Hyponatremia: Special Considerations in Older Patients
Abstract
:1. Introduction
2. Epidemiology
3. Does Hyponatremia Cause Cognitive Impairment?
4. Hyponatremia and Bone Demineralization
4.1. Non-Randomised Rodent Studies
4.2. Case-Control Studies
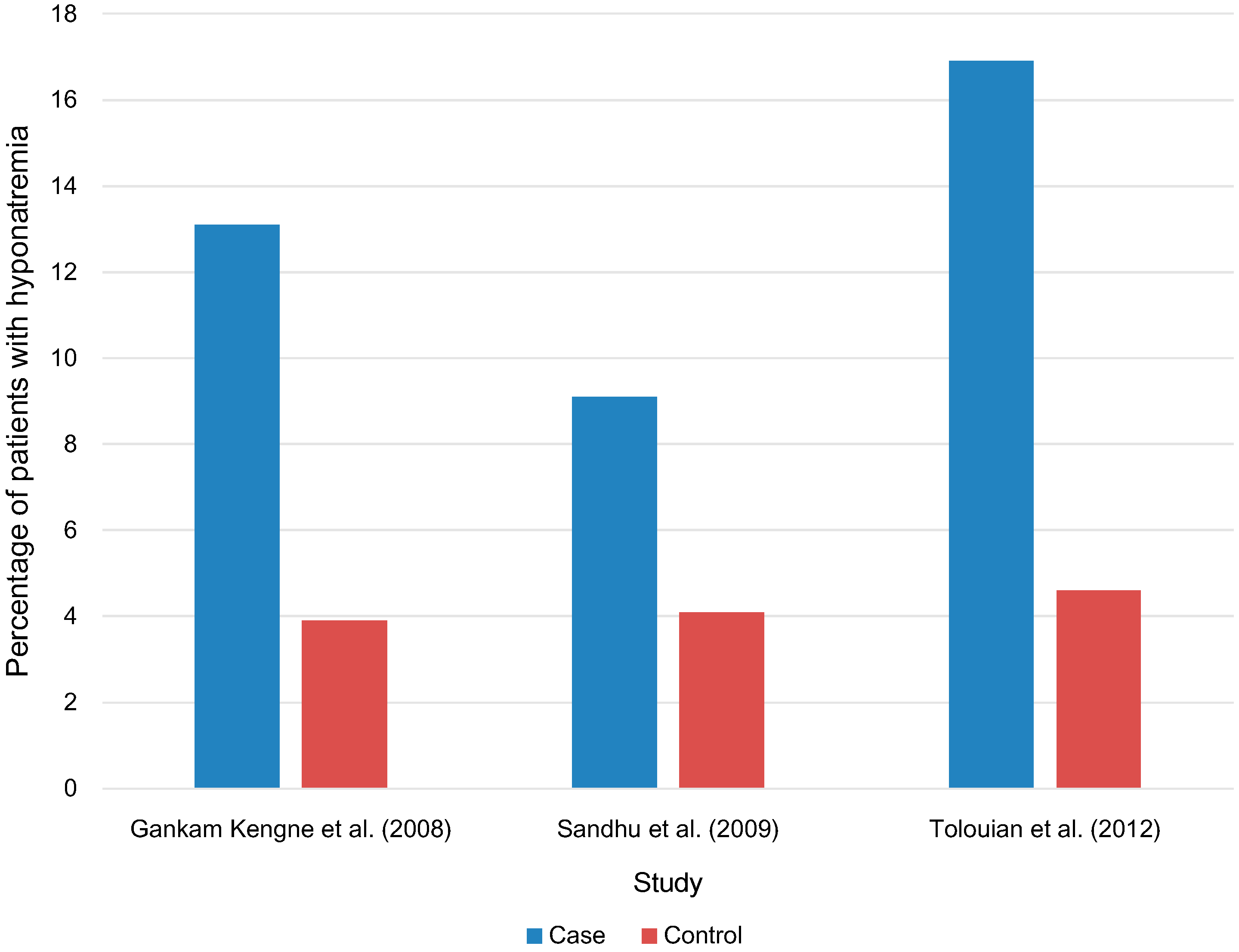
4.3. Cross-Sectional Cohort Studies
| Study | Adjustments |
|---|---|
| Verbalis et al. (2010) [8] | age (years), sex, body mass index, history of diuretic use, physical activity, serum 25-hydroxy-vitamin D levels |
| Kinsella et al. (2010) [23] | age (years), T-score, chronic kidney disease stage, osteoporotic risk factors (amenorrhoea, low dietary calcium (Ca2+) intake, high alcohol intake, maintenance steroids, ever having smoked, family history of osteoporosis and history of liver disease) and osteoporosis treatment (use of Ca2+, vitamin D, antiresorptive therapy and hormonal replacement therapy) |
| Hoorn et al. (2011) [24] | age (years), sex, body mass index, disability index, use of diuretics or psycholeptics, recent falls and prevalent diabetes mellitus |
4.4. Falls
5. Diagnosing the Causes of Hyponatremia
| Hypovolemic hyponatremia |
|---|
| Inadequate fluid intake or replacement |
| Diuretic therapy |
| Diarrhea and vomiting |
| Pancreatitis/third space loss of fluids |
| Renal salt wasting |
| Burns and skin losses |
| Mineralocorticoid deficiency |
| Euvolemic hyponatremia |
| Syndrome of inappropriate antidiuretic hormone |
| Medications |
| Hypothyroidism |
| Fluid loss with inappropriate fluid (salt) replacement |
| Glucocorticoid deficiency |
| Hypervolemic hyponatremia |
| Cardiac failure |
| Cirrhosis |
| Chronic kidney disease |
| Acute kidney injury |
| Nephrotic syndrome |
6. Treatment of Hyponatremia in Older People
| Treatment | Indication | Special Considerations in Older People |
|---|---|---|
| Optimize prescribing | Drug-induced hyponatremia | Medications more likely to be needed due to co-morbidities. |
| Isotonic saline | Hypovolemic hyponatremia | Hypovolemia common due to immobility, confusion and malnutrition. Assessment of volemic state is notoriously difficult so may worsen hyponatremia if underlying causes are misdiagnosed. |
| Hypertonic saline | Severe hyponatremia from any cause | Needs expert monitoring. High potential for over-correction. |
| Fluid restriction | SIADH | Poor tolerability and high failure rate. Will worsen hyponatremia where dehydration is misdiagnosed as SIADH. |
| Demeclocycline | SIADH | Unpredictability of effect requires special caution due to lower resilience. |
| Diuretics | Hypervolemic hyponatremia | Can worsen hyponatremia by increasing urinary sodium excretion. |
| Salt tablets | Hypovolemic hyponatremia | Rarely indicated as dietary sodium intake is usually sufficient and total body sodium is not normally low in most cases of hyponatremia. |
| Lithium | SIADH | Inconsistent results, with high risk of adverse drug effects and toxicity. |
| Urea | SIADH | Only available in some countries. Unpalatable. Higher risk of uremia. |
| Vaptans | SIADH or hypervolemia | Risk of dehydration and over-correction. Expensive. Only licensed for SIADH in Europe. |
6.1. Optimizing Prescribing
6.2. Fluid Therapy or Restriction
6.3. Vaptans
6.4. Are Vaptans Safe in Old Age?
7. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Sherlock, M.; Thompson, C.J. The syndrome of inappropriate antidiuretic hormone: Current and future management options. Eur. J. Endocrin. 2010, 162, 13–18. [Google Scholar] [CrossRef]
- Tzoulis, P.; Bagkeris, E.; Bouloux, P.M. A case-control study of hyponatraemia as an independent risk factor for inpatient mortality. Clin. Endocrinol. 2014, 3, 401–407. [Google Scholar] [CrossRef]
- Nelson, M.; Palmer, J.L.; Fu, J.; Williams, J.L.; Yadav, R.; Guo, Y. Hyponatraemia in cancer patients on an inpatient rehabilitation unit. Eur. J. Cancer Care 2014, 23, 363–369. [Google Scholar] [CrossRef]
- Chua, M.; Hoyle, G.E.; Soiza, R.L. Prognostic implications of hyponatremia in elderly hospitalized patients. Arch. Gerontol. Geriatr. 2007, 45, 253–258. [Google Scholar]
- Soiza, R.L.; Hoyle, G.E.; Chua, M.P.W. Electrolyte and salt disturbances in older people: Causes, management and implications. Rev. Clin. Gerontol. 2008, 18, 143–158. [Google Scholar] [CrossRef]
- Renneboog, B.; Musch, W.; Vandemergel, X.; Manto, M.U.; Decaux, G. Mild Chronic Hyponatremia Is Associated with Falls, Unsteadiness, and Attention Deficits. Am. J. Med. 2006, 119. [Google Scholar] [CrossRef]
- Gankam Kengne, F.; Andres, C.; Sattar, L.; Melot, C.; Decaux, G. Mild hyponatremia and risk of fracture in the ambulatory elderly. QJM 2008, 101, 583–588. [Google Scholar]
- Verbalis, J.G.; Barsony, J.; Sugimura, Y.; Tian, Y.; Adams, D.J.; Carter, E.A.; Resnick, H.E. Hyponatraemia-induced osteoporosis. J. Bone Miner. Res. 2010, 25, 554–563. [Google Scholar]
- Mannesse, C.K.; Vondeling, A.M.; van Marum, R.J.; van Solinge, W.W.; Egberts, T.C.; Jansen, P.A. Prevalence of hyponatremia on geriatric wards compared to other settings over four decades: A systematic review. Ageing Res. Rev. 2013, 12, 165–173. [Google Scholar] [CrossRef]
- Hoyle, G.E.; Chua, M.; Soiza, R.L. Prevalence of hyponatremia in elderly patients. J. Am. Geriatr. Soc. 2006, 54, 1473. [Google Scholar]
- Spasovski, G.; Vanholder, R.; Allolio, B.; Annane, D.; Ball, S.; Bichet, D.; Decaux, G.; Fenske, W.; Hoorn, E.J.; Ichai, C.; et al. Clinical practice guideline on diagnosis and treatment of hyponatraemia. Eur. J. Endocrinol. 2014, 170, G1–G47. [Google Scholar]
- Ayus, J.C.; Arieff, A.I. Pathogenesis and prevention of hyponatremic encephalopathy. Endocrinol. Metab. Clin. N. Am. 1993, 22, 425–446. [Google Scholar]
- Vaghasiya, R.P.; DeVita, M.V.; Panagopoulos, G.; Michelis, M.F. Hyponatremic patients demonstrate improved cognition after an increase in serum sodium. In Proceedings of the Poster Presented at NKF Annual Meeting, Orlando, FL, USA, 6–10 April, 2010.
- Folstein, M.F.; Folstein, S.E.; McHugh, P.R. “Mini-mental state”. A practical guide for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 1975, 12, 189–198. [Google Scholar] [CrossRef]
- MacDonald, A.A.; Joyson, A.; Lee, R.; Seymour, D.G.; Soiza, R.L. The effect of hearing augmentation on cognitive assessment scales at admission to hospital. Am. J. Geriatr. Psych. 2012, 20, 355–361. [Google Scholar] [CrossRef]
- Gunathilake, R.; Oldmeadow, C.; McEvoy, M.; Kelly, B.; Inder, K.; Schofield, P.; Attia, J. Mild hyponatremia is associated with impaired cognition and falls in community-dwelling older persons. J. Am. Geriatr. Soc. 2013, 61, 1838–1839. [Google Scholar]
- Ayus, J.C.; Achinger, S.G.; Arieff, A. Brain cell volume regulation in hyponatremia: Role of sex, age, vasopressin, and hypoxia. Am. J. Physiol. Ren. Physiol. 2008, 295. [Google Scholar] [CrossRef]
- Córdoba, J.; García-Martinez, R.; Simón-Talero, M. Hyponatremic and hepatic encephalopathies: Similarities, differences and coexistence. Metab. Brain Dis. 2010, 25, 73–80. [Google Scholar]
- Das, A.; Dhiman, R.K.; Saraswat, V.A.; Verma, M.; Naik, S.R. Prevalence and natural history of subclinical hepatic encephalopathy in cirrhosis. J. Gastroenterol. Hepatol. 2001, 16, 531–535. [Google Scholar]
- Barsony, J.; Manigrasso, M.B.; Xu, Q.; Tam, H.; Verbalis, J.G. Chronic hyponatraemia exacerbates multiple manifestations of senescence in male rats. Age 2013, 35, 271–288. [Google Scholar] [CrossRef]
- Sandhu, H.S.; Gilles, E.; DeVita, M.V.; Panagopoulos, G.; Michelis, M.F. Hyponatraemia associated with large-bone fracture in elderly patients. Int. Urol. Nephrol. 2009, 41, 733–737. [Google Scholar]
- Tolouian, R.; Alhamad, T.; Farazmand, M.; Mulla, Z.D. The correlation of hip fracture and hyponatraemia in the elderly. J. Nephrol. 2012, 25, 789–793. [Google Scholar] [CrossRef]
- Kinsella, S.; Moran, S.; Sullivan, M.O.; Molloy, M.G.M.; Eustace, J.A. Hyponatraemia independent of osteoporosis is associated with fracture occurrence. Clin. J. Am. Soc. Nephrol. 2010, 5, 275–280. [Google Scholar] [CrossRef]
- Hoorn, E.J.; Rivadeneira, F.; van Meurs, J.B.J.; Ziere, G.; Stricker, B.H.; Hofman, A.; Pols, H.A.P.; Zietse, R.; Uitterlinden, A.G.; Zillikens, M.C.; et al. Mild hyponatraemia as a risk factor for fractures: The Rotterdam study. J. Bone Miner. Res. 2011, 26, 1822–1828. [Google Scholar]
- Soiza, R.L.; Talbot, H.S.C. Management of hyponatraemia in older people: Old threats and new opportunities. Ther. Adv. Drug Saf. 2011, 2, 9–17. [Google Scholar] [CrossRef]
- Verbalis, J.G.; Goldsmith, S.R.; Greenberg, A. Diagnosis, evaluation and treatment of hyponatraemia: Expert panel recommendations. Am. J. Med. 2013, 126, 1–42. [Google Scholar]
- Hoyle, G.E.; Chua, M.; Soiza, R.L. Volaemic assessment of the elderly hyponatraemic patient: Reliability of clinical assessment and validation of bioelectrical impedance analysis. QJM 2011, 104, 35–39. [Google Scholar]
- Cumming, K.; Hoyle, G.E.; Hutchison, J.D.; Soiza, R.L. Bioelectrical impedance analysis is more accurate than clinical examination in determining the volaemic status of elderly patients with fragility fracture and hyponatraemia. J. Nutr. Health Aging 2014. [Google Scholar] [CrossRef]
- Hannon, M.J.; Thompson, C.J. The syndrome of inappropriate antidiuretic hormone: Prevalence, causes and consequences. Eur. J. Endocrinol. 2010, 166. [Google Scholar] [CrossRef]
- Soiza, R.L.; Hoyle, G.E. Syndrome of appropriate antidiuretic hormone: Difficulties with diagnosing syndrome of inappropriate antidiuretic hormone in older people. Int. Med. J. 2011, 41. [Google Scholar] [CrossRef]
- Clayton, J.A.; Le Jeune, I.R.; Hall, I.P. Severe hyponatraemia in medical in-patients: Aetiology, assessment and outcome. QJM 2006, 99, 505–511. [Google Scholar]
- Shapiro, D.S.; Sonnenblick, M.; Galperin, I.; Melkonyan, L.; Munter, G. Severe hyponatraemia in elderly hospitalized patients: Prevalence, aetiology and outcome. Int. Med. J. 2010, 40, 574–580. [Google Scholar] [CrossRef]
- Cumming, K.; Hoyle, G.E.; Hutchison, J.D.; Soiza, R.L. Prevalence, incidence and etiology of hyponatremia in elderly patients with fragility fractures. PLoS One 2014, 9, e88272. [Google Scholar]
- Rosholm, J.; Nybo, H.; Andersen Ranberg, K.; Himmelstrup, B.; Skjelbo, E.; Christensen, K.; Gram, L.F. Hyponatraemia in Very Old Nonhospitalised People: Association with Drug Use. Drugs Aging 2002, 19, 685–693. [Google Scholar]
- Mann, S.J. The silent epidemic of thiazide-induced hyponatremia. J. Clin. Hypertens. 2008, 10, 477–484. [Google Scholar] [CrossRef]
- Movig, K.L.L.; Leufkens, H.G.M.; Lenderink, A.W.; van Den Akker, V.G.A.; Hodiamont, P.P.G.; Goldschmidt, H.M.J.; Egberts, A.C. Association between antidepressant drug use and hyponatraemia: A case-control study. Br. J. Clin. Pharmacol. 2002, 53, 363–369. [Google Scholar]
- Verbalis, J.G.; Grossman, A.; Hoybye, C.; Runkle, I. Review and analysis of differing regulatory indications and expert panel guidelines for the treatment of hyponatraemia. Curr. Med. Res. Opin. 2014, 30, 1201–1207. [Google Scholar] [CrossRef]
- Caslake, R.; Soiza, R.L.; Mangoni, A.A. Practical advice for prescribing in old age. Medicine 2013, 41, 9–12. [Google Scholar]
- Rudge, J.E.; Kim, D. New-onset hyponatraemia after surgery for traumatic hip fracture. Age Ageing 2014. [Google Scholar] [CrossRef]
- Hamzat, H.; Sun, H.; Ford, J.C.; MacLeod, J.; Soiza, R.L.; Mangoni, A.A. Inappropriate prescribing of proton pump inhibitors in older patients: Effects of an educational strategy. Drugs Aging 2012, 29, 681–690. [Google Scholar]
- Smith, D.; Moore, K.; Tormey, W.; Baylis, P.H.; Thompson, C.J. Downward resetting of the osmotic threshold for thirst in patients with SIADH. Am. J. Physiol. Endorin. Metabol. 2004, 287. [Google Scholar] [CrossRef]
- Nzerue, C.M.; Baffoe-Bonnie, H.; You, W.; Falana, B.; Dai, S. Predictors of outcome in hospitalized patients with severe hyponatraemia. J. Natl. Med. Assoc. 2003, 95, 335–343. [Google Scholar]
- Verbalis, J.G.; Goldsmith, S.R.; Greenberg, A.; Schrier, R.W.; Sterns, R.H. Hyponatremia Treatment Guidelines 2007: Expert Panel Recommendations. Am. J. Med. 2007, 120, 1–21. [Google Scholar]
- Moritz, L.; Ayus, J.C. 100 cc 3% sodium chloride bolus: A novel treatment for hyponatraemic encephalopathy. Metabol. Brain. Dis. 2010, 25, 91–96. [Google Scholar] [CrossRef]
- Schrier, R.W.; Gross, P.; Gheorghiade, M.; Berl, T.; Verbalis, J.G.; Czerwiec, F.S.; Orlandi, C.; SALT Investigators. Tolvaptan, a selective oral vasopressin V2-receptor antagonist, for hyponatremia. N. Engl. J. Med. 2006, 355, 2099–2112. [Google Scholar] [CrossRef]
- Gheorghiade, M.; Gottlieb, S.S.; Udelson, J.E.; Konstam, M.A.; Czerwiec, F.; Ouyang, J.; Orlandi, C. Tolvaptan Investigators. Vasopressin V2 receptor blockade with tolvaptan versus fluid restriction in the treatment of hyponatremia. Am. J. Med. 2006, 97, 1064–1067. [Google Scholar]
- Berl, T.; Quittnat-Pelletier, F.; Verbalis, J.G.; Schrier, R.W.; Bichet, D.G.; Ouyang, J.; Czerwiec, F.S.; SALT Investigators. Oral tolvaptan is safe and effective in chronic hyponatremia. J. Am. Soc. Nephrol. 2010, 21, 705–712. [Google Scholar] [CrossRef]
- Konstam, M.A.; Gheorghiade, M.; Burnett, J.C., Jr.; Grinfeld, L.; Maggioni, A.P.; Swedberg, K.; Udelson, J.E.; Zannad, F.; Cook, T.; Ouyang, J.; et al. Effects of oral tolvaptan in patients hospitalized for worsening heart failure: The EVEREST Outcome Trial. JAMA 2007, 297, 1319–1331. [Google Scholar]
- Hauptman, P.J.; Burnett, J.; Gheorgiade, M.; Grinfeld, L.; Konstam, M.A.; Kostic, D.; Krasa, K.B.; Maggioni, A.; Ouyang, J.; Swedberg, K.; et al. Clinical course of patients with hyponatremia and decompensated systolic heart failure and the effect of vasopressin receptor antagonism with tolvaptan. J. Card. Fail. 2013, 19, 390–397. [Google Scholar] [CrossRef]
- Chen, S.; Zhao, J.J.; Tong, N.W.; Guo, X.H.; Qui, M.C.; Yang, G.Y.; Liu, Z.M.; Ma, J.H.; Zhang, Z.W.; Gu, F.; et al. Randomized, double blinded, placebo-controlled trial to evaluate the efficacy and safety of tolvaptan in Chinese patients with hyponatremia caused by SIADH. J. Clin. Pharmacol. 2014. [Google Scholar] [CrossRef]
- Salahudeen, A.K.; Ali, N.; George, M.; Lahoti, A.; Palla, S. Tolvaptan in hospitalized cancer patients with hyponatraemia: A double-blind, randomized, placebo-controlled clinical trial on efficacy and safety. Cancer 2014, 120, 744–751. [Google Scholar]
- Roberts, H.; Khee, T.S.; Philp, I. Setting priorities for measures of performance for geriatric medical services. Age Ageing 1994, 23, 154–157. [Google Scholar]
- Dasta, J.F.; Chiong, J.R.; Christian, R.; Lin, J. Evaluation of costs associated with tolvaptan-mediated hospital length of stay reduction among US patients with the syndrome of inappropriate antidiuretic hormone secretion, based on SALT-1 and SALT-2 trials. Hosp. Pract. (1995) 2012, 40, 7–14. [Google Scholar]
- Shoaf, S.E.; Bramer, S.L.; Bricmont, P.; Zimmer, C.A. Pharmacokinetic and pharmacodynamic interaction between tolvaptan, a non-peptide AVP antagonist, and furosemide or hydrocholorothiazide. J. Cardiovasc. Pharmacol. 2007, 50, 213–222. [Google Scholar]
- Heinrich, S.; Rapp, K.; Rissmann, U.; Becker, C.; Konig, H.H. Cost of falls in old age: A systematic review. Osteoporos. Int. 2010, 21, 891–902. [Google Scholar] [CrossRef]
- Luengo-Fernande, R.; Leal, J.; Gray, A. Dementia 2010: The Economic Burden of Dementia and Associated Research in the United Kingdom; Alzheimer’s Research Trust: Oxford, UK, 2010. [Google Scholar]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Soiza, R.L.; Cumming, K.; Clarke, J.M.; Wood, K.M.; Myint, P.K. Hyponatremia: Special Considerations in Older Patients. J. Clin. Med. 2014, 3, 944-958. https://doi.org/10.3390/jcm3030944
Soiza RL, Cumming K, Clarke JM, Wood KM, Myint PK. Hyponatremia: Special Considerations in Older Patients. Journal of Clinical Medicine. 2014; 3(3):944-958. https://doi.org/10.3390/jcm3030944
Chicago/Turabian StyleSoiza, Roy L., Kirsten Cumming, Jennifer M. Clarke, Karen M. Wood, and Phyo K. Myint. 2014. "Hyponatremia: Special Considerations in Older Patients" Journal of Clinical Medicine 3, no. 3: 944-958. https://doi.org/10.3390/jcm3030944
APA StyleSoiza, R. L., Cumming, K., Clarke, J. M., Wood, K. M., & Myint, P. K. (2014). Hyponatremia: Special Considerations in Older Patients. Journal of Clinical Medicine, 3(3), 944-958. https://doi.org/10.3390/jcm3030944







