Prediction of Discontinuation of Structured Exercise Programme in Chronic Fatigue Syndrome Patients
Abstract
1. Introduction
2. Experimental Section
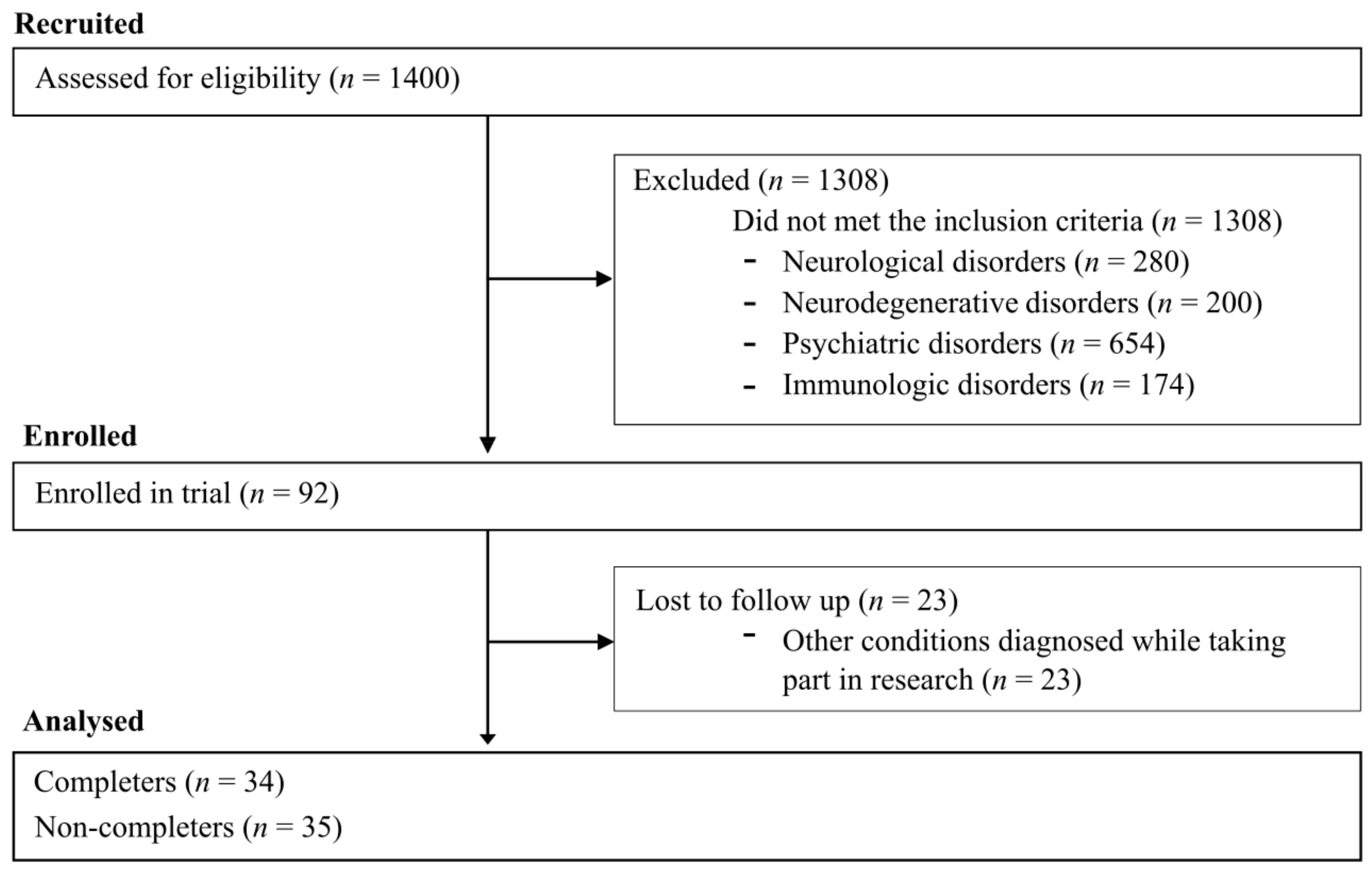
2.1. Participants
Recruitment and Eligibility
2.2. Measures
2.2.1. Fatigue Assessment Tools
2.2.2. Cognitive Function Measurement
2.2.3. Autonomic Nervous System Measurement
2.2.4. Cardiopulmonary Exercise Testing
2.2.5. Body Composition Analysis
2.3. Intervention
2.4. Statistical Analyses
3. Results
3.1. Comparison of Completers vs. Non-Completers before SEP
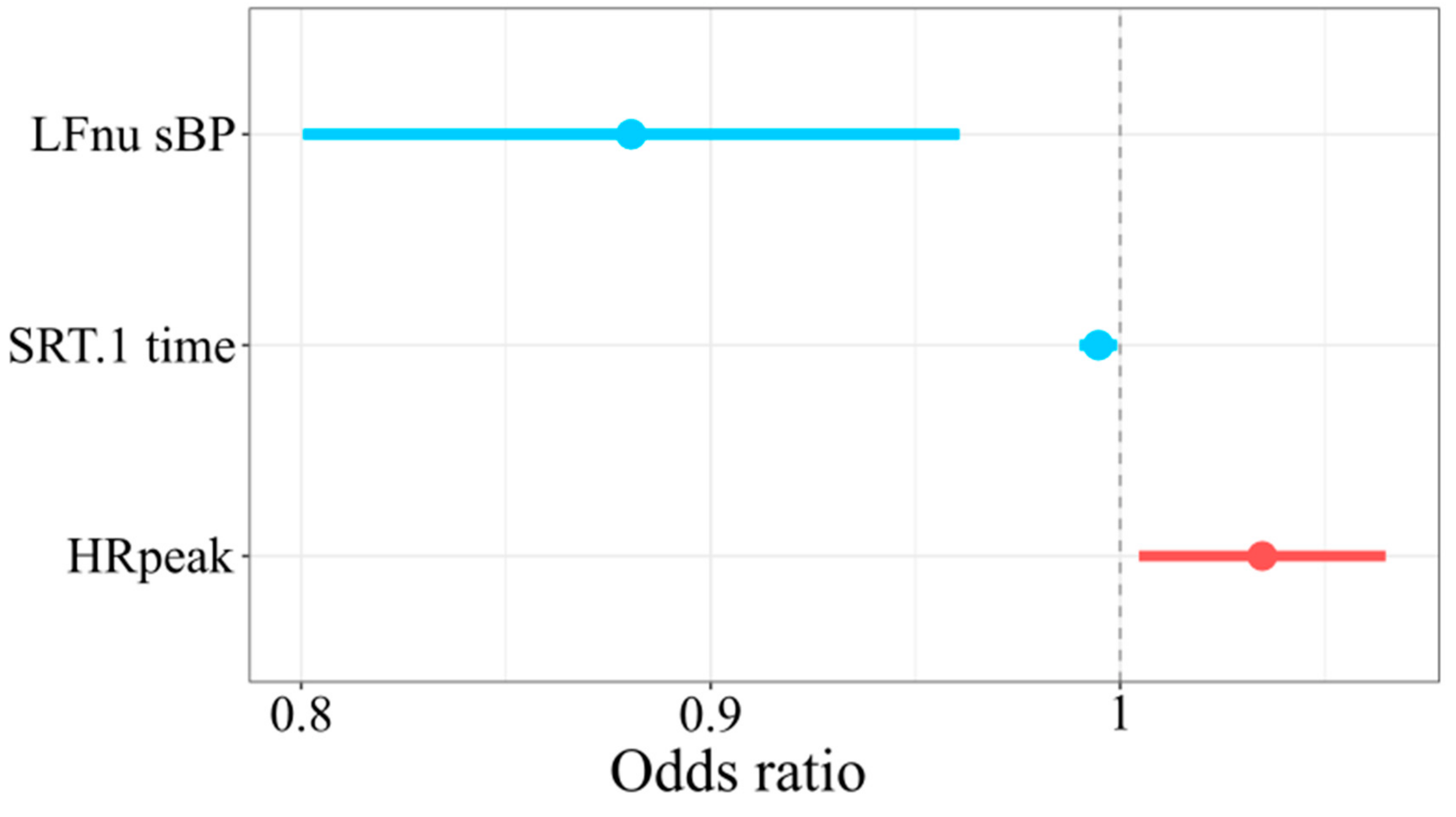
3.2. Predictors of SEP Completion
4. Discussion
4.1. Withdrawal Rate
4.2. Differences between SEP Completers and Non-Completers
4.3. Predictors of SEP Completion
4.4. Study Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments

Conflicts of Interest
Availability of Data
Appendix A
| Variable | Estimate | −95% CI | 95% CI | z Value | Pr(>|z|) |
|---|---|---|---|---|---|
| (Intercept) | 3.15 | −3.07 | 9.38 | 0.99 | 0.32 |
| LFnu sBP | −0.12 | −0.20 | −0.04 | −2.92 | 0.003 |
| SRT.1 reaction time | −0.01 | −0.01 | −0.0008 | −2.29 | 0.02 |
| HRmax baseline CPET | 0.03 | 0.005 | 0.06 | 2.26 | 0.02 |
References
- Costigan, A.; Elliott, C.; McDonald, C.; Newton, J.L. Orthostatic symptoms predict functional capacity in chronic fatigue syndrome: Implications for management. QJM An Int. J. Med. 2010, 103, 589–595. [Google Scholar] [CrossRef] [PubMed]
- De Becker PRoeykens, J.; Reynders, M.; McGregor, N.; De Meirleir, K. Exercise capacity in chronic fatigue syndrome. Arch. Intern. Med. 2000, 160, 3270–3277. [Google Scholar] [CrossRef] [PubMed]
- Ray, C.; Weir, W.; Stewart, D.; Miller, P.; Hyde, G. Ways of coping with chronic fatigue syndrome: Development of an illness management questionnaire. Soc. Sci. Med. 1993, 37, 385–391. [Google Scholar] [CrossRef]
- Nelson, M.J.; Bahl, J.S.; Buckley, J.D.; Thomson, R.L.; Davison, K. Evidence of altered cardiac autonomic regulation in myalgic encephalomyelitis/chronic fatigue syndrome: A systematic review and meta-analysis. Medicine 2019, 98, e17600. [Google Scholar] [CrossRef] [PubMed]
- Davenport, T.E.; Lehnen, M.; Stevens, S.R.; VanNess, J.M.; Stevens, J.; Snell, C.R. Chronotropic intolerance: An overlooked determinant of symptoms and activity limitation in myalgic encephalomyelitis/chronic fatigue syndrome? Front. Pediatrics 2019, 7, 82. [Google Scholar] [CrossRef] [PubMed]
- Robinson, L.J.; Gallagher, P.; Watson, S.; Pearce, R.; Finkelmeyer, A.; Maclachlan, L.; Newton, J.L. Impairments in cognitive performance in chronic fatigue syndrome are common, not related to co-morbid depression but do associate with autonomic dysfunction. PLoS ONE 2019, 14, e0210394. [Google Scholar] [CrossRef] [PubMed]
- Van Campen, C.L.; Rowe, P.C.; Verheugt, F.W.; Visser, F.C. Cognitive function declines following orthostatic stress in adults with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). Front. Neurosci. 2020, 14, 688. [Google Scholar] [CrossRef]
- Komaroff, A.L. Advances in understanding the pathophysiology of chronic fatigue syndrome. JAMA 2019, 322, 499–500. [Google Scholar] [CrossRef]
- Reicker, L.I.; Tombaugh, T.N.; Walker, L.; Freedman, M.S. Reaction time: An alternative method for assessing the effects of multiple sclerosis on information processing speed. Arch. Clin. Neuropsychol. 2007, 22, 655–664. [Google Scholar] [CrossRef]
- White, P.D.; Goldsmith, K.A.; Johnson, A.L.; Potts, L.; Walwyn, R.; De Cesare, J.C.; Baber, H.L.; Burgess, M.; Clark, L.V.; Cox, D.L.; et al. Comparison of adaptive pacing therapy, cognitive behaviour therapy, graded exercise therapy, and specialist medical care for chronic fatigue syndrome (PACE): A randomised trial. Lancet 2011, 377, 823–836. [Google Scholar] [CrossRef]
- Chu, L.; Valencia, I.J.; Garvert, D.W.; Montoya, J.G. Deconstructing post-exertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome: A patient-centered, cross-sectional survey. PLoS ONE 2018, 13, e0197811. [Google Scholar] [CrossRef] [PubMed]
- Knapen, J.; Vancampfort, D.; Moriën, Y.; Marchal, Y. Exercise therapy improves both mental and physical health in patients with major depression. Disabil. Rehabil. 2015, 37, 1490–1495. [Google Scholar] [CrossRef] [PubMed]
- Wilshire, C.E.; Kindlon, T.; Courtney, R.; Matthees, A.; Tuller, D.; Geraghty, K.; Levin, B. Rethinking the treatment of chronic fatigue syndrome—A reanalysis and evaluation of findings from a recent major trial of graded exercise and CBT. BMC Psychol. 2018, 6, 6. [Google Scholar] [CrossRef]
- Kindlon, T. Do graded activity therapies cause harm in chronic fatigue syndrome? J. Health Psychol. 2017, 22, 1146–1154. [Google Scholar] [CrossRef] [PubMed]
- Chalder, T.; Goldsmith, K.A.; White, P.D.; Sharpe, M.; Pickles, A.R. Rehabilitative therapies for chronic fatigue syndrome: A secondary mediation analysis of the PACE trial. Lancet Psychiatry 2015, 2, 141–152. [Google Scholar] [CrossRef]
- Ioannidis, J.P.; Evans, S.J.; Gøtzsche, P.C.; O’neill, R.T.; Altman, D.G.; Schulz, K.; Moher, D. Better reporting of harms in randomized trials: An extension of the CONSORT statement. Ann. Intern. Med. 2004, 141, 781–788. [Google Scholar] [CrossRef]
- Fukuda, K.; Straus, S.E.; Hickie, I.; Sharpe, M.C.; Dobbins, J.G.; Komaroff, A. The chronic fatigue syndrome: A comprehensive approach to its definition and study. Ann. Intern. Med. 1994, 121, 953–959. [Google Scholar] [CrossRef]
- Morriss, R.; Wearden, A.; Mullis, R. Exploring the validity of the Chalder Fatigue scale in chronic fatigue syndrome. J. Psychosom. Res. 1998, 45, 411–417. [Google Scholar] [CrossRef]
- Valko, P.O.; Bassetti, C.L.; Bloch, K.E.; Held, U.; Baumann, C.R. Validation of the fatigue severity scale in a Swiss cohort. Sleep 2008, 31, 1601–1607. [Google Scholar] [CrossRef]
- Frith, J.; Newton, J. Fatigue impact scale. Occup. Med. 2010, 60, 159. [Google Scholar] [CrossRef]
- Zalewski, P.; Kujawski, S.; Tudorowska, M.; Morten, K.; Tafil-Klawe, M.; Klawe, J.J.; Strong, J.; Estévez-López, F.; Murovska, M.; Newton, J.L. The Impact of a Structured Exercise Programme upon Cognitive Function in Chronic Fatigue Syndrome Patients. Brain Sci. 2020, 10, 4. [Google Scholar] [CrossRef]
- Bianchi, A.M.; Mainardi, L.T.; Meloni, C.; Chierchiu, S.; Cerutti, S. Continuous monitoring of the sympatho-vagal balance through spectral analysis. IEEE Eng. Med. Biol. Mag. 1997, 16, 64–73. [Google Scholar] [CrossRef] [PubMed]
- Fortin, J.; Klinger, T.; Wagner, C.; Sterner, H.; Madritsch, C.; Grullenberger, R. The task force monitor—A non-invasive beat-to-beat monitor for hemodynamic and autonomic function of the human body. In Proceedings of the 20th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Austin, TX, USA, 1 November 1998. [Google Scholar]
- Fortin, J.; Marte, W.; Grullenberger, R. Continuous non-invasive blood pressure monitoring using concentrically interlocking control loops. Comput. Biol. Med. 2006, 36, 941–957. [Google Scholar] [CrossRef]
- Fletcher, G.F.; Ades, P.A.; Kligfield, P.; Arena, R.; Balady, G.J.; Bittner, V.A.; Coke, L.A.; Fleg, J.L.; Forman, D.E.; Gerber, T.C.; et al. Exercise standards for testing and training: A scientific statement from the American Heart Association. Circulation 2013, 128, 873–934. [Google Scholar] [CrossRef] [PubMed]
- Balady, G.J.; Arena, R.; Sietsema, K.; Myers, J.; Coke, L.; Fletcher, G.F.; Forman, D.; Franklin, B.; Guazzi, M.; Gulati, M.; et al. Clinician’s guide to cardiopulmonary exercise testing in adults: A scientific statement from the American Heart Association. Circulation 2010, 122, 191–225. [Google Scholar] [CrossRef]
- American College of Sports Medicine. ACSM’s Guidelines for Exercise Testing and Prescription; Linda, S., Pescatello, Deborah, R., Paul, D., Eds.; ThompsonWolters Kluwer Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2010; Volume 8, pp. 35–96. [Google Scholar]
- Andri, S.; Ken, A.; Andreas, A.; Nanina, A.; Tomas, A.; Chandima, A.; Antti, A.; Adrian, B.; Kamil, B.; Ben, B.; et al. DescTools: Tools for Descriptive Statistics. R package version 0.99.36. 2020. Available online: https://cran.r-project.org/package=DescTools (accessed on 24 September 2020).
- Solt, F.; Hu, Y.; Dotwhisker: Dot-and-Whisker Plots of Regression Results. The Comprehensive R Archive Network (CRAN). 2015. Available online: http://CRAN.R-project.org/package=dotwhisker (accessed on 24 September 2020).
- Clark, L.V.; Pesola, F.; Thomas, J.M.; Vergara-Williamson, M.; Beynon, M.; White, P.D. Guided graded exercise self-help plus specialist medical care versus specialist medical care alone for chronic fatigue syndrome (GETSET): A pragmatic randomised controlled trial. Lancet 2017, 390, 363–373. [Google Scholar] [CrossRef]
- Sharpe, M.; Goldsmith, K.A.; Johnson, A.L.; Chalder, T.; Walker, J.; White, P.D. Rehabilitative treatments for chronic fatigue syndrome: Long-term follow-up from the PACE trial. Lancet Psychiatry 2015, 2, 1067–1074. [Google Scholar] [CrossRef]
- Keller, B.A.; Pryor, J.L.; Giloteaux, L. Inability of myalgic encephalomyelitis/chronic fatigue syndrome patients to reproduce VO 2 peak indicates functional impairment. J. Transl. Med. 2014, 12, 104. [Google Scholar] [CrossRef]
- Van Oosterwijck, J.; Nijs, J.; Meeus, M.; Lefever, I.; Huybrechts, L.; Lambrecht, L.; Paul, L. Pain inhibition and postexertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome: An experimental study. J. Intern. Med. 2010, 268, 265–278. [Google Scholar] [CrossRef]
- van Campen, C.L.; Rowe, P.C.; Visser, F.C. Two-Day Cardiopulmonary Exercise Testing in Females with a Severe Grade of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Comparison with Patients with Mild and Moderate Disease. Healthcare 2020, 8, 192. [Google Scholar] [CrossRef]
- Franklin, J.D.; Atkinson, G.; Atkinson, J.M.; Batterham, A.M. Peak oxygen uptake in chronic fatigue syndrome/myalgic encephalomyelitis: A meta-analysis. Int. J. Sports Med. 2019, 40, 77–87. [Google Scholar] [CrossRef]
- Booth, N.E.; Myhill, S.; McLaren-Howard, J. Mitochondrial dysfunction and the pathophysiology of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). Int. J. Clin. Exp. Med. 2012, 5, 208. [Google Scholar] [PubMed]
- Guazzi, M.; Adams, V.; Conraads, V.; Halle, M.; Mezzani, A.; Vanhees, L.; Arena, R.; Fletcher, G.F.; Forman, D.E.; Kitzman, D.W.; et al. Clinical recommendations for cardiopulmonary exercise testing data assessment in specific patient populations. Eur. Heart J. 2012, 33, 2917–2927. [Google Scholar] [CrossRef] [PubMed]
- Scherbakov, N.; Szklarski, M.; Hartwig, J.; Sotzny, F.; Lorenz, S.; Meyer, A.; Grabowski, P.; Doehner, W.; Scheibenbogen, C. Peripheral endothelial dysfunction in myalgic encephalomyelitis/chronic fatigue syndrome. ESC Heart Fail. 2020, 7, 1064–1071. [Google Scholar] [CrossRef]
- Cerutti, C.; Gustin, M.P.; Paultre, C.Z.; Lo, M.; Julien, C.; Vincent, M.; Sassard, J. Autonomic nervous system and cardiovascular variability in rats: A spectral analysis approach. Am. J. Physiol. Heart Circ. Physiol. 1991, 261, H1292–H1299. [Google Scholar] [CrossRef] [PubMed]
- Pagani, M.; Montano, N.; Porta, A.; Malliani, A.; Abboud, F.M.; Birkett, C.; Somers, V.K. Relationship between spectral components of cardiovascular variabilities and direct measures of muscle sympathetic nerve activity in humans. Circulation 1997, 95, 1441–1448. [Google Scholar] [CrossRef] [PubMed]
- Billman, G.E.; Huikuri, H.V.; Sacha, J.; Trimmel, K. An introduction to heart rate variability: Methodological considerations and clinical applications. Front. Physiol. 2015, 6, 55. [Google Scholar] [CrossRef]
- Komaroff, A.L.; Buchwald, D. Symptoms and signs of chronic fatigue syndrome. Rev. Infect. Dis. 1991, 13 (Suppl. 1), S8–S11. [Google Scholar] [CrossRef] [PubMed]
- Grafman, J. Neuropsychological features of chronic fatigue syndrome. In Chronic Fatigue Syndrome; Straus, S.E., Ed.; Marcel Dekker, Inc.: New York, NY, USA, 1994; pp. 263–284. [Google Scholar]
| Variable | Mean (SD) Non-Completers (n = 35) | Mean (SD) Completers (n = 34) | p Value | FDR Adjusted p Value |
|---|---|---|---|---|
| Age (years) | 39.6 (9) | 37.06 (7.9) | 0.25 | 0.57 |
| BMI (kg/m2) | 24.02 (3.5) | 24.52 (3.2) | 0.54 | 0.86 |
| FFM (kg) | 53.76 (11) | 54.45 (9.7) | 0.78 | 0.99 |
| Fat (%) | 24.2 (7) | 25.04 (6.6) | 0.61 | 0.92 |
| Variable | Mean (SD) Non-Completers (n = 35) | Mean (SD) Completers (n = 34) | p Value | FDR Adjusted p Value |
|---|---|---|---|---|
| CFQ (points) | 24.54 (3.9) | 26.12 (3.5) | 0.08 | 0.38 |
| FSS (points) | 48.74 (8.7) | 48.91 (8.9) | 0.94 | 0.99 |
| FIS (points) | 90.91 (27.7) | 93.59 (24.9) | 0.67 | 0.96 |
| Variable | Mean (SD) Non-Completers (n = 35) | Mean (SD) Completers (n = 34) | p Value | FDR Adjusted p Value |
|---|---|---|---|---|
| LFnu-RRI (%) | 51.62 (19) | 56.81 (14.9) | 0.21 | 0.57 |
| HFnu-RRI (%) | 48.38 (19) | 43.19 (14.9) | 0.21 | 0.57 |
| LF/HF-RRI | 1.55 (1.3) | 1.91 (2) | 0.40 | 0.69 |
| LF/HF | 1.42 (0.8) | 1.53 (1.3) | 0.82 | 0.99 |
| LFnu-dBP (%) | 54.24 (14.9) | 50.06 (14.4) | 0.24 | 0.57 |
| HFnu-dBP (%) | 14.23 (11.4) | 13.73 (9.4) | 0.78 | 0.99 |
| LFnu-sBP (%) | 46.99 (13.2) | 37.14 (12.1) | 0.005 | 0.08 |
| HFnu-sBP (%) | 16.61 (10) | 16.46 (11.6) | 0.95 | 0.99 |
| SRT.1 mean reaction time (ms) | 647.91 (174.1) | 547.09 (162.6) | 0.002 | 0.07 |
| Variable | Mean (SD) Non-Completers (n = 19) | Mean (SD) Completers (n = 34) | p Value | FDR Adjusted p Value |
|---|---|---|---|---|
| VO2 AT [mL/kg/min] | 21.89 (5.9) | 21.86 (4.8) | 0.99 | 0.99 |
| VCO2 AT [mL/kg/min] | 21.21 (6.7) | 21.36 (4.9) | 0.93 | 0.99 |
| RER AT | 0.96 (0.1) | 0.98 (0) | 0.95 | 0.99 |
| VE AT [mL/kg/min] | 602.84 (190.8) | 579.86 (128.8) | 0.24 | 0.57 |
| HR AT [bpm] | 136.00 (22.5) | 144.21 (16.4) | 0.14 | 0.57 |
| Load AT [W] | 102.28 (22.3) | 99.26 (44.4) | 0.31 | 0.60 |
| sBP AT [mmHg] | 161.72 (51.5) | 167.18 (23.8) | 0.99 | 0.99 |
| dBP AT [mmHg] | 81.39 (24.1) | 88.59 (14.9) | 0.55 | 0.86 |
| Variable | Mean (SD) Non-Completers (n = 19) | Mean (SD) Completers (n = 34) | p Value | FDR Adjusted p Value |
|---|---|---|---|---|
| VO2peak [mL/min/kg] | 26.33 (7.4) | 29.49 (6.3) | 0.07 | 0.38 |
| VCO2peak [mL/min/kg] | 29.41 (9.8) | 34.04 (7.7) | 0.06 | 0.38 |
| RERpeak | 1.08 (0.1) | 1.15 (0.1) | 0.03 | 0.33 |
| VEpeak [mL/kg/min] | 885.09 (318.8) | 968.35 (239.6) | 0.29 | 0.60 |
| HRpeak [bpm] | 166.39 (25) | 182.35 (21.9) | 0.06 | 0.38 |
| Load peak [W] | 119.84 (47.6) | 132.94 (34.6) | 0.26 | 0.57 |
| sBPpeak [mmHg] | 191.58 (35.0) | 180.94 (26.7) | 0.22 | 0.57 |
| dBPpeak [mmHg] | 90.53 (13.5) | 90.65 (11.1) | 0.97 | 0.99 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kujawski, S.; Cossington, J.; Słomko, J.; Dawes, H.; Strong, J.W.L.; Estevez-Lopez, F.; Murovska, M.; Newton, J.L.; Hodges, L.; Zalewski, P. Prediction of Discontinuation of Structured Exercise Programme in Chronic Fatigue Syndrome Patients. J. Clin. Med. 2020, 9, 3436. https://doi.org/10.3390/jcm9113436
Kujawski S, Cossington J, Słomko J, Dawes H, Strong JWL, Estevez-Lopez F, Murovska M, Newton JL, Hodges L, Zalewski P. Prediction of Discontinuation of Structured Exercise Programme in Chronic Fatigue Syndrome Patients. Journal of Clinical Medicine. 2020; 9(11):3436. https://doi.org/10.3390/jcm9113436
Chicago/Turabian StyleKujawski, Sławomir, Jo Cossington, Joanna Słomko, Helen Dawes, James W.L. Strong, Fernando Estevez-Lopez, Modra Murovska, Julia L. Newton, Lynette Hodges, and Paweł Zalewski. 2020. "Prediction of Discontinuation of Structured Exercise Programme in Chronic Fatigue Syndrome Patients" Journal of Clinical Medicine 9, no. 11: 3436. https://doi.org/10.3390/jcm9113436
APA StyleKujawski, S., Cossington, J., Słomko, J., Dawes, H., Strong, J. W. L., Estevez-Lopez, F., Murovska, M., Newton, J. L., Hodges, L., & Zalewski, P. (2020). Prediction of Discontinuation of Structured Exercise Programme in Chronic Fatigue Syndrome Patients. Journal of Clinical Medicine, 9(11), 3436. https://doi.org/10.3390/jcm9113436









