Clinicopathological Features and Prognostic Factors of Primary Acral Melanomas in Caucasians
Abstract
1. Introduction
2. Materials and Methods
2.1. Clinical Data: Patient Selection and Data Acquisition
2.2. Statistical Methods
3. Results
3.1. Clinicopathological Features
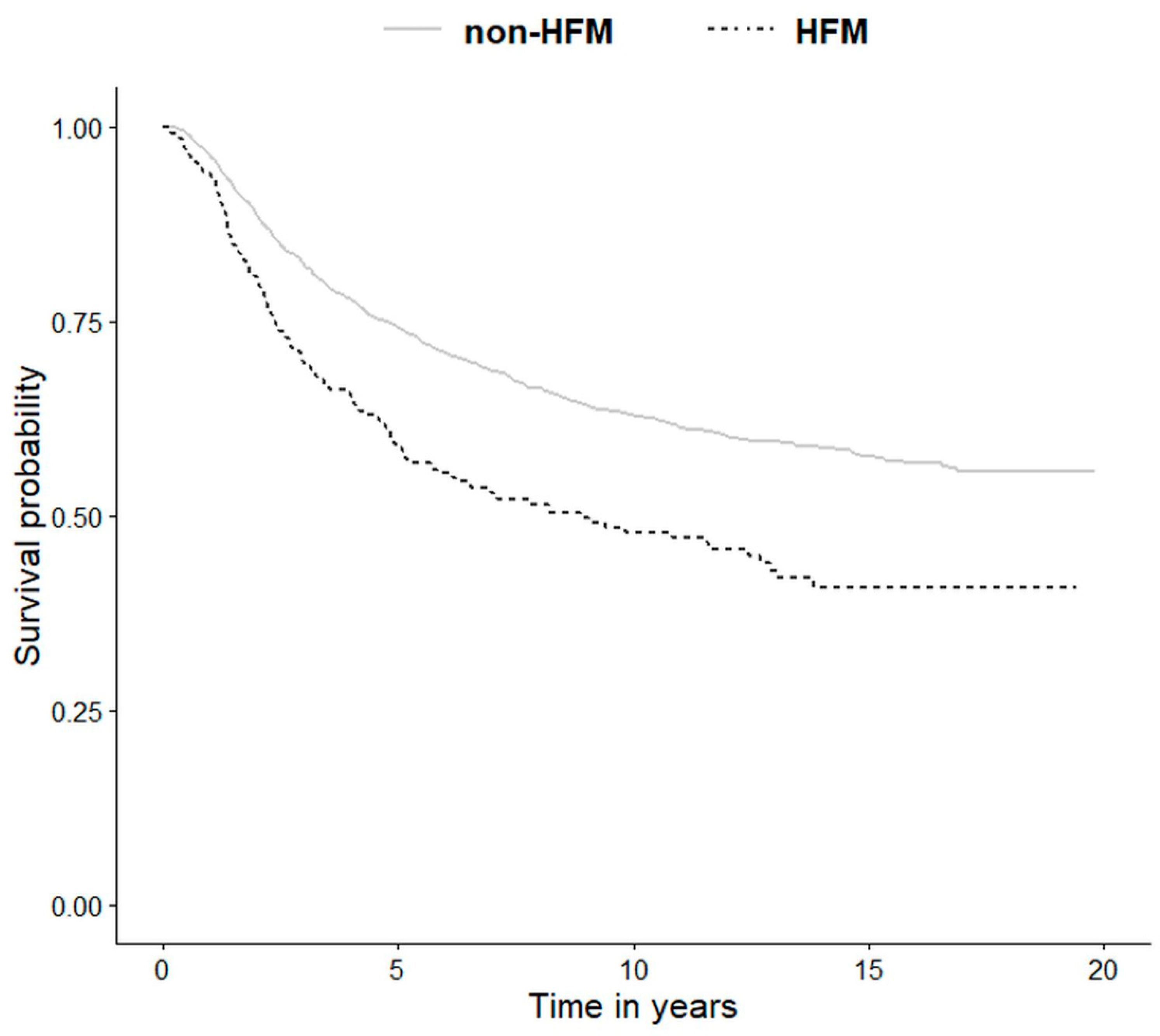
3.2. HFM vs. Non-HFM Patients
3.3. SUM vs. Non-SUM Patients
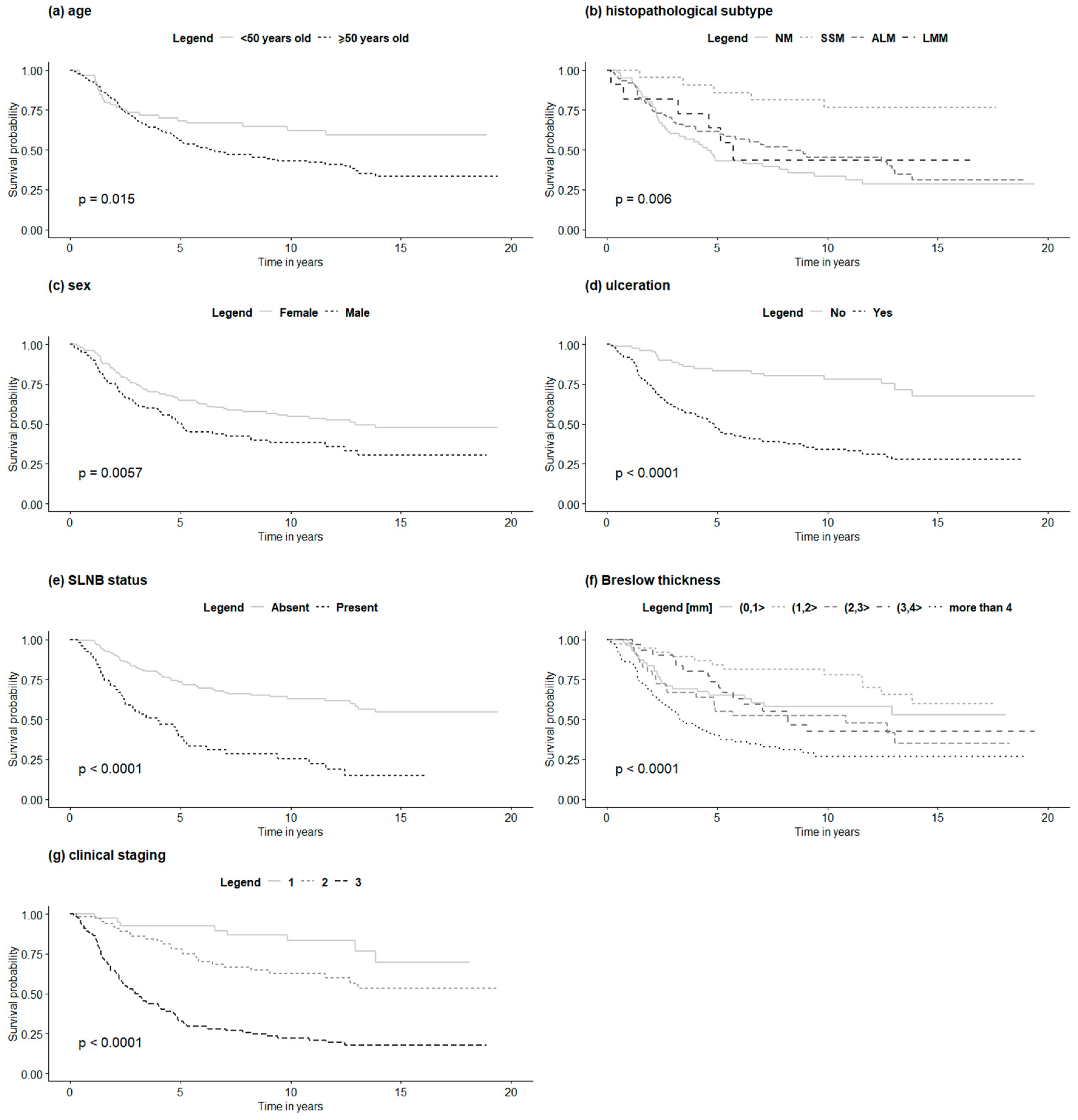
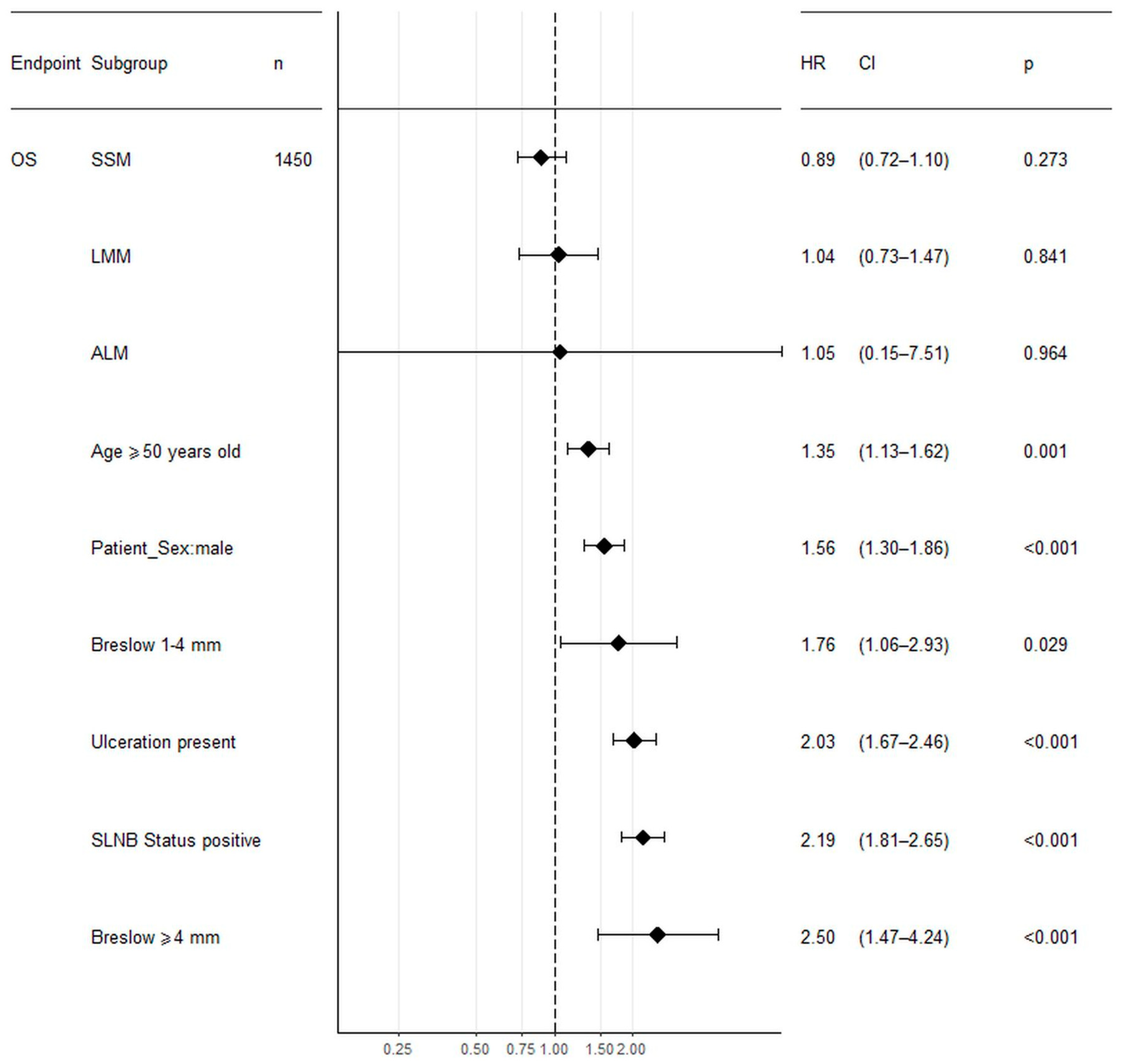
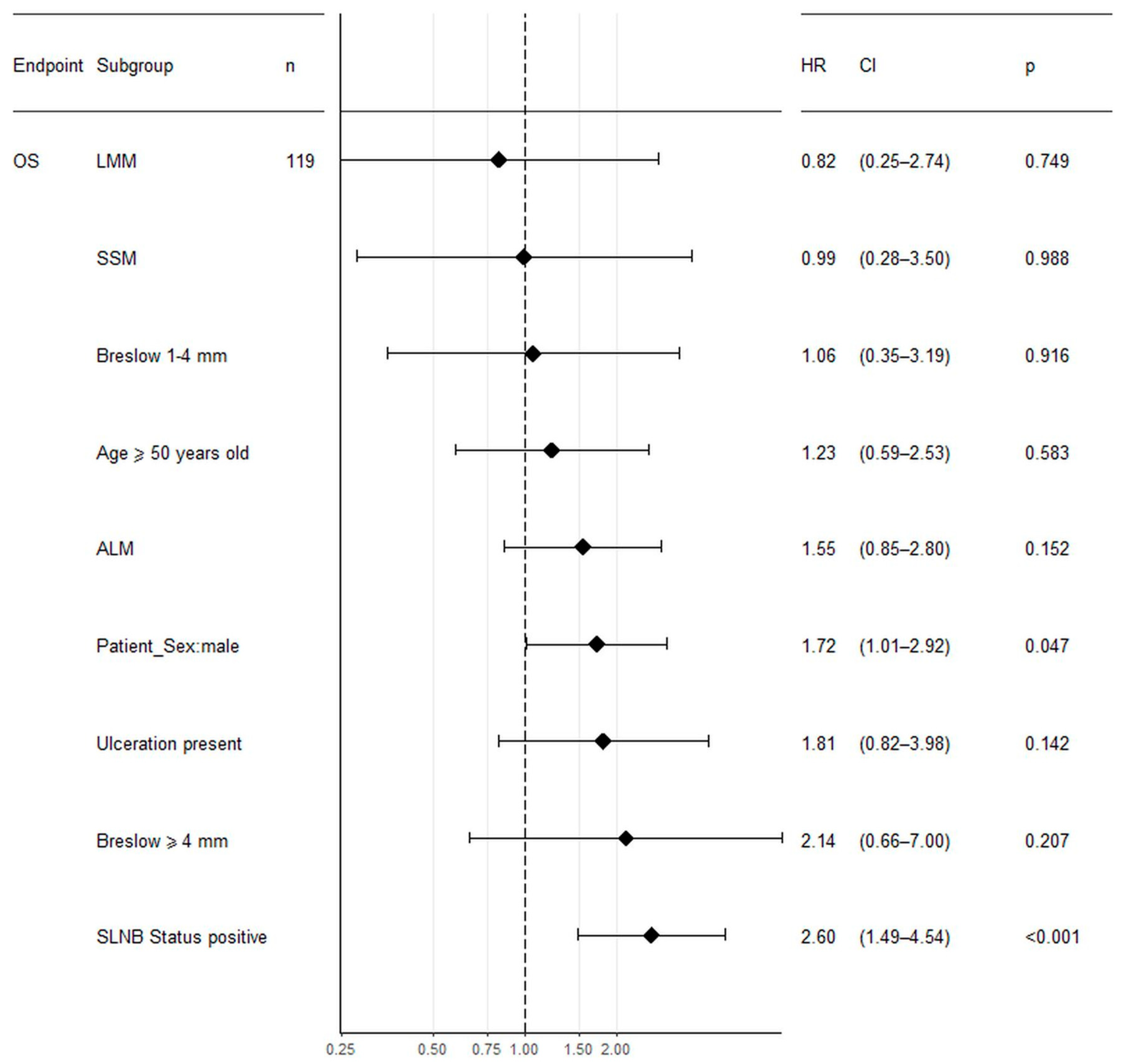
3.4. Survival and Survival Factors in HFM Cohort
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| ALM | acral lentiginous melanoma |
| HFM | hand and foot melanoma |
| LMM | lentigo malignant melanoma |
| NM | nodular melanoma |
| MM | cutaneous melanomas |
| MSNRI | Maria Sklodowska-Curie National Research Institute of Oncology |
| OS | overall survival |
| SLN | sentinel lymph node |
| SSM | superficial spreading melanoma |
| SUM | subungual melanoma |
| UVR | ultraviolet radiation |
References
- Ward, W.H.; Lambreton, F.; Goel, N.; Yu, J.Q.; Farma, J.M. Clinical Presentation and Staging of Melanoma. In Cutaneous Melanoma: Etiology and Therapy; Codon Publications: Brisbane, Australian, 2020. Available online: https://www.ncbi.nlm.nih.gov/pubmed/29461773 (accessed on 23 January 2020).
- Durbec, F.; Martin, L.; Derancourt, C.; Grange, F. Melanoma of the hand and foot: Epidemiological, prognostic and genetic features. A systematic review. Br. J. Dermatol. 2012, 166, 727–739. [Google Scholar] [CrossRef] [PubMed]
- Kuk, D.; Shoushtari, A.N.; Barker, C.A.; Panageas, K.S.; Munhoz, R.R.; Momtaz, P.; Ariyan, C.E.; Brady, M.S.; Coit, D.G.; Bogatch, K.; et al. Prognosis of Mucosal, Uveal, Acral, Nonacral Cutaneous, and Unknown Primary Melanoma from the Time of First Metastasis. Oncologist 2016, 21, 848–854. [Google Scholar] [CrossRef] [PubMed]
- Sheen, Y.S.; Liao, Y.H.; Lin, M.H.; Chen, J.S.; Liau, J.Y.; Tseng, Y.J.; Lee, C.H.; Chang, Y.L.; Chu, C.Y. A clinicopathological analysis of 153 acral melanomas and the relevance of mechanical stress. Sci. Rep. 2017, 7, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Bello, D.M.; Chou, J.F.; Panageas, K.S.; Brady, M.S.; Coit, D.G.; Carvajal, R.D.; Ariyan, C.E. Prognosis of Acral Melanoma: A Series of 281 Patients. Ann. Surg. Oncol. 2013, 20, 3618–3625. Available online: https://link.springer.com/article/10.1245/s10434-013-3089-0 (accessed on 23 January 2020). [CrossRef]
- Whiteman, D.C.; Pavan, W.J.; Bastian, B.C. The melanomas: A synthesis of epidemiological, clinical, histopathological, genetic, and biological aspects, supporting distinct subtypes, causal pathways, and cells of origin. Pigment Cell Melanoma Res. 2011, 24, 879–897. [Google Scholar] [CrossRef]
- Fortin, P.T.; Freiberg, A.A.; Rees, R.; Sondak, V.K.; Johnson, T.M. Malignant melanoma of the foot and ankle. J. Bone Jt. Surg. 1995, 77, 1396–1403. [Google Scholar] [CrossRef]
- Heaton, K.M.; El-Naggar, A.; Ensign, L.G.; Ross, M.I.; Balch, C.M. Surgical Management and Prognostic Factors in Patients with Subungual Melanoma. Ann. Surg. 1994, 219, 197–204. [Google Scholar] [CrossRef]
- Albreski, D.; Sloan, S.B. Melanoma of the feet: Misdiagnosed and misunderstood. Clin. Dermatol. 2009, 27, 556–563. [Google Scholar] [CrossRef]
- Liu, X.K.; Li, J. Acral lentiginous melanoma. Lancet 2018, 391, e21. [Google Scholar] [CrossRef]
- Banfield, C.C.; Redburn, J.C.; Dawber, R.P. The incidence and prognosis of nail apparatus melanoma. A retrospective study of 105 patients in four English regions. Br. J. Dermatol. 1998, 139, 276–279. [Google Scholar] [CrossRef]
- Mole, R.J.; MacKenzie, D.N. Cancer, Melanoma, Subungual. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2019. Available online: http://www.ncbi.nlm.nih.gov/books/NBK482480/ (accessed on 3 September 2019).
- Cohen, T.; Busam, K.J.; Patel, A.; Brady, M.S. Subungual melanoma: Management considerations. Am. J. Surg. 2008, 195, 244–248. [Google Scholar] [CrossRef] [PubMed]
- Blessing, K.; Kernohan, N.M.; Park, K.G.M. Subungual malignant melanoma: Clinicopathological features of 100 cases. Histopathology 1991, 19, 425–430. [Google Scholar] [CrossRef] [PubMed]
- Dika, E.; Patrizi, A.; Fanti, P.A.; Chessa, M.A.; Reggiani, C.; Barisani, A.; Piraccini, B.M. The Prognosis of Nail Apparatus Melanoma: 20 Years of Experience from a Single Institute. Dermatology 2016, 232, 177–184. [Google Scholar] [CrossRef]
- Spencer, J.M. Nail-apparatus melanoma. Lancet 1999, 353, 84–85. [Google Scholar] [CrossRef]
- Kottschade, L.A.; Grotz, T.E.; Dronca, R.S.; Salomao, D.R.; Pulido, J.S.; Wasif, N.; Jakub, J.W.; Bagaria, S.P.; Kumar, R.; Kaur, J.S. Rare Presentations of Primary Melanoma and Special Populations. Am. J. Clin. Oncol. 2014, 37, 635–641. [Google Scholar] [CrossRef]
- O’Leary, J.A.; Berend, K.R.; Johnson, J.L.; Levin, L.S.; Seigler, H.F. Subungual Melanoma. Clin. Orthop. Relat. Res. 2000, 378, 206–212. [Google Scholar] [CrossRef]
- Littleton, T.W.; Murray, P.M.; Baratz, M.E. Subungual Melanoma. Orthop. Clin. N. Am. 2019, 50, 357–366. [Google Scholar] [CrossRef]
- Reilly, D.J.; Aksakal, G.; Gilmour, R.F.; Gyorki, D.E.; Chauhan, A.; Webb, A.; Henderson, M.A. Subungual melanoma: Management in the modern era. J. Plast. Reconstr. Aesthetic Surg. 2017, 70, 1746–1752. [Google Scholar] [CrossRef]
- Bradford, P.T.; Goldstein, A.M.; McMaster, M.L.; Tucker, M.A. Acral Lentiginous Melanoma. Arch. Dermatol. 2009, 145, 427–434. [Google Scholar] [CrossRef] [PubMed]
- Goydos, J.S.; Shoen, S.L. Acral Lentiginous Melanoma. Melanoma 2015, 167, 321–329. Available online: https://link.springer.com/chapter/10.1007%2F978-3-319-22539-5_14 (accessed on 23 January 2020).
- Desai, A.; Ugorji, R.; Khachemoune, A. Acral melanoma foot lesions. Part 1: Epidemiology, aetiology, and molecular pathology. Clin. Exp. Dermatol. 2017, 42, 845–848. Available online: https://www.ncbi.nlm.nih.gov/pubmed/28940724 (accessed on 23 January 2020). [CrossRef] [PubMed]
- Piliang, M.P. Acral Lentiginous Melanoma. Clin. Lab. Med. 2011, 31, 281–288. [Google Scholar] [CrossRef] [PubMed]
- R Development Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2009; ISBN 3-900051-07-0. Available online: http://www.r-project.org (accessed on 7 March 2020).
- Torres-Cabala, C.A.; Wang, W.-L.; Trent, J.; Yang, D.; Chen, S.; Galbincea, J.; Kim, K.B.; Woodman, S.; Davies, M.; Plaza, J.A.; et al. Correlation between KIT expression and KIT mutation in melanoma: A study of 173 cases with emphasis on the acral-lentiginous/mucosal type. Mod. Pathol. 2009, 22, 1446–1456. Available online: https://miami.pure.elsevier.com/en/publications/correlation-between-kit-expression-and-kit-mutation-in-melanomaa (accessed on 23 January 2020). [CrossRef]
- Zebary, A.; Omholt, K.; Vassilaki, I.; Höiom, V.; Lindén, D.; Viberg, L.; Kanter-Lewensohn, L.; Johansson, C.H.; Hansson, J. KIT, NRAS, BRAF and PTEN mutations in a sample of Swedish patients with acral lentiginous melanoma. J. Dermatol. Sci. 2013, 72, 284–289. [Google Scholar] [CrossRef]
- Jung, H.J.; Kweon, S.-S.; Lee, J.-B.; Lee, S.-C.; Yun, S.J. A Clinicopathologic Analysis of 177 Acral Melanomas in Koreans. JAMA Dermatol. 2013, 149, 1281. [Google Scholar] [CrossRef]
- Slingluff, C.L.; Vollmer, R.; Seigler, H.F. Acral with melanoma: A review of 185 patients identification of prognostic variables. J. Surg. Oncol. 1990, 45, 91–98. [Google Scholar] [CrossRef]
- Nunes, L.F.; Quintella Mendes, G.L.; Koifman, R.J. Acral melanoma: A retrospective cohort from the Brazilian National Cancer Institute (INCA). Melanoma Res. 2018, 28, 458–464. [Google Scholar] [CrossRef]
- Erdei, E.; Torres, S.M. A new understanding in the epidemiology of melanoma. Expert Rev. Anticancer Ther. 2010, 10, 1811–1823. [Google Scholar] [CrossRef] [PubMed]
- Nunes, L.F.; Mendes, G.L.Q.; Koifman, R.J. Subungual melanoma: A retrospective cohort of 157 cases from Brazilian National Cancer Institute. J. Surg. Oncol. 2018, 118, 1142–1149. [Google Scholar] [CrossRef]
- Barnes, B.C.; Seigler, H.F.; Saxby, T.S.; Kocher, M.S.; Harrelson, J.M. Melanoma of the foot. J. Bone Jt. Surg. 1994, 76, 892–898. [Google Scholar] [CrossRef]
- Tan, K.-B.; Moncrieff, M.; Thompson, J.F.; McCarthy, S.W.; Shaw, H.M.; Quinn, M.J.; Li, L.X.L.; Crotty, K.A.; Stretch, J.R.; Scolyer, R.A. Subungual Melanoma: A study of 124 cases highlighting features of early lesions, potential pitfalls in diagnosis, and guidelines for histologic reporting. Am. J. Surg. Pathol. 2007, 31, 1902–1912. [Google Scholar] [CrossRef] [PubMed]
- Gershenwald, J.E.; Scolyer, R.A. Melanoma Staging: American Joint Committee on Cancer (AJCC) 8th Edition and Beyond. Ann. Surg. Oncol. 2018, 25, 2105–2110. [Google Scholar] [CrossRef] [PubMed]
- Ito, T.; Wada, M.; Nagae, K.; Nakano-Nakamura, M.; Nakahara, T.; Hagihara, A.; Furue, M.; Uchi, H. Acral lentiginous melanoma: Who benefits from sentinel lymph node biopsy? J. Am. Acad. Dermatol. 2015, 72, 71–77. [Google Scholar] [CrossRef] [PubMed]
- Pavri, S.N.; Han, G.; Khan, S.; Han, D. Does sentinel lymph node status have prognostic significance in patients with acral lentiginous melanoma? J. Surg. Oncol. 2019, 119, 1060–1069. [Google Scholar] [CrossRef] [PubMed]
- Nunes, L.F.; Mendes, G.L.Q.; Koifman, R.J. Sentinel Lymph Node Biopsy in Patients with Acral Melanoma: Analysis of 201 Cases from the Brazilian National Cancer Institute. Dermatol. Surg. 2019, 45, 1026–1034. [Google Scholar] [CrossRef]
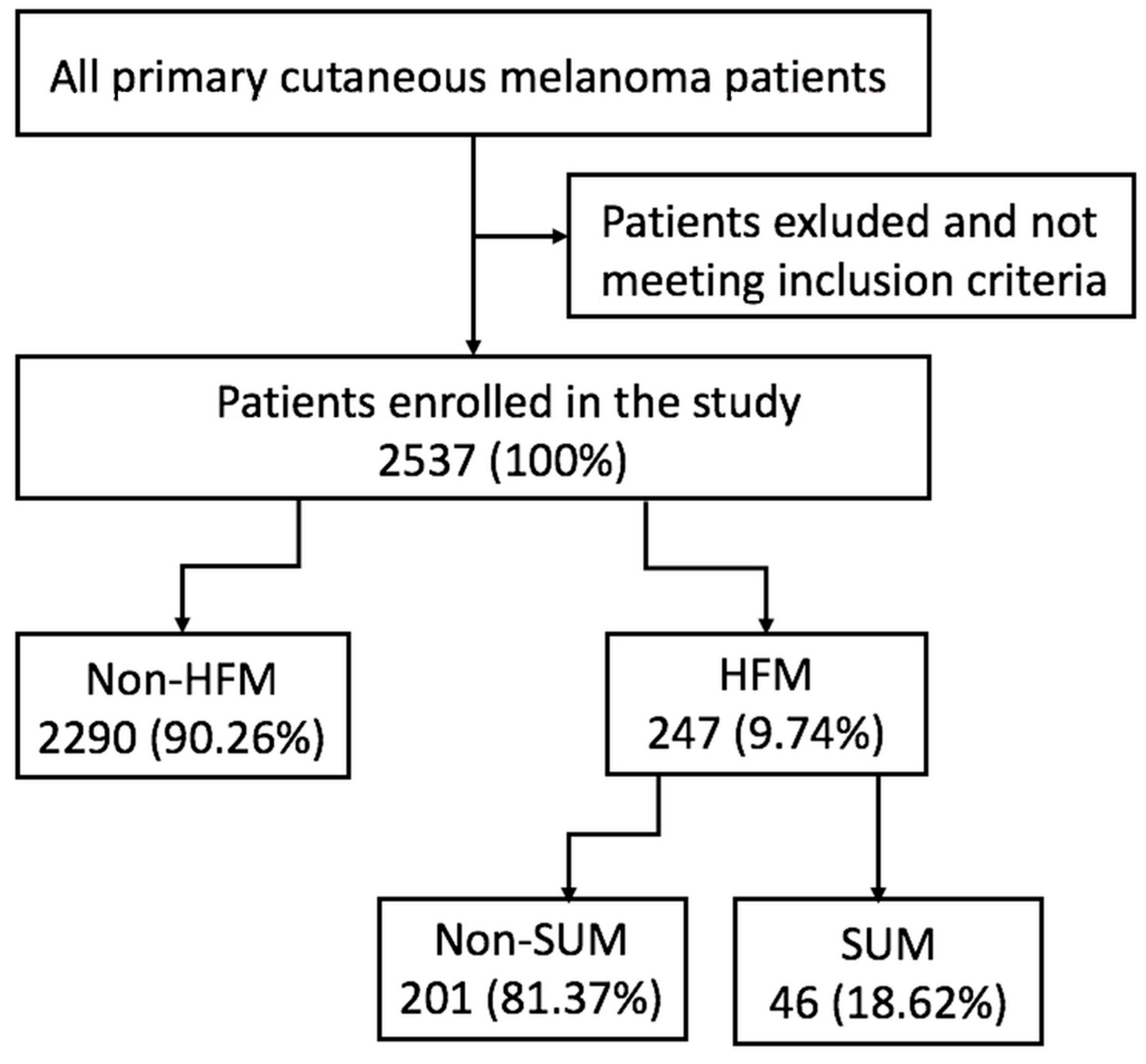
| Variable | Non-HFM, n = 2290 | HFM, n = 247 | |
|---|---|---|---|
| Frequency (%) | Frequency (%) | p-Value | |
| Age (Years) | |||
| ≤50 | 995 (43.3) | 64 (25.9) | <0.001 |
| >50 | 1295 (56.6) | 183 (74.1) | |
| Median | 52.5 | 60.2 | |
| IQR | 20.6 | 20.0 | |
| Mean | 51.7 | 58.5 | |
| Sex | |||
| Female | 1271 (55.5) | 147 (59.5) | 0.25 |
| Male | 1019 (44.5) | 100 (40.5) | |
| Subtype | |||
| NM | 896 (53.8) | 60 (35.3) | <0.001 |
| SSM | 635 (38.1) | 22 (12.9) | |
| ALM | 4 (0.2) | 77 (45.3) | |
| LMM | 131 (7.9) | 11 (6.5) | |
| NA | 624 | 77 | |
| Ulceration | |||
| Absent | 1143 (55.9) | 82 (37.6) | <0.001 |
| Present | 901 (44.1) | 136 (62.4) | |
| NA | 246 | 29 | |
| SLN Biopsy Status | |||
| Negative | 1624 (79.4) | 129 (71.7) | 0.02 |
| Positive | 421 (20.6) | 51 (28.3) | |
| NA | 245 | 67 | |
| Breslow Thickness (mm) | |||
| <1 | 230 (10.4) | 21 (9.6) | <0.001 |
| 1–4 | 1282 (58) | 96 (43.8) | |
| ≥4 | 699 (31.6) | 102 (46.6) | |
| NA | 79 | 28 | |
| Median | 2.2 | 3.3 | |
| IQR | 2.8 | 4.0 | |
| Mean | 3.56 | 4.93 | |
| Clinical Stage | |||
| IA | 337 (15.4) | 15 (7.0) | |
| IB | 409 (18.7) | 25 (11.7) | |
| IIA | 317 (14.5) | 21 (9.8) | |
| IIB | 268 (12.2) | 21 (9.8) | |
| IIC | 136 (6.2) | 22 (10.3) | |
| III | 723 (33.0) | 110 (51.4) | <0.001 |
| NA | 100 | 33 | |
| Variable | Non-SUM, n = 201 | SUM, n = 46 | |
|---|---|---|---|
| Frequency (%) | Frequency (%) | p-Value | |
| Age (Years) | |||
| ≤50 | 57 (28.4) | 7 (15.2) | 0.099 |
| >50 | 144 (71.6) | 39 (84.8) | |
| Median | 59.5 | 66.1 | |
| IQR | 21.9 | 14.0 | |
| Mean | 57.7 | 62.2 | |
| Sex | |||
| Female | 120 (59.7) | 27 (58.7) | 1 |
| Male | 81 (40.3) | 19 (41.3) | |
| Subtype | |||
| NM | 52 (38.2) | 8 (23.5) | 0.0082 |
| SSM | 21 (15.4) | 1 (2.9) | |
| ALM | 53 (39) | 24 (70.6) | |
| LMM | 10 (7.4) | 1 (2.9) | |
| NA | 65 | 12 | |
| Ulceration | |||
| Absent | 70 (39.8) | 12 (28.6) | 0.2423 |
| Present | 106 (60.2) | 30 (71.4) | |
| NA | 25 | 4 | |
| SLN Biopsy Status | |||
| Negative | 107 (73.8) | 22 (62.9) | 0.28 |
| Positive | 38 (26.2) | 13 (37.1) | |
| NA | 56 | 11 | |
| Breslow Thickness (mm) | |||
| <1 | 16 (8.9) | 5 (12.5) | 0.4449 |
| 1–4 | 82 (45.6) | 14 (35.0) | |
| ≥4 | 82 (45.6) | 21 (52.5) | |
| NA | 21 | 6 | |
| Median | 3.1 | 4.0 | |
| IQR | 4.0 | 4.3 | |
| Mean | 4.93 | 5.03 | |
| Clinical Stage | |||
| IA | 14 (7.7) | 1 (3.2) | |
| IB | 21 (11.5) | 4 (13,0) | |
| IIA | 18 (9.8) | 3 (9.7) | |
| IIB | 19 (10.4) | 2 (6.4) | |
| IIC | 17 (9.3) | 5 (16.1) | |
| III | 94 (51.3) | 16 (51.6) | 0.789 |
| NA | 18 | 15 | |
| Variable | Localization of HFM n = 247 | Localization of SUM n = 46 |
|---|---|---|
| Frequency (%) | Frequency (%) | |
| Hand | 38 (15.4) | 15 (32.6) |
| Foot | 209 (84.6) | 31 (67.4) |
| Digital | 76 (30.8) | |
| Subungual | 46 (18.6) | |
| No-digital | 171 (69.2) |
| Hazard Ratio | CI.95 | p-Value | |
|---|---|---|---|
| Non-HFM vs. HFM | 1.64 | 1.36–1.97 | <0.001 |
| Non-SUM vs. SUM | 1.1 | 0.7–1.73 | 0.674 |
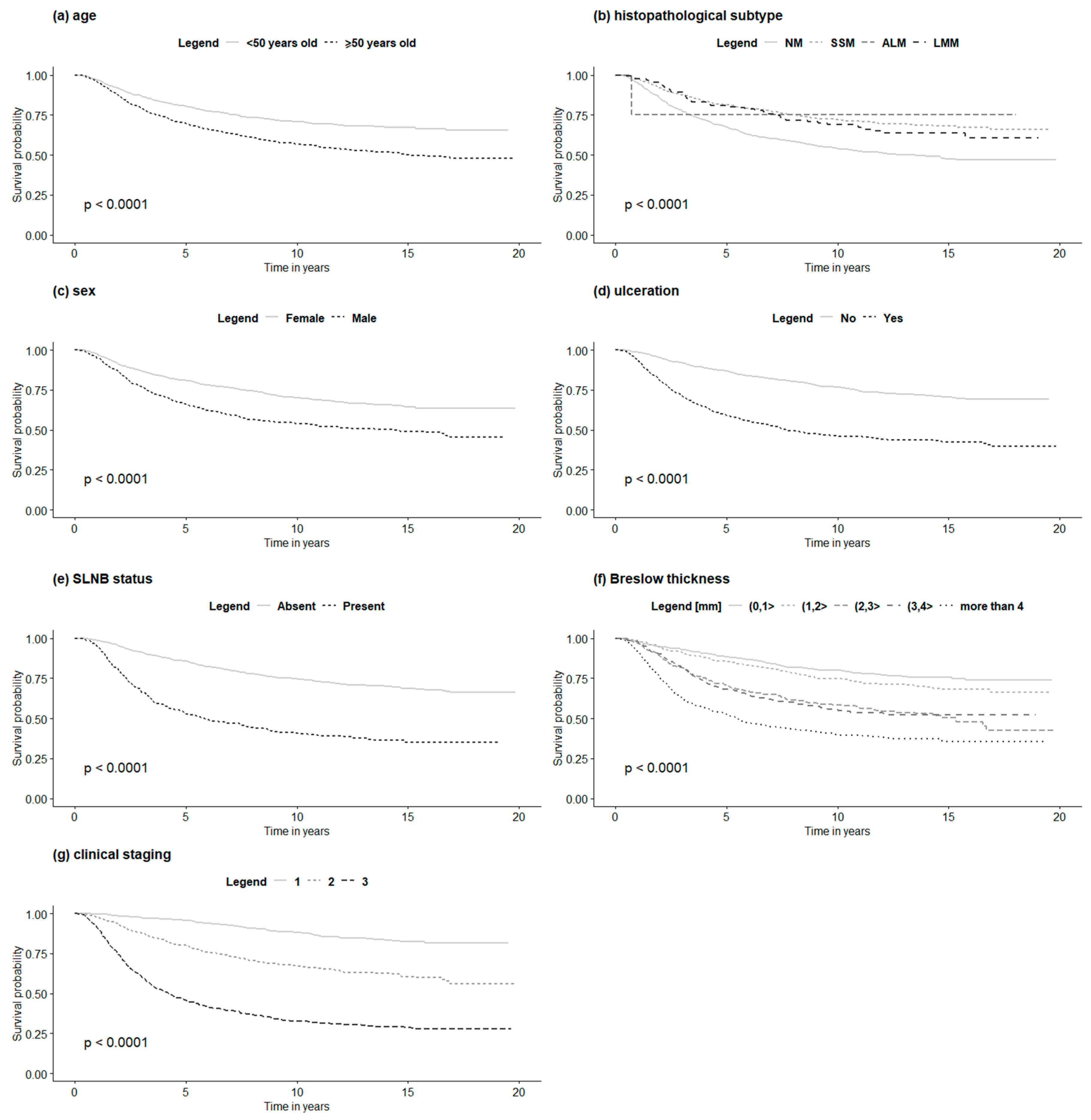
| Univariate analysis in non-HFM group | |||
| Age (years) | 1.03 | 1.02–1.03 | <0.001 |
| Sex—women/men | 1.75 | 1.53–2.01 | <0.001 |
| Subtype—NM, SSM, ALM, LMM | 0.74 | 0.67–0.83 | <0.001 |
| Ulceration—yes/no | 2.83 | 2.44–3.27 | <0.001 |
| SLN biopsy status—positive/negative | 3.18 | 2.72–3.73 | <0.001 |
| Breslow thickness (mm) | 1.08 | 1.07–1.09 | <0.001 |
| Clinical stage | 2.58 | 2.36–2.82 | <0.001 |
| Univariate analysis in HFM group | |||
| Age (years) | 1.03 | 1.01–1.04 | <0.001 |
| Sex—women/men | 1.61 | 1.13–2.27 | 0.008 |
| Subtype—NM, SSM, ALM, LMM | 0.91 | 0.74–1.12 | 0.357 |
| Ulceration—yes/no | 4.02 | 2.45–6.59 | <0.001 |
| SLN biopsy status—positive/negative | 3.14 | 2.06–4.78 | <0.001 |
| Breslow thickness (mm) | 2.21 | 1.60–3.06 | <0.001 |
| Clinical stage | 2.28 | 1.80–2.90 | <0.001 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Borkowska, A.M.; Szumera-Ciećkiewicz, A.; Spałek, M.J.; Teterycz, P.; Czarnecka, A.M.; Rutkowski, P.Ł. Clinicopathological Features and Prognostic Factors of Primary Acral Melanomas in Caucasians. J. Clin. Med. 2020, 9, 2996. https://doi.org/10.3390/jcm9092996
Borkowska AM, Szumera-Ciećkiewicz A, Spałek MJ, Teterycz P, Czarnecka AM, Rutkowski PŁ. Clinicopathological Features and Prognostic Factors of Primary Acral Melanomas in Caucasians. Journal of Clinical Medicine. 2020; 9(9):2996. https://doi.org/10.3390/jcm9092996
Chicago/Turabian StyleBorkowska, Aneta M., Anna Szumera-Ciećkiewicz, Mateusz J. Spałek, Paweł Teterycz, Anna M. Czarnecka, and Piotr Ł. Rutkowski. 2020. "Clinicopathological Features and Prognostic Factors of Primary Acral Melanomas in Caucasians" Journal of Clinical Medicine 9, no. 9: 2996. https://doi.org/10.3390/jcm9092996
APA StyleBorkowska, A. M., Szumera-Ciećkiewicz, A., Spałek, M. J., Teterycz, P., Czarnecka, A. M., & Rutkowski, P. Ł. (2020). Clinicopathological Features and Prognostic Factors of Primary Acral Melanomas in Caucasians. Journal of Clinical Medicine, 9(9), 2996. https://doi.org/10.3390/jcm9092996








