Low Intracellular Water, Overhydration, and Mortality in Hemodialysis Patients
Abstract
1. Introduction
2. Patients and Methods
2.1. Patients
2.2. Biochemistry
2.3. Body Composition, Fluid Volume Parameters, and Nutritional Status
2.4. Statistical Analyses
3. Results
3.1. Patient Characteristics
3.2. Baseline Post-Dialysis Body Composition Parameters
| Variables | Mean ± SD% (n) or Median (IQR) | Variables | Mean ± SD% (n) or Median (IQR) |
|---|---|---|---|
| Age (years) | 64 ± 13 | Serum C Reactive Protein (mg/dL) | 1.3 ± 0.6 |
| Women (% n) | 45 (49) | Serum albumin (g/dL) | 3.8 ± 0.4 |
| Diabetes (% n) | 21 (23) | nPCR (g/kg/day) | 0.7 ± 0.3 |
| Vintage (months) | 59 ± 79 | Plasma BNP (pg/mL) | 6090 (2407–14900) |
| Cardiovascular disease (% n) | 40 (44) | Plasma total CO2 (mmol/L) | 20 ± 3 |
| Predialytic systolic blood pressure | 132 ± 24 | Total Body Water (L) | 32.8 ± 6.8 |
| Predialytic diastolic blood pressure | 67 ± 14 | Extracellular Water (ECW) (L) | 14.4 ± 2.6 |
| Protein Energy Wasting (% n) | 44 (41%) | Intracellular Water (ICW) (L) | 18.5 ± 4.5 |
| kTv | 1.42 ± 0.18 | ECW/ICW | 0.79 ± 0.13 |
| Hemoglobin (g/dL) | 11.6 ± 1.4 | Lean Tissue Mass (kg) | 58 ± 16 |
| Plasma iPTH (pg/mL) | 250 (127–454) | Adipose Tissue Mass (kg) | 30 ± 11 |
| Serum calcium (mg/dL) | 8.8 ± 0.8 | Overhydration (L) | −0.70 ± 1.67 |
| Serum phosphate (mg/dL) | 4.8 ± 1.3 | Interdialytic weigh gain (Kg) | 2.6 ± 0.8 kg |
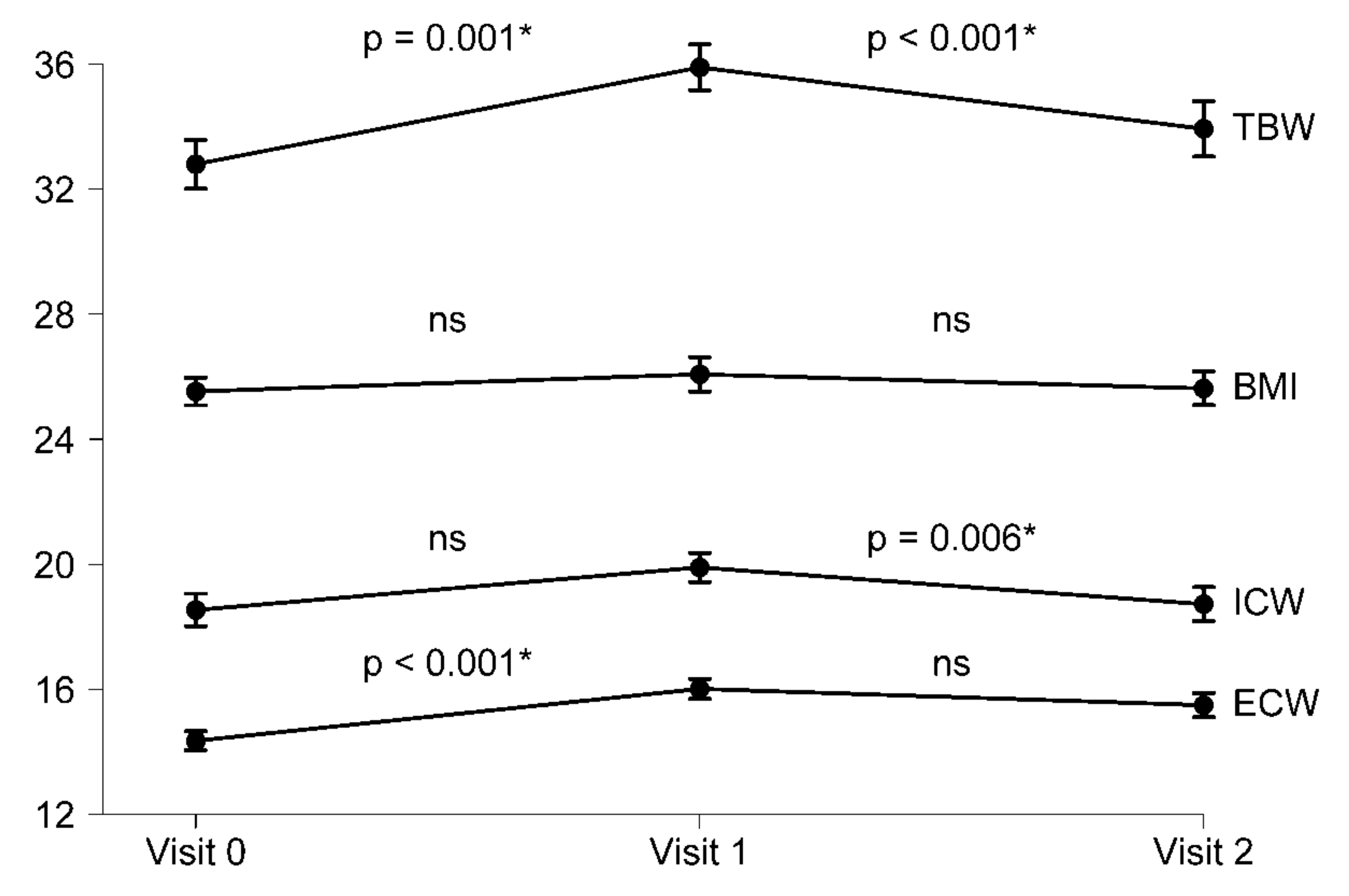
3.3. Changes in Body Composition Over Time
3.4. Variables Associated with Low Post-Dialysis ICW
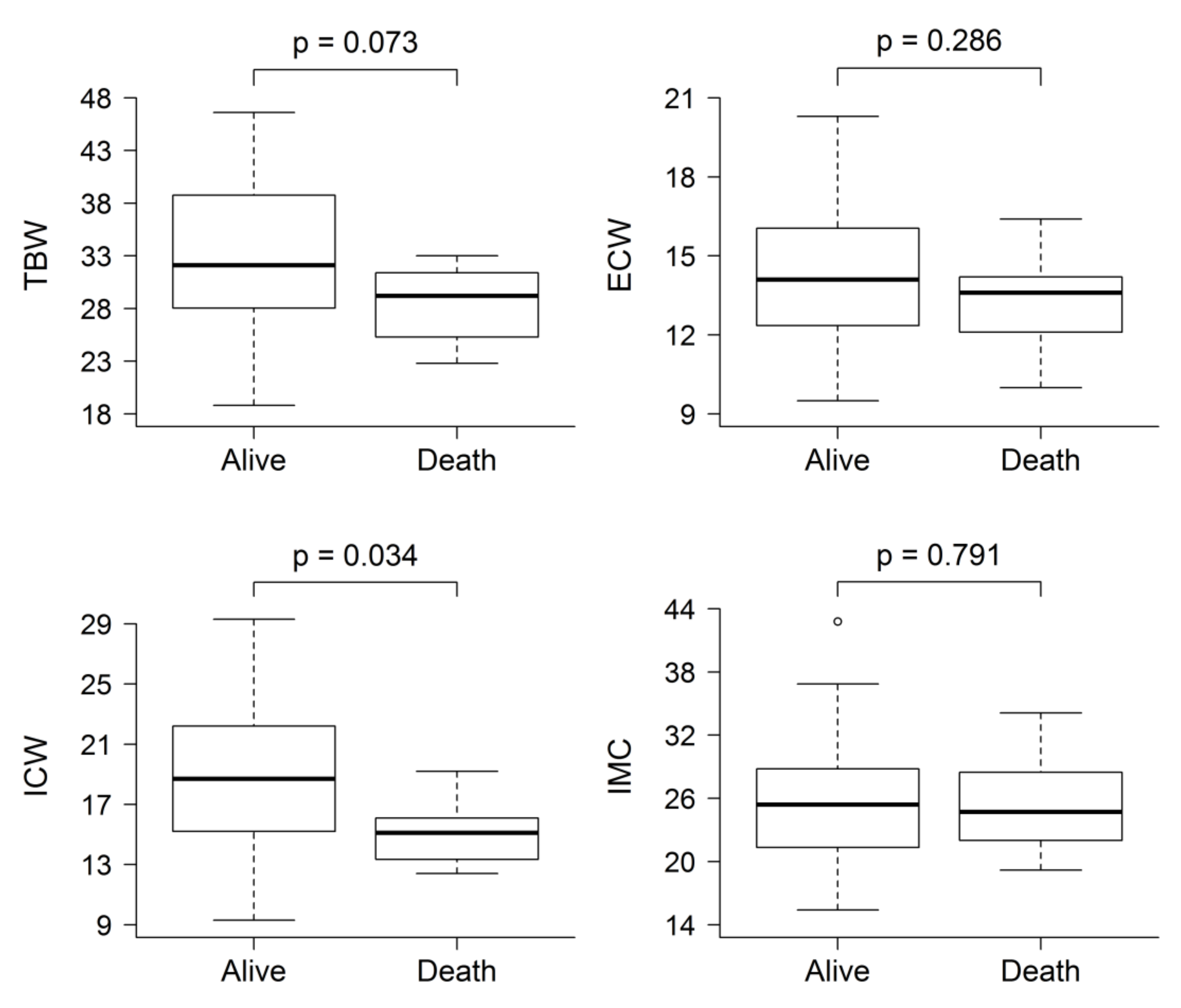
3.5. Overhydration and Mortality: Low ICW as an Independent Risk Factor
4. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Zoccali, C.; Moissl, U.; Chazot, C.; Mallamaci, F.; Tripepi, G.; Arkossy, O.; Wabel, P.; Stuard, S. Chronic Fluid Overload and Mortality in ESRD. J. Am. Soc. Nephrol. 2017, 28, 2491–2497. [Google Scholar] [CrossRef]
- Dekker, M.J.; Kooman, J.P. Fluid status assessment in hemodialysis patients and the association with outcome. Curr. Opin. Nephrol. Hypertens. 2018, 27, 188–193. [Google Scholar] [CrossRef]
- Onofriescu, M.; Siriopol, D.; Voroneanu, L.; Hogas, S.; Nistor, I.; Apetrii, M.; Florea, L.; Veisa, G.; Mititiuc, I.; Kanbay, M.; et al. Overhydration, Cardiac Function and Survival in Hemodialysis Patients. PLoS ONE 2015, 10, e0135691. [Google Scholar] [CrossRef]
- Chamney, P.W.; Wabel, P.; Moissl, U.M.; Müller, M.J.; Bosy-Westphal, A.; Korth, O.; Fuller, N.J. A whole-body model to distinguish excess fluid from the hydration of major body tissues. Am. J. Clin. Nutr. 2007, 85, 80–89. [Google Scholar] [CrossRef]
- Van Der Sande, F.M.; Van De Wal-Visscher, E.R.; Stuard, S.; Moissl, U.; Kooman, J.P. Using Bioimpedance Spectroscopy to Assess Volume Status in Dialysis Patients. Blood Purif. 2019, 49, 178–184. [Google Scholar] [CrossRef] [PubMed]
- Hassan, K.; Hassan, D.; Shturman, A.; Rubinchik, I.; Fadi, H.; Shadi, H.; Atar, S. The impact of sub-clinical over-hydration on left ventricular mass in peritoneal dialysis patients. Int. J. Clin. Exp. Med. 2015, 8, 5890–5896. [Google Scholar] [PubMed]
- Hung, S.-C.; Kuo, K.-L.; Peng, C.-H.; Wu, C.-H.; Lien, Y.-C.; Wang, Y.-C.; Tarng, D.-C. Volume overload correlates with cardiovascular risk factors in patients with chronic kidney disease. Kidney Int. 2014, 85, 703–709. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.-C.; Tsai, Y.-C.; Wu, P.-Y.; Lee, J.-J.; Chen, S.-C.; Chiu, Y.-W.; Hsu, Y.-L.; Chang, J.-M.; Chen, H.-C. Independent Association of Overhydration with All-Cause and Cardiovascular Mortality Adjusted for Global Left Ventricular Longitudinal Systolic Strain and E/E’ Ratio in Maintenance Hemodialysis Patients. Kidney Blood Press. Res. 2018, 43, 1322–1332. [Google Scholar] [CrossRef] [PubMed]
- Tsai, Y.-C.; Tsai, H.-J.; Lee, C.-S.; Chiu, Y.-W.; Kuo, H.-T.; Lee, S.-C.; Chen, T.-H.; Kuo, M.-C. The interaction between N-terminal pro-brain natriuretic peptide and fluid status in adverse clinical outcomes of late stages of chronic kidney disease. PLoS ONE 2018, 13, e0202733. [Google Scholar] [CrossRef]
- Dekker, M.J.; Marcelli, D.; Canaud, B.J.; Carioni, P.; Wang, Y.; Grassmann, A.; Konings, C.J.; Kotanko, P.; Leunissen, K.M.; Levin, N.W.; et al. Impact of fluid status and inflammation and their interaction on survival: A study in an international hemodialysis patient cohort. Kidney Int. 2017, 91, 1214–1223. [Google Scholar] [CrossRef]
- Kalantar-Zadeh, K.; Regidor, D.L.; Kovesdy, C.P.; Van Wyck, D.; Bunnapradist, S.; Horwich, T.B.; Fonarow, G.C. Fluid Retention Is Associated With Cardiovascular Mortality in Patients Undergoing Long-Term Hemodialysis. Circulation 2009, 119, 671–679. [Google Scholar] [CrossRef] [PubMed]
- Gracia-Iguacel, C.; González-Parra, E.; Perez-Gomez, M.V.; Mahíllo-Fernández, I.; Egido, J.; Ortiz, A.; Carrero, J.J. Prevalence of protein-energy wasting syndrome and its association with mortality in haemodialysis patients in a centre in Spain. Nefrologia 2013, 33, 495–505. [Google Scholar] [PubMed]
- Jindal, K.K.; Goldstein, M.B. Urea Kinetic Modelling in Chronic Hemodialysis: Benefits, Problems, and Practical Solutions. Semin. Dial. 2007, 1, 82–85. [Google Scholar] [CrossRef]
- K/DOQI, National Kidney Foundation. Clinical practice guidelines for nutrition in chronic renal failure. Am. J. Kidney Dis. 2000, 35 (Suppl. 2), S1–S140. [Google Scholar]
- Machek, P.; Jirka, T.; Moissl, U.; Chamney, P.; Wabel, P. Guided optimization of fluid status in haemodialysis patients. Nephrol. Dial. Transplant. 2009, 25, 538–544. [Google Scholar] [CrossRef]
- Fouque, D.; Kalantarzadeh, K.; Kopple, J.D.; Cano, N.; Chauveau, P.; Cuppari, L.; A Franch, H.; Guarnieri, G.L.; Ikizler, T.; A Kaysen, G.; et al. A proposed nomenclature and diagnostic criteria for protein–energy wasting in acute and chronic kidney disease. Kidney Int. 2008, 73, 391–398. [Google Scholar] [CrossRef]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Wabel, P.; Chamney, P.; Moissl, U.; Jirka, T. Importance of Whole-Body Bioimpedance Spectroscopy for the Management of Fluid Balance. Blood Purif. 2009, 27, 75–80. [Google Scholar] [CrossRef]
- Rymarz, A.; Gibińska, J.; Zajbt, M.; Piechota, W.; Niemczyk, S. Low lean tissue mass can be a predictor of one-year survival in hemodialysis patients. Ren. Fail. 2018, 40, 231–237. [Google Scholar] [CrossRef]
- Gracia-Iguacel, C.; González-Parra, E.; Mahillo, I.; Ortiz, A. Criteria for classification of protein-energy wasting in dialysis patients: Impact on prevalence. Br. J. Nutr. 2019, 121, 1271–1278. [Google Scholar] [CrossRef]
- Johansen, K.L.; Dalrymple, L.S.; Delgado, C.; Kaysen, G.A.; Kornak, J.; Grimes, B.; Chertow, G.M. Association between Body Composition and Frailty among Prevalent Hemodialysis Patients: A US Renal Data System Special Study. J. Am. Soc. Nephrol. 2013, 25, 381–389. [Google Scholar] [CrossRef] [PubMed]
- Earthman, C.; Traughber, D.; Dobratz, J.; Howell, W. Bioimpedance spectroscopy for clinical assessment of fluid distribution and body cell mass. Nutr. Clin. Pract. 2007, 22, 389–405. [Google Scholar] [CrossRef]
- Dicker, S.E. Changes in the extracellular- and intracellular-fluid phases of tissues during water diuresis in normal and hypoproteinaemic rats. Biochem. J. 1948, 43, 453–461. [Google Scholar] [CrossRef]
- Patrick, J.; Reeds, P.J.; Jackson, A.A.; Seakins, A.; Picou, D.I.M. Total body water in malnutrition: The possible role of energy intake. Br. J. Nutr. 1978, 39, 417–424. [Google Scholar] [CrossRef]
- Hecking, M.; Moissl, U.; Genser, B.; Rayner, H.; Dasgupta, I.; Stuard, S.; Stopper, A.; Chazot, C.; Maddux, F.W.; Canaud, B.; et al. Greater fluid overload and lower interdialytic weight gain are independently associated with mortality in a large international hemodialysis population. Nephrol. Dial. Transplant. 2018, 33, 1832–1842. [Google Scholar] [CrossRef]
- Kim, E.-J.; Choi, M.-J.; Lee, J.-H.; Oh, J.-E.; Seo, J.-W.; Lee, Y.-K.; Yoon, J.-W.; Kim, H.-J.; Noh, J.-W.; Koo, J.-R. Extracellular Fluid/Intracellular Fluid Volume Ratio as a Novel Risk Indicator for All-Cause Mortality and Cardiovascular Disease in Hemodialysis Patients. PLoS ONE 2017, 12, e0170272. [Google Scholar] [CrossRef]
- Tabinor, M.; Elphick, E.; Dudson, M.; Kwok, C.S.; Lambie, M.; Davies, S.J. Bioimpedance-defined overhydration predicts survival in end stage kidney failure (ESKF): Systematic review and subgroup meta-analysis. Sci. Rep. 2018, 8, 4441. [Google Scholar] [CrossRef]
- Ravel, V.A.; Molnar, M.Z.; Streja, E.; Kim, J.C.; Victoroff, A.; Jing, J.; Benner, D.; Norris, K.C.; Kovesdy, C.P.; Kopple, J.D.; et al. Low protein nitrogen appearance as a surrogate of low dietary protein intake is associated with higher all-cause mortality in maintenance hemodialysis patients. J. Nutr. 2013, 143, 1084–1092. [Google Scholar] [CrossRef]
- Lee, B.T.; Ahmed, F.A.; Hamm, L.L.; Teran, F.J.; Chen, C.S.; Liu, Y.; Shah, K.; Rifai, N.; Batuman, V.; Simon, E.E.; et al. Association of C-reactive protein, tumor necrosis factor-alpha, and interleukin-6 with chronic kidney disease. BMC Nephrol. 2015, 16, 77. [Google Scholar] [CrossRef]

| Variable | r | p |
|---|---|---|
| Serum creatinine (mg/dL) | 0.32 | 0.004 |
| Mid upper arm muscle circumference (MUAMC) | 0.41 | <0.0001 |
| The normalized protein catabolic rate (nPCR) | 0.42 | <0.0001 |
| 25 OH vitamin D | 0.39 | 0.001 |
| Interdialytic weight gain (IDWG) | 0.46 | <0.0001 |
| Lean tissue mass (LTM) | 0.56 | <0.0001 |
| Lean tissue index (LTI) | 0.86 | <0.0001 |
| Age | −0.30 | 0.007 |
| Serum C Reactive Protein (CRP) | −0.28 | 0.014 |
| pro-brain natriuretic peptide (pro BNP) | −0.22 | 0.051 |
| Variable | Subgroups | p-Value | |
|---|---|---|---|
| Sex | Women (n = 33) | Men (n = 44) | <0.0001 |
| Baseline post-dialysis ICF (L) | 15.6 ± 3.0 | 20.8 ± 4.2 | |
| Malnutrition (presence PEW) | Yes (n = 31) | No (n = 45) | 0.021 |
| Baseline post-dialysis ICF (L) | 17.1 ± 4.7 | 19.6 ± 4.1 | |
| Hypotension during dialysis | Yes (n = 24) | No (n = 51) | <0.0001 |
| Baseline post-dialysis ICF (L) | 15.7 ± 3.7 | 19.8 ± 4.4 | |
| Dizziness during dialysis | Yes (n = 22) | No (n = 53) | 0.02 |
| Baseline post-dialysis ICF (L) | 16.6 ± 4.3 | 19.3 ± 4.5 | |
| Model/Variables | β Coefficient | SE of the Estimate | 95% CI | p-Value |
|---|---|---|---|---|
| Model 1 (R2 = 0.834) | ||||
| Lean tissue mass | 0.162 | 0.014 | 0.132–0.189 | <0.0001 |
| Mid upper arm muscle circumference | 0.74 | 0.067 | 0.606–0.875 | <0.0001 |
| Sex | 3.001 | 0.465 | 2.072–3.930 | <0.0001 |
| Model 2 (R2 = 0.845) | ||||
| Lean tissue mass | 0.152 | 0.014 | 0.123–0.181 | <0.0001 |
| Mid upper arm muscle circumference | 0.726 | 0.066 | 0.594–0.857 | <0.0001 |
| Sex | 3.131 | 0.458 | 2.215–4.046 | <0.0001 |
| C-Reactive Protein | −0.235 | 0.115 | (−0.465)–(−0.004) | 0.046 |
| Variable | HR | p |
|---|---|---|
| Age | 1.197 (1.051–1.364) | 0.007 |
| Male | 0.977 (0.119–8.044) | 0.983 |
| Davies medium | 11.4 (0.419–312.8) | 0.149 |
| Davies high | 1.213 (0.060–24.58) | 0.900 |
| ICW | 0.627 (0.401–0.979) | 0.040 |
| C-Reactive Protein | 1.150(0.803–1.647) | 0.446 |
| Albumin ≤ 3.8 g/dL | 0.037(0.003–0.438) | 0.009 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gracia-Iguacel, C.; González-Parra, E.; Mahillo, I.; Ortiz, A. Low Intracellular Water, Overhydration, and Mortality in Hemodialysis Patients. J. Clin. Med. 2020, 9, 3616. https://doi.org/10.3390/jcm9113616
Gracia-Iguacel C, González-Parra E, Mahillo I, Ortiz A. Low Intracellular Water, Overhydration, and Mortality in Hemodialysis Patients. Journal of Clinical Medicine. 2020; 9(11):3616. https://doi.org/10.3390/jcm9113616
Chicago/Turabian StyleGracia-Iguacel, Carolina, Emilio González-Parra, Ignacio Mahillo, and Alberto Ortiz. 2020. "Low Intracellular Water, Overhydration, and Mortality in Hemodialysis Patients" Journal of Clinical Medicine 9, no. 11: 3616. https://doi.org/10.3390/jcm9113616
APA StyleGracia-Iguacel, C., González-Parra, E., Mahillo, I., & Ortiz, A. (2020). Low Intracellular Water, Overhydration, and Mortality in Hemodialysis Patients. Journal of Clinical Medicine, 9(11), 3616. https://doi.org/10.3390/jcm9113616





