Functionalisation of Electrospun Cellulose Acetate Membranes with PEDOT and PPy for Electronic Controlled Drug Release
Abstract
1. Introduction
2. Materials and Methods
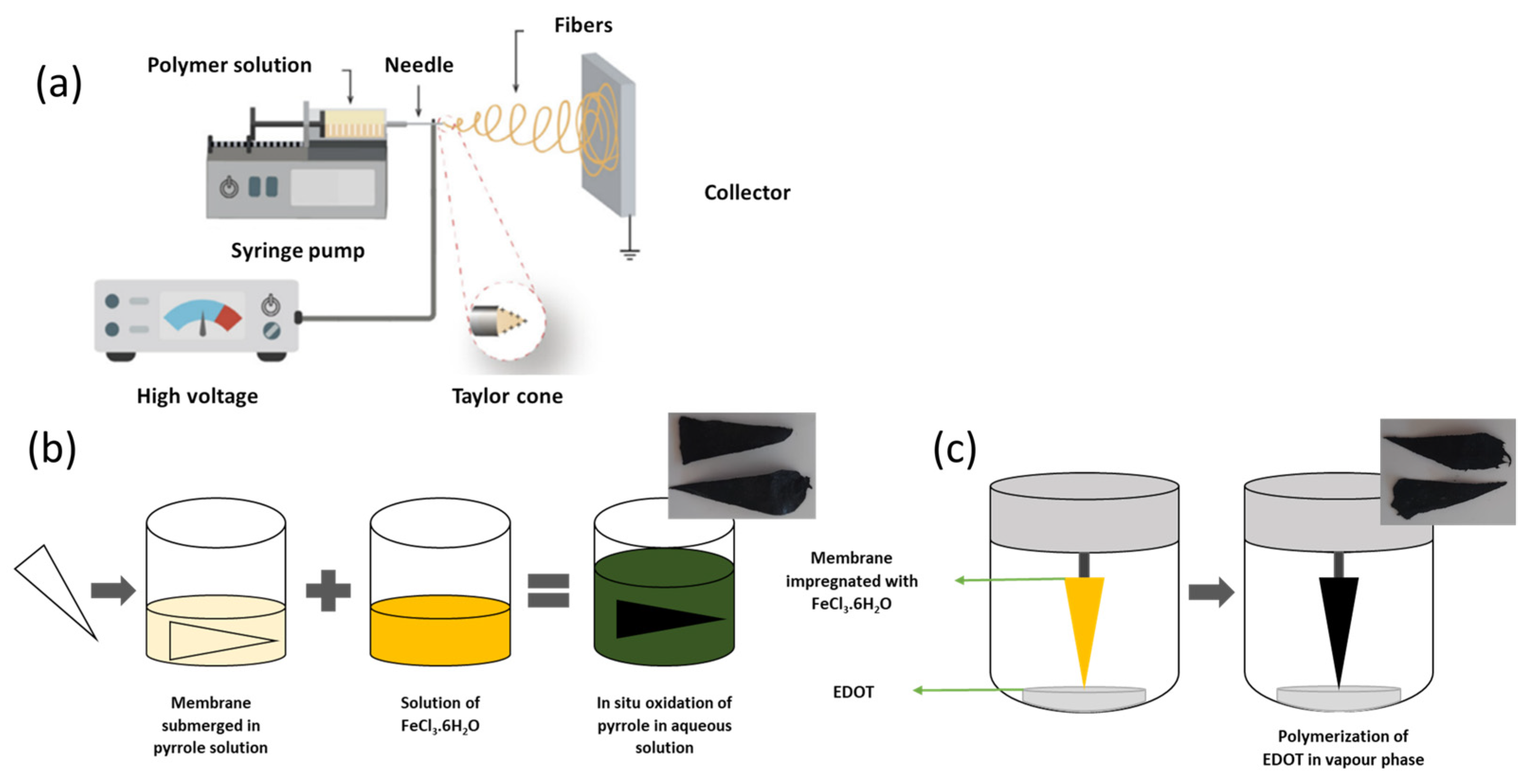
2.1. Production of Membranes
2.2. In Situ Oxidation of Pyrrole in Aqueous Solution
2.3. Vapour Phase Polymerisation of EDOT
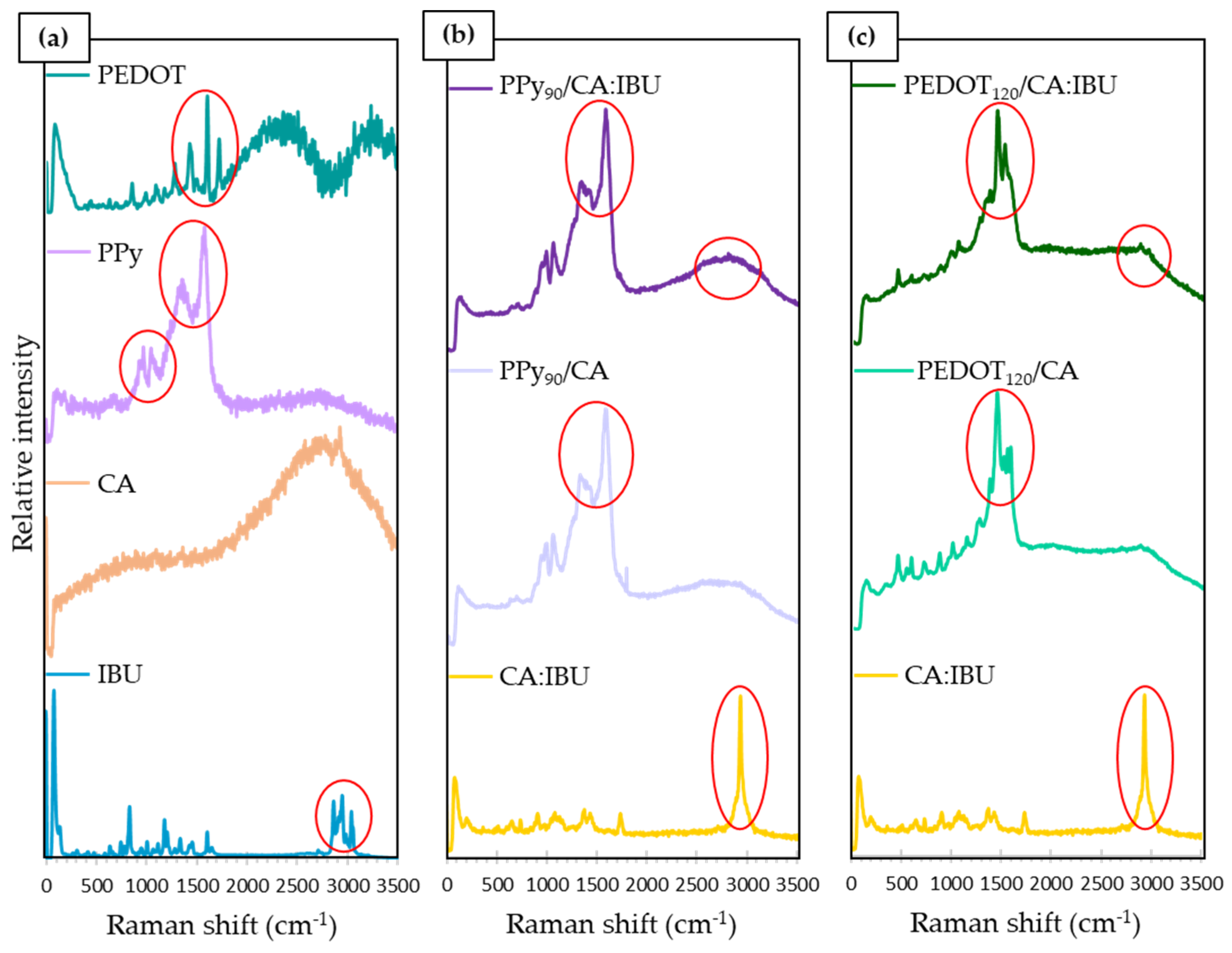
2.4. Characterisation
2.5. Conductivity
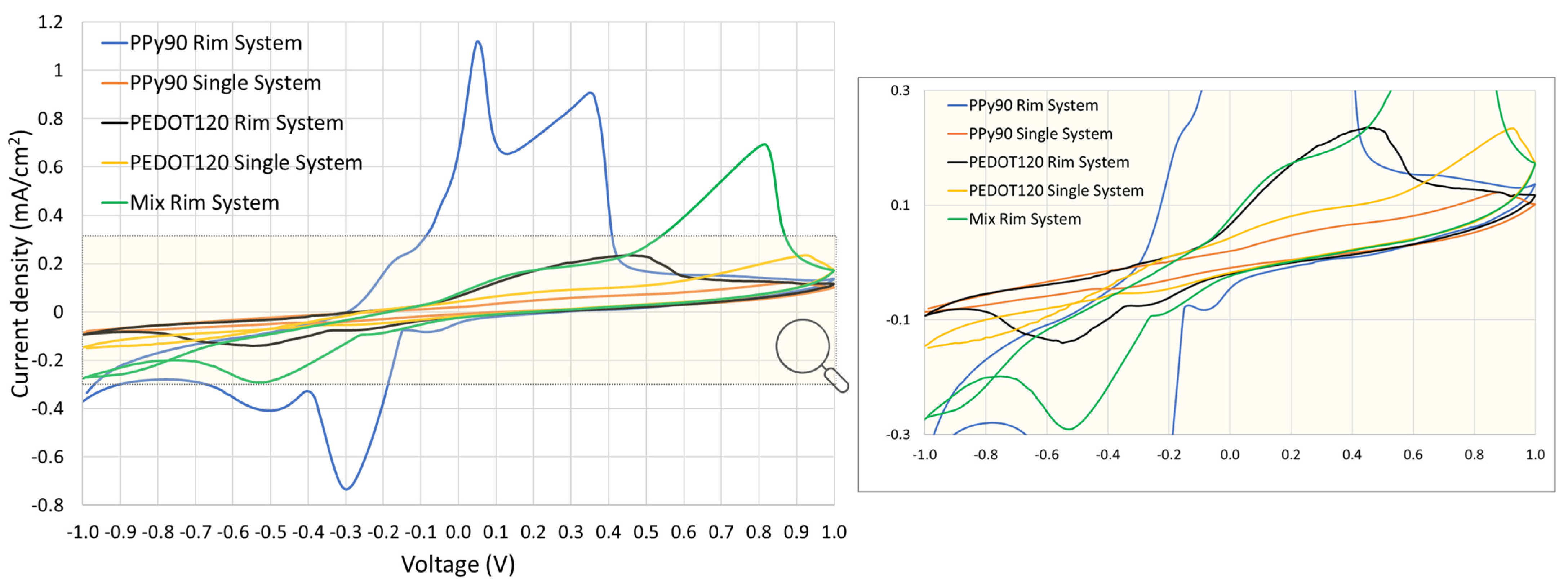
2.6. Cyclic Voltammetry
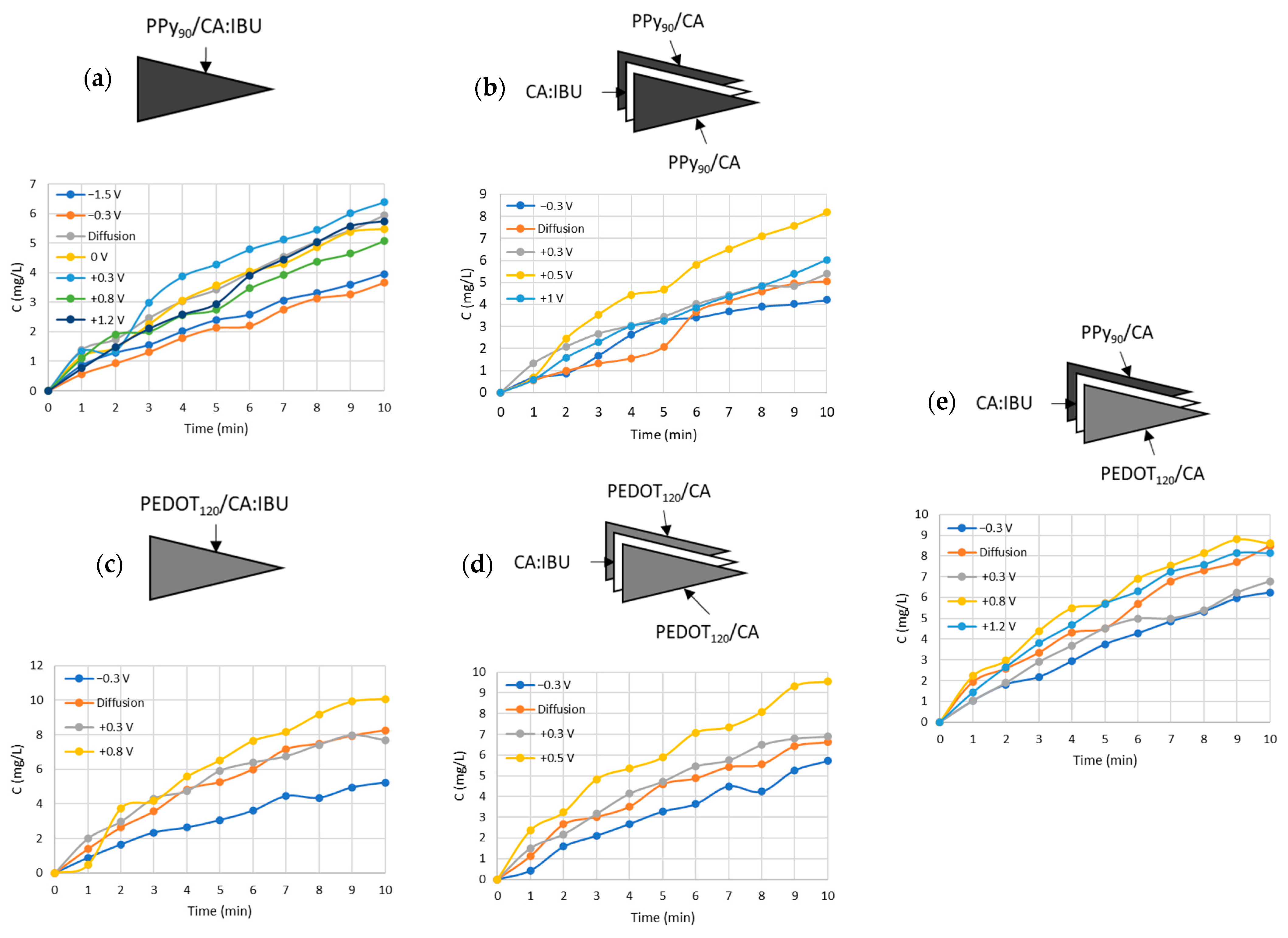
2.7. Drug Release
2.8. Prototype Drug Release
3. Results and Discussion
3.1. Membranes Characteristics
3.2. Morphology
3.3. Cyclic Voltammetry
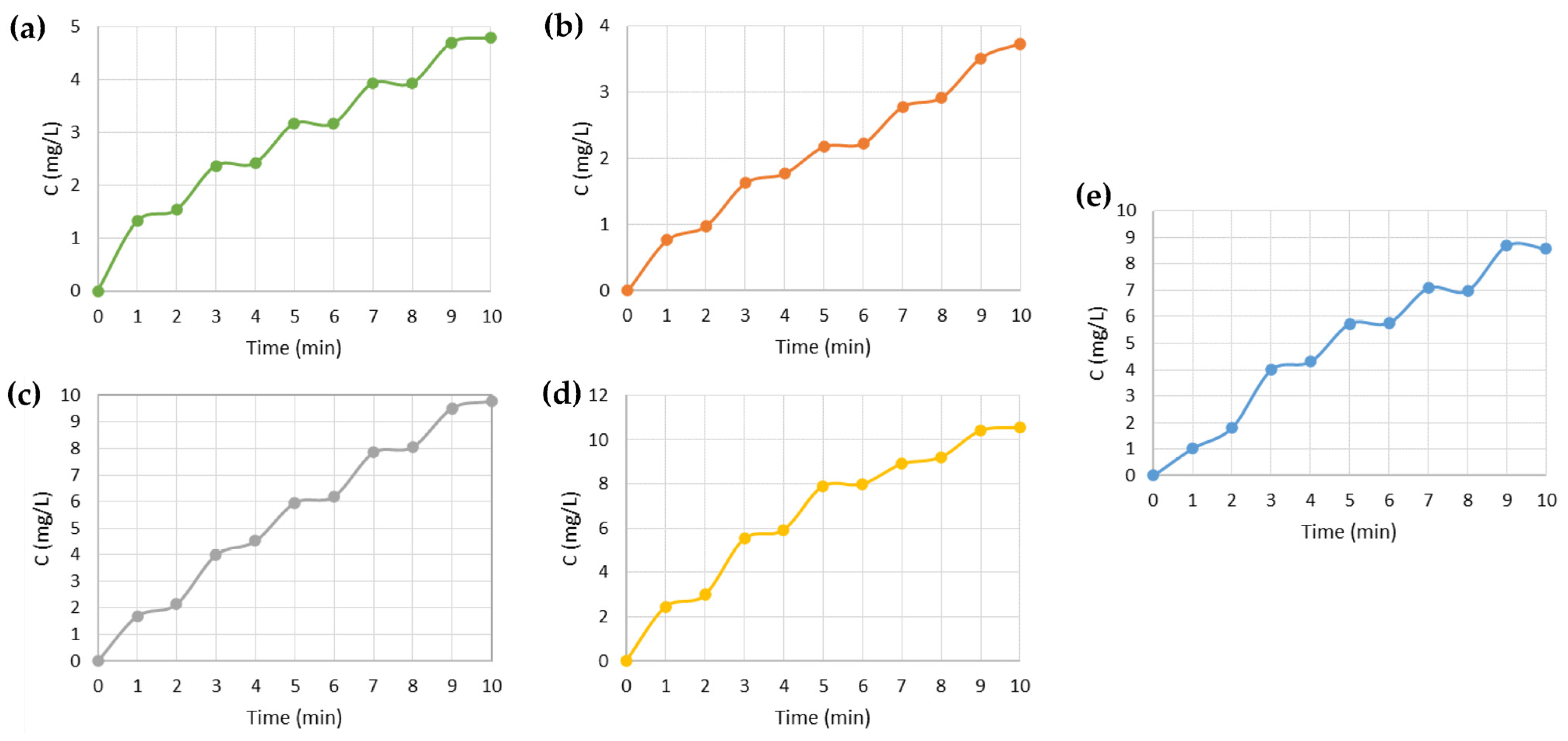
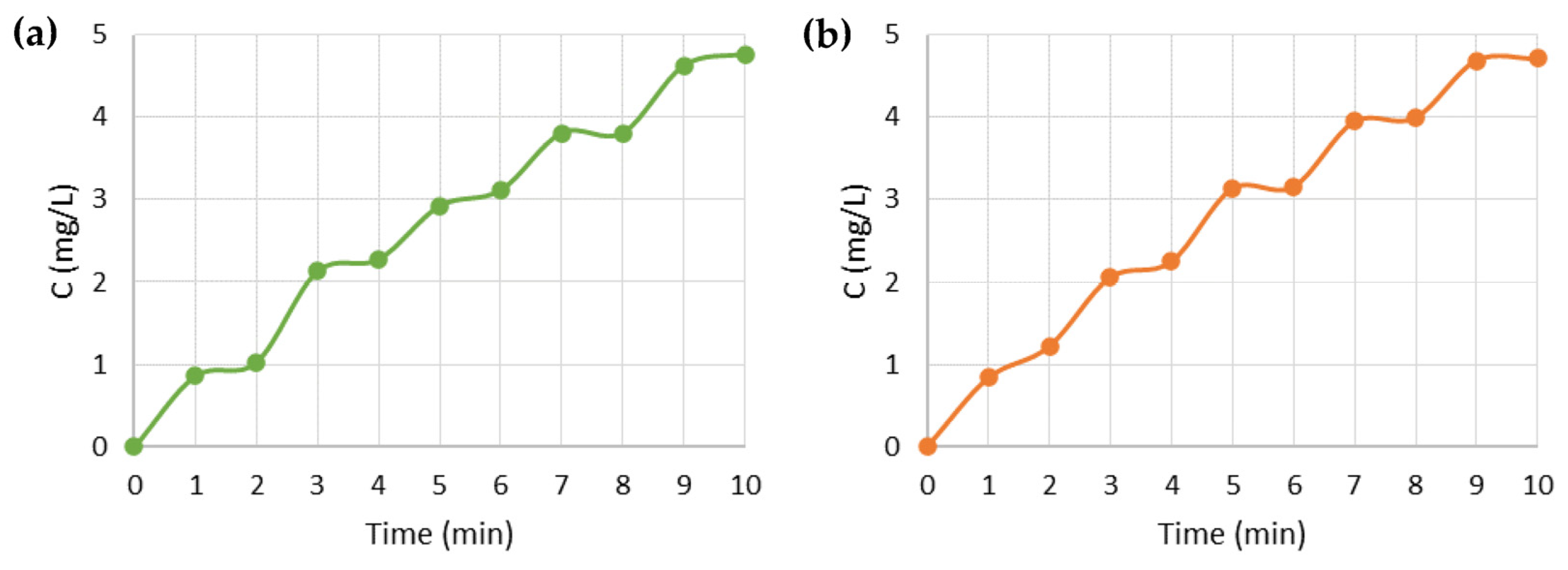
3.4. Drug Release Tests
3.5. Prototype Test
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Park, K. The Controlled Drug Delivery Systems: Past Forward and Future Back. J. Control. Release 2014, 190, 8. [Google Scholar] [CrossRef] [PubMed]
- Park, K. Facing the Truth about Nanotechnology in Drug Delivery. ACS Nano 2013, 7, 7442–7447. [Google Scholar] [CrossRef] [PubMed]
- Bölgen, N.; Vargel, I.; Korkusuz, P.; Menceloǧlu, Y.Z.; Pişkin, E. In Vivo Performance of Antibiotic Embedded Electrospun PCL Membranes for Prevention of Abdominal Adhesions. J. Biomed. Mater. Res. Part B Appl. Biomater. 2007, 81B, 530–543. [Google Scholar] [CrossRef] [PubMed]
- Tungprapa, S.; Jangchud, I.; Supaphol, P. Release Characteristics of Four Model Drugs from Drug-Loaded Electrospun Cellulose Acetate Fiber Mats. Polymer 2007, 48, 5030–5041. [Google Scholar] [CrossRef]
- Taepaiboon, P.; Rungsardthong, U.; Supaphol, P. Vitamin-Loaded Electrospun Cellulose Acetate Nanofiber Mats as Transdermal and Dermal Therapeutic Agents of Vitamin A Acid and Vitamin E. Eur. J. Pharm. Biopharm. 2007, 67, 387–397. [Google Scholar] [CrossRef]
- Chapman, C.A.R.; Cuttaz, E.A.; Goding, J.A.; Green, R.A. Actively Controlled Local Drug Delivery Using Conductive Polymer-Based Devices. Appl. Phys. Lett. 2020, 116, 010501. [Google Scholar] [CrossRef]
- Abaci, U.; Guney, H.Y.; Kadiroglu, U. Morphological and Electrochemical Properties of PPy, PAni Bilayer Films and Enhanced Stability of Their Electrochromic Devices (PPy/PAni–PEDOT, PAni/PPy–PEDOT). Electrochim. Acta 2013, 96, 214–224. [Google Scholar] [CrossRef]
- Laforgue, A.; Robitaille, L. Production of Conductive PEDOT Nanofibers by the Combination of Electrospinning and Vapor-Phase Polymerization. Macromolecules 2010, 43, 4194–4200. [Google Scholar] [CrossRef]
- Cho, B.; Park, K.S.; Baek, J.; Oh, H.S.; Koo Lee, Y.E.; Sung, M.M. Single-Crystal Poly(3,4-Ethylenedioxythiophene) Nanowires with Ultrahigh Conductivity. Nano Lett. 2014, 14, 3321–3327. [Google Scholar] [CrossRef]
- Müller, D.; Rambo, C.R.; Recouvreux, D.O.S.; Porto, L.M.; Barra, G.M.O. Chemical in Situ Polymerization of Polypyrrole on Bacterial Cellulose Nanofibers. Synth. Met. 2011, 161, 106–111. [Google Scholar] [CrossRef]
- Tang, L.; Han, J.; Jiang, Z.; Chen, S.; Wang, H. Flexible Conductive Polypyrrole Nanocomposite Membranes Based on Bacterial Cellulose with Amphiphobicity. Carbohydr. Polym. 2015, 117, 230–235. [Google Scholar] [CrossRef]
- Baptista, A.C.; Ropio, I.; Romba, B.; Nobre, J.P.; Henriques, C.; Silva, J.C.; Martins, J.I.; Borges, J.P.; Ferreira, I. Cellulose-Based Electrospun Fibers Functionalized with Polypyrrole and Polyaniline for Fully Organic Batteries. J. Mater. Chem. A 2017, 6, 256–265. [Google Scholar] [CrossRef]
- Carli, S.; Fioravanti, G.; Armirotti, A.; Ciarpella, F.; Prato, M.; Ottonello, G.; Salerno, M.; Scarpellini, A.; Perrone, D.; Marchesi, E.; et al. A New Drug Delivery System Based on Tauroursodeoxycholic Acid and PEDOT. Chemistry 2019, 25, 2322–2329. [Google Scholar] [CrossRef]
- Gao, S.; Tang, G.; Hua, D.; Xiong, R.; Han, J.; Jiang, S.; Zhang, Q.; Huang, C. Stimuli-Responsive Bio-Based Polymeric Systems and Their Applications. J. Mater. Chem. B 2019, 7, 709–729. [Google Scholar] [CrossRef]
- Guiseppi-Elie, A. Electroconductive Hydrogels: Synthesis, Characterization and Biomedical Applications. Biomaterials 2010, 31, 2701–2716. [Google Scholar] [CrossRef]
- Wadhwa, R.; Lagenaur, C.F.; Cui, X.T. Electrochemically Controlled Release of Dexamethasone from Conducting Polymer Polypyrrole Coated Electrode. J. Control. Release 2006, 110, 531–541. [Google Scholar] [CrossRef]
- Abidian, M.R.; Kim, D.H.; Martin, D.C. Conducting-Polymer Nanotubes for Controlled Drug Release. Adv. Mater. 2006, 18, 405–409. [Google Scholar] [CrossRef]
- Servant, A.; Bussy, C.; Al-Jamal, K.; Kostarelos, K. Design, Engineering and Structural Integrity of Electro-Responsive Carbon Nanotube- Based Hydrogels for Pulsatile Drug Release. J. Mater. Chem. B 2013, 1, 4593–4600. [Google Scholar] [CrossRef]
- Krukiewicz, K.; Zak, J.K. Conjugated Polymers as Robust Carriers for Controlled Delivery of Anti-Inflammatory Drugs. J. Mater. Sci. 2014, 49, 5738–5745. [Google Scholar] [CrossRef]
- Samanta, D.; Mehrotra, R.; Margulis, K.; Zare, R.N. On-Demand Electrically Controlled Drug Release from Resorbable Nanocomposite Films. R. Soc. Chem. 2017, 9, 16429. [Google Scholar] [CrossRef]
- Feiner, R.; Wertheim, L.; Gazit, D.; Kalish, O.; Mishal, G.; Shapira, A.; Dvir, T. A Stretchable and Flexible Cardiac Tissue–Electronics Hybrid Enabling Multiple Drug Release, Sensing, and Stimulation. Small 2019, 15, 1805526. [Google Scholar] [CrossRef] [PubMed]
- Baptista, A.C.; Brito, M.; Marques, A.; Ferreira, I. Electronic Control of Drug Release from Gauze or Cellulose Acetate Fibres for Dermal Applications. J. Mater. Chem. B 2021, 9, 3515–3522. [Google Scholar] [CrossRef] [PubMed]
- Jeong, W.Y.; Kwon, M.; Choi, H.E.; Kim, K.S. Recent Advances in Transdermal Drug Delivery Systems: A Review. Biomater. Res. 2021, 25, 339–351. [Google Scholar] [CrossRef] [PubMed]
- Amjadi, M.; Sheykhansari, S.; Nelson, B.J.; Sitti, M.; Amjadi, M.; Sheykhansari, S.; Sitti, M.; Nelson, B.J. Recent Advances in Wearable Transdermal Delivery Systems. Adv. Mater. 2018, 30, 1704530. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.Y.; Chen, Y.; Huang, Y.Y.; Cheng, C.M. Transdermal Drug Delivery Systems for Fighting Common Viral Infectious Diseases. Drug Deliv. Transl. Res. 2021, 11, 1498–1508. [Google Scholar] [CrossRef]
- Zhang, Y.; Yu, J.; Bomba, H.N.; Zhu, Y.; Gu, Z. Mechanical Force-Triggered Drug Delivery. Chem. Rev. 2016, 116, 12536–12563. [Google Scholar] [CrossRef]
- Tamayol, A.; Hassani Najafabadi, A.; Mostafalu, P.; Yetisen, A.K.; Commotto, M.; Aldhahri, M.; Abdel-Wahab, M.S.; Najafabadi, Z.I.; Latifi, S.; Akbari, M.; et al. Biodegradable Elastic Nanofibrous Platforms with Integrated Flexible Heaters for On-Demand Drug Delivery. Sci. Rep. 2017, 7, 9220. [Google Scholar] [CrossRef]
- Ogawa, Y.; Kato, K.; Miyake, T.; Nagamine, K.; Ofuji, T.; Yoshino, S.; Nishizawa, M.; Ogawa, Y.; Kato, K.; Miyake, T.; et al. Organic Transdermal Iontophoresis Patch with Built-in Biofuel Cell. Adv. Healthc. Mater. 2015, 4, 506–510. [Google Scholar] [CrossRef]
- Bagherifard, S.; Tamayol, A.; Mostafalu, P.; Akbari, M.; Comotto, M.; Annabi, N.; Ghaderi, M.; Sonkusale, S.; Dokmeci, M.R.; Khademhosseini, A. Dermal Patch with Integrated Flexible Heater for on Demand Drug Delivery. Adv. Healthc. Mater. 2016, 5, 175–184. [Google Scholar] [CrossRef]
- Li, M.; Liang, Y.; He, J.; Zhang, H.; Guo, B. Two-Pronged Strategy of Biomechanically Active and Biochemically Multifunctional Hydrogel Wound Dressing to Accelerate Wound Closure and Wound Healing. Chem. Mater. 2020, 32, 9937–9953. [Google Scholar] [CrossRef]
- Zhao, X.; Guo, B.; Wu, H.; Liang, Y.; Ma, P.X. Injectable Antibacterial Conductive Nanocomposite Cryogels with Rapid Shape Recovery for Noncompressible Hemorrhage and Wound Healing. Nat. Commun. 2018, 9, 2784. [Google Scholar] [CrossRef]
- Qu, J.; Liang, Y.; Shi, M.; Guo, B.; Gao, Y.; Yin, Z. Biocompatible Conductive Hydrogels Based on Dextran and Aniline Trimer as Electro-Responsive Drug Delivery System for Localized Drug Release. Int. J. Biol. Macromol. 2019, 140, 255–264. [Google Scholar] [CrossRef]
- Ouyang, Q.; Feng, X.; Kuang, S.; Panwar, N.; Song, P.; Yang, C.; Yang, G.; Hemu, X.; Zhang, G.; Yoon, H.S.; et al. Self-Powered, on-Demand Transdermal Drug Delivery System Driven by Triboelectric Nanogenerator. Nano Energy 2019, 62, 610–619. [Google Scholar] [CrossRef]
- Vadlapatla, R.; Wong, E.Y.; Gayakwad, S.G. Electronic Drug Delivery Systems: An Overview. J. Drug Deliv. Sci. Technol. 2017, 41, 359–366. [Google Scholar] [CrossRef]
- Fry, A. Electronically Enabled Drug-Delivery Devices: Are They Part of the Future? Ther. Deliv. 2012, 3, 805–807. [Google Scholar] [CrossRef]
- Manoukian, M.A.C.; Migdal, C.W.; Tembhekar, A.R.; Harris, J.A.; DeMesa, C. Topical Administration of Ibuprofen for Injured Athletes: Considerations, Formulations, and Comparison to Oral Delivery. Sport. Med.-Open 2017, 3, 36. [Google Scholar] [CrossRef]
- Stott, P.W.; Williams, A.C.; Barry, B.W. Transdermal Delivery from Eutectic Systems: Enhanced Permeation of a Model Drug, Ibuprofen. J. Control. Release 1998, 50, 297–308. [Google Scholar] [CrossRef]
- Brooke, R.; Cottis, P.; Talemi, P.; Fabretto, M.; Murphy, P.; Evans, D. Recent Advances in the Synthesis of Conducting Polymers from the Vapour Phase. Prog. Mater. Sci. 2017, 86, 127–146. [Google Scholar] [CrossRef]
- Ropio, I.; Baptista, A.C.; Nobre, J.P.; Correia, J.; Belo, F.; Taborda, S.; Morais Faustino, B.M.; Borges, J.P.; Kovalenko, A.; Ferreira, I. Cellulose Paper Functionalised with Polypyrrole and Poly(3,4-Ethylenedioxythiophene) for Paper Battery Electrodes. Org. Electron. 2018, 62, 530–535. [Google Scholar] [CrossRef]
- Nagar, B.; Silva, W.O.; Girault, H.H. Voltammetry in Two-Electrode Mode for Rapid Electrochemical Screening Using a Fully Printed and Flexible Multiplexer Sensor. ChemElectroChem 2021, 8, 3700–3706. [Google Scholar] [CrossRef]
- Kokubo, T.; Takadama, H. How Useful Is SBF in Predicting in Vivo Bone Bioactivity? Biomaterials 2006, 27, 2907–2915. [Google Scholar] [CrossRef] [PubMed]
- Freire, J. Anti-Bacterial Surface Protection for Prostheses; Nova School of Science & Technology: Lisboa, Portugal, 2022. [Google Scholar]
- Fan, X.; Yang, Z.; He, N. Hierarchical Nanostructured Polypyrrole/Graphene Composites as Supercapacitor Electrode. RSC Adv. 2015, 5, 15096–15102. [Google Scholar] [CrossRef]
- Chang, S.H.; Chiang, C.H.; Kao, F.S.; Tien, C.L.; Wu, C.G. Unraveling the Enhanced Electrical Conductivity of PEDOT:PSS Thin Films for ITO-Free Organic Photovoltaics. Undefined 2014, 6. [Google Scholar] [CrossRef]
- Sütő, B.; Berkó, S.; Kozma, G.; Kukovecz, Á.; Budai-Szucs, M.; Erös, G.; Kemény, L.; Sztojkov-Ivanov, A.; Gáspár, R.; Csányi, E. Development of Ibuprofen-Loaded Nanostructured Lipid Carrier-Based Gels: Characterization and Investigation of In Vitro and In Vivo Penetration through the Skin. Int. J. Nanomed. 2016, 11, 1201–1212. [Google Scholar] [CrossRef]
- Vueba, M.L.; Pina, M.E.; Batista, L.A.E.; Carvalho, D.E. Conformational Stability of Ibuprofen: Assessed by DFT Calculations and Optical Vibrational Spectroscopy. J. Pharm. Sci. 2008, 97, 845–859. [Google Scholar] [CrossRef]
- Kilmartin, P.A.; Wright, G.A. Photoeffects to Characterise Polypyrrole Electrodes and Bilayers with Polyaniline. Electrochim. Acta 2001, 46, 2787–2794. [Google Scholar] [CrossRef]
- Qu, J.; Zhao, X.; Ma, P.X.; Guo, B. Injectable Antibacterial Conductive Hydrogels with Dual Response to an Electric Field and PH for Localized “Smart” Drug Release. Acta Biomater. 2018, 72, 55–69. [Google Scholar] [CrossRef]


| Systems | OFF (V) | ON (V) |
|---|---|---|
| PPy90 Rim System | −0.3 | +0.5 |
| PPy90 Single System | −0.3 | +0.3 |
| PEDOT120 Rim System | −0.3 | +0.5 |
| PEDOT120 Single System | −0.3 | +0.8 |
| Mix Rim System | −0.3 | +0.8 |
| Systems | Voltage (V) | IBU (µg/L) | IBU (%) |
|---|---|---|---|
| PPy90 Rim System | +0.5 | 12 | 0.38 |
| +1.0 | <LOD | -------- | |
| PPy90 Single System | −0.3 | <LOD | -------- |
| Diffusion | 2.3 | 0.074 | |
| 0 | 24 | 0.77 | |
| +0.3 | 33 | 1.0 | |
| +0.8 | 19 | 0.61 | |
| +1.2 | 14 | 0.45 | |
| PEDOT120 Single System | +0.3 | 12 | 0.38 |
| +0.8 | 24 | 0.77 | |
| Mix Rim System | +0.8 | 25 | 0.80 |
| +1.2 | 16 | 0.51 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lago, B.; Brito, M.; Almeida, C.M.M.; Ferreira, I.; Baptista, A.C. Functionalisation of Electrospun Cellulose Acetate Membranes with PEDOT and PPy for Electronic Controlled Drug Release. Nanomaterials 2023, 13, 1493. https://doi.org/10.3390/nano13091493
Lago B, Brito M, Almeida CMM, Ferreira I, Baptista AC. Functionalisation of Electrospun Cellulose Acetate Membranes with PEDOT and PPy for Electronic Controlled Drug Release. Nanomaterials. 2023; 13(9):1493. https://doi.org/10.3390/nano13091493
Chicago/Turabian StyleLago, Beatriz, Miguel Brito, Cristina M. M. Almeida, Isabel Ferreira, and Ana Catarina Baptista. 2023. "Functionalisation of Electrospun Cellulose Acetate Membranes with PEDOT and PPy for Electronic Controlled Drug Release" Nanomaterials 13, no. 9: 1493. https://doi.org/10.3390/nano13091493
APA StyleLago, B., Brito, M., Almeida, C. M. M., Ferreira, I., & Baptista, A. C. (2023). Functionalisation of Electrospun Cellulose Acetate Membranes with PEDOT and PPy for Electronic Controlled Drug Release. Nanomaterials, 13(9), 1493. https://doi.org/10.3390/nano13091493










