Long-Term Safety and Real-World Effectiveness of Trastuzumab in Breast Cancer
Abstract
1. Introduction
2. Materials and Methods
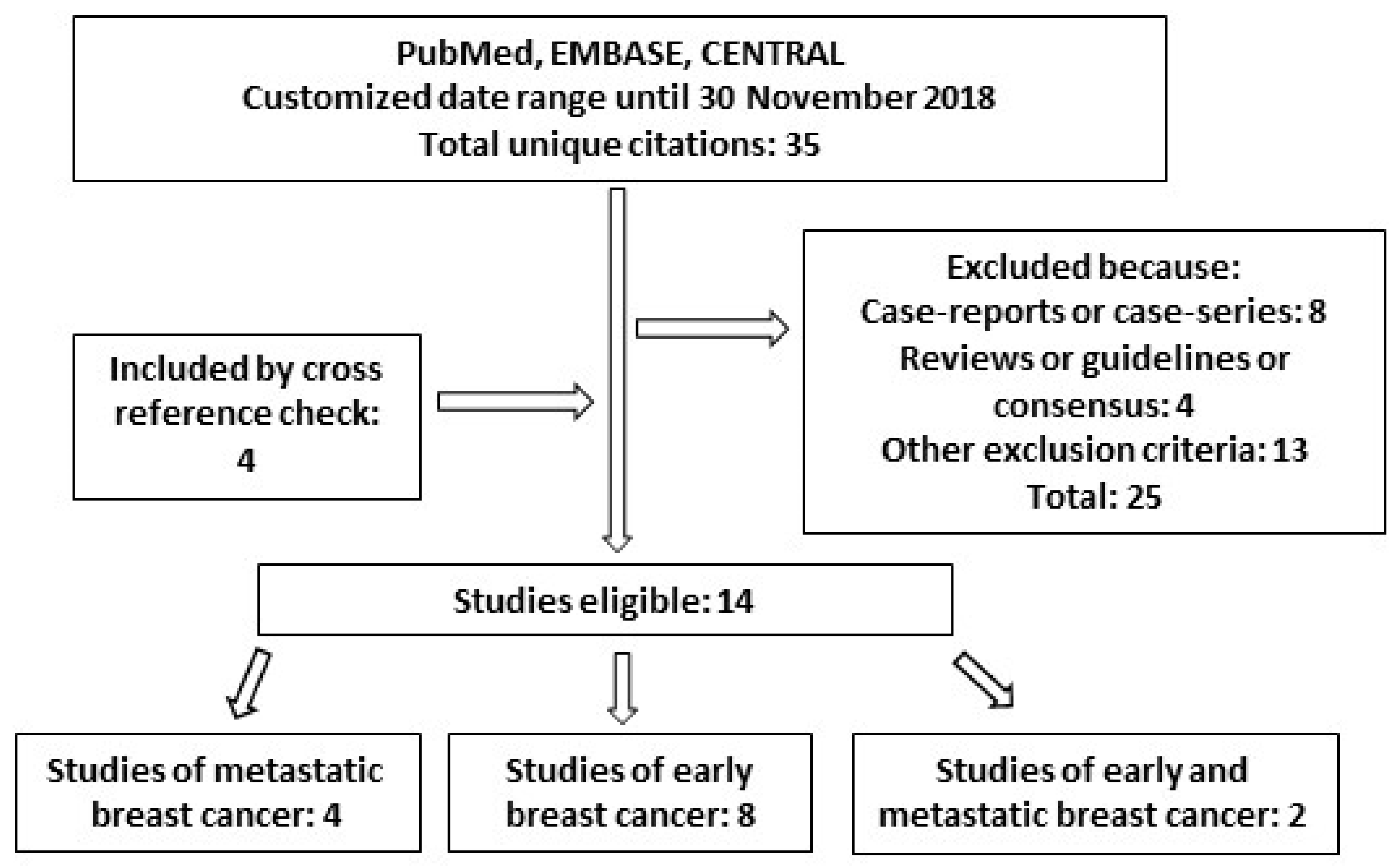
2.1. Long-Term Safety
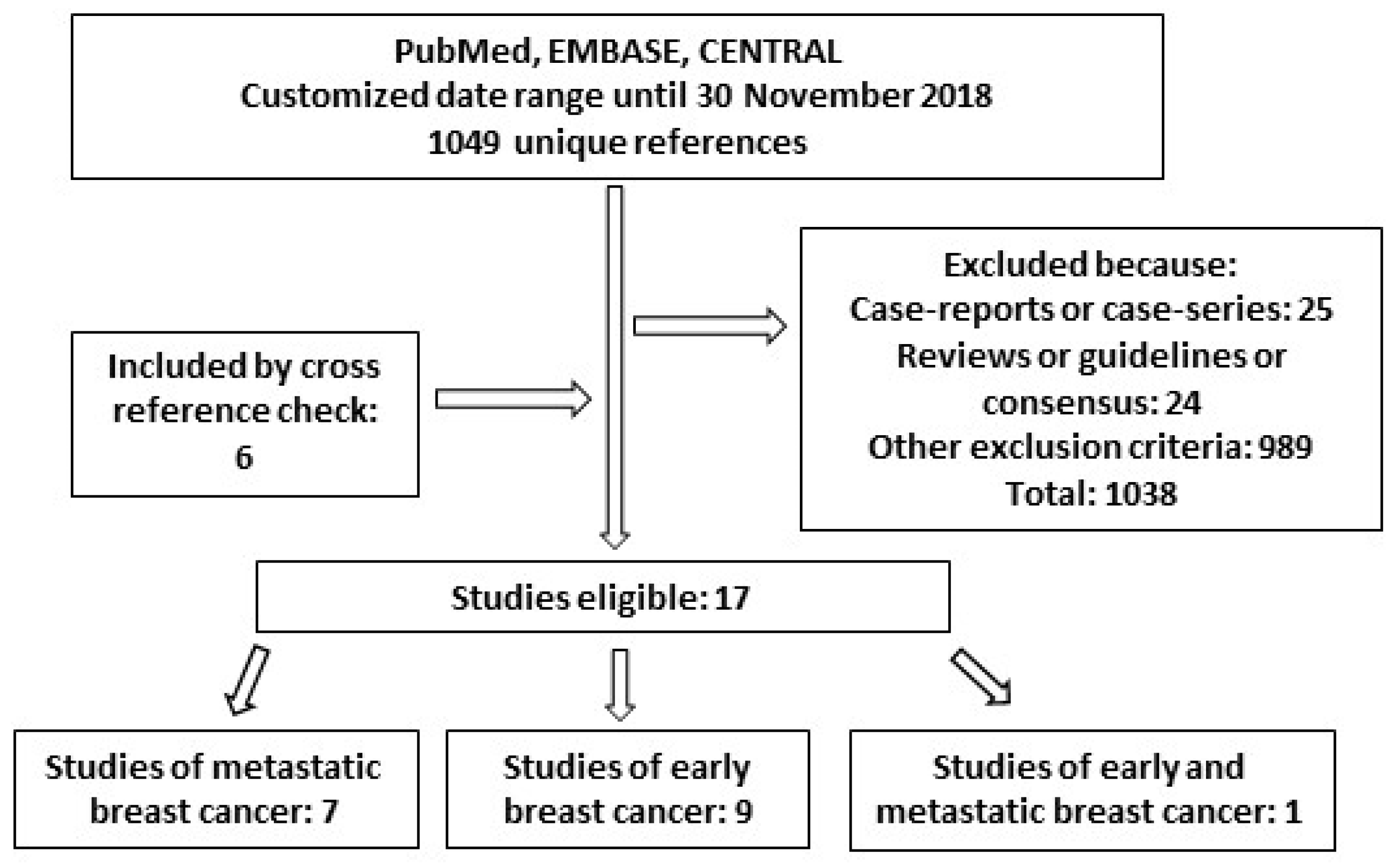
2.2. Real-World Effectiveness
3. Long-Term Safety
3.1. Early Breast Cancer
3.2. Metastatic Breast Cancer
3.3. Early and Metastatic Breast Cancer
4. Real World Effectiveness
4.1. Early Breast Cancer
4.2. Metastatic Breast Cancer
4.3. Early Breast Cancer and Metastatic Breast Cancer
5. Discussion
6. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Owens, M.A.; Horten, B.C.; Da Silva, M.M. HER2amplification ratios by fluorescence in situ hybridization and correlation with immunohistochemistry in a cohort of 6556 breast cancer tissues. Clin. Breast Cancer 2004, 5, 63–69. [Google Scholar] [CrossRef] [PubMed]
- Slamon, D.; Clark, G.; Wong, S.; Levin, W.; Ullrich, A.; McGuire, W. Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 1987, 235, 177–182. [Google Scholar] [CrossRef] [PubMed]
- Viani, G.A.; Afonso, S.L.; Stefano, E.J.; De Fendi, L.I.; Soares, F.V. Adjuvant trastuzumab in the treatment of HER2-positive early breast cancer: A meta-analysis of published randomized trials. BMC Cancer 2007, 7, 153. [Google Scholar] [CrossRef] [PubMed]
- Im, Y.; Odarchenko, P.; Grecea, D.; Komov, D.; Anatoliy, C.V.; Gupta, S.; Shparyk, Y.V.; Caguioa, P.B.; Makhson, A.; Krasnozhon, D.; et al. Double-blind, randomized, parallel group, phase III study to demonstrate equivalent efficacy and comparable safety of CT-P6 and trastuzumab, both in combination with paclitaxel, in patients with metastatic breast cancer (mbc) as first-line treatment. J. Clin. Oncol. 2013, 31, 629. [Google Scholar]
- Stebbing, J.; Baranau, Y.V.; Baryash, V.; Manikhas, A.; Moiseyenko, V.; Dzagnidze, G.; Javrid, E.; Boliukh, D.; Stroyakovskiy, D.; Pikiel, J.; et al. Double-blind, randomized phase III study to compare the efficacy and safety of CT-P6 trastuzumab biosimilar candidate versus trastuzumab as neoadjuvant treatment in her2 positive early breast cancer (ebc). J. Clin. Oncol. 2017, 35, 510. [Google Scholar] [CrossRef]
- Cameron, D.; Piccart-Gebhart, M.J.; Gelber, R.D.; Procter, M.; Goldhirsch, A.; De Azambuja, E.; Castro, G.; Untch, M.; Smith, I.; Gianni, L.; et al. 11 years’ follow-up of trastuzumab after adjuvant chemotherapy in HER2-positive early breast cancer: Final analysis of the HERceptin Adjuvant (HERA) trial. Lancet 2017, 389, 1195–1205. [Google Scholar] [CrossRef]
- Romond, E.H.; Perez, E.A.; Bryant, J.; Suman, V.J.; Geyer, C.E.; Davidson, N.E.; Tan-Chiu, E.; Martino, S.; Paik, S.; Kaufman, P.A.; et al. Trastuzumab plus adjuvant chemotherapy for operable HER2-positive breast cancer. N. Engl. J. Med. 2005, 353, 1673–1684. [Google Scholar] [CrossRef]
- Slamon, D.; Eiermann, W.; Robert, N.; Pienkowski, T.; Martín, M.; Press, M.; Mackey, J.; Glaspy, J.; Chan, A.; Pawlicki, M.; et al. Adjuvant trastuzumab in HER2-positive breast cancer. N. Engl. J. Med. 2011, 365, 1273–1283. [Google Scholar] [CrossRef]
- Natoli, C.; Vici, P.; Sperduti, I.; Grassadonia, A.; Bisagni, G.; Tinari, N.; Michelotti, A.; Zampa, G.; Gori, S.; Moscetti, L.; et al. Effectiveness of neoadjuvant trastuzumab and chemotherapy in HER2-overexpressing breast cancer. J. Cancer Res. Clin. Oncol. 2013, 139, 1229–1240. [Google Scholar] [CrossRef]
- Lidbrink, E.; Erfan, J.; Chmielowska, E.; Otremba, B.; Bouhlel, A.; Lauer, S.; Hermoso, M.L.; Nüesch, E.; Shing, M.; Misra, V. OHERA: A real world study of cardiac events in >3700 patients with her2-positive early breast cancer treated with trastuzumab: Final analysis. Ann. Oncol. 2017, 28 (suppl. 5), v43–v67. [Google Scholar] [CrossRef]
- Goldhar, H.A.; Yan, A.T.; Ko, D.T.; Earle, C.C.; Tomlinson, G.A.; Trudeau, M.E.; Krahn, M.D.; Krzyzanowska, M.K.; Pal, R.S.; Brezden-Masley, C.; et al. The Temporal Risk of Heart Failure Associated With Adjuvant Trastuzumab in Breast Cancer Patients: A Population Study. J. Natl. Cancer Inst. 2015, 108. [Google Scholar] [CrossRef] [PubMed]
- Seferina, S.C.; De Boer, M.; Derksen, M.W.; Berkmortel, F.V.D.; Van Kampen, R.J.; Van De Wouw, A.J.; Joore, M.; Peer, P.G.; Voogd, A.C.; Tjan-Heijnen, V.C.; et al. Cardiotoxicity and Cardiac Monitoring During Adjuvant Trastuzumab in Daily Dutch Practice: A Study of the Southeast Netherlands Breast Cancer Consortium. Oncologist 2016, 21, 555–562. [Google Scholar] [CrossRef] [PubMed]
- Spano, J.P.; Beuzeboc, P.; Coeffic, D.; Arnould, L.; Lortholary, A.; Andre, F.; Ferrero, J.M.; et al. Long term HER2+ metastatic breast cancer survivors treated by trastuzumab: Results from the French cohort study LHORA. Breast 2015, 24, 376–383. [Google Scholar] [CrossRef] [PubMed]
- Rossi, M.; Carioli, G.; Bonifazi, M.; Zambelli, A.; Franchi, M.; Moja, L.; Zambon, A.; Corrao, G.; La Vecchia, C.; Zocchetti, C.; et al. Trastuzumab for HER2+ metastatic breast cancer in clinical practice: Cardiotoxicity and overall survival. Eur. J. Cancer 2016, 52, 41–49. [Google Scholar] [CrossRef] [PubMed]
- Müller, V.; Clemens, M.; Jassem, J.; Al-Sakaff, N.; Auclair, P.; Nüesch, E.; Holloway, D.; Shing, M.; Bang, Y.-J.; et al. Long-term trastuzumab (Herceptin®) treatment in a continuation study of patients with HER2-positive breast cancer or HER2-positive gastric cancer. BMC Cancer 2018, 18, 295. [Google Scholar] [CrossRef] [PubMed]
- Yeo, B.; Kotsori, K.; Mohammed, K.; Walsh, G.; Smith, I. Long-term outcome of HER2 positive metastatic breast cancer patients treated with first-line trastuzumab. Breast 2015, 24, 751–757. [Google Scholar] [CrossRef] [PubMed]
- Huang, P.; Dai, S.; Ye, Z.; Liu, Y.; Chen, Z.; Zheng, Y.; Shao, X.; Lei, L.; Wang, X. Long-term tolerance and cardiac function in breast cancer patients receiving trastuzumab therapy. Oncotarget 2017, 8, 2069–2075. [Google Scholar] [CrossRef]
- Sun, Y.; Li, T.; Zhang, Y.; Zhang, Q. Evaluation of Left Ventricular Ejection Fractions in Breast Cancer Patients Undergoing Long-Term Trastuzumab Treatment. Med. Sci. Monit. 2016, 22, 5035–5040. [Google Scholar] [CrossRef]
- Seferina, S.C.; Lobbezoo, D.J.A.; De Boer, M.; Dercksen, M.W.; Berkmortel, F.V.D.; Van Kampen, R.J.W.; Van De Wouw, A.J.; De Vries, B.; Joore, M.A.; Peer, P.G.M.; et al. Real-Life Use and Effectiveness of Adjuvant Trastuzumab in Early Breast Cancer Patients: A Study of the Southeast Netherlands Breast Cancer Consortium. Oncologist 2015, 20, 856–863. [Google Scholar] [CrossRef]
- Adusumilli, P.; Konatam, M.; Gundeti, S.; Bala, S.; Maddali, L.S. Treatment Challenges and Survival Analysis of Human Epidermal Growth Factor Receptor 2-positive Breast Cancer in Real World. Indian J. Med. Paediatr. Oncol. 2017, 38, 22–27. [Google Scholar] [CrossRef]
- Vici, P.; Pizzuti, L.; Natoli, C.; Moscetti, L.; Mentuccia, L.; Vaccaro, A.; Sergi, D.; Di Lauro, L.; Trenta, P.; Seminara, P.; et al. Outcomes of HER2-positive early breast cancer patients in the pre-trastuzumab and trastuzumab eras: A real-world multicenter observational analysis. The RETROHER study. Breast Cancer Res. Treat. 2014, 147, 599–607. [Google Scholar] [CrossRef] [PubMed]
- Vici, P.; Pizzuti, L.; Sperduti, I.; Frassoldati, A.; Natoli, C.; Gamucci, T.; Tomao, S.; Michelotti, A.; Moscetti, L.; Gori, S.; et al. Triple positive" early breast cancer: An observational multicenter retrospective analysis of outcome. Oncotarget 2016, 7, 17932–17944. [Google Scholar] [CrossRef] [PubMed]
- Mustacchi, G.; Puglisi, F.; Molino, A.; Crivellari, D.; Ghiotto, C.; Ferro, A.; Brunello, A.; Saracchini, S.; Turazza, M.; Cretella, E.; et al. Observational study on adjuvant trastuzumab in HER2-positive early breast cancer patients. Future Oncol. 2015, 11, 1493–1500. [Google Scholar] [CrossRef] [PubMed]
- Gori, S.; Inno, A.; Fiorio, E.; Foglietta, J.; Ferro, A.; Gulisano, M.; Pinotti, G.; Gubiotti, M.; Cavazzini, M.G.; Turazza, M.; et al. The Promher Study: An Observational Italian Study on Adjuvant Therapy for HER2-Positive, pT1a-b pN0 Breast Cancer. PLoS ONE 2015, 10, e0136731. [Google Scholar]
- Takada, M.; Ishiguro, H.; Nagai, S.; Ohtani, S.; Kawabata, H.; Yanagita, Y.; Hozumi, Y.; Shimizu, C.; Takao, S.; Sato, N.; et al. Survival of HER2-positive primary breast cancer patients treated by neoadjuvant chemotherapy plus trastuzumab: A multicenter retrospective observational study (JBCRG-C03 study). Breast Cancer Res. Treat. 2014, 145, 143–153. [Google Scholar] [CrossRef] [PubMed]
- Dall, P.; Koch, T.; Göhler, T.; Selbach, J.; Ammon, A.; Eggert, J.; Gazawi, N.; Rezek, D.; Wischnik, A.; Hielscher, C.; et al. Trastuzumab in Human Epidermal Growth Factor Receptor 2-Positive Early Breast Cancer: Results of a Prospective, Noninterventional Study on Routine Treatment Between 2006 and 2012 in Germany. Oncologist 2017, 22, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Daniels, B.; Kiely, B.E.; Lord, S.J.; Houssami, N.; Lu, C.Y.; Ward, R.L.; Pearson, S.-A. Trastuzumab for metastatic breast cancer: Real world outcomes from an Australian whole-of-population cohort (2001-2016). Breast 2018, 38, 7–13. [Google Scholar] [CrossRef]
- Daniels, B.; Kiely, B.E.; Lord, S.J.; Houssami, N.; Lu, C.Y.; Ward, R.L.; Pearson, S.-A. Long-term survival in trastuzumab-treated patients with HER2-positive metastatic breast cancer: Real-world outcomes and treatment patterns in a whole-of-population Australian cohort (2001–2016). Breast Cancer Res. Treat. 2018, 171, 151–159. [Google Scholar] [CrossRef]
- Parkinson, B.; Viney, R.; Haas, M.; Goodall, S.; Srasuebkul, P.; Pearson, S.-A. Real-World Evidence: A Comparison of the Australian Herceptin Program and Clinical Trials of Trastuzumab for HER2-Positive Metastatic Breast Cancer. PharmacoEconomics 2016, 34, 1039–1050. [Google Scholar] [CrossRef]
- Tripathy, D.; Kaufman, P.A.; Brufsky, A.M.; Mayer, M.; Yood, M.U.; Yoo, B.; Quah, C.; Yardley, D.; Rugo, H.S.; et al. First-line treatment patterns and clinical outcomes in patients with HER2-positive and hormone receptor-positive metastatic breast cancer from registHER. Oncologist 2013, 18, 501–510. [Google Scholar] [CrossRef]
- Kaufman, P.A.; Wang, L.I.; Quah, C.S.; Brufsky, A.M.; Mayer, M.; Rugo, H.S.; Tripathy, D.; Yood, M.U.; Feng, S.; Yardley, D.A.; et al. Treatment patterns and clinical outcomes in elderly patients with HER2-positive metastatic breast cancer from the registHER observational study. Breast Cancer Res. Treat. 2012, 135, 875–883. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Wang, S.; Wang, Y. Disparities of Trastuzumab Use in Resource-Limited or Resource-Abundant Regions and Its Survival Benefit on HER2 Positive Breast Cancer: A Real-World Study from China. Oncologist 2017, 22, 1333–1338. [Google Scholar] [CrossRef] [PubMed]
- Russell, S.D.; Blackwell, K.L.; Lawrence, J.; Pippen, J.E.; Roe, M.T.; Wood, F.; Paton, V.; Holmgren, E.; Mahaffey, K.W.; et al. Independent adjudication of symptomatic heart failure with the use of doxorubicin and cyclophosphamide followed by trastuzumab adjuvant therapy: A combined review of cardiac data from the National Surgical Adjuvant breast and Bowel Project B-31 and the North Central Cancer Treatment Group N9831 clinical trials. J. Clin. Oncol. 2010, 28, 3416–3421. [Google Scholar] [PubMed]
- Rochette, L.; Guenancia, C.; Gudjoncik, A.; Hachet, O.; Zeller, M.; Cottin, Y.; Vergely, C. Anthracyclines/trastuzumab: New aspects of cardiotoxicity and molecular mechanisms. Trends Pharmacol. Sci. 2015, 36, 326–348. [Google Scholar] [CrossRef] [PubMed]
- Chien, J.; Rugo, H.S. The cardiac safety of trastuzumab in the treatment of breast cancer. Expert Opin. Drug Saf. 2010, 9, 335–346. [Google Scholar] [CrossRef]
- Zeglinski, M.; Ludke, A.; Jassal, D.S.; Singal, P.K. Trastuzumab-induced cardiac dysfunction: A “dual-hit”. Exp. Clin. Cardiol. 2011, 16, 70–74. [Google Scholar] [PubMed]
- Piccart-Gebhart, M.J.; Procter, M.; Leyland-Jones, B. Trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer. N. Engl. J. Med. 2005, 353, 1659–1672. [Google Scholar] [CrossRef] [PubMed]
- De Azambuja, E.; Procter, M.J.; Van Veldhuisen, D.J.; Agbor-Tarh, D.; Metzger-Filho, O.; Steinseifer, J.; Untch, M.; Smith, I.E.; Gianni, L.; Baselga, J.; et al. Trastuzumab-associated cardiac events at 8 years of median follow-up in the Herceptin Adjuvant trial (BIG 1-01). J. Clin. Oncol. 2014, 32, 2159–2165. [Google Scholar] [CrossRef] [PubMed]
- Romond, E.H.; Jeong, J.-H.; Rastogi, P.; Swain, S.M.; Geyer, C.E.; Ewer, M.S.; Rathi, V.; Fehrenbacher, L.; Brufsky, A.; Azar, C.A.; et al. Seven-year follow-up assessment of cardiac function in NSABP B-31, a randomized trial comparing doxorubicin and cyclophosphamide followed by paclitaxel (ACP) with ACP plus trastuzumab as adjuvant therapy for patients with node-positive, human epidermal growth factor receptor 2-positive breast cancer. J. Clin. Oncol. 2012, 30, 3792–3799. [Google Scholar] [PubMed]
- Ganz, P.A.; Romond, E.H.; Cecchini, R.S.; Rastogi, P.; Geyer, C.E.; Swain, S.M.; Jeong, J.-H.; Fehrenbacher, L.; Gross, H.M.; Brufsky, A.M.; et al. Long-Term Follow-Up of Cardiac Function and Quality of Life for Patients in NSABP Protocol B-31/NRG Oncology: A Randomized Trial Comparing the Safety and Efficacy of Doxorubicin and Cyclophosphamide (AC) Followed by Paclitaxel With AC Followed by Paclitaxel and Trastuzumab in Patients With Node-Positive Breast Cancer With Tumors Overexpressing Human Epidermal Growth Factor Receptor 2. J. Clin. Oncol. 2017, 35, 3942–3948. [Google Scholar]
- Advani, P.P.; Ballman, K.V.; Dockter, T.J.; Colon-Otero, G.; Perez, E.A. Long-Term Cardiac Safety Analysis of NCCTG N9831 (Alliance) Adjuvant Trastuzumab Trial. J. Clin. Oncol. 2016, 34, 581–587. [Google Scholar] [CrossRef] [PubMed]
- Joensuu, H.; Bono, P.; Kataja, V.; Alanko, T.; Kokko, R.; Asola, R.; Utriainen, T.; Turpeenniemi-Hujanen, T.; Jyrkkiö, S.; Moykkynen, K.; et al. Fluorouracil, epirubicin, and cyclophosphamide with either docetaxel or vinorelbine, with or without trastuzumab, as adjuvant treatments of breast cancer: Final results of the FinHer Trial. J. Clin. Oncol. 2009, 27, 5685–5692. [Google Scholar] [CrossRef]
- Swain, S.M.; Baselga, J.; Kim, S.-B.; Ro, J.; Semiglazov, V.; Campone, M.; Ciruelos, E.; Ferrero, J.-M.; Schneeweiss, A.; Heeson, S.; et al. Pertuzumab, trastuzumab, and docetaxel in HER2-positive metastatic breast cancer. N. Engl. J. Med. 2015, 372, 724–734. [Google Scholar] [CrossRef] [PubMed]
- Buzdar, A.U.; Ibrahim, N.K.; Francis, D.; Booser, D.J.; Thomas, E.S.; Theriault, R.L.; Pusztai, L.; Green, M.C.; Arun, B.K.; Giordano, S.H.; et al. Significantly higher pathologic complete remission rate after neoadjuvant therapy with trastuzumab, paclitaxel, and epirubicin chemotherapy: Results of a randomized trial in human epidermal growth factor receptor 2-positive operable breast cancer. J. Clin. Oncol. 2005, 23, 3676–3685. [Google Scholar] [CrossRef] [PubMed]
- Dawood, S.; Gonzalez-Angulo, A.M.; Peintinger, F.; Broglio, K.; Symmans, W.F.; Kau, S.W.; Islam, R.; Hortobagyi, G.N.; Buzdar, A.U. Efficacy and safety of neoadjuvant trastuzumab combined with paclitaxel and epirubicin: A retrospective review of the M. D. Anderson experience. Cancer 2007, 110, 1195–1200. [Google Scholar] [CrossRef] [PubMed]
- Pizzuti, L.; Barba, M.; Giannarelli, D.; Sergi, D.; Botti, C.; Marchetti, P.; Anzà, M.; Maugeri-Saccà, M.; Natoli, C.; Di Filippo, S.; et al. Neoadjuvant Sequential Docetaxel Followed by High-Dose Epirubicin in Combination With Cyclophosphamide Administered Concurrently With Trastuzumab. The DECT Trial. J. Cell. Physiol. 2016, 231, 2541–2547. [Google Scholar] [CrossRef]
- Untch, M.; Fasching, P.A.; Konecny, G.E.; Hasmüller, S.; Lebeau, A.; Kreienberg, R.; Camara, O.; Müller, V.; Du Bois, A.; Kühn, T.; et al. Pathologic complete response after neoadjuvant chemotherapy plus trastuzumab predicts favorable survival in human epidermal growth factor receptor 2-overexpressing breast cancer: Results from the TECHNO trial of the AGO and GBG study groups. J. Clin. Oncol. 2011, 29, 3351–3357. [Google Scholar] [CrossRef]
- Gianni, L.; Eiermann, W.; Semiglazov, V.; Manikhas, A.; Lluch, A.; Tjulandin, S.; Zambetti, M.; Vazquez, F.; Byakhow, M.; Lichinitser, M.; et al. Neoadjuvant chemotherapy with trastuzumab followed by adjuvant trastuzumab versus neoadjuvant chemotherapy alone, in patients with HER2-positive locally advanced breast cancer (the NOAH trial): A randomised controlled superiority trial with a parallel HER2-negative cohort. Lancet 2010, 375, 377–384. [Google Scholar] [PubMed]
- Untch, M.; Rezai, M.; Loibl, S.; Fasching, P.A.; Huober, J.; Tesch, H.; Bauerfeind, I.; Hilfrich, J.; Eidtmann, H.; Gerber, B.; et al. Neoadjuvant treatment with trastuzumab in HER2-positive breast cancer: Results from the GeparQuattro study. J. Clin. Oncol. 2010, 28, 2024–2031. [Google Scholar] [CrossRef] [PubMed]
| Study [Reference] | Median Follow-Up | Total Patients (N) | Arm and Patients (N) | Duration of H Administration | Cardiotox Secondary | Cardiotox Primary | |
|---|---|---|---|---|---|---|---|
| eBC | HERA trial (BIG 1-01) [6] | 11 years | 5099 | 1 year H (1702) | 1 year | 4.4% | 1% |
| 2 years H (1700) | 2 years | 7.3% | 1% | ||||
| none (1697) | none | 0.9% | 0.1% | ||||
| NSABP B-31 [7] | 7 years | 1861 | AC → P + H (960) | 1 year | 5.3% | 3.9% | |
| AC → P (901) | none | 2.0% | 1.5% | ||||
| NCCTG N9831 (Alliance) [7] | 6 years | 1944 | AC → P (664) | None | - | 0.6% | |
| AC → P → H (710) | 1 year | - | 2.8% | ||||
| AC → P+H (570) | 1 year | - | 3.4% | ||||
| BCIRG 006 study [8] | 65 months | 3222 | AC → T (1073) | None | 11.2% | 0.7% | |
| AC → T+H (1074) | 1 year | 18.6% | 2.0% | ||||
| TCH (1075) | 1 year | 9.4% | 0.4% | ||||
| FinHer Trial [9] | 62 months | 232 | FEC → T or V (116) | None | 10.5% | 1.7% | |
| FEC → T or V + H (115) | 9 weeks | 6.8% | 0.9% | ||||
| Final analysis of the OHERA study [10] | 5 years | 3733 | H + cht | 11.8 months | 17.5% | 2.8% | |
| The Temporal Risk of HF Associated with Adjuvant Trastuzumab in BC Patients: A Population Study [11] | 5.9 years | 19074 | H + cht (3371) | 1 year | 5.2% | ||
| Cht (15,703) | none | 2.5% | |||||
| Cardiotoxicity and Cardiac Monitoring During Adjuvant Trastuzumab in Daily Dutch Practice: A Study of the Southeast Netherlands Breast Cancer Consortium [12] | 5 years | 230 | H + cht | 1 year | 3.9% | 8.7% | |
| MBC | LHORA study (long responder, first line PFS >3 years) [13] | 8 years | 154 | first line treatment with H + cht | 4.5 years | 2.2% | 0.7% |
| Trastuzumab for HER2+ metastatic breast cancer in clinical practice: Cardiotoxicity and overall survival [14] | 5 years | 681 | Any treatment with H | - | 7.2% | ||
| The Rollover Protocol (ROP) Study [15] | >5 years | 19 | Any treatment with H | 8.7 years | 0% | ||
| Long-term outcome of HER2 positive metastatic breast cancer patients treated with first-line trastuzumab [16] | 10 years | 215 | first line treatment with H + cht | 2.6 years | 13% | 2% | |
| e/M BC | Long-term tolerance and cardiac function in breast cancer patients receiving trastuzumab therapy [17] | 5 years | 94 | Adj or metastatic H | 15.7 months | 12.8% | - |
| Evaluation of LVEF in Breast Cancer Patients Undergoing Long-Term Trastuzumab Treatment [18] | 5 years | 105 | Adj or metastatic H | 15.7 months | 5.4% | ||
| Study [Reference] | Median Follow-Up | Patients (N) | Arm And Patients (N) | Duration of H Administration | DFS/PFS/RFS (% or Median) | OS/BCSS (% or Median) | |
|---|---|---|---|---|---|---|---|
| eBC | Effectiveness of neoadjuvant trastuzumab and cht in HER2+ BC [9] | 32 months | 205 | NACT + H | 24 weeks (median) | 5 y DFS 73.3% | 5 y CSS: 82.8% |
| Real-Life Use and Effectiveness of Adjuvant Trastuzumab in eBC Patients: A Study of the Southeast Netherlands Breast Cancer Consortium [19] | 5 years | 476 | Cht + H (230) | 17 cycles (median) | 5 y DFS 80.7% | 5 y OS: 90.7% | |
| Cht (246) | - | 5 y DFS 68.2% | 5 y OS: 77.4% | ||||
| Treatment Challenges and Survival Analysis of Human Epidermal Growth Factor Receptor 2-positive Breast Cancer in Real World [20] | 7 years | 212 | Cht + H (76) | NA | 5 y DFS 92% | 5 y OS: 90.5% | |
| Cht (136) | - | 5 y DFS 52.6% | 5 y OS: 41.7% | ||||
| The RETROHER study [21] | 65 months | 925 | Cht + H (573) | 52 weeks (median) | 5 y DFS 88.6% | OS 5 y: 96%; 10 y: 93.3% | |
| Cht (352) | - | 5 y DFS 71% | OS 5 y: 88.4%; 10 y: 72.3% | ||||
| “Triple positive” early breast cancer: an observational multicenter retrospective analysis of outcome [22] | 78 months | 872 | Cht + H (506) | 52 weeks (median) | 5 y RFS 89.9% | BCSS 5 y: 97.4%; 10 y: 92% | |
| Cht (366) | - | 5 y RFS 78.2% | BCSS 5 y: 93.9%; 10 y: 82% | ||||
| Observational study on adjuvant trastuzumab in HER2-positive early breast cancer patients [23] | 50 months | 1245 | Cht + H | NA | 10.9% RFS | - | |
| No adj therapy | - | 22.6% RFS | - | ||||
| The Promher Study [24] | 39 months | 303 | Cht + H (204) | NA | 5y DFS 95% | - | |
| Cht alone (65) | - | 5y DFS 94.3% | - | ||||
| No adj therapy (34) | - | 5y DFS 69.6% | - | ||||
| JBCRG-C03 study [25] | 42 months | 829 | NACT + H | NA | 3y DFS 87% | - | |
| Trastuzumab in HER2+ eBC: Results of a Prospective, Noninterventional Study on Routine Treatment Between 2006 and 2012 in Germany [26] | 39 months | 4027 | Cht + H | 18 cycles (median) | 3y DFS 90% 5y DFS 82.8% | 3y OS 96.8% 5y OS 90% | |
| MBC | LHORA study (long responder, first line PFS > 3 y) [13] | - | 128 | Cht + H | 5.3 y (median) | Median PFS 6.4y | - |
| Trastuzumab for metastatic breast cancer: Real world outcomes from an Australian whole-of-population cohort (2001–2016) [27] | 6.7 years | 5899 | 2001–08 (3122) | 15 m (median) | - | Median 27 m | |
| 2009–15 (2777) | 18.4 m (median) | - | Median 37.7 m | ||||
| Real-World Evidence: A Comparison of the Australian Herceptin Program and Clinical Trials of Trastuzumab for HER2+ Metastatic Breast Cancer [28] | 1.7 years | 3617 | H + cht | 51.9 weeks (median) | Median PFS 8.3 m | Median 29.8 m | |
| Long-term survival in trastuzumab-treated patients with HER2- positive metastatic breast cancer: real-world outcomes and treatment patterns in a whole-of-population Australian cohort (2001–2016) [29] | 9.4 years | 1082 | H + cht alive > 5 years from initial treatment | 58.9 m (median) | - | Median 78.9 m (from 5th year) | |
| First-Line Treatment Patterns and Clinical Outcomes in Patients With HER2+ and Hormone Receptor-Positive MBC From registHER [30] | 27 months | 964 | HR+/HER2+ (530) | NA | Median PFS 11.7 m | Median 41.5 m | |
| HR−/HER2+ (434) | NA | Median PFS 8.8 m | Median 28.6 m | ||||
| Trastuzumab for HER2+ metastatic breast cancer in clinical practice: Cardiotoxicity and overall survival [14] | 5 years | 681 | H + cht | NA | - | 5 y: 37.2% | |
| Treatment patterns and clinical outcomes in elderly patients with HER2-positive metastatic breast cancer from the registHER observational study [31] | 27 months | 209 | H in first line | NA | Median PFS 11.7 m | Median 31.2 m | |
| No H in first line | - | Median PFS 4.6 m | Median 29.5m | ||||
| e/MBC | Disparities of Trastuzumab Use in Resource-Limited or Resource-Abundant Regions and Its Survival Benefit on HER2 Positive Breast Cancer: A Real-World Study from China [32] | - | 1139 | eBC, yes H (397) | 12 m | Median DFS 30 m | - |
| eBC, no H (486) | - | Median DFS 21 m | - | ||||
| MBC, yes H (366) | 10 m | Median PFS 13 m | - | ||||
| MBC, no H (354) | - | Median PFS 7 m | - |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mazzotta, M.; Krasniqi, E.; Barchiesi, G.; Pizzuti, L.; Tomao, F.; Barba, M.; Vici, P. Long-Term Safety and Real-World Effectiveness of Trastuzumab in Breast Cancer. J. Clin. Med. 2019, 8, 254. https://doi.org/10.3390/jcm8020254
Mazzotta M, Krasniqi E, Barchiesi G, Pizzuti L, Tomao F, Barba M, Vici P. Long-Term Safety and Real-World Effectiveness of Trastuzumab in Breast Cancer. Journal of Clinical Medicine. 2019; 8(2):254. https://doi.org/10.3390/jcm8020254
Chicago/Turabian StyleMazzotta, Marco, Eriseld Krasniqi, Giacomo Barchiesi, Laura Pizzuti, Federica Tomao, Maddalena Barba, and Patrizia Vici. 2019. "Long-Term Safety and Real-World Effectiveness of Trastuzumab in Breast Cancer" Journal of Clinical Medicine 8, no. 2: 254. https://doi.org/10.3390/jcm8020254
APA StyleMazzotta, M., Krasniqi, E., Barchiesi, G., Pizzuti, L., Tomao, F., Barba, M., & Vici, P. (2019). Long-Term Safety and Real-World Effectiveness of Trastuzumab in Breast Cancer. Journal of Clinical Medicine, 8(2), 254. https://doi.org/10.3390/jcm8020254




