An Ultrasensitive Biosensor for Detection of Femtogram Levels of the Cancer Antigen AGR2 Using Monoclonal Antibody Modified Screen-Printed Gold Electrodes
Abstract
1. Introduction
2. Materials and Methods
2.1. Reagents and Materials
2.2. Electrochemical Procedures
2.3. Biomaterials Preparation and Identification by Reference Methods
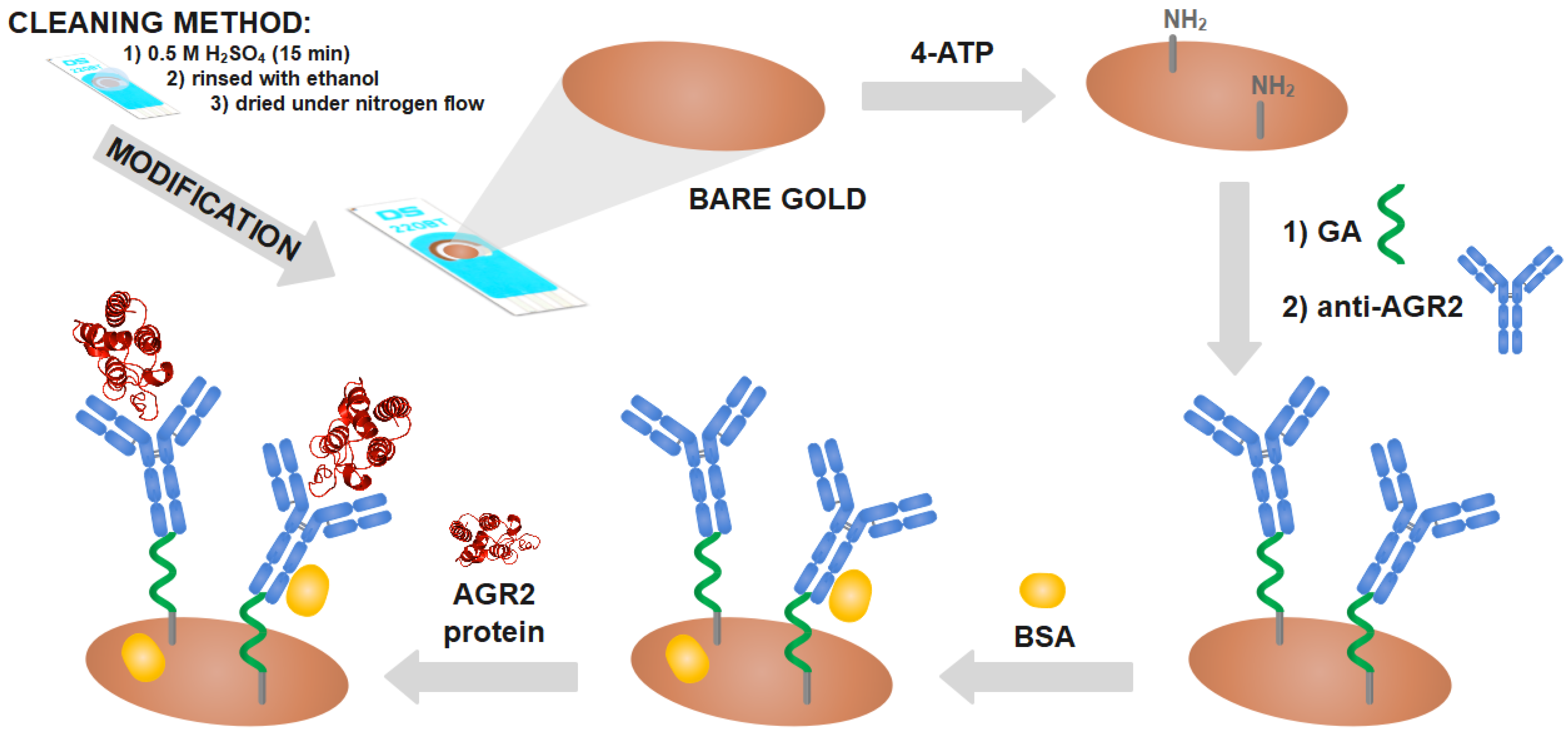
2.4. Preparation of the Immunosensor
3. Results
3.1. Characterization of the Modified Electrode
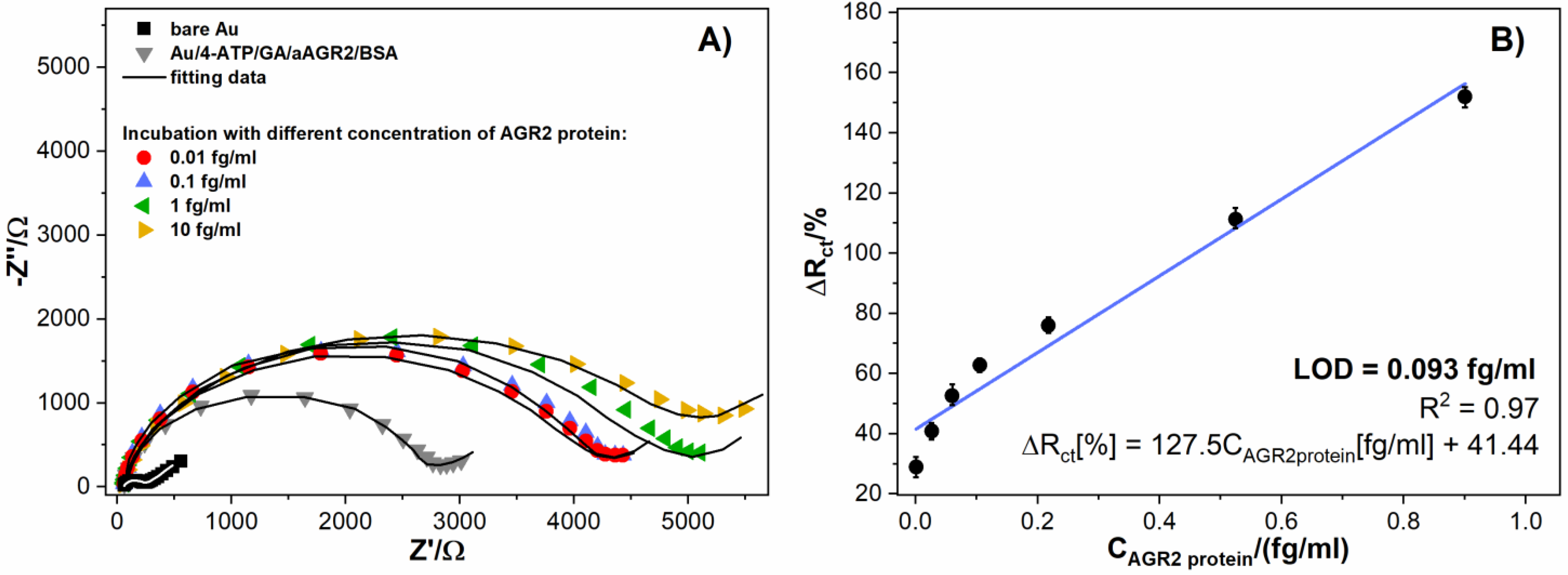
3.2. Impedance Measurements for the Detection of the AGR2 Protein
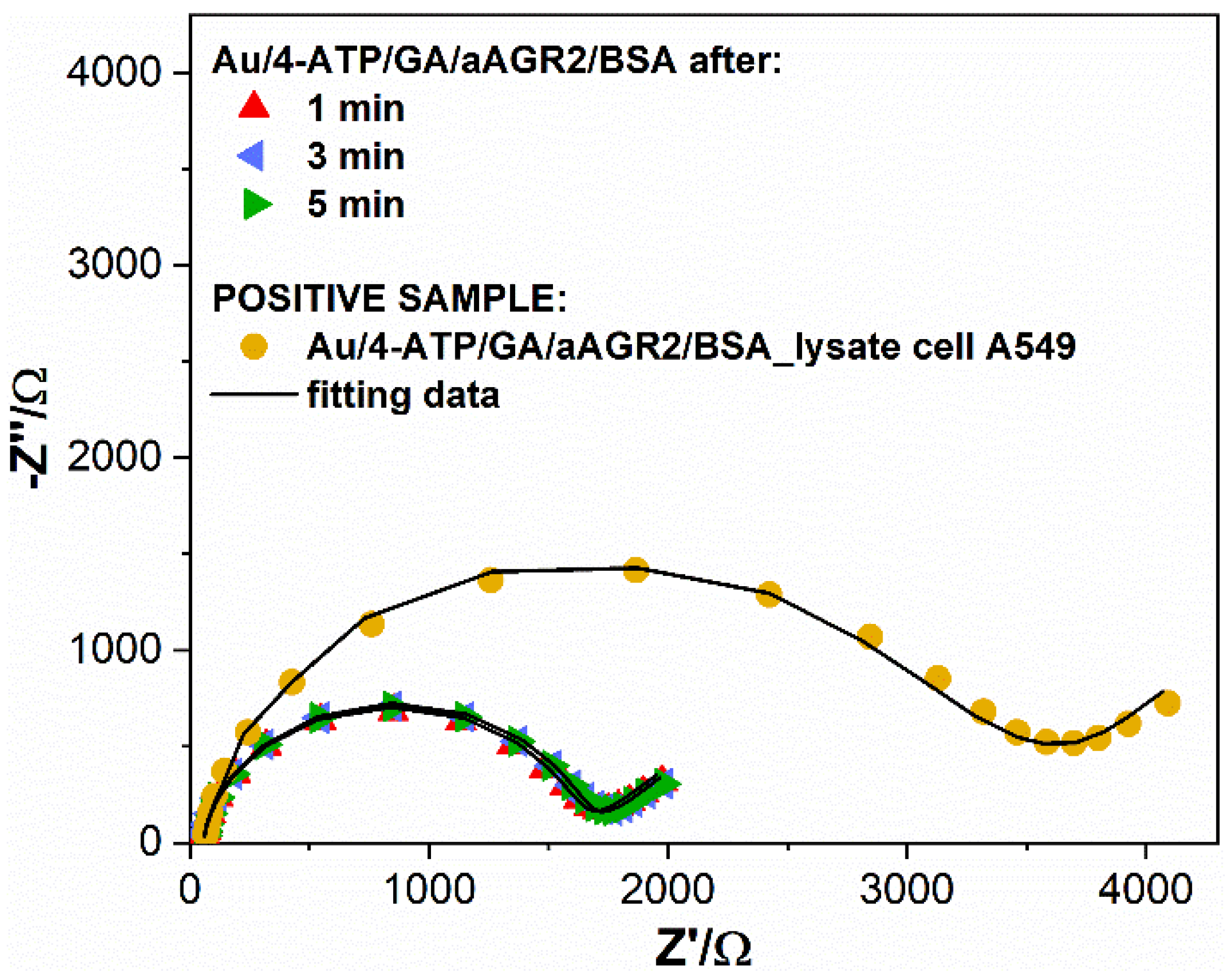
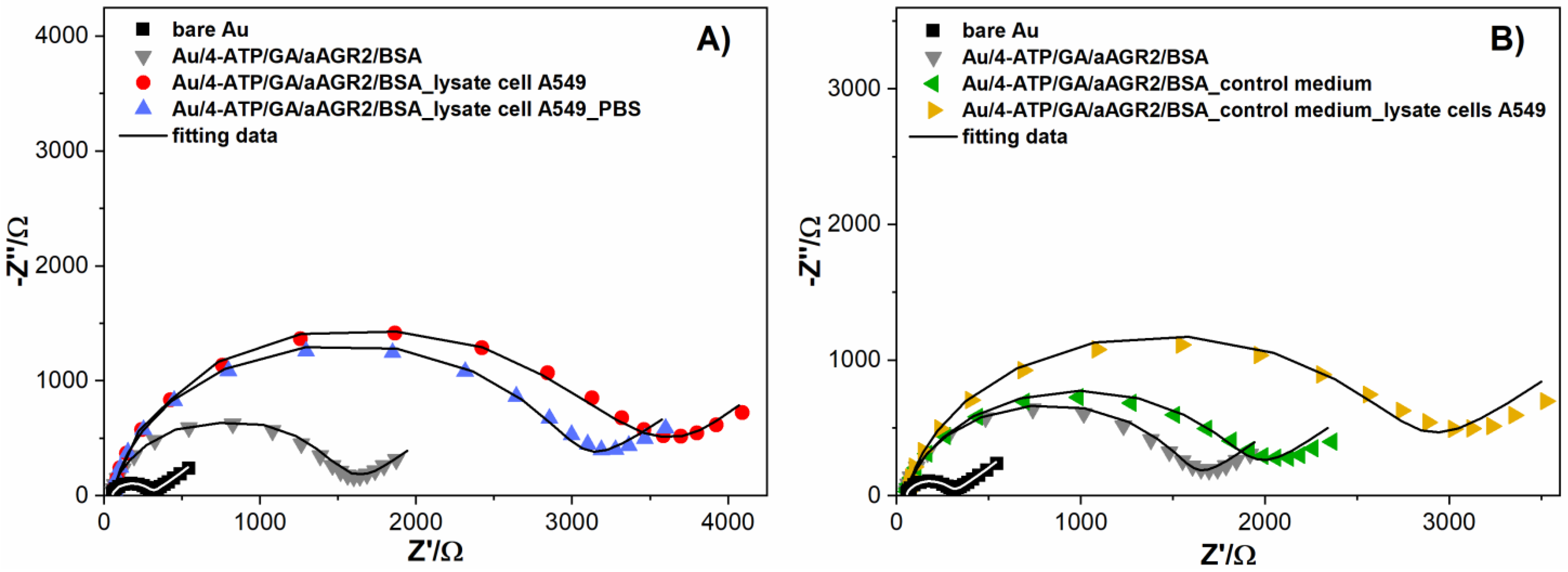
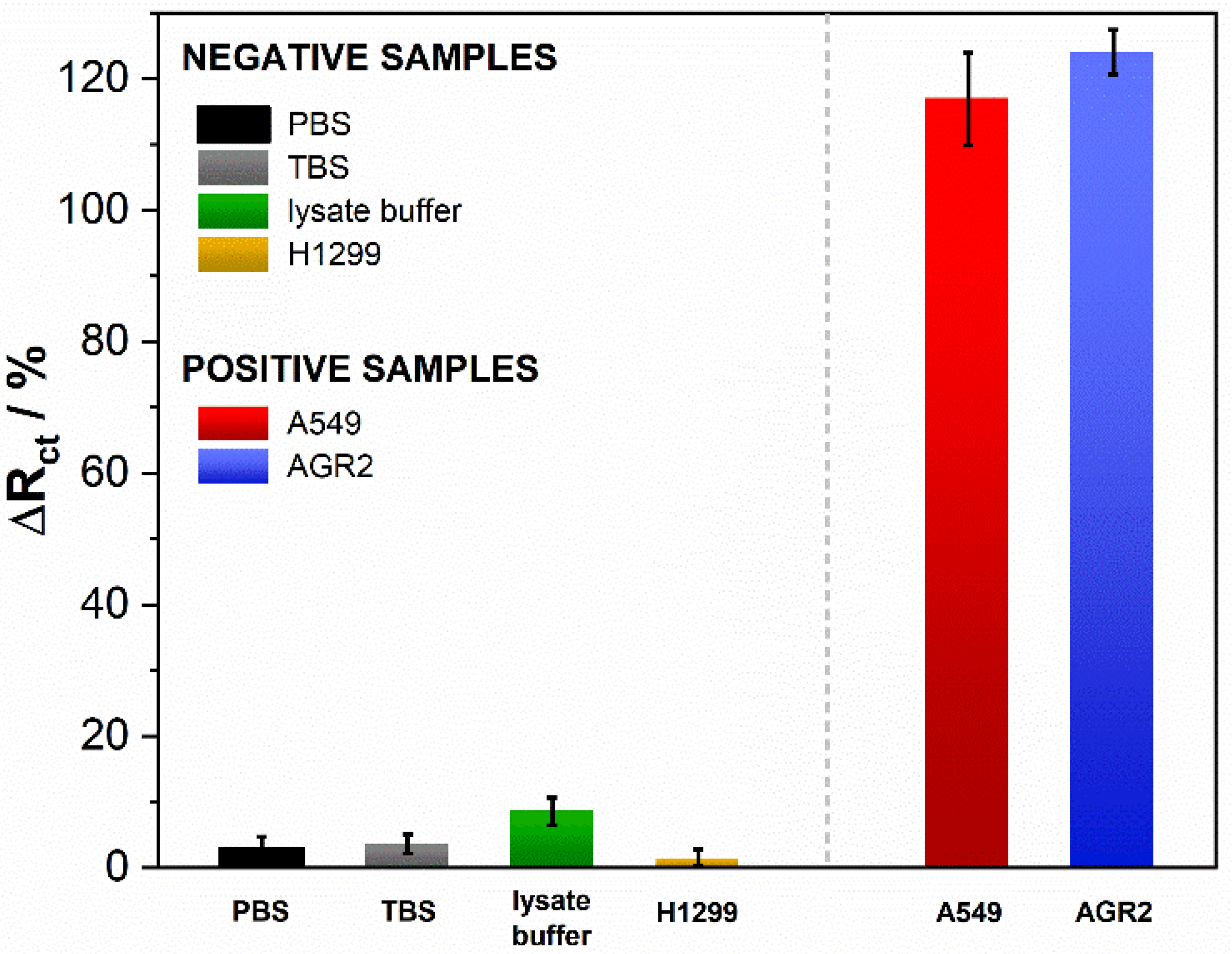
3.3. Biosensor Selectivity, Repeatability and Stability Studies
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Aberger, F.; Weidinger, G.; Grunz, H.; Richter, K. Anterior Specification of Embryonic Ectoderm: The Role of the Xenopus Cement Gland-Specific Gene XAG-2. Mech. Dev. 1998, 72, 115–130. [Google Scholar] [CrossRef]
- Thompson, D.A.; Weigel, R.J. HAG-2, the Human Homologue of TheXenopus LaevisCement Gland Gene XAG-2, Is Coexpressed with Estrogen Receptor in Breast Cancer Cell Lines. Biochem. Biophys. Res. Commun. 1998, 251, 111–116. [Google Scholar] [CrossRef]
- Persson, S.; Rosenquist, M.; Knoblach, B.; Khosravi-Far, R.; Sommarin, M.; Michalak, M. Diversity of the Protein Disulfide Isomerase Family: Identification of Breast Tumor Induced Hag2 and Hag3 as Novel Members of the Protein Family. Mol. Phylogenet. Evol. 2005, 36, 734–740. [Google Scholar] [CrossRef]
- Brychtova, V.; Mohtar, A.; Vojtesek, B.; Hupp, T.R. Mechanisms of Anterior Gradient-2 Regulation and Function in Cancer. Semin. Cancer Biol. 2015, 33, 16–24. [Google Scholar] [CrossRef] [PubMed]
- Tian, S.; Tao, K.; Hu, J.; Liu, Z.; Ding, X.; Chu, Y.; Cui, J.; Shuai, X.; Gao, J.; Cai, K.; et al. The Prognostic Value of AGR2 Expression in Solid Tumours: A Systematic Review and Meta-Analysis. Sci. Rep. 2017, 7, 15500. [Google Scholar] [CrossRef] [PubMed]
- Sive, H.L.; Hattori, K.; Weintraub, H. Progressive Determination during Formation of the Anteroposterior Axis in Xenopus Laevis. Cell 1989, 58, 171–180. [Google Scholar] [CrossRef]
- Patel, P.; Clarke, C.; Barraclough, D.L.; Jowitt, T.A.; Rudland, P.S.; Barraclough, R.; Lian, L.-Y. Metastasis-Promoting Anterior Gradient 2 Protein Has a Dimeric Thioredoxin Fold Structure and a Role in Cell Adhesion. J. Mol. Biol. 2013, 425, 929–943. [Google Scholar] [CrossRef]
- Kumar, A.; Godwin, J.W.; Gates, P.B.; Garza-Garcia, A.A.; Brockes, J.P. Molecular Basis for the Nerve Dependence of Limb Regeneration in an Adult Vertebrate. Science 2007, 318, 772–777. [Google Scholar] [CrossRef]
- Di Valentin, E.; Crahay, C.; Garbacki, N.; Hennuy, B.; Guéders, M.; Noël, A.; Foidart, J.-M.; Grooten, J.; Colige, A.; Piette, J.; et al. New Asthma Biomarkers: Lessons from Murine Models of Acute and Chronic Asthma. Am. J. Physiol. Lung Cell Mol. Physiol. 2009, 296, L185–L197. [Google Scholar] [CrossRef] [PubMed]
- Maurel, M.; Obacz, J.; Avril, T.; Ding, Y.-P.; Papadodima, O.; Treton, X.; Daniel, F.; Pilalis, E.; Hörberg, J.; Hou, W.; et al. Control of Anterior GRadient 2 (AGR2) Dimerization Links Endoplasmic Reticulum Proteostasis to Inflammation. EMBO Mol. Med. 2019, 11. [Google Scholar] [CrossRef]
- Fritzsche, F.R.; Dahl, E.; Pahl, S.; Burkhardt, M.; Luo, J.; Mayordomo, E.; Gansukh, T.; Dankof, A.; Knuechel, R.; Denkert, C.; et al. Prognostic Relevance of AGR2 Expression in Breast Cancer. Clin. Cancer Res. 2006, 12, 1728–1734. [Google Scholar] [CrossRef] [PubMed]
- Chanda, D.; Lee, J.H.; Sawant, A.; Hensel, J.A.; Isayeva, T.; Reilly, S.D.; Siegal, G.P.; Smith, C.; Grizzle, W.; Singh, R.; et al. Anterior Gradient Protein-2 Is a Regulator of Cellular Adhesion in Prostate Cancer. PLoS ONE 2014, 9, e89940. [Google Scholar] [CrossRef] [PubMed]
- Dumartin, L.; Alrawashdeh, W.; Trabulo, S.M.; Radon, T.P.; Steiger, K.; Feakins, R.M.; di Magliano, M.P.; Heeschen, C.; Esposito, I.; Lemoine, N.R.; et al. ER Stress Protein AGR2 Precedes and Is Involved in the Regulation of Pancreatic Cancer Initiation. Oncogene 2017, 36, 3094–3103. [Google Scholar] [CrossRef]
- Lepreux, S.; Bioulac-Sage, P.; Chevet, E. Differential Expression of the Anterior Gradient Protein-2 Is a Conserved Feature during Morphogenesis and Carcinogenesis of the Biliary Tree. Liver Int. 2011, 31, 322–328. [Google Scholar] [CrossRef] [PubMed]
- Gray, T.A.; MacLaine, N.J.; Michie, C.O.; Bouchalova, P.; Murray, E.; Howie, J.; Hrstka, R.; Maslon, M.M.; Nenutil, R.; Vojtesek, B.; et al. Anterior Gradient-3: A Novel Biomarker for Ovarian Cancer That Mediates Cisplatin Resistance in Xenograft Models. J. Immunol. Methods 2012, 378, 20–32. [Google Scholar] [CrossRef]
- Pohler, E.; Craig, A.L.; Cotton, J.; Lawrie, L.; Dillon, J.F.; Ross, P.; Kernohan, N.; Hupp, T.R. The Barrett’s Antigen Anterior Gradient-2 Silences the P53 Transcriptional Response to DNA Damage. Mol. Cell Proteom. 2004, 3, 534–547. [Google Scholar] [CrossRef]
- O’Neill, J.R.; Pak, H.-S.; Pairo-Castineira, E.; Save, V.; Paterson-Brown, S.; Nenutil, R.; Vojtěšek, B.; Overton, I.; Scherl, A.; Hupp, T.R. Quantitative Shotgun Proteomics Unveils Candidate Novel Esophageal Adenocarcinoma (EAC)-Specific Proteins. Mol. Cell Proteom. 2017, 16, 1138–1150. [Google Scholar] [CrossRef] [PubMed]
- Mohtar, M.A.; Hernychova, L.; O’Neill, J.R.; Lawrence, M.L.; Murray, E.; Vojtesek, B.; Hupp, T.R. The Sequence-Specific Peptide-Binding Activity of the Protein Sulfide Isomerase AGR2 Directs Its Stable Binding to the Oncogenic Receptor EpCAM. Mol. Cell Proteom. 2018, 17, 737–763. [Google Scholar] [CrossRef]
- Shriwash, N.; Singh, P.; Arora, S.; Ali, S.M.; Ali, S.; Dohare, R. Identification of Differentially Expressed Genes in Small and Non-Small Cell Lung Cancer Based on Meta-Analysis of MRNA. Heliyon 2019, 5, e01707. [Google Scholar] [CrossRef]
- Fessart, D.; Domblides, C.; Avril, T.; Eriksson, L.A.; Begueret, H.; Pineau, R.; Malrieux, C.; Dugot-Senant, N.; Lucchesi, C.; Chevet, E.; et al. Secretion of Protein Disulphide Isomerase AGR2 Confers Tumorigenic Properties. Elife 2016, 5, e13887. [Google Scholar] [CrossRef]
- Obacz, J.; Sommerova, L.; Sicari, D.; Durech, M.; Avril, T.; Iuliano, F.; Pastorekova, S.; Hrstka, R.; Chevet, E.; Delom, F.; et al. Extracellular AGR3 Regulates Breast Cancer Cells Migration via Src Signaling. Oncol. Lett. 2019, 18, 4449–4456. [Google Scholar] [CrossRef]
- Ho, M.E.; Quek, S.-I.; True, L.D.; Seiler, R.; Fleischmann, A.; Bagryanova, L.; Kim, S.R.; Chia, D.; Goodglick, L.; Shimizu, Y.; et al. Bladder Cancer Cells Secrete While Normal Bladder Cells Express but Do Not Secrete AGR2. Oncotarget 2016, 7, 15747–15756. [Google Scholar] [CrossRef]
- Shi, T.; Gao, Y.; Quek, S.I.; Fillmore, T.L.; Nicora, C.D.; Su, D.; Zhao, R.; Kagan, J.; Srivastava, S.; Rodland, K.D.; et al. A Highly Sensitive Targeted Mass Spectrometric Assay for Quantification of AGR2 Protein in Human Urine and Serum. J. Proteome Res. 2014, 13, 875–882. [Google Scholar] [CrossRef]
- Wayner, E.A.; Quek, S.-I.; Ahmad, R.; Ho, M.E.; Loprieno, M.A.; Zhou, Y.; Ellis, W.J.; True, L.D.; Liu, A.Y. Development of an ELISA to Detect the Secreted Prostate Cancer Biomarker AGR2 in Voided Urine. Prostate 2012, 72, 1023–1034. [Google Scholar] [CrossRef] [PubMed]
- Kani, K.; Malihi, P.D.; Jiang, Y.; Wang, H.; Wang, Y.; Ruderman, D.L.; Agus, D.B.; Mallick, P.; Gross, M.E. Anterior Gradient 2 (AGR2): Blood-Based Biomarker Elevated in Metastatic Prostate Cancer Associated with the Neuroendocrine Phenotype. Prostate 2013, 73, 306–315. [Google Scholar] [CrossRef]
- Edgell, T.A.; Barraclough, D.L.; Rajic, A.; Dhulia, J.; Lewis, K.J.; Armes, J.E.; Barraclough, R.; Rudland, P.S.; Rice, G.E.; Autelitano, D.J. Increased Plasma Concentrations of Anterior Gradient 2 Protein Are Positively Associated with Ovarian Cancer. Clin. Sci. (Lond.) 2010, 118, 717–725. [Google Scholar] [CrossRef]
- Liu, A.Y.; Kanan, A.D.; Radon, T.P.; Shah, S.; Weeks, M.E.; Foster, J.M.; Sosabowski, J.K.; Dumartin, L.; Crnogorac-Jurcevic, T. AGR2, a Unique Tumor-Associated Antigen, Is a Promising Candidate for Antibody Targeting. Oncotarget 2019, 10, 4276–4289. [Google Scholar] [CrossRef]
- Negi, H.; Merugu, S.B.; Mangukiya, H.B.; Li, Z.; Zhou, B.; Sehar, Q.; Kamle, S.; Yunus, F.-U.-N.; Mashausi, D.S.; Wu, Z.; et al. Anterior Gradient-2 Monoclonal Antibody Inhibits Lung Cancer Growth and Metastasis by Upregulating P53 Pathway and without Exerting Any Toxicological Effects: A Preclinical Study. Cancer Lett. 2019, 449, 125–134. [Google Scholar] [CrossRef] [PubMed]
- Garri, C.; Howell, S.; Tiemann, K.; Tiffany, A.; Jalali-Yazdi, F.; Alba, M.M.; Katz, J.E.; Takahashi, T.T.; Landgraf, R.; Gross, M.E.; et al. Identification, Characterization and Application of a New Peptide against Anterior Gradient Homolog 2 (AGR2). Oncotarget 2018, 9, 27363–27379. [Google Scholar] [CrossRef] [PubMed]
- Murray, E.; McKenna, E.O.; Burch, L.R.; Dillon, J.; Langridge-Smith, P.; Kolch, W.; Pitt, A.; Hupp, T.R. Microarray-Formatted Clinical Biomarker Assay Development Using Peptide Aptamers to Anterior Gradient-2. Biochemistry 2007, 46, 13742–13751. [Google Scholar] [CrossRef]
- Gray, T.A.; Murray, E.; Nowicki, M.W.; Remnant, L.; Scherl, A.; Muller, P.; Vojtesek, B.; Hupp, T.R. Development of a Fluorescent Monoclonal Antibody-Based Assay to Measure the Allosteric Effects of Synthetic Peptides on Self-Oligomerization of AGR2 Protein. Protein Sci. 2013, 22, 1266–1278. [Google Scholar] [CrossRef]
- Nidzworski, D.; Siuzdak, K.; Niedziałkowski, P.; Bogdanowicz, R.; Sobaszek, M.; Ryl, J.; Weiher, P.; Sawczak, M.; Wnuk, E.; Goddard, W.A.; et al. A Rapid-Response Ultrasensitive Biosensor for Influenza Virus Detection Using Antibody Modified Boron-Doped Diamond. Sci. Rep. 2017, 7, 15707. [Google Scholar] [CrossRef] [PubMed]
- Malinowska, N.; Białobrzeska, W.; Łęga, T.; Pałka, K.; Dziąbowska, K.; Żołędowska, S.; Czaczyk, E.; Pala, K.; Nidzworski, D. Antibody Modified Gold Electrode as an Impedimetric Biosensor for the Detection of Streptococcus Pyogenes. Sensors 2020, 20, 5324. [Google Scholar] [CrossRef]
- Gray, T.; Alsamman, K.; Murray, E.; Sims, A.; Hupp, T. Engineering a Synthetic Cell Panel to Identify Signalling Components Reprogrammed by the Cell Growth Regulator Anterior Gradient-2. Mol. Biosyst. 2014, 10. [Google Scholar] [CrossRef]
- Randles, J.E.B. Kinetics of Rapid Electrode Reactions. Discuss. Faraday Soc. 1947, 1, 11–19. [Google Scholar] [CrossRef]
- Białobrzeska, W.; Firganek, D.; Czerkies, M.; Lipniacki, T.; Skwarecka, M.; Dziąbowska, K.; Cebula, Z.; Malinowska, N.; Bigus, D.; Bięga, E.; et al. Electrochemical Immunosensors Based on Screen-Printed Gold and Glassy Carbon Electrodes: Comparison of Performance for Respiratory Syncytial Virus Detection. Biosensors 2020, 10, 175. [Google Scholar] [CrossRef]
- Cebula, Z.; Żołędowska, S.; Dziąbowska, K.; Skwarecka, M.; Malinowska, N.; Białobrzeska, W.; Czaczyk, E.; Siuzdak, K.; Sawczak, M.; Bogdanowicz, R.; et al. Detection of the Plant Pathogen Pseudomonas Syringae Pv. Lachrymans on Antibody-Modified Gold Electrodes by Electrochemical Impedance Spectroscopy. Sensors 2019, 19, 5411. [Google Scholar] [CrossRef]
- Niedzialkowski, P.; Slepski, P.; Wysocka, J.; Chamier-Cieminska, J.; Burczyk, L.; Sobaszek, M.; Wcislo, A.; Ossowski, T.; Bogdanowicz, R.; Ryl, J. Multisine Impedimetric Probing of Biocatalytic Reactions for Label-Free Detection of DEFB1 Gene: How to Verify That Your Dog Is Not Human? Sens. Actuators B Chem. 2020, 323, 128664. [Google Scholar] [CrossRef]
- Augustine, S.; Kumar, P.; Malhotra, B.D. Amine-Functionalized MoO3@RGO Nanohybrid-Based Biosensor for Breast Cancer Detection. ACS Appl. Biol. Mater. 2019, 2, 5366–5378. [Google Scholar] [CrossRef]
- Gajdosova, V.; Lorencova, L.; Kasak, P.; Tkac, J. Electrochemical Nanobiosensors for Detection of Breast Cancer Biomarkers. Sensors 2020, 20, 4022. [Google Scholar] [CrossRef]
- Roberts, A.; Tripathi, P.P.; Gandhi, S. Graphene Nanosheets as an Electric Mediator for Ultrafast Sensing of Urokinase Plasminogen Activator Receptor-A Biomarker of Cancer. Biosens. Bioelectron. 2019, 141, 111398. [Google Scholar] [CrossRef] [PubMed]
- Negahdary, M. Aptamers in Nanostructure-Based Electrochemical Biosensors for Cardiac Biomarkers and Cancer Biomarkers: A Review. Biosens. Bioelectron. 2020, 152, 112018. [Google Scholar] [CrossRef]
- Kilic, T.; Valinhas, A.T.D.S.; Wall, I.; Renaud, P.; Carrara, S. Label-Free Detection of Hypoxia-Induced Extracellular Vesicle Secretion from MCF-7 Cells. Sci. Rep. 2018, 8, 9402. [Google Scholar] [CrossRef]
- Nawaz, M.A.H.; Rauf, S.; Catanante, G.; Nawaz, M.H.; Nunes, G.; Marty, J.L.; Hayat, A. One Step Assembly of Thin Films of Carbon Nanotubes on Screen Printed Interface for Electrochemical Aptasensing of Breast Cancer Biomarker. Sensors 2016, 16, 1651. [Google Scholar] [CrossRef] [PubMed]
- Luo, L.; Wang, L.; Zeng, L.; Wang, Y.; Weng, Y.; Liao, Y.; Chen, T.; Xia, Y.; Zhang, J.; Chen, J. A Ratiometric Electrochemical DNA Biosensor for Detection of Exosomal MicroRNA. Talanta 2020, 207, 120298. [Google Scholar] [CrossRef]
- Tang, Y.; Dai, Y.; Huang, X.; Li, L.; Han, B.; Cao, Y.; Zhao, J. Self-Assembling Peptide-Based Multifunctional Nanofibers for Electrochemical Identification of Breast Cancer Stem-like Cells. Anal. Chem. 2019, 91, 7531–7537. [Google Scholar] [CrossRef]
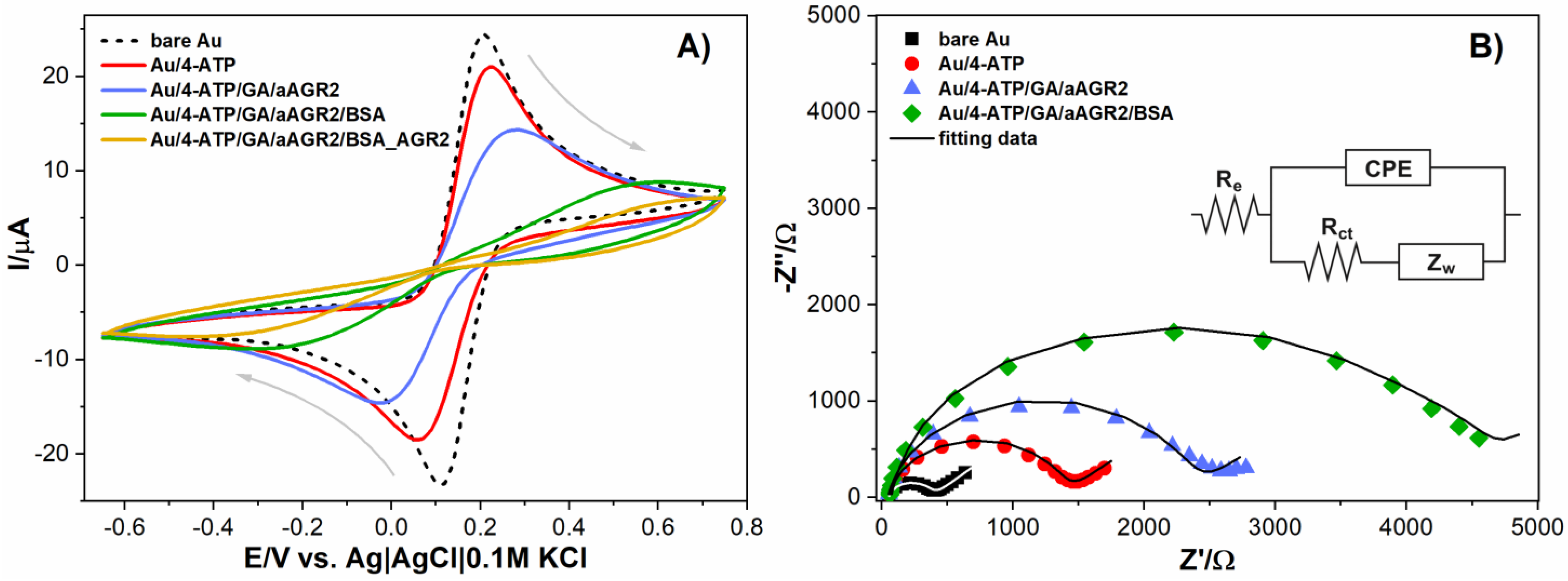
| Sample | Re [Ω] | CPE [μΩ−1sn] | n | Rct [Ω] | AW [Ωs−0.5] |
|---|---|---|---|---|---|
| bare Au | 50.058 | 2.62 | 0.915 | 315.57 | 3.893 |
| Au/4-ATP/GA/aAGR2 | 49.896 | 0.90 | 0.951 | 2223.9 | 701.63 |
| Au/4-ATP/GA/aAGR2/BSA | 53.244 | 0.98 | 0.939 | 2259.2 | 824.3 |
| Au/4-ATP/GA/aAGR2/BSA_protein AGR2 0.01 fg/mL | 48.971 | 1.06 | 0.920 | 3449.3 | 1266.8 |
| Au/4-ATP/GA/aAGR2/BSA_protein AGR2 0.1 fg/mL | 50.617 | 1.09 | 0.920 | 3704.4 | 1308.4 |
| Au/4-ATP/GA/aAGR2/BSA_protein AGR2 1 fg/mL | 67.882 | 1.18 | 0.920 | 4887.6 | 1658.3 |
| Au/4-ATP/GA/aAGR2/BSA_protein AGR2 10 fg/mL | 68.882 | 1.20 | 0.920 | 5790,9 | 1667.6 |
| Detection Substrate | Target Molecules | Turnaround Time | Sensitivity | Limit of Detection | Reference |
|---|---|---|---|---|---|
| ITO (CV, DPV, EIS) | CA15-3 | 15 min | 13 µL−1ng/cm−2 | 0.001 ng/mL | [39,40] |
| FTO (CV) | plasminogen activator receptor | 35 s | - | 4.8 fM | [40,41] |
| Polypyrrole-gold nanocomposite (DPV) | CA125 | 80 min | - | 30.9 ng/mL | [42] |
| AuSPE (EIS, DPV) | MCF-7 | 91 s | 77 EVs/mL | 77 particles/mL | [40,43] |
| SPCE (CV, EIS) | MUC1 | 45 min | - | 0.02 U/mL | [40,44] |
| GCE (DPV, Polylysine modification) | AGR2 | 90 min | - | 2.3 fM | [40,45] |
| GE (DPV, AgNPs modification) | AR-42 | 90 min | - | 6 cells/mL | [40,46] |
| Au (EIS) | AGR2 | 3 min | 127.5%(fg/mL)−1 | 0.093 fg/mL | this work |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Białobrzeska, W.; Dziąbowska, K.; Lisowska, M.; Mohtar, M.A.; Muller, P.; Vojtesek, B.; Krejcir, R.; O’Neill, R.; Hupp, T.R.; Malinowska, N.; et al. An Ultrasensitive Biosensor for Detection of Femtogram Levels of the Cancer Antigen AGR2 Using Monoclonal Antibody Modified Screen-Printed Gold Electrodes. Biosensors 2021, 11, 184. https://doi.org/10.3390/bios11060184
Białobrzeska W, Dziąbowska K, Lisowska M, Mohtar MA, Muller P, Vojtesek B, Krejcir R, O’Neill R, Hupp TR, Malinowska N, et al. An Ultrasensitive Biosensor for Detection of Femtogram Levels of the Cancer Antigen AGR2 Using Monoclonal Antibody Modified Screen-Printed Gold Electrodes. Biosensors. 2021; 11(6):184. https://doi.org/10.3390/bios11060184
Chicago/Turabian StyleBiałobrzeska, Wioleta, Karolina Dziąbowska, Małgorzata Lisowska, M. Aiman Mohtar, Petr Muller, Borivoj Vojtesek, Radovan Krejcir, Robert O’Neill, Ted R. Hupp, Natalia Malinowska, and et al. 2021. "An Ultrasensitive Biosensor for Detection of Femtogram Levels of the Cancer Antigen AGR2 Using Monoclonal Antibody Modified Screen-Printed Gold Electrodes" Biosensors 11, no. 6: 184. https://doi.org/10.3390/bios11060184
APA StyleBiałobrzeska, W., Dziąbowska, K., Lisowska, M., Mohtar, M. A., Muller, P., Vojtesek, B., Krejcir, R., O’Neill, R., Hupp, T. R., Malinowska, N., Bięga, E., Bigus, D., Cebula, Z., Pala, K., Czaczyk, E., Żołędowska, S., & Nidzworski, D. (2021). An Ultrasensitive Biosensor for Detection of Femtogram Levels of the Cancer Antigen AGR2 Using Monoclonal Antibody Modified Screen-Printed Gold Electrodes. Biosensors, 11(6), 184. https://doi.org/10.3390/bios11060184








