Abstract
The aim was to identify effective surgical treatments for patients with rheumatoid arthritis in the foot and/or ankle. A systematic review of the literature was conducted via a data search of the PubMed, Scopus, Cumulative Index to Nursing and Allied Health Literature (CINAHL), and PROSPERO databases, from their inception until June 2019. Only non-randomized controlled trials and cohort studies were included in this review. Two of the present authors independently assessed the quality of each study and extracted the relevant data. A quality assessment of all articles was performed using the methodological index for non-randomized studies criteria. In addition, the Newcastle Ottawa scale was used for cohort studies. Thirteen studies met the inclusion criteria (five cohort studies and eight NRCTs). The total population considered was 923 patients (570 patients had RA), with a mean age of 58.8 years. Regarding the risk of bias, both the NRCTs and the cohort studies had a moderate level of quality. Despite the relatively low quality of these studies, surgical treatment for the foot and/or ankle is shown to reduce pain and improve functionality in patients with RA, in the short term (6–12 months).
1. Introduction
Rheumatoid arthritis (RA) is a systemic, chronic, autoimmune, and polyarticular pathology that produces inflammation, which mainly affects the synovial joints, with progressive cartilage degeneration and erosion, leading to pain and functional limitation [1,2,3,4].
The aetiology of RA is unknown, but there are predisposing risk factors, some of which may be genetic, such as the presence of the Human Leucocyte Antigen (HLA)-DR4 class II histocompatibility antigen. Other relevant factors are gender, women are three times more likely than men to have RA [5]. The prevalence of RA is high, at 0.3%–1.2% and it increases with age (6% higher among those aged 65 years or more) [6].
RA most commonly affects the small joints in the upper limbs, in the hand and the wrist [6], and in the lower ones, in the ankle and foot (90%). The greatest number of deformities are found in the forefoot [7]. Foot problems are strongly related to RA and often develop rapidly; thus, half of all RA patients present foot problems within three years of diagnosis [8]. RA often takes the form of symmetrical small joint polyarthritis, with pain, swelling, and/or stiffness. The symptoms are usually first observed in the forefoot [9] and include hallux valgus, subluxation, and dislocation or erosion of the metatarsophalangeal (MTP) joints, together with hammer toes or claw toes in the lesser toes [10]. RA can also affect the subtalar and mid-tarsal joints and in some cases the ankle joint. In the subtalar joint, synovitis causes pain and stiffness leading to cartilage loss and bone erosion. These changes increase the valgus deformity, causing flattening of the longitudinal arch. Synovitis of the MTP-joint is related to forefoot deformity [11,12].
Clinical practice offers many conservative treatments to relieve the pain of RA, including non-steroidal anti-inflammatory drugs, standard disease modifying anti-rheumatic drugs, biological treatments, specialised footwear and orthotics. [13,14]. If these approaches do not satisfactorily resolve the pain, deformity, or loss of function, or facilitate the use of conventional shoes, various types of surgical treatment may be proposed [15], regardless of the stage of the disease, to be used initially as prophylaxis, and at more advanced levels to correct deformities, recover foot function, and relieve pain [12,16]. Surgical techniques are most commonly applied to the forefoot [17], but the hindfoot and ankle are also treated [18]. The surgical procedures for the forefoot are arthrodesis of the first MTP joint and/or arthroplasties of the MTP joints [19,20] and surgical treatments to the ankle are total arthroplasty and prosthesis [21,22]. Studies have been conducted to describe and examine the role played by different surgical techniques for the foot and ankle for patients with RA [23,24,25] but to date no systematic review has been undertaken to assess their impact on pain relief and improved functionality.
Accordingly, the present paper aims mainly to identify effective surgical treatments for patients with RA in the foot and/or ankle.
2. Methods
The review protocol is registered at the International Prospective Register of Systematic Reviews (PROSPERO).
2.1. Design
This review was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement [26].
2.2. Search Strategy
One member of the research team (ABOA) carried out the literature search, after establishing its aims and checking that no previous studies in this respect had been carried out. The PROSPERO, PubMed, Scopus, and Cumulative Index to Nursing and Allied Health Literature (CINAHL) databases were searched, from their inception until June 2019, using the optimized search strategies described in Appendix A.
2.3. Eligibility Criteria
The PICO (P = population; I = intervention; C = comparator; O = outcome) and the PECO (P = population; E = exposition; C = comparator; O = outcome) frameworks were applied by two reviewers (PCG-GGN), to implement the following inclusion criteria for the studies considered.
- -
- Study population composed of adults aged at least 18 years, diagnosed with RA, and who underwent surgery to the ankle and/or foot.
- -
- Study design: Randomised controlled clinical trials (RCTs) and non-randomised controlled clinical trials (NRCTs) in which surgical treatment to the ankle or foot was performed for patients with RA who experienced pain and were disabled were assessed during the follow-up period
- -
- Cohort studies of patients with RA and/or without RA to evaluate one or more surgical treatments to the foot and/or ankle, with a follow-up period.
- -
- Studies which assessed pain and disability by the following outcomes: Foot Function Index [27], American Orthopaedic Foot and Ankle Score [28], Japanese Society of Surgery of the Foot ankle/hindfoot scale [29,30], Ankle Osteoarthritis Scale [31], Kofoed ankle score, Salford Rheumatoid Arthritis Foot Evaluation- Questionnaire [32], American College of Foot and Ankle Surgeons scoring scale [29], Short-Form 36 Questionnaire [33], or Stanford Health Assessment Questionnaire disability index [34]
The following types of studies were excluded from consideration:
- -
- Studies that examined surgical treatments to the foot or ankle in individual patients with RA (case studies).
- -
- Studies combining conservative and surgical treatment to the foot or ankle in patients with RA, including those describing a relevant post-operative rehabilitation programme.
- -
- Studies assessing pain or disability in juvenile arthritis.
- -
- Studies where the first treatment options were alternatives such as orthopaedic shoes, foot or physiotherapy, not surgery.
2.4. Study Selection
Two blinded reviewers (A.M.-V and M.M.-R) evaluated the search results. The reference lists were reviewed independently to observe the fulfilment or otherwise of the inclusion criteria. Disagreements were resolved by discussion between the two reviewers, and if consensus was not possible, further opinion was sought (from A.B.O.-A, P.C.-G, E.C.-L and G.G.-N). We also planned, if necessary, to send an email to the original authors to obtain further information regarding the study findings, but this measure was not needed for any study.
2.5. Data Extraction
The titles and abstracts were then reviewed independently by two reviewers (AMV and MMR) and full-text versions of the articles considered relevant were obtained. The same reviewers performed the second stage of screening, reading the full text of the selected articles. The following data were extracted from each study, using a standardized template: study details (author and year of publication), study participant characteristics (mean age, sex, details of the foot affected), study design (cohort study or NRCT), follow-up time, and measurement instrument used (mean and SD).
No meta-analysis was carried out, due to the heterogeneity of these studies and the varying outcomes described.
2.6. Quality Assessment of the Studies Included
Two researchers independently assessed the risk of bias in the articles included, using the Methodological Index for Non-Randomised Studies (MINORS) for the NRCTs [35] and the Newcastle-Ottawa Scale (NOS) [36] for the cohort studies.
The MINORS is used to assess the internal and external validity of non-randomised surgical studies (comparative and/or non-comparative). It consists of twelve items, of which eight are used to assess both comparative and non-comparative studies and four are exclusive to comparative studies. The items are scored on the following scale: 0 (not reported), 1 (reported but inadequate) or 2 (reported and adequate). The overall maximum score is 16 for non-comparative studies and 24 for comparative ones. For non-comparative studies, the following range of scores is applied: 0–4, very low quality; 5–8, low quality; 9–12, moderate quality; and 13–16, high quality. For comparative studies, the corresponding scores are 0–6, very low quality; 7–12, low quality; 13–18, moderate quality; and 19–24, high quality [35].
The NOS is a reliable, valid tool for assessing the quality of cohort studies. In this case, the quality score is based on three categories: group selection (four items), inter-group comparability (one item), and outcome and exposure assessment (3 items). A maximum of one point is awarded for each item in the group selection and in the outcome and exposure assessment categories. A maximum of two points is awarded for comparability. Thus, the maximum score with the NOS is 9 points, which represents the highest methodological quality [36].
3. Results
Initially, 289 studies were identified, but 120 were duplicated among the different databases. The remaining 169 were screened against our inclusion/exclusion criteria, using the titles, abstracts, and key words. Eighty-nine studies met the inclusion criteria. After quality appraisal, a further 76 were excluded, and so 13 studies remained in the final analysis. Five of these were cohort studies and eight were NRCTs. None were RCTs. Figure 1 shows the PRISMA flow diagram for the studies included in the review [37].
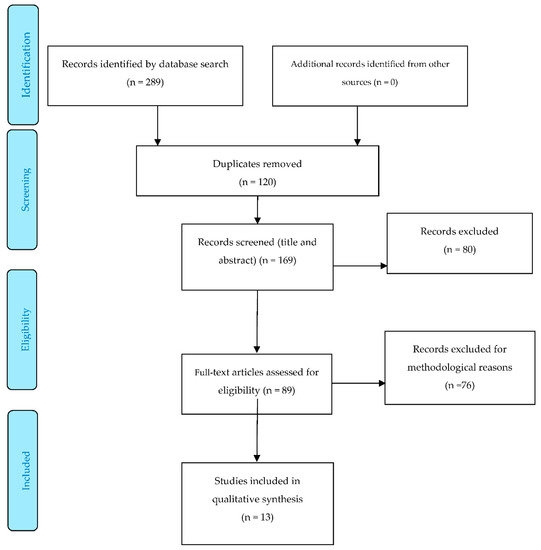
Figure 1.
PRISMA Flow Diagram.
3.1. Study Characteristics
The 13 studies included a total of 923 patients, with a mean age of 58.8 years. Of these, 570 (90.7% of whom were female) had RA. Surgical treatment was predominantly performed on the right foot or ankle (n = 173), although in many of the studies the location was not specified.
The NRCTs included a total of 548 patients (82.48%were women), with a mean age of 58.46 years. The minimum follow-up period was twelve months (mean duration: 44.75 months). The most frequent location of the surgical treatment was in the metatarsophalangeal (MTP) joints and the main technique used was arthroplasty (Table 1).

Table 1.
Characteristics of Non-Randomized Controlled Trials (NRCTs).
The cohort studies included a total of 393 patients (75.31%were women), with a mean age of 59.34 years. The minimum follow-up period was six months (mean duration: 39.8 months). The most frequent location of the surgical treatment was in the first MTP joint, or in various MTP joints, by arthrodesis or arthroplasty (Table 2).

Table 2.
Characteristics of cohort studies.
All studies reported a considerable improvement in pain relief as well as in functional capacity after surgery in the patients with RA, regardless of the technique used (arthroplasty or osteotomy or arthrodesis) or the location of the surgery (MTP joints or small toes or ankle). This combination of techniques achieved the best results, both in relieving pain and in enhancing functionality (p < 0.001). Table 3 summarized the data that help assess the actual outcome of each of the interventions in the studies that were included in this review.

Table 3.
Outcomes in pain relief and functional capacity in included studies.
3.2. Risk of Bias
None of the NRCTs included achieved the maximum MINORS score. The best comparative study received an overall MINORS score of 20 out of 24, and the mean overall score for all comparative studies was 18. The areas of weakest reporting for the comparative studies were the unbiased assessment of the study endpoint, the inclusion of consecutive patients and the use of endpoints appropriate to the study aim. The prospective recruitment of patients and the use of appropriate statistical analyses scored more highly. The best non-comparative study received an overall score of 11 out of 16, and the mean overall MINORS score for all non-comparative studies was 10. The areas of weakest reporting for the non-comparative studies were the unbiased assessment of the study endpoint, the prospective calculation of the study size, the inclusion of consecutive patients, the use of endpoints appropriate to the study aim, and the use of a follow-up period appropriate to the study aim. Table 4 shows the MINORS score obtained by each study.

Table 4.
Quality assessment of the NRCTs studies considered, according to the MINORS score.
In the cohort studies, the scores obtained ranged from five to seven points (out of a possible nine). Two out of four cohort studies scored seven points. All the studies allocated sufficient time for follow-up. The critical appraisal details are presented in Table 5.

Table 5.
Quality assessment of the cohort studies considered, according to the Newcastle-Ottawa Scale (NOS).
4. Discussion
This review has two main aims: to identify the surgical treatment provided to the foot and ankle for patients with RA and to evaluate the risk of bias in studies conducted in this field in order to assess their quality.
Regarding the main objective, many studies have examined records of surgical treatment for the foot and ankle in patients with RA, concluding that the outcome is often very beneficial [41,42,43]. Deformities at this level can play an important role in determining the pain experienced and in provoking loss of functionality. Moreover, they directly reduce the patient’s ability to perform the activities of daily life and may even influence mood [42].
Our findings are based on NRCTs and cohort studies, which show that surgical treatment for these patients usually decreases pain and enhances functionality, assessed over a follow-up period of at least 12 and six months, respectively [19,25]. All of these studies used an objective measuring instrument, providing validity, reliability, and responsiveness, underpinning the measurements obtained for the clinical variables observed in the patients after the surgical technique in question had been performed [25]. These instruments provide a clinical assessment of both pain and functionality, and were used to indicate the change achieved (pre/post-surgery). Despite the objective results obtained for the clinical variables, as regards pain and functionality, we were unable to perform a meta-analysis because the same instrument was not used in every study considered and so the data reported are heterogeneous. In addition, the follow-up time was not uniform, and this factor may have influenced the findings reported, as longer follow-up times after a surgical intervention take into account a greater potential number of recurrences or post-operative complications, thus enabling a more reliable analysis [34,44].
For patients with RA studies, the most common surgical procedures investigated are arthrodesis of the first MTP joint and/or arthroplasties of the MTP joints [19,20,38,43], since these patients are particularly subject to deformities in the forefoot (such as hallux valgus, hallux rigidus, floating of the lesser toes or synovial inflammation of the MTP joints) or in the hindfoot (such as hindfoot valgus or flat foot), which can aggravate pain and disability among this population [10,17]. This combination of techniques was most commonly used in the studies considered and achieved the best results, both in relieving pain and in enhancing functionality (p < 0.001) [19,20,40,43]. However, there is no evidence that this is more effective than arthroplasty in all the metatarsal heads (or the fist metatarsal), because according to the papers included in our analysis, the only related research conducted were case studies [18,45,46], which are considered to present low methodological quality. Moreover, these papers do not address the specific object of our investigation. In contrast to the arthroplasty of the first MTP joint, there is a tendency to preserve the joint by performing shortened osteotomies in the diaphysis of the metatarsals. According to Horita et al. [38] and Ebina et al. [39], the reduction in pain level in the osteotomy group differs from that achieved by arthroplasty, although in terms of functionality, the results are very similar in both cases. Regarding surgical treatments to the ankle, the only studies identified were those by Su et al. [21] Van der Heide et al. [24] and Pedersen et al. [22]. In these cases, the most commonly investigated surgical procedure was that of total arthroplasty, followed by the use of a prosthesis. All these investigations reported improved functionality and reduced pain, although the differences between groups were not statistically significant.
Regarding risk of bias, the results obtained show that the majority of NRCTs considered, both comparative and non-comparative, presented only moderate quality. Only one comparative study was rated as ‘high quality’, with 20 points. The weaknesses common to all the NRCTs were the non-inclusion of consecutive patients, the failure to define endpoints appropriate to the study aim, and the presence of bias in assessments made at the study endpoint. It is important to highlight these deficiencies in the studies considered, since these shortcomings may have significant repercussions in the context of scientific research. If patients are recruited during the investigation, or if large numbers of participants drop out during the course of the study, the results obtained may not be valid or reliable. Furthermore, an unambiguous explanation should be given of the criteria used to assess the main outcome of the study, and this should always be in accordance with the research question originally posed. If the study aim is to compare techniques or population groups, there must be a blind evaluation of the outcomes achieved and a double-blind evaluation of subjective endpoints to provide trustworthy results as a basis for future investigation, and to demonstrate the suitability or otherwise of the research method applied. With respect to the possible presence of bias, the cohort studies considered presented only moderate methodological quality. All were deficient in the selection of the non-exposed cohort and assessment of outcomes. Both of these questions should be taken into account in research of this type, since it is difficult to identify the type of population being evaluated if there is no clear description of the non-exposed cohort and the main outcome cannot be properly assessed in the absence of a blinded independent evaluator.
Recent investigations indicate that patients with RA in the foot and/or ankle commonly receive surgical treatment, which achieves beneficial effects regarding pain relief and enhanced functionality [8,15]. With regard to the specific area of investigation, most of the studies considered focused on the treatment of the forefoot. However, few studies in this area present sufficient methodological quality, the majority being mere series of case studies. Moreover, the size of the sample used, and the follow-up period of the patients involved are in many cases inadequate.
The present systematic review presents numerous strengths: to our knowledge, this is the first such review focusing on surgical treatment to the foot and ankle for patients with RA in which specific review tools are applied to analyse the risk of bias, the study population and the application of a rigorous methodological process. Moreover, our review is based on a literature search of five medical databases, with no limitation on time. Nevertheless, it is also subject to certain limitations. The first is the small number of NRCTs and cohort studies included. In addition, the data considered present considerable heterogeneity, making it impossible to carry out a meta-analysis and hampering the overall assessment made. Finally, the studies reviewed presented a relatively high risk of common bias.
Our findings highlight the problems encountered in clinical practice and in research studies to determine whether a given surgical technique is appropriate for a patient with RA affecting the foot, and the need for further investigation to improve this process. Most of the studies considered applied objective instruments of pain and functionality, in the view that these questions of RA not only influence the activities of daily life, but also have an affective and psychological impact. However, there is no unified criterion as to the most suitable instrument for this purpose, the best follow-up time after surgery (periods of 12–76 months have been cited), or the number of patients to be included in the study population. Attention should be paid to possible confounders, such as adverse treatment effects, recurrences, treatment modality, current pattern of medication, and the duration of the disease. All of these questions are relevant and appropriate consideration of their effects might obviate the need for multiple reinterventions. Surgical interventions are conducted to achieve proper alignment, but also to ensure the functionality of the joint in the foot and/or ankle, and thus prevent recurrence [44].
5. Conclusions
Despite the above-stated limitations, the study findings clearly show that surgical treatment to the foot and/or ankle is beneficial as regards reducing pain and improving functionality in patients with RA (6–12 months). However, the deficient quality of many of the studies considered limits the extent to which definitive conclusions can be drawn. Future research of this type is needed, ensuring homogeneity in the study groups by size and composition, as well as in aspects such as the follow-up period considered and the description of main outcomes, in order to minimise the risk of bias.
Author Contributions
Conceptualisation, A.B.O.-A.; methodology, A.B.O.-A. and G.G.-N.; formal analysis, A.M.-V. and M.M.-R.; writing—original draft preparation, P.C.-G. and E.C.-L.; writing—review and editing, A.B.O.-A. and G.G.-N.; visualisation, G.G.-N.; supervision, A.B.O.-A. All authors have read and agreed to the published version of the manuscript.
Conflicts of Interest
The authors declare no conflict of interest.
Appendix A
Appendix A.1. Searching Strategy

Table A1.
Searching Strategy (Pubmed).
Table A1.
Searching Strategy (Pubmed).
| 1 | Rheumatoid Arthritis |
| 2 | Foot |
| 3 | Feet |
| 4 | Ankle |
| 5 | Bones of lower extremity |
| 6 | Hallux |
| 7 | First Metatarsophalang* |
| 8 | 2 OR 3 OR 4 OR 5 OR 6 OR 7 |
| 9 | 1 AND (2 OR 3 OR 4 OR 5 OR 6 OR 7) |
| 10 | Surgic* |
| 11 | “Non-conservative treatment” |
| 12 | 10 OR 11 |
| 13 | 9 AND 12 |
| 14 | “Pain” |
| 15 | Disab* |
| 16 | Funct* |
| 17 | 14 OR 15 OR 16 |
| 18 | 13 AND 17 |
Appendix A.2. Scopus Search Strategy
((Rheumatoid Arthritis) AND (Foot OR Feet OR Ankle OR Bones of lower extremity OR Hallux OR First Metatarsophalang*) AND (Surgic* OR “non-conservative treatment”) AND (Pain OR Disab* OR Funct*))
Appendix A.3. CINAHL Search Strategy

Table A2.
CINAHL search strategy.
Table A2.
CINAHL search strategy.
| 1 | Rheumatoid Arthritis |
| 2 | Foot |
| 3 | Feet |
| 4 | Ankle |
| 5 | Bones of lower extremity |
| 6 | 2 OR 3 OR 4 OR 5 |
| 7 | 1 AND (2 OR 3 OR 4 OR 5) |
| 8 | Surgic* |
| 9 | “Non-conservative treatment” |
| 10 | 8 OR 9 |
| 11 | 7 AND 10 |
| 12 | “Pain” |
| 13 | Disab* |
| 14 | Funct* |
| 15 | 12 OR 13 OR 14 |
| 16 | 11 AND 15 |
Appendix A.4. PROSPERO Search Strategy
((Rheumatoid Arthritis) AND (surgical) AND (foot OR ankle))
References
- Otter, S.J.; Lucas, K.; Springett, K.; Moore, A.; Davies, K.; Cheek, L.; Young, A.; Walker-Bone, K. Foot pain in rheumatoid arthritis prevalence, risk factors and management: An epidemiological study. Clin. Rheumatol. 2010, 29, 255–271. [Google Scholar] [CrossRef]
- Voshaar, M.A.O.; ten Klooster, P.M.; Taal, E.; van de Laar, M.A. Measurement properties of physical function scales validated for use in patients with rheumatoid arthritis: A systematic review of the literature. Health Qual. Life Outcomes 2011, 9, 99. [Google Scholar] [CrossRef]
- Riskowski, J.L.; Hagedorn, T.J.; Hannan, M.T. Measures of foot function, foot health, and foot pain: American Academy of Orthopedic Surgeons Lower Limb Outcomes Assessment: Foot and Ankle Module (AAOS-FAM), Bristol Foot Score (BFS), Revised Foot Function Index (FFI-R), Foot Health Status Questionnair. Arthritis Care Res. 2011, 63, S229–S239. [Google Scholar] [CrossRef] [PubMed]
- Nishikawa, M.; Owaki, H.; Takahi, K.; Fuji, T. Disease activity, knee function, and walking ability in patients with rheumatoid arthritis 10 years after primary total knee arthroplasty. J. Orthop. Surg. 2014. [Google Scholar] [CrossRef]
- Jaakkola, J.I.; Mann, R.A. A review of rheumatoid arthritis affecting the foot and ankle. Foot Ankle Int. 2004. [Google Scholar] [CrossRef] [PubMed]
- Gabriel, S.E.; Michaud, K. Epidemiological studies in incidence, prevalence, mortality, and comorbidity of the rheumatic diseases. Arthritis Res. Ther. 2009, 11, 229. [Google Scholar] [CrossRef] [PubMed]
- Siddle, H.J.; Hodgson, R.J.; Hensor, E.M.A.; Grainger, A.J.; Redmond, A.C.; Wakefield, R.J.; Helliwell, P.S. Plantar plate pathology is associated with erosive disease in the painful forefoot of patients with rheumatoid arthritis. BMC Musculoskelet. Disord. 2017. [Google Scholar] [CrossRef]
- Stolt, M.; Suhonen, R.; Leino-Kilpi, H. Foot health in patients with rheumatoid arthritis—A scoping review. Rheumatol. Int. 2017, 37, 1413–1422. [Google Scholar] [CrossRef]
- Van Der Leeden, M.; Steultjens, M.P.M.; Ursum, J.; Dahmen, R.; Roorda, L.D.; Van Schaardenburg, D.; Dekker, J. Prevalence and course of forefoot impairments and walking disability in the first eight years of rheumatoid arthritis. Arthritis Care Res. 2008, 59, 1596–1602. [Google Scholar] [CrossRef]
- Van der Leeden, M.; Steultjens, M.; Dekker, J.H.M.; Prins, A.P.A.; Dekker, J. Forefoot joint damage, pain and disability in rheumatoid arthritis patients with foot complaints: The role of plantar pressure and gait characteristics. Rheumatology 2006, 45, 465–469. [Google Scholar] [CrossRef]
- Grondal, L.; Tengstrand, B.; Nordmark, B.; Wretenberg, P.; Stark, A. The foot: Still the most important reason for walking incapacity in rheumatoid arthritis—Distribution of symptomatic joints in 1000 RA patients. Acta Orthop. 2008, 79, 257–261. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.C.; Lee, S.H.; Lin, H.Y.; Liu, F.W.; Chiou, H.J.; Chan, R.C.; Chou, C.L. Short-term effect of ultrasound-guided low-molecular-weight hyaluronic acid injection on clinical outcomes and imaging changes in patients with rheumatoid arthritis of the ankle and foot joints. A randomized controlled pilot trial. Mod. Rheumatol. 2017, 27, 973–980. [Google Scholar] [CrossRef] [PubMed]
- Gijon-Nogueron, G.; Ramos-Petersen, L.; Ortega-Avila, A.B.; Morales-Asencio, J.M.; Garcia-Mayor, S. Effectiveness of foot orthoses in patients with rheumatoid arthritis related to disability and pain: A systematic review and meta-analysis. Qual. Life Res. 2018, 27, 3059–3069. [Google Scholar] [CrossRef] [PubMed]
- Blanco García, F.J. Manual SER de las Enfermedades Reumáticas; Alonso Ruíz, A., Gracia Álvaro, J.M.Á., Andreu Sánchez, J.L., Blanch, I., Rubió, J., Collantes Estévez, E., Cruz Martínez, J., Gratacós Masmitja, A., Laffón Roca, A., Martín Mola, E., Eds.; Buenos Aires: Madrid, Spain, 2004; ISBN 8479038594. [Google Scholar]
- Simon, M.J.K.; Strahl, A.; Mussawy, H.; Rolvien, T.; Schumacher, R.F.; Seller, M.; Rüther, W. Forefoot Reconstruction Following Metatarsal Head Resection Arthroplasty With a Plantar Approach—A 20-Year Follow-Up. Foot Ankle Int. 2019, 40, 769–777. [Google Scholar] [CrossRef] [PubMed]
- Tootle, K.; Hollnagel, J. Lou; Kinmon, K. Surgical Treatment of Severe Hallux Abductovalgus With Dislocation of the First Metatarsophalangeal Joint: A Case Presentation and Surgical Technique. Foot Ankle Spec. 2019, 12, 281–285. [Google Scholar] [CrossRef] [PubMed]
- Stewart, S.; Carroll, M.; Brenton-Rule, A.; Keys, M.; Bell, L.; Dalbeth, N.; Rome, K. Region-specific foot pain and plantar pressure in people with rheumatoid arthritis: A cross-sectional study. Clin. Biomech. 2018, 55, 14–27. [Google Scholar] [CrossRef]
- Triolo, P.; Rosso, F.; Rossi, R.; Cerlon, R.; Cottino, U.; Bonasia, D.E. Fusion of the First Metatarsophalangeal Joint and Second to Fifth Metatarsal Head Resection for Rheumatoid Forefoot Deformity. J. Foot Ankle Surg. 2017, 56, 263–270. [Google Scholar] [CrossRef]
- Rosenbaum, D.; Timte, B.; Schmiegel, A.; Miehlke, R.K.; Hilker, A. First Ray Resection Arthroplasty versus Arthrodesis in the Treatment of the Rheumatoid Foot. Foot Ankle Int. 2011, 32, 589–594. [Google Scholar] [CrossRef]
- Fazal, M.A.; Wong, J.H.M.; Rahman, L. First metatarsophalangeal joint arthrodesis with two orthogonal two hole plates. Acta Orthop. Traumatol. Turc. 2018, 52, 363–366. [Google Scholar] [CrossRef]
- Su, E.P.; Kahn, B.; Figgie, M.P. Total ankle replacement in patients with rheumatoid arthritis. Clin. Orthop. Relat. Res. 2004, 424, 32–38. [Google Scholar] [CrossRef]
- Pedersen, E.; Pinsker, E.; Younger, A.S.; Penner, M.J.; Wing, K.J.; Dryden, P.J.; Glazebrook, M.; Daniels, T.R. Outcome of Total Ankle Arthroplasty in Patients with Rheumatoid Arthritis and Noninflammatory Arthritis. J. Bone Jt. Surg. 2014, 96, 1768–1775. [Google Scholar] [CrossRef] [PubMed]
- Gong, J.; Zhou, B.; Tao, X.; Yuan, C.; Tang, K. Tibiotalocalcaneal arthrodesis with headless compression screws. J. Orthop. Surg. Res. 2016, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Van den Hoogen, F.H.; de Waal Malefijt, M.C. Total ankle prostheses in rheumatoid arthropathy Outcome in 52 patients followed for 1–9 years. Acta Orthop. 2009, 80, 440–444. [Google Scholar] [CrossRef]
- Dodd, L.; Atinga, M.; Foote, J.; Palmer, S. Outcomes after the Stainsby Procedure in the Lesser Toes: An Alternative Procedure for the Correction of Rigid Claw Toe Deformity. J. Foot Ankle Surg. 2011, 50, 522–524. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, 1–34. [Google Scholar] [CrossRef]
- Budiman-Mak, E.; Conrad, K.J.; Roach, K.E. The Foot Function Index: A Measure of Foot Pain and Disability. J. Clin. Epidemiol. 1991, 44, 561–570. [Google Scholar] [CrossRef]
- Kitaoka, H.B.; Alexander, I.J.; Adelaar, R.S.; A. Nunley, J.; Myerson, M.S.; Sanders, M.; Lutter, L.D. Clinical Rating Systems for the Ankle-Hindfoot, Midfoot, Hallux, and Lesser Toes. Foot Ankle Int. 1997, 18, 187–188. [Google Scholar] [CrossRef]
- Niki, H.; Aoki, H.; Inokuchi, S.; Ozeki, S.; Kinoshita, M.; Kura, H.; Tanaka, Y.; Noguchi, M.; Nomura, S.; Hatori, M.; et al. Development and reliability of a standard rating system for outcome measurement of foot and ankle disorders I: Development of standard rating system. J. Orthop. Sci. 2005, 10, 457–465. [Google Scholar] [CrossRef]
- Niki, H.; Aoki, H.; Inokuchi, S.; Ozeki, S.; Kinoshita, M.; Kura, H.; Tanaka, Y.; Noguchi, M.; Nomura, S.; Hatori, M.; et al. Development and reliability of a standard rating system for outcome measurement of foot and ankle disorders II: Interclinician and intraclinician reliability and validity of the newly established standard rating scales and Japanese Orthopaedic Association. J. Orthop. Sci. 2005, 10, 466–474. [Google Scholar] [CrossRef]
- Domsic, R.T.; Saltzman, C.L. Ankle osteoarthritis scale. Foot Ankle Int. 1998. [Google Scholar] [CrossRef]
- Walmsley, S.; Ravey, M.; Graham, A.; Teh, L.S.; Williams, A.E. Development of a patient-reported outcome measure for the foot affected by rheumatoid arthritis. J. Clin. Epidemiol. 2012, 65, 413–422. [Google Scholar] [CrossRef] [PubMed]
- Ware, J.E.; Sherbourne, C.D. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef] [PubMed]
- Fries, J.F.; Spitz, P.; Kraines, R.G.; Holman, H.R. Measurement of patient outcome in arthritis. Arthritis Rheum. 1980, 23, 137–145. [Google Scholar] [CrossRef] [PubMed]
- Slim, K.; Nini, E.; Forestier, D.; Kwiatkowski, F.; Panis, Y.; Chipponi, J. Methodological index for non-randomized studies (Minors): Development and validation of a new instrument. ANZ J. Surg. 2003, 73, 712–716. [Google Scholar] [CrossRef] [PubMed]
- Wells, G.; Shea, B.; O’Connell, D.; Peterson, J. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses; Ottawa Hospital Research Institute: Ottawa, ON, Canada, 2014. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. The PRISMA Group PRISMA 2009 Flow Diagram. PLoS Med. 2009. [Google Scholar] [CrossRef]
- Horita, M.; Nishida, K.; Hashizume, K.; Nasu, Y.; Saiga, K.; Nakahara, R.; Machida, T.; Ohashi, H.; Ozaki, T. Outcomes of Resection and Joint-Preserving Arthroplasty for Forefoot Deformities for Rheumatoid Arthritis. Foot Ankle Int. 2018, 39, 292–299. [Google Scholar] [CrossRef]
- Ebina, K.; Hirao, M.; Hashimoto, J.; Nampei, A.; Shi, K.; Tomita, T.; Futai, K.; Kunugiza, Y.; Noguchi, T.; Yoshikawa, H. Comparison of a self-administered foot evaluation questionnaire (SAFE-Q) between joint-preserving arthroplasty and resection-replacement arthroplasty in forefoot surgery for patients with rheumatoid arthritis. Mod. Rheumatol. 2017, 27, 795–800. [Google Scholar] [CrossRef]
- Fukushi, J.I.; Nakashima, Y.; Okazaki, K.; Yamada, H.; Mawatari, T.; Ohishi, M.; Oyamada, A.; Akasaki, Y.; Iwamoto, Y. Outcome of joint-preserving arthroplasty for rheumatoid forefoot deformities. Foot Ankle Int. 2016, 37, 262–268. [Google Scholar] [CrossRef]
- Bhavikatti, M.; Sewell, M.D.; Al-Hadithy, N.; Awan, S.; Bawarish, M.A. Joint preserving surgery for rheumatoid forefoot deformities improves pain and corrects deformity at midterm follow-up. Foot 2012. [Google Scholar] [CrossRef]
- Benoni, A.C.; Bremander, A.; Nilsdotter, A. Patient-reported outcome after rheumatoid arthritis-related surgery in the lower extremities: A report from the Swedish National Register of Rheuma Surgery (RAKIR). Acta Orthop. 2012, 83, 179–184. [Google Scholar] [CrossRef]
- Donegan, R.J.; Blume, P.A. Functional Results and Patient Satisfaction of First Metatarsophalangeal Joint Arthrodesis Using Dual Crossed Screw Fixation. J. Foot Ankle Surg. 2017, 56, 291–297. [Google Scholar] [CrossRef] [PubMed]
- Thomas, S.; Kinninmonth, A.W.G.; Kumar, C.S. Long-term results of the modified Hoffman procedure in the rheumatoid forefoot. J. Bone Jt. Surg. Ser. A 2005, 87, 748–752. [Google Scholar] [CrossRef] [PubMed]
- Reize, P.; Leichtle, C.I.; Leichtle, U.G.; Schanbacher, J. Long-term results after metatarsal head resection in the treatment of rheumatoid arthritis. Foot Ankle Int. 2006, 27, 586–590. [Google Scholar] [CrossRef]
- Hirao, M.; Ebina, K.; Tsuboi, H.; Nampei, A.; Kushioka, J.; Noguchi, T.; Tsuji, S.; Owaki, H.; Hashimoto, J.; Yoshikawa, H. Outcomes of modified metatarsal shortening offset osteotomy for forefoot deformity in patients with rheumatoid arthritis: Short to mid-term follow-up. Mod. Rheumatol. 2017, 27, 981–989. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).