Sexual Satisfaction and Mental Health in Prison Inmates
Abstract
1. Introduction
1.1. The Sexual Satisfaction and Mental Health Relationship Moderated by Partner Status and Sexual Abstinence
1.1.1. Research Conducted Outside Prisons
1.1.2. Research Conducted in Prison Contexts
1.1.3. Research Questions
2. Experimental Section
2.1. Participants
2.2. Design and Procedure
2.3. Measures
2.3.1. Sexual Satisfaction
2.3.2. Moderating Variables: Sexual Activity Level and Partner Status
2.3.3. Outcome Variable: Mental Health
2.3.4. Control Variables: Sociodemographic, Penitentiary, and Personal, Social, and Sexual Well-Being Variables
2.4. Statistical Analysis
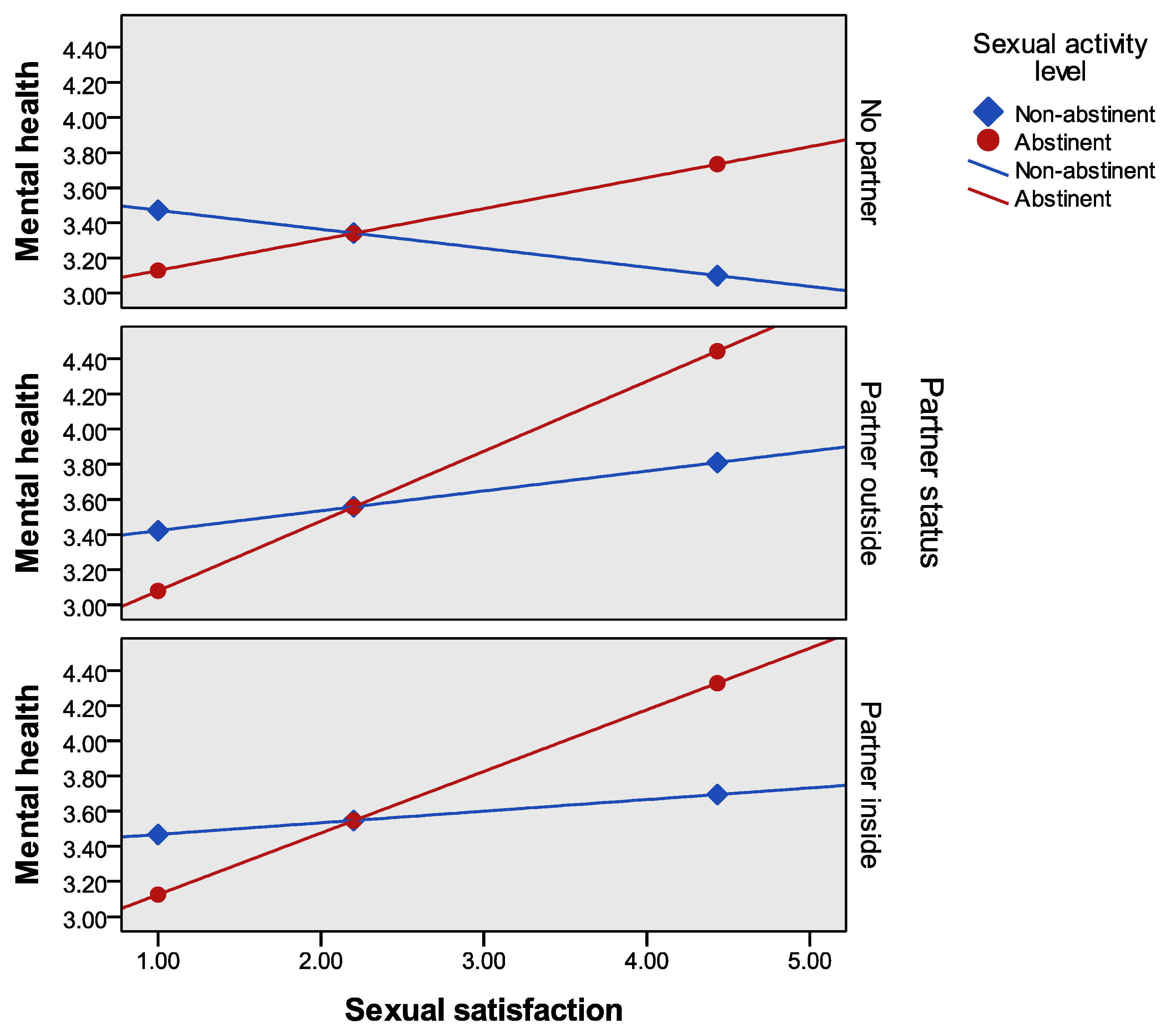
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Walmsley, R. World Prison Population List; International Center for Prison Studies: London, UK, 2013.
- Chang, Z.; Larsson, H.; Lichtenstein, P.; Fazel, S. Psychiatric disorders and violent reoffending: A national cohort study of convicted prisoners in Sweden. Lancet Psychiatry 2015, 2, 891–900. [Google Scholar] [CrossRef]
- Schildbach, C.; Schildbach, S. Yield and efficiency of mental disorder screening at intake to prison: A comparison of DIA-X short-and long-screening-protocols in compensation prisoners. Front. Psychiatry 2018, 9, 538. [Google Scholar] [CrossRef]
- Alevizopoulos, G.; Igoumenou, A. Psychiatric disorders and criminal history in male prisoners in Greece. Int. J. Law Psychiatry 2016, 47, 171–175. [Google Scholar] [CrossRef]
- Daquin, J.C.; Daigle, L.E. Mental disorder and victimisation in prison: Examining the role of mental health treatment. Crim. Behav. Ment. Health 2018, 28, 141–151. [Google Scholar] [CrossRef]
- Fazel, S.; Danesh, J. Serious mental disorder in 23000 prisoners: A systematic review of 62 surveys. Lancet 2002, 359, 545–550. [Google Scholar] [CrossRef]
- White, L.M.; Lau, K.S.L.; Aalsma, M.C. Detained adolescents: Mental health needs, treatment use, and recidivism. J. Am. Acad. Psychiatry Law 2016, 44, 200–212. [Google Scholar] [PubMed]
- Vicens, E.; Tort, V.; Dueñas, R.M.; Muro, A.; Pérez-Arnau, F.; Arroyo, J.M.; Acín, E.; de Vicente, A.; Guerrero, R.; Lluch, J.; et al. The prevalence of mental disorders in Spanish prisons. Crim. Behav. Ment. Health 2011, 21, 321–332. [Google Scholar] [CrossRef] [PubMed]
- Zabala-Baños, M.C.; Segura, A.; Maestre-Miquel, C.; Martínez-Lorca, M.; Rodríguez-Martín, B.; Romero, D.; Rodríguez, M. Prevalencia de trastorno mental y factores de riesgo asociados en tres prisiones de España [Mental disorder prevalence and associated risk factors in three prisons of Spain]. Rev. Esp. Sanid. Penit. 2016, 18, 13–23. [Google Scholar] [CrossRef] [PubMed]
- Hawton, K.; Linsell, L.; Adeniji, T.; Sariaslan, A.; Fazel, S. Self-harm in prisons in England and Wales: An epidemiological study of prevalence, risk factors, clustering, and subsequent suicide. Lancet 2014, 383, 1147–1154. [Google Scholar] [CrossRef]
- Fazel, S.; Cartwright, J.; Norman-Nott, A.; Hawton, K. Suicide in prisoners: A systematic review of risk factors. J. Clin. Psychiatry 2008, 69, 1721–1731. [Google Scholar] [CrossRef]
- Fazel, S.; Grann, M.; Kling, B.; Hawton, K. Prison suicide in 12 countries: An ecological study of 861 suicides during 2003–2007. Soc. Psychiatry Psychiatr. Epidemiol. 2011, 46, 191–195. [Google Scholar] [CrossRef]
- Haglund, A.; Tidemalm, D.; Jokinen, J.; Långström, N.; Liechtenstein, P.; Fazel, S.; Runeson, B. Suicide after release from prison-a population-based cohort study from Sweden. J. Clin. Psychiatry 2014, 75, 1047. [Google Scholar] [CrossRef]
- Pratt, D.; Piper, M.; Appleby, L.; Webb, R.; Shaw, J. Suicide in recently released prisoners: A population-based cohort study. Lancet 2006, 368, 119–123. [Google Scholar] [CrossRef]
- Rivlin, A.; Hawton, K.; Marzano, L.; Fazel, S. Psychiatric disorders in male prisoners who made near-lethal suicide attempts: Case–control study. Br. J. Psychiatry 2010, 197, 313–319. [Google Scholar] [CrossRef]
- Verona, E.; Hicks, B.M.; Patrick, C.J. Psychopathy and suicidality in female offenders: Mediating influences of personality and abuse. J. Consult. Clin. Psychol. 2005, 73, 1065. [Google Scholar] [CrossRef] [PubMed]
- Gonçalves, L.C.; Gonçalves, R.A.; Martins, C.; Dirkzwager, A.J. Predicting infractions and health care utilization in prison: A meta-analysis. Crim. Justice Behav. 2014, 41, 921–942. [Google Scholar] [CrossRef]
- Baillargeon, J.; Binswanger, I.A.; Penn, J.V.; Williams, B.A.; Murray, O.J. Psychiatric disorders and repeat incarcerations: The revolving prison door. Am. J. Psychiatry 2009, 166, 103–109. [Google Scholar] [CrossRef]
- Shaffer, H.J.; Nelson, S.E.; LaPlante, D.A.; LaBrie, R.A.; Albanese, M.; Caro, G. The epidemiology of psychiatric disorders among repeat DUI offenders accepting a treatment-sentencing option. J. Consult. Clin. Psychol. 2007, 75, 795. [Google Scholar] [CrossRef]
- Fazel, S.; Hayes, A.J.; Bartellas, K.; Clerici, M.; Trestman, R. Mental health of prisoners: Prevalence, adverse outcomes, and interventions. Lancet Psychiatry 2016, 3, 871–881. [Google Scholar] [CrossRef]
- Kaeble, D.; Glaze, L.; Tsoutis, A.; Minton, T. Correctional Populations in the United States; NCJ 249513; U.S. Department of Justice: Washington, DC, USA, September 2015.
- Porter, L.C.; DeMarco, L.M. Beyond the dichotomy: Incarceration dosage and mental health. Criminology 2019, 57, 136–156. [Google Scholar] [CrossRef]
- Toch, H. Living in Prison: The Ecology of Survival; Free Press: New York, NY, USA, 1977. [Google Scholar]
- Zamble, E.; Porporino, F.J. Coping, Behavior, and Adaptation in Prison Inmates; Springer-Verlag Publishing: New York, NY, USA, 1988. [Google Scholar]
- Sykes, G.M. The Society of Captives: A Study of a Maximum Security Prison; Princeton University Press: Princeton, NJ, USA, 2007. Original work published 1958. [Google Scholar]
- Massoglia, M. Incarceration as exposure: The prison, infectious disease, and other stress-related illnesses. J. Health Soc. Behav. 2008, 49, 56–71. [Google Scholar] [CrossRef]
- Western, B. Punishment and Inequality in America; Russell Sage Foundation: New York, NY, USA, 2006. [Google Scholar]
- Lopoo, L.M.; Western, B. Incarceration and the formation and stability of marital unions. J. Marriage Fam. 2005, 67, 721–734. [Google Scholar] [CrossRef]
- Allen, S.A.; Wakeman, S.E.; Cohen, R.L.; Rich, J.D. Physicians in US prisons in the era of mass incarceration. Int. J. Prison Health 2010, 6, 100. [Google Scholar]
- Durcan, G.; Zwemstra, J.C. Mental health in prison. In Prisons and Health; Enggist, S., Møller, L., Galea, G., Udesen, U., Eds.; WHO Regional Office for Europe: Copenhagen, Denmark, 2014; pp. 87–95. [Google Scholar]
- King, M.; Nazareth, I.; Levy, G.; Walker, C.; Morris, R.; Weich, S.; Bellón-Saameño, J.A.; Moreno, B.; Svab, I.; Rotar, D.; et al. Prevalence of common mental disorders in general practice attendees across Europe. Br. J. Psychiatry 2008, 192, 362–367. [Google Scholar] [CrossRef]
- Carcedo, R.J. Necesidades Sociales, Emocionales y Sexuales: Estudio en un Centro Penitenciario [Social, Emotional, and Sexual Needs: Study in a Penitentiary]; Servicio de Publicaciones de la Universidad de Salamanca: Salamanca, Spain, 2005. [Google Scholar]
- Levenson, L. Sexual attitudes of males in a protected environment. J. Am. Soc. Psychosom. Dent. Med. 1983, 30, 135–136. [Google Scholar]
- Maeve, M.K. The social construction of love and sexuality in a women’s prison. ANS Adv. Nurs. Sci. 1999, 21, 46–65. [Google Scholar] [CrossRef] [PubMed]
- Neuman, E. El Problema Sexual en las Cárceles [The Sexual Problem in Prisons]; Editorial Universidad: Buenos Aires, Argentina, 1982. [Google Scholar]
- Linville, S.L. Assessing Sexual Attitudes and Behaviors of Incarcerated Males in a Minimum Security Institution; West Virginia University: Morgantown, WV, USA, 1981. [Google Scholar]
- Worley, R.M.; Worley, V. Inmate public autoerotism uncovered: Exploring the dynamics of masturbatory behavior within correctional facilities. Deviant Behav. 2013, 34, 11–24. [Google Scholar] [CrossRef]
- Hensley, C.; Tewksbury, R.; Koscheski, M. Masturbation uncovered: Autoeroticism in a female prison. Prison J. 2001, 81, 491–501. [Google Scholar] [CrossRef]
- Hensley, C.; Tewksbury, R.; Wright, J. Exploring the dynamics of masturbation and consensual same-sex activity within a male maximum security prison. J. Men’s Stud. 2001, 10, 59–71. [Google Scholar] [CrossRef]
- Marcum, C.D. Examining prison sex culture. In Sex in Prison: Myths and Realities; Marcum, C.D., Castle, T.L., Eds.; Lynne Rienner: London, UK, 2014; pp. 1–12. [Google Scholar]
- Fleisher, M.S.; Krienert, J.L. The Myth of Prison Rape: Sexual Culture in American Prisons; Rowman and Littlefield: New York, NY, USA, 2009. [Google Scholar]
- Levan, K. Consensual sex. In Sex in Prison: Myths and Realities; Marcum, C.D., Castle, T.L., Eds.; Lynne Rienner: London, UK, 2014; pp. 13–24. [Google Scholar]
- Beck, A.J.; Harrison, P. Sexual Victimization in Prisons and Jails Reported by Inmates, 2008–2009 (NCJ No. 231169); US Department of Justice, Office of Justice Programs: Washington, DC, USA, 2010.
- Caravaca-Sánchez, F.; Wolff, N. Prevalence and Predictors of Sexual Victimization Among Incarcerated Men and Women in Spanish Prisons. Crim. Justice Behav. 2016, 43, 977–991. [Google Scholar] [CrossRef]
- Tewksbury, R.; Connor, D.P. Sexual victimization. In Sex in Prison: Myths and Realities; Marcum, C.D., Castle, T.L., Eds.; Lynne Rienner: London, UK, 2014; pp. 25–51. [Google Scholar]
- Potter, R.H.; Rosky, J. Health issues. In Sex in Prison: Myths and Realities; Marcum, C.D., Castle, T.L., Eds.; Lynne Rienner: London, UK, 2014; pp. 25–51. [Google Scholar]
- D’Alessio, S.J.; Flexon, J.; Stolzenberg, L. The effect of conjugal visitation on sexual violence in prison. Am. J. Crim. Justice 2013, 38, 13–26. [Google Scholar] [CrossRef]
- Carcedo, R.J.; Perlman, D.; Orgaz, M.B.; López, F.; Fernández-Rouco, N.; Faldowski, R.A. Heterosexual romantic relationships inside of prison: Partner status as predictor of loneliness, sexual satisfaction, and quality of life. Int. J. Offender Ther. Comp. Criminol. 2011, 55, 898–924. [Google Scholar] [CrossRef]
- Byers, E.S.; Demmons, S.; Lawrance, K. Sexual satisfaction within dating relationships: A test of the interpersonal exchange model of sexual satisfaction. J. Soc. Pers. Relatsh. 1998, 15, 257–267. [Google Scholar] [CrossRef]
- Carcedo, R.J.; Perlman, D.; López, F.; Orgaz, M.B. Heterosexual romantic relationships, interpersonal needs, and quality of life in prison. Span. J. Psychol. 2012, 15, 187–198. [Google Scholar] [CrossRef]
- Carcedo, R.J.; Perlman, D.; López, F.; Orgaz, M.B.; Fernández-Rouco, N. The relationship between sexual satisfaction and psychological health of prison inmates. Prison J. 2015, 95, 43–65. [Google Scholar] [CrossRef]
- Sánchez-Fuentes, M.M.; Santos-Iglesias, P.; Sierra, J.C. A systematic review of sexual satisfaction. Int. J. Clin. Health Psychol. 2014, 14, 67–75. [Google Scholar] [CrossRef]
- Shindel, A.W.; Eisenberg, M.L.; Breyer, B.N.; Sharlip, I.D.; Smith, J.F. Sexual function and depressive symptoms among female North American medical students. J. Sex. Med. 2011, 8, 391–399. [Google Scholar] [CrossRef] [PubMed]
- Davison, S.L.; Bell, R.J.; LaChina, M.; Holden, S.L.; Davis, S.R. The relationship between self-reported sexual satisfaction and general well-being in women. J. Sex. Med. 2009, 6, 2690–2697. [Google Scholar] [CrossRef] [PubMed]
- Stephenson, K.R.; Meston, C.M. The conditional importance of sex: Exploring the association between sexual well-being and life satisfaction. J. Sex Marital Ther. 2015, 41, 25–38. [Google Scholar] [CrossRef]
- Cohen, J.N.; Byers, E.S. Beyond lesbian bed death: Enhancing our understanding of the sexuality of sexual-minority women in relationships. J. Sex Res. 2014, 51, 893–903. [Google Scholar] [CrossRef] [PubMed]
- De Ryck, I.; Van Laeken, D.; Nöstlinger, C.; Platteau, T.; Colebunders, R. Sexual satisfaction among men living with HIV in Europe. AIDS Behav. 2012, 16, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Fuentes, M.; Sierra, J.C. Sexual satisfaction in a heterosexual and homosexual Spanish sample: The role of socio-demographic characteristics, health indicators, and relational factors. Sex. Relatsh. Ther. 2015, 30, 226–242. [Google Scholar] [CrossRef]
- Holmberg, D.; Blair, K.L.; Phillips, M. Women’s sexual satisfaction as a predictor of well-being in same-sex versus mixed-sex relationships. J. Sex Res. 2010, 47, 1–11. [Google Scholar] [CrossRef]
- Totenhagen, C.J.; Butler, E.A.; Ridley, C.A. Daily stress, closeness, and satisfaction in gay and lesbian couples. Pers. Relatsh. 2012, 19, 219–233. [Google Scholar] [CrossRef]
- Priebe, S.; Reininghaus, U.; McCabe, R.; Burns, T.; Eklund, M.; Hansson, L.; Junghan, U.; Kallert, T.; van Nieuwenhuizen, C.; Ruggeri, M.; et al. Factors influencing subjective quality of life in patients with schizophrenia and other mental disorders: A pooled analysis. Schizophr. Res. 2010, 121, 251–258. [Google Scholar] [CrossRef] [PubMed]
- Mallis, D.; Moisidis, K.; Kirana, P.S.; Papaharitou, S.; Simos, G.; Hatzichristou, D. Psychology: Moderate and severe erectile dysfunction equally affects life satisfaction. J. Sex. Med. 2006, 3, 442–449. [Google Scholar] [CrossRef]
- Field, N.; Mercer, C.H.; Sonnenberg, P.; Tanton, C.; Clifton, S.; Mitchell, K.R.; Erens, B.; Macdowall, W.; Wu, F.; Datta, J. Associations between health and sexual lifestyles in Britain: Findings from the third National Survey of Sexual Attitudes and Lifestyles (Natsal-3). Lancet 2013, 382, 1830–1844. [Google Scholar] [CrossRef]
- Laxhman, N.; Greenberg, L.; Priebe, S. Satisfaction with sex life among patients with schizophrenia. Schizophr. Res. 2017, 190, 63–67. [Google Scholar] [CrossRef]
- Træen, B.; Štulhofer, A.; Janssen, E.; Carvalheira, A.A.; Hald, G.M.; Lange, T.; Graham, C. Sexual activity and sexual satisfaction among older adults in four European countries. Arch. Sex. Behav. 2019, 48, 815–829. [Google Scholar] [CrossRef]
- Kawachi, I.; Berkman, L.F. Social ties and mental health. J. Urban Health 2001, 78, 458–467. [Google Scholar] [CrossRef] [PubMed]
- Holt-Lunstad, J.; Birmingham, W.; Jones, B.Q. Is there something unique about marriage? The relative impact of marital status, relationship quality, and network social support on ambulatory blood pressure and mental health. Ann. Behav. Med. 2008, 35, 239–244. [Google Scholar] [CrossRef]
- Waite, L.; Gallagher, M. The Case for Marriage: Why Married People Are Happier, Healthier and Better Off Financially; Broadway Books: New York, NY, USA, 2002. [Google Scholar]
- Proulx, C.M.; Helms, H.M.; Buehler, C. Marital quality and personal well-being: A meta-analysis. J. Marriage Fam. 2007, 69, 576–593. [Google Scholar] [CrossRef]
- Lau, J.T.F.; Wang, Q.; Cheng, Y.; Yang, X. Prevalence and risk factors of sexual dysfunction among younger married men in a rural area in China. Urology 2005, 66, 616–622. [Google Scholar] [CrossRef]
- Ventegodt, S. Sex and quality of life in Denmark. Arch. Sex. Behav. 1998, 27, 295–307. [Google Scholar] [CrossRef]
- Taleporos, G.; McCabe, M.P. The impact of sexual esteem, body esteem, and sexual satisfaction on psychological well-being in people with physical disability. Sex. Disabil. 2002, 20, 177–183. [Google Scholar] [CrossRef]
- Walters, A.S.; Williamson, G.M. Sexual satisfaction predicts quality of life: A study of adult amputees. Sex. Disabil. 1998, 16, 103–115. [Google Scholar] [CrossRef]
- Fegg, M.J.; Gerl, A.; Vollmer, T.C.; Gruber, U.; Jost, C.; Meiler, S.; Hiddemann, W. Subjective quality of life and sexual functioning after germ-cell tumour therapy. Br. J. Cancer 2003, 89, 2202–2206. [Google Scholar] [CrossRef]
- López, F. Necesidades en la Infancia y en la Adolescencia. Respuesta Familiar, Escolar y Social [Needs in Childhood and Adolescence. Family, School and Social Response]; Pirámide: Madrid, Spain, 2008. [Google Scholar]
- Demir, M.; Tyrell, F. Friendship and well-being among young adults with/out a romantic partner. In Proceedings of the International Association of Relationship Research Conference, Providence, RI, USA, 17–20 July 2008. [Google Scholar]
- Laumann, E.O.; Paik, A.; Glasser, D.B.; Kang, J.H.; Wang, T.; Levinson, B.; Moreira, E.D., Jr.; Nicolosi, A.; Gingell, C. A cross-national study of subjective sexual well-being among older women and men: Findings from the Global Study of Sexual Attitudes and Behaviors. Arch. Sex. Behav. 2006, 35, 143–159. [Google Scholar] [CrossRef]
- Carcedo, R.J.; Perlman, D.; López, F.; Orgaz, M.B.; Toth, K.; Fernández-Rouco, N. Men and women in the same prison: Interpersonal needs and psychological health of prison inmates. Int. J. Offender Ther. Comp. Criminol. 2008, 52, 641–657. [Google Scholar] [CrossRef]
- Sánchez, M.G. La Abstinencia Sexual Forzosa de las Reclusas en los Establecimientos Carcelarios de Venezuela [Forced Sexual Abstinence of Female Prison Inmates in Venezuela]; Composición Comput: Coro, Venezuela, 1995. [Google Scholar]
- Lindquist, C.H. Social integration and mental well-being among jail inmates. Sociol. Forum. 2000, 15, 431–455. [Google Scholar] [CrossRef]
- Lindquist, C.H.; Lindquist, C.A. Gender differences in distress: Mental health consequences of environmental stress among jail inmates. Behav. Sci. Law 1997, 15, 503–523. [Google Scholar] [CrossRef]
- James, D.J.; Glaze, L.E. Bureau of Justice Statistics Special Report: Mental Health Problems of Prison and Jail Inmates; US Department of Justice: Washington, DC, USA, 2006.
- McDonald, B.; Kulkarni, M.; Andkhoie, M.; Kendall, J.; Gall, S.; Chelladurai, S.; Yaghoubi, M.; McClean, S.; Szafron, M.; Farag, M. Determinants of self-reported mental health and utilization of mental health services in Canada. Int. J. Ment. Health 2017, 46, 299–311. [Google Scholar] [CrossRef]
- Brody, S. The relative health benefits of different sexual activities. J. Sex. Med. 2010, 7, 1336–1361. [Google Scholar] [CrossRef]
- Costa, R.M. Masturbation is related to psychopathology and prostate dysfunction: Comment on Quinsey. Arch. Sex. Behav. 2012, 41, 539–540. [Google Scholar] [CrossRef]
- Das, A. Masturbation in the United States. J. Sex. Marital Ther. 2007, 33, 301–317. [Google Scholar] [CrossRef]
- Snell, W.E. The Multidimensional Sexual Self-Concept Questionnaire. In Handbook of Sexuality Related Measures; Davis, C.M., Yarber, W.L., Bauserman, R., Schreer, G., Davis, S.L., Eds.; Sage: Riverside County, CA, USA, 1995; pp. 521–527. [Google Scholar]
- Lucas, R. Versión Española del WHOQOL [Spanish Version of WHOQOL]; Ergón: Madrid, Spain, 1998. [Google Scholar]
- Skevington, S.M.; McCrate, F.M. Expecting a good quality of life in health: Assessing people with diverse diseases and conditions using the WHOQOL-BREF. Health Expect. 2012, 15, 49–62. [Google Scholar] [CrossRef] [PubMed]
- Jylhä, M. What is self-rated health and why does it predict mortality? Towards a unified conceptual model. Soc. Sci. Med. 2009, 69, 307–316. [Google Scholar] [CrossRef]
- Ditommaso, E.; Brannen, C.; Best, L.A. Measurement and validity characteristics of the short version of the social and emotional loneliness scale for adults. Educ. Psychol. Meas. 2004, 64, 99–119. [Google Scholar] [CrossRef]
- Daryanto, A. Heteroskedasticity Test for SPSS (2nd Version). 2018. Available online: https://sites.google.com/site/ahmaddaryanto/scripts/Heterogeneity-test (accessed on 28 January 2018).
- Hayes, A.F.; Little, T.D. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach, 2nd ed.; Guilford Press: New York, NY, USA, 2018. [Google Scholar]
- Davidson, R.; MacKinnon, J. Estimation and Inference in Econometrics; Oxford University Press: Oxford, UK, 1993. [Google Scholar]
- Bushman, B.J.; Bonacci, A.M.; Van Dijk, M.; Baumeister, R.F. Narcissism, sexual refusal, and aggression: Testing a narcissistic reactance model of sexual coercion. J. Pers. Soc. Psych. 2003, 84, 1027. [Google Scholar] [CrossRef]
- Brehm, J.W. A Theory of Psychological Reactance; Academic Press: New York, NY, USA, 1966. [Google Scholar]
- Brehm, S.S.; Brehm, J.W. Psychological Reactance: A Theory of Freedom and Control; Academic Press: New York, NY, USA, 1981. [Google Scholar]
- Baumeister, R.F.; Bratslavsky, E.; Finkenauer, C.; Vohs, K.D. Bad is stronger than good. Rev. Gen. Psychol. 2001, 5, 323–370. [Google Scholar] [CrossRef]
- Paolini, S.; McIntyre, K. Bad is stronger than good for stigmatized, but not admired outgroups: Meta-analytical tests of intergroup valence asymmetry in individual-to-group generalization experiments. Pers. Soc. Psych. Rev. 2019, 23, 3–47. [Google Scholar] [CrossRef] [PubMed]
- Wright, E.M.; Salisbury, E.J.; Van Voorhis, P. Predicting the prison misconducts of women offenders: The importance of gender-responsive needs. J. Contemp. Crim. Justice 2007, 23, 310–340. [Google Scholar] [CrossRef]
- Gendreau, P.; Little, T.; Goggin, C. A meta-analysis of the predictors of adult offender recidivism: What works! Criminology 1996, 34, 575–608. [Google Scholar] [CrossRef]
- Vallerand, R.J. From motivation to passion: In search of the motivational processes involved in a meaningful life. Can. Psychol. 2012, 53, 42–52. [Google Scholar] [CrossRef]
- Fernández-Rouco, N.; Carcedo, R.J.; Yeadon-Lee, T. Transgender Identities, Pressures and Social Policy: A Study Carried Out in Spain. J. Homosex. 2018, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Hefner, M.K. Queering Prison Masculinity: Exploring the Organization of Gender and Sexuality within Men’s Prison. Men Masc. 2018, 21, 230–253. [Google Scholar] [CrossRef]
| Mean | SD | %(1) | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11a | 11b | 11c | 12 | 13 | 14 | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Sex (0 = male; 1 = female) | 50.673 | 0.032 | −0.033 | −0.348 *** | 0.102 | −0.019 | −0.259 *** | −0.070 | −0.257 *** | −0.485 *** | −0.199 ** | 0.002 | 0.192 ** | −0.364 *** | 0.264 *** | 0.048 | |||
| 2. Age | 35.172 | 7.822 | −0.108 | 0.156 * | 0.006 | −0.164 * | 0.098 | −0.027 | −0.074 | −0.146 * | 0.006 | 0.074 | −0.074 | 0.054 | 0.072 | −0.014 | |||
| 3. Nationality (0 = Spanish; 1 = foreigner) | 53.812 | −0.269 *** | 0.016 | 0.014 | 0.089 | 0.029 | 0.057 | 0.046 | 0.021 | 0.044 | −0.061 | 0.120 | −0.059 | 0.163 * | |||||
| 4. Total time in prison | 54.337 | 48.623 | −0.020 | −0.010 | 0.178 ** | 0.165 * | 0.139 * | 0.265 *** | −0.162 * | −0.204 ** | 0.029 | 0.176 ** | −0.125 | −0.041 | |||||
| 5. Time to parole | 19.878 | 21.763 | −0.088 | 0.029 | 0.025 | 0.001 | −0.062 | −0.081 | 0.082 | 0.004 | −0.018 | 0.055 | −0.141 * | ||||||
| 6. Self-rated health | 3.466 | 1.280 | −0.165 ** | −0.086 | −0.148 * | 0.053 | −0.085 | −0.106 | 0.180 ** | −0.050 | 0.096 | 0.300 *** | |||||||
| 7. Social loneliness | 3.479 | 1.790 | 0.317 *** | 0.274 *** | 0.160 * | 0.233 *** | −0.042 | −0.189 ** | 0.265 *** | −0.211 ** | −0.371 *** | ||||||||
| 8. Family loneliness | 2.175 | 1.690 | 0.086 | 0.132 * | 0.118 | −0.098 | −0.026 | 0.101 | 0.017 | −0.090 | |||||||||
| 9. Romantic loneliness | 4.034 | 2.111 | 0.104 | 0.826 *** | −0.245 *** | −0.579 *** | 0.547 *** | −0.563 *** | −0.198 ** | ||||||||||
| 10. Masturbation frequency | 2.740 | 1.403 | 0.147 * | −0.181 ** | 0.022 | 0.143 * | −0.122 | 0.063 | |||||||||||
| 11a. No partner (0 = other; 1 = no partner) | 34.081 | −0.441 *** | −0.570 *** | 0.600 *** | −0.449 *** | −0.164 * | |||||||||||||
| 11b. Partner inside (0 = other; 1 = partner inside) | 38.565 | −0.486 *** | −0.094 | 0.010 | −0.024 | ||||||||||||||
| 11c. Partner outside (0 = other; 1 = partner outside) | 27.354 | −0.499 *** | 0.428 *** | 0.181 ** | |||||||||||||||
| 12. Sexual activity level (0 = active; 1 = abstinent) | 45.291 | −0.611 *** | −0.252 *** | ||||||||||||||||
| 13. Sexual satisfaction | 2.483 | 3.449 | 0.309 *** | ||||||||||||||||
| 14. Mental health | 1.467 | 0.724 |
| Mental Health | ||||
|---|---|---|---|---|
| B | SE | t | 95% CI | |
| Sociodemographic and penitentiary variables | ||||
| Sex | −0.043 | 0.117 | −0.366 | (−0.273, 0.188) |
| Age | 0.008 | 0.006 | 1.252 | (−0.005, 0.021) |
| Nationality | 0.359 | 0.092 | 3.899 *** | (0.178, 0.541) |
| Total time in prison | 0.001 | 0.001 | 0.996 | (−0.001, 0.003) |
| Time to parole | −0.004 | 0.002 | −2.092 * | (−0.008, 0.001) |
| Personal, social, and sexual well-being variables | ||||
| Self-rated health | 0.133 | 0.036 | 3.685 *** | (0.062, 0.204) |
| Social loneliness | −0.13 | 0.028 | −4.592 *** | (−0.186, −0.074) |
| Family loneliness | −0.002 | 0.027 | −0.072 | (−0.056, 0.052) |
| Romantic loneliness | 0.030 | 0.05 | 0.597 | (−0.069, 0.129) |
| Masturbation frequency | 0.058 | 0.038 | 1.515 | (−0.017, 0.133) |
| Conditional effects | ||||
| Partner outside | −0.271 | 0.324 | −0.835 | (−0.910, 0.369) |
| Partner inside | −0.180 | 0.317 | −0.566 | (−0.805, 0.445) |
| Sexual activity level | −0.628 | 0.224 | −2.800 ** | (−1069, −0.186) |
| Sexual satisfaction | −0.108 | 0.121 | −0.899 | (−0.346, 0.129) |
| Two-way interaction model | ||||
| Sexual satisfaction × Partner status (outside) | 0.221 | 0.124 | 1.781 | (−0.024, 0.467) |
| Sexual satisfaction × Partner status (inside) | 0.175 | 0.116 | 1.500 | (−0.055, 0.404) |
| Sexual satisfaction × Sexual activity level | 0.285 | 0.099 | 2.881 ** | (0.090, 0.479) |
| R2 | 0.355 *** | |||
| Sexual satisfaction at values of the moderators | ||||
| Non-sexual abstinent—No partner | −0.108 | 0.121 | −0.899 | (−0.346, 0.129) |
| Non-sexual abstinent—Partner outside | 0.113 | 0.063 | 1.791 | (−0.011, 0.237) |
| Non-sexual abstinent—Partner inside | 0.066 | 0.057 | 1.157 | (−0.047, 0.179) |
| Sexual abstinent—No partner | 0.176 | 0.089 | 1.990 * | (0.002, 0.351) |
| Sexual abstinent—Partner outside | 0.398 | 0.104 | 3.835 *** | (0.193, 0.602) |
| Sexual abstinent—Partner inside | 0.351 | 0.098 | 3.577 *** | (0.157, 0.544) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Carcedo, R.J.; Perlman, D.; Fernández-Rouco, N.; Pérez, F.; Hervalejo, D. Sexual Satisfaction and Mental Health in Prison Inmates. J. Clin. Med. 2019, 8, 705. https://doi.org/10.3390/jcm8050705
Carcedo RJ, Perlman D, Fernández-Rouco N, Pérez F, Hervalejo D. Sexual Satisfaction and Mental Health in Prison Inmates. Journal of Clinical Medicine. 2019; 8(5):705. https://doi.org/10.3390/jcm8050705
Chicago/Turabian StyleCarcedo, Rodrigo J., Daniel Perlman, Noelia Fernández-Rouco, Fernando Pérez, and Diego Hervalejo. 2019. "Sexual Satisfaction and Mental Health in Prison Inmates" Journal of Clinical Medicine 8, no. 5: 705. https://doi.org/10.3390/jcm8050705
APA StyleCarcedo, R. J., Perlman, D., Fernández-Rouco, N., Pérez, F., & Hervalejo, D. (2019). Sexual Satisfaction and Mental Health in Prison Inmates. Journal of Clinical Medicine, 8(5), 705. https://doi.org/10.3390/jcm8050705








