Calprotectin and Receptor for Advanced Glycation End Products as a Potential Biomarker in Abdominal Aortic Aneurysm
Abstract
1. Introduction
2. Material and Methods
2.1. Study Group
2.2. Control Group
2.3. Study Material
2.4. Study Methods
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
Abbreviations
| AAA | abdominal aortic aneurysm |
| CML | carboxymethyllysine |
| CIMT | carotid intima-media thickness test |
| ELISA | enzyme-linked immunosorbent assay |
| AGE | end products of advanced glycation |
| esRAGE | endogenous secretory receptor for advanced glycation end-products (esRAGE) |
| HMGB-1 | high mobility group box-1 |
| IFNγ | interferon-gamma |
| Il-6 | interleukin-6 |
| Il-8 | interleukin-8 |
| MIF | macrophage migration inhibitory factor |
| MMP-2 | matrix metalloproteinase-2 |
| MMP-2 | matrix metalloproteinase-9 |
| NF-κB | nuclear factor-kappa B |
| tPA | tissue plasminogen activator |
| PAP | plasmin-antiplasmin complexes |
| RAGE | receptor for advanced glycation end products |
| SEP | serum elastin peptides |
| sRAGE | soluble receptor for advanced glycation end products |
| TNF-α | tumor necrosis factor alpha |
References
- Lovell, M.; Harris, K.A.; Derose, G.; Forbes, T.L.; Fortier, M.; Scott, B. A screening program to identify risk factors for abdominal aortic aneurysms. Can. J. Surg. 2006, 49, 113–116. [Google Scholar] [PubMed]
- Howard, D.; Banerjee, A.; Fairhead, J.F.; Handa, A.; Silver, L.E.; Rothwell, P.M.; the Oxford Vascular Study. Age-specific incidence, risk factors and outcome of acute abdominal aortic aneurysms in a defined population. Br. J. Surg. 2015, 102, 907–915. [Google Scholar] [CrossRef] [PubMed]
- Urbonavicius, S.; Urbonaviciene, G.; Honoré, B.; Henneberg, E.W.; Vorum, H.; Lindholt, J.S. Potential circulating biomarkers for abdominal aortic aneurysm expansion and rupture—A systematic review. Eur. J. Vasc. Endovasc. Surg. 2008, 36, 273–280. [Google Scholar] [CrossRef] [PubMed]
- Lindholt, J.; Kristensen, K.L.; Burillo, E.; Martínez-López, D.; Calvo, C.; Ros, E.; Martín-Ventura, J.L.; Sala-Vila, A. Arachidonic Acid, but Not Omega-3 Index, Relates to the Prevalence and Progression of Abdominal Aortic Aneurysm in a Population-Based Study of Danish Men. J. Am. Hear. Assoc. 2018, 7, e007790. [Google Scholar] [CrossRef] [PubMed]
- Marchetti, A.A.; Pratesi, G.; Di Giulio, L.; Battistini, M.; Massoud, R.; Ippoliti, A. EVAR and OPEN treatment of abdominal aortic aneurysm: What is the role of MMP-9 in the follow-up? J. Médecine Vasc. 2017, 42, 21–28. [Google Scholar] [CrossRef]
- Kruzliak, P.; Novak, J.; Novak, M.; Fodor, G.J. Role of calprotectin in cardiometabolic diseases. Cytokine Growth Factor Rev. 2014, 25, 67–75. [Google Scholar] [CrossRef]
- Angel, K.; Provan, S.; Fagerhol, M.K.; Mowinckel, P.; Kvien, T.K.; Atar, D. Effect of 1-year anti-TNF-α therapy on aortic stiffness, carotid atherosclerosis, and calprotectin in inflammatory arthropathies: A controlled study. Am. J. Hypertens. 2012, 25, 644–650. [Google Scholar] [CrossRef] [PubMed]
- Moris, D.; Theocharis, S.; Davakis, S.; Patelis, N.; Agrogiannis, G.; Vlachos, I.S.; Spartalis, E.; Athanasiou, A.; Bakoyiannis, C.; Perrea, D.N.; et al. Serum Calprotectin as a Novel Biomarker in Abdominal Aortic Aneurysm Pathogenesis and Progression: Preliminary Data from Experimental Model in Rats. Curr. Vasc. Pharmacol. 2018, 16, 168–178. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, A.M.; Vianna, M.; Gerlach, M.; Brett, J.; Ryan, J.; Kao, J.; Esposito, C.; Hegarty, H.; Hurley, W.; Clauss, M. Isolation and characterization of two binding proteins for advanced glycosylation end products from bovine lung which are present on the endothelial cell surface. J. Boil. Chem. 1992, 267, 14987–14997. [Google Scholar]
- Basta, G.; Lazzerini, G.; Massaro, M.; Simoncini, T.; Tanganelli, P.; Fu, C.; Kislinger, T.; Stern, D.M.; Schmidt, A.M.; De Caterina, R. Advanced glycation end products activate endothelium through signal-transduction receptor RAGE: A mechanism for amplification of inflammatory responses. Circulation 2002, 105, 816–822. [Google Scholar] [CrossRef] [PubMed]
- Yonekura, H.; Yamamoto, Y.; Sakurai, S.; Petrova, R.G.; Abedin, J.; Li, H.; Yasui, K.; Takeuchi, M.; Makita, Z.; Takasawa, S.; et al. Novel splice variants of the receptor for advanced glycation end-products expressed in human vascular endothelial cells and pericytes, and their putative roles in diabetes-induced vascular injury. Biochem. J. 2003, 370, 1097–1109. [Google Scholar] [CrossRef] [PubMed]
- Prasad, K.; Sarkar, A.; Zafar, M.A.; Shoker, A.; Moselhi, H.E.; Tranquilli, M.; Ziganshin, B.A.; Elefteriades, J.A. Advanced Glycation End Products and its Soluble Receptors in the Pathogenesis of Thoracic Aortic Aneurysm. Aorta (Stamford) 2016, 4, 1–10. [Google Scholar] [PubMed]
- Sarkar, A.; Prasad, K.; Ziganshin, B.A.; Elefteriades, J.A. Reasons to Investigate the Soluble Receptor for Advanced Glycation End-Product (sRAGE) Pathway in Aortic Disease. Aorta (Stamford) 2013, 1, 210–217. [Google Scholar] [CrossRef] [PubMed]
- Reichert, S.; Triebert, U.; Santos, A.N.; Hofmann, B.; Schaller, H.-G.; Schlitt, A.; Schulz, S. Soluble form of receptor for advanced glycation end products and incidence of new cardiovascular events among patients with cardiovascular disease. Atherosclerosis 2017, 266, 234–239. [Google Scholar] [CrossRef] [PubMed]
- Siwik, D.A.; Pagano, P.J.; Colucci, W.S. Oxidative stress regulates collagen synthesis and matrix metalloproteinase activity in cardiac fibroblasts. Am. J. Physiol. Physiol. 2001, 280, C53–C60. [Google Scholar] [CrossRef] [PubMed]
- Geroldi, D.; Falcone, C.; Emanuele, E. Soluble receptor for advanced glycation end products: From disease marker to potential therapeutic target. Curr. Med. Chem. 2006, 13, 1971–1978. [Google Scholar] [CrossRef] [PubMed]
- Fukami, K.; Yamagishi, S.-I.; Okuda, S. Role of AGEs-RAGE system in cardiovascular disease. Curr. Pharm. Des. 2014, 20, 2395–2402. [Google Scholar] [CrossRef] [PubMed]
- Fujita, T. AGE/RAGE Axis in the Development of Abdominal Aortic Aneurysm. Ann. Surg. 2010, 252, 203–205. [Google Scholar] [CrossRef] [PubMed]
- Nakano, K.; Wada, K.; Nomura, R.; Nemoto, H.; Inaba, H.; Kojima, A.; Naka, S.; Hokamura, K.; Mukai, T.; Nakajima, A.; et al. Characterization of aortic aneurysms in cardiovascular disease patients harboring Porphyromonas gingivalis. Oral Dis. 2010, 17, 370–378. [Google Scholar] [CrossRef] [PubMed]
- Shim, C.Y. RAGE and cardiovascular disease. Front. Biosci. 2011, 16, 486. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | Control Group (n = 43) Mean ± SD (Range) or % of Patients | Study Group (n = 32) Mean ± SD (Range) or % of Patients |
|---|---|---|
| Age (years) | 68.3 ± 6.4 (59–82) | 70.3 ± 7.3 (53–88) |
| Sex (% of male) | 93.0 | 93.7 |
| Aorta /AAA diameter (mm) | 19.9 ± 3.0 (12.9–24.2) | 60.4 ± 15.0 (39–105) |
| Underlying disease | ||
| Hypertension (%) | 60.5 | 87.5 |
| Diabetes mellitus type 2 (%) | 21.9 | 14.0 |
| Heart disease (%) | 16.3 | 28.1 |
| Tobacco smoke (%) | 18.7 | 20.2 |
| Study Group (n = 32) Mean ± SD | Control Group (n = 43) Mean ± SD | |
|---|---|---|
| Age (year) | 70.3 ± 7.26 | 68.3 ± 6.43 |
| AAA/Aorta diameter (mm) | 60.4 ± 15.03 | 19.9 ± 3.03 |
| 1st visit | ||
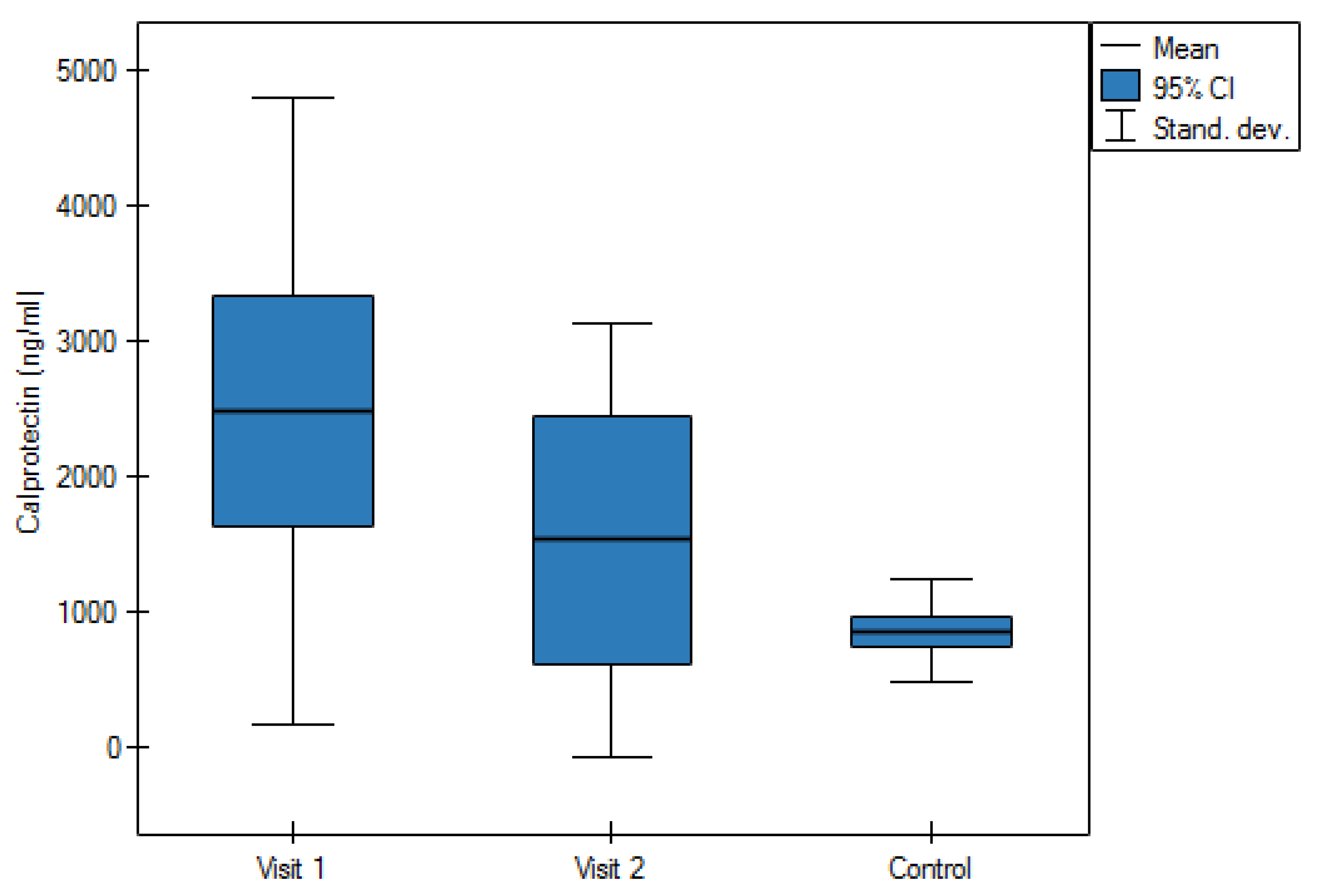
| Calprotectin (ng/mL) | 2513.5 ± 2283.2 | 861.4 ± 378.4 |
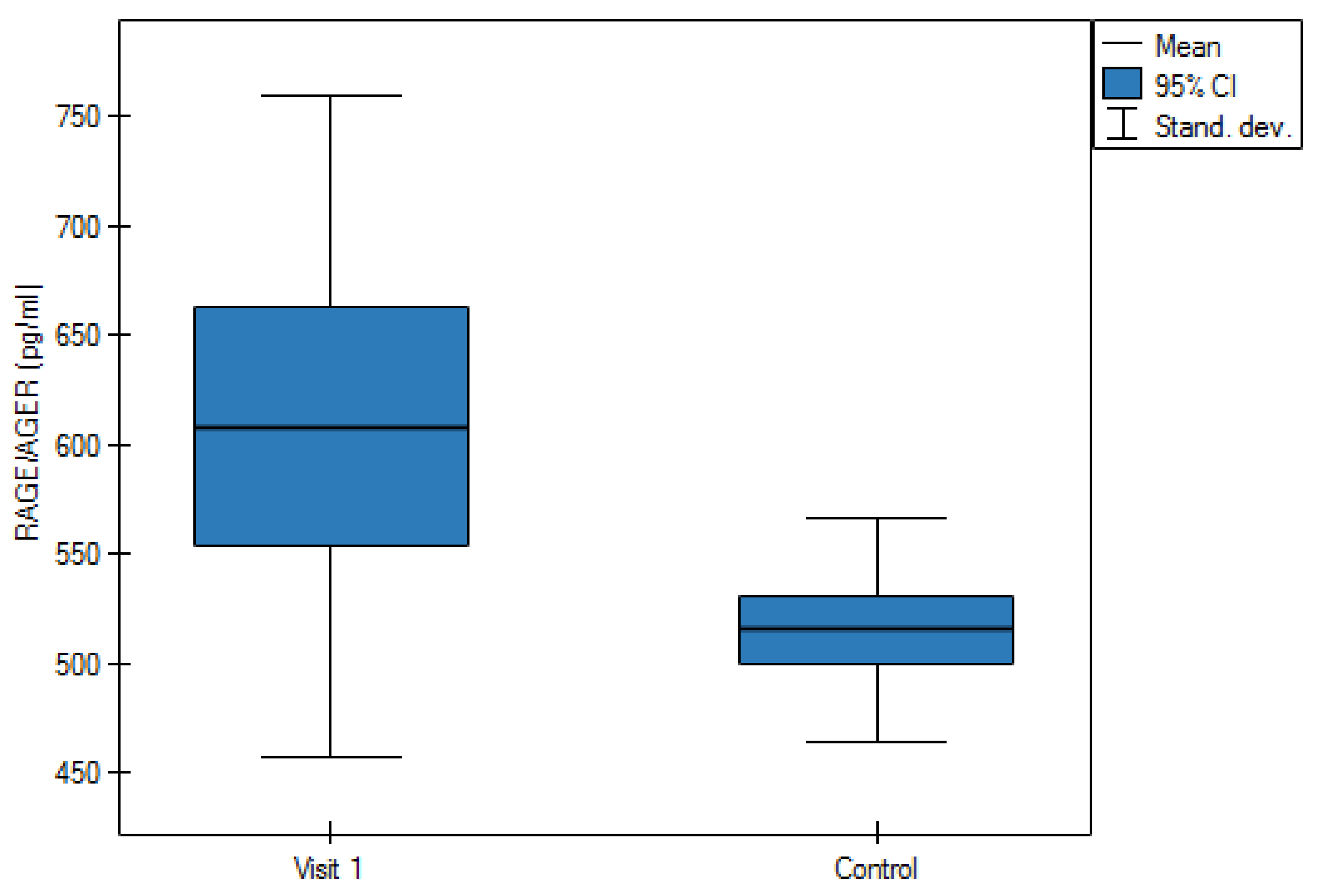
| RAGE/AGER (pg/mL) | 608.4 ± 151.3 | 515.3 ± 51.5 |
| 2nd visit (n = 14) | ||
| Calprotectin (ng/mL) | 1534.1 ± 1600.3 | _ |
| RAGE/AGER (pg/mL) | 657.4 ± 172.4 | _ |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hauzer, W.; Witkiewicz, W.; Gnus, J. Calprotectin and Receptor for Advanced Glycation End Products as a Potential Biomarker in Abdominal Aortic Aneurysm. J. Clin. Med. 2020, 9, 927. https://doi.org/10.3390/jcm9040927
Hauzer W, Witkiewicz W, Gnus J. Calprotectin and Receptor for Advanced Glycation End Products as a Potential Biomarker in Abdominal Aortic Aneurysm. Journal of Clinical Medicine. 2020; 9(4):927. https://doi.org/10.3390/jcm9040927
Chicago/Turabian StyleHauzer, Willy, Wojciech Witkiewicz, and Jan Gnus. 2020. "Calprotectin and Receptor for Advanced Glycation End Products as a Potential Biomarker in Abdominal Aortic Aneurysm" Journal of Clinical Medicine 9, no. 4: 927. https://doi.org/10.3390/jcm9040927
APA StyleHauzer, W., Witkiewicz, W., & Gnus, J. (2020). Calprotectin and Receptor for Advanced Glycation End Products as a Potential Biomarker in Abdominal Aortic Aneurysm. Journal of Clinical Medicine, 9(4), 927. https://doi.org/10.3390/jcm9040927





