Investigation of the Medium- and Long-Term Results of a Pioneering Method in the Treatment of Geriatric Intertrochanteric Femur Fractures: Osteosynthesis Using the WALANT Technique
Abstract
1. Introduction
2. Materials and Methods
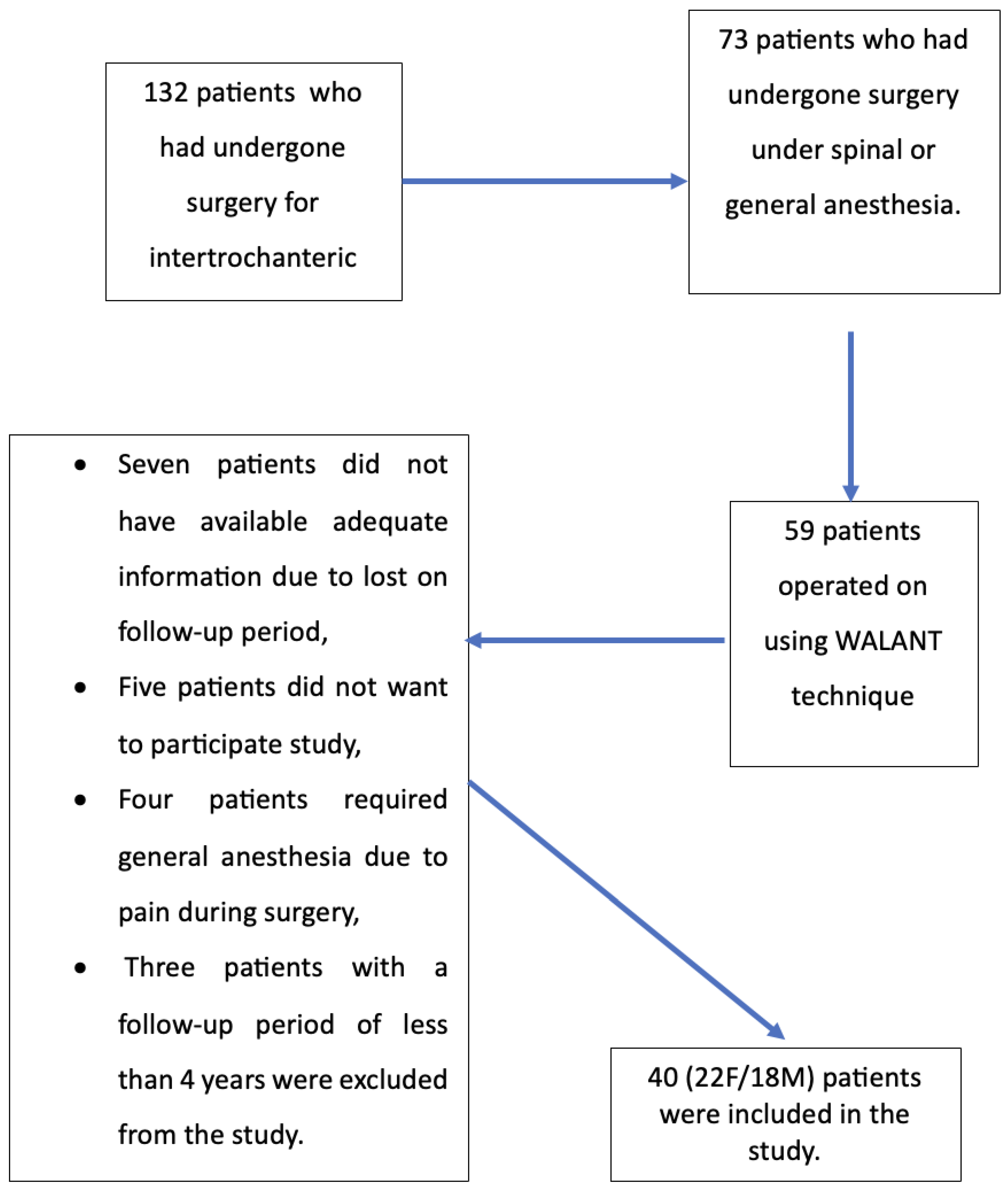
2.1. Study Design
2.2. Functional and Radiological Outcomes
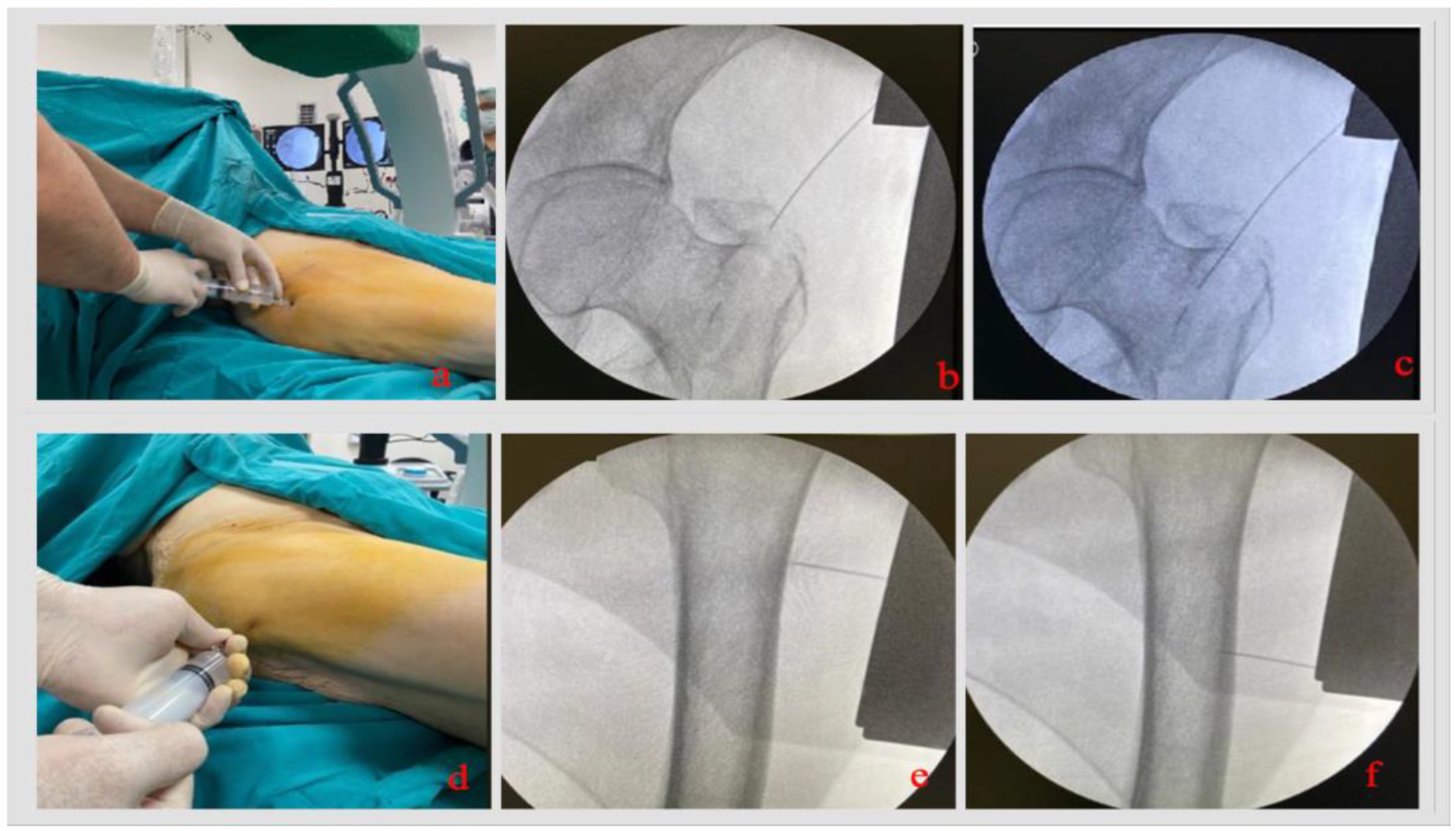
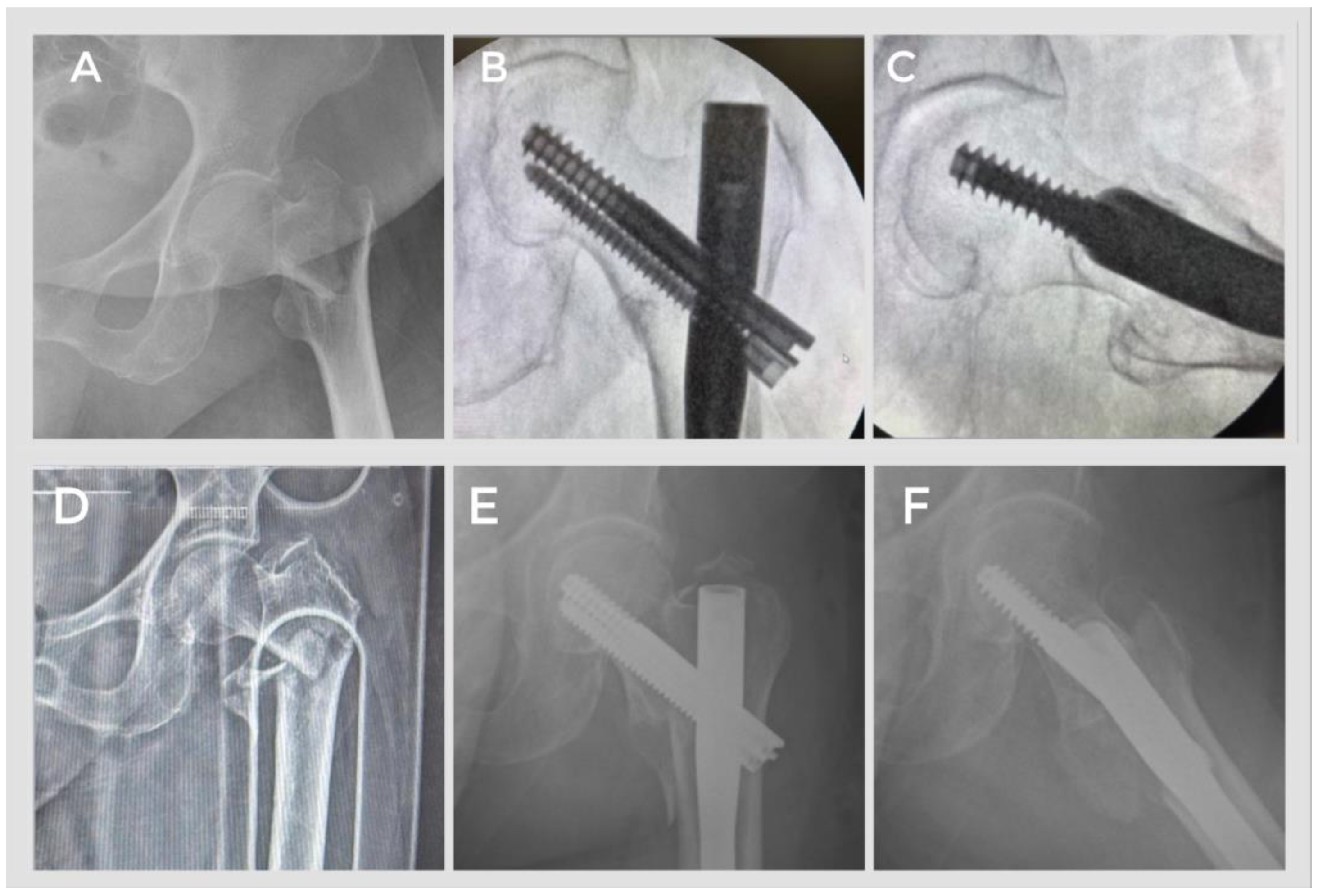
2.3. Surgical Technique
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| WALANT | Wide-awake Local Anesthesia No Tourniquet |
| PFN | Proximal femoral nail |
| HHS | Harris hip score |
| VAS | Visual analog scale |
| AO | Arbeitsgemeinschaft für Osteosynthesefragen |
| TAD | Tip–apex distance |
| AP | Anteroposterior |
| PENG | Pericapsular nerve group |
| S-FICB | Suprainguinal fascia iliaca compartment blockade |
References
- Berry, S.D.; Rothbaum, R.R.; Kiel, D.P.; Lee, Y.; Mitchell, S.L. Association of Clinical Outcomes with Surgical Repair of Hip Fracture vs Nonsurgical Management in Nursing Home Residents with Advanced Dementia. JAMA Intern. Med. 2018, 178, 774–780. [Google Scholar] [CrossRef]
- van de Ree, C.L.; Landers, M.J.; Kruithof, N.; de Munter, L.; Slaets, J.P.; Gosens, T.; de Jongh, M.A. Effect of Frailty on Quality of Life in Elderly Patients after Hip Fracture: A Longitudinal Study. BMJ Open 2019, 9, e025941. [Google Scholar] [CrossRef] [PubMed]
- Man, L.; Ho, A.W.; Wong, S. Excess Mortality for Operated Geriatric Hip Fracture in Hong Kong. Hong Kong Med. J. 2016, 22, 6–10. [Google Scholar] [CrossRef] [PubMed]
- Nijland, L.M.; Karres, J.; Simons, A.E.; Ultee, J.M.; Kerkhoffs, G.M.; Vrouenraets, B.C. The Weekend Effect for Hip Fracture Surgery. Injury 2017, 48, 1536–1541. [Google Scholar] [CrossRef]
- Barceló, M.; Torres, O.H.; Mascaró, J.; Casademont, J. Hip Fracture and Mortality: Study of Specific Causes of Death and Risk Factors. Arch. Osteoporos. 2021, 16, 15. [Google Scholar] [CrossRef]
- Borge, S.J.; Lauritzen, J.B.; Jørgensen, H.L. Hypoalbuminemia Is Associated with 30-Day Mortality in Hip Fracture Patients Independently of Body Mass Index. Scand. J. Clin. Lab. Investig. 2022, 82, 571–575. [Google Scholar] [CrossRef] [PubMed]
- Blanco, J.F.; da Casa, C.; Pablos-Hernández, C.; González-Ramírez, A.; Julián-Enríquez, J.M.; Díaz-Álvarez, A. 30-Day Mortality after Hip Fracture Surgery: Influence of Postoperative Factors. PLoS ONE 2021, 16, e0246963. [Google Scholar] [CrossRef]
- Pincus, D.; Ravi, B.; Wasserstein, D.; Huang, A.; Paterson, J.M.; Nathens, A.B.; Kreder, H.J.; Jenkinson, R.J.; Wodchis, W.P. Association between Wait Time and 30-Day Mortality in Adults Undergoing Hip Fracture Surgery. JAMA 2017, 318, 1994–2003. [Google Scholar] [CrossRef]
- Lizaur-Utrilla, A.; Gonzalez-Navarro, B.; Vizcaya-Moreno, M.F.; Lopez-Prats, F.A. Altered Seric Levels of Albumin, Sodium and Parathyroid Hormone May Predict Early Mortality Following Hip Fracture Surgery in Elderly. Int. Orthop. 2019, 43, 2825–2829. [Google Scholar] [CrossRef]
- Beaupre, L.; Khong, H.; Smith, C.; Kang, S.; Evens, L.; Jaiswal, P.; Powell, J. The Impact of Time to Surgery after Hip Fracture on Mortality at 30-and 90-Days: Does a Single Benchmark Apply to All? Injury 2019, 50, 950–955. [Google Scholar] [CrossRef]
- Bai, J.; Zhang, P.; Liang, X.; Wu, Z.; Wang, J.; Liang, Y. Association between Dementia and Mortality in the Elderly Patients Undergoing Hip Fracture Surgery: A Meta-Analysis. J. Orthop. Surg. Res. 2018, 13, 298. [Google Scholar] [CrossRef] [PubMed]
- Neuman, M.D.; Silber, J.H.; Magaziner, J.S.; Passarella, M.A.; Mehta, S.; Werner, R.M. Survival and Functional Outcomes after Hip Fracture among Nursing Home Residents. JAMA Intern. Med. 2014, 174, 1273–1280. [Google Scholar] [CrossRef] [PubMed]
- Gaumetou, E.; Zilber, S.; Hernigou, P. Non-Simultaneous Bilateral Hip Fracture: Epidemiologic Study of 241 Hip Fractures. Orthop. Traumatol. Surg. Res. 2011, 97, 22–27. [Google Scholar] [CrossRef]
- Aygün, Ü.; Şenocak, E.; Aksay, M.F.; Çiçek, A.C.; Halaç, O.; Toy, S. An Overview of Patients with Intertrochanteric Femoral Fractures Treated with Proximal Femoral Nail Fixation Using Important Criteria. BMC Musculoskelet. Disord. 2024, 25, 1051. [Google Scholar] [CrossRef]
- Takigami, I.; Matsumoto, K.; Ohara, A.; Yamanaka, K.; Naganawa, T.; Ohashi, M.; Date, K.; Shmizu, K. Treatment of Trochanteric Fractures with the PFNA (Proximal Femoral Nail Antirotation) Nail System. Bull. NYU Hosp. Jt. Dis. 2008, 66, 276–279. [Google Scholar]
- Hobday, D.; Welman, T.; O’Neill, N.; Pahal, G.S. A Protocol for Wide Awake Local Anaesthetic No Tourniquet (WALANT) Hand Surgery in the Context of the Coronavirus Disease 2019 (COVID-19) Pandemic. Surgeon 2020, 18, e67–e71. [Google Scholar] [CrossRef]
- Abd Hamid, M.H.; Abdullah, S.; Ahmad, A.A.; Singh, P.S.G.N.; Soh, E.Z.F.; Liu, C.Y.; Sapuan, J. A Randomized Controlled Trial Comparing Wide-Awake Local Anesthesia with No Tourniquet (WALANT) to General Anesthesia in Plating of Distal Radius Fractures with Pain and Anxiety Level Perception. Cureus 2021, 13, e12876. [Google Scholar] [CrossRef] [PubMed]
- Borg, T.; Tahir, M.; Heidari, N. 600 the Use of a Wide-Awake Local Anaesthesia No Tourniquet (WALANT) Technique in Foot and Ankle Procedures-a Randomised Control Trial. Br. J. Surg. 2021, 108, znab134.456. [Google Scholar] [CrossRef]
- Evangelista, T.M.P.; Pua, J.H.C.; Evangelista-Huber, M.T.P. Wide-Awake Local Anesthesia No Tourniquet (WALANT) versus Local or Intravenous Regional Anesthesia with Tourniquet in Atraumatic Hand Cases in Orthopedics: A Systematic Review and Meta-Analysis. J. Hand Surg. 2019, 24, 469–476. [Google Scholar] [CrossRef]
- Gunasagaran, J.; Sean, E.S.; Shivdas, S.; Amir, S.; Ahmad, T.S. Perceived Comfort during Minor Hand Surgeries with Wide Awake Local Anaesthesia No Tourniquet (WALANT) versus Local Anaesthesia (LA)/Tourniquet. J. Orthop. Surg. 2017, 25, 2309499017739499. [Google Scholar] [CrossRef]
- Li, Y.-S.; Chen, C.-Y.; Lin, K.-C.; Tarng, Y.-W.; Hsu, C.-J.; Chang, W.-N. Open Reduction and Internal Fixation of Ankle Fracture Using Wide-Awake Local Anaesthesia No Tourniquet Technique. Injury 2019, 50, 990–994. [Google Scholar] [CrossRef]
- O’Neill, N.; Abdall-Razak, A.; Norton, E.; Kumar, A.; Shah, H.; Khatkar, H.; Alsafi, Z.; Agha, R. Use of Wide-Awake Local Anaesthetic No Tourniquet (WALANT) in Upper Limb and Hand Surgery: A Systematic Review Protocol. Int. J. Surg. Protoc. 2020, 20, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Rhee, P.C.; Fischer, M.M.; Rhee, L.S.; McMillan, H.; Johnson, A.E. Cost Savings and Patient Experiences of a Clinic-Based, Wide-Awake Hand Surgery Program at a Military Medical Center: A Critical Analysis of the First 100 Procedures. J. Hand Surg. 2017, 42, e139–e147. [Google Scholar] [CrossRef] [PubMed]
- Tahir, M.; Chaudhry, E.A.; Ahmed, N.; Mamoon, A.H.; Ahmad, M.; Jamali, A.R.; Mehboob, G. Ankle Fracture Fixation with Use of WALANT (Wide Awake Local Anesthesia with No Tourniquet) Technique: An Attractive Alternative for the Austere Environment. J. Bone Jt. Surg. 2021, 103, 397–404. [Google Scholar]
- Baumgaertner, M.R.; Curtin, S.L.; Lindskog, D.M.; Keggi, J.M. The Value of the Tip-Apex Distance in Predicting Failure of Fixation of Peritrochanteric Fractures of the Hip. J. Bone Jt. Surg. 1995, 77, 1058–1064. [Google Scholar] [CrossRef]
- Hansen, T.B. Fast Track in Hip Arthroplasty. EFORT Open Rev. 2017, 2, 179–188. [Google Scholar] [CrossRef]
- Siu, A.L.; Penrod, J.D.; Boockvar, K.S.; Koval, K.; Strauss, E.; Morrison, R.S. Early Ambulation after Hip Fracture: Effects on Function and Mortality. Arch. Intern. Med. 2006, 166, 766–771. [Google Scholar] [CrossRef]
- Aprato, A.; Bechis, M.; Buzzone, M.; Bistolfi, A.; Daghino, W.; Massè, A. No Rest for Elderly Femur Fracture Patients: Early Surgery and Early Ambulation Decrease Mortality. J. Orthop. Traumatol. 2020, 21, 12. [Google Scholar] [CrossRef]
- Oldmeadow, L.B.; Edwards, E.R.; Kimmel, L.A.; Kipen, E.; Robertson, V.J.; Bailey, M.J. No Rest for the Wounded: Early Ambulation after Hip Surgery Accelerates Recovery. ANZ J. Surg. 2006, 76, 607–611. [Google Scholar] [CrossRef] [PubMed]
- Kalashetty, M.B.; Channappagoudar, R.; Alwandikar, V.; Naik, D.L.; Hulakund, S.; Guddad, A. Comparison of Pericapsular Nerve Group Block with Fascia Iliaca Compartment Block in Adult Patients Undergoing Hip Surgeries: A Double-Blinded Randomized Control Study. Anesth. Essays Res. 2022, 16, 397–401. [Google Scholar] [CrossRef]
- Tang, L.; Fang, P.; Fang, Y.; Lu, Y.; Xu, G.; Liu, X. Comparison of Effects between Combined Lumbar-Sacral Plexus Block plus General Anesthesia and Unilateral Spinal Anesthesia in Elderly Patients Undergoing Hip Fracture Surgery: A Pilot Randomized Controlled Trial. Evid. Based Complement. Altern. Med. 2021, 2021, 6685497. [Google Scholar] [CrossRef] [PubMed]
- Tosounidis, T.H.; Sheikh, H.; Stone, M.H.; Giannoudis, P.V. Pain Relief Management Following Proximal Femoral Fractures: Options, Issues and Controversies. Injury 2015, 46, S52–S58. [Google Scholar] [CrossRef]
- Girón-Arango, L.; Peng, P.W.; Chin, K.J.; Brull, R.; Perlas, A. Pericapsular Nerve Group (PENG) Block for Hip Fracture. Reg. Anesth. Pain Med. 2018, 43, 859–863. [Google Scholar] [CrossRef]
- Morrison, C.; Brown, B.; Lin, D.-Y.; Jaarsma, R.; Kroon, H. Analgesia and Anesthesia Using the Pericapsular Nerve Group Block in Hip Surgery and Hip Fracture: A Scoping Review. Reg. Anesth. Pain Med. 2021, 46, 169–175. [Google Scholar] [CrossRef]
- Fusco, P.; Di Carlo, S.; Paladini, G.; Scimia, P.; Di Martino, E.; Marinangeli, F.; Petrucci, E. Could the Combination of PENG Block and LIA Be a Useful Analgesic Strategy in the Treatment of Postoperative Pain for Hip Replacement Surgery? Reg. Anesth. Pain Med. 2019, online ahead of print, rapm-2018-100277. [Google Scholar] [CrossRef] [PubMed]
- Reza, P.C.; García, P.D.; Vázquez, M.G.; Rodríguez, L.S.; Álvarez, S.L. Pericapsular Nerve Group Block for Hip Surgery. Minerva Anestesiol. 2020, 86, 463–465. [Google Scholar] [CrossRef] [PubMed]
- Tüzün, H.Y.; Bilekli, A.B.; Erşen, Ö. The Factors That Affect Blood Loss in Intertrochanteric Fractures Treated with Proximal Femoral Nail in the Elderly. Eur. J. Trauma Emerg. Surg. 2022, 48, 1879–1884. [Google Scholar] [CrossRef]
- Mattisson, L.; Lapidus, L.J.; Enocson, A. What Is the Influence of a Delay to Surgery >24 Hours on the Rate of Red Blood Cell Transfusion in Elderly Patients With Intertrochanteric or Subtrochanteric Hip Fractures Treated With Cephalomedullary Nails? J. Orthop. Trauma 2018, 32, 403–407. [Google Scholar] [CrossRef]
| n | % | ||
|---|---|---|---|
| Gender | Female | 22 | 55 |
| Male | 18 | 45 | |
| Injured extremity | Right | 21 | 52.5 |
| Left | 19 | 47.5 | |
| Fracture type | 31A1 | 15 | 37.5 |
| 31A2 | 17 | 42.5 | |
| 31A3 | 8 | 20 | |
| Reduction quality | Good | 27 | 67.5 |
| Acceptable | 11 | 27.5 | |
| Poor | 2 | 5 | |
| Comorbid diseases | None | 8 | 20 |
| Hypertension | 32 | 80 | |
| Diabetes mellitus | 13 | 32.5 | |
| Cardiac disease | 12 | 30 | |
| Chronic lung disease | 14 | 35 | |
| Sixth-Month Control | Last Follow-Up | p | |
|---|---|---|---|
| Harris Hip Score | 73.3 ± 3.2 | 74.9 ± 2.5 | 0.288 |
| Pain severity | 32.2 ± 1.8 | 33.7 ± 1.8 | 0.337 |
| Function | 34.3 ± 2.1 | 34.1 ± 1.9 | 0.449 |
| Absence of deformity | 3.1 ± 0.5 | 3.1 ± 0.5 | 0.573 |
| Range of motion | 3.7 ± 0.8 | 3.7 ± 0.7 | 0.573 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Altun, Y.M.; Gedikbaş, M.; Aşçı, M. Investigation of the Medium- and Long-Term Results of a Pioneering Method in the Treatment of Geriatric Intertrochanteric Femur Fractures: Osteosynthesis Using the WALANT Technique. J. Clin. Med. 2025, 14, 6078. https://doi.org/10.3390/jcm14176078
Altun YM, Gedikbaş M, Aşçı M. Investigation of the Medium- and Long-Term Results of a Pioneering Method in the Treatment of Geriatric Intertrochanteric Femur Fractures: Osteosynthesis Using the WALANT Technique. Journal of Clinical Medicine. 2025; 14(17):6078. https://doi.org/10.3390/jcm14176078
Chicago/Turabian StyleAltun, Yusuf Murat, Mete Gedikbaş, and Murat Aşçı. 2025. "Investigation of the Medium- and Long-Term Results of a Pioneering Method in the Treatment of Geriatric Intertrochanteric Femur Fractures: Osteosynthesis Using the WALANT Technique" Journal of Clinical Medicine 14, no. 17: 6078. https://doi.org/10.3390/jcm14176078
APA StyleAltun, Y. M., Gedikbaş, M., & Aşçı, M. (2025). Investigation of the Medium- and Long-Term Results of a Pioneering Method in the Treatment of Geriatric Intertrochanteric Femur Fractures: Osteosynthesis Using the WALANT Technique. Journal of Clinical Medicine, 14(17), 6078. https://doi.org/10.3390/jcm14176078






