Accuracy of a Symptom-Based Approach to Identify Hypertensive Emergencies in the Emergency Department
Abstract
1. Introduction
2. Methods
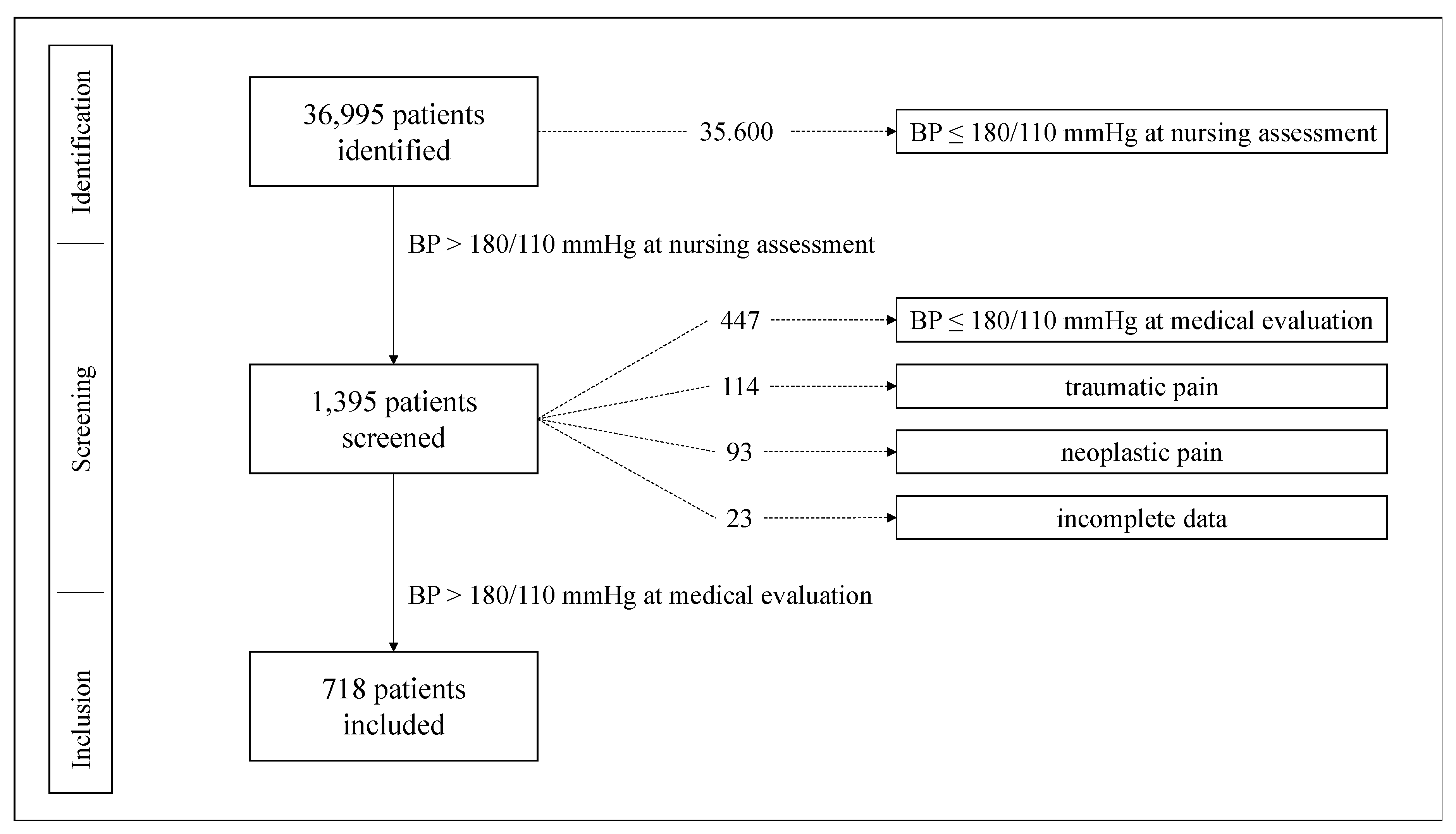
2.1. Inclusion Criteria
2.2. Exclusion Criteria
3. Medical Record Review and Definitions
3.1. Past Medical History
- -
- Cardiovascular risk factors: smoking habit, history of arterial hypertension, diabetes mellitus, dyslipidemia;
- -
- Previous cardiovascular events: coronary artery disease, chronic heart failure, atrial fibrillation (paroxysmal, persistent, and permanent), chronic kidney disease (i.e., glomerular filtration rate < 60 mL/min/1.73 m2), previous ischemic or hemorrhagic stroke, previous transient ischemic attack.
3.2. Ongoing Cardiovascular Therapy
3.3. Presenting Symptoms
- -
- Main symptoms: chest pain (both typical and atypical), dyspnea (as subjective perception), neurological focal signs (motor, sensory, or speech symptoms), headache (regardless of severity), visual impairment (reduced visual acuity or visual fields).
- -
- Less specific symptoms: vertigo, confusion, epistaxis, syncope or pre-syncope, nausea or vomiting, abdominal pain.
- -
- Unspecific symptoms: all other reported symptoms.
3.4. Vital Signs on Admission
3.5. Laboratory Analysis
3.6. Hypertensive Emergency and Uncontrolled Hypertension
- Hypertensive emergency: systolic BP > 180 mm/Hg and/or diastolic BP > 110 mm/Hg and associated aHMOD;
- Uncontrolled hypertension: systolic BP > 180 mm/Hg and/or diastolic BP > 110 mm/Hg without aHMOD.
4. Statistical Analysis
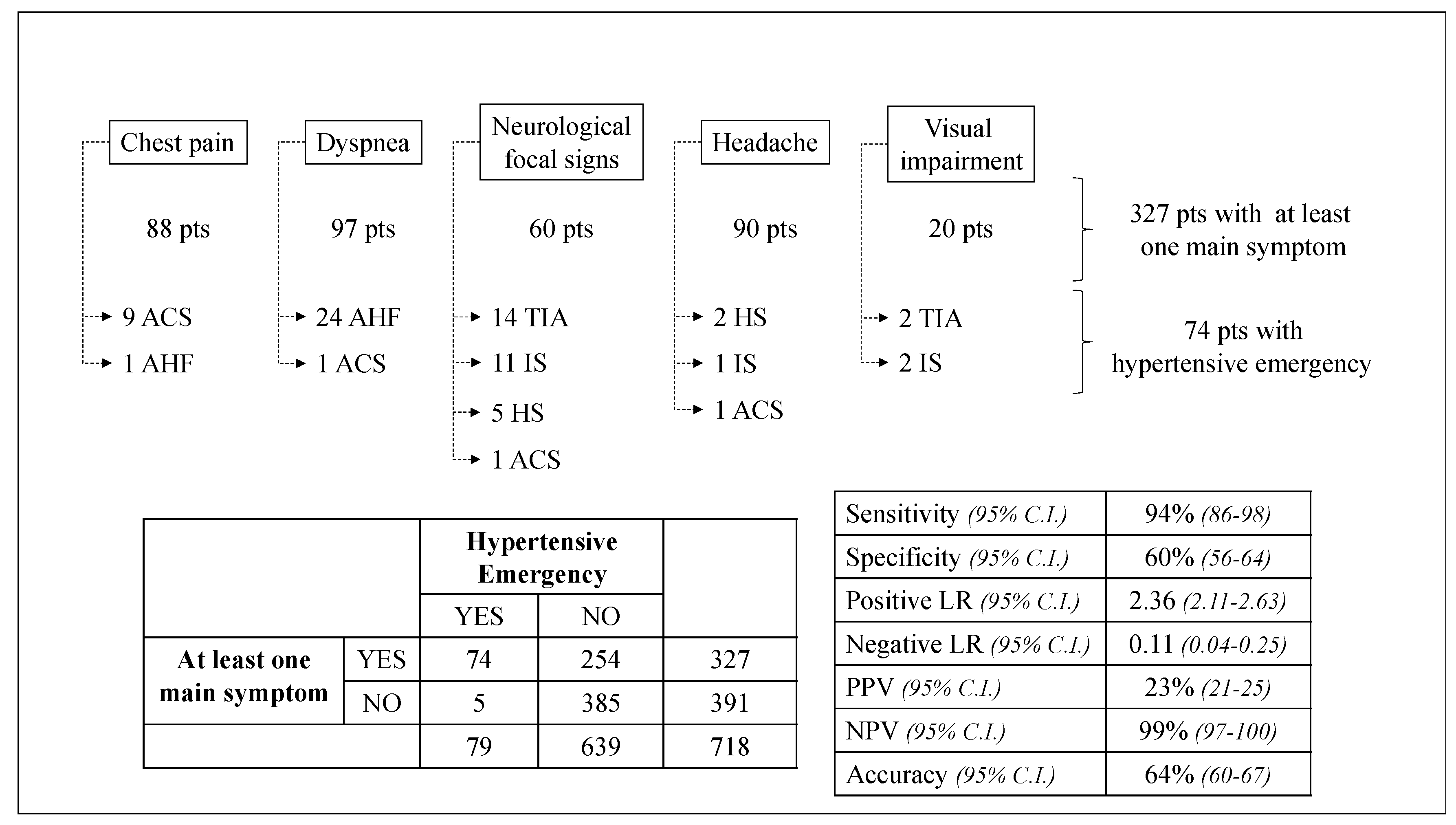
Symptoms Accuracy
5. Results
Symptoms-Based Diagnostic Strategy
6. Discussion
7. Symptoms Accuracy and Clinical Implications
8. Limitations
9. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Van Den Born, B.J.H.; Lip, G.Y.H.; Brguljan-Hitij, J.; Cremer, A.; Segura, J.; Morales, E.; Mahfoud, F.; Amraoui, F.; Persu, A.; Kahan, T.; et al. ESC Council on hypertension position document on the management of hypertensive emergencies. Eur. Hear. J. Cardiovasc. Pharm. 2019, 5, 37–46. [Google Scholar] [CrossRef] [PubMed]
- Janke, A.T.; McNaughton, C.D.; Brody, A.M.; Welch, R.D.; Levy, P.D. Trends in the incidence of hypertensive emergencies in us emergency departments from 2006 to 2013. J. Am. Heart Assoc. 2016, 5, e004511. [Google Scholar] [CrossRef]
- Polgreen, L.A.; Suneja, M.; Tang, F.; Carter, B.L.; Polgreen, P.M. Increasing trend in admissions for malignant hypertension and hypertensive encephalopathy in the United States. Hypertension 2015, 65, 1002–1007. [Google Scholar] [CrossRef] [PubMed]
- Salvetti, M.; Paini, A.; Colonetti, E.; Tarozzi, L.; Bertacchini, F.; Aggiusti, C.; Stassaldi, D.; Rosei, C.A.; Rosei, E.A.; Muiesan, M.L. Hypertensive emergencies and urgencies: A single-centre experience in Northern Italy 2008–2015. J. Hypertens. 2020, 38, 52–58. [Google Scholar] [CrossRef] [PubMed]
- Cremer, A.; Amraoui, F.; Lip, G.Y.H.; Morales, E.; Rubin, S.; Segura, J.; Van Den Born, B.J.; Gosse, P. From malignant hypertension to hypertension-MOD: A modern definition for an old but still dangerous emergency. J. Hum. Hypertens. 2016, 30, 463–466. [Google Scholar] [CrossRef]
- Khwaja, A. KDIGO clinical practice guideline for acute kidney injury. Nephron Clin. Pract. 2012, 120, 179–184. [Google Scholar] [CrossRef]
- Buderer, N.M.F. Statistical methodology: I. incorporating the prevalence of disease into the sample size calculation for sensitivity and specificity. Acad. Emerg. Med. 1996, 3, 895–900. [Google Scholar] [CrossRef]
- Martin, J.F.V.; Higashiama, E.; Garcia, E.; Luizon, M.R.; Cipullo, J.P. Hypertensive crisis profile. Prevalence and clinical presentation. Arq. Bras. Cardiol. 2004, 83, 131–136. [Google Scholar]
- Vilela-Martin, J.F.; Vaz-De-Melo, R.O.; Kuniyoshi, C.H.; Abdo, A.N.R.; Yugar-Toledo, J.C. Hypertensive crisis: Clinical-epidemiological profile. Hypertens. Res. 2011, 34, 367–371. [Google Scholar] [CrossRef]
- Astarita, A.; Covella, M.; Vallelonga, F.; Cesareo, M.; Totaro, S.; Ventre, L.; Aprà, F.; Veglio, F.; Milan, A. Hypertensive emergencies and urgencies in emergency departments. J. Hypertens. 2020, 38, 1203–1210. [Google Scholar] [CrossRef]
- Guiga, H.; Decroux, C.; Michelet, P.; Loundou, A.; Cornand, D.; Silhol, F.; Vaisse, B.; Sarlon-Bartoli, G. Hospital and out-of-hospital mortality in 670 hypertensive emergencies and urgencies. J. Clin. Hypertens. 2017, 19, 1137–1142. [Google Scholar] [CrossRef] [PubMed]
- Kotruchin, P.; Mitsungnern, T.; Ruangsaisong, R.; Imoun, S.; Pongchaiyakul, C. Hypertensive urgency treatment and outcomes in a northeast Thai population: The results from the hypertension registry program. High Blood Press. Cardiovasc. Prev. 2018, 25, 309–315. [Google Scholar] [CrossRef] [PubMed]
- Pinna, G.; Pascale, C.; Fornengo, P.; Arras, S.; Piras, C.; Panzarasa, P.; Carmosino, G.; Franza, O.; Semeraro, V.; Lenti, S.; et al. Hospital admissions for hypertensive crisis in the emergency departments: A large multicenter Italian study. PLoS ONE 2014, 9, e93542. [Google Scholar] [CrossRef]
- Zampaglione, B.; Pascale, C.; Marchisio, M.; Cavallo-Perin, P. Hypertensive urgencies and emergencies: Prevalence and clinical presentation. Hypertension 1996, 27, 144–147. [Google Scholar] [CrossRef] [PubMed]
- Miller, J.B.; Suchdev, K.; Jayaprakash, N.; Hrabec, D.; Sood, A.; Sharma, S.; Levy, P.D. New developments in hypertensive encephalopathy. Curr. Hypertens. Rep. 2018, 20, 13. [Google Scholar] [CrossRef] [PubMed]
- Domek, M.; Gumprecht, J.; Lip, G.Y.H.; Shantsila, A. Malignant hypertension: Does this still exist? J. Hum. Hypertens. 2020, 34, 1–4. [Google Scholar] [CrossRef]
- Van Den Born, B.J.H.; Koopmans, R.P.; Groeneveld, J.O.; Van Montfrans, G.A. Ethnic disparities in the incidence, presentation and complications of malignant hypertension. J. Hypertens. 2006, 24, 2299–2304. [Google Scholar] [CrossRef]
- Berra, E.; Azizi, M.; Capron, A.; Høieggen, A.; Rabbia, F.; Kjeldsen, S.E.; Staessen, J.A.; Wallemacq, P.; Persu, A. Evaluation of adherence should become an integral part of assessment of patients with apparently treatment-resistant hypertension. Hypertension 2016, 68, 297–306. [Google Scholar] [CrossRef]
- Almas, A.; Ghouse, A.; Iftikhar, A.R.; Khursheed, M. Hypertensive crisis, burden, management, and outcome at a tertiary care center in Karachi. Int. J. Chronic Dis. 2014, 2014, 1–7. [Google Scholar] [CrossRef]
- Martínez-Díaz, A.M.; Palazón-Bru, A.; Folgado-de la Rosa, D.M.; Ramírez-Prado, D.; Llópez-Espinós, P.; Beneyto-Ripoll, C.; Gil-Guillén, V.F. A cardiovascular risk score for hypertensive patients previously admitted to hospital. Eur. J. Cardiovasc. Nurs. 2019, 18, 492–500. [Google Scholar] [CrossRef]
- Martínez-Díaz, A.M.; Palazón-Bru, A.; Folgado-de la Rosa, D.M.; Ramírez-Prado, D.; Navarro-Juan, M.; Pérez-Ramírez, N.; Gil-Guillén, V.F. A one-year risk score to predict all-cause mortality in hypertensive inpatients. Eur. J. Intern. Med. 2019, 59, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Dawber, T.R.; Meadors, G.F.; Moore, F.E. Epidemiological approaches to heart disease: The framingham study. Am. J. Public Health 1951, 41, 279–281. [Google Scholar] [CrossRef] [PubMed]
- Body, R.; McDowell, G.; Carley, S.; Mackway-Jones, K. Do risk factors for chronic coronary heart disease help diagnose acute myocardial infarction in the emergency department? Resuscitation 2008, 79, 41–45. [Google Scholar] [CrossRef] [PubMed]
- Han, J.H.; Lindsell, C.J.; Storrow, A.B.; Luber, S.; Hoekstra, J.W.; Hollander, J.E.; Peacock, W.F., IV; Pollack, C.V.; Gibler, W.B. The role of cardiac risk factor burden in diagnosing acute coronary syndromes in the emergency department setting. Ann. Emerg. Med. 2007, 49, 145–152. [Google Scholar] [CrossRef]
| Hypertensive Emergencies (n = 79) | Uncontrolled Hypertension (n = 639) | p-Value | |
|---|---|---|---|
| Demographic Characteristics | |||
| Age (years) | 73.2 ± 13 | 69.5 ± 14 | 0.03 |
| Female sex [n (%)] | 43 (54) | 358 (56) | 0.79 |
| Cardiovascular Risk Factors | |||
| Current smokers [n (%)] | 18 (23) | 138 (22) | 0.81 |
| Arterial hypertension [n (%)] | 61 (77) | 501 (78) | 0.81 |
| Diabetes mellitus [n (%)] | 16 (20) | 108 (17) | 0.46 |
| Dyslipidemia [n (%)] | 14 (18) | 88 (14) | 0.34 |
| No risk factors [n (%)] | 11 (14) | 95 (15) | 0.82 |
| Previous Cardiovascular Events | |||
| Coronary artery disease [n (%)] | 19 (24) | 70 (11) | <0.01 |
| Chronic heart failure [n (%)] | 5 (6) | 15 (2) | 0.04 |
| Atrial fibrillation [n (%)] | 11 (14) | 61 (10) | 0.22 |
| Chronic kidney disease [n (%)] | 8 (10) | 42 (7) | 0.24 |
| Previous stroke [n (%)] | 9 (11) | 40 (6) | 0.09 |
| No previous events [n (%)] | 41 (52) | 462 (72) | <0.01 |
| Vital Signs in ED (Medical Evaluation) | |||
| SBP at admission (mm/Hg) | 193 ± 18 | 188 ± 16 | 0.06 |
| DBP at admission (mm/Hg) | 100 ± 16 | 98 ± 13 | 0.33 |
| SBP at discharge (mm/Hg) | 155 ± 21 | 151 ± 17 | 0.09 |
| DBP at discharge (mm/Hg) | 87 ± 12 | 84 ± 11 | 0.06 |
| HR at admission (bpm) | 88 ± 22 | 84 ± 18 | 0.23 |
| Oxygen saturation at admission (%) | 95 ± 4 | 96 ± 5 | 0.11 |
| Hypertensive Emergencies (n = 79) | Uncontrolled Hypertension (n = 639) | p-Value | |
|---|---|---|---|
| Ongoing Antihypertensive Treatment | |||
| No antihypertensive drugs [n (%)] | 22 (28) | 208 (33) | 0.44 |
| 1 antihypertensive drug [n (%)] | 14 (18) | 149 (23) | 0.26 |
| 2 antihypertensive drugs [n (%)] | 18 (23) | 147 (23) | 0.97 |
| ≥3 antihypertensive drugs [n (%)] | 25 (32) | 135 (21) | 0.03 |
| Specific Pharmacological Classes of Antihypertensive Treatment | |||
| ACE-I [n (%)] | 19 (24) | 151 (24) | 0.93 |
| ARBs [n (%)] | 17 (22) | 146 (23) | 0.79 |
| Beta-Blockers [n (%)] | 38 (48) | 201 (32) | <0.01 |
| Calcium Channel Blockers [n (%)] | 19 (24) | 132 (21) | 0.49 |
| Thiazide diuretics [n (%)] | 6 (8) | 94 (15) | 0.09 |
| Loop diuretics [n (%)] | 21 (27) | 75 (12) | <0.01 |
| Potassium-sparing diuretics [n (%)] | 4 (5) | 30 (5) | 0.88 |
| Alpha-Blockers [n (%)] | 5 (6) | 57 (9) | 0.44 |
| Alpha−2 agonists [n (%)] | 1 (1) | 11 (2) | 0.77 |
| Ongoing Antiplatelet and Anticoagulant Treatment | |||
| Acetylsalicylic acid [n (%)] | 22 (28) | 108 (17) | 0.02 |
| Vitamin K antagonist [n (%)] | 8 (10) | 36 (6) | 0.12 |
| Direct oral anticoagulants [n (%)] | 9 (11) | 45 (7) | 0.17 |
| Hypertensive Emergencies (n = 79) | Uncontrolled Hypertension (n = 639) | p-Value | |
|---|---|---|---|
| Laboratory Data | |||
| Hemoglobin (g/dL) | n = 79 13.4 ± 1.9 | n = 552 13.5 ± 1.9 | 0.86 |
| Creatinine (mg/dL) | n = 79 1.16 ± 0.8 | n = 546 1.08 ± 0.9 | 0.47 |
| Sodium (mEq/L) | n = 79 139 ± 3.1 | n = 546 139 ± 3.9 | 0.87 |
| Potassium (mEq/L) | n = 79 4.1 ± 0.5 | n = 79 4 ± 0.5 | 0.76 |
| Troponin T (ng/L) | n = 43 75.3 ± 133 | n = 268 23.1 ± 49 | 0.02 |
| NTproBNP (pg/mL) | n = 24 7.573 ± 18.649 | n = 86 3.513 ± 10.415 | 0.16 |
| LDH (IU/L) | n = 20 506 ± 43 | n = 112 483 ± 41 | 0.22 |
| Univariate Logistic Regression Analysis | ||||
|---|---|---|---|---|
| Potential Predictors | β Coefficient | 95% CI | Std. Error | p-Value |
| Age (years) | 1.023 | 1.01–1.04 | 0.01 | 0.02 |
| Coronary artery disease | 2.574 | 1.45–4.56 | 0.29 | <0.01 |
| Chronic heart failure | 2.811 | 1.01–7.96 | 0.53 | 0.04 |
| ≥3 antihypertensive drugs | 1.728 | 1.04–2.88 | 0.26 | 0.04 |
| Main symptoms (≥1) | 18.442 | 7.90–43 | 0.43 | <0.01 |
| Multivariate Logistic Regression Analysis | ||||
| Potential Predictors | β Coefficient | 95% CI | Std. Error | p-Value |
| Age (years) | 1.021 | 1.01–1.04 | 0.01 | 0.04 |
| Coronary artery disease | 1.917 | 0.99–3.70 | 0.34 | 0.06 |
| Chronic heart failure | 1.693 | 0.50–5.72 | 0.62 | 0.40 |
| ≥3 antihypertensive drugs | 1.150 | 0.64–2.07 | 0.30 | 0.64 |
| Main symptoms (≥1) | 18.314 | 7.82–42.9 | 0.43 | <0.01 |
| Hypertensive Emergencies (n = 79) | Uncontrolled Hypertension (n = 639) | p-Value | |
|---|---|---|---|
| Main symptoms | |||
| Chest pain [n (%)] | 13 (17) | 75 (12) | 0.23 |
| Dyspnea [n (%)] | 25 (32) | 72 (11) | <0.01 |
| Neurological focal signs [n (%)] | 30 (38) | 30 (5) | <0.01 |
| Headache [n (%)] | 6 (8) | 84 (13) | 0.16 |
| Visual impairment [n (%)] | 4 (5) | 16 (3) | 0.19 |
| Less specific symptoms | |||
| Vertigo/Dizziness [n (%)] | 2 (3) | 61 (10) | 0.04 |
| Confusion [n (%)] | 10 (13) | 61 (10) | 0.38 |
| Epistaxis [n (%)] | 0 (0) | 22 (3) | 0.09 |
| Syncope/pre-syncope [n (%)] | 0 (0) | 25 (4) | 0.07 |
| Nausea/vomiting [n (%)] | 4 (5) | 49 (8) | 0.40 |
| Palpitations [n (%)] | 3 (4) | 48 (8) | 0.23 |
| Abdominal pain [n (%)] | 7 (9) | 69 (11) | 0.60 |
| Totally unspecific symptoms | |||
| Miscellaneous [n (%)] | 0 (0) | 133 (21) | <0.01 |
| No symptoms [n (%)] | 0 (0) | 63 (10) | <0.01 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vallelonga, F.; Carbone, F.; Benedetto, F.; Airale, L.; Totaro, S.; Leone, D.; Astarita, A.; Avenatti, E.; Maule, S.; Veglio, F.; et al. Accuracy of a Symptom-Based Approach to Identify Hypertensive Emergencies in the Emergency Department. J. Clin. Med. 2020, 9, 2201. https://doi.org/10.3390/jcm9072201
Vallelonga F, Carbone F, Benedetto F, Airale L, Totaro S, Leone D, Astarita A, Avenatti E, Maule S, Veglio F, et al. Accuracy of a Symptom-Based Approach to Identify Hypertensive Emergencies in the Emergency Department. Journal of Clinical Medicine. 2020; 9(7):2201. https://doi.org/10.3390/jcm9072201
Chicago/Turabian StyleVallelonga, Fabrizio, Federica Carbone, Francesco Benedetto, Lorenzo Airale, Silvia Totaro, Dario Leone, Anna Astarita, Eleonora Avenatti, Simona Maule, Franco Veglio, and et al. 2020. "Accuracy of a Symptom-Based Approach to Identify Hypertensive Emergencies in the Emergency Department" Journal of Clinical Medicine 9, no. 7: 2201. https://doi.org/10.3390/jcm9072201
APA StyleVallelonga, F., Carbone, F., Benedetto, F., Airale, L., Totaro, S., Leone, D., Astarita, A., Avenatti, E., Maule, S., Veglio, F., Lupia, E., & Milan, A. (2020). Accuracy of a Symptom-Based Approach to Identify Hypertensive Emergencies in the Emergency Department. Journal of Clinical Medicine, 9(7), 2201. https://doi.org/10.3390/jcm9072201







