μg/mL | High specificity and selectivity | Use of labeled reagents, time-consuming steps | [90] |
| Functionally activated microplates | Carboxy-THC CBD | Growth hormone secretagogue receptor/direct competitive | Colorimetric | Synthetic urine | 5.12 ng/mL/ 5–30 ng/mL 7.63 ng/mL/ 5–30 ng/mL | High sensitivity, low sample volumes | Use of labeled reagents, multiple washing steps | [26] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Puiu, M.; Bala, C. Affinity Assays for Cannabinoids Detection: Are They Amenable to On-Site Screening? Biosensors 2022, 12, 608. https://doi.org/10.3390/bios12080608
Puiu M, Bala C. Affinity Assays for Cannabinoids Detection: Are They Amenable to On-Site Screening? Biosensors. 2022; 12(8):608. https://doi.org/10.3390/bios12080608
Chicago/Turabian StylePuiu, Mihaela, and Camelia Bala. 2022. "Affinity Assays for Cannabinoids Detection: Are They Amenable to On-Site Screening?" Biosensors 12, no. 8: 608. https://doi.org/10.3390/bios12080608
APA StylePuiu, M., & Bala, C. (2022). Affinity Assays for Cannabinoids Detection: Are They Amenable to On-Site Screening? Biosensors, 12(8), 608. https://doi.org/10.3390/bios12080608






