Near-Infrared Spectroscopy Monitoring in Cardiac and Noncardiac Surgery: Pairwise and Network Meta-Analyses
Abstract
1. Introduction
2. Materials and Methods
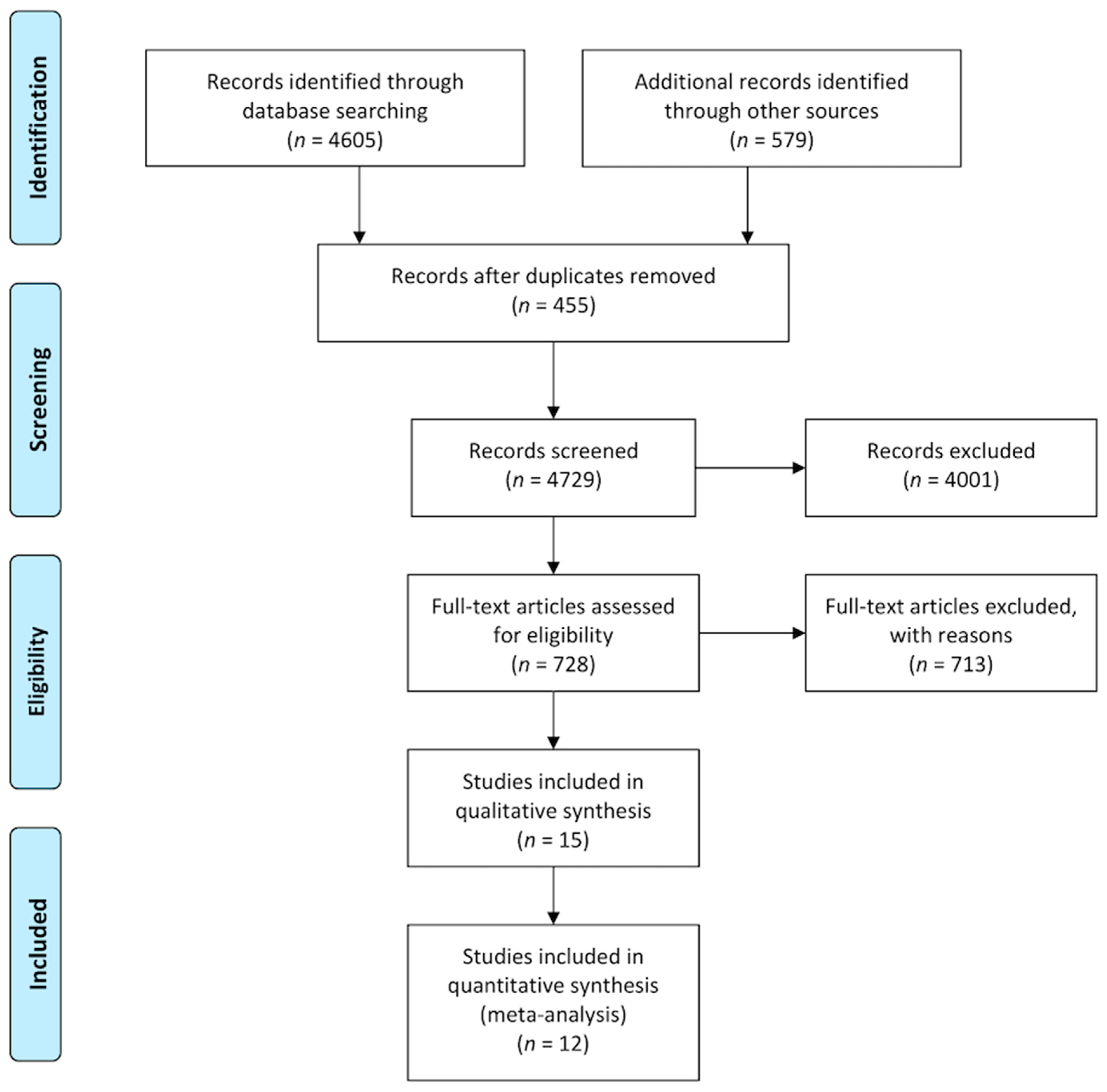
2.1. Systematic Review Process
2.2. Statistical Analysis
3. Results
3.1. Study Characteristics
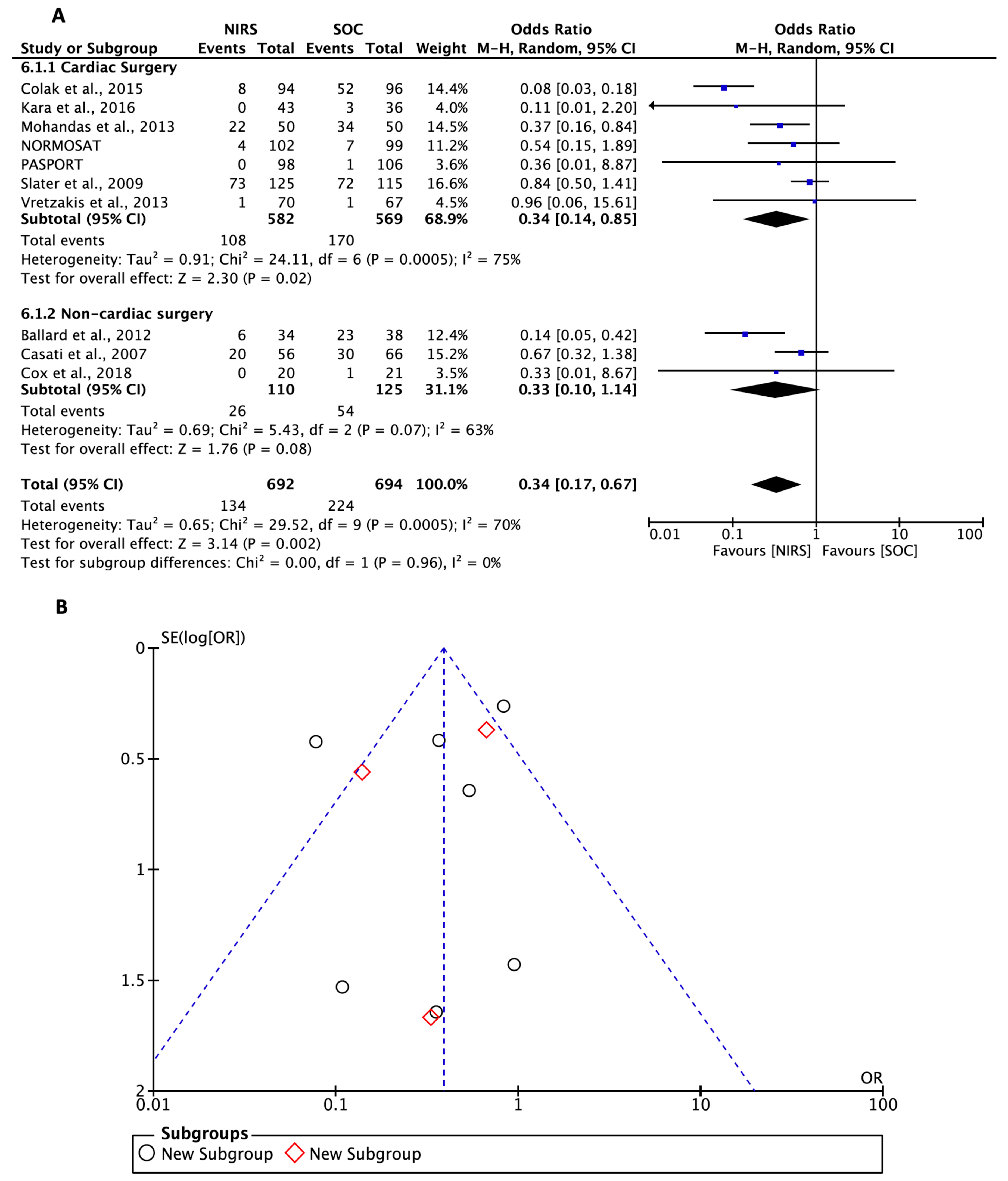
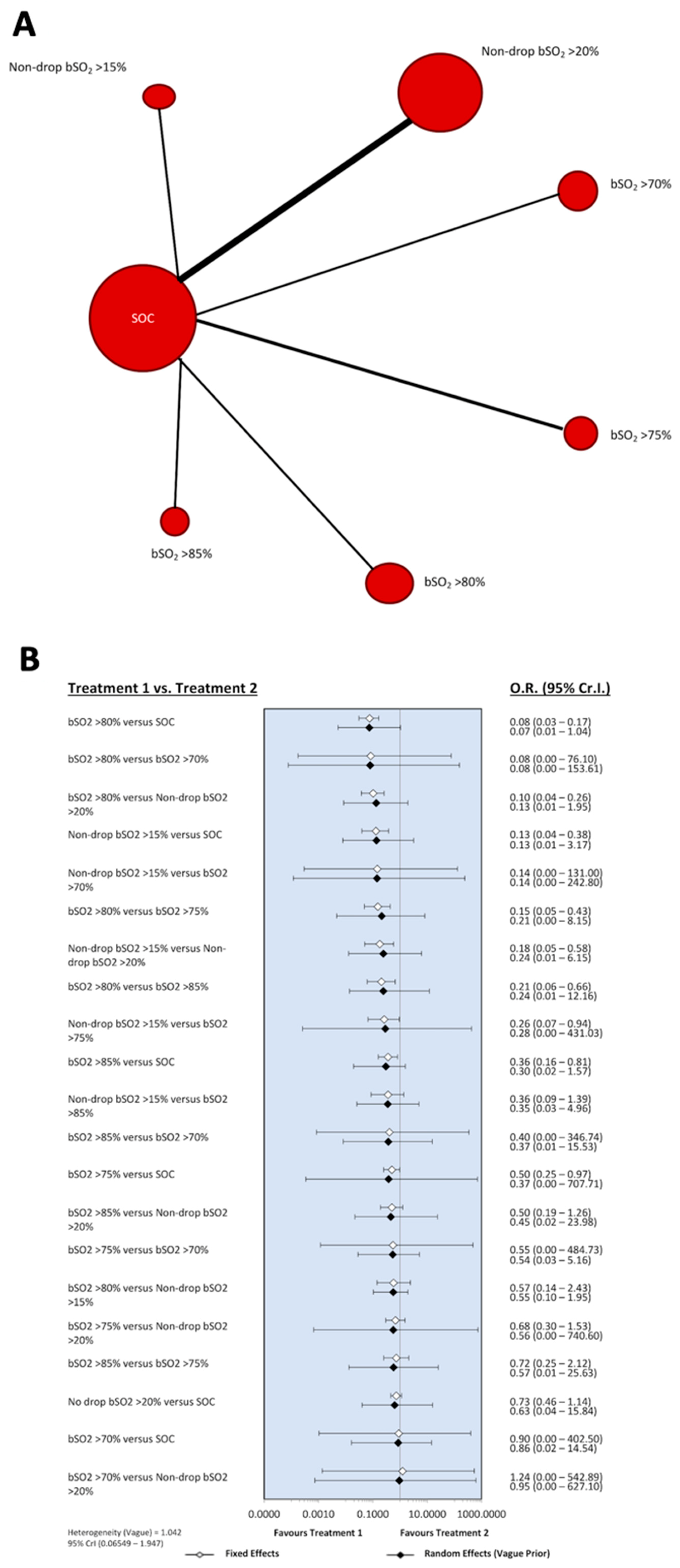
3.2. Outcomes
4. Discussion
4.1. Major Findings
4.2. Strengths and Limitations
4.3. Clinical Implications
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ortega-Loubon, C.; Fernandez-Molina, M.; Carrascal-Hinojal, Y.; Fulquet-Carreras, E. Cardiac surgery-associated acute kidney injury. Ann. Card. Anaesth. 2016, 19, 687–698. [Google Scholar] [CrossRef] [PubMed]
- Ortega-Loubon, C.; Fernandez-Molina, M.; Paneda-Delgado, L.; Jorge-Monjas, P.; Carrascal, Y. Predictors of Postoperative Acute Kidney Injury after Coronary Artery Bypass Graft Surgery. Braz. J. Cardiovasc. Surg. 2018, 33, 323–329. [Google Scholar] [CrossRef] [PubMed]
- Goren, O.; Matot, I. Perioperative acute kidney injury. Br. J. Anaesth. 2015, 115, ii3–ii14. [Google Scholar] [CrossRef] [PubMed]
- Weissman, C. Pulmonary complications after cardiac surgery. Semin. Cardiothorac. Vasc. Anesth. 2004, 8, 185–211. [Google Scholar] [CrossRef] [PubMed]
- Ranucci, M.; Baryshnikova, E.; Pistuddi, V.; Menicanti, L.; Frigiola, A.; Surgical and Clinical Outcome REsearch (SCORE) Group. The effectiveness of 10 years of interventions to control postoperative bleeding in adult cardiac surgery. Interact. Cardiovasc. Thorac. Surg. 2017, 24, 196–202. [Google Scholar] [CrossRef]
- Selnes, O.A.; Gottesman, R.F.; Grega, M.A.; Baumgartner, W.A.; Zeger, S.L.; McKhann, G.M. Cognitive and neurologic outcomes after coronary-artery bypass surgery. N. Engl. J. Med. 2012, 366, 250–257. [Google Scholar] [CrossRef] [PubMed]
- Cubero-Gallego, H.; Lorenzo, M.; Heredia, M.; Gomez, I.; Tamayo, E. Diagnosis of perioperative myocardial infarction after heart valve surgery with new cut-off point of high-sensitivity troponin T and new electrocardiogram or echocardiogram changes. J. Thorac. Cardiovasc. Surg. 2017, 154, 895–903. [Google Scholar] [CrossRef]
- Lomivorotov, V.V.; Efremov, S.M.; Kirov, M.Y.; Fominskiy, E.V.; Karaskov, A.M. Low-Cardiac-Output Syndrome After Cardiac Surgery. J. Cardiothorac. Vasc. Anesth. 2017, 31, 291–308. [Google Scholar] [CrossRef]
- Casati, A.; Fanelli, G.; Pietropaoli, P.; Proietti, R.; Tufano, R.; Danelli, G.; Fierro, G.; De Cosmo, G.; Servillo, G. Continuous monitoring of cerebral oxygen saturation in elderly patients undergoing major abdominal surgery minimizes brain exposure to potential hypoxia. Anesth. Analg. 2005, 101, 740–747. [Google Scholar] [CrossRef]
- Newman, S.; Stygall, J.; Hirani, S.; Shaefi, S.; Maze, M. Postoperative cognitive dysfunction after noncardiac surgery: A systematic review. Anesthesiology 2007, 106, 572–590. [Google Scholar] [CrossRef]
- Serraino, G.F.; Murphy, G.J. Effects of cerebral near-infrared spectroscopy on the outcome of patients undergoing cardiac surgery: A systematic review of randomised trials. BMJ Open 2017, 7, e016613. [Google Scholar] [CrossRef] [PubMed]
- Crosby, G.; Culley, D.J.; Dexter, F. Cognitive outcome of surgery: Is there no place like home? Anesth. Analg. 2014, 118, 898–900. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ortega-Loubon, C.; Fernandez-Molina, M.; Jorge-Monjas, P.; Fierro, I.; Herrera-Calvo, G.; Tamayo, E. The Relevance of Renal Oxygen Saturation Over Other Markers in Cardiac Surgery-Associated Acute Kidney Injury. J. Cardiothorac. Vasc. Anesth. 2018. [Google Scholar] [CrossRef] [PubMed]
- Ortega-Loubon, C.; Fernandez-Molina, M.; Fierro, I.; Jorge-Monjas, P.; Carrascal, Y.; Gomez-Herreras, J.I.; Tamayo, E. Postoperative kidney oxygen saturation as a novel marker for acute kidney injury after adult cardiac surgery. J. Thorac. Cardiovasc. Surg. 2018. [Google Scholar] [CrossRef] [PubMed]
- Mailhot, T.; Cossette, S.; Lambert, J.; Cournoyer, A.; Denault, A.Y. Cerebral oximetry as a biomarker of postoperative delirium in cardiac surgery patients. J. Crit. Care 2016, 34, 17–23. [Google Scholar] [CrossRef] [PubMed]
- Bevan, P.J. Should Cerebral Near-infrared Spectroscopy be Standard of Care in Adult Cardiac Surgery? Heart Lung Circ. 2015, 24, 544–550. [Google Scholar] [CrossRef]
- Hirsch, J.C.; Charpie, J.R.; Ohye, R.G.; Gurney, J.G. Near infrared spectroscopy (NIRS) should not be standard of care for postoperative management. Semin. Thorac. Cardiovasc. Surg. 2010, 13, 51–54. [Google Scholar] [CrossRef]
- Tweddell, J.S.; Ghanayem, N.S.; Hoffman, G.M. Pro: NIRS is “standard of care” for postoperative management. Semin. Thorac. Cardiovasc. Surg. 2010, 13, 44–50. [Google Scholar] [CrossRef]
- Deschamps, A.; Lambert, J.; Couture, P.; Rochon, A.; Lebon, J.S.; Ayoub, C.; Cogan, J.; Denault, A. Reversal of decreases in cerebral saturation in high-risk cardiac surgery. J. Cardiothorac. Vasc. Anesth. 2013, 27, 1260–1266. [Google Scholar] [CrossRef]
- The Cochrane Collaboration. Assessing risk of bias in included studies. In Cochrane Handbook for Systematic Reviews of Interventions—Version 5.1.0.; Higgins, J.P.T., Ed.; John Wiley & Sons: Copenhagen, Denmark, 2011. [Google Scholar]
- Herrera-Gomez, F.; Chimeno, M.M.; Martin-Garcia, D.; Lizaraso-Soto, F.; Maurtua-Briseno-Meiggs, A.; Grande-Villoria, J.; Bustamante-Munguira, J.; Alamartine, E.; Vilardell, M.; Ochoa-Sangrador, C.; et al. Cholesterol-Lowering Treatment in Chronic Kidney Disease: Multistage Pairwise and Network Meta-Analyses. Sci. Rep. 2019, 9, 8951. [Google Scholar] [CrossRef]
- Herrera-Gomez, F.; Del Aguila, W.; Tejero-Pedregosa, A.; Adler, M.; Padilla-Berdugo, R.; Maurtua-Briseno-Meiggs, A.; Pascual, J.; Pascual, M.; San Segundo, D.; Heidt, S.; et al. The number of FoxP3 regulatory T cells in the circulation may be a predictive biomarker for kidney transplant recipients: A multistage systematic review. Int. Immunopharmacol. 2018, 65, 483–492. [Google Scholar] [CrossRef] [PubMed]
- Herrera-Gomez, F.; Monge-Donaire, D.; Ochoa-Sangrador, C.; Bustamante-Munguira, J.; Alamartine, E.; Alvarez, F.J. Correction of Hyponatremia May Be a Treatment Stratification Biomarker: A Two-Stage Systematic Review and Meta-Analysis. J. Clin. Med. 2018, 7, 262. [Google Scholar] [CrossRef] [PubMed]
- Brown, S.; Hutton, B.; Clifford, T.; Coyle, D.; Grima, D.; Wells, G.; Cameron, C. A Microsoft-Excel-based tool for running and critically appraising network meta-analyses—an overview and application of NetMetaXL. Syst. Rev. 2014, 3, 110. [Google Scholar] [CrossRef] [PubMed]
- Hutton, B.; Salanti, G.; Caldwell, D.M.; Chaimani, A.; Schmid, C.H.; Cameron, C.; Ioannidis, J.P.; Straus, S.; Thorlund, K.; Jansen, J.P.; et al. The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: Checklist and explanations. Ann. Intern. Med. 2015, 162, 777–784. [Google Scholar] [CrossRef] [PubMed]
- Shamseer, L.; Moher, D.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A.; Group, P.-P. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: Elaboration and explanation. BMJ 2015, 350, g7647. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Group, P. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- Ballard, C.; Jones, E.; Gauge, N.; Aarsland, D.; Nilsen, O.B.; Saxby, B.K.; Lowery, D.; Corbett, A.; Wesnes, K.; Katsaiti, E.; et al. Optimised anaesthesia to reduce post operative cognitive decline (POCD) in older patients undergoing elective surgery, a randomised controlled trial. PLoS ONE 2012, 7, e37410. [Google Scholar] [CrossRef]
- Casati, A.; Fanelli, G.; Pietropaoli, P.; Proietti, R.; Tufano, R.; Montanini, S. Monitoring cerebral oxygen saturation in elderly patients undergoing general abdominal surgery: A prospective cohort study. Eur. J. Anaesthesiol. 2007, 24, 59–65. [Google Scholar] [CrossRef]
- Colak, Z.; Borojevic, M.; Bogovic, A.; Ivancan, V.; Biocina, B.; Majeric-Kogler, V. Influence of intraoperative cerebral oximetry monitoring on neurocognitive function after coronary artery bypass surgery: A randomized, prospective study. Eur. J. Cardiothorac. Surg. 2015, 47, 447–454. [Google Scholar] [CrossRef]
- Cowie, D.A.; Nazareth, J.; Story, D.A. Cerebral oximetry to reduce perioperative morbidity. Anaesth. Intensive Care 2014, 42, 310–314. [Google Scholar] [CrossRef]
- Cox, R.M.; Jamgochian, G.C.; Nicholson, K.; Wong, J.C.; Namdari, S.; Abboud, J.A. The effectiveness of cerebral oxygenation monitoring during arthroscopic shoulder surgery in the beach chair position: A randomized blinded study. J. Shoulder Elbow. Surg. 2018, 27, 692–700. [Google Scholar] [CrossRef] [PubMed]
- Deschamps, A.; Hall, R.; Grocott, H.; Mazer, C.D.; Choi, P.T.; Turgeon, A.F.; de Medicis, E.; Bussieres, J.S.; Hudson, C.; Syed, S.; et al. Cerebral Oximetry Monitoring to Maintain Normal Cerebral Oxygen Saturation during High-risk Cardiac Surgery: A Randomized Controlled Feasibility Trial. Anesthesiology 2016, 124, 826–836. [Google Scholar] [CrossRef] [PubMed]
- Kara, I.; Erkin, A.; Sacli, H.; Demirtas, M.; Percin, B.; Diler, M.S.; Kirali, K. The Effects of Near-Infrared Spectroscopy on the Neurocognitive Functions in the Patients Undergoing Coronary Artery Bypass Grafting with Asymptomatic Carotid Artery Disease: A Randomized Prospective Study. Ann. Thorac. Cardiovasc. Surg. 2015, 21, 544–550. [Google Scholar] [CrossRef] [PubMed]
- Mohandas, B.S.; Jagadeesh, A.M.; Vikram, S.B. Impact of monitoring cerebral oxygen saturation on the outcome of patients undergoing open heart surgery. Ann. Card. Anaesth. 2013, 16, 102–106. [Google Scholar] [CrossRef]
- Murkin, J.M.; Adams, S.J.; Novick, R.J.; Quantz, M.; Bainbridge, D.; Iglesias, I.; Cleland, A.; Schaefer, B.; Irwin, B.; Fox, S. Monitoring brain oxygen saturation during coronary bypass surgery: A random- ized, prospective study. Anesth. Analg. 2007, 104, 51–58. [Google Scholar] [CrossRef]
- Rogers, C.A.; Stoica, S.; Ellis, L.; Stokes, E.A.; Wordsworth, S.; Dabner, L.; Clayton, G.; Downes, R.; Nicholson, E.; Bennett, S.; et al. Randomized trial of near-infrared spectroscopy for personalized optimization of cerebral tissue oxygenation during cardiac surgery. Br. J. Anaesth. 2017, 119, 384–393. [Google Scholar] [CrossRef] [PubMed]
- Slater, J.P.; Guarino, T.; Stack, J.; Vinod, K.; Bustami, R.T.; Brown, J.M., 3rd; Rodriguez, A.L.; Magovern, C.J.; Zaubler, T.; Freundlich, K.; et al. Cerebral oxygen desaturation predicts cognitive decline and longer hospital stay after cardiac surgery. Ann. Thorac. Surg. 2009, 87, 36–44. [Google Scholar] [CrossRef]
- Vretzakis, G.; Georgopoulou, S.; Stamoulis, K.; Tassoudis, V.; Mikroulis, D.; Giannoukas, A.; Tsilimingas, N.; Karanikolas, M. Monitoring of brain oxygen saturation (INVOS) in a protocol to direct blood transfusions during cardiac surgery: A prospective randomized clinical trial. J. Cardiothorac. Surg. 2013, 8, 145. [Google Scholar] [CrossRef]
- Harilall, Y.; Adam, J.K.; Biccard, B.M.; Reddi, A. The effect of optimising cerebral tissue oxygen saturation on markers of neurological injury during coronary artery bypass graft surgery. Heart, Lung Circ. 2014, 23, 68–74. [Google Scholar] [CrossRef]
- Trafidlo, T.; Gaszynski, T.; Gaszynski, W.; Nowakowska-Domagala, K. Intraoperative monitoring of cerebral NIRS oximetry leads to better postoperative cognitive performance: A pilot study. Int. J. Surg. 2015, 16, 23–30. [Google Scholar] [CrossRef]
- Yu, Y.; Zhang, K.; Zhang, L.; Zong, H.; Meng, L.; Han, R. Cerebral near-infrared spectroscopy (NIRS) for perioperative monitoring of brain oxygenation in children and adults. Cochrane Database Syst. Rev. 2018, 1, CD010947. [Google Scholar] [CrossRef] [PubMed]
- Sterne, J.A.; Sutton, A.J.; Ioannidis, J.P.; Terrin, N.; Jones, D.R.; Lau, J.; Carpenter, J.; Rucker, G.; Harbord, R.M.; Schmid, C.H.; et al. Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ 2011, 343, d4002. [Google Scholar] [CrossRef] [PubMed]
- Terrin, N.; Schmid, C.H.; Lau, J. In an empirical evaluation of the funnel plot, researchers could not visually identify publication bias. J. Clin. Epidemiol. 2005, 58, 894–901. [Google Scholar] [CrossRef] [PubMed]
- Ioannidis, J.P. Why most discovered true associations are inflated. Epidemiology 2008, 19, 640–648. [Google Scholar] [CrossRef]
- Higgins, J.P.; Thompson, S.G.; Deeks, J.J.; Altman, D.G. Measuring inconsistency in meta-analyses. BMJ 2003, 327, 557–560. [Google Scholar] [CrossRef]
- Rothwell, P.M. Subgroup analysis in randomised controlled trials: Importance, indications, and interpretation. Lancet 2005, 365, 176–186. [Google Scholar] [CrossRef]
- Deiner, S.; Silverstein, J.H. Postoperative delirium and cognitive dysfunction. Br. J. Anaesth. 2009, 103, i41–i46. [Google Scholar] [CrossRef]
- Choi, J.Y.; Kim, K.I.; Kang, M.G.; Lee, Y.K.; Koo, K.H.; Oh, J.H.; Park, Y.H.; Suh, J.; Kim, N.H.; Yoo, H.J.; et al. Impact of a delirium prevention project among older hospitalized patients who underwent orthopedic surgery: A retrospective cohort study. BMC Geriatr. 2019, 19, 289. [Google Scholar] [CrossRef]
- Kotfis, K.; Szylinska, A.; Listewnik, M.; Strzelbicka, M.; Brykczynski, M.; Rotter, I.; Zukowski, M. Early delirium after cardiac surgery: An analysis of incidence and risk factors in elderly (>/=65 years) and very elderly (>/=80 years) patients. Clin. Interv. Aging. 2018, 13, 1061–1070. [Google Scholar] [CrossRef]
- Lei, L.; Katznelson, R.; Fedorko, L.; Carroll, J.; Poonawala, H.; Machina, M.; Styra, R.; Rao, V.; Djaiani, G. Cerebral oximetry and postoperative delirium after cardiac surgery: A randomised, controlled trial. Anaesthesia 2017, 72, 1456–1466. [Google Scholar] [CrossRef]
- Radtke, F.M.; Franck, M.; Lendner, J.; Kruger, S.; Wernecke, K.D.; Spies, C.D. Monitoring depth of anaesthesia in a randomized trial decreases the rate of postoperative delirium but not postoperative cognitive dysfunction. Br. J. Anaesth. 2013, 110, i98–i105. [Google Scholar] [CrossRef] [PubMed]
- Murkin, J.M.; Arango, M. Near-infrared spectroscopy as an index of brain and tissue oxygenation. Br. J. Anaesth. 2009, 103, i3–i13. [Google Scholar] [CrossRef] [PubMed]
- Vancraeynest, D.; Pasquet, A.; Roelants, V.; Gerber, B.L.; Vanoverschelde, J.L. Imaging the vulnerable plaque. J. Am. Coll. Cardiol. 2011, 57, 1961–1979. [Google Scholar] [CrossRef] [PubMed]
- Ehlis, A.C.; Schneider, S.; Dresler, T.; Fallgatter, A.J. Application of functional near-infrared spectroscopy in psychiatry. Neuroimage 2014, 85, 478–488. [Google Scholar] [CrossRef] [PubMed]
- Mittnacht, A.J. Near infrared spectroscopy in children at high risk of low perfusion. Curr. Opin. Anaesthesiol. 2010, 23, 342–347. [Google Scholar] [CrossRef] [PubMed]
- Denault, A.; Deschamps, A.; Murkin, J.M. A proposed algorithm for the intraoperative use of cerebral near-infrared spectroscopy. Semin. Cardiothorac. Vasc. Anesth. 2007, 11, 274–281. [Google Scholar] [CrossRef]
- Taillefer, M.C.; Denault, A.Y. Cerebral near-infrared spectroscopy in adult heart surgery: Systematic review of its clinical efficacy. Can. J. Anaesth. 2005, 52, 79–87. [Google Scholar] [CrossRef]
- Pant, S.; Bokor, D.J.; Low, A.K. Cerebral oxygenation using near-infrared spectroscopy in the beach-chair position during shoulder arthroscopy under general anesthesia. Arthroscopy 2014, 30, 1520–1527. [Google Scholar] [CrossRef]
- Laflam, A.; Joshi, B.; Brady, K.; Yenokyan, G.; Brown, C.; Everett, A.; Selnes, O.; McFarland, E.; Hogue, C.W. Shoulder surgery in the beach chair position is associated with diminished cerebral autoregulation but no differences in postoperative cognition or brain injury biomarker levels compared with supine positioning: The anesthesia patient safety foundation beach chair study. Anesth. Analg. 2015, 120, 176–185. [Google Scholar] [CrossRef]
- Chan, M.J.; Chung, T.; Glassford, N.J.; Bellomo, R. Near-Infrared Spectroscopy in Adult Cardiac Surgery Patients: A Systematic Review and Meta-Analysis. J. Cardiothorac. Vasc. Anesth. 2017, 31, 1155–1165. [Google Scholar] [CrossRef]
- Montisci, A.; Travaglini, S.; Miceli, A. The lack of a magic bullet. J. Thorac. Cardiovasc. Surg. 2018. [Google Scholar] [CrossRef]
- Walker, I.A.; Reshamwalla, S.; Wilson, I.H. Surgical safety checklists: Do they improve outcomes? Br. J. Anaesth. 2012, 109, 47–54. [Google Scholar] [CrossRef]
- Hammon, J.W. Brain Protection during Cardiac Surgery: Circa 2012. JECT 2013, 45, 116–121. [Google Scholar]
- Yuan, S.M. S100 and S100beta: Biomarkers of cerebral damage in cardiac surgery with or without the use of cardiopulmonary bypass. Rev. Bras. Cir. Cardiovasc. 2014, 29, 630–641. [Google Scholar] [CrossRef][Green Version]
- Reinsfelt, B.; Ricksten, S.E.; Zetterberg, H.; Blennow, K.; Freden-Lindqvist, J.; Westerlind, A. Cerebrospinal fluid markers of brain injury, inflammation, and blood-brain barrier dysfunction in cardiac surgery. Ann. Thorac. Surg. 2012, 94, 549–555. [Google Scholar] [CrossRef]
- Silva, F.P.; Schmidt, A.P.; Valentin, L.S.; Pinto, K.O.; Zeferino, S.P.; Oses, J.P.; Wiener, C.D.; Otsuki, D.A.; Tort, A.B.; Portela, L.V.; et al. S100B protein and neuron-specific enolase as predictors of cognitive dysfunction after coronary artery bypass graft surgery: A prospective observational study. Eur. J. Anaesthesiol. 2016, 33, 681–689. [Google Scholar] [CrossRef]
- Lindblom, R.P.F.; Shen, Q.; Axen, S.; Landegren, U.; Kamali-Moghaddam, M.; Thelin, S. Protein Profiling in Serum and Cerebrospinal Fluid Following Complex Surgery on the Thoracic Aorta Identifies Biological Markers of Neurologic Injury. J. Cardiovasc. Transl. Res. 2018, 11, 503–516. [Google Scholar] [CrossRef]
- Olbrecht, V.A.; Skowno, J.; Marchesini, V.; Ding, L.; Jiang, Y.; Ward, C.G.; Yu, G.; Liu, H.; Schurink, B.; Vutskits, L.; et al. An International, Multicenter, Observational Study of Cerebral Oxygenation during Infant and Neonatal Anesthesia. Anesthesiology 2018, 128, 85–96. [Google Scholar] [CrossRef]
- Ortega-Loubon, C.; Fierro, I.; Tamayo, E. Should kidney oxygen saturation be monitored to prevent acute kidney injury after adult cardiac surgery? J. Thorac. Cardiovasc. Surg. 2019. [Google Scholar] [CrossRef]

| Explanations | |
|---|---|
| Review question | Which perioperative NIRS target values were most adequate for patients who underwent major surgical procedures? |
| Participants/population | Adult and pediatric individuals who underwent major cardiac or noncardiac surgery. |
| Intervention(s)/exposures(s) | Perioperative near-infrared spectroscopy target values according to current algorithms. |
| Comparators | No brain-oxygenation monitoring or brain-oxygenation monitoring based on non-NIRS technologies. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ortega-Loubon, C.; Herrera-Gómez, F.; Bernuy-Guevara, C.; Jorge-Monjas, P.; Ochoa-Sangrador, C.; Bustamante-Munguira, J.; Tamayo, E.; Álvarez, F.J. Near-Infrared Spectroscopy Monitoring in Cardiac and Noncardiac Surgery: Pairwise and Network Meta-Analyses. J. Clin. Med. 2019, 8, 2208. https://doi.org/10.3390/jcm8122208
Ortega-Loubon C, Herrera-Gómez F, Bernuy-Guevara C, Jorge-Monjas P, Ochoa-Sangrador C, Bustamante-Munguira J, Tamayo E, Álvarez FJ. Near-Infrared Spectroscopy Monitoring in Cardiac and Noncardiac Surgery: Pairwise and Network Meta-Analyses. Journal of Clinical Medicine. 2019; 8(12):2208. https://doi.org/10.3390/jcm8122208
Chicago/Turabian StyleOrtega-Loubon, Christian, Francisco Herrera-Gómez, Coralina Bernuy-Guevara, Pablo Jorge-Monjas, Carlos Ochoa-Sangrador, Juan Bustamante-Munguira, Eduardo Tamayo, and F. Javier Álvarez. 2019. "Near-Infrared Spectroscopy Monitoring in Cardiac and Noncardiac Surgery: Pairwise and Network Meta-Analyses" Journal of Clinical Medicine 8, no. 12: 2208. https://doi.org/10.3390/jcm8122208
APA StyleOrtega-Loubon, C., Herrera-Gómez, F., Bernuy-Guevara, C., Jorge-Monjas, P., Ochoa-Sangrador, C., Bustamante-Munguira, J., Tamayo, E., & Álvarez, F. J. (2019). Near-Infrared Spectroscopy Monitoring in Cardiac and Noncardiac Surgery: Pairwise and Network Meta-Analyses. Journal of Clinical Medicine, 8(12), 2208. https://doi.org/10.3390/jcm8122208








