Periodontal Health and Oral Microbiota in Patients with Rheumatoid Arthritis
Abstract
1. Introduction
2. Experimental Section
2.1. Study Population
2.2. Clinical Assessments
2.3. Collection and Preparation of Gingival Crevicular Fluid, Plaque, Saliva and Blood Samples
2.4. Immunoassay Analysis
2.5. 16S rRNA Sequencing and Quantitative Polymerase Chain Reaction (qPCR)
2.6. Sequence Count Data Processing and Analysis
2.7. Statistical Analysis
3. Results
3.1. Characteristics of the Study Population
3.2. Periodontal and Dental Characteristics in Relation to Periodontitis Severity
3.3. Rheumatological Characteristics in Relation to Periodontal Status
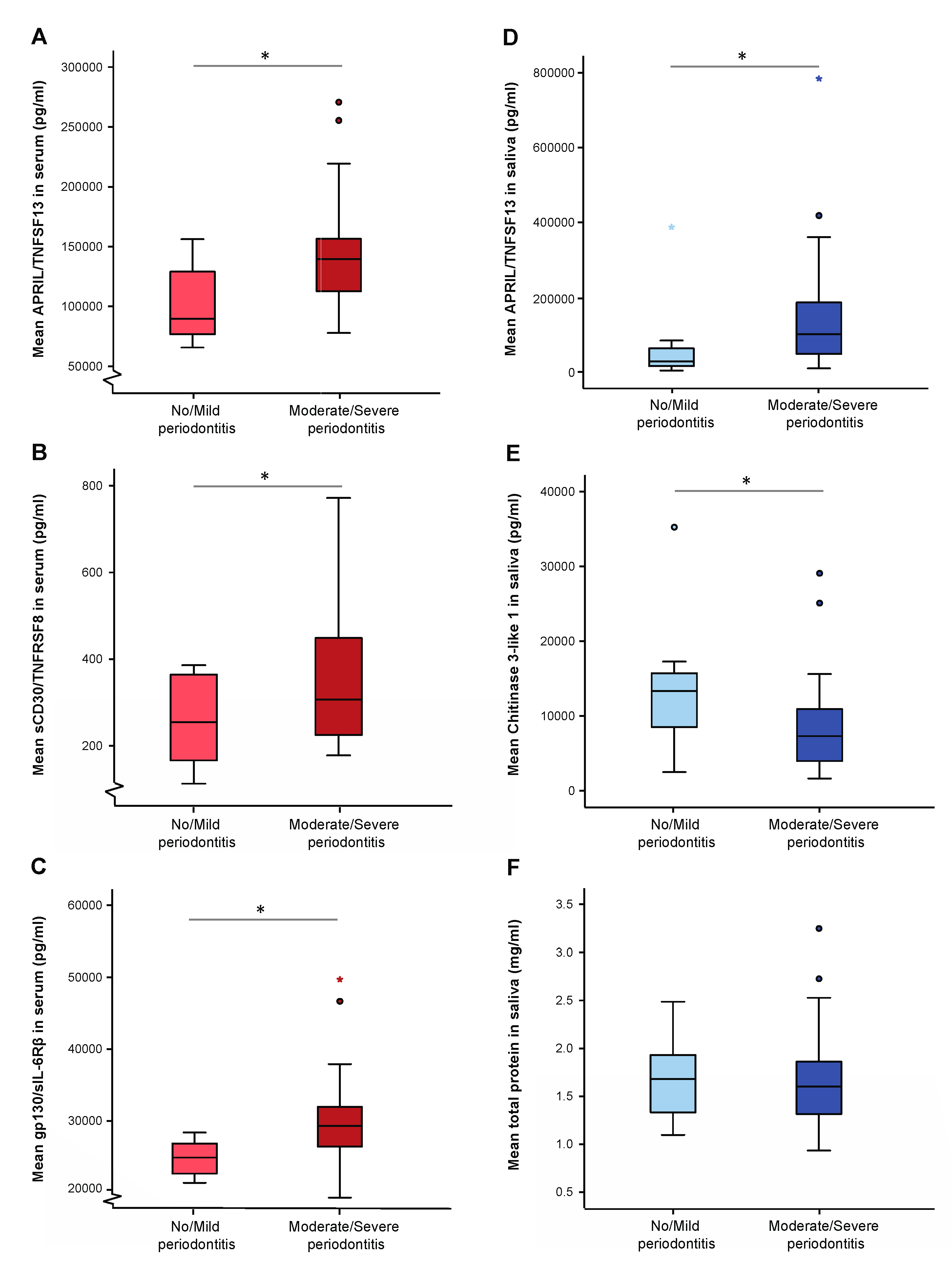
3.4. Levels of Inflammatory Mediators in Serum, Saliva and GCF Samples
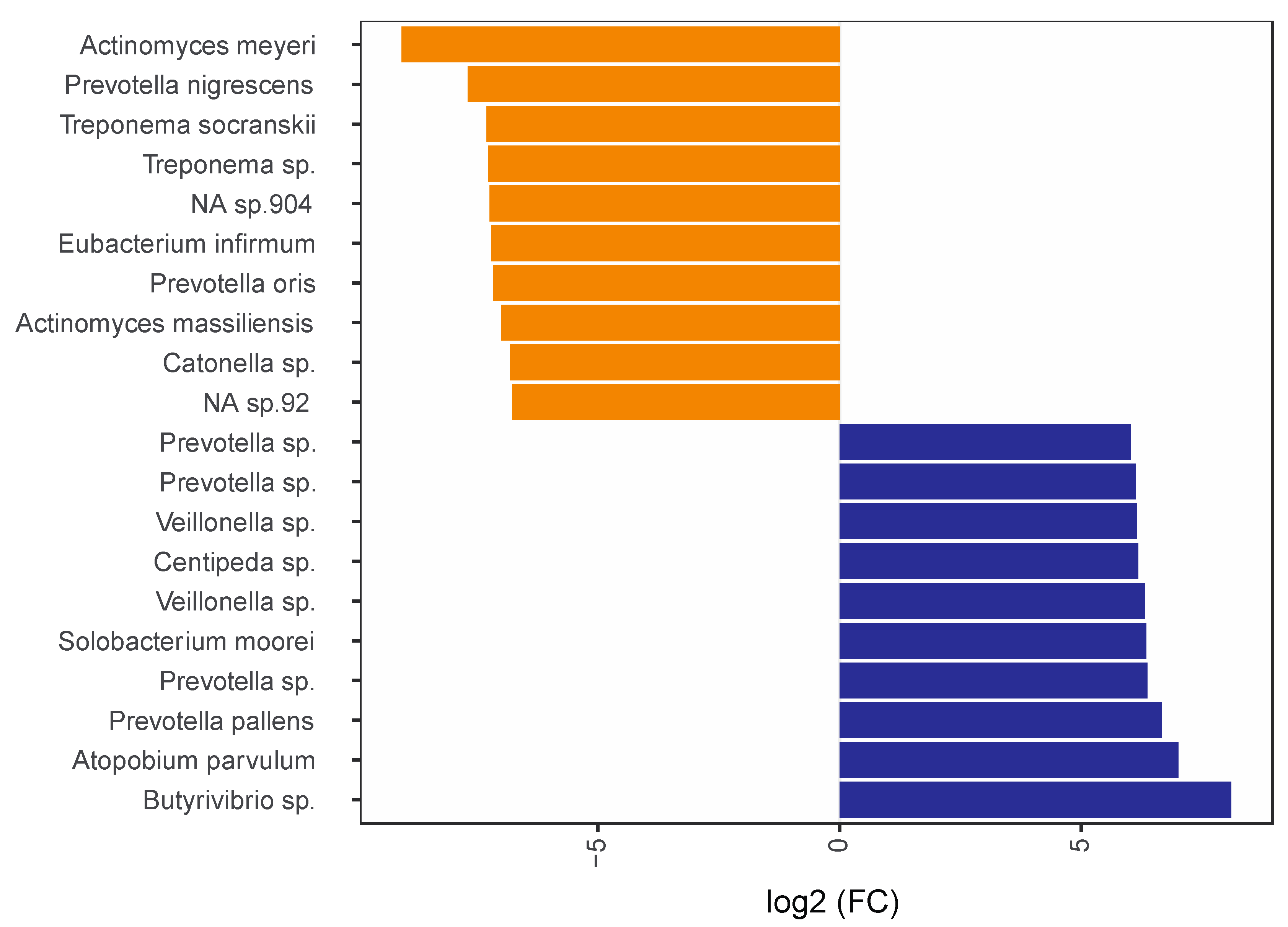
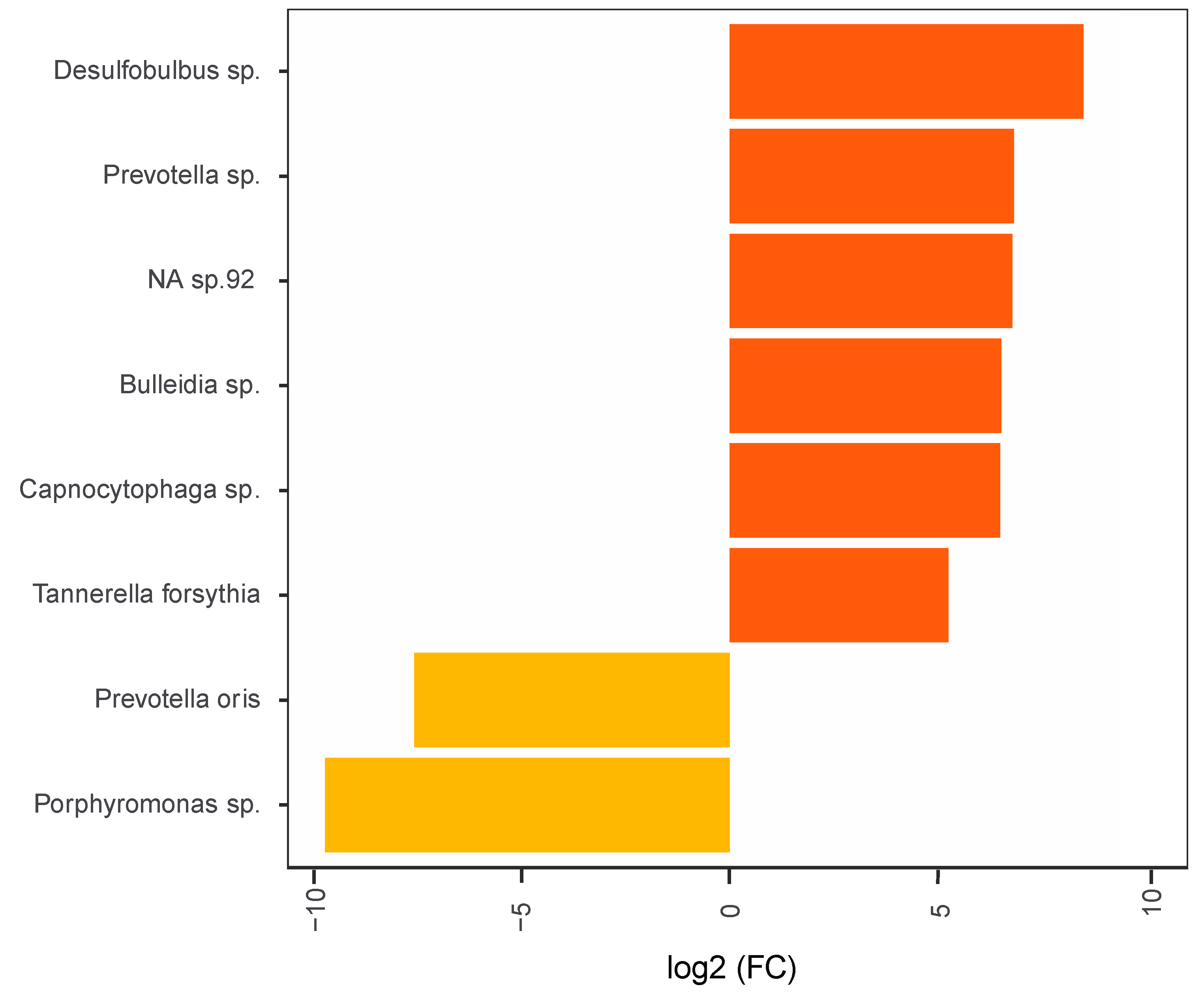
3.5. Microbial Profile of Subgingival Plaque and Saliva Samples
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Fuggle, N.R.; Smith, T.O.; Kaul, A.; Sofat, N. Hand to Mouth: A Systematic Review and Meta-Analysis of the Association between Rheumatoid Arthritis and Periodontitis. Front Immunol. 2016, 7, 80. [Google Scholar] [CrossRef] [PubMed]
- Rosenstein, E.D.; Greenwald, R.A.; Kushner, L.J.; Weissmann, G. Hypothesis: The humoral immune response to oral bacteria provides a stimulus for the development of rheumatoid arthritis. Inflammation 2004, 28, 311–318. [Google Scholar] [CrossRef] [PubMed]
- Leech, M.T.; Bartold, P.M. The association between rheumatoid arthritis and periodontitis. Best Pract. Res. Clin. Rheumatol. 2015, 29, 189–201. [Google Scholar] [CrossRef]
- Klareskog, L.; Catrina, A.I.; Paget, S. Rheumatoid arthritis. Lancet 2009, 373, 659–672. [Google Scholar] [CrossRef]
- McInnes, I.B.; Schett, G. The pathogenesis of rheumatoid arthritis. N. Engl. J. Med. 2011, 365, 2205–2219. [Google Scholar] [CrossRef]
- Bascones, A.; Noronha, S.; Gomez, M.; Mota, P.; Gonzalez Moles, M.A.; Villarroel Dorrego, M. Tissue destruction in periodontitis: Bacteria or cytokines fault? Quintessence Int. 2005, 36, 299–306. [Google Scholar]
- Janssen, K.M.; Vissink, A.; de Smit, M.J.; Westra, J.; Brouwer, E. Lessons to be learned from periodontitis. Curr. Opin. Rheumatol. 2013, 25, 241–247. [Google Scholar] [CrossRef] [PubMed]
- Bartold, P.M.; Marshall, R.I.; Haynes, D.R. Periodontitis and rheumatoid arthritis: A review. J. Periodontol. 2005, 76, 2066–2074. [Google Scholar] [CrossRef]
- Stabholz, A.; Soskolne, W.A.; Shapira, L. Genetic and environmental risk factors for chronic periodontitis and aggressive periodontitis. Periodontol 2000 2010, 53, 138–153. [Google Scholar] [CrossRef]
- Rutger Persson, G. Rheumatoid arthritis and periodontitis—Inflammatory and infectious connections. Review of the literature. J. Oral Microbiol. 2012, 4. [Google Scholar] [CrossRef]
- Hajishengallis, G. Periodontitis: From microbial immune subversion to systemic inflammation. Nat. Rev. Immunol. 2015, 15, 30–44. [Google Scholar] [CrossRef]
- Trouw, L.A.; Huizinga, T.W.; Toes, R.E. Autoimmunity in rheumatoid arthritis: Different antigens—Common principles. Ann. Rheum. Dis. 2013, 72 (Suppl. 2), ii132–ii136. [Google Scholar] [CrossRef]
- Klareskog, L.; Ronnelid, J.; Lundberg, K.; Padyukov, L.; Alfredsson, L. Immunity to citrullinated proteins in rheumatoid arthritis. Annu. Rev. Immunol. 2008, 26, 651–675. [Google Scholar] [CrossRef]
- van der Woude, D.; Catrina, A.I. HLA and anti-citrullinated protein antibodies: Building blocks in RA. Best Pract. Res. Clin. Rheumatol. 2015, 29, 692–705. [Google Scholar] [CrossRef]
- Lundberg, K.; Wegner, N.; Yucel-Lindberg, T.; Venables, P.J. Periodontitis in RA-the citrullinated enolase connection. Nat. Rev. Rheumatol. 2010, 6, 727–730. [Google Scholar] [CrossRef]
- Konig, M.F.; Abusleme, L.; Reinholdt, J.; Palmer, R.J.; Teles, R.P.; Sampson, K.; Rosen, A.; Nigrovic, P.A.; Sokolove, J.; Giles, J.T.; et al. Aggregatibacter actinomycetemcomitans-induced hypercitrullination links periodontal infection to autoimmunity in rheumatoid arthritis. Sci. Transl. Med. 2016, 8, 369ra176. [Google Scholar] [CrossRef]
- Wegner, N.; Wait, R.; Sroka, A.; Eick, S.; Nguyen, K.A.; Lundberg, K.; Kinloch, A.; Culshaw, S.; Potempa, J.; Venables, P.J. Peptidylarginine deiminase from Porphyromonas gingivalis citrullinates human fibrinogen and alpha-enolase: Implications for autoimmunity in rheumatoid arthritis. Arthritis Rheum. 2010, 62, 2662–2672. [Google Scholar] [CrossRef]
- Chen, H.H.; Huang, N.; Chen, Y.M.; Chen, T.J.; Chou, P.; Lee, Y.L.; Chou, Y.J.; Lan, J.L.; Lai, K.L.; Lin, C.H.; et al. Association between a history of periodontitis and the risk of rheumatoid arthritis: A nationwide, population-based, case-control study. Ann. Rheum. Dis. 2013, 72, 1206–1211. [Google Scholar] [CrossRef]
- Lee, J.H.; Lee, J.S.; Park, J.Y.; Choi, J.K.; Kim, D.W.; Kim, Y.T.; Choi, S.H. Association of Lifestyle-Related Comorbidities With Periodontitis: A Nationwide Cohort Study in Korea. Medicine (Baltimore) 2015, 94, e1567. [Google Scholar] [CrossRef] [PubMed]
- Arkema, E.V.; Karlson, E.W.; Costenbader, K.H. A prospective study of periodontal disease and risk of rheumatoid arthritis. J. Rheumatol. 2010, 37, 1800–1804. [Google Scholar] [CrossRef] [PubMed]
- Eriksson, K.; Nise, L.; Kats, A.; Luttropp, E.; Catrina, A.I.; Askling, J.; Jansson, L.; Alfredsson, L.; Klareskog, L.; Lundberg, K.; et al. Prevalence of Periodontitis in Patients with Established Rheumatoid Arthritis: A Swedish Population Based Case-Control Study. PLoS ONE 2016, 11, e0155956. [Google Scholar] [CrossRef]
- Page, R.C.; Eke, P.I. Case definitions for use in population-based surveillance of periodontitis. J. Periodontol. 2007, 78, 1387–1399. [Google Scholar] [CrossRef] [PubMed]
- Aletaha, D.; Neogi, T.; Silman, A.J.; Funovits, J.; Felson, D.T.; Bingham, C.O., 3rd; Birnbaum, N.S.; Burmester, G.R.; Bykerk, V.P.; Cohen, M.D.; et al. 2010 Rheumatoid arthritis classification criteria: An American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010, 62, 2569–2581. [Google Scholar] [CrossRef] [PubMed]
- Prevoo, M.L.; van’t Hof, M.A.; Kuper, H.H.; van Leeuwen, M.A.; van de Putte, L.B.; van Riel, P.L. Modified disease activity scores that include twenty-eight-joint counts. Development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum. 1995, 38, 44–48. [Google Scholar] [CrossRef] [PubMed]
- Fransen, J.; Creemers, M.C.; Van Riel, P.L. Remission in rheumatoid arthritis: Agreement of the disease activity score (DAS28) with the ARA preliminary remission criteria. Rheumatology (Oxford) 2004, 43, 1252–1255. [Google Scholar] [CrossRef]
- Fries, J.F.; Spitz, P.; Kraines, R.G.; Holman, H.R. Measurement of patient outcome in arthritis. Arthritis Rheum. 1980, 23, 137–145. [Google Scholar] [CrossRef]
- Cappelli, D.P.; Mobley, C.C. Prevention in Clinical Oral Health Care, 1st ed.; Elsevier Health Sciences: New York, NY, USA, 2007; p. 6. [Google Scholar]
- Lundmark, A.; Johannsen, G.; Eriksson, K.; Kats, A.; Jansson, L.; Tervahartiala, T.; Rathnayake, N.; Akerman, S.; Klinge, B.; Sorsa, T.; et al. Mucin 4 and matrix metalloproteinase 7 as novel salivary biomarkers for periodontitis. J. Clin. Periodontol. 2017, 44, 247–254. [Google Scholar] [CrossRef]
- Nickles, K.; Scharf, S.; Rollke, L.; Mayer, I.; Mayer, M.; Eickholz, P. Detection of subgingival periodontal pathogens--comparison of two sampling strategies. Clin. Oral Investig. 2016, 20, 571–579. [Google Scholar] [CrossRef]
- Hensvold, A.H.; Frisell, T.; Magnusson, P.K.; Holmdahl, R.; Askling, J.; Catrina, A.I. How well do ACPA discriminate and predict RA in the general population: A study based on 12 590 population-representative Swedish twins. Ann. Rheum. Dis. 2017, 76, 119–125. [Google Scholar] [CrossRef]
- Hugerth, L.W.; Wefer, H.A.; Lundin, S.; Jakobsson, H.E.; Lindberg, M.; Rodin, S.; Engstrand, L.; Andersson, A.F. DegePrime, a program for degenerate primer design for broad-taxonomic-range PCR in microbial ecology studies. Appl. Environ. Microbiol. 2014, 80, 5116–5123. [Google Scholar] [CrossRef]
- Herlemann, D.P.; Labrenz, M.; Jurgens, K.; Bertilsson, S.; Waniek, J.J.; Andersson, A.F. Transitions in bacterial communities along the 2000 km salinity gradient of the Baltic Sea. ISME J. 2011, 5, 1571–1579. [Google Scholar] [CrossRef]
- Lundin, S.; Stranneheim, H.; Pettersson, E.; Klevebring, D.; Lundeberg, J. Increased throughput by parallelization of library preparation for massive sequencing. PLoS ONE 2010, 5, e10029. [Google Scholar] [CrossRef]
- Nonnenmacher, C.; Dalpke, A.; Mutters, R.; Heeg, K. Quantitative detection of periodontopathogens by real-time PCR. J. Microbiol. Methods 2004, 59, 117–125. [Google Scholar] [CrossRef] [PubMed]
- Eriksson, K.; Lonnblom, E.; Tour, G.; Kats, A.; Mydel, P.; Georgsson, P.; Hultgren, C.; Kharlamova, N.; Norin, U.; Jonsson, J.; et al. Effects by periodontitis on pristane-induced arthritis in rats. J. Transl. Med. 2016, 14, 311. [Google Scholar] [CrossRef] [PubMed]
- Callahan, B.J.; McMurdie, P.J.; Rosen, M.J.; Han, A.W.; Johnson, A.J.; Holmes, S.P. DADA2: High-resolution sample inference from Illumina amplicon data. Nat. Methods 2016, 13, 581–583. [Google Scholar] [CrossRef]
- Cole, J.R.; Wang, Q.; Fish, J.A.; Chai, B.; McGarrell, D.M.; Sun, Y.; Brown, C.T.; Porras-Alfaro, A.; Kuske, C.R.; Tiedje, J.M. Ribosomal Database Project: Data and tools for high throughput rRNA analysis. Nucleic Acids Res. 2014, 42, D633–D642. [Google Scholar] [CrossRef]
- Caporaso, J.G.; Kuczynski, J.; Stombaugh, J.; Bittinger, K.; Bushman, F.D.; Costello, E.K.; Fierer, N.; Pena, A.G.; Goodrich, J.K.; Gordon, J.I.; et al. QIIME allows analysis of high-throughput community sequencing data. Nat. Methods 2010, 7, 335–336. [Google Scholar] [CrossRef]
- McMurdie, P.J.; Holmes, S. phyloseq: An R package for reproducible interactive analysis and graphics of microbiome census data. PLoS ONE 2013, 8, e61217. [Google Scholar] [CrossRef]
- Love, M.I.; Huber, W.; Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 2014, 15, 550. [Google Scholar] [CrossRef]
- Catrina, A.I.; Svensson, C.I.; Malmstrom, V.; Schett, G.; Klareskog, L. Mechanisms leading from systemic autoimmunity to joint-specific disease in rheumatoid arthritis. Nat. Rev. Rheumatol. 2017, 13, 79–86. [Google Scholar] [CrossRef]
- Gonzalez, S.M.; Payne, J.B.; Yu, F.; Thiele, G.M.; Erickson, A.R.; Johnson, P.G.; Schmid, M.J.; Cannon, G.W.; Kerr, G.S.; Reimold, A.M.; et al. Alveolar bone loss is associated with circulating anti-citrullinated protein antibody (ACPA) in patients with rheumatoid arthritis. J. Periodontol. 2015, 86, 222–231. [Google Scholar] [CrossRef] [PubMed]
- Choi, I.A.; Kim, J.H.; Kim, Y.M.; Lee, J.Y.; Kim, K.H.; Lee, E.Y.; Lee, E.B.; Lee, Y.M.; Song, Y.W. Periodontitis is associated with rheumatoid arthritis: A study with longstanding rheumatoid arthritis patients in Korea. Korean J. Intern. Med. 2016, 31, 977–986. [Google Scholar] [CrossRef]
- Heasman, P.A.; Hughes, F.J. Drugs, medications and periodontal disease. Br. Dent. J. 2014, 217, 411–419. [Google Scholar] [CrossRef] [PubMed]
- Mikuls, T.R.; Walker, C.; Qiu, F.; Yu, F.; Thiele, G.M.; Alfant, B.; Li, E.C.; Zhao, L.Y.; Wang, G.P.; Datta, S.; et al. The subgingival microbiome in patients with established rheumatoid arthritis. Rheumatology (Oxford) 2018. [Google Scholar] [CrossRef]
- Lopez-Oliva, I.; Paropkari, A.D.; Saraswat, S.; Serban, S.; Yonel, Z.; Sharma, P.; de Pablo, P.; Raza, K.; Filer, A.; Chapple, I.; et al. Dysbiotic Subgingival Microbial Communities in Periodontally Healthy Patients With Rheumatoid Arthritis. Arthritis Rheumatol. 2018, 70, 1008–1013. [Google Scholar] [CrossRef]
- Beyer, K.; Zaura, E.; Brandt, B.W.; Buijs, M.J.; Brun, J.G.; Crielaard, W.; Bolstad, A.I. Subgingival microbiome of rheumatoid arthritis patients in relation to their disease status and periodontal health. PLoS ONE 2018, 13, e0202278. [Google Scholar] [CrossRef]
- Scher, J.U.; Ubeda, C.; Equinda, M.; Khanin, R.; Buischi, Y.; Viale, A.; Lipuma, L.; Attur, M.; Pillinger, M.H.; Weissmann, G.; et al. Periodontal disease and the oral microbiota in new-onset rheumatoid arthritis. Arthritis Rheum. 2012, 64, 3083–3094. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Zhang, D.; Jia, H.; Feng, Q.; Wang, D.; Liang, D.; Wu, X.; Li, J.; Tang, L.; Li, Y.; et al. The oral and gut microbiomes are perturbed in rheumatoid arthritis and partly normalized after treatment. Nat. Med. 2015, 21, 895–905. [Google Scholar] [CrossRef]
- Wells, P.M.; Williams, F.M.K.; Matey-Hernandez, M.L.; Menni, C.; Steves, C.J. ‘RA and the microbiome: Do host genetic factors provide the link? J. Autoimmun. 2019, 99, 104–115. [Google Scholar] [CrossRef]
- Yucel-Lindberg, T.; Bage, T. Inflammatory mediators in the pathogenesis of periodontitis. Expert Rev. Mol. Med. 2013, 15, e7. [Google Scholar] [CrossRef]
- Kobayashi, T.; Yoshie, H. Host Responses in the Link Between Periodontitis and Rheumatoid Arthritis. Curr. Oral Health Rep. 2015, 2, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Thompson, C.; Davies, R.; Choy, E. Anti cytokine therapy in chronic inflammatory arthritis. Cytokine 2016, 86, 92–99. [Google Scholar] [CrossRef]
- Vincent, F.B.; Saulep-Easton, D.; Figgett, W.A.; Fairfax, K.A.; Mackay, F. The BAFF/APRIL system: Emerging functions beyond B cell biology and autoimmunity. Cytokine Growth Factor Rev. 2013, 24, 203–215. [Google Scholar] [CrossRef] [PubMed]
- Abe, T.; AlSarhan, M.; Benakanakere, M.R.; Maekawa, T.; Kinane, D.F.; Cancro, M.P.; Korostoff, J.M.; Hajishengallis, G. The B Cell-Stimulatory Cytokines BLyS and APRIL Are Elevated in Human Periodontitis and Are Required for B Cell-Dependent Bone Loss in Experimental Murine Periodontitis. J. Immunol. 2015, 195, 1427–1435. [Google Scholar] [CrossRef] [PubMed]
- Shabgah, A.G.; Shariati-Sarabi, Z.; Tavakkol-Afshari, J.; Mohammadi, M. The role of BAFF and APRIL in rheumatoid arthritis. J. Cell. Physiol. 2019. [Google Scholar] [CrossRef] [PubMed]
- Kazakova, M.H.; Sarafian, V.S. New Developments in the Pathogenesis of Rheumatoid Arthritis; IntechOpen: London, UK, 2017; pp. 139–151. [Google Scholar]
- Kazakova, M.; Batalov, A.; Deneva, T.; Mateva, N.; Kolarov, Z.; Sarafian, V. Relationship between sonographic parameters and YKL-40 levels in rheumatoid arthritis. Rheumatol. Int. 2013, 33, 341–346. [Google Scholar] [CrossRef]
- Szychlinska, M.A.; Trovato, F.M.; Di Rosa, M.; Malaguarnera, L.; Puzzo, L.; Leonardi, R.; Castrogiovanni, P.; Musumeci, G. Co-Expression and Co-Localization of Cartilage Glycoproteins CHI3L1 and Lubricin in Osteoarthritic Cartilage: Morphological, Immunohistochemical and Gene Expression Profiles. Int. J. Mol. Sci. 2016, 17, 359. [Google Scholar] [CrossRef]
- Coffman, F.D. Chitinase 3-Like-1 (CHI3L1): A putative disease marker at the interface of proteomics and glycomics. Crit. Rev. Clin. Lab. Sci. 2008, 45, 531–562. [Google Scholar] [CrossRef] [PubMed]
- Keles, Z.P.; Keles, G.C.; Avci, B.; Cetinkaya, B.O.; Emingil, G. Analysis of YKL-40 acute-phase protein and interleukin-6 levels in periodontal disease. J. Periodontol. 2014, 85, 1240–1246. [Google Scholar] [CrossRef]
- Knudsen, L.S.; Hetland, M.L.; Johansen, J.S.; Skjodt, H.; Peters, N.D.; Colic, A.; Grau, K.; Nielsen, H.J.; Ostergaard, M. Changes in plasma IL-6, plasma VEGF and serum YKL-40 during Treatment with Etanercept and Methotrexate or Etanercept alone in Patients with Active Rheumatoid Arthritis Despite Methotrexate Therapy. Biomark. Insights 2009, 4, 91–95. [Google Scholar] [CrossRef]
- Williamson, S.; Munro, C.; Pickler, R.; Grap, M.J.; Elswick, R.K., Jr. Comparison of biomarkers in blood and saliva in healthy adults. Nurs. Res. Pract. 2012, 2012, 246178. [Google Scholar] [CrossRef]
- Biyikoglu, B.; Buduneli, N.; Kardesler, L.; Aksu, K.; Oder, G.; Kutukculer, N. Evaluation of t-PA, PAI-2, IL-1beta and PGE(2) in gingival crevicular fluid of rheumatoid arthritis patients with periodontal disease. J. Clin. Periodontol. 2006, 33, 605–611. [Google Scholar] [CrossRef] [PubMed]
- Joseph, R.; Rajappan, S.; Nath, S.G.; Paul, B.J. Association between chronic periodontitis and rheumatoid arthritis: A hospital-based case-control study. Rheumatol. Int. 2013, 33, 103–109. [Google Scholar] [CrossRef]
- Kasser, U.R.; Gleissner, C.; Dehne, F.; Michel, A.; Willershausen-Zonnchen, B.; Bolten, W.W. Risk for periodontal disease in patients with longstanding rheumatoid arthritis. Arthritis Rheum. 1997, 40, 2248–2251. [Google Scholar]
- de Smit, M.J.; Brouwer, E.; Westra, J.; Nesse, W.; Vissink, A.; van Winkelhoff, A.J. Effect of periodontal treatment on rheumatoid arthritis and vice versa. Ned Tijdschr Tandheelkd. 2012, 119, 191–197. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Coburn, B.W.; Sayles, H.R.; Payne, J.B.; Redman, R.S.; Markt, J.C.; Beatty, M.W.; Griffiths, G.R.; McGowan, D.J.; Mikuls, T.R. Performance of self-reported measures for periodontitis in rheumatoid arthritis and osteoarthritis. J. Periodontol. 2015, 86, 16–26. [Google Scholar] [CrossRef] [PubMed]
- Mikuls, T.R.; Payne, J.B.; Yu, F.; Thiele, G.M.; Reynolds, R.J.; Cannon, G.W.; Markt, J.; McGowan, D.; Kerr, G.S.; Redman, R.S.; et al. Periodontitis and Porphyromonas gingivalis in patients with rheumatoid arthritis. Arthritis Rheumatol. 2014, 66, 1090–1100. [Google Scholar] [CrossRef] [PubMed]
- Ortiz, P.; Bissada, N.F.; Palomo, L.; Han, Y.W.; Al-Zahrani, M.S.; Panneerselvam, A.; Askari, A. Periodontal therapy reduces the severity of active rheumatoid arthritis in patients treated with or without tumor necrosis factor inhibitors. J. Periodontol. 2009, 80, 535–540. [Google Scholar] [CrossRef] [PubMed]
- Mayer, Y.; Balbir-Gurman, A.; Machtei, E.E. Anti-tumor necrosis factor-alpha therapy and periodontal parameters in patients with rheumatoid arthritis. J. Periodontol. 2009, 80, 1414–1420. [Google Scholar] [CrossRef]
- Kobayashi, T.; Yokoyama, T.; Ito, S.; Kobayashi, D.; Yamagata, A.; Okada, M.; Oofusa, K.; Narita, I.; Murasawa, A.; Nakazono, K.; et al. Periodontal and serum protein profiles in patients with rheumatoid arthritis treated with tumor necrosis factor inhibitor adalimumab. J. Periodontol. 2014, 85, 1480–1488. [Google Scholar] [CrossRef]
- Coat, J.; Demoersman, J.; Beuzit, S.; Cornec, D.; Devauchelle-Pensec, V.; Saraux, A.; Pers, J.O. Anti-B lymphocyte immunotherapy is associated with improvement of periodontal status in subjects with rheumatoid arthritis. J. Clin. Periodontol. 2015, 42, 817–823. [Google Scholar] [CrossRef] [PubMed]
- Linden, G.J.; Lyons, A.; Scannapieco, F.A. Periodontal systemic associations: Review of the evidence. J. Periodontol. 2013, 84, S8–s19. [Google Scholar] [CrossRef] [PubMed]
- Oliver, J.E.; Silman, A.J. Why are women predisposed to autoimmune rheumatic diseases? Arthritis Res. Ther. 2009, 11, 252. [Google Scholar] [CrossRef] [PubMed]
- Page, R.C.; Beck, J.D. Risk assessment for periodontal diseases. Int. Dent. J. 1997, 47, 61–87. [Google Scholar] [CrossRef] [PubMed]
- Klareskog, L.; Gregersen, P.K.; Huizinga, T.W. Prevention of autoimmune rheumatic disease: State of the art and future perspectives. Ann. Rheum. Dis. 2010, 69, 2062–2066. [Google Scholar] [CrossRef]
| Characteristics | No/Mild Periodontitis (n = 10) | Moderate/Severe Periodontitis (n = 30) | p Value |
|---|---|---|---|
| Gender, no (%) | |||
| Female | 10 (100) | 25 (83) | |
| Male | 0 (0) | 5 (17) | 0.306 |
| Age, mean (±SD) | 50 (14) | 64 (7.8) | 0.004 |
| BMI, mean (±SD) | 26 (6.8) | 24 (5.6) | 0.325 |
| RA duration in years, mean (±SD) | 12 (11) | 10 (10) | 0.406 |
| Comorbidities, no (%) | |||
| Diabetes | 0 (0) | 2 (6.7) | 1.000 |
| Cardiovascular disease | 3 (30) | 8 (27) | 1.000 |
| High blood pressure | 2 (20) | 5 (17) | 1.000 |
| Gastrointestinal disorders | 1 (10) | 6 (20) | 0.739 |
| Osteoporosis | 0 (0) | 3 (11) | 0.552 |
| Asthma | 0 (0) | 5 (17) | 0.306 |
| Sjögren’s syndrome | 0 (0) | 2 (7.4) | 1.000 |
| TMJ | 4 (40) | 8 (27) | 0.451 |
| Medication, no (%) | |||
| Analgesics | 6 (60) | 13 (43) | 0.473 |
| NSAIDs | 1 (10) | 10 (33) | 0.233 |
| DMARDs | 6 (60) | 22 (73) | 0.451 |
| Biological DMARDs | 5 (50) | 11 (37) | 0.482 |
| Glucocorticoids | 5 (50) | 18 (60) | 0.717 |
| Bisphosphonates | 1 (10) | 1 (3.0) | 0.442 |
| Smoking habits, no (%) | |||
| Current smokers | 0 (0) | 5 (17) | 0.306 |
| Ex-smokers | 4 (40) | 19 (73) | 0.119 |
| Never smokers | 6 (60) | 5 (17) | 0.014 |
| Alcohol consumption, no (%) | |||
| Monthly | 7 (70) | 20 (67) | 1.000 |
| Weekly | 5 (50) | 14 (47) | 1.000 |
| Daily | 0 (0) | 3 (10) | 0.560 |
| Never | 2 (20) | 3(10) | 0.584 |
| Education, no (%) | |||
| University degree | 4 (40) | 13 (46) | |
| No university degree | 6 (60) | 5 (54) | 1.000 |
| Place of birth, no (%) | |||
| Sweden | 10 (100) | 24 (83) | |
| Other | 0 (0) | 5 (17) | 0.302 |
| Characteristics | No/Mild Periodontitis (n = 10) | Moderate/Severe Periodontitis (n = 30) | p Value |
|---|---|---|---|
| ACPA status, no (%) | |||
| ACPA-positive | 5 (50) | 25 (86) | |
| ACPA-negative | 5 (50) | 4 (14) | 0.032 |
| RF status, no (%) | |||
| RF-positive | 5 (50) | 22 (73) | |
| RF-negative | 5 (50) | 8 (27) | 0.246 |
| HAQ score (range 0–3), mean (±SD) | 0.7 (0.5) | 0.9 (0.6) | 0.380 |
| DAS28 score (range 1-10), mean (±SD) | 2.7 (1.5) | 3.3 (1.4) | 0.411 |
| Disease activity (DAS28 score), no (%) | |||
| Remission (score < 2.6) | 4 (44) | 10 (37) | 1.000 |
| Low activity (score 2.6–3.2) | 0 (0) | 4 (15) | 0.553 |
| Moderate activity (score 3.2–5.1) | 5 (56) | 9 (33) | 0.432 |
| High activity (score >5.1) | 0 (0) | 4 (15) | 0.553 |
| Serum CRP (ng/mL), mean (±SD) | 5100 (7300) | 4300 (5200) | 0.353 |
| Salivary CRP (ng/mL), mean (±SD) | 1.4 (1.9) | 2.1 (5.4) | 0.749 |
| GCF CRP (ng/mL), mean (±SD) | 2.2 (3.6) | 2.3 (5.4) | 0.617 |
| Variables | No/Mild Periodontitis (n = 9) | Moderate/Severe Periodontitis (n = 29) | p Value |
|---|---|---|---|
| APRIL (TNFSF13) | 5289 (2451) | 4584 (935) | 0.652 |
| BAFF (TNFSF13B) | 2229 (736) | 2982 (1767) | 0.440 |
| sCD30 (TNFRSF8) | 9.0 (11) | 21 (18) | 0.077 |
| sCD163 | 2980 (2727) | 3678 (2835) | 0.400 |
| Chitinase 3-like 1 | 7284 (3881) | 12,885 (9084) | 0.118 |
| gp130 (sIL-6Rß) | 585 (424) | 713 (828) | 0.823 |
| IFN-α2 | 20 (27) | 43 (31) | 0.036 |
| sIL-6Rα | 456 (339) | 786 (594) | 0.175 |
| IL-8 | 761 (372) | 1274 (995) | 0.345 |
| IL-10 | 2.0 (1.6) | 4.3 (5.5) | 0.104 |
| IL-11 | 1.9 (2.1) | 2.6 (4.4) | 0.692 |
| IL-12 (p70) | 2.9 (3.2) | 3.8 (4.4) | 0.635 |
| IL-19 | 14 (13) | 32 (37) | 0.035 |
| IL-20 | 68 (51) | 76 (26) | 0.718 |
| IL-22 | 6.6 (4.5) | 10 (9.1) | 0.353 |
| IL-26 | 15 (11) | 36 (62) | 0.046 |
| IL-27 (p28) | 21 (11) | 21 (10) | 0.810 |
| IL-29 (IFN-γ1) | 52 (61) | 103 (186) | 0.198 |
| IL-32 | 103 (55) | 140 (92) | 0.319 |
| IL-34 | 205 (127) | 184 (101) | 0.436 |
| LIGHT (TNFSF14) | 269 (93) | 314 (117) | 0.328 |
| MMP-1 | 897 (636) | 1294 (534) | 0.049 |
| MMP-3 | 394 (298) | 489 (371) | 0.579 |
| Pentraxin-3 | 375 (261) | 429 (272) | 0.718 |
| sTNF-R1 | 259 (130) | 523 (361) | 0.015 |
| sTNF-R2 | 2075 (5013) | 1976 (5322) | 0.311 |
| TSLP | 24 (20) | 25 (15) | 0.796 |
| TWEAK (TNFSF12) | 27 (17) | 38 (16) | 0.074 |
| Total protein concentration | 0.2 (0.2) | 0.3 (0.3) | 0.503 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Eriksson, K.; Fei, G.; Lundmark, A.; Benchimol, D.; Lee, L.; Hu, Y.O.O.; Kats, A.; Saevarsdottir, S.; Catrina, A.I.; Klinge, B.; et al. Periodontal Health and Oral Microbiota in Patients with Rheumatoid Arthritis. J. Clin. Med. 2019, 8, 630. https://doi.org/10.3390/jcm8050630
Eriksson K, Fei G, Lundmark A, Benchimol D, Lee L, Hu YOO, Kats A, Saevarsdottir S, Catrina AI, Klinge B, et al. Periodontal Health and Oral Microbiota in Patients with Rheumatoid Arthritis. Journal of Clinical Medicine. 2019; 8(5):630. https://doi.org/10.3390/jcm8050630
Chicago/Turabian StyleEriksson, Kaja, Guozhong Fei, Anna Lundmark, Daniel Benchimol, Linkiat Lee, Yue O. O. Hu, Anna Kats, Saedis Saevarsdottir, Anca Irinel Catrina, Björn Klinge, and et al. 2019. "Periodontal Health and Oral Microbiota in Patients with Rheumatoid Arthritis" Journal of Clinical Medicine 8, no. 5: 630. https://doi.org/10.3390/jcm8050630
APA StyleEriksson, K., Fei, G., Lundmark, A., Benchimol, D., Lee, L., Hu, Y. O. O., Kats, A., Saevarsdottir, S., Catrina, A. I., Klinge, B., Andersson, A. F., Klareskog, L., Lundberg, K., Jansson, L., & Yucel-Lindberg, T. (2019). Periodontal Health and Oral Microbiota in Patients with Rheumatoid Arthritis. Journal of Clinical Medicine, 8(5), 630. https://doi.org/10.3390/jcm8050630





