Memory Complaint Is a Surrogate for Memory Decline in the Middle-Aged: A Register-Based Study
Abstract
1. Introduction
2. Materials and Methods
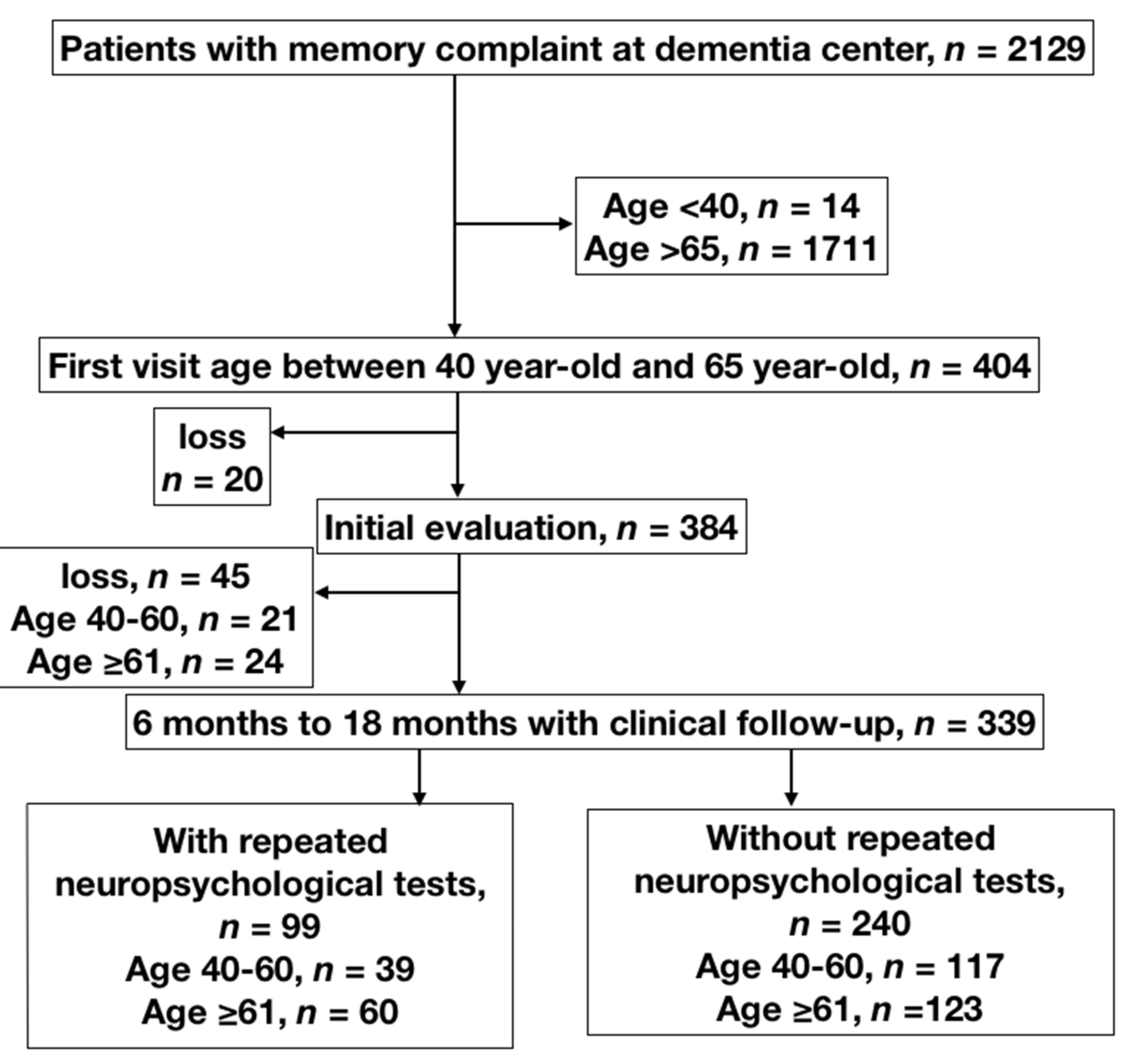
2.1. Study Design and Selection of Participants
2.2. Diagnosis Criteria
2.3. One-Year Cognitive Decline
2.4. Statistical Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Mitchell, A.J.; Beaumont, H.; Ferguson, D.; Yadegarfar, M.; Stubbs, B. Risk of dementia and mild cognitive impairment in older people with subjective memory complaints: Meta-analysis. Acta Psychiatr. Scand. 2014, 130, 439–451. [Google Scholar] [CrossRef] [PubMed]
- Jessen, F.; Amariglio, R.E.; van Boxtel, M.; Breteler, M.; Ceccaldi, M.; Chételat, G.; Dubois, B.; Dufouil, C.; Ellis, K.A.; van der Flier, W.M.; et al. A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease. Alzheimer’s Dement. 2014, 10, 844–852. [Google Scholar] [CrossRef] [PubMed]
- Geerlings, M.I.; Jonker, C.; Bouter, L.M.; Ader, H.J.; Schmand, B. Association between memory complaints and incident Alzheimer’s disease in elderly people with normal baseline cognition. Am. J. Psychiatry 1999, 156, 531–537. [Google Scholar] [CrossRef] [PubMed]
- Jonker, C.; Geerlings, M.I.; Schmand, B. Are memory complaints predictive for dementia? A review of clinical and population-based studies. Int. J. Geriatr. Psychiatry 2000, 15, 983–991. [Google Scholar] [CrossRef]
- Bassett, S.S.; Folstein, M.F. Memory complaint, memory performance, and psychiatric diagnosis: A community study. J. Geriatr. Psychiatry Neurol. 1993, 6, 105–111. [Google Scholar] [CrossRef]
- Andersson, C.; Lindau, M.; Almkvist, O.; Engfeldt, P.; Johansson, S.E.; Eriksdotter Jonhagen, M. Identifying patients at high and low risk of cognitive decline using Rey Auditory Verbal Learning Test among middle-aged memory clinic outpatients. Dement. Geriatr. Cogn. Disord. 2006, 21, 251–259. [Google Scholar] [CrossRef]
- Gallassi, R.; Oppi, F.; Poda, R.; Scortichini, S.; Stanzani Maserati, M.; Marano, G.; Sambati, L. Are subjective cognitive complaints a risk factor for dementia? Neurol. Sci. 2010, 31, 327–336. [Google Scholar] [CrossRef]
- Glodzik-Sobanska, L.; Reisberg, B.; De Santi, S.; Babb, J.S.; Pirraglia, E.; Rich, K.E.; Brys, M.; de Leon, M.J. Subjective memory complaints: Presence, severity and future outcome in normal older subjects. Dement. Geriatr. Cogn. Disord. 2007, 24, 177–184. [Google Scholar] [CrossRef]
- Lautenschlager, N.T.; Flicker, L.; Vasikaran, S.; Leedman, P.; Almeida, O.P. Subjective memory complaints with and without objective memory impairment: Relationship with risk factors for dementia. Am. J. Geriatr. Psychiatry 2005, 13, 731–734. [Google Scholar] [CrossRef] [PubMed]
- Molinuevo, J.L.; Rabin, L.A.; Amariglio, R.; Buckley, R.; Dubois, B.; Ellis, K.A.; Ewers, M.; Hampel, H.; Kloppel, S.; Rami, L.; et al. Implementation of subjective cognitive decline criteria in research studies. Alzheimers Dement. 2017, 13, 296–311. [Google Scholar] [CrossRef]
- Slavin, M.J.; Brodaty, H.; Kochan, N.A.; Crawford, J.D.; Trollor, J.N.; Draper, B.; Sachdev, P.S. Prevalence and Predictors of “Subjective Cognitive Complaints” in the Sydney Memory and Ageing Study. Am. J. Geriatr. Psychiatry 2010, 18, 701–710. [Google Scholar] [CrossRef] [PubMed]
- Mendonca, M.D.; Alves, L.; Bugalho, P. From Subjective Cognitive Complaints to Dementia: Who is at Risk? A Systematic Review. Am. J. Alzheimers Dis. Other Dement. 2016, 31, 105–114. [Google Scholar] [CrossRef]
- Donovan, N.J.; Amariglio, R.E.; Zoller, A.S.; Rudel, R.K.; Gomez-Isla, T.; Blacker, D.; Hyman, B.T.; Locascio, J.J.; Johnson, K.A.; Sperling, R.A.; et al. Subjective cognitive concerns and neuropsychiatric predictors of progression to the early clinical stages of Alzheimer disease. Am. J. Geriatr. Psychiatry 2014, 22, 1642–1651. [Google Scholar] [CrossRef] [PubMed]
- Kryscio, R.J.; Abner, E.L.; Cooper, G.E.; Fardo, D.W.; Jicha, G.A.; Nelson, P.T.; Smith, C.D.; Van Eldik, L.J.; Wan, L.; Schmitt, F.A. Self-reported memory complaints: Implications from a longitudinal cohort with autopsies. Neurology 2014, 83, 1359–1365. [Google Scholar] [CrossRef] [PubMed]
- Amariglio, R.E.; Townsend, M.K.; Grodstein, F.; Sperling, R.A.; Rentz, D.M. Specific subjective memory complaints in older persons may indicate poor cognitive function. J. Am. Geriatr. Soc. 2011, 59, 1612–1617. [Google Scholar] [CrossRef] [PubMed]
- Studart, A.N.; Nitrini, R. Subjective cognitive decline: The first clinical manifestation of Alzheimer’s disease? Dement. Neuropsychol. 2016, 10, 170–177. [Google Scholar] [CrossRef]
- Snitz, B.E.; Wang, T.; Cloonan, Y.K.; Jacobsen, E.; Chang, C.H.; Hughes, T.F.; Kamboh, M.I.; Ganguli, M. Risk of progression from subjective cognitive decline to mild cognitive impairment: The role of study setting. Alzheimers Dement. 2018, 14, 734–742. [Google Scholar] [CrossRef]
- van der Flier, W.M.; van Buchem, M.A.; Weverling-Rijnsburger, A.W.; Mutsaers, E.R.; Bollen, E.L.; Admiraal-Behloul, F.; Westendorp, R.G.; Middelkoop, H.A. Memory complaints in patients with normal cognition are associated with smaller hippocampal volumes. J. Neurol. 2004, 251, 671–675. [Google Scholar] [CrossRef]
- Saykin, A.J.; Wishart, H.A.; Rabin, L.A.; Santulli, R.B.; Flashman, L.A.; West, J.D.; McHugh, T.L.; Mamourian, A.C. Older adults with cognitive complaints show brain atrophy similar to that of amnestic MCI. Neurology 2006, 67, 834–842. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Ptacek, S.; Eriksdotter, M.; Jelic, V.; Porta-Etessam, J.; Kåreholt, I.; Manzano Palomo, S. Subjective cognitive impairment: Towards early identification of Alzheimer disease. Neurol. (Engl. Ed.) 2016, 31, 562–571. [Google Scholar] [CrossRef]
- Cedres, N.; Machado, A.; Molina, Y.; Diaz-Galvan, P.; Hernandez-Cabrera, J.A.; Barroso, J.; Westman, E.; Ferreira, D. Subjective Cognitive Decline Below and Above the Age of 60: A Multivariate Study on Neuroimaging, Cognitive, Clinical, and Demographic Measures. J. Alzheimers Dis. 2019. [Google Scholar] [CrossRef]
- Viviano, R.P.; Hayes, J.M.; Pruitt, P.J.; Fernandez, Z.J.; van Rooden, S.; van der Grond, J.; Rombouts, S.; Damoiseaux, J.S. Aberrant memory system connectivity and working memory performance in subjective cognitive decline. Neuroimage 2019, 185, 556–564. [Google Scholar] [CrossRef]
- Visser, P.J.; Verhey, F.; Knol, D.L.; Scheltens, P.; Wahlund, L.O.; Freund-Levi, Y.; Tsolaki, M.; Minthon, L.; Wallin, A.K.; Hampel, H.; et al. Prevalence and prognostic value of CSF markers of Alzheimer’s disease pathology in patients with subjective cognitive impairment or mild cognitive impairment in the DESCRIPA study: A prospective cohort study. Lancet Neurol. 2009, 8, 619–627. [Google Scholar] [CrossRef]
- Wolfsgruber, S.; Kleineidam, L.; Wagner, M.; Mosch, E.; Bickel, H.; Lupsilonhmann, D.; Ernst, A.; Wiese, B.; Steinmann, S.; Konig, H.H.; et al. Differential Risk of Incident Alzheimer’s Disease Dementia in Stable Versus Unstable Patterns of Subjective Cognitive Decline. J. Alzheimers. Dis. 2016, 54, 1135–1146. [Google Scholar] [CrossRef]
- van Harten, A.C.; Mielke, M.M.; Swenson-Dravis, D.M.; Hagen, C.E.; Edwards, K.K.; Roberts, R.O.; Geda, Y.E.; Knopman, D.S.; Petersen, R.C. Subjective cognitive decline and risk of MCI: The Mayo Clinic Study of Aging. Neurology 2018, 91, e300–e312. [Google Scholar] [CrossRef]
- Paradise, M.B.; Glozier, N.S.; Naismith, S.L.; Davenport, T.A.; Hickie, I.B. Subjective memory complaints, vascular risk factors and psychological distress in the middle-aged: A cross-sectional study. BMC Psychiatry 2011, 11, 108. [Google Scholar] [CrossRef]
- Rossor, M.N.; Fox, N.C.; Mummery, C.J.; Schott, J.M.; Warren, J.D. The diagnosis of young-onset dementia. Lancet Neurol. 2010, 9, 793–806. [Google Scholar] [CrossRef]
- Harvey, R.J.; Skelton-Robinson, M.; Rossor, M.N. The prevalence and causes of dementia in people under the age of 65 years. J. Neurol. Neurosurg. Psychiatry 2003, 74, 1206–1209. [Google Scholar] [CrossRef]
- Kelley, B.J.; Boeve, B.F.; Josephs, K.A. Young-onset dementia: Demographic and etiologic characteristics of 235 patients. Arch. Neurol. 2008, 65, 1502–1508. [Google Scholar] [CrossRef] [PubMed]
- McMurtray, A.; Clark, D.G.; Christine, D.; Mendez, M.F. Early-onset dementia: Frequency and causes compared to late-onset dementia. Dement. Geriatr. Cogn. Disord. 2006, 21, 59–64. [Google Scholar] [CrossRef]
- Stanley, K.; Whitfield, T.; Kuchenbaecker, K.; Sanders, O.; Stevens, T.; Walker, Z. Rate of Cognitive Decline in Alzheimer’s Disease Stratified by Age. J. Alzheimers Dis. 2019, 69, 1153–1160. [Google Scholar] [CrossRef]
- Freyne, A.; Kidd, N.; Coen, R.; Lawlor, B.A. Burden in carers of dementia patients: Higher levels in carers of younger sufferers. Int. J. Geriatr. Psychiatry 1999, 14, 784–788. [Google Scholar] [CrossRef]
- Arai, A.; Matsumoto, T.; Ikeda, M.; Arai, Y. Do family caregivers perceive more difficulty when they look after patients with early onset dementia compared to those with late onset dementia? Int. J. Geriatr. Psychiatry 2007, 22, 1255–1261. [Google Scholar] [CrossRef] [PubMed]
- McKhann, G.; Drachman, D.; Folstein, M.; Katzman, R.; Price, D.; Stadlan, E.M. Clinical diagnosis of Alzheimer’s disease: Report of the NINCDS-ADRDA Work Group under the auspices of Department of Health and Human Services Task Force on Alzheimer’s Disease. Neurology 1984, 34, 939–944. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.C.; Smith, G.E.; Waring, S.C.; Ivnik, R.J.; Tangalos, E.G.; Kokmen, E. Mild cognitive impairment: Clinical characterization and outcome. Arch. Neurol. 1999, 56, 303–308. [Google Scholar] [CrossRef] [PubMed]
- McKhann, G.M.; Knopman, D.S.; Chertkow, H.; Hyman, B.T.; Jack, C.R., Jr.; Kawas, C.H.; Klunk, W.E.; Koroshetz, W.J.; Manly, J.J.; Mayeux, R.; et al. The diagnosis of dementia due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011, 7, 263–269. [Google Scholar] [CrossRef] [PubMed]
- Emre, M.; Aarsland, D.; Brown, R.; Burn, D.J.; Duyckaerts, C.; Mizuno, Y.; Broe, G.A.; Cummings, J.; Dickson, D.W.; Gauthier, S.; et al. Clinical diagnostic criteria for dementia associated with Parkinson’s disease. Mov. Disord. 2007, 22, 1689–1707; quiz 1837. [Google Scholar] [CrossRef] [PubMed]
- Roman, G.C.; Tatemichi, T.K.; Erkinjuntti, T.; Cummings, J.L.; Masdeu, J.C.; Garcia, J.H.; Amaducci, L.; Orgogozo, J.M.; Brun, A.; Hofman, A.; et al. Vascular dementia: Diagnostic criteria for research studies. Report of the NINDS-AIREN International Workshop. Neurology 1993, 43, 250–260. [Google Scholar] [CrossRef] [PubMed]
- Neary, D.; Snowden, J.S.; Gustafson, L.; Passant, U.; Stuss, D.; Black, S.; Freedman, M.; Kertesz, A.; Robert, P.H.; Albert, M.; et al. Frontotemporal lobar degeneration: A consensus on clinical diagnostic criteria. Neurology 1998, 51, 1546–1554. [Google Scholar] [CrossRef]
- Tan, K.S.; Libon, D.J.; Rascovsky, K.; Grossman, M.; Xie, S.X. Differential longitudinal decline on the Mini-Mental State Examination in frontotemporal lobar degeneration and Alzheimer disease. Alzheimer Dis. Assoc. Disord. 2013, 27, 310–315. [Google Scholar] [CrossRef]
- Smits, L.L.; van Harten, A.C.; Pijnenburg, Y.A.; Koedam, E.L.; Bouwman, F.H.; Sistermans, N.; Reuling, I.E.; Prins, N.D.; Lemstra, A.W.; Scheltens, P.; et al. Trajectories of cognitive decline in different types of dementia. Psychol. Med. 2015, 45, 1051–1059. [Google Scholar] [CrossRef] [PubMed]
- Vieira, R.T.; Caixeta, L.; Machado, S.; Silva, A.C.; Nardi, A.E.; Arias-Carrion, O.; Carta, M.G. Epidemiology of early-onset dementia: A review of the literature. Clin. Pr. Epidemiol. Ment. Health 2013, 9, 88–95. [Google Scholar] [CrossRef]
- Draper, B.; Withall, A. Young onset dementia. Intern Med. J. 2016, 46, 779–786. [Google Scholar] [CrossRef] [PubMed]
- Kvello-Alme, M.; Brathen, G.; White, L.R.; Sando, S.B. The Prevalence and Subtypes of Young Onset Dementia in Central Norway: A Population-Based Study. J. Alzheimers Dis. 2019, 69, 479–487. [Google Scholar] [CrossRef] [PubMed]
- Ikejima, C.; Yasuno, F.; Mizukami, K.; Sasaki, M.; Tanimukai, S.; Asada, T. Prevalence and causes of early-onset dementia in Japan: A population-based study. Stroke 2009, 40, 2709–2714. [Google Scholar] [CrossRef] [PubMed]
- Shinagawa, S.; Ikeda, M.; Toyota, Y.; Matsumoto, T.; Matsumoto, N.; Mori, T.; Ishikawa, T.; Fukuhara, R.; Komori, K.; Hokoishi, K.; et al. Frequency and clinical characteristics of early-onset dementia in consecutive patients in a memory clinic. Dement. Geriatr. Cogn. Disord. 2007, 24, 42–47. [Google Scholar] [CrossRef] [PubMed]
- Fujihara, S.; Brucki, S.M.; Rocha, M.S.; Carvalho, A.A.; Piccolo, A.C. Prevalence of presenile dementia in a tertiary outpatient clinic. Arq. Neuropsiquiatr. 2004, 62, 592–595. [Google Scholar] [CrossRef]
- Yokota, O.; Sasaki, K.; Fujisawa, Y.; Takahashi, J.; Terada, S.; Ishihara, T.; Nakashima, H.; Kugo, A.; Ata, T.; Ishizu, H.; et al. Frequency of early and late-onset dementias in a Japanese memory disorders clinic. Eur. J. Neurol. 2005, 12, 782–790. [Google Scholar] [CrossRef]
- Garre-Olmo, J.; Genis Batlle, D.; del Mar Fernandez, M.; Marquez Daniel, F.; de Eugenio Huelamo, R.; Casadevall, T.; Turbau Recio, J.; Turon Estrada, A.; Lopez-Pousa, S.; Registry of Dementia of Girona Study Group. Incidence and subtypes of early-onset dementia in a geographically defined general population. Neurology 2010, 75, 1249–1255. [Google Scholar] [CrossRef]
- Mercy, L.; Hodges, J.R.; Dawson, K.; Barker, R.A.; Brayne, C. Incidence of early-onset dementias in Cambridgeshire, United Kingdom. Neurology 2008, 71, 1496–1499. [Google Scholar] [CrossRef]
- Papageorgiou, S.G.; Kontaxis, T.; Bonakis, A.; Kalfakis, N.; Vassilopoulos, D. Frequency and causes of early-onset dementia in a tertiary referral center in Athens. Alzheimer Dis. Assoc. Disord. 2009, 23, 347–351. [Google Scholar] [CrossRef] [PubMed]
- Sundar, U.; Sharma, A.; Yeolekar, M.E. Presenile dementia--etiology, clinical profile and treatment response at four month follow up. J. Assoc. Physicians India 2004, 52, 953–958. [Google Scholar] [PubMed]
- Panegyres, P.K.; Frencham, K. Course and causes of suspected dementia in young adults: A longitudinal study. Am. J. Alzheimers Dis. Other Dement. 2007, 22, 48–56. [Google Scholar] [CrossRef] [PubMed]
- Gerritsen, A.A.J.; Bakker, C.; Verhey, F.R.J.; Bor, H.; Pijnenburg, Y.A.L.; de Vugt, M.E.; Koopmans, R. The Progression of Dementia and Cognitive Decline in a Dutch 2-Year Cohort Study of People with Young-Onset Dementia. J. Alzheimers Dis. 2018, 63, 343–351. [Google Scholar] [CrossRef]
- Slot, R.E.R.; Sikkes, S.A.M.; Berkhof, J.; Brodaty, H.; Buckley, R.; Cavedo, E.; Dardiotis, E.; Guillo-Benarous, F.; Hampel, H.; Kochan, N.A.; et al. Subjective cognitive decline and rates of incident Alzheimer’s disease and non-Alzheimer’s disease dementia. Alzheimers Dement. 2019, 15, 465–476. [Google Scholar] [CrossRef]
- Bessi, V.; Mazzeo, S.; Padiglioni, S.; Piccini, C.; Nacmias, B.; Sorbi, S.; Bracco, L. From Subjective Cognitive Decline to Alzheimer’s Disease: The Predictive Role of Neuropsychological Assessment, Personality Traits, and Cognitive Reserve. A 7-Year Follow-Up Study. J. Alzheimers Dis. 2018, 63, 1523–1535. [Google Scholar] [CrossRef]
- Nasreddine, Z.S.; Phillips, N.A.; Bedirian, V.; Charbonneau, S.; Whitehead, V.; Collin, I.; Cummings, J.L.; Chertkow, H. The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment. J. Am. Geriatr. Soc. 2005, 53, 695–699. [Google Scholar] [CrossRef]
| Diagnosis | Total Enrollment, n (%) | 1-Year Follow-Up, n (%) | 1-Year Cognitive Decline, n (%) |
|---|---|---|---|
| Subjective cognitive decline | 131 (32%) | 95 (73%) | 7 (7.3%) |
| Objective cognitive impairment | |||
| Neurodegenerative disease | 141 (35%) | 125 (89%) | 46 (36.8%) |
| Mild cognitive decline | 46 (11%) | 40 (87%) | 12 (30%) |
| Alzheimer’s disease | 81 (20%) | 72 (89%) | 27 (37.5%) |
| Parkinson’s disease dementia | 3 (1%) | 2 (67%) | 1 (50%) |
| Frontotemporal lobe degeneration | 11 (3%) | 11 (100%) | 6 (54.5%) |
| Non-neurodegenerative disease | 132 (33%) | 119 (90%) | 9 (7.6%) |
| Structure lesion a | 24 (6%) | 23 (96%) | 5 (21.7%) |
| Vascular dementia | 24 (6%) | 21 (86%) | 0 (0%) |
| Mood disorder b | 84 (21%) | 75 (89%) | 4 (5.3%) |
| Total | 404 (100%) | 339 (84%) | 62 (18.3%) |
| Characteristic | Total | Subjective Cognitive Decline (SCD) | Neurodegenerative Disease (ND) | Non-Neurodegenerative Disease (NND) | pSCD–ND | pSCD–NND | pND–NND | pall |
|---|---|---|---|---|---|---|---|---|
| Number | 404 | 131 | 141 | 132 | ||||
| Age | 58.8 ± 6.0 | 58.4 ± 6.4 | 60.3 ± 4.7 | 57.6 ± 6.4 | 2 × 10−2 | 0.58 | 1 × 10−3 | 6× 10−4 |
| Male, n (%) | 158 (39.1%) | 51 (38.9%) | 63 (44.7%) | 44 (33.3%) | 0.34 | 0.35 | 0.06 | 0.06 |
| Hypertension | 115 (28.5%) | 30 (22.9%) | 40 (28.4%) | 45 (34.1%) | 0.3 | 4.4 × 10−2 | 0.31 | 3× 10−7 |
| DM | 74 (18.4%) | 16 (12.3%) | 32 (22.7%) | 26 (19.7%) | 3.0 × 10−3 | 0.1 | 0.55 | 3× 10−5 |
| Education (year) | 9.7 ± 4.4 | 10.8 ± 4.2 | 9.0 ± 4.2 | 9.3 ± 4.7 | 2.0 × 10−3 | 1.4 × 10−2 | 0.85 | 2× 10−3 |
| 1-year decline | 62 (18.3%) | 7 (7.3%) | 46 (36.8%) | 9 (7.6%) | 1.3 × 10−8 | 0.617 | 1.1 × 10−7 | 1× 10−10 |
| Neuropsychological test | ||||||||
| Number | 384 | 120 | 135 | 129 | ||||
| MMSE | 24.4 ± 6.1 | 27.9 ± 2.9 | 21.3 ± 6.3 | 24.4 ± 6.4 | 5.1 × 10−9 | 3.0 × 10−6 | 1.8 × 10−5 | 3× 10−18 |
| Orientation | 8.4 ± 2.4 | 9.7 ± 0.9 | 7.2 ± 2.8 | 8.4 ± 2.4 | 5.1 × 10−9 | 1.8 × 10−5 | 7.1 × 10−5 | 3× 10−16 |
| Registration | 2.9 ± 0.5 | 3.0 ± 0.2 | 2.8 ± 0.6 | 2.9 ± 0.5 | 1.5 × 10−2 | 0.13 | 0.66 | 2× 10−2 |
| Attention calculation | 3.7 ± 1.7 | 4.4 ± 1.0 | 3.0 ± 1.8 | 3.7 ± 1.7 | 5.1 × 10−9 | 3.4 × 10−4 | 2.3 × 10−3 | 2× 10−11 |
| Recall | 1.6 ± 1.2 | 2.2 ± 0.9 | 0.9 ± 1.0 | 1.8 ± 1.2 | 5.1 × 10−9 | 1.3 × 10−2 | 5.1 × 10−9 | 3× 10−21 |
| Language | 7.9 ± 1.7 | 8.6 ± 1.0 | 7.4 ± 2.0 | 7.8 ± 1.7 | 2.1 × 10−8 | 6.6 × 10−4 | 0.07 | 3× 10−8 |
| 6-item learning | 25.0 ± 6.0 | 28.4 ± 2.1 | 22.3 ± 7.0 | 25.0 ± 6.9 | 7.0 × 10−9 | 1.4 × 10−3 | 9.5 × 10−3 | 5× 10−9 |
| 6-item recall | 4.7 ± 1.8 | 5.8 ± 0.5 | 3.7 ± 1.9 | 4.8 ± 1.9 | 5.1 × 10−9 | 9.1 × 10−4 | 4.1 × 10−5 | 4× 10−13 |
| Global CDR | 0.4 ± 0.5 | 0.2 ± 0.3 | 0.6 ± 0.4 | 0.4 ± 0.5 | 5.1 × 10−9 | 1.7 × 10−5 | 2.6 × 10−4 | 2× 10−15 |
| Sum of box | 0.5 ± 1.1 | 3.0 ±3.0 | 3.0 ± 3.0 | 2.0 ± 3.4 | 5.1 × 10−9 | 3.0 × 10−5 | 1.5 × 10−2 | 9× 10−12 |
| IQCODE | n = 216 | n = 66 | n = 89 | n = 61 | ||||
| 3.5 ± 0.6 | 3.2 ± 0.4 | 3.8 ± 0.5 | 3.6 ± 0.6 | 5.1 × 10−9 | 3.0 × 10−5 | 1.5 × 10−2 | 4× 10−10 | |
| CASI | n = 186 | n = 71 | n = 58 | n = 57 | ||||
| 86.5 ± 12.3 | 96.1 ± 8.1 | 78.4 ± 14.5 | 88.4 ± 9.3 | 5.3 × 10−9 | 3.8 × 10−5 | 0.14 | 4× 10−10 | |
| Neuropsychological test | MMSE | Orientation | Registration | Attention Calculation | Recall | |||||
| Variable | OR, 95% CIs | p | OR, 95% CIs | p | OR, 95% CIs | p | OR, 95% CIs | p | OR, 95% CIs | p |
| Neuropsychological test | 1.126, 1.076–1.178 | 2.52 × 10−7 | 1.366, 1.225–1.522 | 1.72 × 10−8 | 1.04, 0.605–1.789 | 0.885 | 1.35, 1.144–1.595 | 4.0 × 10−4 | 2.208, 1.658–2.941 | 5.93 × 10−8 |
| Age | 1.012, 0.958–1.069 | 0.669 | 1.019, 0.964–1.078 | 0.498 | 1.011, 0.959–1.065 | 0.696 | 1.014, 0.961–1.070 | 0.611 | 1.009, 0.953–1.067 | 0.765 |
| DM | 0.920, 0.410–2.067 | 0.84 | 1.009, 0.443–2.301 | 0.982 | 0.737, 0.348–1.563 | 0.427 | 0.883, 0.406–1.920 | 0.754 | 0.669, 0.304–1.474 | 0.319 |
| Hypertension | 1.322, 0.642–2.723 | 0.449 | 1.278, 0.617–2.649 | 0.509 | 1.199, 0.606–2.370 | 0.602 | 1.203, 0.597–2.423 | 0.605 | 1.310, 0.642–2.670 | 0.458 |
| Education | 1.037, 0.960–1.120 | 0.358 | 1.017, 0.942–1.098 | 0.658 | 0.971, 0.906–1.042 | 0.415 | 1.013, 0.941–1.090 | 0.736 | 1.029, 0.950–1.113 | 0.487 |
| Sex | 0.709, 0.382–1.315 | 0.275 | 0.735, 0.393–1.375 | 0.336 | 0.756, 0.421–1.358 | 0.349 | 0.769, 0.423–1.396 | 0.387 | 0.649, 0.348–1.211 | 0.174 |
| Neuropsychological test | Language | Global CDR | Sum of box | IQCODE a | CASI b | |||||
| Variable | OR, 95% CIs | p | OR, 95% CIs | p | OR, 95% CIs | p | OR, 95% CIs | p | OR, 95% CIs | p |
| Neuropsychological test | 1.312, 1.126–1.531 | 5.23 × 10−4 | 3.296, 1.828–5.911 | 6.30 × 10−5 | 2.775, 1.836–4.194 | 1.0 × 10−6 | 4.254, 2.060–8.783 | 9.1 × 10−5 | 0.918, 0.880–0.958 | 8.6 × 10−5 |
| Age | 1.009, 0.957–1.063 | 0.747 | 1.00, 0.947–1.057 | 0.989 | 1.009, 0.955–1.067 | 0.74 | 1.068, 0.969–1.179 | 0.186 | 0.987, 0.909–1.071 | 0.751 |
| DM | 0.841, 0.386–1.834 | 0.664 | 0.796, 0.359–1.762 | 0.573 | 0.826, 0.366–1.863 | 0.644 | 1.360, 0.428–4.322 | 0.603 | 0.686, 0.167–2.813 | 0.601 |
| Hypertension | 1.275, 0.632–2.574 | 0.497 | 1.482, 0.717–3.063 | 0.288 | 1.494, 0.714–3.126 | 0.286 | 1.870, 0.682–5.129 | 0.224 | 0.544, 0.148–2.003 | 0.36 |
| Education | 1.016, 0.943–1.094 | 0.681 | 1.007, 0.934–1.086 | 0.847 | 1.025, 0.949–1.108 | 0.525 | 0.969, 0.870–1.079 | 0.57 | 1.003, 0.868–1.159 | 0.971 |
| Sex | 0.745, 0.410–1.353 | 0.333 | 0.748, 0.405–1.381 | 0.353 | 0.663, 0.352–1.247 | 0.202 | 0.486, 0.202–1.170 | 0.107 | 0.668, 0.213–2.091 | 0.488 |
| Country | Year | Patient Number | Findings | Reference | ||
|---|---|---|---|---|---|---|
| AD prevalent | AD | VaD | FTLD | |||
| UK | 2003 | 185 | 34% | 18% | 12% | [28] |
| Japan | 2005 | 34 | 38% | 24% | 15% | [48] |
| Spain | 2010 | 144 | 42% | 14% | 10% | [49] |
| Norway | 2019 | 390 | 33% | 5% | 5% | [44] |
| Japan | 2007 | 185 | 39% | 13% | 21% | [46] |
| UK | 2008 | 54 | 35% | 11% | 27% | [50] |
| Greece | 2009 | 114 | 27% | 6% | 25% | [51] |
| VaD prevalent | AD | VaD | FTLD | |||
| Brazil | 2003 | 141 | 21% | 37% | 5% | [47] |
| India | 2004 | 76 | 13% | 44% | - | [52] |
| USA | 2006 | 278 | 17% | 29% | 3% | [30] |
| Japan | 2006 | 671 | 26% | 43% | 3% | [45] |
| FTLD prevalent | AD | VaD | FTLD | |||
| Australia | 2007 | 112 | 12% | 3% | 19% | [53] |
| USA | 2006 | 235 | 1% | 6% | 13% | [29] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wu, Y.-Y.; Hsu, W.-C.; Huang, Y.-H.; Ho, W.-M.; Chen, Y.-C. Memory Complaint Is a Surrogate for Memory Decline in the Middle-Aged: A Register-Based Study. J. Clin. Med. 2019, 8, 1900. https://doi.org/10.3390/jcm8111900
Wu Y-Y, Hsu W-C, Huang Y-H, Ho W-M, Chen Y-C. Memory Complaint Is a Surrogate for Memory Decline in the Middle-Aged: A Register-Based Study. Journal of Clinical Medicine. 2019; 8(11):1900. https://doi.org/10.3390/jcm8111900
Chicago/Turabian StyleWu, Yah-Yuan, Wen-Chuin Hsu, Yu-Hua Huang, Wei-Min Ho, and Yi-Chun Chen. 2019. "Memory Complaint Is a Surrogate for Memory Decline in the Middle-Aged: A Register-Based Study" Journal of Clinical Medicine 8, no. 11: 1900. https://doi.org/10.3390/jcm8111900
APA StyleWu, Y.-Y., Hsu, W.-C., Huang, Y.-H., Ho, W.-M., & Chen, Y.-C. (2019). Memory Complaint Is a Surrogate for Memory Decline in the Middle-Aged: A Register-Based Study. Journal of Clinical Medicine, 8(11), 1900. https://doi.org/10.3390/jcm8111900





