1. Introduction
New blood vessel formation is crucial to supplying nutrients and oxygen to cells and to remove waste products during the engineering of new tissues. For the successful development of a functional vascular network, adequate and clinically applicable biomaterials are required to provide a suitable environment for the construction of new blood vessels and to avoid cellular toxicity. Strategies that have been used to enhance vascularization include the delivery of angiogenic factors such as vascular endothelial growth factor (VEGF) and sphingosine-1-phosphate (S1P) into biomaterials as therapeutic agents to promote blood vessel formation [
1,
2,
3,
4].
Therapeutic approaches for microvasculature formation using mesenchymal stem cells (MSCs) have been developed. MSCs have the potential to differentiate into multiple lineages including vascular and endothelial lineages [
5,
6,
7]. Additionally, MSCs exhibit the features and characteristics of the perivascular cells known as pericyte [
8]. Pericytes contribute to the stabilization, maintenance, and hemodynamic processes of blood vessels by acting as angiogenic stimuli and guiding the sprouting of vessels [
9]. MSCs may similarly contribute to vascular formation and could be an alternative cell source in vascular grafts or tissue engineering. More recently, cell-based approaches proposed to exploit the intrinsic vasculogenic or angiogenic capacity of endothelial cells (ECs) or endothelial progenitor cells with intercellular interactions with MSCs [
10,
11,
12,
13,
14,
15]. The collective data indicate the capability of co-cultures with MSCs and ECs in the development of blood vessels in vivo after cell transplantation. Both cell types are appealing sources for generating functional vascular networks for tissue regeneration applications [
16]. One of the MSCs, adipose-derived mesenchymal stem cells (ADSCs) have emerged as a novel source of neovascularization that secretes various angiogenic factors (including VEGF, angiopoietin, and a variety of microRNAs) more than bone-marrow-derived MSCs [
17,
18]. This finding suggests that ADSCs may be a powerful candidate for blood vessel regeneration.
The design of cellular scaffolds using synthetic and natural polymers and extracellular matrix (ECM) components is a crucial factor for the production of functionally-engineered microvessel structures in vitro. These polymers and the ECM can provide appropriate cell adhesion sites and promote cell proliferation and protein synthesis during vasculogenesis and angiogenesis. In the most current models of engineered blood vessel development, cells are cultured in or on biomaterial-based porous scaffolds such as matrigel, hydroxyapatite, calcium phosphate, beta-tricalcium phosphate (β-TCP), and collagen; all these are favorable microenvironments for vascular morphogenesis [
19,
20]. These various approaches to promoting vascular formation have been successful in the production of microvessels. However, these scaffolds have some properties that are not ideal for tissue engineering applications and which have precluded them from clinical trial evaluation; these include poor mechanical support of cells, immunogenic problems, and inadequate mimicry of the ECM environment.
These barriers might be overcome by the blending of the ECM component protein, and a Food and Drug Administration (FDA) approved polymer to make functional cellular scaffolds. A recent approach for the design of tissue engineering scaffolds is the electrospun fiber scaffold. This method improves cell adhesion, proliferation, and stem cell differentiation. Electrospinning successfully provides three-dimensional (3D) culture conditions and suitable mechanical durability that mimics the fibrous hierarchical structure of the ECM [
21,
22,
23,
24,
25,
26]. For several potential tissue engineering applications and clinical trials, it is desirable to develop scaffolds that are biocompatible and mechanically stable, which can control the scale from the microscopic to nanoscopic level to mimic the real tissue microenvironments.
To accomplish this, we fabricated electrospun nanofibers consisting of blended polycaprolactone (PCL) and gelatin as permissive scaffolds for the formation of functional vascular networks. Additionally, co-culturing of human umbilical vein endothelial cells (HUVECs) and human adipose-derived mesenchymal stem cells (hADSCs) was performed to explore the efficacy of the intercellular interactions in enhancing blood vessel formation through direct cell–cell contact and paracrine signaling on the nanofibrous scaffolds. VEGF and S1P were used as angiogenic factors in the cell culture medium, as the biochemical cues to promote the vascular morphogenesis of HUVECs. After construction of the cellular PCL/gelatin nanofiber scaffolds, we investigated the vasculogenic or angiogenic activities of the monocultured or co-cultured HUVECs, such as cell proliferation, morphogenesis, protein expression, and lumen formation. The results demonstrated that extensive vascular networks could be generated in a co-culture system in a nanofibrous environment.
2. Materials and Methods
2.1. Preparation of Electrospun Fibrous Scaffolds
PCL/gelatin nanofibrous scaffolds were fabricated by using a previous electrospinning process [
27]. The solutions for electrospinning were prepared by dissolving PCL (MW: 80,000; Sigma Aldrich, St. Louis, MO, USA) and gelatin (from bovine skin, Type B; Sigma Aldrich, St. Louis, MO, USA) (1:1 weight ratio) in 2, 2, 2-trifluoroethanol (TFE; Sigma Aldrich, St. Louis, MO, USA) to form a 10%
w/
v solution. A 7.5 kV positive voltage was applied to the PCL/gelatin solution via a 25-gauge stainless steel needle with a continuous flow rate of 1.0 mL/h using a syringe pump (NanoNC, Seoul, Korea) for 20 min at room temperature to generate randomly-oriented, electrospun PCL/gelatin nanofibers. The distance between the tip of the needle and the collecting plate was always at 15 cm. To make nanofibrous scaffolds with same size, cover glasses (18 × 18 mm) wrapped with clean aluminum foil were deposited on the collecting plate during the electrospinning process.
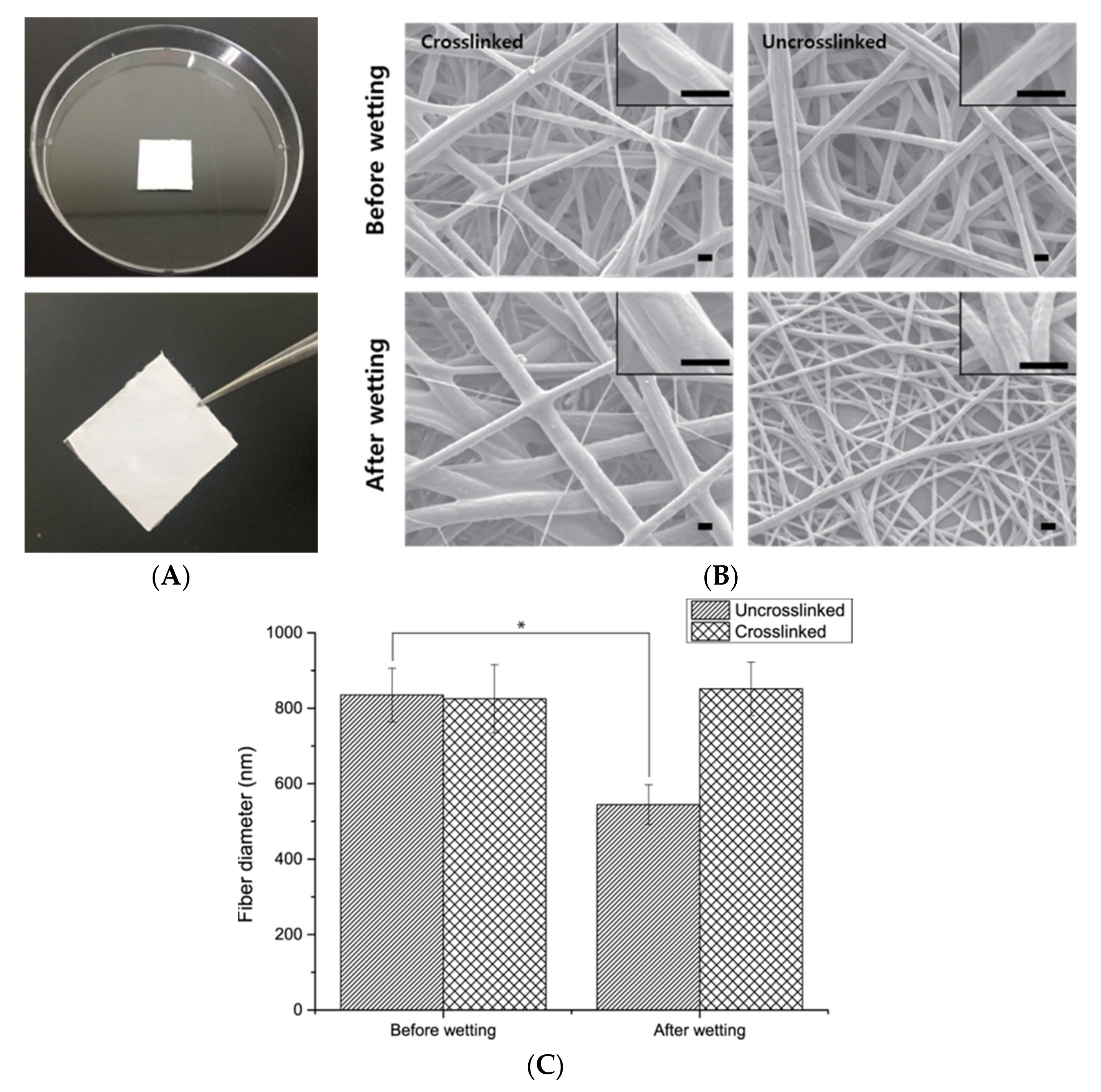
The resultant fibers were crosslinked using a conventional vapor crosslinking method. Briefly, the PCL/gelatin nanofiber sheets were placed in a sealed desiccator containing an aqueous genipin solution (25 mg/mL in dimethyl sulfoxide) at room temperature for 24 h. The PCL/gelatin nanofiber mats were treated in a vacuum oven at 37 °C overnight to eliminate residual organic solvent from the electrospinning process and genipin followed by washing with Dulbecco’s phosphate buffered saline (DPBS). To confirm the crosslinking of gelatin, uncrosslinked and crosslinked PCL/gelatin nanofiber sheets were immersed in distilled water for 24 h and dried at room temperature for 12 h. The morphology of the resultant fibrous scaffolds was observed using scanning electron microscopy (SEM) with a model 7800 F apparatus (JEOL, Tokyo, Japan).
2.2. Isolation and Cultivation of hADSCs
We obtained human adipose tissues from the immediate transverse rectus abdominis musculocutaneous flaps of patients who underwent breast cancer surgery. We got agreements from patients to take adipose tissue at surgery and use them for research. All the experimental protocols using this patient-derived adipose tissue were approved by the Institutional Review Board (IRB, B-1612-374-305) for human subject protection at Seoul National University Bundang Hospital. The tissues were washed with phosphate buffer saline (PBS) containing 1% penicillin/streptomycin and minced with autoclaved scissors, followed by digestion with Dulbecco’s modified Eagle’s medium (DMEM; Welegene Inc., Daegu, Korea) containing 0.1% type I collagenase for 1 h at 37 °C. The tissues were filtered in the 50ml conical tube using a strainer and immersed in DMEM supplemented with 10% fetal bovine serum (FBS; CellSera, Rutherford, Austrailia) and 1% (v/v) penicillin/streptomycin. To obtain pure hADSCs, tissues were washed five times with saline and centrifuged at 1300 rpm for 5 min. Supernatant media and floating mature adipocytes were discarded. The pellets contained pure hADSCs. To determine whether the isolated cells were hADSCs, we observed the expression of the several surface makers of hADSCs using flow cytometry. Briefly, hADSCs at passage four were treated with trypsin– ethylenediaminetetraacetic acid (EDTA) and centrifuged, followed by washing with PBS twice. The collected hADSCs were filtered (35 μm nylon mesh) and diluted with 100 μL PBS in a facs tube (Corning Inc., New York, NY, USA). Each of the tubes was labeled as control (Mouse IgG), negative (CD19, CD45), and positive (CD44, CD73, CD90, CD105) using phycoerythrin-conjugated antibodies (BD Biosciences, San Jose, CA, USA) and wrapped using aluminum foil followed by incubation for 4 h with shaking at room temperature. Labeled hADSCs were analyzed using a flow cytometry device (BD FACS Aria II flow cytometer, BD Bioscience, San Jose, CA, USA).
The hADSCs were seeded in 75 T flasks and cultured in DMEM containing 10% FBS (CellSera) and 1% (v/v) penicillin/streptomycin at 37 °C in a humid atmosphere containing 5% CO2. After a day, the non-adherent cells were discarded, and the adherent cells were cultured in fresh medium. The medium was changed every two days. All the experimental protocols were approved by Seoul National University Bundang Hospital.
2.3. Cultivation of HUVECs
HUVECs (C2517A) were purchased from Lonza Inc. (Basel, Switzerland). The HUVECs were cultured on tissue culture flasks in endothelial basal medium (EBM-2, Lonza, Basel, Switzerland) with Single Quotes endothelial growth supplement (Lonza, Basel, Switzerland) and an antibiotic-antimycotic mixture (1% v/v) at 37 °C in a humid atmosphere containing 5% CO2. The medium was changed, and non-adherent cells were discarded every two days. When the cells reached 90~95% confluence in the culture flasks, HUVECs were subcultured to new flasks using 0.25% trypsin–EDTA solution.
2.4. Co-Culture of ADSCs and HUVECs on Nanofibrous Scaffolds
To confirm the effect of the co-culture system on the vascular structure formation of HUVECs, electrospun PCL/gelatin nanofibrous scaffolds were utilized. First, the PCL/gelatin nanofiber scaffolds were immersed in the EGM-2 medium for 30 min to increase cell attachment at 37 °C. Next, ADSCs and HUVECs (2 × 105 cells per scaffold, cell ratio of 1:3) were seeded on the nanofibrous scaffolds for co-culture system and monocultures were also established. In both the monoculture and co-culture systems, the total number of cells used for seeding was held constant regardless of the cells used. After allowing 2 h for the cell adhesion, the cells on the scaffolds were cultured in HUVEC growth medium for up to seven days. For the two-dimensional (2D) culture system, the same procedures were performed on a 24-well plate (SPL, Gyeonggi, Korea). To enhance the vascular structure formation of ECs and compare the effects of the growth factors on blood vessel development during 2D and 3D growth, S1P and VEGF were supplemented in the cell culture medium at concentrations of 250 nM and 50 ng/mL, respectively. These experiments were also carried using 24-well plates as a negative control. ADSCs and HUVECs were seeded onto the nanofibers and well plate at passage 4–6 and 5–7, respectively.
2.5. Cell Proliferation and Viability
2.5.1. Cell Proliferation
To investigate the proliferation of ADSCs and HUVECs on scaffolds, a Cell Counting Kit-8 assay (CCK-8; Dojindo Laboratories, Kumamoto, Japan) was carried out at one, four, and seven days after cell seeding. Both cell types were seeded on the scaffolds (2 × 105 cells per scaffold preparation for monoculture and co-culture groups) followed by the 10% v/v CCK-8 solution into the culture medium. After the samples were incubated for 4 h at 37 °C, cell proliferation was investigated by measuring the absorbance at 450 nm using a microplate reader (Biotek, Winooski, VT, USA).
2.5.2. Cell Viability Assay
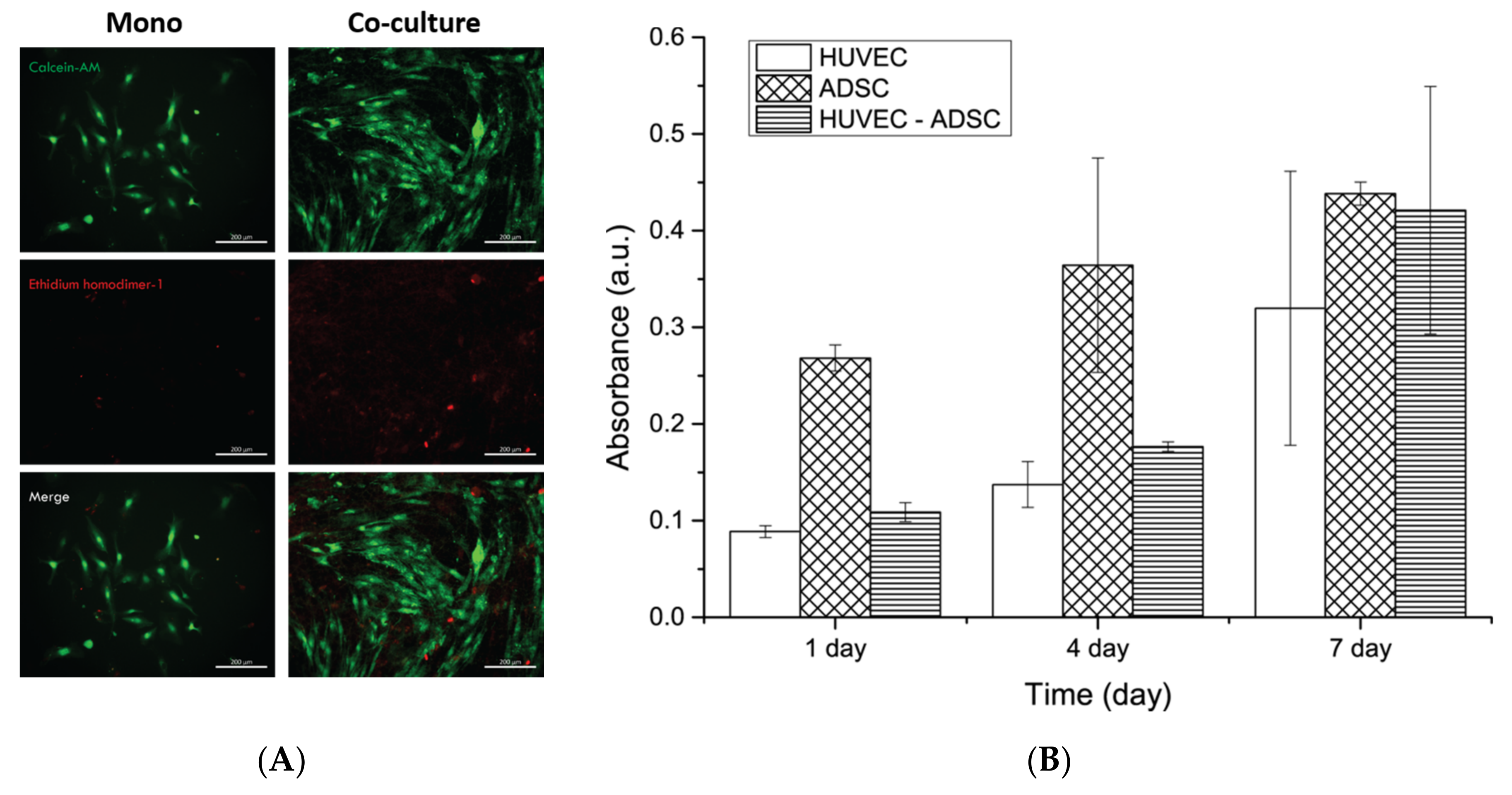
To assess the cell viability, a LIVE/DEAD® Viability/Cytotoxicity Kit for mammalian cells (Invitrogen, Carlsbad, CA, USA), was used according to the manufacturer’s protocol. Briefly, both cells types were seeded on the scaffolds (2 × 105 cells per scaffolds for both monoculture and co-culture groups). At seven days after culture, cell viability was measured by the exposure of cells to LIVE/DEAD solution (4 mM Calcein AM-green; live cells and 2 mM Ethidium homodimer-1-red; dead cells) for 30 min at room temperature. The cells were then visualized under a laser scanning microscope (Carl Zeiss, Oberkochen, Germany).
2.6. Immunofluorescence Analysis of Vascular Formation of HUVECs
For immunofluorescence staining, cell-laden scaffolds were washed and fixed in 4% paraformaldehyde for 10 min at room temperature, then permeabilized with 0.1% Triton X-100 in 1× PBS for 3 min at room temperature. After washing with 1× PBS, the cells were blocked using 1% bovine serum albumin (BSA) in 1× PBS for 1 h at room temperature before incubation overnight at 4 °C with primary antibodies against cluster of differentiation 31/platelet endothelial cell adhesion molecule (CD31/PECAM; 1:25 dilution; R&D Systems, Minneapolis, MN, USA) or podocalyxin (1:500 dilution; Abcam, Cambridge, UK). The samples were washed and then exposed to Alexa Fluor 568-conjugated secondary antibody (1:500 dilution; Abcam, Cambridge, UK) for 1 h at room temperature in the dark. F-actin was labeled with Alexa Fluor 488-conjugated phalloidin (1:300 dilution; Cell Signaling Technology, Danvers, MA, USA) and the nuclei were counterstained with 4′,6-diamidino-2-phenylindole, dihydrochloride (DAPI; Sigma Aldrich, St. Louis, MO, USA). To confirm the lumen structure formation, consecutive z-stack images of HUVECs labeled with phalloidin and DAPI in 2D, and 3D conditions, with an interval thickness of 3 μm, were acquired. The labeled cells were visualized using a laser scanning microscope. Cell length and aspect ratio values were obtained by analyzing the cell bodies expressing the junction proteins using the ZEN 2 software (Carl Zeiss, Oberkochen, Germany).
2.7. Statistical Analysis
All data are presented as the mean ± standard deviation. Each experiment was performed five times, and the differences of data were compared using one-way analysis of variance (ANOVA) followed by Tukey’s post hoc test. A p-value < 0.05 was considered statistically significant and is denoted as (*). The error bars represent the standard deviation between the experimental groups. Statistical analyses were conducted using the SigmaPlot 13.0 (Systat Software Inc., San Jose, CA, USA).
4. Discussion
In this study, we investigated the efficacy of the co-culture of HUVECs and ADSCs in vascular morphogenesis using PCL/gelatin nanofiber scaffolds, which were capable of cell adhesion, proliferation, and assembly into a blood-vessel-like structure. PCL/gelatin fibers were prepared from a uniform blend of PCL and gelatin. Bare PCL fiber is too hydrophobic for cell adherence and proliferation. However, the incorporation of the gelatin component of the ECM renders the fiber more hydrophilic and makes it biocompatible, both of which improve cell adhesion, proliferation, migration, and differentiation in the fibrous environment [
28]. However, because gelatin can be easily dissolved in an aqueous cell culture environment, gelatin crosslinking is necessary to maintain the cell-friendly functions of PCL/gelatin nanofiber scaffolds. Although many studies used glutaraldehyde to crosslink gelatin to prevent dissolution during cell culture, glutaraldehyde is cytotoxic. Hence, we used genipin as the crosslinking agent. Genipin crosslinks spontaneously with proteins and some natural polymers [
29]. On the contrary, because PCL fiber have mechanical properties that support cells in a manner reminiscent of natural ECM, incorporated PCL/gelatin nanofiber scaffolds can endure more vertical and lateral forces by cells than bare gelatin fibers. The fabricated PCL/gelatin nanofibrous scaffolds were biocompatible and allowed appropriate cell viability and proliferation regardless of the cell type during the cell culture periods (
Figure 4A,B).
To observe the effects of co-culture and the presence of growth factors on blood vessel formation, HUVECs were cultured in a 2D system alone or along with ADSCs on PCL/gelatin nanofiber scaffolds with two different growth factors in the culture medium. The co-cultures were suspensions of ADSCs to HUVECs (1:3 ratio) that were seeded on the experimental surfaces. This ratio was used based on the prior finding that higher ADSC and HUVEC ratios can result in more abundant blood vessel regeneration on biocompatible scaffolds [
30]. In these culture conditions, the two types of cells interacted through direct cell–cell interaction and a paracrine effect, in which soluble factors from other types of cells are shared. To enhance vasculature structure formation, we chose two different growth factors, S1P and VEGF, to supplement the culture medium. S1P is a pro-angiogenic factor that tightens the vascular-endothelial junctions and promotes vascular maturation through S1P signaling [
31,
32]. VEGF is commonly used for blood vessel regeneration because it induces the growth of pre-existing or new vessels in several organs [
33]. Although a previous study observed that a cocktail of these growth factors enhanced the angiogenic sprouting of ECs, we chose to add the vasculogenic factors individually, as positive controls in the monoculture and co-culture systems. This was based on our hypothesis that cell–cell interactions between ADSCs and HUVECs are the main cue to enhance vascular structure formation.
Several recent studies reported that scaffolds from synthetic or natural polymers, such as gelatin [
19], hydroxyapatite, calcium phosphate [
20], and beta-tricalcium phosphate [
30], have the potential to organize ECs into vascular phenotypic structures because cultured ECs could express junction proteins. Biomaterials with a coating of ECM proteins, fibronectin, or laminin have also been used to increase cell attachment or proliferation [
34]. These biomaterial-based scaffolds provide a 3D cell culture environment and prevent cells from growing as a monolayer that leads to cell dysfunction. Among the various scaffolds, the nanofiber topography has many advantages over the conventional 2D culture system, because the nanofibrous environments mimic the architecture of the native ECM and promote cell adhesion, proliferation, and differentiation. In addition, the electrospinning process to generate nanofibrous scaffolds is quite fast compared to other methods, and the PCL/gelatin nanofiber scaffolds can create a cell-friendly and in-vivo-like environment without a protein-coating procedure. In this aspect, our co-culture system on PCL/gelatin nanofibrous scaffolds may be a promising and time-saving tool to regenerate blood vessels.
The morphological observations by the camera and SEM (
Figure 2) indicated the successful crosslinking of gelatin in the fibers. Genipin is a natural crosslinker of proteins, collagen, gelatin, and chitosan; it is less cytotoxic than the conventional crosslinker, glutaraldehyde, or other synthetic crosslinkers. Gelatin is a natural polymer that is water-soluble and biocompatible for cells, and with relatively low mechanical properties compared with synthetic polymers. On the contrary, PCL is a Food-and-Drug-Administration-approved synthetic polymer used for implantation, drug delivery system, and tissue engineering, which features relatively low cell compatibility compared to the natural polymer. Having noticed that a mixture of PCL and gelatin in fiber form is effective for blood vessel regeneration, Jiang Y.C. et al. described the PCL/gelatin electrospun microfiber as having proper mechanical traits similar to natural human coronary arteries. However, they only studied the interaction between MSCs and PCL/gelatin fibers, not blood-vessel-like structure formation [
35]. In this study, we confirmed the effect of blood-vessel-like structure formation using the PCL/gelatin nanofiber scaffolds and a co-culture system. Combining these properties, cells in monoculture or co-culture systems can attach and proliferate in the interconnected porous surface of the fabricated PCL/gelatin nanofiber scaffolds to a greater extent than on bare PCL fibers (data not shown). Cell proliferation and viability on the scaffolds were clearly observed (
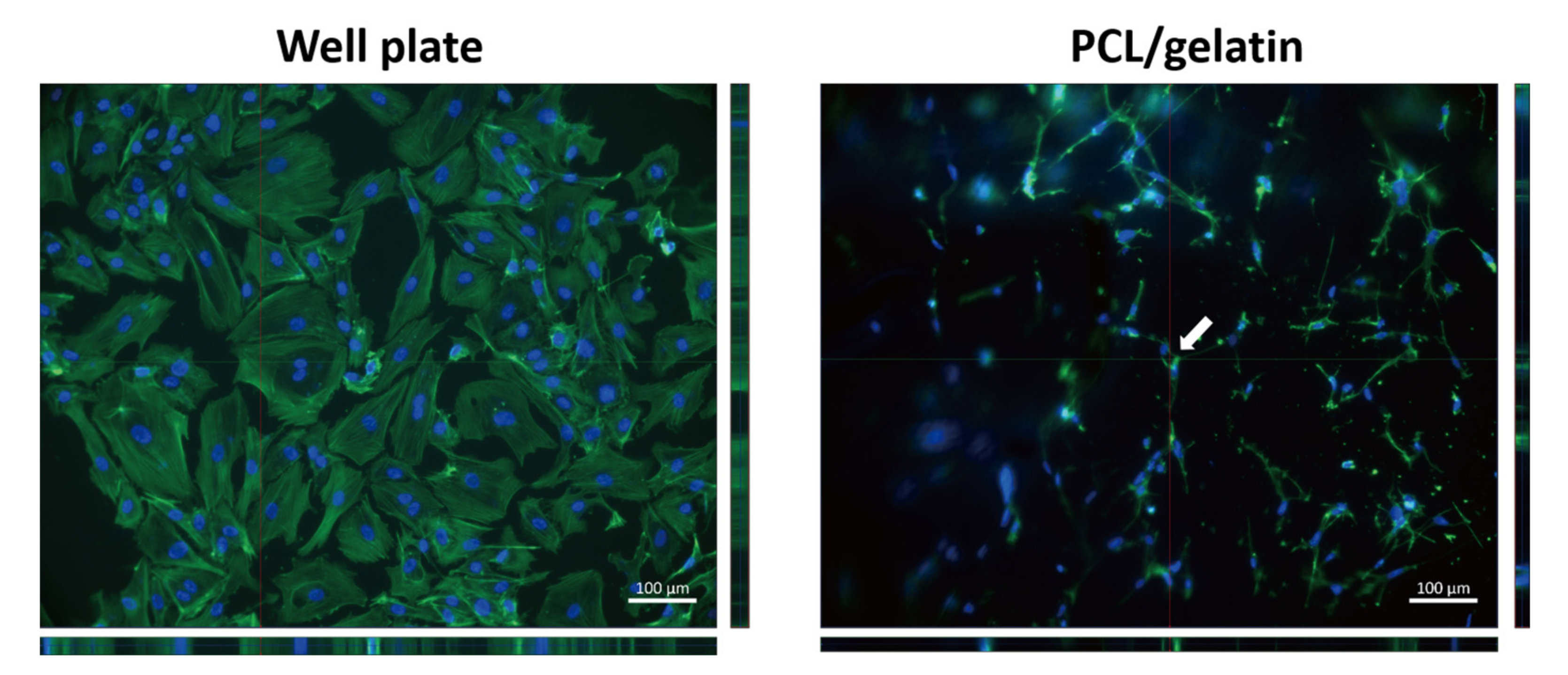
Figure 3). The F-actin staining results revealed the homogenous distribution of actin in the cytoplasm of ADSCs and HUVECs (
Figure 5B). This result indicates that the crosslinked PCL/gelatin scaffolds successfully supported cell adhesion, proliferation, and spreading without pre-coating of proteins regardless of the cell type used.
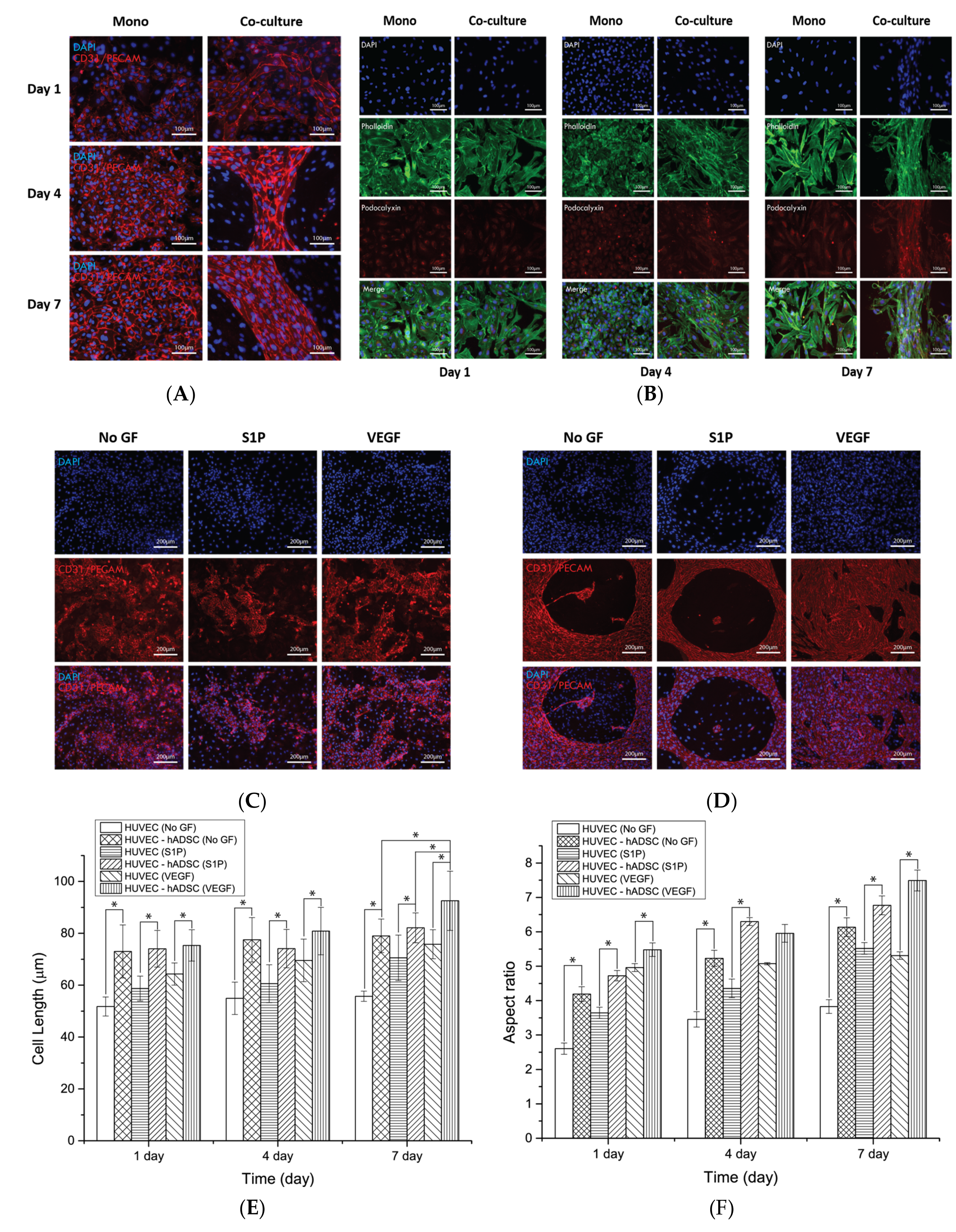
Immunofluorescence examination of HUVECs in monoculture and co-culture systems on a 2D surface allowed the assessment of the blood-vessel-like structure formation. Monoculture of HUVECs in 24-well plates resulted in the formation of cell monolayers with a widespread formation of tight junction proteins similar to the typical findings with mammalian cell cultures on tissue culture plates. Surprisingly, HUVECs seeded with ADSCs assembled with each other to form cell-assembled monolayer structures over four days of culture (
Figure 4). This may have reflected the direct cell–cell interactions between the two types of cells and the contribution of vasculogenic factors from the ADSCs, such as angiopoietin-1 and -2, VEGF, and interleukin-6, which induce the assembly of ECs similar to the de novo generation of blood vessels in vivo [
36]. Additionally, because of the pericyte-like characteristics of perivascular ADSCs, cell compartmentalization between HUVECs and ADSCs was evident on the 2D surface, similar to the blood vessel morphology that consists of assembled ECs and peripheral pericytes (
Figure 4A). However, HUVECs co-cultured with ADSCs in the 24-well plates did not show the capillary structure or cell sprouting. Furthermore, the addition of angiogenic factors to the mono- and co-cultures did not significantly change the behavior of HUVECs (
Figure 4C,D). Only a slight increase in the proliferation, expression of junction proteins, and body length of HUVECs in VEGF-loaded co-culture group was observed. These results imply that cellular interactions in the co-culture condition mainly affect the behavior of HUVECs, rather than the angiogenic factors present in the 2D environment. The immunofluorescence results for podocalyxin shown in
Figure 4B revealed the uniform distribution in HUVECs regardless of the culture condition. The expression was increased in a time-dependent manner in both the monoculture and co-culture groups. A previous study reported that podocalyxin-mediated control of vascular permeability and surface expression on the endothelial membrane precludes cell dysfunction and loss of blood flow [
37]. These results support the present findings that HUVECs grown in mono- or co-culture on the 2D surface are functional, although blood-vessel-like structures do not form.
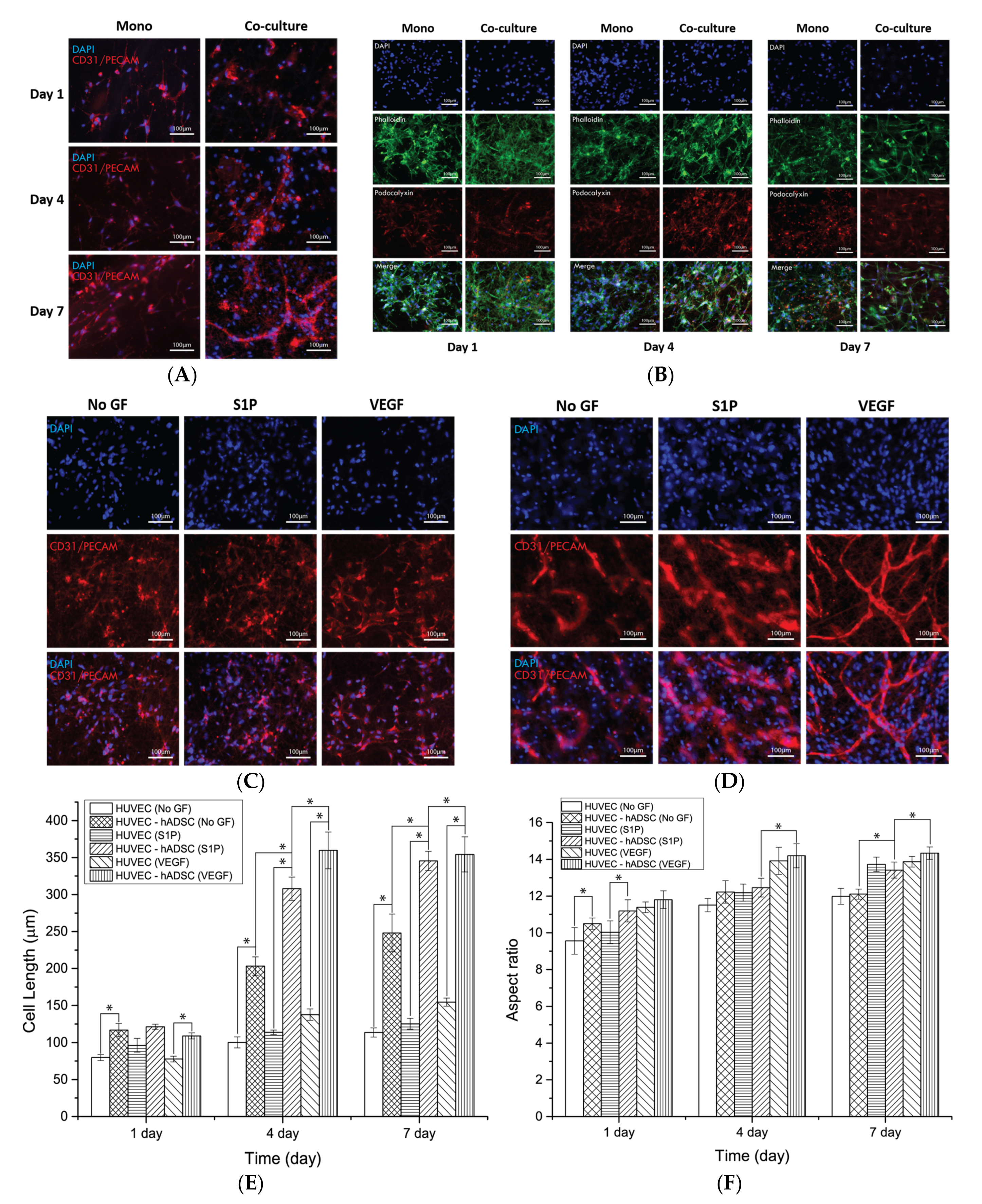
The immunofluorescence assay was also used to observe the expression of tight junction proteins and podocalyxin of HUVECs alone or with ADSCs on PCL/gelatin nanofiber scaffolds. The expression of the cell adhesion molecule CD31/PECAM-1 at the intercellular interface was also used to indicate the microvessel-like structure. In the monocultured HUVECs, the level of CD31/PECAM expression steadily increased and many tight junction proteins were observed on the scaffolds after 7 days of culture. Some elongated structure, but no apparent vasculature-like networks, were observed during the experimental periods. On the other hand, obvious microcapillary-like structure and blood-vessel-like networks were observed in the co-culture group. Co-cultured ECs with pluripotent stem cells or organotypic cells may facilitate the vascular network formation on 3D constructs since these types of cells can produce vasculogenic or angiogenic cytokines and factors [
20,
30,
38]. Additionally, the ECM produced by ADSCs may promote the blood-vessel-like formation of ECs when these cells are co-cultured directly on the scaffolds. Although co-cultured HUVECs on the 2D surface also achieved the cell-assembled structure, there was no microcapillary-like structure. The latter emerged only on the PCL/gelatin nanofibrous scaffolds. This is probably the result of the provision of a natural ECM-mimicking environment by the PCL/gelatin nanofibers. In addition, angiogenic factors enhanced the microvessel structure formation of HUVECs in the co-culture groups (
Figure 5D). In the co-culture system on our scaffolds, VEGF effectively triggered cell assembly, elongation, sprouting, and microvessel structure formation, whereas S1P was less effective than VEGF in the case of cell behavior. This is probably because VEGF is involved in all the vasculogenesis and angiogenesis processes of ECs. Recent studies compared the difference of cell behavior in the 2D and 3D environment. These studies identified that 3D cell culture models improved cell–cell interactions, cell–ECM interactions, protein expression, and gene expression than 2D cell culture models due to more in-vivo-like architecture, and our data also show that HUVECs in the nanofibrous environment more closely resemble the in vivo blood vessel networks than those in the 2D environment. This may support our results that growth factors work only in the nanofibrous environment because interactions between cells and growth factors more often occur in the 3D environment rather than the 2D environment. Furthermore, continuous expression of podocalyxin was observed in both the monoculture and co-culture groups and the elongation of HUVECs into blood-vessel-like structures was confirmed through the expression of protein at cell junction sites (
Figure 5B). These results imply that the fabricated PCL/gelatin nanofiber scaffolds are effective for the formation of mature blood vessel networks.
To assess functional blood vessels, it is important to observe lumen formation, which is one of the key steps in vascular morphogenesis or new blood vessel development. In this study, the distinct lumen formation of HUVECs was observed only on PCL/gelatin nanofibrous scaffolds; no luminal structure was observed in 2D culture system at day seven of culture. Without any signaling molecules, HUVECs produced a lumen structure on the nanofiber topography. Our results demonstrated that functionally-engineered blood vessels could be successfully produced by culturing the cells on fabricated PCL/gelatin nanofiber scaffolds. Further studies will need to assess the cocktail effect of angiogenic factors, the cell distribution of luminal structure in the co-culture system on PCL/gelatin nanofiber scaffolds, and the anastomosis of the engineered new blood vessel with natural blood vessels.