Salivary Gland Dysfunction, Protein Glycooxidation and Nitrosative Stress in Children with Chronic Kidney Disease
Abstract
1. Introduction
2. Material and Methods
2.1. Ethical Issues
2.2. Patients
2.3. Saliva Collection
2.4. Dental Examination
2.5. Blood Collection
2.6. Total Protein Assay
2.7. Redox Assays
2.8. Protein Glycooxidation Products
2.9. Oxidative Stress Products
2.10. Nitrosative Stress Products
2.11. Statistical Analysis
3. Results
3.1. Clinical Characteristics
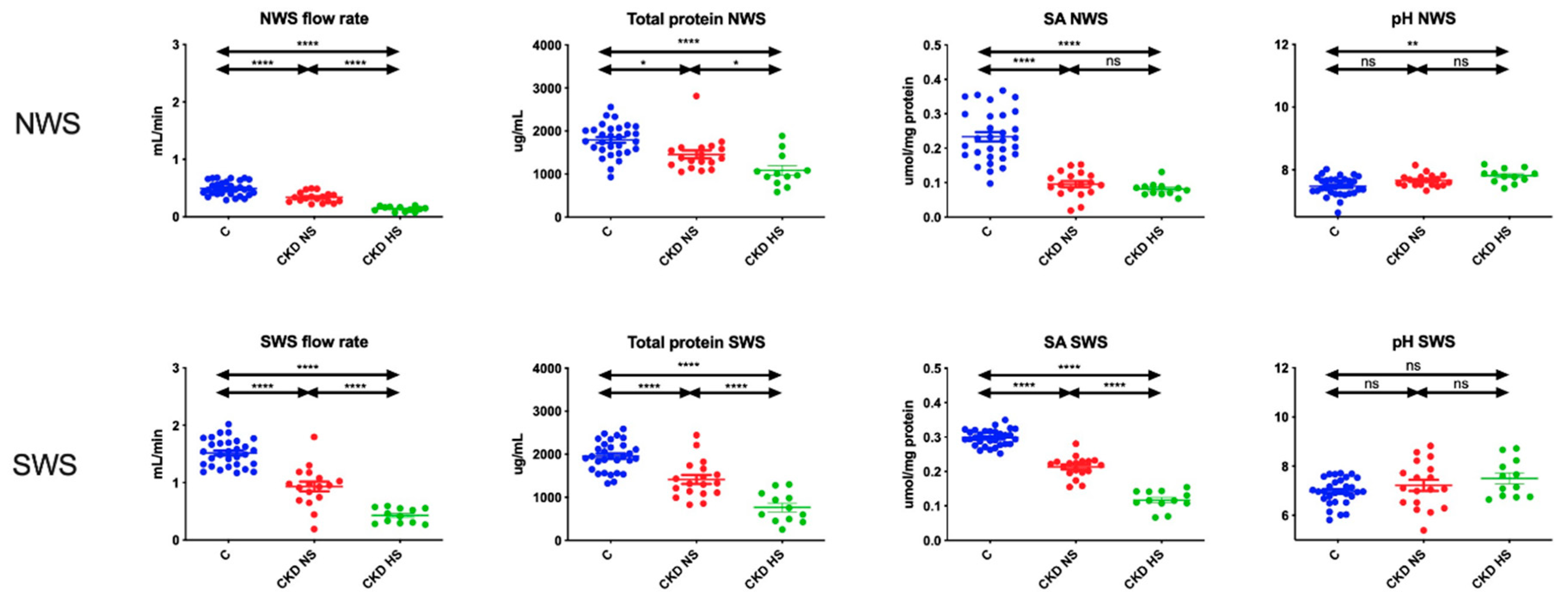
3.2. Salivary Gland Function and Salivary pH
3.3. Dental Examination
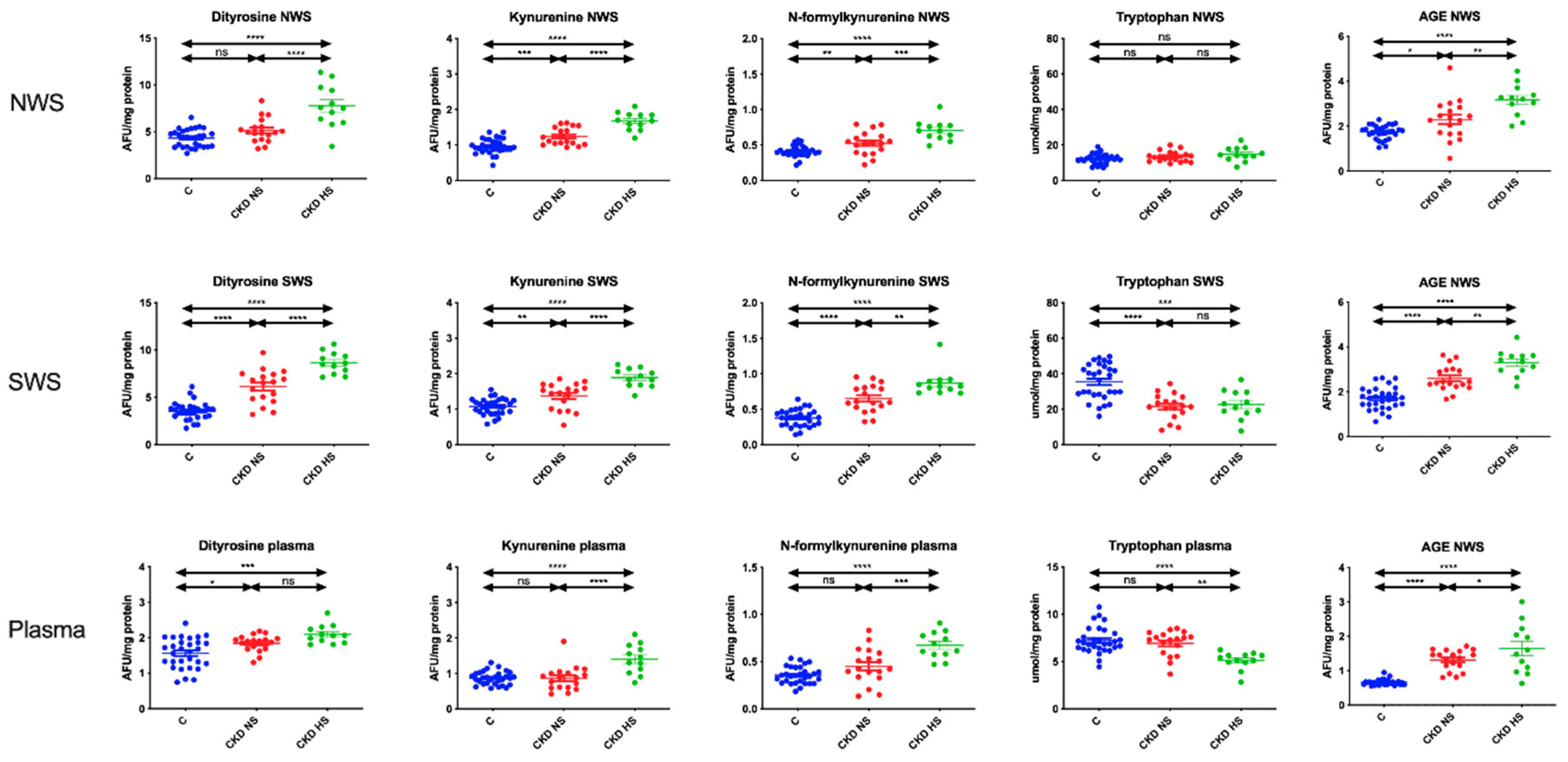
3.4. Glycooxidation Products
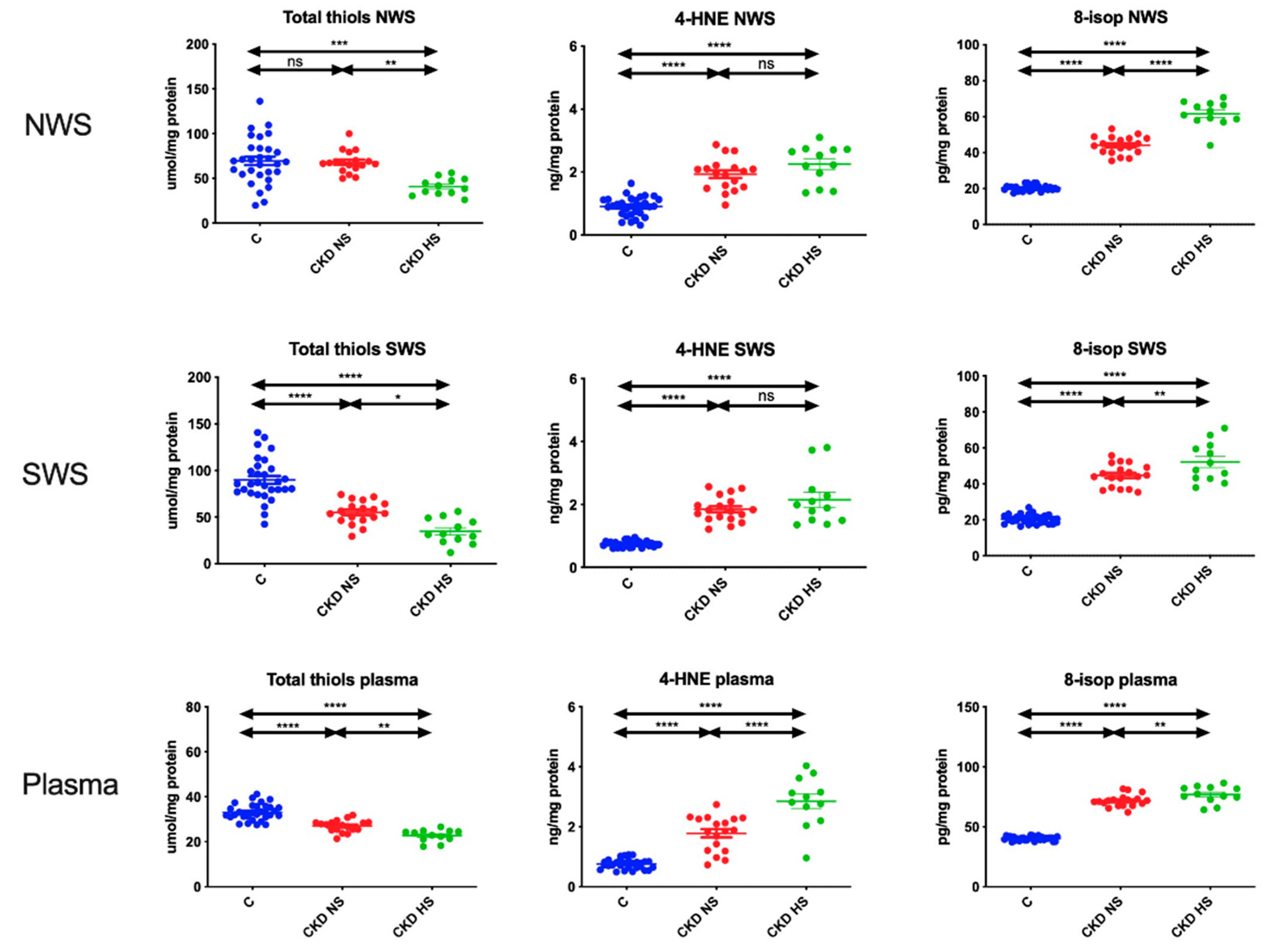
3.5. Oxidative Stress Products
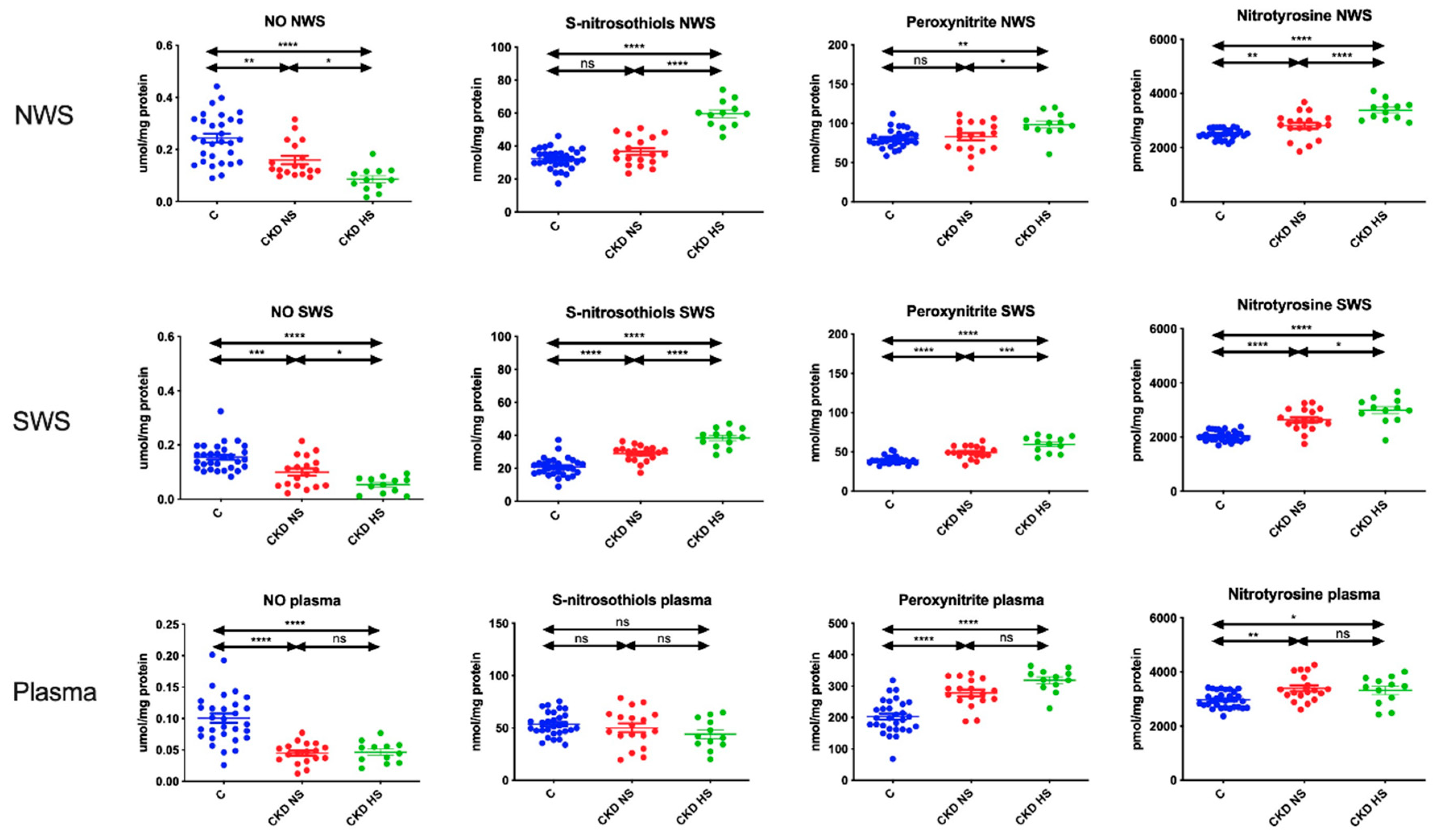
3.6. Nitrosative Stress Products
3.7. Correlations
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Levey, A.S.; De Jong, P.E.; Coresh, J.; Nahas, M.E.; Astor, B.C.; Matsushita, K.; Gansevoort, R.T.; Kasiske, B.L.; Eckardt, K.U. The definition, classification, and prognosis of chronic kidney disease: A KDIGO Controversies Conference report. Kidney Int. 2011. [Google Scholar] [CrossRef] [PubMed]
- Becherucci, F.; Roperto, R.M.; Materassi, M.; Romagnani, P. Chronic kidney disease in children. Clin. Kidney J. 2016. [Google Scholar] [CrossRef] [PubMed]
- Maciejczyk, M.; Szulimowska, J.; Skutnik, A.; Taranta-Janusz, K.; Wasilewska, A.; Wiśniewska, N.; Zalewska, A. Salivary Biomarkers of Oxidative Stress in Children with Chronic Kidney Disease. J. Clin. Med. 2018, 7, 209. [Google Scholar] [CrossRef] [PubMed]
- Tomino, Y. Pathogenesis and treatment of chronic kidney disease: A review of our recent basic and clinical data. Kidney Blood Press. Res. 2014. [Google Scholar] [CrossRef] [PubMed]
- Modaresi, A.; Nafar, M.; Sahraei, Z. Oxidative stress in chronic kidney disease. Iran. J. Kidney Dis. 2015, 9, 165–179. [Google Scholar] [PubMed]
- Putri, A.Y.; Thaha, M. Role Of Oxidative Stress On Chronic Kidney Disease Progression. Acta Med. Indones. 2014, 46, 244–252. [Google Scholar]
- Sureshbabu, A.; Ryter, S.W.; Choi, M.E. Oxidative stress and autophagy: Crucial modulators of kidney injury. Redox Biol. 2015, 4, 208–214. [Google Scholar] [CrossRef]
- Beetham, K.S.; Howden, E.J.; Small, D.M.; Briskey, D.R.; Rossi, M.; Isbel, N.; Coombes, J.S. Oxidative stress contributes to muscle atrophy in chronic kidney disease patients. Redox Rep. 2015, 20, 126–132. [Google Scholar] [CrossRef]
- Li, H.Y.; Hou, F.F.; Zhang, X.; Chen, P.Y.; Liu, S.X.; Feng, J.X.; Liu, Z.Q.; Shan, Y.X.; Wang, G.B.; Zhou, Z.M.; et al. Advanced Oxidation Protein Products Accelerate Renal Fibrosis in a Remnant Kidney Model. J. Am. Soc. Nephrol. 2007, 18, 528–538. [Google Scholar] [CrossRef]
- Fogo, A.B. Mechanisms of progression of chronic kidney disease. Pediatr. Nephrol. 2007. [Google Scholar] [CrossRef]
- Zhou, L.L.; Cao, W.; Xie, C.; Tian, J.; Zhou, Z.; Zhou, Q.; Zhu, P.; Li, A.; Liu, Y.; Miyata, T.; et al. The receptor of advanced glycation end products plays a central role in advanced oxidation protein products-induced podocyte apoptosis. Kidney Int. 2012, 82, 759–770. [Google Scholar] [CrossRef]
- Zhou, L.; Hou, F.F.; Wang, G.B.; Yang, F.; Xie, D.; Wang, Y.P.; Tian, J.W. Accumulation of advanced oxidation protein products induces podocyte apoptosis and deletion through NADPH-dependent mechanisms. Kidney Int. 2009, 76, 1148–1160. [Google Scholar] [CrossRef] [PubMed]
- Nakanishi, T.; Kuragano, T.; Nanami, M.; Nagasawa, Y.; Hasuike, Y. Misdistribution of Iron and Oxidative Stress in Chronic Kidney Disease. Free Radic. Biol. Med. 2018. [Google Scholar] [CrossRef] [PubMed]
- Zalewska, A.; Ziembicka, D.; Żendzian-Piotrowska, M.; Maciejczyk, M. The Impact of High-Fat Diet on Mitochondrial Function, Free Radical Production, and Nitrosative Stress in the Salivary Glands of Wistar Rats. Oxid. Med. Cell. Longev. 2019, 2019, 2606120. [Google Scholar] [CrossRef] [PubMed]
- Fejfer, K.; Buczko, P.; Niczyporuk, M.; Ładny, J.R.; Hady, H.R.; Knaś, M.; Waszkiel, D.; Klimiuk, A.; Zalewska, A.; Maciejczyk, M. Oxidative Modification of Biomolecules in the Nonstimulated and Stimulated Saliva of Patients with Morbid Obesity Treated with Bariatric Surgery. Biomed Res. Int. 2017, 2017. [Google Scholar] [CrossRef] [PubMed]
- Maciejczyk, M.; Taranta-Janusz, K.; Wasilewska, A.; Kossakowska, A.; Zalewska, A. A Case-Control Study of Salivary Redox Homeostasis in Hypertensive Children. Can Salivary Uric Acid be a Marker of Hypertension? J. Clin. Med. 2020, 9, 837. [Google Scholar] [CrossRef]
- Skutnik-Radziszewska, A.; Maciejczyk, M.; Fejfer, K.; Krahel, J.; Flisiak, I.; Kołodziej, U.; Zalewska, A. Salivary Antioxidants and Oxidative Stress in Psoriatic Patients: Can Salivary Total Oxidant Status and Oxidative Status Index Be a Plaque Psoriasis Biomarker? Oxid. Med. Cell. Longev. 2020, 2020, 9086024. [Google Scholar] [CrossRef]
- Silvestre-Rangil, J.; Bagán, L.; Silvestre, F.J.; Bagán, J.V. Oral manifestations of rheumatoid arthritis. A cross-sectional study of 73 patients. Clin. Oral Investig. 2016. [Google Scholar] [CrossRef]
- Żukowski, P.; Maciejczyk, M.; Waszkiel, D. Sources of free radicals and oxidative stress in the oral cavity. Arch. Oral Biol. 2018, 92, 8–17. [Google Scholar] [CrossRef]
- Zalewska, A.; Maciejczyk, M.; Szulimowska, J.; Imierska, M.; Błachnio-Zabielska, A. High-Fat Diet Affects Ceramide Content, Disturbs Mitochondrial Redox Balance, and Induces Apoptosis in the Submandibular Glands of Mice. Biomolecules 2019, 9, 877. [Google Scholar] [CrossRef]
- Maciejczyk, M.; Matczuk, J.; Żendzian-Piotrowska, M.; Niklińska, W.; Fejfer, K.; Szarmach, I.; Ładny, J.R.; Zieniewska, I.; Zalewska, A. Eight-Week Consumption of High-Sucrose Diet Has a Pro-Oxidant Effect and Alters the Function of the Salivary Glands of Rats. Nutrients 2018, 10, 1530. [Google Scholar] [CrossRef] [PubMed]
- Maciejczyk, M.; Szulimowska, J.; Taranta-Janusz, K.; Werbel, K.; Wasilewska, A.; Zalewska, A. Salivary FRAP as A Marker of Chronic Kidney Disease Progression in Children. Antioxidants 2019, 8, 409. [Google Scholar] [CrossRef] [PubMed]
- Maciejczyk, M.; Żukowski, P.; Zalewska, A. Salivary Biomarkers in Kidney Diseases. In Saliva in Health and Disease; Tvarijonaviciute, A., Martínez-Subiela, S., López-Jornet, P., Lamy, E., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 193–219. ISBN 978-3-030-37681-9. [Google Scholar]
- Klassen, J.T.; Krasko, B.M. The dental health status of dialysis patients. J. Can. Dent. Assoc. 2002. [Google Scholar]
- Zalewska, A.; Kossakowska, A.; Taranta-Janusz, K.; Zięba, S.; Fejfer, K.; Salamonowicz, M.; Kostecka-Sochoń, P.; Wasilewska, A.; Maciejczyk, M. Dysfunction of Salivary Glands, Disturbances in Salivary Antioxidants and Increased Oxidative Damage in Saliva of Overweight and Obese Adolescents. J. Clin. Med. 2020, 9, 548. [Google Scholar] [CrossRef] [PubMed]
- Skutnik-Radziszewska, A.; Maciejczyk, M.; Flisiak, I.; Kołodziej, J.K.U.; Kotowska-Rodziewicz, A.; Klimiuk, A.; Zalewska, A. Enhanced Inflammation and Nitrosative Stress in the Saliva and Plasma of Patients with Plaque Psoriasis. J. Clin. Med. 2020, 9, 745. [Google Scholar] [CrossRef]
- Saleh, J.; Figueiredo, M.A.Z.; Cherubini, K.; Salum, F.G. Salivary hypofunction: An update on aetiology, diagnosis and therapeutics. Arch. Oral Biol. 2015, 60, 242–255. [Google Scholar] [CrossRef]
- Maciejczyk, M.; Zalewska, A.; Ładny, J.R. Salivary Antioxidant Barrier, Redox Status, and Oxidative Damage to Proteins and Lipids in Healthy Children, Adults, and the Elderly. Oxid. Med. Cell. Longev. 2019, 2019, 1–12. [Google Scholar] [CrossRef]
- Schwartz, G.J.; Muñoz, A.; Schneider, M.F.; Mak, R.H.; Kaskel, F.; Warady, B.A.; Furth, S.L. New Equations to Estimate GFR in Children with CKD. J. Am. Soc. Nephrol. 2009, 20, 629–637. [Google Scholar] [CrossRef]
- National Kidney Foundation K/DOQI clinical practice guidelines for chronic kidney disease: Evaluation, classification, and stratification. Am. J. Kidney Dis. 2002, 39, S1–S266.
- NIH The Fourth Report on the Diagnosis, Evaluation, and Treatment of High Blood Pressure in Children and Adolescents. Natl. Inst. Health 2005, 05–5267, 1–60. [CrossRef]
- Klimiuk, A.; Maciejczyk, M.; Choromańska, M.; Fejfer, K.; Waszkiewicz, N.; Zalewska, A. Salivary Redox Biomarkers in Different Stages of Dementia Severity. J. Clin. Med. 2019, 8, 840. [Google Scholar] [CrossRef] [PubMed]
- Maciejczyk, M.; Kossakowska, A.; Szulimowska, J.; Klimiuk, A.; Knaś, M.; Car, H.; Niklińska, W.; Ładny, J.R.; Chabowski, A.; Zalewska, A. Lysosomal Exoglycosidase Profile and Secretory Function in the Salivary Glands of Rats with Streptozotocin-Induced Diabetes. J. Diabetes Res. 2017, 2017, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Bernfeld, P. Amylases, alpha and beta. Methods Enzymol. I 1955. [Google Scholar] [CrossRef]
- World Health Organization. Oral Health Surveys: Basic Methods; WHO Publications Center USA: Albany, NY, USA, 2013; ISBN 9789241548649. [Google Scholar]
- Borys, J.; Maciejczyk, M.; Krȩtowski, A.J.; Antonowicz, B.; Ratajczak-Wrona, W.; Jablonska, E.; Zaleski, P.; Waszkiel, D.; Ladny, J.R.; Zukowski, P.; et al. The redox balance in erythrocytes, plasma, and periosteum of patients with titanium fixation of the jaw. Front. Physiol. 2017, 8. [Google Scholar] [CrossRef]
- Rice-Evans, C.A.; Diplock, A.T.; Symons, M.C.R. Assay of antioxidant nutrients and antioxidant enzymes. Lab. Tech. Biochem. Mol. Biol. 1991, 22, 185–206. [Google Scholar] [CrossRef]
- Kalousová, M.; Zima, T.; Tesař, V.; Dusilová-Sulková, S.; Škrha, J. Advanced glycoxidation end products in chronic diseases - Clinical chemistry and genetic background. Mutat. Res.-Fundam. Mol. Mech. Mutagen. 2005. [Google Scholar]
- Ellman, G.L. Tissue sulfhydryl groups. Arch. Biochem. Biophys. 1959, 82, 70–77. [Google Scholar] [CrossRef]
- Grisham, M.B.; Johnson, G.G.; Lancaster, J.R. Quantitation of nitrate and nitrite in extracellular fluids. Methods Enzymol. 1996, 268, 237–246. [Google Scholar] [CrossRef]
- Borys, J.; Maciejczyk, M.; Antonowicz, B.; Krętowski, A.; Sidun, J.; Domel, E.; Dąbrowski, J.R.; Ładny, J.R.; Morawska, K.; Zalewska, A. Glutathione Metabolism, Mitochondria Activity, and Nitrosative Stress in Patients Treated for Mandible Fractures. J. Clin. Med. 2019, 8, 127. [Google Scholar] [CrossRef]
- Wink, D.A.; Kim, S.; Coffin, D.; Cook, J.C.; Vodovotz, Y.; Chistodoulou, D.; Jourd’heuil, D.; Grisham, M.B. Detection of S-nitrosothiols by fluorometric and colorimetric methods. Methods Enzymol. 1999, 301, 201–211. [Google Scholar] [CrossRef]
- Beckman, J.S.; Ischiropoulos, H.; Zhu, L.; van der Woerd, M.; Smith, C.; Chen, J.; Harrison, J.; Martin, J.C.; Tsai, M. Kinetics of superoxide dismutase- and iron-catalyzed nitration of phenolics by peroxynitrite. Arch. Biochem. Biophys. 1992, 298, 438–445. [Google Scholar] [CrossRef]
- Davidovich, E.; Schwarz, Z.; Davidovitch, M.; Eidelman, E.; Bimstein, E. Oral findings and periodontal status in children, adolescents and young adults suffering from renal failure. J. Clin. Periodontol. 2005. [Google Scholar] [CrossRef]
- Bosch, J.A.; Veerman, E.C.I.; de Geus, E.J.; Proctor, G.B. α-Amylase as a reliable and convenient measure of sympathetic activity: Don’t start salivating just yet! Psychoneuroendocrinology 2011, 36, 449–453. [Google Scholar] [CrossRef] [PubMed]
- Beal, M.F. Oxidatively modified proteins in aging and disease. Free Radic. Biol. Med. 2002. [Google Scholar] [CrossRef]
- Ghisaidoobe, A.B.T.; Chung, S.J. Intrinsic tryptophan fluorescence in the detection and analysis of proteins: A focus on Förster resonance energy transfer techniques. Int. J. Mol. Sci. 2014, 15, 22518–22538. [Google Scholar] [CrossRef]
- Ott, C.; Jacobs, K.; Haucke, E.; Navarrete Santos, A.; Grune, T.; Simm, A. Role of advanced glycation end products in cellular signaling. Redox Biol. 2014, 2, 411–429. [Google Scholar] [CrossRef]
- Knaś, M.; Maciejczyk, M.; Daniszewska, I.; Klimiuk, A.; Matczuk, J.; Kołodziej, U.; Waszkiel, D.; Ładny, J.R.; Żendzian-Piotrowska, M.; Zalewska, A. Oxidative Damage to the Salivary Glands of Rats with Streptozotocin-Induced Diabetes-Temporal Study: Oxidative Stress and Diabetic Salivary Glands. J. Diabetes Res. 2016, 2016, 1–13. [Google Scholar] [CrossRef]
- Nogueira, F.N.; Romero, A.C.; da Silva Pedrosa, M.; Ibuki, F.K.; Bergamaschi, C.T. Oxidative stress and the antioxidant system in salivary glands of rats with experimental chronic kidney disease. Arch. Oral Biol. 2020, 113, 104709. [Google Scholar] [CrossRef]
- Pérez, P.; Kwon, Y.J.; Alliende, C.; Leyton, L.; Aguilera, S.; Molina, C.; Labra, C.; Julio, M.; Leyton, C.; González, M.J. Increased acinar damage of salivary glands of patients with Sjögren’s syndrome is paralleled by simultaneous imbalance of matrix metalloproteinase 3/tissue inhibitor of metalloproteinases 1 and matrix metalloproteinase 9/tissue inhibitor of metalloprotein. Arthritis Rheum. 2005. [Google Scholar] [CrossRef]
- Proctor, G.B.; Carpenter, G.H. Regulation of salivary gland function by autonomic nerves. Auton. Neurosci. 2007, 133, 3–18. [Google Scholar] [CrossRef]
- Chaudhary, K.; Malhotra, K.; Sowers, J.; Aroor, A. Uric acid-key ingredient in the recipe for cardiorenal metabolic syndrome. CardioRenal Med. 2013. [Google Scholar] [CrossRef] [PubMed]
- Clodfelter, W.H.; Basu, S.; Bolden, C.; Dos Santos, P.C.; King, S.B.; Kim-Shapiro, D.B. The relationship between plasma and salivary NOx. Nitric oxide Biol. Chem. 2015, 47, 85–90. [Google Scholar] [CrossRef]
- Klimiuk, A.; Zalewska, A.; Sawicki, R.; Knapp, M.; Maciejczyk, M. Salivary Oxidative Stress Increases With the Progression of Chronic Heart Failure. J. Clin. Med. 2020, 9, 769. [Google Scholar] [CrossRef] [PubMed]
- Hu, J.; Iragavarapu, S.; Nadkarni, G.N.; Huang, R.; Erazo, M.; Bao, X.; Verghese, D.; Coca, S.; Ahmed, M.K.; Peter, I. Location-Specific Oral Microbiome Possesses Features Associated With CKD. Kidney Int. Rep. 2018. [Google Scholar] [CrossRef] [PubMed]
- Maciejczyk, M.; Zalewska, A.; Gerreth, K. Salivary Redox Biomarkers in Selected Neurodegenerative Diseases. J. Clin. Med. 2020, 9, 497. [Google Scholar] [CrossRef]
- López-Pintor, R.-M.; López-Pintor, L.; Casañas, E.; de Arriba, L.; Hernández, G. Risk factors associated with xerostomia in haemodialysis patients. Med. Oral Patol. Oral Cir. Bucal 2017, 22, e185–e192. [Google Scholar] [CrossRef] [PubMed]
- de Azambuja Berti-Couto, S.; Couto-Souza, P.H.; Jacobs, R.; Nackaerts, O.; Rubira-Bullen, I.R.F.; Westphalen, F.H.; Moysés, S.J.; Ignácio, S.A.; da Costa, M.B.; Tolazzi, A.L. Clinical diagnosis of hyposalivation in hospitalized patients. J. Appl. Oral Sci. 2012. [Google Scholar] [CrossRef]
| C (n = 30) | CKD NS (n = 18) | CKD HS (n = 12) | ANOVA p | ||
|---|---|---|---|---|---|
| NWS flow (mL min−1) | mean ± SD | 0.495 ± 0.1 | 0.338 ± 0.09 | 0.138 ± 0.04 | <0.0001 |
| min | 0.292 | 0.219 | 0.0730 | ||
| max | 0.682 | 0.494 | 0.199 | ||
| Men n | 15 | 7 | 8 | NA | |
| Age (years) | 13 ± 3.5 | 14 ± 3.2 | 12 ± 3.7 | NS | |
| CKD n | stage 1 | - | 6 | 0 | NA |
| stage 2 | - | 5 | 0 | NA | |
| stage 3 | - | 7 | 0 | NA | |
| stage 4 | - | 0 | 6 | NA | |
| stage 5 | - | 0 | 6 | NA | |
| eGFR (mL/min/1.73 m2) | 136 ± 6.9 | 84 ± 43 | 18 ± 7.4 | < 0.0001 | |
| Serum creatinine (mg/dL) | 0.41 ± 0.09 | 1.2 ± 0.54 | 4.6 ± 0.58 | <0.0001 | |
| Serum urea (mg/dL) | 18 ± 2.6 | 44 ± 4.7 | 124 ± 13 | <0.0001 | |
| Albuminuria (mg/24 h) | 8 ± 0.9 | 51 ± 23 | 815 ± 236 | <0.0001 | |
| Proteinuria (mg/24 h) | 58.4 ± 3.5 | 403 ± 165 | 845 ± 248 | <0.0001 | |
| Hgb (g/dL) | 14.5 ± 0.3 | 13 ± 0.49 | 11 ± 0.51 | <0.0001 | |
| Hct (%) | 39.7 ± 1.1 | 38 ± 1.2 | 33 ± 1.3 | <0.0001 | |
| Serum iron (μg/dL) | 82 ± 2.1 | 68 ± 6.7 | 91 ± 8.6 | <0.0001 | |
| Hypertension n | - | 1 | 11 | NA | |
| Dialysis n | - | 0 | 6 | NA | |
| Drugs per day n | 0 | - | 2 | 0 | NA |
| 1–2 | - | 10 | 4 | NA | |
| 3–4 | - | 6 | 8 | NA | |
| Drugs n | iron | - | 9 | 10 | NA |
| loop diuretics | - | 10 | 9 | NA | |
| ACEI | - | 10 | 9 | NA | |
| β-blockers | - | 3 | 5 | NA | |
| CCB | - | 3 | 3 | NA | |
| C (n = 30) | CKD NS (n = 18) | CKD HS (n = 12) | ANOVA p | |
|---|---|---|---|---|
| DMFT | 2.5 ± 0.5 | 2.7 ± 0.7 | 2.8 ± 0.6 | NS |
| dmft | 9.8 ± 0.5 | 10.1 ± 0.5 | 10.3 ± 0.7 | NS |
| GI | 0 ± 0.1 | 0 ± 0.2 | 0 ± 0.2 | NS |
| SBI | 0 ± 0.1 | 0 ± 0.1 | 0 ± 0.1 | NS |
| C (n = 30) | CKD (n = 30) | |||||
|---|---|---|---|---|---|---|
| eGFR | serum Cr | serum urea | eGFR | serum Cr | serum urea | |
| Dityrosine NWS | 0.086 | 0.163 | 0.22 | −0.579 | 0.72 | 0.713 |
| Kynurenine NWS | 0.17 | 0.246 | 0.057 | −0.562 | 0.71 | 0.691 |
| N-formylkynurenine NWS | 0.225 | 0.322 | 0.118 | −0.527 | 0.641 | 0.585 |
| Tryptophan NWS | 0.095 | 0.218 | 0.216 | 0.203 | −0.102 | −0.097 |
| AGE NWS | 0.228 | 0.041 | −0.015 | −0.531 | 0.555 | 0.568 |
| Total thiols NWS | 0.13 | −0.164 | −0.144 | 0.431 | −0.675 | −0.649 |
| 4-HNE NWS | 0.135 | 0.154 | 0.163 | −0.512 | 0.533 | 0.476 |
| 8-isop NWS | −0.017 | 0.096 | −0.032 | −0.592 | 0.819 | 0.76 |
| NO NWS | −0.072 | −0.089 | −0.132 | 0.609 | −0.594 | −0.531 |
| S-nitrosothiols NWS | −0.014 | 0.268 | 0.543 | −0.675 | 0.551 | 0.525 |
| Peroxynitrite NWS | 0.039 | −0.073 | −0.236 | −0.537 | 0.631 | 0.579 |
| Nitrotyrosine NWS | 0.194 | 0.018 | −0.034 | −0.565 | 0.625 | 0.593 |
| Dityrosine SWS | 0.037 | 0.076 | −0.349 | −0.632 | 0.721 | 0.601 |
| Kynurenine SWS | 0.217 | −0.249 | −0.146 | −0.48 | 0.586 | 0.626 |
| N-formylkynurenine SWS | 0.219 | −0.456 | −0.028 | −0.457 | 0.509 | 0.49 |
| Tryptophan SWS | 0.041 | 0.247 | 0.049 | 0.255 | −0.296 | −0.193 |
| AGE SWS | −0.138 | −0.134 | −0.123 | −0.413 | 0.372 | 0.39 |
| Total thiols SWS | 0.106 | 0.379 | 0.007 | 0.674 | −0.736 | −0.657 |
| 4-HNE SWS | −0.057 | −0.251 | −0.081 | −0.286 | 0.306 | 0.227 |
| 8-isop SWS | −0.136 | −0.306 | 0.203 | −0.417 | 0.464 | 0.55 |
| NO SWS | −0.123 | 0.176 | 0.353 | 0.661 | −0.52 | −0.452 |
| S-nitrosothiols SWS | −0.484 | 0.106 | 0.257 | −0.357 | 0.448 | 0.417 |
| Peroxynitrite SWS | 0.198 | −0.459 | −0.031 | −0.29 | 0.341 | 0.243 |
| Nitrotyrosine SWS | −0.068 | −0.015 | −0.156 | −0.41 | 0.367 | 0.2 |
| C (n = 30) | CKD (n = 30) | |||||||
|---|---|---|---|---|---|---|---|---|
| NWS Flow | Total Protein NWS | SA NWS | pH NWS | NWS Flow | Total Protein NWS | SA NWS | pH NWS | |
| Dityrosine NWS | −0.092 | −0.128 | 0.061 | 0.002 | −0.754 | −0.633 | −0.522 | 0.561 |
| Kynurenine NWS | −0.042 | 0.051 | 0.123 | −0.152 | −0.722 | −0.521 | −0.362 | 0.388 |
| N-formylkynurenine NWS | −0.166 | 0.255 | 0.154 | −0.133 | −0.663 | −0.52 | −0.24 | 0.545 |
| Tryptophan NWS | −0.009 | −0.107 | −0.073 | −0.217 | 0.242 | 0.363 | 0.348 | −0.14 |
| AGE NWS | −0.111 | −0.236 | −0.063 | −0.141 | −0.618 | −0.358 | −0.367 | 0.403 |
| Total thiols NWS | −0.013 | 0.265 | 0.063 | −0.18 | 0.6 | 0.395 | 0.09 | −0.34 |
| 4-HNE NWS | 0.161 | 0.156 | −0.12 | −0.191 | −0.628 | −0.632 | −0.403 | 0.619 |
| 8-isop NWS | 0.163 | 0.335 | 0.043 | −0.254 | −0.711 | −0.385 | −0.316 | 0.422 |
| NO NWS | −0.24 | 0.149 | 0.183 | −0.093 | 0.577 | 0.343 | 0.439 | 0.032 |
| S-nitrosothiols NWS | 0.214 | 0.259 | 0.058 | −0.332 | −0.725 | −0.397 | −0.255 | 0.285 |
| Peroxynitrite NWS | −0.069 | −0.021 | 0.297 | 0.101 | −0.666 | −0.872 | −0.486 | 0.508 |
| Nitrotyrosine NWS | 0.063 | 0.094 | −0.282 | 0.538 | −0.594 | −0.402 | −0.354 | 0.268 |
| SWS Flow | Total Protein SWS | SA SWS | pH SWS | SWS Flow | Total Protein SWS | SA SWS | pH SWS | |
| Dityrosine SWS | −0.041 | 0.082 | −0.118 | 0.152 | −0.534 | −0.513 | −0.584 | 0.088 |
| Kynurenine SWS | 0.16 | −0.168 | 0.155 | 0.039 | −0.466 | −0.394 | −0.473 | 0.099 |
| N-formylkynurenine SWS | 0.24 | 0.06 | −0.129 | 0.143 | −0.442 | −0.482 | −0.478 | −0.016 |
| Tryptophan SWS | 0.277 | −0.301 | −0.055 | −0.192 | 0.026 | 0.083 | −0.026 | 0.035 |
| AGE SWS | −0.488 | 0.078 | −0.051 | −0.123 | −0.553 | −0.401 | −0.513 | −0.008 |
| Total thiols SWS | 0.037 | 0.177 | −0.271 | −0.202 | 0.566 | 0.509 | 0.538 | −0.192 |
| 4-HNE SWS | −0.127 | 0.126 | 0.11 | 0.22 | −0.119 | 0.02 | −0.151 | 0.014 |
| 8-isop SWS | 0.045 | −0.114 | −0.027 | 0.116 | −0.216 | −0.318 | −0.369 | −0.346 |
| NO SWS | 0.245 | −0.267 | −0.091 | −0.066 | 0.589 | 0.448 | 0.612 | −0.187 |
| S-nitrosothiols SWS | 0.152 | 0.302 | −0.294 | −0.051 | −0.466 | −0.329 | −0.47 | 0.052 |
| Peroxynitrite SWS | 0.349 | −0.001 | 0.036 | 0.239 | −0.242 | −0.297 | −0.516 | −0.095 |
| Nitrotyrosine SWS | 0.084 | 0.025 | −0.003 | 0.074 | −0.266 | −0.521 | −0.232 | 0.067 |
| C (n = 30) | CKD (n = 30) | |||
|---|---|---|---|---|
| NWS & plasma | SWS & plasma | NWS & plasma | SWS & plasma | |
| Dityrosine | 0.825 | −0.106 | 0.173 | 0.106 |
| Kynurenine | 0.698 | 0.140 | 0.504 | 0.629 |
| N-formylkynurenine | 0.327 | −0.019 | 0.268 | 0.060 |
| Tryptophan | 0.507 | 0.208 | −0.374 | 0.043 |
| AGE | 0.781 | 0.461 | −0.268 | 0.314 |
| Total thiols | −0.042 | 0.084 | 0.387 | 0.335 |
| 4-HNE | 0.473 | 0.210 | 0.257 | 0.262 |
| 8-isop | 0.041 | −0.208 | 0.349 | 0.350 |
| NO | 0.030 | −0.209 | 0.016 | −0.078 |
| S-nitrosothiols | −0.045 | 0.174 | −0.059 | 0.025 |
| Peroxynitrite | 0.121 | −0.340 | 0.224 | 0.334 |
| Nitrotyrosine | 0.096 | −0.054 | 0.165 | 0.140 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maciejczyk, M.; Szulimowska, J.; Taranta-Janusz, K.; Wasilewska, A.; Zalewska, A. Salivary Gland Dysfunction, Protein Glycooxidation and Nitrosative Stress in Children with Chronic Kidney Disease. J. Clin. Med. 2020, 9, 1285. https://doi.org/10.3390/jcm9051285
Maciejczyk M, Szulimowska J, Taranta-Janusz K, Wasilewska A, Zalewska A. Salivary Gland Dysfunction, Protein Glycooxidation and Nitrosative Stress in Children with Chronic Kidney Disease. Journal of Clinical Medicine. 2020; 9(5):1285. https://doi.org/10.3390/jcm9051285
Chicago/Turabian StyleMaciejczyk, Mateusz, Julita Szulimowska, Katarzyna Taranta-Janusz, Anna Wasilewska, and Anna Zalewska. 2020. "Salivary Gland Dysfunction, Protein Glycooxidation and Nitrosative Stress in Children with Chronic Kidney Disease" Journal of Clinical Medicine 9, no. 5: 1285. https://doi.org/10.3390/jcm9051285
APA StyleMaciejczyk, M., Szulimowska, J., Taranta-Janusz, K., Wasilewska, A., & Zalewska, A. (2020). Salivary Gland Dysfunction, Protein Glycooxidation and Nitrosative Stress in Children with Chronic Kidney Disease. Journal of Clinical Medicine, 9(5), 1285. https://doi.org/10.3390/jcm9051285







