Efficacy and Safety of a Novel Submucosal Injection Solution for Resection of Gastrointestinal Lesions
Abstract
1. Introduction
2. Materials and Methods
2.1. Primary Outcomes
2.2. Injection Solution
2.3. Prospective Study
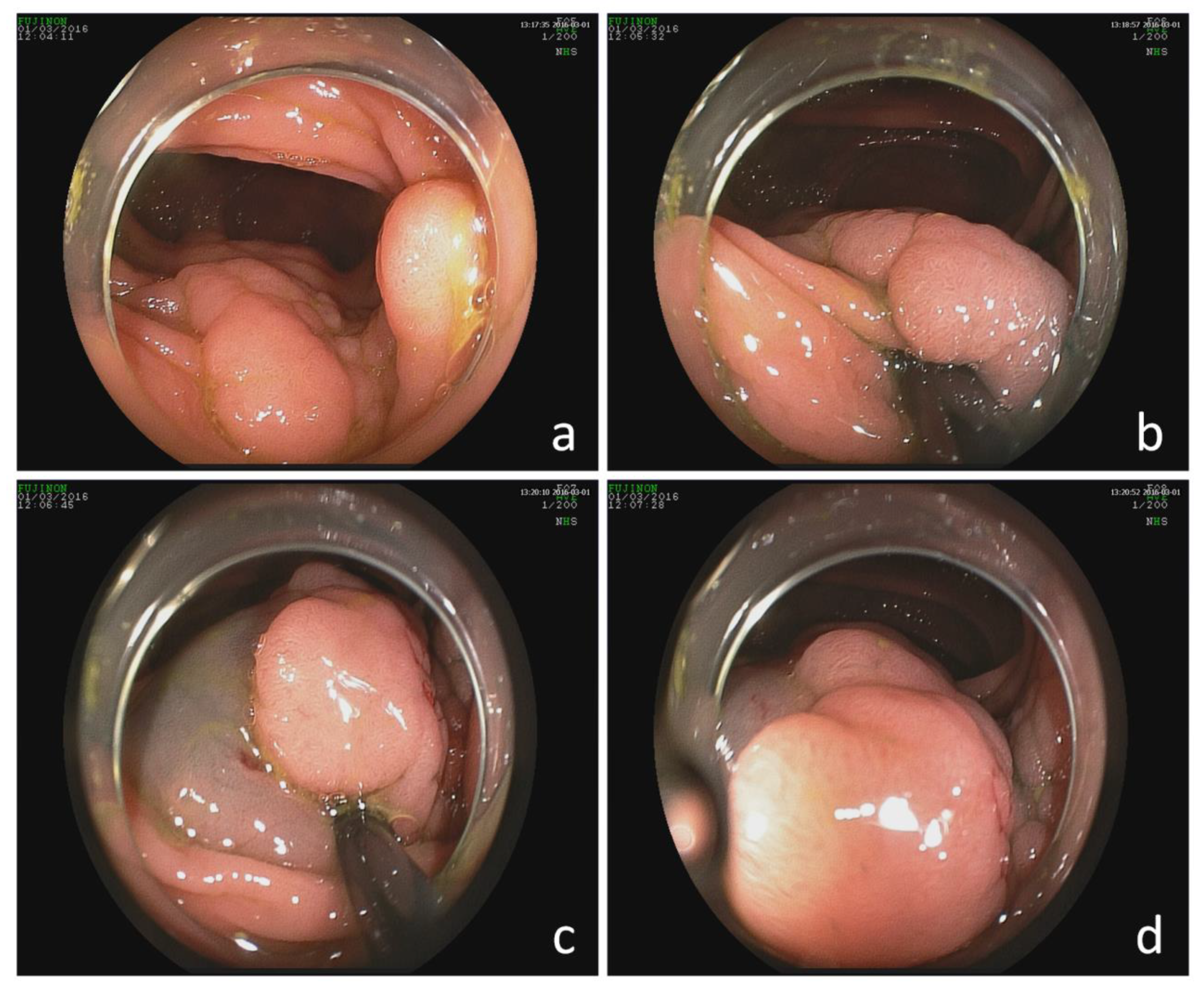
2.4. EMR/ESD Procedure
2.5. Follow-Up of Patients after EMR/ESD
2.6. Statistical Analysis
3. Results
3.1. Clinical Study: Efficacy and Safety
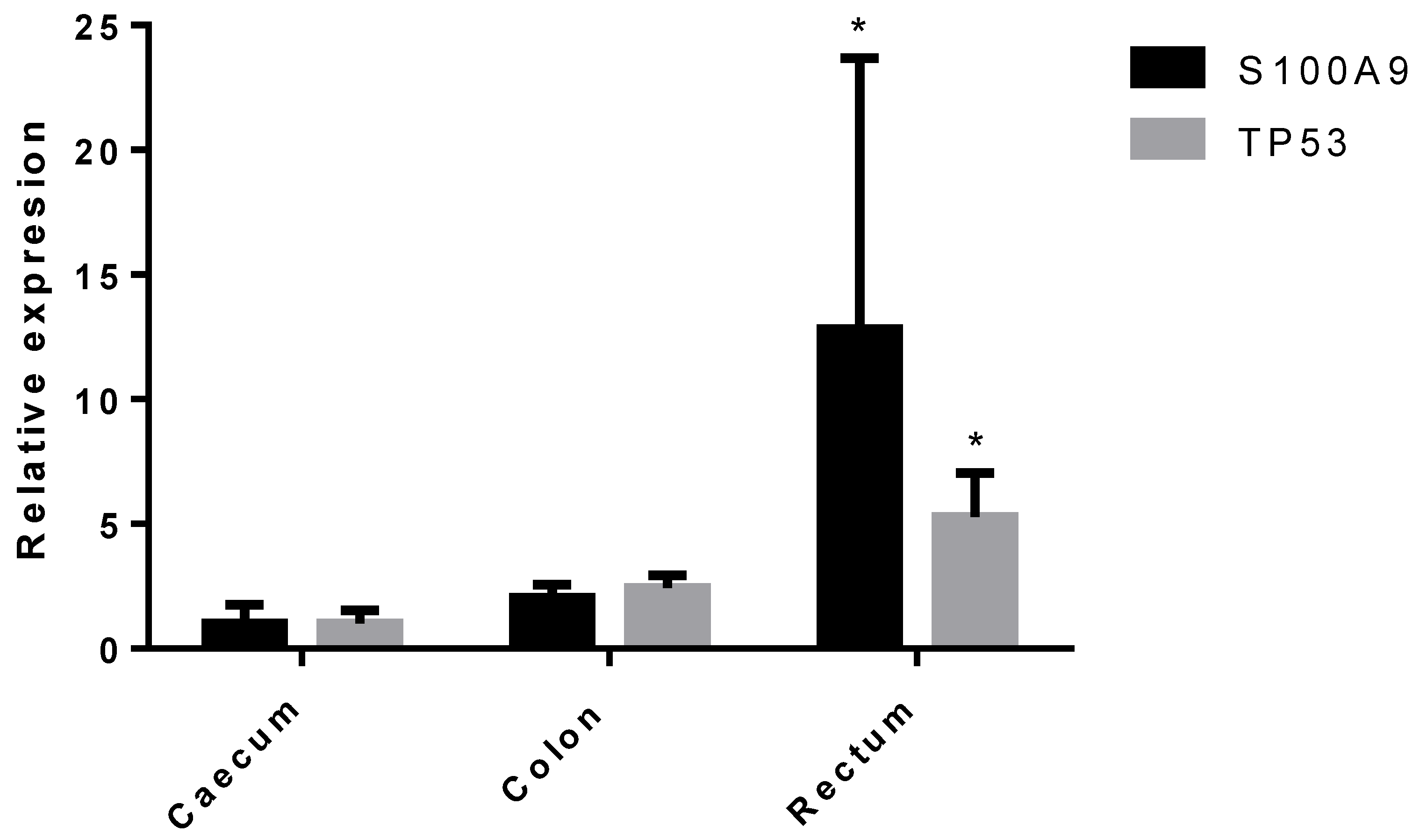
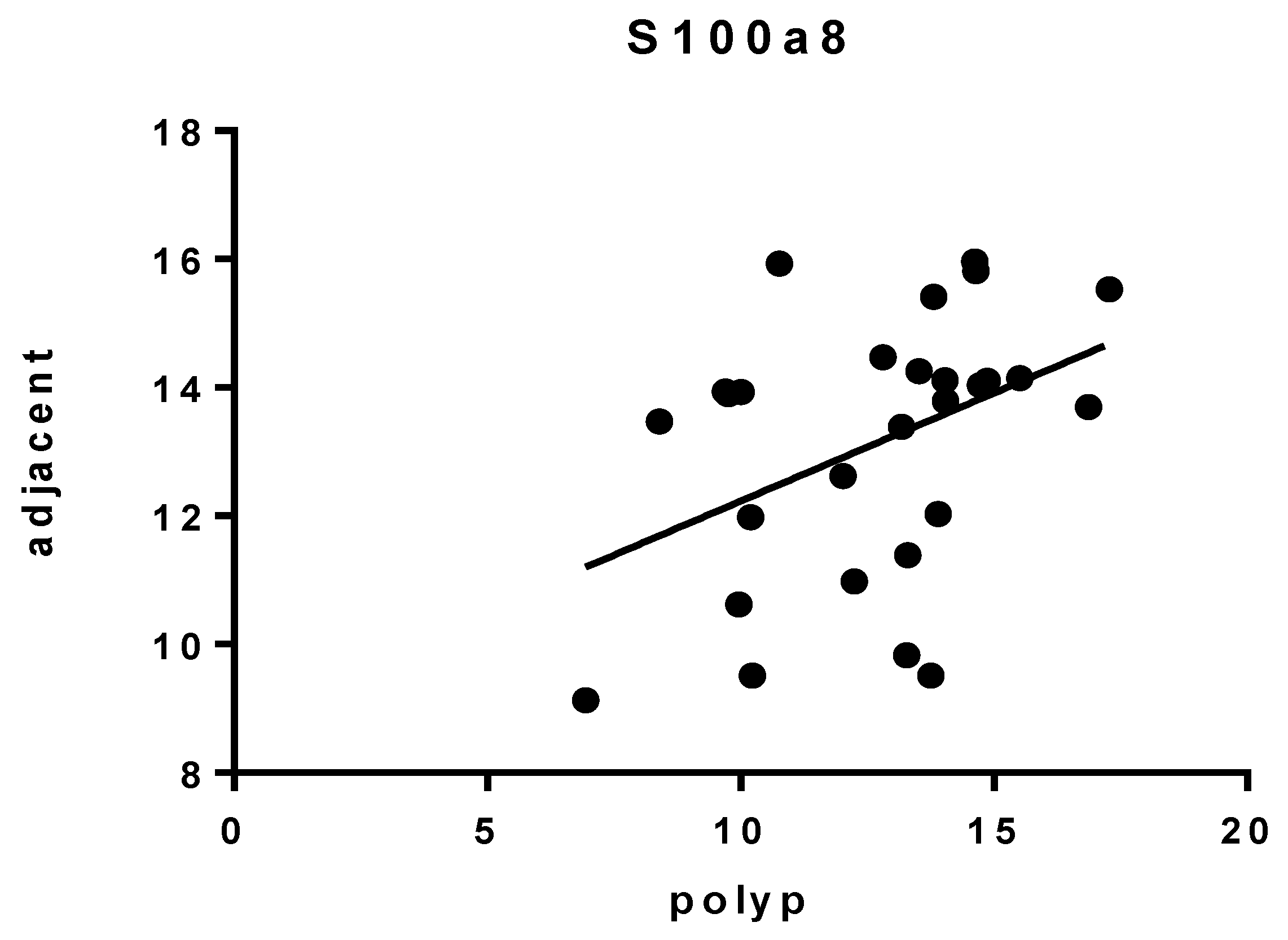
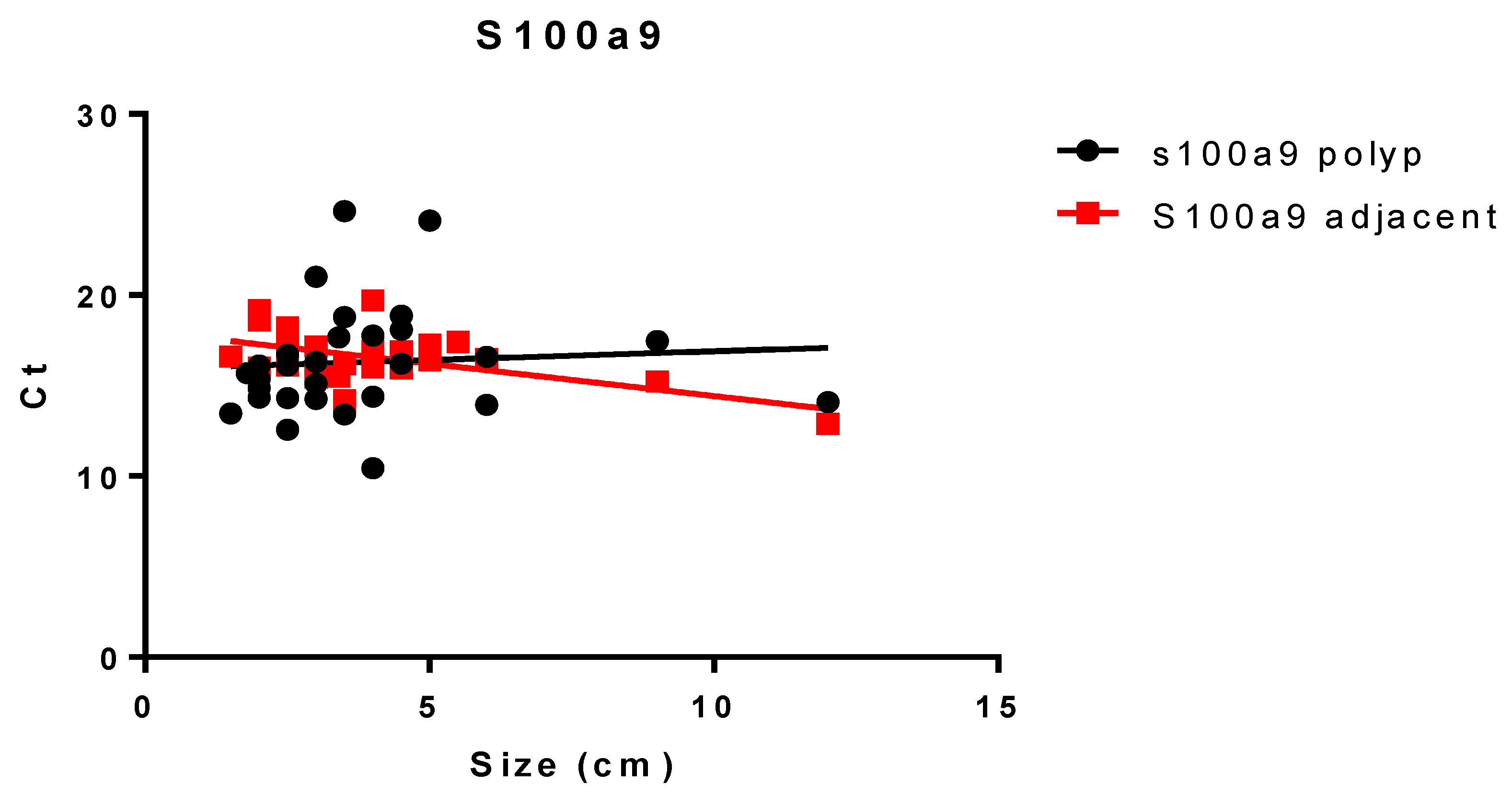
3.2. Results of the Expression of Markers by PCR
4. Discussion
5. Conclusions
6. Patents
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Kruszewski, W.J. Endoscopic methods in the treatment of early-stage esophageal cancer. Videosurg. Other Miniinvasive Tech. 2014, 9, 125–130. [Google Scholar] [CrossRef] [PubMed]
- Kantsevoy, S.V.; Adler, D.G.; Conway, J.D.; Diehl, D.L.; Farraye, F.A.; Kwon, R.; Mamula, P.; Rodríguez, S.; Shah, R.J.; Wong Kee Song, L.M.; et al. Endoscopic mucosal resection and endoscopic submucosal dissection. Gastrointest. Endosc. 2008, 68, 11–18. [Google Scholar] [CrossRef] [PubMed]
- Ono, H.; Kondo, H.; Gotoda, T.; Shirao, K.; Yamaguchi, H.; Saito, D.; Hosokawa, K.; Shimoda, T.; Yoshida, S. Endoscopic mucosal resection for treatment of early gastric cancer. Gut 2001, 2, 225–229. [Google Scholar] [CrossRef] [PubMed]
- Moss, A.; Bourke, M.J.; Williams, S.J.; Hourigan, L.F.; Brown, G.; Tam, W.; Singh, R.; Zanati, S.; Chen, R.Y.; Byth, K.; et al. Endoscopic mucosal resection outcomes and prediction of submucosal cancer from advanced colonic mucosal neoplasia. Gastroenterology 2011, 140, 1909–1918. [Google Scholar] [CrossRef]
- Park, Y.M.; Cho, E.; Kang, H.Y.; Kim, J.M. The effectiveness and safety of endoscopic submucosal dissection compared with endoscopic mucosal resection for early gastric cancer: A systematic review and metaanalysis. Surg. Endosc. 2011, 25, 2666–2677. [Google Scholar] [CrossRef]
- Lian, J.; Chen, S.; Zhang, Y.; Qiu, F. A meta-analysis of endoscopic submucosal dissection and EMR for early gastric cancer. Gastrointest. Endosc. 2012, 76, 763–770. [Google Scholar] [CrossRef]
- Cao, Y.; Liao, C.; Tan, A.; Gao, Y.; Mo, Z.; Gao, F. Meta-analysis of endoscopic submucosal dissection versus endoscopic mucosal resection for tumors of the gastrointestinal tract. Endoscopy 2009, 41, 751–757. [Google Scholar] [CrossRef]
- Uraoka, T.; Saito, Y.; Yamamoto, K.; Fujii, T. Submucosal injection solution for gastrointestinal tract endoscopic mucosal resection and endoscopic submucosal dissection. Drug Des. Dev. Ther. 2009, 2, 131–138. [Google Scholar] [CrossRef]
- Larghi, A.; Waxman, I. State of the art on endoscopic mucosal resection and endoscopic submucosal dissection. Gastrointest. Endosc. Clin. N. Am. 2007, 17, 441–469. [Google Scholar] [CrossRef]
- Yandrapu, H.; Desai, M.; Siddique, S.; Vennalganti, P.; Vennalaganti, S.; Parasa, S.; Rai, T.; Kanakadandi, V.; Bansal, A.; Titi, M.; et al. Normal saline solution versus other viscous solutions for submucosal injection during endoscopic mucosal resection: A systematic review and meta-analysis. Gastrointest. Endosc. 2017, 85, 693–699. [Google Scholar] [CrossRef]
- Ferreira, A.O.; Moleiro, J.; Torres, J.; Dinis-Ribeiro, M. Solutions for submucosal injection in endoscopic resection: A systematic review and meta-analysis. Endosc. Int. Open 2016, 4, E1–E16. [Google Scholar] [CrossRef] [PubMed]
- Moss, A.; Bourke, M.J.; Kwan, V.; Tran, K.; Godfrey, C.; McKay, G.; Hopper, A.D. Succinylated gelatin substantially increases en bloc resection size in colonic EMR: A randomized, blinded trial in a porcine model. Gastrointest. Endosc. 2010, 71, 589–595. [Google Scholar] [CrossRef] [PubMed]
- Polymeros, D.; Kotsalidis, G.; Triantafyllou, K.; Karamanolis, G.; Panagiotides, J.G.; Ladas, S.D. Comparative performance of novel solutions for submucosal injection in porcine stomachs: An ex vivo study. Dig. Liver. Dis. 2010, 42, 226–229. [Google Scholar] [CrossRef] [PubMed]
- Fujishiro, M.; Yahagi, N.; Kashimura, K.; Matsuura, T.; Nakamura, M.; Kakushima, N.; Kodashima, S.; Ono, S.; Kobayashi, K.; Hashimoto, T.; et al. Tissue damage of different submucosal injection solutions for EMR. Gastrointest. Endosc. 2005, 62, 933–942. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Park, J.-H.; Park, D.H.; Chung, I.K.; Kim, H.S.; Park, S.H.; Kim, S.J.; Cho, H.D. Clinical efficacy of EMR with submucosal injection of a fibrinogen mixture: A prospective randomized trial. Gastrointest. Endosc. 2006, 64, 691–696. [Google Scholar] [CrossRef] [PubMed]
- Matsui, Y.; Inomata, M.; Izumi, K.; Sonoda, K.; Shiraishi, N.; Kitano, S. Hyaluronic acid stimulates tumor-cell proliferation at wound sites. Gastrointest. Endosc. 2004, 60, 539–543. [Google Scholar] [CrossRef]
- Hyun, J.J.; Chun, H.R.; Chun, H.J.; Jeen, Y.T.; Baeck, C.W.; Yu, S.K.; Kim, Y.S.; Lee, H.S.; Um, S.H.; Lee, S.W.; et al. Comparison of the characteristics of submucosal injection solutions used in endoscopic mucosal resection. Scand. J. Gastroenterol. 2006, 41, 488–492. [Google Scholar] [CrossRef]
- Giday, S.A.; Magno, P.; Buscaglia, J.M.; Canto, M.I.; Ko, C.W.; Shin, E.J.; Xia, L.; Wroblewski, L.M.; Clarke, J.O.; Kalloo, A.N.; et al. Is blood the ideal submucosal cushioning agent? A comparative study in a porcine model. Endoscopy 2006, 38, 1230–1234. [Google Scholar] [CrossRef]
- Yeh, R.W.; Triadafilopoulos, G. Submucosal injection: Safety cushion at what cost? Gastrointest. Endosc. 2005, 62, 943–945. [Google Scholar] [CrossRef]
- Participants in the Paris Workshop. The Paris endoscopic classification of superficial neoplastic lesions: Esophagus, stomach, and colon November 30 to December 1 2002. Gastrointest. Endosc. 2003, 58, S3–S43. [Google Scholar] [CrossRef]
- Kudo, S.; Tamura, S.; Nakajima, T.; Yamano, H.; Kusaka, H.; Watanabe, H. Diagnosis of colorectal tumors lesions by magnifying endoscopy. Gastrointest. Endosc. 1996, 44, 8–14. [Google Scholar] [CrossRef]
- Suk Jung, Y.; Il Park, D. Submucosal injection solutions for endoscopic mucosal resection and endoscopic submucosal dissection of gastrointestinal neoplasms. Gastrointest. Interv. 2013, 2, 73–77. [Google Scholar] [CrossRef]
- Girotra, M.; Triadafilopoulos, G.; Friedland, S. Utility and performance characteristics of a novel submucosal injection agent (EleviewTM) for endoscopic mucosal resection an endoscopic submucosal dissection. Transl. Gastroenterol. Hepatol. 2018, 3, 32. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, N.; Naito, Y.; Kugai, M.; Inoue, K.; Uchiyama, K.; Takagi, T.; Ishikawa, T.; Handa, O.; Konishi, H.; Wakabayashi, N.; et al. Efficacy of hyaluronic acid in endoscopic mucosal resection of colorectal tumors. J. Gastroenterol. Hepatol. 2011, 26, 286–291. [Google Scholar] [CrossRef] [PubMed]
- Varadarajulu, S.; Tamhane, A.; Slaughter, R.L. Evaluation of dextrose 50% as a medium for injection-assisted polypectomy. Endoscopy 2006, 38, 907–912. [Google Scholar] [CrossRef] [PubMed]
- Spadaccini, M.; Hassan, C.; Maselli, R.; D’Amico, F.; Lamonaca, L.; Craviotto, V.; Repici, A. Efficacy and safety of SIC-8000 (Eleview®) for submucosal injection for endoscopic mucosal resection and endoscopic submucosal dissection in an in vivo porcine. Dig. Liver Dis. 2018, 50, 260–266. [Google Scholar] [CrossRef]
- Duan, L.; Wu, R.; Ye, L.; Wang, H.; Yang, X.; Zhang, Y. S100A8 and S100A9 Are Associated with Colorectal Carcinoma Progression and Contribute to Colorectal Carcinoma Cell Survival and Migration via Wnt/β-Catenin Pathway. PLoS ONE 2013, 8, e62092. [Google Scholar] [CrossRef]
- Rubio, C.A.; Rodesjö, M.; Duvander, A.; Mathies, M.; Garberg, L.; Shetye, J. p53 Up-regulation During Colorectal Carcinogenesis. Anticancer Res. 2014, 34, 6973–6979. [Google Scholar]
- Sousa, W.A.; Rodrigues, L.V.; Silva, R.G., Jr.; Vieira, F.L. Immunohistochemical evaluation of p53 and Ki-67 proteins in colorectal adenomas. Arq. Gastroenterol. 2012, 49, 35–40. [Google Scholar] [CrossRef][Green Version]
- Sikorska, A.; Flisikowska, T.; Stachowiak, M.; Kind, A.; Schnieke, A.; Flisikowski, K.; Switonski, M. Elevated expression of p53 in early colon polyps in a pig model of human familial adenomatous polyposis. J. Appl. Genet. 2018, 59, 485–491. [Google Scholar] [CrossRef]

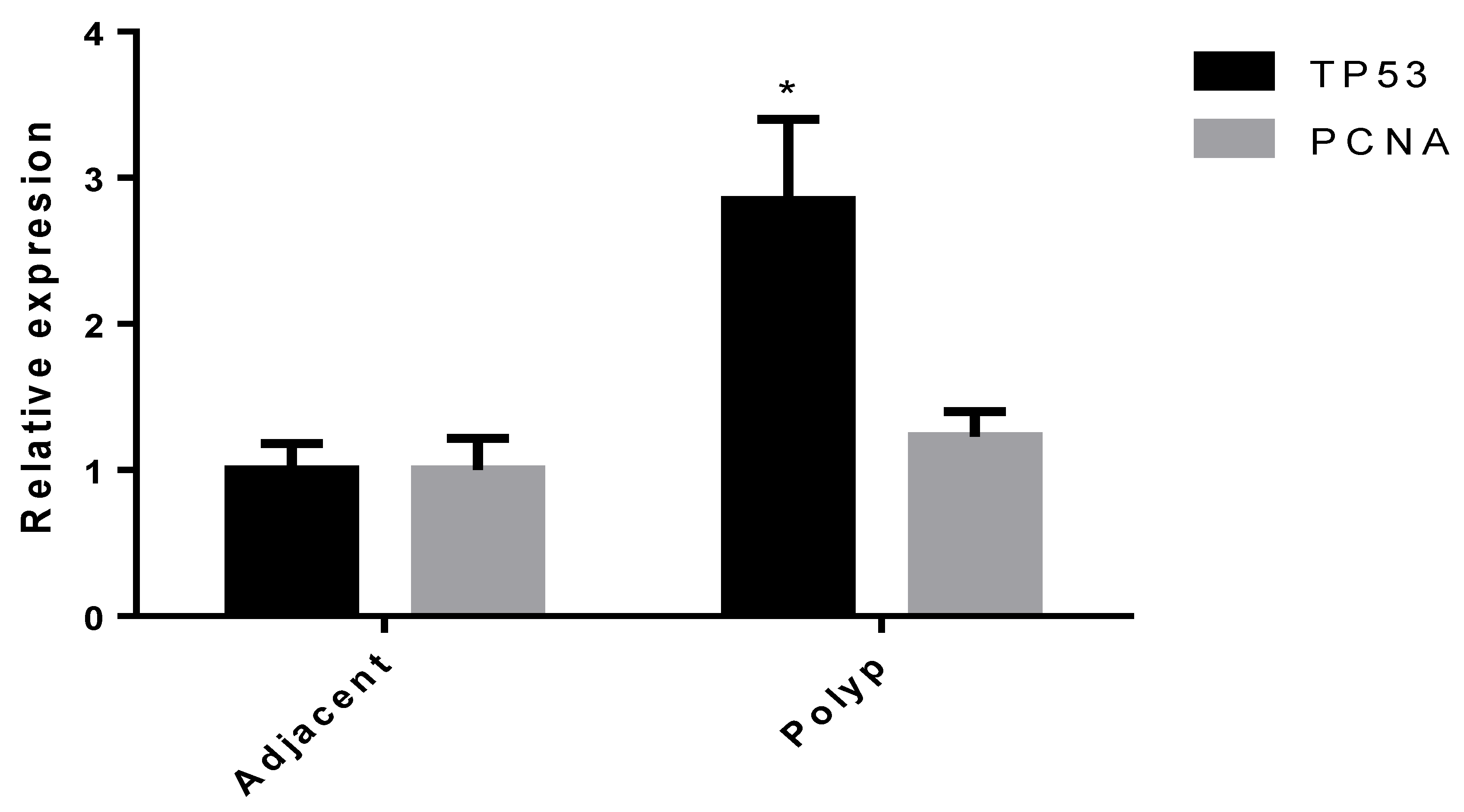
| EMR | ESD | |
| Patients | 72.2% men (13/18) | 77.8% men (14/18) |
| Age (years) | 69.2 (range: 37–86) | 66.0 (range: 36–85) |
| Previous polypectomy | 0.33 (range: 0–2) | 0.75 (range: 0–5) |
| Lesion site (%) | 77.8% in colon (14/18) | 66.7% in colon (12/18) |
| Comorbidities | ||
| Dyslipemia (%) | 48.5 | 64.7 |
| Cardiovascular Pathology (%) | 34.2 | 17.7 |
| Hypertension (%) | 69.9 | 70.6 |
| Diabetes mellitus (%) | 50.0 | 41.2 |
| Chronic obstructive pulmonary disease (%) | 21.4 | 17.6 |
| Smoker (%) | 50.0 | 45.4 |
| Enolism (%) | 42.9 | 12.5 |
| Hemorrhoids (%) | 70.0 | 76.5 |
| Background other type of cancer (%) / family history of CCR (%) | 21.4 | 66.7 |
| Patient Code | Lesions (n) | Paris Classification | Size of Lesion (cm) |
|---|---|---|---|
| 2 | 2 | 0-IIa/0-IIc/IIa | 2.2/1.2 |
| 3 | 1 | 0-Is/IIa | 3.5 |
| 4 | 1 | 0-IIa | 2 |
| 5 | 1 | 0-Is | 4 |
| 6 | 1 | 0-Is | 5 |
| 7 | 1 | 0-IIa | 1.5 |
| 8 | 2 | 0-IIa/0-IIb | 2/2.5 |
| 9 | 1 | 0-Is/IIa | 3.5 |
| 10 | 2 | 0-IIa/0-Is | 1/2.5 |
| 11 | 1 | 0-Is | 4 |
| 12 | 1 | 0-IIa | 2.2 |
| 13 | 1 | 0-IIa | 2.4 |
| 14 | 1 | 0-IIs | 2.5 |
| 15 | 1 | 0-IIa | 1.5 |
| 16 | 1 | 0-IIb | 2.5 |
| 17 | 1 | 0-IIa | 2.4 |
| 18 | 2 | 0-Is/0-IIa | 4/1.5 |
| 19 | 1 | 0-Is | 4 |
| 20 | 1 | 0-Is | 12 |
| 21 | 1 | 0-Is | 3 |
| 22 | 1 | 0-IIc/IIa | 1.8 |
| 23 | 1 | 0-IIb | 4.5 |
| 24 | 1 | 0-Is | 6 |
| 25 | 1 | 0-IIa | 2 |
| 26 | 1 | 0-IIa | 3 |
| 27 | 1 | 0-Is/IIa | 9 |
| 28 | 1 | IIa+IIb | 3 |
| 29 | 1 | 0-IIa | 4.5 |
| 30 | 1 | 0-IIc/IIa | 2 |
| 31 | 1 | 0-Is/IIa | 3 |
| 32 | 1 | 0-IIa | 2 |
| 33 | 1 | 0-Is/IIa | 6 |
| 35 | 1 | 0-IIa | 2 |
| 36 | 1 | 0-Is/IIa | 4.5 |
| 38 | 1 | 0-Is | 3 |
| 39 | 1 | 0-Is | 3.5 |
| Resection Technique Data | EMR | ESD |
| Malignancy of tissue (%) | 27.8 (5/18) | 23.5 (4/17) |
| Excised polyps (n) | 2.9 (range: 1.5–4) | 3.6 (range: 2–9) |
| Resections for complete removal of lesions (n) | 5.5 (range: 4–10) | 2.1 (range: 1–6) |
| Solution injections / polyp (n) | 3.3 (range: 1–6) | 4.1 (range: 1–10) |
| Polyps re-injected (n) | 3 | 2 |
| Injected volume (mL) | 30.7 (range: 7–50) | 41.1 (range: 20–110) |
| Polyp lift (min) | 63.9 (range: 45–90) | 77.4 (range: 40–90) a |
| Intervention time (min) | 75.8 (range: 40–120) | 121.8 (range: 45–420) |
| Polyp lift/intervention time ratio | 0.84 | 0.64 |
| b Time to resorption/intervention time ratio | 1 | 1 |
| Complications | ||
| Bleeding during intervention | 100% | 100% |
| Type of bleeding | ||
| Severe bleeding (%) | 0 | 6.7 |
| Moderate bleeding (%) | 6.7 | 13.4 |
| Mild bleeding (%) | 92.4 | 79.9 |
| Others (%) | 0 | 0 |
| Adverse effects due to the submucosal injection solution | 0 | 0 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moles-Aranda, C.; González-Pérez, R.; Gallego-Rojo, F.J.; Martínez-Augustin, O.; Clares-Naveros, B.; Sánchez de Medina, F.; Morales-Molina, J.A. Efficacy and Safety of a Novel Submucosal Injection Solution for Resection of Gastrointestinal Lesions. J. Clin. Med. 2020, 9, 1162. https://doi.org/10.3390/jcm9041162
Moles-Aranda C, González-Pérez R, Gallego-Rojo FJ, Martínez-Augustin O, Clares-Naveros B, Sánchez de Medina F, Morales-Molina JA. Efficacy and Safety of a Novel Submucosal Injection Solution for Resection of Gastrointestinal Lesions. Journal of Clinical Medicine. 2020; 9(4):1162. https://doi.org/10.3390/jcm9041162
Chicago/Turabian StyleMoles-Aranda, Cristina, Raquel González-Pérez, Francisco Javier Gallego-Rojo, Olga Martínez-Augustin, Beatriz Clares-Naveros, Fermín Sánchez de Medina, and José Antonio Morales-Molina. 2020. "Efficacy and Safety of a Novel Submucosal Injection Solution for Resection of Gastrointestinal Lesions" Journal of Clinical Medicine 9, no. 4: 1162. https://doi.org/10.3390/jcm9041162
APA StyleMoles-Aranda, C., González-Pérez, R., Gallego-Rojo, F. J., Martínez-Augustin, O., Clares-Naveros, B., Sánchez de Medina, F., & Morales-Molina, J. A. (2020). Efficacy and Safety of a Novel Submucosal Injection Solution for Resection of Gastrointestinal Lesions. Journal of Clinical Medicine, 9(4), 1162. https://doi.org/10.3390/jcm9041162






