Impact of Cumulative Corticosteroid Dosage on Preventable Hospitalization among Taiwanese Patients with Ankylosing Spondylitis and Inflammatory Bowel Disease
Abstract
1. Introduction
2. Patients and Methods
2.1. Participants: Defining the Cohort and Baseline Health Status
2.2. Medication Dosage
2.3. Outcome: Rate of Preventable Hospitalization for Ambulatory Care-Sensitive Conditions
2.4. Statistical Analysis
3. Results
3.1. Cohort Demographic Data
3.2. Corticosteroid and DMARD Usage
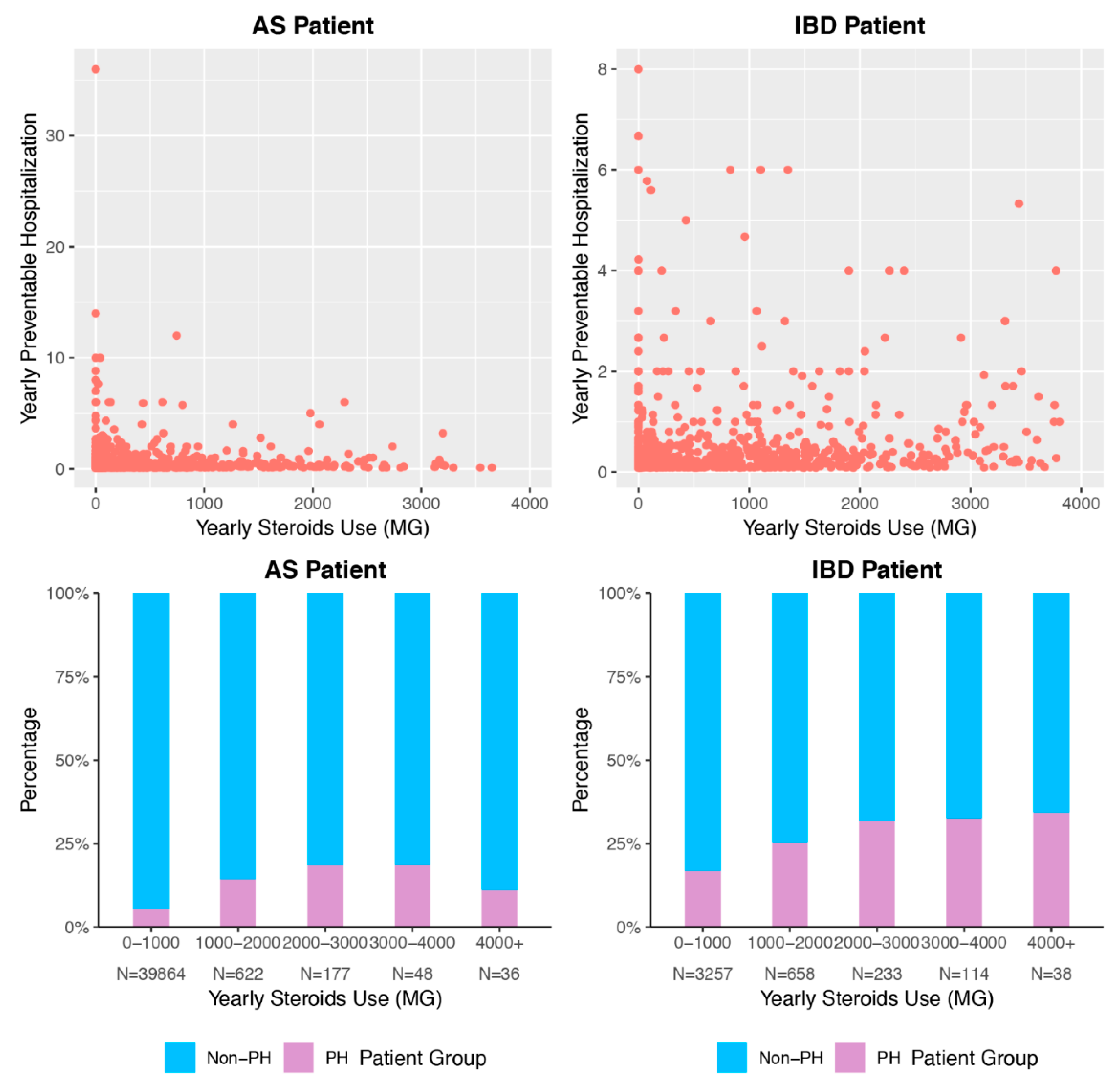
3.3. Cumulative Corticosteroid Usage and Preventable Hospitalization
3.4. Association Between Corticosteroid Usage and Preventable Hospitalization
4. Discussion
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Disclaimer
References
- Terdiman, J.P.; Gruss, C.B.; Heidelbaugh, J.J.; Sultan, S.; Falck–Ytter, Y.T. American Gastroenterological Association Institute Guideline on the Use of Thiopurines, Methotrexate, and Anti–TNF-α Biologic Drugs for the Induction and Maintenance of Remission in Inflammatory Crohn’s Disease. Gastroenterology 2013, 145, 1459–1463. [Google Scholar] [CrossRef]
- Singh, J.A.; Saag, K.G.; Bridges, S.L., Jr.; Akl, E.A.; Bannuru, R.R.; Sullivan, M.C.; Vaysbrot, E.; McNaughton, C.; Osani, M.; Shmerling, R.H.; et al. 2015 American College of Rheumatology Guideline for the Treatment of Rheumatoid Arthritis. Arthritis Rheumatol. 2016, 68, 1–26. [Google Scholar] [CrossRef]
- Tunnicliffe, D.J.; Singh-Grewal, D.; Kim, S.; Craig, J.C.; Tong, A. Diagnosis, Monitoring, and Treatment of Systemic Lupus Erythematosus: A Systematic Review of Clinical Practice Guidelines. Arthritis Care Res. 2015, 67, 1440–1452. [Google Scholar] [CrossRef]
- Ward, M.M.; Deodhar, A.; Akl, E.A.; Lui, A.; Ermann, J.; Gensler, L.S.; Smith, J.A.; Borenstein, D.; Hiratzka, J.; Weiss, P.F.; et al. American College of Rheumatology/Spondylitis Association of America/Spondyloarthritis Research and Treatment Network 2015 Recommendations for the Treatment of Ankylosing Spondylitis and Nonradiographic Axial Spondyloarthritis. Arthritis Rheumatol. 2016, 68, 282–298. [Google Scholar] [CrossRef]
- Braun, J.; Sieper, J. Therapy of ankylosing spondylitis and other spondyloarthritides: Established medical treatment, anti-TNF-α therapy and other novel approaches. Arthritis Res. 2002, 4, 307–321. [Google Scholar] [CrossRef]
- Card, T.; West, J.; Hubbard, R.; Logan, R.F.A. Hip fractures in patients with inflammatory bowel disease and their relationship to corticosteroid use: a population based cohort study. Gut 2004, 53, 251–255. [Google Scholar] [CrossRef]
- Del Rincon, I.; Battafarano, D.F.; Restrepo, J.F.; Erikson, J.M.; Escalante, A. Glucocorticoid dose thresholds associated with all-cause and cardiovascular mortality in rheumatoid arthritis. Arthritis Rheumatol. 2014, 66, 264–272. [Google Scholar] [CrossRef]
- Dixon, W.G.; Abrahamowicz, M.; Beauchamp, M.E.; Ray, D.W.; Bernatsky, S.; Suissa, S.; Sylvestre, M.P. Immediate and delayed impact of oral glucocorticoid therapy on risk of serious infection in older patients with rheumatoid arthritis: A nested case-control analysis. Ann. Rheum. Dis. 2012, 71, 1128–1133. [Google Scholar] [CrossRef]
- Lewis, J.D.; Scott, F.I.; Brensinger, C.M.; Roy, J.A.; Osterman, M.T.; Mamtani, R.; Bewtra, M.; Chen, L.; Yun, H.; Xie, F.; et al. Increased Mortality Rates With Prolonged Corticosteroid Therapy When Compared With Antitumor Necrosis Factor-alpha-Directed Therapy for Inflammatory Bowel Disease. Am. J. Gastroenterol. 2018, 113, 405–417. [Google Scholar] [CrossRef]
- England, B.R.; Sayles, H.; Michaud, K.; Caplan, L.; Davis, L.A.; Cannon, G.W.; Sauer, B.C.; Solow, E.B.; Reimold, A.M.; Kerr, G.S.; et al. Cause-Specific Mortality in Male US Veterans With Rheumatoid Arthritis. Arthritis Care Res. 2016, 68, 36–45. [Google Scholar] [CrossRef]
- Aniwan, S.; Pardi, D.S.; Tremaine, W.J.; Loftus, E.V., Jr. Increased Risk of Acute Myocardial Infarction and Heart Failure in Patients With Inflammatory Bowel Diseases. Clin. Gastroenterol. Hepatol. Off. Clin. Pract. J. Am. Gastroenterol. Assoc. 2018, 16, 1607–1615. [Google Scholar] [CrossRef] [PubMed]
- Strehl, C.; Bijlsma, J.W.; de Wit, M.; Boers, M.; Caeyers, N.; Cutolo, M.; Dasgupta, B.; Dixon, W.G. Defining conditions where long-term glucocorticoid treatment has an acceptably low level of harm to facilitate implementation of existing recommendations: Viewpoints from an EULAR task force. Ann. Rheum. Dis. 2016, 75, 952–957. [Google Scholar] [CrossRef]
- Palmowski, Y.; Buttgereit, T.; Dejaco, C.; Bijlsma, J.W.; Matteson, E.L.; Voshaar, M.; Boers, M.; Buttgereit, F. “Official View” on Glucocorticoids in Rheumatoid Arthritis: A Systematic Review of International Guidelines and Consensus Statements. Arthritis Care Res. 2017, 69, 1134–1141. [Google Scholar] [CrossRef] [PubMed]
- Peschken, C.A.; Esdaile, J.M. Rheumatic diseases in North America’s indigenous peoples. Semin. Arthritis Rheum. 1999, 28, 368–391. [Google Scholar] [CrossRef]
- Hung, S.I.; Chung, W.H.; Liou, L.B.; Chu, C.C.; Lin, M.; Huang, H.P.; Lin, Y.L.; Lan, J.L.; Yang, L.C.; Hong, H.S.; et al. HLA-B*5801 allele as a genetic marker for severe cutaneous adverse reactions caused by allopurinol. Proc. Natl. Acad. Sci. USA 2005, 102, 4134–4139. [Google Scholar] [CrossRef] [PubMed]
- Inokuma, S. Leflunomide-induced interstitial pneumonitis might be a representative of disease-modifying antirheumatic drug-induced lung injury. Exp. Opin. Drug Saf. 2011, 10, 603–611. [Google Scholar] [CrossRef] [PubMed]
- National Health Insurance Research Database, Taiwan. Available online: http://nhird.nhri.org.tw/en/index.htm (accessed on 5 July 2018).
- Rezaie, A.; Quan, H.; Fedorak, R.N.; Panaccione, R.; Hilsden, R.J. Development and validation of an administrative case definition for inflammatory bowel diseases. Can. J. Gastroenterol. 2012, 26, 711–717. [Google Scholar] [CrossRef]
- Singh, J.A.; Holmgren, A.R.; Krug, H.; Noorbaloochi, S. Accuracy of the diagnoses of spondylarthritides in veterans affairs medical center databases. Arthritis Rheum. 2007, 57, 648–655. [Google Scholar] [CrossRef]
- Mowat, C.; Andrew, C.; Windsor, A.C.J.; Ahmad, T.; Arnott, I.; Driscoll, R.; Mitton, S.; Orchard, T.; Rutter, M.; Younge, L.; et al. Guidelines for the management of inflammatory bowel disease in adults. Gut 2011, 60, 571–607. [Google Scholar] [CrossRef]
- Quan, H.; Sundararajan, V.; Halfon, P.; Fong, A.; Burnand, B.; Luthi, J.C.; Saunders, L.D.; Beck, C.A.; Feasby, T.E.; Ghali, W.A. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med. Care 2005, 43, 1130–1139. [Google Scholar] [CrossRef]
- Elixhauser, A.; Steiner, C.; Harris, D.R.; Coffey, R.M. Comorbidity measures for use with administrative data. Med. Care 1998, 36, 8–27. [Google Scholar] [CrossRef]
- Lee, H.S.; Choe, J.; Lee, H.J.; Hwang, S.W.; Park, S.H.; Yang, D.H.; Kim, K.J.; Ye, B.D.; Byeon, J.S.; Myung, S.J.; et al. Change in the diagnosis of inflammatory bowel disease: A hospital-based cohort study from Korea. Intest. Res. 2016, 14, 258–263. [Google Scholar] [CrossRef]
- Ogdie, A.; Nowell, W.B.; Reynolds, R.; Gavigan, K.; Venkatachalam, S.; de la Cruz, M.; Flood, E.; Schwartz, E.J.; Romero, B.; Park, Y. FRI0180 Diagnosis journey of patients with ankylosing spondylitis in the united states. Ann. Rheum. Dis. 2018, 77 (Suppl. 2), 631–632. [Google Scholar]
- Wasko, M.C.M.; Hubert, H.B.; Lingala, V.B.; Elliott, J.R.; Luggen, M.E.; Fries, J.F.; Ward, M.M. Hydroxychloroquine and Risk of Diabetes in Patients With Rheumatoid Arthritis. JAMA. 2007, 298, 187–193. [Google Scholar] [CrossRef]
- Gao, J.; Moran, E.; Li, Y.F.; Almenoff, P.L. Predicting potentially avoidable hospitalizations. Med. Care 2014, 52, 164–171. [Google Scholar] [CrossRef] [PubMed]
- Waljee, A.K.; Wiitala, W.L.; Govani, S.; Stidham, R.; Saini, S.; Hou, J.; Feagins, L.A.; Khan, N.; Good, C.B.; Vijan, S.; et al. Corticosteroid Use and Complications in a US Inflammatory Bowel Disease Cohort. PLoS ONE 2016, 11, e0158017. [Google Scholar] [CrossRef] [PubMed]
- Wolfe, F.; Caplan, L.; Michaud, K. Treatment for rheumatoid arthritis and the risk of hospitalization for pneumonia: associations with prednisone, disease-modifying antirheumatic drugs, and anti-tumor necrosis factor therapy. Arthritis Rheum. 2006, 54, 628–634. [Google Scholar] [CrossRef]
- Duru, N.; van der Goes, M.C.; Jacobs, J.W.; Andrews, T.; Boers, M.; Buttgereit, F.; Caeyers, N.; Cutolo, M.; Halliday, S.; Da Silva, J.A.; et al. EULAR evidence-based and consensus-based recommendations on the management of medium to high-dose glucocorticoid therapy in rheumatic diseases. Ann. Rheum. Dis. 2013, 72, 1905–1913. [Google Scholar] [CrossRef] [PubMed]
| Variable | AS Group n = 40,747 | IBD Group n = 4290 |
|---|---|---|
| DEMOGRAPHICS | ||
| Age, mean (SD) | 38.3 (13.2) | 50.9 (15.7) |
| Female gender, n (%) | 14,092 (34.8%) | 3234 (75.38%) |
| Years followed in database, mean (SD) 1 | 6.4 (3.0) | 6.7 (3.3) |
| Occupation type, n (%) | ||
| Civil servants, teachers, military personnel, and veterans | 2468 (6.06%) | 217 (5.06%) |
| Non-manual workers and professionals | 15,795 (38.76%) | 1063 (24.78%) |
| Manual workers | 9207 (22.60%) | 1514 (35.29%) |
| Others | 3940 (9.67%) | 353 (8.23%) |
| Dependents of insured individuals | 7909 (19.41%) | 1105 (25.76%) |
| Missing | 1428 (3.50%) | 38 (0.89%) |
| Urbanization, n (%) | ||
| Urban | 25,266 (62.01%) | 2589 (60.35%) |
| Suburban | 11,524 (28.28%) | 1299 (30.28%) |
| Rural | 2529 (6.21%) | 364 (8.48%) |
| Missing | 1428 (3.50%) | 38 (0.89%) |
| Monthly income level (median USD for 1:30 exchange rate), n (%) | ||
| Quartile 0 (42) | 11,569 (28.39%) | 1177 (27.44%) |
| Quartile 1 (670) | 9624 (23.62%) | 1395 (32.52%) |
| Quartile 2 (960) | 9545 (23.43%) | 960 (22.38%) |
| Quartile 3 (1687) | 10,009 (24.56%) | 758 (17.67%) |
| Inpatient visits within one year prior to the diagnosis, n (%) | ||
| Never | 36,598 (89.82%) | 3474 (80.98%) |
| 1 | 3163 (7.76%) | 547 (12.75%) |
| 2 | 697 (1.71%) | 150 (3.50%) |
| ≥3 | 289 (0.71%) | 119 (2.77%) |
| Elixhauser comorbidity score, n (%) | ||
| 0 | 27,268 (66.92%) | 1839 (42.87%) |
| 1 | 8916 (21.88%) | 1218 (28.39%) |
| 2 | 2988 (7.33%) | 644 (15.01%) |
| 3 | 1023 (2.51%) | 330 (7.69%) |
| ≥4 | 552 (1.35%) | 259 (6.04%) |
| BASELINE MEDICAL CONTACT | ||
| Total outpatient visits during one year prior to index date | ||
| Mean (SD) | 18.95 (15.61) | 30.33 (21.49) |
| Median (IQR) | 15 (8–25) | 26 (15–40) |
| Visits to a rheumatologist in the six months post index date | ||
| Mean (SD) | 2.81 (2.47) | 1.01 (2.14) |
| Median (IQR) | 2 (1–4) | 0 (0–1) |
| Visits to a gastroenterologist in the six months post index date | ||
| Mean (SD) | 0.24 (0.93) | 1.00 (2.32) |
| Median (IQR) | 0 (0–0) | 0 (0–1) |
| PREVENTABLE HOSPITALIZATIONS FOR AMBULATORY CARE SENSITIVE CONDITIONS DURING STUDY PERIOD | ||
| Reason for hospitalization, n (%) | ||
| Bacterial Pneumonia | 561 (1.38) | 273 (6.36) |
| Urinary Tract Infection Admission Rate | 432 (1.06) | 243 (5.66) |
| Diabetes Long-Term Complications | 177 (0.43) | 88 (2.05) |
| Diabetes Short-Term Complications | 31 (0.08) | 20 (0.47) |
| Heart Failure | 77 (0.19) | 37 (0.86) |
| Hypertension | 119 (0.29) | 72 (1.68) |
| Uncontrolled Diabetes | 55 (0.13) | 16 (0.37) |
| Lower-Extremity Amputation among Patients with Diabetes | 0 (0) | 1 (0.02) |
| Overall | 1219 (2.89) | 551 (12.84) |
| Number of total quarters with any preventable hospitalization, n (%) | ||
| 1 | 893 (2.19) | 368 (8.58) |
| 2 | 158 (0.39) | 98 (2.28) |
| 3 | 69 (0.17) | 52 (1.21) |
| 4 | 21 (0.05) | 16 (0.37) |
| 5 | 20 (0.05) | 6 (0.14) |
| ≥6 | 18 (0.04) | 11 (0.26) |
| Q –1 | Q1 | Q2 | Q3 | Q4 | |
|---|---|---|---|---|---|
| AS patients who received corticosteroids (total n = 40,747) | |||||
| n (%) Receiving Corticosteroids | 4558 (11.2%) | 7525 (18.5%) | 5346 (13.1%) | 4776 (11.7%) | 4569 (11.3%) |
| Median Dose (mg) (IQR) | 90.0 (35.0–166.9) | 140.0 (56.0–315.0) | 105.0 (40.0–320.0) | 94.7 (36.0, 280.0) | 90.0 (30.0, 280.0) |
| Mean Dose (SD) | 142.0 (217.1) | 239.0 (306.3) | 237.7 (360.0) | 221.6 (362.6) | 206.3 (313.1) |
| Median Duration (days) (IQR) | 9.0 (6.0–17.0) | 16.0 (6.0–44.0) | 14.0 (6.0–56.0) | 13.0 (5.0, 53.0) | 10.0 (4.0–48.0) |
| Mean Duration (SD) | 14.2 (14.6) | 28.4 (26.8) | 31.6 (32.7) | 29.9 (32.8) | 28.2 (31.9) |
| Median Daily Dose (mg/day) (IQR) | 10.0 (4.0, 15.0) | 7.9 (4.6, 13.0) | 6.6 (3.8, 11.5) | 6.7 (3.5, 12.0) | 6.7 (3.1, 12.0) |
| Mean Daily Dose (mg/day) (SD) | 10.7 [9.4] | 9.7 (8.5) | 8.6 (7.7) | 8.9 (8.3) | 8.9 (8.8) |
| IBD patients who received corticosteroids (total n = 4290) | |||||
| n (%) Receiving Corticosteroids | 863 (20.1%) | 1298 (30.3%) | 1316 (30.7%) | 1327 (30.9%) | 1289 (30.4%) |
| Median Dose (mg) (IQR) | 120.0 (50.0, 245.6) | 280.0 (90.0, 543.0) | 280.0 (90.6, 598.9) | 308.3 (90.0, 610.0) | 324.0 (112.0, 650.0) |
| Mean Dose (SD) | 203.3 (275.8) | 387.1 (398.4) | 417.7 (450.8) | 427.4 (450.1) | 444.6 (462.3) |
| Median Duration (days) (IQR) | 16.0 (7.0, 28.0) | 39.0 (10.0, 74.0) | 42.0 (11.8, 83.0) | 50.0 (13.0, 85.0) | 51.0 (15.0, 85.0) |
| Mean Duration (SD) | 22.9 (21.3) | 43.4 (32.6) | 46.5 (34.4) | 49.1 (35.3) | 50.5 (34.9) |
| Median Daily Dose (mg/day) (IQR) | 7.5 (4.0, 12.0) | 8.0 (5.0, 13.7) | 7.8 (5.0, 12.5) | 7.5 (5.0, 11.9) | 7.8 (5.0, 12.0) |
| Mean Daily Dose (mg/day) (SD) | 9.1 (7.5) | 9.6 (7.4) | 9.4 (7.3) | 9.2 (7.2) | 9.3 (7.3) |
| AS (n = 40,747) | IBD (n = 4290) | |||||
|---|---|---|---|---|---|---|
| User | Non-User | % | User | Non-User | % | |
| Steroid | 25,928 | 14,819 | 63.63% | 3677 | 613 | 85.71% |
| Biologic DMARD | 1210 | 39,537 | 2.97% | 255 | 4035 | 5.94% |
| Adalimumab | 709 | 40,038 | 1.74% | 134 | 4156 | 3.12% |
| Etanercept | 522 | 40,225 | 1.28% | 134 | 4156 | 3.12% |
| Golimumab | 90 | 40,657 | 0.22% | 10 | 4280 | 0.23% |
| Ustekinumab | 4 | 40,743 | 0.01% | 0 | 4290 | 0.00% |
| Synthetic DMARD | 27,165 | 13,582 | 66.67% | 3133 | 1157 | 73.03% |
| Azathioprine | 598 | 40,149 | 1.47% | 602 | 3688 | 14.03% |
| Cyclophosphamide | 148 | 40,599 | 0.36% | 164 | 4126 | 3.82% |
| Cyclosporine | 462 | 40,285 | 1.13% | 262 | 4028 | 6.11% |
| Hydroxychloroquine | 3578 | 37,169 | 8.78% | 2493 | 1797 | 58.11% |
| Leflunomide | 607 | 40,140 | 1.49% | 328 | 3962 | 7.65% |
| Methotrexate | 3850 | 36,897 | 9.45% | 1146 | 3144 | 26.71% |
| Minocycline | 3416 | 37,331 | 8.38% | 355 | 3935 | 8.28% |
| Mycophenolate | 30 | 40,717 | 0.07% | 32 | 4258 | 0.75% |
| Sulfasalazine | 24,630 | 16,117 | 60.45% | 1325 | 2965 | 30.89% |
| Patients with AS (n = 40,747) | Patients with IBD (n = 4290) | |||
|---|---|---|---|---|
| Odds Ratio | p-Value | Odds Ratio | p-Value | |
| Preventable hospitalization within current quarter | 4.455 (3.672–5.405) | <0.0001 | 4.376 (3.417–5.605) | <0.0001 |
| Corticosteroid | 1.055 (1.037–1.074) | <0.0001 | 1.064 (1.046–1.082) | <0.0001 |
| Biologic DMARD (CI) | ||||
| Adalimumab | 1.289 (0.728–2.283) | 0.384 | 1.725 (0.916–3.250) | 0.091 |
| Etanercept | 1.790 (1.009–3.177) | 0.047 | 0.649 (0.289–1.457) | 0.295 |
| Synthetic DMARD (CI) | ||||
| Azathioprine | 1.273 (0.901–1.799) | 0.171 | 1.106 (0.847–1.444) | 0.458 |
| Cyclophosphamide | 1.441 (0.802–2.590) | 0.221 | 0.845 (0.495–1.442) | 0.537 |
| Cyclosporin | 1.002 (0.608–1.650) | 0.995 | 1.078 (0.714–1.627) | 0.721 |
| Hydroxychloroquine | 1.241 (1.105–1.518) | 0.035 | 1.086 (0.945–1.248) | 0.243 |
| Leflunomide | 0.850 (0.464–1.557) | 0.599 | 1.042 (0.713–1.523) | 0.832 |
| Methotrexate | 1.015 (0.964–1.069) | 0.573 | 1.008 (0.810–1.256) | 0.940 |
| Minocycline | 1.047 (0.848–1.293) | 0.670 | 0.701 (0.313–1.570) | 0.387 |
| Sulfasalazine | 0.954 (0.873–1.042) | 0.294 | 0.838 (0.675–1.040) | 0.108 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wallace, B.I.; Harris, C.A.; Wang, L.; Liu, M.; Chen, J.-S.; Kuo, C.-F.; Chung, K.C. Impact of Cumulative Corticosteroid Dosage on Preventable Hospitalization among Taiwanese Patients with Ankylosing Spondylitis and Inflammatory Bowel Disease. J. Clin. Med. 2019, 8, 614. https://doi.org/10.3390/jcm8050614
Wallace BI, Harris CA, Wang L, Liu M, Chen J-S, Kuo C-F, Chung KC. Impact of Cumulative Corticosteroid Dosage on Preventable Hospitalization among Taiwanese Patients with Ankylosing Spondylitis and Inflammatory Bowel Disease. Journal of Clinical Medicine. 2019; 8(5):614. https://doi.org/10.3390/jcm8050614
Chicago/Turabian StyleWallace, Beth I., Chelsea A. Harris, Lu Wang, Mochuan Liu, Jung-Sheng Chen, Chang-Fu Kuo, and Kevin C. Chung. 2019. "Impact of Cumulative Corticosteroid Dosage on Preventable Hospitalization among Taiwanese Patients with Ankylosing Spondylitis and Inflammatory Bowel Disease" Journal of Clinical Medicine 8, no. 5: 614. https://doi.org/10.3390/jcm8050614
APA StyleWallace, B. I., Harris, C. A., Wang, L., Liu, M., Chen, J.-S., Kuo, C.-F., & Chung, K. C. (2019). Impact of Cumulative Corticosteroid Dosage on Preventable Hospitalization among Taiwanese Patients with Ankylosing Spondylitis and Inflammatory Bowel Disease. Journal of Clinical Medicine, 8(5), 614. https://doi.org/10.3390/jcm8050614





