Maintained Clinical Remission in Ankylosing Spondylitis Patients Switched from Reference Infliximab to Its Biosimilar: An 18-Month Comparative Open-Label Study
Abstract
:1. Introduction
2. Materials and Methods
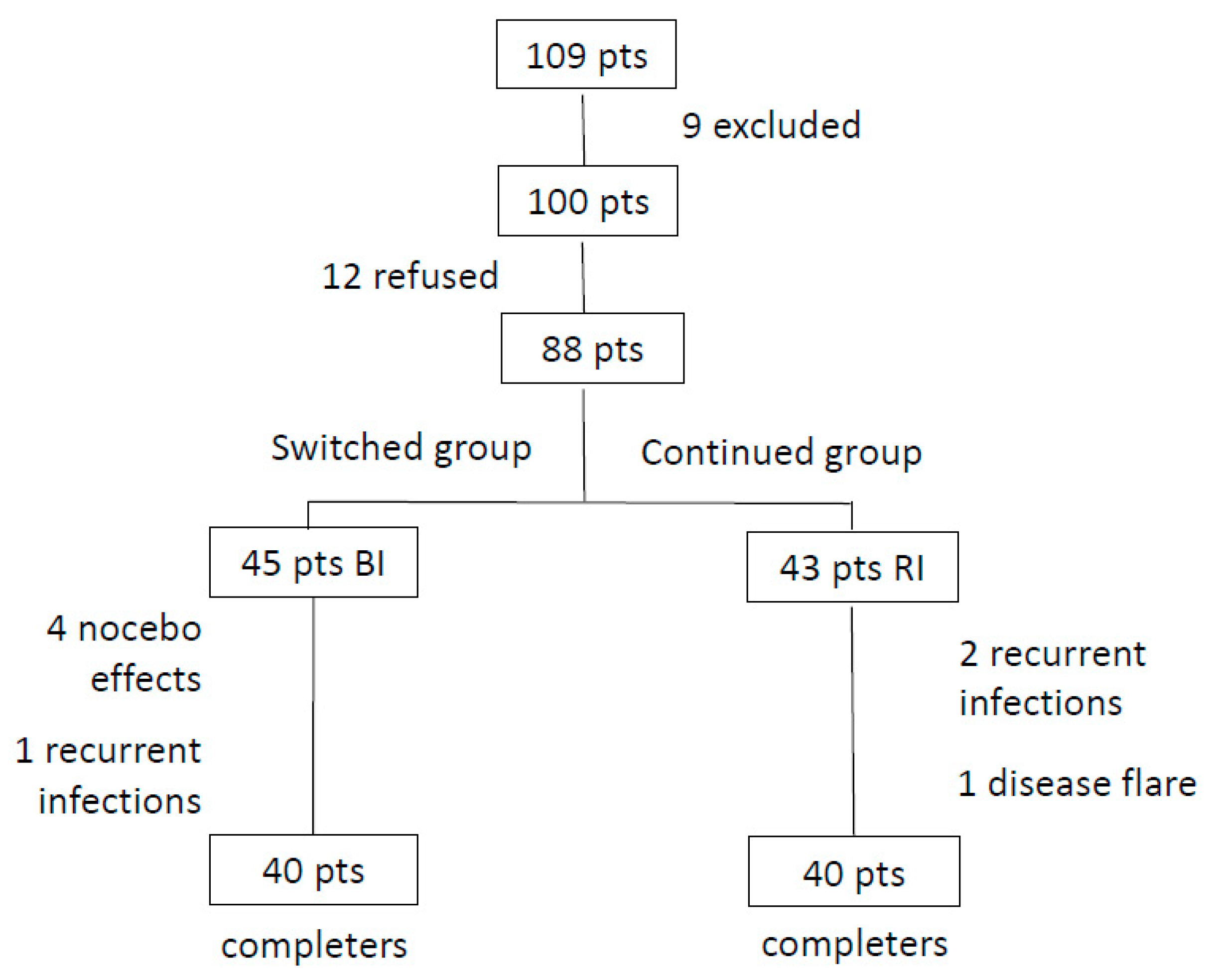
3. Results
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Dörner, T.; Kay, J. Biosimilars in rheumatology: Current perspectives and lessons learnt. Nat. Rev. Rheumatol. 2015, 11, 713–724. [Google Scholar] [CrossRef] [PubMed]
- Park, W.; Yoo, D.H.; Miranda, P.; Brzosko, M.; Wiland, P.; Gutierrez-Ureña, S.; Mikazane, H.; Lee, Y.A.; Smiyan, S.; Lim, M.J.; et al. Efficacy and safety of switching from reference infliximab to CT-P13 compared with maintenance of CT-P13 in ankylosing spondylitis: 102-week data from the PLANETAS extension study. Ann. Rheum. Dis. 2017, 76, 346–354. [Google Scholar] [CrossRef] [PubMed]
- Yoo, D.H.; Prodanovic, N.; Jaworski, J.; Miranda, P.; Ramiterre, E.; Lanzon, A.; Baranauskaite, A.; Wiland, P.; Abud-Mendoza, C.; Oparanov, B.; et al. Efficacy and safety of CT-P13 (biosimilar infliximab) in patients with rheumatoid arthritis: Comparison between switching from reference infliximab to CT-P13 and continuing CT-P13 in the PLANETRA extension study. Ann. Rheum. Dis. 2017, 76, 355–363. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, Y.; Yamanaka, H.; Takeuchi, T.; Inoue, M.; Saito, K.; Saeki, Y.; Lee, S.J.; Nambu, Y. Safety and efficacy of CT-P13 in Japanese patients with rheumatoid arthritis in an extension phase or after switching from infliximab. Mod. Rheumatol. 2017, 27, 237–245. [Google Scholar] [CrossRef] [PubMed]
- Scherlinger, M.; Germain, V.; Labadie, C.; Barnetche, T.; Truchetet, M.E.; Bannwarth, B.; Mehsen-Cetre, N.; Richez, C.; Schaeverbeke, T.; FHU ACRONIM. Switching from originator infliximab to biosimilar CT-P13 in real-life: The weight of patient acceptance. Joint Bone Spine. 2018, 85, 561–567. [Google Scholar] [CrossRef] [PubMed]
- Jones, A.; Ciurtin, C.; Ismajli, M.; Leandro, M.; Sengupta, R.; Machado, P.M. Biologics for treating axial spondyloarthritis. Expert Opin. Biol. Ther. 2018, 18, 641–652. [Google Scholar] [CrossRef] [PubMed]
- Calin, A.; Garrett, S.; Whitelock, H.; Kennedy, L.G.; O’Hea, J.; Mallorie, P.; Jenkinson, T. A new approach to defining functional ability in ankylosing spondylitis: The development of the Bath Ankylosing Spondylitis Functional Index. J. Rheumatol. 1994, 21, 2281–2285. [Google Scholar] [PubMed]
- Lukas, C.; Landewé, R.; Sieper, J.; Dougados, M.; Davis, J.; Braun, J.; van der Linden, S.; van der Heijde, D. Assessment of SpondyloArthritis international Society. Development of an ASAS-endorsed disease activity score (ASDAS) in patients with ankylosing spondylitis. Ann. Rheum. Dis. 2009, 68, 18–24. [Google Scholar] [CrossRef] [PubMed]
- Machado, P.; Landewé, R.; Lie, E.; Kvien, T.K.; Braun, J.; Baker, D.; van der Heijde, D.; Assessment of SpondyloArthritis international Society. Ankylosing Spondylitis Disease Activity Score (ASDAS): Defining cut-off values for disease activity states and improvement scores. Ann. Rheum. Dis. 2011, 70, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Blair, H.A.; Deeks, E.D. Infliximab Biosimilar (CT-P13; Infliximab-dyyb): A Review in Autoimmune Inflammatory Diseases. Bio Drugs. 2016, 30, 469–480. [Google Scholar] [CrossRef] [PubMed]
- Kay, J.; Schoels, M.M.; Dörner, T.; Emery, P.; Kvien, T.K.; Smolen, J.S.; Breedveld, F.C. Task Force on the Use of Biosimilars to Treat Rheumatological Diseases. Consensus-based recommendations for the use of biosimilars to treat rheumatological diseases. Ann. Rheum. Dis. 2018, 77, 165–174. [Google Scholar] [CrossRef] [PubMed]
- Jørgensen, K.K.; Olsen, I.C.; Goll, G.L.; Lorentzen, M.; Bolstad, N.; Haavardsholm, E.A.; Lundin, K.E.A.; Mørk, C.; Jahnsen, J.; Kvien, T.K.; et al. Switching from originator infliximab to biosimilar CT-P13 compared with maintained treatment with originator infliximab (NOR-SWITCH): A 52-week, randomised, double-blind, non-inferiority trial. Lancet 2017, 389, 2304–2316. [Google Scholar]
- Kravvariti, E.; Kitas, G.D.; Mitsikostas, D.D.; Sfikakis, P.P. Nocebos in rheumatology: Emerging concepts and their implications for clinical practice. Nat. Rev. Rheumatol. 2018, 14, 727–740. [Google Scholar] [CrossRef] [PubMed]
- Tweehuysen, L.; van den Bemt, B.J.F.; van Ingen, I.L.; de Jong, A.J.L.; van der Laan, W.H.; van den Hoogen, F.H.J.; den Broeder, A.A. Subjective Complaints as the Main Reason for Biosimilar Discontinuation After Open-Label Transition From Reference Infliximab to Biosimilar Infliximab. Arthritis Rheumatol. 2018, 70, 60–68. [Google Scholar] [CrossRef] [PubMed]
- Scherlinger, M.; Langlois, E.; Germain, V.; Schaeverbeke, T. Acceptance rate and sociological factors involved in the switch from originator to biosimilar etanercept (SB4). Semin. Arthritis Rheum. 2019, 48, 927–932. [Google Scholar] [CrossRef] [PubMed]
- Tweehuysen, L.; Huiskes, V.J.B.; van den Bemt, B.J.F.; Vriezekolk, J.E.; Teerenstra, S.; van den Hoogen, F.H.J.; van den Ende, C.H.; den Broeder, A.A. Open-Label, Non-Mandatory Transitioning From Originator Etanercept to Biosimilar SB4: Six-Month Results From a Controlled Cohort Study. Arthritis Rheumatol. 2018, 70, 1408–1418. [Google Scholar] [CrossRef] [PubMed]
- Lyman, G.H.; Zon, R.; Harvey, R.D.; Schilsky, R.L. Rationale, Opportunities, and Reality of Biosimilar Medications. N. Engl. J. Med. 2018, 378, 2036–2044. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Switched Group (BI) n:45 | Continued Group (RI) n:43 | p-Value |
|---|---|---|---|
| Mean age (years) (SD) | 36.1 (4.6) | 35.7 (4.3) | NS |
| Male/female | 39/6 | 40 (3) | NS |
| Mean disease duration (years) (SD) | 7.8 (3.0) | 7.6 (2.8) | NS |
| Mean follow-up (years) (SD) | 7.0 (1.1) | 6.9 (0.9) | NS |
| BMI (kgr/m2) >25 | 5 (11.1) | 4 (9.3) | NS |
| Current smokers n (%) | 10 (22.2) | 8 (18.6) | NS |
| Ex-smokers n (%) | 9 (20) | 9 (20.9) | NS |
| Mean treatment with BI/RI | 6.4 (0.9) | 6.5 (0.8) | NS |
| Mean treatment with RI and clinical remission (years) (SD) | 3.6 (0.8) | NS | |
| Axial disease n (%) | 45 (100) | 43 (100) | NS |
| Peripheral disease n (%) | 4 (9) | 3 (7) | NS |
| Methotrexate intake n (%) | 3 (7) | 2 (5) | NS |
| Mean BASDAI (SD) | 3.7 (0.2) | 3.6 (0.4) | NS |
| Mean ASDAS (SD) | 1.0 (0.2) | 1.1 (0.2) | NS |
| Mean ESR mm/h (SD) | 18.5 (2.2) | 19.3 (1.7) | NS |
| Mean CRP mg/L (SD) | 6.0 (0.8) | 5.8 (0.6) | NS |
| Parameters | Switched Group (BI) | Continued Group (RI) | p-Value |
|---|---|---|---|
| At switching | |||
| BASDAI (SD) | 3.7 (0.2) | 3.6 (0.4) | NS |
| ASDAS (SD) | 1.0 (0.2) | 1.1 (0.2) | NS |
| ESR mm/h (SD) | 18.5 (2.2) | 19.3 (1.7) | NS |
| CRP mg/l (SD) | 6.0 (0.8) | 5.8 (0.6) | NS |
| End of the study | |||
| BASDAI (SD) | 3.7 (0.4) | 3.8 (0.2) | N5 |
| ASDAS (SD) | 1.0 (0.2) | 1.1 (0.1) | NS |
| ESR mm/h (SD) | 19.5 (1.5) | 20.0 (1.6) | NS |
| CRP mg/l (SD) | 6.0 (1.0) | 6.1 (1.1) | NS |
| Adverse Events * n (%) | Switched Group (BI) | Continued Group (RI) | p-Value |
|---|---|---|---|
| Upper respiratory tract infections | 3 (6.6) | 2 (4.6) | NS |
| Urinary tract infections | 2 (4.4) | 2 (4.6) | NS |
| Skin infections | 2 (2.2) | 1 (2.3) | NS |
| Increased liver enzymes | 2 (4.4) | 2 (4.6) | NS |
| Diarrhea | 1 (2.2) | 2 (4.6) | NS |
| Viral infections | 2 (4.4) | 1 (2.3) | NS |
| Headache | 1 (2.2) | 0 (0) | NS |
| Hypertension | 1 (2.2) | 1 (2.3) | NS |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kaltsonoudis, E.; Pelechas, E.; Voulgari, P.V.; Drosos, A.A. Maintained Clinical Remission in Ankylosing Spondylitis Patients Switched from Reference Infliximab to Its Biosimilar: An 18-Month Comparative Open-Label Study. J. Clin. Med. 2019, 8, 956. https://doi.org/10.3390/jcm8070956
Kaltsonoudis E, Pelechas E, Voulgari PV, Drosos AA. Maintained Clinical Remission in Ankylosing Spondylitis Patients Switched from Reference Infliximab to Its Biosimilar: An 18-Month Comparative Open-Label Study. Journal of Clinical Medicine. 2019; 8(7):956. https://doi.org/10.3390/jcm8070956
Chicago/Turabian StyleKaltsonoudis, Evripidis, Eleftherios Pelechas, Paraskevi V. Voulgari, and Alexandros A. Drosos. 2019. "Maintained Clinical Remission in Ankylosing Spondylitis Patients Switched from Reference Infliximab to Its Biosimilar: An 18-Month Comparative Open-Label Study" Journal of Clinical Medicine 8, no. 7: 956. https://doi.org/10.3390/jcm8070956
APA StyleKaltsonoudis, E., Pelechas, E., Voulgari, P. V., & Drosos, A. A. (2019). Maintained Clinical Remission in Ankylosing Spondylitis Patients Switched from Reference Infliximab to Its Biosimilar: An 18-Month Comparative Open-Label Study. Journal of Clinical Medicine, 8(7), 956. https://doi.org/10.3390/jcm8070956




