Early Predictors of Clinical Deterioration in a Cohort of 239 Patients Hospitalized for Covid-19 Infection in Lombardy, Italy
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Laboratory Test, Demographic, and Medical History
2.3. Statistical Methods
3. Results
Prognostic Index
4. Discussion
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Zhu, N.; Zhang, D.; Wang, W.; Li, X.; Yang, B.; Song, J.; Zhao, X.; Huang, B.; Shi, W.; Lu, R.; et al. A Novel Coronavirus from Patients with Pneumonia in China, 2019. N. Engl. J. Med. 2020, 382, 727–733. [Google Scholar] [CrossRef] [PubMed]
- Phelan, A.L.; Katz, R.; Gostin, L.O. The Novel Coronavirus Originating in Wuhan, China. JAMA 2020, 323, 709. [Google Scholar] [CrossRef] [PubMed]
- Coronaviridae Study Group of the International Committee on Taxonomy of Viruses; Gorbalenya, A.E. The species Severe acute respiratory syndrome-related coronavirus: Classifying 2019-nCoV and naming it SARS-CoV-2. Nat. Microbiol. 2020, 5, 536–544. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Rolling Updates on Coronavirus Disease (COVID-19). Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen (accessed on 24 April 2020).
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef]
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus–Infected Pneumonia in Wuhan, China. JAMA 2020, 323, 1061. [Google Scholar] [CrossRef]
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Spina, S.; Marrazzo, F.; Migliari, M.; Stucchi, R.; Sforza, A.; Fumagalli, R. The response of Milan’s Emergency Medical System to the COVID-19 outbreak in Italy. Lancet 2020, 395, 49–50. [Google Scholar] [CrossRef]
- Grasselli, G.; Pesenti, A.; Cecconi, M. Critical Care Utilization for the COVID-19 Outbreak in Lombardy, Italy. JAMA 2020, 323, 1545. [Google Scholar] [CrossRef]
- Onder, G.; Rezza, G.; Brusaferro, S. Case-Fatality Rate and Characteristics of Patients Dying in Relation to COVID-19 in Italy. JAMA 2020. [Google Scholar] [CrossRef]
- Remuzzi, A.; Remuzzi, G. COVID-19 and Italy: What next? Lancet 2020, 395, 1225–1228. [Google Scholar] [CrossRef]
- Rosenbaum, L. Facing Covid-19 in Italy—Ethics, Logistics, and Therapeutics on the Epidemic’s Front Line. N. Engl. J. Med. 2020, 382, 1873–1875. [Google Scholar] [CrossRef] [PubMed]
- Lipsitch, M.; Swerdlow, D.L.; Finelli, L. Defining the Epidemiology of Covid-19—Studies Needed. N. Engl. J. Med. 2020, 382, 1194–1196. [Google Scholar] [CrossRef] [PubMed]
- Ruan, Q.; Yang, K.; Wang, W.; Jiang, L.; Song, J. Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China. Intensive Care Med. 2020, 46, 846–848. [Google Scholar] [CrossRef] [PubMed]
- Ranieri, V.M.; Rubenfeld, G.D.; Thompson, B.T.; Ferguson, N.D.; Caldwell, E.; Fan, E.; Camporota, L.; Slutsky, A.S. Acute Respiratory Distress Syndrome. JAMA 2012, 307, 2526–2533. [Google Scholar] [CrossRef]
- Khwaja, A. KDIGO Clinical Practice Guidelines for Acute Kidney Injury. Nephron 2012, 120, 179–184. [Google Scholar] [CrossRef]
- World Health Organization. Coronavirus Disease (COVID-19) Technical Guidance: Laboratory Testing for 2019-nCoV in Humans. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/technical-guidance/laboratory-guidance (accessed on 24 April 2020).
- Alhazzani, W.; Møller, M.H.; Arabi, Y.M.; Loeb, M.; Gong, M.N.; Fan, E.; Oczkowski, S.; Levy, M.M.; Derde, L.; Dzierba, A.; et al. Surviving Sepsis Campaign: Guidelines on the management of critically ill adults with Coronavirus Disease 2019 (COVID-19). Intensive Care Med. 2020, 46, 854–887. [Google Scholar] [CrossRef]
- Harrell, F.E., Jr.; Lee, K.L.; Mark, D.B. Multivariable prognostic models: Issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat. Med. 1996, 15, 361–387. [Google Scholar] [CrossRef]
- Newson, R.B. Comparing the Predictive Powers of Survival Models Using Harrell’s C or Somers’ D. Stata J. Promot. Commun. Stat. Stata 2010, 10, 339–358. [Google Scholar] [CrossRef]
- Collins, G.S.; Reitsma, J.B.; Altman, D.G.; Moons, K.G. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): The TRIPOD statement. BMJ 2015, 350, 7594. [Google Scholar] [CrossRef]
- Royston, P.; Altman, D.G. External validation of a Cox prognostic model: Principles and methods. BMC Med. Res. Methodol. 2013, 13, 33. [Google Scholar] [CrossRef] [PubMed]
- Van Houwelingen, J. Validation, calibration, revision and combination of prognostic survival models. Stat. Med. 2000, 19, 3401–3415. [Google Scholar] [CrossRef]
- Wynants, L.; Van Calster, B.; Bonten, M.M.J.; Collins, G.S.; A Debray, T.P.; De Vos, M.; Haller, M.C.; Heinze, G.; Moons, K.G.M.; Riley, R.D.; et al. Prediction models for diagnosis and prognosis of covid-19 infection: Systematic review and critical appraisal. BMJ 2020, 369, m1328. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Yu, Y.; Xu, J.; Shu, H.; Xia, J.; Liu, H.; Wu, Y.; Zhang, L.; Yu, Z.; Fang, M.; et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: A single-centered, retrospective, observational study. Lancet Respir. Med. 2020, 8, 475–481. [Google Scholar] [CrossRef]
- Prin, M.; Wunsch, H. International comparisons of intensive care: Informing outcomes and improving standards. Curr. Opin. Crit. Care 2012, 18, 700–706. [Google Scholar] [CrossRef] [PubMed]
- Rhodes, A.; Evans, L.E.; Alhazzani, W.; Levy, M.M.; Antonelli, M.; Ferrer, R.; Kumar, A.; Sevransky, J.E.; Sprung, C.L.; Nunnally, M.E.; et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Intensive Care Med. 2017, 43, 304–377. [Google Scholar] [CrossRef] [PubMed]
- Villar, J.; Pérez-Méndez, L.; López, J.; Belda, J.; Blanco, J.; Saralegui, I.; Suarez-Sipmann, F.; López, J.; Lubillo, S.; Kacmarek, R.M.; et al. An Early PEEP/FiO2Trial Identifies Different Degrees of Lung Injury in Patients with Acute Respiratory Distress Syndrome. Am. J. Respir. Crit. Care Med. 2007, 176, 795–804. [Google Scholar] [CrossRef] [PubMed]
- Karbing, D.S.; Panigada, M.; Bottino, N.; Spinelli, E.; Protti, A.; Rees, S.E.; Gattinoni, L. Changes in shunt, ventilation/perfusion mismatch, and lung aeration with PEEP in patients with ARDS: A prospective single-arm interventional study. Crit. Care 2020, 24, 111–113. [Google Scholar] [CrossRef] [PubMed]
- Cooke, C.R.; Kahn, J.M.; Caldwell, E.; Okamoto, V.N.; Heckbert, S.R.; Hudson, L.D.; Rubenfeld, G.D. Predictors of hospital mortality in a population-based cohort of patients with acute lung injury. Crit. Care Med. 2008, 36, 1412–1420. [Google Scholar] [CrossRef]
- Vincent, J.L.; Moreno, R.; Takala, J.; Willatts, S.; De Mendonça, A.; Bruining, H.; Reinhart, C.K.; Suter, P.M.; Thijs, L.G. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 1996, 22, 707–710. [Google Scholar] [CrossRef]
- Knaus, W.A.; Draper, E.A.; Wagner, D.P.; Zimmerman, J.E. APACHE II: A severity of disease classification system. Crit. Care Med. 1985, 13, 818–829. [Google Scholar] [CrossRef] [PubMed]
- Seymour, C.W.; Liu, V.X.; Iwashyna, T.J.; Brunkhorst, F.M.; Rea, T.D.; Scherag, A.; Rubenfeld, G.; Kahn, J.M.; Shankar-Hari, M.; Singer, M.; et al. Assessment of Clinical Criteria for Sepsis. JAMA 2016, 315, 762–774. [Google Scholar] [CrossRef] [PubMed]
- Chen, T.; Wu, D.; Chen, H.; Yan, W.; Yang, D.; Chen, G.; Ma, K.; Xu, D.; Yu, H.; Wang, H.; et al. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: Retrospective study. BMJ 2020, 368, m1091. [Google Scholar] [CrossRef] [PubMed]
- Angus, D.C.; Van Der Poll, T. Severe Sepsis and Septic Shock. N. Engl. J. Med. 2013, 369, 840–851. [Google Scholar] [CrossRef]
- Guan, W.-J.; Ni, Z.-Y.; Hu, Y.; Liang, W.-H.; Ou, C.-Q.; He, J.-X.; Liu, L.; Shan, H.; Lei, C.-L.; Hui, D.S.; et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef]
- Blackburn, R.; Zhao, H.; Pebody, R.; Hayward, A.; Warren-Gash, C. Laboratory-Confirmed Respiratory Infections as Predictors of Hospital Admission for Myocardial Infarction and Stroke: Time-Series Analysis of English Data for 2004–2015. Clin. Infect. Dis. 2018, 67, 8–17. [Google Scholar] [CrossRef]
- Alatassi, A.; Habbal, M.; Tamim, H.; Sadat, M.; Al Qasim, E.; Arabi, Y.M. Association between troponin-I levels and outcome in critically ill patients admitted to non-cardiac intensive care unit with high prevalence of cardiovascular risk factors. BMC Anesthesiol. 2018, 18, 54. [Google Scholar] [CrossRef]
- Wang, H.E.; Muntner, P.; Chertow, G.M.; Warnock, D.G. Acute kidney injury and mortality in hospitalized patients. Am. J. Nephrol. 2012, 35, 349–355. [Google Scholar] [CrossRef]
- Royal College of Radiology Position on the Role of CT in Patients Suspected with Covid-19 Infection. Available online: https://www.rcr.ac.uk/college/coronavirus-covid-19-what-rcr-doing/rcr-position-role-ct-patients-suspected-covid-19 (accessed on 24 April 2020).
| Mean ± SD; Median (IQR) or n (%) | |
|---|---|
| Demographic Characteristics | |
| Age (years; n = 239) | 63.9 ± 14.0; 65.2 (53.8–74.5) |
| ≥65 | 120 (50.2) |
| <65 | 119 (49.8) |
| Gender (n = 239) | |
| Female | 70 (29.3) |
| Male | 169 (70.7) |
| Clinical Characteristics | |
| Signs and Symptoms at Admission | |
| Systolic blood pressure (mmHg; n = 238) | 125 ± 16.8; 125 (115–135) |
| Pulse (beats per minute; n = 238) | 82 ± 14; 81 (71–90) |
| Respiratory rate (breaths per minute; n = 232) | 19.3 ± 3.2; 18 (18–20) |
| Temperature (°C; n = 239) | 37.3 ± 0.97; 37.3 (36.5–38.0) |
| Body mass index (N=194) | 27.1 ± 4.76; 26.3 (24.0–29.4) |
| Cough (n = 216) | 168 (77.8) |
| Myalgia (n = 176) | 22 (12.5) |
| PaO2 (mmHg; n = 226) | 73.9 ± 20.0; 73.0 (63.0–80.0) |
| PaCO2 (mmHg; n = 201) | 36.0 ± 8.30; 35.0 (31.0–39.0) |
| Ratio of PaO2 to FiO2 (n = 226) | 265 ± 121; 282 (161–357) |
| Comorbid Conditions | |
| Hypertension (n = 239) | 120 (50.2) |
| Diabetes type 2 (n = 239) | 52 (21.8) |
| Coronary heart disease (n = 239) | 40 (16.7) |
| Atrial fibrillation (n = 239) | 27 (11.3) |
| Active neoplasia (n = 239) | 23 (9.6) |
| Chronic obstructive pulmonary disease (n = 239) | 22 (9.2) |
| Chronic kidney disease (n = 238) | 20 (8.4) |
| Other (n = 239) | 26 (10.9) |
| Comorbidities (n = 239) | |
| 0 | 80 (33.5) |
| 1 | 70 (29.3) |
| ≥2 | 89 (37.2) |
| Imaging Features (n = 235) | |
| Normal/non-specific signs | 17 (7.2) |
| Ground-glass opacity | 162 (68.9) |
| Consolidation | 56 (23.8) |
| Laboratory Characteristics | |
| Blood Routine | |
| White blood cells (×109/L; normal range 4.0–10.0; n = 238) | 7.70 ± 5.25; 6.34 (4.93–9.39) |
| Lymphocytes (×109/L; normal range 1.0–4.0; n = 237) | 1.06 ± 0.73; 0.90 (0.70–1.20) |
| Platelets (×109/L; normal range 150–400; n = 238) | 206 ± 85.7; 195 (148–240) |
| Hemoglobin (g/dL; normal range 13.0–16.0; n = 239) | 13.9 ± 1.88; 14.0 (12.7–15.2) |
| Infection-Related Biomarkers | |
| Procalcitonin (ng/mL; normal range 0.05–0.5; n = 222) | 0.62 ± 1.62; 0.16 (0.08–0.38) |
| Interleukin-6 (pg/mL; normal range < 6.4; n = 114) | 73.4 ± 98.6; 43.5 (16.0–89.0) |
| Serum ferritin (ng/mL; normal range 23.9–336.2; n = 212) | 765 ± 858; 498 (228–933) |
| C-reactive protein (mg/dL; normal range < 1.0; n = 239) | 9.70 ± 8.19; 7.73 (2.69–14.7) |
| Blood Biochemistry | |
| Alanine aminotransferase (U/L; normal range < 51; n = 239) | 36.5 ± 37.6; 27.0 (17.0–42.0) |
| Aspartate aminotransferase (U/L; normal range < 51; n = 239) | 46.2 ± 39.9; 35.0 (25.0–54.0) |
| Gamma-glutamyl transpeptidase (U/L; normal range < 55; n = 218) | 61.9 ± 79.5; 41.0 (22.0–69.0) |
| Alkaline phosphatase (U/L; normal range 40–150; n = 214) | 87.5 ± 49.1; 74.0 (59.0–93.0) |
| Total bilirubin (mg/dL; normal range 0.3–1.2; n = 239) | 0.80 ± 1.06; 0.60 (0.50–0.80) |
| Direct bilirubin (mg/dL; normal range < 0.3; n = 229) | 0.26 ± 0.63; 0.20 (0.10–0.30) |
| Indirect bilirubin (mg/dL; normal range 0.05–1.10; n = 218) | 0.60 ± 0.42; 0.50 (0.40–0.70) |
| Serum creatinine (mg/dL; normal range 0.67–1.17; n = 239) | 1.11 ± 0.74; 0.93 (0.75–1.17) |
| Creatine kinase (U/L; normal range < 172; n = 239) | 271 ± 629; 120 (68.0–226) |
| Lactate dehydrogenase (U/L; normal range < 248; n = 234) | 363 ± 177; 316 (243–422) |
| Triglycerides (mg/dL; normal range 10–150; n = 210) | 143 ± 108; 120 (92.0–157) |
| Coagulation Function and Other Biomarkers | |
| Fibrinogen (mg/dL; normal range 160–400; n = 229) | 570 ± 162; 556 (450–665) |
| D-dimer (μg/mL; normal range 0.2–0.35; n = 212) | 1.56 ± 4.27; 0.47 (0.29–0.89) |
| Troponin-I (ng/L; normal range 1–19.8; n = 206) | 128 ± 1242; 8.10 (3.20–22.0) |
| Log-Rank Test | Univariable Cox PH Model | Multivariable Cox PH Model | ||||||
|---|---|---|---|---|---|---|---|---|
| Baseline Parameter | Chi-Squared (d.f.) | p-Value | HR | (95% CI) | p-Value | Adjusted HR | (95% CI) | p-Value |
| Demographic characteristics | ||||||||
| Age (per 10-year increase) | ― | ― | 1.23 | (1.03–1.45) | 0.020 | |||
| Age (≥65 vs. <65 years) | 3.63 (1) | 0.057 | 1.57 | (0.97–2.54) | 0.065 | |||
| Gender (male vs. female) | 1.92 (1) | 0.16 | 1.47 | (0.84–2.56) | 0.18 | |||
| Clinical Characteristics | ||||||||
| Signs and Symptoms at Admission | ||||||||
| Systolic blood pressure (per 10 mmHg increase) | ― | ― | 1.06 | (0.92–1.22) | 0.43 | |||
| Systolic blood pressure (≥140 vs. <140 mmHg) | 0.01 (1) | 0.92 | 1.03 | (0.58–1.82) | 0.93 | |||
| Pulse (per 10 beats per minute increase) | ― | ― | 1.16 | (0.98–1.37) | 0.085 | |||
| Pulse (≥100 vs. <100 beats per minute) | 3.09 (1) | 0.079 | 1.71 | (0.92–3.19) | 0.090 | |||
| Respiratory rate (per 1 breath per minute increase) | ― | ― | 1.15 | (1.09–1.21) | <0.001 | |||
| Respiratory rate (≥20 vs. <20 breaths per minute) | 18.9 (1) | <0.001 | 2.79 | (1.71–4.58) | <0.001 | 1.89 | (1.11–3.23) | 0.020 |
| Temperature (per 1 °C increase) | ― | ― | 0.87 | (0.68–1.12) | 0.28 | |||
| Temperature (≥37.3 vs. <37.3 °C) | 0.12 (1) | 0.73 | 0.92 | (0.58–1.47) | 0.74 | |||
| Body mass index (per 1 kg/m2 increase) | ― | ― | 1.01 | (0.96–1.06) | 0.61 | |||
| Body mass index | ||||||||
| <25 | 0.07 (2) | 0.97 | 1.00 | (reference) | ||||
| 25–30 | 0.97 | (0.55–1.73) | 0.93 | |||||
| >30 | 0.91 | (0.45–1.84) | 0.80 | |||||
| Cough | 0.04 (1) | 0.85 | 0.95 | (0.53–1.69) | 0.85 | |||
| Myalgia | 1.55 (1) | 0.21 | 0.54 | (0.19–1.49) | 0.23 | |||
| PaO2 (per 10 mm Hg increase) | ― | ― | 0.94 | (0.82–1.08) | 0.41 | |||
| PaO2 (≥60 vs. <60 mm Hg) | 8.22 (1) | 0.004 | 0.48 | (0.28–0.81) | 0.006 | |||
| PaCO2 (per 1 mmHg increase) | ― | ― | 1.08 | (1.06–1.11) | <0.001 | |||
| PaCO2 (≥45 vs. <45 mm Hg) | 111 (1) | <0.001 | 15.2 | (7.58–30.4) | <0.001 | |||
| Ratio of PaO2 to FiO2 (per 10 units increase) | ― | ― | 0.92 | (0.90–0.94) | <0.001 | |||
| PaO2/FiO2 > 300 | 74.0 (3) | <0.001 | 1.00 | (reference) | 1.00 | (reference) | ||
| 200 < PaO2/FiO2 ≤ 300 | 3.37 | (1.49–7.61) | 0.003 | 1.96 | (0.82–4.67) | 0.129 | ||
| 100 < PaO2/FiO2 ≤ 200 | 10.6 | (5.09–22.2) | <0.001 | 5.16 | (2.34–11.4) | <0.001 | ||
| 100 ≤ PaO2/FiO2 | 12.3 | (5.43–27.9) | <0.001 | 7.29 | (3.05–17.4) | <0.001 | ||
| Comorbid Conditions | ||||||||
| Hypertension | 2.69 (1) | 0.10 | 1.47 | (0.91–2.37) | 0.11 | |||
| Diabetes type 2 | 1.02 (1) | 0.31 | 1.30 | (0.77–2.21) | 0.33 | |||
| Coronary heart disease | 9.23 (1) | 0.002 | 2.15 | (1.28–3.62) | 0.004 | 2.02 | (1.13–3.64) | 0.018 |
| Atrial fibrillation | 1.25 (1) | 0.26 | 1.43 | (0.75–2.72) | 0.28 | |||
| Active neoplasia | 0.18 (1) | 0.68 | 1.17 | (0.56–2.44) | 0.68 | |||
| Chronic obstructive pulmonary disease | 1.05 (1) | 0.30 | 1.43 | (0.71–2.87) | 0.32 | |||
| Chronic kidney disease | 2.75 (1) | 0.097 | 1.77 | (0.88–3.57) | 0.11 | |||
| Any comorbid condition | 5.99 (1) | 0.014 | 1.98 | (1.12–3.51) | 0.019 | |||
| Imaging Features | ||||||||
| Normal/non-specific signs | 33.9 (2) | <0.001 | 1.00 | (reference) | ||||
| Ground-glass opacity | 1.33 | (0.41–4.34) | 0.63 | |||||
| Consolidation | 4.67 | (1.43–15.3) | 0.011 | |||||
| Laboratory characteristics | ||||||||
| Blood Routine | ||||||||
| White blood cells (per 1 × 109/L increase) | ― | ― | 1.05 | (1.02–1.08) | <0.001 | |||
| White blood cells (×109/L) | ||||||||
| <4 | 5.69 (2) | 0.058 | 1.19 | (0.58–2.45) | 0.64 | |||
| 4–10 | 1.00 | (reference) | ||||||
| >10 | 1.85 | (1.09–3.15) | 0.022 | |||||
| Lymphocytes (per 1 × 109/L increase) | ― | ― | 0.60 | (0.35–1.01) | 0.055 | |||
| Lymphocytes (≥1 vs. <1 × 109/L) | 5.42 (1) | 0.020 | 0.57 | (0.35–0.93) | 0.025 | |||
| Platelets (per 100 × 109/L increase) | ― | ― | 1.26 | (0.97–1.65) | 0.088 | |||
| Platelets (≥150 vs. <150 × 109/L) | 0.35 (1) | 0.56 | 0.86 | (0.50–1.46) | 0.57 | |||
| Hemoglobin (per 1 g/dL increase) | ― | ― | 0.83 | (0.74–0.93) | 0.002 | |||
| Hemoglobin (≥13 vs. <13 g/dL) | 3.33 (1) | 0.068 | 0.65 | (0.40–1.05) | 0.077 | |||
| Infection-Related Biomarkers | ||||||||
| Procalcitonin (per 1 ng/mL increase) | ― | ― | 1.11 | (1.02–1.21) | 0.016 | |||
| Procalcitonin (≥0.5 vs. <0.5 ng/mL) | 20.2 (1) | <0.001 | 2.86 | (1.74–4.69) | <0.001 | |||
| Interleukin-6 (per 100 pg/mL increase) | ― | ― | 1.31 | (1.00–1.73) | 0.049 | |||
| Interleukin-6 (≥100 vs. <100 pg/mL) | 8.81 (1) | 0.003 | 4.34 | (1.50–12.6) | 0.007 | |||
| Serum ferritin (per 100 ng/mL increase) | ― | ― | 1.03 | (1.01–1.06) | 0.004 | |||
| Serum ferritin (≥336.2 vs. <336.2 ng/mL) | 6.96 (1) | 0.008 | 2.49 | (1.23–5.04) | 0.012 | |||
| C-reactive protein (per 1 mg/dL increase) | ― | ― | 1.09 | (1.06–1.11) | <0.001 | 1.06 | (1.03–1.10) | <0.001 |
| C-reactive protein (≥5 vs. <5 mg/dL) | 18.4 (1) | <0.001 | 3.63 | (1.90–6.92) | <0.001 | |||
| Blood Biochemistry | ||||||||
| Alanine aminotransferase (per 10 U/L increase) | ― | ― | 1.03 | (0.98–1.08) | 0.24 | |||
| Alanine aminotransferase (≥50 vs. <50 U/L) | 1.52 (1) | 0.22 | 1.41 | (0.80–2.46) | 0.23 | |||
| Aspartate aminotransferase (per 10 U/L increase) | ― | ― | 1.05 | (1.01–1.09) | 0.010 | |||
| Aspartate aminotransferase (≥50 vs. <50 U/L) | 6.62 (1) | 0.010 | 1.85 | (1.13–3.01) | 0.014 | |||
| Gamma-glutamyl transpeptidase (per 100 U/L increase) | ― | ― | 0.96 | (0.66–1.41) | 0.85 | |||
| Gamma-glutamyl transpeptidase (≥55 vs. <55 U/L) | 1.03 (1) | 0.31 | 1.33 | (0.76–2.34) | 0.32 | |||
| Alkaline phosphatase (per 100 U/L increase) | ― | ― | 0.92 | (0.50–1.69) | 0.79 | |||
| Alkaline phosphatase (≥150 vs. <150 U/L) | 0.57 (1) | 0.45 | 0.64 | (0.20–2.07) | 0.46 | |||
| Total bilirubin (per 1 mg/dL increase) | ― | ― | 1.03 | (0.86–1.23) | 0.73 | |||
| Total bilirubin (≥1.2 vs. <1.2 mg/dL) | 2.85 (1) | 0.091 | 1.68 | (0.90–3.12) | 0.103 | |||
| Direct bilirubin (per 1 mg/dL increase) | ― | ― | 1.06 | (0.80–1.41) | 0.67 | |||
| Direct bilirubin (≥0.3 vs. <0.3 mg/dL) | 8.69 (1) | 0.003 | 2.00 | (1.23–3.24) | 0.005 | |||
| Indirect bilirubin (per 1 mg/dL increase) | ― | ― | 0.27 | (0.07–0.98) | 0.047 | |||
| Indirect bilirubin (≥1.1 vs. <1.1 mg/dL) | 0.06 (1) | 0.81 | 0.87 | (0.27–2.78) | 0.82 | |||
| Serum creatinine (per 1 mg/dL increase) | ― | ― | 1.39 | (1.15–1.69) | 0.001 | |||
| Serum creatinine (≥1.10 vs. <1.10 mg/dL) | 17.8 (1) | <0.001 | 2.60 | (1.62–4.17) | <0.001 | 2.00 | (1.17–3.41) | 0.011 |
| Creatine kinase (per 100 U/L increase) | ― | ― | 1.01 | (0.98–1.04) | 0.61 | |||
| Creatine kinase (≥172 vs. <172 U/L) | 4.21 (1) | 0.040 | 1.61 | (1.01–2.58) | 0.047 | |||
| Lactate dehydrogenase (per 100 U/L increase) | ― | ― | 1.39 | (1.27–1.52) | <0.001 | |||
| Lactate dehydrogenase (≥250 vs. <250 U/L) | 8.12 (1) | 0.004 | 2.62 | (1.30–5.33) | 0.007 | |||
| Triglycerides (per 100 mg/dL increase) | ― | ― | 1.11 | (0.96–1.29) | 0.17 | |||
| Triglycerides (≥150 vs. <150 mg/dL) | 2.93 (1) | 0.087 | 1.69 | (0.92–3.12) | 0.093 | |||
| Coagulation Function and Other Biomarkers | ||||||||
| Fibrinogen (per 100 mg/dL increase) | ― | ― | 1.32 | (1.14–1.52) | <0.001 | |||
| Fibrinogen (≥400 vs. <400 mg/dL) | 1.19 (1) | 0.28 | 1.53 | (0.70–3.35) | 0.29 | |||
| D-dimer (per 1 μg/L increase) | ― | ― | 1.06 | (1.03–1.09) | <0.001 | |||
| D-dimer (≥0.35 vs. <0.35 μg/L) | 17.9 (1) | <0.001 | 3.58 | (1.87–6.86) | <0.001 | |||
| Troponin-I (per 1000 ng/L increase) | ― | ― | 1.15 | (1.03–1.27) | 0.010 | |||
| Troponin-I (≥20 vs. <20 ng/L) | 23.0 (1) | <0.001 | 3.08 | (1.87–5.08) | <0.001 | |||
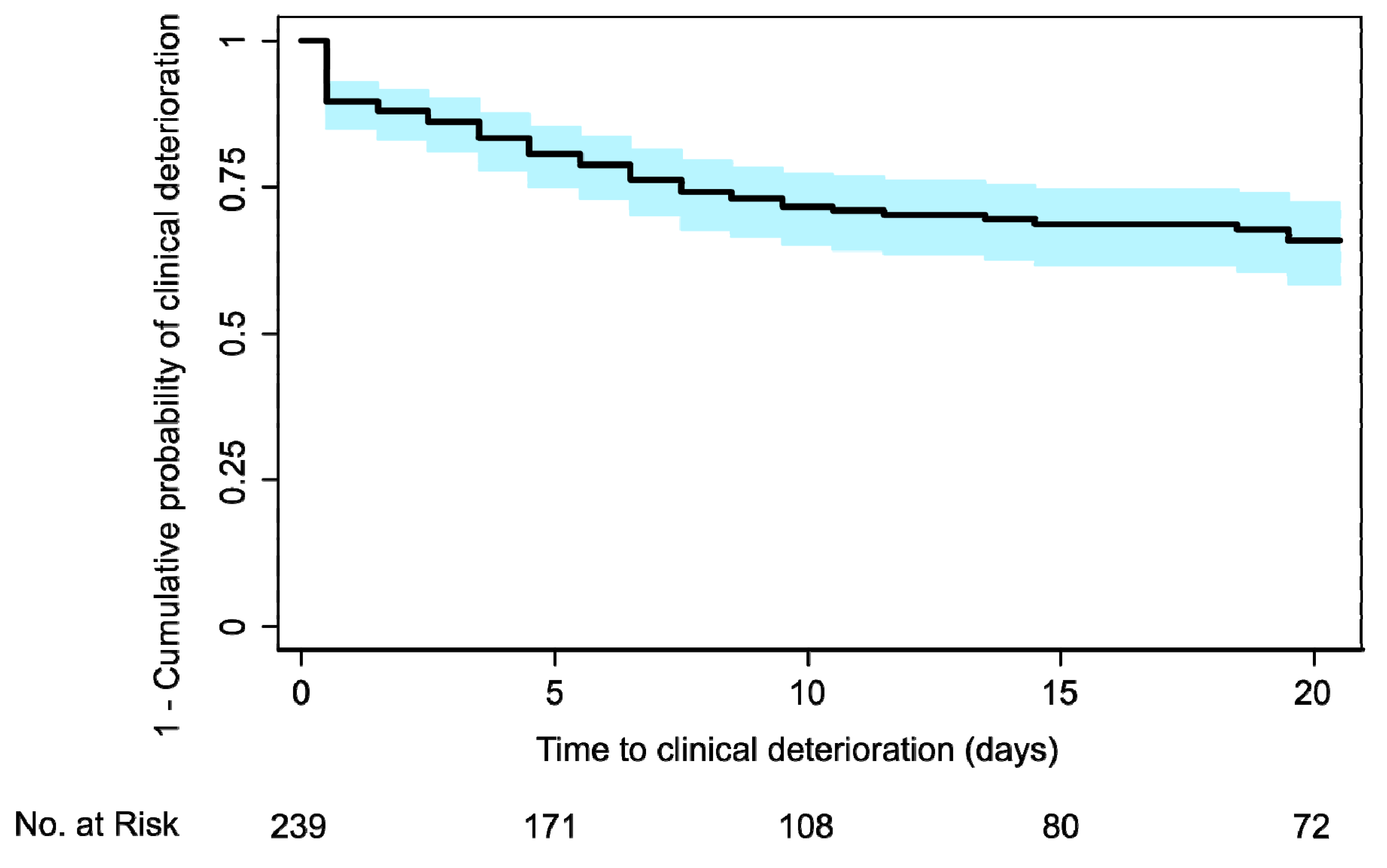
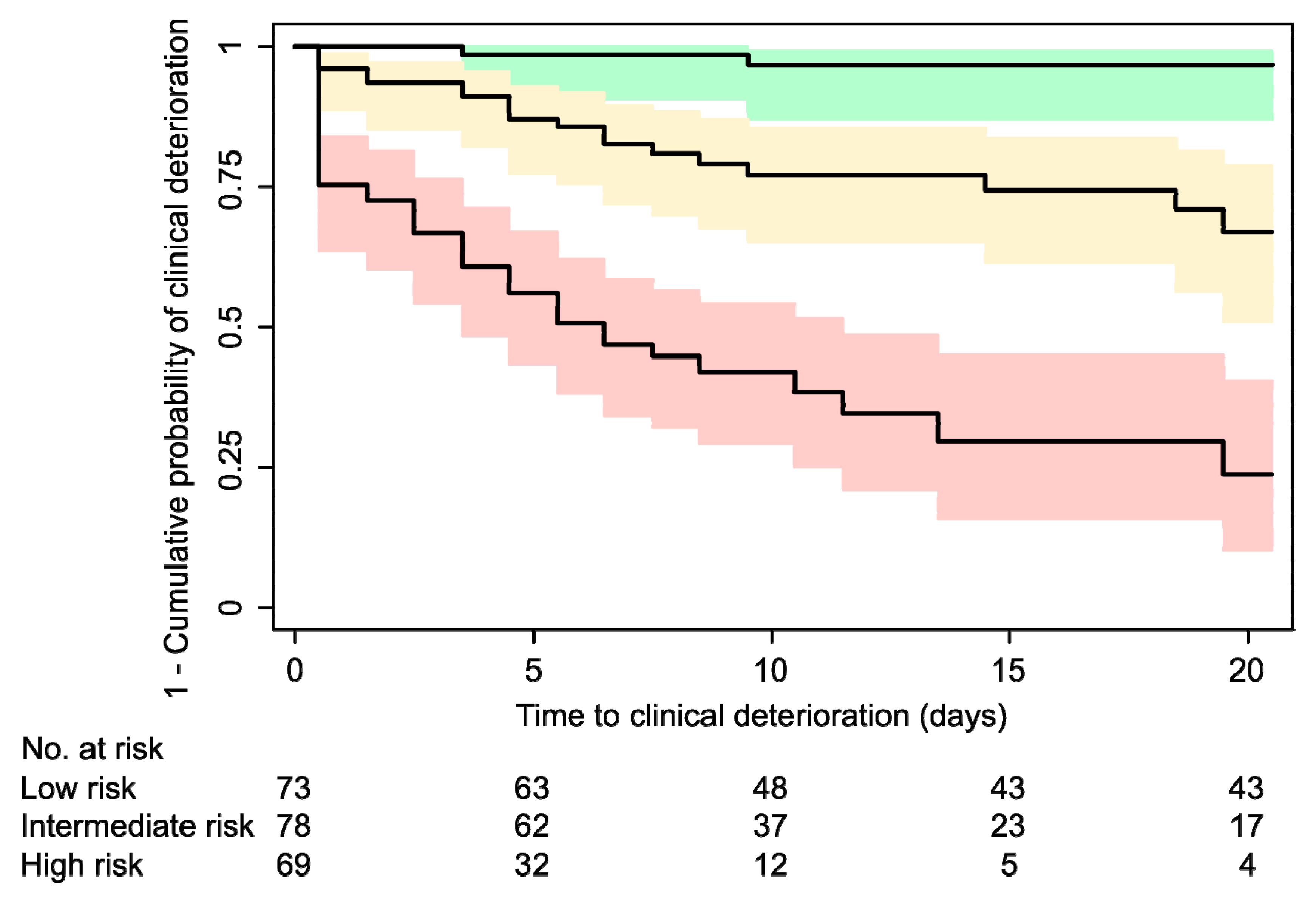
| Risk Category | Score Range | Observed 20-Day Event-Free Survival 1 | Observed 20-Day Survival 2 |
|---|---|---|---|
| “Low risk” | score ≤ 15 | 0.97 (95% CI, 0.87 to 0.99) | 0.98 (95% CI, 0.87 to 0.99) |
| “Intermediate risk” | 15 < score < 40 | 0.67 (95% CI, 0.51 to 0.79) | 0.76 (95% CI, 0.58 to 0.87) |
| “High risk” | score ≥ 40 | 0.24 (95% CI, 0.10 to 0.40) | 0.49 (95% CI, 0.28 to 0.66) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cecconi, M.; Piovani, D.; Brunetta, E.; Aghemo, A.; Greco, M.; Ciccarelli, M.; Angelini, C.; Voza, A.; Omodei, P.; Vespa, E.; et al. Early Predictors of Clinical Deterioration in a Cohort of 239 Patients Hospitalized for Covid-19 Infection in Lombardy, Italy. J. Clin. Med. 2020, 9, 1548. https://doi.org/10.3390/jcm9051548
Cecconi M, Piovani D, Brunetta E, Aghemo A, Greco M, Ciccarelli M, Angelini C, Voza A, Omodei P, Vespa E, et al. Early Predictors of Clinical Deterioration in a Cohort of 239 Patients Hospitalized for Covid-19 Infection in Lombardy, Italy. Journal of Clinical Medicine. 2020; 9(5):1548. https://doi.org/10.3390/jcm9051548
Chicago/Turabian StyleCecconi, Maurizio, Daniele Piovani, Enrico Brunetta, Alessio Aghemo, Massimiliano Greco, Michele Ciccarelli, Claudio Angelini, Antonio Voza, Paolo Omodei, Edoardo Vespa, and et al. 2020. "Early Predictors of Clinical Deterioration in a Cohort of 239 Patients Hospitalized for Covid-19 Infection in Lombardy, Italy" Journal of Clinical Medicine 9, no. 5: 1548. https://doi.org/10.3390/jcm9051548
APA StyleCecconi, M., Piovani, D., Brunetta, E., Aghemo, A., Greco, M., Ciccarelli, M., Angelini, C., Voza, A., Omodei, P., Vespa, E., Pugliese, N., Parigi, T. L., Folci, M., Danese, S., & Bonovas, S., for the Humanitas Covid-19 Task Force. (2020). Early Predictors of Clinical Deterioration in a Cohort of 239 Patients Hospitalized for Covid-19 Infection in Lombardy, Italy. Journal of Clinical Medicine, 9(5), 1548. https://doi.org/10.3390/jcm9051548








